Recreational Drug Misuse and Its Potential Contribution to Male Fertility Levels’ Decline: A Narrative Review
Abstract
1. Introduction
1.1. Psychoactive Substances’ Intake and Related Medical Untoward Consequences; Male Infertility: Definition, Causes, and Risk Factors
1.2. Drug Use as a Risk Factor for Male Infertility
2. Materials and Methods
2.1. Screening and Selection Process
2.2. Inclusion and Exclusion Criteria
2.3. Data Analysis and Presentation
3. Results
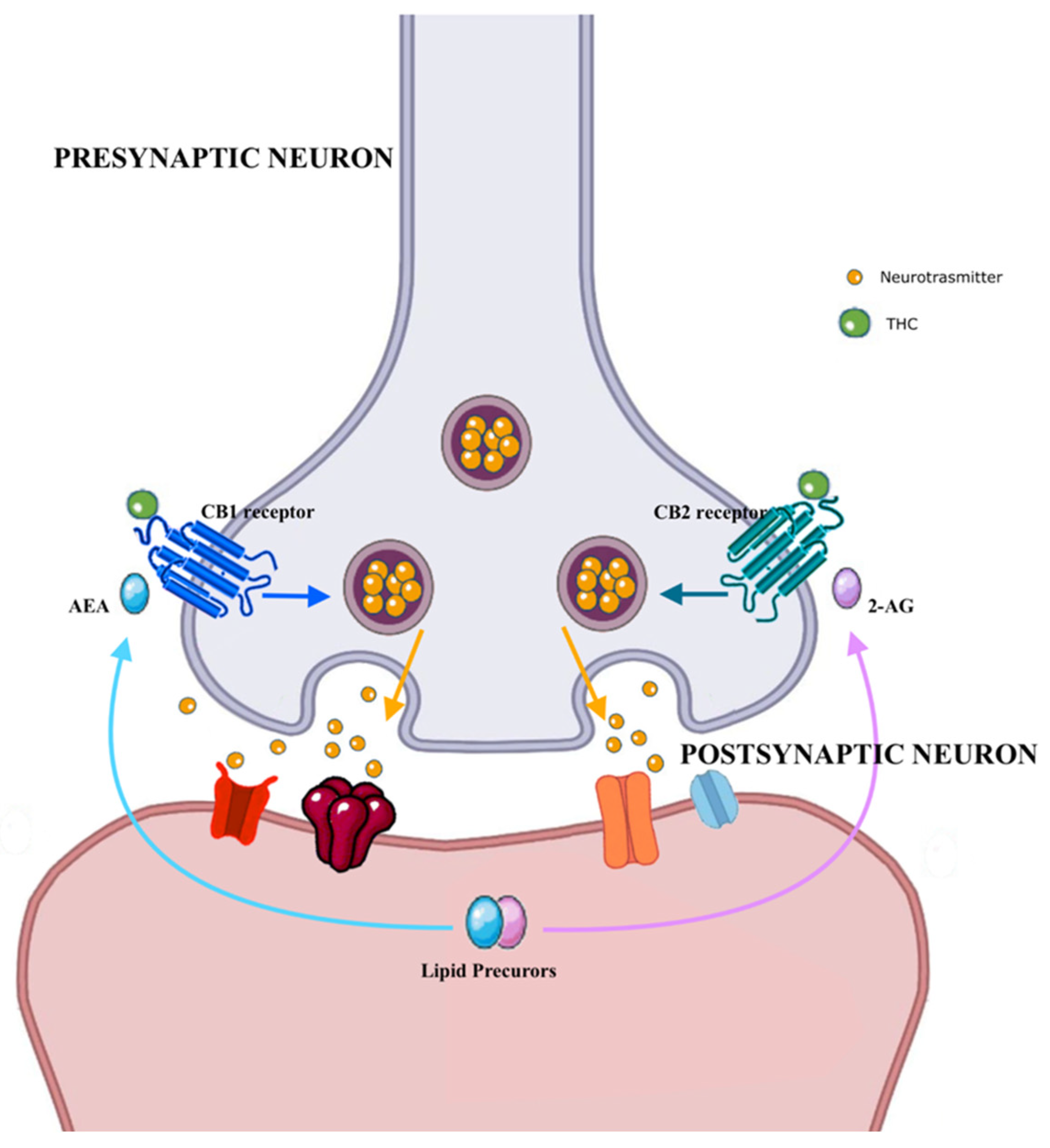
3.1. Cannabis
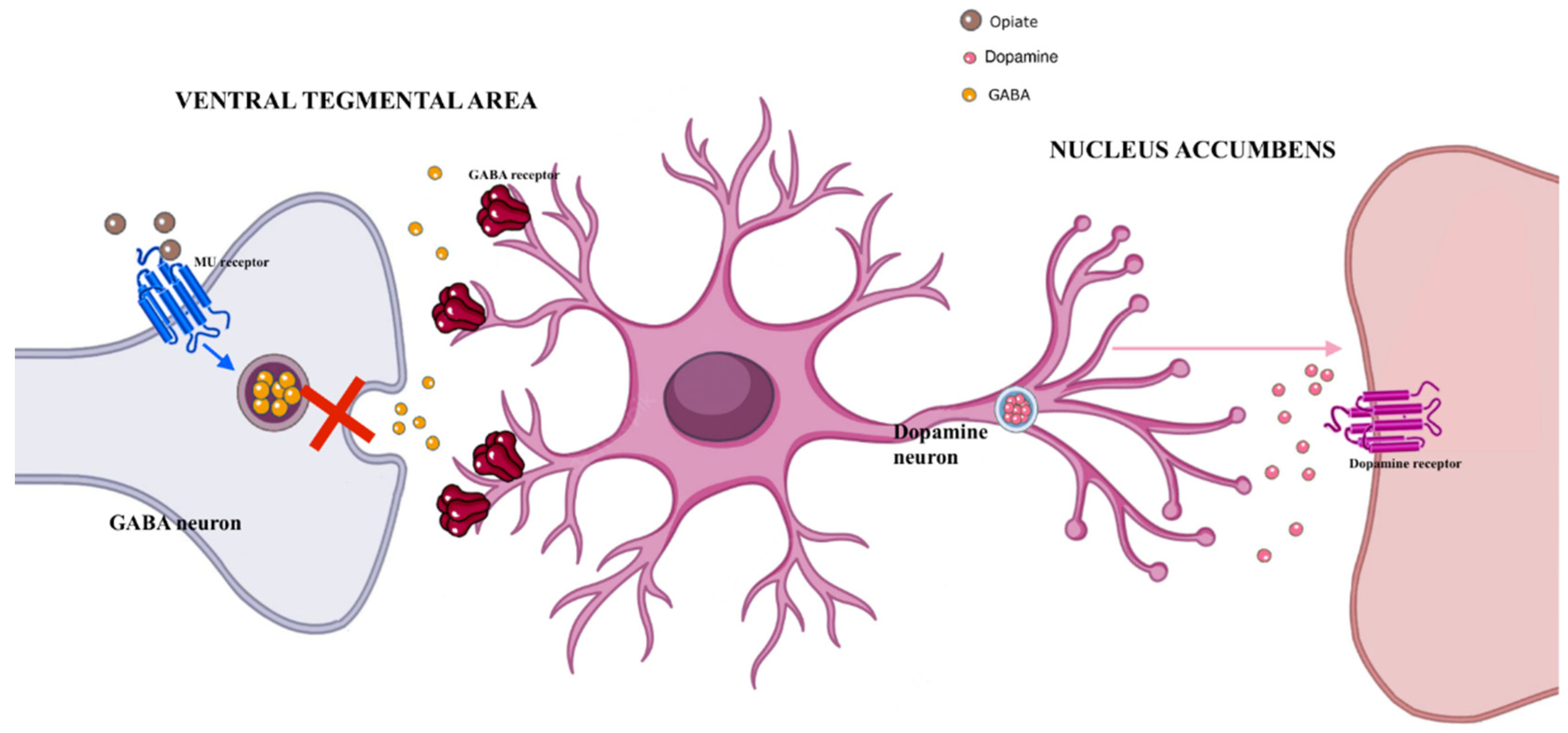
3.2. Opiates/Opioids
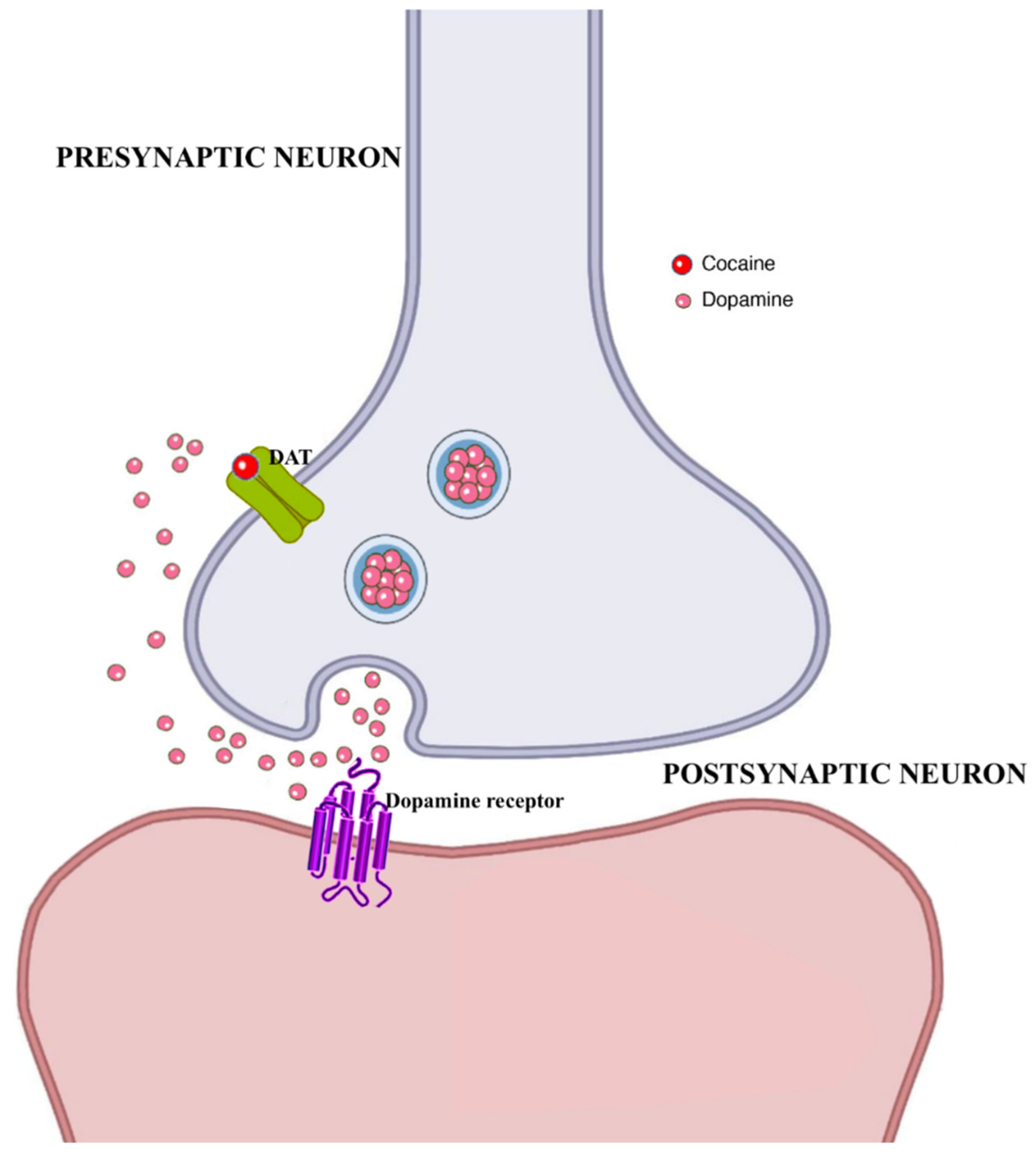
3.3. Cocaine
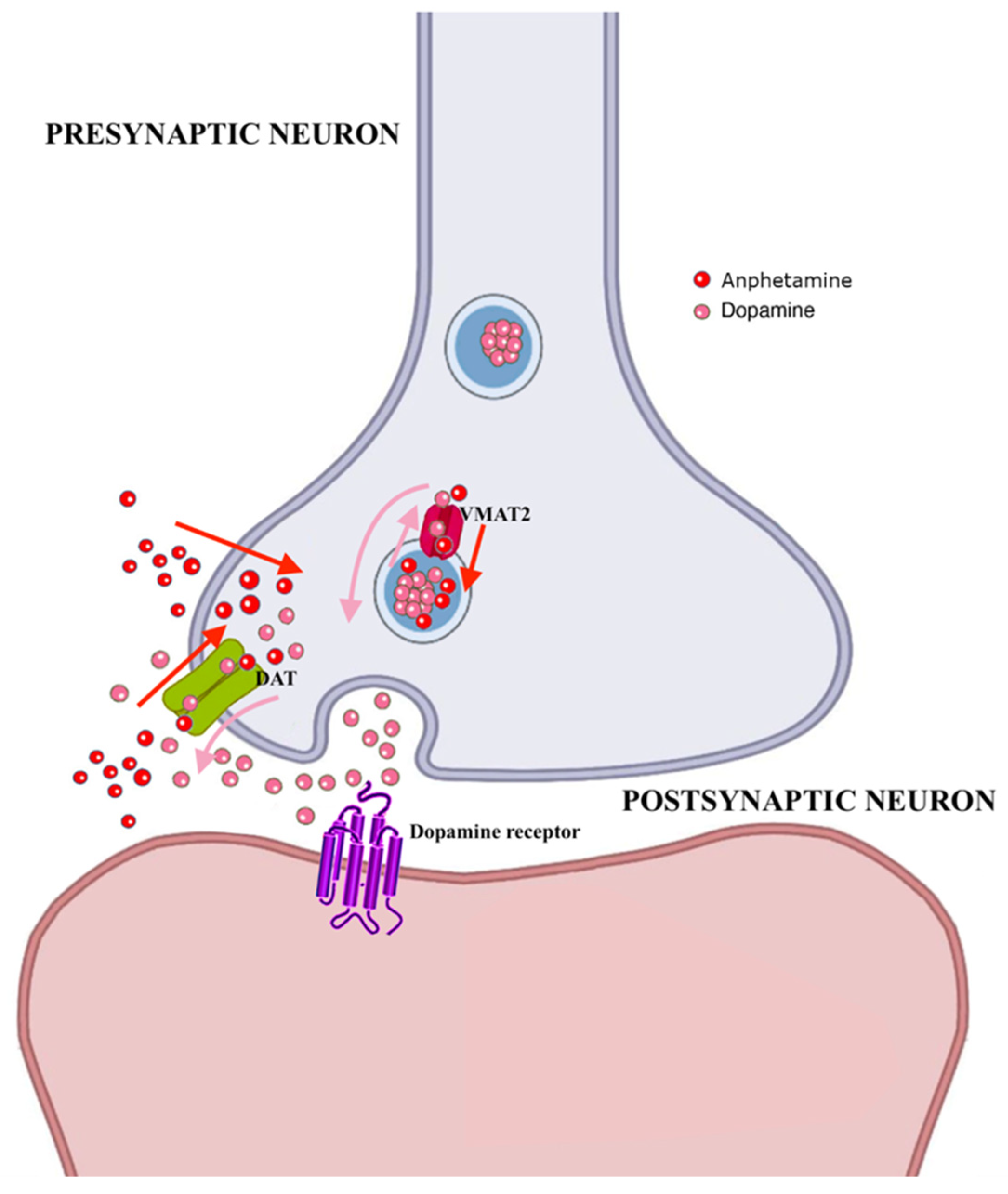
3.4. Amphetamine-Type Stimulants (ATS)
3.5. Novel Psychoactive Substances (NPS); ‘Herbal Highs’; and Psychedelics
4. Discussion
4.1. Male Infertility Measurement; Methodological Issues
4.2. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ahmad, S.; Hlaing, S.W.; Haris, M.; Attar, N. Marijuana: Cardiovascular effects and legal considerations. A clinical case-based review. Br. J. Cardiol. 2022, 29, 11. [Google Scholar] [CrossRef]
- Schifano, F.; Orsolini, L.; Papanti, D.; Corkery, J. NPS: Medical Consequences Associated with Their Intake. Curr. Top. Behav. Neurosci. 2017, 32, 351–380. [Google Scholar] [CrossRef] [PubMed]
- Zangani, C.; Schifano, F.; Napoletano, F.; Arillotta, D.; Gilgar, L.; Guirguis, A.; Corkery, J.M.; Gambini, O.; Vento, A. The e-Psychonauts’ ‘Spiced’ World; Assessment of the Synthetic Cannabinoids’ Information Available Online. Curr. Neuropharmacol. 2020, 18, 966–1051. [Google Scholar] [CrossRef] [PubMed]
- Catalani, V.; Corkery, J.M.; Guirguis, A.; Napoletano, F.; Arillotta, D.; Zangani, C.; Vento, A.; Schifano, F. Psychonauts’ psychedelics: A systematic, multilingual, web-crawling exercise. Eur. Neuropsychopharmacol. J. Eur. Coll. Neuropsychopharmacol. 2021, 49, 69–92. [Google Scholar] [CrossRef]
