Screening of Cognitive Changes in Adults with Intellectual Disabilities: A Systematic Review
Abstract
1. Introduction
1.1. Down Syndrome Intellectual Disability
1.2. Other Intellectual Disability
1.3. The Present Study
2. Materials and Methods
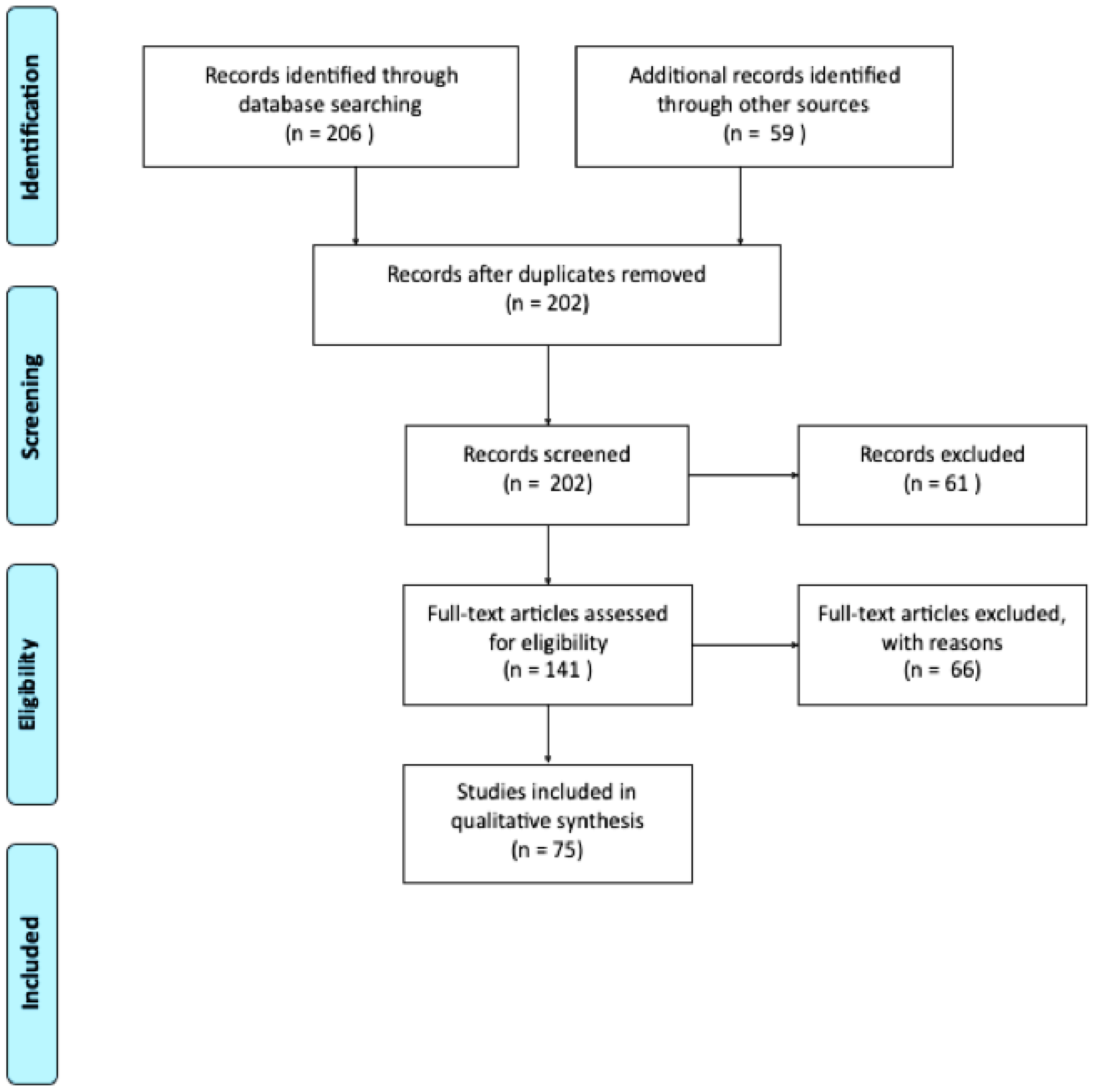
2.1. Literature Search
2.2. Eligibility Criteria and Data Extraction
2.3. Quality Assessment
3. Results
Descriptive Synthesis
4. Discussion and Implications
4.1. Longitudinal Studies
4.1.1. Longitudinal Studies in Participants with Down Syndrome
4.1.2. Longitudinal Studies Including Participants with DS and Other ID
4.2. Cross-Sectional Studies
4.2.1. Cross-Sectional Studies in Participants with Down Syndrome
4.2.2. Cross-Sectional Studies Including Participants with DS and Other ID
4.2.3. Other Measures
4.2.4. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
Appendix A
| Article | Study City/Country | Population | Instruments | Comparison | Outcomes | Quality Assessment Scale (0/8) |
|---|---|---|---|---|---|---|
| [3] ^ | USA | DS: N = 30 DAT: N = 18 Elderly controls N = 25 | MMSE; NBAP | Between groups | DS individuals showed more signs of indifference; inappropriateness; pragnosia and scores were consistent also in individuals with DAT | 7 |
| [11] ^ | UK | DS N = 14 | The Prudhoe Cognitive Function Test (PCFT) | inter-rater reliability and test retest reliability | 0.99 (p < 0.01) represents excellent inter-rater reliability to detect cognitive deterioration aspects of dementia. High reliability and temporal stability. | 4 |
| [16] # | UK | DS N = 78; Mild ID N = 33 | CAMCOG; CaD; SR; ToL; SB; CaODB | Changes in behaviour | Disinhibited behaviour and apathy were both associated with impaired performance in executive function. | 5 |
| [20] # | USA | oID N = 10 DS no dementia N = 10 DS/dementia N = 10 | BPT; SIB | Between groups | The BPT test was sensitive to functional declines because of dementia in DS. | 5 |
| [24] * # | USA | DS/NO AD N = 17 Normal controls N = 11 DS/AD N = 17 Normal AD controls N = 12 Group 2 DS/AD N = 52 DS/NO AD N = 78 | BPT; SIB; DMR | Between groups A beta levels in plasma | No association between plasma Aβ and scores on the SIB and DMR; Lack of sensitivity of SIB and DMR to detect dementia or cognitive decline in DS adults. | 7 |
| [47] * | UK | Ntotal = 62 DS N = 26 DS/dementia N = 36 DS no dementia | MMSE; DMR; DSDS | Between instruments | Positive correlation in the diagnosis of dementia between DMR and the DSDS with specificity and sensitivity at 0.92 in both cases. | 4 |
| [48] * | USA | ID N = 38 ID/DS N = 26 ID with dementia N = 19 ID no dementia N = 19 | DSDS; DMR; Reiss Screen; Shultz MMSE | Between groups | Both DSDS and DQMR assess similar elements of dementia; Both subscales of DSDS differentiated between groups | 5 |
| [85] * # | Netherlands | DS N = 39 | WPPSI-R; FANT; NPEMID; DMR; SRZ/SRZ-P; FP/FS | Between instruments | 56% of participants preferred facial pictograms scales over drawn face stimuli | 4 |
| [53] * # | UK | DS N = 90 (mean age 38.97, SD ± 9.18) N = 37 males; N = 16 females | SIB; DMR | SIB vs. DMR criterion validity | The SIB has good concurrent criterion validity when compared to DMR; The SIB has a good validity specifically as a measure of cognitive ability in people with DS: It correlates only with the cognitive functioning component of the DMR. | 4 |
| [54] * # | The Netherlands | DS N = 106 (mean age = 37; n = 56 men) DS/possible dementia N = 49 (age range = 40 years and over) | SRZ/SRZ-P; DMR; FAS; CAS; NRS | Between instruments | Adults with DS have generally a better comprehension of faces rather than numbers and more comprehension of pain affect rather than pain intensity. | 4 |
| [55] * # | USA | DS N = 20 | WAIS-III; DMR; WGTA; Tasks: ODL, RL; DNMP; DNMS | Between instruments | DMR is the strongest predictor of reversal learning error scores, suggesting symptoms of dementia effect on reversal learning | 4 |
| [56] * # | UK | 36 > age DS/no dementia N = 130; 36 > age DS/dementia N = 51;16–35 DS N = 124 | KBIT-2; Short ABS; DLD; CANTAB; CAMCOG; NAID; ACTB; OMQ; ToL; BRIEF-A; NEPSY | Between groups and instruments | Poor performance for adults with cognitive decline and dementia; Majority of tasks have high completion rate for adults who do not have a diagnosis of dementia | 4 |
| [57] * # | Netherlands | DS N = 26 N = 14 More able group N = 12 Less able group | DLD; DRS-2; VABD-II; ABAS-II; PAS-ADD | Inter-informant agreement | Differences in scores are merely attributable to differing informants’ perspectives. | 4 |
| [58] # | USA | DS N = 63, n = 31 male; n = 32 female age range (30–53) | Several neuropsychological batteries | Between groups | Many adults with Down syndrome can tolerate amyloid-β deposition without deleterious effects on cognitive functioning. | 4 |
| [59] # | UK | N = 33 DS | SIB; VABS | The utility of SIB in people with DS | For DS and DAT, SIB could be of used in the longitudinal study by comparing age-matched DS and other ID groups | 4 |
| [61] * # | USA | DS N = 55; oID N = 75; | BVSR; PPVT; SICD-AASH; LIPS; BSID; TSI-M; PP; DTVMI; DSADS; DSDS; DMR; SoIB; RSMB; PIMRA; DASH-II; DSI; MAS | Between groups and age groups | Performance of older adults did not change over time, but that of younger adults with DS and adults without DS improved; Adults with DS showed significant and unique declines only in test of verbal fluency | 5 |
| [62] * | Italy | ID N = 63 ID/DAT N = 15 DAT/DS N = 13 | Italian translation of the AADS scale (AADS-I) DMR | Subjects with DAT scored significantly higher on both DMR subscales compared to the subgroup without DAT | 4 | |
| [63] * | Italy | ID N = 61 ID/DS N = 22 ID/oID N = 39 | AFAST; ADL; IADL; DMR | AFAST-I clinical significance | Good internal consistency of the AFAST-I (0.92); AFAST-I assesses several difficulty levels of autonomy. | 4 |
