Larval Therapy and Larval Excretions/Secretions: A Potential Treatment for Biofilm in Chronic Wounds? A Systematic Review
Abstract
1. Introduction
1.1. Chronic Wounds
1.2. Larval Therapy
2. Materials and Methods
2.1. Eligibility Criteria
2.2. Information Sources
2.3. Search
2.4. Selection of Sources of Evidence
2.5. Data Charting Process
2.6. Data Items
3. Results
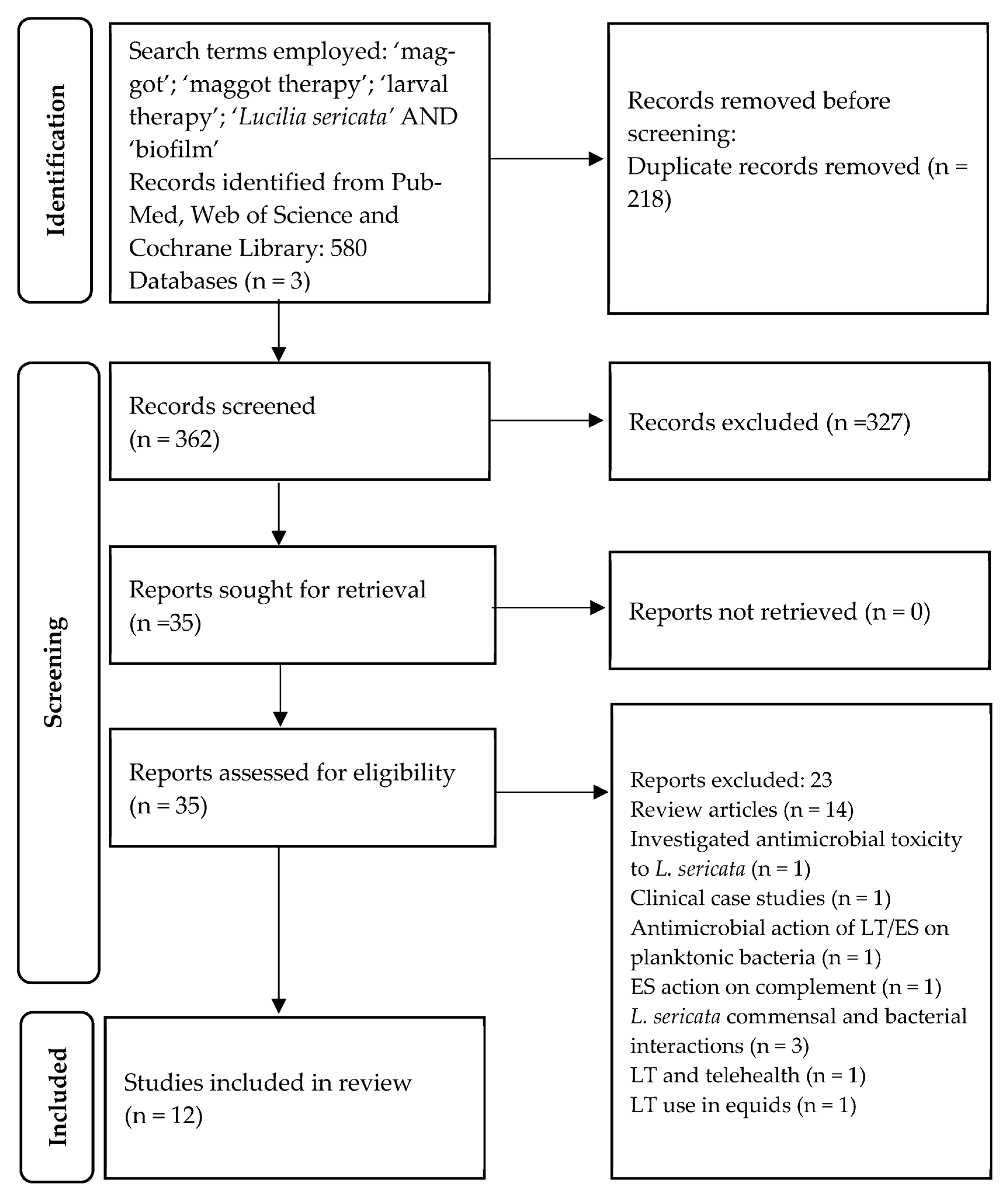
3.1. Search Results
3.2. Characteristics of Evidence Sources
3.3. Synthesis of Results
4. Discussion
4.1. ES Collection Protocol
4.2. Biofilm Models
4.3. Bacteria
4.4. Media
4.5. Inocula
4.6. Biofilm Age
4.7. Treatment Time
4.8. Vector
4.9. Mode of Action
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Martinengo, L.; Olsson, M.; Bajpai, R.; Soljak, M.; Upton, Z.; Schmidtchen, A.; Car, J.; Järbrink, K. Prevalence of chronic wounds in the general population: Systematic review and meta-analysis of observational studies. Ann. Epidemiol. 2019, 29, 8–15. [Google Scholar] [CrossRef]
- Wu, Y.-K.; Cheng, N.-C.; Cheng, C.-M. Biofilms in Chronic Wounds: Pathogenesis and Diagnosis. Trends Biotechnol. 2019, 37, 505–517. [Google Scholar] [CrossRef]
- Whitaker, I.S.; Twine, C.; Whitaker, M.J.; Welck, M.; Brown, C.S.; Shandall, A. Larval therapy from antiquity to the present day: Mechanisms of action, clinical applications and future potential. Postgrad. Med. J. 2007, 83, 409–413. [Google Scholar] [CrossRef] [PubMed]
- Baer, W.S. The Classic: The Treatment of Chronic Osteomyelitis With the Maggot (Larva of the Blow Fly). Clin. Orthop. Relat. Res. 2011, 469, 920–944. [Google Scholar] [CrossRef]
- Broughton, G.; Janis, J.E.; Attinger, C.E. The Basic Science of Wound Healing. Plast. Reconstr. Surg. 2006, 117, 12S–34S. [Google Scholar] [CrossRef] [PubMed]
- Menke, N.B.; Ward, K.R.; Witten, T.M.; Bonchev, D.G.; Diegelmann, R.F. Impaired Wound Healing. Clin. Dermatol. 2007, 25, 19–25. [Google Scholar] [CrossRef] [PubMed]
- Roberts, D.J.; Nagpal, S.K.; Forster, A.J.; Brandys, T.; Murphy, C.; Jennings, A.; Strauss, S.A.; Vishnyakova, E.; Lawson, J.; McIsaac, D.I. Disability, pain, and wound-specific concerns self-reported by adults at risk of limb loss: A cross-sectional study using the World Health Organization Disability Assessment Schedule 2.0. PLoS ONE 2021, 16, e0253288. [Google Scholar] [CrossRef]
- Gottrup, F. A specialized wound-healing center concept: Importance of a multidisciplinary department structure and surgical treatment facilities in the treatment of chronic wounds. Am. J. Surg. 2004, 187, S38–S43. [Google Scholar] [CrossRef]
- Järbrink, K.; Ni, G.; Sönnergren, H.; Schmidtchen, A.; Pang, C.; Bajpai, R.; Car, J. Prevalence and incidence of chronic wounds and related complications: A protocol for a systematic review. Syst. Rev. 2016, 5, 152. [Google Scholar] [CrossRef]
- Cho, N.H.; Shaw, J.E.; Karuranga, S.; Huang, Y.; da Rocha Fernandes, J.D.; Ohlrogge, A.W.; Malanda, B. IDF Diabetes Atlas: Global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res. Clin. Pract. 2018, 138, 271–281. [Google Scholar] [CrossRef]
- Wicke, C.; Bachinger, A.; Coerper, S.; Beckert, S.; Witte, M.B.; Königsrainer, A. Aging influences wound healing in patients with chronic lower extremity wounds treated in a specialized wound care center. Wound Repair Regen. 2009, 17, 25–33. [Google Scholar] [CrossRef] [PubMed]
- Renner, R.; Erfurt-Berge, C. Depression and quality of life in patients with chronic wounds: Ways to measure their influence and their effect on daily life. Chronic Wound Care Manag. Res. 2017, 4, 143–151. [Google Scholar] [CrossRef]
- Hussey, G.; Young, T. The impact of psychological factors on wound healing. Wounds Int. 2020, 11, 58–62. Available online: https://www.woundsme.com/uploads/resources/e265031ed764f32e01098046e3b29a58.pdf (accessed on 3 November 2021).
