Non-Invasive Prediction of Site-Specific Coronary Atherosclerotic Plaque Progression using Lipidomics, Blood Flow, and LDL Transport Modeling
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Lipidomics Analysis
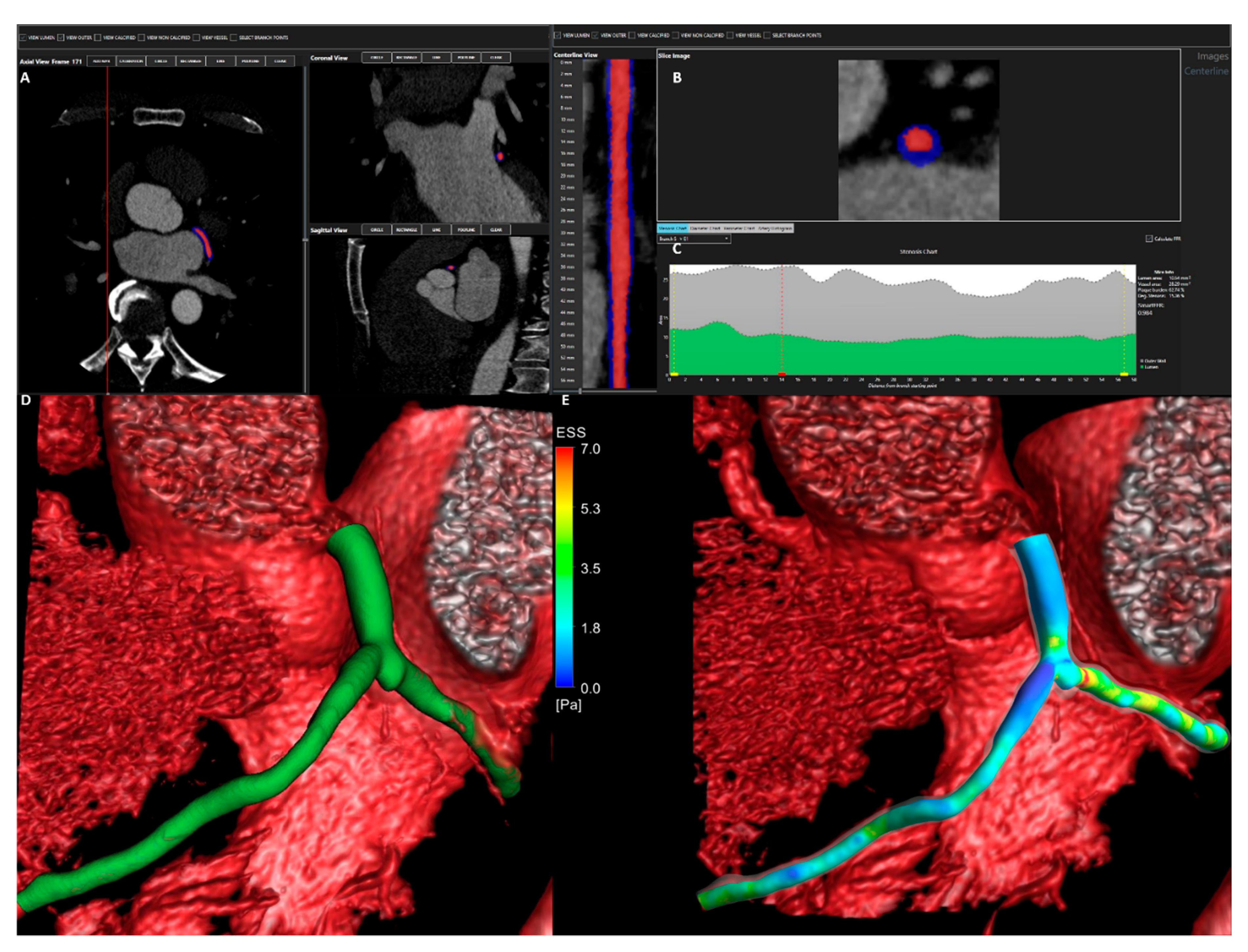
2.3. CCTA Analysis and Three-Dimensional (3D) Reconstruction
2.4. Blood Flow, LDL Transport Modeling, and Non-Invasive FFR Calculation
2.5. Statistics
3. Results
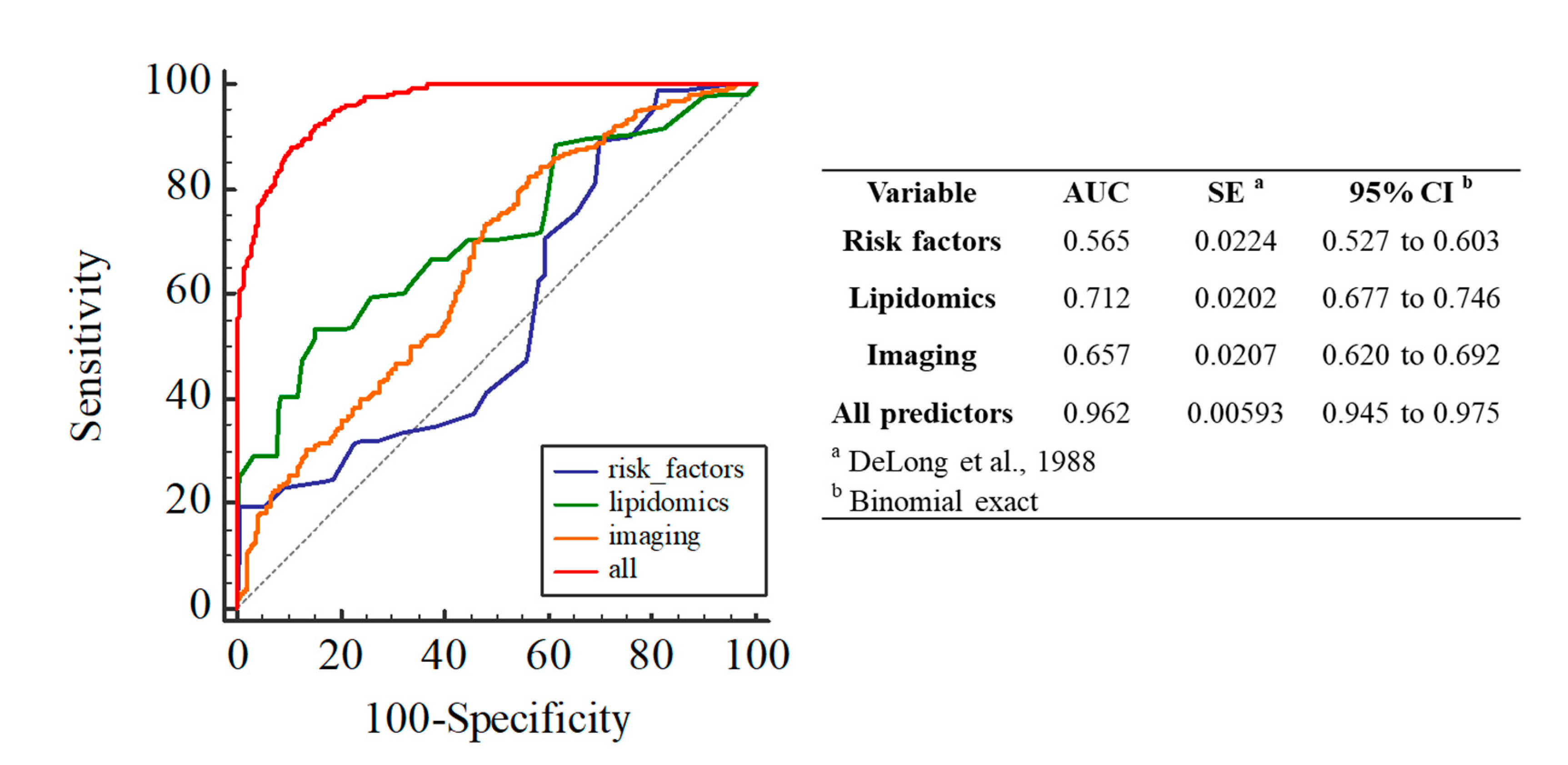
3.1. Prediction of Plaque Progression
3.2. Prediction of Single Features of Plaque Progression
3.3. Interaction of ESS, LDL Concentration, and SmartFFR to Predict Plaque Progression
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Benjamin, E.J.; Virani, S.S.; Callaway, C.W.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Chiuve, S.E.; Cushman, M.; Delling, F.N.; Deo, R.; et al. Heart Disease and Stroke Statistics-2018 Update: A Report from the American Heart Association. Circulation 2018, 137, e67–e492. [Google Scholar] [CrossRef] [PubMed]
- Clemente, A.; Seitun, S.; Mantini, C.; Gentile, G.; Federici, D.; Barison, A.; Rossi, A.; Cuman, M.; Pizzuto, A.; Ait-Ali, L.; et al. Cardiac CT Angiography: Normal and Pathological Anatomical Features—A Narrative Review. Cardiovasc. Diagn. Ther. 2020, 10, 1918–1945. [Google Scholar] [CrossRef]
- Stone, P.H.; Maehara, A.; Coskun, A.U.; Maynard, C.C.; Zaromytidou, M.; Siasos, G.; Andreou, I.; Fotiadis, D.; Stefanou, K.; Papafaklis, M.; et al. Role of Low Endothelial Shear Stress and Plaque Characteristics in the Prediction of Nonculprit Major Adverse Cardiac Events: The PROSPECT Study. JACC Cardiovasc. Imaging 2017. [Google Scholar] [CrossRef] [PubMed]
- Samady, H.; Eshtehardi, P.; McDaniel, M.C.; Suo, J.; Dhawan, S.S.; Maynard, C.; Timmins, L.H.; Quyyumi, A.A.; Giddens, D.P. Coronary Artery Wall Shear Stress Is Associated with Progression and Transformation of Atherosclerotic Plaque and Arterial Remodeling in Patients With Coronary Artery Disease. Circulation 2011, 124, 779–788. [Google Scholar] [CrossRef] [PubMed]
- Sakellarios, A.; Bourantas, C.V.; Papadopoulou, S.L.; Kitslaar, P.H.; Girasis, C.; Stone, G.W.; Reiber, J.H.C.; Michalis, L.K.; Serruys, P.W.; de Feyter, P.J.; et al. The Effect of Coronary Bifurcation and Haemodynamics in Prediction of Atherosclerotic Plaque Development: A Serial Computed Tomographic Coronary Angiographic Study. EuroIntervention 2017, 13, e1084–e1091. [Google Scholar] [CrossRef]