- Salonia, A.; Minhas, S. EAU Guidelines on Sexual and Reproductive Health. Edn. Presented at the EAU Annual Congress Amsterdam; EAU Guidelines Office: Arnhem, The Netherlands, 2022. [Google Scholar]
- Eisenberg, M.L.; Lathi, R.B.; Baker, V.L.; Westphal, L.M.; Milki, A.A.; Nangia, A.K. Frequency of the male infertility evaluation: Data from the national survey of family growth. J. Urol. 2013, 189, 1030–1034. [Google Scholar] [CrossRef]
- Boeri, L.; Capogrosso, P.; Ventimiglia, E.; Pederzoli, F.; Cazzaniga, W.; Chierigo, F.; Dehò, F.; Montanari, E.; Montorsi, F.; Salonia, A. Heavy cigarette smoking and alcohol consumption are associated with impaired sperm parameters in primary infertile men. Asian J. Androl. 2019, 21, 478–485. [Google Scholar] [CrossRef] [PubMed]
- Jensen, T.K.; Gottschau, M.; Madsen, J.O.B.; Andersson, A.-M.; Lassen, T.H.; Skakkebæk, N.E.; Swan, S.H.; Priskorn, L.; Juul, A.; Jørgensen, N. Habitual alcohol consumption associated with reduced semen quality and changes in reproductive hormones; a cross-sectional study among 1221 young Danish men. BMJ Open 2014, 4, e005462. [Google Scholar] [CrossRef] [PubMed]
- Gaskins, A.J.; Mendiola, J.; Afeiche, M.; Jørgensen, N.; Swan, S.H.; Chavarro, J.E. Physical activity and television watching in relation to semen quality in young men. Br. J. Sport. Med. 2015, 49, 265–270. [Google Scholar] [CrossRef] [PubMed]
- Gaskins, A.J.; Afeiche, M.C.; Hauser, R.; Williams, P.L.; Gillman, M.W.; Tanrikut, C.; Petrozza, J.C.; Chavarro, J.E. Paternal physical and sedentary activities in relation to semen quality and reproductive outcomes among couples from a fertility center. Hum. Reprod. 2014, 29, 2575–2582. [Google Scholar] [CrossRef]
- Eisenberg, M.L.; Kim, S.; Chen, Z.; Sundaram, R.; Schisterman, E.F.; Louis, G.M.B. The relationship between male BMI and waist circumference on semen quality: Data from the LIFE study. Hum. Reprod. 2015, 30, 493–494. [Google Scholar] [CrossRef]
- Li, Y.; Lin, H.; Li, Y.; Cao, J. Association between socio-psycho-behavioral factors and male semen quality: Systematic review and meta-analyses. Fertil. Steril. 2011, 95, 116–123. [Google Scholar] [CrossRef] [PubMed]
