Drowsiness Transitions Detection Using a Wearable Device
Abstract
1. Introduction
2. Methodology
3. Materials and Methods
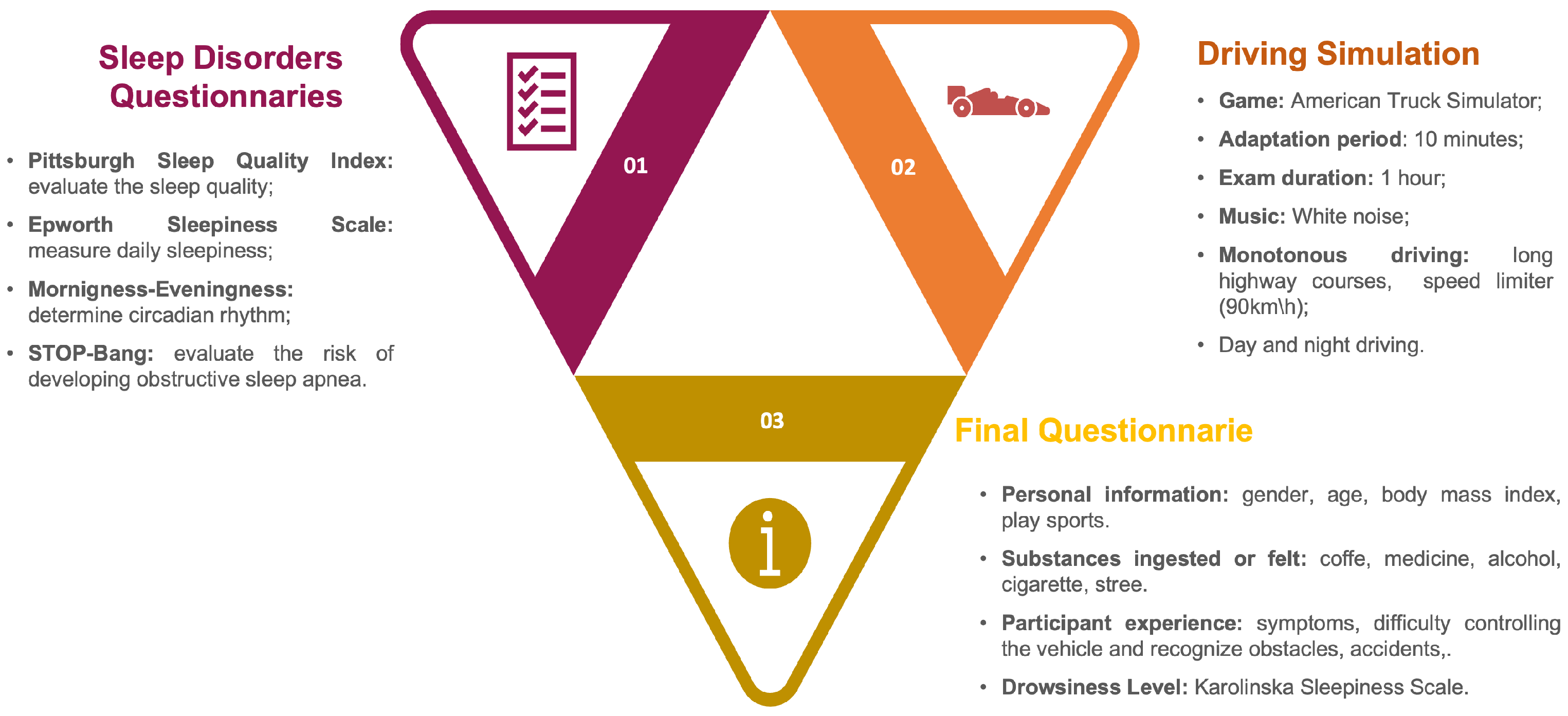
3.1. Driving Simulation Procedure
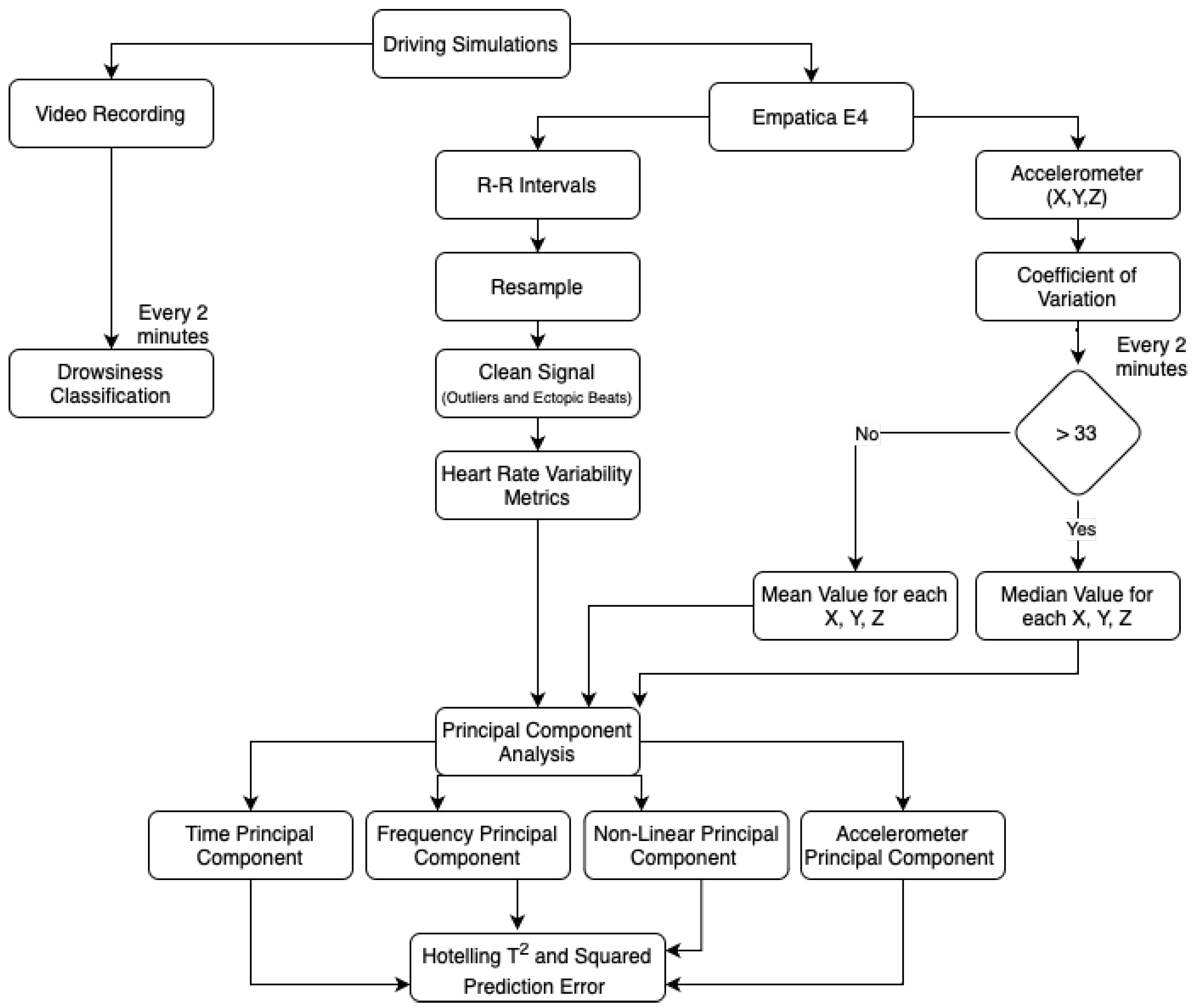
3.2. Analysis Procedure
3.3. Implementation Details
3.4. Participants Information
4. Results
4.1. Variables Description
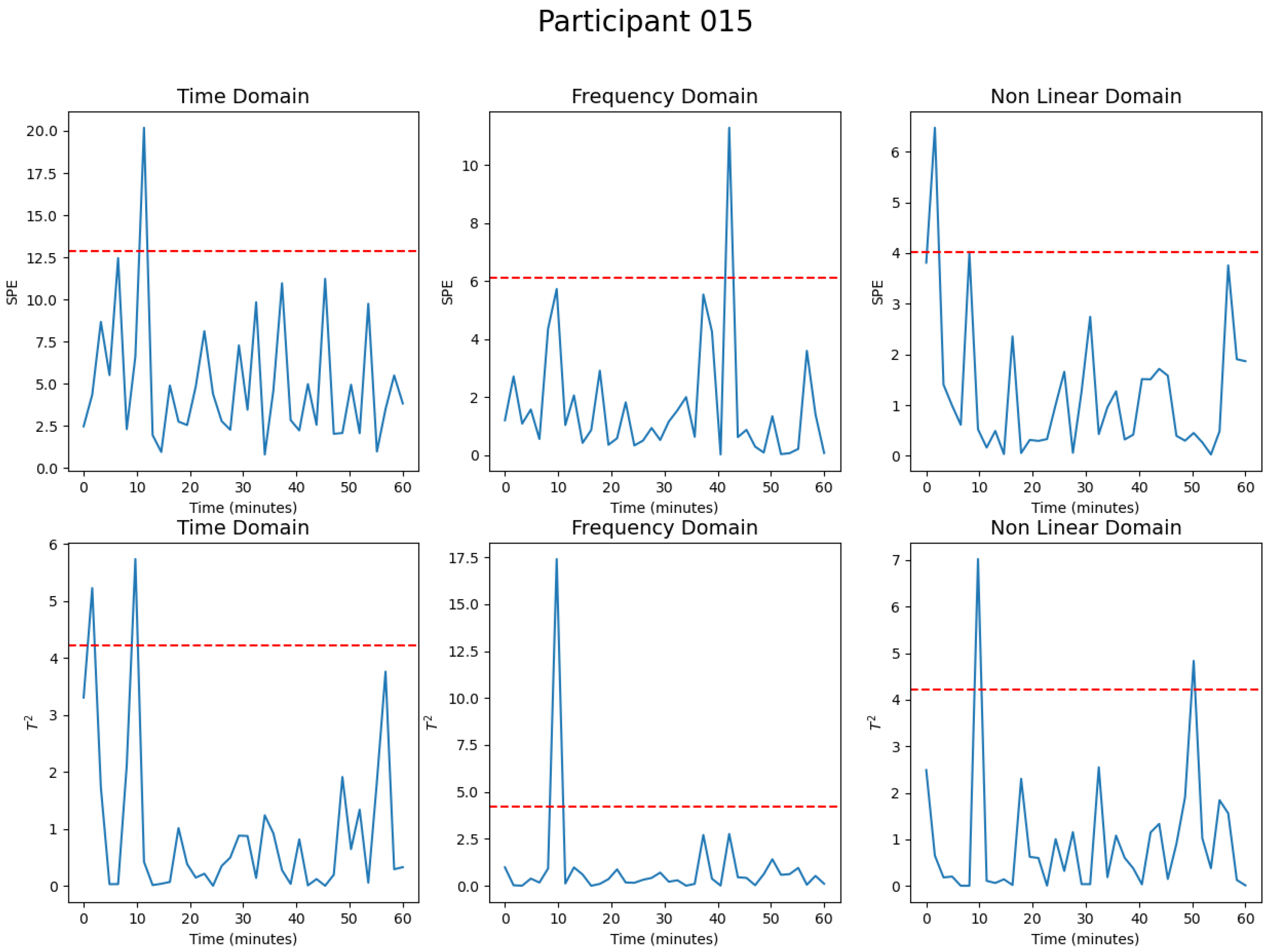
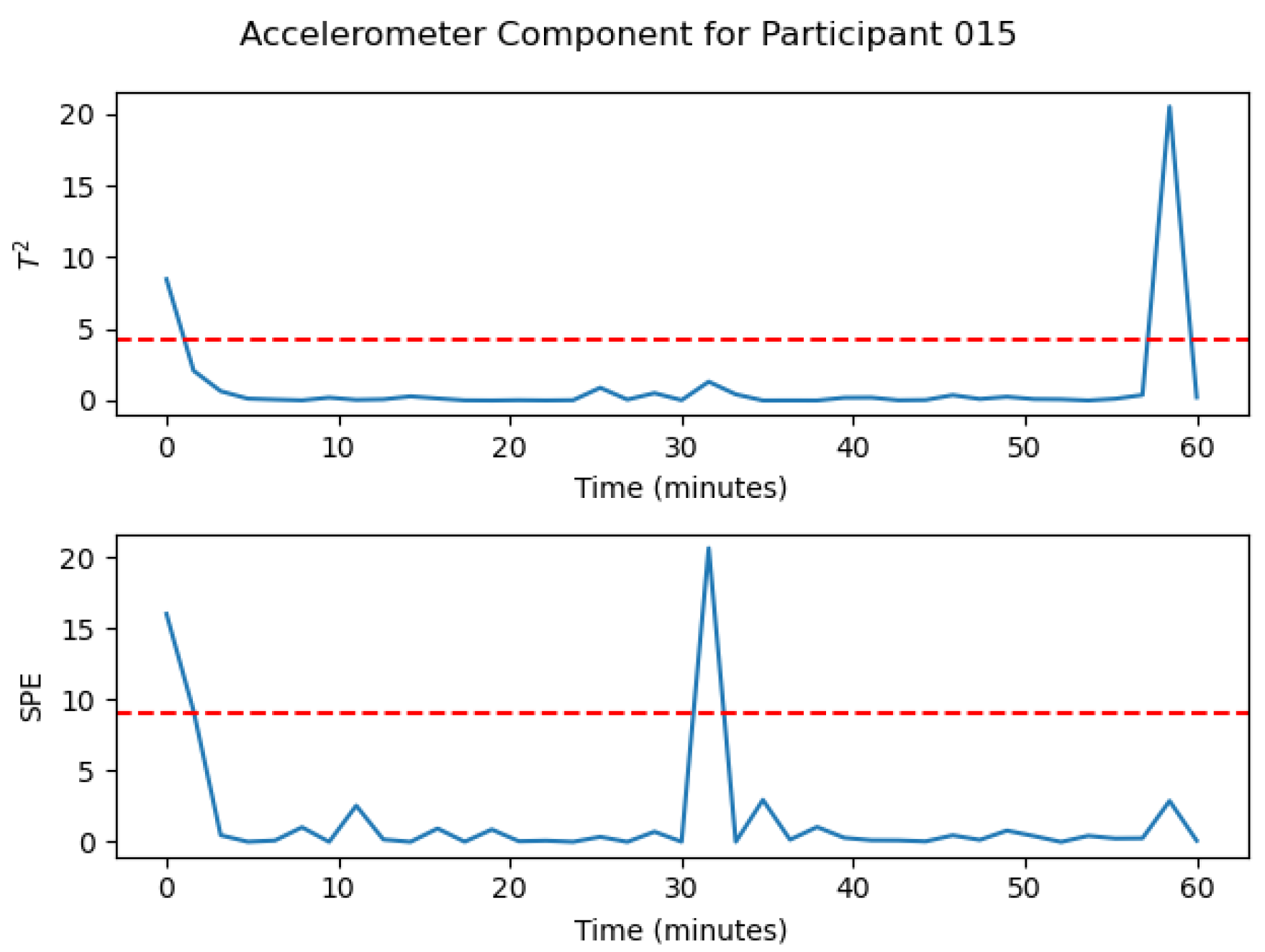
4.2. MSPC-PCA Analysis
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| MSPC-PCA | Multivariate Statistical Process Control, considering Principal Component Analysis |
| ULC | Upper Limit Control |
Appendix A. MSPC-PCA Statistics and Limits Control in Python
- ##############################################################
