Workplace Sexual Harassment and the Risk of Chronic Disease in a Prospective Cohort Study
Abstract
1. Introduction
2. Materials and Methods
3. Results
3.1. Baseline Characteristics
3.2. Chronic Disease Incidence
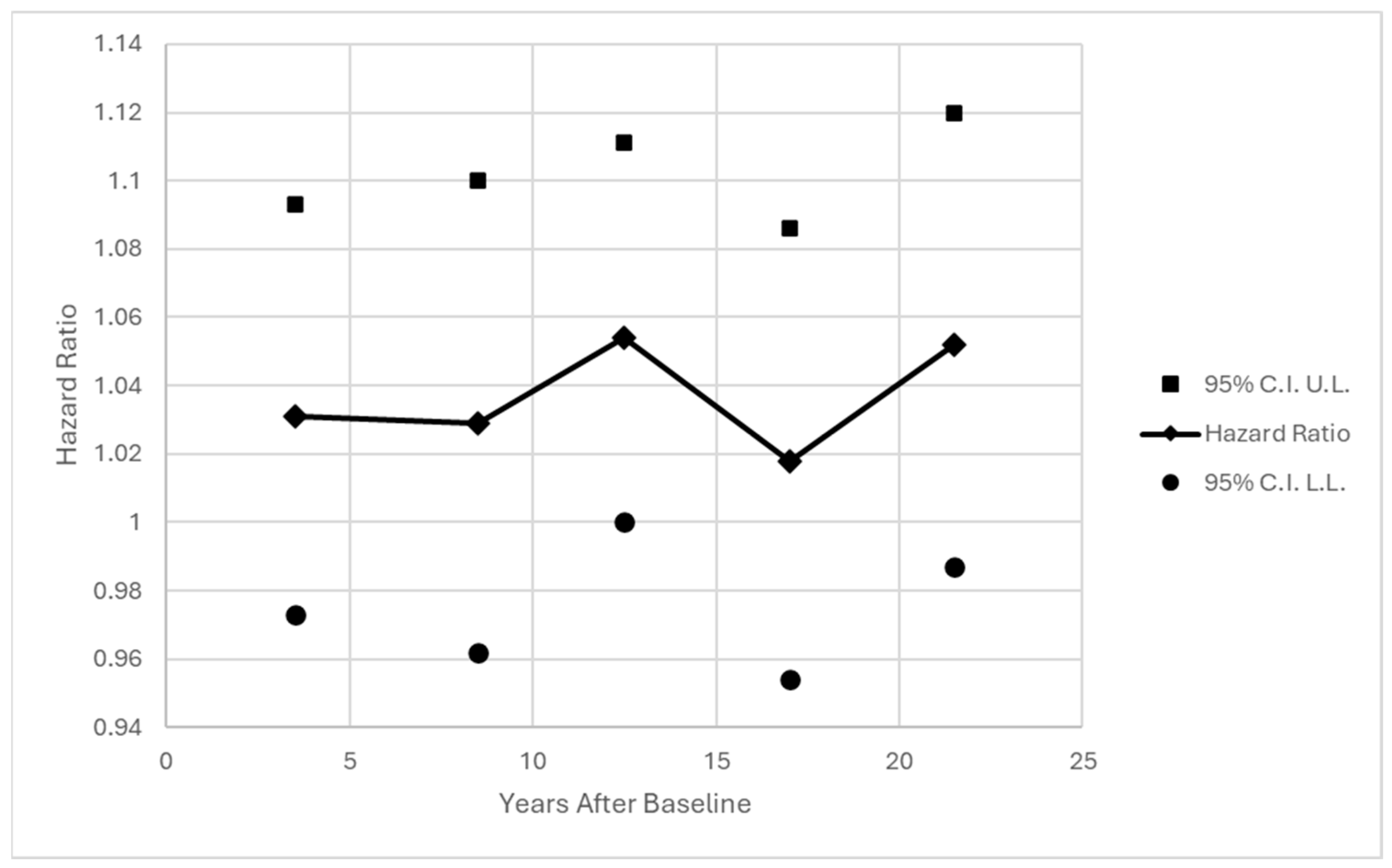
3.3. Initial Models Testing SEQ at Baseline Only
3.4. Model Building, Testing Possible Covariates
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Abdulla, A. M., Lin, T. W., & Rospenda, K. M. (2023). Workplace harassment and health: A long term follow up. Journal of Occupational and Environmental Medicine, 65(11), 899–904. [Google Scholar] [CrossRef]
- Baechle, J., Chen, N., Makhijani, P., Winer, S., Furman, D., & Winer, D. (2023). Chronic inflammation and the hallmarks of aging. Molecular Metabolism, 74, 101755. [Google Scholar] [CrossRef]
- Blindow, K. J., Cedstrand, E., Elling, D. L., Hagland, M., & Bodin, T. (2024). Gender-based violence and harassment at work and health and occupational outcomes. A systematic review of prospective studies. BMC Public Health, 24, 1788. [Google Scholar] [CrossRef]
- Blindow, K. J., Thern, E., Hernando-Rodriguez, J. C., Nyberg, A., & Magnusson Hanson, L. L. (2023). Gender-based harassment in Swedish workplaces and alcohol-related morbidity and mortality: A prospective cohort study. Scandinavian Journal of Work, Environment & Health, 49(6), 395–404. [Google Scholar] [CrossRef]
- Boffetta, P., & Hashibe, M. (2006). Alcohol and cancer. The Lancet Oncology, 7(2), 149–156. [Google Scholar] [CrossRef] [PubMed]
- Bolton, D. (2023). A revitalized biopsychosocial model: Core theory, research paradigms, and clinical implications. Psychological Medicine, 53, 7504–7511. [Google Scholar] [CrossRef]
- Buchanan, N. T., & Ormerod, A. J. (2002). Racialized sexual harassment in the lives of African American women. In C. M. West (Ed.), Violence in the lives of black women: Battered, black, and blue (1st ed., pp. 107–124). Routledge. [Google Scholar]
- Cahalen, D., Cisin, I. H., & Crossley, H. M. (1969). American drinking practices. Rutgers Center on Alcohol Studies. [Google Scholar]
- Centers for Disease Control and Prevention. (2023). Most recent national asthma data. Available online: https://www.cdc.gov/asthma/most_recent_national_asthma_data.htm (accessed on 12 January 2026).
