Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Protocol and Registration
2.2. Inclusion and Exclusion Criteria
2.3. Outcome and Exposure Measures
2.4. Search Methods for Identification of Studies
2.5. Data Collection
2.6. Quality and Risk of Bias
2.7. Data Analysis
3. Results
3.1. Hypertension
3.2. Cardiovascular Disease
3.3. Diabetes
3.4. Chronic Respiratory Disease
3.5. Cancer
3.6. Chronic Kidney Disease
3.7. Chronic Liver Disease
3.8. Cerebrovascular Diseases
3.9. Smoking
3.10. Age
3.11. Gender
3.12. Heterogeneity Assessment
3.13. Publication Bias Assessment
3.14. Risk of Bias and Quality of the Studies
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- WHO Coronavirus Disease (COVID-19) Dashboard. Available online: https://covid19.who.int/ (accessed on 2 April 2022).
- Zhang, X.; Tan, Y.; Ling, Y.; Lu, G.; Liu, F.; Yi, Z.; Jia, X.; Wu, M.; Shi, B.; Xu, S.; et al. Viral and host factors related to the clinical outcome of COVID-19. Nature 2020, 583, 437–440. [Google Scholar] [CrossRef] [PubMed]
- Richardson, S.; Hirsch, J.S.; Narasimhan, M.; Crawford, J.M.; McGinn, T.; Davidson, K.W.; Barnaby, D.P.; Becker, L.B.; Chelico, J.D.; Cohen, S.L.; et al. Presenting Characteristics, Comorbidities and Outcomes among 5700 Patients Hospitalized with COVID-19 in the New York City Area. JAMA 2020, 323, 2052–2059. [Google Scholar] [CrossRef]
- Liua, Y.; Gua, Z.; Xi, S.; Liu, Y.; Gu, Z.; Xia, S.; Shi, B.; Zhou, X.N.; Shi, Y.; Liu, J. What are the underlying transmission patterns of COVID-19 outbreak? An age-specific social contact characterization. EClinicalMedicine 2020, 22, 100354. [Google Scholar] [CrossRef] [PubMed]
- Cai, X.; Wu, G.; Zhang, J.; Yang, L. Risk Factors for Acute Kidney Injury in Adult Patients with COVID-19: A Systematic Review and Meta-Analysis. Front. Med. 2021, 8, 719472. [Google Scholar] [CrossRef] [PubMed]
- Gülsen, A.; König, I.R.; Jappe, U.; Drömann, D. Effect of comorbid pulmonary disease on the severity of COVID-19: A systematic review and meta-analysis. Respirology 2021, 26, 552–565. [Google Scholar] [CrossRef]
- Aveyard, P.; Gao, M.; Lindson, N.; Hartmann-Boyce, J.; Watkinson, P.; Young, D.; Coupland, C.A.C.; Tan, P.S.; Clift, A.K.; Harrison, D.; et al. Association between pre-existing respiratory disease and its treatment, and severe COVID-19: A population cohort study. Lancet Respir. Med. 2021, 9, 909–923. [Google Scholar] [CrossRef]
- Mishra, P.; Parveen, R.; Bajpai, R.; Samim, M.; Agarwal, N.B. Impact of cardiovascular diseases on severity of COVID-19 patients: A systematic review. Ann. Acad. Med. Singap. 2021, 50, 52–60. [Google Scholar] [CrossRef]
- Harrison, S.L.; Buckley, B.J.R.; Rivera-Caravaca, J.M.; Zhang, J.; Lip, G.Y.H. Cardiovascular risk factors, cardiovascular disease, and COVID-19: An umbrella review of systematic reviews. Eur. Heart J. Qual. Care Clin. Outcomes 2021, 7, 330–339. [Google Scholar] [CrossRef]
- Hessami, A.; Shamshirian, A.; Heydari, K.; Pourali, F.; Alizadeh-Navaei, R.; Moosazadeh, M.; Abrotan, S.; Shojaie, L.; Sedighi, S.; Shamshirian, D.; et al. Cardiovascular diseases burden in COVID-19: Systematic review and meta-analysis. Am. J. Emerg. Med. 2021, 46, 382–391. [Google Scholar] [CrossRef]
- Geng, J.; Yu, X.; Bao, H.; Feng, Z.; Yuan, X.; Zhang, J.; Chen, X.; Chen, Y.; Li, C.; Yu, H. Chronic Diseases as a Predictor for Severity and Mortality of COVID-19: A Systematic Review with Cumulative Meta-Analysis. Front. Med. 2021, 8, 588013. [Google Scholar] [CrossRef]
- Li, X.; Zhong, X.; Wang, Y.; Zeng, X.; Luo, T.; Liu, Q. Clinical determinants of the severity of COVID-19: A systematic review and meta-analysis. PLoS ONE 2021, 16, e0250602. [Google Scholar] [CrossRef]
- Li, X.; Guan, B.; Su, T.; Liu, W.; Chen, M.; Bin, W.K.; Guan, X.; Gary, T.; Zhu, Z. Impact of cardiovascular disease and cardiac injury on in-hospital mortality in patients with COVID-19: A systematic review and meta-analysis. Heart 2020, 106, 1142–1147. [Google Scholar] [CrossRef]
- Yang, J.; Zheng, Y.; Gou, X.; Pu, K.; Chen, Z.; Guo, Q.; Ji, R.; Wang, H.; Wang, Y.; Zhou, Y. Prevalence of comorbidities in the novel Wuhan coronavirus (COVID-19) infection: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020, 94, 91–95. [Google Scholar] [CrossRef]
- Zheng, Z.; Peng, F.; Xu, B.; Zhao, J.; Liu, H.; Peng, J.; Li, Q.; Jiang, C.; Zhou, Y.; Liu, S.; et al. Risk factors of critical and mortal COVID-19 cases: A systematic literature review and meta-analysis. J. Infect. 2020, 81, e16–e25. [Google Scholar] [CrossRef]
- Ssentongo, P.; Ssentongo, A.E.; Heilbrunn, E.S.; Ba, D.M.; Chinchilli, V.M. Association of cardiovascular disease and 10 other pre-existing comorbidities with COVID-19 mortality: A systematic review and meta-analysis. PLoS ONE 2020, 15, e0238215. [Google Scholar] [CrossRef]
- Pranata, R.; Huang, I.; Lim, M.A.; Wahjoepramono, E.J.; July, J. Impact of cerebrovascular and cardiovascular diseases on mortality and severity of COVID-19-systematic review, meta-analysis, and meta-regression. J. Stroke Cerebrovasc. Dis. 2020, 29, 104949. [Google Scholar] [CrossRef]
- Chidambaram, V.; Tun, N.L.; Haque, W.Z.; Majella, M.G.; Sivakumar, R.K.; Kumar, A.; Hsu, A.T.; Ishak, I.A.; Nur, A.A.; Ayeh, S.K.; et al. Factors associated with disease severity and mortality among patients with COVID-19: A systematic review and meta-analysis. PLoS ONE 2020, 15, e0241541. [Google Scholar] [CrossRef]
- Dessie, Z.G.; Zewotir, T. Mortality-related risk factors of COVID-19: A systematic review and meta-analysis of 42 studies and 423,117 patients. BMC Infect. Dis. 2021, 21, 855. [Google Scholar] [CrossRef]
- Yang, L.; Chai, P.; Yu, J.; Fan, X. Effects of cancer on patients with COVID-19: A systematic review and meta-analysis of 63,019 participants. Cancer Biol. Med. 2021, 18, 298–307. [Google Scholar] [CrossRef]
- Peravali, M.; Joshi, I.; Ahn, J.; Kim, C. A Systematic Review and Meta-Analysis of Clinical Characteristics and Outcomes in Patients with Lung Cancer with Coronavirus Disease 2019. JTO Clin. Res. Rep. 2021, 2, 100141. [Google Scholar] [CrossRef]
- Tian, Y.; Qiu, X.; Wang, C.; Zhao, J.; Jiang, X.; Niu, W.; Huang, J.; Zhang, F. Cancer associates with risk and severe events of COVID-19: A systematic review and meta-analysis. Int. J. Cancer. 2021, 148, 363–374. [Google Scholar] [CrossRef]
- Mohammed, S.A.; Eid, K.M.; Anyiam, F.E.; Wadaaallah, H.; Muhamed, M.A.M.; Morsi, M.H.; Dahman, N.B.H. Liver injury with COVID-19: Laboratory and histopathological outcome-systematic review and meta-analysis. Egypt. Liver J. 2022, 12, 9. [Google Scholar] [CrossRef]
- Middleton, P.; Hsu, C.; Lythgoe, M.P. Clinical outcomes in COVID-19 and cirrhosis: A systematic review and meta-analysis of observational studies. BMJ Open Gastroenterol. 2021, 8, e000739. [Google Scholar] [CrossRef]
- Kovalic, A.J.; Satapathy, S.K.; Thuluvath, P.J. Prevalence of chronic liver disease in patients with COVID-19 and their clinical outcomes: A systematic review and meta-analysis. Hepatol. Int. 2020, 14, 612–620. [Google Scholar] [CrossRef] [PubMed]
- Jdiaa, S.S.; Mansour, R.; El Alayli, A.; Gautam, A.; Thomas, P.; Mustafa, R.A. COVID-19 and chronic kidney disease: An updated overview of reviews. J. Nephrol. 2022, 35, 69–85. [Google Scholar] [CrossRef] [PubMed]
- Singh, J.; Malik, P.; Patel, N.; Pothuru, S.; Israni, A.; Chakinala, R.C.; Hussain, M.R.; Chidharla, A.; Patel, H.; Patel, S.K.; et al. Kidney disease and COVID-19 disease severity-systematic review and meta-analysis. Clin. Exp. Med. 2022, 22, 125–135. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.F.; Zhang, Z.; Pan, X.L.; Xing, G.L.; Zhang, Y.; Liu, Z.S.; Tu, S.H. The chronic kidney disease and acute kidney injury involvement in COVID-19 pandemic: A systematic review and meta-analysis. PLoS ONE 2021, 16, e0244779. [Google Scholar] [CrossRef] [PubMed]
- Cai, R.; Zhang, J.; Zhu, Y.; Liu, L.; Liu, Y.; He, Q. Mortality in chronic kidney disease patients with COVID-19: A systematic review and meta-analysis. Int. Urol. Nephrol. 2021, 53, 1623–1629. [Google Scholar] [CrossRef]
- Han, S.; Zhuang, Q.; Chiang, J.; Tan, S.H.; Chua, G.W.Y.; Xie, C.; Chua, M.L.K.; Soon, Y.Y.; Yang, V.S. Impact of cancer diagnoses on the outcomes of patients with COVID-19: A systematic review and meta-analysis. BMJ Open 2022, 12, e044661. [Google Scholar] [CrossRef]
- Ng, W.H.; Tipih, T.; Makoah, N.A.; Vermeulen, J.G.; Goedhals, D.; Sempa, J.B. Comorbidities in SARS-CoV-2 Patients: A Systematic Review and Meta-Analysis. mBio 2021, 12, e03647-20. [Google Scholar] [CrossRef]
- Zhou, Y.; Yang, Q.; Chi, J.; Dong, B.; Lv, W.; Shen, L.; Wang, Y. Comorbidities and the risk of severe or fatal outcomes associated with coronavirus disease 2019: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020, 99, 47–56. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; The PRISMA Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [Green Version]
- Degarege, A.; Naveed, Z.; Kabayundo, J. Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis. 2020. Available online: https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020184440 (accessed on 6 July 2020).
- NIH. COVID-19 Treatment Guidelines. Management of Persons with COVID-19. Available online: https://www.covid19treatmentguidelines.nih.gov/overview/management-of-covid-19/ (accessed on 5 August 2020).
- Effective Public Health Practice Project. Quality Assessment Tool for Quantitative Studies. Available online: https://healthsci.mcmaster.ca/merst/ephpp (accessed on 4 May 2022).
- Higgins, J.P.T.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ 2003, 327, 557–560. [Google Scholar] [CrossRef] [Green Version]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Baker, W.L.; White, C.M.; Cappelleri, J.C.; Kluger, J.; Coleman, C.I. Understanding heterogeneity in meta-analysis: The role of meta-regression. Int. J. Clin. Pract. 2009, 63, 1426–1434. [Google Scholar] [CrossRef]
- Hayashino, Y.; Noguchi, Y.; Fukui, T. Systematic evaluation and comparison of statistical tests for publication bias. J. Epidemiol. 2005, 15, 235–243. [Google Scholar] [CrossRef] [Green Version]
- Abbas, H.M.; Nassir, K.F.; Aga, Q.A.A.K.; Al-Gharawi, A.A.; Rasheed, J.I.; Al-Obaidy, M.W.; Jubouri, A.M.A.; Jaber, A.S.; Aga, L.A.A.K. Presenting the characteristics, smoking versus diabetes, and outcome among patients hospitalized with COVID-19. J. Med. Virol. 2021, 93, 1556–1567. [Google Scholar] [CrossRef]
- Acar, H.C.; Can, G.; Karaali, R.; Börekçi, Ş.; Balkan, İ.; Gemicioğlu, B.; Konukoğlu, D.; Erginöz, E.; Erdoğan, M.S.; Tabak, F. An easy-to-use nomogram for predicting in-hospital mortality risk in COVID-19: A retrospective cohort study in a university hospital. BMC Infect. Dis. 2021, 21, 148. [Google Scholar] [CrossRef]
- Adamuz, J.; González-Samartino, M.; Jiménez-Martínez, E.; Tapia-Pérez, M.; López-Jiménez, M.M.; Rodríguez-Fernández, H.; Castro-Navarro, T.; Zuriguel-Pérez, E.; Carratala, J.; Juvé-Udina, M.E. Risk of acute deterioration and care complexity individual factors associated with health outcomes in hospitalised patients with COVID-19: A multicentre cohort study. BMJ Open 2021, 11, e041726. [Google Scholar] [CrossRef]
- Agarwal, M.A.; Ziaeian, B.; Lavie, C.J.; Fonarow, G.C. Cardiovascular disease in hospitalized patients with a diagnosis of coronavirus from the pre-COVID-19 era in united states: National analysis from 2016–2017. Mayo Clin. Proc. 2020, 95, 2674–2683. [Google Scholar] [CrossRef]
- Aggarwal, S.; Garcia-Telles, N.; Aggarwal, G.; Lavie, C.; Lippi, G.; Henry, B.M. Clinical features, laboratory characteristics, and outcomes of patients hospitalized with coronavirus disease 2019 (COVID-19): Early report from the United States. Diagnosis 2020, 7, 91–96. [Google Scholar] [CrossRef]
- Ahmad, M.; Beg, B.M.; Majeed, A.; Areej, S.; Riffat, S.; Rasheed, M.A.; Mahmood, S.; Mushtaq, R.M.Z.; Hafeez, M.A. Epidemiological and clinical characteristics of COVID-19: A retrospective multi-center study in pakistan. Front. Public Health 2021, 9, 644199. [Google Scholar] [CrossRef]
- Aiswarya, D.; Arumugam, V.; Dineshkumar, T.; Gopalakrishnan, N.; Lamech, T.M.; Nithya, G.; Sastry, B.; Vathsalyan, P.; Dhanapriya, J.; Sakthirajan, R. Use of remdesivir in patients with COVID-19 on hemodialysis: A study of safety and tolerance. Kidney Int. Rep. 2021, 6, 586–593. [Google Scholar] [CrossRef]
- Akbariqomi, M.; Hosseini, M.S.; Rashidiani, J.; Sedighian, H.; Biganeh, H.; Heidari, R.; Moghaddam, M.M.; Farnoosh, G.; Kooshki, H. Clinical characteristics and outcome of hospitalized COVID-19 patients with diabetes: A single-center, retrospective study in iran. Diabetes Res. Clin. Pract. 2020, 169, 108467. [Google Scholar] [CrossRef]
- Akhtar, Z.; Gallagher, M.M.; Yap, Y.G.; Leung, L.W.M.; Elbatran, A.I.; Madden, B.; Ewasiuk, V.; Gregory, L.; Breathnach, A.; Chen, Z.; et al. Prolonged QT predicts prognosis in COVID-19. Pacing Clin. Electrophysiol. 2021, 44, 875–882. [Google Scholar] [CrossRef]
- Alahmari, A.A.; Khan, A.A.; Elganainy, A.; Almohammadi, E.L.; Hakawi, A.M.; Assiri, A.M.; Jokhdar, H.A. Epidemiological and clinical features of COVID-19 patients in Saudi Arabia. J. Infect. Public Health 2021, 14, 437–443. [Google Scholar] [CrossRef]
- Alasia, D.; Owhonda, G.; Maduka, O.; Nwadiuto, I.; Arugu, G.; Tobin-West, C.; Azi, E.; Oris-Onyiri, V.; Urang, I.J.; Abikor, V.; et al. Clinical and epidemiological characteristics of 646 hospitalised SARS-cov-2 positive patients in rivers state nigeria: A prospective observational study. Pan Afr. Med. J. 2021, 38, 25. [Google Scholar] [CrossRef]
- Albani, F.; Sepe, L.; Fusina, F.; Prezioso, C.; Baronio, M.; Caminiti, F.; Maio, A.D.; Faggian, B.; Franceschetti, M.E.; Massari, M. Thromboprophylaxis with enoxaparin is associated with a lower death rate in patients hospitalized with SARS-CoV-2 infection. A cohort study. EClinicalMedicine 2020, 27, 100562. [Google Scholar] [CrossRef]
- Alberici, F.; Delbarba, E.; Manenti, C.; Econimo, L.; Valerio, F.; Pola, A.; Maffei, C.; Possenti, S.; Lucca, B.; Cortinovis, R.; et al. A report from the brescia renal COVID task force on the clinical characteristics and short-term outcome of hemodialysis patients with SARS-CoV-2 infection. Kidney Int. 2020, 98, 20–26. [Google Scholar] [CrossRef]
- Alfraij, A.; Alamir, A.A.B.; Al-Otaibi, A.M.; Alsharrah, D.; Aldaithan, A.; Kamel, A.M.; Almutairi, M.; Alshammari, S.; Almazyad, M.; Macarambon, J.M.; et al. Characteristics and outcomes of coronavirus disease 2019 (COVID-19) in critically ill pediatric patients admitted to the intensive care unit: A multicenter retrospective cohort study. J. Infect. Public Health 2021, 14, 193–200. [Google Scholar] [CrossRef]
- Algado-Sellés, N.; Gras-Valentí, P.; Chico-Sánchez, P.; Mora-Muriel, J.G.; Soler-Molina, V.M.; Hernández-Maldonado, M.; Lameiras-Azevedo, A.S.; Jiménez-Sepúlveda, N.J.; Gómez-Sotero, I.L.; Villanueva-Ruiz, C.O.; et al. Frequency, associated risk factors, and characteristics of COVID-19 among healthcare personnel in a spanish health department. Am. J. Prev. Med. 2020, 59, e221–e229. [Google Scholar] [CrossRef] [PubMed]
- Alguwaihes, A.M.; Sabico, S.; Hasanato, R.; Al-Sofiani, M.; Megdad, M.; Albader, S.S.; Alsari, M.H.; Alelayan, A.; Alyusuf, E.Y.; Alzahrani, S.H.; et al. Severe vitamin D deficiency is not related to SARS-CoV-2 infection but may increase mortality risk in hospitalized adults: A retrospective case–control study in an arab gulf country. Aging Clin. Exp. Res. 2021, 33, 1415–1422. [Google Scholar] [CrossRef] [PubMed]
- Aliberti, M.J.R.; Covinsky, K.E.; Garcez, F.B.; Smith, A.K.; Curiati, P.K.; Lee, S.J.; Dias, M.B.; Melo, V.J.D.; do Rego-Júnior, O.F.; Richinho, V.D.P.; et al. A fuller picture of COVID-19 prognosis: The added value of vulnerability measures to predict mortality in hospitalised older adults. Age Ageing 2021, 50, 32–39. [Google Scholar] [CrossRef] [PubMed]
- Allameh, S.F.; Nemati, S.; Ghalehtaki, R.; Mohammadnejad, E.; Aghili, S.M.; Khajavirad, N.; Beigmohammadi, M.; Salehi, M.; Mirfazaelian, H.; Edalatifard, M.; et al. Clinical Characteristics and Outcomes of 905 COVID-19 Patients Admitted to Imam Khomeini Hospital Complex in the Capital City of Tehran, Iran. Arch. Iran. Med. 2020, 23, 766–775. [Google Scholar] [CrossRef]
- Allard, L.; Ouedraogo, E.; Molleville, J.; Bihan, H.; Giroux-Leprieur, B.; Sutton, A.; Baudry, C.; Josse, C.; Didier, M.; Deutsch, D.; et al. Malnutrition: Percentage and association with prognosis in patients hospitalized for coronavirus disease 2019. Nutrients 2020, 12, 3679. [Google Scholar] [CrossRef]
- Allenbach, Y.; Saadoun, D.; Maalouf, G.; Vieira, M.; Hellio, A.; Boddaert, J.; Gros, H.; Salem, J.E.; Rigon, M.R.; Menyssa, C.; et al. Development of a multivariate prediction model of intensive care unit transfer or death: A French prospective cohort study of hospitalized COVID-19 patients. PLoS ONE 2020, 15, e0240711. [Google Scholar] [CrossRef]
- Almaghlouth, N.K.; Davis, M.G.; Davis, M.A.; Anyiam, F.E.; Guevara, R.; Antony, S.J. Risk factors for mortality among patients with SARS-CoV-2 infection: A longitudinal observational study. J. Med. Virol. 2021, 93, 2021–2028. [Google Scholar] [CrossRef]
- Aloisio, E.; Chibireva, M.; Serafini, L.; Pasqualetti, S.; Falvella, F.S.; Dolci, A.; Panteghini, M. A comprehensive appraisal of laboratory biochemistry tests as major predictors of COVID-19 severity. Arch. Pathol. Lab. Med. 2020, 144, 1457–1464. [Google Scholar] [CrossRef]
- Alqahtani, A.M.; Al Malki, Z.S.; Alalweet, R.M.; Almazrou, S.H.; Alanazi, A.S.; Alanazi, M.A.; AlShehri, A.A.; AlGhamdi, S. Assessing the severity of illness in patients with coronavirus disease in Saudi Arabia: A retrospective descriptive cross-sectional study. Front. Public Health 2020, 8, 593256. [Google Scholar] [CrossRef]
- Al-Rousan, N.; Al-Najjar, H. Data Analysis of Coronavirus CoVID-19 Epidemic in South Korea Based on Recovered and Death Cases. J. Med. Virol. 2020, 92, 1603–1608. [Google Scholar] [CrossRef] [Green Version]
- Al-Salameh, A.; Lanoix, J.P.; Bennis, Y.; Andrejak, C.; Brochot, E.; Deschasse, G.; Dupont, H.; Goeb, V.; Jaureguy, M.; Lion, S.; et al. Characteristics and outcomes of COVID-19 in hospitalized patients with and without diabetes. Diabetes Metab. Res. 2021, 37, e3388. [Google Scholar] [CrossRef]
- Al-Samkari, H.; Leaf, R.S.K.; Dzik, W.H.; Carlson, J.C.T.; Fogerty, A.E.; Waheed, A.; Goodarzi, K.; Bendapudi, P.K.; Bornikova, L.; Gupta, S.; et al. COVID-19 and coagulation: Bleeding and thrombotic manifestations of SARS-CoV-2 infection. Blood 2020, 136, 489–500. [Google Scholar] [CrossRef]
- Alser, O.; Mokhtari, A.; Naar, L.; Langeveld, K.; Breen, K.A.; Moheb, M.E.; Kapoen, C.; Gaitanidis, A.; Christensen, M.A.; Maurer, L.R.; et al. Multisystem outcomes and predictors of mortality in critically ill patients with COVID-19: Demographics and disease acuity matter more than comorbidities or treatment modalities. J. Trauma Acute Care Surg. 2021, 90, 880–890. [Google Scholar] [CrossRef]
- Alsharidah, S.; Ayed, M.; Ameen, R.M.; Alhuraish, F.; Rouheldeen, N.A.; Alshammari, F.R.; Embaireeg, A.; Almelahi, M.; Adel, M.; Dawoud, M.E.; et al. COVID-19 convalescent plasma treatment of moderate and severe cases of SARS-CoV-2 infection: A multicenter interventional study. Int. J. Infect. Dis. 2021, 103, 439–446. [Google Scholar] [CrossRef]
- Altschul, D.J.; Unda, S.R.; Benton, J.; Ramos, R.d.l.G.; Cezayirli, P.; Mehler, M.; Eskandar, E.N. A novel severity score to predict inpatient mortality in COVID-19 patients. Sci. Rep. 2020, 10, 16726. [Google Scholar] [CrossRef]
- Alzaid, F.; Julla, J.B.; Diedisheim, M.; Potier, C.; Potier, L.; Velho, G.; Gaborit, B.; Manivet, P.; Germain, S.; Vidal-Trecan, T.; et al. Monocytopenia, monocyte morphological anomalies and hyperinflammation characterise severe COVID-19 in type 2 diabetes. EMBO Mol. Med. 2020, 12, e13038. [Google Scholar] [CrossRef]
- Amanat, M.; Rezaei, N.; Roozbeh, M.; Shojaei, M.; Tafakhori, A.; Zoghi, A.; Darazam, I.A.; Salehi, M.; Karimialavijeh, E.; Lima, B.S.; et al. Neurological manifestations as the predictors of severity and mortality in hospitalized individuals with COVID-19: A multicenter prospective clinical study. BMC Neurol. 2021, 21, 116. [Google Scholar] [CrossRef]
- Amo, J.D.; Polo, R.; Moreno, S.; Diaz, A.; Martinez, E.; Arribas, J.R.; Jarrin, I.; Hernan, M.A. Incidence and severity of COVID-19 in HIV-positive persons receiving antiretroviral therapy: A cohort study. Ann. Intern. Med. 2020, 173, 536–541. [Google Scholar]
- Anaklı, İ.; Özcan, P.E.; Polat, Ö.; Orhun, G.; Alay, G.H.; Tuna, V.; Çeliksoy, E.; Kılıç, M.; Mercan, M.; Ali, A.; et al. Prognostic value of antithrombin levels in COVID-19 patients and impact of fresh frozen plasma treatment: A retrospective study. Turk. J. Hematol. 2021, 38, 15–21. [Google Scholar] [CrossRef]
- Anantharaman, A.; Dusendang, J.R.; Schmittdiel, J.A.; Harzstark, A.L. SARS-CoV-2 clinical outcomes in patients with cancer in a large integrated health care system in northern California. Oncologist 2021, 26, e500–e504. [Google Scholar] [CrossRef]
- Andargie, T.E.; Tsuji, N.; Seifuddin, F.; Jang, M.K.; Yuen, P.S.; Kong, H.; Tunc, I.; Singh, K.; Charya, A.; Wilkins, K.; et al. Cell-free DNA maps COVID-19 tissue injury and risk of death and can cause tissue injury. JCI Insight 2021, 6, 147610. [Google Scholar] [CrossRef]
- Angelidi, A.M.; Belanger, M.J.; Lorinsky, M.K.; Karamanis, D.; Chamorro-Pareja, N.; Ognibene, J.; Palaiodimos, L.; Mantzoros, C.S. Vitamin D status is associated with in-hospital mortality and mechanical ventilation: A cohort of COVID-19 hospitalized patients. Mayo Clin. Proc. 2021, 96, 875–886. [Google Scholar] [CrossRef]
- Angelis, V.; Tippu, Z.; Joshi, K.; Reis, S.; Gronthoud, F.; Fribbens, C.; Okines, A.; Stanway, S.; Cottier, E.; McGrath, S.; et al. Defining the true impact of coronavirus disease 2019 in the at-risk population of patients with cancer. Eur. J. Cancer 2020, 136, 99–106. [Google Scholar] [CrossRef]
- Annweiler, G.; Corvaisier, M.; Gautier, J.; Dubée, V.; Legrand, E.; Sacco, G.; Annweiler, C. Vitamin D supplementation associated to better survival in hospitalized frail elderly COVID-19 patients: The GERIA-COVID quasi-experimental study. Nutrients 2020, 12, 3377. [Google Scholar] [CrossRef]
- Antúnez-Montes, O.Y.; Escamilla, M.I.; Figueroa-Uribe, A.F.; Arteaga-Menchaca, E.; Lavariega-Saráchaga, M.; Salcedo-Lozada, P.; Melchior, P.; de Oliveira, R.B.; Tirado Caballero, J.C.; Redondo, H.P.; et al. COVID-19 and Multisystem Inflammatory Syndrome in Latin American Children: A Multinational Study. Pediatr Infect Dis. J. 2021, 40, e1–e6. [Google Scholar] [CrossRef]
- Aoun, M.; Khalil, R.; Mahfoud, W.; Fatfat, H.; Khalil, L.B.; Alameddine, R.; Afiouni, N.; Ibrahim, I.; Hassan, M.; Zarzour, H.; et al. Age and multimorbidities as poor prognostic factors for COVID-19 in hemodialysis: A Lebanese national study. BMC Nephrol. 2021, 22, 73. [Google Scholar] [CrossRef]
- Apea, V.J.; Wan, Y.I.; Dhairyawan, R.; Puthucheary, Z.A.; Pearse, R.M.; Orkin, C.M.; Prowle, J.R. Ethnicity and outcomes in patients hospitalised with COVID-19 infection in east London: An observational cohort study. BMJ Open 2021, 11, e042140. [Google Scholar] [CrossRef]
- Atkins, J.L.; Masoli, J.A.H.; Delgado, J.; Pilling, L.C.; Kuo, C.; Kuchel, G.A.; Melzer, D. Preexisting comorbidities predicting COVID-19 and mortality in the UK biobank community cohort. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2020, 75, 2224–2230. [Google Scholar] [CrossRef]
- Attauabi, M.; Seidelin, J.B.; Felding, O.K.; Wewer, M.D.; Arp, L.K.V.; Sarikaya, M.Z.; Egeberg, A.; Vladimirova, N.; Bendtsen, F.; Burisch, J. Coronavirus disease 2019, immune-mediated inflammatory diseases and immunosuppressive therapies—A Danish population-based cohort study. J. Autoimmun. 2021, 118, 102613. [Google Scholar] [CrossRef]
- Auld, S.C.; Caridi-Scheible, M.; Blum, J.M.; Robichaux, C.; Kraft, C.; Jacob, J.T.; Jabaley, C.S.; Carpenter, D.; Kaplow, R.; Hernandez-Romieu, A.C.; et al. ICU and ventilator mortality among critically ill adults with coronavirus disease 2019. Crit. Care Med. 2020, 48, e799–e804. [Google Scholar] [CrossRef]
- Avcı, H.; Karabulut, B.; Farasoglu, A.; Boldaz, E.; Evman, M. Relationship between anosmia and hospitalisation in patients with coronavirus disease 2019: An otolaryngological perspective. J. Laryngol. Otol. 2020, 134, 710–716. [Google Scholar] [CrossRef] [PubMed]
- Avruscio, G.; Camporese, G.; Campello, E.; Bernardi, E.; Persona, P.; Passarella, C.; Noventa, F.; Cola, M.; Navalesi, P.; Cattelan, A.; et al. COVID-19 and venous thromboembolism in intensive care or medical ward. Clin. Transl. Sci. 2020, 13, 1108–1114. [Google Scholar] [CrossRef] [PubMed]
- Aw, D.; Woodrow, L.; Ogliari, G.; Harwood, R. Association of frailty with mortality in older inpatients with covid-19: A cohort study. Age Ageing 2020, 49, 915–922. [Google Scholar] [CrossRef] [PubMed]
- Awad, N.; Schiller, D.S.; Fulman, M.; Chak, A. Impact of hydroxychloroquine on disease progression and ICU admissions in patients with SARS-CoV-2 infection. Am. J. Health Syst. Pharm. 2021, 78, 689–696. [Google Scholar] [CrossRef] [PubMed]
- Azar, K.M.J.; Shen, Z.; Romanelli, R.J.; Lockhart, S.H.; Smits, K.; Robinson, S.; Brown, S.; Pressman, A.R. Disparities in outcomes among COVID-19 patients in a large health care system in California. Health Aff. 2020, 39, 1253–1262. [Google Scholar] [CrossRef]
