Additively Manufactured Porous Ti6Al4V for Bone Implants: A Review
Abstract
:1. Introduction
2. Methodology
3. Bone Structure, Its Properties, and Bone Healing Mechanism
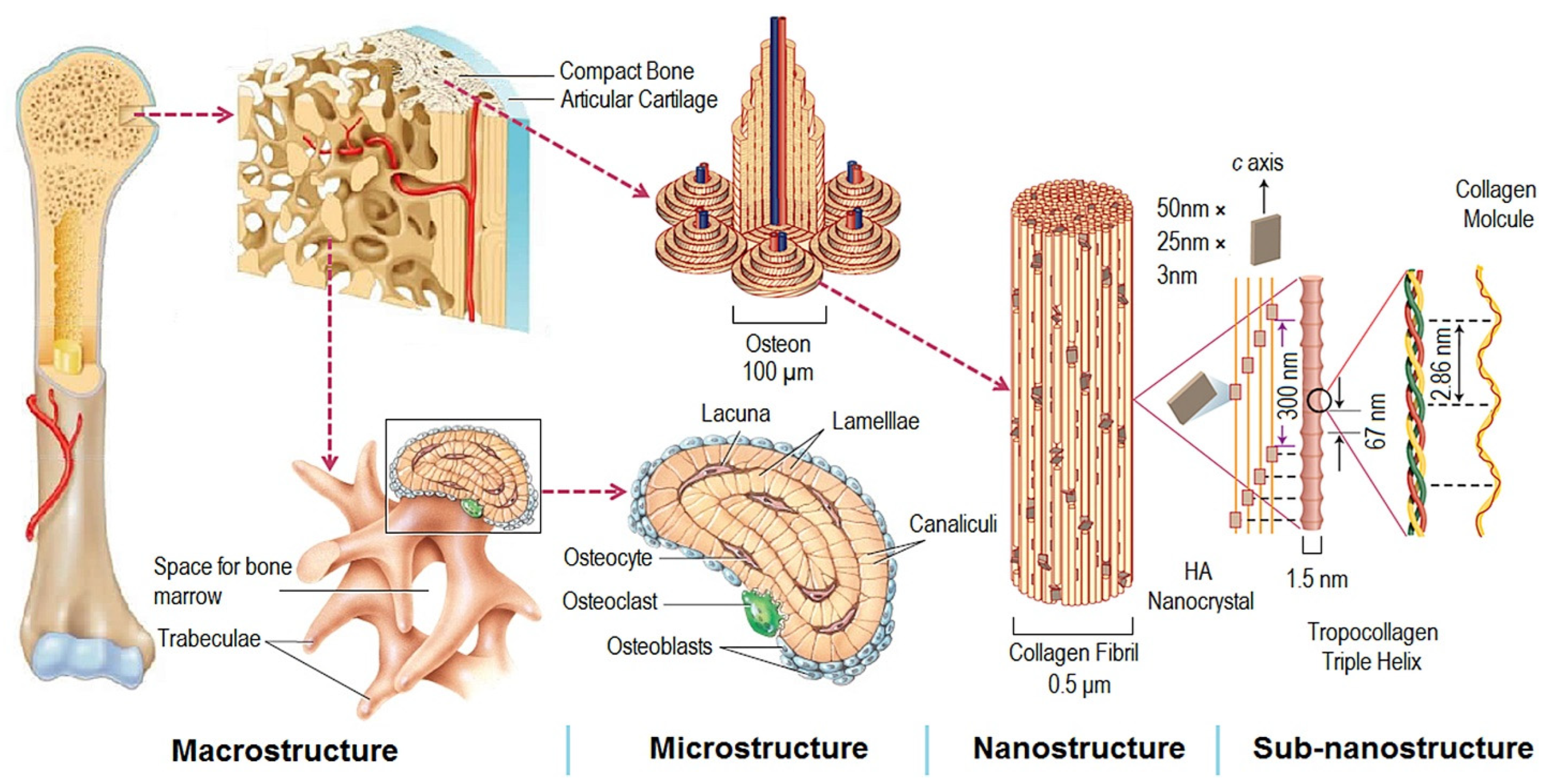
3.1. Bone Structure
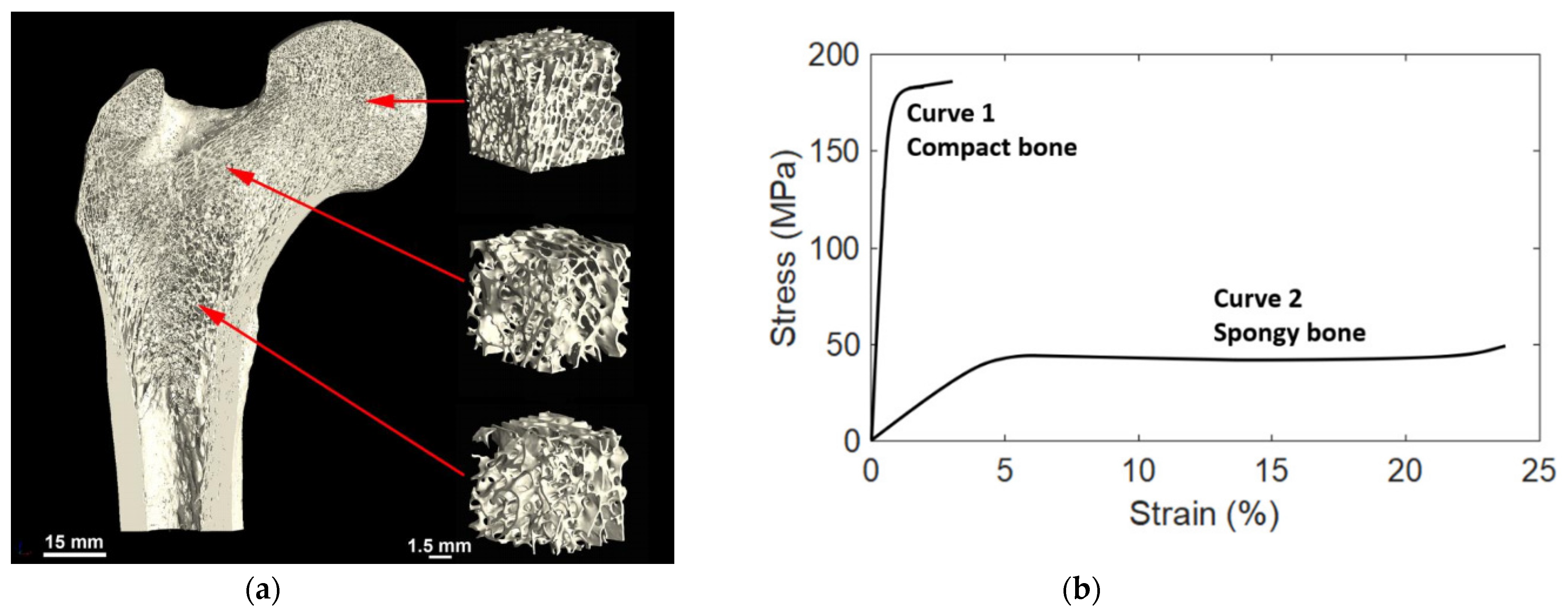
3.2. Mechanical Properties
3.3. Bone Healing Mechanism
- Inflammation is the first step of the healing mechanism, and this starts right after the bone breaks. After the bone fractures, the blood vessels’ connections in the bone are also ruptured and this results in bleeding into the fractured area. This process is called inflammation where the blood starts to clot in the fractured site and swelling is observed. Inflammation lasts for several days and thus provides the initial framework and stability to the fractured bone for developing new bone;
- The bone production step follows the inflammation step in the healing process. The clotted blood from inflammation is gradually replaced by the growth of soft callus cartilage and fibrous tissues. Eventually, when healing progresses, this soft callus cartilage is replaced with hard bone known as a hard callus. This bone is thus detectable by x-rays afterward;
- Bone remodeling is the final phase of the healing process and could last for weeks or several months. The hard callus bone continues to form and becomes compact, returns to its original shape and form, ruptured blood vessels grow, and blood circulation improves in the area. Sufficient healing of the bone after several weeks gradually remodels the bone for usual weight-bearing activities such as standing and walking, and it provides necessary support to the structure [60]. More importantly, the loading magnitude and loading frequency have significant effects on bone remodeling and thus have a major impact on the bone healing process [41].
3.4. Hindrance for Bone Healing
3.5. Need for Porous Structure and Its Advantages
- Provide space and 3D structure for bone ingrowth.
4. Porosity Designs
4.1. Non-Gradient (Uniform) Porous Structure

| Author | Process | Porosity Design | Strength (Compressive/Tensile) | Young’s Modulus | Other Findings |
|---|---|---|---|---|---|
| Li et al. [65] | EBM | Porous scaffolds with three pore sizes (300~400, 400~500, and 500~700 μm) with porosity of 80% Measured pores size: 315, 485, and 574 μm, respectively; Measured Porosity: 33.8, 50.9, and 61.3%, respectively. | Compressive Strength: 115.2–33.1 MPa | 3.7–1.7 MPa | In vivo study on Goats for 3, 6, and 12 months identified that depth of bone ingrowth increased over time and no implant dislocation was observed; Porous Ti64 scaffold with an intended pore size of 300 to 400 μm are most suitable for cell adhesion and proliferation. |
| Melancon et al. [71] | L-PBF | Tetrahedron and Octet -truss unit cells were studied over the entire design space, which includes porosity, strut thickness, unit cell size, pore size, height, width, and depth. | Depend on the unit cell design parameter | Depend on the unit cell design parameter | Proposed a systematic approach integrating computed tomography, mechanical testing, and statistical analysis of geometric imperfections to generate statistical-based numerical models of high strength additively manufactured porous biomaterials; The proposed methodology reduced the error between predicted and tested mechanical properties from 49% to 11% (elastic modulus) and 41% to 7.6% (yield strength) |
| Ødegaard et al. [77] | EBM | P TPMS lattice at 35° angle Lattice- and pore diameter: 800 µm Designed porosity 50% | N/A | N/A | qPCR analysis suggests that the BMSCs differentiated into osteoblasts; Staining of alkaline phosphatase at day 7 and calcium deposits at day 28 suggest bone matrix is mineralization. |
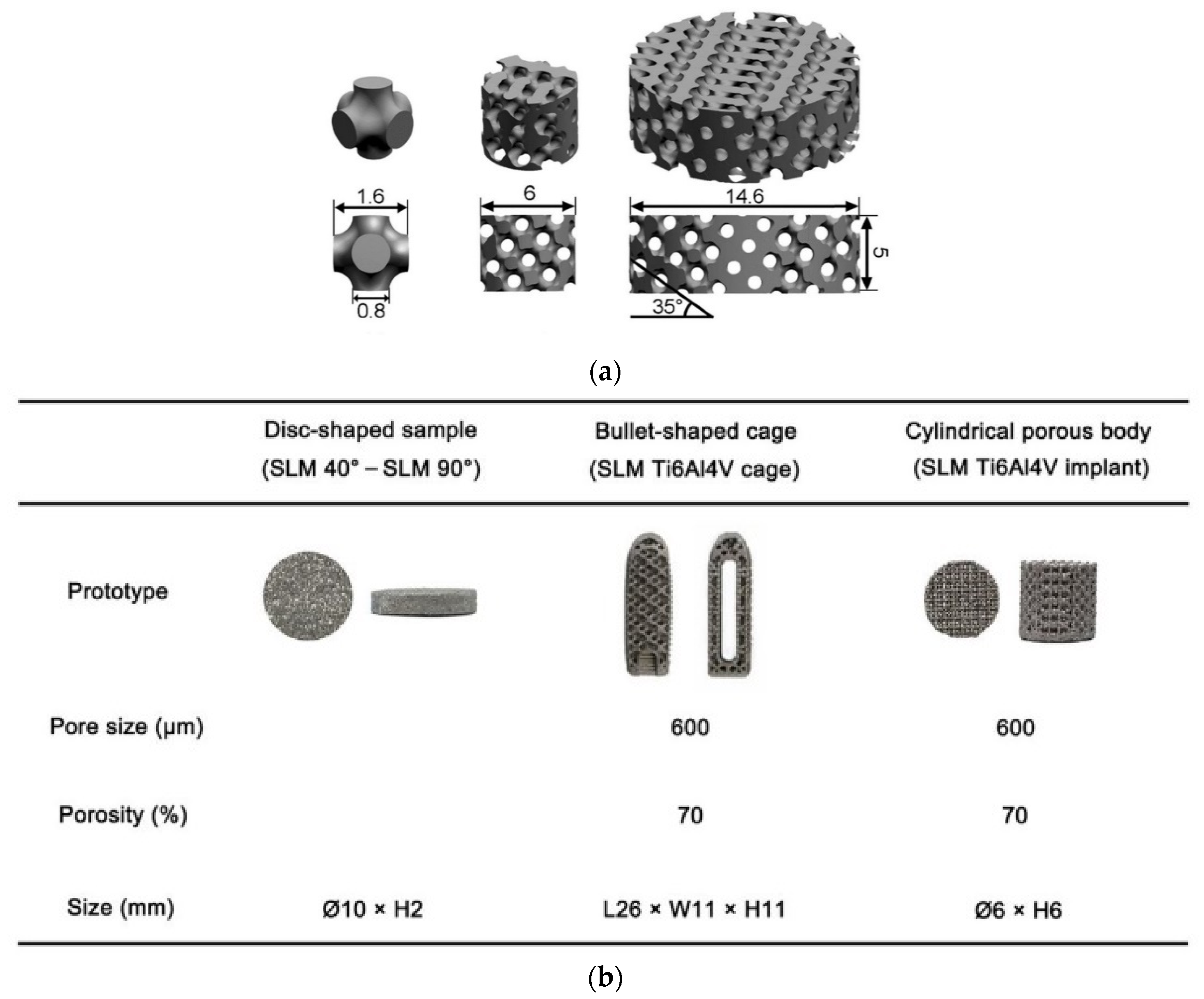
| Chen et al. [78] | L-PBF | Bullet-shaped cage and Cylindrical porous body with a designated pore size of 600 µm and porosity of 70%. In vivo Test Subject: Beagle dogs | Bullet-shaped cage: Compressive Strength = 94.7 MPa at 0.29% strain | Bullet-shaped cage: −0.51 GPa | Bullet-shaped cage showed mechanical properties comparable to commercial PEEK cage; Cylindrical porous Ti body and commercial tantalum implant (casting Ta implant) with same porosity and pore size exhibited similar bone ingrowth at 4 and 12 weeks; Great potential of L-PBF-fabricated porous Ti64 cage as spinal fusion implant |
| Hudak et al. [79] | L-PBF | Pore size: 200, 400 and 600 µm Structure: Cubic and Trabecular | Tensile: 302 ± 8.09 to 1631.08 ± 41.49 MPa | 3.80 ± 0.42 to 10.50 ± 0.58 GPa | Yield: 198.45 ± 83.29 to 1055.03 ± 135.90 MPa; 200 µm and cubic structure |
| Wieding et al. [80] | L-PBF | 3 different scaffold designs with 70% porosity D1—struts with a rectangular cross-section (CS), vertical orientation, width: 400 µm, height: 800 µm D2—struts with rectangular CS, vertical strut shifted half the strut height in the x-z plane D3—orientated diagonally to vertical axis and exhibited circular CS | Compressive Strength (MPa) D1: 155 ± 7 D2: 145 ± 2 D3: 164 ± 6 | (GPa) D1: 5.1 ± 0.3 D2: 3.7 ± 0.2 D3: 6.7 ± 0.3 | Ultimate Compressive Strain (%) D1: 5.22 ± 0.34 D2: 6.70 ± 0.56 D3: 3.45 ± 0.50 |
| Balci et al. [84] | L-PBF (Ti64 ELI) | Vertebra: Size—102 to 1719 µm Average diameter—767 ± 264 µm Femur: Size—90 to 1434 µm Average diameter—624 ± 245 µm | N/A | N/A | Bone structure successfully imitated at 1:1 and 1:1.25 productional scales |
| Tsai et al. [86] | L-PBF | Pore size below 500 µm Volume porosity 60% | N/A | N/A | Implants with Ti64 cages compared to Ti and Ta implants— - More pronounced volumes of new bone - Higher crystallinity volumes - High-quality bone formed |
| Coffiginez et al. [91] | DIW | Macro- and micro-interconnected porosity network (42.7% total porosity, which is made up of 34.5% macropores and 8.2% of micropores) Strut Size: 710 µm; Pores Size: 1492 µm | Compressive Strength: 700 MPa | 28–30 GPa | Yield Strength: 265 MPa Implant printable using low-cost printers with 25 wt.% Pluronic F-127 hydrogel loaded with 50 vol. % Ti64 powder particles; Partial sintering at 1200 °C showed an interconnected network of micronic pores within struts; Good proliferation of osteoblast-like cells on scaffolds with loaded Ti64 powder |
| Kan et al. [92] | EBM | Custom-made augment based on 3D reconstruction bone model Human Test Subject Mean Porosity: 61.3 ± 0.4% | N/A | 1.7 ± 0.2 GPa | Thin-layer CT and 3D reconstruction bone models are effective in evaluating periprosthetic bone loss preoperatively; Effective reconstruction of periprosthetic bone defect and restoration of knee prostheses; Stable Protheses even after 3 years. |
| Umar et al. [93] | L-PBF | Stochastic porous lattice structure tested in uniaxial compression in 10 load orientations relative to the structure | N/A | N/A | Modified stochastic lattices have a similar stiffness to cancellous bone and have controllable anisotropy. Standard deviation of Young’s modulus: 52.5 MPa–95.9 MPa |
| Elsayed et al. [94] | DIW | Filament diameter—800 µm Spanning a distance of 1200, 1600, and 2400 µm in X-Y direction and 600 µm height in Z direction resulted in different pore sizes and porosities | N/A | N/A | Total porosity (vol%) of 800 × 400: 53.0 ± 4.7 800 × 800: 58.8 ± 4.2 800 × 1600: 68.1 ± 4.4 |