- Centers for Disease Control and Prevention. (2024). National diabetes statistics report. Available online: https://www.cdc.gov/diabetes/php/data-research/index.html (accessed on 12 January 2026).
- Chan, D. K. S., Chow, S. Y., Lam, C. B., & Cheung, S. F. (2008). Examining the job-related, psychological, and physical outcomes of workplace sexual harassment: A meta-analytic review. Psychology of Women Quarterly, 32(4), 362–376. [Google Scholar] [CrossRef]
- Crimmins, E. M., Shim, H., Zhang, Y. S., & Kim, J. K. (2019). Differences between men and women in mortality and the health dimensions of the morbidity process. Clinical Chemistry, 65(1), 135–145. [Google Scholar] [CrossRef]
- Cullen, M., Lemeshow, A., Russo, L., Barnes, D., Ababio, Y., & Habtezion, A. (2022). Disease-specific health disparities: A targeted review focusing on race and ethnicity. Healthcare, 10(4), 603. [Google Scholar] [CrossRef]
- Dai, X., Gil, G. F., Reitsma, M. B., Ahmad, N. S., Anderson, J. A., Bisignano, C., Carr, S., Feldman, R., Hay, S. I., He, J., Iannucci, V., Lawlor, H. R., Malloy, M. J., Marczak, L. B., McLaughlin, S. A., Morikawa, L., Mullany, E. C., Nicholson, S. I., O’Connell, E. M., … Gakidou, E. (2022). Health effects associated with smoking: A burden of proof study. Nature Medicine, 28(10), 2045–2055. [Google Scholar] [CrossRef] [PubMed]
- Diez-Canseco, F., Toyama, M., Hidalgo-Padilla, L., & Bird, V. J. (2022). Systematic review of policies and interventions to prevent sexual harassment in the workplace in order to prevent depression. International Journal of Environmental Research and Public Health, 19(20), 13278. [Google Scholar] [CrossRef]
- Dillman, D. A., Smyth, J. D., & Christian, L. M. (2014). Internet, phone, mail, and mixed-mode surveys: The tailored design method. Wiley. [Google Scholar]
- Eaton, W. W., Armenian, H., Gallo, J., Pratt, L., & Ford, D. E. (1996). Depression and risk for onset of type II diabetes: A prospective population-based study. Diabetes Care, 19(10), 1097–1102. [Google Scholar] [CrossRef]
- Engel, G. L. (1977). The need for a new medical model: A challenge for biomedicine. Science, 196(4286), 129–136. [Google Scholar] [CrossRef] [PubMed]
- Equal Employment Opportunity Commission. (1980). CM-615 harassment. Available online: https://www.eeoc.gov/laws/guidance/cm-615-harassment (accessed on 12 January 2026).
