A Case Study of Photosensitivity Associated with Anaplasma spp. Infection in Cattle
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
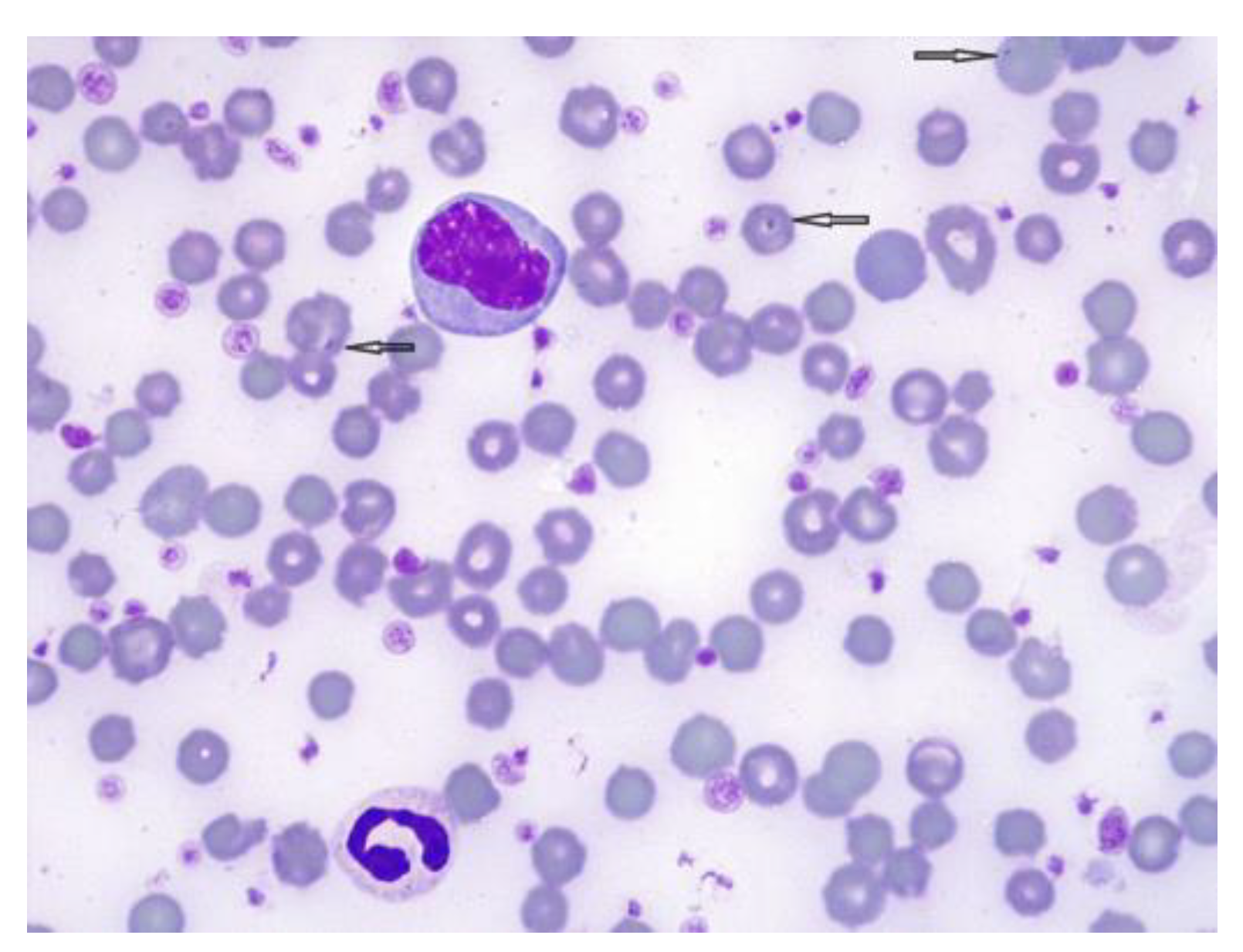
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Constable, P.D.; Hinchcliff, K.W.; Done, S.H.; Grünberg, W. Veterinary Medicine: A Textbook of the Diseases of Cattle, Horses, Sheep, Pigs, and Goats, 11th ed.; Elsevier: St. Louis, MO, USA, 2017; Volume 1, pp. 1549–1552. [Google Scholar]
- Buergelt, C.D.; Edward, G.C.; Del Piero, F. Bovine Pathology A Text and Color Atlas; CABI: Oxfordshire, UK, 2017; pp. 161–176. [Google Scholar]
- Ghergariu, G.; Rowlands, G.J.; Pop, A.L.; Danielescu, N.; Moldovan, N.A. A comparative study of metabolic profiles obtained in dairy herds in Romania. Br. Vet. J. 1984, 140, 600–608. [Google Scholar] [CrossRef] [PubMed]
- Matei, I.A.; Kalmár, Z.; Lupşe, M.; D’Amico, G.; Ionică, A.M.; Dumitrache, M.O.; Gherman, C.M.; Mihalca, A.D. The risk of exposure to rickettsial infections and human granulocytic anaplasmosis associated with Ixodes ricinus tick bites in human in Romania: A multiannual study. Ticks Tick Borne Dis. 2017, 8, 375–378. [Google Scholar] [CrossRef] [PubMed]
- Aktas, M.; Çolak, S. Molecular detection and phylogeny of Anaplasma spp. in cattle reveals the presence of novel strains closely related to A. phagocytophilum in Turkey. Ticks Tick Borne Dis. 2021, 12, 101604. [Google Scholar] [CrossRef] [PubMed]
- Kovalchuk, S.N.; Babii, A.V.; Arkhipova, A.L. Real-time PCR assay with an endogenous internal amplification control for detection and quantification of Anaplasma marginale in bovine blood. Ticks Tick Borne Dis. 2020, 11, 101334. [Google Scholar] [CrossRef]
- Moraga Fernandez, A.; Ortiz, J.A.; Jabbar, A.; Ghafar, A.; Cabezas-Cruz, A.; de la Fuente, G.; de la Fuente, J.; Fernandez de Mera, I.G. Fatal cases of bovine anaplasmosis in a herd infected with different Anaplasma marginale genotypes in southern Spain. Ticks Tick Borne Dis. 2022, 13, 101864. [Google Scholar] [CrossRef]
- George, J.W.; Snipes, J.; Lane, V.M. Comparison of bovine hematology reference intervals from 1957–2006. Vet. Clin. Pathol. 2010, 39, 138–148. [Google Scholar] [CrossRef]
- Kaneko, J.J.; Harvey, J.W.; Bruss, M.L. Clinical Biochemistry of Domestic Animals, 6th ed.; Academic Press: Burlington, MA, USA, 2008. [Google Scholar]
