Altered Neural Activity Associated with Mindfulness during Nociception: A Systematic Review of Functional MRI
Abstract
:1. Introduction
2. Materials and Methods
2.1. Literature Search and Selection Criteria
2.2. Data Extraction and Synthesis
2.3. Assessment of Study Consistency
3. Results
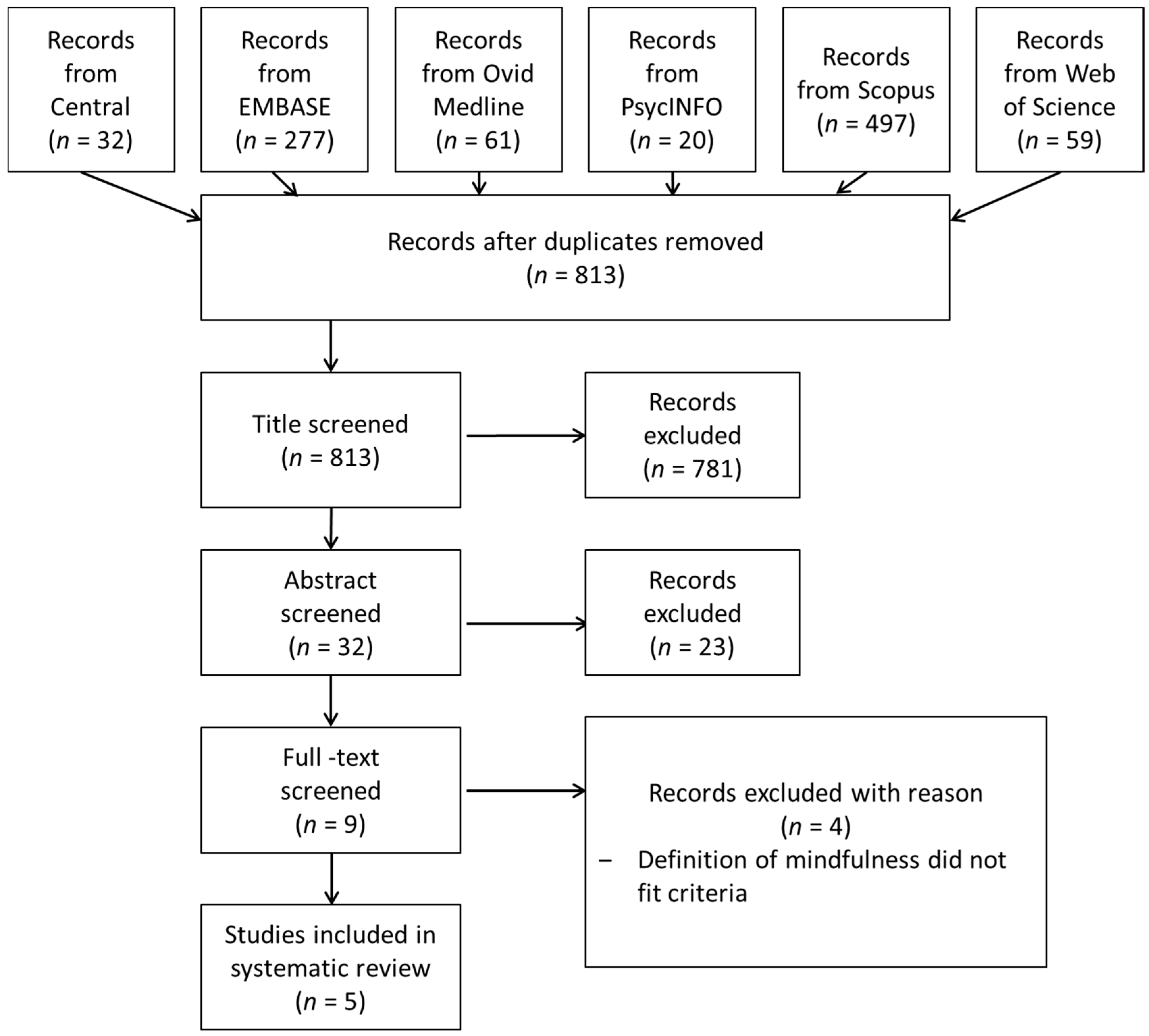
3.1. Identification of Studies
3.2. Details of Included Studies
3.3. Behavioural Data
3.4. Neural Activity
3.4.1. Identification of Neural Activity
3.4.2. Trends in General Pain and Pain Intensity
3.4.3. Anticipation of Pain and Mindfulness
3.4.4. Unpleasantness of Pain and Mindfulness
3.5. Study Consistency
4. Discussions
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| ACC | anterior cingulate cortex |
| ATB | attention to breath |
| CEN | central executive network |
| dlPFC | dorsolateral prefrontal cortex |
| FA | focused attention |
| FMI | Freiburg Mindfulness Inventory |
| fMRI | functional Magnetic Resonance Imaging |
| MCC | midcingulate cortex |
| OP | open presence |
| PET | Positron Emission Tomography |
| SI | primary somatosensory cortex |
| SII | secondary somatosensory cortex |
| SN | salience network |
References
- Merskey, H.; Bogduk, N. IASP Taxonomy; IASP Press: Seattle, WS, USA, 1994. [Google Scholar]
- Melzack, R.; Casey, K.L. The Skin Senses; Charles C Thomas: Springfield, IL, USA, 1968. [Google Scholar]
- Rainville, P.; Duncan, G.H.; Price, D.D.; Carrier, B.; Bushnell, M.C. Pain affect encoded in human anterior cingulate but not somatosensory cortex. Science 1997, 277, 968–971. [Google Scholar] [CrossRef] [PubMed]
- Friebel, U.; Eickhoff, S.B.; Lotze, M. Coordinate-based meta-analysis of experimentally induced and chronic persistent neuropathic pain. NeuroImage 2001, 58, 1070–1080. [Google Scholar] [CrossRef] [PubMed]
- Wager, T.D.; Rilling, J.K.; Smith, E.E.; Sokolik, A.; Casey, K.L.; Davidson, R.J.; Kosslyn, S.M.; Rose, R.M.; Cohen, J.D. Placebo-induced changes in FMRI in the anticipation and experience of pain. Science 2004, 303, 1162–1167. [Google Scholar] [CrossRef] [PubMed]
- Peyron, R.; Laurent, B.; Garcia-Larrea, L. Functional imaging of brain responses to pain. A review and meta-analysis (2000). Neurophysiol. Clin. 2000, 30, 263–288. [Google Scholar] [CrossRef]
- Tolle, T.R.; Kaufmann, T.; Siessmeier, T.; Lautenbacher, S.; Berthele, A.; Munz, F.; Willoch, F.; Schwaiger, M.; Conrad, B.; Bartenstein, P.; et al. Region-specific encoding of sensory and affective components of pain in the human brain: A positron emission tomography correlation analysis. Ann. Neurol. 1999, 45, 40–47. [Google Scholar] [CrossRef]
- Gard, T.; Hoelzel, B.K.; Sack, A.T.; Hempel, H.; Lazar, S.W.; Vaitl, D.; Ott, U. Pain attenuation through mindfulness is associated with decreased cognitive control and increased sensory processing in the brain. Cereb. Cortex 2012, 22, 2692–2702. [Google Scholar] [CrossRef] [PubMed]