- Bourantas, C.V.; Papadopoulou, S.L.; Serruys, P.W.; Sakellarios, A.; Kitslaar, P.H.; Bizopoulos, P.; Girasis, C.; Zhang, Y.J.; de Vries, T.; Boersma, E.; et al. Noninvasive Prediction of Atherosclerotic Progression: The PROSPECT-MSCT Study. JACC Cardiovasc. Imaging 2016, 9, 1009–1011. [Google Scholar] [CrossRef] [PubMed]
- Sakellarios, A.I.; Papafaklis, M.I.; Siogkas, P.; Athanasiou, L.S.; Exarchos, T.P.; Stefanou, K.; Bourantas, C.V.; Naka, K.K.; Michalis, L.K.; Parodi, O.; et al. Patient-Specific Computational Modeling of Subendothelial LDL Accumulation in a Stenosed Right Coronary Artery: Effect of Hemodynamic and Biological Factors. Am. J. Physiol. Heart Circ. Physiol. 2013, 304, H1455–H1470. [Google Scholar] [CrossRef]
- Olgac, U.; Knight, J.; Poulikakos, D.; Saur, S.C.; Alkadhi, H.; Desbiolles, L.M.; Cattin, P.C.; Kurtcuoglu, V. Computed High Concentrations of Low-Density Lipoprotein Correlate with Plaque Locations in Human Coronary Arteries. J. Biomech. 2011, 44, 2466–2471. [Google Scholar] [CrossRef]
- Tarbell, J.M. Mass Transport in Arteries and the Localization of Atherosclerosis. Annu. Rev. Biomed. Eng. 2003, 5, 79–118. [Google Scholar] [CrossRef]
- Sakellarios, A.; Bourantas, C.V.; Papadopoulou, S.L.; Tsirka, Z.; de Vries, T.; Kitslaar, P.H.; Girasis, C.; Naka, K.K.; Fotiadis, D.I.; Veldhof, S.; et al. Prediction of Atherosclerotic Disease Progression Using LDL Transport Modelling: A Serial Computed Tomographic Coronary Angiographic Study. Eur. Heart J. Cardiovasc. Imaging 2016. [Google Scholar] [CrossRef]
- Smit, J.M.; van Rosendael, A.R.; El Mahdiui, M.; Neglia, D.; Knuuti, J.; Saraste, A.; Buechel, R.R.; Teresinska, A.; Pizzi, M.N.; Roque, A.; et al. Impact of Clinical Characteristics and Statins on Coronary Plaque Progression by Serial Computed Tomography Angiography. Circ. Cardiovasc. Imaging 2020, 13, e009750. [Google Scholar] [CrossRef] [PubMed]
- Liga, R.; Vontobel, J.; Rovai, D.; Marinelli, M.; Caselli, C.; Pietila, M.; Teresinska, A.; Aguade-Bruix, S.; Pizzi, M.N.; Todiere, G.; et al. Multicentre Multi-Device Hybrid Imaging Study of Coronary Artery Disease: Results from the EValuation of INtegrated Cardiac Imaging for the Detection and Characterization of Ischaemic Heart Disease (EVINCI) Hybrid Imaging Population. Eur. Heart J. Cardiovasc. Imaging 2016, 17, 951–960. [Google Scholar] [CrossRef]
