Gaze-Contingent Eye-Tracking Training in Brain Disorders: A Systematic Review
Abstract
:1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Information Sources
2.3. Search Strategy
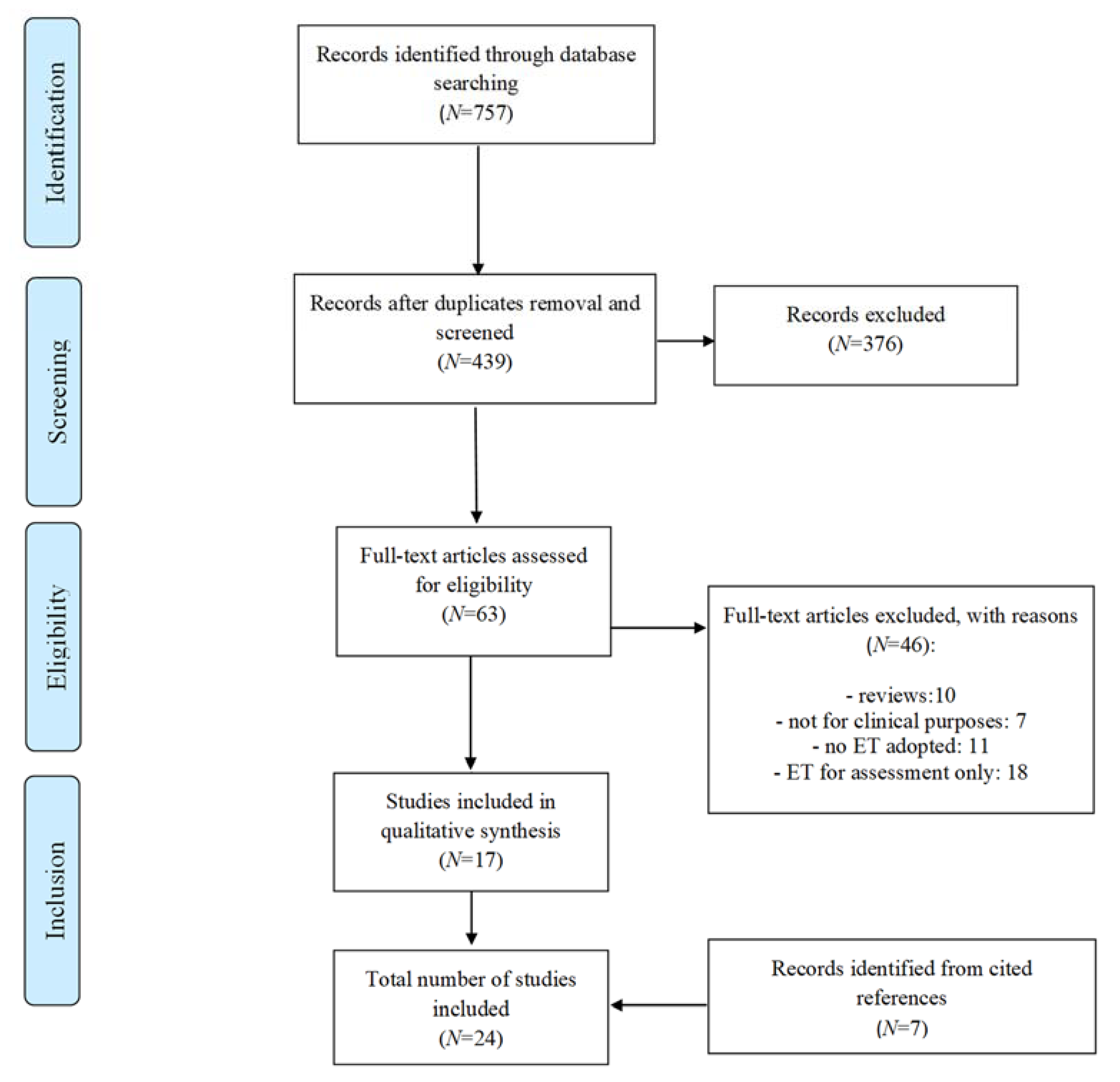
2.4. Study Selection
2.5. Data Collection Process
2.6. Quality Assessment and Risk of Bias
3. Results
3.1. Neurodevelopmental Conditions
3.2. Psychiatric Conditions
3.3. Neurological Conditions
3.4. Risk of Bias
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Poletti, B.; Carelli, L.; Solca, F.; Lafronza, A.; Pedroli, E.; Faini, A.; Ticozzi, N.; Ciammola, A.; Meriggi, P.; Cipresso, P.; et al. An eye-tracker controlled cognitive battery: Overcoming verbal-motor limitations in ALS. J. Neurol. 2017, 264, 1136–1145. [Google Scholar] [CrossRef] [PubMed]
- Poletti, B.; Carelli, L.; Solca, F.; Lafronza, A.; Pedroli, E.; Faini, A.; Zago, S.; Ticozzi, N.; Ciammola, A.; Morelli, C.; et al. An eye-tracking controlled neuropsychological battery for cognitive assessment in neurological diseases. Neurol. Sci. 2017, 38, 595–603. [Google Scholar] [CrossRef] [PubMed]
- Poletti, B.; Carelli, L.; Faini, A.; Solca, F.; Meriggi, P.; Lafronza, A.; Ciringione, L.; Pedroli, E.; Ticozzi, N.; Ciammola, A.; et al. The arrows and colors cognitive test (ACCT): A new verbal-motor free cognitive measure for executive functions in ALS. PLoS ONE 2018, 13, e0200953. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tao, L.; Wang, Q.; Liu, D.; Wang, J.; Zhu, Z.; Feng, L. Eye tracking metrics to screen and assess cognitive impairment in patients with neurological disorders. Neurol. Sci. 2020, 41, 1697–1704. [Google Scholar] [CrossRef]
- MacAskill, M.R.; Anderson, T.J. Eye movements in neurodegenerative diseases. Curr. Opin. Neurol. 2016, 29, 61–68. [Google Scholar] [CrossRef] [Green Version]
- Donaghy, C.; Pinnock, R.; Abrahams, S.; Cardwell, C.; Hardiman, O.; Patterson, V.; McGivern, R.C.; Gibson, J.M. Ocular fixation instabilities in motor neurone disease. A marker of frontal lobe dysfunction? J. Neurol. 2009, 256, 420–426. [Google Scholar] [CrossRef]
- Donaghy, C.; Thurtell, M.J.; Pioro, E.P.; Gibson, J.M.; Leigh, R.J. Eye movements in amyotrophic lateral sclerosis and its mimics: A review with illustrative cases. J. Neurol. Neurosurg. Psychiatry 2011, 82, 110–116. [Google Scholar] [CrossRef]
- Poletti, B.; Solca, F.; Carelli, L.; Diena, A.; Colombo, E.; Torre, S.; Maranzano, A.; Greco, L.; Cozza, F.; Lizio, A.; et al. Association of clinically evident eye movement abnormalities with motor and cognitive features in patients with motor neuron disorders. Neurology 2021, 97, e1835–e1846. [Google Scholar] [CrossRef]
- Ewenczyk, C.; Mesmoudi, S.; Gallea, C.; Welter, M.L.; Gaymard, B.; Demain, A.; Yahia Cherif, L.; Degos, B.; Benali, H.; Pouget, P.; et al. Antisaccades in Parkinson disease: A new marker of postural control? Neurology 2017, 88, 853–861. [Google Scholar] [CrossRef]
- Nemanich, S.T.; Earhart, G.M. Freezing of gait is associated with increased saccade latency and variability in Parkinson’s disease. Clin. Neurophysiol. 2016, 127, 2394–2401. [Google Scholar] [CrossRef] [Green Version]