| Soro et al. [95] | L-PBF | Porous structure based on Schwartz primitive unit-cell and three designed porosity levels: 25%, 42%, and 64%. Strut Size: 500 μm–700 μm Pore Size: 250 μm–700 μm | N/A | 14.3–36.1 GPa | Yield Strength: 86 MPa–319 MPa; 25% wt.% tantalum concentration reduces the weight, cost and lowers the intrinsic elastic modulus of the implants; Significantly higher ductility of implants, which is desirable for surgical handling and enhanced adaptability of implants |
4.2. Gradient (Non-Uniform) Porous Structure
| Author | Process | Porosity Design | Strength (Compressive/Tensile) | Young’s Modulus | Other Findings |
|---|---|---|---|---|---|
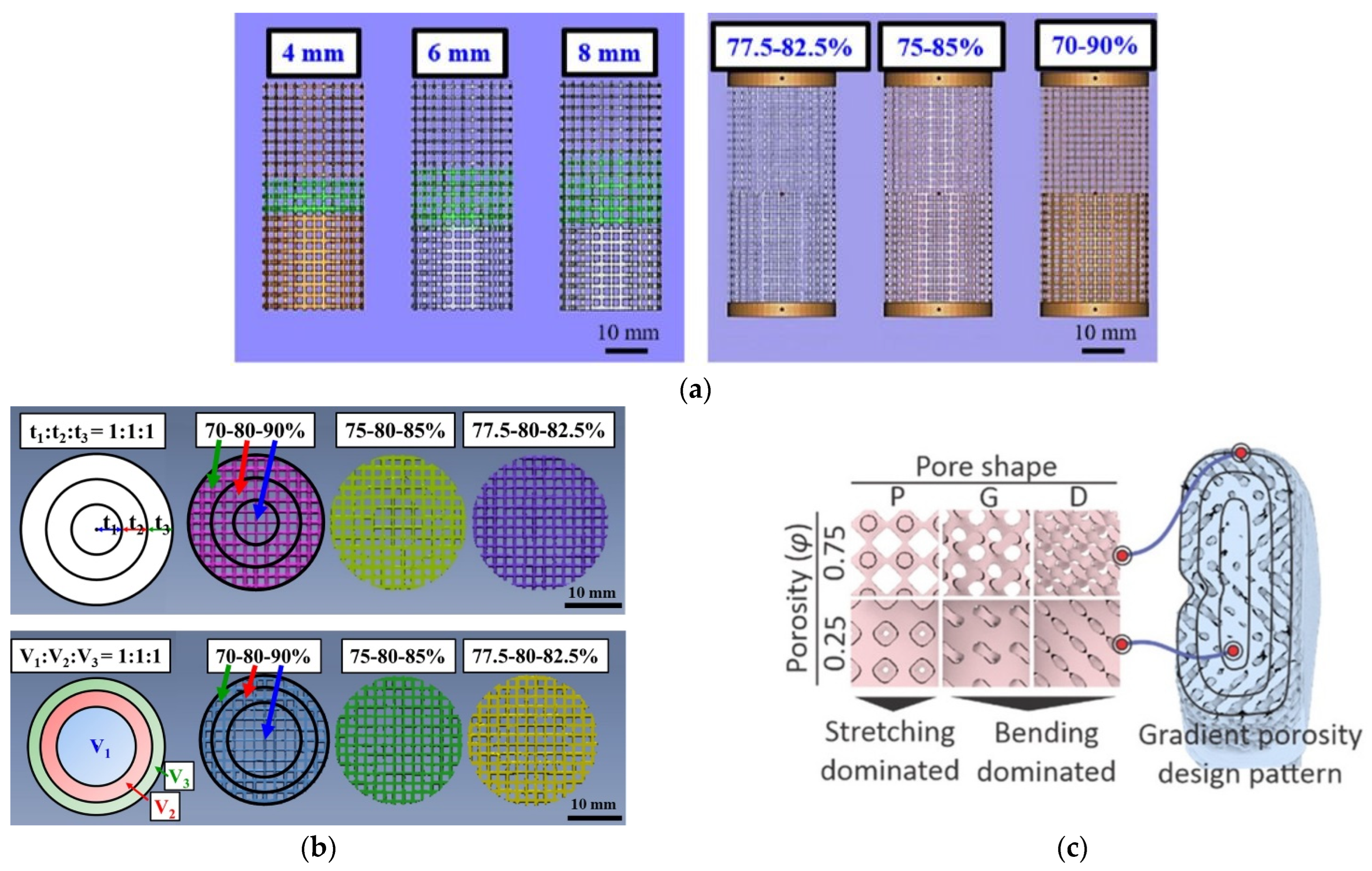
| Wu et al. (2021) [96] | L-PBF (Ti64 ELI) | Tibia bone-inspired radial-gradient porosity Designed Three types of porosity variations: 5% (77.5%–80%–82.5%), 10% (75 %–80%–85 %), and 20% (70%–80%–90%) Designs: Same region thickness and same region volume fraction | Compressive Strength (MPa): Same Region Thickness: 5%–20%: 104.8–130.8 Same Region Volume fraction: 5%–20%: 95.3–98.7 | Same Region Thickness (GPa): 5%–20%: 8.3–10.1 Same Region Volume fraction (GPa): 5%–20%: 7.9–8.2 | Same Region Thickness: Actual Porosity: 5%: 78.2, 10%: 77.6, 20%: 76.1 Elastic Limit (%): 5%–20%: 1.18–1.20 Same Region Thickness: Actual Porosity: 5%: 79.9, 10%: 79.4, 20%: 79.4 Elastic Limit (%): 5%–20%: 1.14–1.15 |
| Wu et al. (2018) [97] | EBM (Ti64 ELI) | 1—Porosity of 90% on top and 70% on bottom with the gradual transition region of 4, 6 and 8 mm 2—Sharp transition with porosity variation of 5% (77.5%–82.5%), 10% (75%–85%) and 20% (70%–90%) | Compression Stress (MPa) Transition region 4 mm: 23.5 ± 0.9 6 mm: 25.3 ± 0.8 8 mm: 25.0 ± 1.0 Sharp interface 5%: 49.9 ± 0.1 10%: 17.6 ± 1.0 20%: 22.2 ± 0.7 | (GPa) Transition region 4 mm: 7.4 ± 0.4 6 mm: 7.0 ± 0.1 8 mm: 7.0 ± 0.3 Sharp interface 5%: 8.1 ± 0.6 10%: 5.0 ± 0.4 20%: 6.6 ± 0.2 | Strain at failure (%) Transition region 4 mm: 0.63 ± 0.04 6 mm: 0.65 ± 0.07 8 mm: 0.62 ± 0.01 Sharp interface 5%: 0.91 ± 0.03 10%: 0.85 ± 0.08 20%: 0.56 ± 0.05 |
| Onal et al. [98] | L-PBF | Continuous Gradient structure generated by changing the strut diameter of a body center cubic (BCC) unit cell linearly across cell layers for a smooth transition while minimizing the effect of stress discontinuity. Two gradient designs: One with thinner struts inside (Dense-Out) and the other with thicker struts inside (Dense-In). Gradient structures designed porosity: 62%, designed pore size: 0.94 mm–1.33 mm designed strut diameter 0.40 mm–0.82 mm | Dense-In: Compressive yield Stress: 114 MPa Compressive Maximum Strength: 150 MPa Dense-Out: Compressive yield Stress: 86 MPa Compressive Maximum Strength: 128 MPa | Between the stress of 20 MPa and 50 MPa Dense-In: 3.9 GPa Dense-Out: 3.5 GPa | Optimal gradient structures should have small pores in their core (~900 μm) to increase mechanical strength and large pores (~1100 μm) in outer surface to enhance cell penetration and proliferation while avoiding pore occlusion; Static mechanical properties of gradient structure follow the rule of mixtures and are in the range of their uniform structures. |
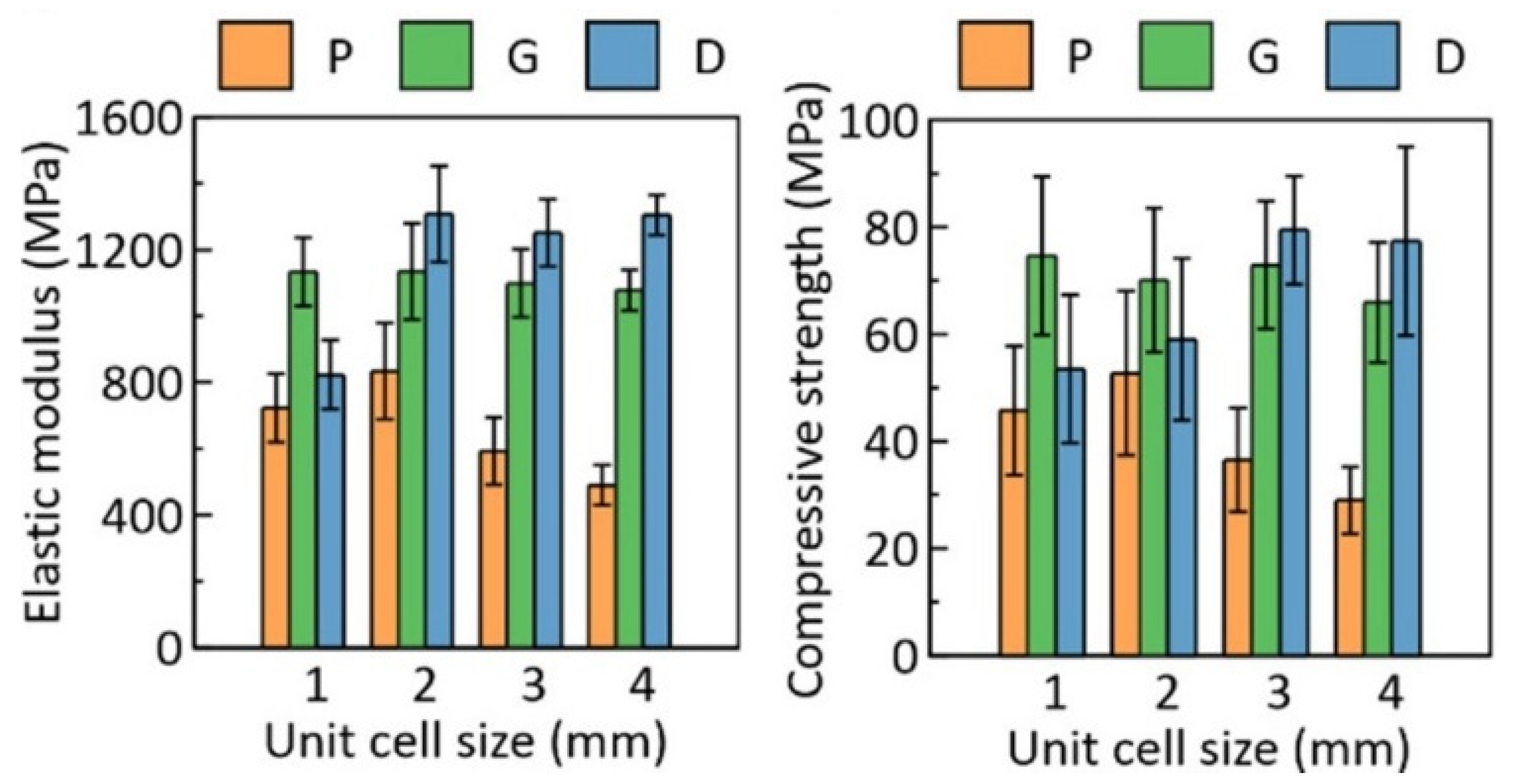
| Davoodi et al. [99] | L- PBF | TPMS -based scaffolds with P, G, and D unit cell shapes Porosity Gradient: 0.25–0.75 linearly varying from center to surface | Figure 7 | Figure 7 | High improvement of fluid permeability (about 140% for D unit cell structure and 277% for P unit cell structure); Significant enhancement of strength and deformability of bending–dominated architectures when compared to stretching dominated architectures; Majority of pores are spherical keyhole voids |
| Vee San et al. [104] | L-PBF | Cylindrical implant with pores sizes of 700 µm and 1500 µm to design porosities of 75% and 53%, respectively; Sharp interface between two porosity design sections Struts in 700 µm and 1500 µm implant sections designed with Ø 300 µm and 700 µm height, and Ø 750 µm and 1500 µm height. FEA analysis using mechano-regulation algorithm | N/A | N/A | Over prediction of the extent of bone-to-implant contact by FEA models when compared to histology results; Bone remodeling reduced the maximum Von Mises stress of Ti64 implants by more than 20%, but the maximum implant stress is still not within safety limits of additively manufactured Ti64. |
| Xiong et al. [105] | L-PBF | Scaffold designed with a hollow cylinder with inner diameters of 3.5 mm and three layers of local porosities along the radial direction. 85% porosity for inner layer (diameter of 3.5–10 mm), 65% porosity for intermediate layer (10–12 mm) and 45% porosity for outer layer (12–15 mm). Diamond-lie unit cell (DU) scaffold, honeycomb-like unit cell (HU) scaffold, and two additional types of scaffolds (DS and HS) created with a support structure made up of four quasi-cuboid rods embedded to the middle and outer scaffold layer of DU and HU. Strut length = 500 μm | Compressive Strength (MPa): D scaffold: 170.53 H Scaffold: 162.96 DS scaffold: 419.81 HS Scaffold: 536.90 | (GPa): D scaffold: 4.72 H Scaffold: 3.79 DS scaffold: 10.07 HS Scaffold: 10.99 | Yield Strength (MPa): D scaffold: 126.81, H Scaffold: 110.85, DS scaffold: 350.09, HS Scaffold: 423.82 Toughness (MJ/m3): D scaffold: 86.88, H Scaffold: 280.96, DS scaffold: 213.04, HS Scaffold: 527.46 The addition of support structure in functionally graded material scaffold significantly improved strength and toughness while maintaining elastic modulus and slightly lowering overall porosity |
4.3. Fatigue Behavior of Porous Ti64 Structures
| Author | Process | Porosity Design | Fatigue Studies | Key Findings |
|---|---|---|---|---|
| Kelly et al. [63] | L-PBF (TI64 ELI) | Porous structure with repeating diamond unit cell with a designed pore size of 300–400 μm. Resulted in an average porosity of 45.4% and an average strut size of 174 μm. Post-processing of samples included Hot Isostatic pressing (HIP), surface treatment, and anodization treatment | Tensile fatigue test at a frequency of 5Hz with R = 0.1 | Reduced surface roughness after surface treatment but no improvement of fatigue strength. Fatigue behavior at 2 × 106 cycles: Max. Stress applied = 40 MPa and Stress Amplitude = 18 MPa |
| Xiong et al. [69] | L-PBF | Porous scaffold (Ø 4 mm, height 8 mm) with dense cores of varying diameters (1.2 mm, 1.8 mm, and 2.4 mm). Diamond unit cells with a pore size of 400 μm and strut size of 200 μm | Compression–compression loading tests at a constant loading frequency of 15 Hz and constant load ratio (R) = 0.1 | Inserting a dense core into a porous scaffold is an effective way of strengthening the mechanical properties and fatigue strength; High normalized fatigue strength at 106 cycles of approximately 0.5 and high effective fatigue strength of approximately 165.46 MPa was observed for porous structure with 1.8 mm core; Debris dropping from the tested samples observed at loading cycle far short of fatigue failure |
