Identity of blaCTX-M Carrying Plasmids in Sequential ESBL-E. coli Isolates from Patients with Recurrent Urinary Tract Infections
Abstract
1. Introduction
2. Materials and Methods
2.1. Patients and Isolates
2.2. Phylogenetics Analysis of ESBL E. coli
2.3. Detection of blaCTX-M Genes
2.4. Plasmid Extraction and Replicon Typing of Plasmids
2.5. Optical DNA Mapping of Plasmids
3. Results
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Shamsrizi, P.; Gladstone, B.P.; Carrara, E.; Luise, D.; Cona, A.; Bovo, C.; Tacconelli, E. Variation of effect estimates in the analysis of mortality and length of hospital stay in patients with infections caused by bacteria-producing extended-spectrum beta-lactamases: A systematic review and meta-analysis. BMJ Open 2020, 10, e030266. [Google Scholar] [CrossRef]
- Pitout, J.D.; Laupland, K.B. Extended-spectrum beta-lactamase-producing Enterobacteriaceae: An emerging public-health concern. Lancet Infect. Dis. 2008, 8, 159–166. [Google Scholar] [CrossRef]
- Lindblom, A.; Karami, N.; Magnusson, T.; Ahren, C. Subsequent infection with extended-spectrum beta-lactamase-producing Enterobacteriaceae in patients with prior infection or fecal colonization. Eur. J. Clin. Microbiol. Infect. Dis. 2018, 37, 1491–1497. [Google Scholar] [CrossRef]
- Petty, N.K.; Ben Zakour, N.L.; Stanton-Cook, M.; Skippington, E.; Totsika, M.; Forde, B.M.; Phan, M.D.; Gomes Moriel, D.; Peters, K.M.; Davies, M.; et al. Global dissemination of a multidrug resistant Escherichia coli clone. Proc. Natl. Acad. Sci. USA 2014, 111, 5694–5699. [Google Scholar] [CrossRef]
- Karami, N.; Lindblom, A.; Yazdanshenas, S.; Linden, V.; Ahren, C. Recurrence of urinary tract infections with extended-spectrum beta-lactamase-producing Escherichia coli caused by homologous strains among which clone ST131-O25b is dominant. J. Glob. Antimicrob. Resist. 2020, 22, 126–132. [Google Scholar] [CrossRef]
- Bevan, E.R.; Jones, A.M.; Hawkey, P.M. Global epidemiology of CTX-M beta-lactamases: Temporal and geographical shifts in genotype. J. Antimicrob. Chemother. 2017, 72, 2145–2155. [Google Scholar] [CrossRef] [PubMed]
- Matsumura, Y.; Pitout, J.D.; Gomi, R.; Matsuda, T.; Noguchi, T.; Yamamoto, M.; Peirano, G.; DeVinney, R.; Bradford, P.A.; Motyl, M.R.; et al. Global Escherichia coli Sequence Type 131 Clade with blaCTX-M-27 Gene. Emerg. Infect. Dis. 2016, 22, 1900–1907. [Google Scholar] [CrossRef] [PubMed]
- Mathers, A.J.; Peirano, G.; Pitout, J.D. The role of epidemic resistance plasmids and international high-risk clones in the spread of multidrug-resistant Enterobacteriaceae. Clin. Microbiol. Rev. 2015, 28, 565–591. [Google Scholar] [CrossRef]
- Bi, D.; Zheng, J.; Li, J.J.; Sheng, Z.K.; Zhu, X.; Ou, H.Y.; Li, Q.; Wei, Q. In Silico Typing and Comparative Genomic Analysis of IncFIIK Plasmids and Insights into the Evolution of Replicons, Plasmid Backbones, and Resistance Determinant Profiles. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef]
- Bahl, M.I.; Hansen, L.H.; Sorensen, S.J. Persistence mechanisms of conjugative plasmids. Methods Mol. Biol. 2009, 532, 73–102. [Google Scholar] [CrossRef]
- Yang, Q.E.; Sun, J.; Li, L.; Deng, H.; Liu, B.T.; Fang, L.X.; Liao, X.P.; Liu, Y.H. IncF plasmid diversity in multi-drug resistant Escherichia coli strains from animals in China. Front. Microbiol. 2015, 6, 964. [Google Scholar] [CrossRef] [PubMed]