- Golding, C.V.; Danchaivijitr, C.; Hodgson, T.L.; Tabrizi, S.J.; Kennard, C. Identification of an oculomotor biomarker of preclinical Huntington disease. Neurology 2006, 67, 485–487. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.S.; Jankovic, J.; Hood, A.J.; Jeter, C.B.; Sereno, A.B. Reflexive and volitional saccades: Biomarkers of Huntington disease severity and progression. J. Neurol. Sci. 2012, 313, 35–41. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jaafari, N.; Rigalleau, F.; Rachid, F.; Delamillieure, P.; Millet, B.; Olié, J.P.; Gil, R.; Rotge, J.Y.; Vibert, N. A critical review of the contribution of eye movement recordings to the neuropsychology of obsessive compulsive disorder. Acta Psychiatr. Scand. 2011, 124, 87–101. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, N.; Laurent, E.; Noiret, N.; Chopard, G.; Haffen, E.; Bennabi, D.; Vandel, P. Eye movement in unipolar and bipolar depression: A systematic review of the literature. Front. Psychol. 2015, 6, 1809. [Google Scholar] [CrossRef] [Green Version]
- Morita, K.; Miura, K.; Kasai, K.; Hashimoto, R. Eye movement characteristics in schizophrenia: A recent update with clinical implications. Neuropsychopharmacol. Rep. 2020, 40, 2–9. [Google Scholar] [CrossRef] [Green Version]
- Bittencourt, J.; Velasques, B.; Teixeira, S.; Basile, L.F.; Salles, J.I.; Nardi, A.E.; Budde, H.; Cagy, M.; Piedade, R.; Ribeiro, P. Saccadic eye movement applications for psychiatric disorders. Neuropsychiatr. Dis. Treat. 2013, 9, 1393–1409. [Google Scholar] [CrossRef] [Green Version]
- Sweeney, J.A.; Takarae, Y.; Macmillan, C.; Luna, B.; Minshew, N.J. Eye movements in neurodevelopmental disorders. Curr. Opin. Neurol. 2004, 17, 37–42. [Google Scholar] [CrossRef]
- Canu, D.; Ioannou, C.; Müller, K.; Martin, B.; Fleischhaker, C.; Biscaldi, M.; Beauducel, A.; Smyrnis, N.; van Elst, L.T.; Klein, C. Visual search in neurodevelopmental disorders: Evidence towards a continuum of impairment. Eur. Child Adolesc. Psychiatry 2021, 1–18. [Google Scholar] [CrossRef]
- Suslow, T.; Hußlack, A.; Kersting, A.; Bodenschatz, C.M. Attentional biases to emotional information in clinical depression: A systematic and meta-analytic review of eye tracking findings. J. Affect. Disord. 2020, 274, 632–642. [Google Scholar] [CrossRef]
- Lima, L.K.S.D.; Assis, E.D.B.D.; Torro, N. Facial expressions and eye tracking in individuals with social anxiety disorder: A systematic review. Psicol. Reflex. Crít. 2019, 32, 9. [Google Scholar]
- Gunther, K.E.; Brown, K.M.; Fu, X.; MacNeill, L.; Jones, M.; Ermanni, B.; Pérez-Edgar, K. Mobile eye tracking captures changes in attention over time during a naturalistic threat paradigm in behaviorally inhibited children. Affect. Sci. 2021, 2, 495–505. [Google Scholar] [CrossRef] [PubMed]
