Disruptions in Effective Connectivity within and between Default Mode Network and Anterior Forebrain Mesocircuit in Prolonged Disorders of Consciousness
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. MRI Acquisition
2.3. Preprocessing
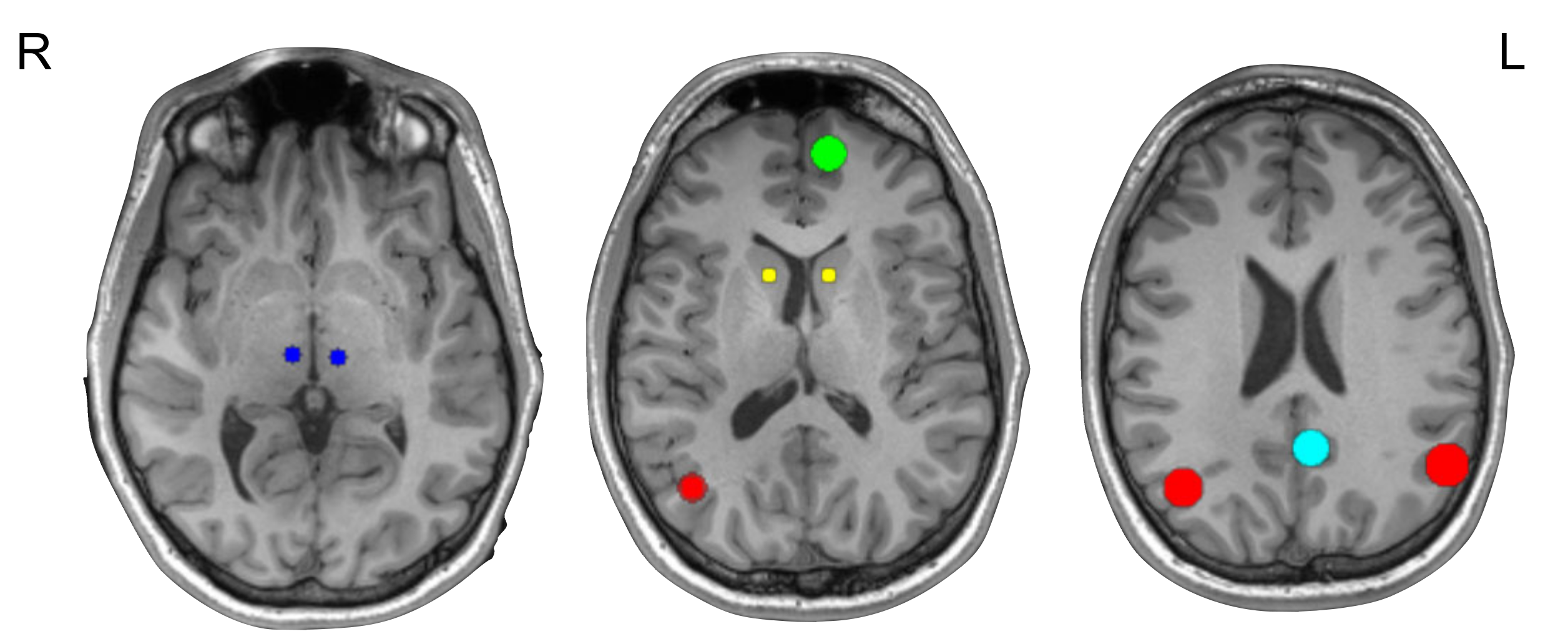
2.4. Selection of ROIs
2.5. General Linear Model
2.6. Dynamic Causal Modelling
2.7. Parameter Estimations—Parametric Empirical Bayes (PEB), Bayesian Model Reduction (BMR) and Bayesian Model Averaging (BMA)
2.8. Correlations with CRS-R
3. Results
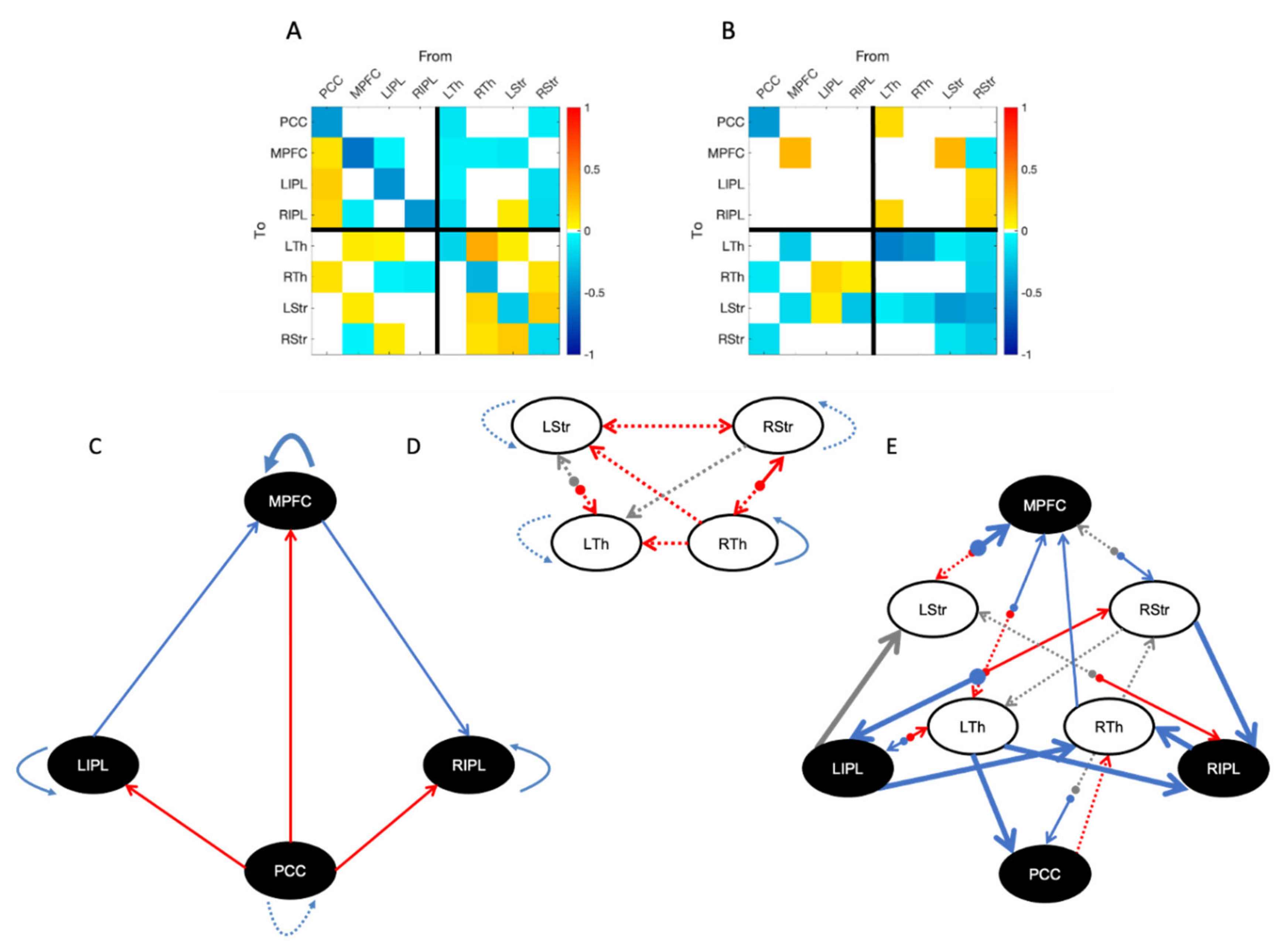
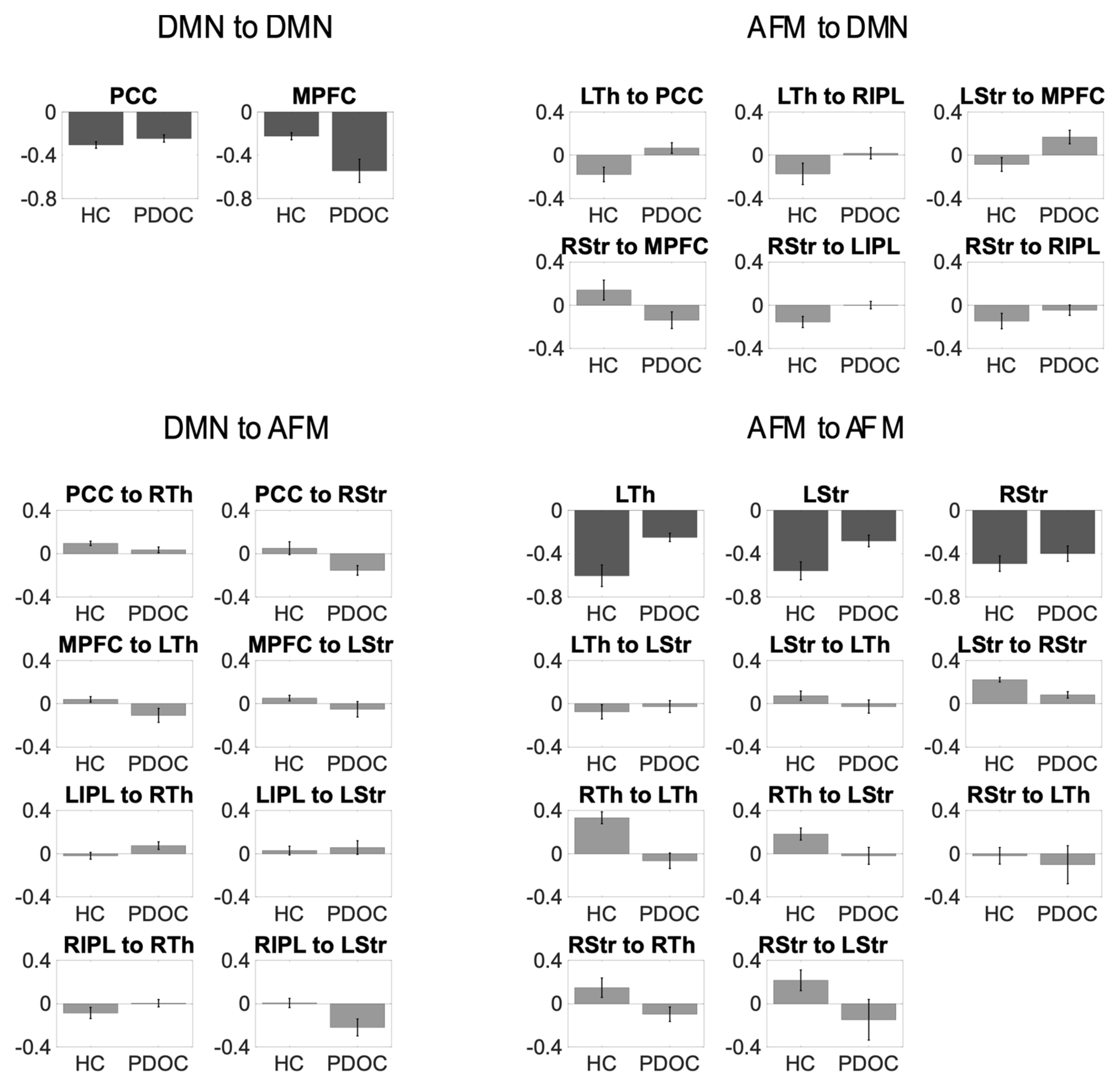
3.1. Effective Connectivity
3.2. CRS-R and Effective Connectivity
4. Discussion
4.1. The AFM and Extrinsic Connections to the DMN
4.2. The DMN and Extrinsic Connections to the AFM
4.3. Clinical Severity
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Stender, J.; Gosseries, O.; Bruno, M.-A.; Charland-Verville, V.; Vanhaudenhuyse, A.; Demertzi, A.; Chatelle, C.; Thonnard, M.; Thibaut, A.; Heine, L.; et al. Diagnostic Precision of PET Imaging and Functional MRI in Disorders of Consciousness: A Clinical Validation Study. Lancet 2014, 384, 514–522. [Google Scholar] [CrossRef]
- Di Perri, C.; Bahri, M.A.; Amico, E.; Thibaut, A.; Heine, L.; Antonopoulos, G.; Charland-Verville, V.; Wannez, S.; Gomez, F.; Hustinx, R.; et al. Neural Correlates of Consciousness in Patients Who Have Emerged from a Minimally Conscious State: A Cross-Sectional Multimodal Imaging Study. Lancet Neurol. 2016, 15, 830–842. [Google Scholar] [CrossRef]
- Snider, S.B.; Edlow, B.L. MRI in Disorders of Consciousness. Curr. Opin. Neurol. 2020, 33, 676–683. [Google Scholar] [CrossRef]
