Microbial Risk Assessment of Escherichia coli O157:H7 in Beef Imported from the United States of America to Taiwan
Abstract
1. Introduction
2. Materials and Methods
2.1. Hazard Identification
2.2. Exposure Assessment
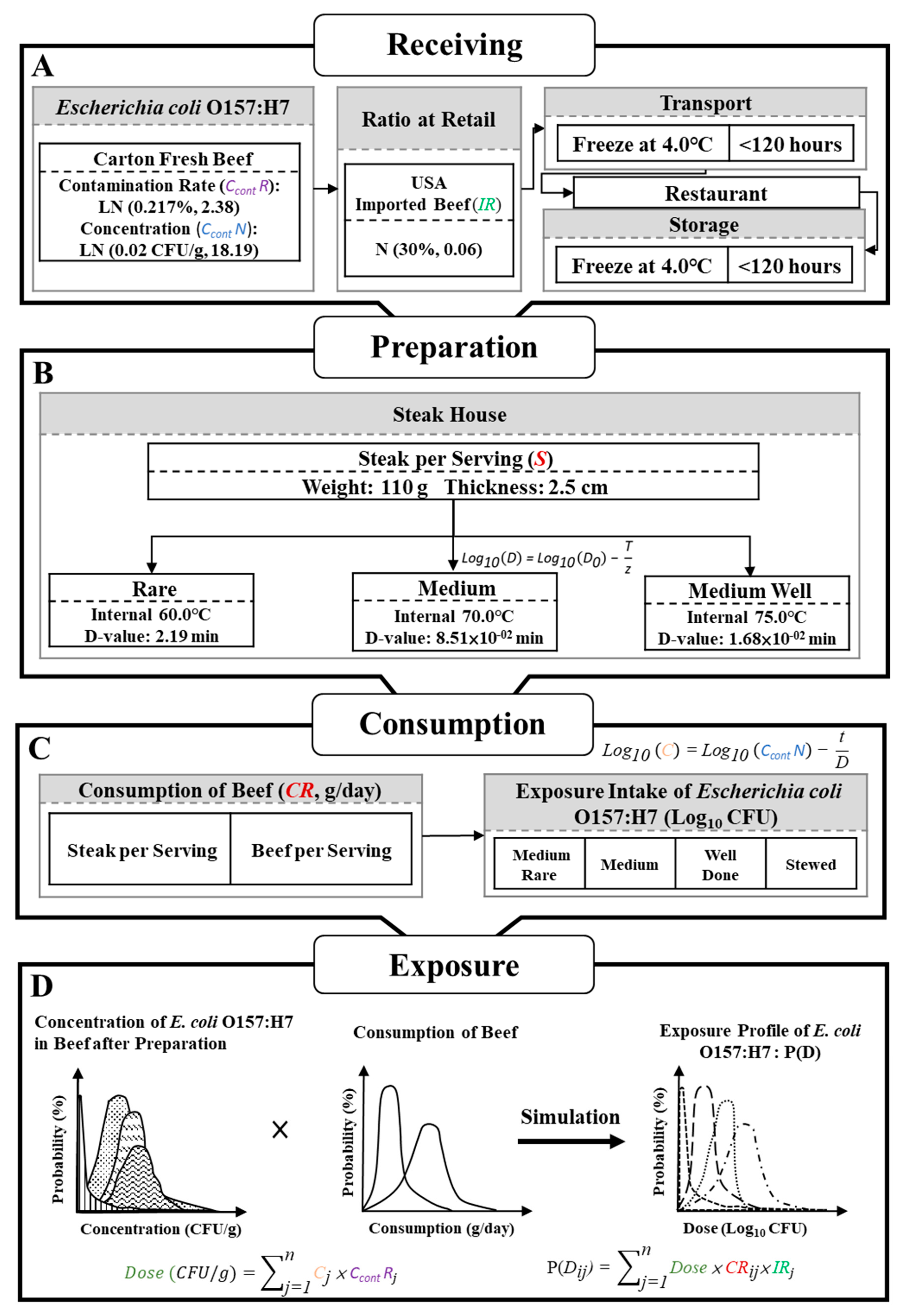
2.2.1. Model Framework
2.2.2. Contamination Rate and Concentration of E. coli
2.2.3. Consumption and Preparation
2.2.4. Probabilistic Analysis Method
2.3. Dose Response