- Azwar, M.K.; Setiati, S.; Rizka, A.; Fitriana, I.; Saldi, S.R.F.; Safitri, E.D. Clinical Profile of Elderly Patients with COVID-19 Hospitalised in Indonesia’s National General Hospital. Acta Med. Indones. 2020, 52, 199–205. [Google Scholar]
- Baggio, J.A.O.; Machado, M.F.; Carmo, R.F.D.; Armstrong, A.D.C.; Santos, A.D.D.; Souza, C.D.F. COVID-19 in Brazil: Spatial risk, social vulnerability, human development, clinical manifestations and predictors of mortality—A retrospective study with data from 59,695 individuals. Epidemiol. Infect. 2021, 149, e100. [Google Scholar] [CrossRef]
- Bailey, L.C.; Razzaghi, H.; Burrows, E.K.; Bunnell, H.T.; Camacho, P.E.F.; Christakis, D.A.; Eckrich, D.; Kitzmiller, M.; Lin, S.M.; Magnusen, B.C.; et al. Assessment of 135,794 pediatric patients tested for severe acute respiratory syndrome coronavirus 2 across the United States. JAMA Pediatrics 2021, 175, 176–184. [Google Scholar] [CrossRef]
- Bannaga, A.S.; Tabuso, M.; Farrugia, A.; Chandrapalan, S.; Somal, K.; Lim, V.K.; Mohamed, S.; Nia, G.J.; Mannath, J.; Wong, J.L.H.; et al. C-reactive protein and albumin association with mortality of hospitalised SARS-CoV-2 patients: A tertiary hospital experience. Clin. Med. 2020, 20, 463–467. [Google Scholar] [CrossRef]
- Baqui, P.; Bica, I.; Marra, V.; Ercole, A.; van der Schaar, M. Ethnic and regional variations in hospital mortality from COVID-19 in Brazil: A cross-sectional observational study. Lancet Glob. Health 2020, 8, e1018–e1026. [Google Scholar] [CrossRef]
- Barbui, T.; Vannucchi, A.M.; Alvarez-Larran, A.; Iurlo, A.; Masciulli, A.; Carobbio, A.; Ghirardi, A.; Ferrari, A.; Rossi, G.; Elli, E.; et al. High mortality rate in COVID-19 patients with myeloproliferative neoplasms after abrupt withdrawal of ruxolitinib. Leukemia 2021, 35, 485–493. [Google Scholar] [CrossRef]
- Barron, E.; Bakhai, C.; Kar, P.; Weaver, A.; Bradley, D.; Ismail, H.; Knighton, P.; Holman, N.; Khunti, K.; Satta, N.; et al. Type 1 and type 2 diabetes and COVID-19 related mortality in England: A whole population study. Diabetes Prim. Care 2020, 22, 60. [Google Scholar]
- Bartoletti, M.; Marconi, L.; Scudeller, L.; Pancaldi, L.; Tedeschi, S.; Giannella, M.; Rinaldi, M.; Bussini, L.; Valentini, I.; Ferravante, A.F.; et al. Efficacy of corticosteroid treatment for hospitalized patients with severe COVID-19: A multicentre study. Clin. Microbiol. Infect. 2021, 27, 105–111. [Google Scholar] [CrossRef]
- Başaran, N.Ç.; Uyaroğlu, O.A.; Dizman, G.T.; Özışık, L.; Şahin, T.K.; Taş, Z.; İnkaya, A.Ç.; Karahan, S.; Alp, Ş.; Alp, A.; et al. Outcome of noncritical COVID-19 patients with early hospitalization and early antiviral treatment outside the ICU. Turk. J. Med. Sci. 2021, 51, 411–420. [Google Scholar] [CrossRef]
- Bauer, A.Z.; Gore, R.; Sama, S.R.; Rosiello, R.; Garber, L.; Sundaresan, D.; McDonald, A.; Arruda, P.; Kriebel, D. Hypertension, medications, and risk of severe COVID-19: A Massachusetts community-based observational study. J. Clin. Hypertens. 2021, 23, 21–27. [Google Scholar] [CrossRef]
- Becerra-Muñoz, V.M.; Núñez-Gil, I.J.; Eid, C.M.; Aguado, M.G.; Romero, R.; Huang, J.; Mulet, A.; Ugo, F.; Rametta, F.; Liebetrau, C.; et al. Clinical profile and predictors of in-hospital mortality among older patients hospitalised for COVID-19. Age Ageing 2021, 50, 326–334. [Google Scholar] [CrossRef]
- Bedock, D.; Lassen, P.B.; Mathian, A.; Moreau, P.; Couffignal, J.; Ciangura, C.; Poitou-Bernert, C.; Jeannin, A.C.; Mosbah, H.; Fadlallah, J.; et al. Prevalence and severity of malnutrition in hospitalized COVID-19 patients. Clin. Nutr. ESPEN 2020, 40, 214–219. [Google Scholar] [CrossRef]
- Belli, L.S.; Fondevila, C.; Cortesi, P.A.; Conti, S.; Karam, V.; Adam, R.; Coilly, A.; Ericzon, B.G.; Loinaz, C.; Cuervas-Mons, V.; et al. Protective role of tacrolimus, deleterious role of age and comorbidities in liver transplant recipients with COVID-19: Results from the ELITA/ELTR multi-center European study. Gastroenterology 2021, 160, 1151–1163.e3. [Google Scholar] [CrossRef]
- Berenguer, J.; Ryan, P.; Rodríguez-Baño, J.; Jarrín, I.; Carratalà, J.; Pachón, J.; Yllescas, M.; Arriba, J.R.; COVID-19@Spain Study Group; Fundación SEIMC-GESIDA; et al. Characteristics and predictors of death among 4035 consecutively hospitalized patients with COVID-19 in Spain. Clin. Microbiol. Infect. 2020, 26, 1525–1536. [Google Scholar] [CrossRef]
- Bernard, A.; Cottenet, J.; Bonniaud, P.; Piroth, L.; Arveux, P.; Tubert-Bitter, P.; Quantin, C.; Marosi, C.; Abraham, D. Comparison of cancer patients to non-cancer patients among COVID-19 inpatients at a national level. Cancers 2021, 13, 1436. [Google Scholar] [CrossRef]
- Bertsimas, D.; Lukin, G.; Mingardi, L.; Nohadani, O.; Orfanoudaki, A.; Stellato, B.; Wiberg, H.; Gonzalez-Garcia, S.; Parra-Calderón, C.L.; Robinson, K.; et al. COVID-19 mortality risk assessment: An international multi-center study. PLoS ONE 2020, 15, e0243262. [Google Scholar] [CrossRef]
- Betti, M.; Bertolotti, M.; Ferrante, D.; Roveta, A.; Pelazza, C.; Giacchero, F.; Penpa, S.; Massarino, C.; Bolgeo, T.; Cassinari, A.; et al. Baseline clinical characteristics and prognostic factors in hospitalized COVID-19 patients aged ≤65 years: A retrospective observational study. PLoS ONE 2021, 16, e0248829. [Google Scholar] [CrossRef]
- Bezzio, C.; Saibeni, S.; Variola, A.; Allocca, M.; Massari, A.; Gerardi, V.; Casini, V.; Ricci, C.; Zingone, F.; Amato, A.; et al. Outcomes of COVID-19 in 79 patients with IBD in Italy: An IG-IBD study. Gut 2020, 69, 1213–1217. [Google Scholar] [CrossRef] [PubMed]
- Bhargava, A.; Fukushima, E.A.; Levine, M.; Zhao, W.; Tanveer, F.; Szpunar, S.M.; Saravolatz, L. Predictors for severe COVID-19 infection. Clin. Infect. Dis. 2020, 71, 1962–1968. [Google Scholar] [CrossRef]
- Bhatt, A.S.; Jering, K.S.; Vaduganathan, M.; Claggett, B.L.; Cunningham, J.W.; Rosenthal, N.; Signorovitch, J.; Thune, J.J.; Vardeny, O.; Solomon, S.D. Clinical outcomes in patients with heart failure hospitalized with COVID-19. JACC Heart Fail. 2021, 9, 65–73. [Google Scholar] [CrossRef] [PubMed]
- Bi, Q.; Wu, Y.; Mei, S.; Ye, C.; Zou, X.; Zhang, Z.; Liu, X.; Wei, L.; Truelove, S.A.; Zhang, T.; et al. Epidemiology and transmission of COVID-19 in 391 cases and 1286 of their close contacts in Shenzhen, China: A retrospective cohort study. Lancet Infect. Dis. 2020, 20, 911–919. [Google Scholar] [CrossRef]
- Bi, X.; Su, Z.; Yan, H.; Du, J.; Wang, J.; Chen, L.; Peng, M.; Chen, S.; Shen, B.; Li, J. Prediction of Severe Illness Due to COVID-19 Based on an Analysis of Initial Fibrinogen to Albumin Ratio and Platelet Count. Platelets 2020, 31, 674–679. [Google Scholar] [CrossRef]
- Bianchetti, A.; Rozzini, R.; Guerini, F.; Boffelli, S.; Ranieri, P.; Minelli, G.; Bianchetti, L.; Trabucchi, M. Clinical presentation of COVID19 in dementia patients. J. Nutr. Health Aging 2020, 24, 560–562. [Google Scholar] [CrossRef]
- Bielza, R.; Sanz, J.; Zambrana, F.; Arias, E.; Malmierca, E.; Portillo, L.; Thuissard, I.J.; Lung, A.; Neira, M.; Moral, M.; et al. Clinical characteristics, frailty, and mortality of residents with COVID-19 in nursing homes of a region of madrid. J. Am. Med. Dir. Assoc. 2021, 22, 245. [Google Scholar] [CrossRef] [PubMed]
- Bode, B.; Garrett, V.; Messler, J.; McFarland, R.; Crowe, J.; Booth, R.; Klonoff, D.C. Glycemic characteristics and clinical outcomes of COVID-19 patients hospitalized in the United States. J. Diabetes Sci. Technol. 2020, 14, 813–821. [Google Scholar] [CrossRef] [PubMed]
- Boero, E.; Rovida, S.; Schreiber, A.; Berchialla, P.; Charrier, L.; Cravino, M.M.; Converso, M.; Gollini, P.; Puppo, M.; Gravina, A.; et al. The COVID-19 worsening score (COWS)—A predictive bedside tool for critical illness. Echocardiography 2021, 38, 207–216. [Google Scholar] [CrossRef]
- Bolouri, H.; Speake, C.; Skibinski, D.; Long, S.A.; Hocking, A.M.; Campbell, D.J.; Hamerman, J.A.; Malhotra, U.; Buckner, J.H.; Benaroya Research Institute COVID-19 Research Team. The COVID-19 immune landscape is dynamically and reversibly correlated with disease severity. J. Clin. Investig. 2021, 131, e143648. [Google Scholar] [CrossRef]
- Bossini, N.; Alberici, F.; Delbarba, E.; Valerio, F.; Manenti, C.; Possenti, S.; Econimo, L.; Maffei, C.; Pola, A.; Terlizzi, V.; et al. Kidney Transplant Patients with SARS-CoV-2 Infection: The Brescia Renal COVID Task Force Experience. Am. J. Transplant. 2020, 20, 3019–3029. [Google Scholar] [CrossRef]
- Botta, M.; Tsonas, A.M.; Pillay, J.; Boers, L.S.; Algera, A.G.; Bos, L.D.J.; Dongelmans, D.A.; Hollmann, M.W.; Horn, J.; Vlaar, A.P.J.; et al. Ventilation management and clinical outcomes in invasively ventilated patients with COVID-19 (PRoVENT-COVID): A national, multicentre, observational cohort study. Lancet Respir. Med. 2021, 9, 139–148. [Google Scholar] [CrossRef]
- Bottio, T.; Bagozzi, L.; Fiocco, A.; Nadali, M.; Caraffa, R.; Bifulco, O.; Ponzoni, M.; Lombardi, C.M.; Metra, M.; Russo, C.F.; et al. COVID-19 in heart transplant recipients: A multicenter analysis of the Northern Italian outbreak. JACC Heart. Fail. 2021, 9, 52–61. [Google Scholar] [CrossRef]
- Brandão Neto, R.A.; Marchini, J.F.; Marino, L.O.; Alencar, J.C.G.; Lazar Neto, F.; Ribeiro, S.; Salvetti, F.V.; Rahhal, H.; Gomez Gomez, L.M.; Bueno, C.G.; et al. Mortality and other outcomes of patients with coronavirus disease pneumonia admitted to the emergency department: A prospective observational Brazilian study. PLoS ONE 2021, 16, e0244532. [Google Scholar]
- Bravi, F.; Flacco, M.E.; Carradori, T.; Volta, C.A.; Cosenza, G.; De Togni, A.; Acuti Martellucci, C.; Parruti, G.; Mantovani, L.; Manzoli, L. Predictors of severe or lethal COVID-19, including angiotensin converting enzyme inhibitors and angiotensin II receptor blockers, in a sample of infected italian citizens. PLoS ONE 2020, 15, e0235248. [Google Scholar] [CrossRef]
- Brenner, E.J.; Ungaro, R.C.; Gearry, R.B.; Kaplan, G.G.; Kissous-Hunt, M.; Lewis, J.D.; Ng, S.C.; Rahier, J.F.; Reinisch, W.; Ruemmele, F.M.; et al. Corticosteroids, but not TNF antagonists, are associated with adverse COVID-19 outcomes in patients with inflammatory bowel diseases: Results from an international registry. Gastroenterology 2020, 159, 481–491.e3. [Google Scholar] [CrossRef]
- Brouns, S.H.; Brüggemann, R.; Linkens, A.E.M.J.H.; Magdelijns, F.J.; Joosten, H.; Heijnen, R.; Ten Cate-Hoek, A.J.; Schols, J.M.G.A.; Ten Cate, H.; Spaetgens, B. Mortality and the use of antithrombotic therapies among nursing home residents with COVID-19. J. Am. Geriatr. Soc. 2020, 68, 1647–1652. [Google Scholar] [CrossRef]
- Brüggemann, R.A.G.; Spaetgens, B.; Gietema, H.A.; Brouns, S.H.A.; Stassen, P.M.; Magdelijns, F.J.; Rennenberg, R.J.; Henry, R.M.A.; Mulder, M.M.G.; van Bussel, B.C.T.; et al. The prevalence of pulmonary embolism in patients with COVID-19 and respiratory decline: A three-setting comparison. Thromb Res. 2020, 196, 486–490. [Google Scholar] [CrossRef]
- Byeon, K.H.; Kim, D.W.; Kim, J.; Choi, B.Y.; Choi, B.; Cho, K.D. Factors Affecting the Survival of Early COVID-19 Patients in South Korea: An Observational Study Based on the Korean National Health Insurance Big Data. Int. J. Infect. Dis. 2021, 105, 588–594. [Google Scholar] [CrossRef]
- Cabello, A.; Zamarro, B.; Nistal, S.; Victor, V.; Hernández, J.; Prieto-Pérez, L.; Carrillo, I.; Álvarez, B.; Fernández-Roblas, R.; Hernández-Segurado, M.; et al. COVID-19 in people living with HIV: A multicenter case-series study. Int. J. Infect. Dis. 2021, 102, 310–315. [Google Scholar] [CrossRef]
- Cabezudo-García, P.; Ciano-Petersen, N.; Mena-Vázquez, N.; Pons-Pons, G.; Castro-Sánchez, M.V.; Serrano-Castro, P. Incidence and case fatality rate of COVID-19 in patients with active epilepsy. Neurology 2020, 95, e1417–e1425. [Google Scholar] [CrossRef]
- Cai, G.; Gao, Y.; Zeng, S.; Yu, Y.; Liu, X.; Liu, D.; Wang, Y.; Yu, R.; Desai, A.; Li, C.; et al. Immunological alternation in COVID-19 patients with cancer and its implications on mortality. Oncoimmunology 2021, 10, 1854424. [Google Scholar] [CrossRef]
- Cai, Q.; Chen, F.; Wang, T.; Luo, F.; Liu, X.; Wu, Q.; He, Q.; Wang, Z.; Liu, Y.; Liu, L.; et al. Obesity and COVID-19 severity in a designated hospital in shenzhen, china. Diabetes Care 2020, 43, 1392–1398. [Google Scholar] [CrossRef]
- Cai, S.H.; Liao, W.; Chen, S.W.; Liu, L.L.; Liu, S.Y.; Zheng, Z.D. Association between obesity and clinical prognosis in patients infected with SARS-CoV-2. Infect. Dis. Poverty 2020, 9, 80. [Google Scholar] [CrossRef]
- Cai, Y.; Shi, S.; Yang, F.; Yi, B.; Chen, X.; Li, J.; Wen, Z. Fasting blood glucose level is a predictor of mortality in patients with COVID-19 independent of diabetes history. Diabetes Res. Clin. Pract. 2020, 169, 108437. [Google Scholar] [CrossRef]
- Caillard, S.; Chavarot, N.; Francois, H.; Matignon, M.; Greze, C.; Kamar, N.; Gatault, P.; Thaunat, O.; Legris, T.; Frimat, L.; et al. Is COVID-19 infection more severe in kidney transplant recipients? Am. J. Transplant. 2021, 21, 1295–1303. [Google Scholar] [CrossRef] [PubMed]
- Caliskan, T.; Saylan, B. Smoking and comorbidities are associated with COVID-19 severity and mortality in 565 patients treated in Turkey: A retrospective observational study. Rev. Assoc. Med. Bras. 2020, 66, 1679–1684. [Google Scholar] [CrossRef] [PubMed]
- Capdevila-Reniu, A.; Pellice, M.; Prieto-González, S.; Ventosa, H.; Ladino, A.; Naval, J.; Rodriguez-Nuñez, O.; César Milisenda, J.; Moreno-Lozano, P.J.; Soriano, A.; et al. Clinical characteristics and outcome of patients aged over 80 years with COVID-19. Medicine 2021, 100, e24750. [Google Scholar] [CrossRef] [PubMed]
- Cariou, B.; Hadjadj, S.; Wargny, M.; Pichelin, M.; Al-Salameh, A.; Allix, I.; Amadou, C.; Arnault, G.; Baudoux, F.; Bauduceau, B.; et al. Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: The CORONADO study. Diabetologia 2020, 63, 1500–1515. [Google Scholar] [CrossRef]
- Carubbi, F.; Salvati, L.; Alunno, A.; Maggi, F.; Borghi, E.; Mariani, R.; Mai, F.; Paoloni, M.; Ferri, C.; Desideri, G.; et al. Ferritin is associated with the severity of lung involvement but not with worse prognosis in patients with COVID-19: Data from two italian COVID-19 units. Sci. Rep. 2021, 11, 4863. [Google Scholar] [CrossRef]
- Catteau, L.; Dauby, N.; Montourcy, M.; Bottieau, E.; Hautekiet, J.; Goetghebeur, E.; van Ierssel, S.; Duysburgh, E.; Van Oyen, H.; Wyndham-Thomas, C.; et al. Low-dose hydroxychloroquine therapy and mortality in hospitalised patients with COVID-19: A nationwide observational study of 8075 participants. Int. J. Antimicrob. Agents 2020, 56, 106144. [Google Scholar] [CrossRef]
- Cattelan, A.M.; Di Meco, E.; Trevenzoli, M.; Frater, A.; Ferrari, A.; Villano, M.; Gomiero, F.; Carretta, G.; Sasset, L. Clinical characteristics and laboratory biomarkers changes in COVID-19 patients requiring or not intensive or sub-intensive care: A comparative study. BMC Infect. Dis. 2020, 20, 934. [Google Scholar] [CrossRef]
- CDC COVID-19 Response Team. Preliminary Estimates of the Prevalence of Selected Underlying Health Conditions among Patients with Coronavirus Disease 2019—United States, February 12–March 28, 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 382–386. [Google Scholar] [CrossRef]
- Cekerevac, I.; Turnic, T.N.; Draginic, N.; Andjic, M.; Zivkovic, V.; Simovic, S.; Susa, R.; Novkovic, L.; Mijailovic, Z.; Andjelkovic, M.; et al. Predicting severity and intrahospital mortality in COVID-19: The place and role of oxidative stress. Oxid. Med. Cell. Longev. 2021, 2021, 6615787. [Google Scholar] [CrossRef]
- Cen, Y.; Chen, X.; Shen, Y.; Zhang, X.H.; Lei, Y.; Xu, C.; Jiang, W.R.; Xu, H.T.; Chen, Y.; Zhu, J.; et al. Risk factors for disease progression in patients with mild to moderate coronavirus disease 2019—A multi-centre observational study. Clin. Microbiol. Infect. 2020, 26, 1242–1247. [Google Scholar] [CrossRef]
- Chand, S.; Kapoor, S.; Orsi, D.; Fazzari, M.J.; Tanner, T.G.; Umeh, G.C.; Islam, M.; Dicpinigaitis, P.V. COVID-19-associated critical Illness—Report of the first 300 patients admitted to intensive care units at a new york city medical center. J. Intensive Care Med. 2020, 35, 963–970. [Google Scholar] [CrossRef]
- Chang, M.C.; Hwang, J.M.; Jeon, J.H.; Kwak, S.G.; Park, D.; Moon, J.S. Fasting plasma glucose level independently predicts the mortality of patients with coronavirus disease 2019 infection: A multicenter, retrospective cohort study. Endocrinol. Metab. 2020, 35, 595–601. [Google Scholar] [CrossRef]
- CDC COVID-19 Responese Team. Characteristics of Health Care Personnel with COVID-19—United States, February 12–April 9, 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 477–481. [Google Scholar] [CrossRef] [Green Version]
- Chaudhry, F.; Bulka, H.; Rathnam, A.S.; Said, O.M.; Lin, J.; Lorigan, H.; Bernitsas, E.; Rube, J.; Korzeniewski, S.J.; Memon, A.B.; et al. COVID-19 in multiple sclerosis patients and risk factors for severe infection. J. Neurol. Sci. 2020, 418, 117147. [Google Scholar] [CrossRef]
- Chen, C.; Wang, F.; Chen, P.; Jiang, J.; Cui, G.; Zhou, N.; Moroni, F.; Moslehi, J.J.; Ammirati, E.; Wang, D.W. Mortality and pre-hospitalization use of renin-angiotensin system inhibitors in hypertensive COVID-19 patients. J. Am. Heart Assoc. 2020, 9, e017736. [Google Scholar] [CrossRef]
- Chen, J.; Bai, H.; Liu, J.; Chen, G.; Liao, Q.; Yang, J.; Wu, P.; Wei, J.; Ma, D.; Chen, G.; et al. Distinct clinical characteristics and risk factors for mortality in female inpatients with coronavirus disease 2019 (COVID-19): A sex-stratified, large-scale cohort study in Wuhan, China. Clin. Infect. Dis. 2020, 71, 3188–3195. [Google Scholar] [CrossRef]
- Chen, J.; Qi, T.; Liu, L.; Ling, Y.; Qian, Z.; Li, T.; Li, F.; Xu, Q.; Zhang, Y.; Xu, S.; et al. Clinical progression of patients with COVID-19 in Shanghai, China. J. Infect. 2020, 80, e1–e6. [Google Scholar] [CrossRef]
- Chen, L.; Liu, S.; Tian, J.; Pan, H.; Liu, Y.; Hu, J.; Wang, M.; Hou, X. Disease progression patterns and risk factors associated with mortality in deceased patients with COVID-19 in Hubei province, China. Immun. Inflamm. Dis. 2020, 8, 584–594. [Google Scholar] [CrossRef]
- Chen, Q.; Zheng, Z.; Zhang, C.; Zhang, X.; Wu, H.; Wang, J.; Wang, S.; Zheng, C. Clinical characteristics of 145 patients with corona virus disease 2019 (COVID-19) in Taizhou, Zhejiang, China. Infection 2020, 48, 543–551. [Google Scholar] [CrossRef]
- Chen, R.; Liang, W.; Jiang, M. Risk factors of fatal outcome in hospitalized subjects with coronavirus disease 2019 from a nationwide analysis in China. Chest 2020, 158, 97–105. [Google Scholar] [CrossRef]
- Chen, T.; Dai, Z.; Mo, P.; Li, X.; Ma, Z.; Song, S.; Chen, X.; Luo, M.; Liang, K.; Gao, S.; et al. Clinical characteristics and outcomes of older patients with coronavirus disease 2019 (COVID-19) in Wuhan, China: A single-centered, retrospective study. J. Gerontol. A Biol. Sci. Med. Sci. 2020, 75, 1788–1795. [Google Scholar] [CrossRef]
- Chen, Y.; Yang, D.; Cheng, B.; Chen, J.; Peng, A.; Yang, C.; Liu, C.; Xiong, M.; Deng, A.; Zhang, Y.; et al. Clinical characteristics and outcomes of patients with diabetes and COVID-19 in association with glucose-lowering medication. Diabetes Care 2020, 43, 1399–1407. [Google Scholar] [CrossRef]
- Chen, Z.; Zhang, F.; Hu, W.; Chen, Q.; Li, C.; Wu, L.; Zhang, Z.; Li, B.; Ye, Q.; Mei, J.; et al. Laboratory markers associated with COVID-19 progression in patients with or without comorbidity: A retrospective study. J. Clin. Lab. Anal. 2021, 35, e23644. [Google Scholar] [CrossRef]
- Cheng, S.; Wu, D.; Li, J.; Zou, Y.; Wan, Y.; Shen, L.; Zhu, L.; Shi, M.; Hou, L.; Xu, T.; et al. Risk factors for the critical illness in SARS-CoV-2 infection: A multicenter retrospective cohort study. Respir. Res. 2020, 21, 277. [Google Scholar] [CrossRef] [PubMed]
- Chilimuri, S.; Sun, H.; Alemam, A.; Mantri, N.; Shehi, E.; Tejada, J.; Yugay, A.; Nayudu, S.K. Predictors of mortality in adults admitted with COVID-19: Retrospective cohort study from New York City. West J. Emerg. Med. 2020, 21, 779–784. [Google Scholar] [CrossRef] [PubMed]
- Choron, R.L.; Butts, C.A.; Bargoud, C.; Krumrei, N.J.; Teichman, A.L.; Schroeder, M.E.; Bover Manderski, M.T.; Cai, J.; Song, C.; Rodricks, M.B.; et al. Fever in the ICU: A predictor of mortality in mechanically ventilated COVID-19 patients. J. Intensive Care Med. 2021, 36, 484–493. [Google Scholar] [CrossRef] [PubMed]
- Choudhuri, J.; Carter, J.; Nelson, R.; Skalina, K.; Osterbur-Badhey, M.; Johnston, A.; Goldstein, D.; Paroder, M.; Szymanski, J. SARS-CoV-2 PCR cycle threshold at hospital admission associated with patient mortality. PLoS ONE 2020, 15, e0244777. [Google Scholar] [CrossRef]
- Ciceri, F.; Castagna, A.; Rovere-Querini, P.; De Cobelli, F.; Ruggeri, A.; Galli, L.; Conte, C.; De Lorenzo, R.; Poli, A.; Ambrosio, A.; et al. Early predictors of clinical outcomes of COVID-19 outbreak in Milan, Italy. Clin. Immunol. 2020, 217, 108509. [Google Scholar] [CrossRef]
- Cillóniz, C.; Torres, A.; Garcia-Vidal, C.; Moreno-Garcia, E.; Amaro, R.; Soler, N.; Marcos, M.A.; Rico, V.; Gabarrús, A.; Nicolás, J.M.; et al. The value of C-reactive protein-to-lymphocyte ratio in predicting the severity of SARS-CoV-2 pneumonia. Arch. Bronconeumol. 2021, 57, 79–82. [Google Scholar] [CrossRef]
- Çınar, T.; Hayıroğlu, M.İ.; Çiçek, V.; Kılıç, Ş.; Asal, S.Ü.; Yavuz, S.; Selçuk, M.; Yalçınkaya, E.; Keser, N.; Orhan, A.L. Is prognostic nutritional index a predictive marker for estimating all-cause in-hospital mortality in COVID-19 patients with cardiovascular risk factors? Heart Lung. 2021, 50, 307–312. [Google Scholar] [CrossRef]
- Cizmecioglu, A.; Akay Cizmecioglu, H.; Goktepe, M.H.; Emsen, A.; Korkmaz, C.; Esenkaya Tasbent, F.; Colkesen, F.; Artac, H. Apoptosis-induced T-cell lymphopenia is related to COVID-19 severity. J. Med. Virol. 2021, 93, 2867–2874. [Google Scholar] [CrossRef]
- Colaneri, M.; Sacchi, P.; Zuccaro, V.; Biscarini, S.; Sachs, M.; Roda, S.; Pieri, T.C.; Valsecchi, P.; Piralla, A.; Seminari, E.; et al. Clinical characteristics of coronavirus disease (COVID-19) early findings from a teaching hospital in Pavia, North Italy, 21 to 28 February 2020. Eurosurveillance 2020, 25, 2000460. [Google Scholar] [CrossRef] [Green Version]
- Geriatric Medicine Research Collaborative; Covid Collaborative; Welch, C. Age and frailty are independently associated with increased COVID-19 mortality and increased care needs in survivors: Results of an international multi-centre study. Age Ageing 2021, 50, 617–630. [Google Scholar]
- COVID-ICU Group on behalf of the REVA Network and the COVID-ICU Investigators. Clinical characteristics and day-90 outcomes of 4244 critically ill adults with COVID-19: A prospective cohort study. Intensive Care Med. 2021, 47, 60–73. [Google Scholar] [CrossRef]
- Covino, M.; De Matteis, G.; Burzo, M.L.; Santoro, M.; Fuorlo, M.; Sabia, L.; Sandroni, C.; Gasbarrini, A.; Franceschi, F.; Gambassi, G. Angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers and prognosis of hypertensive patients hospitalised with COVID-19. Intern. Med. J. 2020, 50, 1483–1491. [Google Scholar] [CrossRef]
- Covino, M.; De Matteis, G.; Burzo, M.L.; Russo, A.; Forte, E.; Carnicelli, A.; Piccioni, A.; Simeoni, B.; Gasbarrini, A.; Franceschi, F.; et al. Predicting in-hospital mortality in COVID-19 older patients with specifically developed scores. J. Am. Geriatr. Soc. 2021, 69, 37–43. [Google Scholar] [CrossRef]
- Covino, M.; De Matteis, G.; Santoro, M.; Sabia, L.; Simeoni, B.; Candelli, M.; Ojetti, V.; Franceschi, F. Clinical characteristics and prognostic factors in COVID-19 patients aged ≥80 years. Geriatr. Gerontol. Int. 2020, 20, 704–708. [Google Scholar] [CrossRef]
- Covino, M.; Sandroni, C.; Santoro, M.; Sabia, L.; Simeoni, B.; Bocci, M.G.; Ojetti, V.; Candelli, M.; Antonelli, M.; Gasbarrini, A.; et al. Predicting intensive care unit admission and death for COVID-19 patients in the emergency department using early warning scores. Resuscitation 2020, 156, 84–91. [Google Scholar] [CrossRef]
- Cummings, M.J.; Baldwin, M.R.; Abrams, D.; Jacobson, S.D.; Meyer, B.J.; Balough, E.M.; Aaron, J.G.; Claassen, J.; Rabbani, L.E.; Hastie, J.; et al. Epidemiology, clinical course, and outcomes of critically ill adults with COVID-19 in New York City: A prospective cohort study. Lancet 2020, 395, 1763–1770. [Google Scholar] [CrossRef]
- Dagher, L.; Shi, H.; Zhao, Y.; Wetherbie, A.; Johnsen, E.; Sangani, D.; Nedunchezhian, S.; Brown, M.; Miller, P.; Denson, J.; et al. New-onset atrial arrhythmias associated with mortality in black and white patients hospitalized with COVID-19. Pacing Clin. Electrophysiol. 2021, 44, 856–864. [Google Scholar] [CrossRef]
- Dai, S.-P.; Zhao, X.; Wu, J. Effects of comorbidities on the elderly patients with COVID-19: Clinical characteristics of elderly patients infected with COVID-19 from Sichuan, China. J. Nutr. Health Aging 2021, 25, 18–24. [Google Scholar] [CrossRef]
- De Smet, D.; De Smet, K.; Herroelen, P.; Gryspeerdt, S.; Martens, G.A. Serum 25(OH)D level on hospital admission associated with COVID-19 stage and mortality. Am. J. Clin. Pathol. 2021, 155, 381–388. [Google Scholar] [CrossRef]