- Boly, M.; Phillips, C.; Tshibanda, L.; Vanhaudenhuyse, A.; Schabus, M.; Dang-Vu, T.T.; Moonen, G.; Hustinx, R.; Maquet, P.; Laureys, S. Intrinsic Brain Activity in Altered States of Consciousness: How Conscious Is the Default Mode of Brain Function? Ann. N. Y. Acad. Sci. 2008, 1129, 119–129. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Espejo, D.; Soddu, A.; Cruse, D.; Palacios, E.M.; Junque, C.; Vanhaudenhuyse, A.; Rivas, E.; Newcombe, V.; Menon, D.K.; Pickard, J.D.; et al. A Role for the Default Mode Network in the Bases of Disorders of Consciousness. Ann. Neurol. 2012, 72, 335–343. [Google Scholar] [CrossRef] [PubMed]
- Crone, J.S.; Schurz, M.; Höller, Y.; Bergmann, J.; Monti, M.; Schmid, E.; Trinka, E.; Kronbichler, M. Impaired Consciousness Is Linked to Changes in Effective Connectivity of the Posterior Cingulate Cortex within the Default Mode Network. NeuroImage 2015, 110, 101–109. [Google Scholar] [CrossRef]
- Fernández-Espejo, D.; Junque, C.; Cruse, D.; Bernabeu, M.; Roig-Rovira, T.; Fábregas, N.; Rivas, E.; Mercader, J.M. Combination of Diffusion Tensor and Functional Magnetic Resonance Imaging during Recovery from the Vegetative State. BMC Neurol. 2010, 10, 77. [Google Scholar] [CrossRef]
- Lant, N.D.; Gonzalez-Lara, L.E.; Owen, A.M.; Fernández-Espejo, D. Relationship between the Anterior Forebrain Mesocircuit and the Default Mode Network in the Structural Bases of Disorders of Consciousness. NeuroImage Clin. 2016, 10, 27–35. [Google Scholar] [CrossRef]
- Cauda, F.; Micon, B.M.; Sacco, K.; Duca, S.; D’Agata, F.; Geminiani, G.; Canavero, S. Disrupted Intrinsic Functional Connectivity in the Vegetative State. J. Neurol. Neurosurg. Psychiatry 2009, 80, 429–431. [Google Scholar] [CrossRef]