- Nazar, M.; Khan, M.A.; Shah, A.A.; Rahman, S.U.; Khan, I.; Ullah, A.; Khan, I.U.; Shuaib, M. Occurrence and transplacental transmission of Anaplasma marginale in dairy cattle. Slov. Vet. Res. 2018, 55, 183–191. [Google Scholar] [CrossRef]
- Ziam, H.; Kernif, T.; Saidani, K.; Kelanemer, R.; Hammaz, Z.; Geysen, D. Bovine piroplasmosis-anaplasmosis and clinical signs of tropical theileriosis in the plains of Djurdjura (north Algeria). Vet. Med. Sci. 2020, 6, 720–729. [Google Scholar] [CrossRef]
- Atif, F.A. Anaplasma marginale and Anaplasma phagocytophilum: Rickettsiales pathogens of veterinary and public health significance. Parasitol. Res. 2015, 114, 3941–3957. [Google Scholar] [CrossRef]
- Scott, D.W. Skin Diseases. In Rebhuns Diseases of Dairy Cattle, 3rd ed.; Peek, S.F., Divers, T.J., Eds.; Elsevier: St. Louis, MO, USA, 2018; pp. 357–388. [Google Scholar]
- Moroni, P.; Nydam, D.V.; Ospina, P.A.; Scilieri-Smith, J.C.; Virkler, P.D.; Watters, R.D.; Welcome, F.L.; Zurakowski, M.J.; Ducharme, N.G.; Yeager, A.E. Diseases of the Teats and Udder. In Rebhuns Diseases of Dairy Cattle, 3rd ed.; Peek, S.F., Divers, T.J., Eds.; Elsevier: St. Louis, MO, USA, 2018; pp. 389–465. [Google Scholar]
- Nieman, C.C.; Schaefer, D.M.; Maroney, M.; Nelson, K.; Albrecht, K.A. Hepatogenous photosensitivity outbreak after coccidiosis in grazing Holstein steers. Vet. Sci. 2020, 7, 186. [Google Scholar] [CrossRef]
- Rowe, L.D. Photosensitization problems in livestock. Vet. Clin. N. Am. Food Anim. Pract. 1989, 5, 301–323. [Google Scholar] [CrossRef] [PubMed]
- Minervino, A.H.H.; Barrêto Júnior, R.A.; Rodrigues, F.A.M.L.; Ferreira, R.N.F.; Reis, L.F.; Headley, S.A.; Ortolani, E.I. Hepatogenous photosensitization associated with liver copper accumulation in buffalos. Res. Vet. Sci. 2010, 88, 519–522. [Google Scholar] [CrossRef] [PubMed]
- Haargis, A.M.; Ginn, P.E. The integument. In Pathologic Basis of Veterinary Disease, 4th ed.; McGavin, M.M., Zachary, J.F., Eds.; Mosby/Elsevier: St. Louis, MO, USA, 2007; pp. 1107–1261. [Google Scholar]