- Lutz, A.; McFarlin, D.R.; Perlman, D.M.; Salomons, T.V.; Davidson, R.J. Altered anterior insula activation during anticipation and experience of painful stimuli in expert meditators. NeuroImage 2013, 64, 538–546. [Google Scholar] [CrossRef] [PubMed]
- Brown, C.A.; Jones, A.K.P. Meditation experience predicts less negative appraisal of pain: Electrophysiological evidence for the involvement of anticipatory neural responses. Pain 2010, 150, 428–438. [Google Scholar] [CrossRef] [PubMed]
- Zeidan, F.; Martucci, K.T.; Kraft, R.A.; Gordon, N.S.; McHaffie, J.G.; Coghill, R.C. Brain mechanisms supporting the modulation of pain by mindfulness meditation. J. Neurosci. 2011, 31, 5540–5548. [Google Scholar] [CrossRef] [PubMed]
- Zeidan, F.; Emerson, N.M.; Farris, S.R.; Ray, J.N.; Jung, Y.; McHaffie, J.G.; Coghill, R.C. Mindfulness meditation-based pain relief employs different neural mechanisms than placebo and sham mindfulness meditation-induced analgesia. J. Neurosci. 2015, 35, 15307–15325. [Google Scholar] [CrossRef] [PubMed]
- Perlman, D.M.; Salomons, T.V.; Davidson, R.J.; Lutz, A. Differential Effects on Pain Intensity and Unpleasantness of Two Meditation Practices. Emotion 2010, 10, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Grant, J.A.; Rainville, P. Pain sensitivity and analgesic effects of mindful states in zen meditators: A cross-sectional study. Psychosom. Med. 2009, 71, 106–114. [Google Scholar] [CrossRef] [PubMed]
- Brown, K.W.; Ryan, R.M. The benefits of being present: Mindfulness and its role in psychological well-being. J. Pers. Soc. Psychol. 2003, 84, 822–848. [Google Scholar] [CrossRef] [PubMed]
- Kabat-Zinn, J. Mindfulness-based interventions in context: Past, present, and future. Clin. Psychol. Sci. Pract. 2003, 10, 144–156. [Google Scholar] [CrossRef]
- Germer, C.K.; Neff, K.D. Self-compassion in clinical practice. J. Clin. Psychol. 2013, 69, 856–867. [Google Scholar] [CrossRef] [PubMed]
- Neff, K.D.; Germer, C.K. A pilot study and randomized controlled trial of the mindful self-compassion program. J. Clin. Psychol. 2013, 69, 28–44. [Google Scholar] [CrossRef] [PubMed]
- Luders, E.; Toga, A.W.; Lepore, N.; Gaser, C. The underlying anatomical correlates of long-term meditation: Larger hippocampal and frontal volumes of gray matter. NeuroImage 2009, 45, 672–678. [Google Scholar] [CrossRef] [PubMed]
- Lazar, S.W.; Kerr, C.E.; Wasserman, R.H.; Gray, J.R.; Greve, D.N.; Treadway, M.T.; McGarvey, M.; Quinn, B.T.; Dusek, J.A.; Benson, H.; et al. Meditation experience is associated with increased cortical thickness. Neuroreport 2005, 16, 1893–1897. [Google Scholar] [CrossRef] [PubMed]