- Boly, M.; Tshibanda, L.; Vanhaudenhuyse, A.; Noirhomme, Q.; Schnakers, C.; Ledoux, D.; Boveroux, P.; Garweg, C.; Lambermont, B.; Phillips, C.; et al. Functional Connectivity in the Default Network during Resting State Is Preserved in a Vegetative but Not in a Brain Dead Patient. Hum. Brain Mapp. 2009, 30, 2393–2400. [Google Scholar] [CrossRef]
- Soddu, A.; Vanhaudenhuyse, A.; Bahri, M.A.; Bruno, M.; Boly, M.; Demertzi, A.; Tshibanda, J.; Phillips, C.; Stanziano, M.; Ovadia-Caro, S.; et al. Identifying the Default-mode Component in Spatial IC Analyses of Patients with Disorders of Consciousness. Hum. Brain Mapp. 2011, 33, 778–796. [Google Scholar] [CrossRef]
- Amico, E.; Marinazzo, D.; Di Perri, C.; Heine, L.; Annen, J.; Martial, C.; Dzemidzic, M.; Kirsch, M.; Bonhomme, V.; Laureys, S.; et al. Mapping the Functional Connectome Traits of Levels of Consciousness. NeuroImage 2017, 148, 201–211. [Google Scholar] [CrossRef]
- Vanhaudenhuyse, A.; Noirhomme, Q.; Tshibanda, L.J.F.; Bruno, M.A.; Boveroux, P.; Schnakers, C.; Soddu, A.; Perlbarg, V.; Ledoux, D.; Brichant, J.-F.; et al. Default Network Connectivity Reflects the Level of Consciousness in Non-Communicative Brain-Damaged Patients. Brain 2010, 133, 161–171. [Google Scholar] [CrossRef]
- Gusnard, D.A.; Raichle, M.E. Searching for a Baseline: Functional Imaging and the Resting Human Brain. Nat. Rev. Neurosci. 2001, 2, 685–694. [Google Scholar] [CrossRef]
- Laureys, S.; Goldman, S.; Phillips, C.; Van Bogaert, P.; Aerts, J.; Luxen, A.; Franck, G.; Maquet, P. Impaired Effective Cortical Connectivity in Vegetative State: Preliminary Investigation Using PET. Neuroimage 1999, 9, 377–382. [Google Scholar] [CrossRef]
