Mycoplasma agalactiae: The Sole Cause of Classical Contagious Agalactia?
Abstract
Simple Summary
Abstract
1. Introduction
2. General Consideration about Contagious Agalactia
2.1. Clinical Findings and Epidemiology
2.2. Pathological Findings in Experimental and Natural Infection
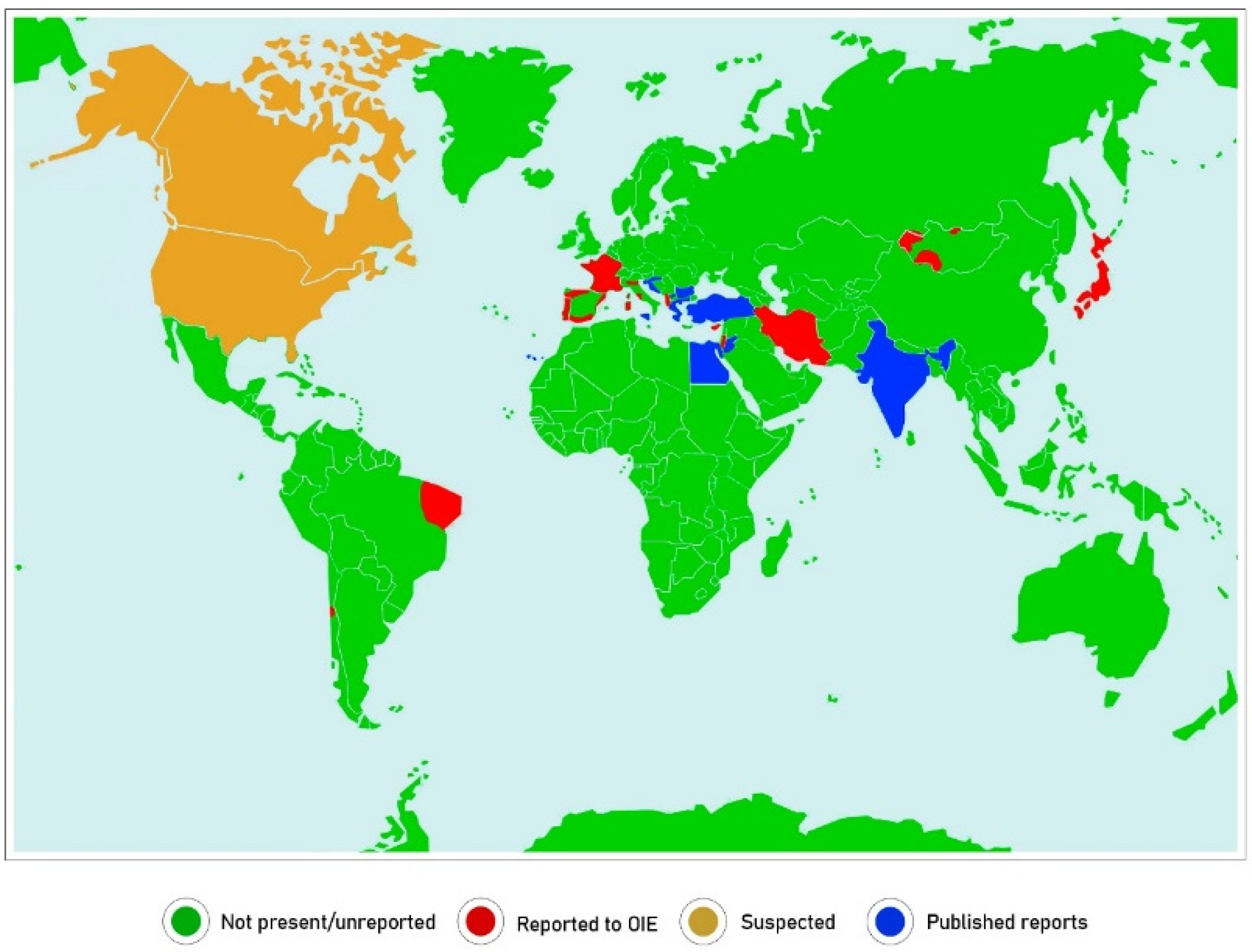
2.3. Geographical Location
2.4. Characteristics of the Causative Mycoplasmas
2.5. Legislation
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Acknowledgments
Conflicts of Interest
References
- World Organization for Animal Health (OIE). Chapter 3.7.3 Contagious Agalactia. In Manual of Diagnostic Tests and Vaccines for Terrestrial Animals (Terrestrial Manual), 8th ed.; OIE: Paris, France, 2019; Volume 1, pp. 1430–1440. Available online: https://www.oie.int/fileadmin/Home/eng/ Health_standards/tahm/3.07.03_CONT_AGALACT.pdf (accessed on 1 May 2021).