- Crawford, H.; Moss, J.; Oliver, C.; Elliott, N.; Anderson, G.M.; McCleery, J.P. Visual preference for social stimuli in individuals with autism or neurodevelopmental disorders: An eye-tracking study. Mol. Autism 2016, 7, 1–12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Skaramagkas, V.; Giannakakis, G.; Ktistakis, E.; Manousos, D.; Karatzanis, I.; Tachos, N.; Tripoliti, E.E.; Marias, K.; Fotiadis, D.I.; Tsiknakis, M. Review of eye tracking metrics involved in emotional and cognitive processes. IEEE Rev. Biomed. Eng. 2021. [Google Scholar] [CrossRef] [PubMed]
- McConkie, G.W.; Rayner, K. The span of the effective stimulus during a fixation in reading. Percept. Psychophys. 1975, 17, 578–586. [Google Scholar] [CrossRef] [Green Version]
- Wang, Q.; Celebi, F.M.; Flink, L.; Greco, G.; Wall, C.A.; Prince, E.B.; Lansiquot, S.; Chawarska, K.; Kim, E.S.; Boccanfuso, L.; et al. Interactive eye tracking for gaze strategy modification. In Proceedings of the 14th International Conference on Interaction Design and Children, Boston, MA, USA, 21–24 June 2015. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [Green Version]
- Ackley, B.J.; Swan, B.A.; Ladwig, G.; Tucker, S. Evidence-Based Nursing Care Guidelines: Medical-Surgical Interventions; Mosby Elsevier: St. Louis, MO, USA, 2008; p. 7. [Google Scholar]
- Woolridge, S.M.; Harrison, G.W.; Best, M.W.; Bowie, C.R. Attention bias modification in depression: A randomized trial using a novel, reward-based, eye-tracking approach. J. Behav. Ther. Exp. Psychiatry 2021, 71, 101621. [Google Scholar] [CrossRef]
- Vazquez, C.; Blanco, I.; Sanchez, A.; McNally, R.J. Attentional bias modification in depression through gaze contingencies and regulatory control using a new eye-tracking intervention paradigm: Study protocol for a placebo-controlled trial. BMC Psychiatry 2016, 16, 439. [Google Scholar] [CrossRef] [Green Version]
- Lee, T.L.; Yeung, M.K.; Sze, S.L.; Chan, A.S. Computerized eye-tracking training improves the saccadic eye movements of children with attention-deficit/hyperactivity disorder. Brain Sci. 2020, 10, 1016. [Google Scholar] [CrossRef]
- Lee, T.L.; Yeung, M.K.; Sze, S.L.; Chan, A.S. Eye-tracking training improves inhibitory control in children with attention-deficit/hyperactivity disorder. Brain Sci. 2021, 11, 314. [Google Scholar] [CrossRef]
- Lazarov, A.; Pine, D.S.; Bar-Haim, Y. Gaze-contingent music reward therapy for social anxiety disorder: A randomized controlled trial. Am. J. Psychiatry 2017, 174, 649–656. [Google Scholar] [CrossRef] [Green Version]
- Kvamme, T.L.; Pedersen, M.U.; Overgaard, M.; Thomsen, K.R.; Voon, V. Pilot study: Improving attention bias modification of alcohol cues through concealed gaze-contingent feedback in alcohol dependence. Addict. Behav. Rep. 2019, 10, 100231. [Google Scholar] [CrossRef]
- Dovigo, L.; Caprì, T.; Iannizzotto, G.; Nucita, A.; Semino, M.; Giannatiempo, S.; Zocca, L.; Fabio, R.A. Social and cognitive interactions through an interactive school service for RTT patients at the COVID-19 time. Front. Psychol. 2021, 12, 676238. [Google Scholar] [CrossRef]
- Iannizzotto, G.; Nucita, A.; Fabio, R.; Caprì, T.; Lo Bello, L. Remote eye-tracking for cognitive telerehabilitation and interactive school tasks in times of COVID-19. Information 2020, 11, 296. [Google Scholar] [CrossRef]