| Wu et al. [106] | L-PBF | Cylindrical specimens with a sandwiched architecture such that 49 vol.% porosity lattice was built in between top and bottom solid Ti64. Height of top and bottom solids = 5 mm each. Medium porous structure height = 15 mm. Diameter of specimen = 13 mm. New unit cells were designed with 12 planes, 4 struts inclined at 45°, and 3 straight struts along three main axes (x, y, and z). The length of the unit cell in x, y, and z-direction were 2 mm, 2 mm, and 1.44 mm, respectively. Strut Width = 250 μm. Samples HIPed at 1000 °C/150 MPa for 1 h followed by furnace cooling | Compression fatigue test at a frequency of 10 Hz and R = 0.1 | The HIP process improved fatigue endurance ratio and fatigue strength at 106 cycles from 0.3 to 0.55 and 43 MPa to 55 MPa mostly due to the phase transformation from brittle α’- martensite to tough α + β mixed phases after HIP. |
| Lietaert et al. [107] | L-PBF (Ti64 ELI) | Gradient porous design with the highest porosity at the middle. 20% structural density at middle and linearly increasing structural density towards the end (20% to 100%). Diamond unit cell type used. Sample total height 105 mm and diameter 10 mm | Low frequency cyclic test at stress amplitudes: 10, 30 and 50 MPa Compression–compression tests at stress ratio (R) of 10, tension-tension test at R = 0.1 and tension-compression test at R = −1 | Most fracture sites are located close to the nodes due to the high stresses at these locations; Compression–compression and tension–tension fatigue regimes lead to a shorter fatigue life than tension–compression loading due to the presence of a mean local tensile stress for the first two load conditions |
| Mahmoud et al. [110] | L-PBF | Three gyroid designs: G4 with uniform porosity and strut size 400 μm G2 with uniform porosity and strut size 200 μm G24 with functionally graded porosity and strut size 400 μm | Compression-compression fatigue testing at a frequency of 15 Hz and load ratio of R = −1 | G2 had the highest normalized fatigue properties (approximately twice) compared to G4 and G24, as G2 designs higher ductility, lower internal defects, and small surface area per strut; Compressive strength of G24 was higher than G4 and G2, thus can be more beneficial for load-bearing implants |
| S. Zhao et al. (2016) [112] | EBM | Three reticulated meshes: cubic, G7, and the rhombic dodecahedron with porosity of 63.2%, 64.5%, and 62.1%, respectively | High-cycle compression fatigue test with R = 0.1 and frequency of 10 Hz in air | Normalized fatigue strength ranges from 0.10–0.25 at 106 cycles; Cyclic ratcheting was dominating mechanism that determined the compressive fatigue of meshes; Optimization of buckling and bending deformation through cell shape design, cellular solids with high fatigue strength and low modulus can be fabricated |
| Hrabe et al. [113] | EBM | Regular periodic porous structure with the diamond unit cell, relative densities ranging from 0.17–0.40 and pore sizes ranging from approximately 500 μm to 1500 μm | Compression-compression fatigue test at a frequency of 15Hz and load ratio R = 0.1 | Normalized fatigue strengths of 0.15 to 0.25 for 106 cycles. Lower fatigue lifetime than solid material due to stress concentrations from strut surface features, stress concentrations from closed porosity within struts, and microstructure with less than optimal high-cycle fatigue resistance. |
| Wu et al. (2020) [114] | L-PBF | Porous specimen design with new cuboctahedron unit cell same as previous study by Wu et al. [107] Strut width adjusted to build three types of specimens with three different porosities (33 vol.%, 50%, and 84 vol.%) between the solid top and bottom sections Samples HIPed at 1000 °C/150 MPa for 1 h followed by furnace cooling | Compression fatigue test at a frequency of 10 Hz and R = 0.1 | Fatigue endurance ratio at 106 cycles for L-PBF specimen decreased from 0.5 to 0.15 with an increase in porosity from 33 vol.% to 84 vol.%. However, for the HIPed samples with different porosities, the fatigue endurance ratio was higher than 0.45 at 106 cycles |
| M. Dallago et al. [115] | L-PBF | Six different cellular structures: regular cubic cells CUB-NS single staggered cubic cells CUB-S double staggered cubic cells CUB-2S regular cylindrical cells CYL-R single staggered cylindrical cells CYL-S double staggered cylindrical cells CYL-2S | Axial fatigue test with 1 kN load cell operating at 120 Hz frequency with zero mean stress and R = −1 | HIPing treatment considerably reduces internal porosity but doesn’t have a clear effect on fatigue resistance; Cellular structures designed with less fine geometrical details appeared to be less affected by internal porosity |
| S. Zhao et al. (2018) [116] | EBM | Three designs with rhombic dodecahedron structures: G1 with strut angle of 42° G2 with strut angle of 39° G3 with strut angle of 36° | High-cycle compression fatigue test with R = 0.1 and frequency of 10 Hz in air | Designed graded cellular structures exhibited a combination of low density, high fatigue strength, and energy absorption, which in turn are significantly superior to cellular metallic structures with uniform density; Cracks initiated and propagated in the constituent meshes from high to low strength progressively until the graded cellular structure failed with increased fatigue cycles |
| Pérez-Sánchez et al. [117] | EBM | Two types of single struts: 1 mm and 0.6 mm diameter manufactured at 45° and 90° build inclination | Fatigue 3-point bending test at a frequency of 15 Hz and load ratio of R = 0.1 | Mechanical properties from static testing and fatigue behavior of 45° build orientation struts were better than that of 90° vertical struts; Abrupt decrease in the fatigue curve was observed in low cycles, obtaining the fatigue strength for 106 cycles between 15% and 25% of the flexural strength |
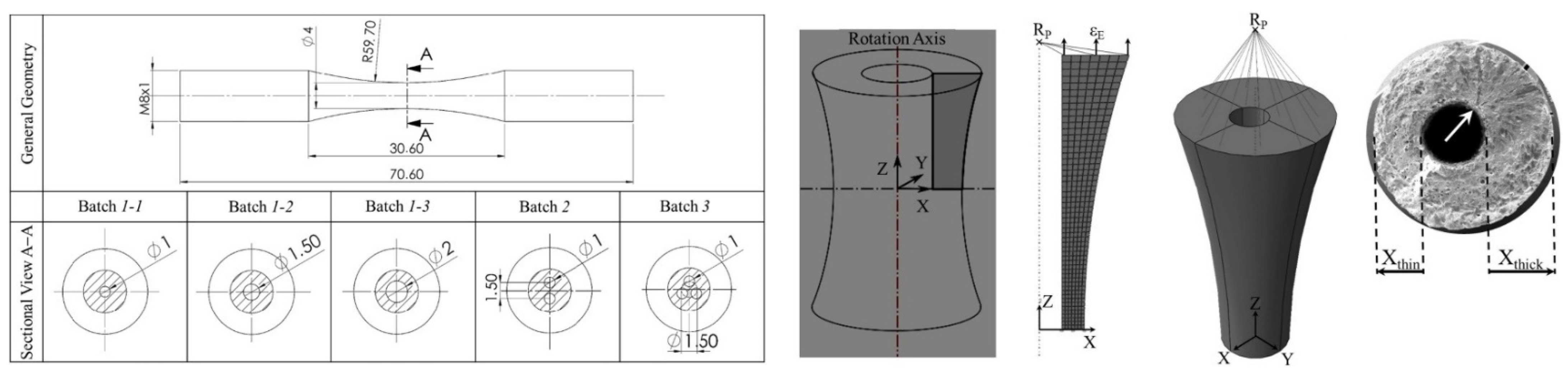
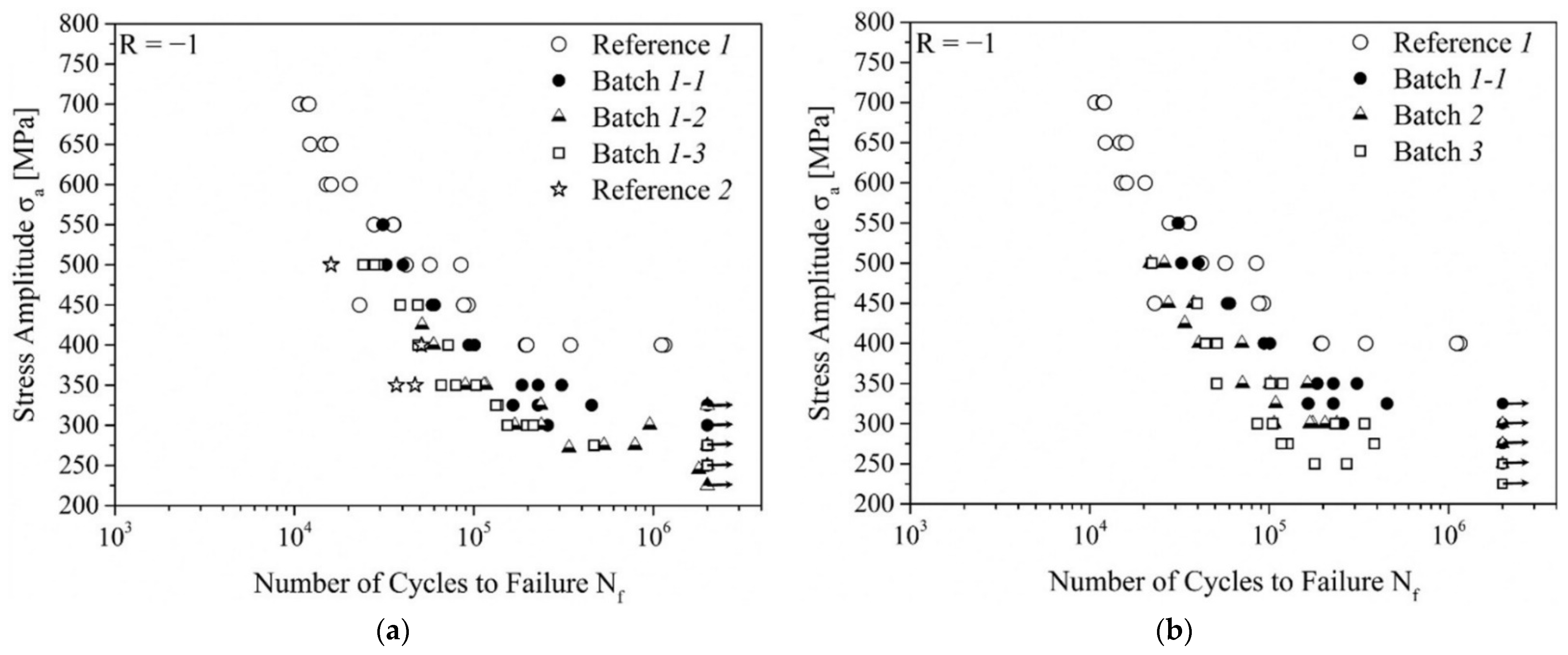
| Günther et al. [118] | L-PBF | Figure 8 | Resonant testing machine with symmetrical push-pull loading at R = −1 and 105 Hz | Figure 9 |
5. Multifunctional Implant Design and Development
| Author | Process | Multifunctionality Design | Test Subject | Study Duration | Key Findings |
|---|---|---|---|---|---|
| Rahmani et al. [68] | L-PBF | 99.9% purity wollastonite (CaSiO3) with a particle size of 1–5 µm filled and sintered (frittage) inside an argon-atomized Ti64 cellular lattice structure via an SPS machine; Five different TPMS scaffold structures | N/A | N/A | L-PBF-manufactured Ti64 lattice can be sintered via SPS along with CaSiO3 for load-bearing bone replacements; Rectangular and honeycomb were identified to be novel cellular scaffolds for high compressive load-bearing and biological application respectively; Rectangular scaffold suitable for oxygen transport and fluid permeability, whereas honeycomb is best for the growth of cells. |
| Goto et al. [83] | EBM | ACaHW treatment (NaOH, CaCl2, heat, and water) | Rabbits | 4, 8, and 12 weeks | Treated implants showed direct bonding of bone to the metal surface without the interposition of fibrous tissue (higher affinity to the bone than the untreated one) |