- Siogkas, P.; Sakellarios, A.; Exarchos, T.P.; Athanasiou, L.; Karvounis, E.; Stefanou, K.; Fotiou, E.; Fotiadis, D.I.; Naka, K.K.; Michalis, L.K.; et al. Multiscale-Patient-Specific Artery and Atherogenesis Models. IEEE Trans. Biomed. Eng. 2011, 58, 3464–3468. [Google Scholar] [CrossRef] [PubMed]
- Folch, J.; Lees, M.; Sloane Stanley, G.H. A Simple Method for the Isolation and Purification of Total Lipides from Animal Tissues. J. Biol. Chem. 1957, 226, 497–509. [Google Scholar] [CrossRef]
- Wentzel, J.J.; Chatzizisis, Y.S.; Gijsen, F.J.; Giannoglou, G.D.; Feldman, C.L.; Stone, P.H. Endothelial Shear Stress in the Evolution of Coronary Atherosclerotic Plaque and Vascular Remodelling: Current Understanding and Remaining Questions. Cardiovasc. Res. 2012, 96, 234–243. [Google Scholar] [CrossRef] [PubMed]
- Siogkas, P.K.; Anagnostopoulos, C.D.; Liga, R.; Exarchos, T.P.; Sakellarios, A.I.; Rigas, G.; Scholte, A.; Papafaklis, M.I.; Loggitsi, D.; Pelosi, G.; et al. Noninvasive CT-Based Hemodynamic Assessment of Coronary Lesions Derived from Fast Computational Analysis: A Comparison against Fractional Flow Reserve. Eur. Radiol. 2018. [Google Scholar] [CrossRef]
- Knuuti, J.; Wijns, W.; Saraste, A.; Capodanno, D.; Barbato, E.; Funck-Brentano, C.; Prescott, E.; Storey, R.F.; Deaton, C.; Cuisset, T.; et al. 2019 ESC Guidelines for the Diagnosis and Management of Chronic Coronary Syndromes. Eur. Heart J. 2019. [Google Scholar] [CrossRef]
- Bourantas, C.V.; Raber, L.; Sakellarios, A.; Ueki, Y.; Zanchin, T.; Koskinas, K.C.; Yamaji, K.; Taniwaki, M.; Heg, D.; Radu, M.D.; et al. Utility of Multimodality Intravascular Imaging and the Local Hemodynamic Forces to Predict Atherosclerotic Disease Progression. JACC Cardiovasc. Imaging 2019. [Google Scholar] [CrossRef]
- Stone, P.H.; Saito, S.; Takahashi, S.; Makita, Y.; Nakamura, S.; Kawasaki, T.; Takahashi, A.; Katsuki, T.; Nakamura, S.; Namiki, A.; et al. Prediction of Progression of Coronary Artery Disease and Clinical Outcomes Using Vascular Profiling of Endothelial Shear Stress and Arterial Plaque Characteristics The PREDICTION Study. Circulation 2012, 126, 172–181. [Google Scholar] [CrossRef]