- Perreau, P. Les mycoplasmoses de la chevre. Cah. Med. Vet. 1979, 48, 71–85. [Google Scholar]
- Nicholas, R.A.J. Contagious Agalactia: An update. In Mycoplasmas of Ruminants: Pathogenicity, Diagnostics, Epidemiology and Molecular Genetics; Frey, J., Sarris, K., Eds.; Commission of the European Community: Luxembourg, 1996; pp. 60–62. [Google Scholar]
- Da Massa, A.J.; Brooks, D.L.; Holmberg, C.A.; Moe, A.I. Caprine mycoplasmosis: An outbreak of mastitis and arthritis requiring the destruction of 700 goats. Vet. Rec. 1987, 120, 409–413. [Google Scholar] [CrossRef] [PubMed]
- Spickler, A.R. Contagious Agalactia. Available online: cfsph.iastate.edu/diseaseinfo/factsheets/ https://www.cfsph.iastate.edu/diseaseinfo/disease/?disease=contagious-agalactia&lang=en (accessed on 22 April 2021).
- European Parliamentary Research Service. The Sheep and Goat Sector in the EU Main Features, Challenges and Prospects. Briefing. 2017. Available online: https://www.europarl.europa.eu/RegData/etudes/BRIE/2017/608663/E (accessed on 21 April 2021).
- Bergonier, D.; Berthelot, X.; Poumarat, F. Contagious agalactia of small ruminants: Current knowledge concerning epidemiology, diagnosis and control. Rev. Sci. Tech. 1997, 16, 848–873. [Google Scholar] [CrossRef] [PubMed]
- Garrido, F.; Leon, J.L.; Cuellar, L.; Diaz, M.A. Contagious Agalactia and Other Mycoplasmal Diseases of Ruminants; Lambert, M., Jones, G., Eds.; Commission of the European Community: Luxembourg, 1987. [Google Scholar]
- Loria, G.R.; Nicholas, R.A. Contagious agalactia: The shepherd’s nightmare. Vet. J. 2013, 198, 5–6. [Google Scholar] [CrossRef] [PubMed]
- Tolone, M.; Sutera, A.M.; Borrello, S.; Tumino, S.; Scatassa, M.L.; Portolano, B.; Puleio, R.; Nicholas, R.A.J.; Loria, G.R. Effect of Mycoplasma agalactiae mastitis on milk production and composition in Valle dell Belice dairy sheep. Ital. J. Anim. Sci. 2019, 18, 1067–1072. [Google Scholar] [CrossRef]
- Jaÿ, M.; Tardy, F. Contagious Agalactia In Sheep And Goats: Current Perspectives. Vet. Med. 2019, 10, 229–247. [Google Scholar] [CrossRef]
- De La Fe, C.; Gutiérrez, A.; Poveda, J.B.; Assunção, P.; Ramirez, A.S.; Fabelo, F. First isolation of Mycoplasma capricolum subsp capricolum, one of the causal agents of caprine contagious agalactia, on the island of Lanzarote (Spain). Vet. J. 2005, 173, 440–442. [Google Scholar] [CrossRef]
- Agnello, S.; Chetta, M.; Vicari, D.; Mancuso, R.; Manno, C.; Puleio, R.; Console, A.; Nicholas, R.A.; Loria, G.R. Severe outbreaks of polyarthritis in kids caused by Mycoplasma mycoides subspecies capri in Sicily. Vet. Rec. 2012, 170, 416. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Martín, A.; Amores, J.; Paterna, A.; De la Fe, C. Contagious agalactia due to Mycoplasma spp. in small dairy ruminants: Epidemiology and prospects for diagnosis and control. Vet. J. 2013, 198, 48–56. [Google Scholar] [CrossRef]
- Thiaucourt, F.; Bölske, G. Contagious caprine pleuropneumonia and other pulmonary mycoplasmoses of sheep and goats. Rev. Sci. Tech. 1996, 15, 1397–1414. [Google Scholar] [CrossRef]