- Muller, V.; Karami, N.; Nyberg, L.K.; Pichler, C.; Torche Pedreschi, P.C.; Quaderi, S.; Fritzsche, J.; Ambjornsson, T.; Ahren, C.; Westerlund, F. Rapid Tracing of Resistance Plasmids in a Nosocomial Outbreak Using Optical DNA Mapping. ACS Infect. Dis. 2016, 2, 322–328. [Google Scholar] [CrossRef] [PubMed]
- Stillwell, T.; Green, M.; Barbadora, K.; Ferrelli, J.G.; Roberts, T.L.; Weissman, S.J.; Nowalk, A. Outbreak of KPC-3 Producing Carbapenem-Resistant Klebsiella pneumoniae in a US Pediatric Hospital. J. Pediatric. Infect. Dis. Soc. 2015, 4, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Nyberg, L.K.; Quaderi, S.; Emilsson, G.; Karami, N.; Lagerstedt, E.; Muller, V.; Noble, C.; Hammarberg, S.; Nilsson, A.N.; Sjoberg, F.; et al. Rapid identification of intact bacterial resistance plasmids via optical mapping of single DNA molecules. Sci. Rep. 2016, 6, 30410. [Google Scholar] [CrossRef] [PubMed]
- Nilsson, A.N.; Emilsson, G.; Nyberg, L.K.; Noble, C.; Stadler, L.S.; Fritzsche, J.; Moore, E.R.; Tegenfeldt, J.O.; Ambjornsson, T.; Westerlund, F. Competitive binding-based optical DNA mapping for fast identification of bacteria–multi-ligand transfer matrix theory and experimental applications on Escherichia coli. Nucleic. Acids. Res. 2014, 42, e118. [Google Scholar] [CrossRef] [PubMed]
- Saar, K.L.; Zhang, Y.; Muller, T.; Kumar, C.P.; Devenish, S.; Lynn, A.; Lapinska, U.; Yang, X.; Linse, S.; Knowles, T.P.J. On-chip label-free protein analysis with downstream electrodes for direct removal of electrolysis products. Lab. Chip. 2017, 18, 162–170. [Google Scholar] [CrossRef] [PubMed]
- Muller, V.; Rajer, F.; Frykholm, K.; Nyberg, L.K.; Quaderi, S.; Fritzsche, J.; Kristiansson, E.; Ambjornsson, T.; Sandegren, L.; Westerlund, F. Direct identification of antibiotic resistance genes on single plasmid molecules using CRISPR/Cas9 in combination with optical DNA mapping. Sci. Rep. 2016, 6, 37938. [Google Scholar] [CrossRef]
- Bikkarolla, S.K.; Nordberg, V.; Rajer, F.; Muller, V.; Kabir, M.H.; Kk, S.; Dvirnas, A.; Ambjornsson, T.; Giske, C.G.; Naver, L.; et al. Optical DNA Mapping Combined with Cas9-Targeted Resistance Gene Identification for Rapid Tracking of Resistance Plasmids in a Neonatal Intensive Care Unit Outbreak. MBio 2019, 10. [Google Scholar] [CrossRef]
- Johnning, A.; Karami, N.; Tang Hallback, E.; Muller, V.; Nyberg, L.; Buongermino Pereira, M.; Stewart, C.; Ambjornsson, T.; Westerlund, F.; Adlerberth, I.; et al. The resistomes of six carbapenem-resistant pathogens-a critical genotype-phenotype analysis. Microb. Genom. 2018, 4. [Google Scholar] [CrossRef]
- Lin, Y.L.; Sewunet, T.; Kk, S.; Giske, C.G.; Westerlund, F. Optical maps of plasmids as a proxy for clonal spread of MDR bacteria: A case study of an outbreak in a rural Ethiopian hospital. J. Antimicrob. Chemother. 2020, 75, 2804–2811. [Google Scholar] [CrossRef]
- Lindblom, A.; Kk, S.; Muller, V.; Oz, R.; Sandstrom, H.; Ahren, C.; Westerlund, F.; Karami, N. Interspecies plasmid transfer appears rare in sequential infections with extended-spectrum beta-lactamase (ESBL)-producing Enterobacteriaceae. Diagn. Microbiol. Infect. Dis. 2019, 93, 380–385. [Google Scholar] [CrossRef] [PubMed]
- EUCAST. Available online: https://www.eucast.org/clinical_breakpoints/ (accessed on 10 May 2021).
