Healthcare Waste Management: A Case Study from Sudan
Abstract
1. Introduction
- Low vaccination rates among HCPs, lack of taking occupational precaution measurements e.g., personal protective equipment (PPE) [32];
- Examine how used needles are managed including handling, storage, transportation, treatment and disposal;
- Examine the possible factors (barriers and challenges, etc.), which led to the current used needles management situation;
- Suggest practical steps for an improved and safer system of needles’ management in Khartoum.
2. The Case Study
- Almost all types of wastes being mixed together;
- The partial separation of wastes existing only in a few hospitals;
- Most of the workers being illiterate or having very low education levels, and there being a shortage of personal protective equipment (PPE) (e.g., boots, aprons, gloves);
- At the hospital level, no policies or rules being found except in a few centers;
- Limited training and that which is provided being inefficient;
- In the majority of the hospitals (75%), the transportation of HCW to temporary storage areas being done manually;
- A colour-coding system often not being implemented.
3. Materials and Methods
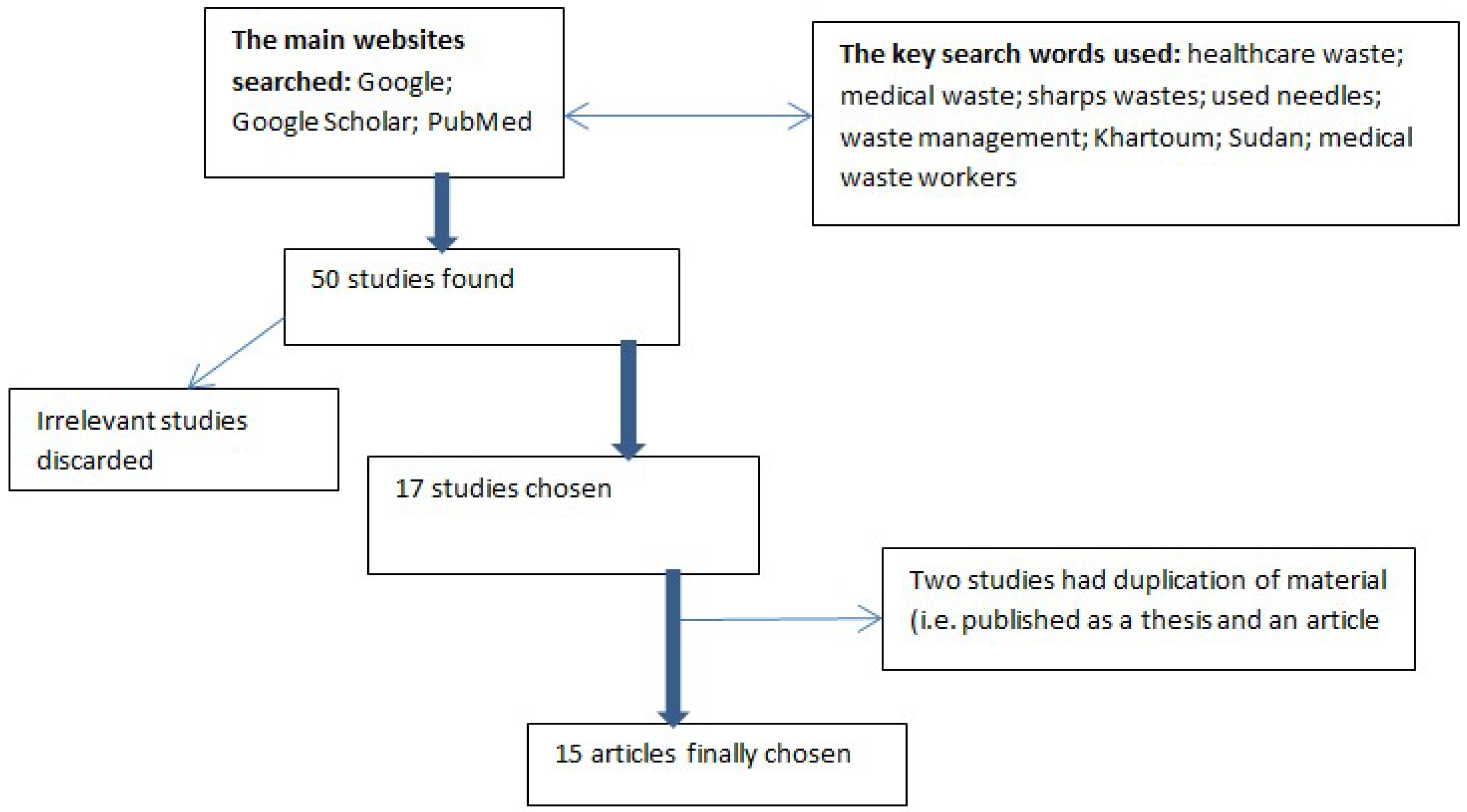
3.1. Content Analyses
3.2. Direct Observations
3.3. Interviews about Used Needles Management Issues with the HCP
3.4. Data Collection and Analysis
- The published data were categorised according to the geographical area, i.e., state;
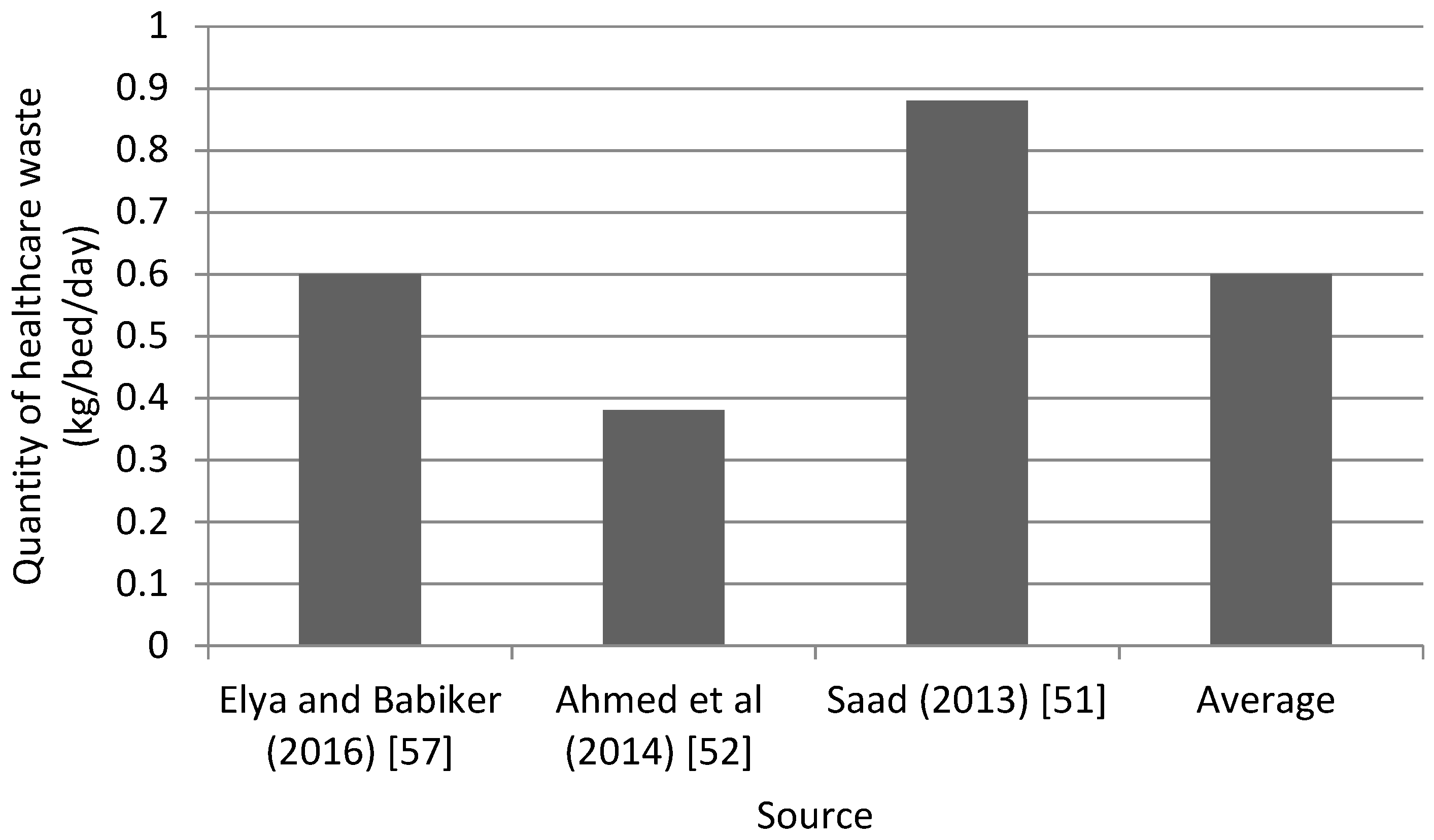
- The HCW production (kg/bed/day) was estimated;
- The main existing practices of managing used needles;