- Gil, M.C.; Peña, F.J.; Hermoso De Mendoza, J.; Gomez, L. Genital lesions in an outbreak of caprine contagious agalactia caused by Mycoplasma agalactiae and Mycoplasma putrefaciens. J. Vet. Med. B Infect. Dis. Vet. Public Health 2003, 50, 484–487. [Google Scholar] [CrossRef]
- Hajizadeh, A.; Ghaderi, R.; Ayling, R.D. Species of Mycoplasma causing contagious agalactia in small ruminants in Northwest Iran. Vet. Ital. 2018, 54, 205–210. [Google Scholar] [CrossRef]
- Corona, L.; Amores, J.; Onni, T.; de la Fe, C.; Tola, S. Characterization of Mycoplasma mycoides subsp. capri isolates by SDS-PAGE, immunoblotting and PFGE. Small Rumin. Res. 2013, 115, 140–144. [Google Scholar] [CrossRef]
- Hasso, S.A.; Al-Omran, A.H. Antibody response patterns in goats experimentally infected with Mycoplasma agalactiae. Small Rumin. Res. 1994, 14, 79–81. [Google Scholar] [CrossRef]
- Johnson, G.C.; Fales, W.H.; Shoemake, B.M.; Adkins, P.R.; Middleton, J.R.; Williams, F., III; Zinn, M.; Mitchell, W.J.; Calcutt, M.J. An outbreak of Mycoplasma mycoides subspecies capri arthritis in young goats: A case study. J. Vet. Diagn. Invest. 2019, 31, 453–457. [Google Scholar] [CrossRef]
- Tatay-Dualde, J.; Prats-van der Ham, M.; de la Fe, C.; Gómez-Martín, Á.; Paterna, A.; Corrales, J.C.; Contreras, A.; Sánchez, A. Multilocus sequence typing of Mycoplasma mycoides subsp. capri to assess its genetic variability in a contagious agalactia endemic area. Vet. Microbiol. 2016, 191, 60–64. [Google Scholar] [CrossRef] [PubMed]
- D’Angelo, A.R.; Di Provvido, A.; Di Francesco, G.; Sacchini, F.; De Caro, C.; Nicholas, R.A.; Scacchia, M. Experimental infection of goats with an unusual strain of Mycoplasma mycoides subsp. capri isolated in Jordan: Comparison of different diagnostic methods. Vet. Ital. 2010, 46, 189–207, (In English and Italian). [Google Scholar]
- Rodríguez, J.L.; Gutiérrez, C.; Brooks, D.L.; DaMassa, A.J.; Orós, J.; Fernández, A. A pathological and immunohistochemical study of goat kids undergoing septicaemic disease caused by Mycoplasma capricolum subsp. capricolum, Mycoplasma mycoides subsp. capri and Mycoplasma mycoides subsp. mycoides (large colony type). Zent. Vet. B 1998, 45, 141–149. [Google Scholar] [CrossRef] [PubMed]
- DaMassa, A.J.; Brooks, D.L.; Holmberg, C.A. Pathogenicity of Mycoplasma capricolum and Mycoplasma putrefaciens. Isr. J. Med. Sci. 1984, 20, 975–978. [Google Scholar] [PubMed]
- Adler, H.E.; DaMassa, A.J.; Brooks, D.L. Caprine mycoplasmosis: Mycoplasma putrefaciens, a new cause of mastitis in goats. Am. J. Vet. Res. 1980, 41, 1677–1679. [Google Scholar] [PubMed]
- OIE. Animal Health Information WAHIS Interface; 2005–2019. Available online: https://www.oie.int/wahis_2/public/wahid.php/Diseaseinformation/Diseasetimelines/index/newlang/en?header_disease_type_hidden=0&header_disease_id_hidden=0&header_selected_disease_name_hidden=0&header_disease_type=0&header_disease_id_terrestrial=47&header_disease_id_aquatic=−999&header_firstyear=2005&header_lastyear=2019 (accessed on 11 January 2021).
