The Use of Interpreters in Medical Education: A Narrative Literature Review
Abstract
1. Introduction
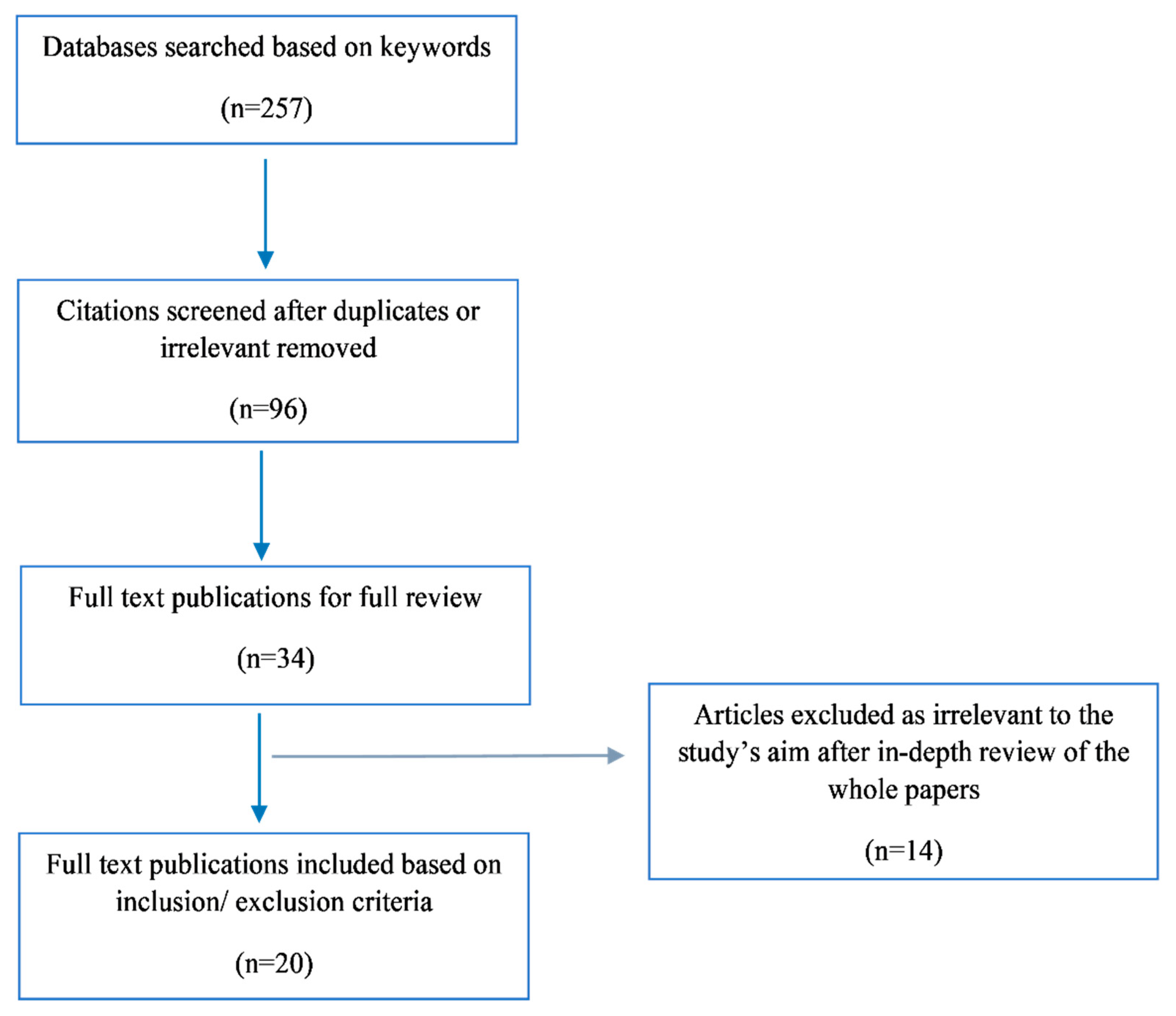
2. Methodology
3. Results
3.1. Use of Interpreters during Undergraduate Medical/Health Care Curricula
- The trainee asked the patient one question at a time.
- The trainee presented information at a pace that was easy to follow for both patient and interpreter—that is, information was given in digestible chunks
- The trainee addressed the patient as “you” and not as “he” or “she.”
- The trainee appropriately closed the encounter: at a minimum, asked the patient if he or she had any questions.