- Helldal, L.; Karami, N.; Floren, K.; Welinder-Olsson, C.; Moore, E.R.; Ahren, C. Shift of CTX-M genotypes has determined the increased prevalence of extended-spectrum beta-lactamase-producing Escherichia coli in south-western Sweden. Clin. Microbiol. Infect. 2013, 19, E87–E90. [Google Scholar] [CrossRef] [PubMed]
- Clermont, O.; Christenson, J.K.; Denamur, E.; Gordon, D.M. The Clermont Escherichia coli phylo-typing method revisited: Improvement of specificity and detection of new phylo-groups. Environ. Microbiol. Rep. 2013, 5, 58–65. [Google Scholar] [CrossRef] [PubMed]
- Helldal, L.; Karami, N.; Welinder-Olsson, C.; Moore, E.R.; Ahren, C. Evaluation of MLVA for epidemiological typing and outbreak detection of ESBL-producing Escherichia coli in Sweden. BMC Microbiol. 2017, 17, 8. [Google Scholar] [CrossRef] [PubMed]
- Tenover, F.C.; Arbeit, R.D.; Goering, R.V.; Mickelsen, P.A.; Murray, B.E.; Persing, D.H.; Swaminathan, B. Interpreting chromosomal DNA restriction patterns produced by pulsed-field gel electrophoresis: Criteria for bacterial strain typing. J. Clin. Microbiol. 1995, 33, 2233–2239. [Google Scholar] [CrossRef] [PubMed]
- Wirth, T.; Falush, D.; Lan, R.; Colles, F.; Mensa, P.; Wieler, L.H.; Karch, H.; Reeves, P.R.; Maiden, M.C.; Ochman, H.; et al. Sex and virulence in Escherichia coli: An evolutionary perspective. Mol. Microbiol. 2006, 60, 1136–1151. [Google Scholar] [CrossRef]