- Fridman, E.A.; Beattie, B.J.; Broft, A.; Laureys, S.; Schiff, N.D. Regional Cerebral Metabolic Patterns Demonstrate the Role of Anterior Forebrain Mesocircuit Dysfunction in the Severely Injured Brain. Proc. Natl. Acad. Sci. USA 2014, 111, 6473–6478. [Google Scholar] [CrossRef] [PubMed]
- Norton, L.; Hutchison, R.M.; Young, G.B.; Lee, D.H.; Sharpe, M.D.; Mirsattari, S.M. Disruptions of Functional Connectivity in the Default Mode Network of Comatose Patients. Neurology 2012, 78, 175–181. [Google Scholar] [CrossRef] [PubMed]
- Fischer, D.; Threlkeld, Z.D.; Bodien, Y.G.; Kirsch, J.E.; Huang, S.Y.; Schaefer, P.W.; Rapalino, O.; Hochberg, L.R.; Rosen, B.R.; Edlow, B.L. Intact Brain Network Function in an Unresponsive Patient with COVID-19. Ann. Neurol. 2020, 88. [Google Scholar] [CrossRef] [PubMed]
- Buckner, R.L.; Carroll, D.C. Self-Projection and the Brain. Trends Cogn. Sci. 2007, 11, 49–57. [Google Scholar] [CrossRef] [PubMed]
- Schiff, N.D. Recovery of Consciousness after Brain Injury: A Mesocircuit Hypothesis. Trends Neurosci. 2010, 33, 1–9. [Google Scholar] [CrossRef]
- Fernández-Espejo, D.; Bekinschtein, T.; Monti, M.M.; Pickard, J.D.; Junque, C.; Coleman, M.R.; Owen, A.M. Diffusion Weighted Imaging Distinguishes the Vegetative State from the Minimally Conscious State. NeuroImage 2011, 54, 103–112. [Google Scholar] [CrossRef]
- Williams, S.T.; Conte, M.M.; Goldfine, A.M.; Noirhomme, Q.; Gosseries, O.; Thonnard, M.; Beattie, B.; Hersh, J.; Katz, D.I.; Victor, J.D.; et al. Common Resting Brain Dynamics Indicate a Possible Mechanism Underlying Zolpidem Response in Severe Brain Injury. eLife 2013, 2, e01157. [Google Scholar] [CrossRef]
- Brown, E.N.; Lydic, R.; Schiff, N.D. General Anesthesia, Sleep, and Coma. Available online: https://www.nejm.org/doi/10.1056/NEJMra0808281 (accessed on 28 February 2021).
