Tinnitus and Metacognitive Beliefs—Results of a Cross-Sectional Observational Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample and Setting
2.2. Measures
2.2.1. Tinnitus Sample Case History (TSCH)
2.2.2. Tinnitus Handicap Inventory (THI)
2.2.3. Beck Anxiety Inventory (BAI)
2.2.4. Beck Depression Inventory (BDI)
2.2.5. Metacognition Questionnaire-30 (MCQ-30)
2.2.6. Penn State Worry Questionnaire (PSWQ)
2.2.7. Tonal Audiometry
2.3. Statistical Analyses
3. Results
3.1. Meta-Cognitions in Patients with Tinnitus
3.2. The Association of Tinnitus Distress with Meta-Cognitions, Anxiety, Depression and Worry
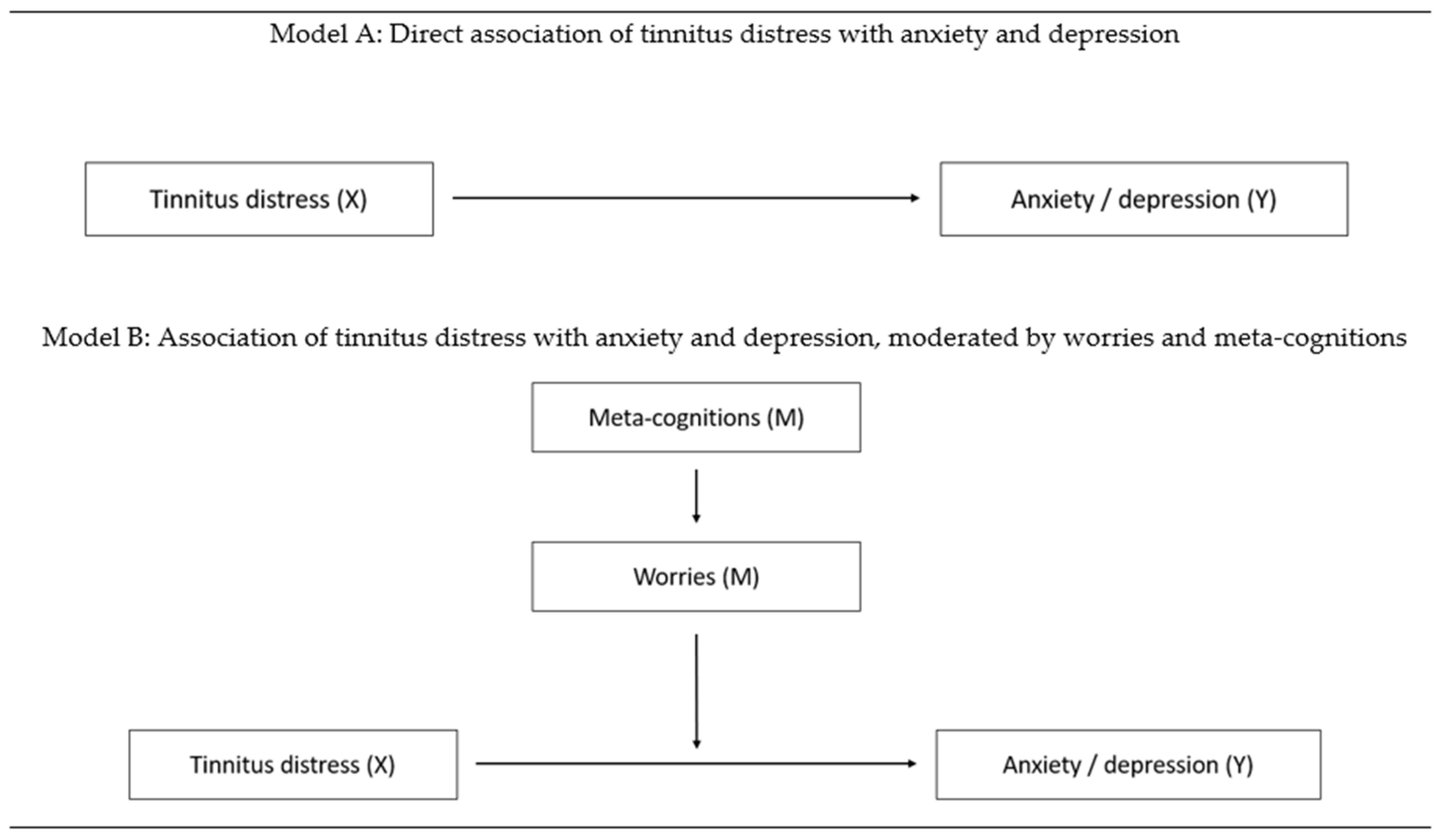
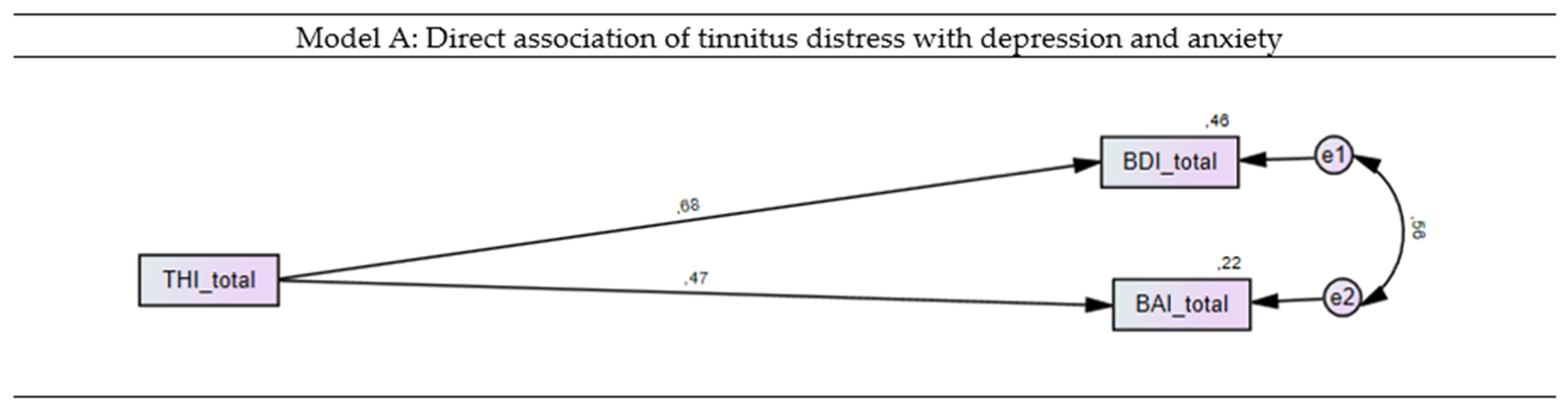
3.3. Direct Association of Tinnitus Distress with Depression and Anxiety
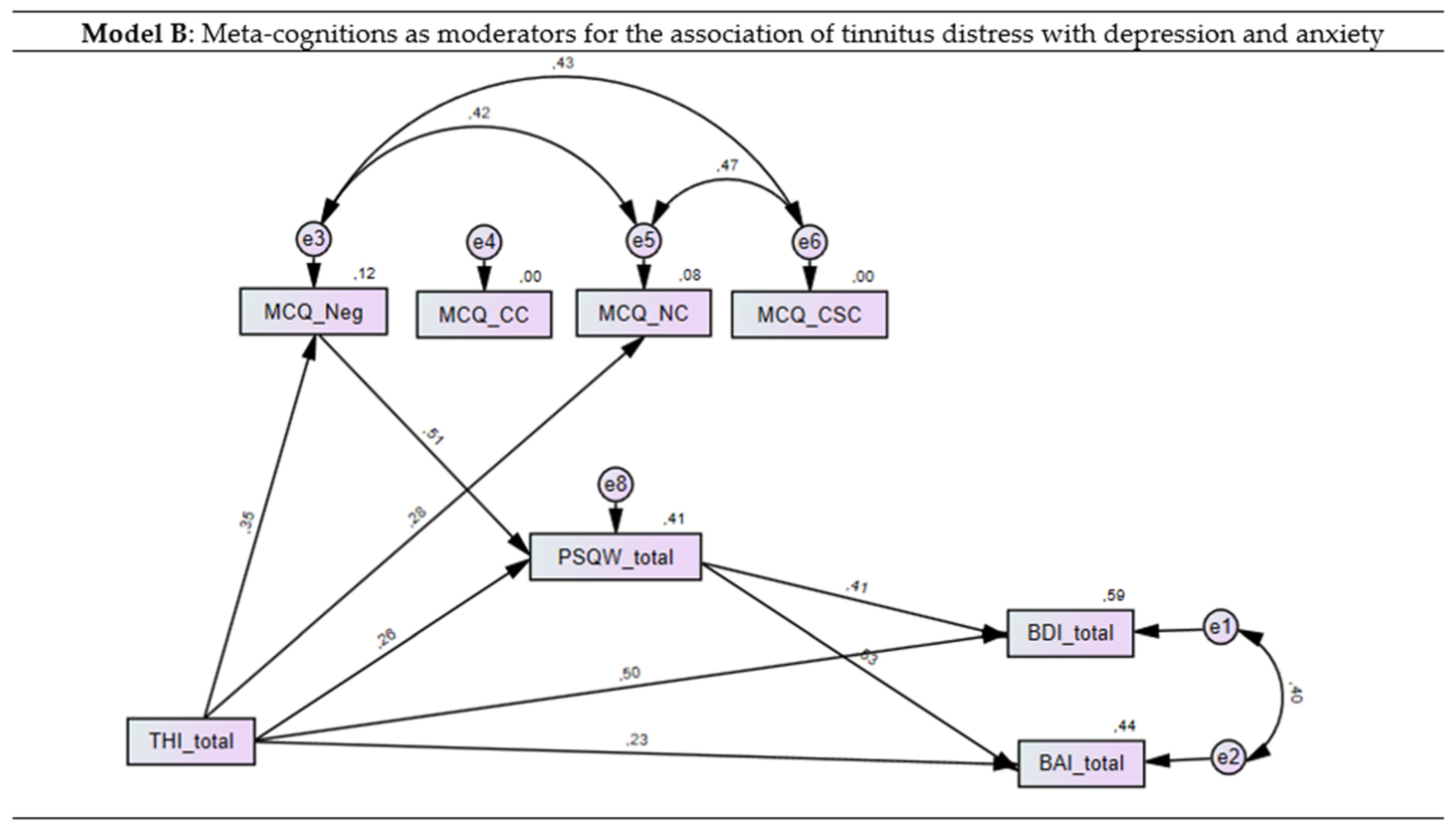
3.4. Meta-Cognitions and Worries as Moderators for the Association of Tinnitus Distress with Anxiety and Depression
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Cima, R.F.F.; Mazurek, B.; Haider, H.; Kikidis, D.; Lapira, A.; Norena, A.; Hoare, D.J. A multidisciplinary European guideline for tinnitus: Diagnostics, assessment, and treatment. HNO 2019, 67, 10–42. [Google Scholar] [CrossRef] [PubMed]
- Henry, J.A.; Dennis, K.C.; Schechter, M.A. General review of tinnitus: Prevalence, mechanisms, effects, and management. JSLHR 2005, 48, 1204–1235. [Google Scholar] [CrossRef]
- Baguley, D.; McFerran, D.; Hall, D. Tinnitus. Lancet 2013, 382, 1600–1607. [Google Scholar] [CrossRef]
- Kara, E.; Aydin, K.; Akbulut, A.A.; Karakol, S.N.; Durmaz, S.; Yener, H.M.; Gozen, E.D.; Kara, H. Assessment of Hidden Hearing Loss in Normal Hearing Individuals with and Without Tinnitus. J. Int. Adv. Otol. 2020, 16, 87–92. [Google Scholar] [CrossRef]
- Edvall, N.K.; Gunan, E.; Genitsaridi, E.; Lazar, A.; Mehraei, G.; Billing, M.; Tullberg, M.; Bulla, J.; Whitton, J.; Canlon, B.; et al. Impact of Temporomandibular Joint Complaints on Tinnitus-Related Distress. Front. Neurosci. 2019, 13, 879. [Google Scholar] [CrossRef]