- Fallon, E. A., Boring, M. A., Foster, A. L., Stowe, E. W., Lites, T. D., Odom, E. L., & Seth, P. (2023). Prevalence of diagnosed arthritis—United States, 2019–2021. Morbidity and Mortality Weekly Report (MMWR), 72, 1101–1107. [Google Scholar] [CrossRef] [PubMed]
- Ferketich, A. K., Schwartzbaum, J. A., Frid, D. J., & Moeschberger, M. L. (2000). Depression as an antecedent to heart disease among women and men in the NHANES I study. Archives of Internal Medicine, 160(9), 1261–1268. [Google Scholar] [CrossRef]
- Fitzgerald, L. F. (1996). Sexual harassment: The definition and measurement of a construct. In M. A. Paludi (Ed.), Sexual harassment on college campuses: Abusing the ivory power (pp. 21–44). State University of NY Press. [Google Scholar]
- Ganster, D., & Rosen, C. (2013). Work stress and employee health. Journal of Management, 39, 1085–1122. [Google Scholar] [CrossRef]
- Graham, E. A., Deschênes, S. S., Khalil, M. N., Danna, S., Filion, K. B., & Schmitz, N. (2020). Measures of depression and risk of type 2 diabetes: A systematic review and meta-analysis. Journal of Affective Disorders, 265, 224–232. [Google Scholar] [CrossRef] [PubMed]
- Jakubowski, K. P., Murray, V., Stokes, N., & Thurston, R. C. (2021). Sexual violence and cardiovascular disease risk: A systematic review and meta-analysis. Maturitas, 153, 48–60. [Google Scholar] [CrossRef]
- Joynt Maddox, K. E., Elkind, M. S. V., Aparicio, H. J., Commodore-Mensah, Y., de Ferranti, S. D., Dowd, W. N., Hernandez, A. F., Khavjou, O., Michos, E. D., Palaniappan, L., Penko, J., Poudel, R., Roger, V. L., Kazi, D. S., & American Heart Association. (2024). Forecasting the burden of cardiovascular disease and stroke in the United States through 2050-prevalence of risk factors and disease: A presidential advisory from the American Heart Association. Circulation, 150(4), e65–e88. [Google Scholar] [CrossRef]
- Karasek, R. A., & Theorell, T. (1990). Healthy work: Stress, productivity, and the reconstruction of working life. Basic Books. [Google Scholar]
- Liang, T. (2024). Sexual harassment at work: Scoping review of reviews. Psychology Research and Behavior Management, 17, 1635–1660. [Google Scholar] [CrossRef]
- Livingston, J. A., Wang, W., Testa, M., Derrick, J. L., Nickerson, A. B., Miller, K. E., Haas, J. L., & Espelage, D. L. (2022). Peer sexual harassment, affect, and substance use: Daily level associations among adolescents. Journal of Adolescence, 94(7), 955–968. [Google Scholar] [CrossRef]
- LoConte, N. K., Brewster, A. M., Kaur, J. S., Merrill, J. K., & Alberg, A. J. (2018). Alcohol and cancer: A statement of the American Society of Clinical Oncology. Journal of Clinical Oncology, 36(1), 83–93. [Google Scholar] [CrossRef]
- Magley, V. J., Hulin, C. L., Fitzgerald, L. F., & DeNardo, M. (1999). Outcomes of self-labeling sexual harassment. Journal of Applied Psychology, 84(3), 390–402. [Google Scholar] [CrossRef] [PubMed]
- McGinley, M., Richman, J. A., & Rospenda, K. M. (2011). Duration of sexual harassment and generalized harassment in the workplace over ten years: Effects on deleterious drinking outcomes. Journal of Addictive Diseases, 30(3), 229–242. [Google Scholar] [CrossRef]
- McNair, D. M., Lorr, M., & Droppleman, L. (1981). Profile of mood states. Educational and Industrial Testing Service. [Google Scholar]
- McNight, P. E., McKnight, K. M., Sdani, S., & Figueredo, A. J. (2007). Missing data: A gentle introduction. Guilford Press. [Google Scholar]