- Asked patient one question at a time
- Addressed patient directly
- Maintained direct eye contact with patient
- Listened to interpreter without unnecessary interruption
- Asked interpreter questions about incomplete interpretations
- Spoke in short, simple sentences with pauses for interpretation
3.2. Developing Students’ Skills through Training in How to Use Interpreters in Health Care Interviews or Consultations
4. Critical Appraisal of the Articles Reviewed
5. Discussion
- What is the effect of the use of interpreters on the quality of medical education?
- What are the levels of confidence and self-efficacy of medical students in using interpreters in medical education (e.g., when they interact and interview LEP patients in their clinical placements)?
- What are the facilitators and barriers for using interpreters in medical education for medical students, their supervisors, and the patients?
- How do patients experience and understand the use of interpreters?
- What are the perspectives of interpreters, health care providers (e.g., clinics, hospitals, health care facilities, etc.), and medical educators?
- How is the use of interpreters in medical education associated with health outcomes?
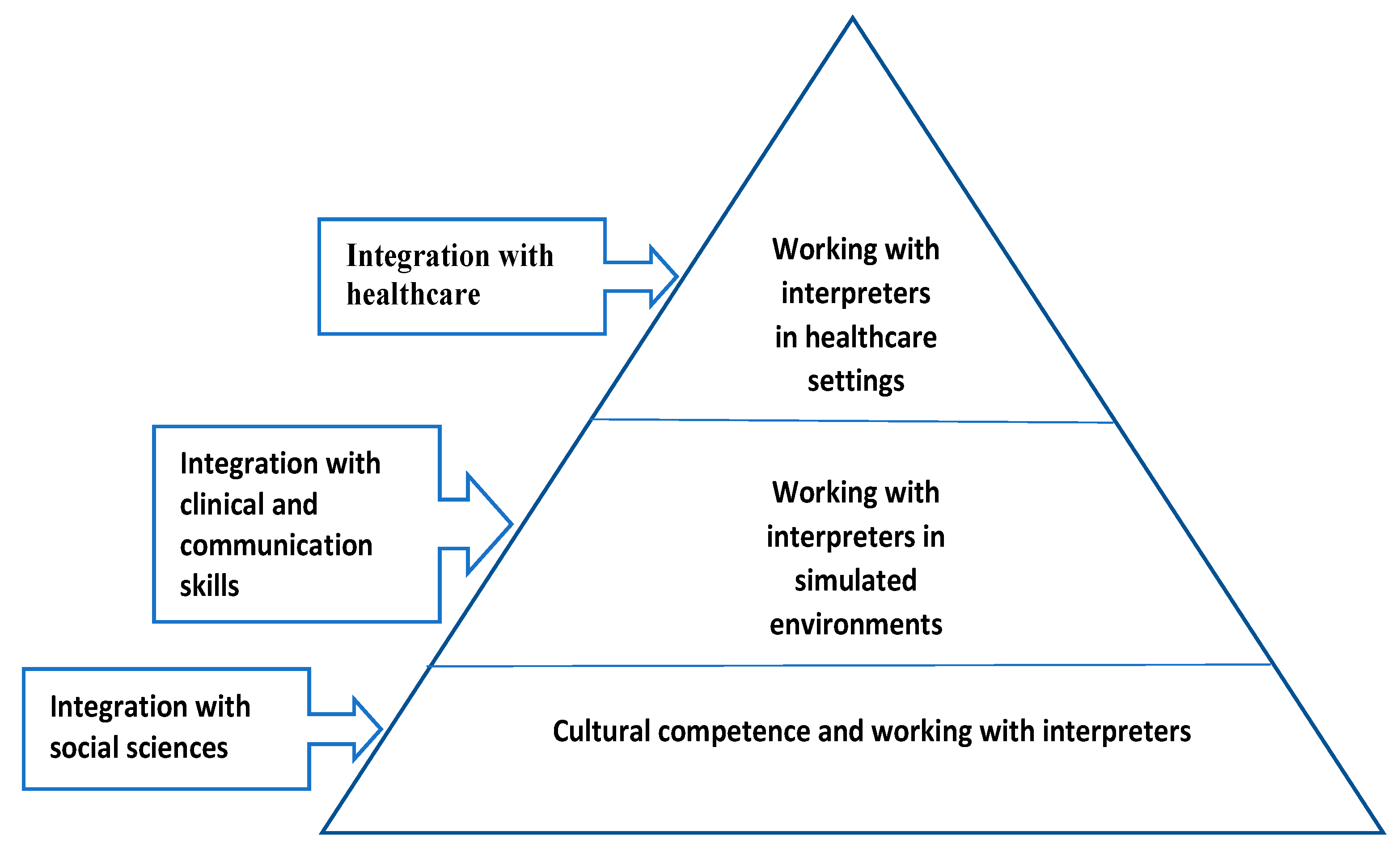
- What skills do students develop when collaborating with interpreters during their medical education?
