Using Light for Therapy of Glioblastoma Multiforme (GBM)
Abstract
1. Introduction
2. The Problem
3. Development of the Concept of PDT
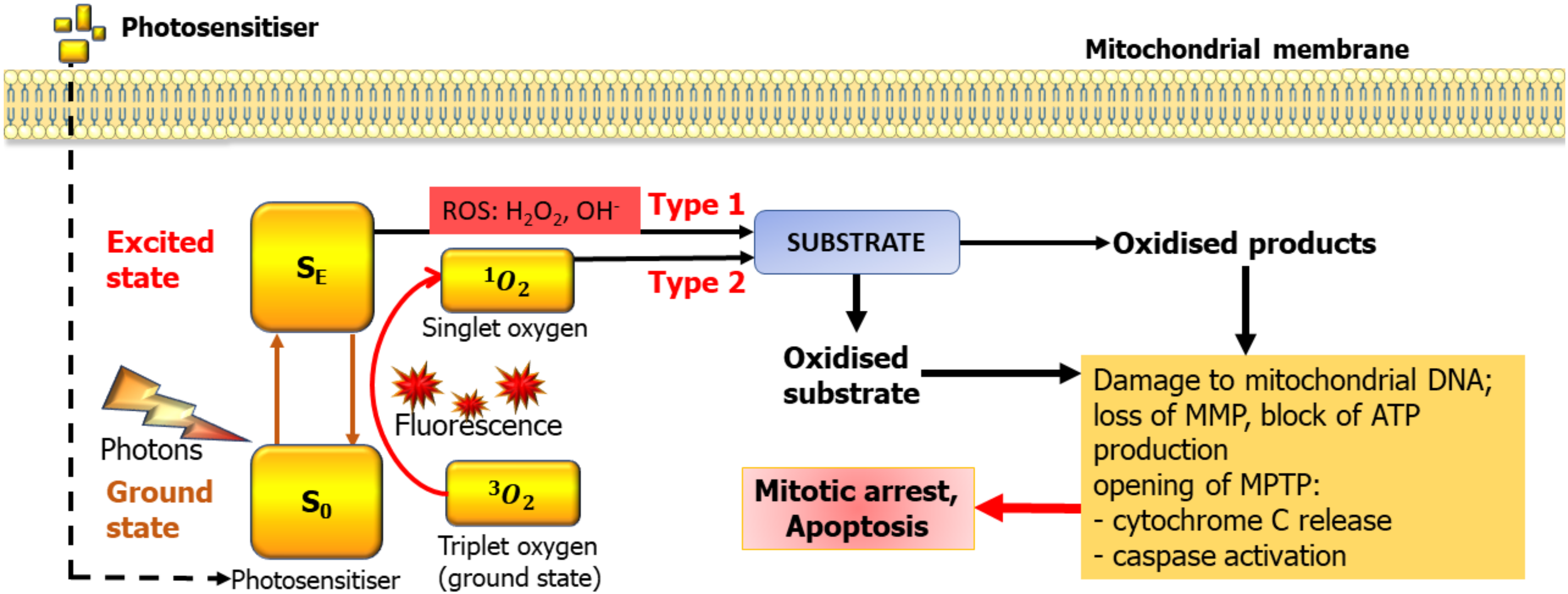
4. Principles of PDT
5. PDT of GBM with Porphyrins
6. Technical Aspects of Light Delivery into the Brain
7. Challenges for Development of PDT for GBM
8. Mitochondria as a Target for PDT
9. Conclusions
10. Perspectives
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Jiang, Y.; Uhrbom, L. On the origin of glioma. Ups. J. Med. Sci. 2012, 117, 113–121. [Google Scholar] [CrossRef] [PubMed]
- Florian, I.S.; Ungureanu, G.; Berce, C. Risk factors for gliomas. An extensive review. Rom. Neurosurg. 2013, 20, 5–21. [Google Scholar] [CrossRef]
- Ostrom, Q.T.; Bauchet, L.; Davis, F.G.; Deltour, I.; Fisher, J.L.; Langer, C.E.; Pekmezci, M.; Schwartzbaum, J.A.; Turner, M.C.; Walsh, K.M.; et al. The epidemiology of glioma in adults: A state of the science review. Neuro-Oncology 2014, 16, 896–913. [Google Scholar] [CrossRef] [PubMed]
- Louis, D.N.; Perry, A.; Reifenberger, G.; von Deimling, A.; Figarella-Branger, D.; Cavenee, W.K.; Ohgaki, H.; Wiestler, O.D.; Kleihues, P.; Ellison, D.W. The 2016 World Health Organization Classification of Tumors of the Central Nervous System: A summary. Acta Neuropathol. 2016, 131, 803–820. [Google Scholar] [CrossRef]
- Perry, A.; Wesseling, P. Histologic classification of gliomas. In Handbook of Clinical Neurology; Elsevier: Amsterdam, The Netherlands, 2016; Volume 134, pp. 71–95. ISBN 9780128029978. [Google Scholar]
- Thon, N.; Kreth, S.; Kreth, F.W. Personalized treatment strategies in glioblastoma: MGMT promoter methylation status. Onco Targets Ther. 2013, 6, 1363–1372. [Google Scholar] [CrossRef]
- Koschmann, C.; Lowenstein, P.R.; Castro, M.G. ATRX mutations and glioblastoma: Impaired DNA damage repair, alternative lengthening of telomeres, and genetic instability. Mol. Cell. Oncol. 2016, 3. [Google Scholar] [CrossRef]
- Liu, J.; Zhang, X.; Yan, X.; Sun, M.E.I.; Fan, Y.; Huang, Y. Significance of TERT and ATRX mutations in glioma. Oncol. Lett. 2019, 17, 95–102. [Google Scholar] [CrossRef]
- Zhao, Z.; Zhang, K.; Wang, Z.; Wang, K.; Liu, X.; Wu, F.A.N.; Chen, J. A comprehensive review of available omics data resources and molecular profiling for precision glioma studies (Review). Biomed. Rep. 2019, 10, 3–9. [Google Scholar] [CrossRef]
- Lara-Velazquez, M.; Al-Kharboosh, R.; Jeanneret, S.; Vazquez-Ramos, C.; Mahato, D.; Tavanaiepour, D.; Rahmathulla, G.; Quinone-Hinojosa, A. Advances in brain tumor surgery for glioblastoma in adults. Brain Sci. 2017, 7, 166. [Google Scholar] [CrossRef] [PubMed]
- Bharathiraja, S.; Seo, H.; Manivasagan, P.; Moorthy, M.S.; Park, S.; Oh, J. In vitro photodynamic effect of phycocyanin against breast cancer cells. Molecules 2016, 21, 1470. [Google Scholar] [CrossRef]
- Kawazoe, K.; Isomoto, H.; Yamaguchi, N.; Inoue, N.; Uehara, R.; Matsushima, K.; Ichikawa, T.; Takeshima, F.; Nonaka, T.; Nanashima, A.; et al. Effects of photodynamic therapy for superficial esophageal squamous cell carcinoma in vivo and in vitro. Oncol. Lett. 2010, 1, 877–882. [Google Scholar] [CrossRef] [PubMed]