- Birkett, C.I.; Ludlam, H.A.; Woodford, N.; Brown, D.F.; Brown, N.M.; Roberts, M.T.; Milner, N.; Curran, M.D. Real-time TaqMan PCR for rapid detection and typing of genes encoding CTX-M extended-spectrum ß-lactamases. J. Med. Microbiol. 2007, 56, 52–55. [Google Scholar] [CrossRef]
- Villa, L.; Carattoli, A. Plasmid Typing and Classification. Methods Mol. Biol. 2020, 2075, 309–321. [Google Scholar] [CrossRef]
- Alizadehheidari, M.; Werner, E.; Noble, C.; Reiter-Schad, M.; Nyberg, L.K.; Fritzsche, J.; Mehlig, B.; Tegenfeldt, J.O.; Ambjörnsson, T.; Persson, F.; et al. Nanoconfined Circular and Linear DNA: Equilibrium Conformations and Unfolding Kinetics. Macromolecules 2015, 48, 871–878. [Google Scholar] [CrossRef]
- Persson, F.; Tegenfeldt, J.O. DNA in nanochannels–directly visualizing genomic information. Chem. Soc. Rev. 2010, 39, 985–999. [Google Scholar] [CrossRef] [PubMed]
- Dvirnas, A.; Pichler, C.; Stewart, C.L.; Quaderi, S.; Nyberg, L.K.; Muller, V.; Kumar Bikkarolla, S.; Kristiansson, E.; Sandegren, L.; Westerlund, F.; et al. Facilitated sequence assembly using densely labeled optical DNA barcodes: A combinatorial auction approach. PLoS ONE 2018, 13, e0193900. [Google Scholar] [CrossRef] [PubMed]
- Manges, A.R.; Geum, H.M.; Guo, A.; Edens, T.J.; Fibke, C.D.; Pitout, J.D.D. Global Extraintestinal Pathogenic Escherichia coli (ExPEC) Lineages. Clin. Microbiol. Rev. 2019, 32. [Google Scholar] [CrossRef]
- Kondratyeva, K.; Salmon-Divon, M.; Navon-Venezia, S. Meta-analysis of Pandemic Escherichia coli ST131 Plasmidome Proves Restricted Plasmid-clade Associations. Sci. Rep. 2020, 10, 36. [Google Scholar] [CrossRef]