- De Smet, R.; Mellaerts, B.; Vandewinckele, H.; Lybeert, P.; Frans, E.; Ombelet, S.; Lemahieu, W.; Symons, R.; Ho, E.; Frans, J.; et al. Frailty and mortality in hospitalized older adults with COVID-19: Retrospective observational study. J. Am. Med. Dir. Assoc. 2020, 21, 928. [Google Scholar] [CrossRef]
- De Souza, C.D.F.; de Arruda Magalhães, A.J.; Lima, A.J.P.D.; Nunes, D.N.; de Fátima Machado Soares, É.; de Castro Silva, L.; Santos, L.G.; dos Santos Cardoso, V.I.; Nobre, Y.V.S.; do Carmo, R.F. Clinical manifestations and factors associated with mortality from COVID-19 in older adults: Retrospective population-based study with 9807 older brazilian COVID-19 patients. Geriatr. Gerontol. Int. 2020, 20, 1177–1181. [Google Scholar] [CrossRef]
- De Souza, R.; Mhatre, S.; Qayyumi, B.; Chitkara, G.; Madke, T.; Joshi, M.; Bharmal, R.; Asgaonkar, D.S.; Lakhani, P.; Gupta, S.; et al. Clinical course and outcome of patients with COVID-19 in Mumbai City: An observational study. BMJ Open 2021, 11, e042943. [Google Scholar] [CrossRef]
- Deeb, A.; Khawaja, K.; Sakrani, N.; AlAkhras, A.; Al Mesabi, A.; Trehan, R.; Kumar, P.C.; Babiker, Z.; Nagelkerke, N.; Fru-Nsutebu, E. Impact of ethnicity and underlying comorbidity on COVID-19 inhospital mortality: An observational study in Abu Dhabi, UAE. Biomed. Res. Int. 2021, 2021, 6695707. [Google Scholar] [CrossRef]
- Deng, G.; Yin, M.; Chen, X.; Zeng, F. Clinical determinants for fatality of 44,672 patients with COVID-19. Crit Care 2020, 24, 179. [Google Scholar] [CrossRef]
- Deng, Q.; Hu, B.; Zhang, Y.; Wang, H.; Zhou, X.; Hu, W.; Cheng, Y.; Yan, J.; Ping, H.; Zhou, Q. Suspected myocardial injury in patients with COVID-19: Evidence from front-line clinical observation in Wuhan, China. Int. J. Cardiol. 2020, 311, 116–121. [Google Scholar] [CrossRef]
- Derikx, L.A.A.P.; Lantinga, M.A.; de Jong, D.J.; van Dop, W.A.; Creemers, R.H.; Römkens, T.E.H.; Jansen, J.M.; Mahmmod, N.; West, R.L.; Tan, A.C.I.T.L.; et al. Clinical outcomes of covid-19 in patients with inflammatory bowel disease: A nationwide cohort study. J. Crohn’s Colitis 2021, 15, 529–539. [Google Scholar] [CrossRef]
- Di Castelnuovo, A.; Bonaccio, M.; Costanzo, S.; Gialluisi, A.; Antinori, A.; Berselli, N.; Blandi, L.; Bruno, R.; Cauda, R.; Guaraldi, G.; et al. Common cardiovascular risk factors and in-hospital mortality in 3894 patients with COVID-19: Survival analysis and machine learning-based findings from the multicentre italian CORIST study. Nutr. Metab. Cardiovasc. Dis. 2020, 30, 1899–1913. [Google Scholar] [CrossRef]
- Di Cosimo, S.; Tagliaferri, B.; Generali, D.; Giudici, F.; Agustoni, F.; Bernardo, A.; Borgonovo, K.; Farina, G.; Luchena, G.; Luciani, A.; et al. Baseline characteristics and outcomes of cancer patients infected with SARS-CoV-2 in the Lombardy region, Italy (AIOM-L CORONA): A multicenter, observational, ambispective, cohort study. Cancers 2021, 13, 1324. [Google Scholar] [CrossRef]
- Du, H.; Pan, X.; Liu, N.; Chen, J.; Chen, X.; Werring, D.J.; Ambler, G.; Li, X.; Chen, R.; Zhang, Y.; et al. The effect of vascular risk factor burden on the severity of COVID-19 illness, a retrospective cohort study. Respir. Res. 2020, 21, 241. [Google Scholar] [CrossRef]
- Du, R.H.; Liang, L.R.; Yang, C.Q.; Wang, W.; Cao, T.Z.; Li, M.; Guo, G.Y.; Du, J.; Zheng, C.L.; Zhu, Q.; et al. Predictors of Mortality for Patients with COVID-19 Pneumonia Caused by SARS-CoV-2: A Prospective Cohort Study. Eur. Respir. J. 2020, 55, 2000524. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Du, R.H.; Liu, L.M.; Yin, W.; Wang, W.; Guan, L.L.; Yuan, M.L.; Li, Y.L.; Hu, Y.; Li, X.Y.; Sun, B.; et al. Hospitalization and Critical Care of 109 Decedents with COVID-19 Pneumonia in Wuhan, China. Ann. Am. Thorac. Soc. 2020, 17, 839–846. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Duan, J.; Wang, X.; Chi, J.; Chen, H.; Bai, L.; Hu, Q.; Han, X.; Hu, W.; Zhu, L.; Wang, X.; et al. Correlation between the variables collected at admission and progression to severe cases during hospitalization among patients with COVID-19 in Chongqing. J. Med. Virol. 2020, 92, 2616–2622. [Google Scholar] [CrossRef] [PubMed]
- Duarte, M.B.O.; Leal, F.; Argenton, J.L.P.; Carvalheira, J.B.C. Outcomes of COVID-19 patients under cytotoxic cancer chemotherapy in Brazil. Cancers 2020, 12, 3490. [Google Scholar] [CrossRef] [PubMed]
- Duclos, G.; Bazalguette, F.; Allaouchiche, B.; Mohammedi, N.; Lopez, A.; Gazon, M.; Besch, G.; Bouvet, L.; Muller, L.; Mathon, G.; et al. Can thoracic ultrasound on admission predict the outcome of critically ill patients with SARS-CoV-2? A French multi-centric ancillary retrospective study. Adv. Ther. 2021, 38, 2599–2612. [Google Scholar] [CrossRef]
- Dudley, J.P.; Lee, N.T. Disparities in Age-Specific Morbidity and Mortality from SARS-CoV-2 in China and the Republic of Korea. Clin. Infect. Dis. 2020, 71, 863–865. [Google Scholar] [CrossRef] [Green Version]
- Elamari, S.; Motaib, I.; Zbiri, S.; Elaidaoui, K.; Chadli, A.; Elkettani, C. Characteristics and outcomes of diabetic patients infected by the SARS-CoV-2. Pan Afr. Med. J. 2020, 37, 32. [Google Scholar] [CrossRef]
- Elhadi, M.; Alsoufi, A.; Abusalama, A.; Alkaseek, A.; Abdeewi, S.; Yahya, M.; Mohammed, A.; Abdelkabir, M.; Huwaysh, M.; Amkhatirah, E.; et al. Epidemiology, outcomes, and utilization of intensive care unit resources for critically ill COVID-19 patients in Libya: A prospective multi-center cohort study. PLoS ONE 2021, 16, e0251085. [Google Scholar] [CrossRef]
- Escobar, A.L.; Rodriguez, T.D.M.; Monteiro, J.C. Lethality and characteristics of deaths due to COVID-19 in Rondônia: An observational study. Epidemiol. Serviços Saúde 2020, 30, e2020763. [Google Scholar] [CrossRef]
- Escosteguy, C.C.; Eleuterio, T.A.; Pereira, A.G.L.; Marques, M.R.V.E.; Brandão, A.D.; Batista, J.P.M. COVID-19: A cross-sectional study of suspected cases admitted to a federal hospital in Rio de Janeiro, Brazil, and factors associated with hospital death. Epidemiol. Serviços Saúde 2020, 30, e2020750. [Google Scholar] [CrossRef]
- Etienne, N.; Karmochkine, M.; Slama, L.; Pavie, J.; Batisse, D.; Usubillaga, R.; Letembet, V.A.; Brazille, P.; Canouï, E.; Slama, D.; et al. HIV infection and COVID-19: Risk factors for severe disease. AIDS 2020, 34, 1771–1774. [Google Scholar] [CrossRef]
- Fadini, G.P.; Morieri, M.L.; Boscari, F.; Fioretto, P.; Maran, A.; Busetto, L.; Bonora, B.M.; Selmin, E.; Arcidiacono, G.; Pinelli, S.; et al. Newly-diagnosed diabetes and admission hyperglycemia predict COVID-19 severity by aggravating respiratory deterioration. Diabetes Res. Clin. Pract. 2020, 168, 108374. [Google Scholar] [CrossRef]
- Falcone, M.; Tiseo, G.; Barbieri, G.; Galfo, V.; Russo, A.; Virdis, A.; Forfori, F.; Corradi, F.; Guarracino, F.; Carrozzi, L. Role of low-molecular-weight heparin in hospitalized patients with severe acute respiratory syndrome coronavirus 2 pneumonia: A prospective observational study. Open Forum Infect. Dis. 2020, 7, ofaa563. [Google Scholar] [CrossRef]
- Favà, A.; Cucchiari, D.; Montero, N.; Toapanta, N.; Centellas, F.J.; Vila-Santandreu, A.; Coloma, A.; Meneghini, M.; Manonelles, A.; Sellarés, J.; et al. Clinical characteristics and risk factors for severe COVID-19 in hospitalized kidney transplant recipients: A multicentric cohort study. Am. J. Transplant. 2020, 20, 3030–3041. [Google Scholar] [CrossRef]
- Feng, Y.; Ling, Y.; Bai, T.; Xie, Y.; Huang, J.; Li, J.; Xiong, W.; Yang, D.; Chen, R.; Lu, F.; et al. COVID-19 with Different Severity: A Multi-center Study of Clinical Features. Am. J. Respir. Crit. Care Med. 2020, 201, 1380–1388. [Google Scholar] [CrossRef]
- Ferguson, J.; Rosser, J.I.; Quintero, O.; Scott, J.; Subramanian, A.; Gumma, M.; Rogers, A.; Kappagoda, S. Characteristics and outcomes of coronavirus disease patients under nonsurge conditions, Northern California, USA, March–April 2020. Emerg. Infect. Dis. 2020, 26, 1679–1685. [Google Scholar] [CrossRef]
- Fernandes, D.M.; Oliveira, C.R.; Guerguis, S.; Eisenberg, R.; Choi, J.; Kim, M.; Abdelhemid, A.; Agha, R.; Agarwal, S.; Aschner, J.L.; et al. Severe acute respiratory syndrome coronavirus 2 clinical syndromes and predictors of disease severity in hospitalized children and youth. J. Pediatr. 2021, 230, 23–31.e10. [Google Scholar] [CrossRef]
- Ferrando, C.; Mellado-Artigas, R.; Gea, A.; Arruti, E.; Aldecoa, C.; Bordell, A.; Adalia, R.; Zattera, L.; Ramasco, F.; Monedero, P.; et al. Patient characteristics, clinical course and factors associated to ICU mortality in critically ill patients infected with SARS-CoV-2 in Spain: A prospective, cohort, multicentre study. Rev. Esp. Anestesiol. Reanim. 2020, 67, 425–437. [Google Scholar] [CrossRef]
- Ferrando-Vivas, P.; Doidge, J.; Thomas, K.; Gould, D.W.; Mouncey, P.; Shankar-Hari, M.; Young, J.D.; Rowan, K.M.; Harrison, D.A.; ICNARC COVID-19 Team 2021. Prognostic factors for 30-day mortality in critically ill patients with coronavirus disease 2019: An observational cohort study. Crit. Care Med. 2021, 49, 102–111. [Google Scholar] [CrossRef]
- Ferrari, B.L.; Ferreira, C.G.; Menezes, M.; De Marchi, P.; Canedo, J.; Melo, A.C.; Jácome, A.A.; Reinert, T.; Paes, R.D.; Sodré, B.; et al. Determinants of COVID-19 mortality in patients with cancer from a community oncology practice in Brazil. JCO Glob. Oncol. 2021, 7, 46–55. [Google Scholar] [CrossRef]
- Fox, T.; Ruddiman, K.; Lo, K.B.; Peterson, E.; DeJoy, R., 3rd; Salacup, G.; Pelayo, J.; Bhargav, R.; Gul, F.; Albano, J.; et al. The relationship between diabetes and clinical outcomes in COVID-19: A single-center retrospective analysis. Acta Diabetol. 2021, 58, 33–38. [Google Scholar] [CrossRef]
- Foy, B.H.; Carlson, J.C.T.; Reinertsen, E.; Padros, I.; Valls, R.; Pallares Lopez, R.; Palanques-Tost, E.; Mow, C.; Westover, M.B.; Aguirre, A.D.; et al. Association of red blood cell distribution width with mortality risk in hospitalized adults with SARS-CoV-2 infection. JAMA Netw. Open. 2020, 3, e2022058. [Google Scholar] [CrossRef]
- Freites Nuñez, D.D.; Leon, L.; Mucientes, A.; Rodriguez-Rodriguez, L.; Urgelles, J.F.; Madrid García, A.; Colomer, J.I.; Jover, J.A.; Fernandez-Gutierrez, B.; Abasolo, L.; et al. Risk factors for hospital admissions related to COVID-19 in patients with autoimmune inflammatory rheumatic diseases. Ann. Rheum. Dis. 2020, 79, 1393–1399. [Google Scholar] [CrossRef]
- Frontera, J.A.; Valdes, E.; Huang, J.; Lewis, A.; Lord, A.S.; Zhou, T.; Kahn, D.E.; Melmed, K.; Czeisler, B.M.; Yaghi, S.; et al. Prevalence and impact of hyponatremia in patients with coronavirus disease 2019 in New York City. Crit. Care Med. 2020, 48, e1211–e1217. [Google Scholar] [CrossRef]
- Fu, J.; Kong, J.; Wang, W.; Wu, M.; Yao, L.; Wang, Z.; Jin, J.; Wu, D.; Yu, X. The clinical implication of dynamic neutrophil to lymphocyte ratio and D-dimer in COVID-19: A retrospective study in Suzhou, China. Thromb. Res. 2020, 192, 3–8. [Google Scholar] [CrossRef]
- Galiero, R.; Pafundi, P.C.; Simeon, V.; Rinaldi, L.; Perrella, A.; Vetrano, E.; Caturano, A.; Alfano, M.; Beccia, D.; Nevola, R.; et al. Impact of chronic liver disease upon admission on COVID-19 in-hospital mortality: Findings from COVOCA study. PLoS ONE 2020, 15, e0243700. [Google Scholar] [CrossRef]
- Gao, C.; Cai, Y.; Zhang, K.; Zhou, L.; Zhang, Y.; Zhang, X.; Li, Q.; Li, W.; Yang, S.; Zhao, X.; et al. Association of hypertension and antihypertensive treatment with COVID-19 mortality: A retrospective observational study. Eur. Heart J. 2020, 41, 2058–2066. [Google Scholar] [CrossRef]
- Gao, J.; Huang, X.; Gu, H.; Lou, L.; Xu, Z. Predictive criteria of severe cases in COVID-19 patients of early stage: A retrospective observational study. J. Clin. Lab Anal. 2020, 34, e23562. [Google Scholar] [CrossRef]
- Genet, B.; Vidal, J.S.; Cohen, A.; Boully, C.; Beunardeau, M.; Marine Harlé, L.; Gonçalves, A.; Boudali, Y.; Hernandorena, I.; Bailly, H.; et al. COVID-19 in-hospital mortality and use of renin-angiotensin system blockers in geriatrics patients. J. Am. Med. Dir. Assoc. 2020, 21, 1539–1545. [Google Scholar] [CrossRef]
- Ghaffari, M.; Ansari, H.; Beladimoghadam, N.; Aghamiri, S.H.; Haghighi, M.; Nabavi, M.; Mansouri, B.; Mehrpour, M.; Assarzadegan, F.; Hesami, O.; et al. Neurological features and outcome in COVID-19: Dementia can predict severe disease. J. Neurovirol. 2021, 27, 86–93. [Google Scholar] [CrossRef]
- Giannoglou, D.; Meimeti, E.; Provatopoulou, X.; Stathopoulos, K.; Roukas, I.; Galanis, P. Predictors of mortality in hospitalized COVID-19 patients in Athens, Greece. Int. J. Caring Sci. 2020, 13, 1689–1698. [Google Scholar]
- Goicoechea, M.; Sánchez Cámara, L.A.; Macías, N.; Muñoz de Morales, A.; Rojas, Á.; Bascuñana, A.; Arroyo, D.; Vega, A.; Abad, S.; Verde, E.; et al. COVID-19: Clinical course and outcomes of 36 hemodialysis patients in Spain. Kidney Int. 2020, 98, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Gomez, J.M.D.; Du-Fay-de-Lavallaz, J.M.; Fugar, S.; Sarau, A.; Simmons, J.A.; Clark, B.; Sanghani, R.M.; Aggarwal, N.T.; Williams, K.A.; Doukky, R.; et al. Sex differences in COVID-19 hospitalization and mortality. J. Women’s Health 2021, 30, 646–653. [Google Scholar] [CrossRef] [PubMed]
- Gong, J.; Ou, J.; Qiu, X.; Jie, Y.; Chen, Y.; Yuan, L.; Cao, J.; Tan, M.; Xu, W.; Zheng, F.; et al. A Tool to Early Predict Severe Corona Virus Disease 2019 (COVID-19): A Multicenter Study using the Risk Nomogram in Wuhan and Guangdong, China. Clin. Infect. Dis. 2020, 71, 833–840. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- González-Gancedo, J.; Morales-Cané, I.; Rodríguez-Muñoz, P.M.; Hidalgo-Lopezosa, P.; Del Rocío Valverde-León, M.; Fernández-Martínez, M.E.; Fabbian, F.; Rodríguez-Borrego, M.A.; López-Soto, P.J. Mortality and critical conditions in COVID-19 patients at private hospitals: Weekend effect? Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 3377–3385. [Google Scholar] [PubMed]
- Goodall, J.W.; Reed, T.A.N.; Ardissino, M.; Bassett, P.; Whittington, A.M.; Cohen, D.L.; Vaid, N. Risk factors for severe disease in patients admitted with COVID-19 to a hospital in London, England: A retrospective cohort study. Epidemiol. Infect. 2020, 148, e251. [Google Scholar] [CrossRef]
- Grasselli, G.; Greco, M.; Zanella, A.; Albano, G.; Antonelli, M.; Bellani, G.; Bonanomi, E.; Cabrini, L.; Carlesso, E.; Castelli, G.; et al. Risk factors associated with mortality among patients with COVID-19 in intensive care units in Lombardy, Italy. JAMA Intern. Med. 2020, 180, 1345–1355. [Google Scholar] [CrossRef]
- Grasselli, G.; Zangrillo, A.; Zanella, A.; Antonelli, M.; Cabrini, L.; Castelli, A.; Cereda, D.; Coluccello, A.; Foti, G.; Fumagalli, R.; et al. Baseline Characteristics and Outcomes of 1591 Patients Infected With SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA 2020, 323, 1574–1581. [Google Scholar] [CrossRef] [Green Version]
- Gu, T.; Mack, J.A.; Salvatore, M.; Sankar, S.P.; Valley, T.S.; Singh, K.; Nallamothu, B.K.; Kheterpal, S.; Lisabeth, L.; Fritsche, L.G.; et al. Characteristics Associated with Racial/Ethnic Disparities in COVID-19 Outcomes in an Academic Health Care System. JAMA Netw. Open 2020, 3, e2025197. [Google Scholar] [CrossRef]
- Guan, W.J.; Liang, W.H.; Zhao, Y.; Liang, H.R.; Chen, Z.S.; Li, Y.M.; Liu, X.Q.; Chen, R.C.; Tang, C.L.; Wang, T.; et al. Comorbidity and its impact on 1590 patients with Covid-19 in China: A Nationwide Analysis. Eur. Respir. J. 2020, 55, 2000547. [Google Scholar] [CrossRef] [Green Version]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.C.; et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef]
- Guarneri, V.; Bassan, F.; Zagonel, V.; Milella, M.; Zaninelli, M.; Cattelan, A.M.; Vianello, A.; Gori, S.; Aprile, G.; Azzarello, G.; et al. Epidemiology and clinical course of severe acute respiratory syndrome coronavirus 2 infection in cancer patients in the veneto oncology network: The rete oncologica veneta COVID-19 study. Eur. J. Cancer 2021, 147, 120–127. [Google Scholar] [CrossRef]
- Guo, W.; Li, M.; Dong, Y.; Zhou, H.; Zhang, Z.; Tian, C.; Qin, R.; Wang, H.; Shen, Y.; Du, K.; et al. Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab. Res. Rev. 2020, 36, e3319. [Google Scholar] [CrossRef] [Green Version]
- Guo, Y.; Liu, X.; Deng, M.; Liu, P.; Li, F.; Xie, N.; Pang, Y.; Zhang, X.; Luo, W.; Peng, Y.; et al. Epidemiology of COVID-19 in older persons, wuhan, china. Age Ageing 2020, 49, 706–712. [Google Scholar] [CrossRef]
- Gupta, S.; Hayek, S.S.; Wang, W.; Chan, L.; Mathews, K.S.; Melamed, M.L.; Brenner, S.K.; Leonberg-Yoo, A.; Schenck, E.J.; Radbel, J.; et al. Factors associated with death in critically ill patients with coronavirus disease 2019 in the US. JAMA Intern. Med. 2020, 180, 1436–1447. [Google Scholar] [CrossRef]
- Haase, N.; Plovsing, R.; Christensen, S.; Poulsen, L.M.; Brøchner, A.C.; Rasmussen, B.S.; Helleberg, M.; Jensen, J.U.S.; Andersen, L.P.K.; Siegel, H.; et al. Characteristics, interventions, and longer term outcomes of COVID-19 ICU patients in Denmark-A nationwide, observational study. Acta Anaesthesiol. Scand. 2021, 65, 68–75. [Google Scholar] [CrossRef]
- Halvatsiotis, P.; Kotanidou, A.; Tzannis, K.; Jahaj, E.; Magira, E.; Theodorakopoulou, M.; Konstandopoulou, G.; Gkeka, E.; Pourzitaki, C.; Kapravelos, N.; et al. Demographic and clinical features of critically ill patients with COVID-19 in Greece: The burden of diabetes and obesity. Diabetes Res. Clin. Pract. 2020, 166, 108331. [Google Scholar] [CrossRef]
- Han, H.; Xie, L.; Liu, R.; Yang, J.; Liu, F.; Wu, K.; Chen, L.; Hou, W.; Feng, Y.; Zhu, C. Analysis of heart injury laboratory parameters in 273 COVID-19 patients in one hospital in Wuhan, China. J. Med. Virol. 2020, 92, 819–823. [Google Scholar] [CrossRef]
- Hashemi, N.; Viveiros, K.; Redd, W.D.; Zhou, J.C.; McCarty, T.R.; Bazarbashi, A.N.; Hathorn, K.E.; Wong, D.; Njie, C.; Shen, L.; et al. Impact of chronic liver disease on outcomes of hospitalized patients with COVID-19: A multicentre United States experience. Liver Int. 2020, 40, 2515–2521. [Google Scholar] [CrossRef]
- Hatami, H.; Soleimantabar, H.; Ghasemian, M.; Delbari, N.; Aryannezhad, S. Predictors of Intensive Care Unit Admission among Hospitalized COVID-19 Patients in a Large University Hospital in Tehran, Iran. J. Res. Health Sci. 2021, 21, 1–10. [Google Scholar] [CrossRef]
- He, F.; Shang, X.; Fu, T.; Lin, J.; Li, F.; Qiu, Y.; Wu, C.; Wang, Z. Risk of severe coronavirus disease in imported and secondary cases in Zhejiang province, China. J. Public Health 2021, 43, 35–41. [Google Scholar] [CrossRef]
- Hendra, H.; Vajgel, G.; Antonelou, M.; Neradova, A.; Manson, B.; Clark, S.G.; Kostakis, I.D.; Caplin, B.; Salama, A.D. Identifying prognostic risk factors for poor outcome following COVID-19 disease among in-centre haemodialysis patients: Role of inflammation and frailty. J. Nephrol. 2021, 34, 315–323. [Google Scholar] [CrossRef]
- Hoffmann, C.; Casado, J.L.; Härter, G.; Vizcarra, P.; Moreno, A.; Cattaneo, D.; Meraviglia, P.; Spinner, C.D.; Schabaz, F.; Grunwald, S.; et al. Immune deficiency is a risk factor for severe COVID-19 in people living with HIV. HIV Med. 2021, 22, 372–378. [Google Scholar] [CrossRef]
- Hu, F.; Guo, Y.; Lin, J.; Zeng, Y.; Wang, J.; Li, M.; Cong, L. Association of serum uric acid levels with COVID-19 severity. BMC Endocr. Disord. 2021, 21, 97. [Google Scholar] [CrossRef]
- Hu, H.; Yao, N.; Qiu, Y. Comparing rapid scoring systems in mortality prediction of critical ill patients with novel coronavirus disease. Acad. Emerg. Med. 2020, 27, 461–468. [Google Scholar] [CrossRef] [Green Version]
- Hu, J.; Zhou, J.; Dong, F.; Tan, J.; Wang, S.; Li, Z.; Zhang, X.; Zhang, H.; Ming, J.; Huang, T. Combination of serum lactate dehydrogenase and sex is predictive of severe disease in patients with COVID-19. Medicine 2020, 99, e22774. [Google Scholar] [CrossRef]
- Hu, L.; Chen, S.; Fu, Y.; Gao, Z.; Long, H.; Ren, H.W.; Zuo, Y.; Wang, J.; Li, H.; Xu, Q.B.; et al. Risk Factors Associated with Clinical Outcomes in 323 COVID-19 Hospitalized Patients in Wuhan, China. Clin. Infect. Dis. 2020, 71, 2089–2098. [Google Scholar] [CrossRef]
- Hu, X.; Deng, H.; Wang, Y.; Chen, L.; Gu, X.; Wang, X. Predictive value of the prognostic nutritional index for the severity of coronavirus disease 2019. Nutrition 2021, 84, 111123. [Google Scholar] [CrossRef]
- Huang, R.; Zhu, L.; Xue, L.; Liu, L.; Yan, X.; Wang, J.; Zhang, B.; Xu, T.; Ji, F.; Zhao, Y.; et al. Clinical findings of patients with coronavirus disease 2019 in jiangsu province, china: A retrospective, multi-center study. PLoS Negl. Trop. Dis. 2020, 14, e0008280. [Google Scholar] [CrossRef]
- Huang, S.; Wang, J.; Liu, F.; Liu, J.; Cao, G.; Yang, C.; Liu, W.; Tu, C.; Zhu, M.; Xiong, B. COVID-19 patients with hypertension have more severe disease: A multicenter retrospective observational study. Hypertens. Res. 2020, 43, 824–831. [Google Scholar] [CrossRef]
- Huang, Y.; Chen, Z.; Wang, Y.; Han, L.; Qin, K.; Huang, W.; Huang, Y.; Wang, H.; Shen, P.; Ba, X.; et al. Clinical characteristics of 17 patients with COVID-19 and systemic autoimmune diseases: A retrospective study. Ann. Rheum. Dis. 2020, 79, 1163–1169. [Google Scholar] [CrossRef]
- Huang, Y.; Guo, H.; Zhou, Y.; Guo, J.; Wang, T.; Zhao, X.; Li, H.; Sun, Y.; Bian, X.; Fang, C. The associations between fasting plasma glucose levels and mortality of COVID-19 in patients without diabetes. Diabetes Res. Clin. Pract. 2020, 169, 108448. [Google Scholar] [CrossRef] [PubMed]
- Hussein, M.H.; Toraih, E.A.; Attia, A.S.; Burley, N.; Zhang, A.D.; Roos, J.; Houghton, A.; Aniemeka, N.; Omar, M.; Aboueisha, M.; et al. Asthma in COVID-19 patients: An extra chain fitting around the neck? Respir. Med. 2020, 175, 106205. [Google Scholar] [CrossRef] [PubMed]
- Hwang, J.M.; Kim, J.H.; Park, J.S.; Chang, M.C.; Park, D. Neurological diseases as mortality predictive factors for patients with COVID-19: A retrospective cohort study. Neurol. Sci. 2020, 41, 2317–2324. [Google Scholar] [CrossRef] [PubMed]
- Iaccarino, G.; Grassi, G.; Borghi, C.; Ferri, C.; Salvetti, M.; Volpe, M. Age and multimorbidity predict death among COVID-19 patients: Results of the SARS-RAS study of the italian society of hypertension. Hypertension 2020, 76, 366–372. [Google Scholar] [CrossRef] [PubMed]
- Iaccarino, G.; Grassi, G.; Borghi, C.; Carugo, S.; Fallo, F.; Ferri, C.; Giannattasio, C.; Grassi, D.; Letizia, C.; Mancusi, C.; et al. Gender differences in predictors of intensive care units admission among COVID-19 patients: The results of the SARS-RAS study of the italian society of hypertension. PLoS ONE 2020, 15, e0237297. [Google Scholar] [CrossRef] [PubMed]
- Imam, Z.; Odish, F.; Gill, I.; O’Connor, D.; Armstrong, J.; Vanood, A.; Ibironke, O.; Hanna, A.; Ranski, A.; Halalau, A. Older age and comorbidity are independent mortality predictors in a large cohort of 1305 COVID-19 patients in Michigan, United States. J. Intern. Med. 2020, 288, 469–476. [Google Scholar] [CrossRef]
- Incerti, D.; Rizzo, S.; Li, X.; Yau, V.; Keebler, D.; Chia, J.; Tsai, L. Prognostic model to identify and quantify risk factors for mortality among hospitalised patients with COVID-19 in the USA. BMJ Open 2021, 11, e047121. [Google Scholar] [CrossRef]
- Inciardi, R.M.; Adamo, M.; Lupi, L.; Cani, D.S.; Pasquale, M.D.; Tomasoni, D.; Italia, L.; Zaccone, G.; Tedino, C.; Fabbricatore, D.; et al. Characteristics and outcomes of patients hospitalized for COVID-19 and cardiac disease in Northern Italy. Eur. Heart J. 2020, 41, 1821–1829. [Google Scholar] [CrossRef]
- Islam, M.Z.; Riaz, B.K.; Islam, A.N.M.S.; Khanam, F.; Akhter, J.; Choudhury, R.; Farhana, N.; Jahan, N.A.; Uddin, M.J.; Efa, S.S. Risk factors associated with morbidity and mortality outcomes of COVID-19 patients on the 28th day of the disease course: A retrospective cohort study in bangladesh. Epidemiol. Infect. 2020, 148, e263. [Google Scholar] [CrossRef]
- Jain, P.; Sinha, N.; Prasad, M.; Padole, V. Clinical and laboratory profile of COVID-19 patients admitted at a tertiary care center in new delhi and assessment of factors predicting disease severity. Indian J. Med. Spec. 2021, 12, 59–63. [Google Scholar] [CrossRef]
- Jang, J.G.; Hur, J.; Choi, E.Y.; Hong, K.S.; Lee, W.; Ahn, J.H. Prognostic factors for severe coronavirus disease 2019 in Daegu, Korea. J. Korean Med. Sci. 2020, 35, e209. [Google Scholar] [CrossRef]
- Jegede, O.; Raman, A.A.; Tiongson, B.; Garlapati, P.R.; Hershberger, J.; Gayam, V. Clinical characteristics, hospital course, and outcomes among COVID-19 positive patients with mental illness in a community hospital in New York City. Int. J. Ment. Health 2021, 50, 4–15. [Google Scholar] [CrossRef]
- Ji, D.; Zhang, D.; Xu, J.; Chen, Z.; Yang, T.; Zhao, P.; Chen, G.; Cheng, G.; Wang, Y.; Bi, J.; et al. Prediction for Progression Risk in Patients with COVID-19 Pneumonia: The CALL Score. Clin. Infect. Dis. 2020, 71, 1393–1399. [Google Scholar] [CrossRef] [Green Version]
- Ji, X.Y.; Ma, Y.; Shi, N.N.; Liang, N.; Chen, R.B.; Liu, S.H.; Shi, S.; Wu, G.H.; Li, J.K.; Chen, H.; et al. Clinical characteristics and treatment outcome of COVID-19 patients with stroke in China: A multicenter retrospective study. Phytomedicine 2021, 81, 153433. [Google Scholar] [CrossRef]
- Jiang, N.; Liu, Y.N.; Bao, J.; Li, R.; Ni, W.T.; Tan, X.Y.; Xu, Y.; Peng, L.P.; Wang, X.R.; Zeng, Y.M.; et al. Clinical features and risk factors associated with severe COVID-19 patients in China. Chin. Med. J. 2021, 134, 944–953. [Google Scholar] [CrossRef]