- The Impact of Psychological Factors on Wound Healing—Wounds International. Available online: https://www.woundsinternational.com/resources/details/impact-psychological-factors-wound-healing (accessed on 3 November 2021).
- Sen, C.K.; Gordillo, G.M.; Roy, S.; Kirsner, R.; Lambert, L.; Hunt, T.K.; Gottrup, F.; Gurtner, G.C.; Longaker, M.T. Human Skin Wounds: A Major And Snowballing Threat to Public Health and the Economy. Wound Repair Regen. 2009, 17, 763–771. [Google Scholar] [CrossRef] [PubMed]
- Phillips, C.J.; Humphreys, I.; Fletcher, J.; Harding, K.; Chamberlain, G.; Macey, S. Estimating the costs associated with the management of patients with chronic wounds using linked routine data. Int. Wound J. 2015, 13, 1193–1197. [Google Scholar] [CrossRef] [PubMed]
- Frykberg, R.G.; Banks, J.; Deptuła, M.; Karpowicz, P.; Wardowska, A.; Sass, P.; Sosnowski, P.; Mieczkowska, A.; Filipowicz, N.; Dzierżyńska, M.; et al. Challenges in the Treatment of Chronic Wounds. Adv. Wound Care 2015, 4, 560–582. [Google Scholar] [CrossRef] [PubMed]
- Guest, J.F.; Ayoub, N.; McIlwraith, T.; Uchegbu, I.; Gerrish, A.; Weidlich, D.; Vowden, K.; Vowden, P. Health economic burden that wounds impose on the National Health Service in the UK. BMJ Open 2015, 5, e009283. [Google Scholar] [CrossRef] [PubMed]
- Scarborough, P.; Bhatnagar, P.; Wickramasinghe, K.; Allender, S.; Foster, C.; Rayner, M. The economic burden of ill health due to diet, physical inactivity, smoking, alcohol and obesity in the UK: An update to 2006-07 NHS costs. J. Public Health 2011, 33, 527–535. [Google Scholar] [CrossRef]
- Guo, S.; DiPietro, L.A. Factors Affecting Wound Healing. J. Dent. Res. 2010, 89, 219–229. [Google Scholar] [CrossRef]
- Castilla, D.M.; Liu, Z.-J.; Velazquez, O.C. Oxygen: Implications for Wound Healing. Adv. Wound Care 2012, 1, 225–230. [Google Scholar] [CrossRef]
- Metcalf, D.G.; Bowler, P.G. Biofilm delays wound healing: A review of the evidence. Burns Trauma 2015, 1, 5–12. [Google Scholar] [CrossRef]
- Gould, L.; Abadir, P.; Brem, H.; Carter, M.; Conner-Kerr, T.; Davidson, J.; DiPietro, L.A.; Falanga, V.; Fife, C.E.; Gardner, S.E.; et al. Chronic Wound Repair and Healing in Older Adults: Current Status and Future Research. J. Am. Geriatr. Soc. 2015, 63, 427–438. [Google Scholar] [CrossRef] [PubMed]
- Thomason, H.A.; Williams, H.; Hardman, M.J. Sex and Sex Hormones Mediate Wound Healing. In Sex and Gender Differences in Infection and Treatments for Infectious Diseases; Springer: Berlin/Heidelberg, Germany, 2015; pp. 31–48. [Google Scholar] [CrossRef]
- Gouin, J.-P.; Kiecolt-Glaser, J.K. The Impact of Psychological Stress on Wound Healing: Methods and Mechanisms. Immunol. Allergy Clin. N. Am. 2011, 31, 81–93. [Google Scholar] [CrossRef]
- Blakytny, R.; Jude, E. The molecular biology of chronic wounds and delayed healing in diabetes. Diabet. Med. 2006, 23, 594–608. [Google Scholar] [CrossRef] [PubMed]
- Pierpont, Y.N.; Dinh, T.P.; Salas, R.E.; Johnson, E.L.; Wright, T.G.; Robson, M.C.; Payne, W.G. Obesity and Surgical Wound Healing: A Current Review. ISRN Obes. 2014, 2014, 638936. [Google Scholar] [CrossRef] [PubMed]
- Levine, J.M. The Effect of Oral Medication on Wound Healing. Adv. Ski. Wound Care 2017, 30, 137–142. [Google Scholar] [CrossRef]
- Curtis, B.J.; Hlavin, S.; Brubaker, A.L.; Kovacs, E.J.; Radek, K.A. Episodic Binge Ethanol Exposure Impairs Murine Macrophage Infiltration and Delays Wound Closure by Promoting Defects in Early Innate Immune Responses. Alcohol. Clin. Exp. Res. 2014, 38, 1347–1355. [Google Scholar] [CrossRef] [PubMed]
- McDaniel, J.C.; Browning, K.K.; McDaniel, J.C.; Browning, K.K. Smoking, Chronic Wound Healing, and Implications for Evidence-Based Practice. J. Wound, Ostomy Cont. Nurs. 2014, 41, 415–423. [Google Scholar] [CrossRef]
- Wild, T.; Rahbarnia, A.; Kellner, M.; Sobotka, L.; Eberlein, T. Basics in nutrition and wound healing. Nutrition 2010, 26, 862–866. [Google Scholar] [CrossRef]
- Edwards, R.; Harding, K.G. Bacteria and wound healing. Curr. Opin. Infect. Dis. 2004, 17, 91–96. [Google Scholar] [CrossRef]
- Davey, M.E.; O’Toole, G.A. Microbial Biofilms: From Ecology to Molecular Genetics. Microbiol. Mol. Biol. Rev. 2000, 64, 847–867. [Google Scholar] [CrossRef]
- Donlan, R.M. Biofilms: Microbial Life on Surfaces. Emerg. Infect. Dis. 2002, 8, 881–890. [Google Scholar] [CrossRef] [PubMed]
- Costerton, J.W.; Stewart, P.S.; Greenberg, E.P. Bacterial biofilms: A common cause of persistent infections. Science 1999, 284, 1318–1322. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Singh, S.K.; Chowdhury, I.; Singh, R. Understanding the Mechanism of Bacterial Biofilms Resistance to Antimicrobial Agents. Open Microbiol. J. 2017, 11, 53–62. [Google Scholar] [CrossRef] [PubMed]
- Karygianni, L.; Ren, Z.; Koo, H.; Thurnheer, T. Biofilm Matrixome: Extracellular Components in Structured Microbial Communities. Trends Microbiol. 2020, 28, 668–681. [Google Scholar] [CrossRef]
- Persat, A.; Nadell, C.D.; Kim, M.K.; Ingremeau, F.; Siryaporn, A.; Drescher, K.; Wingreen, N.S.; Bassler, B.L.; Gitai, Z.; Stone, H.A. The mechanical world of bacteria. Cell 2015, 161, 988–997. [Google Scholar] [CrossRef]