2.4. Risk Characterization
3. Results
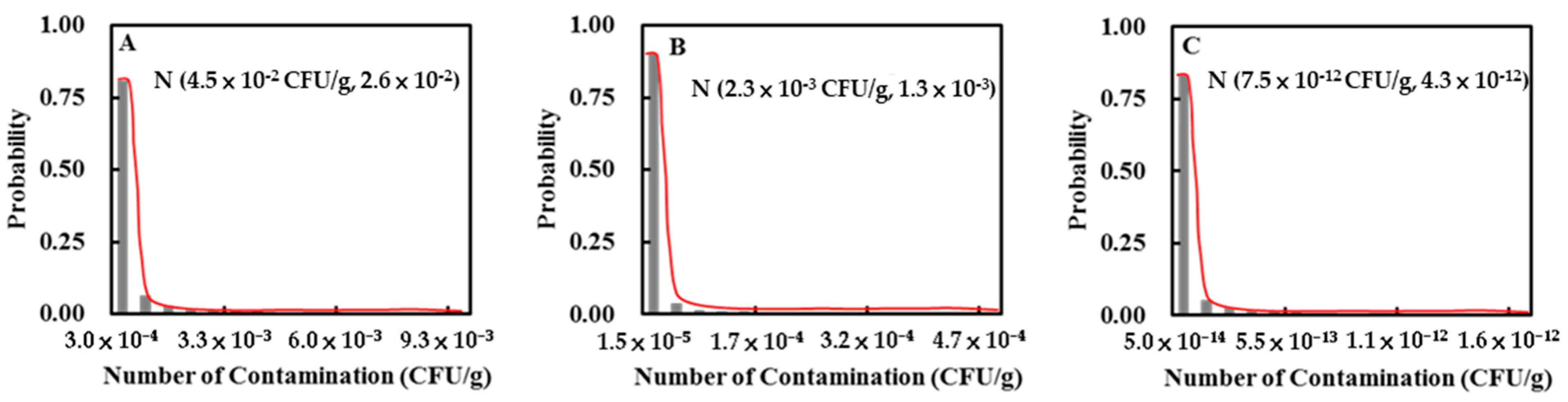
3.1. Distribution of Variables
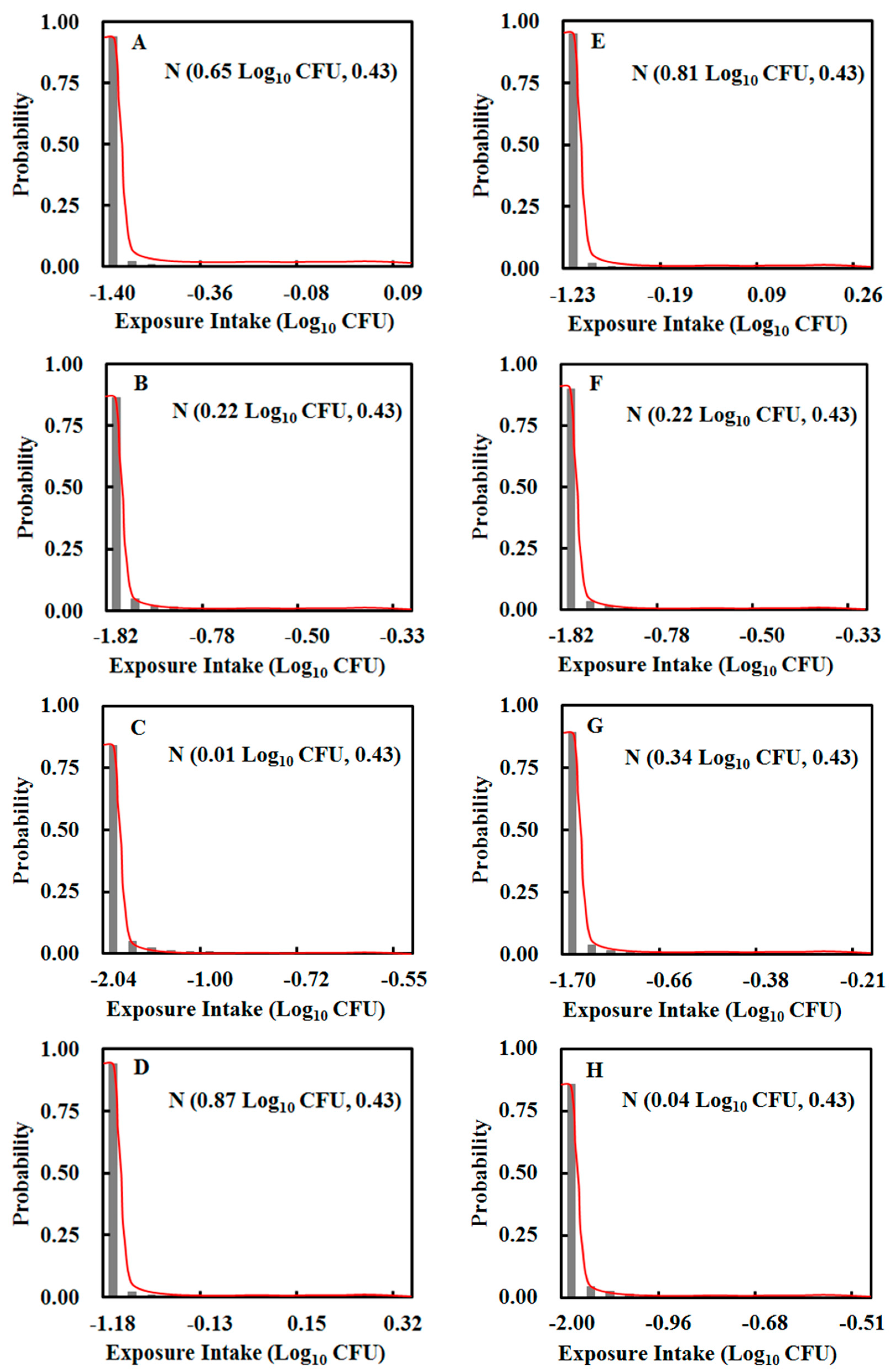
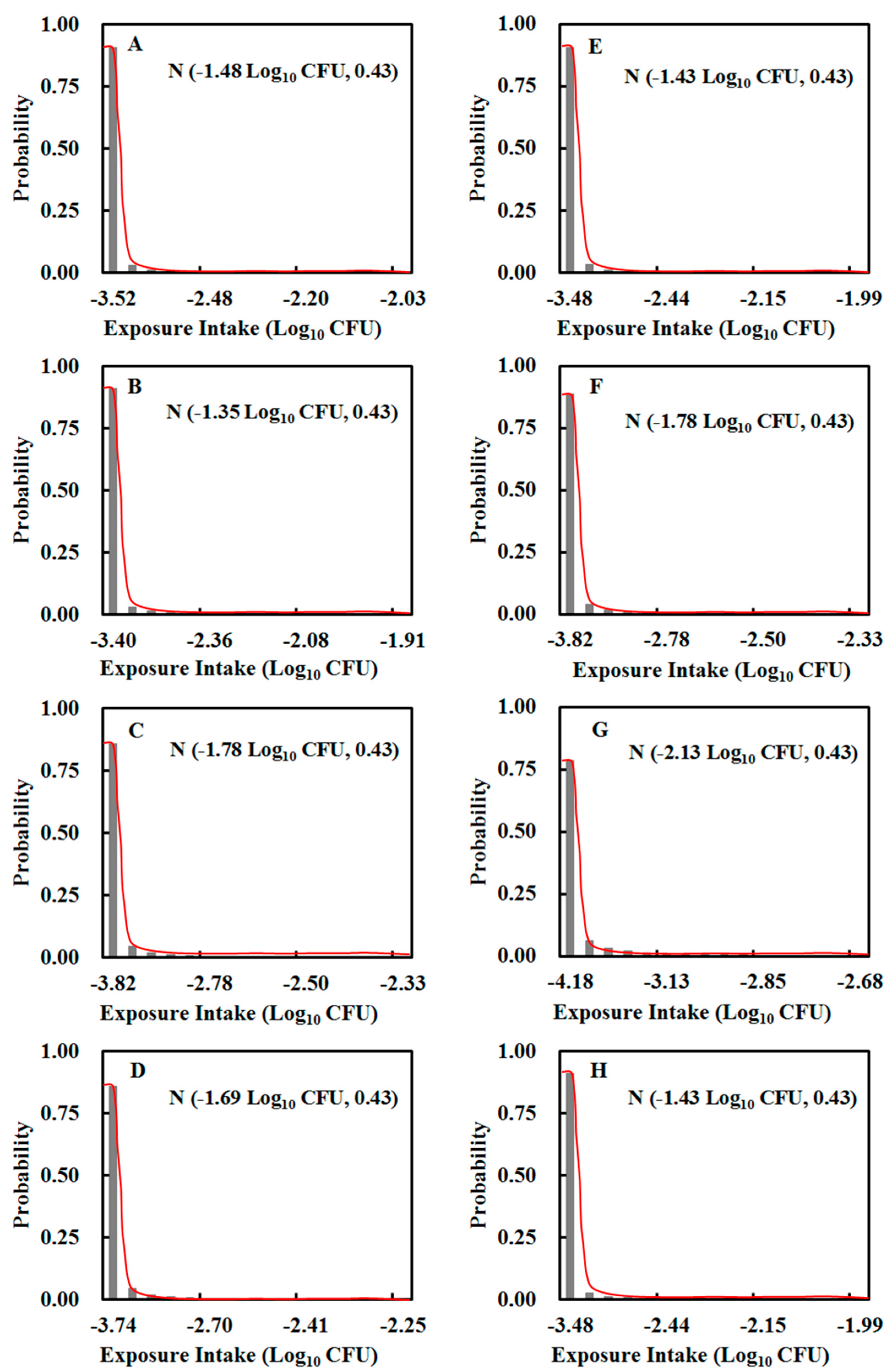
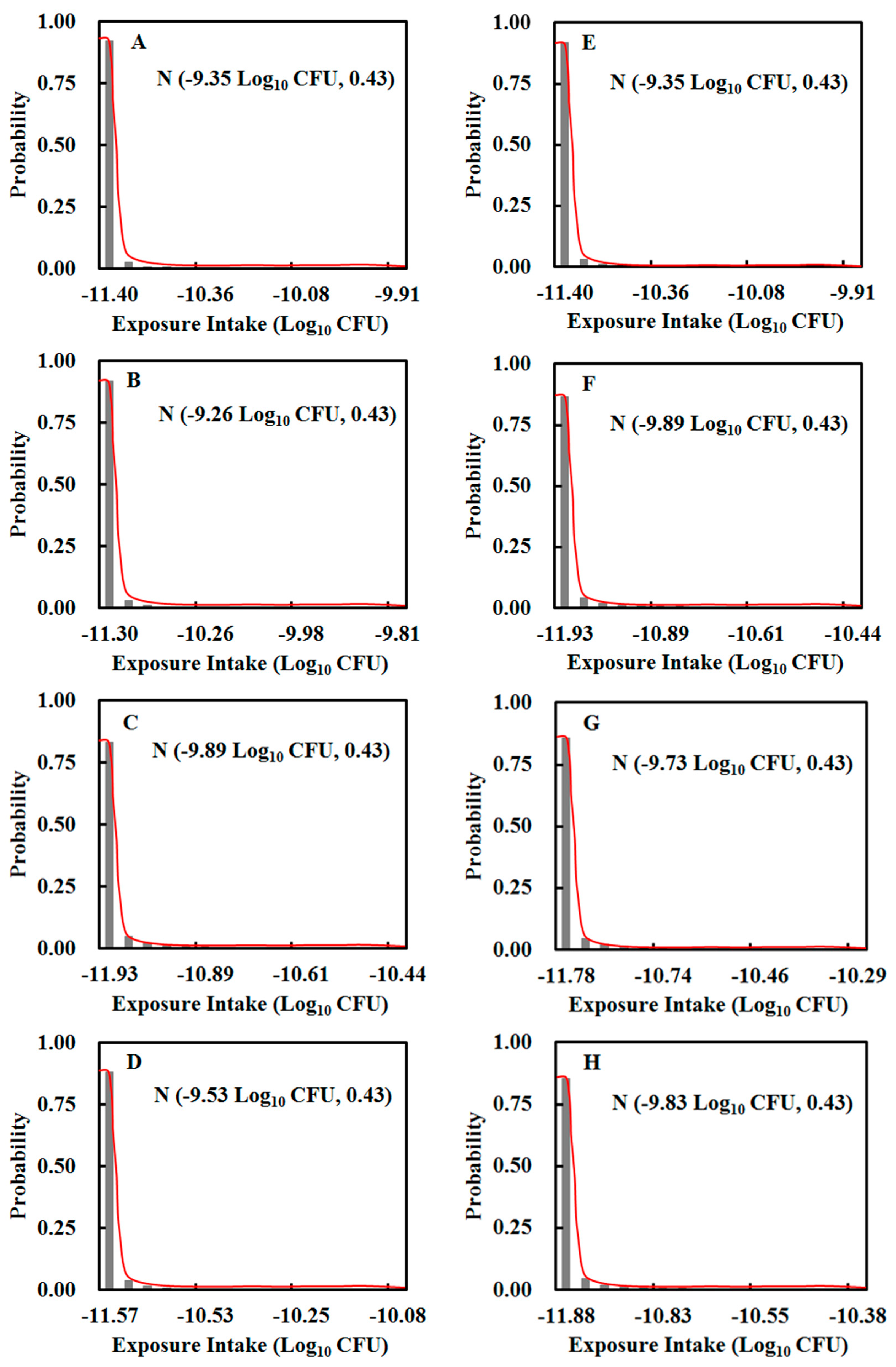
3.2. Intake of E. coli O157:H7
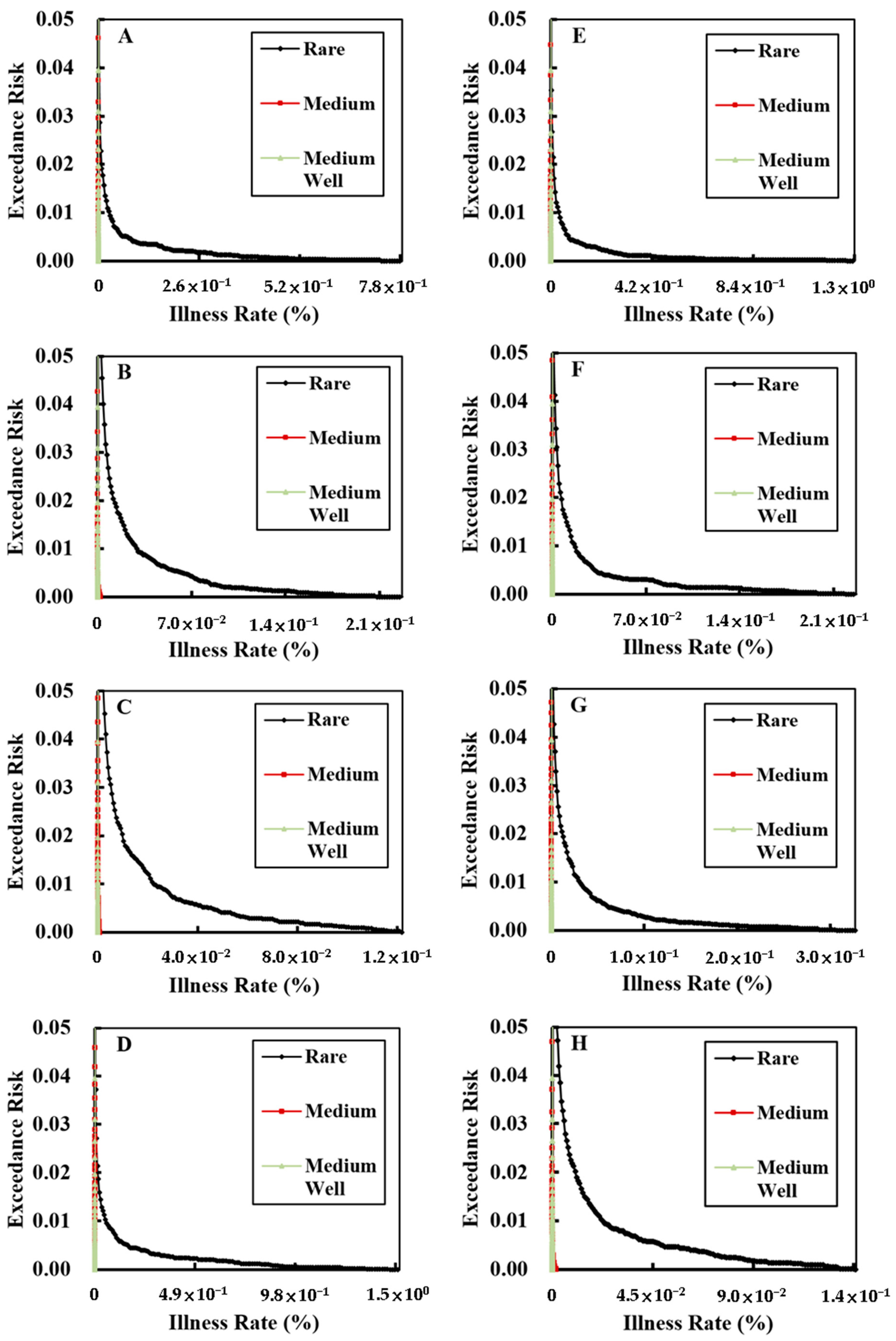
3.3. Exceedance Risk
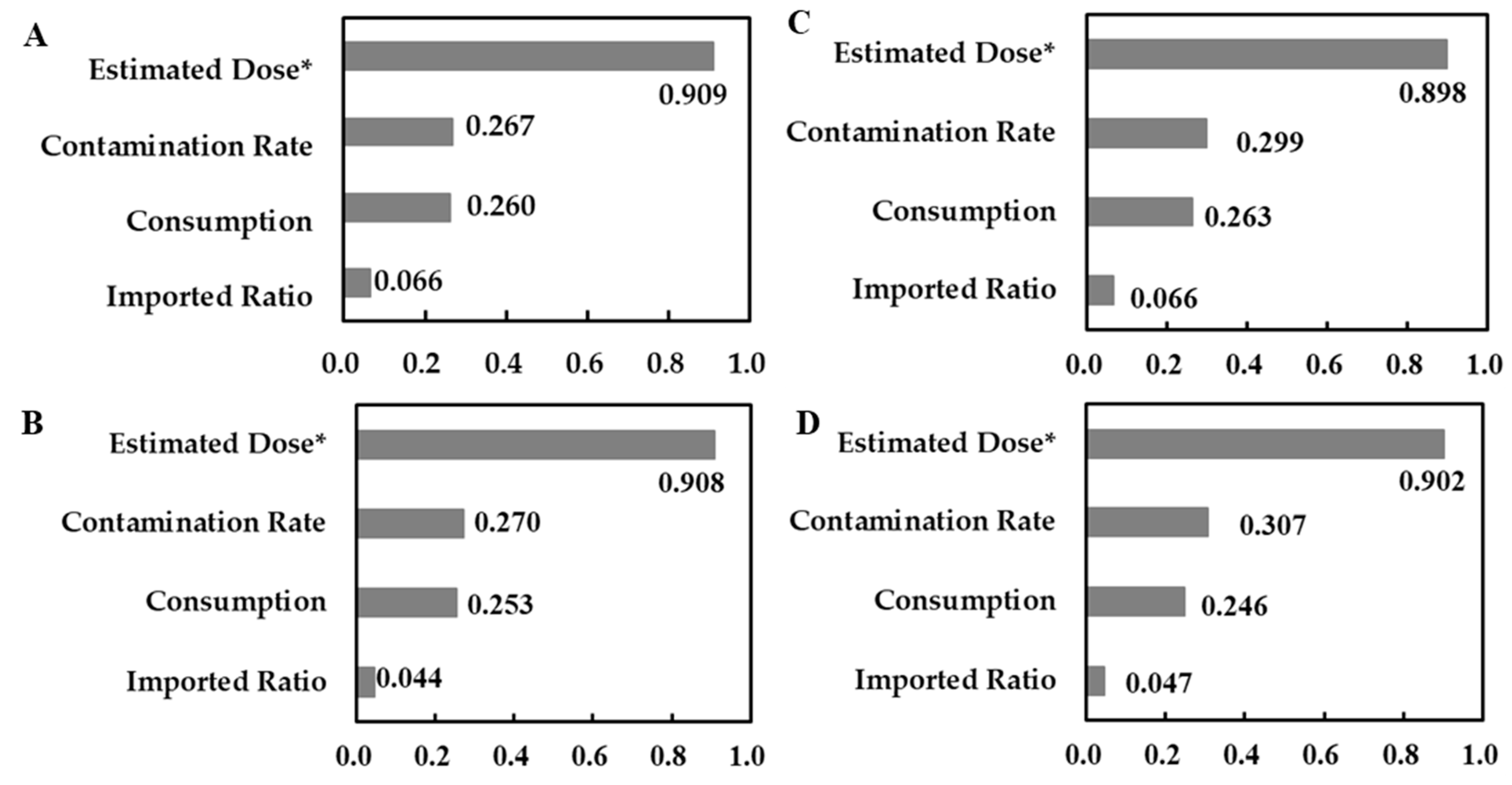
3.4. Sensitivity Analysis
4. Discussion