- Jiang, Y.; Abudurexiti, S.; An, M.M.; Cao, D.; Wei, J.; Gong, P. Risk factors associated with 28-day all-cause mortality in older severe COVID-19 patients in Wuhan, China: A retrospective observational study. Sci. Rep. 2020, 10, 22369. [Google Scholar] [CrossRef]
- Jimeno, S.; Ventura, P.S.; Castellano, J.M.; García-Adasme, S.I.; Miranda, M.; Touza, P.; Lllana, I.; López-Escobar, A. Prognostic implications of neutrophil-lymphocyte ratio in COVID-19. Eur. J. Clin. Investig. 2021, 51, e13404. [Google Scholar] [CrossRef]
- Jørgensen, M.J.; Holter, J.C.; Christensen, E.E.; Schjalm, C.; Tonby, K.; Pischke, S.E.; Jenum, S.; Skeie, L.G.; Nur, S.; Lind, A.; et al. Increased interleukin-6 and macrophage chemoattractant protein-1 are associated with respiratory failure in COVID-19. Sci. Rep. 2020, 10, 21697. [Google Scholar] [CrossRef]
- Jose, J.; Al-Dorzi, H.M.; Al-Omari, A.; Al-Hameed, F.; Sadat, M.; Qasim, E.A.; Alraddadi, B.; Harthy, A.A.; Mekhlafi, G.A.A.; Almotairi, A.; et al. Critically ill patients with diabetes and middle east respiratory syndrome: A multi-center observational study. BMC Infect. Dis. 2021, 21, 84. [Google Scholar] [CrossRef]
- Jung, C.; Bruno, R.R.; Wernly, B.; Joannidis, M.; Oeyen, S.; Zafeiridis, T.; Marsh, B.; Andersen, F.H.; Moreno, R.; Fernandes, A.M.; et al. Inhibitors of the renin-angiotensin-aldosterone system and COVID-19 in critically ill elderly patients. Eur. Heart J. Cardiovasc. Pharmacother. 2021, 7, 76–77. [Google Scholar] [CrossRef]
- Kaeuffer, C.; Hyaric, C.L.; Fabacher, T.; Mootien, J.; Dervieux, B.; Ruch, Y.; Hugerot, A.; Zhu, Y.J.; Pointurier, V.; Clere-Jehl, R.; et al. Clinical characteristics and risk factors associated with severe COVID-19: Prospective analysis of 1045 hospitalised cases in North-Eastern France, march 2020. Eurosurveillance 2020, 25, 2000895. [Google Scholar] [CrossRef]
- Kalligeros, M.; Shehadeh, F.; Mylona, E.K.; Benitez, G.; Beckwith, C.G.; Chan, P.A.; Mylonakis, E. Association of Obesity with Disease Severity among Patients with COVID-19. Obesity 2020, 28, 1200–1204. [Google Scholar] [CrossRef]
- Karahan, S.; Katkat, F. Impact of serum 25(OH) vitamin D level on mortality in patients with COVID-19 in Turkey. J. Nutr. Health Aging 2021, 25, 189–196. [Google Scholar] [CrossRef]
- Karimi, M.; Haghpanah, S.; Zarei, T.; Azarkeivan, A.; Shirkavand, A.; Matin, S.; Tavakoli, M.A.; Zahedi, Z.; Sanctis, V.D. Prevalence and severity of coronavirus disease 2019 (COVID-19) in transfusion dependent and non-transfusion dependent β-thalassemia patients and effects of associated comorbidities: An Iranian nationwide study. Acta Bio Med. Atenei Parm. 2020, 91, e2020007. [Google Scholar]
- Karlsson, L.K.; Jakobsen, L.H.; Hollensberg, L.; Ryg, J.; Midttun, M.; Frederiksen, H.; Glenthøj, A.; Kodahl, A.R.; Secher-Johnsen, J.; Nielsen, L.K.; et al. Clinical presentation and mortality in hospitalized patients aged 80+ years with COVID-19—A retrospective cohort study. Arch. Gerontol. Geriatr. 2021, 94, 104335. [Google Scholar] [CrossRef]
- Kaya, H.; Kaji, M.; Usuda, D. Soluble interleukin-2 receptor levels on admission associated with mortality in coronavirus disease 2019. Int. J. Infect. Dis. 2021, 105, 522–524. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.; Althunayyan, S.; Alsofayan, Y.; Alotaibi, R.; Mubarak, A.; Arafat, M.; Assiri, A.; Jokhdar, H. Risk factors associated with worse outcomes in COVID-19: A retrospective study in Saudi Arabia. East Mediterr. Health J. 2020, 26, 1371–1380. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.W.; Byeon, K.H.; Kim, J.; Cho, K.D.; Lee, N. The correlation of comorbidities on the mortality in patients with COVID-19: An observational study based on the korean national health insurance big data. J. Korean Med. Sci. 2020, 35, e243. [Google Scholar] [CrossRef] [PubMed]
- Kim, E.J.; Lee, Y.H.; Park, J.S.; Lee, J.; Lee, S.Y.; Kim, Y.; Kwon, Y.S.; Jang, J.G.; Shin, K.C.; Kim, K.C.; et al. Clinical features and prognostic factors of critically ill patients with COVID-19 in Daegu, South Korea: A multi-center retrospective study. Medicine 2021, 100, e24437. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.W.; Kim, S.M.; Kim, Y.K.; Kim, J.Y.; Lee, Y.M.; Kim, B.O.; Hwangbo, S.; Park, T. Clinical characteristics and outcomes of COVID-19 cohort patients in Daegu metropolitan city outbreak in 2020. J. Korean Med. Sci. 2021, 36, e12. [Google Scholar] [CrossRef] [PubMed]
- Krause, M.; Douin, D.J.; Kim, K.K.; Fernandez-Bustamante, A.; Bartels, K. Characteristics and outcomes of mechanically ventilated COVID-19 patients-an observational cohort study. J. Intensive Care Med. 2021, 36, 271–276. [Google Scholar] [CrossRef]
- Krishnamoorthy, G.; Arsene, C.; Jena, N.; Mogulla, S.M.; Coakley, R.; Khine, J.; Khosrodad, N.; Klein, A.; Sule, A.A. Racial disparities in COVID-19 hospitalizations do not lead to disparities in outcomes. Public Health 2021, 190, 93–98. [Google Scholar] [CrossRef]
- Krishnan, S.; Patel, K.; Desai, R.; Sule, A.; Paik, P.; Miller, A.; Barclay, A.; Cassella, A.; Lucaj, J.; Royster, Y.; et al. Clinical comorbidities, characteristics, and outcomes of mechanically ventilated patients in the state of Michigan with SARS-CoV-2 pneumonia. J. Clin. Anesth. 2020, 67, 110005. [Google Scholar] [CrossRef]
- Kunal, S.; Sharma, S.M.; Sharma, S.K.; Gautam, D.; Bhatia, H.; Mahla, H.; Sharma, S.; Bhandari, S. Cardiovascular complications and its impact on outcomes in COVID-19. Indian Heart J. 2020, 72, 593–598. [Google Scholar] [CrossRef]
- Kute, V.B.; Bhalla, A.K.; Guleria, S.; Ray, D.S.; Bahadur, M.M.; Shingare, A.; Hegde, U.; Gang, S.; Raju, S.; Patel, H.V.; et al. Clinical profile and outcome of COVID-19 in 250 kidney transplant recipients: A multicenter cohort study from India. Transplantation 2021, 105, 851–860. [Google Scholar] [CrossRef]
- Laake, J.H.; Buanes, E.A.; Småstuen, M.C.; Kvåle, R.; Olsen, B.F.; Rustøen, T.; Strand, K.; Sørensen, V.; Hofsø, K. Characteristics, Management and Survival of ICU Patients with Coronavirus Disease-19 in Norway, March–June 2020. A Prospective Observational Study. Acta Anaesthesiol. Scand. 2021, 65, 618–628. [Google Scholar] [CrossRef]
- Lara, O.D.; O’Cearbhaill, R.E.; Smith, M.J.; Sutter, M.E.; Knisely, A.; McEachron, J.; Gabor, L.R.; Jee, J.; Fehniger, J.E.; Lee, Y.C.; et al. COVID-19 outcomes of patients with gynecologic cancer in New York City. Cancer 2020, 126, 4294–4303. [Google Scholar] [CrossRef]
- Lee, J.; Jo, S.J.; Cho, Y.; Lee, J.H.; Oh, I.Y.; Park, J.J.; Cho, Y.S.; Choi, D.J. Effects of renin-angiotensin system blockers on the risk and outcomes of severe acute respiratory syndrome coronavirus 2 infection in patients with hypertension. Korean J. Intern. Med. 2021, 36, S123–S131. [Google Scholar] [CrossRef]
- Lee, L.Y.; Cazier, J.B.; Angelis, V.; Arnold, R.; Bisht, V.; Campton, N.A.; Chackathayil, J.; Cheng, V.W.; Curley, H.M.; Fittall, M.W.; et al. COVID-19 mortality in patients with cancer on chemotherapy or other anticancer treatments: A prospective cohort study. Lancet 2020, 395, 1919–1926. [Google Scholar] [CrossRef]
- Lee, S.C.; Son, K.J.; Han, C.H.; Jung, J.Y.; Park, S.C. Impact of comorbid asthma on severity of coronavirus disease (COVID-19). Sci. Rep. 2020, 10, 21805. [Google Scholar] [CrossRef]
- Lee, Y.R.; Kang, M.K.; Song, J.E.; Kim, H.J.; Kweon, Y.O.; Tak, W.Y.; Jang, S.Y.; Park, J.G.; Lee, C.; Hwang, J.S.; et al. Clinical outcomes of coronavirus disease 2019 in patients with pre-existing liver diseases: A multicenter study in South Korea. Clin. Mol. Hepatol. 2020, 26, 562–576. [Google Scholar] [CrossRef]
- Lei, C.; Lin, W.; Deng, X.; Hu, F.; Chen, F.; Cai, W.; Li, Y.; Wen, C.; Guan, Y.; Wang, J.; et al. Factors associated with clinical outcomes in patients with coronavirus disease 2019 in Guangzhou, China. J. Clin. Virol. 2020, 133, 104661. [Google Scholar] [CrossRef]
- Lei, F.; Liu, Y.M.; Zhou, F.; Qin, J.J.; Zhang, P.; Zhu, L.; Zhang, X.J.; Cai, J.; Lin, L.; Ouyang, S.; et al. Longitudinal association between markers of liver injury and mortality in COVID-19 in China. Hepatology 2020, 72, 389–398. [Google Scholar] [CrossRef] [PubMed]
- Leung, C. Risk factors for predicting mortality in elderly patients with COVID-19: A review of clinical data in China. Mech. Ageing Dev. 2020, 188, 111255. [Google Scholar] [CrossRef]
- Li, G.; Liu, Y.; Jing, X.; Wang, Y.; Miao, M.; Tao, L.; Zhou, Z.; Xie, Y.; Huang, Y.; Lei, J.; et al. Mortality risk of COVID-19 in elderly males with comorbidities: A multi-country study. Aging 2020, 13, 27–60. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Xu, F.; Yin, X.; Wu, N.; Li, Y.; Zhang, T.; Chen, D.; Liu, K.; Qiu, Q. Lactic dehydrogenase-lymphocyte ratio for predicting prognosis of severe COVID-19. Medicine 2021, 100, e24441. [Google Scholar] [CrossRef]
- Li, H.Y.; Wang, J.W.; Xu, L.W.; Zhao, X.L.; Feng, J.X.; Xu, Y.Z. Clinical analysis of 132 cases COVID-19 from Wuhan. Medicine 2020, 99, e22847. [Google Scholar] [CrossRef]
- Li, K.; Chen, D.; Chen, S.; Feng, Y.; Chang, C.; Wang, Z.; Wang, N.; Zhen, G. Predictors of fatality including radiographic findings in adults with COVID-19. Respir. Res. 2020, 21, 146. [Google Scholar] [CrossRef]
- Li, K.; Wu, J.; Wu, F.; Guo, D.; Chen, L.; Fang, Z.; Li, C. The Clinical and Chest CT Features Associated with Severe and Critical COVID-19 Pneumonia. Investig. Radiol. 2020, 55, 327–331. [Google Scholar] [CrossRef]
- Li, T.; Lu, L.; Zhang, W.; Tao, Y.; Wang, L.; Bao, J.; Liu, B.; Duan, J. Clinical characteristics of 312 hospitalized older patients with COVID-19 in Wuhan, China. Arch. Gerontol. Geriatr. 2020, 91, 104185. [Google Scholar] [CrossRef]
- Li, X.; Xu, S.; Yu, M.; Wang, K.; Tao, Y.; Zhou, Y.; Shi, J.; Zhou, M.; Wu, B.; Yang, Z.; et al. Risk factors for severity and mortality in adult COVID-19 inpatients in Wuhan. J. Allergy Clin. Immunol. 2020, 146, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Lian, J.; Jin, X.; Hao, S.; Cai, H.; Zhang, S.; Zheng, L.; Jia, H.; Hu, J.; Gao, J.; Zhang, Y.; et al. Analysis of Epidemiological and Clinical Features in Older Patients with Corona Virus Disease 2019 (COVID-19) out of Wuhan. Clin. Infect. Dis. 2020, 71, 740–747. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lièvre, A.; Turpin, A.; Ray-Coquard, I.; Le Malicot, K.; Thariat, J.; Ahle, G.; Neuzillet, C.; Paoletti, X.; Bouché, O.; Aldabbagh, K.; et al. Risk factors for coronavirus disease 2019 (COVID-19) severity and mortality among solid cancer patients and impact of the disease on anticancer treatment: A French nationwide cohort study (GCO-002 CACOVID-19). Eur. J. Cancer 2020, 141, 62–81. [Google Scholar] [CrossRef] [PubMed]
- Lim, J.P.; Low, K.Y.H.; Lin, N.J.J.; Lim, C.Z.Q.; Ong, S.W.X.; Tan, W.Y.T.; Tay, W.C.; Tan, H.N.; Young, B.E.; Lye, D.C.B.; et al. Predictors for development of critical illness amongst older adults with COVID-19: Beyond age to age-associated factors. Arch. Gerontol. Geriatr. 2021, 94, 104331. [Google Scholar] [CrossRef]
- Lin, L.; Jiang, X.; Zhang, Z.; Huang, S.; Zhang, Z.; Fang, Z.; Gu, Z.; Gao, L.; Shi, H.; Mai, L.; et al. Gastrointestinal symptoms of 95 cases with SARS-CoV-2 infection. Gut 2020, 69, 997–1001. [Google Scholar] [CrossRef]
- Ling, S.F.; Broad, E.; Murphy, R.; Pappachan, J.M.; Pardesi-Newton, S.; Kong, M.; Jude, E.B. High-dose cholecalciferol booster therapy is associated with a reduced risk of mortality in patients with COVID-19: A cross-sectional multi-centre observational study. Nutrients 2020, 12, 3799. [Google Scholar] [CrossRef]
- Liu, D.; Wang, Y.; Wang, J.; Liu, J.; Yue, Y.; Liu, W.; Zhang, F.; Wang, Z. Characteristics and outcomes of a sample of patients with COVID-19 identified through social media in Wuhan, China: Observational study. J. Med. Internet Res. 2020, 22, e20108. [Google Scholar] [CrossRef]
- Liu, J.; Tu, C.; Zhu, M.; Wang, J.; Yang, C.; Liu, W.; Xiong, B. The clinical course and prognostic factors of severe COVID-19 in Wuhan, China: A retrospective case-control study. Medicine 2021, 100, e23996. [Google Scholar] [CrossRef]
- Liu, S.; Luo, H.; Wang, Y.; Cuevas, L.E.; Wang, D.; Ju, S.; Yang, Y. Clinical characteristics and risk factors of patients with severe COVID-19 in Jiangsu province, China: A retrospective multicentre cohort study. BMC Infect. Dis. 2020, 20, 584. [Google Scholar] [CrossRef]
- Liu, Y.; Du, X.; Chen, J.; Jin, Y.; Peng, L.; Wang, H.H.X.; Luo, M.; Chen, L.; Zhao, Y. Neutrophil-to-lymphocyte ratio as an independent risk factor for mortality in hospitalized patients with COVID-19. J. Infect. 2020, 81, e6–e12. [Google Scholar] [CrossRef]
- Lohia, P.; Sreeram, K.; Nguyen, P.; Choudhary, A.; Khicher, S.; Yarandi, H.; Kapur, S.; Badr, M.S. Preexisting respiratory diseases and clinical outcomes in COVID-19: A multihospital cohort study on predominantly African American population. Respir. Res. 2021, 22, 37. [Google Scholar] [CrossRef]
- Long, H.; Nie, L.; Xiang, X.; Li, H.; Zhang, X.; Fu, X.; Ren, H.; Liu, W.; Wang, Q.; Wu, Q. D-dimer and prothrombin time are the significant indicators of severe COVID-19 and poor prognosis. Biomed. Res. Int. 2020, 2020, 6159720. [Google Scholar] [CrossRef]
- Lorente, L.; Martín, M.M.; Argueso, M.; Solé-Violán, J.; Perez, A.; Marcos, Y.; Ramos, J.A.; Ramos-Gómez, L.; López, S.; Franco, A.; et al. Association between red blood cell distribution width and mortality of COVID-19 patients. Anaesth. Crit. Care Pain Med. 2021, 40, 100777. [Google Scholar] [CrossRef]
- Lorente, L.; Martín, M.M.; Franco, A.; Barrios, Y.; Cáceres, J.J.; Solé-Violán, J.; Perez, A.; Marcos, Y.; Ramos, J.A.; Ramos-Gómez, L.; et al. HLA genetic polymorphisms and prognosis of patients with COVID-19. Med. Intensiva 2021, 45, 96–103. [Google Scholar] [CrossRef]
- Louapre, C.; Collongues, N.; Stankoff, B.; Giannesini, C.; Papeix, C.; Bensa, C.; Deschamps, R.; Créange, A.; Wahab, A.; Pelletier, J.; et al. Clinical characteristics and outcomes in patients with coronavirus disease 2019 and multiple sclerosis. JAMA Neurol. 2020, 77, 1079–1088. [Google Scholar] [CrossRef]
- Lu, Y.; Huang, Z.; Wang, M.; Tang, K.; Wang, S.; Gao, P.; Xie, J.; Wang, T.; Zhao, J. Clinical characteristics and predictors of mortality in young adults with severe COVID-19: A retrospective observational study. Ann. Clin. Microbiol. Antimicrob. 2021, 20, 3. [Google Scholar] [CrossRef]
- Lucar, J.; Wingler, M.J.B.; Cretella, D.A.; Ward, L.M.; Sims Gomillia, C.E.; Chamberlain, N.; Shimose, L.A.; Brock, J.B.; Harvey, J.; Wilhelm, A.; et al. Epidemiology, clinical features, and outcomes of hospitalized adults with COVID-19: Early experience from an academic medical center in Mississippi. South Med. J. 2021, 114, 144–149. [Google Scholar] [CrossRef]
- Lunski, M.J.; Burton, J.; Tawagi, K.; Maslov, D.; Simenson, V.; Barr, D.; Yuan, H.; Johnson, D.; Matrana, M.; Cole, J.; et al. Multivariate mortality analyses in COVID-19: Comparing patients with cancer and patients without cancer in Louisiana. Cancer 2021, 127, 266–274. [Google Scholar] [CrossRef]
- Luo, H.; Liu, S.; Wang, Y.; Phillips-Howard, P.A.; Ju, S.; Yang, Y.; Wang, D. Age differences in clinical features and outcomes in patients with COVID-19, Jiangsu, China: A retrospective, multicentre cohort study. BMJ Open 2020, 10, e039887. [Google Scholar] [CrossRef]
- Maguire, D.; Woods, M.; Richards, C.; Dolan, R.; Veitch, J.W.; Sim, W.M.J.; Kemmett, O.E.H.; Milton, D.C.; Randall, S.L.W.; Bui, L.D.; et al. Prognostic factors in patients admitted to an urban teaching hospital with COVID-19 infection. J. Transl. Med. 2020, 18, 354. [Google Scholar] [CrossRef]
- Mak, J.K.L.; Kuja-Halkola, R.; Wang, Y.; Hägg, S.; Jylhävä, J. Frailty and comorbidity in predicting community COVID-19 mortality in the UK biobank: The effect of sampling. J. Am. Geriatr. Soc. 2021, 69, 1128–1139. [Google Scholar] [CrossRef]
- Marengoni, A.; Zucchelli, A.; Grande, G.; Fratiglioni, L.; Rizzuto, D. The impact of delirium on outcomes for older adults hospitalised with COVID-19. Age Ageing 2020, 49, 923–926. [Google Scholar] [CrossRef]
- Marouf, N.; Cai, W.; Said, K.N.; Daas, H.; Diab, H.; Chinta, V.R.; Hssain, A.A.; Nicolau, B.; Sanz, M.; Tamimi, F. Association between periodontitis and severity of COVID-19 infection: A case–control study. J. Clin. Periodontol. 2021, 48, 483–491. [Google Scholar] [CrossRef]
- Martinez-Lopez, J.; Mateos, M.; Encinas, C.; Sureda, A.; Hernandez-Rivas, J.; Lopez de la Guia, A.; Conde, D.; Krsnik, I.; Prieto, E.; Riaza Grau, R. Multiple myeloma and SARS-CoV-2 infection: Clinical characteristics and prognostic factors of inpatient mortality. Blood Cancer J. 2020, 10, 103. [Google Scholar] [CrossRef]
- Martins, A.; Mouro, M.; Caldas, J.; Silva-Pinto, A.; Santos, A.S.; Xerinda, S.; Ferreira, A.; Figueiredo, P.; Sarmento, A.; Santos, L. Clinical characteristics and outcomes of critically ill COVID-19 patients admitted to an infectious diseases intensive care unit in Portugal. Crit. Care Shock 2021, 24, 32–40. [Google Scholar]
- Mash, R.J.; Presence-Vollenhoven, M.; Adeniji, A.; Christoffels, R.; Doubell, K.; Eksteen, L.; Hendrikse, A.; Hutton, L.; Jenkins, L.; Kapp, P.; et al. Evaluation of patient characteristics, management and outcomes for COVID-19 at district hospitals in the Western Cape, South Africa: Descriptive observational study. BMJ Open 2021, 11, e047016. [Google Scholar] [CrossRef]
- Mather, J.F.; Seip, R.L.; McKay, R.G. Impact of famotidine use on clinical outcomes of hospitalized patients with COVID-19. Am. J. Gastroenterol. 2020, 115, 1617–1623. [Google Scholar] [CrossRef]
- Mato, A.R.; Roeker, L.E.; Lamanna, N.; Allan, J.N.; Leslie, L.; Pagel, J.M.; Patel, K.; Osterborg, A.; Wojenski, D.; Kamdar, M.; et al. Outcomes of COVID-19 in patients with CLL: A multicenter international experience. Blood 2020, 136, 1134–1143. [Google Scholar] [CrossRef]
- Matsuzawa, Y.; Ogawa, H.; Kimura, K.; Konishi, M.; Kirigaya, J.; Fukui, K.; Tsukahara, K.; Shimizu, H.; Iwabuchi, K.; Yamada, Y.; et al. Renin-angiotensin system inhibitors and the severity of coronavirus disease 2019 in Kanagawa, Japan: A retrospective cohort study. Hypertens Res. 2020, 43, 1257–1266. [Google Scholar] [CrossRef]
- Mayer, M.A.; Vidal-Alaball, J.; Puigdellívol-Sánchez, A.; Marín Gomez, F.X.; Leis, A.; Mendioroz Peña, J. Clinical characterization of patients with COVID-19 in primary care in Catalonia: Retrospective observational study. JMIR Public Health Surveill. 2021, 7, e25452. [Google Scholar] [CrossRef]
- Mehta, H.B.; Li, S.; Goodwin, J.S. Risk factors associated with SARS-CoV-2 infections, hospitalization, and mortality among US nursing home residents. JAMA Netw. Open 2021, 4, e216315. [Google Scholar] [CrossRef] [PubMed]
- Mehta, V.; Goel, S.; Kabarriti, R.; Cole, D.; Goldfinger, M.; Acuna-Villaorduna, A.; Pradhan, K.; Thota, R.; Reissman, S.; Sparano, J.A.; et al. Case Fatality Rate of Cancer Patients with COVID-19 in a New York Hospital System. Cancer Discov. 2020, 10, 935–941. [Google Scholar] [CrossRef] [PubMed]
- Ménager, P.; Brière, O.; Gautier, J.; Riou, J.; Sacco, G.; Brangier, A.; Annweiler, C.; Geria-Covid Study Group OBOT. Regular use of VKA prior to COVID-19 associated with lower 7-day survival in hospitalized frail elderly COVID-19 patients: The GERIA-COVID cohort study. Nutrients 2020, 13, 39. [Google Scholar] [CrossRef] [PubMed]
- Mendes, A.; Serratrice, C.; Herrmann, F.R.; Genton, L.; Périvier, S.; Scheffler, M.; Fassier, T.; Huber, P.; Jacques, M.; Prendki, V.; et al. Predictors of in-hospital mortality in older patients with COVID-19: The COVIDAge study. J. Am. Med. Dir. Assoc. 2020, 21, 1546. [Google Scholar] [CrossRef] [PubMed]
- Messika, J.; Eloy, P.; Roux, A.; Hirschi, S.; Nieves, A.; Le Pavec, J.; Sénéchal, A.; Saint Raymond, C.; Carlier, N.; Demant, X.; et al. COVID-19 in lung transplant recipients. Transplantation 2021, 105, 177–186. [Google Scholar] [CrossRef] [PubMed]
- Middeldorp, S.; Coppens, M.; van Haaps, T.F.; Foppen, M.; Vlaar, A.P.; Müller, M.C.A.; Bouman, C.C.S.; Beenen, L.F.M.; Kootte, R.S.; Heijmans, J.; et al. Incidence of venous thromboembolism in hospitalized patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1995–2002. [Google Scholar] [CrossRef] [PubMed]
- Moghaddam, A.; Heller, R.A.; Sun, Q.; Seelig, J.; Cherkezov, A.; Seibert, L.; Hackler, J.; Seemann, P.; Diegmann, J.; Pilz, M.; et al. Selenium deficiency is associated with mortality risk from COVID-19. Nutrients 2020, 12, 2098. [Google Scholar] [CrossRef]
- Morrison, A.R.; Johnson, J.M.; Griebe, K.M.; Jones, M.C.; Stine, J.J.; Hencken, L.N.; To, L.; Bianchini, M.L.; Vahia, A.T.; Swiderek, J.; et al. Clinical characteristics and predictors of survival in adults with coronavirus disease 2019 receiving tocilizumab. J. Autoimmun. 2020, 114, 102512. [Google Scholar] [CrossRef]
- Mostaza, J.M.; García-Iglesias, F.; González-Alegre, T.; Blanco, F.; Varas, M.; Hernández-Blanco, C.; Hontañón, V.; Jaras-Hernández, M.J.; Martínez-Prieto, M.; Menéndez-Saldaña, A.; et al. Clinical course and prognostic factors of COVID-19 infection in an elderly hospitalized population. Arch. Gerontol. Geriatr. 2020, 91, 104204. [Google Scholar] [CrossRef]
- Murthy, S.; Archambault, P.M.; Atique, A.; Carrier, F.M.; Cheng, M.P.; Codan, C.; Daneman, N.; Dechert, W.; Douglas, S.; Fiest, K.M.; et al. Characteristics and outcomes of patients with COVID-19 admitted to hospital and intensive care in the first phase of the pandemic in Canada: A national cohort study. CMAJ Open 2021, 9, E181–E188. [Google Scholar] [CrossRef]
- Nachega, J.B.; Ishoso, D.K.; Otokoye, J.O.; Hermans, M.P.; Machekano, R.N.; Sam-Agudu, N.A.; Bongo-Pasi Nswe, C.; Mbala-Kingebeni, P.; Madinga, J.N.; Mukendi, S.; et al. Clinical characteristics and outcomes of patients hospitalized for COVID-19 in Africa: Early insights from the Democratic Republic of the Congo. Am. J. Trop. Med. Hyg. 2020, 103, 2419–2428. [Google Scholar] [CrossRef]
- Nachtigall, I.; Lenga, P.; Jóźwiak, K.; Thürmann, P.; Meier-Hellmann, A.; Kuhlen, R.; Brederlau, J.; Bauer, T.; Tebbenjohanns, J.; Schwegmann, K.; et al. Clinical course and factors associated with outcomes among 1904 patients hospitalized with COVID-19 in Germany: An observational study. Clin. Microbiol. Infect. 2020, 26, 1663–1669. [Google Scholar] [CrossRef]
- Nakamura, S.; Kanemasa, Y.; Atsuta, Y.; Fujiwara, S.; Tanaka, M.; Fukushima, K.; Kobayashi, T.; Shimoyama, T.; Omuro, Y.; Sekiya, N.; et al. Characteristics and outcomes of coronavirus disease 2019 (COVID-19) patients with cancer: A single-center retrospective observational study in Tokyo, Japan. Int. J. Clin. Oncol. 2021, 26, 485–493. [Google Scholar] [CrossRef]
- Ñamendys-Silva, S.A.; Alvarado-Ávila, P.E.; Domínguez-Cherit, G.; Rivero-Sigarroa, E.; Sánchez-Hurtado, L.A.; Gutiérrez-Villaseñor, A.; Romero-González, J.P.; Rodríguez-Bautista, H.; García-Briones, A.; Garnica-Camacho, C.; et al. Outcomes of patients with COVID-19 in the intensive care unit in Mexico: A multicenter observational study. Heart Lung 2021, 50, 28–32. [Google Scholar] [CrossRef]
- COVIDSurg Collaborative. Mortality and pulmonary complications in patients undergoing surgery with perioperative SARS-CoV-2 infection: An international cohort study. Lancet 2020, 396, 27–38. [Google Scholar] [CrossRef]
- Ng, J.H.; Hirsch, J.S.; Wanchoo, R.; Sachdeva, M.; Sakhiya, V.; Hong, S.; Jhaveri, K.D.; Fishbane, S.; Northwell COVID-19 Research Consortium and the Northwell Nephrology COVID-19 Research Consortium. Outcomes of patients with end-stage kidney disease hospitalized with COVID-19. Kidney Int. 2020, 98, 1530–1539. [Google Scholar] [CrossRef]
- Nie, L.; Dai, K.; Wu, J.; Zhou, X.; Hu, J.; Zhang, C.; Zhan, Y.; Song, Y.; Fan, W.; Hu, Z.; et al. Clinical characteristics and risk factors for in-hospital mortality of lung cancer patients with COVID-19: A multicenter, retrospective, cohort study. Thorac. Cancer 2021, 12, 57–65. [Google Scholar] [CrossRef]
- Nie, Y.; Li, J.; Huang, X.; Guo, W.; Zhang, X.; Ma, Y.; Wang, H.; Qi, M.; Tang, X.; Shen, X.; et al. Epidemiological and clinical characteristics of 671 COVID-19 patients in Henan province, China. Int. J. Epidemiol. 2020, 49, 1085–1095. [Google Scholar] [CrossRef]
- Nikpouraghdam, M.; Jalali Farahani, A.; Alishiri, G.; Heydari, S.; Ebrahimnia, M.; Samadinia, H.; Sepandi, M.; Jafari, N.J.; Izadi, M.; Qazvini, A.; et al. Epidemiological characteristics of coronavirus disease 2019 (COVID-19) patients in Iran: A single center study. J. Clin. Virol. 2020, 127, 104378. [Google Scholar] [CrossRef]
- Núñez-Gil, I.J.; Fernández-Ortiz, A.; Eid, C.M.; Huang, J.; Romero, R.; Becerra-Muñoz, V.M.; Uribarri, A.; Feltes, G.; Trabattoni, D.; Fernández-Rozas, I.; et al. Underlying heart diseases and acute COVID-19 outcomes. Cardiol. J. 2021, 28, 202–214. [Google Scholar] [CrossRef]
- O’Horo, J.C.; Cerhan, J.R.; Cahn, E.J.; Bauer, P.R.; Temesgen, Z.; Ebbert, J.; Abril, A.; Abu Saleh, O.M.; Assi, M.; Berbari, E.F.; et al. Outcomes of COVID-19 with the mayo clinic model of care and research. Mayo Clin. Proc. 2021, 96, 601–618. [Google Scholar] [CrossRef]
- Okoh, A.K.; Sossou, C.; Dangayach, N.S.; Meledathu, S.; Phillips, O.; Raczek, C.; Patti, M.; Kang, N.; Hirji, S.A.; Cathcart, C.; et al. Coronavirus disease 19 in minority populations of Newark, New Jersey. Int. J. Equity Health 2020, 19, 93. [Google Scholar] [CrossRef]