- Berne, C.; Ducret, A.; Hardy, G.G.; Brun, Y.V. Adhesins Involved in Attachment to Abiotic Surfaces by Gram-Negative Bacteria. Microbiol. Spectr. 2015, 3. [Google Scholar] [CrossRef]
- Renner, L.D.; Weibel, D.B. Physicochemical regulation of biofilm formation. MRS Bull. 2011, 36, 347–355. [Google Scholar] [CrossRef]
- Dunne, W.M. Bacterial adhesion: Seen any good biofilms lately? Clin. Microbiol. Rev. 2002, 15, 155–166. [Google Scholar] [CrossRef]
- Sauer, K. The genomics and proteomics of biofilm formation. Genome Biol. 2003, 4, 219. [Google Scholar] [CrossRef]
- Kuchma, S.L.; O’Toole, G.A. Surface-induced and biofilm-induced changes in gene expression. Curr. Opin. Biotechnol. 2000, 11, 429–433. [Google Scholar] [CrossRef] [PubMed]
- Malone, M.; Bjarnsholt, T.; McBain, A.J.; James, G.A.; Stoodley, P.; Leaper, D.; Tachi, M.; Schultz, G.; Swanson, T.; Wolcott, R.D. The prevalence of biofilms in chronic wounds: A systematic review and meta-analysis of published data. J. Wound Care 2017, 26, 20–25. [Google Scholar] [CrossRef]
- Ceri, H.; Olson, M.E.; Stremick, C.; Read, R.R.; Morck, D.; Buret, A. The Calgary Biofilm Device: New technology for rapid determination of antibiotic susceptibilities of bacterial biofilms. J. Clin. Microbiol. 1999, 37, 1771–1776. [Google Scholar] [CrossRef]
- Bowler, P.; Murphy, C.; Wolcott, R. Biofilm exacerbates antibiotic resistance: Is this a current oversight in antimicrobial stewardship? Antimicrob. Resist. Infect. Control. 2020, 9, 1–5. [Google Scholar] [CrossRef]
- Fux, C.A.; Costerton, J.W.; Stewart, P.S.; Stoodley, P. Survival strategies of infectious biofilms. Trends Microbiol. 2005, 13, 34–40. [Google Scholar] [CrossRef]
- Savage, V.J.; Chopra, I.; O’Neill, A.J. Staphylococcus aureus Biofilms Promote Horizontal Transfer of Antibiotic Resistance. Antimicrob. Agents Chemother. 2013, 57, 1968–1970. [Google Scholar] [CrossRef] [PubMed]
- Madsen, J.S.; Burmølle, M.; Hansen, L.H.; Sørensen, S.J. The interconnection between biofilm formation and horizontal gene transfer. FEMS Immunol. Med. Microbiol. 2012, 65, 183–195. [Google Scholar] [CrossRef] [PubMed]
- Van Meervenne, E.; De Weirdt, R.; Van Coillie, E.; Devlieghere, F.; Herman, L.; Boon, N. Biofilm models for the food industry: Hot spots for plasmid transfer? Pathog. Dis. 2014, 70, 332–338. [Google Scholar] [CrossRef] [PubMed]
- Wolcott, R. Disrupting the biofilm matrix improves wound healing outcomes. J. Wound Care 2015, 24, 366–371. [Google Scholar] [CrossRef]
- Schultz, G.; Bjarnsholt, T.; James, G.A.; Leaper, D.J.; McBain, A.J.; Malone, M.; Stoodley, P.; Swanson, T.; Tachi, M.; Wolcott, R.D.; et al. Consensus guidelines for the identification and treatment of biofilms in chronic nonhealing wounds. Wound Repair Regen. 2017, 25, 744–757. [Google Scholar] [CrossRef]
- Jones, C.E.; Kennedy, J.P. Treatment Options to Manage Wound Biofilm. Adv. Wound Care 2012, 1, 120–126. [Google Scholar] [CrossRef] [PubMed]
- Ammons, M.C. Anti-Biofilm Strategies and the Need for Innovations in Wound Care. Recent Patents Anti-Infective Drug Discov. 2010, 5, 10–17. [Google Scholar] [CrossRef] [PubMed]
- Malone, M.; Swanson, T. Biofilm-based wound care: The importance of debridement in biofilm treatment strategies. Br. J. Community Nurs. 2017, 22, S20–S25. [Google Scholar] [CrossRef]
- Snyder, R.J.; Bohn, G.; Hanft, J.; Harkless, L.; Kim, P.; Lavery, L.; Schultz, G.; Wolcott, R. Wound Biofilm: Current Perspectives and Strategies on Biofilm Disruption and Treatments. Wounds A Compend. Clin. Res. Pr. 2017, 29, S1–S17. [Google Scholar]
- Percival, S.; Suleman, L. Slough and biofilm: Removal of barriers to wound healing by desloughing. J. Wound Care 2015, 24, 498–510. [Google Scholar] [CrossRef] [PubMed]
- LuTheryn, G.; Glynne-Jones, P.; Webb, J.; Carugo, D. Ultrasound-mediated therapies for the treatment of biofilms in chronic wounds: A review of present knowledge. Microb. Biotechnol. 2019, 13, 613–628. [Google Scholar] [CrossRef]
- Kataoka, Y.; Kunimitsu, M.; Nakagami, G.; Koudounas, S.; Weller, C.D.; Sanada, H. Effectiveness of ultrasonic debridement on reduction of bacteria and biofilm in patients with chronic wounds: A scoping review. Int. Wound J. 2020, 18, 176–186. [Google Scholar] [CrossRef] [PubMed]
- Weed, T.; Ratliff, C.; Drake, D.B. Quantifying Bacterial Bioburden During Negative Pressure Wound Therapy. Ann. Plast. Surg. 2004, 52, 276–279. [Google Scholar] [CrossRef]
- Tahir, S.; Malone, M.; Hu, H.; Deva, A.; Vickery, K. The Effect of Negative Pressure Wound Therapy with and without Instillation on Mature Biofilms In Vitro. Materials 2018, 11, 811. [Google Scholar] [CrossRef]
- Bradley, B.H.; Cunningham, M. Biofilms in chronic wounds and the potential role of negative pressure wound therapy. J. Wound, Ostomy Cont. Nurs. 2013, 40, 143–149. [Google Scholar] [CrossRef]
- Shi, E.; Shofler, D. Maggot debridement therapy: A systematic review. Br. J. Community Nurs. 2014, 19, S6–S13. [Google Scholar] [CrossRef]
- WHO. The Evolving Threat of Antimicrobial Resistance: Options for Action; WHO: Geneva, Switzerland, 2014; pp. 1–119.