| [64] * # | Spain | ID N = 146; Mild ID N = 62; Moderate ID N = 84; ID/DS N = 103, ID/oID N = 43; | DMR; K-BIT I; CAMDEX-DS; CAMCOG-DS | Between instruments | High degree of diagnostic validity between the CAMDEX-DS and the CAMCOG-DS; Reliability scored 0.93. | 4 |
| [65] * | Italy | N = 58 DS; n = 40 no dementia; n = 3 dementia N = 142 oID, n = 126 no dementia; n = 2 dementia | DSQIID; DMR | Between instruments | Reliability of the DSQIID-I was 0.94; | 5 |
| [66] * | UK | ID/oID N = 76 DS N = 12 | DMR; ABS | Between instruments | DMR gives a general indicator of cognitive and affective symptoms that could indicate dementia. | 5 |
| [67] * # | USA | N = 63 men; mild ID N = 40; moderate ID N = 44; severe and profound ID N = 30; ID/DAT N = 71; ID/no DAT N = 43 | RADD; DMR; BADLS; SIB; BPT | Between groups | RADD has efficacy for assessing cognitive functions relevant to AD in DS; RADD differentiated participants based on their dementia status | 5 |
| [69] # | UK | N = 77 DS Group 1 age 30–44 (N = 45) Group 2 age 45 years and over (N = 29) | CAMCOG; MMSE | Between instruments | Younger group scored higher in the total CAMCOG and MMSE scores on all subtests except Attention/Calculation; CAMCOG can be used when possible dementia is being considered. | 4 |
| [71] # | Ireland | Moderate ID group: ID/dementia n = 19 ID/no dementia n = 29 Severe ID group: ID/dementia n = 11 ID/no dementia n = 11 | DSMSE; TSI | Between groups | The TSI is useful to monitor the progression of dementia longitudinally in severe MR. TSI-Reliability 0.89. | 5 |
| [72] * # | Ireland | No DAT/DS N = 14 DS/DAT N = 16 | CAS-ID; DSMSE; TSI; DLSQ | CAS-ID to other validated tests | Good measure cognitive and functional decline in individuals with DS and AD. | 5 |
| [73] ^ | USA | DAT N = 13 DAT/DS N = 6 Normal controls N = 31 | OMT; TSI; ABMT; O; PRT; NEPSY; PPV-III | Between groups | The functional level of the DAT group was significantly lower than that of the normal control group; DAT groups scores significantly lower than the normal group; | 7 |
| [75] ^ | Canada | N = 31 DS N = 41 oID | Tasks: VS; MN; RA; NF; SAE; CO; WR; FM; Matrices | Between groups | People with DS performed poorly in two verbal tasks; Phonological tasks are more likely to be sensitive in the detection of cognitive decline among people with DS | 5 |
| [76] # | USA | DS young: N = 16 DS old: N = 16 oID young: N = 16 oID old: N = 15 | WAIS or WAIS-R; Stanford-Binet ratio IQ; DRS; PPVT-R-Form M; MAT; CAS | Between groups | DS old group performed poorly in most test. In the tasks that involved verbal output both DS groups performed poorly | 5 |
| [77] * | USA | Dementia N = 10 DS = 6; ID/oID = 4 No dementia N = 12 DS = 4; ID/oID = 8 | CTT; BNT; TCOWAT; FOME; ESDCL | Between groups | Deficits in the Dementia group in areas consistent with diagnosis of dementia for persons with ID | 7 |
| [78] ^ | Finland | DS: N = 15 group ID/oID: N = 15 | Tasks: DSB; CS; NWR; NWS; DSF; CB; VST | working memory performance | The DS group performed significantly more poorly in working memory tasks that measured phonological loop | 5 |
| [80] * | Australia | DS = 33 | PPVT-4; DBC-A; ABDQ; ABAS-II | Age is associated with decrease in adaptive behaviour independent of dementia and health status; Age-related changes are domain specific rather than pervasive | 4 | |
| [81] * | Australia | N = 55 total; DS N = 47; AD or suspected: N = 10 | ABDQ; RCPM; PPV; ASM; VSM; TACL-III | Between groups | Adults with DS may show failure in continuing developing in productive syntax. | 5 |
| [86] # | Switzerland & Belgium | DS N = 47 | EVIP; PN; ISADYLE; STMT; CBTT; NEPSY; RPCM | Vocabulary knowledge verbal abilities | Dissociation between productive and receptive vocabulary measures in verbal short-term memory abilities in DS participants. | 4 |
| [87] # | USA | DS n = 28 N = 19 young adults N = 9 older adults | PPVT-R, Block Pattern subtest of HNTLA; WISC-R; BDDE; DSF; OPS; BTS; DS | The relation of EEG alpha background to cognitive function | Older patients with DS with decreased alpha waves backgrounds had fewer visuospatial skills, decreased attention span, and dementia | 4 |
| [88] # | UK | N = 70 DS; n = 39 female, n = 31 male. | BPVS; VABS; CAMDEX; ECT | Between age groups | Participants with highest risk of developing dementia scored significantly higher in identification test | 4 |
| [89] * # | UK | N = 63 DS; N = 74 oID; Mild ID n = 27; Moderate ID n = 69; Severe ID n = 38; profound ID n = 4 | DQ; IBR-MSE | Between instruments | Good agreement between DQ and the IBR Mental Status Exam; Disagreement is greater for individuals who are lower functioning and for those with DS | 5 |
| [90] # | USA | ID/oID N = 40 ID/DS:Healthy N = 44 Questionable DAT N = 10 Early-Stage DAT N = 5 Middle-Stage DAT N = 7 | WISC-R; CRT; SRT; | Levels of decline across stages of dementia | Group differences: (i.e., healthy with DS, ‘questionable’, early-stage dementia and middle-stage dementia) for each subtest | 4 |
| [91] * # | UK | DS N = 48 Control group oID N = 42 | CAMCOG; BPVS | Between groups | Significant negative correlation between mean myo-inositol concentration and overall cognitive ability in DS group | 5 |
| [92] ^ | USA | DS n = 53 Williams syndrome n = 10 Mixed aetiology n = 39 | Short term memory and dual task processing tasks | Between groups | Dual task performance declined significantly in DS; No aetiology group differences on single tasks. | 6 |
| [93] ^ | USA | DS N = 9 oID N = 24 DAT/DS N = 15 DAT/oID N = 11 | r-PRMT; OMT; TSI; NEPSY | Between groups | The r-PRMT discriminates between those with DAT from those without DAT; Controls with DS showed higher scores. | 5 |