- Belladelli, F.; Boeri, L.; Capogrosso, P.; Cazzaniga, W.; Ventimiglia, E.; Candela, L.; Pozzi, E.; Baudo, A.; Alfano, M.; Abbate, C.; et al. Substances of abuse consumption among patients seeking medical help for uro-andrological purposes: A sociobehavioral survey in the real-life scenario. Asian J. Androl. 2021, 23, 456–461. [Google Scholar] [CrossRef] [PubMed]
- Chiappini, S.; Guirguis, A.; John, A.; Corkery, J.M.; Schifano, F. COVID-19: The Hidden Impact on Mental Health and Drug Addiction. Front. Psychiatry 2020, 11, 767. [Google Scholar] [CrossRef] [PubMed]
- Drug, E.M.C.F.; Addiction, D. European Drug Report 2021: Trends and Development; Publications Office of the European Union: Luxembourg, 2021. [Google Scholar]
- de Jong, A.M.E.; Menkveld, R.; Lens, J.W.; Nienhuis, S.E.; Rhemrev, J.P.T. Effect of alcohol intake and cigarette smoking on sperm parameters and pregnancy. Andrologia 2014, 46, 112–117. [Google Scholar] [CrossRef] [PubMed]
- Jensen, T.K.; Swan, S.; Jørgensen, N.; Toppari, J.; Redmon, B.; Punab, M.; Drobnis, E.Z.; Haugen, T.B.; Zilaitiene, B.; Sparks, A.E.; et al. Alcohol and male reproductive health: A cross-sectional study of 8344 healthy men from Europe and the USA. Hum. Reprod. 2014, 29, 1801–1809. [Google Scholar] [CrossRef]
- Jordan, T.; Ngo, B.; Jones, C.A. The use of cannabis and perceptions of its effect on fertility among infertility patients. Hum. Reprod. Open 2020, 2020, hoz041. [Google Scholar] [CrossRef]
- Nielsen, J.E.; Rolland, A.D.; Rajpert-De Meyts, E.; Janfelt, C.; Jørgensen, A.; Winge, S.B.; Kristensen, D.M.; Juul, A.; Chalmel, F.; Jégou, B.; et al. Characterisation and localisation of the endocannabinoid system components in the adult human testis. Sci. Rep. 2019, 9, 12866. [Google Scholar] [CrossRef]
- Alagbonsi, I.A.; Olayaki, L.A. Ameliorative effect of combined melatonin and vitamin C on Cannabis sativa -induced reproductive hormonal toxicity. J. Afr. Ass. Physiol. Sci. 2016, 4, 14–24. [Google Scholar]