- Haider, H.F.; Hoare, D.J.; Costa, R.F.P.; Potgieter, I.; Kikidis, D.; Lapira, A.; Nikitas, C.; Caria, H.; Cunha, N.T.; Paço, J.C. Pathophysiology, Diagnosis and Treatment of Somatosensory Tinnitus: A Scoping Review. Front. Neurosci. 2017, 11, 207. [Google Scholar] [CrossRef]
- Shore, S.E.; Roberts, L.E.; Langguth, B. Maladaptive plasticity in tinnitus--triggers, mechanisms and treatment. Nat. Rev. Neurol. 2016, 12, 150–160. [Google Scholar] [CrossRef]
- Schlee, W.; Pryss, R.C.; Probst, T.; Schobel, J.; Bachmeier, A.; Reichert, M.; Langguth, B. Measuring the Moment-to-Moment Variability of Tinnitus: The TrackYourTinnitus Smart Phone App. Front. Aging Neurosci. 2016, 8, 294. [Google Scholar] [CrossRef]
- Pattyn, T.; Van Den Eede, F.; Vanneste, S.; Cassiers, L.; Veltman, D.J.; Van De Heyning, P.; Sabbe, B.C.G. Tinnitus and anxiety disorders: A review. Hear. Res. 2016, 333, 255–265. [Google Scholar] [CrossRef]
- Bhatt, J.M.; Bhattacharyya, N.; Lin, H.W. Relationships between tinnitus and the prevalence of anxiety and depression. Laryngoscope 2017, 127, 466–469. [Google Scholar] [CrossRef]
- Trevis, K.J.; McLachlan, N.M.; Wilson, S.J. A systematic review and meta-analysis of psychological functioning in chronic tinnitus. Clin. Psychol. Rev. 2018, 60, 62–86. [Google Scholar] [CrossRef] [PubMed]
- Salazar, J.W.; Meisel, K.; Smith, E.R.; Quiggle, A.; Mccoy, D.B.; Amans, M.R. Depression in Patients with Tinnitus: A Systematic Review. Otolaryngol. Head Neck Surg. 2019, 161, 28–35. [Google Scholar] [CrossRef] [PubMed]
- Capobianco, L.; Faija, C.; Husain, Z.; Wells, A. Metacognitive beliefs and their relationship with anxiety and depression in physical illnesses: A systematic review. PLoS ONE 2020, 15, e0238457. [Google Scholar] [CrossRef] [PubMed]
- Lenzo, V.; Sardella, A.; Martino, G.; Quattropani, M.C. A Systematic Review of Metacognitive Beliefs in Chronic Medical Conditions. Front. Psychol. 2020, 10, 2875. [Google Scholar] [CrossRef] [PubMed]