- Fakhar-e-Alam, M.; Usman Ali, S.M.; Ali, S.; Firdous, S.; Atif, M.; Ibupoto, Z.H.; Willander, M.; Kashif, M.; Hashim, U. Photodynamic damage in liver carcinoma HepG2 cells. In Proceedings of the International Conference on Biomedical Engineering (ICoBE), Penang, Malaysia, 27–28 February 2012; Institute of Electrical and Electronics Engineers (IEEE): Piscataway, NJ, USA, 2012; pp. 237–241. [Google Scholar]
- Abdulrehman, G.; Xv, K.; Li, Y.; Kang, L. Effects of meta-tetrahydroxyphenylchlorin photodynamic therapy on isogenic colorectal cancer SW480 and SW620 cells with different metastatic potentials. Lasers Med. Sci. 2018, 33, 1581–1590. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, A.F.; De Almeida, D.R.Q.; Terra, L.F.; Baptista, M.S.; Labriola, L. Photodynamic therapy in cancer treatment—An update review. J. Cancer Metastasis Treat. 2019, 5, 1–20. [Google Scholar] [CrossRef]
- DiRisio, A.C.; Goswami, H.; Shi, C.; Yunusa, I.; Smith, T.R.; Mekary, R.A.; Broekman, M.L. P09.53 The timing of postoperative chemoradiation treatment (Stupp Protocol) after GBM resection: A systematic review. Neuro Oncol. 2017, 19, iii82. [Google Scholar] [CrossRef][Green Version]
- Sewell, J.; Pan, E. Current Challenges in the Treatment of Glioblastoma. Clin. Oncol. 2016, 1, 1–2. [Google Scholar]
- Castano, A.P.; Demidova, T.N.; Hamblin, M.R. Mechanisms in photodynamic therapy: Part three—Photosensitizer pharmacokinetics, biodistribution, tumor localization and modes of tumor destruction. Photodiagnosis Photodyn. Ther. 2005, 2, 91–106. [Google Scholar] [CrossRef]
- Dolmans, D.E.J.G.J.; Fukumura, D.; Jain, R.K. Photodynamic therapy for cancer. Nat. Rev. Cancer 2003, 3, 380–387. [Google Scholar] [CrossRef] [PubMed]
- Dougherty, T.J.; Gomer, C.J.; Henderson, B.W.; Jori, G.; Kessel, D.; Korbelik, M.; Moan, J.; Peng, Q. Photodynamic therapy. J. Natl. Cancer Inst. 1998, 90, 889–905. [Google Scholar] [CrossRef]
- Dougherty, T.J. Photodynamic therapy (PDT) of malignant tumors. Crit. Rev. Oncol. Hematol. 1984, 2, 83–116. [Google Scholar] [CrossRef]
- Kelly, J.F.; Snell, M.E. Hematoporphyrin derivative: A possible aid in the diagnosis and therapy of carcinoma of the bladder. J. Urol. 1976, 115, 150–151. [Google Scholar] [CrossRef]
- Tomio, L.; Zorat, P.L.; Corti, L.; Calzavara, F.; Reddi, E.; Jori, G. Effect of hematoporphyrin and red light on AH-130 solid tumors in rats. Acta Radiol. Oncol. Radiat. Ther. Phys. Biol. 1983, 22, 49–53. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Diamond, I.; Mcdonagh, A.; Wilson, C.; Granelli, S.; Nielsen, S.; Jaenicke, R. Photodynamic therapy of malignant tumours. Lancet 1972, 300, 1175–1177. [Google Scholar] [CrossRef]
- Perria, C.; Capuzzo, T.; Cavagnaro, G.; Datti, R.; Francaviglia, N.; Rivano, C.; Tercero, V.E. Fast attempts at the photodynamic treatment of human gliomas. J. Neurosurg. Sci. 1980, 24, 119–129. [Google Scholar] [PubMed]