- Bonini, S.A.; Bonini, S.A.; Premoli, M.; Tambaro, S.; Kumar, A.; Maccarinelli, G.; Memo, M.; Mastinu, A. Cannabis sativa: A comprehensive ethnopharmacological review of a medicinal plant with a long history. J. Ethnopharmacol. 2018, 227, 300–315. [Google Scholar] [CrossRef]
- Alagbonsi, I.A.; Olayaki, L.A.; Salman, T.M. Melatonin and vitamin C exacerbate Cannabis sativa-induced testicular damage when administered separately but ameliorate it when combined in rats. J. Basic Clin. Physiol. Pharmacol. 2016, 27, 277–287. [Google Scholar] [CrossRef]
- Verhaeghe, F.; Premoli, M.; Tambaro, S.; Kumar, A.; Maccarinelli, G.; Memo, M.; Mastinu, A. Cannabis consumption might exert deleterious effects on sperm nuclear quality in infertile men. Reprod. Biomed. Online 2020, 40, 270–280. [Google Scholar] [CrossRef] [PubMed]
- Hehemann, M.C.; Raheem, O.A.; Rajanahally, S.; Holt, S.; Chen, T.; Fustok, J.N.; Song, K.; Rylander, H.; Chow, E.; Ostrowski, K.A.; et al. Evaluation of the impact of marijuana use on semen quality: A prospective analysis. Ther. Adv. Urol. 2021, 13, 17562872211032484. [Google Scholar] [CrossRef] [PubMed]
- Carroll, K.; Pottinger, A.M.; Wynter, S.; DaCosta, V. Marijuana use and its influence on sperm morphology and motility: Identified risk for fertility among Jamaican men. Andrology 2020, 8, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Gundersen, T.D.; Gundersen, T.D.; Jørgensen, N.; Andersson, A.-M.; Bang, A.K.; Nordkap, L.; Skakkebæk, N.E.; Priskorn, L.; Juul, A.; Jensen, T.K. Association Between Use of Marijuana and Male Reproductive Hormones and Semen Quality: A Study Among 1215 Healthy Young Men. Am. J. Epidemiol. 2015, 182, 473–481. [Google Scholar] [CrossRef] [PubMed]
- WHO Laboratory Manual for the Examination and Processing of Human Semen; World Health Organization: Geneva, Switzerland, 2021; Available online: https://apps.who.int/iris/handle/10665/44261 (accessed on 1 October 2022).