- Wells, A.; Purdon, C.L. Metacognition and cognitive-behaviour therapy: A special issue. Clin. Psychol. Psychother. 1999, 6, 71–72. [Google Scholar] [CrossRef]
- Wells, A. Emotional Disorders and Metacognition: Innovative Cognitive Therapy; John Wiley & Sons Ltd.: Baffins Lane, UK, 2000; p. 103. [Google Scholar]
- Allott, R.; Wells, A.; Morrison, A.P.; Waller, R. Distress in Parkinson’s disease: Contributions of disease fac- tors and metacognitive style. Br. J. Psychiatry 2005, 187, 182–183. [Google Scholar] [CrossRef] [PubMed]
- Brown, R.G.; Fernie, B.A. Metacognitions, anxiety, and distress related to motor fluctuations in Parkinson’s disease. J. Psychosom. Res. 2015, 78, 143–148. [Google Scholar] [CrossRef]
- Compare, A.; Brugnera, A.; Spada, M.M.; Zarbo, C.; Tasca, G.A.; Sassaroli, S.; Caselli, G.; Ruggiero, G.M.; Wittstein, I. The Role of Emotional Competence in Takotsubo Cardiomyopathy. Psychosom. Med. 2018, 80, 377–384. [Google Scholar] [CrossRef]
- Fisher, P.L.; Noble, A.J. Anxiety and depression in people with epilepsy: The contribution of metacognitive beliefs. Seizure 2017, 50, 153–159. [Google Scholar] [CrossRef]
- Fisher, P.L.; Reilly, J.; Noble, A. Metacognitive beliefs and illness perceptions are associated with emotional distress in people with epilepsy. Epilepsy Behav. 2018, 86, 9–14. [Google Scholar] [CrossRef]
- Ferraro, L.; Barbera, D.L.; Messina, A.; Galioto, S.; Marinaro, A.; Caruso, C.; Rizzo, R.; Cascia, C.L. Metacognitive Therapy in Patients with Tinnitus: A Single Group Study. J. Contemp. Psychother. 2019, 49, 133–140. [Google Scholar] [CrossRef]
- Caldirola, D.; Teggi, R.; Dacco, S.; Sangiorgio, E.; Bussi, M.; Perna, G. Role of worry in patients with chronic tinnitus and sensorineural hearing loss: A preliminary study. Eur. Arch. Otorhinolaryngol. 2016, 273, 4145–4151. [Google Scholar] [CrossRef] [PubMed]
- Langguth, B.; Goodey, R.; Azevedo, A.; Bjorne, A.; Cacace, A.; Crocetti, A.; Del Bo, L.; De Ridder, D.; Diges, I.; Elbert, T.; et al. Consensus for tinnitus patient assessment and treatment outcome measurement: Tinnitus Research Initiative meeting, Regensburg, July 2006. Prog. Brain Res. 2007, 166, 525–536. [Google Scholar] [PubMed]