- Yamamoto, H.; Kihara, Y.; Kitagawa, T.; Ohashi, N.; Kunita, E.; Iwanaga, Y.; Kobuke, K.; Miyazaki, S.; Kawasaki, T.; Fujimoto, S.; et al. Coronary Plaque Characteristics in Computed Tomography and 2-Year Outcomes: The PREDICT Study. J. Cardiovasc. Comput. Tomogr. 2018, 12, 436–443. [Google Scholar] [CrossRef]
- Norgaard, B.L.; Leipsic, J.; Gaur, S.; Seneviratne, S.; Ko, B.S.; Ito, H.; Jensen, J.M.; Mauri, L.; De Bruyne, B.; Bezerra, H.; et al. Diagnostic Performance of Noninvasive Fractional Flow Reserve Derived from Coronary Computed Tomography Angiography in Suspected Coronary Artery Disease: The NXT Trial (Analysis of Coronary Blood Flow Using CT Angiography: Next Steps). J. Am. Coll. Cardiol. 2014, 63, 1145–1155. [Google Scholar] [CrossRef] [PubMed]
- Seitun, S.; Clemente, A.; Lorenzi, C.D.; Benenati, S.; Chiappino, D.; Mantini, C.; Sakellarios, A.I.; Cademartiri, F.; Bezante, G.P.; Porto, I. Cardiac CT Perfusion and FFRCTA: Pathophysiological Features in Ischemic Heart Disease. Cardiovasc. Diagn. Ther. 2020, 10, 1954–1978. [Google Scholar] [CrossRef]
- Toia, P.; Grutta, L.L.; Sollami, G.; Clemente, A.; Gagliardo, C.; Galia, M.; Maffei, E.; Midiri, M.; Cademartiri, F. Technical Development in Cardiac CT: Current Standards and Future Improvements—A Narrative Review. Cardiovasc. Diagn. Ther. 2020, 10, 2018–2035. [Google Scholar] [CrossRef] [PubMed]
- Kohno, S.; Keenan, A.L.; Ntambi, J.M.; Miyazaki, M. Lipidomic Insight into Cardiovascular Diseases. Biochem. Biophys. Res. Commun. 2018, 504, 590–595. [Google Scholar] [CrossRef] [PubMed]

| All Patients (N = 187) | |
|---|---|
| Age (years) | 60.73 ± 8.11 |
| Gender (male) | 107 (57.2%) |
| BMI | 27.31 ± 3.52 |
| Current smoker | 25 (13.4%) |
| Family history of CAD | 92 (49.2%) |
| Risk factors | |
| Diabetes mellitus | 27 (14.4%) |
| Hypertension | 111 (59.4%) |
| Dyslipidemia | 127 (67.9%) |
| Obesity | 33 (17.6%) |
| Clinical presentation * | |
| Atypical angina | 86 (46.0%) |
| Typical angina | 48 (25.7%) |
| Other symptoms | 22 (11.8%) |
| No symptoms | 12 (6.4%) |
| Imaging presentation | |
| No CAD | 47 (25.1%) |
| Non-obstructive CAD | 113 (60.4%) |
| Obstructive CAD | 27 (14.4%) |
| Biohumoral data | |
| Total cholesterol | 190.60 ± 49.50 |
| Low density lipoprotein (LDL) cholesterol | 114.09 ± 42.39 |
| High density lipoprotein (HDL) cholesterol | 54.27 ± 17.37 |
| Triglycerides | 112.79 ± 57.03 |
| Glucose | 105.50 ± 24.04 |
| Studied vessels | (n = 480) |