- Nassan, F.L.; Arvizu, M.; Mínguez-Alarcón, L.; Williams, P.L.; Attaman, J.; Petrozza, J.; Hauser, R.; Chavarro, J. Marijuana smoking and markers of testicular function among men from a fertility centre. Hum. Reprod. 2019, 34, 715–723. [Google Scholar] [CrossRef]
- Belladelli, F.; Del Giudice, F.; Kasman, A.; Kold Jensen, T.; Jørgensen, N.; Salonia, A.; Eisenberg, M.L. The association between cannabis use and testicular function in men: A systematic review and meta-analysis. Andrology 2021, 9, 503–510. [Google Scholar] [CrossRef]
- Chiappini, S.; Vickers-Smith, R.; Guirguis, A.; Corkery, J.M.; Martinotti, G.; Harris, D.R.; Schifano, F. Pharmacovigilance Signals of the Opioid Epidemic over 10 Years: Data Mining Methods in the Analysis of Pharmacovigilance Datasets Collecting Adverse Drug Reactions (ADRs) Reported to EudraVigilance (EV) and the FDA Adverse Event Reporting System (FAERS). Pharmaceuticals 2022, 15, 675. [Google Scholar] [CrossRef] [PubMed]
- Butelman, E.R.; Fry, R.S.; Kimani, R.; Reed, B.; Kreek, M.J. Neuroendocrine effects of naltrexone versus nalmefene in humans. Hum. Psychopharmacol. 2020, 35, e2726. [Google Scholar] [CrossRef]
- Koohsari, M.; Ahangar, N.; Mohammadi, E.; Amiri, F.T.; Shaki, F. Effects of tramadol administration on male reproductive toxicity in Wistar rats The role of oxidative stress, mitochondrial dysfunction, apoptosis-related gene expression, and nuclear factor kappa B signalling. Bratisl. Lek. Listy 2020, 121, 400–410. [Google Scholar] [CrossRef]
- Akhgari, M.; Jokar, F.; Bahmanabadi, L.; Aleagha, A.E. Street-level heroin seizures in Iran: A survey of components. J. Subst. Use 2012, 17, 348–355. [Google Scholar] [CrossRef]
- Heidari, Z.; Mahmoudzadeh-Sagheb, H.; Kohan, F. A Quantitative and Qualitative Study of Rat Testis Following Administration of Methadone and Buprenorphine. Int. J. High Risk Behav. Addict. 2012, 1, 14–17. [Google Scholar] [CrossRef]
- Takzare, N.; Samizadeh, E.; Shoar, S.; Majidi Zolbin, M.; Naderan, M.; Lashkari, A.; Bakhtiarian, A. Impacts of morphine addiction on spermatogenesis in rats. Int. J. Reprod. Biomed. 2016, 14, 303–308. [Google Scholar] [CrossRef] [PubMed]
- Urizar-Arenaza, I.; Osinalde, N.; Akimov, V.; Puglia, M.; Muñoa-Hoyos, I.; Gómez-Giménez, B.; Gianzo, M.; Ganzabal, T.; Blagoev, B.; Kratchmarova, I.; et al. Kappa- opioid receptor regulates human sperm functions via SPANX-A/D protein family. Reprod. Biol. 2020, 20, 300–306. [Google Scholar] [CrossRef] [PubMed]
- Paice, J.A.; Penn, R.D.; Ryan, W.G. Altered sexual function and decreased testosterone in patients receiving intraspinal opioids. J. Pain Symptom Manag. 1994, 9, 126–131. [Google Scholar] [CrossRef]
- Mirin, S.M.; Mendelson, J.H.; Ellingboe, J.; Meyer, R.E. Acute effects of heroin and naltrexone on testosterone and gonadotropin secretion: A pilot study. Psychoneuroendocrinology 1976, 1, 359–369. [Google Scholar] [CrossRef]
- Bolelli, G.; Lafisca, S.; Flamigni, C.; Lodi, S.; Franceschetti, F.; Filicori, M.; Mosca, R. Heroin addiction: Relationship between the plasma levels of testosterone, dihydrotestosterone, androstenedione, LH, FSH, and the plasma concentration of heroin. Toxicology 1979, 15, 19–29. [Google Scholar] [CrossRef]
- Nazmara, Z.; Najafi, M.; Movahedin, M.; Zandiyeh, Z.; Shirinbayan, P.; Asgari, H.R.; Roshanpajouh, M.; Maki, C.B.; Bashiri, Z.; Koruji, M. Correlation Between Protamine-2 and miRNA-122 in Sperm from Heroin-addicted Men: A Case-Control Study. Urol. J. 2020, 17, 638–644. [Google Scholar] [CrossRef]
- Nazmara, Z.; Najafi, M.; Rezaei-Mojaz, S.; Movahedin, M.; Zandiyeh, Z.; Shirinbayan, P.; Roshanpajouh, M.; Asgari, H.R.; Hosseini Jafari Lavasani, L.; Koruji, M. The Effect of Heroin Addiction on Human Sperm Parameters, Histone-to-Protamine Transition, and Serum Sexual Hormones Levels. Urol. J. 2019, 16, 289–294. [Google Scholar] [CrossRef]
- Safarinejad, M.R.; Asgari, S.A.; Farshi, A.; Ghaedi, G.; Kolahi, A.A.; Iravani, S.; Khoshdel, A.R. The effects of opiate consumption on serum reproductive hormone levels, sperm parameters, seminal plasma antioxidant capacity and sperm DNA integrity. Reprod. Toxicol. 2013, 36, 18–23. [Google Scholar] [CrossRef]
- Bassiony, M.M.; Youssef, U.M.; El-Gohari, H. Free Testosterone and Prolactin Levels and Sperm Morphology and Function Among Male Patients With Tramadol Abuse: A Case-Control Study. J. Clin. Psychopharmacol. 2020, 40, 405–408. [Google Scholar] [CrossRef]