- Lu, H.; Song, Y.; Xu, M.; Wang, X.; Li, X.; Liu, J. The brain structure correlates of individual differences in trait mindfulness: A voxel-based morphometry study. Neuroscience 2014, 272, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Taylor, V.A.; Daneault, V.; Grant, J.; Scavone, G.; Breton, E.; Roffe-Vidal, S.; Courtemanche, J.; Lavarenne, A.S.; Marrelec, G.; Benali, H.; et al. Impact of meditation training on the default mode network during a restful state. Soc. Cogn. Affect. Neurosci. 2013, 8, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Grant, J.A.; Courtemanche, J.; Rainville, P. A non-elaborative mental stance and decoupling of executive and pain-related cortices predicts low pain sensitivity in Zen meditators. Pain 2011, 152, 150–156. [Google Scholar] [CrossRef] [PubMed]
- Walach, H.; Buchheld, N.; Buttenmüller, V.; Kleinknecht, N.; Schmidt, S. Measuring mindfulness—The Freiburg Mindfulness Inventory (FMI). Personal. Individ. Differ. 2006, 40, 1543–1555. [Google Scholar] [CrossRef]
- Bressler, S.L.; Menon, V. Large-scale brain networks in cognition: Emerging methods and principles. Trends Cogn. Sci. 2010, 14, 277–290. [Google Scholar] [CrossRef] [PubMed]
- Rosazza, C.; Minati, L. Resting-state brain networks: Literature review and clinical applications. Neurol. Sci. 2011, 32, 773–785. [Google Scholar] [CrossRef] [PubMed]
- Bunge, S.A.; Ochsner, K.N.; Desmond, J.E.; Glover, G.H.; Gabrieli, J.D.E. Prefrontal regions involved in keeping information in and out of mind. Brain 2001, 124, 2074–2086. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, J.; Minoshima, S.; Casey, K.L. Keeping pain out of mind: The role of the dorsolateral prefrontal cortex in pain modulation. Brain 2003, 126, 1079–1091. [Google Scholar] [CrossRef] [PubMed]
- Wiech, K.; Ploner, M.; Tracey, I. Neurocognitive aspects of pain perception. Trends Cogn. Sci. 2008, 12, 306–313. [Google Scholar] [CrossRef] [PubMed]
- Menon, V. Salience Network. In Brain Mapping: An Encyclopedic Reference; Toga, A.W., Ed.; Academic Press: Waltham, MA, USA, 2015; Volume 2, pp. 597–611. [Google Scholar]
- Reiner, K.; Tibi, L.; Lipsitz, J.D. Do mindfulness-based interventions reduce pain intensity? A critical review of the literature. Pain Med. 2013, 14, 230–242. [Google Scholar] [CrossRef] [PubMed]
- Iannetti, G.D.; Mouraux, A. From the neuromatrix to the pain matrix (and back). Exp. Brain Res. 2010, 205, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Menon, V.; Uddin, L.Q. Saliency, switching, attention and control: A network model of insula function. Brain Struct. Funct. 2010, 214, 655–667. [Google Scholar] [CrossRef] [PubMed]
- Curtis, C.E.; D’Esposito, M. Persistent activity in the prefrontal cortex during working memory. Trends Cogn. Sci. 2003, 7, 415–423. [Google Scholar] [CrossRef]
- Jeurissen, D.; Sack, A.T.; Roebroeck, A.; Russ, B.E.; Pascual-Leone, A. TMS affects moral judgment, showing the role of DLPFC and TPJ in cognitive and emotional processing. Front. Neurosci. 2014, 8, 18. [Google Scholar] [CrossRef] [PubMed]
- Shackman, A.J.; McMenamin, B.W.; Maxwell, J.S.; Greischar, L.L.; Davidson, R.J. Right dorsolateral prefrontal cortical activity and behavioral inhibition. Psychol. Sci. (Wiley-Blackwell) 2009, 20, 1500–1506. [Google Scholar] [CrossRef] [PubMed]