- Wang, Q.; Wall, C.A.; Barney, E.C.; Bradshaw, J.L.; Macari, S.L.; Chawarska, K.; Shic, F. Promoting social attention in 3-year-olds with ASD through gaze-contingent eye tracking. Autism Res. 2020, 13, 61–73. [Google Scholar] [CrossRef] [Green Version]
- García-Baos, A.; D’Amelio, T.; Oliveira, I.; Collins, P.; Echevarria, C.; Zapata, L.P.; Liddle, E.; Supèr, H. Novel interactive eye-tracking game for training attention in children with attention-deficit/hyperactivity disorder. Prim. Care Companion CNS Disord. 2019, 21, 26348. [Google Scholar] [CrossRef]
- Lévy-Bencheton, D.; Pélisson, D.; Prost, M.; Jacquin-Courtois, S.; Salemme, R.; Pisella, L.; Tilikete, C. The effects of short-lasting anti-saccade training in homonymous hemianopia with and without saccadic adaptation. Front. Behav. Neurosci. 2016, 9, 332. [Google Scholar] [CrossRef] [Green Version]
- Caprì, T.; Nucita, A.; Iannizzotto, G.; Mohammadhasani, N.; Fabio, R. Eye-gaze digital games improve motivational and attentional abilities in RETT syndrome. J. Spec. Educ. Rehabilit. 2019, 19, 105–126. [Google Scholar] [CrossRef]
- Perra, O.; Wass, S.; McNulty, A.; Sweet, D.; Papageorgiou, K.A.; Johnston, M.; Bilello, D.; Patterson, A.; Alderdice, F. Very preterm infants engage in an intervention to train their control of attention: Results from the feasibility study of the Attention Control Training (ACT) randomised trial. Pilot Feasibility Stud. 2021, 7, 66. [Google Scholar] [CrossRef]
- Goodwin, A.; Salomone, S.; Bolton, P.; Charman, T.; Jones, E.J.H.; Mason, L.; Pickles, A.; Robinson, E.; Smith, T.; Sonuga-Barke, E.J.S.; et al. Attention training for infants at familial risk of ADHD (INTERSTAARS): Study protocol for a randomised controlled trial. Trials 2016, 17, 608. [Google Scholar] [CrossRef] [Green Version]
- Garcia-Zapirain, B.; de la Torre Díez, I.; López-Coronado, M. Dual system for enhancing cognitive abilities of children with ADHD using leap motion and eye-tracking technologies. J. Med. Syst. 2017, 41, 111. [Google Scholar] [CrossRef]
- Verghese, A.; Mattingley, J.B.; Palmer, P.E.; Dux, P.E. From eyes to hands: Transfer of learning in the Simon task across motor effectors. Atten. Percept. Psychophys 2018, 80, 193–210. [Google Scholar] [CrossRef] [Green Version]
- Wass, S.; Porayska-Pomsta, K.; Johnson, M.H. Training attentional control in infancy. Curr. Biol. 2011, 21, 1543–1547. [Google Scholar] [CrossRef] [Green Version]
- Ballieux, H.; Wass, S.V.; Tomalski, P.; Kushnerenko, E.; Karmiloff-Smith, A.; Johnson, M.; Moore, D. Applying gaze-contingent training within community settings to infants from diverse SES backgrounds. J. Appl. Dev. Psychol. 2016, 43, 8–17. [Google Scholar] [CrossRef] [Green Version]
- Ferrari, G.R.; Möbius, M.; van Opdorp, A.; Becker, E.S.; Rinck, M. Can’t look away: An eye-tracking based attentional disengagement training for depression. Cognit. Ther. Res. 2016, 40, 672–686. [Google Scholar] [CrossRef] [Green Version]