- Popovic, E.A.; Kaye, A.H.; Hill, J.S. Photodynamic therapy of brain tumors. Semin. Surg. Oncol. 1995, 11, 335–345. [Google Scholar] [CrossRef] [PubMed]
- Rosenthal, M.A.; Kavar, B.; Uren, S.; Kaye, A.H. Promising survival in patients with high-grade gliomas following therapy with a novel boronated porphyrin. J. Clin. Neurosci. 2003, 10, 425–427. [Google Scholar] [CrossRef]
- Stylli, S.S.; Kaye, A.H.; MacGregor, L.; Howes, M.; Rajendra, P. Photodynamic therapy of high grade glioma—Long term survival. J. Clin. Neurosci. 2005, 12, 389–398. [Google Scholar] [CrossRef]
- Muller, P.J.; Wilson, B.C. Photodynamic therapy of brain tumors—A work in progress. Lasers Surg. Med. 2006, 38, 384–389. [Google Scholar] [CrossRef]
- Kostron, H.; Fiegele, T.; Akatuna, E. Combination of FOSCAN® mediated fluorescence guided resection and photodynamic treatment as new therapeutic concept for malignant brain tumors. Med. Laser Appl. 2006, 21, 285–290. [Google Scholar] [CrossRef]
- Stepp, H.; Beck, T.; Pongratz, T.; Meinel, T.; Kreth, F.-W.; Tonn, J.C.; Stummer, W. ALA and malignant glioma: Fluorescence-guided resection and photodynamic treatment. J. Environ. Pathol. Toxicol. Oncol. 2007, 26, 157–164. [Google Scholar] [CrossRef]
- Beck, T.J.; Kreth, F.W.; Beyer, W.; Mehrkens, J.H.; Obermeier, A.; Stepp, H.; Stummer, W.; Baumgartner, R. Interstitial photodynamic therapy of nonresectable malignant glioma recurrences using 5-aminolevulinic acid induced protoporphyrin IX. Lasers Surg. Med. 2007, 39, 386–393. [Google Scholar] [CrossRef]
- Eljamel, M.S.; Goodman, C.; Moseley, H. ALA and Photofrin® Fluorescence-guided resection and repetitive PDT in glioblastoma multiforme: A single centre Phase III randomised controlled trial. Lasers Med. Sci. 2008, 23, 361–367. [Google Scholar] [CrossRef] [PubMed]
- Kaneko, S. Recent advances in PDD and PDT for malignant brain tumors. In Proceedings of the 6th Asian Pacific Laser Symposium, Nagoya, Japan, 30 January–1 February 2008. [Google Scholar]
- Akimoto, J.; Haraoka, J.; Aizawa, K. Preliminary clinical report on safety and efficacy of photodynamic therapy using talaporfin sodium for malignant gliomas. Photodiagnosis Photodyn. Ther. 2012, 9, 91–99. [Google Scholar] [CrossRef] [PubMed]
- Lyons, M.; Phang, I.; Eljamel, S. The effects of PDT in primary malignant brain tumours could be improved by intraoperative radiotherapy. Photodiagnosis Photodyn. Ther. 2012, 9, 40–45. [Google Scholar] [CrossRef] [PubMed]
- Johansson, A.; Faber, F.; Kniebühler, G.; Stepp, H.; Sroka, R.; Egensperger, R.; Beyer, W.; Kreth, F.W. Protoporphyrin IX fluorescence and photobleaching during interstitial photodynamic therapy of malignant gliomas for early treatment prognosis. Lasers Surg. Med. 2013, 45, 225–234. [Google Scholar] [CrossRef]
- Muragaki, Y.; Akimoto, J.; Maruyama, T.; Iseki, H.; Ikuta, S.; Nitta, M.; Maebayashi, K.; Saito, T.; Okada, Y.; Kaneko, S.; et al. Phase II clinical study on intraoperative photodynamic therapy with talaporfin sodium and semiconductor laser in patients with malignant brain tumors. J. Neurosurg. 2013, 119, 845–852. [Google Scholar] [CrossRef]