- Mendonça, M.F.F.; Pimentel, L.A.; Leal, P.V.; Filho, J.C.O.; Caymmi, L.G.; Silva, A.W.O.; Jesus, R.S.; Peixoto, T.C. Hepatogenous photosensitization in ruminants and horses caused by the ingestion of Chamaecrista serpens in Brazil. Toxicon 2021, 193, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Valli, V.E.O.; Bienzle, D.; Kiupel, M. Hematopoietic system: Anthrax. In Jubb, Kennedy and Palmer’s Pathology of Domestic Animals, 6th ed.; Maxie, M.G., Ed.; Elsevier: St. Louis, MO, USA, 2016; Volume 2, pp. 171–174. [Google Scholar]
- Clothier, K.A. Bovine Anaplasmosis. In Large Animal Internal Medicine, 6th ed.; Smith, B.P., Metre, D.C.V., Pusterla, N., Eds.; Elsevier: St. Louis, MO, USA, 2020; pp. 1164–1169. [Google Scholar]
- Zygner, W.; Rodo, A.; Gójska-Zygner, O.; Górski, P.; Bartosik, J.; Kotomski, G. Disorders in blood circulation as a probable cause of death in dogs infected with Babesia canis. J. Vet. Res. 2021, 65, 277–285. [Google Scholar] [CrossRef] [PubMed]
- Kocan, K.M.; de la Fuente, J.; Guglielmone, A.A.; Mel´endez, R.D. Antigens and alternatives for control of Anaplasma marginale infection in cattle. Clin. Microbiol. Rev. 2003, 16, 698–712. [Google Scholar] [CrossRef] [PubMed]
- Subramanian, B.; Vijayalakshmi, P.; Perumal, S.V.; Selvi, D. Clinical and haematobiochemical changes in cattle with Anaplasma marginale infection. Int. J. Chem. Stud. 2019, 7, 4373–4376. [Google Scholar]
- Ashuma, A.S.; Singla, L.D.; Kaur, P.; Bal, M.S.; Batth, B.K.; Juyal, P.D. Prevalence and haemato-biochemical profile of Anaplasma marginale infection in dairy animals of Punjab (India). Asian Pac. J. Trop. Med. 2013, 6, 139–144. [Google Scholar] [CrossRef]
- Das, D.; Sarma, K.; Roychoudhury, P.; Chethan, G.E.; Ravindran, R.; Islam, S.J.; Prasad, H.; Rajesh, J.B.; Behera, B.; Choudhury, F.A. Gross and histopathological findings of naturally occurring Anaplasma marginale infection in cattle. Indian J. Anim. Res. 2021, 1, 5. [Google Scholar] [CrossRef]
- Smith Tomas, H. The Cattle Health. Handbook Preventive care, Disease Treatments and Emergency Procedures for Promoting the Well-Being of Your Beef or Dairy Herd; Storey Publishing: North Adams, MA, USA, 2009; pp. 200–204. [Google Scholar]
- White, S.D. Environmental diseases. In Large Animal Internal Medicine, 6th ed.; Smith, B.P., Metre, D.C.V., Pusterla, N., Eds.; Elsevier: St. Louis, MO, USA, 2020; pp. 1344–1345. [Google Scholar]