- Reporting of training, PPE, vaccination status and NSI issues;
- The key mentioned barriers and recommendations from the published research regarding used needles management in Sudan.
4. Results
4.1. Content Analyses
4.1.1. NSIs Reported by SFMOH
4.1.2. Current Used Needles Management in Sudan
- Waste minimisation and segregation: there was no plan; irrational use of injections is common; lack of waste segregation.
- Waste handling: manual handling of HCW from the wards to the storage area, this increases the possibility of NSIs, especially as misuse of safety boxes is common; no or partial availability of PPE; partial segregation of waste; auto-retracted syringes are used in few of the observed hospitals.
- Storage: the storage area was not secure; there was a delay in disposing needles.
- Transportation: the vehicles (compactor, lorries, tipper, trailer) were not fulfilling the WHO standards [75]; lack of commitment to scheduling times.
- Treatment: no technologies such as autoclave or disinfection were used to treat used needles; no needle cutters; there is a possibility of the reuse of needles.
- Disposal: based on the review findings, many options are employed in Sudan to dispose of the used needles generated either in HCFs or in the home, as follows: (i) placed in a safety box or locally made sharps container (plastic bottle) and disposed of through burning in an incinerator, or buried; (ii) mixed with other HCW and disposed through a landfill site, or by burning; (iii) mixed with healthcare domestic waste and disposed of through an open dumpsite, burnt in the open environment, or a landfill site; (iv) disposed on the ground.