- Mirowsky, J., & Ross, C. E. (1990). Control or defense? Depression and the sense of control over good and bad outcomes. Journal of Health and Social Behavior, 30, 71–86. [Google Scholar] [CrossRef]
- Nakada, S., Celis-Morales, C., Pell, J., & Ho, F. (2025). Shared and distinct pathways from anxiety disorder and depression to cardiovascular disease: A UK Biobank prospective cohort study. European Journal of Preventive Cardiology, zwaf110. [Google Scholar] [CrossRef]
- Nakata, A. (2012). Psychosocial job stress and immunity: A systematic review. Methods in Molecular Biology, 934, 39–75. [Google Scholar] [CrossRef] [PubMed]
- National Center for Health Statistics. (2023, June). History of cancer. Centers for Disease Control and Prevention. Available online: https://www.cdc.gov/nchs/hus/topics/history-of-cancer.htm (accessed on 12 January 2026).
- Ngo, S. T., Steyn, F. J., & McCombe, P. A. (2014). Gender differences in autoimmune disease. Frontiers in Neuroendocrinology, 35(3), 347–369. [Google Scholar] [CrossRef]
- Okechukwu, C. A., Krieger, N., Chen, J., Sorensen, G., Li, Y., & Barbeau, E. M. (2010). The association of workplace hazards and smoking in a U.S. multiethnic working-class population. Public Health Reports, 125(2), 225–233. [Google Scholar] [CrossRef]
- Paradies, Y., Ben, J., Denson, N., Elias, A., Priest, N., Pieterse, A., Gupta, A., Kelaher, M., & Gee, G. (2015). Racism as a determinant of health: A systematic review and meta-analysis. PLoS ONE, 10, e0138511. [Google Scholar] [CrossRef]
- Pokorny, A. D., Miller, B. A., & Kaplan, H. B. (1972). The brief MAST: A shortened version of the Michigan alcoholism screening test. American Journal of Psychiatry, 129(3), 342–345. [Google Scholar] [CrossRef] [PubMed]
- Prakash, K. C., Madsen, I. E. H., Rugulies, R., Xu, T., Westerlund, H., Nyberg, A., Kivimaki, M., & Hanson, L. L. M. (2024). Exposure to workplace sexual harassment and risk of cardiometabolic disease: A prospective cohort study of 88,904 Swedish men and women. European Journal of Preventive Cardiology, 31, 1633–1642. [Google Scholar]
- Pratt, L. A., Ford, D. E., Crum, R. M., Armenian, H. K., Gallo, J. J., & Eaton, W. W. (1996). Depression, psychotropic medication, and risk of myocardial infarction. Circulation, 94(12), 3123–3129. [Google Scholar] [CrossRef]
- Rehm, J., Gmel, G. E., Sr., Gmel, G., Hasan, O. S. M., Imtiaz, S., Popova, S., Probst, C., Roerecke, M., Room, R., Samokhvalov, A. V., & Shield, K. D. (2017). The relationship between different dimensions of alcohol use and the burden of disease—An update. Addiction, 112(6), 968–1001. [Google Scholar] [CrossRef]
- Rehm, J., & Shield, K. D. (2013). Global alcohol-attributable deaths from cancer, liver cirrhosis, and injury in 2010. Alcohol Research: Current Reviews, 35(2), 174–183. [Google Scholar] [CrossRef]
- Richman, J. A., Shinsako, S. A., Rospenda, K. M., Flaherty, J. A., & Freels, S. (2002). Workplace harassment/abuse and alcohol-related outcomes: The mediating role of psychological distress. Journal of Studies on Alcohol, 63(4), 412–419. [Google Scholar] [CrossRef]
- Rospenda, K. M., Fujishiro, K., McGinley, M., Wolff, J. M., & Richman, J. A. (2017). Effects of workplace generalized and sexual harassment on abusive drinking among first year male and female college students: Does prior drinking experience matter? Substance Use & Misuse, 52(7), 892–904. [Google Scholar] [CrossRef]