| [94] * | USA | DS N = 14 Typically, Development N = 82 WS n = 41 | DLD; KBIT | Between groups | Individuals with DS demonstrated age-related effects on gray matter associated with dementia | 5 |
| [95] ^ | Spain | DS/no DAT N = 75; DS/DAT N = 15 | Modified Cued Recall Test (mCRT) | Between groups | Healthy DS achieved higher total scores and committed fewer intrusion errors; In DS-DAT with advanced DAT the mCRT is not useful. | 5 |
| [96] # | UK | DS Total N = 49 DS/dementia N = 19 DS/no dementia N = 30 | ACTB; CANTAB; NAID; ToL; VF; F-NT; GA; OM | ACTB validity | Only 3 tests of the ACTB differentiated between demented and non-demented DS groups. | 5 |
| [97] * # | UK | Total DS N = 128 DS/Dementia N = 23/128 | CSDS; CAMDEX; KBIT-2 | Development of CS-DS | Good reliability (0.84) and validity using two raters and over two time points. | 5 |
| [98] # | Israel | NSD N = 18; DS N = 14; | LLPI; PPVS; RSPM; PFT; S; CVMT; IC; TFB; HMGT; MTT; NVMT; TMT | Between groups | Participation in cognitively stimulating activities influence cognitive performance in adults with ID with and without DS. | 5 |
| [99] # | Spain | ID N = 69 ID/DS N = 65/69 COMTVal158Met N = 93; VNTR-DAT1 N = 57 | K-BIT; CANTAB; WAIS-III; SFWGT; WCFST; TOLDx | Between groups | Met allele carriers showed worse adaptive social skills and self-direction. | 6 |
| [100] * # | Netherlands | DS N = 224 | PS; DFPA; WPPSI-R; FANT; NPEMID; FSID | Pain experience | Structural differences and atypical patterns of brain activation in DS individuals. | 4 |
| [101] * # | Spain | DS N = 63 adults IDmild N = 39 IDmod N = 24 | KBIT-2; ABS-RC:2; CAMDEX-DS; BT-ID; WCFST; BRIEF; TOLDXTM | Between groups | Psychometric properties of the TOLDXTM version for people with ID were satisfactory on all variables; Sensitivity (0.76), Specificity (0.81). | 4 |
| Article | Study City/Country | Population | Instruments | Comparison | Outcomes | Quality Assessment Scale (0/8) |
|---|---|---|---|---|---|---|
| [2] # | UK | DS N = 30 | Several multidomain | Follow up | Those with cognitive deterioration show a significant decline on measures of executive function between baseline and 16 months follow up | 7 |
| [4] * # | Ireland | N = 77 | DLSQ-NIA; DLD; DSMSE; TSI | Follow-up | Over 20 years follow-up, 97.4% developed dementia | 6 |
| [8] # | Ireland, USA | DS N = 77 | SIB; DSMSE; DLSQ; DMR | Follow-up | After 20 years, 75 individuals developed dementia at a 20-year follow-up. | 6 |
| [10] * | USA | MR/oID N = 117 MR/DS N = 126 | DMR; RS; Part I of AMDAB | Between groups | Equivalent or maybe lower risk for dementia between MR participants and general population | 7 |
| [15] # | UK | DS N = 61 | CAMDEX; CAMCOG; | Longitudinal comparison | People with a diagnosis of AD at baseline were at least 6 more times likely to diagnosed with AD at time 2 | 7 |
| [42] * # | USA | N = 1 | BPT; DMR; SIB; RADD; WAIS III; VABS-II | Follow-up | The prevalence of APP disomy in patients with DS resulting from PT21 appears to be very rare since only 2 cases. | 7 |
| [43] * # | USA | DS/DAT No seizure N = 29; Seizure group N = 24 | SIB; BPT; DMR; VABS | Between groups; | Cognitive decline is more marked in demented individuals with DS who have seizures compared to those who do not. | 6 |
| [44] * # | USA | DS N = 34 N = 19/34 retested one year later | WAIS-III; NBAP; DMR; and other tests | Validity and reliability of instruments. | NBAP was the strongest predictor of dementia-status. Strong correlation between the pragnosia scale scores and the DMR | 6 |
| [45] # * | UK | DS N = 8 | HSSA; DMR; RCPM; WAIS-R; MEAMS; | Neuropsychological assessment | All patients score below normal population in RCPM Difficult sensitivity in the DMR to distinguished between dementia and depression | 6 |
| [38] # * | USA | DS N = 561 | MSRT; MMMSE-DS; TSI; CF-T; WISC-R-blocks tests; DSMSE (BLOCK-T); DLD; ABSI; Reiss Screen | Follow-up Assessment | The overall summary score of the DLD showed clear changes with MNI onset | 5 |
| [51] * | Germany | baseline sample n = 102 ID; n = 22 DS; | WDTIM; DSQIDD | Follow up | WDTIM very suitable for mild to moderate ID but limited for severe ID. | 5 |
| [83] * | UK | DS N = 92 | The PCFT; The ABS | Longitudinal comparison | Participants with low scores and deterioration on PCFT and ABS later showed dementia | 6 |
| [84] * # | UK | DS N = 14; ID/oID N = 4 males | RCPM; BPVS-II; CAMCOG; DMR; Mini PASADD; ABS-CR2 | Longitudinal comparison | After 2 years, 38.8% of participants were diagnosed with dementia. | 7 |
| [102] ^ | USA | DS N = 14 | NeuroTrax | Follow-up | No significant changes in scores from point to the next in memory, executive function, verbal, visual spatial and global scores | 6 |
| [103] # ^ | Canada | N = 18 DS; N = 18 oID | PPVT; WISC | Between groups | Younger DS participants, showed less decline in full-scale scores; Cognitive ability, is more stable over time in DS sample | 7 |
| [104] # | USA | N = 90 | WAIS-R; ICAT | Between individuals | The declining group with initial lower scores had lower levels of adaptive behaviour, were rated as more depressed and had a higher frequency of problem behaviours. | 6 |
| [105] ^ | USA | DS N = 28; ID/oID N = 5; MR/oID N = 13 | Tasks: O; ON; VMC; C MS Test: BMT | Between groups | All groups showed comparable improvements in performance tasks from initial testing to second testing on memory; Functional deterioration did not occur among adults with DS. | 7 |
| [106] # | USA | DS/MR N = 91, MR/oID N = 64 | IBR-MSE; SRT; VMT; WISC | Between groups | All individuals with possible DAT declined in tasks regarding orientation to time, and object naming. | 7 |