- Abrahamse, H.; Hamblin, M.R. New photosensitizers for photodynamic therapy. Biochem. J. 2016, 473, 347–364. [Google Scholar] [CrossRef]
- Baptista, M.S.; Cadet, J.; Di Mascio, P.; Ghogare, A.A.; Greer, A.; Hamblin, M.R.; Lorente, C.; Nunez, S.C.; Ribeiro, M.S.; Thomas, A.H.; et al. Type I and Type II Photosensitized Oxidation Reactions: Guidelines and Mechanistic Pathways. Photochem. Photobiol. 2017. [Google Scholar] [CrossRef]
- Akimoto, J. Photodynamic Therapy for Malignant Brain Tumors. Jpn. J. Neursurg. 2016, 25, 905–911. [Google Scholar] [CrossRef]
- Robertson, C.A.; Evans, D.H.; Abrahamse, H. Photodynamic therapy (PDT): A short review on cellular mechanisms and cancer research applications for PDT. J. Photochem. Photobiol. B Biol. 2009, 96, 1–8. [Google Scholar] [CrossRef]
- Zhao, B.; He, Y.Y. Recent advances in the prevention and treatment of skin cancer using photodynamic therapy. Expert Rev. Anticancer Ther. 2010, 10, 1797–1809. [Google Scholar] [CrossRef]
- Yano, T.; Hatogai, K.; Morimoto, H.; Yoda, Y.; Kaneko, K. Photodynamic therapy for esophageal cancer. Ann. Transl. Med. 2014, 2. [Google Scholar]
- Moghissi, K.; Dixon, K.; Thorpe, J.A.C.; Stringer, M.; Oxtoby, C. Photodynamic therapy (PDT) in early central lung cancer: A treatment option for patients ineligible for surgical resection. Thorax 2007, 62, 391–395. [Google Scholar] [CrossRef] [PubMed]
- Moghissi, K.; Dixon, K.; Gibbins, S. A Surgical View of Photodynamic Therapy in Oncology: A Review. Surg. J. 2015, 1, e1–e15. [Google Scholar]
- Mahmoudi, K.; Garvey, K.L.; Bouras, A.; Cramer, G.; Stepp, H.; Jesu Raj, J.G.; Bozec, D.; Busch, T.M.; Hadjipanayis, C.G. 5-aminolevulinic acid photodynamic therapy for the treatment of high-grade gliomas. J. Neurooncol. 2019, 141, 595–607. [Google Scholar] [CrossRef]
- Stummer, W.; Stocker, S.; Wagner, S.; Stepp, H.; Fritsch, C.; Goetz, C.; Goetz, A.E.; Kiefmann, R.; Reulen, H.J. Intraoperative detection of malignant gliomas by 5-aminolevulinic acid-induced porphyrin fluorescence. Neurosurgery 1998, 42, 518–526. [Google Scholar]
- Valdés, P.A.; Leblond, F.; Anthony, K.; Harris, B.T.; Wilson, B.C.; Fan, X.; Tosteson, T.D.; Hartov, A.; Ji, S.; Erkmen, K.; et al. Quantitative fluorescence in intracranial tumor: Implications for ALA-induced PpIX as an intraoperative biomarker—Clinical article. J. Neurosurg. 2011, 115, 11–17. [Google Scholar] [CrossRef]
- Stummer, W.; Tonn, J.C.; Goetz, C.; Ullrich, W.; Stepp, H.; Bink, A.; Pietsch, T.; Pichlmeier, U. 5-Aminolevulinic acid-derived tumor fluorescence: The diagnostic accuracy of visible fluorescence qualities as corroborated by spectrometry and histology and postoperative imaging. Neurosurgery 2014, 74, 310–319. [Google Scholar] [CrossRef]
- Olzowy, B.; Hundt, C.S.; Stocker, S.; Bise, K.; Reulen, H.J.; Stummer, W. Photoirradiation therapy of experimental malignant glioma with 5-aminolevulinic acid. J. Neurosurg. 2002, 97, 970–976. [Google Scholar] [CrossRef]
