Efficacy of Web-Based Weight Loss Maintenance Programs: A Randomized Controlled Trial Comparing Standard Features Versus the Addition of Enhanced Personalized Feedback over 12 Months
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
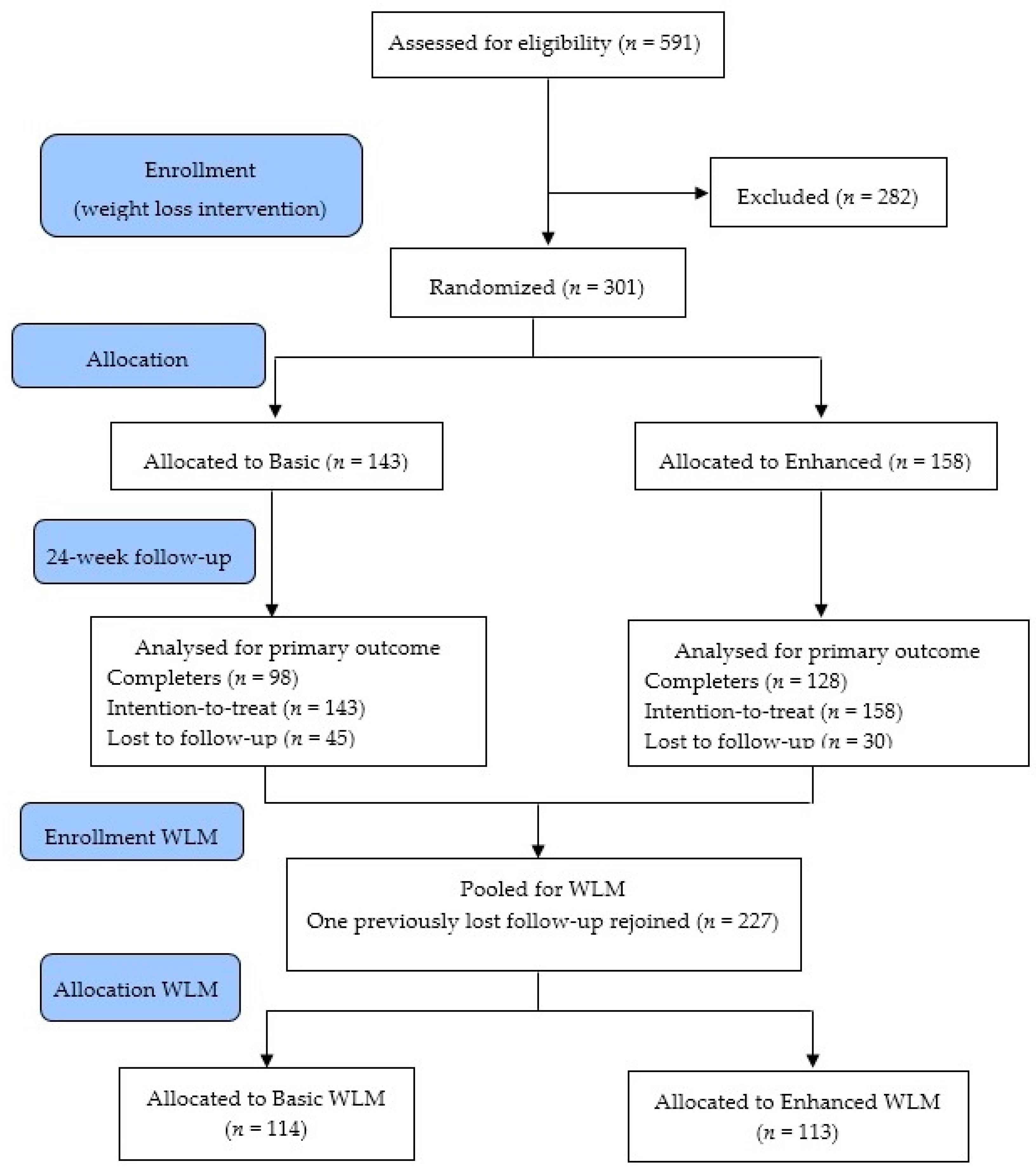
2.2. Study Design
2.3. Measures
2.4. Data Analysis
3. Results
4. Discussion
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- NCD Risk Factor Collaboration. Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 2017. [Google Scholar] [CrossRef]
- Collins, C.E.; Neve, M.J.; Williams, R.; Young, M.; Morgan, P.J.; Fletcher, K.R.C. Effectiveness of interventions with a dietary component on weight loss maintenance: A systematic review. JBI Database Syst. Rev. Implement. Rep. 2013, 11, 317–414. [Google Scholar] [CrossRef]
- Bond, D.S.; Phelan, S.; Leahey, T.M.; Hill, J.O.; Wing, R.R. Weight-loss maintenance in successful weight losers: Surgical vs non-surgical methods. Int. J. Obes. 2009, 33, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Burke, L.E.; Steenkiste, A.; Music, E.; Styn, M.A. A descriptive study of past experiences with weight-loss treatment. J. Am. Diet. Assoc. 2008, 108, 640–647. [Google Scholar] [CrossRef] [PubMed]
- Douketis, J.D.; Macie, C.; Thabane, L.; Williamson, D.F. Systematic review of long-term weight loss studies in obese adults: Clinical significance and applicability to clinical practice. Int. J. Obes. 2005, 29, 1153–1167. [Google Scholar] [CrossRef] [PubMed]
- Wadden, T.A.; Crerand, C.E.; Brock, J. Behavioral treatment of obesity. Psychiatr. Clin. N. Am. 2005, 28, 151–170. [Google Scholar] [CrossRef] [PubMed]
- Dombrowski, S.; Knittle, K.; Avenell, A.; Araujo-Soares, V.; Sniehotta, F. Long term maintenance of weight loss with non-surgical interventions in obese adults: Systematic review and meta-analyses of randomised controlled trials. BMJ 2014, 348. [Google Scholar] [CrossRef] [PubMed]
- Painter, S.L.; Ahmed, R.; Hill, J.O.; Kushner, R.F.; Lindquist, R.; Brunning, S.A.M. What matters in weight loss? An in-depth analysis of self-monitoring. J. Med. Internet Res. 2017, 19, e160. [Google Scholar] [CrossRef] [PubMed]
- Balk-Møller, N.C.; Poulsen, S.K.; Larsen, T.M. Effect of a nine-month web- and app-based workplace intervention to promote healthy lifestyle and weight loss for employees in the social welfare and health care sector: A randomized controlled trial. J. Med. Internet Res. 2017, 19, e108. [Google Scholar] [CrossRef] [PubMed]
- Watson, S.; Woodside, J.V.; Ware, L.J.; Hunter, S.J.; McGrath, A.; Cardwell, C.R.; Appleton, K.M.; Young, I.S.; Mckinlev, M.C. Effect of a web-based behavior change program on weight loss and cardiovascular risk factors in overweight and obese adults at high risk of developing cardiovascular disease: Randomized controlled trial. J. Med. Internet Res. 2015, 17, e177. [Google Scholar] [CrossRef] [PubMed]