- import numpy as np
- from scipy.stats import chi2, f
- # function to compute the Hotelling T^2 statistic
- def hotelling_t2(scores):
- std = scores.std()
- hotelling = (scores**2)/(std**2)
- return hotelling
- # function to calculate the Hotelling T^2 control limit
- def hotelling_limit_control(scores, level_confidence):
- k = 1
- n = len(scores)
- d1 = (k*(n+1)*(n-1)) / (n*(n-k))
- ulc_t2 = d1 * f.ppf(level_confidence, k, n-k)
- return ulc_t2
- # function to compute the SPE statistic
- def q_statistic(input_features, loadings, scores):
- estimation_x = np.dot(scores, loadings)
- error = input_features - estimation_x
- q_statistic = np.sum(error**2, axis=1)
- return q_statistic
- # function to calculate the SPE control limit
- def q_limit_control(statistic_q, level_confidance):
- d1 = statistic_q.var()[0]/(2*statistic_q.mean()[0])
- df = (2*statistic_q.mean()[0]**2)/statistic_q.var()[0]
- ulc_spe = d1 * chi2.ppf(level_confidance, df)
- return ulc_spe
- ##############################################################
References
- Dernocoeur, K. Asleep at the wheel. Emerg. Med. Serv. 2000, 29, 32. [Google Scholar] [PubMed]
- Kortelainen, J.M.; Mendez, M.O.; Bianchi, A.M.; Matteucci, M.; Cerutti, S. Sleep staging based on signals acquired through bed sensor. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 776–785. [Google Scholar] [CrossRef] [PubMed]
- Bendak, S.; Rashid, H.S. Fatigue in aviation: A systematic review of the literature. Int. J. Ind. Ergon. 2020, 76, 102928. [Google Scholar] [CrossRef]