| [107] ^ | Netherlands | DS N = 307 | ESDC; SSIMR | Scores between instruments | ESDC it is easy to use, and the symptoms can be assessed quantitatively. | 6 |
| [108] * | USA | DS/DAT N = 14; DS/NO-DAT N = 71 | DSDS; SRT | Follow up | Participants with early-stage DAT exhibited significantly greater decline over the 3-year period preceding their diagnosis; Decline in SRT distinguished between groups. | 6 |
| [9] ^ | USA | ID/oID N = 66; DS/no DAT N = 75 DS/DAT N = 19 | mCRT | Between groups | Participants with DAT had lower total scores that participants without DAT; Poor performance on the adaptation of CRT was associated with early-stage DAT. | 7 |
| [109] # | USA | ID/oID N = 28; ID/DS N = 42 | WISC-R | Sex-related changes | Male participants with ID no DS performed better than female participants with ID oID; Females with DS performed better than males with ID in object assembly and block design | 6 |
| [110] ^ | UK | DS N = 57 | Single domain tasks | Between groups | Poor performance and decline in performance on delayed response and conditioned associative learning is associated with dementia in DS adults. | 6 |
| [111] # | USA | DS/DA N = 5, DS no-dementia N = 25 | Multi-domain | Longitudinal comparison | DS adults who developed DA at early stages showed progressive impairment in selective attention and in ability to selectively attend to stimuli. | 7 |
| [112] * | Australia | Time 2 n = 28; Mild/moderate ID n = 20 Severe/profound ID n = 8 | PPVT-4; ABDQ; DBC-A | Follow-up | Adults with DS may experience different ageing patterns for behavioural and emotional problems | 6 |
| [113] # | UK | DS N = 27 of 50 | LIPS; BPVS; WPPSI; RBMT-C; NAID | Cognitive changes over a 50-year period | Tests of dementia showed falling off in performance even for those without confirmed dementia | 6 |
| [114] # | Spain | DS sample N = 41; DS-AD n = 13; DS-MNI n = 14; DS-Control n = 14 | CAMCOG-DS; ADVM; WM; DVM; TO | Between groups | DS-AD groups showed significant poorer performance in all tests, especially in verbal and working memory; MNI-DS showed poorer performance than control DS in the CAMCOG and DVM. | 7 |
Appendix B. List of Instruments and Acronyms
| Scales, Questionnaires and Inventories |
|---|
|
| Batteries |
|---|
|
| Tests |
|---|
|
| Tasks |
|---|
|
References
- Strydom, A.; Chan, T.; King, M.; Hassiotis, A.; Livingston, G. Incidence of dementia in older adults with Intellectual disabilities. Res. Dev. Disabil. 2013, 34, 1881–1885. [Google Scholar] [CrossRef] [PubMed]
- Adams, D.; Oliver, C. The relationship between acquired impairments of executive function and behaviour change in adults with Down syndrome. J. Intellect. Disabil. Res. 2010, 54, 393–405. [Google Scholar] [CrossRef]
- Nelson, L.; Lott, I.; Touchette, P.; Satz, P.; D’Elia, L. Detection of Alzheimer disease in individuals with Down syndrome. Am. J. Ment. Retard. 1995, 99, 616–622. [Google Scholar]
- McCarron, M.; McCallion, P.; Reilly, E.; Dunne, P.; Carroll, R.; Mulryan, N. A prospective 20-year longitudinal follow-up of dementia in persons with Down syndrome. J. Intellect. Disabil. Res. 2017, 61, 843–852. [Google Scholar] [CrossRef] [PubMed]
- Strydom, A.; Livingston, G.; King, M.; Hassiotis, A. Prevalence of dementia in Intellectual disability using different diagnostic criteria. Br. J. Psychiatry 2007, 191, 150–157. [Google Scholar] [CrossRef]
- Takenoshita, S.; Terada, S.; Kuwano, R.; Inoue, T.; Cyoju, A.; Suemitsu, S.; Yamada, N. Prevalence of dementia in people with Intellectual disabilities: Cross-sectional study. Int. J. Geriatr. Psychiatry 2020, 35, 414–422. [Google Scholar] [CrossRef] [PubMed]
- Wisniewski, K.E.; Wisniewski, H.M.; Wen, G.Y. Occurrence of neuropathological changes and dementia of Alzheimer’s disease in Down’s syndrome. Ann. Neurol. Off. J. Am. Neurol. Assoc. Child Neurol. Soc. 1985, 17, 278–282. [Google Scholar] [CrossRef] [PubMed]
- McCarron, M.; McCallion, P.; Reilly, E.; Mulryan, N. A prospective 14-year longitudinal follow-up of dementia in persons with Down syndrome. J. Intellect. Disabil. Res. 2014, 58, 61–70. [Google Scholar] [CrossRef] [PubMed]
- Devenny, D.A.; Zimmerli, E.J.; Kittler, P.; Krinsky-McHale, S.J. Cued recall in early-stage dementia in adults with Down’s syndrome. J. Intellect. Disabil. Res. 2002, 46, 472–483. [Google Scholar] [CrossRef]
- Zigman, W.B.; Schupf, N.; Devenny, D.A.; Miezejeski, C.; Ryan, R.; Urv, T.K.; Schubert, R.; Silverman, W. Incidence and prevalence of dementia in elderly adults with mental retardation without Down syndrome. Am. J. Ment. Retard. 2004, 109, 126–141. [Google Scholar] [CrossRef]
- Margallo-Lana, M.L.; Moore, P.B.; Tyrer, S.P.; Dawson, H.; Jenkins, K.; Kay, D.W. The Prudhoe Cognitive Function Test, a scale to assess cognitive function in adults with Down’s syndrome: Inter-rater and test–retest reliability. J. Intellect. Disabil. Res. 2003, 47, 488–492. [Google Scholar] [CrossRef] [PubMed]
- Nieuwenhuis-Mark, R.E. Diagnosing Alzheimer’s dementia in Down syndrome: Problems and possible solutions. Res. Dev. Disabil. 2009, 30, 827–838. [Google Scholar] [CrossRef] [PubMed]
- Prasher, V.; Farooq, A.; Holder, R. The Adaptive Behaviour Dementia Questionnaire (ABDQ): Screening questionnaire for dementia in Alzheimer’s disease in adults with Down syndrome. Res. Dev. Disabil. 2004, 25, 385–397. [Google Scholar] [CrossRef] [PubMed]
- Zeilinger, E.L.; Stiehl, K.A.; Weber, G. A systematic review on assessment instruments for dementia in persons with Intellectual disabilities. Res. Dev. Disabil. 2013, 34, 3962–3977. [Google Scholar] [CrossRef] [PubMed]
- Ball, S.L.; Holland, A.J.; Huppert, F.A.; Treppner, P.; Watson, P.; Hon, J. The modified CAMDEX informant interview is a valid and reliable tool for use in the diagnosis of dementia in adults with Down’s syndrome. J. Intellect. Disabil. Res. 2004, 48, 611–620. [Google Scholar] [CrossRef]