- Rospenda, K. M., Richman, J. A., & Shannon, C. A. (2009). Prevalence and mental health correlates of harassment and discrimination in the workplace: Results from a national study. Journal of Interpersonal Violence, 24(5), 819–843. [Google Scholar] [CrossRef]
- Rugulies, R., Sorensen, K., ALdrich, P. T., Folker, A. P., Frilborg, M. K., Kjaer, S., Nielsen, M. B. D., Sorensen, J. K., & Madsen, I. E. H. (2020). Onset of workplace sexual harassment and subsequent depressive symptoms and incident depressive disorder in the Danish workforce. Journal of Affective Disorders, 277, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Seelig, A. D., Rivera, A. C., Powell, T. M., Williams, E. C., Peterson, A. V., Littman, A. J., Maynard, C., Street, A. E., Bricker, J. B., & Boyko, E. J. (2017). Patterns of smoking and unhealthy alcohol use following sexual trauma among U.S. service members. Journal of Traumatic Stress, 30(5), 502–511. [Google Scholar] [CrossRef] [PubMed]
- Siegrist, J., & Rödel, A. (2006). Work stress and health risk behavior. Scandinavian Journal of Work, Environment & Health, 32(6), 473–481. [Google Scholar] [CrossRef]
- Sørensen, J., Framke, E., Pedersen, J., Alexanderson, K., Bonde, J., Farrants, K., Flachs, E., Hanson, L., Nyberg, S., Kivimäki, M., Madsen, I., & Rugulies, R. (2021). Work stress and loss of years lived without chronic disease: An 18-year follow-up of 1.5 million employees in Denmark. European Journal of Epidemiology, 37, 389–400. [Google Scholar] [CrossRef]
- Tasdighi, E., Yao, Z., Dardari, Z. A., Jha, K. K., Osuji, N., Rajan, T., Boakye, E., Matsushita, K., Simonsick, E. M., Lima, J. A. C., Lloyd-Jones, D. M., Cohen, D. L., Appel, L. J., Khera, A., Hall, M. E., Rodriguez, C. J., Judd, S., Cole, S. A., Ramachandran, V. S., … Blaha, M. J. (2025). Association between cigarette smoking status, intensity, and cessation duration with long-term incidence of nine cardiovascular and mortality outcomes: The Cross-Cohort Collaboration (CCC). PLoS Medicine, 22(11), e1004561. [Google Scholar] [CrossRef] [PubMed]
- Thurston, R. C., Chang, Y., Matthews, K. A., Von Känel, R., & Koenen, K. (2019). Association of sexual harassment and sexual assault with midlife women’s mental and physical health. JAMA Internal Medicine, 179(1), 48–53. [Google Scholar] [CrossRef]
- Vasilenko, S. A., Evans-Polce, R. J., & Lanza, S. T. (2017). Age trends in rates of substance use disorders across ages 18–90: Differences by gender and race/ethnicity. Drug and Alcohol Dependence, 180, 260–264. [Google Scholar] [CrossRef]
- Wasti, S. A., Bergman, M. E., Glomb, T. M., & Drasgow, F. (2000). Test of the cross-cultural generalizability of a model of sexual harassment. Journal of Applied Psychology, 85, 766–778. [Google Scholar] [CrossRef] [PubMed]
- Williams, D. R. (2018). Stress and the mental health of populations of color: Advancing our understanding of race-related stressors. Journal of Health and Social Behavior, 59(4), 466–485. [Google Scholar] [CrossRef] [PubMed]
- Willness, C. R., Steel, P., & Lee, K. (2007). A meta-analysis of the antecedents and consequences of workplace sexual harassment. Personnel Psychology, 60(1), 127–162. [Google Scholar] [CrossRef]
- Wilsnack, S. C., Klassen, A. D., Schur, B. E., & Wilsnack, R. W. (1991). Predicting onset and chronicity of women’s problem drinking: A five-year longitudinal analysis. American Journal of Public Health, 81, 305–318. [Google Scholar] [CrossRef]
- World Health Organization (WHO). (2016). Noncommunicable diseases. Available online: http://www.who.int/topics/noncommunicable_diseases/en/ (accessed on 12 January 2026).