- Altevogt, B.M.; Colten, H.R. (Eds.) Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem; National Academies Press: Washington, DC, USA, 2006. [Google Scholar]
- Moradi, A.; Nazari, S.S.H.; Rahmani, K. Sleepiness and the risk of road traffic accidents: A systematic review and meta-analysis of previous studies. Transp. Res. Part Traffic Psychol. Behav. 2019, 65, 620–629. [Google Scholar] [CrossRef]
- Ramzan, M.; Khan, H.U.; Awan, S.M.; Ismail, A.; Ilyas, M.; Mahmood, A. A survey on state-of-the-art drowsiness detection techniques. IEEE Access 2019, 7, 61904–61919. [Google Scholar] [CrossRef]
- Barr, L.; Popkin, S.; Howarth, H. An Evaluation of Emerging Driver Fatigue Detection Measures and Technologies; Technical report, United States; Department of Transportation, Federal Motor Carrier Safety: Washington, DC, USA, 2009. [Google Scholar]
- Ingre, M.; Åkerstedt, T.; Peters, B.; Anund, A.; Kecklund, G. Subjective sleepiness, simulated driving performance and blink duration: Examining individual differences. J. Sleep Res. 2006, 15, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Bennett, M.S. Heart Rate Variability: Using Biometrics to Improve Outcomes in Trauma-Informed Organizations; A B.I.G. Publishing Project. 2020. Available online: https://www.scribd.com/book/469800653/Heart-Rate-Variability-Using-Biometrics-to-Improve-Outcomes-in-Trauma-Informed-Organizations (accessed on 20 January 2023).