4.1. Quantitative Microbial Risk Assessment (QMRA) for E. coli O157:H7
4.2. Uncertainty
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Variable | Description | Distributional Assumption |
|---|---|---|
| Ccont R | Rate of contamination | Log-normal distribution [16] |
| Ccont N | Bacterial concentration was based on the number | Log-normal distribution [17] |
| IR | Beef import rate | Normal distribution [9] |
| CR | Consumption rate | Log-normal distribution [18] |
| S | Size (weight, thickness) | 2.5 cm and 110 g per serving [15] |
| D | The time (min) required to kill 90% of the population of a particular species of bacterium at a specific heating temperature. | Rare: 2.19 min; Medium: 8.51 × 10−2 min; Medium well: 1.68 × 10−2 min [19] |
| C | The residual amount of bacteria (CFU/g) in the beef after cooking | [19] |
| Dose | The distribution of bacteria (CFU/g) after cooking beef under different conditions was combined with the distribution of the contamination rate (%) | Log-normal distribution |
| Dij | Dij is the probability distribution of exposure to bacteria of individual for each sex and age exposure group via the consumption of food cluster. | |
| PI (D) | Probability of illness from dose: Beta Binomial model | PI(D) = 1 − (1 − PI(1))D [17] |
| PI (1) | Probability of illness from exposure to one organism | Beta (α, β) [17] |
| α | Susceptibility parameter | 0.267 [17] |
| β | Susceptibility parameter | ln β~ Normal (5.435, 2.47) a [17] |
| P(ED) | P(ED) is the exceedance risk of the incidence of a specific foodborne illness |
References
- Taiwan Food and Drug Administration Annual Statistics of Food Poisoning. Available online: http://www.cdway.com.tw/demo/abook25/b106/mobile/index.html (accessed on 25 October 2018).