- Wright, B. J., Eddy, P. J., & Kent, S. (2020). Work stress, immune, and inflammatory markers. In T. Theorell (Ed.), Handbook of socioeconomic determinants of occupational health (pp. 1–19). Springer International Publishing. [Google Scholar]
- Wu, M., Zhu, Y., Lv, J., Guo, Y., Yang, L., Chen, Y., Tang, W., Xiang, S., Sun, X., Chen, J., Chen, Z., Yu, C., & Li, L. (2022). Association of anxiety with cardiovascular disease in a Chinese cohort of 0.5 million adults. Journal of Affective Disorders, 315, 291–296. [Google Scholar] [CrossRef]
- Xu, S., Huang, Y., Xiao, J., Zhu, W., Wang, L., Tang, H., Hu, Y., & Liu, T. (2015). The association between job strain and coronary heart disease: A meta-analysis of prospective cohort studies. Annals of Medicine, 47, 512–518. [Google Scholar] [CrossRef] [PubMed]


| Survey Wave | Years Since Baseline | Dates | Eligible Sample | Completed Questionnaires | Response Rate (%) | Respondent Compensation |
|---|---|---|---|---|---|---|
| T1 | 0 | 10/1996–2/1997 | 4790 | 2492 | 52.0 | $20 |
| T2 | 1 | 11/1997–4/1998 | 2491 | 2038 | 81.8 | $20 |
| T3 | 5 | 5/2001–1/2002 | 2486 | 1730 | 69.6 | $30 |
| T4 | 6 | 9/2002–1/2003 | 2472 | 1654 | 66.9 | $30 |
| T5 | 7 | 11/2003–3/2004 | 2458 | 1453 | 59.1 | $30 |
| T6 | 8 | 9/2005–2/2006 | 2434 | 1517 | 62.3 | $30 |
| T7 | 9 | 9/2006–4/2007 | 2411 | 1461 | 60.6 | $30 |
| T8 | 10 | 10/2007–2/2008 | 2393 | 1444 | 60.3 | $25 |
| T9 | 23 | 6/2020–2/2021 | 2035 | 920 | 45.2 | $50 |
| Variable | n | % | |||
|---|---|---|---|---|---|
| Age | ≤30 | 130 | 26.6 | ||
| 31–40 | 167 | 34.2 | |||
| 41–50 | 128 | 26.3 | |||
| >50 | 63 | 12.9 | |||
| mean | SD | min | max | ||
| Age | years | 38.3 | 9.6 | 22 | 68 |
| n | % | ||||
| Gender | Female | 301 | 57.3 | ||
| Male | 224 | 42.7 | |||
| Race | White | 340 | 64.7 | ||
| Black | 87 | 16.6 | |||
| Hispanic | 25 | 4.8 | |||
| Asian | 64 | 12.2 | |||
| Other | 9 | 1.7 | |||
| Occupation Group at Baseline | Clerical/Administrative | 86 | 16.4 | ||
| Faculty | 205 | 39.0 | |||
| Graduate Student | 192 | 36.6 | |||
| Service/Maintenance | 42 | 8.0 | |||
| n | % | ||||
| Any Sexual Harassment (SEQ) | =19 (none) | 284 | 54.1 | ||
| >19 (any) | 241 | 45.9 | |||
| mean | SD | min | max | ||
| Sexual Harassment Scale (SEQ) | 19 to 57 | 21.3 | 3.9 | 19 | 45 |
| Datapoints After BL = | 0 | 1 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Predicting Incidence in Year(s) = | 1 | 2–3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12–23 |
| Total at Risk for First Chronic Dx | 525 | 511 | 486 | 479 | 470 | 458 | 435 | 427 | 417 | 408 | 399 |