- De Oliveira Silva, F.R.; Bellini, M.H.; Tristão, V.R.; Schor, N.; Vieira, N.D.; Courrol, L.C. Intrinsic fluorescence of protoporphyrin IX from blood samples can yield information on the growth of prostate tumours. J. Fluoresc. 2010, 20, 1159–1165. [Google Scholar] [CrossRef]
- Shimizu, K.; Nitta, M.; Komori, T.; Maruyama, T.; Yasuda, T.; Fujii, Y.; Masamune, K.; Kawamata, T.; Maehara, T.; Muragaki, Y. Intraoperative photodynamic diagnosis using talaporfin sodium simultaneously applied for photodynamic therapy against malignant glioma: A prospective clinical study. Front. Neurol. 2018, 9. [Google Scholar] [CrossRef]
- Akimoto, J.; Fukami, S.; Ichikawa, M.; Mohamed, A.; Kohno, M. Intraoperative photodiagnosis for malignant glioma using photosensitizer talaporfin sodium. Front. Surg. 2019, 6. [Google Scholar] [CrossRef] [PubMed]
- Dupont, C.; Vermandel, M.; Leroy, H.A.; Quidet, M.; Lecomte, F.; Delhem, N.; Mordon, S.; Reyns, N. INtraoperative photoDYnamic Therapy for GliOblastomas (INDYGO): Study Protocol for a Phase i Clinical Trial. Clin. Neurosurg. 2019, 84, E414–E419. [Google Scholar] [CrossRef]
- Regula, J.; MacRobert, A.J.; Gorchein, A.; Buonaccorsi, G.A.; Thorpe, S.M.; Spencer, G.M.; Hatfield, A.R.W.; Bown, S.G. Photosensitisation and photodynamic therapy of oesophageal, duodenal, and colorectal tumours using 5 aminolaevulinic acid induced protoporphyrin IX—A pilot study. Gut 1995, 36, 67–75. [Google Scholar] [CrossRef]
- Schwake, M.; Nemes, A.; Dondrop, J.; Schroeteler, J.; Schipmann, S.; Senner, V.; Stummer, W.; Ewelt, C. In-Vitro Use of 5-ALA for Photodynamic Therapy in Pediatric Brain Tumors. Neurosurgery 2018, 83, 1328–1337. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Gu, Y.; Zuo, Z.; Huang, N. Choosing optimal wavelength for photodynamic therapy of port wine stains by mathematic simulation. J. Biomed. Opt. 2011, 16, 98001. [Google Scholar] [CrossRef] [PubMed]
- Afonso, S.G.; Enríquez de Salamanca, R.; Batlle, A.M. The photodynamic and non-photodynamic actions of porphyrins. Braz. J. Med. Biol. Res./Rev. Bras. Pesqui. Med. Biol. 1999, 32, 255–266. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.Y.; Luk, S.K.; Chuang, C.P.; Yip, S.P.; To, S.S.T.; Yung, Y.M.B. TP53 regulates human AlkB homologue 2 expression in glioma resistance to Photofrin-mediated photodynamic therapy. Br. J. Cancer 2010, 103, 362–369. [Google Scholar] [CrossRef]
- Kammerer, R.; Buchner, A.; Palluch, P.; Pongratz, T.; Oboukhovskij, K.; Beyer, W.; Johansson, A.; Stepp, H.; Baumgartner, R.; Zimmermann, W. Induction of immune mediators in glioma and prostate cancer cells by non-lethal photodynamic therapy. PLoS ONE 2011, 6. [Google Scholar] [CrossRef]
- Namatame, H.; Akimoto, J.; Matsumura, H.; Haraoka, J.; Aizawa, K. Photodynamic therapy of C6-implanted glioma cells in the rat brain employing second-generation photosensitizer talaporfin sodium. Photodiagnosis Photodyn. Ther. 2008, 5, 198–209. [Google Scholar] [CrossRef]