- Emmert, K.; Kopel, R.; Sulzer, J.; Brühl, A.B.; Berman, B.D.; Linden, D.E.J.; Horovitzh, S.G.; Breimhorsti, M.; Cariaj, A.; Frank, S.; et al. Meta-analysis of real-time fMRI neurofeedback studies using individual participant data: How is brain regulation mediated? NeuroImage 2016, 124, 806–812. [Google Scholar] [CrossRef] [PubMed]
- Kabat-Zinn, J. An outpatient program in behavioral medicine for chronic pain patients based on the practice of mindfulness meditation: Theoretical considerations and preliminary results. Gen. Hosp. Psychiatry 1982, 4, 33–47. [Google Scholar] [CrossRef]
- Kabat-Zinn, J.; Lipworth, L.; Burney, R. The clinical use of mindfulness meditation for the self-regulation of chronic pain. J. Behav. Med. 1985, 8, 163–190. [Google Scholar] [CrossRef] [PubMed]
- Brown, C.A.; Jones, A.K.P. Psychobiological correlates of improved mental health in patients with musculoskeletal pain after a mindfulness-based pain management program. Clin. J. Pain 2013, 29, 233–244. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.; Lu, H.; Chen, H.; Geng, G.; Wang, J. Mindfulness intervention in the management of chronic pain and psychological comorbidity: A meta-analysis. Int. J. Nurs. Sci. 2014, 1, 215–223. [Google Scholar] [CrossRef]
- La Cour, P.; Petersen, M. Effects of mindfulness meditation on chronic pain: A randomized controlled trial. Pain Med. 2015, 16, 641–652. [Google Scholar] [CrossRef] [PubMed]
- Nakata, H.; Sakamoto, K.; Kakigi, R. Meditation reduces pain-related neural activity in the anterior cingulate cortex, insula, secondary somatosensory cortex, and thalamus. Front. Psychol. 2014, 5. [Google Scholar] [CrossRef] [PubMed]
| First Author (Year) | Population | (NM/NC) 1 | Training | Mindfulness Measure 2 | Stimulus (Time) 3 | Initial Pain Ratings 4 | Stimulation Region |
|---|---|---|---|---|---|---|---|
| Gard (2012) [8] | Mindfulness Practitioners | NM = 17 NC = 17 | Vispassana | FMI | Elec: 103+ V, 833 Hz (0.1 s) | I: ~4.6/10 U: ~4.4/10 A: ~3.1/10 | Left lower arm |
| Grant (2011) [23] | Meditation Practitioners | NM = 13 NC = 13 | Zen Mediation | Years of practice | Therm: Av. Zen 49.9 °C Av. Cntrl 47.9 °C (10 s) | I: 6–7/10 | Lateral, posterior left calf |
| Lutz (2013) [9] | Meditation Practitioners | NM = 14 NC = 14 | Nyingma, Kagyu | >10,000 h of training | Therm: Av. 48.1 °C (10 s) | P: 8/10 | Inside of left forearm |
| Zeidan (2011) [11] | Healthy Controls | NC = 15 | 4 days of training | FMI | Therm: 49 °C (12 s) | I: 4.8/10 U: 4.8/10 | Posterior right calf |
| Zeidan (2015) [12] | Healthy Controls | NC = 75 | 4 days of training | FMI | Therm: 49 °C (12 s) | I: 4.8/10 U: 5/10 | Posterior right calf |
| Brain Regions | Pain Dimension | Author | Contrast | Component | t-Value/Z Score (p-Value) |
|---|---|---|---|---|---|
| Anterior Cingulate Cortex | |||||
| General | Lutz | Mf > H | Anterior Middle | t = 3.9 (p > 0.005) | |
| General | Grant | Mf > H | Dorsal | t = 3.64 (p > 0.001) | |
| Intensity | Grant | Mf > H | Dorsal | t = 2.22 (p = 0.04) | |