| Age (years) | |||||||||||
| Age Mean | 38.3 | 39.5 | 41.2 | 42.1 | 43.0 | 43.9 | 44.8 | 45.8 | 46.7 | 47.7 | 48.7 |
| Age SD | 9.6 | 9.6 | 9.4 | 9.4 | 9.3 | 9.3 | 9.4 | 9.4 | 9.4 | 9.4 | 9.4 |
| Sexual Harassment (SEQ): Scale 19–57 | |||||||||||
| SEQ N | 525 | 428 | 368 | 367 | 370 | 354 | 305 | 344 | 345 | 313 | |
| new measure (X) | X | X | X | X | X | X | X | ||||
| retrospective (*) | * | * | * | ||||||||
| SEQ Mean | 21.3 | 21.1 | 21.0 | 20.7 | 20.9 | 20.6 | 20.4 | 20.7 | 21.1 | 21.0 | |
| SEQ SD | 3.9 | 4.1 | 3.7 | 3.6 | 3.7 | 3.4 | 2.7 | 3.4 | 3.8 | 3.4 | |
| % > 19 | 45.9 | 40.4 | 32.1 | 33.0 | 34.3 | 33.3 | 33.1 | 37.5 | 45.2 | 45.7 | |
| Depressive Symptoms (DEPR): Scale 0–21 | |||||||||||
| DEPR N | 503 | 444 | 383 | 388 | 332 | 354 | 359 | 339 | |||
| DEPR Mean | 3.23 | 3.92 | 3.53 | 3.60 | 3.06 | 3.19 | 3.20 | 3.09 | |||
| DEPR SD | 3.60 | 4.17 | 3.82 | 3.76 | 3.43 | 3.46 | 3.53 | 3.28 | |||
| Drinks per Day Past 30 Days (DRINKS): Categories 0–7 | |||||||||||
| ANX: Scale 0–36 | |||||||||||
| ANX N | 513 | 437 | 362 | 377 | 322 | 336 | 343 | 329 | |||
| ANX Mean | 7.9 | 7.5 | 6.8 | 7.0 | 6.2 | 6.7 | 6.3 | 6.5 | |||
| ANX SD | 6.2 | 6.0 | 5.4 | 5.7 | 5.1 | 5.3 | 5.1 | 5.1 | |||
| DRINKS N | 508 | 449 | 333 | 331 | 302 | 338 | 336 | 315 | |||
| DRINKS Mean | 1.40 | 1.32 | 1.32 | 1.24 | 1.28 | 1.28 | 1.29 | 1.37 | |||
| DRINKS SD | 1.33 | 1.26 | 1.07 | 1.10 | 1.05 | 1.03 | 1.06 | 1.13 | |||
| Times Intoxicated (INTOX): Categories 0–7 | |||||||||||
| INTOX N | 522 | 453 | 384 | 386 | 307 | 361 | 361 | 341 | |||
| INTOX Mean | 0.61 | 0.57 | 0.73 | 0.67 | 0.52 | 0.56 | 0.55 | 0.57 | |||
| INTOX SD | 1.03 | 0.94 | 1.19 | 1.10 | 0.88 | 0.99 | 1.05 | 1.05 | |||
| Days Drank Past 30 Days (ALCDAYS): 0–30 | |||||||||||
| ALCDAYS N | 517 | 449 | 381 | 382 | 332 | 352 | 347 | 328 | |||
| ALCDAYS Mean | 5.47 | 5.90 | 5.72 | 5.89 | 7.35 | 7.55 | 7.35 | 7.96 | |||
| ALCDAYS SD | 7.09 | 7.55 | 7.71 | 7.76 | 8.41 | 8.77 | 8.71 | 9.09 | |||
| Alcohol Misuse (BMAST): Scale 0–17 | |||||||||||
| BMAST N | 524 | 454 | 319 | 314 | 252 | 361 | 300 | 287 | |||
| BMAST Mean | 0.58 | 0.53 | 0.43 | 0.37 | 0.55 | 0.47 | 0.47 | 0.41 | |||
| BMAST SD | 1.52 | 1.46 | 1.19 | 1.42 | 1.49 | 1.30 | 1.37 | 1.17 | |||
| Cigarette Smoking (CIGS): 0 = no, 1 = yes | |||||||||||
| CIGS N | 514 | 429 | 378 | 335 | 294 | 338 | 330 | 292 | |||
| CIGS Mean | 0.23 | 0.19 | 0.15 | 0.19 | 0.17 | 0.17 | 0.14 | 0.15 | |||
| CIGS SD | 0.42 | 0.39 | 0.36 | 0.39 | 0.37 | 0.37 | 0.35 | 0.36 | |||