4.1.3. HCWM in the Rural HCFs
- Lack of water and sanitation;
- No electricity for operations such as autoclave, steam sterilisation and incineration;
- Lack of transportation, especially in the rainy season;
- Lack of the awareness among doctors and nurses, etc.
4.2. Observations
4.2.1. Safety Box Usage
4.2.2. Observation of HCWM Practices
4.3. Interviews
- Lack of awareness regarding the danger and the long-term consequences (hepatitis and HIV) of such practices among HCP, especially those who are in direct contact with waste, such as waste workers
- No enforced policy in place, such as colour coding and labelling for waste disposal
- Lack of resources, i.e., shortage of safety boxes and insufficient budget for HCWM
- No dedicated department to deal with HCWM, i.e., that can monitor, evaluate and take appropriate actions accordingly
- Lack of training, especially among waste workers.
- Limited budgets for training purposes, in addition to the inefficient management of the allocated budget
- The decisions makers are perhaps not aware of the cost effectiveness of training i.e., through training, the segregation and recycling of waste will increase
- Lack of HCWM experts.
5. Discussion
- Short-term recommendations:
- Workshops for the involved parties such as the Ministry of Health, hospital administrations, public health personnel, HCW disposal companies, physicians, nurses, researchers, pharmacists, diabetes organisations and societies, diabetes educators, etc. The materials for the workshop should be organised with the involvement of all parties
- Patients’ educational sessions about the safe disposal of sharps, especially at home
- Provision to patients of safe disposal tools, such as a safety box and a community drop safety box, this can be organised with pharmaceutical companies and non-governmental organisation (NGOs)
- Community involvement through the launching of campaigns for safe sharps disposal (posters, brochures, media sessions, etc.). Public awareness about the hazards and risks of HCW is a key of success [95]
- Knowing the main stakeholders and their influence regarding waste management
- Rapid assessment of HCW among the HCFs, including the availability of an incinerator for each HCF. For this purpose, the WHO Individualised Rapid Assessment Tool (I-RAT) can be used [96].
- Medium-term recommendations:
- Encourage the use of the available HCWM technologies
- Training and periodic updating of the staff on different aspects related to safe HCWM, such as OSH, rational usage of medicines and operation of sharps pits and incinerators. Meanwhile, the ten proposed recommendations by Laing et al. [98] to improve rational medicine usage in developing countries can be adopted in the Sudan context. Provision of training was found to be effective in reducing the rate and underreporting of NSIs [99]
- Allocation of enough resources such as budget, safety boxes, personnel, and vehicles for HCWM and PPE. However, PPE should be used as the last option of protection in the hierarchy of hazard controls [100]. The strategy for HCW should focus on the most effective control measures e.g., minimisation of needle usage, use of engineering (e.g., auto-retracting syringes, safety boxes, etc.), and administrative (e.g., setting of policies, training, etc.) [101]
- Conducting audits for HCWM
- Documentation should be encouraged to identify the amount of waste and to trace the waste from the generating facility to the end of disposal. In addition, record keeping should be introduced at all HCF levels
- Establishment of sharps pits or incinerators according to the needs based on the results of the initial survey.
- Long-term recommendations:
- Development and effective implementation of HCWM legislation
- An environmental impact assessment should be implemented for all HCFs and should be mandatory before establishing any new facility
- Alternative technologies can be used. However, before selecting any technology, basic information should be available: (a) the size of the target facility, whether it is small, medium, large, or at the national level; (b) the estimated amount of waste generated; and (c) the cost of the needed technology.
6. Conclusions
- Policies regarding the safe handling and disposal of sharps, vaccination, OSH, reporting of NSIs, PEP, and colour coding and labelling for waste disposal;
- Initiatives to raise awareness of safe sharps disposal among HCP and the public through education, training and the launching of campaigns, i.e., posters, brochures, media sessions, etc.
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO. Injection Safety. 2012. Available online: http://www.wpro.who.int/mediacentre/factsheets/fs_20120204/en/ (accessed on 18 December 2017).
- Caniato, M.; Tudor, T.L.; Vaccari, M. Assessment of health-care waste management in a humanitarian crisis: A case study of the Gaza Strip. Waste Manage. 2016, 58, 386–396. [Google Scholar] [CrossRef] [PubMed]
- Health Care without Harm. Treating Sharps Waste. 2017. Available online: https://noharm-global.org/issues/global/treating-sharps-waste (accessed on 23 July 2017).
- CDC. Sharps Safety for Healthcare Settings. 2015. Available online: https://www.cdc.gov/sharpssafety/ (accessed on 30 July 2017).