- Al-Momani, W.; Halablab, M.A.; Abo-Shehada, M.N.; Miles, K.; McAuliffe, L.; Nicholas, R.A.J. Isolation and molecular identification of small ruminant mycoplasmas in Jordan. Small Rumin. Res. 2006, 65, 106–112. [Google Scholar] [CrossRef]
- Maksimovic, Z.; Bacic, A.; Rifatbegovic, M. Mycoplasmas isolated from ruminants in Bosnia and Herzegovina between 1995 and 2015. Veterinaria 2016, 65, 27–31. [Google Scholar]
- Cokrevski, S.; Crcev, D.; Loria, G.R.; Nicholas, R.A.J. Outbreaks of contagious agalactia in small ruminants in the Republic of Macedonia. Vet. Rec. 2001, 148, 667. [Google Scholar] [CrossRef]
- Goçmen, H.; Rosales, R.; Ayling, R.; Ülgen, M. Comparison of PCR tests for the detection of Mycoplasma agalactiae in sheep and goats. Turk. J. Vet. Anim. Sci. 2016, 40, 421–427. [Google Scholar] [CrossRef]
- Ariza-Miguel, J.; Rodriguez-Lazaro, D.; Hernandez, M. A survey of Mycoplasma agalactiae in dairy sheep farms in Spain. BMC Vet. Res. 2012, 8, 171. [Google Scholar] [CrossRef] [PubMed]
- Amores, J.; Sánchez, A.; Gómez-Martín, Á.; Corrales, J.C.; Contreras, A.; de la Fe, C. Surveillance of Mycoplasma agalactiae and Mycoplasma mycoides subsp. capri in dairy goat herds. Small Rumin. Res. 2012, 102, 89–93. [Google Scholar] [CrossRef]
- De La Fe, C.; Assunção, P.; Antunes, T.; Rosales, R.S.; Poveda, J.B. Microbiological survey for Mycoplasma spp. in a contagious agalactia endemic area. Vet. J. 2005, 170, 257–259. [Google Scholar] [CrossRef] [PubMed]
- Chazel, M.; Tardy, F.; Le Grand, D.; Calavas, D.; Poumarat, F. Mycoplasmoses of ruminants in France: Recent data from the national surveillance network. BMC Vet. Res. 2010, 6, 32. [Google Scholar] [CrossRef]
- Filioussis, G.; Giadinis, N.D.; Petridou, E.J.; Karavanis, E.; Papageorgiou, K.; Karatzias, H. Congenital polyarthritis in goat kids attributed to Mycoplasma agalactiae. Vet. Rec. 2011, 169, 364. [Google Scholar] [CrossRef]
- Bruno, H.L.S.; Alves, J.G.S.; Mota, A.R.; Campos, A.C.; Junior, J.W.P.; Santos, S.R.; Mota, R.A. Mycoplasma aagalctiae in semen and milk of goat from Pernambuco, Brazil. Pesqui. Vet. Bras. 2013, 33, 1309–1312. [Google Scholar]
- Sirand-Pugnet, P.; Citti, C.; Barré, A.; Blanchard, A. Evolution of mollicutes: Down a bumpy road with twists and turns. Res. Microbiol. 2007, 158, 754–766. [Google Scholar] [CrossRef] [PubMed]
- Loria, G.R.; Puleio, R.; Filioussis, G.; Rosales, R.S.; Nicholas, R.A.J. Contagious Agalactia: Costs and Control Revisited Scientific and Technical Review; OIE: Paris, France, 2019; Volume 38. [Google Scholar]
- Verbisck-Bucker, G.; González-Candela, M.; Galián, J.; Cubero-Pablo, M.J.; Martín-Atance, P.; León-Vizcaíno, L. Epidemiology of Mycoplasma agalactiae infection in free-ranging Spanish ibex (Capra pyrenaica) in Andalusia, southern Spain. J. Wildl. Dis. 2008, 44, 369–380. [Google Scholar] [CrossRef] [PubMed]