| Jia et al. [127] | EBM-MAO | Silver nanoparticles (AgNPs) deposition onto the micro-roughened surface | In-vitro | 5 days | Micro-nanoporous MAO layer stimulated cell adhesion and considerably increased the cell number and improved cell morphology while subsequent nano-silver immobilization, inspired by the mussel’s adhesive versatility, yielded potential antibacterial surfaces |
| Hengel et al. [128] | L-PBF (Ti64-ELI) | Miniaturized implant geometry optimized for murine femora implantation; Hexagonal unit cell, Total Length 4 cm and diameter 0.5 mm. A surface-to-volume ratio of 35.6 Biofunctionalized using plasma electrolytic oxidation to locally release both osteogenic (i.e., strontium) and anti-bacterial (i.e., silver ions) agents, along with the incorporation of hydroxyapatite into the surface of the implant in a same single-step | In vitro and Ex vivo (mouse) | In-vitro: 1, 3, 7 and 11 days Ex-vivo: 24 h | Tremendous potential use of synergistic antibacterial behavior between silver ions and strontium allowing for simultaneously reduced required dose of silver ions by 4–32 folds while inducing osteogenic behavior |
| Li et al. [129] | 3DF 1 | Ti64-β-TCP hybrid scaffold with interconnected porous network | Dogs | 12 weeks | Hierarchical porous structure and mechanical properties between cancellous and cortical bone. Enhanced bioactivity of hybrid scaffolds with 10 wt.% TCP ceramic as compared to the scaffold without and with a lower concentration of TCP |
| Perets et al. [130] | L-PBF | Permanent matrix of Ti lattice infiltrated with biodegradable Mg-based alloy (Mg-2.4%Nd-0.6%Y-0.3%Zr) | In-vitro | 24 h and 48 h | Stable stress–strain curve and higher Ultimate Compressive Strength and Yield point compared to Ti- lattice; positive cell viability response compliant to the ISO-10990-5 requirements |
| Bartolomeu et al. [131] | L-PBF | Dense Ti64 and/or Ti64 cellular structure fabricated on top of NiTi cellular structure to create multi-material implant design | N/A | N/A | Effective mechanical interlocking (shear strength of ≈33.2 MPa) between NiTi and Ti64 material in the transition region; the austenite phase on the NiTi region indicated the need for further investigations regarding thermal treatments for the martensite shape-memory phase |
| Lei et al. [132] | L-PBF | Surface bio-activation by alkaline-heat treatment (5 mol L−1 NaOH, 98% wt. for 1 h at 60 °C) | In-vitro | 1, 3, and 7 days | The overall distribution of cells on regular porous scaffolds was similar to the orderly arrangement of cultivated crops in the field, and the microporous structure of scaffolds with an aperture close to cell size was more suitable for cell proliferation and adhesion |
| Kayacan et al. [133] | L-PBF | Transitive porous implants of semispherical and elliptical pores of 500 µm at outer region and cell development channels of 200 µm at the inner region | Sheep | 12 weeks | Semispherical porous structure resulted in the formation of a strong and durable bond between tissues and implant Due to the transitive porous structure, a strong and durable tissue bond could be formed at the bone–implant interface |
| Zhang et al. (2018) [134] | L-PBF | Porous scaffolds with 5 strut sizes—0.2, 0.25, 0.3, 0.35, and 0.4 µm Hydroxyapatite layer coated at the surface to promote osteoconductivity | Beagle Dogs | 1, 4, and 6 months | No infection of the surgical sites, implants dislocation, or adverse reactions, such as inflammation or foreign body reaction around the implantation sites; Beagles limp on their right legs in the first two weeks, but they can walk freely after one-month implantation. After four months, the implants had little effect on their movement. After six months, new bone tissues gradually grow into porous implants. The damaged legs were completely repaired, and it was hard to detect the initial injury from the beagle’s gait walking. |
| Li et al. (2019) [135] | L-PBF (Ti64 ELI) | Alkali–acid-heat (AH) treatment on the porous Ti64 scaffold (AH-porous Ti64) followed by hydrothermal treatment to enable HA coating with nanopillar-like morphology (HT/AH-porous Ti64) | In-vitro | ALP activity: 7, 14, and 21 days | HT/AH-porous Ti64 exhibited the highest apatite formation ability and best affinity to fibronectin and vitronectin; In vitro studies indicated improved adhesion and differentiation on the HT/AH-porous Ti64 as compared with the porous Ti64 and AH-porous Ti64 |
| San Cheong et al. [136] | L-PBF | Hydroxyapatite (HA) Coating on the porous scaffolds with pore sizes of 700 and 1500 µm; FEA and in vivo analysis | Sheep | 6 weeks | Novel Finite Element algorithms to simulate bone ingrowth to improve implant design; FEA models results showed that reduction in implant stiffness increases bone ingrowth; Osteoconductive HA coating improved osteointegration—bone volume increases by >10%. |
| Bandyopadhyaya et al. [137] | LENSTM (Ta and Ti64) | 30 vol.% porous Ti64 (30Ti64) 30 vol.% porous Ti64 with titania (TiO2) nanotube modified surface (30TNT) 30 vol.% with porous Ta (30Ta) | Rat | 5 and 12 weeks | 30TNT showed comparable osteoid formation to 30Ta around the implant, which is significantly higher than 30Ti64 controls at 5 weeks; 30Ta outperform 30TNT and 30Ti64 at 12 weeks |
| MacBarb et al. [138] | EBM (Ti64 ELI) | AM discs with a 1.25 mm thick- solid base and a 0.75 mm thick- porous surface layer; Layer of nanocrystalline HA (~20 nm thick) coated to the disc surface using a dip, spin, and heat treatment technique; Target Pore size—300 μm and porosity 60–70% porosity; Measured mean Pore size 290.6 µm and mean porosity of 60.0% | In-vitro | 2, 7, 14, and 21 days | Cells on AM discs exhibited expedited proliferative activity when compared to titanium plasma spray (TPS) coated samples; 48% higher calcium production on AM discs than on TPS discs; No significant enhancement of cellular activities with HA-coating; Additive manufactured porous titanium surfaces can be alternative to TPS-coating for orthopedic spinal implants |
6. Current Challenges and Literature Gaps
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wauthle, R.; Ahmadi, S.M.; Yavari, S.A.; Mulier, M.; Zadpoor, A.A.; Weinans, H.; Van Humbeeck, J.; Kruth, J.-P.; Schrooten, J. Revival of pure titanium for dynamically loaded porous implants using additive manufacturing. Mater. Sci. Eng. C Mater. Biol. Appl. 2015, 54, 94–100. [Google Scholar] [CrossRef] [PubMed]
- Galante, J.; Rostoker, W.; Lueck, R.; Ray, R.D. Sintered fiber metal composites as a basis for attachment of implants to bone. JBJS 1971, 53, 101–114. [Google Scholar] [CrossRef]
- Levine, B. A New Era in Porous Metals: Applications in Orthopaedics. Adv. Eng. Mater. 2008, 10, 788–792. [Google Scholar] [CrossRef]
- Andani, M.T.; Moghaddam, N.S.; Haberland, C.; Dean, D.; Miller, M.J.; Elahinia, M. Metals for bone implants. Part 1. Powder metallurgy and implant rendering. Acta Biomater. 2014, 10, 4058–4070. [Google Scholar] [CrossRef]
- Exhibit 19. HCUP estimates of the total number of target procedures. Content last reviewed April 2018. Agency for Healthcare Research and Quality, Rockville, MD. Available online: https://www.ahrq.gov/research/findings/final-reports/ssi/ssiexh19.html (accessed on 16 November 2021).