- Ball, S.L.; Holland, A.J.; Watson, P.C.; Huppert, F.A. Theoretical exploration of the neural bases of behavioural disinhibition, apathy and executive dysfunction in preclinical Alzheimer’s disease in people with Down’s syndrome: Potential involvement of multiple frontal-subcortical neuronal circuits. J. Intellect. Disabil. Res. 2010, 54, 320–336. [Google Scholar] [CrossRef]
- Elliott-King, J.; Shaw, S.; Bandelow, S.; Devshi, R.; Kassam, S.; Hogervorst, E. A critical literature review of the effectiveness of various instruments in the diagnosis of dementia in adults with Intellectual disabilities. Alzheimer’s Dement. Diagn. Assess. Dis. Monit. 2016, 4, 126–148. [Google Scholar] [CrossRef]
- Benejam, B.; Videla, L.; Vilaplana, E.; Barroeta, I.; Carmona-Iragui, M.; Altuna, M.; Valldeneu, S.; Fernandez, S.; Giménez, S.; Iulita, F.; et al. Diagnosis of prodromal and Alzheimer’s disease dementia in adults with Down syndrome using neuropsychological tests. Alzheimer’s Dement. Diagn. Assess. Dis. Monit. 2020, 12, e12047. [Google Scholar]
- Lin, L.P.; Hsu, S.W.; Hsia, Y.C.; Wu, C.L.; Chu, C.; Lin, J.D. Association of early-onset dementia with activities of daily living (ADL) in middle-aged adults with Intellectual disabilities: The caregiver’s perspective. Res. Dev. Disabil. 2014, 35, 626–631. [Google Scholar] [CrossRef]
- Powell, D.; Caban-Holt, A.; Jicha, G.; Robertson, W.; Davis, R.; Gold, B.T.; Schmitt, F.A.; Head, E. Frontal white matter integrity in adults with Down syndrome with and without dementia. Neurobiol. Aging 2014, 35, 1562–1569. [Google Scholar] [CrossRef]
- Masellis, M.; Sherborn, K.; Neto, P.R.; Sadovnick, D.A.; Hsiung, G.Y.; Black, S.E.; Prasad, S.; Williams, M.; Gauthier, S. Early-onset dementias: Diagnostic and etiological considerations. Alzheimer’s Res. Ther. 2013, 5, 1–22. [Google Scholar] [CrossRef] [PubMed]
- Head, E.; Powell, D.; Gold, B.T.; Schmitt, F.A. Alzheimer’s disease in Down syndrome. Eur. J. Neurodegener. Dis. 2012, 1, 353. [Google Scholar] [PubMed]
- Rumble, B.; Retallack, R.; Hilbich, C.; Simms, G.; Multhaup, G.; Martins, R.; Hockey, A.; Montgomery, P.; Beyreuther, K.; Masters, C.L. Amyloid A4 protein and its precursor in Down’s syndrome and Alzheimer’s disease. N. Engl. J. Med. 1989, 320, 1446–1452. [Google Scholar] [CrossRef] [PubMed]
- Head, E.; Doran, E.; Nistor, M.; Hill, M.; Schmitt, F.A.; Haier, R.J.; Lott, I.T. Plasma amyloid-β as a function of age, level of Intellectual disability, and presence of dementia in Down syndrome. J. Alzheimer’s Dis. 2011, 23, 399–409. [Google Scholar] [CrossRef] [PubMed]
- Prasher, V.P.; Sajith, S.G.; Rees, S.D.; Patel, A.; Tewari, S.; Schupf, N.; Zigman, W.B. Significant effect of APOE epsilon 4 genotype on the risk of dementia in Alzheimer’s disease and mortality in persons with Down syndrome. Int. J. Geriatr. Psychiatry 2008, 23, 1134–1140. [Google Scholar] [CrossRef] [PubMed]
- Rohn, T.T.; McCarty, K.L.; Love, J.E.; Head, E. Is apolipoprotein E4 an important risk factor for dementia in persons with Down syndrome? J. Parkinson’s Dis. Alzheimer’s Dis. 2014, 1, 7. [Google Scholar]
- Startin, C.M.; Hamburg, S.; Hithersay, R.; Al-Janabi, T.; Mok, K.Y.; Hardy, J.; Strydom, A.; Fisher, E.; Nizetic, D.; Tybulewicz, V.; et al. Cognitive markers of preclinical and prodromal Alzheimer’s disease in Down syndrome. Alzheimer’s Dement. 2019, 15, 245–257. [Google Scholar] [CrossRef]
- Lautarescu, B.A.; Holland, A.J.; Zaman, S.H. The early presentation of dementia in people with Down syndrome: A systematic review of longitudinal studies. Neuropsychol. Rev. 2017, 27, 31–45. [Google Scholar] [CrossRef]
- Haveman, M.; Heller, T.; Lee, L.; Maaskant, M.; Shooshtari, S.; Strydom, A. Major health risks in aging persons with Intellectual disabilities: An overview of recent studies. J. Policy Pract. Intell. Disabil. 2010, 7, 59–69. [Google Scholar] [CrossRef]
- Shooshtari, S.; Martens, P.J.; Burchill, C.A.; Dik, N.; Naghipur, S. Prevalence of depression and dementia among adults with developmental disabilities in Manitoba, Canada. Int. J. Fam. Med. 2011, 2011, 319574. [Google Scholar] [CrossRef]
- Strydom, A.; Shooshtari, S.; Lee, L.; Raykar, V.; Torr, J.; Tsiouris, J.; Jokinen, N.; Courtenay, K.; Bass, N.; Sinnema, M.; et al. Dementia in Older Adults With Intellectual Disabilities—Epidemiology, Presentation, and Diagnosis. J. Pol. Pract. Intellect. Disabil. 2010, 7, 96–110. [Google Scholar] [CrossRef]
- Chaplin, E.; Paschos, D.; O’Hara, J.; McCarthy, J.; Holt, G.; Bouras, N.; Tsakanikos, E. Mental ill-health and care pathways in adults with Intellectual disability across different residential types. Res. Dev. Disabil. 2010, 31, 458–463. [Google Scholar] [CrossRef] [PubMed]
- Perry, J.; Linehan, C.; Kerr, M.; Salvador-Carulla, L.; Zeilinger, E.; Weber, G.; Walsh, P.; Van Schrojenstein Lantman-de-Valk, H.; Haveman, M.; Azema, B.; et al. The P15—A multinational assessment battery for collecting data on health indicators relevant to adults with Intellectual disabilities. J. Intellect. Disabil. Res. 2010, 54, 981–991. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Int. J. Surg. 2010, 8, 336–341. [Google Scholar] [CrossRef]
- Campbell, M.; McKenzie, J.E.; Sowden, A.; Katikireddi, S.V.; Brennan, S.E.; Ellis, S.; Hartmann-Boyce, J.; Ryan, R.; Shepperd, S.; Thomas, J.; et al. Synthesis without meta-analysis (SWiM) in systematic reviews: Reporting guideline. Br. Med. J. 2020, 16, 368. [Google Scholar] [CrossRef]
- Wells, G.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. Newcastle-Ottawa Quality Assessment Scale Cohort Studies. 2015. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 1 January 2015).