- Li, H.; Jiang, Y.; Rajpurkar, A.; Dunbar, J.C.; Dhabuwala, C.B. Cocaine induced apoptosis in rat testes. J. Urol. 1999, 162, 213–216. [Google Scholar] [CrossRef]
- Li, H.; Xu, L.; Dunbar, J.C.; Dhabuwala, C.B. Role of mitochondrial cytochrome c in cocaine-induced apoptosis in rat testes. Urology 2003, 61, 646–650. [Google Scholar] [CrossRef]
- Yang, G.-S.; Wang, W.; Wang, Y.-M.; Chen, Z.-D.; Wang, S.; Fang, J.-J. Effect of cocaine on germ cell apoptosis in rats at different ages. Asian J. Androl. 2006, 8, 569–575. [Google Scholar] [CrossRef] [PubMed]
- George, V.K.; Li, H.; Teloken, C.; Grignon, D.J.; Lawrence, W.D.; Dhabuwala, C.B. Effects of long-term cocaine exposure on spermatogenesis and fertility in peripubertal male rats. J. Urol. 1996, 155, 327–331. [Google Scholar] [CrossRef]
- Rodriguez, M.C.; Sanchez-Yague, J.; Paniagua, R. Effects of cocaine on testicular structure in the rat. Reprod. Toxicol. 1992, 6, 51–55. [Google Scholar] [CrossRef]
- Bracken, M.B.; Eskenazi, B.; Sachse, K.; McSharry, J.E.; Hellenbrand, K.; Leo-Summers, L. Association of cocaine use with sperm concentration, motility, and morphology. Fertil. Steril. 1990, 53, 315–322. [Google Scholar] [CrossRef]
- Samplaski, M.K.; Bachir, B.G.; Lo, K.C.; Grober, E.D.; Lau, S.; Jarvi, K.A. Cocaine Use in the Infertile Male Population: A Marker for Conditions Resulting in Subfertility. Curr. Urol. 2015, 8, 38–42. [Google Scholar] [CrossRef]
- Aguilera-Mijares, S.; Sang, J.M.; Wang, L.; Barath, J.; Card, K.G.; Lachowsky, N.J.; Lal, A.; Roth, E.; Hogg, R.S.; Moore, D.M. Variations in Sexual Behaviors by Use of Specific Substances Among Vancouver Gay, Bisexual, and Other Men Who Have Sex with Men: An Event-Level Analysis. Arch. Sex. Behav. 2021, 50, 2875–2886. [Google Scholar] [CrossRef]
- Nudmamud-Thanoi, S.; Thanoi, S. Methamphetamine induces abnormal sperm morphology, low sperm concentration and apoptosis in the testis of male rats. Andrologia 2011, 43, 278–282. [Google Scholar] [CrossRef]
- Yamamoto, Y.; Yamamoto, K.; Hayase, T. Effect of methamphetamine on male mice fertility. J. Obstet. Gynaecol. Res. 1999, 25, 353–358. [Google Scholar] [CrossRef]
- Yamamoto, Y.; Yamamoto, K.; Hayase, T.; Abiru, H.; Shiota, K.; Mori, C. Methamphetamine induces apoptosis in seminiferous tubules in male mice testis. Toxicol. Appl. Pharmacol. 2002, 178, 155–160. [Google Scholar] [CrossRef]
- Kaewman, P.; Nudmamud-Thanoi, S.; Thanoi, S. GABAergic Alterations in the Rat Testis after Methamphetamine Exposure. Int. J. Med. Sci. 2018, 15, 1349–1354. [Google Scholar] [CrossRef]
- Aryan, A.; Abdollahifar, M.-A.; Karbalay-Doust, S.; Forozesh, M.; Mahmoudiasl, G.-R.; Akaberi-Nasrabadi, S.; Bahmanpour, S. Methamphetamine can induce alteration of histopathology and sex determination gene expression through the oxidative stress pathway in the testes of human post-mortem. Andrologia 2022, 54, e14441. [Google Scholar] [CrossRef] [PubMed]
- Renoux, C.; Shin, J.-Y.; Dell’Aniello, S.; Fergusson, E.; Suissa, S. Prescribing trends of attention-deficit hyperactivity disorder (ADHD) medications in UK primary care, 1995–2015. Br. J. Clin. Pharmacol. 2016, 82, 858–868. [Google Scholar] [CrossRef] [PubMed]
- Adriani, W.; Leo, D.; Guarino, M.; Natoli, A.; Di Consiglio, E.; De Angelis, G.; Traina, E.; Testai, E.; Perrone-Capano, C.; Laviola, G. Short-term effects of adolescent methylphenidate exposure on brain striatal gene expression and sexual/endocrine parameters in male rats. Ann. N. Y. Acad. Sci. 2006, 1074, 52–73. [Google Scholar] [CrossRef] [PubMed]
- Manjanatha, M.G.; Shelton, S.D.; Dobrovolsky, V.N.; Shaddock, J.G.; McGarrity, L.G.; Doerge, D.R.; Twaddle, N.W.; Lin, C.-J.; Chen, J.J.; Mattison, D.R.; et al. Pharmacokinetics, dose-range, and mutagenicity studies of methylphenidate hydrochloride in B6C3F1 mice. Environ. Mol. Mutagen. 2008, 49, 585–593. [Google Scholar] [CrossRef]
- Pham, M.N.; Hudnall, M.T.; Fantus, R.J.; Lai, J.D.; Ambulkar, S.S.; Wren, J.M.; Bennett, N.E.; Auffenberg, G.B.; Chu, D.I.; Brannigan, R.E.; et al. The adverse association between stimulant use for attention deficit hyperactivity disorder (ADHD) and semen parameters. Andrologia 2022, 54, e14315. [Google Scholar] [CrossRef]
- Shalev, H.; Mizrakli, Y.; Zeadna, A.; Harlev, A.; Levitas, E.; Ifergane, G.; Lunenfeld, E.; Novack, V.; Har-Vardi, I.; Levitas, E. Does methylphenidate use affect sperm parameters in patients undergoing infertility investigation? A retrospective analysis of 9769 semen samples. Arch. Gynecol. Obstet. 2021, 304, 539–546. [Google Scholar] [CrossRef]