- Sherman, R.A. Maggot versus conservative debridement therapy for the treatment of pressure ulcers. Wound Repair Regen. 2002, 10, 208–214. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, D.G.; Salas, P.; Short, B.; Martin, B.R.; Kimbriel, H.R.; Nixon, B.P.; Boulton, A.J. Maggot therapy in lower-extremity hospice wound care: Fewer amputations and more antibiotic-free days. J. Am. Podiatr. Med. Assoc. 2005, 95, 254–257. [Google Scholar] [CrossRef]
- Nishijima, A.; Yamamoto, N.; Yoshida, R.; Hozawa, K.; Yanagibayashi, S.; Takikawa, M.; Hayasaka, R.; Nishijima, J.; Okada, T.; Sekido, M. Maggot debridement therapy for a patient with critical limb ischaemia and severe cardiac dysfunction: Possibility of limb salvage. Case Rep. Plast. Surg. Hand Surg. 2017, 4, 42–47. [Google Scholar] [CrossRef]
- Abela, G. Benefits of maggot debridement therapy on leg ulcers: A literature review. Br. J. Community Nurs. 2017, 22, S14–S19. [Google Scholar] [CrossRef]
- Naik, G.; Harding, K.G. Maggot debridement therapy: The current perspectives. Chronic Wound Care Manag. Res. 2017, 4, 121–128. [Google Scholar] [CrossRef]
- Thomas, S. Cost of managing chronic wounds in the UK, with particular emphasis on maggot debridement therapy. J. Wound Care 2006, 15, 465–469. [Google Scholar] [CrossRef]
- Chan, D.C.W.; Fong, D.H.F.; Leung, J.Y.Y.; Patil, N.G.; Leung, G.K.K. Maggot debridement therapy in chronic wound care. Hong Kong Med. J. 2007, 13, 382–386. [Google Scholar] [PubMed]
- Mumcuoglu, K.Y.; Ingber, A.; Gilead, L.; Stessman, J.; Friedmann, R.; Schulman, H.; Bichucher, H. Maggot therapy for the treatment of intractable wounds. Int. J. Dermatol. 1999, 38, 623–627. [Google Scholar] [CrossRef]
- Vistnes, L.M.; Lee, R.; Ksander, G.A. Proteolytic activity of blowfly larvae secretions in experimental burns. Surgery 1981, 90, 835–841. [Google Scholar]
- Lerch, K.; Linde, H.-J.; Lehn, N.; Grifka, J. Bacteria ingestion by blowfly larvae: An in vitro study. Dermatology 2003, 207, 362–366. [Google Scholar] [CrossRef]
- Prete, P.E. Growth effects of Phaenicia sericata larval extracts on fibroblasts: Mechanism for wound healing by maggot therapy. Life Sci. 1997, 60, 505–510. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Wang, S.; Diao, Y.; Zhang, J.; Lv, D. Fatty acid extracts from Lucilia sericata larvae promote murine cutaneous wound healing by angiogenic activity. Lipids Health Dis. 2010, 9, 24. [Google Scholar] [CrossRef]
- Pritchard, D.I.; Čeřovský, V.; Nigam, Y.; Pickles, S.F.; Cazander, G.; Nibbering, P.H.; Bültemann, A.; Jung, W. TIME management by medicinal larvae. Int. Wound J. 2015, 13, 475–484. [Google Scholar] [CrossRef]
- Moya-López, J.M.; Costela-Ruiz, V.P.; García-Recio, E.M.; Sherman, R.A.M.; De Luna-Bertos, E.P. Advantages of maggot debridement therapy for chronic wounds: A bibliographic review. Adv. Ski. Wound Care 2020, 33, 515–525. [Google Scholar] [CrossRef] [PubMed]
- Nigam, Y. The principles of maggot therapy and its role in contemporary wound care. Nurs. Times 2021, 117, 39–44. Available online: https://www.nursingtimes.net/clinical-archive/tissue-viability/the-principles-of-maggot-therapy-and-its-role-in-contemporary-wound-care-16-08-2021/ (accessed on 1 June 2022).
- Steenvoorde, P.; Buddingh, T.J.; Van Engeland, A.; Oskam, J. Maggot therapy and the “Yuk” factor: An issue for the patient? Wound Repair Regen. 2005, 13, 350–352. [Google Scholar] [CrossRef]
- Bazalinski, D.; Mita, J.; Scisło, L.; Wiech, P. Perception and Readiness to Undertake Maggot Debridement Therapy with the Use of Lucilia sericata Larvae in the Group of Nurses. Int. J. Environ. Res. Public Health 2022, 19, 2895. [Google Scholar] [CrossRef]
- Stadler, F. The maggot therapy supply chain: A review of the literature and practice. Med. Veter. Entomol. 2019, 34, 1–9. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef] [PubMed]
- Van Der Plas, M.J.A.; Jukema, G.N.; Wai, S.-W.; Dogterom-Ballering, H.C.M.; Lagendijk, E.L.; Van Gulpen, C.; Van Dissel, J.T.; Bloemberg, G.V.; Nibbering, P.H. Maggot excretions/secretions are differentially effective against biofilms of Staphylococcus aureus and Pseudomonas aeruginosa. J. Antimicrob. Chemother. 2007, 61, 117–122. [Google Scholar] [CrossRef] [PubMed]
- Harris, L.G.; Bexfield, A.; Nigam, Y.; Rohde, H.; Ratcliffe, N.A.; Mack, D. Disruption of Staphylococcus epidermidis biofilms by medicinal maggot Lucilia sericata excretions/secretions. Int. J. Artif. Organs 2009, 32, 555–564. [Google Scholar] [CrossRef] [PubMed]
- Cazander, G.; van Veen, K.E.B.; Bouwman, L.H.; Bernards, A.T.; Jukema, G.N. The Influence of Maggot Excretions on PAO1 Biofilm Formation on Different Biomaterials. Clin. Orthop. Relat. Res. 2009, 467, 536–545. [Google Scholar] [CrossRef]
- van der Plas, M.J.A.; Dambrot, C.; Dogterom-Ballering, H.C.M.; Kruithof, S.; van Dissel, J.T.; Nibbering, P.H. Combinations of maggot excretions/secretions and antibiotics are effective against Staphylococcus aureus biofilms and the bacteria derived therefrom. J. Antimicrob. Chemother. 2010, 65, 917–923. [Google Scholar] [CrossRef]
- Cazander, G.; van de Veerdonk, M.C.; Vandenbroucke-Grauls, C.M.J.E.; Schreurs, M.W.J.; Jukema, G.N. Maggot excretions inhibit biofilm formation on biomaterials. Clin. Orthop. Relat. Res. 2010, 468, 2789–2796. [Google Scholar] [CrossRef] [PubMed]
- Brown, A.; Horobin, A.; Blount, D.G.; Hill, P.J.; English, J.; Rich, A.; Williams, P.M.; Pritchard, D.I. Blow fly Lucilia sericata nuclease digests DNA associated with wound slough/eschar and with Pseudomonas aeruginosa biofilm. Med. Veter. Entomol. 2012, 26, 432–439. [Google Scholar] [CrossRef]
- Jiang, K.-C.; Sun, X.-J.; Wang, W.; Liu, L.; Cai, Y.; Chen, Y.-C.; Luo, N.; Yu, J.-H.; Cai, D.-Y.; Wang, A.-P. Excretions/Secretions from Bacteria-Pretreated Maggot Are More Effective against Pseudomonas aeruginosa Biofilms. PLoS ONE 2012, 7, e49815. [Google Scholar] [CrossRef]
- Harris, L.G.; Nigam, Y.; Sawyer, J.; Mack, D.; Pritchard, D.I. Lucilia sericata Chymotrypsin Disrupts Protein Adhesin-Mediated Staphylococcal Biofilm Formation. Appl. Environ. Microbiol. 2013, 79, 1393–1395. [Google Scholar] [CrossRef]