- Newman, C.W.; Jacobson, G.P.; Spitzer, J.B. Development of the Tinnitus Handicap Inventory. Arch. Otolaryngol. Head Neck Surg. 1996, 122, 143–148. [Google Scholar] [CrossRef] [PubMed]
- Passi, S.; Ralli, G.; Capparelli, E.; Mammone, A.; Scacciatelli, D.; Cianfrone, G. The THI questionnaire: Psychometric data for reliability and validity of the Italian version. Int. Tinnitus J. 2008, 14, 26–33. [Google Scholar] [PubMed]
- Salviati, M.; Macri, F.; Terlizzi, S.; Melcore, C.; Provenzano, A.; Capparelli, E.; Altissimi, G.; Cianfrone, G. The Tinnitus Handicap Inventory as a screening test for psychiatric comorbidity in patients with tinnitus. Psychosomatics 2013, 54, 248–256. [Google Scholar] [CrossRef]
- Altissimi, G.; Salviati, M.; Turchetta, R.; Orlando, M.P.; Greco, A.; De Vincentiis, M.; Ciofalo, A.; Marinelli, C.; Testugini, V.; Mazzei, F.; et al. When alarm bells ring: Emergency tinnitus. Eur. Rev. Med. Pharmacol. Sci. 2016, 20, 2955–2973. [Google Scholar]
- Beck, A.T.; Epstein, N.; Brown, G.; Steer, R.A. An inventory for measuring clinical anxiety: Psychometric properties. J. Consult. Clin. Psychol. 1988, 56, 893–897. [Google Scholar] [CrossRef]
- Sica, C.; Ghisi, M. The Italian versions of the Beck Anxiety Inventory and the Beck Depression Inventory-II: Psychometric properties and discriminant power. In Leading-Edge Psychological Tests and Testing Research; Lange, M.A., Ed.; Nova Science Publishers: Hauppauge, NY, USA, 2007; pp. 27–50. [Google Scholar]
- Beck, A.T.; Steer, R.A.; Brown, G.K. Manual for the Beck Depression Inventory–II; Psychological Corporation: San Antonio, TX, USA, 1996. [Google Scholar]
- Montano, A.; Flebus, G.B. Presentation of the Beck Depression Inventory—Second edition (BDI-II): Confirmation of bifactorial structure in a sample of the Italian population. Psicoter. Cogn. Comport. 2006, 12, 67–82. [Google Scholar]