| Left anterior descending artery | 162 (33.75%) |
| Left circumflex coronary artery | 144 (30.00%) |
| Right coronary artery | 174 (36.25%) |
| Medications at discharge | |
| Aspirin | 100 (53.77%) |
| ARB | 32 (17.1%) |
| Beta-blockers | 67 (35.8%) |
| ACE inhibitors | 50 (26.7%) |
| Calcium channel blockers | 28 (15.0%) |
| Statins | 85 (45.5%) |
| Baseline | Follow-Up | Delta | ||||||
|---|---|---|---|---|---|---|---|---|
| Mean | Std. Dev. | Mean | SD | p-Value Baseline vs. Follow-Up | Mean | SD | p-Value Baseline vs. Change between Follow-Up and Baseline | |
| Lumen area (mm2) | 6.86 | 3.89 | 6.34 | 3.90 | <0.0001 | −0.56 | 2.95 | <0.0001 |
| Plaque area (mm2) | 7.16 | 4.30 | 7.29 | 4.62 | <0.0001 | 0.14 | 4.41 | <0.0001 |
| Plaque burden | 51.02 | 14.66 | 52.96 | 17.85 | <0.0001 | 1.79 | 19.27 | <0.0001 |
| Minimum ESS (Pa) | 1.78 | 2.36 | ||||||
| Normalized max. LDL concentration | 0.24 | 0.12 | ||||||
| SmartFFR | 0.89 | 0.12 | ||||||
| Baseline | Follow-up | Delta | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | p-Value Baseline vs. Follow-up | Mean | SD | p-Value Baseline vs. Delta | ||
| Segments with progression N = 1557 | Lumen area (mm2) | 7.47 | 3.92 | 5.74 | 3.75 | <0.0001 | −1.79 | 2.73 | <0.0001 |
| Plaque area (mm2) | 6.02 | 3.68 | 9.17 | 4.75 | <0.0001 | 3.38 | 3.63 | <0.0001 | |
| Plaque burden | 44.52 | 13.28 | 62.48 | 14.16 | <0.0001 | 18.89 | 11.43 | <0.0001 | |
| Minimum ESS (Pa) | 1.61 | 1.72 | |||||||
| Normalized max. LDL concentration | 0.24 | 0.12 | |||||||
| SmartFFR | 0.91 | 0.09 | |||||||
| Segments without progression N = 2443 | Lumen area (mm2) | 6.47 | 3.83 | 6.72 | 3.95 | <0.0001 | 0.18 | 2.83 | <0.0001 |
| Plaque area (mm2) | 7.88 | 4.50 | 6.12 | 4.13 | <0.0001 | −1.81 | 3.62 | <0.0001 | |
| Plaque burden | 55.16 | 13.99 | 47.04 | 17.35 | <0.0001 | −8.44 | 15.35 | <0.0001 | |
| Minimum ESS (Pa) | 2.00 | 2.89 | |||||||
| Normalized max. LDL concentration | 0.24 | 0.12 | |||||||
| SmartFFR | 0.88 | 0.14 | |||||||
| Dependent Variable | Effect | Univariate Linear Regression Analysis | Multivariate Linear Regression Analysis | ||
|---|---|---|---|---|---|
| Estimated Regression Coefficient (95% CI) | p-Value | Estimated Regression Coefficient (95% CI) | p-Value | ||
| Plaque progression (at least 2 out of 3 of the criteria below) | Age (years) | 0.006 (0.000 to 0.012) | 0.0429 | 0.011 (0.003 to 0.019) | 0.0067 |