- OSSDSIGN AB Annual Report 2020. OSSDSIGN AB. 8 June 2020. Available online: https://www.ossdsign.com/reports-engelska (accessed on 16 November 2021).
- Rezwan, K.; Chen, Q.Z.; Blaker, J.J.; Boccaccini, A.R. Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 2006, 27, 3413–3431. [Google Scholar] [CrossRef]
- Devin, J.E.; Attawia, M.A.; Laurencin, C.T. Three-dimensional degradable porous polymer-ceramic matrices for use in bone repair. J. Biomater. Sci. Polym. Ed. 1996, 7, 661–669. [Google Scholar] [CrossRef]
- Spector, M.; Michno, M.J.; Smarook, W.H.; Kwiatkowski, G.T. A high-modulus polymer for porous orthopedic implants: Biomechanical compatibility of porous implants. J. Biomed. Mater. Res. 1978, 12, 665–677. [Google Scholar] [CrossRef]
- Johnson, K.D.; Frierson, K.E.; Keller, T.S.; Cook, C.; Scheinberg, R.; Zerwekh, J.; Meyers, L.; Sciadini, M.F. Porous ceramics as bone graft substitutes in long bone defects: A biomechanical, histological, and radiographic analysis. J. Orthop. Res. 1996, 14, 351–369. [Google Scholar] [CrossRef]
- Sopyan, I.; Mel, M.; Ramesh, S.; Khalid, K.A. Porous hydroxyapatite for artificial bone applications. Sci. Technol. Adv. Mater. 2007, 8, 116–123. [Google Scholar] [CrossRef] [Green Version]
- Uchida, A.; Nade, S.M.; McCartney, E.R.; Ching, W. The use of ceramics for bone replacement. A comparative study of three different porous ceramics. J. Bone Jt. Surg. 1984, 66, 269–275. [Google Scholar] [CrossRef]
- Will, J.; Melcher, R.; Treul, C.; Travitzky, N.; Kneser, U.; Polykandriotis, E.; Horch, R.E.; Greil, P. Porous ceramic bone scaffolds for vascularized bone tissue regeneration. J. Mater. Sci. Mater. Med. 2008, 19, 2781–2790. [Google Scholar] [CrossRef] [PubMed]
- Chen, Z.; Yan, X.; Chang, Y.; Xie, S.; Ma, W.; Zhao, G.; Liao, H.; Fang, H.; Liu, M.; Cai, D. Effect of polarization voltage on the surface componentization and biocompatibility of micro-arc oxidation modified selective laser melted Ti6Al4V. Mater. Res. Express 2019, 6, 086425. [Google Scholar] [CrossRef]
- Li, Y.; Jahr, H.; Zhou, J.; Zadpoor, A.A. Additively manufactured biodegradable porous metals. Acta Biomater. 2020, 115, 29–50. [Google Scholar] [CrossRef]
- Yuan, L.; Ding, S.; Wen, C. Additive manufacturing technology for porous metal implant applications and triple minimal surface structures: A review. Bioact. Mater. 2019, 4, 56–70. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Xu, S.; Zhou, S.; Xu, W.; Leary, M.; Choong, P.; Qian, M.; Brandt, M.; Xie, Y.M. Topological design and additive manufacturing of porous metals for bone scaffolds and orthopaedic implants: A review. Biomaterials 2016, 83, 127–141. [Google Scholar] [CrossRef] [PubMed]
- Revilla-León, M.; Sadeghpour, M.; Özcan, M. A Review of the Applications of Additive Manufacturing Technologies Used to Fabricate Metals in Implant Dentistry. J. Prosthodont. 2020, 29, 579–593. [Google Scholar] [CrossRef] [PubMed]
- Ryan, G.; Pandit, A.; Apatsidis, D.P. Fabrication methods of porous metals for use in orthopaedic applications. Biomaterials 2006, 27, 2651–2670. [Google Scholar] [CrossRef]
- Wang, Z.; Wang, C.; Li, C.; Qin, Y.; Zhong, L.; Chen, B.; Li, Z.; Liu, H.; Chang, F.; Wang, J. Analysis of factors influencing bone ingrowth into three-dimensional printed porous metal scaffolds: A review. J. Alloys Compd. 2017, 717, 271–285. [Google Scholar] [CrossRef]
- Zhao, W.; Huang, Z.; Liu, L.; Wang, W.; Leng, J.; Liu, Y. Porous bone tissue scaffold concept based on shape memory PLA/Fe3O4. Compos. Sci. Technol. 2021, 203, 108563. [Google Scholar] [CrossRef]
- Zerankeshi, M.M.; Bakhshi, R.; Alizadeh, R. Polymer/metal composite 3D porous bone tissue engineering scaffolds fabricated by additive manufacturing techniques: A review. Bioprinting 2022, 25, e00191. [Google Scholar] [CrossRef]
- Attar, H.; Ehtemam-Haghighi, S.; Soro, N.; Kent, D.; Dargusch, M.S. Additive manufacturing of low-cost porous titanium-based composites for biomedical applications: Advantages, challenges and opinion for future development. J. Alloys Compd. 2020, 827, 154263. [Google Scholar] [CrossRef]
- Bose, S.; Koski, C.; Vu, A.A. Additive manufacturing of natural biopolymers and composites for bone tissue engineering. Mater. Horiz. 2020, 7, 2011–2027. [Google Scholar] [CrossRef]
- Neumann, M.; Epple, M. Composites of Calcium Phosphate and Polymers as Bone Substitution Materials. Eur. J. Trauma 2006, 32, 125–131. [Google Scholar] [CrossRef]
- Ødegaard, K.S.; Torgersen, J.; Elverum, C.W. Structural and Biomedical Properties of Common Additively Manufactured Biomaterials: A Concise Review. Metals 2020, 10, 1677. [Google Scholar] [CrossRef]
- Jing, Z.; Zhang, T.; Xiu, P.; Cai, H.; Wei, Q.; Fan, D.; Lin, X.; Song, C.-L.; Liu, Z. Functionalization of 3D-printed titanium alloy orthopedic implants: A literature review. Biomed. Mater. 2020, 15, 052003. [Google Scholar] [CrossRef] [PubMed]
- Carter, L.N.; Addison, O.; Naji, N.; Seres, P.; Wilman, A.H.; Shepherd, D.E.; Grover, L.; Cox, S. Reducing MRI susceptibility artefacts in implants using additively manufactured porous Ti-6Al-4V structures. Acta Biomater. 2020, 107, 338–348. [Google Scholar] [CrossRef] [PubMed]
- Frydman, G.H.; Marini, R.P.; Bakthavatchalu, V.; Biddle, K.E.; Muthupalani, S.; Vanderburg, C.R.; Lai, B.; Bendapudi, P.K.; Tompkins, R.G.; Fox, J.G. Local and systemic changes associated with long-term, percutaneous, static implantation of titanium alloys in rhesus macaques (Macaca mulatta). Comp. Med. 2017, 67, 165–175. [Google Scholar]
- Guo, T.; Gulati, K.; Arora, H.; Han, P.; Fournier, B.; Ivanovski, S. Race to invade: Understanding soft tissue integration at the transmucosal region of titanium dental implants. Dent. Mater. 2021, 37, 816–831. [Google Scholar] [CrossRef]
- Drnovšek, N.; Rade, K.; Milačič, R.; Štrancar, J.; Novak, S. The properties of bioactive TiO2 coatings on Ti-based implants. Surf. Coat. Technol. 2012, 209, 177–183. [Google Scholar] [CrossRef]
- Kim, K.T.; Eo, M.Y.; Nguyen, T.T.H.; Kim, S.M. General review of titanium toxicity. Int. J. Implant. Dent. 2019, 5, 10. [Google Scholar] [CrossRef] [Green Version]
- Noumbissi, S.; Scarano, A.; Gupta, S. A Literature Review Study on Atomic Ions Dissolution of Titanium and Its Alloys in Implant Dentistry. Materials 2019, 12, 368. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wennerberg, A.; Ide-Ektessabi, A.; Hatkamata, S.; Sawase, T.; Johansson, C.; Albrektsson, T.; Martinelli, A.; Sodervall, U.; Odelius, H. Titanium release from implants prepared with different surface roughness. Clin. Oral Implant. Res. 2004, 15, 505–512. [Google Scholar] [CrossRef] [PubMed]
- Ng, S.; Das, S.; Ting, Y.-P.; Wong, R.; Chanchareonsook, N. Benefits and Biosafety of Use of 3D-Printing Technology for Titanium Biomedical Implants: A Pilot Study in the Rabbit Model. Int. J. Mol. Sci. 2021, 22, 8480. [Google Scholar] [CrossRef] [PubMed]
- Přikrylová, J.; Procházková, J.; Podzimek, Š. Side effects of dental metal implants: Impact on human health (metal as a risk factor of implantologic treatment). BioMed Res. Int. 2019, 2019, 2519205. [Google Scholar] [CrossRef] [PubMed]