- Wells, A.; Cartwright-Hatton, S. A short form of the metacognitions questionnaire: Properties of the MCQ-30. Behav. Res. Ther. 2004, 42, 385–396. [Google Scholar] [CrossRef]
- Quattropani, M.C.; Lenzo, V.; Mucciardi, M.; Toffle, M.E. Psychometric properties of the Italian version of the Short Form of the Metacognitions Questionnaire (MCQ-30). BPA 2014, 269, 29–41. [Google Scholar]
- Meyer, T.J.; Miller, M.L.; Metzger, R.L.; Borkovec, T.D. Development and validation of the Penn State Worry Questionnaire. Behav. Res. Ther. 1990, 28, 487–495. [Google Scholar] [CrossRef]
- Morani, S.; Pricci, D.; Sanavio, E. “Penn State Worry Questionnaire” e “Worry Domains Questionnaire”. Presentazione delle versioni italiane ed analisi della fedeltà. Psicoter. Cogn. Comport. 1999, 5, 13–34. [Google Scholar]
- McKenna, L.; Handscomb, L.; Hoare, D.J.; Hall, D.A. A scientific cognitive-behavioral model of tinnitus: Novel conceptualizations of tinnitus distress. Front. Neurol. 2014, 5, 196. [Google Scholar] [CrossRef]
- Leaver, A.M.; Seydell-Greenwald, A.; Rauschecker, J.P. Auditory-limbic interactions in chronic tinnitus: Challenges for neuroimaging research. Hear. Res. 2016, 334, 49–57. [Google Scholar] [CrossRef]
- Yuki, S.; Nakatani, H.; Nakai, T.; Okanoya, K.; Tachibana, R.O. Regulation of action selection based on metacognition in humans via a ventral and dorsal medial prefrontal cortical network. Cortex 2019, 119, 336–349. [Google Scholar] [CrossRef]
- Strumila, R.; Lengvenyte, A.; Vainutiene, V.; Lesinskas, E. The role of questioning environment, personality traits, depressive and anxiety symptoms in tinnitus severity perception. Psychiatr. Q. 2017, 88, 865–877. [Google Scholar] [CrossRef]
- Ziai, K.; Moshtaghi, O.; Mahboubi, H.; Djalilian, H.R. Tinnitus Patients Suffering from Anxiety and Depression: A Review. Int. Tinnitus J. 2017, 21, 68–73. [Google Scholar] [CrossRef]
- Huntley, C.D.; Fisher, P.L. Examining the role of positive and negative metacognitive beliefs in depression. Scand. J. Psychol. 2016, 57, 446–452. [Google Scholar] [CrossRef]