- Schifano, F.; Chiappini, S.; Corkery, J.M.; Scherbaum, N.; Guirguis, A. The e-psychonaut drugs’ psychopharmacology. Curr. Opin. Pharmacol. 2021, 57, 165–174. [Google Scholar] [CrossRef]
- Markowitz, E.H.; Brosseau, G.E.J.; Markowitz, E. Genetic effects of LSD treatment on the post-meiotic stages of spermatogenesis in Drosophila melanogaster. Mutat. Res. 1969, 8, 337–342. [Google Scholar] [CrossRef]
- Estop, A.M.; Cieply, K.; Vankirk, V.; Munne, S.; Garver, K. Cytogenetic studies in human sperm. Hum. Genet. 1991, 87, 447–451. [Google Scholar] [CrossRef]
- Hakim, L.Y. Influence of khat on seminal fluid among presumed infertile couples. East Afr. Med. J. 2002, 79, 22–28. [Google Scholar] [CrossRef] [PubMed]
- Ajayi, A.F.; Akhigbe, R.E. The physiology of male reproduction: Impact of drugs and their abuse on male fertility. Andrologia 2020, 52, e13672. [Google Scholar] [CrossRef] [PubMed]
- Fronczak, C.M.; Kim, E.D.; Barqawi, A.B. The insults of illicit drug use on male fertility. J. Androl. 2012, 33, 515–528. [Google Scholar] [CrossRef] [PubMed]
- Omes, C.; Tomasoni, V.; de Amici, M.; Testa, G.; Torre, C.; Nappi, R.E. Calprotectin as a novel diagnostic approach to screen male infertility risk: A pilot study. Immunobiology 2022, 227, 152291. [Google Scholar] [CrossRef]
- Bu, F.-L.; Feng, X.; Yang, X.-Y.; Ren, J.; Cao, H.-J. Relationship between caffeine intake and infertility: A systematic review of controlled clinical studies. BMC Women’s Health 2020, 20, 125. [Google Scholar] [CrossRef]
- Ricci, E.; Viganò, P.; Cipriani, S.; Somigliana, E.; Chiaffarino, F.; Bulfoni, A.; Parazzini, F. Coffee and caffeine intake and male infertility: A systematic review. Nutr. J. 2017, 16, 37. [Google Scholar] [CrossRef]
- Kasman, A.M.; Thoma, M.E.; McLain, A.C.; Eisenberg, M.L. Association between use of marijuana and time to pregnancy in men and women: Findings from the National Survey of Family Growth. Fertil. Steril. 2018, 109, 866–871. [Google Scholar] [CrossRef]
- Nazmara, Z.; Ebrahimi, B.; Makhdoumi, P.; Noori, L.; Mahdavi, S.A.; Hassanzadeh, G. Effects of illicit drugs on structural and functional impairment of testis, endocrinal disorders, and molecular alterations of the semen. Iran. J. Basic Med. Sci. 2021, 24, 856–867. [Google Scholar] [CrossRef]
- Alghobary, M.; Mostafa, T. Addiction and human male fertility: A systematic review and a critical appraisal. Andrology 2022, 10, 1073–1095. [Google Scholar] [CrossRef]
| Drug | Author | Year | Country | Study Design | Sample Size | Population Description | Outcomes Being Analyzed | Main Findings |
|---|---|---|---|---|---|---|---|---|
| Cannabis | Hehemann et al. | 2021 | U.S. | Prospective | 409 | 71 current users 103 past users | Semen quality | Current use was associated with increased odds of abnormal morphology [OR 2.15, 95%CI: 1.21–3.79] and abnormal semen volume (OR 2.76, 95%CI: 1.19–6.42), while odds of less than WHO reference value sperm motility were reduced (OR 0.47, 95%CI: 0.25–0.91) |
| Cannabis | Carroll et al. | 2020 | Jamaica | Cross-sectional | 229 | 47% current users | Semen quality | Recent- and large-quantity use were 2.6 times (OR 2.6; 95%CI, 1.0–6.8) and 4.3 times (OR 4.3; 95%CI, 1.1–15.9) at greater risk of asthenozoospermia. Moderate quantity users were 3.4 times (OR 3.4; 95%CI, 1.5–7.9) more likely to be diagnosed with teratozoospermia |
| Cannabis | Gundersen et al. | 2015 | Denmark | Prospective | 1215 | 45% recent users | Semen quality, reproductive hormone levels | Regular marijuana smoking associated with a 28% (95%CI: −48, −1) lower sperm concentration and a 29% (95%CI: −46, −1) lower total sperm count. The combined use of marijuana and other recreational drugs reduced the sperm concentration by 52% (95%CI: −68, −27) and total sperm count by 55% (95%CI: −71, −31). Marijuana smokers had higher levels of testosterone |
| Cannabis | Nassan et al. | 2019 | U.S. | Cross-sectional | 662 | 365 patients never used cannabis | Semen quality, reproductive hormone levels | Men who had ever smoked marijuana had significantly higher sperm concentration (62.7 million/mL (95%CI: 56.0, 70.3)) than men who had never smoked marijuana ((45.4 million/mL (38.6, 53.3)). No significant differences in sperm concentration between current and past marijuana smokers. A similar pattern was observed for total sperm count. Marijuana smokers had significantly lower FSH concentrations than never marijuana smokers |