- Miki, Y.; Akimoto, J.; Omata, H.; Moritake, K.; Hiranuma, M.; Hironaka, C.; Fujiwara, Y.; Beppu, M. Concomitant treatment with temozolomide enhances apoptotic cell death in glioma cells induced by photodynamic therapy with talaporfin sodium. Photodiagnosis Photodyn. Ther. 2014, 11, 556–564. [Google Scholar] [CrossRef]
- Miki, Y.; Akimoto, J.; Moritake, K.; Hironaka, C.; Fujiwara, Y. Photodynamic therapy using talaporfin sodium induces concentration-dependent programmed necroptosis in human glioblastoma T98G cells. Lasers Med. Sci. 2015, 30, 1739–1745. [Google Scholar] [CrossRef] [PubMed]
- Inglut, C.T.; Baglo, Y.; Liang, B.J.; Cheema, Y.; Stabile, J.; Woodworth, G.F.; Huang, H.C. Systematic Evaluation of Light-Activatable Biohybrids for Anti-Glioma Photodynamic Therapy. J. Clin. Med. 2019, 8, 1269. [Google Scholar] [CrossRef] [PubMed]
- Fisher, C.J.; Niu, C.; Foltz, W.; Chen, Y.; Sidorova-Darmos, E.; Eubanks, J.H.; Lilge, L. ALA-PpIX mediated photodynamic therapy of malignant gliomas augmented by hypothermia. PLoS ONE 2017, 12. [Google Scholar] [CrossRef] [PubMed]
- Yuan, S.X.; Li, J.L.; Xu, X.K.; Chen, W.; Chen, C.; Kuang, K.Q.; Wang, F.Y.; Wang, K.; Li, F.C. Underlying mechanism of the photodynamic activity of hematoporphyrin-induced apoptosis in U87 glioma cells. Int. J. Mol. Med. 2018, 41, 2288–2296. [Google Scholar] [CrossRef] [PubMed]
- Gillet, J.P.; Varma, S.; Gottesman, M.M. The clinical relevance of cancer cell lines. J. Natl. Cancer Inst. 2013, 105, 452–458. [Google Scholar] [CrossRef] [PubMed]
- Bady, P.; Diserens, A.C.; Castella, V.; Kalt, S.; Heinimann, K.; Hamou, M.F.; Delorenzi, M.; Hegi, M.E. DNA fingerprinting of glioma cell lines and considerations on similarity measurements. Neuro Oncol. 2012, 14, 701–711. [Google Scholar] [CrossRef]
- Allen, M.; Bjerke, M.; Edlund, H.; Nelander, S.; Westermark, B. Origin of the U87MG glioma cell line: Good news and bad news. Sci. Transl. Med. 2016, 8. [Google Scholar] [CrossRef]
- Smith, S.J.; Diksin, M.; Chhaya, S.; Sairam, S.; Estevez-Cebrero, M.A.; Rahman, R. The invasive region of glioblastoma defined by 5ALA guided surgery has an altered cancer stem cell marker profile compared to central Tumour. Int. J. Mol. Sci. 2017, 18, 2452. [Google Scholar]
- Ding, H.; Yu, H.; Dong, Y.; Tian, R.; Huang, G.; Boothman, D.A.; Sumer, B.D.; Gao, J. Photoactivation switch from type II to type i reactions by electron-rich micelles for improved photodynamic therapy of cancer cells under hypoxia. J. Control. Release 2011, 156, 276–280. [Google Scholar] [CrossRef]
- Wang, Y.; Lei, T.; Wang, Z. Minimally invasive neuronavigator-guided microsurgery and photodynamic therapy for gliomas. J. Huazhong Univ. Sci. Technol. Med. Sci. 2009, 29, 395–398. [Google Scholar] [CrossRef]
- Bisland, S.K.; Lilge, L.; Lin, A.; Rusnov, R.; Wilson, B.C. Metronomic photodynamic therapy as a new paradigm for photodynamic therapy: Rationale and preclinical evaluation of technical feasibility for treating malignant brain tumors. Photochem. Photobiol. 2004, 80, 22–30. [Google Scholar] [CrossRef] [PubMed]