- Takanashi, J.I.; Taneichi, H.; Misaki, T.; Yahata, Y.; Okumura, A.; Ishida, Y.I.; Miyawaki, T.; Okabe, N.; Sata, T.; Mizuguchi, M. Clinical and radiologic features of encephalopathy during 2011 E. coli O111 outbreak in Japan. Neurology 2014, 82, 564–572. [Google Scholar] [CrossRef] [PubMed]
- Burger, R. Improving Food Safety Through a One Health Approach: h: Workshop Summary. A1 EHEC O104: H4 in Germany 2011: Large Outbreak of Bloody Diarrhea and Haemolytic Uraemic Syndrome by Shiga Toxin-Producing E. coli via Contaminated Food; The National Academies Press: Washington, DC, USA, 2011. [Google Scholar] [CrossRef]
- Xu, J.G.; Cheng, B.K.; Jing, H.Q. Escherichia coli O157: H7 and Shiga-like-toxin-producing Escherichia coli in China. World J. Gastroenterol. 1999, 5, 191–194. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. E. coli. Available online: https://www.who.int/news-room/fact-sheets/detail/e-coli (accessed on 25 October 2018).
- Kiermeier, A.; Jenson, I.; Sumner, J. Risk assessment of Escherichia coli O157 illness from consumption of hamburgers in the United States made from Australian manufacturing beef. Risk Anal. 2015, 35, 77–89. [Google Scholar] [CrossRef] [PubMed]
- Donnenberg, M. Escherichia coli: Pathotypes and Principles of Pathogenesis, 2nd ed.; Michael, D., Ed.; Academic Press: Cambridge, MA, USA, 2013. [Google Scholar]
- Jay, M.T.; Garrett, V.; Mohle-Boetani, J.C.; Barros, M.; Farrar, J.A.; Rios, R.; Sobel, J. A multistate outbreak of Escherichia coli O157: H7 infection linked to consumption of beef tacos at a fast-food restaurant chain. Clin. Infect. Dis. 2004, 39, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Council of Agriculture, Executive Yuan. Available online: http://agrstat.coa.gov.tw/sdweb/public/trade/TradeCoa.aspx (accessed on 25 October 2018).
- Gansheroff, L.J.; O’Brien, A.D. Escherichia coli O157: H7 in beef cattle presented for slaughter in the US: Higher prevalence rates than previously estimated. Proc. Natl. Acad. Sci. USA 2000, 97, 2959–2961. [Google Scholar] [CrossRef] [PubMed]
- Lang, A.L.; Tsai, Y.L.; Mayer, C.L.; Patton, K.C.; Palmer, C.J. Multiplex PCR for detection of the heat-labile toxin gene and shiga-like toxin I and II genes in Escherichia coli isolated from natural waters. Appl. Environ. Microbiol. 1994, 60, 3145–3149. [Google Scholar] [CrossRef] [PubMed]
- Doyle, M.P. Escherichia coli O157: H7 and its significance in foods. Int. J. Food Microbiol. 1991, 12, 289–301. [Google Scholar] [CrossRef]
- Gill, A.; Huszczynski, G. Enumeration of Escherichia coli O157: H7 in outbreak-associated beef patties. J. Food Prot. 2016, 79, 1266–1268. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention Reports of Selected Escherichia coli Outbreak Investigations. Available online: https://www.cdc.gov/ecoli/outbreaks.html (accessed on 25 October 2018).
- Chan, S.H.; Moss, B.W.; Farmer, L.J.; Gordon, A.; Cuskelly, G.J. Comparison of consumer perception and acceptability for steaks cooked to different endpoints: Validation of photographic approach. Food Chem. 2013, 136, 1597–1602. [Google Scholar] [CrossRef] [PubMed]
- United States Department of Agriculture. Results: Raw Ground Beef and Raw Ground Beef Components Analyzed for Escherichia coli O157:H7 and non-O157 STEC, Calendar Year 2012. Available online: https://www.fsis.usda.gov/wps/portal/fsis/topics/data-collection-and-reports/microbiology/ec/summary-data/summary-data (accessed on 25 October 2018).