| Opiates/opioids | Nazmara et al. | 2020 | Iran | Case-control | 48 | 24 addicted 24 healthy controls | Semen quality, levels of protamine-2gene and miRNA-122 in seminal plasma | White blood cell count in semen (1.69 ± 0.41 vs. 8.61 ± 1.73, p = 0.001), motility (65.51 ± 2.57 vs. 41.96 ± 3.58, p = 0.001) and survival rate (87.41 ± 1.00 vs. 71.50 ± 4.59, p = 0.002) of sperm cells was significantly different between the healthy and addicted groups. Protamine-2 gene and protein expression in the addicted group were significantly lower than the healthy group, whilst seminal miRNA-122 levels in addicted men were higher than in healthy men |
| Opiates/opioids | Nazmara et al. | 2019 | Iran | Case-control | 50 | 25 heroin abusers 25 healthy controls | Semen quality, sexual hormones levels, sperm histone replacement abnormalities | Sperm motility, viability, and sperm histone replacement abnormalities were significantly different in addicted group vs. non-exposed ones (p < 0.05). Serum sex hormone levels were not significantly different between groups |
| Opiates/opioids | Safarinejad et al. | 2012 | Iran | Case-control | 288 | 142 heroin abusers 146 healthy controls | Semen quality, sperm function, seminal plasma antioxidant capacity, sperm DNA integrity | The mean ± SD sperm concentration in opiate users and in control subjects was 22.2 ± 4.4 and 66.3 ± 8.3 million per ml, respectively (p = 0.002). A significant increase in the amount of fragmented DNA was found in opiate consumers compared with that in controls (36.4 ± 3.8% vs. 27.1 ± 2.4%, p = 0.004). Significantly decreased levels of catalase-like and superoxide dismutase-like activity were observed in heroin abusers |
| Opiates | Bassiony et al. | 2020 | Egypt | Case-control | 90 | 60 tramadol abusers 30 healthy controls | Semen quality, sexual hormones levels | Tramadol abusers had higher prolactin and lower free testosterone levels and they were more likely to have lower sperm counts and higher levels of abnormal motility and abnormal sperm morphology |
| Amphetamine-type stimulants (ATS) | Pham et al. | 2022 | U.S. | Retrospective cohort study | 8861 | 106 men out of the total were prescribed with stimulants for ADHD | Semen quality | Stimulant use was associated with reduced total motile sperm count in the setting of decreased semen volume, but not sperm concentration, motility and morphology |
| Amphetamine-type stimulants (ATS) | Shalev et al. | 2021 | Israel | Retrospective cohort study | 9769 | 293 men out of the total were prescribed with methylphenidate | Semen quality | Methylphenidate exposure did not affect sperm morphology but was associated with increased sperm concentration as well as increased total sperm count and total sperm motility among current and past users |
| Herbal highs/Khat | Hakim et al. | 2002 | Ethiopia | Prospective cross-sectional | 214 | 184 khat users 30 healthy controls | Semen quality | No statistically significant difference in seminal quality parameters between groups |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schifano, N.; Chiappini, S.; Mosca, A.; Miuli, A.; Santovito, M.C.; Pettorruso, M.; Capogrosso, P.; Dehò, F.; Martinotti, G.; Schifano, F. Recreational Drug Misuse and Its Potential Contribution to Male Fertility Levels’ Decline: A Narrative Review. Brain Sci. 2022, 12, 1582. https://doi.org/10.3390/brainsci12111582
Schifano N, Chiappini S, Mosca A, Miuli A, Santovito MC, Pettorruso M, Capogrosso P, Dehò F, Martinotti G, Schifano F. Recreational Drug Misuse and Its Potential Contribution to Male Fertility Levels’ Decline: A Narrative Review. Brain Sciences. 2022; 12(11):1582. https://doi.org/10.3390/brainsci12111582
Chicago/Turabian StyleSchifano, Nicolò, Stefania Chiappini, Alessio Mosca, Andrea Miuli, Maria Chiara Santovito, Mauro Pettorruso, Paolo Capogrosso, Federico Dehò, Giovanni Martinotti, and Fabrizio Schifano. 2022. "Recreational Drug Misuse and Its Potential Contribution to Male Fertility Levels’ Decline: A Narrative Review" Brain Sciences 12, no. 11: 1582. https://doi.org/10.3390/brainsci12111582
APA StyleSchifano, N., Chiappini, S., Mosca, A., Miuli, A., Santovito, M. C., Pettorruso, M., Capogrosso, P., Dehò, F., Martinotti, G., & Schifano, F. (2022). Recreational Drug Misuse and Its Potential Contribution to Male Fertility Levels’ Decline: A Narrative Review. Brain Sciences, 12(11), 1582. https://doi.org/10.3390/brainsci12111582