- Bento, T. Revisões sistemáticas em desporto e saúde: Orientações para o planeamento, elaboração, redação e avaliação. Motricidade 2014, 10, 107–123. [Google Scholar] [CrossRef]
- Krinsky-McHale, S.J.; Zigman, W.B.; Lee, J.H.; Schupf, N.; Pang, D.; Listwan, T.; Kovacs, C.; Silverman, W. Promising outcome measures of early Alzheimer’s dementia in adults with Down syndrome. Alzheimer’s Dement. Diagn. Assess. Dis. Monit. 2020, 12, e12044. [Google Scholar]
- Evenhuis, H.M.; Eurlings, H.A.; Kengen, M.M. Dementia Questionnaire for Mentally Retarded Persons (DMR): For Diagnosis of Dementia in Mentally Retarded People; Hooge Burch Institute for Mentally Retarded People: Zwammerdam, The Netherlands, 1990. [Google Scholar]
- Evenhuis, H.M.; Sjoukes, L.; Koot, H.M.; Kooijman, A.C. Does visual impairment lead to additional disability in adults with Intellectual disabilities? J. Intellect. Disabil. Res. 2009, 53, 19–28. [Google Scholar] [CrossRef]
- Margallo-Lana, M.L.; Tyrer, S.P.; Moore, P.B. Overview of the neuropsychological assessment of dementia in Intellectual disability. In Neuropsychological Assessments of Dementia in Down Syndrome and Intellectual Disabilities; Springer: London, UK, 2009. [Google Scholar]
- Doran, E.; Keator, D.; Head, E.; Phelan, M.J.; Kim, R.; Totoiu, M.; Barrio, J.R.; Small, G.W.; Potkin, S.G.; Lott, I.T. Down syndrome, partial trisomy 21, and absence of Alzheimer’s disease: The role of APP. J. Alzheimer’s Dis. 2017, 56, 459–470. [Google Scholar] [CrossRef]
- Lott, I.T.; Doran, E.; Nguyen, V.Q.; Tournay, A.; Movsesyan, N.; Gillen, D.L. Down syndrome and dementia: Seizures and cognitive decline. J. Alzheimer’s Dis. 2012, 29, 177–185. [Google Scholar] [CrossRef] [PubMed]
- Nelson, L.D.; Scheibel, K.E.; Ringman, J.M.; Sayre, J.W. An experimental approach to detecting dementia in Down syndrome: A paradigm for Alzheimer’s disease. Brain Cognit. 2007, 64, 92–103. [Google Scholar] [CrossRef] [PubMed]
- Thompson, S.B. A neuropsychological test battery for identifying dementia in people with Down’s syndrome. Br. J. Dev. Disabil. 1994, 40, 135–142. [Google Scholar] [CrossRef]
- Prasher, V.P. Neuropsychological Assessments of Dementia in Down Syndrome and Intellectual Disabilities; Springer: Berlin/Heidelberg, Germany, 2009. [Google Scholar]
- Deb, S.; Braganza, J. Comparison of rating scales for the diagnosis of dementia in adults with Down’s syndrome. J. Intellect. Disabil. Res. 1999, 43, 400–407. [Google Scholar] [CrossRef]
- Shultz, J.; Aman, M.; Kelbley, T.; LeClear Wallace, C.; Burt, D.B.; Primeaux-Hart, S.; Loveland, K.; Thorpe, L.; Bogos, E.S.; Timon, J.; et al. Evaluation of screening tools for dementia in older adults with mental retardation. Am. J. Ment. Retard. 2004, 109, 98–110. [Google Scholar] [CrossRef]
- Panisset, M.; Roudier, M.; Saxton, J.; Boiler, F. Severe impairment battery: A neuropsychological test for severely demented patients. Arch. Neurol. 1994, 51, 41–45. [Google Scholar] [CrossRef] [PubMed]
- Saxton, J.; McGonigle-Gibson, K.; Swihart, A.; Boller, F. The Severe Impairment Battery (SIB) Manual; Alzheimer’s Disease Research Center: Pittsburgh, PA, USA, 1993. [Google Scholar]
- Kuske, B.; Wolff, C.; Gövert, U.; Müller, S.V. Early detection of dementia in people with an Intellectual disability—A German pilot study. J. Appl. Res. Intellect. Disabil. 2017, 30, 49–57. [Google Scholar] [CrossRef]
- Deb, S.; Hare, M.; Prior, L.; Bhaumik, S. Dementia screening questionnaire for individuals with Intellectual disabilities. Br. J. Psychiatry 2007, 190, 440–444. [Google Scholar] [CrossRef]
- Hutchinson, N.; Oakes, P. Further Evaluation of the Criterion Validity of the Severe Impairment Battery for the Assessment of Cognitive Functioning in Adults with Down Syndrome. J. Appl. Res. Intellect. Disabil. 2011, 24, 172–180. [Google Scholar] [CrossRef]
- De Knegt, N.C.; Evenhuis, H.M.; Lobbezoo, F.; Schuengel, C.; Scherder, E.J.A. Does format matter for comprehension of a facial affective scale and a numeric scale for pain by adults with Down syndrome? Res. Dev. Disabil. 2013, 34, 3442–3448. [Google Scholar] [CrossRef]
- Nelson, L.; Johnson, J.K.; Freedman, M.; Lott, I.; Groot, J.; Chang, M.; Head, E. Learning and memory as a function of age in Down syndrome: A study using animal-based tasks. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2005, 29, 443–453. [Google Scholar] [CrossRef]
- Startin, C.M.; Hamburg, S.; Hithersay, R.; Davies, A.; Rodger, E.; Aggarwal, N.; Al-Janabi, T.; Strydom, A. The LonDownS adult cognitive assessment to study cognitive abilities and decline in Down syndrome. Wellcome Open Res. 2016, 1, 11. [Google Scholar] [CrossRef] [PubMed]
- Walker, B.; MacBryer, S.; Jones, A.; Law, J. Interinformant agreement of the dementia questionnaire for people with learning disabilities. Br. J. Learn. Disabil. 2015, 43, 227–233. [Google Scholar] [CrossRef]
- Hartley, S.L.; Handen, B.L.; Devenny, D.A.; Hardison, R.; Mihaila, I.; Price, J.C.; Christian, B.T. Cognitive functioning in relation to brain amyloid-β in healthy adults with Down syndrome. Brain J. Neurol. 2014, 137 Pt 9, 2556–2563. [Google Scholar] [CrossRef]
- Witts, P.; Elders, S. The Severe Impairment Battery: Assessing cognitive ability in adults with Down syndrome. Br. J. Clin. Psychol. 1998, 37, 213–216. [Google Scholar] [CrossRef] [PubMed]
- Boada, M.; Alegret, M.; Buendia, M.; Hernández, I.; Viñas, G.; Espinosa, A.; Lara, S.; Guitart, M.; Tárraga, L. The usefulness of standard neuropsychological testing for adults with Down syndrome and dementia. Int. Med. Rev. Down Syndrome 2008, 12, 2–7. [Google Scholar] [CrossRef]
- Burt, D.B.; Primeaux-Hart, S.; Loveland, K.A.; Cleveland, L.A.; Lewis, K.R.; Lesser, J.; Pearson, P.L. Aging in Adults with Intellectual Disabilities. Am. J. Ment. Retard. 2005, 110, 268–284. [Google Scholar] [CrossRef]
- De Vreese, L.P.; Mantesso, U.; De Bastiani, E.; Marangoni, A.; Gomiero, T. Psychometric evaluation of the Italian version of the AADS questionnaire: A caregiver-rated tool for the assessment of behavioral deficits and excesses in persons with intellectual disabilities and dementia. Int. Psychogeriatr. 2011, 23, 1124–1132. [Google Scholar] [CrossRef]
- De Vreese, L.P.; Gomiero, T.; Uberti, M.; De Bastiani, E.; Weger, E.; Mantesso, U.; Marangoni, A. Functional abilities and cognitive decline in adult and aging intellectual disabilities. Psychometric validation of an Italian version of the Alzheimer’s Functional Assessment Tool (AFAST): Analysis of its clinical significance with linear statistics and artificial neural networks. J. Intellect. Disabil. Res. 2015, 59, 370–384. [Google Scholar]
- Esteba-Castillo, S.; Dalmau-Bueno, A.; Ribas-Vidal, N.; Vilà-Alsina, M.; Novell-Alsina, R.; García-Alba, J. Adaptation and validation of CAMDEX-DS (Cambridge Examination for Mental Disorders of Older People with Down’s Syndrome and others with Intellectual disabilities) in Spanish population with Intellectual disabilities. Rev. Neurol. 2013, 57, 337. [Google Scholar]