| Triglycerides (mg/dl) | 0.001 (0.000 to 0.002) | 0.0417 | 0.001 (−0.001 to 0.002) | 0.2955 | |
| CE_18_3 (μM) | 0.003 (0.001 to 0.005) | 0.0138 | 0.001 (−0.003 to 0.004) | 0.7102 | |
| CE_20_3 (μM) | 0.008 (0.003 to 0.014) | 0.0043 | 0.006 (−0.006 to 0.018) | 0.3336 | |
| CE_20_4 (μM) | 0.002 (0.000 to 0.003) | 0.0203 | 0.000 (−0.003 to 0.004) | 0.7980 | |
| PC_36_0 (μM) | 0.009 (−0.001 to 0.018) | 0.0845 | - | - | |
| PC_36_3 (μM) | 0.000 (−0.000 to 0.001) | 0.0756 | - | - | |
| TG_54_2__TG_18_1_18_18_0 (μM) | 0.002 (−0.000 to 0.004) | 0.0872 | - | - | |
| PS_38_6 (μM) | 0.169 (0.017 to 0.321) | 0.0292 | −0.128 (−0.374 to 0.118) | 0.3046 | |
| PS_40_6 (μM) | 0.325 (−0.054 to 0.705) | 0.0921 | - | - | |
| SM_42_1 (μM) | 0.002 (−0.000 to 0.005) | 0.0892 | - | - | |
| Baseline plaque burden | −0.012 (−0.013 to −0.011) | <.0001 | −0.011 (−0.013 to −0.010) | <0.0001 | |
| Minimum ESS (Pa) | −0.056 (−0.074 to −0.038) | <0.0001 | 0.004 (−0.004 to 0.011) | 0.3653 | |
| Maximum LDL concentration | 0.075 (0.045 to 0.105) | <.0001 | −0.004 (−0.033 to 0.024) | 0.7593 | |
| SmartFFR | 0.385 (0.116 to 0.654) | 0.0052 | −0.027 (−0.379 to 0.326) | 0.8816 | |
| Lumen area reduction by 20% | Diabetes Mellitus | −0.180 (−0.316 to −0.045) | 0.0093 | 0.068 (−0.152 to 0.289) | 0.5393 |
| Hypertension | −0.077 (−0.161 to 0.006) | 0.0700 | −0.101 (−0.229 to 0.028) | 0.1221 | |
| CE_16_0 (μM) | −0.000 (−0.000 to −0.000) | 0.0330 | −0.000 (−0.001 to 0.000) | 0.5564 | |
| CE_16_1 (μM) | −0.000 (−0.001 to 0.000) | 0.0609 | −0.000 (−0.001 to 0.000) | 0.5856 | |
| CE_18_1 (μM) | −0.000 (−0.000 to −0.000) | 0.0439 | 0.000 (−0.000 to 0.000) | 0.8448 | |
| PS_36_1 (μM) | 0.007 (−0.001 to 0.015) | 0.0865 | −0.000 (−0.001 to 0.001) | 0.7504 | |
| Baseline plaque burden | −0.006 (−0.007 to −0.006) | < 0.0001 | −0.004 (−0.005 to −0.002) | <0.0001 | |
| Minimum ESS (Pa) | −0.102 (−0.117 to −0.088) | < 0.0001 | −0.021 (−0.027 to −0.014) | <0.0001 | |
| Maximum LDL concentration | 0.118 (0.093 to 0.142) | < 0.0001 | 0.057 (0.017 to 0.097) | 0.0051 | |
| SmartFFR | 0.226 (0.011 to 0.441) | 0.0394 | 0.087 (−0.219 to 0.394) | 0.5720 | |
| Dependent Variable | Effect | Univariate Logistic Regression Analysis | Multivariate Logistic Regression Analysis | ||
|---|---|---|---|---|---|