- Cassin, M.H.; Lammerding, A.M.; Todd, E.C.; Ross, W.; McColl, R.S. Quantitative risk assessment for Escherichia coli O157: H7 in ground beef hamburgers. Int. J. Food Microbiol. 1998, 41, 21–44. [Google Scholar] [CrossRef]
- Taiwan Food and Drug Administration National Food Consumption Database. Available online: http://tnfcds.cmu.edu.tw/index.php?action=index (accessed on 25 October 2018).
- Huang, L.; Juneja, V.K. A new kinetic model for thermal inactivation of microorganisms: Development and validation using Escherichia coli O157: H7 as a test organism. J. Food Prot. 2001, 64, 2078–2082. [Google Scholar] [CrossRef] [PubMed]
- Ebel, E.; Schlosser, W.; Kause, J.; Orloski, K.; Roberts, T.; Narrod, C.; Malcolm, S.; Coleman, M.; Powell, M. Draft risk assessment of the public health impact of Escherichia coli O157:H7 in ground beef. J. Food Prot. 2004, 67, 1991–1999. [Google Scholar] [CrossRef] [PubMed]
| Age Group | Sex | Daily Consumption (g/day) |
|---|---|---|
| 4–12 | Male and female | LN 1 (52.69, 2.60) |
| 13–18 | Male | LN (78.34, 2.10) |
| 13–18 | Female | LN (61.32, 2.24) |
| 19–65 | Male | LN (74.53, 2.41) |
| 19–65 | Female | LN (53.08, 2.75) |
| >65 | Male | LN (40.14, 2.21) |
| >65 | Female | LN (70.44, 1.33) |
| 19–49 | Female | LN (54.71, 2.81) |
| Group | Intake (Log CFU 1) | Group | Intake (Log CFU) |
|---|---|---|---|
| Males aged 13–18 years | Males aged >65 years | ||
| Rare | N b (−1.74, 0.24) | Rare | N (−1.78, 0.18) |
| Medium | N (−3.35, 0.18) | Medium | N (−3.77, 0.18) |
| Medium–well | N (−11.27, 0.14) | Medium–well | N (−11.86, 0.23) |
| Females aged 13–18 years | Females aged >65 years | ||
| Rare | N (−1.94, 0.26) | Rare | N (−1.65, 0.18) |
| Medium | N (−3.75, 0.21) | Medium | N (−4.05, 0.31) |
| Medium–well | N (−11.83, 0.27) | Medium–well | N (−11.71, 0.21) |
| Males aged 19–65 years | Males and females aged 4–12 years | ||
| Rare | N (−1.15, 0.13) | Rare | N (−1.37, 0.13) |
| Medium | N (−3.67, 0.21) | Medium | N (−3.49, 0.14) |
| Medium–well | N (−11.52, 0.18) | Medium–well | N (−11.37, 0.14) |
| Females aged 19–65 years | Females aged 19–49 years (of childbearing age) | ||
| Rare | N (−1.21, 0.13) | Rare | N (−1.92, 0.24) |
| Medium | N (−3.44, 0.17) | Medium | N (−3.45, 0.14) |
| Medium–well | N (−11.36, 0.16) | Medium–well | N (−11.79, 0.24) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lien, K.-W.; Yang, M.-X.; Ling, M.-P. Microbial Risk Assessment of Escherichia coli O157:H7 in Beef Imported from the United States of America to Taiwan. Microorganisms 2020, 8, 676. https://doi.org/10.3390/microorganisms8050676
Lien K-W, Yang M-X, Ling M-P. Microbial Risk Assessment of Escherichia coli O157:H7 in Beef Imported from the United States of America to Taiwan. Microorganisms. 2020; 8(5):676. https://doi.org/10.3390/microorganisms8050676
Chicago/Turabian StyleLien, Keng-Wen, Meng-Xuan Yang, and Min-Pei Ling. 2020. "Microbial Risk Assessment of Escherichia coli O157:H7 in Beef Imported from the United States of America to Taiwan" Microorganisms 8, no. 5: 676. https://doi.org/10.3390/microorganisms8050676
APA StyleLien, K.-W., Yang, M.-X., & Ling, M.-P. (2020). Microbial Risk Assessment of Escherichia coli O157:H7 in Beef Imported from the United States of America to Taiwan. Microorganisms, 8(5), 676. https://doi.org/10.3390/microorganisms8050676