- Ryum, T.; Kennair, L.; Hjemdal, O.; Hagen, R.; Halvorsen, J.Ø.; Solem, S. Worry and Metacognitions as Predictors of Anxiety Symptoms: A Prospective Study. Front. Psychol. 2017, 8, 924. [Google Scholar] [CrossRef]
- Cook, S.A.; Salmon, P.; Dunn, G.; Holcombe, C.; Cornford, P.; Fisher, P. The association of metacognitive beliefs with emotional distress after diagnosis of cancer. Health Psychol. 2015, 34, 207–215. [Google Scholar] [CrossRef] [PubMed]
- Purewal, R.; Fisher, P.L. The contribution of illness perceptions and metacognitive beliefs to anxiety and depression in adults with diabetes. Diabetes Res. Clin. Pract. 2018, 136, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Tunkel, D.E.; Bauer, C.A.; Sun, G.H.; Rosenfeld, R.M.; Chandrasekhar, S.S.; Cunningham, E.R., Jr.; Archer, S.M.; Blakley, B.W.; Carter, J.M.; Granieri, E.C.; et al. Clinical practice guideline: Tinnitus. Otolaryngol. Head Neck Surg. 2014, 151 (Suppl. 2), S1–S40. [Google Scholar] [CrossRef] [PubMed]
- Aazh, H.; Baguley, D.M.; Moore, B.C.J. Factors Related to Insomnia in Adult Patients with Tinnitus and/or Hyperacusis: An Exploratory Analysis. J. Am. Acad. Audiol. 2019, 30, 802–809. [Google Scholar] [CrossRef]
- Meric, C.; Gartner, M.; Collet, L.; Chery-Croze, S. Psychopathological profile of tinnitus sufferers: Evidence concerning the relationship between tinnitus features and impact on life. Audiol. Neurootol. 1998, 3, 240–252. [Google Scholar] [CrossRef]
- Durai, M.; Searchfield, G. Anxiety and depression, personality traits relevant to tinnitus: A scoping review. Int. J. Audiol. 2016, 55, 605–615. [Google Scholar] [CrossRef]
- Gomaa, M.A.; Elmagd, M.H.; Elbadry, M.M.; Kader, R.M. Depression, Anxiety and Stress Scale in patients with tinnitus and hearing loss. Eur. Arch. Otorhinolaryngol. 2014, 271, 2177–2184. [Google Scholar] [CrossRef]
- Udupi, V.A.; Uppunda, A.K.; Mohan, K.M.; Alex, J.; Mahendra, M.H. The relationship of perceived severity of tinnitus with depression, anxiety, hearing status, age and gender in individuals with tinnitus. Int. Tinnitus J. 2013, 18, 29–34. [Google Scholar] [CrossRef]