| Odds Ratio | p-Value | Odds Ratio | p-Value | ||
| Plaque progression | Age (years) | 1.028 (1.001 to 1.056) | 0.0401 | 1.067 (1.023 to 1.114) | 0.0026 |
| Triglycerides (mg/dl) | 1.004 (1.000 to 1.009) | 0.0605 | 1.000 (0.992 to 1.009) | 0.9453 | |
| CE_16_1 (μM) | 1.002 (1.000 to 1.004) | 0.0650 | 1.002 (1.000 to 1.005) | 0.0751 | |
| CE_18_3 (μM) | 1.011 (1.003 to 1.019) | 0.0095 | 1.004 (0.979 to 1.030) | 0.7523 | |
| CE_20_3 (μM) | 1.035 (1.011 to 1.060) | 0.0043 | 1.021 (0.959 to 1.086) | 0.5153 | |
| CE_20_4 (μM) | 1.006 (1.000 to 1.013) | 0.0552 | 1.002 (0.982 to 1.023) | 0.8269 | |
| PC_36_0 (μM) | 1.044 (0.999 to 1.091) | 0.0534 | 1.025 (0.950 to 1.106) | 0.5219 | |
| TG_54_2__TG_18_1_18_1_18_0 (μM) | 1.008 (0.999 to 1.016) | 0.0783 | 1.009 (0.996 to 1.022) | 0.1831 | |
| PS_38_5 (μM) | 1.512 (1.006 to 2.275) | 0.0469 | 2.742 (1.116 to 6.734) | 0.0278 | |
| SM_38_1 (μM) | 1.017 (0.999 to 1.034) | 0.0581 | 1.032 (0.987 to 1.079) | 0.1717 | |
| SM_42_1 (μM) | 1.012 (1.000 to 1.023) | 0.0464 | 1.029 (1.005 to 1.054) | 0.0168 | |
| Baseline lumen area (mm2) | 1.882 (1.493 to 2.371) | < 0.0001 | 1.171 (0.776 to 1.767) | 0.4517 | |
| Baseline plaque area (mm2) | 2.613 (2.140 to 3.191) | < 0.0001 | 1.626 (1.117 to 2.366) | 0.0112 | |
| Baseline plaque burden | 1.066 (1.053 to 1.079) | < 0.0001 | 1.066 (1.044 to 1.087) | <0.0001 | |
| SmartFFR | 5.671 (1.751 to 18.370) | 0.0038 | 1.043 (0.773 to 1.407) | 0.7814 | |
| Minimum ESS (Pa) | 1.194 (1.081 to 1.319) | 0.0005 | 1.069 (0.737 to 1.550) | 0.7239 | |
| Maximum LDL concentration | 1.164 (0.992 to 1.367) | 0.0634 | 1.094 (0.170 to 7.038) | 0.9245 | |
| Lumen reduction | Hypertension | 1.570 (1.017 to 2.423) | 0.0418 | 1.599 (1.025 to 2.495) | 0.0385 |
| Age (years) | 1.026 (1.001 to 1.052) | 0.0436 | 1.001 (0.965 to 1.038) | 0.9622 | |
| Diabetes | 2.025 (1.083 to 3.788) | 0.0272 | 1.085 (0.514 to 2.289) | 0.8305 | |
| Hypertension | 1.644 (1.029 to 2.626) | 0.0377 | 3.116 (1.595 to 6.089) | 0.0009 | |
| Triglycerides (mg/dl) | 1.004 (1.000 to 1.007) | 0.0634 | 1.003 (0.996 to 1.010) | 0.3980 | |
| Cer_d18_1_16_0 (μM) | 1.110 (0.985 to 1.250) | 0.0859 | 1.192 (1.017 to 1.397) | 0.0297 | |
| CE_16_0 (μM) | 1.001 (1.000 to 1.002) | 0.0039 | 1.001 (0.998 to 1.004) | 0.3945 | |
| CE_16_1 (μM) | 1.002 (1.000 to 1.003) | 0.0077 | 1.000 (0.998 to 1.003) | 0.7316 | |