- Forcolin, F.; Buendia, R.; Candefjord, S.; Karlsson, J.; Sjöqvist, B.A.; Anund, A. Comparison of outlier heartbeat identification and spectral transformation strategies for deriving heart rate variability indices for drivers at different stages of sleepiness. Traffic Inj. Prev. 2018, 19, S112–S119. [Google Scholar] [CrossRef]
- Shaffer, F.; Ginsberg, J.P. An overview of heart rate variability metrics and norms. Front. Public Health 2017, 5, 258. [Google Scholar] [CrossRef]
- Stancin, I.; Cifrek, M.; Jovic, A. A review of EEG signal features and their application in driver drowsiness detection systems. Sensors 2021, 21, 3786. [Google Scholar] [CrossRef]
- Iqbal, S.; Mahgoub, I.; Du, E.; Leavitt, M.A.; Asghar, W. Advances in healthcare wearable devices. NPJ Flex. Electron. 2021, 5, 1–14. [Google Scholar] [CrossRef]
- Yan, C.; Coenen, F.; Yue, Y.; Yang, X.; Zhang, B. Video-based classification of driving behavior using a hierarchical classification system with multiple features. Int. J. Pattern Recognit. Artif. Intell. 2016, 30, 1650010. [Google Scholar] [CrossRef]
- Kundinger, T.; Sofra, N.; Riener, A. Assessment of the potential of wrist-worn wearable sensors for driver drowsiness detection. Sensors 2020, 20, 1029. [Google Scholar] [CrossRef]
- Strine, T.W.; Chapman, D.P. Associations of frequent sleep insufficiency with health-related quality of life and health behaviors. Sleep Med. 2005, 6, 23–27. [Google Scholar] [CrossRef] [PubMed]
- Hoddes, E.; Zarcone, V.; Smythe, H.; Phillips, R.; Dement, W.C. Quantification of sleepiness: A new approach. Psychophysiology 1973, 10, 431–436. [Google Scholar] [CrossRef] [PubMed]
- Weinbeer, V.; Muhr, T.; Bengler, K.; Baur, C.; Radlmayr, J.; Bill, J. Highly automated driving: How to get the driver drowsy and how does drowsiness influence various take-over-aspects? In Proceedings of the 8. Tagung Fahrerassistenz, München, Germany, 22–23 November 2017. [Google Scholar]
- Abe, E.; Fujiwara, K.; Hiraoka, T.; Yamakawa, T.; Kano, M. Development of drowsiness detection method by integrating heart rate variability analysis and multivariate statistical process control. SICE J. Control Meas. Syst. Integr. 2016, 9, 10–17. [Google Scholar] [CrossRef]
- Antunes, A.R.; Braga, A.C.; Gonçalves, J. Drowsiness detection using multivariate statistical process control. In Proceedings of the International Conference on Computational Science and Its Applications, Malaga, Spain, 4–7 July 2022; Springer: Berlin/Heidelberg, Germany, 2022; pp. 571–585. [Google Scholar]
- Antunes, A.R.; Meneses, M.V.; Gonçalves, J.; Braga, A.C. An Intelligent System to Detect Drowsiness at the Wheel. In Proceedings of the 2022 10th International Symposium on Digital Forensics and Security (ISDFS), Istanbul, Turkey, 6–7 June 2022; pp. 1–6. [Google Scholar]
- Ahmed, M.; Mahmood, A.N.; Hu, J. A survey of network anomaly detection techniques. J. Netw. Comput. Appl. 2016, 60, 19–31. [Google Scholar] [CrossRef]
- Chandola, V.; Banerjee, A.; Kumar, V. Anomaly detection: A survey. ACM Comput. Surv. (CSUR) 2009, 41, 1–58. [Google Scholar] [CrossRef]
- Ferrer, A. Multivariate statistical process control based on principal component analysis (MSPC-PCA): Some reflections and a case study in an autobody assembly process. Qual. Eng. 2007, 19, 311–325. [Google Scholar] [CrossRef]
- MacGregor, J.F. Using on-line process data to improve quality: Challenges for statisticians. Int. Stat. Rev. 1997, 65, 309–323. [Google Scholar] [CrossRef]