- Pepin, J.; Abou Chakra, C.N.; Pépin, E.; Nault, V.; Valiquette, L. Evolution of the global burden of viral infections from unsafe medical injections, 2000-2010. PLoS ONE 2014, 9, e99677. [Google Scholar] [CrossRef] [PubMed]
- Chartier, Y.; Emmanuel, J.; Pieper, U.; Annette, P.; Rushbrook, P.; Stringer, S.; Townend, W.; Stringer, W.; Zghondi, R. Safe Management of Wastes from Health-Care Activities, 2nd ed.; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- Ahmed, A.A; Awooda, E.M.; Elbeshir, E.I. Dentists knowledge, attitude and practice towards dental waste management in private clinics-Khartoum locality. Int. J. Latest Res. Sci. Technol. 2014, 3, 93–96. [Google Scholar]
- Caniato, M.; Tudor, T.; Vaccari, M. International governance structures for health-care waste management: A systematic review of scientific literature. J. Environ. Manage. 2015, 153, 93–107. [Google Scholar] [CrossRef] [PubMed]
- Vaccari, M.; Tudor, T.; Perteghella, A. Costs associated with the management of waste from healthcare facilities: An analysis at national and site level. Waste Manage. Res. 2018, 36, 39–47. [Google Scholar] [CrossRef] [PubMed]
- Waljee, J.F.; Malay, S.; Chung, K.C. Sharps Injuries: The Risks and Relevance to Plastic Surgeons. Plast. Reconstr. Surg. 2013, 131, 784–791. [Google Scholar] [CrossRef] [PubMed]
- Lavoie, M.C.; Verbeek, J.H.; Pahwa, M. Devices for preventing percutaneous exposure injuries caused by needles in healthcare personnel. Cochrane Db. Syst. Rev. 2014. [Google Scholar] [CrossRef] [PubMed]
- McDowell, C.L. First Hand: The Surgeon and Hepatitis, C. J. Hand Surg. 2012, 37, 1693–1694. [Google Scholar] [CrossRef]
- Adib-Hajbaghery, M.; Lotfi, M.S. Behavior of Healthcare Workers after Injuries from Sharp Instruments. Trauma Mon. 2013, 18, 75–80. [Google Scholar] [CrossRef] [PubMed]
- Naghavi, S.H.R.; Shabestari, O.; Alcolado, J. Post-traumatic stress disorder in trainee doctors with previous needlestick injuries. Occup. Med. 2013, 63, 260–265. [Google Scholar] [CrossRef] [PubMed]
- Basel Convention. Basel Convention on the Control of Transboundary Movements of Hazardous Wastes and Their Disposal. 2011. Available online: http://www.basel.int/portals/4/basel%20convention/docs/text/baselconventiontext-e.pdf (accessed on 2 November 2016).
- Ream, P.S.; Tipple, A.F.; Barros, D.X.; Souza, A.C.; Pereira, M.S. Biological risk among hospital housekeepers. J. Arch. Environ. Occup. Health. 2014, 71, 59–65. [Google Scholar] [CrossRef] [PubMed]
- Bokhoree, C.; Beeharry, Y.; Makoondlall-Chadee, T.; Doobah, T.; Soomary, N. Assessment of environmental and health risks associated with the management of medical waste in Mauritius. Apcbee Procedia. 2014, 9, 36–41. [Google Scholar] [CrossRef]
- Ndejjo, R.; Musinguzi, G.; Yu, X.; Buregyeya, E.; Musoke, D.; Wang, J.S.; Halage, A.A.; Whalen, C.; Bazeyo, W.; Williams, P.; et al. Occupational health hazards among healthcare workers in Kampala, Uganda. Inter. J. Env. Res. Pub. Heal. 2015. [Google Scholar] [CrossRef]
- Vaccari, M.; Perteghella, A.; Stolfini, M.; Tudor, T. Overcoming public health risks to staff during the management of waste from healthcare facilities: Case studies from Italy. Int. J. Technol. Health. Care Qual. Assess. 2018, 31. [Google Scholar] [CrossRef] [PubMed]
- Tibbetts, J. Garbage collection is one of the most hazardous jobs. Can. Med. Assoc. J. 2013, 185, 284. [Google Scholar] [CrossRef] [PubMed]
- Sefouhi, L.; Kalla, M.; Bahmed, L.; Aouragh, L. The risk assessment for the healthcare waste in the hospital of Batna city. Algeria. Inter. J. Env. Sci. Develop. 2013, 4, 442–445. [Google Scholar] [CrossRef]
- Alwabr, G.M.; Al-Mikhlafi, A.S.; Al-Hakimi, S.A.; Dughish, M.A. Risk assessment of the current handling of medical waste in hospitals of Sana’a city Yemen. Inter. J. Sci. Technol. 2017, 3, 1–9. [Google Scholar] [CrossRef]
- Biodex. Sharps Container Shields. 2017. Available online: http://m.biodex.com/nuclear-medicine/products/syringe-vial-shields/sharps-container-shields (accessed on 6 August 2017).
- WHO. WHO Guideline on the Use of Safety-Engineered Syringes for Intramuscular, Intradermal and Subcutaneous Injections in Health-Care Settings. 2015. Available online: http://apps.who.int/iris/bitstream/10665/170470/1/WHO_HIS_SDS_2015.5_eng.pdf shields (accessed on 29 July 2017).