- Castro, D.J.; Saxton, R.E.; Fetterman, H.R.; Castro, D.J.; Ward, P.H. Rhodamine-123 as a new photochemosensitizing agent with the argon laser: “nonthermal” and thermal effects on human squamous carcinoma cells in vitro. Laryngoscope 1987, 97, 554–561. [Google Scholar] [CrossRef] [PubMed]
- Powers, S.K.; Pribil, S.; Gillespie, G.Y.; Watkins, P.J. Laser photochemotherapy of rhodamine-123 sensitized human glioma cells in vitro. J. Neurosurg. 1986, 64, 918–923. [Google Scholar] [CrossRef] [PubMed]
- Nadakavukaren, K.K.; Nadakavukaren, J.J.; Chen, L.B. Increased rhodamine 123 uptake by carcinoma cells. Cancer Res. 1985, 45, 6093–6099. [Google Scholar] [PubMed]
- Appaix, F.; Girod, S.; Boisseau, S.; Römer, J.; Vial, J.C.; Albrieux, M.; Maurin, M.; Depaulis, A.; Guillemain, I.; van der Sanden, B. Specific in vivo staining of astrocytes in the whole brain after intravenous injection of sulforhodamine dyes. PLoS ONE 2012, 7. [Google Scholar] [CrossRef]
- Gibson, S.L.; Hilf, R. Photosensitization of mitochondrial cytochrome c oxidase by hematoporphyrin derivative and related porphyrins in vitro and in vivo. Cancer Res. 1983, 43, 4191–4197. [Google Scholar]
- Salet, C. Hematoporphyrin and hematoporphyrin-derivative photosensitization of mitochondria. Biochimie 1986, 68, 865–868. [Google Scholar] [CrossRef]
- Chen, J.Y.; Mak, N.K.; Yow, C.M.; Fung, M.C.; Chiu, L.C.; Leung, W.N.; Cheung, N.H. The binding characteristics and intracellular localization of temoporfin (mTHPC) in myeloid leukemia cells: Phototoxicity and mitochondrial damage. Photochem. Photobiol. 2000, 72, 541–547. [Google Scholar] [CrossRef]
- Hermes-Lima, M.; Castilho, R.F.; Valle, V.G.R.; Bechara, E.J.H.; Vercesi, A.E. Calcium-dependent mitochondrial oxidative damage promoted by 5-aminolevulinic acid. BBA Mol. Basis Dis. 1992, 1180, 201–206. [Google Scholar] [CrossRef]
- Zorova, L.D.; Popkov, V.A.; Plotnikov, E.Y.; Silachev, D.N.; Pevzner, I.B.; Jankauskas, S.S.; Babenko, V.A.; Zorov, S.D.; Balakireva, A.V.; Juhaszova, M.; et al. Mitochondrial membrane potential. Anal. Biochem. 2018, 552, 50–59. [Google Scholar] [CrossRef]
- Forrest, M.D. Why cancer cells have a more hyperpolarised mitochondrial membrane potential and emergent prospects for therapy. bioRxiv 2015, 1–42. [Google Scholar]
- Yassine, A.-A.; Lilge, L.; Betz, V. Optimizing interstitial photodynamic therapy with custom cylindrical diffusers. J. Biophotonics 2019, 12, e201800153. [Google Scholar] [CrossRef] [PubMed]
| Reference | Number of Treated Glioblastomas | Photosensitiser | Light | Median Survival Time (Months) | ||||
|---|---|---|---|---|---|---|---|---|
| Trade Name | Agent | Dose | Localisation | Wavelength (nm) | Energy Density (J/cm2) | |||
| Perria et al. (1980) [25] | Not defined | Photofrin® | Hematoporphyrin derivative (HpD) | 5 mg/kg | Cell membrane; mitochondria | 628 | 720–2400 | 6.9 |
| Povovic et al. (1995) [26] | Newly diagnosed, 38 Recurrent, 40 | Photofrin® | Hematoporphyrin derivative (HpD) | 2–2.5 mg/kg | Cell membrane; mitochondria | 628 | 70–260 | Newly diagnosed, 24 Recurrent, 9 |