- Gomiero, T.; Bertelli, M.; Deb, S.; Weger, E.; Marangoni, A.; De Bastiani, E.; De Vreese, L.P. A Multicentre Italian Validation Study in Aging Adults with Down Syndrome and Other Forms of Intellectual Disabilities: Dementia Screening Questionnaire for Individuals with Intellectual Disabilities. Curr. Alzheimer Res. 2017, 14, 709–721. [Google Scholar] [CrossRef]
- Kirk, L.J.; Hick, R.; Laraway, A. Assessing dementia in people with learning disabilities: The relationship between two screening measures. J. Intellect. Disabil. 2006, 10, 357–364. [Google Scholar] [CrossRef] [PubMed]
- Walsh, D.M.; Doran, E.; Silverman, W.; Tournay, A.; Movsesyan, N.; Lott, I.T. Rapid assessment of cognitive function in down syndrome across Intellectual level and dementia status. J. Intellect. Disabil. Res. 2015, 59, 1071–1079. [Google Scholar] [CrossRef] [PubMed]
- Holland, A.J.; Ball, S.L. The Cambridge Examination for Mental Disorders of Older People with Down’s Syndrome and Others with intellectual disabilities (CAMDEX-DS). In Neuropsychological Assessments of Dementia in Down Syndrome and Intellectual Disabilities; Springer: London, UK, 2009; pp. 107–127. [Google Scholar]
- Hon, J.; Huppert, F.A.; Holland, A.J.; Watson, P. Neuropsychological assessment of older adults with Down’s syndrome: An epidemiological study using the Cambridge Cognitive Examination (CAMCOG). Br. J. Clin. Psychol. 1999, 38 Pt 2, 155–165. [Google Scholar] [CrossRef]
- Huppert, F.A.; Brayne, C.; Gill, C.; Paykel, E.S.; Beardsall, L. CAMCOG—A concise neuropsychological test to assist dementia diagnosis: Socio-demographic determinants in an elderly population sample. Br. J. Clin. Psychol. 1995, 34, 529–541. [Google Scholar] [CrossRef] [PubMed]
- Cosgrave, M.P.; McCarron, M.; Anderson, M.; Tyrrell, J.; Gill, M.; Lawlor, B.A. Cognitive decline in Down syndrome: A validity/reliability study of the test for severe impairment. Am. J. Ment. Retard. AJMR 1998, 103, 193–197. [Google Scholar] [CrossRef]
- McCarron, M.; Gill, M.; Lawlor, B.; Beagly, C. A pilot study of the reliability and validity of the Caregiver Activity Survey—Intellectual Disability (CAS-ID). J. Intellect. Disabil. Res. 2002, 46 Pt 8, 605–612. [Google Scholar] [CrossRef]
- Pyo, G.; Kripakaran, K.; Curtis, K.; Curtis, R.; Markwell, S. A preliminary study of the validity of memory tests recommended by the Working Group for individuals with moderate to severe Intellectual disability. J. Intellect. Disabil. Res. 2007, 51 Pt 5, 377–386. [Google Scholar] [CrossRef]
- Tyrer, P.; Tyrer, F.; Hanney, M.; Tyrer, S. Measuring Outcomes Including Use of Rating Scales and Instruments in People with Intellectual Disability. Oxf. Textb. Psychiatry Intellect. Disabil. 2020, 43. [Google Scholar] [CrossRef]
- Das, J.P.; Mishra, R.K. Assessment of cognitive decline associated with aging: A comparison of individuals with Down syndrome and other etiologies. Res. Dev. Disabil. 1995, 16, 11–25. [Google Scholar] [CrossRef]
- Das, J.P.; Divis, B.; Alexander, J.; Parrila, R.K.; Naglieri, J.A. Cognitive decline due to aging among persons with Down syndrome. Res. Dev. Disabil. 1995, 16, 461–478. [Google Scholar] [CrossRef]
- Palmer, G.A. Neuropsychological profiles of persons with mental retardation and dementia. Res. Dev. Disabil. 2006, 27, 299–308. [Google Scholar] [CrossRef] [PubMed]
- Numminen, H.; Service, E.; Ahonen, T.; Ruoppila, I. Working memory and everyday cognition in adults with Down’s syndrome. J. Intellect. Disabil. Res. 2001, 45 Pt 2, 157–168. [Google Scholar] [CrossRef]
- Kalsy, S.; McQuillan, S.; Oliver, C.; Hall, S.; Oyebode, J. The Adults with Down’s Syndrome Project: The Assessment of Adults with Developmental Disabilities (AADS) Questionnaire; University of Birmingham & South Birmingham Primary Care NHS Trust: Birmingham, UK, 2002. [Google Scholar]
- Makary, A.T.; Testa, R.; Tonge, B.J.; Einfeld, S.L.; Mohr, C.; Gray, K.M. Association between adaptive behaviour and age in adults with Down syndrome without dementia: Examining the range and severity of adaptive behaviour problems. J. Intellect. Disabil. Res. JIDR. 2015, 59, 689–702. [Google Scholar] [CrossRef] [PubMed]
- Iacono, T.; Torr, J.; Wong, H.Y. Relationships amongst age, language and related skills in adults with Down syndrome. Res. Dev. Disabil. 2010, 31, 568–576. [Google Scholar] [CrossRef] [PubMed]
- Prasher, V.P.; Sachdeva, N.; Tarrant, N. Diagnosing dementia in adults with Down’s syndrome. Neurodegener. Dis. Manag. 2015, 5, 249–256. [Google Scholar] [CrossRef]
- Margallo-Lana, M.L.; Moore, P.B.; Kay, D.W.; Perry, R.H.; Reid, B.E.; Berney, T.P.; Tyrer, S.P. Fifteen-year follow-up of 92 hospitalized adults with Down’s syndrome: Incidence of cognitive decline, its relationship to age and neuropathology. J. Intellect. Disabil. Res. 2007, 51, 463–477. [Google Scholar] [CrossRef]
- Strydom, A.; Hassiotis, A. Diagnostic instruments for dementia in older people with Intellectual disability in clinical practice. Aging Ment. Health 2003, 7, 431–437. [Google Scholar] [CrossRef]
- de Knegt, N.C.; Schuengel, C.; Lobbezoo, F.; Visscher, C.M.; Evenhuis, H.M.; Boel, J.A.; Scherder, E.J. Comprehension of pictograms for pain quality and pain affect in adults with Down syndrome. J. Intell. Devel. Disabil. 2016, 41, 222–232. [Google Scholar] [CrossRef]
- Majerus, S.; Barisnikov, K. Verbal short-term memory shows a specific association with receptive but not productive vocabulary measures in Down syndrome. J. Intellect. Disabil. Res. 2018, 62, 10–20. [Google Scholar] [CrossRef]
- Devinsky, O.; Sato, S.; Conwit, R.A.; Schapiro, M.B. Relation of EEG alpha background to cognitive function, brain atrophy, and cerebral metabolism in Down’s syndrome: Age-specific changes. Arch. Neurol. 1990, 47, 58–62. [Google Scholar] [CrossRef]
- Crayton, L.; Oliver, C.; Holland, A.; Bradbury, J.; Hall, S. The neuropsychological assessment of age related cognitive deficits in adults with Down’s syndrome. J. Appl. Res. Intellect. Disabil. 1998, 11, 255–272. [Google Scholar] [CrossRef]
- Burt, D.B.; Primeaux-Hart, S.; Phillips, N.B.; Greene, T.; Loveland, K.A.; Cummings, E.; Lewis, K.R.; Lesser, J.; Cleveland, L.; Chen, Y.R. Assessment of orientation: Relationship between informant report and direct measures. Ment. Retard. 1999, 37, 364–370. [Google Scholar] [CrossRef]
- Devenny, D.A.; Krinsky-McHale, S.J.; Sersen, G.; Silverman, W.P. Sequence of cognitive decline in dementia in adults with Down’s syndrome. J. Intellect. Disabil. Res. 2000, 44, 654–665. [Google Scholar] [CrossRef]
- Beacher, F.; Simmons, A.; Daly, E.; Prasher, V.; Adams, C.; Margallo-Lana, M.L.; Morris, R.; Lovestone, S.; Murphy, K.; Murphy, D.G. Hippocampal myo-inositol and cognitive ability in adults with Down syndrome: An in vivo proton magnetic resonance spectroscopy study. Arch. Gen. Psychiatry 2005, 62, 1360–1365. [Google Scholar] [CrossRef] [PubMed]