- Cowan, L.J.; Stechmiller, J.K.; Phillips, P.L.; Yang, Q.; Schultz, G.S. Chronic Wounds, Biofilms and Use of Medicinal Larvae. Ulcers 2013, 2013, 487024. [Google Scholar] [CrossRef]
- Bohova, J.; Majtan, J.; Majtan, V.; Takac, P. Selective Antibiofilm Effects of Lucilia sericata Larvae Secretions/Excretions against Wound Pathogens. Evidence-Based Complement. Altern. Med. 2014, 2014, 857360. [Google Scholar] [CrossRef]
- Liu, J.; Jiang, J.; Zong, J.; Li, B.; Pan, T.; Diao, Y.; Zhang, Z.; Zhang, X.; Lu, M.; Wang, S. Antibacterial and anti-biofilm effects of fatty acids extract of dried Lucilia sericata larvae against Staphylococcus aureus and Streptococcus pneumoniae in vitro. Nat. Prod. Res. 2019, 35, 1702–1705. [Google Scholar] [CrossRef] [PubMed]
- Becerikli, M.; Wallner, C.; Dadras, M.; Wagner, J.M.; Dittfeld, S.; Jettkant, B.; Gestmann, F.; Mehlhorn, H.; Mehlhorn-Diehl, T.; Lehnhardt, M.; et al. Maggot Extract Interrupts Bacterial Biofilm Formation and Maturation in Combination with Antibiotics by Reducing the Expression of Virulence Genes. Life 2022, 12, 237. [Google Scholar] [CrossRef]
- Høiby, N.; Bjarnsholt, T.; Moser, C.; Bassi, G.L.; Coenye, T.; Donelli, G.; Hall-Stoodley, L.; Holá, V.; Imbert, C.; Kirketerp-Møller, K.; et al. ESCMID* guideline for the diagnosis and treatment of biofilm infections 2014. Clin. Microbiol. Infect. 2015, 21 (Suppl. 1), S1–S25. [Google Scholar] [CrossRef]
- Mudge, E.; Price, P.; Neal, W.; Harding, K. A randomized controlled trial of larval therapy for the debridement of leg ulcers: Results of a multicenter, randomized, controlled, open, observer blind, parallel group study. Wound Repair Regen. 2013, 22, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Soares, M.; Iglesias, C.P.; Bland, J.M.; Cullum, N.; Dumville, J.C.; Nelson, E.A.; Torgerson, D.J.; Worthy, G. VenUS II on behalf of the VenUS II team Cost effectiveness analysis of larval therapy for leg ulcers. BMJ 2009, 338, b825. [Google Scholar] [CrossRef]
- Kerridge, A.; Lappin-Scott, H.; Stevens, J.R. Antibacterial properties of larval secretions of the blowfly, Lucilia sericata. Med. Veter. Entomol. 2005, 19, 333–337. [Google Scholar] [CrossRef]
- Polat, E.; Bolaban, D.; Sirekbasan, S. In-vivo and In-Vitro Examination of the Effect of Lucilia sericata Larvae and Secretions on the Bacteria in Open Wounds. Cyprus J. Med. Sci. 2020, 5, 113–116. [Google Scholar] [CrossRef]
- Amiri, Z.S.; Akbarzadeh, K.; Douraghi, M.; Abdi, K.M.; Afshar, A.A.; Ghaffari, J.; Kordshouli, R.S.; Akbari, M.; Rafinejad, J. Effectiveness of maggot extractions and secretion (E/S) of Lucilia sericata in reducing wound surface in experimental scalding burn injury. Nusant. Biosci. 2020, 13. [Google Scholar] [CrossRef]
- Manniello, M.D.; Moretta, A.; Salvia, R.; Scieuzo, C.; Lucchetti, D.; Vogel, H.; Sgambato, A.; Falabella, P. Insect antimicrobial peptides: Potential weapons to counteract the antibiotic resistance. Cell. Mol. Life Sci. 2021, 78, 4259–4282. [Google Scholar] [CrossRef] [PubMed]
- Sahoo, A.; Swain, S.S.; Behera, A.; Sahoo, G.; Mahapatra, P.K.; Panda, S.K. Antimicrobial Peptides Derived From Insects Offer a Novel Therapeutic Option to Combat Biofilm: A Review. Front. Microbiol. 2021, 12, 661195. [Google Scholar] [CrossRef]
- Moretta, A.; Scieuzo, C.; Petrone, A.M.; Salvia, R.; Manniello, M.D.; Franco, A.; Lucchetti, D.; Vassallo, A.; Vogel, H.; Sgambato, A.; et al. Antimicrobial Peptides: A New Hope in Biomedical and Pharmaceutical Fields. Front. Cell. Infect. Microbiol. 2021, 11, 668632. [Google Scholar] [CrossRef] [PubMed]
- Pickles, S.F.; Pritchard, D.I. Quality control of a medicinal larval (Lucilia sericata) debridement device based on released gelatinase activity. Med. Veter. Entomol. 2017, 31, 200–206. [Google Scholar] [CrossRef]
- Hermanns, R.; Mateescu, C.; Thrasyvoulou, A.; Tananaki, C.; Wagener, F.A.; Cremers, N.A. Defining the standards for medical grade honey. J. Apic. Res. 2019, 59, 125–135. [Google Scholar] [CrossRef]
- Oropeza, K. What’s the buzz about medical-grade honey? Nursing 2014, 44, 59. [Google Scholar] [CrossRef]
- Pita-Calvo, C.; Guerra-Rodríguez, M.E.; Vázquez, M. Analytical Methods Used in the Quality Control of Honey. J. Agric. Food Chem. 2017, 65, 690–703. [Google Scholar] [CrossRef]
- Carter, D.A.; Blair, S.E.; Cokcetin, N.N.; Bouzo, D.; Brooks, P.; Schothauer, R.; Harry, E.J. Therapeutic Manuka Honey: No Longer So Alternative. Front. Microbiol. 2016, 7, 569. [Google Scholar] [CrossRef] [PubMed]
- Schwarzer, S.; James, G.A.; Goeres, D.; Bjarnsholt, T.; Vickery, K.; Percival, S.L.; Stoodley, P.; Schultz, G.; Jensen, S.O.; Malone, M. The efficacy of topical agents used in wounds for managing chronic biofilm infections: A systematic review. J. Infect. 2020, 80, 261–270. [Google Scholar] [CrossRef]
- Lebeaux, D.; Chauhan, A.; Rendueles, O.; Beloin, C. From in vitro to in vivo Models of Bacterial Biofilm-Related Infections. Pathogens 2013, 2, 288–356. [Google Scholar] [CrossRef]
- Roberts, A.E.; Kragh, K.N.; Bjarnsholt, T.; Diggle, S.P. The Limitations of In Vitro Experimentation in Understanding Biofilms and Chronic Infection. J. Mol. Biol. 2015, 427, 3646–3661. [Google Scholar] [CrossRef] [PubMed]
- Khatoon, Z.; McTiernan, C.D.; Suuronen, E.J.; Mah, T.-F.; Alarcon, E.I. Bacterial biofilm formation on implantable devices and approaches to its treatment and prevention. Heliyon 2018, 4, e01067. [Google Scholar] [CrossRef]
- Guzmán-Soto, I.; McTiernan, C.; Gonzalez-Gomez, M.; Ross, A.; Gupta, K.; Suuronen, E.J.; Mah, T.-F.; Griffith, M.; Alarcon, E.I. Mimicking biofilm formation and development: Recent progress in in vitro and in vivo biofilm models. Iscience 2021, 24, 102443. [Google Scholar] [CrossRef] [PubMed]
- James, G.A.; Swogger, E.; Wolcott, R.; deLancey Pulcini, E.; Secor, P.; Sestrich, J.; Costerton, J.W.; Stewart, P.S. Biofilms in chronic wounds. Wound Repair Regen. 2008, 16, 37–44. [Google Scholar] [CrossRef]