- Marinho, T.A.; Lopes, C.L.R.; Teles, S.A.; Reis, N.R.S.; Carneiro, M.A.D.S.; Andrade, A.A.D.; Martins, R.M.B. Prevalence of hepatitis C virus infection among recyclable waste collectors in Central-West Brazil. Mem. Inst. Oswaldo Cruz. 2013, 108, 519–522. [Google Scholar] [CrossRef] [PubMed]
- Majeed, A.; Batool, S.A.; Chaudhry, M.N.; Siddique, R.A. Scavenging demeanor in Bahawalpur, Pakistan: Social and health perspective. J. Mater. Cycles Waste Manag. 2017, 19, 815–826. [Google Scholar] [CrossRef]
- Alemayehu, T.; Worku, A.; Assefa, N. Medical Waste Collectors in Eastern Ethiopia are Exposed to High Sharp Injury and Blood and Body Fluids Contamination. J. Prev. Infect. Control. 2016, 2, 1–10. [Google Scholar] [CrossRef]
- Mol, M.P.; Gonçalves, J.P.; Silva, E.A.; Scarponi, C.F.; Greco, D.B.; Cairncross, S.; Heller, L. Seroprevalence of hepatitis B and C among domestic and healthcare waste handlers in Belo Horizonte, Brazil. Waste Manage. Res. 2016, 34, 875–883. [Google Scholar] [CrossRef] [PubMed]
- Tadesse, M.; Tadesse, T. Epidemiology of needle stick injuries among health-care workers in Awassa City, Southern Ethiopia. Trop. Doct. 2010, 40, 111–113. [Google Scholar] [CrossRef] [PubMed]
- Elseviers, M.M.; Arias-Guillén, M.; Gorke, A.; Arens, H.J. Sharps injuries amongst healthcare workers: Review of incidence, transmissions and costs. J. Ren Care. 2014, 40, 150–156. [Google Scholar] [CrossRef] [PubMed]
- Himmelreich, H.; Rabenau, H.F.; Rindermann, M.; Stephan, C.; Bickel, M.; Marzi, I.; Wicker, S. The Management of Needle stick Injuries. Dtsch. Ärzteblatt Int. 2013, 110, 61–67. [Google Scholar]
- Westermann, C.; Peters, C.; Lisiak, B.; Lamberti, M.; Nienhaus, A. The prevalence of hepatitis C among healthcare workers: A systematic review and meta-analysis. Occup. Environ. Med. 2015, 72, 880–888. [Google Scholar] [CrossRef] [PubMed]
- Nail, A.; Eltiganni, S.; Imam, A. Seroprevalence of Hepatitis B and C among health care workers in Omdurman, Sudan. Sudan J. Med. Sci. 2008, 3, 201–206. [Google Scholar] [CrossRef]
- Elduma, A.H.; Saeed, N.S. Hepatitis B virus infection among staff in three hospitals in Khartoum, Sudan, 2006–07. East Mediterr Health J. 2011, 17, 474–478. [Google Scholar] [CrossRef]
- WHO. Health-Care Waste Fact Sheet N.°253. 2016. Available online: http://www.who.int/mediacentre/factsheets/fs253/en/ (accessed on 31 October 2016).
- Di Bella, V.; Ali, M.; Vaccari, M. Constraints to healthcare waste treatment in low-income countries-A case study from Somaliland. Waste Manage. Res. 2012, 30, 572–575. [Google Scholar] [CrossRef] [PubMed]
- Hanafi, M.I.; Mohamed, A.M.; Kassem, M.S.; Shawki, M. Needlestick injuries among health care workers of University of Alexandria Hospitals. East Mediterr Health J. 2011, 17, 26–35. [Google Scholar] [CrossRef] [PubMed]
- Afridi, A.A.K.; Kumar, A.; Sayani, R. Needle stick injuries–risk and preventive factors: A study among health care workers in tertiary care hospitals in Pakistan. Glob. J. Health Sci. 2013, 5, 85–92. [Google Scholar] [CrossRef] [PubMed]
- MacCannell, T.; Laramie, A.K.; Gomaa, A.; Perz, J.F. Occupational exposure of health care personnel to hepatitis B and hepatitis C: Prevention and surveillance strategies. Clin. Liver. Dis. 2010, 14, 23–36. [Google Scholar] [CrossRef] [PubMed]
- Centre for Disease Control (CDC). Evaluation of Safety Devices for Preventing Percutaneous Injuries among Healthcare Workers during Phlebotomy Procedures-Minneapolis-St. Paul, New York City, and San Francisco. Morb. Mortal Wkly. Rep. 1997, 46, 21–23. [Google Scholar]
- Sudan Central Bureau of Statistics. Censuses. 2017. Available online: http://www.cbs.gov.sd/en/files.php?id=7#&panel1-2 (accessed on 28 July 2017).
- SFMOH. Annual Health Statistical Report, 2015. 2016. Available online: http://www.fmoh.gov.sd/yearlyReports/Annual2015.pdf (accessed on 6 December 2017).
- Pai, R.; Rodrigues, L.L.; Mathew, A.O.; Hebbar, S. Impact of urbanization on municipal solid waste management: A system dynamics approach. Int. J. Renew. Energy Environ. Eng. 2014, 2, 31–37. [Google Scholar]
- Dahiya, R. Projections for the population growth and its impact on solid waste generation of medium sized north Indian city. Int. J. Tech. Res. Appl. 2015, 3, 57–61. [Google Scholar]
- Das, S.; Bhattacharyya, B.K. Estimation of municipal solid waste generation and future trends in greater metropolitan regions of Kolkata, India. J. Ind. Eng. Manag. Innovat. 2014, 1, 31–38. [Google Scholar] [CrossRef]
- UN. Independence of South Sudan. 2011. Available online: http://www.un.org/en/peacekeeping/missions/past/unmis/referendum.shtml (accessed on 18 February 2016).