| Intensity | Zeidan (2011) | Mf > H | Anterior | Z = 5.35 Z = 5.30 Z = 5.29 | |
| Intensity | Zeidan (2015) | Mf > H | Subgenual | Z = 5.61 | |
| Anticipation | Lutz | Mf > H | Bilateral | t = 3.1 (p < 0.005) t = −4 (p < 0.0005) | |
| Anticipation 1 | Gard | Mf > H | Rostral/VM/mFG | t = 2.8 (p = 0.009) | |
| Insula | |||||
| General | Grant | Mf > H | Posterior/Thalamus/BG | t = 3.61 (p > 0.001) t = 4.61 (p > 0.001) | |
| General | Lutz | Mf > H | Anterior | t = 3.4 (p < 0.005) | |
| Intensity | Grant | Mf > H | Anterior Middle/iFG/Thalamus/BG | t = 2.44 (p = 0.02) t = 2.46 (p = 0.02) t = 2.98 (p = 0.007) t = 3.29 (p = 0.003) | |
| Intensity | Zeidan (2011) | Mf > H | Anterior | Z = 3.04 | |
| Intensity | Zeidan (2015) | Mf > H | Anterior | Z = 4.05 | |
| Anticipation Unpleasantness | Lutz | Mf > H | Anterior Posterior | t = −3.8 (p < 0.005) t = −4.5 (p < 0.0005) | |
| Unpleasantness | Zeidan (2011) | Mf > H | Anterior | Z = 2.73 | |
| Unpleasantness 2 | Gard | Mf > H | /Somatosensory | t = 3.59 (p = 0.001) | |
| Somatosensory I | |||||
| General | Zeidan (2015) | Mf > H | Z = 3.07 | ||
| Somatosensory II | |||||
| General | Grant | Mf > H | /Parietal Operculum | t = 4.39 (p < 0.001) | |
| Unpleasantness 2 | Gard | Mf > H | /Insula | t = 3.59 (p = 0.001) | |
| Prefrontal Cortex | |||||
| General | Gard | H > Mf | Lateral/mFG | t = 4.03 (p < 0.001) t = 3.87 (p < 0.001) | |
| General | Zeidan (2015) | H > Mf | Dorsolateral | Z = 4.10 Z = 3.82 Z = 4.65 | |
| Intensity | Grant | H > Mf | Dorsolateral | t = 2.22 (p = 0.04) t = 2.84 (p = 0.009) t = 3.54 (p = 0.002) | |
| Anticipation 1 | Gard | Mf > H | VM/mFG/rACC | t = 2.8 (p = 0.009) | |
| Thalamus | |||||
| General | Grant | Mf > H | /BG/Insula | t = 4.61 (p > 0.001) | |
| Intensity | /BG/Insula | t = 3.29 (p = 0.003) | |||
| Unpleasantness | Zeidan (2011) | H > Mf | Z = 6.74 Z = 3.12 | ||
| General | Zeidan (2015) | H > Mf | Z = 5.75 Z = 4.63 | ||
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bilevicius, E.; Kolesar, T.A.; Kornelsen, J. Altered Neural Activity Associated with Mindfulness during Nociception: A Systematic Review of Functional MRI. Brain Sci. 2016, 6, 14. https://doi.org/10.3390/brainsci6020014
Bilevicius E, Kolesar TA, Kornelsen J. Altered Neural Activity Associated with Mindfulness during Nociception: A Systematic Review of Functional MRI. Brain Sciences. 2016; 6(2):14. https://doi.org/10.3390/brainsci6020014
Chicago/Turabian StyleBilevicius, Elena, Tiffany A. Kolesar, and Jennifer Kornelsen. 2016. "Altered Neural Activity Associated with Mindfulness during Nociception: A Systematic Review of Functional MRI" Brain Sciences 6, no. 2: 14. https://doi.org/10.3390/brainsci6020014
APA StyleBilevicius, E., Kolesar, T. A., & Kornelsen, J. (2016). Altered Neural Activity Associated with Mindfulness during Nociception: A Systematic Review of Functional MRI. Brain Sciences, 6(2), 14. https://doi.org/10.3390/brainsci6020014