- Kittler, P.M.; Krinsky-McHale, S.J.; Devenny, D.A. Dual-task processing as a measure of executive function: A comparison between adults with Williams and down syndromes. Am. J. Ment. Retard. 2008, 113, 117–132. [Google Scholar] [CrossRef]
- Pyo, G.; Ala, T.; Kyrouac, G.A.; Verhulst, S.J. A pilot study of a test for visual recognition memory in adults with moderate to severe Intellectual disability. Res. Dev. Disabil. 2010, 31, 1475–1480. [Google Scholar] [CrossRef] [PubMed]
- Koran, M.E.; Hohman, T.J.; Edwards, C.M.; Vega, J.N.; Pryweller, J.R.; Slosky, L.E.; Crockett, G.; de Rey, L.V.; Meda, S.A.; Dankner, N.; et al. Differences in age-related effects on brain volume in Down syndrome as compared to Williams syndrome and typical development. J. Neurodev. Disord. 2014, 6, 8. [Google Scholar] [CrossRef] [PubMed]
- Benejam, B.; Fortea, J.; Molina-López, R.; Videla, S. Patterns of performance on the modified cued recall test in Spanish adults with down syndrome with and without dementia. Am. J. Intellect. Dev. Disabil. 2015, 120, 481–489. [Google Scholar] [CrossRef]
- Sinai, A.; Hassiotis, A.; Rantell, K.; Strydom, A. Assessing specific cognitive deficits associated with dementia in older adults with Down syndrome: Use and validity of the Arizona Cognitive Test Battery (ACTB). PLoS ONE 2016, 11, e0153917. [Google Scholar] [CrossRef]
- Startin, C.M.; Rodger, E.; Fodor-Wynne, L.; Hamburg, S.; Strydom, A. Developing an informant questionnaire for cognitive abilities in Down syndrome: The Cognitive Scale for Down Syndrome (CS-DS). PLoS ONE 2016, 11, e0154596. [Google Scholar] [CrossRef]
- Lifshitz-Vahav, H.; Shnitzer, S.; Mashal, N. Participation in recreation and cognitive activities as a predictor of cognitive performance of adults with/without Down syndrome. Aging Ment. Health 2016, 20, 955–964. [Google Scholar] [PubMed]
- Del Hoyo, L.; Xicota, L.; Langohr, K.; Sánchez-Benavides, G.; de Sola, S.; Cuenca-Royo, A.; Rodriguez, J.; Rodríguez-Morató, J.; Farré, M.; Dierssen, M.; et al. VNTR-DAT1 and COMTVal158Met genotypes modulate mental flexibility and adaptive behavior skills in Down syndrome. Front. Behav. Neurosci. 2016, 10, 193. [Google Scholar] [PubMed]
- De Knegt, N.C.; Lobbezoo, F.; Schuengel, C.; Evenhuis, H.M.; Scherder, E.J. Pain and cognitive functioning in adults with Down syndrome. Pain Med. 2017, 18, 1264–1277. [Google Scholar] [PubMed]
- García-Alba, J.; Esteba-Castillo, S.; López, M.Á.; Hidalgo, E.R.; Vidal, N.R.; Díaz, F.M.; Novell-Alsina, R. Validation and Normalization of the Tower of London-Drexel University Test 2 nd Edition in an Adult Population with Intellectual Disability. Span. J. Psychol. 2017, 20. [Google Scholar] [CrossRef]
- Gutman, M.; Moskovic, E.; Jeret, J.S. Computerised cognitive testing of individuals with Down’s syndrome and Alzheimer’s disease. J. Intellect. Disabil. Res. 2016, 60, 179–181. [Google Scholar] [CrossRef]
- Gibson, D.; Groeneweg, G.; Jerry, P.; Harris, A. Age and pattern of Intellectual decline among Down Syndrome and other mentally retarded adults. Int. J. Rehabil. Res. 1988, 11, 47–55. [Google Scholar] [CrossRef]
- Harper, D.C.; Wadsworth, J.S. Dementia and depression in elders with mental retardation: A pilot study. Res. Dev. Disabil. 1990, 11, 177–198. [Google Scholar] [CrossRef]
- Devenny, D.A.; Hill, A.L.; Patxot, O.; Silverman, W.P.; Wisniewski, K.E. Ageing in higher functioning adults with Down’s syndrome: An interim report in a longitudinal study. J. Intellect. Disabil. Res. 1992, 36, 241–250. [Google Scholar] [PubMed]
- Devenny, D.A.; Silverman, W.P.; Hill, A.L.; Jenkins, E.; Sersen, E.A.; Wisniewski, K.E. Normal ageing in adults with Down’s syndrome: A longitudinal study. J. Intellect. Disabil. Res. 1996, 40, 208–221. [Google Scholar]
- Visser, F.E.; Aldenkamp, A.P.; Van Huffelen, A.C.; Kuilman, M. Prospective study of the prevalence of Alzheimer-type dementia in institutionalized individuals with Down syndrome. Am. J. Ment. Retard. 1997, 101, 400–412. [Google Scholar] [PubMed]
- Krinsky-McHale, S.J.; Devenny, D.A.; Silverman, W.P. Changes in explicit memory associated with early dementia in adults with Down’s syndrome. J. Intellect. Disabil. Res. 2002, 46, 198–208. [Google Scholar] [CrossRef] [PubMed]
- Kittler, P.; Krinsky-McHale, S.J.; Devenny, D.A. Sex differences in performance over 7 years on the Wechsler Intelligence Scale for Children–Revised among adults with Intellectual disability. J. Intellect. Disabil. Res. 2004, 48, 114–122. [Google Scholar] [CrossRef] [PubMed]
- Oliver, C.; Holland, T.; Hall, S.; Crayton, L. Effects of increasing task load on memory impairment in adults with Down syndrome. Am. J. Ment. Retard. 2005, 110, 339–345. [Google Scholar] [CrossRef]
- Krinsky-McHale, S.J.; Devenny, D.A.; Kittler, P.; Silverman, W. Selective attention deficits associated with mild cognitive impairment and early stage Alzheimer’s disease in adults with Down syndrome. Am. J. Ment. Retard. 2008, 113, 369–386. [Google Scholar] [CrossRef]
- Makary, A.T.; Testa, R.; Einfeld, S.L.; Tonge, B.J.; Mohr, C.; Gray, K.M. The association between behavioural and emotional problems and age in adults with Down syndrome without dementia: Examining a wide spectrum of behavioural and emotional problems. Res. Dev. Disabil. 2014, 35, 1868–1877. [Google Scholar] [CrossRef]
- Carr, J.; Collins, S. 50 years with Down syndrome: A longitudinal study. J. Appl. Res. Intellect. Disabil. 2018, 31, 743–750. [Google Scholar] [CrossRef]
- García-Alba, J.; Ramírez-Toraño, F.; Esteba-Castillo, S.; Bruña, R.; Moldenhauer, F.; Novell, R.; Romero-Medina, V.; Maestú, F.; Fernández, A. Neuropsychological and neurophysiological characterization of mild cognitive impairment and Alzheimer’s disease in Down syndrome. Neurobiol. Aging 2019, 84, 70–79. [Google Scholar] [CrossRef]
| Cross-Sectional Studies | Longitudinal Studies | ||
|---|---|---|---|
| Down Syndrome | 2776 | Down Syndrome | 1874 |
| Other ID | 1231 | Other ID | 531 |
| Male | 1396 | Male | 110 |
| Female | 1143 | Female | 450 |
| Missing Data | 1482 | Missing Data | 1284 |
| Total | 4007 | Total | 2405 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Paiva, A.F.; Nolan, A.; Thumser, C.; Santos, F.H. Screening of Cognitive Changes in Adults with Intellectual Disabilities: A Systematic Review. Brain Sci. 2020, 10, 848. https://doi.org/10.3390/brainsci10110848
Paiva AF, Nolan A, Thumser C, Santos FH. Screening of Cognitive Changes in Adults with Intellectual Disabilities: A Systematic Review. Brain Sciences. 2020; 10(11):848. https://doi.org/10.3390/brainsci10110848
Chicago/Turabian StylePaiva, Andreia F., Adam Nolan, Charlotte Thumser, and Flávia H. Santos. 2020. "Screening of Cognitive Changes in Adults with Intellectual Disabilities: A Systematic Review" Brain Sciences 10, no. 11: 848. https://doi.org/10.3390/brainsci10110848
APA StylePaiva, A. F., Nolan, A., Thumser, C., & Santos, F. H. (2020). Screening of Cognitive Changes in Adults with Intellectual Disabilities: A Systematic Review. Brain Sciences, 10(11), 848. https://doi.org/10.3390/brainsci10110848