| CE_18_1 (μM) | 1.001 (1.000 to 1.001) | 0.0131 | 1.000 (0.999 to 1.002) | 0.5703 | |
| SM_36_2 (μM) | 1.040 (1.000 to 1.081) | 0.0513 | 1.148 (0.999 to 1.318) | 0.0511 | |
| SM_38_2 (μM) | 1.080 (1.007 to 1.158) | 0.0319 | 1.097 (0.855 to 1.408) | 0.4665 | |
| Baseline lumen area | 2.904 (2.271 to 3.713) | <0.0001 | 1.974 (1.230 to 3.166) | 0.0048 | |
| Baseline plaque burden | 1.038 (1.025 to 1.051) | <0.0001 | 1.018 (1.000 to 1.037) | 0.0456 | |
| SmartFFR | 3.271 (1.103 to 9.704) | 0.0327 | 1.399 (0.179 to 10.901) | 0.7488 | |
| Minimum ESS (Pa) | 1.656 (1.470 to 1.865) | <0.0001 | 1.516 (1.165 to 1.972) | 0.0020 | |
| Maximum LDL concentration | 1.612 (1.341 to 1.938) | <0.0001 | 1.326 (0.864 to 2.034) | 0.0014 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sakellarios, A.I.; Tsompou, P.; Kigka, V.; Siogkas, P.; Kyriakidis, S.; Tachos, N.; Karanasiou, G.; Scholte, A.; Clemente, A.; Neglia, D.; et al. Non-Invasive Prediction of Site-Specific Coronary Atherosclerotic Plaque Progression using Lipidomics, Blood Flow, and LDL Transport Modeling. Appl. Sci. 2021, 11, 1976. https://doi.org/10.3390/app11051976
Sakellarios AI, Tsompou P, Kigka V, Siogkas P, Kyriakidis S, Tachos N, Karanasiou G, Scholte A, Clemente A, Neglia D, et al. Non-Invasive Prediction of Site-Specific Coronary Atherosclerotic Plaque Progression using Lipidomics, Blood Flow, and LDL Transport Modeling. Applied Sciences. 2021; 11(5):1976. https://doi.org/10.3390/app11051976
Chicago/Turabian StyleSakellarios, Antonis I., Panagiota Tsompou, Vassiliki Kigka, Panagiotis Siogkas, Savvas Kyriakidis, Nikolaos Tachos, Georgia Karanasiou, Arthur Scholte, Alberto Clemente, Danilo Neglia, and et al. 2021. "Non-Invasive Prediction of Site-Specific Coronary Atherosclerotic Plaque Progression using Lipidomics, Blood Flow, and LDL Transport Modeling" Applied Sciences 11, no. 5: 1976. https://doi.org/10.3390/app11051976
APA StyleSakellarios, A. I., Tsompou, P., Kigka, V., Siogkas, P., Kyriakidis, S., Tachos, N., Karanasiou, G., Scholte, A., Clemente, A., Neglia, D., Parodi, O., Knuuti, J., Michalis, L. K., Pelosi, G., Rocchiccioli, S., & Fotiadis, D. I. (2021). Non-Invasive Prediction of Site-Specific Coronary Atherosclerotic Plaque Progression using Lipidomics, Blood Flow, and LDL Transport Modeling. Applied Sciences, 11(5), 1976. https://doi.org/10.3390/app11051976