- Jackson, J.E.; Mudholkar, G.S. Control procedures for residuals associated with principal component analysis. Technometrics 1979, 21, 341–349. [Google Scholar] [CrossRef]
- Alcala, C.F.; Qin, S.J. Analysis and generalization of fault diagnosis methods for process monitoring. J. Process Control 2011, 21, 322–330. [Google Scholar] [CrossRef]
- Chung, F.; Abdullah, H.R.; Liao, P. STOP-Bang questionnaire: A practical approach to screen for obstructive sleep apnea. Chest 2016, 149, 631–638. [Google Scholar] [CrossRef]
- Johns, M.W. A new method for measuring daytime sleepiness: The Epworth sleepiness scale. Sleep 1991, 14, 540–545. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds, C.F., III; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Horne, J.A.; Östberg, O. Individual differences in human circadian rhythms. Biol. Psychol. 1977, 5, 179–190. [Google Scholar] [CrossRef]
- Cech, J.; Soukupova, T. Real-time eye blink detection using facial landmarks. Cent. Mach. Percept. Dep. Cybern. Fac. Electr. Eng. Czech Tech. Univ. Prague 2016, 1–8. [Google Scholar]
- Shafiq, M.; Gu, Z. Deep residual learning for image recognition: A survey. Appl. Sci. 2022, 12, 8972. [Google Scholar] [CrossRef]
- Akhter, N.; Tharewal, S.; Gite, H.; Kale, K. Microcontroller based RR-Interval measurement using PPG signals for Heart Rate Variability based biometric application. In Proceedings of the 2015 International Conference on Advances in Computing, Communications and Informatics (ICACCI), Kochi, India, 10–13 August 2015; pp. 588–593. [Google Scholar]
- Regalia, G.; Onorati, F.; Lai, M.; Caborni, C.; Picard, R.W. Multimodal wrist-worn devices for seizure detection and advancing research: Focus on the Empatica wristbands. Epilepsy Res. 2019, 153, 79–82. [Google Scholar] [CrossRef] [PubMed]
- Bindu, K.H.; Raghava, M.; Dey, N.; Rao, C.R. Coefficient of Variation and Machine Learning Applications; CRC Press: Boca Raton, FL, USA, 2019. [Google Scholar]
- VanRossum, G.; Drake, F.L. The Python Ladnguage Reference; Python Software Foundation: Amsterdam, The Netherlands, 2010. [Google Scholar]
- McKinney, W. Pandas: A foundational Python library for data analysis and statistics. Python High Perform. Sci. Comput. 2011, 14, 1–9. [Google Scholar]
- Ari, N.; Ustazhanov, M. Matplotlib in python. In Proceedings of the 11th International Conference on Electronics, Computer and Computation (ICECCO), Abuja, Nigeria, 29 September–1 October 2014; pp. 1–6. [Google Scholar]
- Taskesen, E. pca: A Python Package for Principal Component Analysis. 2020. Available online: https://erdogant.github.io/pca (accessed on 28 March 2022).
- Harris, C.R.; Millman, K.J.; Van Der Walt, S.J.; Gommers, R.; Virtanen, P.; Cournapeau, D.; Wieser, E.; Taylor, J.; Berg, S.; Smith, N.J.; et al. Array programming with NumPy. Nature 2020, 585, 357–362. [Google Scholar] [CrossRef]
- Virtanen, P.; Gommers, R.; Oliphant, T.E.; Haberland, M.; Reddy, T.; Cournapeau, D.; Burovski, E.; Peterson, P.; Weckesser, W.; Bright, J.; et al. SciPy 1.0: Fundamental algorithms for scientific computing in Python. Nat. Methods 2020, 17, 261–272. [Google Scholar] [CrossRef] [PubMed]
- Waskom, M.L. Seaborn: Statistical data visualization. J. Open Source Softw. 2021, 6, 3021. [Google Scholar] [CrossRef]
- Leng, L.B.; Giin, L.B.; Chung, W.Y. Wearable driver drowsiness detection system based on biomedical and motion sensors. In Proceedings of the 2015 IEEE Sensors, Busan, Korea, 1–4 November 2015; pp. 1–4. [Google Scholar]