- Birkenhauer, E.; Neethirajan, S.; Weese, J.S. Collagen and hyaluronan at wound sites influence early polymicrobial biofilm adhesive events. BMC Microbiol. 2014, 14, 191. [Google Scholar] [CrossRef]
- Werthén, M.; Henriksson, L.; Jensen, P.; Sternberg, C.; Givskov, M.; Bjarnsholt, T. An in vitro model of bacterial infections in wounds and other soft tissues. Apmis 2010, 118, 156–164. [Google Scholar] [CrossRef] [PubMed]
- Brackman, G.; Cos, P.; Maes, L.; Nelis, H.J.; Coenye, T. Quorum sensing inhibitors increase the susceptibility of bacterial biofilms to antibiotics in vitro and in vivo. Antimicrob. Agents Chemother. 2011, 55, 2655–2661. [Google Scholar] [CrossRef] [PubMed]
- Hakonen, B.; Lönnberg, L.K.; Larkö, E.; Blom, K. A Novel Qualitative and Quantitative Biofilm Assay Based on 3D Soft Tissue. Int. J. Biomater. 2014, 2014, 768136. [Google Scholar] [CrossRef] [PubMed]
- Price, B.L.; Lovering, A.M.; Bowling, F.L.; Dobson, C.B. Development of a novel collagen wound model to simulate the activity and distribution of antimicrobials in soft tissue during diabetic foot infection. Antimicrob. Agents Chemother. 2016, 60, 6880–6889. [Google Scholar] [CrossRef] [PubMed]
- Wolcott, R.; Kennedy, J.; Dowd, S. Regular debridement is the main tool for maintaining a healthy wound bed in most chronic wounds. J. Wound Care 2009, 18, 54–56. [Google Scholar] [CrossRef]
- Greene, E.; Avsar, P.; Moore, Z.; Nugent, L.; O’Connor, T.; Patton, D. What is the effect of larval therapy on the debridement of venous leg ulcers? A systematic review. J. Tissue Viability 2021, 30, 301–309. [Google Scholar] [CrossRef]
- Hobson, R.P. On an enzyme from blow-fly larvae [Lucilia sericata] which digests collagen in alkaline solution. Biochem. J. 1931, 25, 1458–1463. [Google Scholar] [CrossRef]
- Pritchard, D.I.; Brown, A.P. Degradation of MSCRAMM target macromolecules in VLU slough by Lucilia sericata chymotrypsin 1 (ISP) persists in the presence of tissue gelatinase activity. Int. Wound J. 2013, 12, 414–421. [Google Scholar] [CrossRef] [PubMed]
- Alipour, H.; Raz, A.; Zakeri, S.; Djadid, N.D. Molecular characterization of matrix metalloproteinase-1 (MMP-1) in Lucilia sericata larvae for potential therapeutic applications. Electron. J. Biotechnol. 2017, 29, 47–56. [Google Scholar] [CrossRef]
- Alipour, H.; Raz, A.; Djadid, N.D.; Zakeri, S. Expression of a New Recombinant Collagenase Protein of Lucilia sericata in SF9 Insect Cell as a Potential for Wound Healing. Iran. J. Biotechnol. 2019, 17, 16–24. [Google Scholar] [CrossRef]
- Alipour, H.; Raz, A.; Zakeri, S.; Djadid, N.D. Therapeutic applications of collagenase (metalloproteases): A review. Asian Pac. J. Trop. Biomed. 2016, 6, 975–981. [Google Scholar] [CrossRef]
- Serra, R.; Grande, R.; Butrico, L.; Rossi, A.; Settimio, U.F.; Caroleo, B.; Amato, B.; Gallelli, L.; de Franciscis, S. Chronic wound infections: The role of Pseudomonas aeruginosa and Staphylococcus aureus. Expert Rev. Anti-Infective Ther. 2015, 13, 605–613. [Google Scholar] [CrossRef] [PubMed]
- Bertesteanu, S.; Triaridis, S.; Stankovic, M.; Lazar, V.; Chifiriuc, M.C.; Vlad, M.; Grigore, R. Polymicrobial wound infections: Pathophysiology and current therapeutic approaches. Int. J. Pharm. 2014, 463, 119–126. [Google Scholar] [CrossRef]
- Murray, J.L.; Connell, J.L.; Stacy, A.; Turner, K.H.; Whiteley, M. Mechanisms of synergy in polymicrobial infections. J. Microbiol. 2014, 52, 188–199. [Google Scholar] [CrossRef]
- Nedelea, A.; Plant, R.L.; Robins, L.I.; Maddocks, S.E. Testing the efficacy of topical antimicrobial treatments using a two- and five-species chronic wound biofilm model. J. Appl. Microbiol. 2021, 132, 715–724. [Google Scholar] [CrossRef] [PubMed]
- Di Giulio, M.; Di Lodovico, S.; Fontana, A.; Traini, T.; Di Campli, E.; Pilato, S.; D’Ercole, S.; Cellini, L. Graphene Oxide affects Staphylococcus aureus and Pseudomonas aeruginosa dual species biofilm in Lubbock Chronic Wound Biofilm model. Sci. Rep. 2020, 10, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Wijesinghe, G.; Dilhari, A.; Gayani, B.; Kottegoda, N.; Samaranayake, L.; Weerasekera, M. Influence of Laboratory Culture Media on in vitro Growth, Adhesion, and Biofilm Formation of Pseudomonas aeruginosa and Staphylococcus aureus. Med. Princ. Pr. 2018, 28, 28–35. [Google Scholar] [CrossRef]
- Chen, X.; Thomsen, T.; Winkler, H.; Xu, Y. Influence of biofilm growth age, media, antibiotic concentration and exposure time on Staphylococcus aureus and Pseudomonas aeruginosa biofilm removal in vitro. BMC Microbiol. 2020, 20, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Pouget, C.; Dunyach-Remy, C.; Bernardi, T.; Provot, C.; Tasse, J.; Sotto, A.; Lavigne, J.-P. A Relevant Wound-Like in vitro Media to Study Bacterial Cooperation and Biofilm in Chronic Wounds. Front. Microbiol. 2022, 13, 705479. [Google Scholar] [CrossRef]
- Chen, X.; Lorenzen, J.; Xu, Y.; Jonikaite, M.; Thaarup, I.C.; Bjarnsholt, T.; Kirketerp-Møller, K.; Thomsen, T.R. A novel chronic wound biofilm model sustaining coexistence of Pseudomonas aeruginosa and Staphylococcus aureus suitable for testing of antibiofilm effect of antimicrobial solutions and wound dressings. Wound Repair Regen. 2021, 29, 820–829. [Google Scholar] [CrossRef]
- Kadam, S.; Madhusoodhanan, V.; Dhekane, R.; Bhide, D.; Ugale, R.; Tikhole, U.; Kaushik, K.S. Milieu matters: An in vitro wound milieu to recapitulate key features of, and probe new insights into, mixed-species bacterial biofilms. Biofilm 2021, 3, 100047. [Google Scholar] [CrossRef]
- Cutting, K.F. Wound exudate: Composition and functions. Br. J. Community Nurs. 2003, 8 (Suppl. 3), S4–S9. [Google Scholar] [CrossRef]
- Karayiannakis, A.; Zbar, A.; Polychronidis, A.; Simopoulos, C. Serum and Drainage Fluid Vascular Endothelial Growth Factor Levels in Early Surgical Wounds. Eur. Surg. Res. 2003, 35, 492–496. [Google Scholar] [CrossRef] [PubMed]
- Lantis, J.C.; Marston, W.A.; Farber, A.; Kirsner, R.S.; Zhang, Y.; Lee, T.D.; Cargill, D.I.; Slade, H.B. The influence of patient and wound variables on healing of venous leg ulcers in a randomized controlled trial of growth-arrested allogeneic keratinocytes and fibroblasts. J. Vasc. Surg. 2013, 58, 433–439. [Google Scholar] [CrossRef] [PubMed]