- Ny, S.; Sandegren, L.; Salemi, M.; Giske, C.G. Genome and plasmid diversity of Extended-Spectrum beta-Lactamase-producing Escherichia coli ST131-tracking phylogenetic trajectories with Bayesian inference. Sci. Rep. 2019, 9, 10291. [Google Scholar] [CrossRef] [PubMed]
- Amarsy, R.; Gueret, D.; Benmansour, H.; Flicoteaux, R.; Bercot, B.; Meunier, F.; Mougari, F.; Jacquier, H.; Pean de Ponfilly, G.; Clermont, O.; et al. Determination of Escherichia coli phylogroups in elderly patients with urinary tract infection or asymptomatic bacteriuria. Clin. Microbiol. Infect. 2019, 25, 839–844. [Google Scholar] [CrossRef] [PubMed]
- Hagel, S.; Makarewicz, O.; Hartung, A.; Weiss, D.; Stein, C.; Brandt, C.; Schumacher, U.; Ehricht, R.; Patchev, V.; Pletz, M.W. ESBL colonization and acquisition in a hospital population: The molecular epidemiology and transmission of resistance genes. PLoS ONE 2019, 14, e0208505. [Google Scholar] [CrossRef] [PubMed]
- Titelman, E.; Hasan, C.M.; Iversen, A.; Naucler, P.; Kais, M.; Kalin, M.; Giske, C.G. Faecal carriage of extended-spectrum beta-lactamase-producing Enterobacteriaceae is common 12 months after infection and is related to strain factors. Clin. Microbiol. Infect. 2014, 20, O508–O515. [Google Scholar] [CrossRef]
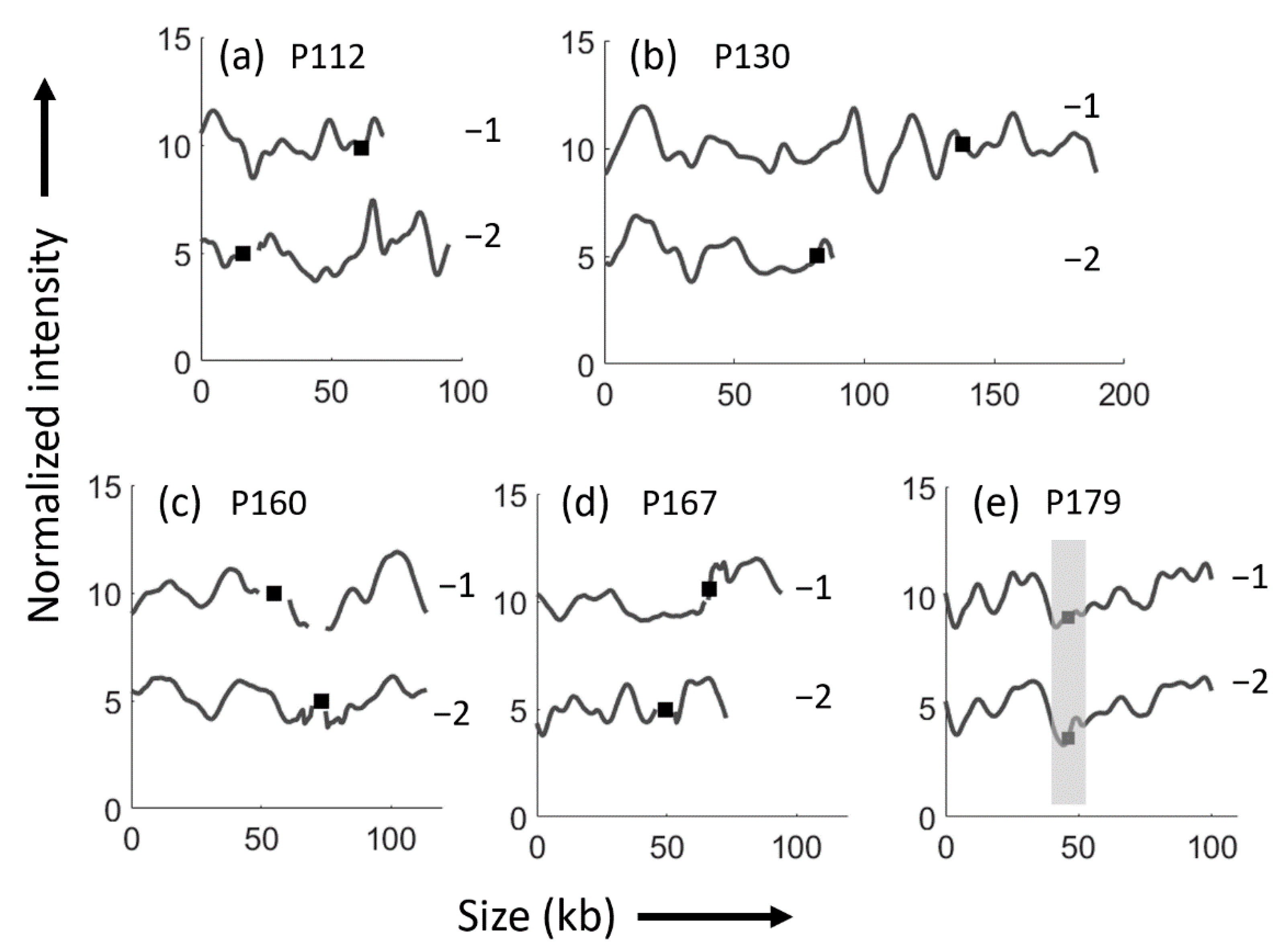
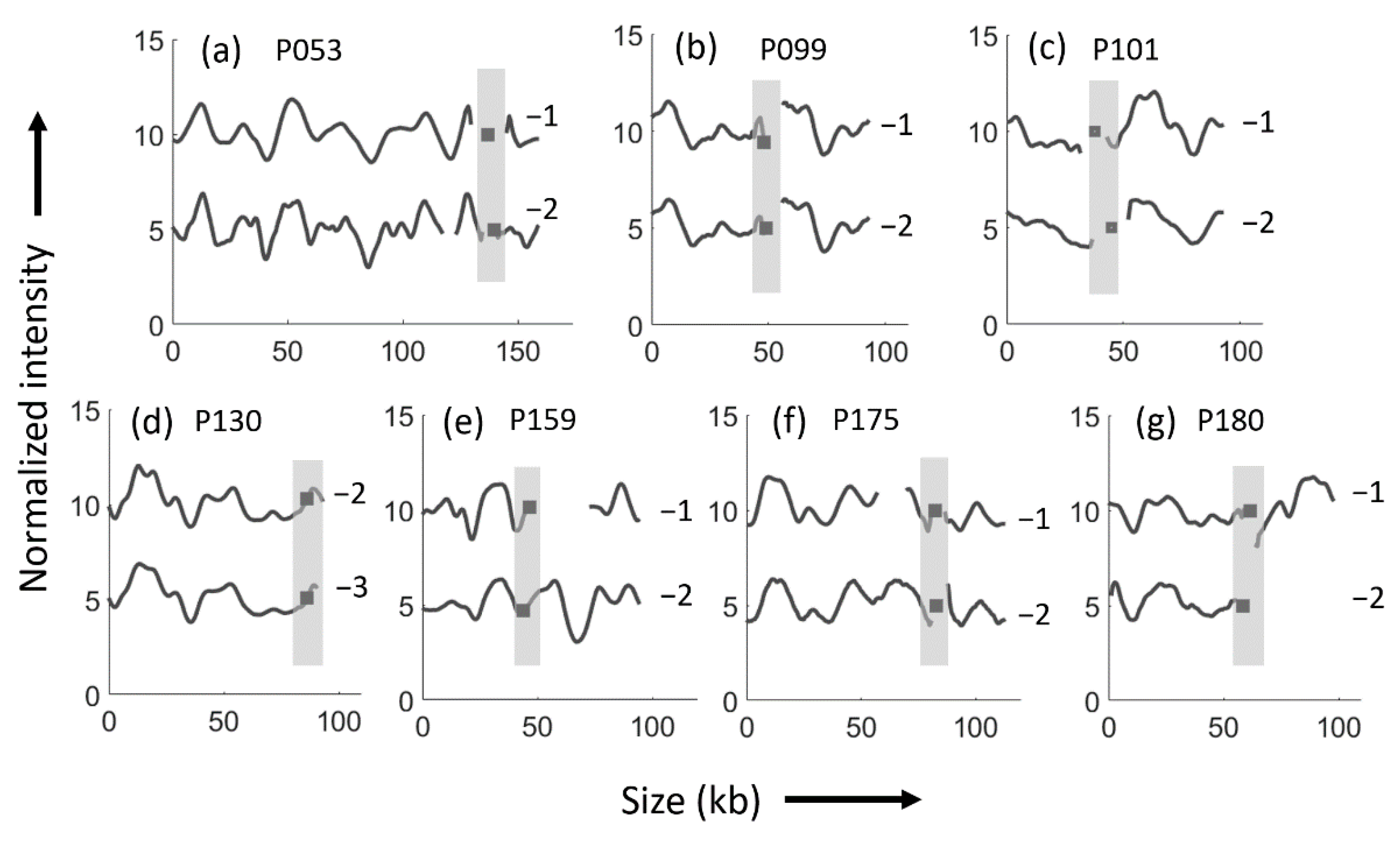

| Patient and Isolate | Year of Isolation | Sex/Age (Year) | Time from the First Isolate (Month) | Consecutive Isolate Identical 1 | ST | PFGE—Similarity (%) 2 | Phylo Group | CTX-M Gene | Replicon Type (Inc) | Size of Plasmid (kb) |