- Fridman, E.A.; Schiff, N.D. Neuromodulation of the Conscious State Following Severe Brain Injuries. Curr. Opin. Neurobiol. 2014, 29, 172–177. [Google Scholar] [CrossRef]
- Chatelle, C.; Thibaut, A.; Gosseries, O.; Bruno, M.-A.; Demertzi, A.; Bernard, C.; Hustinx, R.; Tshibanda, L.; Bahri, M.A.; Laureys, S. Changes in Cerebral Metabolism in Patients with a Minimally Conscious State Responding to Zolpidem. Front. Hum. Neurosci. 2014, 8, 917. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, G.; Santhanam, P.; Hu, X. Instantaneous and Causal Connectivity in Resting State Brain Networks Derived from Functional MRI Data. Neuroimage 2011, 54, 1043–1052. [Google Scholar] [CrossRef] [PubMed]
- Van den Heuvel, M.P.; Sporns, O. Rich-Club Organization of the Human Connectome. J. Neurosci. 2011, 31, 15775–15786. [Google Scholar] [CrossRef]
- Hagmann, P.; Cammoun, L.; Gigandet, X.; Meuli, R.; Honey, C.J.; Van Wedeen, J.; Sporns, O. Mapping the Structural Core of Human Cerebral Cortex. PLoS Biol. 2008, 6, e159. [Google Scholar] [CrossRef]
- Chen, P.; Xie, Q.; Wu, X.; Huang, H.; Lv, W.; Chen, L.; Guo, Y.; Zhang, S.; Hu, H.; Wang, Y.; et al. Abnormal Effective Connectivity of the Anterior Forebrain Regions in Disorders of Consciousness. Neurosci. Bull. 2018, 34, 647–658. [Google Scholar] [CrossRef]
- Giacino, J.T.; Kalmar, K.; Whyte, J. The JFK Coma Recovery Scale-Revised: Measurement Characteristics and Diagnostic Utility. Arch. Phys. Med. Rehabil. 2004, 85, 2020–2029. [Google Scholar] [CrossRef]
- Beukema, S.; Gonzalez-Lara, L.E.; Finoia, P.; Kamau, E.; Allanson, J.; Chennu, S.; Gibson, R.M.; Pickard, J.D.; Owen, A.M.; Cruse, D. A Hierarchy of Event-Related Potential Markers of Auditory Processing in Disorders of Consciousness. NeuroImage Clin. 2016, 12, 359–371. [Google Scholar] [CrossRef] [PubMed]
- Fiacconi, C.M.; Owen, A.M. Using Facial Electromyography to Detect Preserved Emotional Processing in Disorders of Consciousness: A Proof-of-Principle Study. Clin. Neurophysiol. 2016, 127, 3000–3006. [Google Scholar] [CrossRef]
- Gibson, R.M.; Fernández-Espejo, D.; Gonzalez-Lara, L.E.; Kwan, B.Y.; Lee, D.H.; Owen, A.M.; Cruse, D. Multiple Tasks and Neuroimaging Modalities Increase the Likelihood of Detecting Covert Awareness in Patients with Disorders of Consciousness. Front. Hum. Neurosci. 2014, 8. [Google Scholar] [CrossRef] [PubMed]
- Gibson, R.M.; Chennu, S.; Fernández-Espejo, D.; Naci, L.; Owen, A.M.; Cruse, D. Somatosensory Attention Identifies Both Overt and Covert Awareness in Disorders of Consciousness. Ann. Neurol. 2016, 80, 412–423. [Google Scholar] [CrossRef]
- Naci, L.; Owen, A.M. Making Every Word Count for Nonresponsive Patients. JAMA Neurol. 2013, 70, 1235–1241. [Google Scholar] [CrossRef]
- Fernández-Espejo, D.; Rossit, S.; Owen, A.M. Thalamocortical Mechanism for the Absence of Overt Motor Behavior in Covertly Aware Patients. JAMA Neurol. 2015, 72, 1442–1450. [Google Scholar] [CrossRef] [PubMed]
- Yan, C.-G.; Wang, X.-D.; Zuo, X.-N.; Zang, Y.-F. DPABI: Data Processing & Analysis for (Resting-State) Brain Imaging. Neuroinformatics 2016, 14, 339–351. [Google Scholar] [CrossRef] [PubMed]
- Bastos-Leite, A.J.; Ridgway, G.R.; Silveira, C.; Norton, A.; Reis, S.; Friston, K.J. Dysconnectivity within the Default Mode in First-Episode Schizophrenia: A Stochastic Dynamic Causal Modeling Study with Functional Magnetic Resonance Imaging. Schizophr. Bull. 2015, 41, 144–153. [Google Scholar] [CrossRef]