- Sidambe, A.T. Biocompatibility of Advanced Manufactured Titanium Implants-A Review. Materials 2014, 7, 8168–8188. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Aufa, A.N.; Hassan, M.Z.; Ismail, Z. Recent advances in Ti-6Al-4V additively manufactured by selective laser melting for biomedical implants: Prospect development. J. Alloys Compd. 2022, 896, 163072. [Google Scholar] [CrossRef]
- Fazel, M.; Salimijazi, H.R.; Shamanian, M.; Minneboo, M.; Modaresifar, K.; van Hengel, I.A.; Fratila-Apachitei, L.E.; Apachitei, I.; Zadpoor, A.A. Osteogenic and antibacterial surfaces on additively manufactured porous Ti-6Al-4V implants: Combining silver nanoparticles with hydrothermally synthesized HA nanocrystals. Mater Sci. Eng. C Mater. Biol. Appl. 2021, 120, 111745. [Google Scholar] [CrossRef]
- Spece, H.; Basgul, C.; Andrews, C.E.; MacDonald, D.W.; Taheri, M.L.; Kurtz, S.M. A systematic review of preclinical in vivo testing of 3D printed porous Ti6Al4V for orthopedic applications, part I: Animal models and bone ingrowth outcome measures. J. Biomed. Mater. Res. Part B Appl. Biomater. 2021, 109, 1436–1454. [Google Scholar] [CrossRef]
- Zhang, X.-Y.; Fang, G.; Zhou, J. Additively Manufactured Scaffolds for Bone Tissue Engineering and the Prediction of their Mechanical Behavior: A Review. Materials 2017, 10, 50. [Google Scholar] [CrossRef] [Green Version]
- Murr, L.E. Strategies for creating living, additively manufactured, open-cellular metal and alloy implants by promoting osseointegration, osteoinduction and vascularization: An overview. J. Mater. Sci. Technol. 2019, 35, 231–241. [Google Scholar] [CrossRef]
- Lowther, M.; Louth, S.; Davey, A.; Hussain, A.; Ginestra, P.; Carter, L.; Eisenstein, N.; Grover, L.; Cox, S. Clinical, industrial, and research perspectives on powder bed fusion additively manufactured metal implants. Addit. Manuf. 2019, 28, 565–584. [Google Scholar] [CrossRef] [Green Version]
- Ahmadi, S.; Hedayati, R.; Jain, R.A.K.; Li, Y.; Leeflang, S.; Zadpoor, A. Effects of laser processing parameters on the mechanical properties, topology, and microstructure of additively manufactured porous metallic biomaterials: A vector-based approach. Mater. Des. 2017, 134, 234–243. [Google Scholar] [CrossRef]
- Raghavendra, S.; Molinari, A.; Fontanari, V.; Luchin, V.; Zappini, G.; Benedetti, M.; Johansson, F.; Klarin, J. Tensile and compression properties of variously arranged porous Ti-6Al-4V additively manufactured structures via SLM. Procedia Struct. Integr. 2018, 13, 149–154. [Google Scholar] [CrossRef]
- Hanks, B.; Berthel, J.; Frecker, M.; Simpson, T.W. Mechanical properties of additively manufactured metal lattice structures: Data review and design interface. Addit. Manuf. 2020, 35, 101301. [Google Scholar] [CrossRef]
- Loginov, Y.N.; Koptyug, A.; Popov, V.V.; Belikov, S.V.; Mukanov, G.; Golodnov, A.I.; Stepanov, S.I. Compression deformation and fracture behavior of additively manufactured Ti–6Al–4V cellular structures. Int. J. Lightweight Mater. Manuf. 2022, 5, 126–135. [Google Scholar] [CrossRef]
- Zadpoor, A.A. Additively manufactured porous metallic biomaterials. J. Mater. Chem. B 2019, 7, 4088–4117. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zadpoor, A.A. Mechanics of additively manufactured biomaterials. J. Mech. Behav. Biomed. Mater. 2017, 70, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Hedayati, R.; Ahmadi, S.; Lietaert, K.; Pouran, B.; Li, Y.; Weinans, H.; Rans, C.; Zadpoor, A.A. Isolated and modulated effects of topology and material type on the mechanical properties of additively manufactured porous biomaterials. J. Mech. Behav. Biomed. Mater. 2018, 79, 254–263. [Google Scholar] [CrossRef]
- Sarker, A.; Leary, M.; Fox, K. Metallic additive manufacturing for bone-interfacing implants. Biointerphases 2020, 15, 050801. [Google Scholar] [CrossRef]
- Attarilar, S.; Ebrahimi, M.; Djavanroodi, F.; Fu, Y.; Wang, L.; Yang, J. 3D Printing Technologies in Metallic Implants: A Thematic Review on the Techniques and Procedures. Int. J. Bioprinting 2021, 7, 21–46. [Google Scholar] [CrossRef]
- Muthaiah, V.S.; Indrakumar, S.; Suwas, S.; Chatterjee, K. Surface engineering of additively manufactured titanium alloys for enhanced clinical performance of biomedical implants: A review of recent developments. Bioprinting 2022, 25, e00180. [Google Scholar] [CrossRef]
- Li, J.; Cui, X.; Hooper, G.J.; Lim, K.S.; Woodfield, T.B.F. Rational design, bio-functionalization and biological performance of hybrid additive manufactured titanium implants for orthopaedic applications: A review. J. Mech. Behav. Biomed. Mater. 2020, 105, 103671. [Google Scholar] [CrossRef] [PubMed]
- Wegst, U.G.; Bai, H.; Saiz, E.; Tomsia, A.P.; Ritchie, R.O. Bioinspired structural materials. Nat. Mater. 2015, 14, 23–36. [Google Scholar] [CrossRef] [PubMed]
- Yadroitsava, I.; du Plessis, A.; Yadroitsev, I. Bone Regeneration on Implants of Titanium Alloys Produced by Laser Powder Bed Fusion: A Review, in Titanium for Consumer Applications; Froes, F., Qian, M., Niinom, M.I., Eds.; Elsevier: Amsterdam, The Netherlands, 2019; pp. 197–233. [Google Scholar]
- Lin, C.-Y.; Kang, J.-H. Mechanical Properties of Compact Bone Defined by the Stress-Strain Curve Measured Using Uniaxial Tensile Test: A Concise Review and Practical Guide. Materials 2021, 14, 4224. [Google Scholar] [CrossRef]
- Currey, J. The Structure and Mechanical Properties of Bone, in Bioceramics and Their Clinical Applications; Kokubo, T., Ed.; Woodhead Publishing: Solston, UK, 2008; pp. 3–27. [Google Scholar]
- Kim, T.; See, C.W.; Li, X.; Zhu, D. Orthopedic implants and devices for bone fractures and defects: Past, present and perspective. Eng. Regen. 2020, 1, 6–18. [Google Scholar] [CrossRef]
- Bone Healing. Available online: https://www.foothealthfacts.org/conditions/bone-healing (accessed on 17 November 2021).
- Bone Healing after Implantation. Available online: http://dentalis-implants.com/resources/bone-maintenance/bone-healing-after-implantation/ (accessed on 25 November 2021).
- Niinomi, M.; Nakai, M. Titanium-Based Biomaterials for Preventing Stress Shielding between Implant Devices and Bone. Int. J. Biomater. 2011, 2011, 836587. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kelly, C.N.; Evans, N.T.; Irvin, C.W.; Chapman, S.C.; Gall, K.; Safranski, D.L. The effect of surface topography and porosity on the tensile fatigue of 3D printed Ti-6Al-4V fabricated by selective laser melting. Mater. Sci. Eng. C Mater. Biol. Appl. 2019, 98, 726–736. [Google Scholar] [CrossRef]
- Kelly, C.N.; Wang, T.; Crowley, J.; Wills, D.; Pelletier, M.H.; Westrick, E.R.; Adams, S.B.; Gall, K.; Walsh, W.R. High-strength, porous additively manufactured implants with optimized mechanical osseointegration. Biomaterials 2021, 279, 121206. [Google Scholar] [CrossRef]
- Li, G.; Wang, L.; Pan, W.; Yang, F.; Jiang, W.; Wu, X.; Kong, X.; Dai, K.; Hao, Y. In vitro and in vivo study of additive manufactured porous Ti6Al4V scaffolds for repairing bone defects. Sci. Rep. 2016, 6, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Titanium Alloy Guide; RMI Titanium Company: Niles, OH, USA, 2000; pp. 1–48.