|---|---|---|---|---|---|---|---|---|---|---|
| P112-1 | 2008 | M/65 | - | 131 | 50 | B2 | 27 | FIA, FIB, FII, N | 70 | |
| -2 | 2 | - | 141 | B2 | 27 | FII, N | 86 | |||
| P160-1 | 2011 | F/34 | - | 58 | 50 | B2 | 27 | FIA, FIB, FII, I1, Y, B/O | 104 | |
| -2 | 4 | - | 43 | B1 | 27 | FIB, FII, B/O | 114 | |||
| P167-1 | 2009 | F/20 | - | 2141 | 45 | F | 15 | FIA, FIB, FII, I1 | 89 | |
| -2 | 1 | - | 131 | B2 | 15 | FIA, FIB, FII | 73 | |||
| P179-1 | 2011 | F/2 | - | 394 | 44 | D | 15 | FII, K/B | 100 | |
| -2 | 6 | - | 80 | B2 | 15 | K/B | 100 | |||
| P130-1 | 2009 | F/59 | - | 131 | 61 | B2 | 15 | FIA, FIB, FII, B/O | 189 | |
| -2 | 6 | - | 131 | B2 | 15 | FIA, FIB, FII, I1 | 93 | |||
| -3 3 | 8 | + | 100 | B2 | 15 | FIA, FIB, FII, I1 | 93 | |||
| P053-1 | 2013 | F/85 | - | 617 | 100 | A | 15 | FIA, FIB, FII | 150 | |
| -2 | 5 | + | A | 15 | FIA, FIB, FII | 150 | ||||
| P099-1 | 2010 | F/71 | - | 69 | 83 | D | 14 | FIB, FII, B/O | 93 | |
| -2 | 6 | + | D | 14 | FIB, FII | 93 | ||||
| P101-1 | 2010 | F/71 | - | 12 | 90 | B2 | 15 | FII, I1 | 94 | |
| -2 | 5 | + | B2 | 15 | FII, I1 | 82 | ||||
| P159-1 | 2010 | M/33 | - | 354 | 90 | F | 3 | FIA, FIB, FII | 71 | |
| -2 | 6 | + | F | 3 | FIA, FIB, FII | 95 | ||||
| P175-1 | 2009 | M/2 | - | 131 | 97 | B2 | 14 | FIA, FIB, FII I1 | 104 | |
| -2 | 5 | + | B2 | 14 | FIA, FIB, FII I1 | 113 | ||||
| P180-1 | 2012 | M/1 | - | 131 | 95 | B2 | 15 | FIA, FIB, FII | 98 | |