- Caldwell, M.D. Bacteria and Antibiotics in Wound Healing. Surg. Clin. N. Am. 2020, 100, 757–776. [Google Scholar] [CrossRef]
- Xu, L.; McLennan, S.V.; Lo, L.; Natfaji, A.; Bolton, T.; Liu, Y.; Twigg, S.M.; Yue, D.K. Bacterial load predicts healing rate in neuropathic diabetic foot ulcers. Diabetes Care 2007, 30, 378–380. [Google Scholar] [CrossRef]
- Serena, T.; Bowler, P.; Schultz, G.; D’Souza, A.; Rennie, M. Are Semi-Quantitative Clinical Cultures Inadequate? Comparison to Quantitative Analysis of 1053 Bacterial Isolates from 350 Wounds. Diagnostics 2021, 11, 1239. [Google Scholar] [CrossRef]
- Wolcott, R.; Rumbaugh, K.; James, G.; Schultz, G.; Phillips, P.; Yang, Q.; Watters, C.; Stewart, P.; Dowd, S. Biofilm maturity studies indicate sharp debridement opens a time-dependent therapeutic window. J. Wound Care 2010, 19, 320–328. [Google Scholar] [CrossRef]
- Chau, N.P.T.; Chung, N.H.; Jeon, J.G. Relationships between the antibacterial activity of sodium hypochlorite and treatment time and biofilm age in early Enterococcus faecalis biofilms. Int. Endod. J. 2014, 48, 782–789. [Google Scholar] [CrossRef] [PubMed]
- Stewart, P.S. Antimicrobial Tolerance in Biofilms. Microbiol. Spectr. 2015, 3, 3. [Google Scholar] [CrossRef] [PubMed]
- Phillips, P.L.; Yang, Q.; Schultz, G.S. The effect of negative pressure wound therapy with periodic instillation using antimicrobial solutions on Pseudomonas aeruginosa biofilm on porcine skin explants. Int. Wound J. 2013, 10, 48–55. [Google Scholar] [CrossRef] [PubMed]
- Dabiri, G.; Damstetter, E.; Phillips, T.; Croitoru, D.; Naderi-Azad, S.; Sachdeva, M.; Piguet, V.; Alavi, A.; Veld, R.C.O.; Walboomers, X.F.; et al. Choosing a Wound Dressing Based on Common Wound Characteristics. Adv. Wound Care 2016, 5, 32–41. [Google Scholar] [CrossRef]
- Dhar, Y.; Han, Y. Current developments in biofilm treatments: Wound and implant infections. Eng. Regen. 2020, 1, 64–75. [Google Scholar] [CrossRef]
- Smith, A.G.; Powis, R.A.; Pritchard, D.I.; Britland, S.T. Greenbottle (Lucilia sericata) larval secretions delivered from a prototype hydrogel wound dressing accelerate the closure of model wounds. Biotechnol. Prog. 2006, 22, 1690–1696. [Google Scholar] [CrossRef] [PubMed]
- Britland, S.; Smith, A.; Finter, W.; Eagland, D.; Vowden, K.; Vowden, P.; Telford, G.; Brown, A.; Pritchard, D. Recombinant Lucilia sericata chymotrypsin in a topical hydrogel formulation degrades human wound eschar ex vivo. Biotechnol. Prog. 2011, 27, 870–874. [Google Scholar] [CrossRef]
- eMcCarthy, H.; Rudkin, J.; Black, N.; Egallagher, L.; O’Neill, E.; O’Gara, J.P. Methicillin resistance and the biofilm phenotype in Staphylococcus aureus. Front. Cell. Infect. Microbiol. 2015, 5, 1. [Google Scholar] [CrossRef]
- Moormeier, D.E.; Bayles, K.W. Staphylococcus aureus biofilm: A complex developmental organism. Mol. Microbiol. 2017, 104, 365–376. [Google Scholar] [CrossRef]
- Whiteley, M.; Bangera, M.G.; Bumgarner, R.E.; Parsek, M.R.; Teitzel, G.M.; Lory, S.; Greenberg, E.P. Gene expression in Pseudomonas aeruginosa biofilms. Nature 2001, 413, 860–864. [Google Scholar] [CrossRef]
- Wei, Q.; Ma, L.Z. Biofilm Matrix and Its Regulation in Pseudomonas aeruginosa. Int. J. Mol. Sci. 2013, 14, 20983–21005. [Google Scholar] [CrossRef] [PubMed]
- McKenna, C.H.; Asgari, D.; Crippen, T.L.; Zheng, L.; Sherman, R.A.; Tomberlin, J.K.; Meisel, R.P.; Tarone, A.M. Gene expression in Lucilia sericata (Diptera: Calliphoridae) larvae exposed to Pseudomonas aeruginosa and Acinetobacter baumannii identifies shared and microbe-specific induction of immune genes. Insect Mol. Biol. 2021, 31, 85–100. [Google Scholar] [CrossRef] [PubMed]
- Gajula, B.M.; Munnamgi, S.M.; Basu, S.M. How bacterial biofilms affect chronic wound healing: A narrative review. Int. J. Surgery Glob. Health 2020, 3, e16. [Google Scholar] [CrossRef]
- Bi, Y.; Xia, G.; Shi, C.; Wan, J.; Liu, L.; Chen, Y.; Wu, Y.; Zhang, W.; Zhou, M.; He, H.; et al. Therapeutic strategies against bacterial biofilms. Fundam. Res. 2021, 1, 193–212. [Google Scholar] [CrossRef]
- Mishra, R.; Panda, A.K.; De Mandal, S.; Shakeel, M.; Bisht, S.S.; Khan, J. Natural Anti-biofilm Agents: Strategies to Control Biofilm-Forming Pathogens. Front. Microbiol. 2020, 11, 566325. [Google Scholar] [CrossRef] [PubMed]
- Zhang, K.; Li, X.; Yu, C.; Wang, Y. Promising Therapeutic Strategies Against Microbial Biofilm Challenges. Front. Cell. Infect. Microbiol. 2020, 10, 359. [Google Scholar] [CrossRef]
- Serena, T.E.; Jalodi, O.; Serena, L.; Patel, K.; Mynti, M. Evaluation of the combination of a biofilm-disrupting agent and negative pressure wound therapy: A case series. J. Wound Care 2021, 30, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Woodburn, K.W.; Jaynes, J.M.; Clemens, L.E. Evaluation of the Antimicrobial Peptide, RP557, for the Broad-Spectrum Treatment of Wound Pathogens and Biofilm. Front. Microbiol. 2019, 10, 1688. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Zhao, Y.; Zhao, X.; Liu, S.; Xia, X.; Zhang, S.; Wang, Y.; Zhang, H.; Xu, Y.; Chen, S.; et al. The Antimicrobial Peptide MPX Can Kill Staphylococcus aureus, Reduce Biofilm Formation, and Effectively Treat Bacterial Skin Infections in Mice. Front. Vet. Sci. 2022, 9, 327. [Google Scholar] [CrossRef]
- Alves, P.J.; Barreto, R.T.; Barrois, B.M.; Gryson, L.G.; Meaume, S.; Monstrey, S.J. Update on the role of antiseptics in the management of chronic wounds with critical colonisation and/or biofilm. Int. Wound J. 2020, 18, 342–358. [Google Scholar] [CrossRef] [PubMed]
- Mihai, M.M.; Preda, M.; Lungu, I.; Gestal, M.C.; Popa, M.I.; Holban, A.M. Nanocoatings for Chronic Wound Repair—Modulation of Microbial Colonization and Biofilm Formation. Int. J. Mol. Sci. 2018, 19, 1179. [Google Scholar] [CrossRef] [PubMed]
- Blanco-Fernandez, B.; Castaño, O.; Mateos-Timoneda, M.; Engel, E.; Pérez-Amodio, S. Nanotechnology Approaches in Chronic Wound Healing. Adv. Wound Care 2021, 10, 234–256. [Google Scholar] [CrossRef] [PubMed]