- Hageman, P.A.; Pullen, C.H.; Hertzog, M.; Pozehl, B.; Eisenhauer, C.; Boeckner, L.S. Web-based interventions alone or supplemented with peer-led support or professional email counseling for weight loss and weight maintenance in women from rural communities: Results of a clinical trial. J. Obes. 2017, 2017. [Google Scholar] [CrossRef] [PubMed]
- Sidhu, M.S.; Daley, A.; Jolly, K. Evaluation of a text supported weight maintenance programme ‘lighten up plus’ following a weight reduction programme: Randomised controlled trial. Int. J. Behav. Nutr. Phys. Act. 2016, 13. [Google Scholar] [CrossRef] [PubMed]
- Sorgente, A.; Pietrabissa, G.; Manzoni, G.M.; Re, F.; Simpson, S.; Perona, S.; Rossi, A.; Cattivelli, R.; Innamorati, M.; Jackson, J.B.; et al. Web-based interventions for weight loss or weight loss maintenance in overweight and obese people: A systematic review of systematic reviews. J. Med. Internet Res. 2017, 19, e229. [Google Scholar] [CrossRef] [PubMed]
- Hutchesson, M.J.; Rollo, M.; Krukowski, R.; Ells, L.; Harvey, J.; Morgan, P.J.; Callister, R.; Plotnikoff, R.; Collins, C.E. Ehealth interventions for the prevention and treatment of overweight and obesity in adults: A systematic review with meta-analysis. Obes. Rev. 2015, 16, 376–392. [Google Scholar] [CrossRef] [PubMed]
- Collins, C.E.; Morgan, P.J.; Neve, M.J.; Callister, R. Efficacy of standard versus enhanced features in a web-based commercial weight-loss program for obese adults, part 2: Randomized controlled trial. J. Med. Internet Res. 2013, 15, e140. [Google Scholar] [CrossRef] [PubMed]
- Gold, B.; Burke, S.; Pintauro, S.; Buzzell, P.; Harvey-Berino, J. Weight loss on the web: A pilot study comparing a structured behavioral intervention to a commercial program. Obesity 2007, 15, 155–164. [Google Scholar] [CrossRef] [PubMed]
- Collins, C.E.; Morgan, P.J.; Jones, P.; Fletcher, K.; Martin, J.; Aguiar, E.J.; Lucas, A.; Neve, M.J.; Callister, R. A 12-week commercial web-based weight-loss program for overweight and obese adults: Randomized controlled trial comparing basic versus enhanced features. J. Med. Internet Res. 2012, 14, e57. [Google Scholar] [CrossRef] [PubMed]
- Collins, C.E.; Morgan, P.J.; Jones, P.; Fletcher, K.; Martin, J.; Aguiar, E.J.; Lucas, A.; Neve, M.; McElduff, P.; Callister, R. Evaluation of a commercial web-based weight loss and weight loss maintenance program in overweight and obese adults: A randomised controlled trial. BMC Public Health 2010, 10, 669. [Google Scholar] [CrossRef] [PubMed]
- Bamia, C.; Orfanos, P.; Ferrari, P.; Overvad, K.; Hundborg, H.H.; Tjønneland, A.; Olsen, A.; Kesse, E.; Boutron-Ruault, M.; Clavel-Chapelon, F.; et al. Dietary patterns among older europeans: The epic-elderly study. Br. J. Nutr. 2005, 94, 100–113. [Google Scholar] [CrossRef] [PubMed]