- Budd, R.J.; Pugh, R. Tinnitus coping style and its relationship to tinnitus severity and emotional distress. J. Psychosom. Res. 1996, 41, 327–335. [Google Scholar] [CrossRef]
- Beck, A.T. Cognitive Therapy and the Emotional Disorders; International Universities Press: New York, NY, USA, 1976. [Google Scholar]
- Wells, A. Metacognitive Therapy for Anxiety and Depression; Guilford Press: New York, NY, USA, 2009. [Google Scholar]
- Handscomb, L.E.; Hall, D.A.; Shorter, G.W.; Hoare, D.J. Positive and Negative Thinking in Tinnitus: Factor Structure of the Tinnitus Cognitions Questionnaire. Ear Hear. 2017, 38, 126–132. [Google Scholar] [CrossRef]
- Conrad, I.; Kleinstäuber, M.; Jasper, K.; Hiller, W.; Andersson, G.; Weise, C. The Role of Dysfunctional Cognitions in Patients with Chronic Tinnitus. Ear Hear. 2015, 36, e279–e289. [Google Scholar] [CrossRef] [PubMed]
| Mean | (SD) | |
|---|---|---|
| Age | 49.1 | (13.9) |
| Tinnitus loudness (0–100) | 52.2 | (24.7) |
| Awareness of tinnitus a | 79.8 | (28.0) |
| Annoyed by tinnitus a | 49.8 | (32.7) |
| N | % | |
| Tinnitus: family history | 31 | 29.0% |
| Missing | 5 | 4.7% |
| Duration tinnitus | ||
| <3 months | 17 | 15.9% |
| 3–6 months | 7 | 6.7% |
| >6 months | 81 | 77.1% |
| Missing | 2 | 1.9% |
| Tinnitus perception at onset | ||
| Gradual | 71 | 78.9% |
| Abrupt | 19 | 21.1% |
| Missing | 17 | 15.9% |
| Pulsating tinnitus | 18 | 17.1% |
| Missing | 2 | 1.9% |
| Tinnitus location | ||
| right ear | 15 | 14.2% |
| left ear | 23 | 21.7% |
| both ears | 62 | 58.5% |
| inside the head | 6 | 5.7% |
| Missing | 1 | 0.9% |
| Tinnitus loudness varies from day to day | 34 | 32.4% |
| Missing | 2 | 1.9% |
| Tinnitus manifestation | ||
| Intermittent | 23 | 22.5% |
| Constant | 79 | 77.5% |
| Missing | 5 | 4.7% |
| Tinnitus sound | ||
| Tone | 49 | 48.5% |
| Noise | 24 | 23.8% |
| Crickets | 10 | 9.9% |
| Other | 18 | 17.8% |
| Missing | 6 | 5.6% |
| Objective hearing problem b | 68 | 63.6% |