- Di, X.; Biswal, B.B. Identifying the Default Mode Network Structure Using Dynamic Causal Modeling on Resting-State Functional Magnetic Resonance Imaging. NeuroImage 2014, 86, 53–59. [Google Scholar] [CrossRef] [PubMed]
- Li, B.; Wang, X.; Yao, S.; Hu, D.; Friston, K. Task-Dependent Modulation of Effective Connectivity within the Default Mode Network. Front. Psychol. 2012, 3, 206. [Google Scholar] [CrossRef]
- Fox, M.D.; Snyder, A.Z.; Vincent, J.L.; Corbetta, M.; Van Essen, D.C.; Raichle, M.E. The Human Brain Is Intrinsically Organized into Dynamic, Anticorrelated Functional Networks. Proc. Natl. Acad. Sci. USA 2005, 102, 9673–9678. [Google Scholar] [CrossRef]
- Di Martino, A.; Scheres, A.; Margulies, D.S.; Kelly, A.M.C.; Uddin, L.Q.; Shehzad, Z.; Biswal, B.; Walters, J.R.; Castellanos, F.X.; Milham, M.P. Functional Connectivity of Human Striatum: A Resting State FMRI Study. Cereb. Cortex 2008, 18, 2735–2747. [Google Scholar] [CrossRef] [PubMed]
- Brett, M.; Anton, J.; Valabrègue, R.; Poline, J.B. Region of Interest Analysis Using an SPM Toolbox. Available online: /paper/Region-of-interest-analysis-using-an-SPM-toolbox-Brett-Anton/19ba0249dcada4bbdc3366d37e1f3362f324e904 (accessed on 11 February 2021).
- Friston, K.J.; Kahan, J.; Biswal, B.; Razi, A. A DCM for Resting State FMRI. NeuroImage 2014, 94, 396–407. [Google Scholar] [CrossRef]
- Friston, K.J.; Litvak, V.; Oswal, A.; Razi, A.; Stephan, K.E.; van Wijk, B.C.; Ziegler, G.; Zeidman, P. Bayesian Model Reduction and Empirical Bayes for Group (DCM) Studies. NeuroImage 2016, 128, 413–431. [Google Scholar] [CrossRef]
- Zeidman, P.; Jafarian, A.; Seghier, M.L.; Litvak, V.; Cagnan, H.; Price, C.J.; Friston, K.J. A Tutorial on Group Effective Connectivity Analysis, Part 2: Second Level Analysis with PEB. NeuroImage 2019, 200, 12–25. [Google Scholar] [CrossRef] [PubMed]
- Litvak, V.; Garrido, M.; Zeidman, P.; Friston, K. Empirical Bayes for Group (DCM) Studies: A Reproducibility Study. Front. Hum. Neurosci. 2015, 9, 670. [Google Scholar] [CrossRef] [PubMed]
- JASP; Version 0.14.1 [Computer Software]; JASP Team: 2020. Available online: https://jasp-stats.org/ (accessed on 1 April 2021).
- Thibaut, A.; Schiff, N.; Giacino, J.; Laureys, S.; Gosseries, O. Therapeutic Interventions in Patients with Prolonged Disorders of Consciousness. Lancet Neurol. 2019, 18, 600–614. [Google Scholar] [CrossRef]
- Schiff, N.D. Posterior Medial Corticothalamic Connectivity and Consciousness. Ann. Neurol. 2012, 72, 305–306. [Google Scholar] [CrossRef] [PubMed]
- Vanhaudenhuyse, A.; Demertzi, A.; Schabus, M.; Noirhomme, Q.; Bredart, S.; Boly, M.; Phillips, C.; Soddu, A.; Luxen, A.; Moonen, G.; et al. Two Distinct Neuronal Networks Mediate the Awareness of Environment and of Self. J. Cogn. Neurosci. 2011, 23, 570–578. [Google Scholar] [CrossRef]
- Sharp, D.J.; Beckmann, C.F.; Greenwood, R.; Kinnunen, K.M.; Bonnelle, V.; De Boissezon, X.; Powell, J.H.; Counsell, S.J.; Patel, M.C.; Leech, R. Default Mode Network Functional and Structural Connectivity after Traumatic Brain Injury. Brain 2011, 134, 2233–2247. [Google Scholar] [CrossRef]
- Lutkenhoff, E.S.; Chiang, J.; Tshibanda, L.; Kamau, E.; Kirsch, M.; Pickard, J.D.; Laureys, S.; Owen, A.M.; Monti, M.M. Thalamic and Extrathalamic Mechanisms of Consciousness after Severe Brain Injury. Ann. Neurol. 2015, 78, 68–76. [Google Scholar] [CrossRef]