- Cullen, J.M.; Stalker, M.J. Liver and Biliary System. In Jubb, Kennedy and Palmer’s Pathology of Domestic Animals, 6th ed.; Maxie, M.G., Ed.; Elsevier: Louis, MO, USA, 2016; Volume 2, pp. 258–352. [Google Scholar]
- Rubel, W.; Schoneberg, C.; Wolf, A.; Ganter, M.; Bauer, B.U. Seroprevalence and Risk Factors of Anaplasma spp. in German Small Ruminant Flocks. Animals 2021, 11, 2793. [Google Scholar] [CrossRef]
- Movilla, R.; García, C.; Siebert, S.; Roura, X. Countrywide serological evaluation of canine prevalence for Anaplasma spp., Borrelia burgdorferi (sensu lato), Dirofilaria immitis and Ehrlichia canis in Mexico. Parasit. Vectors 2016, 9, 421. [Google Scholar] [CrossRef]
- Yang, X.; Fu, M.; Yu, Z.; Wang, J.; Song, J.; Zhao, G. Molecular Characterization of Anaplasma spp. among Dairy, Cashmere, and Meat Goats in Shaanxi Province, Northwestern China. Animals 2022, 12, 1566. [Google Scholar] [CrossRef] [PubMed]
- Khan, Z.; Shehla, S.; Alouffi, A.; Kashif Obaid, M.; Zeb Khan, A.; Almutairi, M.M.; Numan, M.; Aiman, O.; Alam, S.; Ullah, S.; et al. Molecular Survey and Genetic Characterization of Anaplasma marginale in Ticks Collected from Livestock Hosts in Pakistan. Animals 2022, 12, 1708. [Google Scholar] [CrossRef] [PubMed]
- Pusterla, N.; Leutenegger, C.M.; Crossley, B.M.; Hietela, S. Molecular diagnostics. In Large Animal Internal Medicine, 6th ed.; Smith, B.P., Metre, D.C.V., Pusterla, N., Eds.; Elsevier: St. Louis, MO, USA, 2020; pp. 461–476. [Google Scholar]
- Das, D.; Sarma, K.; Eregowda, C.G.; Roychoudhury, P.; Rajesh, J.B.; Behera, P.; Prasad, H.; Lalrinkima, H.; Aktar, F.; Bora, N.; et al. Naturally occurring Anaplasma marginale infection in cattle: Molecular prevalence and associated risk factors, haemato-biochemical alterations, oxidant/antioxidant status and serum trace mineral levels. Microb. Pathog. 2022, 167, 105575. [Google Scholar] [CrossRef] [PubMed]
- Rymaszewska, A.; Grenda, S. Bacteria of the genus Anaplasma characteristics of Anaplasma and their vectors: A review. Vet. Med. 2008, 53, 573–584. [Google Scholar] [CrossRef]
- Ben Said, M.; Belkahia, H.; Messadi, L. Anaplasma spp. in North Africa: A review on molecular epidemiology, associated risk factors and genetic characteristics. Ticks Tick Borne Dis. 2018, 9, 543–555. [Google Scholar] [CrossRef]