- Neve, M.; Morgan, P.J.; Jones, P.R.; Collins, C.E. Effectiveness of web-based interventions in achieving weight loss and weight loss maintenance in overweight and obese adults: A systematic review with meta-analysis. Obes. Rev. 2010, 11, 306–321. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Subgroup or Mean (SD) | Treatment Group | p-Value | ||
|---|---|---|---|---|---|
| Basic WLM (n = 114) | Enhanced WLM (n = 113) | All (n = 227) | |||
| Sex | Men | 48 (42%) | 52 (46%) | 100 (44%) | 0.55 |
| Country of birth | Australia | 108 (95%) | 100 (88%) | 208 (92%) | 0.23 |
| Highest level of education | School | 37 (32%) | 28 (25%) | 65 (29%) | 0.49 |
| Trade/Diploma | 41 (36%) | 40 (35%) | 81 (35%) | ||
| University Degree | 24 (21%) | 28 (25%) | 52 (23%) | ||
| Higher University Degree | 12 (11%) | 17 (15%) | 29 (13%) | ||
| Weekly household income (AUS$) | <$700 | 12 (11%) | 7 (6.4%) | 19 (8.8%) | 0.60 |
| $700 to <$1000 | 6 (5.7%) | 5 (4.5%) | 11 (5.1%) | ||
| $1000 to <$1400 | 13 (12%) | 11 (10%) | 24 (11%) | ||
| $1500 or more | 71 (67%) | 84 (76%) | 155 (72%) | ||
| Age (years) | mean (SD) | 43.3 (9.7) | 41.3 (10.3) | 42.3 (10.1) | 0.14 |
| Height (m) | mean (SD) | 1.70 (0.09) | 1.72 (0.09) | 1.71 (0.09) | 0.17 |
| Weight (kg) | mean (SD) | 88.5 (14.5) | 89.3 (15.6) | 88.9 (15.1) | 0.70 |
| Body mass index (kg/m2) | mean (SD) | 30.6 (4.1) | 30.1 (4.1) | 30.4 (4.1) | 0.45 |
| Waist circumference at umbilicus (cm) | mean (SD) | 100.6 (11.1) | 98.5 (11.7) | 99.6 (11.4) | 0.18 |
| Waist circumference at narrowest point (cm) | mean (SD) | 93.2 (11.5) | 92.2 (11.9) | 92.7 (11.7) | 0.52 |
| Waist to height ratio at umbilicus | mean (SD) | 0.59 (0.07) | 0.57 (0.07) | 0.58 (0.07) | 0.04 |
| Waist to height ratio at narrowest point | mean (SD) | 0.55 (0.07) | 0.54 (0.06) | 0.54 (0.06) | 0.15 |
| Weight loss at baseline entry to study (24 weeks) | mean (SD) | −4.38 (5.30) | −4.47 (6.37) | −4.42 (5.84) | 0.91 |
| Systolic blood pressure (mmHg) | mean (SD) | 117.5 (13) | 117.7 (12) | 117.6 (12.5) | 0.92 |
| Diastolic blood pressure (mmHg) | mean (SD) | 77.6 (10.6) | 77.2 (9.2) | 77.4 (9) | 0.76 |
| Resting heart rate (bpm) | mean (SD) | 64.6 (9.5) | 64.7 (10.2) | 64.6 (9.8) | 0.94 |
| Total serum cholesterol (mmol/L) | mean (SD) | 5.2 (1.1) | 4.8(1.0) | 5.0 (1.1) | 0.03 |
| LDL cholesterol (mmol/L) | mean (SD) | 3.1 (1.0) | 2.9 (0.8) | 3.0 (0.9) | 0.08 |
| HDL cholesterol (mmol/L) | mean (SD) | 1.3 (0.3) | 1.3 (0.3) | 1.3 (0.3) | 0.41 |
| Triglycerides (mmol/L) | mean (SD) | 1.5 (1.0) | 1.3 (0.7) | 1.4 (0.9) | 0.16 |
| Glucose (mmol/L) | mean (SD) | 4.6 (0.6) | 4.5 (0.7) | 4.6 (0.7) | 0.08 |
| Insulin (mIU/L) | mean (SD) | 6.6 (5.5) | 6.9 (6.2) | 6.7 (5.9) | 0.73 |
| Characteristic | Treatment Group Mean Change (SD) | Absolute Difference between Groups LSM (95% CI) | p Values for Group Effect | |