- Fernández-Espejo, D.; Junque, C.; Bernabeu, M.; Roig-Rovira, T.; Vendrell, P.; Mercader, J.M. Reductions of Thalamic Volume and Regional Shape Changes in the Vegetative and the Minimally Conscious States. J. Neurotrauma 2010, 27, 1187–1193. [Google Scholar] [CrossRef] [PubMed]
- Lutkenhoff, E.S.; Wright, M.J.; Shrestha, V.; Real, C.; McArthur, D.L.; Buitrago-Blanco, M.; Vespa, P.M.; Monti, M.M. The Subcortical Basis of Outcome and Cognitive Impairment in TBI: A Longitudinal Cohort Study. Neurology 2020, 95, e2398–e2408. [Google Scholar] [CrossRef]
- Rosazza, C.; Andronache, A.; Sattin, D.; Bruzzone, M.G.; Marotta, G.; Nigri, A.; Ferraro, S.; Rossi Sebastiano, D.; Porcu, L.; Bersano, A.; et al. Multimodal Study of Default-Mode Network Integrity in Disorders of Consciousness. Ann. Neurol. 2016, 79, 841–853. [Google Scholar] [CrossRef] [PubMed]
- Cain, J.A.; Spivak, N.M.; Coetzee, J.P.; Crone, J.S.; Johnson, M.A.; Lutkenhoff, E.S.; Real, C.; Buitrago-Blanco, M.; Vespa, P.M.; Schnakers, C.; et al. Ultrasonic Thalamic Stimulation in Chronic Disorders of Consciousness. Brain Stimul. Basic Transl. Clin. Res. Neuromodulation 2021, 14, 301–303. [Google Scholar] [CrossRef]
- Boly, M.; Massimini, M.; Tsuchiya, N.; Postle, B.R.; Koch, C.; Tononi, G. Are the Neural Correlates of Consciousness in the Front or in the Back of the Cerebral Cortex? Clinical and Neuroimaging Evidence. J. Neurosci. 2017, 37, 9603–9613. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Zhang, L.; Guo, Y.; Shi, L.; Gao, J.; Wang, X.; Hu, Y. Effects of High-Definition Transcranial Direct-Current Stimulation on Resting-State Functional Connectivity in Patients With Disorders of Consciousness. Front. Hum. Neurosci. 2020, 14, 560586. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Bai, Y.; Xia, X.; Li, J.; Wang, X.; Dai, Y.; Dang, Y.; He, J.; Liu, C.; Zhang, H. Effects of Long-Lasting High-Definition Transcranial Direct Current Stimulation in Chronic Disorders of Consciousness: A Pilot Study. Front. Neurosci. 2019, 13, 412. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Liu, Y.; Zheng, Y.; Li, D.; Liang, X.; Chen, Y.; Cui, Y.; Yap, P.-T.; Qiu, S.; Zhang, H.; et al. Large-Scale Dynamic Causal Modeling of Major Depressive Disorder Based on Resting-State Functional Magnetic Resonance Imaging. Hum. Brain Mapp. 2020, 41, 865–881. [Google Scholar] [CrossRef]
- Sharaev, M.G.; Zavyalova, V.V.; Ushakov, V.L.; Kartashov, S.I.; Velichkovsky, B.M. Effective Connectivity within the Default Mode Network: Dynamic Causal Modeling of Resting-State FMRI Data. Front. Hum. Neurosci. 2016, 10, 14. [Google Scholar] [CrossRef]
- Liu, X.; Li, J.; Gao, J.; Zhou, Z.; Meng, F.; Pan, G.; Luo, B. Association of Medial Prefrontal Cortex Connectivity with Consciousness Level and Its Outcome in Patients with Acquired Brain Injury. J. Clin. Neurosci. 2017, 42, 160–166. [Google Scholar] [CrossRef]
- Silva, S.; de Pasquale, F.; Vuillaume, C.; Riu, B.; Loubinoux, I.; Geeraerts, T.; Seguin, T.; Bounes, V.; Fourcade, O.; Demonet, J.-F.; et al. Disruption of Posteromedial Large-Scale Neural Communication Predicts Recovery from Coma. Neurology 2015, 85, 2036–2044. [Google Scholar] [CrossRef] [PubMed]