- Udombana, N.J. When neutrality is a sin: The Darfur crisis and the crisis of humanitarian intervention in Sudan. Hum. Rights Q. 2005, 27, 1149–1199. [Google Scholar] [CrossRef]
- Gramizzi, C.; Tubiana, J. New War, Old Enemies: Conflict Dynamics in South Kordofan; The Small Arms Project: Geneva, Switzerland, 2013. [Google Scholar]
- UNDP. Sudan. Human Development Indicators. 2016. Available online: http://hdr.undp.org/en/countries/profiles/SDN (accessed on 29 July 2017).
- Minoglou, M.; Gerassimidou, S.; Komilis, D. Healthcare Waste Generation Worldwide and Its Dependence on Socio-Economic and Environmental Factors. Sustainability 2017, 9, 220. [Google Scholar] [CrossRef]
- Saad, S.A. Management of Hospitals Solid Waste in Khartoum State. Environ. Monit. Assess. 2013, 185, 8567–8582. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, N.O.; Gasmelseed, G.A.; Musa, A.E. Assessment of Medical Solid Waste Management in Khartoum State Hospitals. Jpn. J. Ind. Appl. Math. 2014, 2, 201–205. [Google Scholar]
- Idris, MGM. Medical Waste Management in Some Hospitals in Sudan. University of Khartoum, 2016. Available online: http://khartoumspace.uofk.edu/handle/123456789/20910 (accessed on 6 September 2016).
- Eltayeb, E.; Magdah, E.; Abdelelah, M.; Mohamed, E.; Khouya, K.; Benkaddour, R. Knowledge, Attitude and Practice towards Collection and Disposal of Medical Waste among Medical Waste Workers in Khartoum State Hospitals, Sudan (2013–2016). Appl. J. Environ. Eng. Sci. 2017, 3, 268–279. [Google Scholar]
- Abd Elgadir, A. Assessment of Medical Immunization Waste Management in Khartoum (Doctoral Dissertation, UOFK). Available online: http://khartoumspace.uofk.edu/handle/123456789/7628 (accessed on 13 August 2017).
- Fath, E.I.A.; Magdi, B. Evaluation of Laboratory Biosafety in Khartoum State Primary Health Care Centers, Sudan. Med. Saf. Global Health. 2016, 5, 126. [Google Scholar]
- Elya, T.B.; Babiker, A.B. Assessment of Medical Waste Management in Port Sudan Teaching Hospital, Sudan. Int. J. Sci. Res. 2016, 5, 586–589. [Google Scholar]
- Tairab, M.A.O. Knowledge, Attitudes and Practices towards Medical Waste Hazards among Health Cleaners at Bahari and Sharq Al-Neel Hospitals. Master’s Thesis, University of Khartoum, Khartoum, Sudan, June 2009. [Google Scholar]
- The Interim National Constitution of the Republic of the Sudan. 2005. Available online: http://www.refworld.org/pdfid/4ba749762.pdf (accessed on 9 November 2016).
- Environmental Protection Act 2001. Sudan Parliament. Available online: http://www.parliament.gov.sd/ar/index.php/site/LigsualtionVeiw/210 (accessed on 24 December 2014).
- Higher Council for Environment and Natural Resources. National Implementation Plan for the Stockholm Covention on POPs. 2007. Available online: http://www.pops.int/documents/implementation/nips/submissions/NIP_Sudan.pdf (accessed on 9 November 2016).
- UNEP. Sudan Ratifies Paris Climate Agreement. 2017. Available online: http://www.unep.org/disastersandconflicts/news/sudan-ratifies-paris-climate-agreement (accessed on 10 August 2017).
- KSMOH. Guideline to the Safe Disposal of Medical Waste. 2012. Available online: http://ksmoh.gov.sd/dpre.pdf (accessed on 25 July 2017).
- Abdalgadir, M.A.; Osman, F.F.A.; Bushara, M.O.E.; Alawneh, S.M.A. 2016. Knowledge Attitude and Practice of the Workers towards Health Care Waste Safety Measures in Khartoum State Governmental Hospitals. Eur. J. Pharm. Med. Res. 2015, 3, 580–584. [Google Scholar]
- Hassan, E.M.A.; Bashir, N.F. Evaluation of Medical Waste Treatment in Sudanese Hospitals. Inter. J. Env. Res. Eng. Sci. 2016, 4, 49–54. [Google Scholar]
- Yousif, M.; Elfadil, H.; Eldalo, A.; Nasr. Sudanese patients’ perception on injections. Saudi J. Health Sci. 2012, 1, 99–102. [Google Scholar] [CrossRef]
- Osman, O.B.; Osman, F.F.A.; Mohamed, M.H.; Ahmed, H.R.M. Effect of health awareness interventions on knowledge, attitudes and practices of health providers and workers involve in health care waste aspects at Khartoum North Teaching hospital. Eur. J. Pharm. Med. Res. 2015, 2, 124–132. [Google Scholar]
- Elhassan, R.M.; Ibrahim, M.A. The Effect of Handling of Laboratory Wastes on Liver Function Tests among Handlers in National Laboratory for Public Health in Khartoum State. Eur. Acad. Res. 2016, 4, 1060–1069. [Google Scholar]
- Elnour, A.M.; Moussa, M.M.R.; El-Borgy, M.D.; Fadelella, N.E.; Mahmoud, A.H. Impacts of health education on knowledge and practice of hospital staff with regard to Healthcare waste management at White Nile State main hospitals, Sudan. Int. J. Health Sci. 2015, 9, 315–331. [Google Scholar]
- SHO. Environmental Health, Category Guidelines/SOPs. 2017. Available online: http://sho.gov.sd/controller/knowledge_hub.php?mid=110&sm_id=&lid=1# (accessed on 20 August 2017).