- Otero, J.A.; Briongos Figuero, L.S.; Gabella Mattín, M.; Usategui Martín, I.; Cubero Morais, P.; Cuellar Olmedo, L.; Inglada Galiana, L.; Dueñas Gutiérrez, C.; Carretero Gómez, J.; Corral Gudino, L.; et al. The nutritional status of the elderly patient infected with COVID-19: The forgotten risk factor? Curr. Med. Res. Opin. 2021, 37, 549–554. [Google Scholar] [CrossRef]
- Oto, O.A.; Ozturk, S.; Turgutalp, K.; Arici, M.; Alpay, N.; Merhametsiz, O.; Sipahi, S.; Ogutmen, M.B.; Yelken, B.; Altiparmak, M.R.; et al. Predicting the outcome of COVID-19 infection in kidney transplant recipients. BMC Nephrol. 2021, 22, 100. [Google Scholar] [CrossRef]
- Ouldali, N.; Yang, D.D.; Madhi, F.; Levy, M.; Gaschignard, J.; Craiu, I.; Guiddir, T.; Schweitzer, C.; Wiedemann, A. Factors associated with severe SARS-CoV-2 infection. Pediatrics 2021, 147, e2020023432. [Google Scholar] [CrossRef]
- Özdemir, İ.; Özlek, B.; Çetin, N. Permanent atrial fibrillation portends poor outcomes in hospitalized patients with COVID-19: A retrospective observational study. J. Electrocardiol. 2021, 65, 113–120. [Google Scholar] [CrossRef]
- Ozturk, S.; Turgutalp, K.; Arici, M.; Odabas, A.R.; Altiparmak, M.R.; Aydin, Z.; Cebeci, E.; Basturk, T.; Soypacaci, Z.; Sahin, G.; et al. Mortality analysis of COVID-19 infection in chronic kidney disease, haemodialysis and renal transplant patients compared with patients without kidney disease: A nationwide analysis from Turkey. Nephrol. Dial. Transplant. 2020, 35, 2083–2095. [Google Scholar] [CrossRef]
- Park, B.E.; Lee, J.H.; Park, H.K.; Kim, H.N.; Jang, S.Y.; Bae, M.H.; Yang, D.H.; Park, H.S.; Cho, Y.; Lee, B.Y.; et al. Impact of cardiovascular risk factors and cardiovascular diseases on outcomes in patients hospitalized with COVID-19 in Daegu metropolitan city. J. Korean Med. Sci. 2021, 36, e15. [Google Scholar] [CrossRef]
- Park, J.G.; Kang, M.K.; Lee, Y.R.; Song, J.E.; Kim, N.Y.; Kweon, Y.O.; Tak, W.Y.; Jang, S.Y.; Lee, C.; Kim, B.S.; et al. Fibrosis-4 index as a predictor for mortality in hospitalised patients with COVID-19: A retrospective multicentre cohort study. BMJ Open 2020, 10, e041989. [Google Scholar] [CrossRef]
- Parlak, S.; Çıvgın, E.; Beşler, M.; Kayıpmaz, A. The effect of hepatic steatosis on COVID-19 severity: Chest computed tomography findings. Saudi J. Gastroenterol. 2021, 27, 105–110. [Google Scholar]
- Pascual, J.; Melilli, E.; Jiménez-Martín, C.; González-Monte, E.; Zárraga, S.; Gutiérrez-Dalmau, A.; López-Jiménez, V.; Juega, J.; Muñoz-Cepeda, M.; Lorenzo, I.; et al. COVID-19-related mortality during the first 60 days after kidney transplantation. Eur. Urol. 2020, 78, 641–643. [Google Scholar] [CrossRef] [PubMed]
- Passamonti, F.; Cattaneo, C.; Arcaini, L.; Bruna, R.; Cavo, M.; Merli, F.; Angelucci, E.; Krampera, M.; Cairoli, R.; Della Porta, M.G.; et al. Clinical characteristics and risk factors associated with COVID-19 severity in patients with haematological malignancies in italy: A retrospective, multicentre, cohort study. Lancet Haematol. 2020, 7, e737–e745. [Google Scholar] [CrossRef]
- Patel, A.; Abdulaal, A.; Ariyanayagam, D.; Killington, K.; Denny, S.J.; Mughal, N.; Hughes, S.; Goel, N.; Davies, G.W.; Moore, L.S.P.; et al. Investigating the association between ethnicity and health outcomes in SARS-CoV-2 in a London secondary care population. PLoS ONE 2020, 15, e0240960. [Google Scholar] [CrossRef] [PubMed]
- Pei, G.; Zhang, Z.; Peng, J.; Liu, L.; Zhang, C.; Yu, C.; Ma, Z.; Huang, Y.; Liu, W.; Yao, Y.; et al. Renal Involvement and Early Prognosis in Patients with COVID-19 Pneumonia. J. Am. Soc. Nephrol. 2020, 31, 1157–1165. [Google Scholar] [CrossRef]
- Peiró, Ó.; Carrasquer, A.; Sánchez-Gimenez, R.; Lal-Trehan, N.; Del-Moral-Ronda, V.; Bonet, G.; Fort-Gallifa, I.; Picó-Plana, E.; Bastón-Paz, N.; Gutiérrez, C.; et al. Biomarkers and short-term prognosis in COVID-19. Biomarkers 2021, 26, 119–126. [Google Scholar] [CrossRef]
- Pepe, M.; Maroun-Eid, C.; Romero, R.; Arroyo-Espliguero, R.; Fernàndez-Rozas, I.; Aparisi, A.; Becerra-Muñoz, V.M.; Garcìa Aguado, M.; Brindicci, G.; Huang, J.; et al. Clinical presentation, therapeutic approach, and outcome of young patients admitted for COVID-19, with respect to the elderly counterpart. Clin. Exp. Med. 2021, 21, 249–268. [Google Scholar] [CrossRef]
- Pereira, M.R.; Mohan, S.; Cohen, D.J.; Husain, S.A.; Dube, G.K.; Ratner, L.E.; Arcasoy, S.; Aversa, M.M.; Benvenuto, L.J.; Dadhania, D.M.; et al. COVID-19 in Solid Organ Transplant Recipients: Initial Report from the US Epicenter. Am. J. Transplant. 2020, 20, 1800–1808. [Google Scholar] [CrossRef]
- Pinato, D.J.; Lee, A.J.X.; Biello, F.; Seguí, E.; Aguilar-Company, J.; Carbó, A.; Bruna, R.; Bower, M.; Rizzo, G.; Benafif, S.; et al. Presenting features and early mortality from SARS-CoV-2 infection in cancer patients during the initial stage of the COVID-19 pandemic in Europe. Cancers 2020, 12, 1841. [Google Scholar] [CrossRef]
- Piñeiro, G.J.; Molina-Andújar, A.; Hermida, E.; Blasco, M.; Quintana, L.F.; Rojas, G.M.; Mercadal, J.; Castro, P.; Sandoval, E.; Andrea, R.; et al. Severe acute kidney injury in critically ill COVID-19 patients. J. Nephrol. 2021, 34, 285–293. [Google Scholar] [CrossRef]
- Pizzini, A.; Aichner, M.; Sahanic, S.; Böhm, A.; Egger, A.; Hoermann, G.; Kurz, K.; Widmann, G.; Bellmann-Weiler, R.; Weiss, G.; et al. Impact of vitamin D deficiency on COVID-19—A prospective analysis from the CovILD registry. Nutrients 2020, 12, 2775. [Google Scholar] [CrossRef]
- Plotnikow, G.A.; Matesa, A.; Nadur, J.M.; Alonso, M.; Nuñez, I.I.; Vergara, G.; Alfageme, M.J.; Vitale, A.; Gil, M.; Kinzler, V.; et al. Characteristics and outcomes of patients infected with nCoV19 requiring invasive mechanical ventilation in Argentina. Rev. Bras. Ter. Intensiv. 2020, 32, 348–353. [Google Scholar] [CrossRef]
- Pongpirul, W.A.; Wiboonchutikul, S.; Charoenpong, L.; Panitantum, N.; Vachiraphan, A.; Uttayamakul, S.; Pongpirul, K.; Manosuthi, W.; Prasithsirikul, W. Clinical course and potential predictive factors for pneumonia of adult patients with coronavirus disease 2019 (COVID-19): A retrospective observational analysis of 193 confirmed cases in Thailand. PLoS Negl. Trop. Dis. 2020, 14, e0008806. [Google Scholar] [CrossRef]
- Prado-Galbarro, F.; Sanchez-Piedra, C.; Gamiño-Arroyo, A.E.; Cruz-Cruz, C. Determinants of survival after severe acute respiratory syndrome coronavirus 2 infection in Mexican outpatients and hospitalised patients. Public Health 2020, 189, 66–72. [Google Scholar] [CrossRef]
- Qian, J.; Zhao, L.; Ye, R.Z.; Li, X.J.; Liu, Y.L. Age-dependent gender differences in COVID-19 in mainland China: Comparative study. Clin. Infect. Dis. 2020, 71, 2488–2494. [Google Scholar] [CrossRef]
- Qin, C.; Zhou, L.; Hu, Z.; Zhang, S.; Yang, S.; Tao, Y.; Xie, C.; Ma, K.; Shang, K.; Wang, W.; et al. Dysregulation of immune response in patients with COVID-19 in Wuhan, China. Clin. Infect. Dis. 2020, 71, 762–768. [Google Scholar] [CrossRef]
- Qin, L.; Li, X.; Shi, J.; Yu, M.; Wang, K.; Tao, Y.; Zhou, Y.; Zhou, M.; Xu, S.; Wu, B.; et al. Gendered effects on inflammation reaction and outcome of COVID-19 patients in Wuhan. J. Med. Virol. 2020, 92, 2684–2692. [Google Scholar] [CrossRef]
- Qin, W.; Bai, W.; Liu, K.; Liu, Y.; Meng, X.; Zhang, K.; Zhang, M. Clinical course and risk factors of disease deterioration in critically ill patients with COVID-19. Hum. Gene Ther. 2021, 32, 310–315. [Google Scholar] [CrossRef]
- Qin, W.; Dong, F.; Zhang, Z.; Hu, B.; Chen, S.; Zhu, Z.; Li, F.; Wang, X.; Zhang, Y.; Wang, Y.; et al. Low molecular weight heparin and 28-day mortality among patients with coronavirus disease 2019: A cohort study in the early epidemic era. Thromb. Res. 2021, 198, 19–22. [Google Scholar] [CrossRef]
- Qu, R.; Ling, Y.; Zhang, Y.H.; Wei, L.Y.; Chen, X.; Li, X.M.; Liu, X.Y.; Liu, H.M.; Guo, Z.; Ren, H.; et al. Platelet-to-lymphocyte ratio is associated with prognosis in patients with coronavirus disease-19. J. Med. Virol. 2020, 92, 1533–1541. [Google Scholar] [CrossRef]
- Quisi, A.; Alıcı, G.; Harbalıoğlu, H.; Genç, Ö.; Er, F.; Allahverdiyev, S.; Yıldırım, A.; Kurt, I.H. The CHA2DS2-VASc score and in-hospital mortality in patients with COVID-19: A multicenter retrospective cohort study. Turk Kardiyol. Dern. Ars. 2020, 48, 656–663. [Google Scholar]
- Raimondi, F.; Novelli, L.; Ghirardi, A.; Russo, F.M.; Pellegrini, D.; Biza, R.; Trapasso, R.; Giuliani, L.; Anelli, M.; Amoroso, M.; et al. Covid-19 and gender: Lower rate but same mortality of severe disease in women-an observational study. BMC Pulm. Med. 2021, 21, 96. [Google Scholar] [CrossRef]
- Rajter, J.C.; Sherman, M.S.; Fatteh, N.; Vogel, F.; Sacks, J.; Rajter, J. Use of ivermectin is associated with lower mortality in hospitalized patients with COVID-19 (ICON study). Chest 2020, 159, 85–92. [Google Scholar] [CrossRef]
- Ramaswamy, A.; Nayak, L.; Roy Moulik, N.; Sengar, M.; Chinnaswamy, G.; Jobanputra, K.; Shah, M.J.; Kapoor, A.; Joshi, A.; Kumar, A.; et al. COVID-19 in cancer patients on active systemic therapy—Outcomes from LMIC scenario with an emphasis on need for active treatment. Cancer Med. 2020, 9, 8747–8753. [Google Scholar] [CrossRef]
- Ramos-Rincon, J.M.; Buonaiuto, V.; Ricci, M.; Martín-Carmona, J.; Paredes-Ruíz, D.; Calderón-Moreno, M.; Rubio-Rivas, M.; Beato-Pérez, J.L.; Arnalich-Fernández, F.; Monge-Monge, D.; et al. Clinical characteristics and risk factors for mortality in very old patients hospitalized with COVID-19 in Spain. J. Gerontol. A Biol. Sci. Med. Sci. 2021, 76, e28–e37. [Google Scholar] [CrossRef]
- Rastad, H.; Ejtahed, H.S.; Shafiee, G.; Safari, A.; Shahrestanaki, E.; Khodaparast, Z.; Hassani, N.S.; Rezaei, M.; Nazari, M.; Zakani, A.; et al. The risk factors associated with COVID-19-related death among patients with end-stage renal disease. BMC Nephrol. 2021, 22, 33. [Google Scholar] [CrossRef]
- Recinella, G.; Marasco, G.; Serafini, G.; Maestri, L.; Bianchi, G.; Forti, P.; Zoli, M. Prognostic role of nutritional status in elderly patients hospitalized for COVID-19: A monocentric study. Aging Clin. Exp. Res. 2020, 32, 2695–2701. [Google Scholar] [CrossRef]
- Ren, L.; Yao, D.; Cui, Z.; Chen, S.; Yan, H. Corona virus disease 2019 patients with different disease severity or age range: A single-center study of clinical features and prognosis. Medicine 2020, 99, e22899. [Google Scholar] [CrossRef]
- Rieg, S.; von Cube, M.; Kalbhenn, J.; Utzolino, S.; Pernice, K.; Bechet, L.; Baur, J.; Lang, C.N.; Wagner, D.; Wolkewitz, M.; et al. COVID-19 in-hospital mortality and mode of death in a dynamic and non-restricted tertiary care model in Germany. PLoS ONE 2020, 15, e0242127. [Google Scholar] [CrossRef]
- Rivera-Izquierdo, M.; Del Carmen Valero-Ubierna, M.; R-delAmo, J.L.; Fernández-García, M.Á.; Martínez-Diz, S.; Tahery-Mahmoud, A.; Rodríguez-Camacho, M.; Gámiz-Molina, A.B.; Barba-Gyengo, N.; Gámez-Baeza, P.; et al. Sociodemographic, clinical and laboratory factors on admission associated with COVID-19 mortality in hospitalized patients: A retrospective observational study. PLoS ONE 2020, 15, e0235107. [Google Scholar] [CrossRef]
- Rivinius, R.; Kaya, Z.; Schramm, R.; Boeken, U.; Provaznik, Z.; Heim, C.; Knosalla, C.; Schoenrath, F.; Rieth, A.; Berchtold-Herz, M.; et al. COVID-19 among heart transplant recipients in germany: A multicenter survey. Clin. Res. Cardiol. 2020, 109, 1531–1539. [Google Scholar] [CrossRef]
- Roberts, M.B.; Izzy, S.; Tahir, Z.; Al Jarrah, A.; Fishman, J.A.; El Khoury, J. COVID-19 in solid organ transplant recipients: Dynamics of disease progression and inflammatory markers in ICU and non-ICU admitted patients. Transpl. Infect. Dis. 2020, 22, e13407. [Google Scholar] [CrossRef] [PubMed]
- Robertson, J.; Gostner, J.M.; Nilsson, S.; Andersson, L.M.; Fuchs, D.; Gisslen, M. Serum neopterin levels in relation to mild and severe COVID-19. BMC Infect. Dis. 2020, 20, 942. [Google Scholar] [CrossRef] [PubMed]
- Rodilla, E.; López-Carmona, M.D.; Cortes, X.; Cobos-Palacios, L.; Canales, S.; Sáez, M.C.; Campos Escudero, S.; Rubio-Rivas, M.; Díez Manglano, J.; Freire Castro, S.J.; et al. Impact of arterial stiffness on all-cause mortality in patients hospitalized with COVID-19 in Spain. Hypertension 2021, 77, 856–867. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, A.; Moreno, G.; Gómez, J.; Carbonell, R.; Picó-Plana, E.; Benavent Bofill, C.; Sánchez Parrilla, R.; Trefler, S.; Esteve Pitarch, E.; Canadell, L.; et al. Severe infection due to the SARS-CoV-2 coronavirus: Experience of a tertiary hospital with COVID-19 patients during the 2020 pandemic. Med. Intensiva 2020, 44, 525–533. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Diaz, C.E.; Guilamo-Ramos, V.; Mena, L.; Hall, E.; Honermann, B.; Crowley, J.S.; Baral, S.; Prado, G.J.; Marzan-Rodriguez, M.; Beyrer, C.; et al. Risk for COVID-19 Infection and Death among Latinos in the United States: Examining Heterogeneity in Transmission Dynamics. Ann. Epidemiol. 2020, 52, 46–53.e2. [Google Scholar] [CrossRef]
- Rodríguez-Molinero, A.; Gálvez-Barrón, C.; Miñarro, A.; Macho, O.; López, G.F.; Robles, M.T.; Dapena, M.D.; Martínez, S.; Milà Ràfols, N.; Monaco, E.E.; et al. Association between COVID-19 prognosis and disease presentation, comorbidities and chronic treatment of hospitalized patients. PLoS ONE 2020, 15, e0239571. [Google Scholar] [CrossRef]
- Roedl, K.; Jarczak, D.; Thasler, L.; Bachmann, M.; Schulte, F.; Bein, B.; Weber, C.F.; Schäfer, U.; Veit, C.; Hauber, H.P.; et al. Mechanical ventilation and mortality among 223 critically ill patients with coronavirus disease 2019: A multicentric study in Germany. Aust. Crit. Care 2021, 34, 167–175. [Google Scholar] [CrossRef]
- Rokni, M.; Ahmadikia, K.; Asghari, S.; Mashaei, S.; Hassanali, F. Comparison of clinical, para-clinical and laboratory findings in survived and deceased patients with COVID-19: Diagnostic role of inflammatory indications in determining the severity of illness. BMC Infect. Dis. 2020, 20, 869. [Google Scholar] [CrossRef]
- Ronderos Botero, D.M.; Omar, A.M.S.; Sun, H.K.; Mantri, N.; Fortuzi, K.; Choi, Y.; Adrish, M.; Nicu, M.; Bella, J.N.; Chilimuri, S. COVID-19 in the healthy patient population: Demographic and clinical phenotypic characterization and predictors of in-hospital outcomes. Arter. Thromb. Vasc. Biol. 2020, 40, 2764–2775. [Google Scholar] [CrossRef]
- Rosenthal, N.; Cao, Z.; Gundrum, J.; Sianis, J.; Safo, S. Risk factors associated with in-hospital mortality in a US national sample of patients with COVID-19. JAMA Netw. Open 2020, 3, e2029058. [Google Scholar] [CrossRef]
- Rossi, L.; Malagoli, A.; Biagi, A.; Zanni, A.; Sticozzi, C.; Comastri, G.; Pannone, L.; Gandolfi, S.; Vergara, P.; Villani, G.Q. Renin-angiotensin system inhibitors and mortality in patients with COVID-19. Infection 2021, 49, 287–294. [Google Scholar] [CrossRef]
- Rottoli, M.; Bernante, P.; Belvedere, A.; Balsamo, F.; Garelli, S.; Giannella, M.; Cascavilla, A.; Tedeschi, S.; Ianniruberto, S.; Del Turco, E.R.; et al. How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients? Results from a single Italian centre. Eur. J. Endocrinol. 2020, 183, 389–397. [Google Scholar] [CrossRef]
- Russo, V.; Di Maio, M.; Mottola, F.F.; Pagnano, G.; Attena, E.; Verde, N.; Di Micco, P.; Silverio, A.; Scudiero, F.; Nunziata, L.; et al. Clinical characteristics and prognosis of hospitalized COVID-19 patients with incident sustained tachyarrhythmias: A multicenter observational study. Eur. J. Clin. Investig. 2020, 50, e13387. [Google Scholar] [CrossRef]
- Rüthrich, M.M.; Giessen-Jung, C.; Borgmann, S.; Classen, A.Y.; Dolff, S.; Grüner, B.; Hanses, F.; Isberner, N.; Köhler, P.; Lanznaster, J.; et al. COVID-19 in cancer patients: Clinical characteristics and outcome-an analysis of the LEOSS registry. Ann. Hematol. 2021, 100, 383–393. [Google Scholar] [CrossRef]
- Rutten, J.J.S.; van Loon, A.M.; van Kooten, J.; van Buul, L.W.; Joling, K.J.; Smalbrugge, M.; Hertogh, C.M. Clinical suspicion of COVID-19 in nursing home residents: Symptoms and mortality risk factors. J. Am. Med. Dir. Assoc. 2020, 21, 1791. [Google Scholar] [CrossRef]
- Saand, A.R.; Flores, M.; Kewan, T.; Alqaisi, S.; Alwakeel, M.; Griffiths, L.; Wang, X.; Han, X.; Burton, R.; Al-Jaghbeer, M.J.; et al. Does inpatient hyperglycemia predict a worse outcome in COVID-19 intensive care unit patients? J. Diabetes 2021, 13, 253–260. [Google Scholar] [CrossRef]
- Sadeghi, A.; Dooghaie, M.A.; Eslami, P.; Pirsalehi, A.; Shojaee, S.; Sanadgol, G.; Jalilian Khave, L.; Vahidi, M.; Asadzadeh Aghdaei, H.; Nazemalhosseini Mojarad, E. The characteristics of cancerous patients infected with COVID-19 in hospital setting. Acta Biomed. 2020, 91, e2020145. [Google Scholar]
- Saeed, O.; Castagna, F.; Agalliu, I.; Xue, X.; Patel, S.R.; Rochlani, Y.; Kataria, R.; Vukelic, S.; Sims, D.B.; Alvarez, C.; et al. Statin use and in-hospital mortality in patients with diabetes mellitus and COVID-19. J. Am. Heart Assoc. 2020, 9, e018475. [Google Scholar] [CrossRef]
- Saez-Giménez, B.; Berastegui, C.; Barrecheguren, M.; Revilla-López, E.; Los Arcos, I.; Alonso, R.; Aguilar, M.; Mora, V.M.; Otero, I.; Reig, J.P.; et al. COVID-19 in lung transplant recipients: A multicenter study. Am. J. Transplant. 2021, 21, 1816–1824. [Google Scholar] [CrossRef]
- Saggi, S.J.; Nath, S.; Culas, R.; Hittalae, S.; Burza, A.; Srinivasan, M.; Abdul, R.; Silver, B.; Lora, A.; Ibtida, I.; et al. Early experience with methylprednisolone on SARS-CoV-2 infection in the African American population—A retrospective analysis. Clin. Med. Insights Circ. Respir. Pulm. Med. 2020, 14, 1179548420980699. [Google Scholar] [CrossRef]
- Saha, A.; Ahsan, M.M.; Quader, M.T.; Naher, S.; Akter, F.; Mehedi, H.M.H.; Ullah Chowdhury, A.A.; Karim, M.H.; Rahman, T.; Parvin, A. Clinical Characteristics and Outcomes of COVID-19 Infected Diabetic Patients Admitted in ICUs of the Southern Region of Bangladesh. Diabetes Metab. Syndr. 2021, 15, 229–235. [Google Scholar] [CrossRef] [PubMed]
- Sai, F.; Liu, X.; Li, L.; Ye, Y.; Zhu, C.; Hang, Y.; Huang, C.; Tian, L.; Huang, H.; Xu, X. Clinical characteristics and risk factors for mortality in patients with coronavirus disease 2019 in intensive care unit: A single-center, retrospective, observational study in China. Ann. Palliat. Med. 2021, 10, 2859–2868. [Google Scholar] [CrossRef] [PubMed]
- Saifi, E.S.; Giorgi-Pierfranceschi, M.; Salvetti, M.; Maninetti, L.; Cavalli, I.; Muiesan, M.L. Factors associated with survival in older patients affected by COVID-19: A retrospective cohort study. Arch. Gerontol. Geriatr. 2021, 94, 104349. [Google Scholar] [CrossRef] [PubMed]
- Salazar, M.R.; González, S.E.; Regairaz, L.; Ferrando, N.S.; González Martínez, V.V.; Carrera Ramos, P.M.; Muñoz, L.; Pesci, S.A.; Vidal, J.M.; Kreplak, N.; et al. Risk factors for COVID-19 mortality: The effect of convalescent plasma administration. PLoS ONE 2021, 16, e0250386. [Google Scholar] [CrossRef]
- Saleh, N.Y.; Aboelghar, H.M.; Salem, S.S.; Ibrahem, R.A.; Khalil, F.O.; Abdelgawad, A.S.; Mahmoud, A.A. The severity and atypical presentations of COVID-19 infection in pediatrics. BMC Pediatr. 2021, 21, 144. [Google Scholar] [CrossRef]
- Sands, K.E.; Wenzel, R.P.; McLean, L.E.; Korwek, K.M.; Roach, J.D.; Miller, K.M.; Poland, R.E.; Burgess, L.H.; Jackson, E.S.; Perlin, J.B. Patient characteristics and admitting vital signs associated with coronavirus disease 2019 (COVID-19)–related mortality among patients admitted with noncritical illness. Infect. Control Hosp. Epidemiol. 2021, 42, 399–405. [Google Scholar] [CrossRef]
- Sano, T.; Kimizuka, Y.; Fujikura, Y.; Hisada, T.; Watanabe, C.; Suematsu, R.; Izumi, K.; Sugiura, H.; Miyata, J.; Shinmoto, H.; et al. COVID-19 in Older Adults: Retrospective Cohort Study in a Tertiary Hospital in Japan. Geriatr. Gerontol. Int. 2020, 20, 1044–1049. [Google Scholar] [CrossRef]
- Santos, C.S.; Morales, C.M.; Álvarez, E.D.; Castro, C.Á.; Robles, A.L.; Sandoval, T.P. Determinants of COVID-19 disease severity in patients with underlying rheumatic disease. Clin. Rheumatol. 2020, 39, 2789–2796. [Google Scholar] [CrossRef]
- Santos, M.M.; Lucena, E.E.S.; Lima, K.C.; Brito, A.A.C.; Bay, M.B.; Bonfada, D. Survival and predictors of deaths of patients hospitalised due to COVID-19 from a retrospective and multicentre cohort study in Brazil. Epidemiol. Infect. 2020, 148, e198. [Google Scholar] [CrossRef]
- Santus, P.; Radovanovic, D.; Saderi, L.; Marino, P.; Cogliati, C.; De Filippis, G.; Rizzi, M.; Franceschi, E.; Pini, S.; Giuliani, F.; et al. Severity of respiratory failure at admission and in-hospital mortality in patients with COVID-19: A prospective observational multicentre study. BMJ Open 2020, 10, e043651. [Google Scholar] [CrossRef]
- Sapey, E.; Gallier, S.; Mainey, C.; Nightingale, P.; McNulty, D.; Crothers, H.; Evison, F.; Reeves, K.; Pagano, D.; Denniston, A.K.; et al. Ethnicity and risk of death in patients hospitalised for COVID-19 infection in the UK: An observational cohort study in an urban catchment area. BMJ Open Respir. Res. 2020, 7, e000644. [Google Scholar] [CrossRef]
- Scarfò, L.; Chatzikonstantinou, T.; Rigolin, G.M.; Quaresmini, G.; Motta, M.; Vitale, C.; Garcia-Marco, J.A.; Hernández-Rivas, J.Á.; Mirás, F.; Baile, M.; et al. COVID-19 severity and mortality in patients with chronic lymphocytic leukemia: A joint study by ERIC, the European research initiative on CLL and CLL campus. Leukemia 2020, 34, 2354–2363. [Google Scholar] [CrossRef]
- Schultze, A.; Walker, A.J.; MacKenna, B.; Morton, C.E.; Bhaskaran, K.; Brown, J.P.; Rentsch, C.T.; Williamson, E.; Drysdale, H.; Croker, R.; et al. Risk of COVID-19-related death among patients with chronic obstructive pulmonary disease or asthma prescribed inhaled corticosteroids: An observational cohort study using the OpenSAFELY platform. Lancet Respir. Med. 2020, 8, 1106–1120. [Google Scholar] [CrossRef]
- Seo, J.; Son, M. Update on association between exposure to renin-angiotensin-aldosterone system inhibitors and coronavirus disease 2019 in South Korea. Korean J. Intern. Med. 2021, 36, S114–S122. [Google Scholar] [CrossRef]
- Shah, G.L.; DeWolf, S.; Lee, Y.J.; Tamari, R.; Dahi, P.B.; Lavery, J.A.; Ruiz, J.; Devlin, S.M.; Cho, C.; Peled, J.U.; et al. Favorable outcomes of COVID-19 in recipients of hematopoietic cell transplantation. J. Clin. Investig. 2020, 130, 6656–6667. [Google Scholar] [CrossRef]
- Shahriarirad, R.; Khodamoradi, Z.; Erfani, A.; Hosseinpour, H.; Ranjbar, K.; Emami, Y.; Mirahmadizadeh, A.; Lotfi, M.; Shirazi Yeganeh, B.; Nejad, A.D.; et al. Epidemiological and clinical features of 2019 novel coronavirus diseases (COVID-19) in the south of Iran. BMC Infect. Dis. 2020, 20, 427. [Google Scholar] [CrossRef]
- Shao, S.; Zhao, Z.; Wang, F.; Chang, D.; Liu, Y.; Liu, S.; Xu, X.; Li, X.; Jiang, C.; Tang, Z. Risk factors associated with disease aggravation among 126 hospitalized patients with COVID-19 in different places in China: A retrospective observational study. Medicine 2020, 99, e22971. [Google Scholar] [CrossRef]
- Sharifpour, M.; Rangaraju, S.; Liu, M.; Alabyad, D.; Nahab, F.B.; Creel-Bulos, C.M.; Jabaley, C.S.; Emory COVID-19 Quality & Clinical Research Collaborative. C-reactive protein as a prognostic indicator in hospitalized patients with COVID-19. PLoS ONE 2020, 15, e0242400. [Google Scholar] [CrossRef]
- Sharma, A. Estimating older adult mortality from COVID-19. J. Gerontol. B Psychol. Sci. Soc. Sci. 2021, 76, e68–e74. [Google Scholar] [CrossRef]
- Shi, J.; Li, Y.; Zhou, X.; Zhang, Q.; Ye, X.; Wu, Z.; Jiang, X.; Yu, H.; Shao, L.; Ai, J.W.; et al. Lactate dehydrogenase and susceptibility to deterioration of mild COVID-19 patients: A multicenter nested case-control study. BMC Med. 2020, 18, 168. [Google Scholar] [CrossRef]
- Shi, M.; Chen, L.; Yang, Y.; Zhang, J.; Xu, J.; Xu, G.; Li, B.; Yin, Y. Analysis of clinical features and outcomes of 161 patients with severe and critical COVID-19: A multicenter descriptive study. J. Clin. Lab. Anal. 2020, 34, e23415. [Google Scholar] [CrossRef]
- Shi, Y.; Yu, X.; Zhao, H.; Wang, H.; Zhao, R.; Sheng, J. Host susceptibility to severe COVID-19 and establishment of a host risk score: Findings of 487 cases outside Wuhan. Crit. Care 2020, 24, 108. [Google Scholar] [CrossRef] [Green Version]
- Shields, A.M.; Burns, S.O.; Savic, S.; Richter, A.G. COVID-19 in patients with primary and secondary immunodeficiency: The United Kingdom Experience. J. Allergy. Clin. Immunol. 2021, 147, 870–875.e1. [Google Scholar] [CrossRef]
- Siepmann, T.; Sedghi, A.; Barlinn, J.; de With, K.; Mirow, L.; Wolz, M.; Gruenewald, T.; Helbig, S.; Schroettner, P.; Winzer, S.; et al. Association of history of cerebrovascular disease with severity of COVID-19. J. Neurol. 2021, 268, 773–784. [Google Scholar] [CrossRef]
- Simonnet, A.; Chetboun, M.; Poissy, J.; Raverdy, V.; Noulette, J.; Duhamel, A.; Labreuche, J.; Mathieu, D.; Pattou, F.; Jourdain, M.; et al. High prevalence of obesity in severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) requiring invasive mechanical ventilation. Obesity 2020, 28, 1994. [Google Scholar] [CrossRef]