- Demertzi, A.; Gómez, F.; Crone, J.S.; Vanhaudenhuyse, A.; Tshibanda, L.; Noirhomme, Q.; Thonnard, M.; Charland-Verville, V.; Kirsch, M.; Laureys, S.; et al. Multiple FMRI System-Level Baseline Connectivity Is Disrupted in Patients with Consciousness Alterations. Cortex 2014, 52, 35–46. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Zou, Q.; Hu, J.; Tang, W.; Mao, Y.; Gao, L.; Zhu, J.; Jin, Y.; Lu, L.; Zhang, Y.; et al. Intrinsic Functional Connectivity Patterns Predict Consciousness Level and Recovery Outcome in Acquired Brain Injury. J. Neurosci. 2015, 35, 12932–12946. [Google Scholar] [CrossRef] [PubMed]
- Friston, K.J. Functional and Effective Connectivity: A Review. Brain Connect. 2011, 1, 13–36. [Google Scholar] [CrossRef]
| Patient No. | Sex | Age (y) | Interval Since Ictus (Months) | Etiology | Diagnosis | CRS-R on Day of Scan | Max CRS-R on Week of Scan | Auditory Function | Visual Function | Motor Function | Oromotor/ Verbal | Communication | Arousal | Number of CRS-R Scores Taken on Week of Scan |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Male | 38 | 150 | Traumatic | VS | 6 | 6 | 1 | 0 | 2 | 1 | 0 | 2 | 1 |
| 2 | Male | 33 | 176 | Non-Traumatic | MCS | 9 | 10 | 1 | 3 | 2 | 1 | 0 | 2–3 | 5 |
| 3 | Male | 27 | 88 | Traumatic | VS | 7 | 7 | 1–2 | 0–1 | 2 | 1 | 0 | 1–2 | 5 |
| 4 | Female | 44 | 245 | Traumatic | VS | 3 | 5 | 0–1 | 0–1 | 0–2 | 0–1 | 0 | 0–2 | 4 |
| 5 | Female | 46 | 230 | Non-Traumatic | MCS | - | 10 | 1–2 | 3 | 2 | 1 | 0 | 1–2 | 2 |
| 6 | Male | 57 | 37 | Non-Traumatic | VS | - | 6 | 1 | 0–1 | 0–2 | 1 | 0 | 1–2 | 3 |
| 7 | Male | 27 | 36 | Non-Traumatic | MCS | - | 13 | 3 | 3 | 0–2 | 2 | 0 | 3 | 3 |
| 8 | Female | 20 | 67 | Non-Traumatic | VS | 6 | 8 | 1–2 | 0–1 | 1–2 | 1 | 0 | 2 | 4 |
| 9 | Female | 35 | 24 | Non-Traumatic | VS | 5 | 5 | 0–1 | 0 | 0–2 | 1 | 0 | 1–2 | 3 |
| 10 | Male | 19 | 2 | Non-Traumatic | VS | 6–7 | 7 | 2 | 1 | 1 | 0–1 | 0 | 2 | 3 |
| 11 | Female | 25 | 68 | Traumatic | MCS | 8 | 9 | 1–2 | 3 | 1 | 1 | 0 | 2 | 5 |
| 12 | Female | 43 | 55 | Non-Traumatic | VS | 5 | 7 | 1 | 0–1 | 2 | 1 | 0 | 1–2 | 3 |
| 13 | Male | 20 | 48 | Non-Traumatic | VS | 5 | 6 | 1 | 0–1 | 0–2 | 1 | 0 | 1–2 | 3 |
| 14 | Female | 51 | 11 | Non-Traumatic | VS | 4 | 4 | 3–4 | 1 | 0–1 | 0–1 | 0 | 1 | 5 |
| 15 | Female | 52 | 78 | Non-Traumatic | VS | 6 | 6 | 1 | 0 | 1–2 | 1 | 0 | 1–2 | 4 |
| 16 | Male | 40 | 38 | Traumatic | MCS | 7 | 7 | 1 | 0–3 | 0–1 | 0–1 | 0 | 1–2 | 5 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Coulborn, S.; Taylor, C.; Naci, L.; Owen, A.M.; Fernández-Espejo, D. Disruptions in Effective Connectivity within and between Default Mode Network and Anterior Forebrain Mesocircuit in Prolonged Disorders of Consciousness. Brain Sci. 2021, 11, 749. https://doi.org/10.3390/brainsci11060749
Coulborn S, Taylor C, Naci L, Owen AM, Fernández-Espejo D. Disruptions in Effective Connectivity within and between Default Mode Network and Anterior Forebrain Mesocircuit in Prolonged Disorders of Consciousness. Brain Sciences. 2021; 11(6):749. https://doi.org/10.3390/brainsci11060749
Chicago/Turabian StyleCoulborn, Sean, Chris Taylor, Lorina Naci, Adrian M. Owen, and Davinia Fernández-Espejo. 2021. "Disruptions in Effective Connectivity within and between Default Mode Network and Anterior Forebrain Mesocircuit in Prolonged Disorders of Consciousness" Brain Sciences 11, no. 6: 749. https://doi.org/10.3390/brainsci11060749
APA StyleCoulborn, S., Taylor, C., Naci, L., Owen, A. M., & Fernández-Espejo, D. (2021). Disruptions in Effective Connectivity within and between Default Mode Network and Anterior Forebrain Mesocircuit in Prolonged Disorders of Consciousness. Brain Sciences, 11(6), 749. https://doi.org/10.3390/brainsci11060749