- Alsudanalyoum. Healthcare Waste Incinerators in Khartoum State and Hepatitis. 2017. Available online: http://alsudanalyoum.com/2017/07/30/page/3/ (accessed on 8 November 2017).
- Alnilin. Healthcare Waste on the Road. 2013. Available online: http://www.alnilin.com/689461.htm (accessed on 29 September 2017).
- Sudaress. Healthcare Waste, Information and Facts. 2013. Available online: https://www.sudaress.com/rayaam/308497 (accessed on 15 October 2017).
- Seedbed. Hospital Waste. 2017. Available online: http://seedbed.nl/hospital-waste.html (accessed on 20 November 2017).
- WHO. Technologies. 2017. Available online: https://www.healthcare-waste.org/resources/technologies/ (accessed on 2 August 2017).
- Mansab, M.R. Sharp waste management at Kidongo Chekundu National Mental Hospital Zanzibar Tanzania”. Master’s Thesis, The Open University of Tanzania, Salaam, Tanzania, September 2014. Available online: http://repository.out.ac.tz/605/1/MANSAB_MANSAB_RAMADHAN_-DISSERTATION.pdf (assessed on 10 August 2017).
- Abeje, G.; Azage, M. Hepatitis B vaccine knowledge and vaccination status among health care workers of Bahir Dar City Administration, Northwest Ethiopia: A cross sectional study. BMC Infect. Dis. 2015, 15, 30. [Google Scholar] [CrossRef] [PubMed]
- Udofia, E.A.; Fobil, J.N.; Gulis, G. Solid medical waste management in Africa. Afr. J. Environ. Sci. Technol. 2015, 9, 244–254. [Google Scholar]
- Udofia, E.A.; Gulis, G.; Fobil, J. Solid medical waste: A cross sectional study of household disposal practices and reported harm in Southern Ghana. BMC Public Health 2017, 17, 464. [Google Scholar] [CrossRef] [PubMed]
- ANA. 7 Things to Do in Response to Needle Stick Injury. 2010. Available online: http://www.nursingworld.org/DocumentVault/OccupationalEnvironment/Needles/7-Responses.pdf (accessed on 22 August 2017).
- NIOSH. Emergency Sharps Information. 2016. Available online: https://www.cdc.gov/niosh/topics/bbp/emergnedl.html (accessed on 17 August 2017).
- Health Authority of Abu Dhabi. Medical Waste Management in Health Care Facilities. 2009. Available online: https://www.haad.ae/haad/Portals/0/Policies_Docs/Policy%20on%20Medical%20Waste%20Mangement%20in%20the%20HCFs.pdf (accessed on 14 November 2017).
- La Torre, G.; Scalingi, S.; Garruto, V.; Siclari, M.; Chiarini, M.; Mannocci, A. Knowledge, Attitude and Behaviours towards Recommended Vaccinations among Healthcare Workers. Healthcare (Basel) 2017, 5, E13. [Google Scholar] [CrossRef] [PubMed]
- Elmukashfi, T. Sero-Epidemiological Survey of Hepatitis B Markers among Health Care Workers in Public Hospitals in Khartoum State in the Year 2004. Ph.D. Thesis, University of Khartoum, Khartoum, Sudan, July 2015. [Google Scholar]
- Sudan Labor Law. 1997. Available online: http://www.ilo.org/dyn/natlex/docs/WEBTEXT/49122/65103/E97SDN01.htm (accessed on 1 August 2017).
- Amsalu, A.; Worku, M.; Tadesse, E.; Shimelis, T. The exposure rate to hepatitis B and C viruses among medical waste handlers in three government hospitals, southern Ethiopia. Epidemiol. Health 2016, 38, 1–8. [Google Scholar] [CrossRef]
- CDC. Recommended Vaccines for Healthcare Workers. 2017. Available online: https://www.cdc.gov/vaccines/adults/rec-vac/hcw.html (accessed on 21 August 2017).
- Tudor, T.L.; Noonan, C.L.; Jenkin, L.E.T. Healthcare waste management: A case study from the National Health Service in Cornwall, United Kingdom. Waste Manag. 2005, 25, 606–615. [Google Scholar] [CrossRef] [PubMed]
- Lavee, D. Is municipal solid waste recycling economically efficient? Environ. Manage. 2007, 40, 926–943. [Google Scholar] [CrossRef] [PubMed]
- Alam, M.Z.; Islam, M.S.; Islam, M.R. Medical Waste Management: A Case Study on Rajshahi City Corporation in Bangladesh. J Environ Sci Nat. Resour. 2015, 6, 173–178. [Google Scholar] [CrossRef]
- Hossain, M.S.; Santhanam, A.; Norulaini, N.N.; Omar, A.M. Clinical solid waste management practices and its impact on human health and environment–A review. Waste Manage. 2011, 31, 754–766. [Google Scholar] [CrossRef] [PubMed]
- Shannon, A.L.; Woolridge, A. Medical Waste. In Waste; Michigan Department of Natural Resources and Environment: Lansing, MI, USA, 2011; pp. 329–339. [Google Scholar]
- Kumar, R.; Somrongthong, R.; Ahmed, J. Impact of waste management training intervention on knowledge, attitude and practices of teaching hospital workers in Pakistan. Pak. J. Med. Sci. 2016, 32, 705–710. [Google Scholar] [CrossRef] [PubMed]
- Almahi, A.Y.Y. Assessment of the Radioactive Waste Management in Nuclear Medicine Departments in Khartoum State Hospitals. Available online: http://repository.sustech.edu/handle/123456789/14321 (accessed on 11 August 2017).