| Rosenthal et al. (2003) [27] | Newly diagnosed, 7 Recurrent, 9 | BOPP | Boronated porphyrin | 0.25–8 mg/kg | Various, including mitochondria | 630 | 25–100 | Newly diagnosed, 7 Recurrent, 11 |
| Stylli et al. (2005) [28] | Newly diagnosed, 31 Recurrent, 55 | Photofrin® | Hematoporphyrin derivative (HpD) | 5 mg/kg | Cell membrane; mitochondria | 628 | 70–240 | 14.3 |
| Muller and Wilson, (2006) [29] | Newly diagnosed, 12 Recurrent, 37 | Photofrin® | Hematoporphyrin derivative (HpD) | 2 mg/kg | Cell membrane; mitochondria | 630 | Mean, 58 Maximum, 150 | 7.6 |
| Kostron et al. (2006) [30] | Recurrent, 26 | Foscan® | mTHPC metatetrahydroxyphenylchlorin | 0.15 mg/kg | Golgi apparatus, endoplasmic reticulum, and mitochondria | 630 | 20 | Recurrent, 8.5 |
| Stepp H. et al. (2007) [31] | Newly diagnosed, 20 | Levulan | 5-ALA | 20 mg/kg | mitochondria | 633 | 200 mW/cm2 | Newly diagnosed, 15.2 |
| Beck T.J. et al., (2007) [32] | Recurrent GBM, 10 | Levulan | 5-ALA | 20 mg/kg | mitochondria | 633 | Total 4320–11,520 J (200 mW/cm) | 15 |
| Eljamel (2008) [33] | Newly diagnosed, 13 | Photofrin® | Hematoporphyrin derivative (HpD) 5-ALA | 2 mg/kg | Cell membrane; mitochondria | 630 | 100 × 5 sessions | Newly diagnosed, Mean survival 52.8 weeks |
| Kaneko et al., (2008) [34] | Total, 35 | Photofrin® | Hematoporphyrin derivative (HpD) | 2 mg/m2 | Cell membrane; mitochondria | 630 | 180 | Total, 20.5 |
| Akimoto et al. (2012) [35] | Newly diagnosed, 4 Recurrent, 6 | Laserphyrin® | Talaporfin sodium | 40 mg/m2 | - | 664 | 27 | Newly diagnosed, 31 Reccurent, 9 |
| Lyons M. et al. (2012) [36] | Total, 73 | Photofrin® | Hematoporphyrin derivative (HpD) | 2 mg/kg | Cell membrane; mitochondria | 630 | 100 | Mean survival 62.9 weeks |
| Levulan | 5-ALA | |||||||
| Johansson et al. (2013) [37] | Total, 5 | Levulan | 5-ALA | 20–30 mg/kg | Cell membrane; mitochondria | 630 | 720 | - |
| Muragaki et al. (2013) [38] | Newly diagnosed, 13 | Laserphyrin® | Talaporfin sodium | 40 mg/m2 | - | 664 | 27 | Newly diagnosed, 24.8 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vasilev, A.; Sofi, R.; Rahman, R.; Smith, S.J.; Teschemacher, A.G.; Kasparov, S. Using Light for Therapy of Glioblastoma Multiforme (GBM). Brain Sci. 2020, 10, 75. https://doi.org/10.3390/brainsci10020075
Vasilev A, Sofi R, Rahman R, Smith SJ, Teschemacher AG, Kasparov S. Using Light for Therapy of Glioblastoma Multiforme (GBM). Brain Sciences. 2020; 10(2):75. https://doi.org/10.3390/brainsci10020075
Chicago/Turabian StyleVasilev, Alex, Roba Sofi, Ruman Rahman, Stuart J. Smith, Anja G. Teschemacher, and Sergey Kasparov. 2020. "Using Light for Therapy of Glioblastoma Multiforme (GBM)" Brain Sciences 10, no. 2: 75. https://doi.org/10.3390/brainsci10020075
APA StyleVasilev, A., Sofi, R., Rahman, R., Smith, S. J., Teschemacher, A. G., & Kasparov, S. (2020). Using Light for Therapy of Glioblastoma Multiforme (GBM). Brain Sciences, 10(2), 75. https://doi.org/10.3390/brainsci10020075