- Allison, R.W.; Meinkoth, J.H. Anemia caused by rickettsia, mycoplasma, and protozoa. In Schalm’s Veterinary Hematology, 6th ed.; Weiss, D.J., Wardrop, K.J., Eds.; Wiley-Blackwell: Ames, IA, USA, 2010; pp. 199–210. [Google Scholar]
- Galon, E.M.S.; Ybañez, R.H.D.; Adjou Moumouni, P.F. Molecular survey of tick-borne pathogens infecting backyard cattle and water buffaloes in Quezon province, Philippines. J. Vet. Med. Sci. 2020, 82, 886–890. [Google Scholar] [CrossRef]

| Hematological Parameters | Values | Reference [8] |
|---|---|---|
| Leucocytes | 13.61 * | 4.9–12 × 109/L |
| Lymphocytes | 4.53 | 1.6–5.6 × 109/L |
| Monocytes | 0.2 | 0–0.8 × 109/L |
| Neutrophils | 8.62 * | 1.8–6.3 × 109/L |
| Eosinophils | 0.1 | 0–0.9 × 109/L |
| Basophils | 0.1 | 0–0.3 × 109/L |
| RBC | 3.33 * | 5.1–7.6 × 1012/L |
| Hemoglobin | 5.4 * | 8.5–12.2 g/dL |
| HCT | 17.8 * | 22–33% |
| MCV | 50 | 38–50 fL |
| MCH | 16.1 | 14–18 pg |
| MCHC | 30.1 * | 36–39 g/dL |
| Thrombocytes | 641 | 200,000–650,000 per μL |
| Biochemical Parameters | Values | Reference [9] |
|---|---|---|
| Albumin | 1.5 * | 3.03–3.55 g/dL |
| ALP | 148 | 0–488 IU/L |
| ALT | 58 * | 11–40 IU/L |
| AST | 154 * | 78–132 IU/L |
| GGT | 241 * | 15–39 IU/L |
| Amylase | 40 | 40–161 IU/L |
| Total bilirubin | 0.6 * | 0.01–0.5 mg/dL |
| Urea nitrogen | 16 * | 20–30 mg/dL |
| Calcium | 9.7 | 9.7–12.4 mEq/L |
| Phosphorus | 5.6 | 5.6–6.5 mEq/L |
| Creatinine | 1.0 | 1.0–2.0 mg/dL |
| Glucose | 72 | 45–75 mg/dL |
| Sodium | 138 | 132–152 mEq/L |
| Potassium | 4.5 | 3.9–5.8 mEq/L |
| Total protein | 7.6 * | 6.74–7.46 g/dL |
| Globulin | 6.1 * | 3–3.48 g/dL |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Anton, A.; Solcan, G. A Case Study of Photosensitivity Associated with Anaplasma spp. Infection in Cattle. Animals 2022, 12, 3568. https://doi.org/10.3390/ani12243568
Anton A, Solcan G. A Case Study of Photosensitivity Associated with Anaplasma spp. Infection in Cattle. Animals. 2022; 12(24):3568. https://doi.org/10.3390/ani12243568
Chicago/Turabian StyleAnton, Alina, and Gheorghe Solcan. 2022. "A Case Study of Photosensitivity Associated with Anaplasma spp. Infection in Cattle" Animals 12, no. 24: 3568. https://doi.org/10.3390/ani12243568
APA StyleAnton, A., & Solcan, G. (2022). A Case Study of Photosensitivity Associated with Anaplasma spp. Infection in Cattle. Animals, 12(24), 3568. https://doi.org/10.3390/ani12243568