- Singh, B.M.; Bateman, J.; Viswanath, A.; Klaire, V.; Mahmud, S.; Nevill, A.; Dunmore, S.J. Risk of COVID-19 hospital admission and COVID-19 mortality during the first COVID-19 wave with a special emphasis on ethnic minorities: An observational study of a single, deprived, multiethnic UK health economy. BMJ Open 2021, 11, e046556. [Google Scholar] [PubMed]
- Singh, S.; Bilal, M.; Pakhchanian, H.; Raiker, R.; Kochhar, G.S.; Thompson, C.C. Impact of obesity on outcomes of patients with coronavirus disease 2019 in the United States: A multicenter electronic health records network study. Gastroenterology 2020, 159, 2221–2225.e6. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Khan, A.; Chowdhry, M.; Bilal, M.; Kochhar, G.S.; Clarke, K. Risk of severe coronavirus disease 2019 in patients with inflammatory bowel disease in the united states: A multicenter research network study. Gastroenterology 2020, 159, 1575–1578.e4. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Khan, A. Clinical characteristics and outcomes of coronavirus disease 2019 among patients with preexisting liver disease in the United States: A multicenter research network study. Gastroenterology 2020, 159, 768–771.e3. [Google Scholar] [CrossRef]
- Smati, S.; Tramunt, B.; Wargny, M.; Caussy, C.; Gaborit, B.; Vatier, C.; Vergès, B.; Ancelle, D.; Amadou, C.; Bachir, L.A.; et al. Relationship between obesity and severe COVID-19 outcomes in patients with type 2 diabetes: Results from the CORONADO study. Diabetes Obes. Metab. 2021, 23, 391–403. [Google Scholar] [CrossRef]
- Smith, A.A.; Fridling, J.; Ibrahim, D.; Porter, P.S., Jr. Identifying patients at greatest risk of mortality due to COVID-19: A New England perspective. West J. Emerg. Med. 2020, 21, 785–789. [Google Scholar]
- Smith, M.; Lara, O.D.; O’Cearbhaill, R.; Knisely, A.; McEachron, J.; Gabor, L.; Carr, C.; Blank, S.; Prasad-Hayes, M.; Frey, M.; et al. Inflammatory markers in gynecologic oncology patients hospitalized with COVID-19 infection. Gynecol. Oncol. 2020, 159, 618–622. [Google Scholar] [CrossRef]
- Snipelisky, D.; Johnson, R.; Prasad, R.; Lakhani, B.; Ellington, J. Characteristics and outcomes based on perceived illness severity in SARS-CoV-2. South Med. J. 2020, 113, 618–622. [Google Scholar] [CrossRef]
- Soh, T.V.; Dzawani, M.; Noorlina, N.; Nik, F.; Norazmi, A. Clinical Characteristics of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV2) Patients in Hospital Tengku Ampuan Afzan. Med. J. Malays. 2020, 75, 479–484. [Google Scholar]
- Soleimani, A.; Kazemian, S.; Karbalai Saleh, S.; Aminorroaya, A.; Shajari, Z.; Hadadi, A.; Talebpour, M.; Sadeghian, H.; Payandemehr, P.; Sotoodehnia, M.; et al. Effects of angiotensin receptor blockers (ARBs) on in-hospital outcomes of patients with hypertension and confirmed or clinically suspected COVID-19. Am. J. Hypertens. 2020, 33, 1102–1111. [Google Scholar] [CrossRef]
- Song, J.; Hu, W.; Yu, Y.; Shen, X.; Wang, Y.; Yan, J.; Yang, X.; Gong, S.; Wang, M. A comparison of clinical characteristics and outcomes in elderly and younger patients with COVID-19. Med. Sci. Monit. 2020, 26, e925047. [Google Scholar] [CrossRef]
- Song, J.W.; Zhang, C.; Fan, X.; Meng, F.P.; Xu, Z.; Xia, P.; Cao, W.J.; Yang, T.; Dai, X.P.; Wang, S.Y.; et al. Immunological and inflammatory profiles in mild and severe cases of COVID-19. Nat. Commun. 2020, 11, 3410. [Google Scholar] [CrossRef]
- Stachura, T.; Celejewska-Wójcik, N.; Polok, K.; Górka, K.; Lichołai, S.; Wójcik, K.; Krawczyk, J.; Kozłowska, A.; Przybyszowski, M.; Włoch, T.; et al. A clinical profile and factors associated with severity of the disease among polish patients hospitalized due to COVID-19—An observational study. Adv. Respir. Med. 2021, 89, 124–134. [Google Scholar] [CrossRef]
- Stall, N.M.; Wu, W.; Lapointe-Shaw, L.; Fisman, D.N.; Giannakeas, V.; Hillmer, M.P.; Rochon, P.A. Sex- and age-specific differences in COVID-19 testing, cases, and outcomes: A population-wide study in Ontario, Canada. J. Am. Geriatr. Soc. 2020, 68, 2188–2191. [Google Scholar] [CrossRef]
- Stefan, G.; Mehedinti, A.M.; Andreiana, I.; Zugravu, A.D.; Cinca, S.; Busuioc, R.; Miler, I.; Stancu, S.; Petrescu, L.; Dimitriu, I.; et al. Clinical features and outcome of maintenance hemodialysis patients with COVID-19 from a tertiary nephrology care center in Romania. Ren. Fail. 2021, 43, 49–57. [Google Scholar] [CrossRef]
- Steinberg, E.; Wright, E.; Kushner, B. In young adults with COVID-19, obesity is associated with adverse outcomes. West J. Emerg. Med. 2020, 21, 752–755. [Google Scholar] [CrossRef]
- Suleyman, G.; Fadel, R.A.; Malette, K.M.; Hammond, C.; Abdulla, H.; Entz, A.; Demertzis, Z.; Hanna, Z.; Failla, A.; Dagher, C.; et al. Clinical characteristics and morbidity associated with coronavirus disease 2019 in a series of patients in metropolitan detroit. JAMA Netw. Open 2020, 3, e2012270. [Google Scholar] [CrossRef]
- Sun, H.; Ning, R.; Tao, Y.; Yu, C.; Deng, X.; Zhao, C.; Meng, S.; Tang, F.; Xu, D. Risk factors for mortality in 244 older adults with COVID-19 in Wuhan, China: A retrospective study. J. Am. Geriatr. Soc. 2020, 68, E19–E23. [Google Scholar] [CrossRef]
- Sun, L.; Shen, L.; Fan, J.; Gu, F.; Hu, M.; An, Y.; Zhou, Q.; Fan, H.; Bi, J. Clinical Features of Patients with Coronavirus Disease 2019 (COVID-19) from a Designated Hospital in Beijing, China. J. Med. Virol. 2020, 92, 2055–2066. [Google Scholar] [CrossRef]
- Sun, S.; Cai, X.; Wang, H.; He, G.; Lin, Y.; Lu, B.; Chen, C.; Pan, Y.; Hu, X. Abnormalities of peripheral blood system in patients with COVID-19 in Wenzhou, China. Clin. Chim. Acta 2020, 507, 174–180. [Google Scholar]
- Suresh, S.; Siddiqui, M.; Abu Ghanimeh, M.; Jou, J.; Simmer, S.; Mendiratta, V.; Russell, S.; Al-Shammari, M.; Chatfield, A.; Alsheik, E.; et al. Association of obesity with illness severity in hospitalized patients with COVID-19: A retrospective cohort study. Obes. Res. Clin. Pract. 2021, 15, 172–176. [Google Scholar] [CrossRef]
- Swann, O.V.; Holden, K.A.; Turtle, L.; Pollock, L.; Fairfield, C.J.; Drake, T.M.; Seth, S.; Egan, C.; Hardwick, H.E.; Halpin, S.; et al. Clinical characteristics of children and young people admitted to hospital with COVID-19 in United Kingdom: Prospective multicentre observational cohort study. BMJ 2020, 370, m3249. [Google Scholar] [CrossRef]
- Szymanski, J.; Mohrmann, L.; Carter, J.; Nelson, R.; Chekuri, S.; Assa, A.; Spund, B.; Reyes-Gil, M.; Uehlinger, J.; Baron, S.; et al. ABO blood type association with SARS-CoV-2 infection mortality: A single-center population in New York City. Transfusion 2021, 61, 1064–1070. [Google Scholar] [CrossRef]
- Talavera, B.; García-Azorín, D.; Martínez-Pías, E.; Trigo, J.; Hernández-Pérez, I.; Valle-Peñacoba, G.; Simón-Campo, P.; de Lera, M.; Chavarría-Miranda, A.; López-Sanz, C.; et al. Anosmia is associated with lower in-hospital mortality in COVID-19. J. Neurol. Sci. 2020, 419, 117163. [Google Scholar] [CrossRef] [PubMed]
- Tang, N.; Bai, H.; Chen, X.; Gong, J.; Li, D.; Sun, Z. Anticoagulant treatment is associated with decreased mortality in severe coronavirus disease 2019 patients with coagulopathy. J. Thromb. Haemost. 2020, 18, 1094–1099. [Google Scholar] [CrossRef] [PubMed]
- Tang, O.; Bigelow, B.F.; Sheikh, F.; Peters, M.; Zenilman, J.M.; Bennett, R.; Katz, M.J. Outcomes of nursing home COVID-19 patients by initial symptoms and comorbidity: Results of universal testing of 1970 residents. J. Am. Med. Dir. Assoc. 2020, 21, 1767. [Google Scholar] [CrossRef] [PubMed]
- Tao, Z.; Xu, J.; Chen, W.; Yang, Z.; Xu, X.; Liu, L.; Chen, R.; Xie, J.; Liu, M.; Wu, J.; et al. Anemia is associated with severe illness in COVID-19: A retrospective cohort study. J. Med. Virol. 2021, 93, 1478–1488. [Google Scholar] [CrossRef]
- Tatum, D.; Taghavi, S.; Houghton, A.; Stover, J.; Toraih, E.; Duchesne, J. Neutrophil-to-lymphocyte ratio and outcomes in Louisiana COVID-19 patients. Shock 2020, 54, 652–658. [Google Scholar] [CrossRef]
- Tedeschi, S.; Giannella, M.; Bartoletti, M.; Trapani, F.; Tadolini, M.; Borghi, C.; Viale, P. Clinical impact of renin-angiotensin system inhibitors on in-hospital mortality of patients with hypertension hospitalized for COVID-19. Clin. Infect. Dis. 2020, 71, 899–901. [Google Scholar] [CrossRef]
- Tehrani, S.; Killander, A.; Astrand, P.; Jakobsson, J.; Gille-Johnson, P. Risk factors for death in adult COVID-19 patients: Frailty predicts fatal outcome in older patients. Int. J. Infect. Dis. 2021, 102, 415–421. [Google Scholar] [CrossRef]
- Tejpal, A.; Gianos, E.; Cerise, J.; Hirsch, J.S.; Rosen, S.; Kohn, N.; Lesser, M.; Weinberg, C.; Majure, D.; Satapathy, S.K.; et al. Sex-based differences in COVID-19 outcomes. J. Women’s Health 2021, 30, 492–501. [Google Scholar] [CrossRef]
- Telle, K.E.; Grøsland, M.; Helgeland, J.; Håberg, S.E. Factors associated with hospitalization, invasive mechanical ventilation treatment and death among all confirmed COVID-19 cases in Norway: Prospective cohort study. Scand. J. Public Health 2021, 49, 41–47. [Google Scholar] [CrossRef]
- Temkin-Greener, H.; Guo, W.; Mao, Y.; Cai, X.; Li, Y. COVID-19 pandemic in assisted living communities: Results from seven states. J. Am. Geriatr. Soc. 2020, 68, 2727–2734. [Google Scholar] [CrossRef]
- Tesoriero, J.M.; Swain, C.E.; Pierce, J.L.; Zamboni, L.; Wu, M.; Holtgrave, D.R.; Gonzalez, C.J.; Udo, T.; Morne, J.E.; Hart-Malloy, R.; et al. COVID-19 outcomes among persons living with or without diagnosed HIV infection in New York state. JAMA Netw. Open 2021, 4, e2037069. [Google Scholar] [CrossRef]
- Tessitore, E.; Carballo, D.; Poncet, A.; Perrin, N.; Follonier, C.; Assouline, B.; Carballo, S.; Girardin, F.; Mach, F. Mortality and high risk of major adverse events in patients with COVID-19 and history of cardiovascular disease. Open Heart 2021, 8, e001526. [Google Scholar] [CrossRef]
- Thomson, R.J.; Hunter, J.; Dutton, J.; Schneider, J.; Khosravi, M.; Casement, A.; Dhadwal, K.; Martin, D. Clinical characteristics and outcomes of critically ill patients with COVID-19 admitted to an intensive care unit in London: A prospective observational cohort study. PLoS ONE 2020, 15, e0243710. [Google Scholar] [CrossRef]
- Tian, J.; Yuan, X.; Xiao, J.; Zhong, Q.; Yang, C.; Liu, B.; Cai, Y.; Lu, Z.; Wang, J.; Wang, Y.; et al. Clinical characteristics and risk factors associated with COVID-19 disease severity in patients with cancer in Wuhan, China: A multicentre, retrospective, cohort study. Lancet Oncol. 2020, 21, 893–903. [Google Scholar] [CrossRef]
- Tian, S.; Hu, N.; Lou, J.; Chen, K.; Kang, X.; Xiang, Z.; Chen, H.; Wang, D.; Liu, N.; Liu, D.; et al. Characteristics of COVID-19 infection in Beijing. J. Infect. 2020, 80, 401–406. [Google Scholar] [CrossRef] [Green Version]
- To, K.K.; Tsang, O.T.; Leung, W.S.; Tam, A.R.; Wu, T.C.; Lung, D.C.; Yip, C.C.; Cai, J.P.; Chan, J.M.; Chik, T.S.; et al. Temporal profiles of viral load in posterior oropharyngeal saliva samples and serum antibody responses during infection by SARS-CoV-2: An observational cohort study. Lancet Infect. Dis. 2020, 20, 565–574. [Google Scholar] [CrossRef] [Green Version]
- Tobolowsky, F.A.; Bardossy, A.C.; Currie, D.W.; Schwartz, N.G.; Zacks, R.L.T.; Chow, E.J.; Dyal, J.W.; Ali, H.; Kay, M.; Duchin, J.S.; et al. Signs, symptoms, and comorbidities associated with onset and prognosis of COVID-19 in a nursing home. J. Am. Med. Dir. Assoc. 2021, 22, 498–503. [Google Scholar] [CrossRef]
- Toh, D.J.; Rowe, E.; Nelson, R.; O’Connell, A.; Lim, K.; Fielke, L.; He, J.; Faunt, J. Outcomes for the First Wave of Hospitalised Patients with COVID-19 in the South Australian Context: A Retrospective Audit. Intern. Med. J. 2021, 51, 189–198. [Google Scholar] [CrossRef]
- Tomasoni, D.; Inciardi, R.M.; Lombardi, C.M.; Tedino, C.; Agostoni, P.; Ameri, P.; Barbieri, L.; Bellasi, A.; Camporotondo, R.; Canale, C.; et al. Impact of heart failure on the clinical course and outcomes of patients hospitalized for COVID-19. Results of the cardio-COVID-Italy multicentre study. Eur. J. Heart Fail. 2020, 22, 2238–2247. [Google Scholar] [CrossRef]
- Tong, M.; Jiang, Y.; Xia, D.; Xiong, Y.; Zheng, Q.; Chen, F.; Zou, L.; Xiao, W.; Zhu, Y. Elevated expression of serum endothelial cell adhesion molecules in COVID-19 patients. J. Infect. Dis. 2020, 222, 894–898. [Google Scholar] [CrossRef]
- Trecarichi, E.M.; Mazzitelli, M.; Serapide, F.; Pelle, M.C.; Tassone, B.; Arrighi, E.; Perri, G.; Fusco, P.; Scaglione, V.; Davoli, C.; et al. Clinical characteristics and predictors of mortality associated with COVID-19 in elderly patients from a long-term care facility. Sci. Rep. 2020, 10, 20834. [Google Scholar] [CrossRef]
- Trifan, G.; Goldenberg, F.D.; Caprio, F.Z.; Biller, J.; Schneck, M.; Khaja, A.; Terna, T.; Brorson, J.; Lazaridis, C.; Bulwa, Z.; et al. Characteristics of a diverse cohort of stroke patients with SARS-CoV-2 and outcome by sex. J. Stroke Cerebrovasc. Dis. 2020, 29, 105314. [Google Scholar] [CrossRef]
- Tsantes, A.E.; Frantzeskaki, F.; Tsantes, A.G.; Rapti, E.; Rizos, M.; Kokoris, S.I.; Paramythiotou, E.; Katsadiotis, G.; Karali, V.; Flevari, A.; et al. The haemostatic profile in critically ill COVID-19 patients receiving therapeutic anticoagulant therapy: An observational study. Medicine 2020, 99, e23365. [Google Scholar] [CrossRef] [PubMed]
- Tschopp, J.; L’Huillier, A.G.; Mombelli, M.; Mueller, N.J.; Khanna, N.; Garzoni, C.; Meloni, D.; Papadimitriou-Olivgeris, M.; Neofytos, D.; Hirsch, H.H.; et al. First experience of SARS-CoV-2 infections in solid organ transplant recipients in the swiss transplant cohort study. Am. J. Transplant. 2020, 20, 2876–2882. [Google Scholar] [CrossRef] [PubMed]
- Tu, Y.; Yang, P.; Zhou, Y.; Wen, X.; Li, Q.; Zhou, J.; Wang, J.; Hu, J.; He, N.; Wang, K.; et al. Risk factors for mortality of critically ill patients with COVID-19 receiving invasive ventilation. Int. J. Med. Sci. 2021, 18, 1198–1206. [Google Scholar] [CrossRef] [PubMed]
- Turgay, Y.Ö.; Kaya, Ş. The atherogenic index of plasma as a predictor of mortality in patients with COVID-19. Heart Lung 2021, 50, 329–333. [Google Scholar] [CrossRef]
- Turgutalp, K.; Ozturk, S.; Arici, M.; Eren, N.; Gorgulu, N.; Islam, M.; Uzun, S.; Sakaci, T.; Aydin, Z.; Sengul, E.; et al. Determinants of mortality in a large group of hemodialysis patients hospitalized for COVID-19. BMC Nephrol. 2021, 22, 29. [Google Scholar] [CrossRef]
- UlHaq, Z.; Shahzad, M.; Khattak, M.I.; Fazid, S.; Ullah, N.; Shireen, A.; Ulhaq, N.; Izhar, A.; Farooq, U.; Darwesh, N.M.; et al. Clinical Characteristics, Mortality and Associated risk Factors in COVID-19 Patients Reported in Ten Major hospitals of Khyber Pakhtunkhwa, Pakistan. J. Ayub. Med. Coll. Abbottabad 2020, 32, S633–S639. [Google Scholar]
- Vallecillo, G.; Anguera, M.; Martin, N.; Robles, M.J. Effectiveness of an acute care for elders unit at a long-term care facility for frail older patients with COVID-19. Geriatr. Nurs. 2021, 42, 544–547. [Google Scholar] [CrossRef]
- Vanhems, P.; Gustin, M.P.; Elias, C.; Henaff, L.; Dananché, C.; Grisi, B.; Marion, E.; Khanafer, N.; Hilliquin, D.; Gardes, S.; et al. Factors associated with admission to intensive care units in COVID-19 patients in Lyon-France. PLoS ONE 2021, 16, e0243709. [Google Scholar] [CrossRef]
- Venturini, S.; Orso, D.; Cugini, F.; Crapis, M.; Fossati, S.; Callegari, A.; Pellis, T.; Tonizzo, M.; Grembiale, A.; Rosso, A.; et al. Classification and analysis of outcome predictors in non-critically ill COVID-19 patients. Intern. Med. J. 2021, 51, 506–514. [Google Scholar] [CrossRef]
- Vera-Zertuche, J.M.; Mancilla-Galindo, J.; Tlalpa-Prisco, M.; Aguilar-Alonso, P.; Aguirre-García, M.M.; Segura-Badilla, O.; Lazcano-Hernández, M.; Rocha-González, H.I.; Navarro-Cruz, A.R.; Kammar-García, A.; et al. Obesity is a strong risk factor for short-term mortality and adverse outcomes in mexican patients with COVID-19: A national observational study. Epidemiol. Infect. 2021, 149, e109. [Google Scholar] [CrossRef]
- Verity, R.; Okell, L.C.; Dorigatti, I.; Winskill, P.; Whittaker, C.; Imai, N.; Cuomo-Dannenburg, G.; Thompson, H.; Walker, P.G.T.; Fu, H.; et al. Estimates of the severity of coronavirus disease 2019: A model-based analysis. Lancet Infect. Dis. 2020, 20, 669–677. [Google Scholar] [CrossRef]
- Verma, S.; Lumba, R.; Dapul, H.M.; Gold-von Simson, G.; Phoon, C.K.; Lighter, J.L.; Farkas, J.S.; Vinci, A.; Noor, A.; Raabe, V.N.; et al. Characteristics of hospitalized children with SARS-CoV-2 in the New York City metropolitan area. Hosp. Pediatr. 2021, 11, 71–78. [Google Scholar] [CrossRef]
- Viana-Llamas, M.C.; Arroyo-Espliguero, R.; Silva-Obregón, J.A.; Uribe-Heredia, G.; Núñez-Gil, I.; García-Magallón, B.; Torán-Martínez, C.G.; Castillo-Sandoval, A.; Díaz-Caraballo, E.; Rodríguez-Guinea, I.; et al. Hypoalbuminemia on admission in COVID-19 infection: An early predictor of mortality and adverse events. A retrospective observational study. Med. Clin. 2021, 156, 428–436. [Google Scholar] [CrossRef]
- Villa, L.; Krüger, T.; Seikrit, C.; Mühlfeld, A.S.; Kunter, U.; Werner, C.; Kleines, M.; Schulze-Hagen, M.; Dreher, M.; Kersten, A.; et al. Time on previous renal replacement therapy is associated with worse outcomes of COVID-19 in a regional cohort of kidney transplant and dialysis patients. Medicine 2021, 100, e24893. [Google Scholar] [CrossRef]
- Vizcarra, P.; Pérez-Elías, M.J.; Quereda, C.; Moreno, A.; Vivancos, M.J.; Dronda, F.; Casado, J.L.; COVID-19 ID Team. Description of COVID-19 in HIV-infected individuals: A single-centre, prospective cohort. Lancet HIV 2020, 7, e554–e564. [Google Scholar] [CrossRef]
- Vrillon, A.; Mhanna, E.; Aveneau, C.; Lebozec, M.; Grosset, L.; Nankam, D.; Albuquerque, F.; Razou Feroldi, R.; Maakaroun, B.; Pissareva, I.; et al. COVID-19 in adults with dementia: Clinical features and risk factors of mortality-a clinical cohort study on 125 patients. Alzheimers Res. Ther. 2021, 13, 77. [Google Scholar] [CrossRef]
- Vrotsou, K.; Rotaeche, R.; Mateo-Abad, M.; Machón, M.; Vergara, I. Variables associated with COVID-19 severity: An observational study of non-paediatric confirmed cases from the general population of the Basque country, Spain. BMJ Open 2021, 11, e049066. [Google Scholar] [CrossRef]
- Vu, C.A.; DeRonde, K.J.; Vega, A.D.; Maxam, M.; Holt, G.; Natori, Y.; Zamora, J.G.; Salazar, V.; Boatwright, R.; Morris, S.R.; et al. Effects of tocilizumab in COVID-19 patients: A cohort study. BMC Infect. Dis. 2020, 20, 964. [Google Scholar] [CrossRef]
- Wan, S.; Xiang, Y.; Fang, W.; Zheng, Y.; Li, B.; Hu, Y.; Lang, C.; Huang, D.; Sun, Q.; Xiong, Y.; et al. Clinical features and treatment of COVID-19 patients in northeast Chongqing. J. Med. Virol. 2020, 92, 797–806. [Google Scholar] [CrossRef]
- Wang, D.; Yin, Y.; Hu, C.; Liu, X.; Zhang, X.; Zhou, S.; Jian, M.; Xu, H.; Prowle, J.; Hu, B.; et al. Clinical course and outcome of 107 patients infected with the novel coronavirus, SARS-CoV-2, discharged from two hospitals in Wuhan, China. Crit. Care 2020, 24, 188. [Google Scholar] [CrossRef]
- Wang, F.; Cao, J.; Yu, Y.; Ding, J.; Eshak, E.S.; Liu, K.; Mubarik, S.; Shi, F.; Wen, H.; Zeng, Z.; et al. Epidemiological characteristics of patients with severe COVID-19 infection in Wuhan, China: Evidence from a retrospective observational study. Int. J. Epidemiol. 2021, 49, 1940–1950. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Qu, M.; Zhou, X.; Zhao, K.; Lai, C.; Tang, Q.; Xian, W.; Chen, R.; Li, X.; Li, Z.; et al. The timeline and risk factors of clinical progression of COVID-19 in Shenzhen, China. J. Transl. Med. 2020, 18, 270. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Luo, F.M.; Liu, D.; Liu, J.S.; Wang, Y.; Chen, H.; Tian, P.W.; Fan, T.; Tang, L.; Yu, H.; et al. Differences in the clinical characteristics and outcomes of COVID-19 patients in the epicenter and peripheral areas of the pandemic from China: A retrospective, large-sample, comparative analysis. BMC Infect. Dis. 2021, 21, 206. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Zhang, Q.; Zhao, X.; Dong, H.; Wu, C.; Wu, F.; Yu, B.; Lv, J.; Zhang, S.; Wu, G.; et al. Low high-density lipoprotein level is correlated with the severity of COVID-19 patients: An observational study. Lipids Health Dis. 2020, 19, 204. [Google Scholar] [CrossRef]
- Wang, J.; Guo, S.; Zhang, Y.; Gao, K.; Zuo, J.; Tan, N.; Du, K.; Ma, Y.; Hou, Y.; Li, Q.; et al. Clinical features and risk factors for severe inpatients with COVID-19: A retrospective study in China. PLoS ONE 2020, 15, e0244125. [Google Scholar] [CrossRef]
- Wang, J.; Xu, Z.; Wang, J.; Feng, R.; An, Y.; Ao, W.; Gao, Y.; Wang, X.; Xie, Z. CT characteristics of patients infected with 2019 novel coronavirus: Association with clinical type. Clin. Radiol. 2020, 75, 408–414. [Google Scholar] [CrossRef]
- Wang, J.; Zhang, H.; Qiao, R.; Ge, Q.; Zhang, S.; Zhao, Z.; Tian, C.; Ma, Q.; Shen, N. Thrombo-inflammatory features predicting mortality in patients with COVID-19: The FAD-85 score. J. Int. Med. Res. 2020, 48, 300060520955037. [Google Scholar] [CrossRef]
- Wang, J.; Zhu, L.; Xue, L.; Liu, L.; Yan, X.; Yan, X.; Huang, S.; Zhang, B.; Xu, T.; Li, C.; et al. Risk factors of liver injury in patients with coronavirus disease 2019 in Jiangsu, China: A retrospective, multi-center study. J. Med. Virol. 2021, 93, 3305–3311. [Google Scholar] [CrossRef]
- Wang, L.; He, W.; Yu, X.; Hu, D.; Bao, M.; Liu, H.; Zhou, J.; Jiang, H. Coronavirus disease 2019 in elderly patients: Characteristics and prognostic factors based on 4-week follow-up. J. Infect. 2020, 80, 639–645. [Google Scholar] [CrossRef]
- Wang, P.; Sha, J.; Meng, M.; Wang, C.; Yao, Q.; Zhang, Z.; Sun, W.; Wang, X.; Qie, G.; Bai, X.; et al. Risk factors for severe COVID-19 in middle-aged patients without comorbidities: A multicentre retrospective study. J. Transl. Med. 2020, 18, 461. [Google Scholar] [CrossRef]
- Wang, S.; Chen, Z.; Lin, Y.; Lin, L.; Lin, Q.; Fang, S.; Shi, Y.; Zhuang, X.; Ye, Y.; Wang, T.; et al. Clinical characteristics of 199 discharged patients with COVID-19 in Fujian province: A multicenter retrospective study between 22 January and 27 February 2020. PLoS ONE 2020, 15, e0242307. [Google Scholar] [CrossRef]
- Wang, S.; Ma, P.; Zhang, S.; Song, S.; Wang, Z.; Ma, Y.; Xu, J.; Wu, F.; Duan, L.; Yin, Z.; et al. Fasting blood glucose at admission is an independent predictor for 28-day mortality in patients with COVID-19 without previous diagnosis of diabetes: A multi-centre retrospective study. Diabetologia 2020, 63, 2102–2111. [Google Scholar] [CrossRef]
- Wang, T.; Tang, C.; Chen, R.; Ruan, H.; Liang, W.; Guan, W.; Sang, L.; Tang, R.; Zhong, N.; Li, S. Clinical features of coronavirus disease 2019 patients with mechanical ventilation: A nationwide study in China. Crit. Care Med. 2020, 48, e809–e812. [Google Scholar] [CrossRef]
- Wang, W.; Chen, L.; He, Q.; Wang, M.; Liu, M.; Deng, T.; Deng, X.; Yang, J.; Jiang, O.; Li, R.; et al. Clinical characteristics of inpatients with coronavirus disease 2019 (COVID-19) in Sichuan province. BMC Infect. Dis. 2021, 21, 155. [Google Scholar] [CrossRef]
- Wang, W.; Shen, M.; Tao, Y.; Fairley, C.K.; Zhong, Q.; Li, Z.; Chen, H.; Ong, J.J.; Zhang, D.; Zhang, K.; et al. Elevated glucose level leads to rapid COVID-19 progression and high fatality. BMC Pulm. Med. 2021, 21, 64. [Google Scholar] [CrossRef]
- Wang, X.; Fang, J.; Zhu, Y.; Chen, L.; Ding, F.; Zhou, R.; Ge, L.; Wang, F.; Chen, Q.; Zhang, Y.; et al. Clinical characteristics of non-critically ill patients with novel coronavirus infection (COVID-19) in a Fangcang hospital. Clin. Microbiol. Infect. 2020, 26, 1063–1068. [Google Scholar] [CrossRef]
- Wang, Y.; Luo, H.; Liu, S.; Hao, T.; Mortimer, K.; Yang, Y.; Wang, D.; Ju, S. Respiratory failure among patients with COVID-19 in Jiangsu province, China: A multicentre retrospective cohort study. Epidemiol. Infect. 2021, 149, e31. [Google Scholar] [CrossRef]
- Wang, Y.; Shu, H.; Liu, H.; Li, X.; Zhou, X.; Zou, X.; Pan, S.; Xu, J.; Xu, D.; Zhao, X.; et al. The peak levels of highly sensitive troponin I predicts in-hospital mortality in COVID-19 patients with cardiac injury: A retrospective study. Eur. Heart J. Acute Cardiovasc. Care 2021, 10, 6–15. [Google Scholar] [CrossRef]
- Wang, Y.; Yao, S.; Liu, X.; Cao, Y.; Wang, Y.; Xie, M. Risk factors of coronavirus disease 2019-related mortality and optimal treatment regimens: A retrospective study. Med. Sci. Monit. 2021, 27, e926751. [Google Scholar] [CrossRef]
- Wang, Y.; Zhou, Y.; Yang, Z.; Xia, D.; Hu, Y.; Geng, S. Clinical characteristics of patients with severe pneumonia caused by the SARS-CoV-2 in Wuhan, China. Respiration 2020, 99, 649–657. [Google Scholar] [CrossRef]
- Wang, Z.; Ye, D.; Wang, M.; Zhao, M.; Li, D.; Ye, J.; Liu, J.; Xu, Y.; Zhang, J.; Pan, W.; et al. Clinical features of COVID-19 patients with different outcomes in Wuhan: A retrospective observational study. Biomed. Res. Int. 2020, 2020, 2138387. [Google Scholar] [CrossRef]
- Wang, Z.; Zheutlin, A.; Kao, Y.H.; Ayers, K.; Gross, S.; Kovatch, P.; Nirenberg, S.; Charney, A.; Nadkarni, G.; De Freitas, J.K.; et al. Hospitalised COVID-19 patients of the mount sinai health system: A retrospective observational study using the electronic medical records. BMJ Open 2020, 10, e040441. [Google Scholar] [CrossRef]
- Wargny, M.; Potier, L.; Gourdy, P.; Pichelin, M.; Amadou, C.; Benhamou, P.Y.; Bonnet, J.B.; Bordier, L.; Bourron, O.; Chaumeil, C.; et al. Predictors of hospital discharge and mortality in patients with diabetes and COVID-19: Updated results from the nationwide CORONADO study. Diabetologia 2021, 64, 778–794. [Google Scholar] [CrossRef]