- Price, R.B.; Greven, I.M.; Siegle, G.J.; Koster, E.H.; De Raedt, R. A novel attention training paradigm based on operant conditioning of eye gaze: Preliminary findings. Emotion 2016, 16, 110–116. [Google Scholar] [CrossRef]
- Sanchez-Lopez, A.; Everaert, J.; Van Put, J.; De Raedt, R.; Koster, E.H.W. Eye-gaze contingent attention training (ECAT): Examining the causal role of attention regulation in reappraisal and rumination. Biol. Psychol. 2019, 142, 116–125. [Google Scholar] [CrossRef] [Green Version]
- Perra, O.; Wass, S.; McNulty, A.; Sweet, D.; Papageorgiou, K.; Johnston, M.; Patterson, A.; Bilello, D.; Alderdice, F. Training attention control of very preterm infants: Protocol for a feasibility study of the Attention Control Training (ACT). Pilot Feasibility Stud. 2020, 6, 17. [Google Scholar] [CrossRef] [Green Version]
- Martínez-Moreno, J.M.; Solana, J.; Sánchez, R.; González, S.; Sánchez-González, P.; Gómez, C.; Morell, M.; Cáceres, C.; Roig, T.; Tormos, J.M.; et al. Cognitive neurorehabilitation based on interactive video technology. Stud. Health Technol. Inform. 2013, 190, 27–29. [Google Scholar]
- Simon, J.R.; Craft, J.L.; Webster, J.B. Reactions toward the stimulus source: Analysis of correct responses and errors over a fiveday period. J. Exp. Psychol. 1973, 101, 175–178. [Google Scholar] [CrossRef]
- Vermeir, J.F.; White, M.J.; Johnson, D.; Crombez, G.; Van Ryckeghem, D.M.L. The effects of gamification on computerized cognitive training: Systematic review and meta-analysis. JMIR Serious Games 2020, 8, e18644. [Google Scholar] [CrossRef]
- MacLeod, C.; Mathews, A.; Tata, P. Attentional bias in emotional disorders. J. Abnorm. Psychol. 1986, 95, 15–20. [Google Scholar] [CrossRef]
- Rosch, J.L.; Vogel-Walcutt, J.J. A review of eye-tracking applications as tools for training. Cognit. Technol. Work 2013, 15, 313–327. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carelli, L.; Solca, F.; Tagini, S.; Torre, S.; Verde, F.; Ticozzi, N.; Ferrucci, R.; Pravettoni, G.; Aiello, E.N.; Silani, V.; et al. Gaze-Contingent Eye-Tracking Training in Brain Disorders: A Systematic Review. Brain Sci. 2022, 12, 931. https://doi.org/10.3390/brainsci12070931
Carelli L, Solca F, Tagini S, Torre S, Verde F, Ticozzi N, Ferrucci R, Pravettoni G, Aiello EN, Silani V, et al. Gaze-Contingent Eye-Tracking Training in Brain Disorders: A Systematic Review. Brain Sciences. 2022; 12(7):931. https://doi.org/10.3390/brainsci12070931
Chicago/Turabian StyleCarelli, Laura, Federica Solca, Sofia Tagini, Silvia Torre, Federico Verde, Nicola Ticozzi, Roberta Ferrucci, Gabriella Pravettoni, Edoardo Nicolò Aiello, Vincenzo Silani, and et al. 2022. "Gaze-Contingent Eye-Tracking Training in Brain Disorders: A Systematic Review" Brain Sciences 12, no. 7: 931. https://doi.org/10.3390/brainsci12070931
APA StyleCarelli, L., Solca, F., Tagini, S., Torre, S., Verde, F., Ticozzi, N., Ferrucci, R., Pravettoni, G., Aiello, E. N., Silani, V., & Poletti, B. (2022). Gaze-Contingent Eye-Tracking Training in Brain Disorders: A Systematic Review. Brain Sciences, 12(7), 931. https://doi.org/10.3390/brainsci12070931