- Ahmadi, S.M.; Jain, R.K.A.K.; Zadpoor, A.A.; Ayas, C.; Popovich, V.A. Effects of heat treatment on microstructure and mechanical behaviour of additive manufactured porous Ti6Al4V. Int. Conf. Smart Mater. Res. 2018, 293, 012009. [Google Scholar] [CrossRef]
- Rahmani, R.; Antonov, M.; Kollo, L.; Holovenko, Y.; Prashanth, K.G. Mechanical Behavior of Ti6Al4V Scaffolds Filled with CaSiO3 for Implant Applications. Appl. Sci. 2019, 9, 3844. [Google Scholar] [CrossRef] [Green Version]
- Xiong, Y.; Wang, W.; Gao, R.; Zhang, H.; Dong, L.; Qin, J.; Wang, B.; Jia, W.; Li, X. Fatigue behavior and osseointegration of porous Ti-6Al-4V scaffolds with dense core for dental application. Mater. Des. 2020, 195, 108994. [Google Scholar] [CrossRef]
- Koch, K.; Hargreaves, B.; Pauly, K.B.; Chen, W.; Gold, G.; King, K. Magnetic resonance imaging near metal implants. J. Magn. Reson. Imaging 2010, 32, 773–787. [Google Scholar] [CrossRef] [PubMed]
- Melancon, D.; Bagheri, Z.; Johnston, R.; Liu, L.; Tanzer, M.; Pasini, D. Mechanical characterization of structurally porous biomaterials built via additive manufacturing: Experiments, predictive models, and design maps for load-bearing bone replacement implants. Acta Biomater. 2017, 63, 350–368. [Google Scholar] [CrossRef]
- Yadroitsev, I.; Krakhmalev, P.; Yadroitsava, I. Hierarchical design principles of selective laser melting for high quality metallic objects. Addit. Manuf. 2015, 7, 45–56. [Google Scholar] [CrossRef]
- Gibson, I.; Rosen, D.; Stucker, B. Powder Bed Fusion Processes, in Additive Manufacturing Technologies: 3D Printing, Rapid Prototyping, and Direct Digital Manufacturing; Gibson, I., Rosen, D., Stucker, B., Eds.; Springer: New York, NY, USA, 2015; pp. 107–145. [Google Scholar]
- Weißmann, V.; Drescher, P.; Seitz, H.; Hansmann, H.; Bader, R.; Seyfarth, A.; Klinder, A.; Jonitz-Heincke, A. Effects of Build Orientation on Surface Morphology and Bone Cell Activity of Additively Manufactured Ti6Al4V Specimens. Materials 2018, 1, 915. [Google Scholar] [CrossRef] [Green Version]
- Sarker, A.; Tran, N.; Rifai, A.; Brandt, M.; Tran, P.; Leary, M.; Fox, K.; Williams, R. Rational design of additively manufactured Ti6Al4V implants to control Staphylococcus aureus biofilm formation. Materialia 2019, 5, 100250. [Google Scholar] [CrossRef]
- Huber, F.; Papke, T.; Scheitler, C.; Hanrieder, L.; Merklein, M.; Schmidt, M. In Situ Formation of a Metastable β-Ti Alloy by Laser Powder Bed Fusion (L-PBF) of Vanadium and Iron Modified Ti-6Al-4V. Metals 2018, 8, 1067. [Google Scholar] [CrossRef] [Green Version]
- Ødegaard, K.S.; Ouyang, L.; Ma, Q.; Buene, G.; Wan, D.; Elverum, C.W.; Torgersen, J.; Standal, T.; Westhrin, M. Revealing the influence of electron beam melted Ti-6Al-4V scaffolds on osteogenesis of human bone marrow-derived mesenchymal stromal cells. J. Mater Sci. Mater Med. 2021, 32, 97. [Google Scholar] [CrossRef]
- Chen, C.; Hao, Y.; Bai, X.; Ni, J.; Chung, S.-M.; Liu, F.; Lee, I.-S. 3D printed porous Ti6Al4V cage: Effects of additive angle on surface properties and biocompatibility; bone ingrowth in Beagle tibia model. Mater. Des. 2019, 175, 107824. [Google Scholar] [CrossRef]
- Hudák, R.; Schnitzer, M.; Králová, Z.; Gorejová, R.; Mitrík, L.; Rajťúková, V.; Tóth, T.; Kovačević, M.; Riznič, M.; Oriňaková, R.; et al. Additive Manufacturing of Porous Ti6Al4V Alloy: Geometry Analysis and Mechanical Properties Testing. Appl. Sci. 2021, 11, 2611. [Google Scholar] [CrossRef]
- Wieding, J.; Jonitz, A.; Bader, R. The Effect of Structural Design on Mechanical Properties and Cellular Response of Additive Manufactured Titanium Scaffolds. Materials 2012, 5, 1336–1347. [Google Scholar] [CrossRef]
- Wieding, J.; Fritsche, A.; Heinl, P.; Körner, C.; Cornelsen, M.; Seitz, H.; Mittelmeier, W.; Bader, R. Biomechanical behavior of bone scaffolds made of additive manufactured tricalciumphosphate and titanium alloy under different loading conditions. J. Appl. Biomater. Funct Mater 2013, 11, e159–e166. [Google Scholar] [CrossRef] [PubMed]
- El-Sayed, M.A.; Essa, K.; Ghazy, M.; Hassanin, H. Design optimization of additively manufactured titanium lattice structures for biomedical implants. Int. J. Adv. Manuf. Technol. 2020, 110, 2257–2268. [Google Scholar] [CrossRef]
- Goto, M.; Matsumine, A.; Yamaguchi, S.; Takahashi, H.; Akeda, K.; Nakamura, T.; Asanuma, K.; Matsushita, T.; Kokubo, T.; Sudo, A. Osteoconductivity of bioactive Ti-6Al-4V implants with lattice-shaped interconnected large pores fabricated by electron beam melting. J. Biomater. Appl. 2021, 35, 1153–1167. [Google Scholar] [CrossRef]
- Balcı, A.; Küçükaltun, F.; Aycan, M.F.; Usta, Y.; Demir, T. Reproducibility of Replicated Trabecular Bone Structures from Ti6Al4V Extralow Interstitials Powder by Selective Laser Melting. Arab. J. Sci. Eng. 2021, 46, 2527–2541. [Google Scholar] [CrossRef]
- Chen, Y.; Frith, J.; Dehghan-Manshadi, A.; Attar, H.; Kent, D.; Soro, N.D.M.; Bermingham, M.; Dargusch, M.S. Mechanical properties and biocompatibility of porous titanium scaffolds for bone tissue engineering. J. Mech. Behav. Biomed. Mater. 2017, 75, 169–174. [Google Scholar] [CrossRef]
- Tsai, P.-I.; Lam, T.-N.; Wu, M.-H.; Tseng, K.-Y.; Chang, Y.-W.; Sun, J.-S.; Li, Y.-Y.; Lee, M.-H.; Chen, S.-Y.; Chang, C.-K.; et al. Multi-scale mapping for collagen-regulated mineralization in bone remodeling of additive manufacturing porous implants. Mater. Chem. Phys. 2019, 230, 83–92. [Google Scholar] [CrossRef]
- Mitsak, A.G.; Kemppainen, J.M.; Harris, M.T.; Hollister, S.J. Effect of Polycaprolactone Scaffold Permeability on Bone Regeneration In Vivo. Tissue Eng. Part A 2011, 17, 1831–1839. [Google Scholar] [CrossRef] [Green Version]
- Arjunan, A.; Demetriou, M.; Baroutaji, A.; Wang, C.J. Mechanical performance of highly permeable laser melted Ti6Al4V bone scaffolds. J. Mech. Behav. Biomed. Mater. 2020, 102, 103517. [Google Scholar] [CrossRef]
- Hameed, P.; Liu, C.-F.; Ummethala, R.; Singh, N.; Huang, H.-H.; Manivasagam, G.; Prashanth, K.G. Biomorphic porous Ti6Al4V gyroid scaffolds for bone implant applications fabricated by selective laser melting. Prog. Addit. Manuf. 2021, 6, 455–469. [Google Scholar] [CrossRef]
- Zhang, S.; Wei, Q.; Cheng, L.; Li, S.; Shi, Y. Effects of scan line spacing on pore characteristics and mechanical properties of porous Ti6Al4V implants fabricated by selective laser melting. Mater. Des. 2014, 63, 185–193. [Google Scholar] [CrossRef]
- Coffigniez, M.; Gremillard, L.; Balvay, S.; Lachambre, J.; Adrien, J.; Boulnat, X. Direct-ink writing of strong and biocompatible titanium scaffolds with bimodal interconnected porosity. Addit. Manuf. 2021, 39, 101859. [Google Scholar] [CrossRef]
- Kan, T.; Xie, K.; Qu, Y.; Ai, S.; Jiang, W.; Wu, H.; Wang, L.; Yan, M. 3D-Printed Porous Titanium Augments for Reconstruction of Massive Bone Defect in Complex Revision Total Knee Arthroplasty: Implant Design and Surgical Technique. J. Shanghai Jiaotong Univ. 2021, 26, 334–338. [Google Scholar] [CrossRef]
- Umar, H.; Ghouse, S.; Nai, K.; Jeffers, J. Additively manufactured Ti6Al4V and ss316l stochastic structures with improved stiffness isotropy for biomaterial applications. Orthop. Proc. 2021, 103-B, 17. [Google Scholar] [CrossRef]
- Elsayed, H.; Rebesan, P.; Giacomello, G.; Pasetto, M.; Gardin, C.; Ferroni, L.; Zavan, B.; Biasetto, L. Direct ink writing of porous titanium (Ti6Al4V) lattice structures. Mater. Sci. Eng. C Mater. Biol. Appl. 2019, 103, 109794. [Google Scholar] [CrossRef]
- Soro, N.; Attar, H.; Brodie, E.; Veidt, M.; Molotnikov, A.; Dargusch, M.S. Evaluation of the mechanical compatibility of additively manufactured porous Ti-25Ta alloy for load-bearing implant applications. J. Mech. Behav. Biomed. Mater. 2019, 97, 149–158. [Google Scholar] [CrossRef]
- Wu, Y.; Kuo, C.; Wu, T.; Liu, T.; Chen, Y.; Guo, X.; Huang, J. Empirical rule for predicting mechanical properties of Ti-6Al-4V bone implants with radial-gradient porosity bionic structures. Mater. Today Commun. 2021, 27, 102346. [Google Scholar] [CrossRef]
- Wu, Y.; Kuo, C.; Shie, M.; Su, Y.; Wei, L.-J.; Chen, S.; Huang, J. Structural design and mechanical response of gradient porous Ti-6Al-4V fabricated by electron beam additive manufacturing. Mater. Des. 2018, 158, 256–265. [Google Scholar] [CrossRef]
- Onal, E.; Frith, J.E.; Jurg, M.; Wu, X.H.; Molotnikov, A. Mechanical Properties and In Vitro Behavior of Additively Manufactured and Functionally Graded Ti6Al4V Porous Scaffolds. Metals 2018, 8, 200. [Google Scholar] [CrossRef] [Green Version]
- Davoodi, E.; Montazerian, H.; Esmaeilizadeh, R.; Darabi, A.C.; Rashidi, A.; Kadkhodapour, J.; Jahed, H.; Hoorfar, M.; Milani, A.S.; Weiss, P.S.; et al. Additively Manufactured Gradient Porous Ti–6Al–4V Hip Replacement Implants Embedded with Cell-Laden Gelatin Methacryloyl Hydrogels. ACS Appl. Mater. Interfaces 2021, 13, 22110–22123. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.-Y.; Fang, G.; Leeflang, S.; Zadpoor, A.A.; Zhou, J. Topological design, permeability and mechanical behavior of additively manufactured functionally graded porous metallic biomaterials. Acta Biomater. 2019, 84, 437–452. [Google Scholar] [CrossRef] [PubMed]
- Murphy, C.M.; O’Brien, F.J. Understanding the effect of mean pore size on cell activity in collagen-glycosaminoglycan scaffolds. Cell Adhes. Migr. 2010, 4, 377–381. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, F.; Li, J.; Kou, H.; Zhou, L. Porous Ti6Al4V alloys with enhanced normalized fatigue strength for biomedical applications. Mater. Sci. Eng. C Mater. Biol. Appl. 2016, 60, 485–488. [Google Scholar] [CrossRef] [PubMed]
- Van Bael, S.; Chai, Y.C.; Truscello, S.; Moesen, M.; Kerckhofs, G.; Van Oosterwyck, H.; Kruth, J.-P.; Schrooten, J. The effect of pore geometry on the in vitro biological behavior of human periosteum-derived cells seeded on selective laser-melted Ti6Al4V bone scaffolds. Acta Biomater. 2012, 8, 2824–2834. [Google Scholar] [CrossRef] [PubMed]
- Vee San, C.; Mumith, A.; Coathup, M.J.; Blunn, G.W.; Fromme, P. Bone remodeling in additive manufactured porous implants changes the stress distribution. In Health Monitoring of Structural and Biological Systems XIV; International Society for Optics and Photonics: Bellingham, WA, USA, 2020. [Google Scholar] [CrossRef]
- Xiong, Y.-Z.; Gao, R.-N.; Zhang, H.; Dong, L.-L.; Li, J.-T.; Li, X. Rationally designed functionally graded porous Ti6Al4V scaffolds with high strength and toughness built via selective laser melting for load-bearing orthopedic applications. J. Mech. Behav. Biomed. Mater. 2020, 104, 103673. [Google Scholar] [CrossRef] [PubMed]