- Loria, G.R.; Ruocco, L.; Ciaccio, G.; Iovino, F.; Nicholas, R.A.J.; Borrello, S. The Implications of EU Regulation 2016/429 on Neglected Diseases of Small Ruminants including Contagious Agalactia with Particular Reference to Italy. Animals 2010, 10, 900. [Google Scholar] [CrossRef] [PubMed]
- Commission Delegated Regulation (EU). 2018/1629 of 25 July 2018 Amending the List of Diseases Set Out in Annex II to Regulation (EU) 2016/429 of the European Parliament and of the Council on Transmissible Animal Diseases and Amending and Repealing Certain Acts in the Area of Animal Health (Animal Health Law); Commission Delegated Regulation (EU): Brussels, Belgium, 25 July 2018. [Google Scholar]
| PATHOGENS | M. agalactiae | M. m. capri M. c. capricolum M. putrefaciens * | |
|---|---|---|---|
| GENE CLUSTER | M. bovis | M. mycoides | |
| HOST SPECIES | Sheep; goats | Goats; sheep (±) | |
| CLINICAL FORM | sheep | subacute/chronic | Not reported |
| goats | acute/chronic | hyperacute/subacute (Mmc, Mcc) | |
| MORTALITY | sheep | low | Not reported |
| goats | low | High (especially in kids) | |
| MORBIDITY | sheep | >50% | Not reported |
| goats | >70% | >80% | |
| TYPICAL SYNDROMES | Mammary Articular Ocular Others | Pulmonary Articular Ocular Others | |
| PATHOLOGY | Frequent (>60% of cases) | Chronic interstitial mastitis (Unilateral or bilateral) | - Primary interstitial pneumonia and pleurisy; - Severe fibrin purulent polyarthritis; - Septicemia (kids) |
| Rare (<15% of cases) | - Keratoconjunctivitis; - Fibrinopurulent arthritis; - Pneumonia and pleurisy; - Abortion | - Chronic interstitial mastitis (unilateral or bilateral); - Keratoconjunctivitis; - Abortion | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Migliore, S.; Puleio, R.; Nicholas, R.A.J.; Loria, G.R. Mycoplasma agalactiae: The Sole Cause of Classical Contagious Agalactia? Animals 2021, 11, 1782. https://doi.org/10.3390/ani11061782
Migliore S, Puleio R, Nicholas RAJ, Loria GR. Mycoplasma agalactiae: The Sole Cause of Classical Contagious Agalactia? Animals. 2021; 11(6):1782. https://doi.org/10.3390/ani11061782
Chicago/Turabian StyleMigliore, Sergio, Roberto Puleio, Robin A. J. Nicholas, and Guido R. Loria. 2021. "Mycoplasma agalactiae: The Sole Cause of Classical Contagious Agalactia?" Animals 11, no. 6: 1782. https://doi.org/10.3390/ani11061782
APA StyleMigliore, S., Puleio, R., Nicholas, R. A. J., & Loria, G. R. (2021). Mycoplasma agalactiae: The Sole Cause of Classical Contagious Agalactia? Animals, 11(6), 1782. https://doi.org/10.3390/ani11061782