- Choi, M.; Koo, G.; Seo, M.; Kim, S.W. Wearable device-based system to monitor a driver’s stress, fatigue, and drowsiness. IEEE Trans. Instrum. Meas. 2017, 67, 634–645. [Google Scholar] [CrossRef]



| Drank Coffee | Had Medicine | Drank Alcohol | Smoke Cigarette | Felt Stress | |
|---|---|---|---|---|---|
| No | 24 | 45 | 5 | 53 | 41 |
| Yes | 33 | 12 | 52 | 4 | 16 |
| Symptom | 0 | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|---|
| Sicken | 45 | 9 | 0 | 1 | 2 | 0 |
| Vision Problems | 21 | 19 | 11 | 3 | 3 | 0 |
| Headache | 33 | 10 | 7 | 7 | 0 | 0 |
| Fatigue | 15 | 7 | 13 | 12 | 7 | 3 |
| Itching Eyes | 22 | 12 | 8 | 6 | 6 | 3 |
| Concentrate Problems | 12 | 16 | 11 | 7 | 9 | 2 |
| Anxiety | 38 | 8 | 5 | 3 | 2 | 1 |
| Level | Description | Count |
|---|---|---|
| 1 | Extremely alert | 1 |
| 2 | Very alert | 1 |
| 3 | Alert | 5 |
| 4 | Rather alert | 9 |
| 5 | Neither alert nor sleepy | 5 |
| 6 | Some signs of sleepiness | 9 |
| 7 | Sleepy, but no effort to keep awake | 12 |
| 8 | Sleepy, some effort to keep awake | 11 |
| 9 | Very sleepy, great effort keeping awake, fighting sleep | 4 |
| Domain | Metrics | Description |
|---|---|---|
| Time | mean_nni | Mean of the R–R intervals. |
| median_nni | Median of the R–R intervals. | |
| range_nni | Difference between the maximum and the minimum of the R–R intervals. | |
| sdnn | Standard Deviation of the R–R intervals. | |
| sdsd | Standard deviation of differences between adjacent R–R intervals. | |
| rmssd | Square root of the mean of the sum of the squares of differences between adjacent R–R intervals. | |
| nni_50 | Intervals’ number differences of successive R–R intervals greater than 50 ms. | |
| pnni_50 | Derived Proportion by dividing nni_50 by the R–R intervals’ total number. | |
| nni_20 | Intervals’ number differences of successive R–R intervals greater than 20 ms. | |
| pnni_20 | Derived Proportion by dividing nni_20 by the R–R intervals’ total number. | |
| cvsd | rmssd divided mean_nni. | |
| cvnni | sdnn divided by mean_nni. | |
| mean_hr | Heart rate mean. | |
| min_hr | Heart rate minimum. | |
| max_hr | Heart rate maximum. | |
| std_hr | Standard deviation of the heart rate. | |
| Frequency | power_vlf | Variance in HRV in the very low frequency. |
| power_lf | Variance in HRV in the low frequency | |
| power_hf | Variance in HRV in the high frequency | |
| total_power | Total power density spectral. | |
| lf_hf_ratio | lf/hf ratio. | |
| Non-Linear | csi | Cardiac Sympathetic Index. |
| cvi | Cadiac Vagal Index. | |
| modified_csi | Modified csi. | |
| sampen | Sample entropy. |
| Drowsiness Classification | Precision | Recall |
|---|---|---|
| First Classification [21] | 0.37 | 0.21 |
| Improved Classification | 0.83 | 0.47 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Antunes, A.R.; Braga, A.C.; Gonçalves, J. Drowsiness Transitions Detection Using a Wearable Device. Appl. Sci. 2023, 13, 2651. https://doi.org/10.3390/app13042651
Antunes AR, Braga AC, Gonçalves J. Drowsiness Transitions Detection Using a Wearable Device. Applied Sciences. 2023; 13(4):2651. https://doi.org/10.3390/app13042651
Chicago/Turabian StyleAntunes, Ana Rita, Ana Cristina Braga, and Joaquim Gonçalves. 2023. "Drowsiness Transitions Detection Using a Wearable Device" Applied Sciences 13, no. 4: 2651. https://doi.org/10.3390/app13042651
APA StyleAntunes, A. R., Braga, A. C., & Gonçalves, J. (2023). Drowsiness Transitions Detection Using a Wearable Device. Applied Sciences, 13(4), 2651. https://doi.org/10.3390/app13042651