- Webb, G.J.; Marjot, T.; Cook, J.A.; Aloman, C.; Armstrong, M.J.; Brenner, E.J.; Catana, M.A.; Cargill, T.; Dhanasekaran, R.; García-Juárez, I.; et al. Outcomes following SARS-CoV-2 infection in liver transplant recipients: An international registry study. Lancet Gastroenterol. Hepatol. 2020, 5, 1008–1016. [Google Scholar] [CrossRef]
- Wei, C.; Liu, Y.; Liu, Y.; Zhang, K.; Su, D.; Zhong, M.; Meng, X. Clinical characteristics and manifestations in older patients with COVID-19. BMC Geriatr. 2020, 20, 395. [Google Scholar] [CrossRef]
- Wei, X.; Su, J.; Yang, K.; Wei, J.; Wan, H.; Cao, X.; Tan, W.; Wang, H. Elevations of serum cancer biomarkers correlate with severity of COVID-19. J. Med. Virol. 2020, 92, 2036–2041. [Google Scholar] [CrossRef]
- Wei, X.; Zeng, W.; Su, J.; Wan, H.; Yu, X.; Cao, X.; Tan, W.; Wang, H. Hypolipidemia is associated with the severity of COVID-19. J. Clin. Lipidol. 2020, 14, 297–304. [Google Scholar] [CrossRef]
- Wei, Z.Y.; Qiao, R.; Chen, J.; Huang, J.; Wu, H.; Wang, W.J.; Yu, H.; Xu, J.; Wang, C.; Gu, C.H.; et al. The influence of pre-existing hypertension on coronavirus disease 2019 patients. Epidemiol. Infect. 2021, 149, e4. [Google Scholar] [CrossRef] [PubMed]
- Wen, X.S.; Jiang, D.; Gao, L.; Zhou, J.Z.; Xiao, J.; Cheng, X.C.; He, B.; Chen, Y.; Lei, P.; Tan, X.W.; et al. Clinical characteristics and predictive value of lower CD4(+)T cell level in patients with moderate and severe COVID-19: A multicenter retrospective study. BMC Infect. Dis. 2021, 21, 57. [Google Scholar] [CrossRef] [PubMed]
- Williams, M.; Mi, E.; Le Calvez, K.; Chen, J.; Pakzad-Shahabi, L.; Dadhania, S.; Wang, J.; Ho, A.; Rabinowicz, S. Estimating the risk of death from COVID-19 in adult cancer patients. Clin. Oncol. 2021, 33, e172–e179. [Google Scholar] [CrossRef] [PubMed]
- Wollenstein-Betech, S.; Silva, A.A.B.; Fleck, J.L.; Cassandras, C.G.; Paschalidis, I.C. Physiological and socioeconomic characteristics predict COVID-19 mortality and resource utilization in Brazil. PLoS ONE 2020, 15, e0240346. [Google Scholar] [CrossRef]
- Wu, C.; Chen, X.; Cai, Y.; Xia, J.; Zhou, X.; Xu, S.; Huang, H.; Zhang, L.; Zhou, X.; Du, C.; et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern. Med. 2020, 180, 934–943. [Google Scholar] [CrossRef] [Green Version]
- Wu, F.; Zhou, Y.; Wang, Z.; Xie, M.; Shi, Z.; Tang, Z.; Li, X.; Li, X.; Lei, C.; Li, Y.; et al. Clinical characteristics of COVID-19 infection in chronic obstructive pulmonary disease: A multicenter, retrospective, observational study. J. Thorac. Dis. 2020, 12, 1811–1823. [Google Scholar] [CrossRef]
- Wu, J.; Li, W.; Shi, X.; Chen, Z.; Jiang, B.; Liu, J.; Wang, D.; Liu, C.; Meng, Y.; Cui, L. Early antiviral treatment contributes to alleviate the severity and improve the prognosis of patients with novel coronavirus disease (COVID-19). J. Intern. Med. 2020, 288, 128–138. [Google Scholar] [CrossRef] [Green Version]
- Wu, M.; Ji, J.J.; Zhong, L.; Shao, Z.Y.; Xie, Q.F.; Liu, Z.Y.; Wang, C.L.; Su, L.; Feng, Y.W.; Liu, Z.F.; et al. Thymosin α1 therapy in critically ill patients with COVID-19: A multicenter retrospective cohort study. Int. Immunopharmacol. 2020, 88, 106873. [Google Scholar] [CrossRef]
- Xie, J.; Wu, W.; Li, S.; Hu, Y.; Hu, M.; Li, J.; Yang, Y.; Huang, T.; Zheng, K.; Wang, Y.; et al. Clinical characteristics and outcomes of critically ill patients with novel coronavirus infectious disease (COVID-19) in China: A retrospective multicenter study. Intensive Care Med. 2020, 46, 1863–1872. [Google Scholar] [CrossRef]
- Xie, Y.; You, Q.; Wu, C.; Cao, S.; Qu, G.; Yan, X.; Han, X.; Wang, C.; Zhang, H. Impact of cardiovascular disease on clinical characteristics and outcomes of coronavirus disease 2019 (COVID-19). Circ. J. 2020, 84, 1277–1283. [Google Scholar] [CrossRef]
- Xiong, F.; Tang, H.; Liu, L.; Tu, C.; Tian, J.B.; Lei, C.T.; Liu, J.; Dong, J.W.; Chen, W.L.; Wang, X.H.; et al. Clinical characteristics of and medical interventions for COVID-19 in hemodialysis patients in Wuhan, China. J. Am. Soc. Nephrol. 2020, 31, 1387–1397. [Google Scholar] [CrossRef]
- Xiong, S.; Liu, L.; Lin, F.; Shi, J.; Han, L.; Liu, H.; He, L.; Jiang, Q.; Wang, Z.; Fu, W.; et al. Clinical characteristics of 116 hospitalized patients with COVID-19 in Wuhan, China: A single-centered, retrospective, observational study. BMC Infect. Dis. 2020, 20, 787. [Google Scholar] [CrossRef]
- Xu, B.; Fan, C.; Wang, A.; Zou, Y.; Yu, Y.; He, C.; Xia, W.; Zhang, J.; Miao, Q. Suppressed T cell-mediated immunity in patients with COVID-19: A clinical retrospective study in Wuhan, China. J. Infect. 2020, 81, e51–e60. [Google Scholar] [CrossRef]
- Xu, J.; Xie, J.; Du, B.; Tong, Z.; Qiu, H.; Bagshaw, S.M. Clinical characteristics and outcomes of patients with severe COVID-19 induced acute kidney injury. J. Intensive Care Med. 2021, 36, 319–326. [Google Scholar] [CrossRef]
- Xu, J.; Yang, X.; Yang, L.; Zou, X.; Wang, Y.; Wu, Y.; Zhou, T.; Yuan, Y.; Qi, H.; Fu, S.; et al. Clinical course and predictors of 60-day mortality in 239 critically ill patients with COVID-19: A multicenter retrospective study from Wuhan, China. Crit. Care 2020, 24, 394. [Google Scholar] [CrossRef]
- Xu, P.P.; Tian, R.H.; Luo, S.; Zu, Z.Y.; Fan, B.; Wang, X.M.; Xu, K.; Wang, J.T.; Zhu, J.; Shi, J.C.; et al. Risk factors for adverse clinical outcomes with COVID-19 in China: A multicenter, retrospective, observational study. Theranostics 2020, 10, 6372–6383. [Google Scholar] [CrossRef]
- Yan, C.; Chang, Y.; Yu, H.; Xu, J.; Huang, C.; Yang, M.; Wang, Y.; Wang, D.; Yu, T.; Wei, S.; et al. Clinical factors and quantitative CT parameters associated with ICU admission in patients of COVID-19 pneumonia: A multicenter study. Front. Public Health 2021, 9, 648360. [Google Scholar] [CrossRef]
- Yan, Q.; Zuo, P.; Cheng, L.; Li, Y.; Song, K.; Chen, Y.; Dai, Y.; Yang, Y.; Zhou, L.; Yu, W.; et al. Acute kidney injury is associated with in-hospital mortality in older patients with COVID-19. J. Gerontol. A Biol. Sci. Med. Sci. 2021, 76, 456–462. [Google Scholar] [CrossRef] [PubMed]
- Yan, Y.; Yang, Y.; Wang, F.; Ren, H.; Zhang, S.; Shi, X.; Yu, X.; Dong, K. Clinical characteristics and outcomes of patients with severe covid-19 with diabetes. BMJ Open Diabetes Res. Care 2020, 8, e001343. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.; Liu, F.; Liu, W.; Cao, G.; Liu, J.; Huang, S.; Zhu, M.; Tu, C.; Wang, J.; Xiong, B. Myocardial injury and risk factors for mortality in patients with COVID-19 pneumonia. Int. J. Cardiol. 2021, 326, 230–236. [Google Scholar] [CrossRef] [PubMed]
- Yang, D.; Xiao, Y.; Chen, J.; Chen, Y.; Luo, P.; Liu, Q.; Yang, C.; Xiong, M.; Zhang, Y.; Liu, X. COVID-19 and chronic renal disease: Clinical characteristics and prognosis. QJM 2020, 113, 799–805. [Google Scholar] [CrossRef]
- Yang, G.; Tan, Z.; Zhou, L.; Yang, M.; Peng, L.; Liu, J.; Cai, J.; Yang, R.; Han, J.; Huang, Y.; et al. Effects of ARBs and ACEIs on Virus Infection, Inflammatory Status and Clinical Outcomes in COVID-19 Patients with Hypertension: A Single Center Retrospective Study. Hypertension 2020, 76, 51–58. [Google Scholar] [CrossRef]
- Yang, K.; Sheng, Y.; Huang, C.; Jin, Y.; Xiong, N.; Jiang, K.; Lu, H.; Liu, J.; Yang, J.; Dong, Y.; et al. Clinical characteristics, outcomes, and risk factors for mortality in patients with cancer and COVID-19 in Hubei, China: A multicentre, retrospective, cohort study. Lancet Oncol. 2020, 21, 904–913. [Google Scholar] [CrossRef]
- Yang, Q.; Xie, L.; Zhang, W.; Zhao, L.; Wu, H.; Jiang, J.; Zou, J.; Liu, J.; Wu, J.; Chen, Y.; et al. Analysis of the clinical characteristics, drug treatments and prognoses of 136 patients with coronavirus disease 2019. J. Clin. Pharm. Ther. 2020, 45, 609–616. [Google Scholar] [CrossRef]
- Yang, R.; Gui, X.; Zhang, Y.; Xiong, Y. The role of essential organ-based comorbidities in the prognosis of COVID-19 infection patients. Expert Rev. Respir. Med. 2020, 14, 835–838. [Google Scholar] [CrossRef]
- Yang, X.; Yang, Q.; Wang, Y.; Wu, Y.; Xu, J.; Yu, Y.; Shang, Y. Thrombocytopenia and its association with mortality in patients with COVID-19. J. Thromb. Haemost. 2020, 18, 1469–1472. [Google Scholar] [CrossRef]
- Yao, Q.; Wang, P.; Wang, X.; Qie, G.; Meng, M.; Tong, X.; Bai, X.; Ding, M.; Liu, W.; Liu, K.; et al. Retrospective study of risk factors for severe SARS-Cov-2 infections in hospitalized adult patients. Pol. Arch. Intern. Med. 2020, 130, 390–399. [Google Scholar] [CrossRef] [Green Version]
- Yarza, R.; Bover, M.; Paredes, D.; López-López, F.; Jara-Casas, D.; Castelo-Loureiro, A.; Baena, J.; Mazarico, J.M.; Folgueira, M.D.; Meléndez-Carmona, M.Á.; et al. SARS-CoV-2 infection in cancer patients undergoing active treatment: Analysis of clinical features and predictive factors for severe respiratory failure and death. Eur. J. Cancer 2020, 135, 242–250. [Google Scholar] [CrossRef]
- Yayla, B.C.C.; Aykac, K.; Ozsurekci, Y.; Ceyhan, M. Characteristics and management of children with COVID-19 in a tertiary care hospital in Turkey. Clin. Pediatr. 2021, 60, 170–177. [Google Scholar] [CrossRef]
- Yehia, B.R.; Winegar, A.; Fogel, R.; Fakih, M.; Ottenbacher, A.; Jesser, C.; Bufalino, A.; Huang, R.; Cacchione, J. Association of race with mortality among patients hospitalized with coronavirus disease 2019 (COVID-19) at 92 US hospitals. JAMA Netw. Open 2020, 3, e2018039. [Google Scholar] [CrossRef]
- Yu, C.; Lei, Q.; Li, W.; Wang, X.; Liu, W.; Fan, X.; Li, W. Clinical characteristics, associated factors, and predicting COVID-19 mortality risk: A retrospective study in Wuhan, China. Am. J. Prev. Med. 2020, 59, 168–175. [Google Scholar] [CrossRef]
- Yu, X.; Sun, X.; Cui, P.; Pan, H.; Lin, S.; Han, R.; Jiang, C.; Fang, Q.; Kong, D.; Zhu, Y.; et al. Epidemiological and Clinical Characteristics of 333 Confirmed Cases with Coronavirus Disease 2019 in Shanghai, China. Transbound. Emerg. Dis. 2020, 67, 1697–1707. [Google Scholar] [CrossRef]
- Yu, Y.; Liu, T.; Shao, L.; Li, X.; He, C.K.; Jamal, M.; Luo, Y.; Wang, Y.; Liu, Y.; Shang, Y.; et al. Novel biomarkers for the prediction of COVID-19 progression a retrospective, multi-center cohort study. Virulence 2020, 11, 1569–1581. [Google Scholar] [CrossRef]
- Dong, Y.; Mo, X.; Hu, Y.; Qi, X.; Jiang, F.; Jiang, Z.; Tong, S. Epidemiology of COVID-19 among children in China. Pediatrics 2020, 145, e20200702. [Google Scholar] [CrossRef] [Green Version]
- Yue, T.; Zhou, W.; He, J.; Wang, H.; Liu, Y.; Wang, B.; Zhu, Q.; Xia, H.; Hu, H. Combined clinical and imaging features better predict the critical outcomes of patients with SARS-COV-2. Medicine 2021, 100, e25083. [Google Scholar] [CrossRef]
- Zachariah, P.; Johnson, C.L.; Halabi, K.C.; Ahn, D.; Sen, A.I.; Fischer, A.; Banker, S.L.; Giordano, M.; Manice, C.S.; Diamond, R.; et al. Epidemiology, clinical features, and disease severity in patients with coronavirus disease 2019 (COVID-19) in a children’s hospital in New York City, New York. JAMA Pediatr. 2020, 174, e202430. [Google Scholar] [CrossRef]
- Zelner, J.; Trangucci, R.; Naraharisetti, R.; Cao, A.; Malosh, R.; Broen, K.; Masters, N.; Delamater, P. Racial disparities in coronavirus disease 2019 (COVID-19) mortality are driven by unequal infection risks. Clin. Infect. Dis. 2021, 72, e88–e95. [Google Scholar] [CrossRef]
- Zeng, H.; Lu, Q.; Yang, Q.; Wang, X.; Yue, D.; Zhang, L.; Li, H.; Liu, W.; Li, H. Longitudinal profile of laboratory parameters and their application in the prediction for fatal outcome among patients infected with SARS-CoV-2: A retrospective cohort study. Clin. Infect. Dis. 2021, 72, 626–633. [Google Scholar] [CrossRef]
- Zeng, Z.; Ma, Y.; Zeng, H.; Huang, P.; Liu, W.; Jiang, M.; Xiang, X.; Deng, D.; Liao, X.; Chen, P.; et al. Simple nomogram based on initial laboratory data for predicting the probability of ICU transfer of COVID-19 patients: Multicenter retrospective study. J. Med. Virol. 2021, 93, 434–440. [Google Scholar] [CrossRef]
- Zhang, G.; Zhang, J.; Wang, B.; Zhu, X.; Wang, Q.; Qiu, S. Analysis of clinical characteristics and laboratory findings of 95 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A retrospective analysis. Respir. Res. 2020, 21, 74. [Google Scholar] [CrossRef]
- Zhang, H.; Cao, X.; Kong, M.; Mao, X.; Huang, L.; He, P.; Pan, S.; Li, J.; Lu, Z. Clinical and hematological characteristics of 88 patients with COVID-19. Int. J. Lab. Hematol. 2020, 42, 780–787. [Google Scholar] [CrossRef]
- Zhang, H.; Wang, L.; Chen, Y.; Wu, Q.; Chen, G.; Shen, X.; Wang, Q.; Yan, Y.; Yu, Y.; Zhong, Y.; et al. Outcomes of novel coronavirus disease 2019 (COVID-19) infection in 107 patients with cancer from Wuhan, China. Cancer 2020, 126, 4023–4031. [Google Scholar] [CrossRef]
- Zhang, J.; Hao, Y.; Ou, W.; Ming, F.; Liang, G.; Qian, Y.; Cai, Q.; Dong, S.; Hu, S.; Wang, W.; et al. Serum interleukin-6 is an indicator for severity in 901 patients with SARS-CoV-2 infection: A cohort study. J. Transl. Med. 2020, 18, 406. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Liu, P.; Wang, M.; Wang, J.; Chen, J.; Yuan, W.; Li, M.; Xie, Z.; Dong, W.; Li, H.; et al. The clinical data from 19 critically ill patients with coronavirus disease 2019: A single-centered, retrospective, observational study. J. Public Health 2020, 21, 361–364. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Fan, T.; Yang, S.; Feng, H.; Hao, B.; Lu, Z.; Xiong, R.; Shen, X.; Jiang, W.; Wang, W.; et al. Comparison of clinical characteristics of COVID-19 between elderly patients and young patients: A study based on a 28-day follow-up. Aging 2020, 12, 19898–19910. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Sun, W.; Wang, Y.; Wang, X.; Liu, Y.; Zhao, S.; Long, D.; Chen, L.; Yu, L. Clinical course and mortality of stroke patients with coronavirus disease 2019 in Wuhan, China. Stroke 2020, 51, 2674–2682. [Google Scholar] [CrossRef]
- Zhang, L.; Zhu, F.; Xie, L.; Wang, C.; Wang, J.; Chen, R.; Jia, P.; Guan, H.Q.; Peng, L.; Chen, Y.; et al. Clinical characteristics of COVID-19-infected cancer patients: A retrospective case study in three hospitals within Wuhan, China. Ann. Oncol. 2020, 31, 894–901. [Google Scholar] [CrossRef]
- Zhang, N.; Wang, C.; Zhu, F.; Mao, H.; Bai, P.; Chen, L.L.; Zeng, T.; Peng, M.M.; Qiu, K.L.; Wang, Y.; et al. Risk factors for poor outcomes of diabetes patients with COVID-19: A single-center, retrospective study in early outbreak in China. Front. Endocrinol. 2020, 11, 571037. [Google Scholar] [CrossRef]
- Zhang, N.; Xu, X.; Zhou, L.Y.; Chen, G.; Li, Y.; Yin, H.; Sun, Z. Clinical characteristics and chest CT imaging features of critically ill COVID-19 patients. Eur. Radiol. 2020, 30, 6151–6160. [Google Scholar] [CrossRef]
- Zhang, N.; Zhang, H.; Tang, Y.; Zhang, H.; Ma, A.; Xu, F.; Sun, Y.; Jiang, L.; Shan, F. Risk factors for illness severity in patients with COVID-19 pneumonia: A prospective cohort study. Int. J. Med. Sci. 2021, 18, 921–928. [Google Scholar] [CrossRef]
- Zhang, Q.; Wei, Y.; Chen, M.; Wan, Q.; Chen, X. Clinical analysis of risk factors for severe COVID-19 patients with type 2 diabetes. J. Diabetes Complicat. 2020, 34, 107666. [Google Scholar] [CrossRef]
- Zhang, R.; Ouyang, H.; Fu, L.; Wang, S.; Han, J.; Huang, K.; Jia, M.; Song, Q.; Fu, Z. CT features of SARS-CoV-2 pneumonia according to clinical presentation: A retrospective analysis of 120 consecutive patients from Wuhan city. Eur. Radiol. 2020, 30, 4417–4426. [Google Scholar] [CrossRef] [Green Version]
- Zhang, S.; Guo, M.; Duan, L.; Wu, F.; Hu, G.; Wang, Z.; Huang, Q.; Liao, T.; Xu, J.; Ma, Y.; et al. Development and validation of a risk factor-based system to predict short-term survival in adult hospitalized patients with COVID-19: A multicenter, retrospective, cohort study. Crit. Care 2020, 24, 438. [Google Scholar] [CrossRef]
- Zhang, W.; Li, C.; Xu, Y.; He, B.; Hu, M.; Cao, G.; Li, L.; Wu, S.; Wang, X.; Zhang, C.; et al. Hyperglycemia and correlated high levels of inflammation have a positive relationship with the severity of coronavirus disease 2019. Mediat. Inflamm. 2021, 2021, 8812304. [Google Scholar] [CrossRef]
- Zhang, Y.; Sha, T.; Wu, F.; Hu, H.; Chen, Z.; Li, H.; Han, J.; Song, W.; Huang, Q.; Zeng, Z. Hypertension in patients hospitalized with COVID-19 in Wuhan, China. Int. Heart J. 2021, 62, 337–343. [Google Scholar] [CrossRef]
- Zhang, Y.; Zheng, L.; Liu, L.; Zhao, M.; Xiao, J.; Zhao, Q. Liver impairment in COVID-19 patients: A retrospective analysis of 115 cases from a single centre in Wuhan city, China. Liver Int. 2020, 40, 2095–2103. [Google Scholar] [CrossRef] [Green Version]
- Zhao, J.; Zhu, M.; Su, X.; Huang, M.; Yang, Y.; Huang, J.; Songshi, N.; Cao, Q.; Gu, Q.; Li, J.; et al. Clinical features and risk factors for severe-critically ill COVID-19 adult patients in Jiangsu, China: A multiple-centered, retrospective study. Medicine 2021, 100, e24332. [Google Scholar] [CrossRef]
- Zhao, M.; Wang, M.; Zhangm, J.; Gu, J.; Zhang, P.; Xu, Y.; Ye, J.; Wang, Z.; Ye, D.; Pan, W.; et al. Comparison of clinical characteristics and outcomes of patients with coronavirus disease 2019 at different ages. Aging 2020, 12, 10070–10086. [Google Scholar] [CrossRef]
- Zhao, X.; Li, Y.; Ge, Y.; Shi, Y.; Lv, P.; Zhang, J.; Fu, G.; Zhou, Y.; Jiang, K.; Lin, N.; et al. Evaluation of nutrition risk and its association with mortality risk in severely and critically ill COVID-19 patients. JPEN J. Parenter. Enteral Nutr. 2021, 45, 32–42. [Google Scholar] [CrossRef]
- Zhao, Y.; Nie, H.X.; Hu, K.; Wu, X.J.; Zhang, Y.T.; Wang, M.M.; Wang, T.; Zheng, Z.S.; Li, X.C.; Zeng, S.L. Abnormal immunity of non-survivors with COVID-19: Predictors for mortality. Infect. Dis. Poverty 2020, 9, 108. [Google Scholar] [CrossRef]
- Zheng, B.; Cai, Y.; Zeng, F.; Lin, M.; Zheng, J.; Chen, W.; Qin, G.; Guo, Y. An interpretable model-based prediction of severity and crucial factors in patients with COVID-19. Biomed. Res. Int. 2021, 2021, 8840835. [Google Scholar] [CrossRef]
- Zheng, K.I.; Gao, F.; Wang, X.B.; Sun, Q.F.; Pan, K.H.; Wang, T.Y.; Ma, H.L.; Chen, Y.P.; Liu, W.Y.; George, J.; et al. Obesity as a risk factor for greater severity of COVID-19 in patients with metabolic associated fatty liver disease. Metabolism 2020, 108, 154244. [Google Scholar] [CrossRef]
- Zheng, T.; Yang, C.; Wang, H.Y.; Chen, X.; Yu, L.; Wu, Z.L.; Sun, H. Clinical Characteristics and Outcomes of COVID-19 Patients with Gastrointestinal Symptoms Admitted to Jianghan Fangcang Shelter Hospital in Wuhan, China. J. Med. Virol. 2020, 92, 2735–2741. [Google Scholar] [CrossRef]
- Zhong, Y.; Zhao, L.; Wu, G.; Hu, C.; Wu, C.; Xu, M.; Dong, H.; Zhang, Q.; Wang, G.; Yu, B.; et al. Impact of renin-angiotensin system inhibitors use on mortality in severe COVID-19 patients with hypertension: A retrospective observational study. J. Int. Med. Res. 2020, 48, 300060520979151. [Google Scholar] [CrossRef] [PubMed]
- Zhou, J.; Chen, B.; Wang, Y.; Wu, F. Epidemiological and clinical characteristics of 217 cases of COVID-19 in Jiangsu province, China. Med. Sci. Monit. 2021, 27, e930853. [Google Scholar] [CrossRef] [PubMed]
- Zhou, J.; Ma, Y.; Liu, Y.; Xiang, Y.; Tao, C.; Yu, H.; Huang, J. A correlation analysis between the nutritional status and prognosis of COVID-19 patients. J. Nutr. Health Aging 2021, 25, 84–93. [Google Scholar] [CrossRef]
- Zhou, S.; Mi, S.; Luo, S.; Wang, Y.; Ren, B.; Cai, L.; Wu, M. Risk factors for mortality in 220 patients with COVID-19 in Wuhan, China: A single-center, retrospective study. Ear Nose Throat J. 2021, 100, 140S–147S. [Google Scholar] [CrossRef]
- Zhou, W.; Liu, Y.; Xu, B.; Wang, S.; Li, S.; Liu, H.; Huang, Z.; Luo, Y.; Hu, M.; Wu, W.; et al. Early identification of patients with severe COVID-19 at increased risk of in-hospital death: A multicenter case-control study in Wuhan. J. Thorac. Dis. 2021, 13, 1380–1395. [Google Scholar] [CrossRef]
- Zhou, Y.; He, Y.; Yang, H.; Yu, H.; Wang, T.; Chen, Z.; Yao, R.; Liang, Z. Development and validation a nomogram for predicting the risk of severe COVID-19: A multi-center study in Sichuan, China. PLoS ONE 2020, 15, e0233328. [Google Scholar] [CrossRef]
- Zhou, Y.; He, Y.; Yang, H.; Yu, H.; Wang, T.; Chen, Z.; Yao, R.; Liang, Z. Exploiting an early warning nomogram for predicting the risk of ICU admission in patients with COVID-19: A multi-center study in China. Scand. J. Trauma Resusc. Emerg, Med. 2020, 28, 106. [Google Scholar] [CrossRef]
- Zhu, B.; Jin, S.; Wu, L.; Hu, C.; Wang, Z.; Bu, L.; Sun, H.; Wang, X.; Qu, S.; Chen, D. J-shaped association between fasting blood glucose levels and COVID-19 severity in patients without diabetes. Diabetes Res. Clin. Pract. 2020, 168, 108381. [Google Scholar] [CrossRef]
- Zhu, Y.; Zhang, J.; Li, Y.; Liu, F.; Zhou, Q.; Peng, Z. Association between thrombocytopenia and 180-day prognosis of COVID-19 patients in intensive care units: A two-center observational study. PLoS ONE 2021, 16, e0248671. [Google Scholar] [CrossRef]
- Zieleskiewicz, L.; Markarian, T.; Lopez, A.; Taguet, C.; Mohammedi, N.; Boucekine, M.; Baumstarck, K.; Besch, G.; Mathon, G.; Duclos, G.; et al. Comparative study of lung ultrasound and chest computed tomography scan in the assessment of severity of confirmed COVID-19 pneumonia. Intensive Care Med. 2020, 46, 1707–1713. [Google Scholar] [CrossRef] [PubMed]
- Zou, X.; Li, S.; Fang, M.; Hu, M.; Bian, Y.; Ling, J.; Yu, S.; Jing, L.; Li, D.; Huang, J. Acute physiology and chronic health evaluation II score as a predictor of hospital mortality in patients of coronavirus disease 2019. Crit. Care Med. 2020, 48, e657–e665. [Google Scholar] [CrossRef]
- Zou, Y.; Guo, H.; Zhang, Y.; Zhang, Z.; Liu, Y.; Wang, J.; Lu, H.; Qian, Z. Analysis of coagulation parameters in patients with COVID-19 in Shanghai, China. Biosci. Trends. 2020, 14, 285–289. [Google Scholar] [CrossRef]
- Zuniga, M.; Moreno-Moral, A.; Ocana-Granados, A.; Padilla-Moreno, F.A.; Castillo-Fernández, A.M.; Guillamón-Fernández, D.; Ramírez-Sánchez, C.; Sanchez-Palop, M.; Martínez-Colmenero, J.; Pimentel-Villar, M.A.; et al. High-dose corticosteroid pulse therapy increases the survival rate in COVID-19 patients at risk of hyper-inflammatory response. PLoS ONE 2021, 16, e0243964. [Google Scholar]
- Zuo, P.; Tong, S.; Yan, Q.; Cheng, L.; Li, Y.; Song, K.; Chen, Y.; Dai, Y.; Gao, H.; Zhang, C. Decreased prealbumin level is associated with increased risk for mortality in elderly hospitalized patients with COVID-19. Nutrition 2020, 78, 110930. [Google Scholar] [CrossRef]
- Odegaard, J.I.; Chawla, A. Connecting type 1 and type 2 diabetes through innate immunity. Cold Spring Harbor Perspect. Med. 2012, 2, a007724. [Google Scholar] [CrossRef]
- Bajaj, V.; Gadi, N.; Spihlman, A.P.; Wu, S.C.; Choi, C.H.; Moulton, V.R. Aging, Immunity and COVID-19: How Age Influences the Host Immune Response to Coronavirus Infections? Front. Physiol. 2021, 11, 571416. [Google Scholar] [CrossRef]
- Prasad, S.; Sung, B.; Aggarwal, B.B. Age-associated chronic diseases require age-old medicine: Role of chronic inflammation. Prev. Med. 2012, 54, S29–S37. [Google Scholar] [CrossRef] [Green Version]
- Banoun, H. Evolution of SARS-CoV-2: Review of Mutations, Role of the Host Immune System. Nephron 2021, 145, 392–403. [Google Scholar] [CrossRef]
- Rochman, N.D.; Wolf, Y.I.; Faure, G.; Mutz, P.; Zhang, F.; Koonin, E.V. Ongoing global and regional adaptive evolution of SARS-CoV-2. Proc. Natl. Acad. Sci. USA 2021, 118, e2104241118. [Google Scholar] [CrossRef]
- Markov, P.V.; Katzourakis, A.; Stilianakis, N.I. Antigenic evolution will lead to new SARS-CoV-2 variants with unpredictable severity. Nat. Rev. Microbiol. 2022, 20, 251–252. [Google Scholar] [CrossRef]
- Nikolaidis, M.; Markoulatos, P.; Van de Peer, Y.; Oliver, S.G.; Amoutzias, G.D. The Neighborhood of the Spike Gene Is a Hotspot for Modular Intertypic Homologous and Nonhomologous Recombination in Coronavirus Genomes. Mol. Biol. Evol. 2022, 39, msab292. [Google Scholar] [CrossRef] [PubMed]
- Nikolaidis, M.; Papakyriakou, A.; Chlichlia, K.; Markoulatos, P.; Oliver, S.G.; Amoutzias, G.D. Comparative Analysis of SARS-CoV-2 Variants of Concern, Including Omicron, Highlights Their Common and Distinctive Amino Acid Substitution Patterns, Especially at the Spike ORF. Viruses 2022, 14, 707. [Google Scholar] [CrossRef] [PubMed]
- Singh, J.; Pandit, P.; McArthur, A.G.; Banerjee, A.; Mossman, K. Evolutionary trajectory of SARS-CoV-2 and emerging variants. Virol. J. 2021, 18, 166. [Google Scholar] [CrossRef]
- Arora, P.; Rocha, C.; Kempf, A.; Nehlmeier, I.; Graichen, L.; Winkler, M.S.; Lier, M.; Schulz, S.; Jäck, H.M.; Cossmann, A.; et al. The spike protein of SARS-CoV-2 variant A.30 is heavily mutated and evades vaccine-induced antibodies with high efficiency. Cell. Mol. Immunol. 2021, 18, 2673–2675. [Google Scholar] [CrossRef]
- Bauchner, H.; Golub, R.M.; Zylke, J. Editorial Concern—Possible Reporting of the Same Patients with COVID-19 in Different Reports. JAMA 2020, 323, 1256. [Google Scholar] [CrossRef] [Green Version]
- Scientific Paper Claiming Smokers Less Likely to Acquire Covid Retracted over Tobacco Industry Links. Available online: https://www.theguardian.com/science/2021/apr/22/scientific-paper-claiming-smokers-less-likely-to-acquire-covid-retracted-over-tobacco-industry-links (accessed on 30 April 2022).