- Wu, M.-W.; Chen, J.-K.; Lin, B.-H.; Chiang, P.-H. Improved fatigue endurance ratio of additive manufactured Ti-6Al-4V lattice by hot isostatic pressing. Mater. Des. 2017, 134, 163–170. [Google Scholar] [CrossRef]
- Lietaert, K.; Cutolo, A.; Boey, D.; Van Hooreweder, B. Fatigue life of additively manufactured Ti6Al4V scaffolds under tension-tension, tension-compression and compression-compression fatigue load. Sci. Rep. 2018, 8, 4957. [Google Scholar] [CrossRef] [Green Version]
- Razavi, S.M.J.; Bordonaro, G.G.; Ferro, P.; Torgersen, J.; Berto, F. Fatigue Behavior of Porous Ti-6Al-4V Made by Laser-Engineered Net Shaping. Materials 2018, 11, 284. [Google Scholar] [CrossRef] [Green Version]
- Li, P.; Warner, D.; Fatemi, A.; Phan, N. Critical assessment of the fatigue performance of additively manufactured Ti–6Al–4V and perspective for future research. Int. J. Fatigue 2016, 85, 130–143. [Google Scholar] [CrossRef]
- Mahmoud, D.; Al-Rubaie, K.S.; Elbestawi, M.A. The influence of selective laser melting defects on the fatigue properties of Ti6Al4V porosity graded gyroids for bone implants. Int. J. Mech. Sci. 2021, 193, 106180. [Google Scholar] [CrossRef]
- Ren, D.; Li, S.; Wang, H.; Hou, W.; Hao, Y.; Jin, W.; Yang, R.; Misra, R.D.K.; Murr, L.E. Fatigue behavior of Ti-6Al-4V cellular structures fabricated by additive manufacturing technique. J. Mater. Sci. Technol. 2019, 35, 285–294. [Google Scholar] [CrossRef]
- Zhao, S.; Li, S.; Hou, W.; Hao, Y.; Yang, R.; Misra, R. The influence of cell morphology on the compressive fatigue behavior of Ti-6Al-4V meshes fabricated by electron beam melting. J. Mech. Behav. Biomed. Mater. 2016, 59, 251–264. [Google Scholar] [CrossRef] [PubMed]
- Hrabe, N.W.; Heinl, P.; Flinn, B.; Körner, C.; Bordia, R.K. Compression-compression fatigue of selective electron beam melted cellular titanium (Ti-6Al-4V). J. Biomed. Mater. Res. Part B Appl. Biomater. 2011, 99, 313–320. [Google Scholar] [CrossRef]
- Wu, M.-W.; Chen, J.-K.; Lin, B.-H.; Chiang, P.-H.; Tsai, M.-K. Compressive fatigue properties of additive-manufactured Ti-6Al-4V cellular material with different porosities. Mater. Sci. Eng. A 2020, 790, 139695. [Google Scholar] [CrossRef]
- Dallago, M.; Fontanari, V.; Winiarski, B.; Zanini, F.; Carmignato, S.; Benedetti, M. Fatigue properties of Ti6Al4V cellular specimens fabricated via SLM: CAD vs real geometry. Procedia Struct. Integr. 2017, 7, 116–123. [Google Scholar] [CrossRef]
- Zhao, S.; Li, S.; Wang, S.; Hou, W.; Li, Y.; Zhang, L.; Hao, Y.; Yang, R.; Misra, R.; Murr, L. Compressive and fatigue behavior of functionally graded Ti-6Al-4V meshes fabricated by electron beam melting. Acta Mater. 2018, 150, 1–15. [Google Scholar] [CrossRef]
- Pérez-Sánchez, A.; Yánez, A.; Cuadrado, A.; Martel, O.; Nuño, N. Fatigue behaviour and equivalent diameter of single Ti-6Al-4V struts fabricated by Electron Bean Melting orientated to porous lattice structures. Mater. Des. 2018, 155, 106–115. [Google Scholar] [CrossRef]
- Günther, J.; Leuders, S.; Koppa, P.; Tröster, T.; Henkel, S.; Biermann, H.; Niendorf, T. On the effect of internal channels and surface roughness on the high-cycle fatigue performance of Ti-6Al-4V processed by SLM. Mater. Des. 2018, 143, 1–11. [Google Scholar] [CrossRef]
- Li, F.; Li, J.; Huang, T.; Kou, H.; Zhou, L. Compression fatigue behavior and failure mechanism of porous titanium for biomedical applications. J. Mech. Behav. Biomed. Mater. 2017, 65, 814–823. [Google Scholar] [CrossRef]
- Yavari, S.A.; Ahmadi, S.; van der Stok, J.; Wauthle, R.; Riemslag, A.; Janssen, M.; Schrooten, J.; Weinans, H.; Zadpoor, A.A. Effects of bio-functionalizing surface treatments on the mechanical behavior of open porous titanium biomaterials. J. Mech. Behav. Biomed. Mater. 2014, 36, 109–119. [Google Scholar] [CrossRef] [PubMed]
- Ahmadi, S.M.; Kumar, R.; Borisov, E.V.; Petrov, R.; Leeflang, S.; Li, Y.; Tümer, N.; Huizenga, R.; Ayas, C.; Zadpoor, A.A.; et al. From microstructural design to surface engineering: A tailored approach for improving fatigue life of additively manufactured meta-biomaterials. Acta Biomater. 2019, 83, 153–166. [Google Scholar] [CrossRef] [PubMed]
- Günther, J.; Pessard, E.; Morel, F.; Prigent, S. Fatigue behavior of Ti-6Al-4V additively manufactured by selective laser and electron beam melting—On the impact of the chemical composition, process-induced porosity and surface roughness. Int. J. Fatigue 2017, 140, 105811. [Google Scholar]
- Leuders, S.; Lieneke, T.; Lammers, S.; Tröster, T.; Niendorf, T. On the fatigue properties of metals manufactured by selective laser melting—The role of ductility. J. Mater. Res. 2014, 29, 1911–1919. [Google Scholar] [CrossRef]
- Kasperovich, G.; Hausmann, J. Improvement of fatigue resistance and ductility of TiAl6V4 processed by selective laser melting. J. Mater. Processing Technol. 2015, 220, 202–214. [Google Scholar] [CrossRef]
- Demirci, S.; Dalmış, R.; Dikici, T.; Tünçay, M.M.; Kaya, N.; Güllüoğlu, A.N. Effect of surface modifications of additively manufactured Ti-6Al-4V alloys on apatite formation ability for biomedical applications. J. Alloys Compd. 2021, 887, 161445. [Google Scholar] [CrossRef]
- Chudinova, E.A.; Surmeneva, M.A.; Timin, A.S.; Karpov, T.E.; Wittmar, A.; Ulbricht, M.; Ivanova, A.; Loza, K.; Prymak, O.; Koptyug, A.; et al. Adhesion, proliferation, and osteogenic differentiation of human mesenchymal stem cells on additively manufactured Ti6Al4V alloy scaffolds modified with calcium phosphate nanoparticles. Colloids Surf. B Biointerfaces 2019, 176, 130–139. [Google Scholar] [CrossRef]
- Jia, Z.; Li, M.; Xiu, P.; Xu, X.; Cheng, Y.; Zheng, Y.; Xi, T.; Wei, S.; Liu, Z. A novel cytocompatible, hierarchical porous Ti6Al4V scaffold with immobilized silver nanoparticles. Mater. Lett. 2015, 157, 143–146. [Google Scholar] [CrossRef]
- Van Hengel, I.A.J.; Gelderman, F.S.A.; Athanasiadis, S.; Minneboo, M.; Weinans, H.; Fluit, A.C.; van der Eerden, B.C.J.; Fratila-Apachitei, L.E.; Apachitei, I.; Zadpoor, A.A. Functionality-packed additively manufactured porous titanium implants. Mater. Today Bio. 2020, 7, 100060. [Google Scholar] [CrossRef]
- Li, J.; Yuan, H.; Chandrakar, A.; Moroni, L.; Habibovic, P. 3D porous Ti6Al4V-beta-tricalcium phosphate scaffolds directly fabricated by additive manufacturing. Acta Biomater. 2021, 126, 496–510. [Google Scholar] [CrossRef]
- Perets, T.; Ben Ghedalia-Peled, N.; Vago, R.; Goldman, J.; Shirizly, A.; Aghion, E. In vitro behavior of bioactive hybrid implant composed of additively manufactured titanium alloy lattice infiltrated with Mg-based alloy. Mater. Sci. Eng. C 2021, 129, 112418. [Google Scholar] [CrossRef] [PubMed]
- Bartolomeu, F.; Costa, M.M.; Alves, N.; Miranda, G.; Silva, F.S. Additive manufacturing of NiTi-Ti6Al4V multi-material cellular structures targeting orthopedic implants. Opt. Lasers Eng. 2020, 134, 106208. [Google Scholar] [CrossRef]
- Lei, H.; Yi, T.; Fan, H.; Pei, X.; Wu, L.; Xing, F.; Li, M.; Liu, L.; Zhou, C.; Fan, Y.; et al. Customized additive manufacturing of porous Ti6Al4V scaffold with micro-topological structures to regulate cell behavior in bone tissue engineering. Mater. Sci. Eng. C 2021, 120, 111789. [Google Scholar] [CrossRef] [PubMed]
- Kayacan, M.C.; Baykal, Y.B.; Karaaslan, T.; Özsoy, K.; Alaca, I.; Duman, B.; Delikanlı, Y.E. Monitoring the osseointegration process in porous Ti6Al4V implants produced by additive manufacturing: An experimental study in sheep. J. Appl. Biomater. Funct. Mater. 2018, 16, 68–75. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhang, B.; Pei, X.; Zhou, C.; Fan, Y.; Jiang, Q.; Ronca, A.; D’Amora, U.; Chen, Y.; Li, H.; Sun, Y.; et al. The biomimetic design and 3D printing of customized mechanical properties porous Ti6Al4V scaffold for load-bearing bone reconstruction. Mater. Des. 2018, 152, 30–39. [Google Scholar] [CrossRef]
- Li, J.-L.; Wang, S.; Cao, F.; Lin, X.; Wei, X.-W.; Zhao, Z.-H.; Dou, X.-J.; Yu, W.-T.; Yang, K.; Zhao, D.-W. Fabrication and Characterization of Nanopillar-Like HA Coating on Porous Ti6Al4V Scaffold by a Combination of Alkali-Acid-Heat and Hydrothermal Treatments. Acta Metall. Sin. Engl. Lett. 2019, 32, 1075–1088. [Google Scholar] [CrossRef] [Green Version]
- Cheong, V.S.; Fromme, P.; Mumith, A.; Coathup, M.J.; Blunn, G.W. Novel adaptive finite element algorithms to predict bone ingrowth in additive manufactured porous implants. J. Mech. Behav. Biomed. Mater. 2018, 87, 230–239. [Google Scholar] [CrossRef] [Green Version]
- Bandyopadhyay, A.; Mitra, I.; Shivaram, A.; Dasgupta, N.; Bose, S. Direct comparison of additively manufactured porous titanium and tantalum implants towards in vivo osseointegration. Addit. Manuf. 2019, 28, 259–266. [Google Scholar] [CrossRef]
- MacBarb, R.F.; Lindsey, D.P.; Bahney, C.S.; Woods, S.A.; Wolfe, M.L.; Yerby, S.A. Fortifying the Bone-Implant Interface Part 1: An In Vitro Evaluation of 3D-Printed and TPS Porous Surfaces. Int. J. Spine Surg. 2017, 11, 105–115. [Google Scholar] [CrossRef] [Green Version]
- Koju, N.; Sikder, P.; Ren, Y.; Zhou, H.; Bhaduri, S.B. Biomimetic coating technology for orthopedic implants. Curr. Opin. Chem. Eng. 2017, 15, 49–55. [Google Scholar] [CrossRef] [Green Version]
| Property | Upper Limit | Lower Limit | Modal Value |
|---|---|---|---|
| Young’s Modulus of Elasticity (E) | 45 GPa | 6 GPa | 15 GPa |
| Tensile Yield Stress | N/A | 10 MPa | 120 MPa |
| Tensile Strength | 300 MPa | 15 MPa | 150 MPa |
| Ultimate Tensile Strain | 0.12 | 0.002 | 0.03 |
| Compressive Strength | N/A | N/A | 250 MPa |
| Bending Strength | N/A | N/A | 250 MPa |
| Fatigue Life at 0–100 MPa Tension | N/A | 200 | 1000 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Koju, N.; Niraula, S.; Fotovvati, B. Additively Manufactured Porous Ti6Al4V for Bone Implants: A Review. Metals 2022, 12, 687. https://doi.org/10.3390/met12040687
Koju N, Niraula S, Fotovvati B. Additively Manufactured Porous Ti6Al4V for Bone Implants: A Review. Metals. 2022; 12(4):687. https://doi.org/10.3390/met12040687
Chicago/Turabian StyleKoju, Naresh, Suyash Niraula, and Behzad Fotovvati. 2022. "Additively Manufactured Porous Ti6Al4V for Bone Implants: A Review" Metals 12, no. 4: 687. https://doi.org/10.3390/met12040687
APA StyleKoju, N., Niraula, S., & Fotovvati, B. (2022). Additively Manufactured Porous Ti6Al4V for Bone Implants: A Review. Metals, 12(4), 687. https://doi.org/10.3390/met12040687