| Psychological Workload (PSYCHWL): Scale 0–25 | |||||||||||
| PSYCHWL N | 491 | 416 | 330 | 317 | 276 | 341 | 314 | ||||
| PSYCHWL Mean | 10.2 | 9.6 | 9.5 | 9.9 | 9.5 | 9.8 | 9.9 | ||||
| PSYCHWL SD | 4.4 | 3.9 | 4.3 | 4.1 | 4.1 | 4.3 | 4.2 | ||||
| Decision Latitude (DECLAT): Scale 12–60 | |||||||||||
| DECLAT N | 511 | 421 | 343 | 322 | 282 | 351 | 315 | ||||
| DECLAT Mean | 38.4 | 38.5 | 39.1 | 38.9 | 38.6 | 39.0 | 39.2 | ||||
| DECLAT SD | 6.2 | 5.8 | 5.8 | 5.5 | 6.2 | 6.1 | 6.0 |
| Models with Single Trend Continuous SEQ | |||||
| Beta | SE | Chi-Square | p-Value | HR | |
| Model 1: | |||||
| SEQ at Baseline | 0.03681 | 0.01487 | 6.1287 | 0.0133 | 1.038 |
| Model 2: | |||||
| SEQ at Baseline | 0.03029 | 0.01520 | 3.9693 | 0.0463 | 1.031 |
| DEPR at Baseline | 0.04766 | 0.01684 | 8.0082 | 0.0047 | 1.049 |
| Model 3: | |||||
| SEQ at Baseline | 0.03021 | 0.01524 | 3.9289 | 0.0475 | 1.031 |
| DEPR at Baseline | 0.04064 | 0.01714 | 5.6243 | 0.0177 | 1.041 |
| DRINKS previous year | 0.11966 | 0.04821 | 6.1609 | 0.0131 | 1.127 |
| Models with Binary Indicator SEQ > 19 | |||||
| Beta | SE | Chi-Square | p-Value | HR | |
| Model 1: | |||||
| SEQ > 19 at Baseline | 0.36272 | 0.12636 | 8.2404 | 0.0041 | 1.437 |
| Model 2: | |||||
| SEQ > 19 at Baseline | 0.30819 | 0.12808 | 5.7897 | 0.0161 | 1.361 |
| DEPR at Baseline | 0.04607 | 0.01692 | 7.4143 | 0.0065 | 1.047 |
| Model 3: | |||||
| SEQ > 19 at Baseline | 0.30532 | 0.12808 | 5.6827 | 0.0171 | 1.357 |
| DEPR at Baseline | 0.03966 | 0.01713 | 5.3610 | 0.0206 | 1.040 |
| DRINKS previous year | 0.11872 | 0.04811 | 6.0890 | 0.0136 | 1.126 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Freels, S.; Lin, T.W.; Johnson, T.P.; Rospenda, K.M. Workplace Sexual Harassment and the Risk of Chronic Disease in a Prospective Cohort Study. Behav. Sci. 2026, 16, 223. https://doi.org/10.3390/bs16020223
Freels S, Lin TW, Johnson TP, Rospenda KM. Workplace Sexual Harassment and the Risk of Chronic Disease in a Prospective Cohort Study. Behavioral Sciences. 2026; 16(2):223. https://doi.org/10.3390/bs16020223
Chicago/Turabian StyleFreels, Sally, Tracy W. Lin, Timothy P. Johnson, and Kathleen M. Rospenda. 2026. "Workplace Sexual Harassment and the Risk of Chronic Disease in a Prospective Cohort Study" Behavioral Sciences 16, no. 2: 223. https://doi.org/10.3390/bs16020223
APA StyleFreels, S., Lin, T. W., Johnson, T. P., & Rospenda, K. M. (2026). Workplace Sexual Harassment and the Risk of Chronic Disease in a Prospective Cohort Study. Behavioral Sciences, 16(2), 223. https://doi.org/10.3390/bs16020223