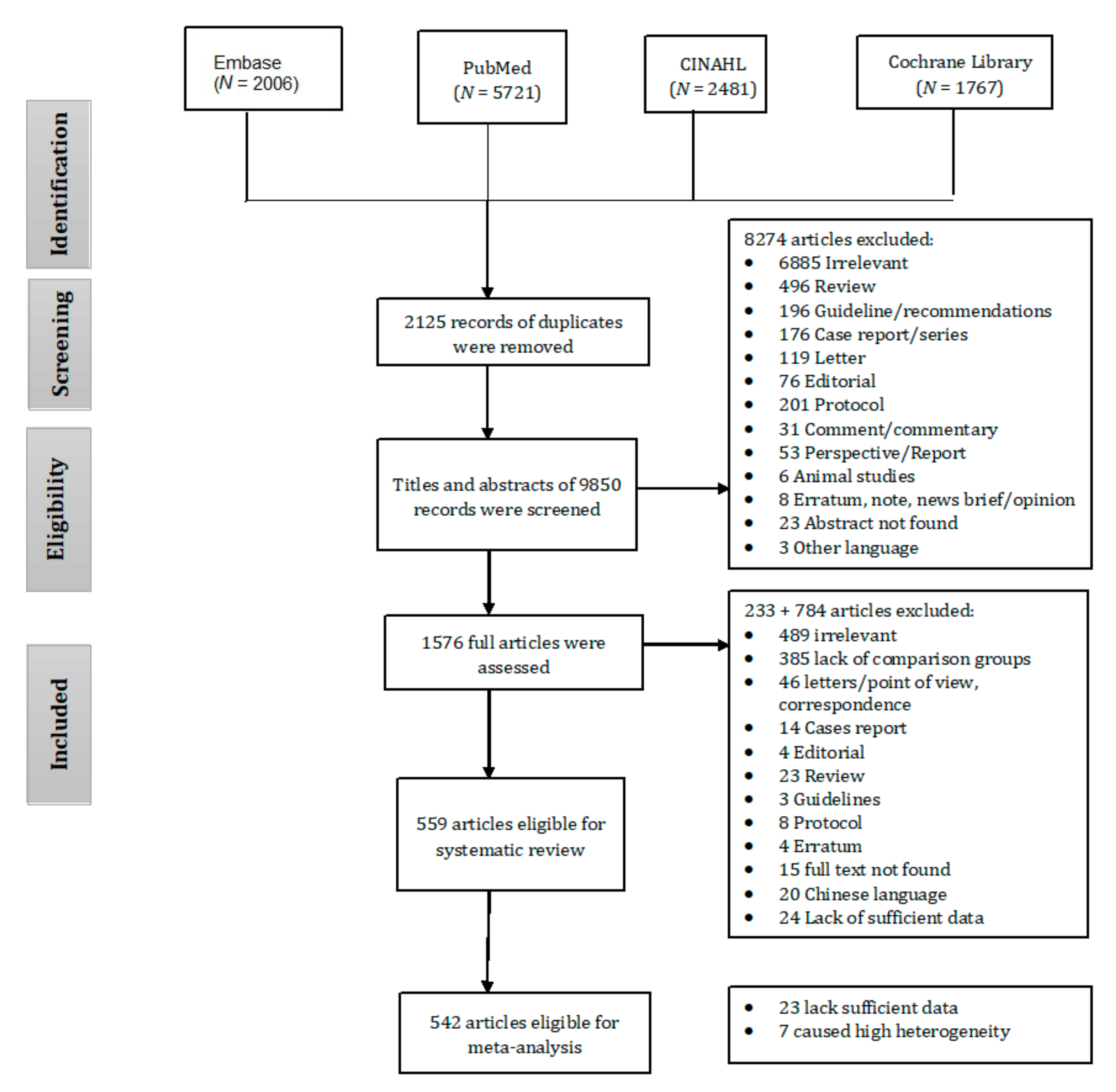
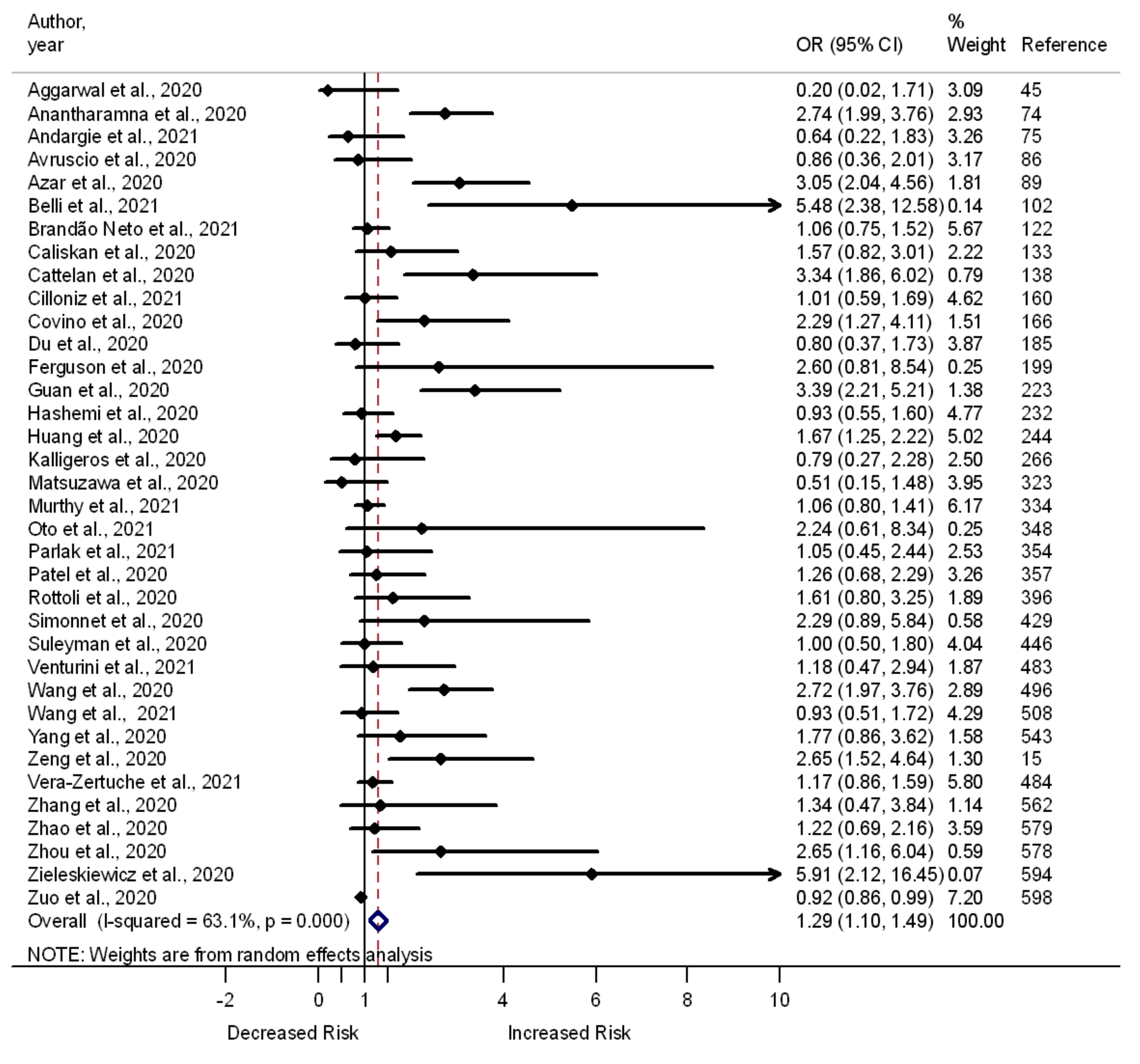
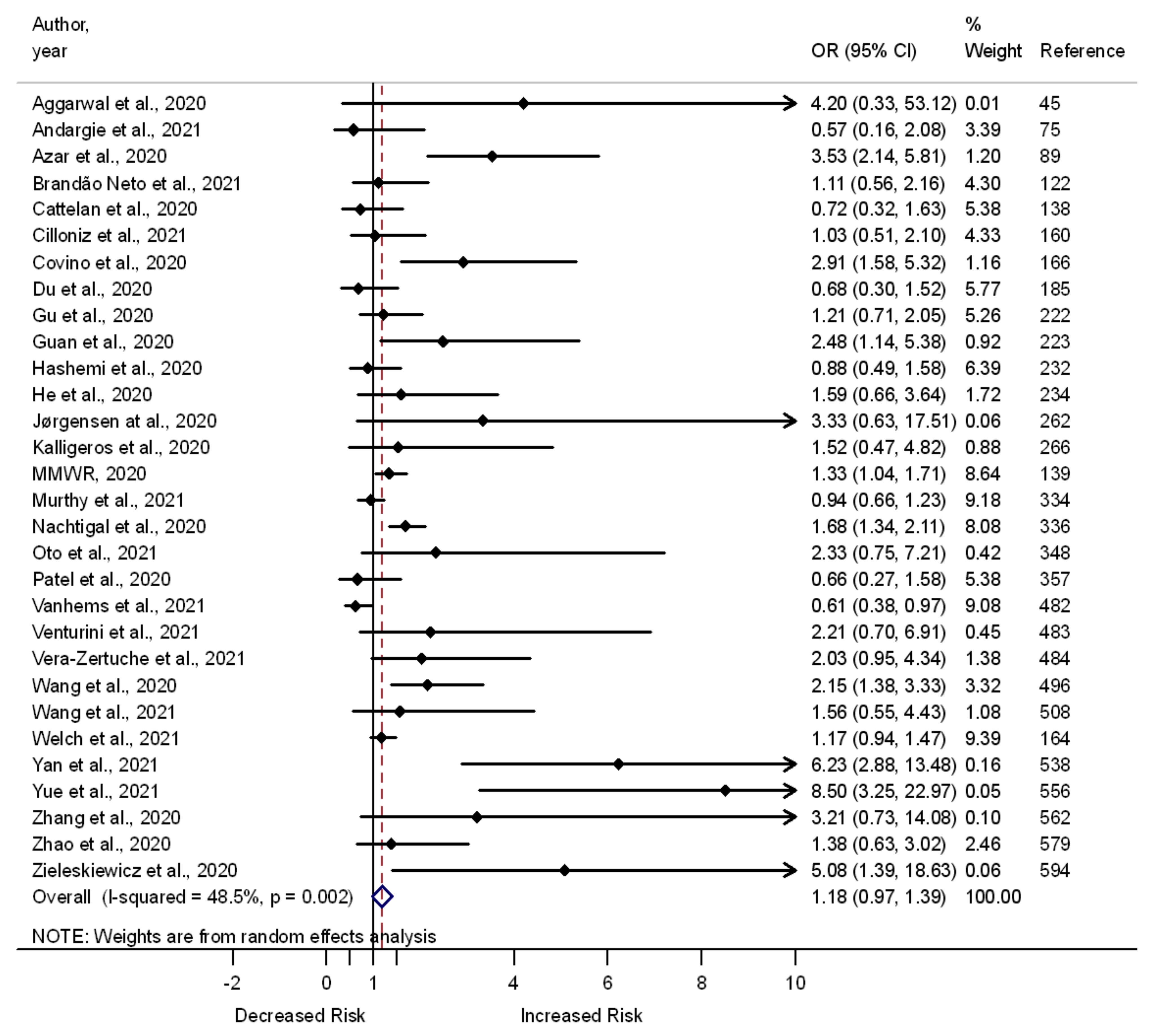
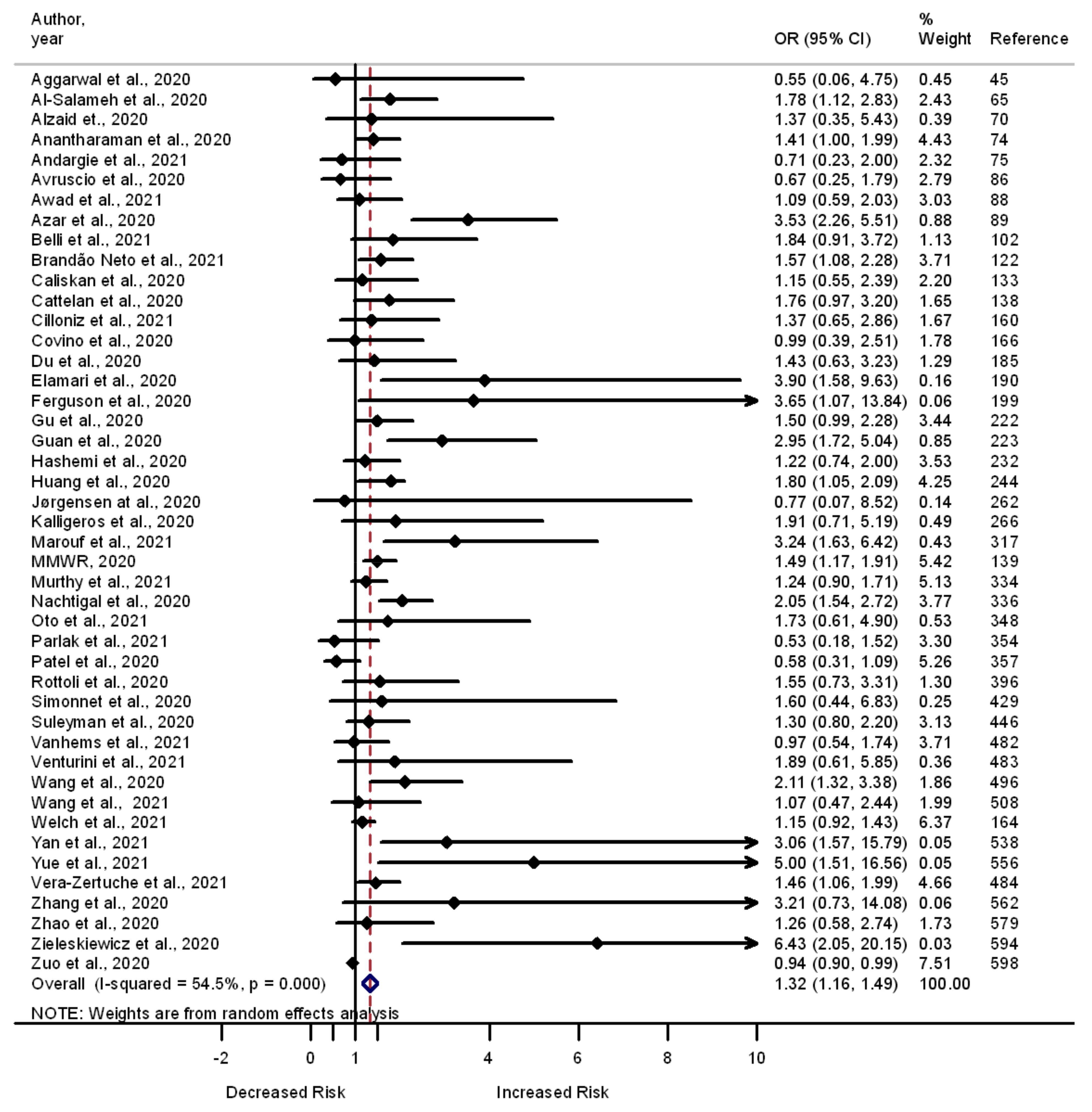
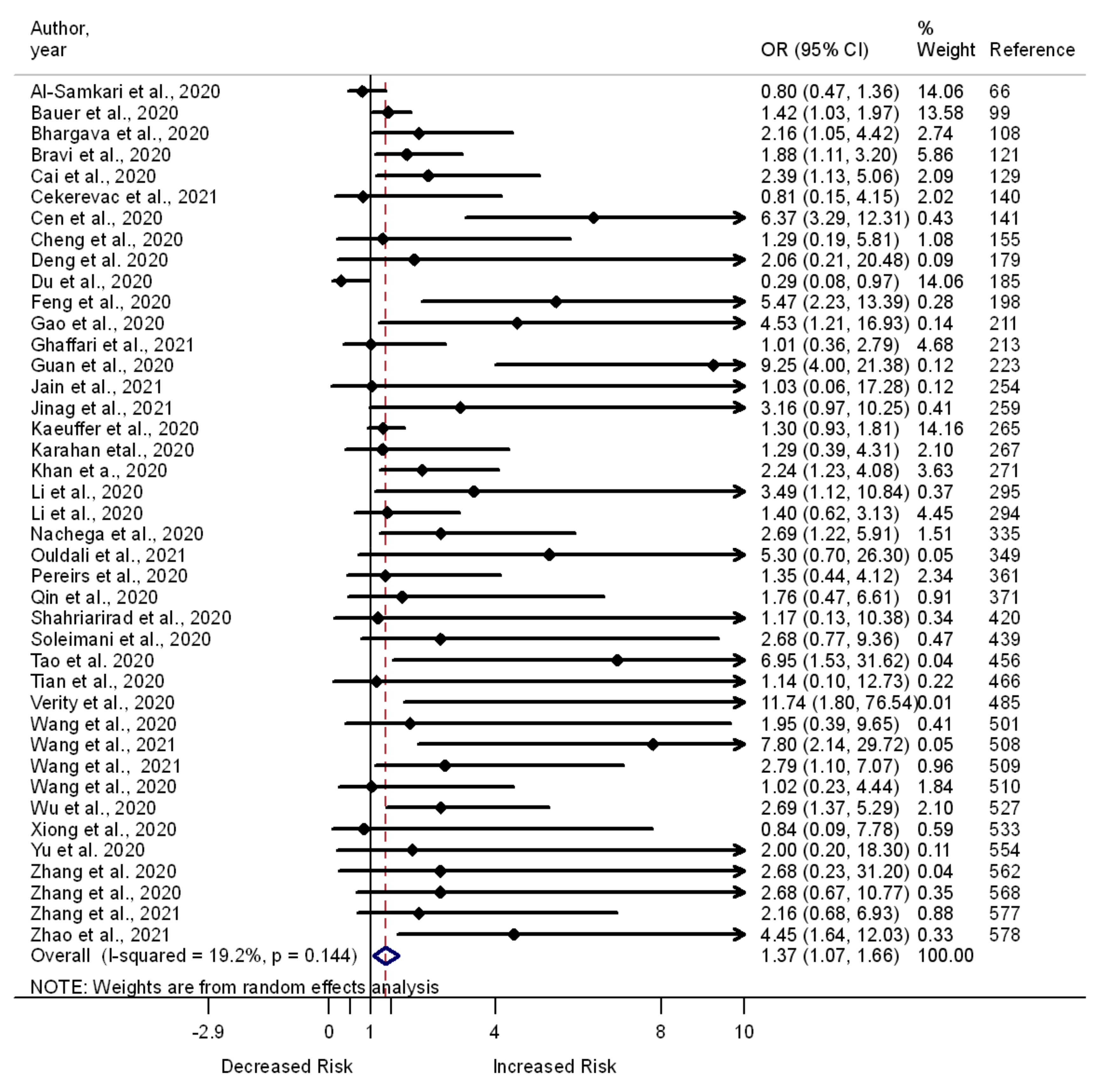
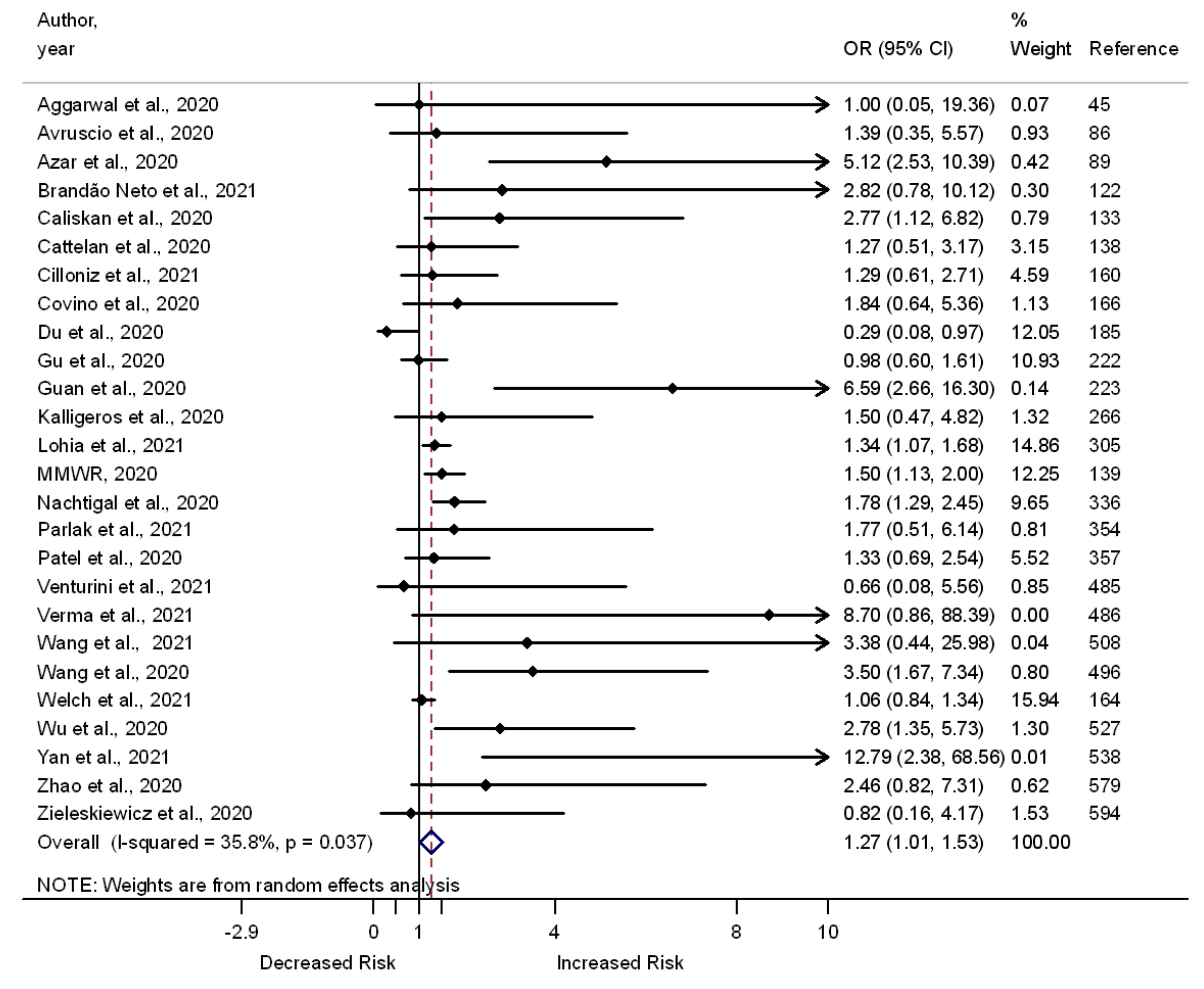

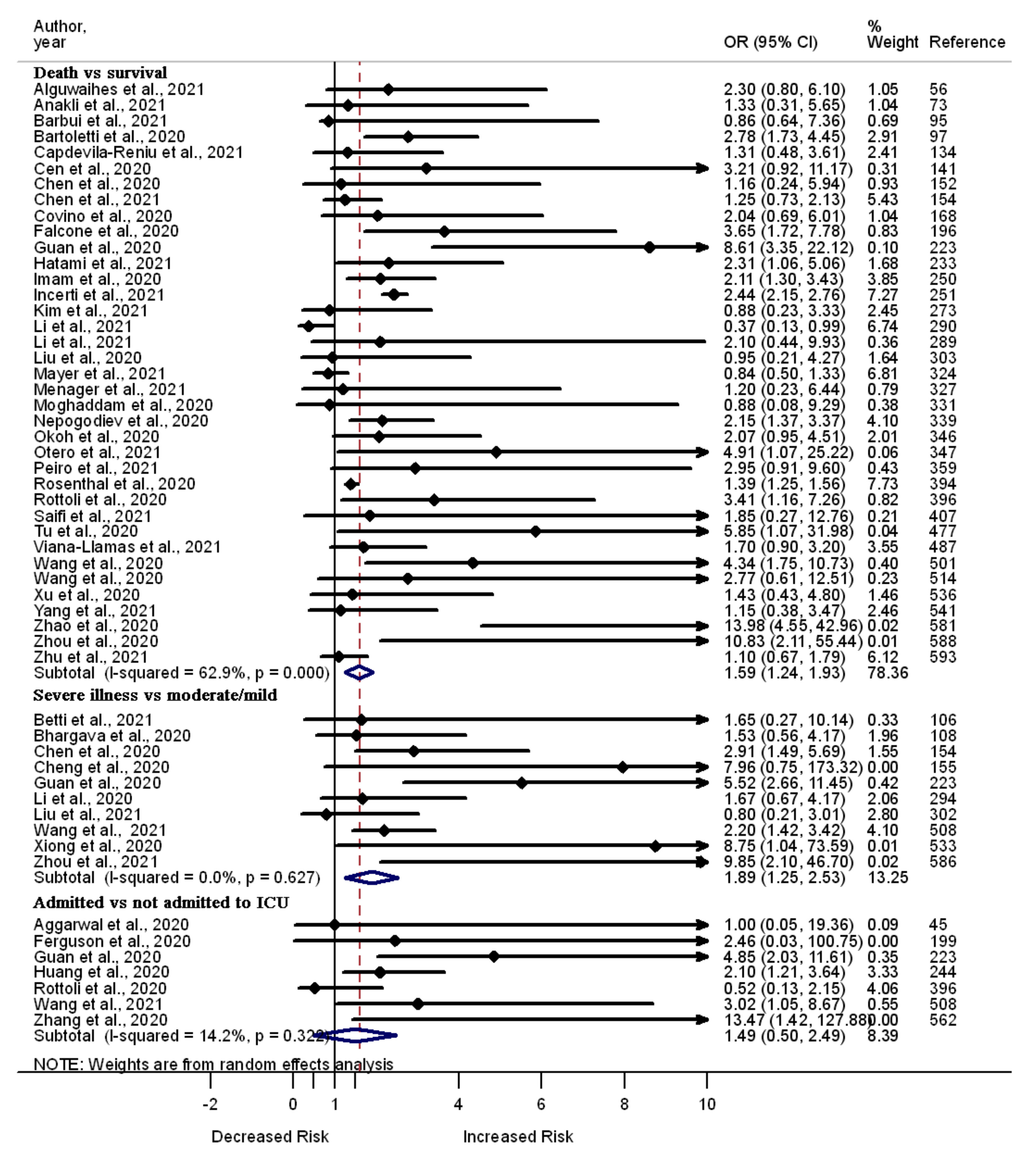
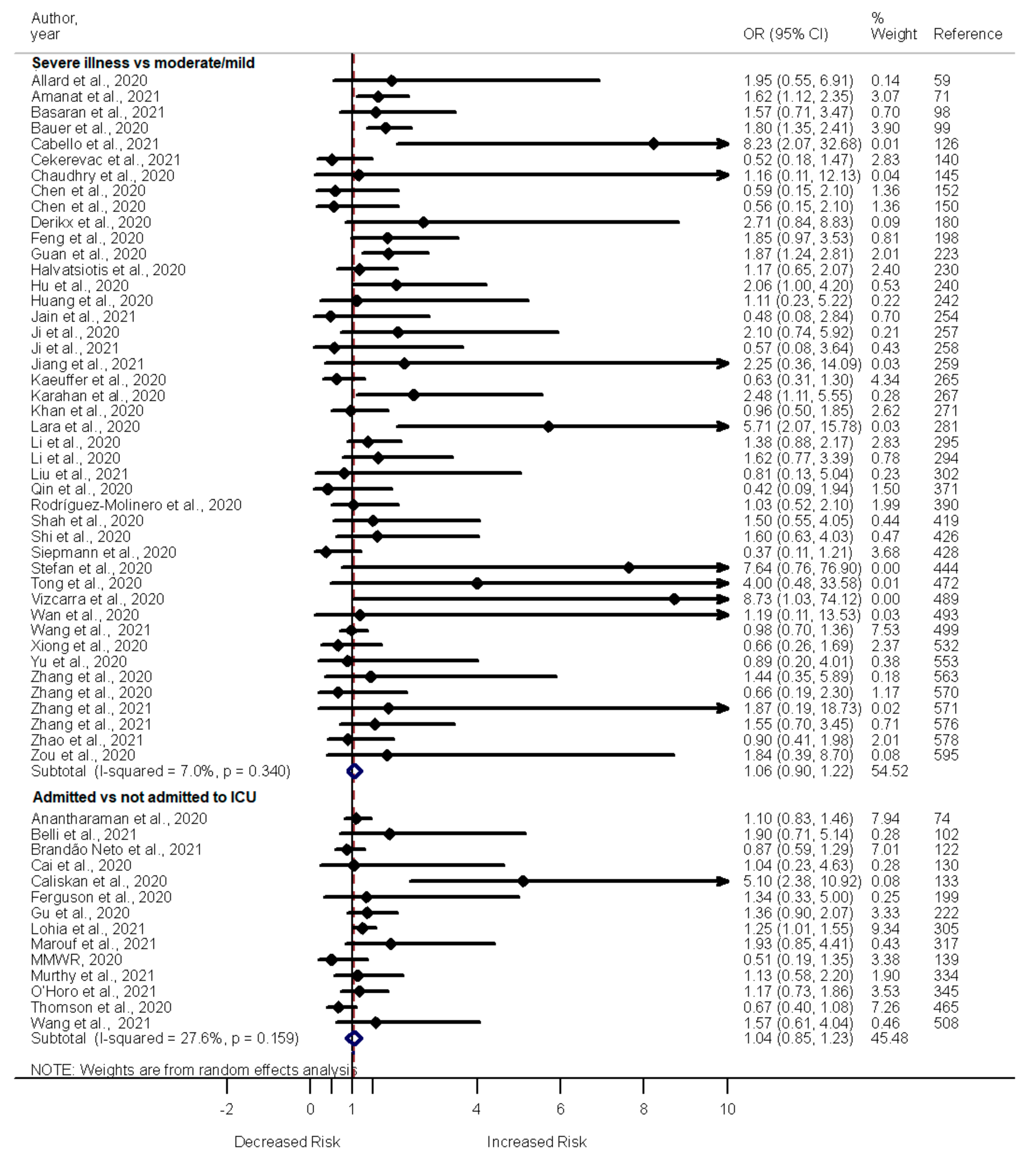
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Degarege, A.; Naveed, Z.; Kabayundo, J.; Brett-Major, D. Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis. Pathogens 2022, 11, 563. https://doi.org/10.3390/pathogens11050563
Degarege A, Naveed Z, Kabayundo J, Brett-Major D. Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis. Pathogens. 2022; 11(5):563. https://doi.org/10.3390/pathogens11050563
Chicago/Turabian StyleDegarege, Abraham, Zaeema Naveed, Josiane Kabayundo, and David Brett-Major. 2022. "Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis" Pathogens 11, no. 5: 563. https://doi.org/10.3390/pathogens11050563
APA StyleDegarege, A., Naveed, Z., Kabayundo, J., & Brett-Major, D. (2022). Heterogeneity and Risk of Bias in Studies Examining Risk Factors for Severe Illness and Death in COVID-19: A Systematic Review and Meta-Analysis. Pathogens, 11(5), 563. https://doi.org/10.3390/pathogens11050563