- Kusiluka, L.J.M.; Mkhandi, D.N.H.; Hango, M. Management of Medical Wastes: Public Awareness and Associated Health Risks. J. Open Univ. Tanzan. 2013, 15, 34–51. [Google Scholar]
- WHO. Individualised Rapid Assessment Tool (I-RAT). 2009. Available online: http://www.who.int/water_sanitation_health/facilities/waste/hcwmtool/en/ (accessed on 8 October 2016).
- Dabora, M.A.M.A. Efficiency of Recombinant DNA Vaccine against Hepatitis B Virus in Health Care Workers in Some Hospital in Khartoum State. Master’s Thesis, Sudan University of Science & Technology, Khartoum, Sudan, January 2014. [Google Scholar]
- Laing, R.O.; Hogerzeil, H.V.; Ross-Degnan, D. Ten recommendations to improve use of medicines in developing countries. Health Policy Plan. 2001, 16, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Yilmaz, L. Effect of the Training Provided for Nurses on Sharp-Needle stick Injuries and Reporting Process. International Journal of Caring Sciences, 2016, 9, 561. Int. J. Caring Sci. 2016, 9, 561. [Google Scholar]
- NIOSH. Hierarchy of Controls. 2015. Available online: https://www.cdc.gov/niosh/topics/hierarchy/default.html (accessed on 22 September 2017).
- RCN. Sharps Safety. 2013. Available online: http://www.gla.ac.uk/media/media_511552_en.pdf (accessed on 23 August 2017).
| Reference | Issues | |||
|---|---|---|---|---|
| Training | PPE 1 | NSIs 2 | Vaccination | |
| [64] | Only 45% were trained on HCWM 3 | 46.5% of did not have PPE | 42.9% injured while working | 69% vaccinated against hepatitis |
| [57] | No hospital personnel were trained about HCWM and, infection control | Manual handling of waste without using PPE | 27% had NSIs | 4% of the HCP 4 were vaccinated |
| [7] | Training was available only in 40% of the investigated HCFs 5 | PPE only 30% in the investigated hospitals | - | - |
| [65] | Called for HCP training and education | Deficiency in protective measures | - | Recommended vaccination for workers, especially those at risk |
| [66] | - | - | Unacceptable injection disposal practices led to 26.1% NSIs | 26.3% of the injections given in the community were used for vaccination |
| [67] | After the intervention, an improvement in the knowledge, attitudes and practices regarding HCWM were reported | - | Decrease in the rate of NSIs and, HBV 6 infection | After the awareness intervention programme, the utilisation of HBV vaccination increased from 11% to 48% |
| 53] | The training programmes for HCP with respect to HCW 7 handling were not efficient | - | - | There was no recurrent medical follow-up and vaccination for HCPs |
| [68] | Recommended periodic training for HCPs | Only 62% were wearing PPE while handling HCW | Only 8% had NSIs | The study was carried on already-vaccinated HCPs |
| [58] | 61.7% do not receive any training in handling hazardous wastes | 95.8% of them used PPE | 91.3% checked with physicians after NSIs | 91.6% did not receive HBV vaccination |
| [69] | Improvement of the HCPs knowledge after educational intervention programme | More PPE were used by the staff after the programme | NSIs were more often reported by the staff | 69% of the study participants in the intervention group were not vaccinated |
| [55] | 42% of HCP were not trained. The training period was not enough for those who received training, and the provision of an education and training programme were recommended | PPE were not used properly i.e., either lack of PPE or they were not aware of its importance | Only 7.5% of HCP knew that HCW is a source of HBV | - |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hassan, A.A.; Tudor, T.; Vaccari, M. Healthcare Waste Management: A Case Study from Sudan. Environments 2018, 5, 89. https://doi.org/10.3390/environments5080089
Hassan AA, Tudor T, Vaccari M. Healthcare Waste Management: A Case Study from Sudan. Environments. 2018; 5(8):89. https://doi.org/10.3390/environments5080089
Chicago/Turabian StyleHassan, Ahmed Ali, Terry Tudor, and Mentore Vaccari. 2018. "Healthcare Waste Management: A Case Study from Sudan" Environments 5, no. 8: 89. https://doi.org/10.3390/environments5080089
APA StyleHassan, A. A., Tudor, T., & Vaccari, M. (2018). Healthcare Waste Management: A Case Study from Sudan. Environments, 5(8), 89. https://doi.org/10.3390/environments5080089