|---|---|---|---|---|
| Basic | Enhanced | Enhanced vs. Basic | Difference at Specified Time | |
| Weight (kg) | 1.3 (5.1) | 1.5 (4.4) | 0.15 (−1.09, 1.39) | 0.81 |
| Systolic blood pressure (mmHg) | 1.1 (12.1) | 1.1 (10.2) | 0.24 (−2.59, 3.08) | 0.87 |
| Diastolic blood pressure (mmHg) | −1.5 (8.1) | −0.1 (6.5) | 1.15 (−0.76, 3.06) | 0.24 |
| Body mass index (kg/m2) | 0.5 (1.9) | 0.5 (1.6) | 0.02 (−0.46, 0.50) | 0.93 |
| Pulse rate (bpm) | −0.3 (6.7) | 0.5 (5.8) | 0.74 (−0.88, 2.35) | 0.37 |
| Waist circumference at umbilicus (cm) | 3.8 (5.4) | 3.3 (4.9) | 0.76 (−0.63, 2.16) | 0.28 |
| Waist circumference at narrowest point (cm) | 2.6 (4.6) | 2.6 (4.6) | 0.11 (−1.12, 1.35) | 0.86 |
| Waist to height ratio at umbilicus | 0.0 (0.0) | 0.0 (0.0) | 0.01 (−0.00, 0.01) | 0.21 |
| Waist to height ratio at narrowest point | 0.0 (0.0) | 0.0 (0.0) | 0.00 (−0.01, 0.01) | 0.80 |
| Total serum cholesterol (mmol/L) | 0.1 (0.8) | 0.2 (0.7) | 0.07 (−0.12, 0.26) | 0.50 |
| LDL cholesterol (mmol/L) | 0.0 (0.6) | 0.1 (0.5) | 0.01 (−0.15, 0.16) | 0.94 |
| HDL cholesterol (mmol/L) | 0.0 (0.2) | 0.0 (0.2) | 0.00 (−0.06, 0.06) | 0.88 |
| Triglycerides (mmol/L) | 0.0 (0.5) | 0.2 (0.5) | 0.13 (−0.02, 0.27) | 0.10 |
| Glucose (mmol/L) | 0.1 (0.5) | 0.2 (0.5) | 0.08 (−0.05, 0.22) | 0.20 |
| Insulin (mIU/L) | 1.6 (4.2) | 0.89 (6.5) | 0.61 (−0.719, 2.01) | 0.39 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Collins, C.E.; Morgan, P.J.; Hutchesson, M.J.; Oldmeadow, C.; Barker, D.; Callister, R. Efficacy of Web-Based Weight Loss Maintenance Programs: A Randomized Controlled Trial Comparing Standard Features Versus the Addition of Enhanced Personalized Feedback over 12 Months. Behav. Sci. 2017, 7, 76. https://doi.org/10.3390/bs7040076
Collins CE, Morgan PJ, Hutchesson MJ, Oldmeadow C, Barker D, Callister R. Efficacy of Web-Based Weight Loss Maintenance Programs: A Randomized Controlled Trial Comparing Standard Features Versus the Addition of Enhanced Personalized Feedback over 12 Months. Behavioral Sciences. 2017; 7(4):76. https://doi.org/10.3390/bs7040076
Chicago/Turabian StyleCollins, Clare E., Philip J. Morgan, Melinda J. Hutchesson, Christopher Oldmeadow, Daniel Barker, and Robin Callister. 2017. "Efficacy of Web-Based Weight Loss Maintenance Programs: A Randomized Controlled Trial Comparing Standard Features Versus the Addition of Enhanced Personalized Feedback over 12 Months" Behavioral Sciences 7, no. 4: 76. https://doi.org/10.3390/bs7040076
APA StyleCollins, C. E., Morgan, P. J., Hutchesson, M. J., Oldmeadow, C., Barker, D., & Callister, R. (2017). Efficacy of Web-Based Weight Loss Maintenance Programs: A Randomized Controlled Trial Comparing Standard Features Versus the Addition of Enhanced Personalized Feedback over 12 Months. Behavioral Sciences, 7(4), 76. https://doi.org/10.3390/bs7040076