| Missing | ||
| Subjective hearing problem | 63 | 61.8% |
| Missing | 5 | 4.7% |
| Hyperacusis | 67 | 66.3% |
| Missing | 6 | 5.6% |
| Headache | 65 | 61.9% |
| Missing | 2 | 1.9% |
| Vertigo/dizziness | 79 | 76.0 |
| Missing | 3 | 2.8% |
| Temporomandibular disorder | 34 | 33.7% |
| Missing | 6 | 5.6% |
| Neck pain | 60 | 57.7% |
| Missing | 3 | 2.8% |
| Other pain | 27 | 27.6% |
| Missing | 9 | 8.4% |
| MCQ Pos | MCQ Neg | MCQ CC | MCQ NC | MCQ CSC | |
|---|---|---|---|---|---|
| MCQ pos | - | 0.26 ** | 0.26 ** | 0.34 *** | 0.39 *** |
| MCQ neg | - | - | 0.11 | 0.49 *** | 0.43 *** |
| MCQ CC | - | - | - | 0.094 | 0.085 |
| MCQ NC | - | - | - | - | 0.47 *** |
| MCQ CSC | - | - | - | - | - |
| MCQ Pos | MCQ Neg | MCQ CC | MCQ NC | MCQ CSC | |
|---|---|---|---|---|---|
| THI total score | 0.13 | 0.38 *** | 0.15 | 0.32 ** | 0.10 |
| BDI | −0.16 | 0.51 *** | 0.23 * | 0.29 ** | 0.19 |
| BAI | 0.02 | 0.50 *** | 0.33 ** | 0.26 ** | 0.15 |
| PSWQ total score | 0.11 | 0.61 *** | 0.20 * | 0.31 ** | 0.36 *** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Natalini, E.; Fioretti, A.; Riedl, D.; Moschen, R.; Eibenstein, A. Tinnitus and Metacognitive Beliefs—Results of a Cross-Sectional Observational Study. Brain Sci. 2021, 11, 3. https://doi.org/10.3390/brainsci11010003
Natalini E, Fioretti A, Riedl D, Moschen R, Eibenstein A. Tinnitus and Metacognitive Beliefs—Results of a Cross-Sectional Observational Study. Brain Sciences. 2021; 11(1):3. https://doi.org/10.3390/brainsci11010003
Chicago/Turabian StyleNatalini, Eleonora, Alessandra Fioretti, David Riedl, Roland Moschen, and Alberto Eibenstein. 2021. "Tinnitus and Metacognitive Beliefs—Results of a Cross-Sectional Observational Study" Brain Sciences 11, no. 1: 3. https://doi.org/10.3390/brainsci11010003
APA StyleNatalini, E., Fioretti, A., Riedl, D., Moschen, R., & Eibenstein, A. (2021). Tinnitus and Metacognitive Beliefs—Results of a Cross-Sectional Observational Study. Brain Sciences, 11(1), 3. https://doi.org/10.3390/brainsci11010003