| -2 | 5 | + | B2 | 15 | FIA, FII | 62 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Karami, N.; KK, S.; Yazdanshenas, S.; Lin, Y.-L.; Jaén-Luchoro, D.; Ekedahl, E.; Parameshwaran, S.; Lindblom, A.; Åhrén, C.; Westerlund, F. Identity of blaCTX-M Carrying Plasmids in Sequential ESBL-E. coli Isolates from Patients with Recurrent Urinary Tract Infections. Microorganisms 2021, 9, 1138. https://doi.org/10.3390/microorganisms9061138
Karami N, KK S, Yazdanshenas S, Lin Y-L, Jaén-Luchoro D, Ekedahl E, Parameshwaran S, Lindblom A, Åhrén C, Westerlund F. Identity of blaCTX-M Carrying Plasmids in Sequential ESBL-E. coli Isolates from Patients with Recurrent Urinary Tract Infections. Microorganisms. 2021; 9(6):1138. https://doi.org/10.3390/microorganisms9061138
Chicago/Turabian StyleKarami, Nahid, Sriram KK, Shora Yazdanshenas, Yii-Lih Lin, Daniel Jaén-Luchoro, Elina Ekedahl, Sanjana Parameshwaran, Anna Lindblom, Christina Åhrén, and Fredrik Westerlund. 2021. "Identity of blaCTX-M Carrying Plasmids in Sequential ESBL-E. coli Isolates from Patients with Recurrent Urinary Tract Infections" Microorganisms 9, no. 6: 1138. https://doi.org/10.3390/microorganisms9061138
APA StyleKarami, N., KK, S., Yazdanshenas, S., Lin, Y.-L., Jaén-Luchoro, D., Ekedahl, E., Parameshwaran, S., Lindblom, A., Åhrén, C., & Westerlund, F. (2021). Identity of blaCTX-M Carrying Plasmids in Sequential ESBL-E. coli Isolates from Patients with Recurrent Urinary Tract Infections. Microorganisms, 9(6), 1138. https://doi.org/10.3390/microorganisms9061138