- Yang, T.; Tan, Y.; Zhang, W.; Yang, W.; Luo, J.; Chen, L.; Liu, H.; Yang, G.; Lei, X. Effects of ALA-PDT on the Healing of Mouse Skin Wounds Infected With Pseudomonas aeruginosa and Its Related Mechanisms. Front. Cell Dev. Biol. 2020, 8, 585132. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Ogawa, R.; Xiao, B.; Feng, Y.; Wu, Y.; Chen, L.; Gao, X.; Chen, H. Antimicrobial photodynamic therapy in skin wound healing: A systematic review of animal studies. Int. Wound J. 2019, 17, 285–299. [Google Scholar] [CrossRef] [PubMed]
| Title | Test Agent | Biofilms | Results Summary | Reference |
|---|---|---|---|---|
| Maggot excretions/secretions are differentially effective against biofilms of Staphylococcus aureus and Pseudomonas aeruginosa | ES | S. aureus P. aeruginosa | A quantity of 0.2 µg of ES abolished S. aureus biofilm formation: 8 h incubation. Degradation of P. aeruginosa biofilms > 10 h incubation; required 10-fold more ES than S. aureus biofilms. Boiling of ES abrogated their effects on S. aureus but not on P. aeruginosa biofilms. | [84] |
| Disruption of Staphylococcus epidermidis biofilms by medicinal maggot Lucilia sericata excretions/secretions | ES | S. epidermidis | In the presence of ES, S. epidermidis 1457 and 5179-R1 nascent biofilm formation was inhibited, and pre-formed biofilms were disrupted. ES activity was temperature- and time-dependent, inactivated by heat treatment, and disruption depended on the mechanism of intercellular adhesion. | [85] |
| The Influence of Maggot Excretions on PAO1 Biofilm Formation on Different Biomaterials | ES | P. aeruginosa | Maggot ES prevents and inhibits PAO1 biofilm formation and degrades existing biofilms. ES still had considerable biofilm-reduction properties after storage at room temperature for 1 month. ES from instar-3 maggots were more effective than ES from instar-1 maggots. | [86] |
| Combinations of maggot excretions/secretions and antibiotics are effective against Staphylococcus aureus biofilms and the bacteria derived therefrom | ES | S. aureus | A quantity of 20–200 mg/L ES eradicated S. aureus biofilms within 3 h. Enhanced antimicrobial activity of daptomycin against biofilms. | [87] |
| Maggot excretions inhibit biofilm formation on biomaterials | ES | S. aureus S. epidermidis K. oxytoca E. faecalis E. cloacae | The presence of excretions/secretions reduced biofilm formation on all biomaterials. A maximum of 92% of biofilm reduction was measured. | [88] |
| Blow fly Lucilia sericata nuclease digests DNA associated with wound slough/eschar and with Pseudomonas aeruginosa biofilm | ES | P. aeruginosa | A quantity of 20 µg/mL ES resulted in an ~50% reduction in pre-formed biofilms. | [89] |
| Excretions/secretions from bacteria-pretreated maggot are more effective against Pseudomonas aeruginosa biofilms | ES | P. aeruginosa | Researchers stated that ES obtained from larvae pre-treated with 1 × 106 CFU/mL P. aeruginosa displayed enhanced inhibition of nascent biofilm formation. | [90] |
| Lucilia sericata chymotrypsin disrupts protein adhesin-mediated staphylococcal biofilm formation | Recombinant larval derived enzyme | S. aureus S. epidermidis | Chymotrypsin derived from maggot excretions/secretions disrupts protein-dependent bacterial biofilm-formation mechanisms. | [91] |
| Chronic Wounds, Biofilms and Use of Medicinal Larvae | L. sericata larvae | S. aureus P. aeruginosa | Biofilms of P. aeruginosa and S. aureus grown on dermal pig explants were eradicated (6-log reduction) following a 48-h application of live L. sericata larvae. Following 24 h exposure, a 5-log reduction was observed. | [92] |
| Selective Antibiofilm Effects of Lucilia sericata Larvae Secretions/Excretions against Wound Pathogens | ES | S. aureus E. cloacae P. mirabilis | Maggot ES at 100 mg/mL concentration significantly reduced biofilm formation and disrupted established biofilm of E. cloacae. Heat-treated ES did not show any antibiofilm activity towards E. cloacae. Similar results were obtained in the case of S. aureus; however, the heat-treatment of maggot ES did not affect its antibiofilm activity. | [93] |
| Antibacterial and antibiofilm effects of fatty acids extract of dried Lucilia sericata larvae against Staphylococcus aureus and Streptococcus pneumoniae in vitro | Fatty acid extraction from dried and crushed L. sericata larvae | S. aureus S. pneumoniae | The fatty acid extract successfully inhibited the formation of biofilm and degraded mature biofilm produced by both species tested. Antibiofilm effects were concentration dependent. | [94] |
| Maggot Extract Interrupts Bacterial Biofilm Formation and Maturation in Combination with Antibiotics by Reducing the Expression of Virulence Genes | L. sericata extract | S. aureus P. aeruginosa | Significant reduction in observed biofilms in ex vivo human-dermal-skin explant model for both bacteria treated. | [95] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Morris, D.; Flores, M.; Harris, L.; Gammon, J.; Nigam, Y. Larval Therapy and Larval Excretions/Secretions: A Potential Treatment for Biofilm in Chronic Wounds? A Systematic Review. Microorganisms 2023, 11, 457. https://doi.org/10.3390/microorganisms11020457
Morris D, Flores M, Harris L, Gammon J, Nigam Y. Larval Therapy and Larval Excretions/Secretions: A Potential Treatment for Biofilm in Chronic Wounds? A Systematic Review. Microorganisms. 2023; 11(2):457. https://doi.org/10.3390/microorganisms11020457
Chicago/Turabian StyleMorris, Daniel, Micah Flores, Llinos Harris, John Gammon, and Yamni Nigam. 2023. "Larval Therapy and Larval Excretions/Secretions: A Potential Treatment for Biofilm in Chronic Wounds? A Systematic Review" Microorganisms 11, no. 2: 457. https://doi.org/10.3390/microorganisms11020457
APA StyleMorris, D., Flores, M., Harris, L., Gammon, J., & Nigam, Y. (2023). Larval Therapy and Larval Excretions/Secretions: A Potential Treatment for Biofilm in Chronic Wounds? A Systematic Review. Microorganisms, 11(2), 457. https://doi.org/10.3390/microorganisms11020457