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
Appendix A
| In-Text Citation | Article | Type of Research and Participants | Aim/ Key Findings | Was There a Clear Aim or Research Question? | Was the Methodology Appropriate? | Was the Research Design Appropriate to Address the Aim? | Was the Recruitment Strategy Appropriate to the Aims of the Research? | Was the Data Collected in a Way That Addressed the Research Issue? | Have Ethical Issues Been Taken into Consideration? | Was the Data Analysis Sufficiently Rigorous? | Is There a Clear Statement of Findings? | How Valuable is the Research? |
| 13 | Himmelstein J., Wright W.S., Wiederman M.W. U.S. medical school curricula on working with medical interpreters and/or patients with limited English proficiency. Adv Med Educ Pract. 2018;9:729–733. | Survey, 38 Schools | Aim: to describe curricula offered by the United States medical schools to teach students to work with medical interpreters and patients with LEP. Key findings: Of the 38 respondents, 29 had curriculum to prepare students to work with medical interpreters and/or patients with LEP and 10 of those had experiences with standardized patients to actually practice. The other 9 schools did not have training part of formal curriculum. | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| 18 | Itaya LE, Glassman P, Gregorczyk S, Bailit HL. Dental school patients with limited English proficiency: the California experience. J Dent Educ. 2009;73(9):1055–1064. | Survey, 122 students, 56 faculty members from 5 dental schools | Aim: to survey dental schools in California with respect to the number, communication strategies, impact on education and clinic finances, and student and faculty perceptions regarding serving LEP patients in their clinics. Key findings: The results of this survey suggest that dental schools face serious challenges in complying with federal standards for the treatment of LEP patients. Most students believed the current system of using untrained interpreters (e.g., family/friends) was adequate, but they also said it was more difficult to treat LEP patients. | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes |
| 19 | Simon L, Hum L, Nalliah R. Training to Care for Limited English Proficient Patients and Provision of Interpreter Services at U.S. Dental School Clinics. J Dent Educ. 2017;81(2):169–177. | Survey, 325 students | Aim: to survey dental students about their clinical experience with LEP patients, the interpreter resources available at their dental school clinics, and the extent of instruction on these topics. Key findings: The majority of responding students (56.3%) indicated there was some form of interpreter services available on their clinic floor. 43.7% indicated their dental school clinic lacked formal interpreter services, and 35.4% reported that their institution did not take language into account when assigning LEP patients to student clinicians. 37.2% reported that no curricular content pertaining to LEP patients was available. | Yes | Yes | Yes | No | Yes | Can’t tell | Yes | Yes | Yes |
| 20 | Omoruyi EA, Dunkle J, Dendy C, McHugh E, Barratt MS. Cross Talk: Evaluation of a Curriculum to Teach Medical Students How to Use Telephone Interpreter Services. Acad Pediatr. 2018;18(2):214–219. | Web-based training/ pre-post test, 176 students | Aim: to determine if training improves self-reported competency. Key findings: Self-assessment showed that students improved competency in telephone interpretation use. Comparing Average Scores of Audio Files in non-curriculum and curriculum groups, there was higher scores in the curriculum students. | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
| 21 | Mazori AY, Maron MI, Osterbur ML Badhey, et al. Enhancing Medical Student-Interpreter Collaboration in an Urban Free Clinic. Fam Med. 2019;51(7):593–597. | Randomized control trial, 76 trainees (36 control, 40 intervention) | Aim: to explore the effectiveness of working with interpreters in a clinic. Key findings: The students that had the intervention training scored higher by the interpreters since they were more likely to ask patient 1 question at a time, listen to interpreter without unnecessary interruption, and speak in short/simple sentences with pauses. | Yes | Yes | Yes | Yes | Yes | Can’t tell | Yes | Yes | Yes |
| 22 | Kalet A, Gany F, Senter L. Working with interpreters: an interactive Web-based learning module. Acad Med. 2002;77(9):927. | Web-based training/ pre-post test, 160 students, no control group | Hypothesis: what is the effectiveness of a web-based module aimed at teaching students effective strategies for working with interpreters and diverse patient populations? Students improved by 20% on MCQ post-test and 86% of students were satisfied with learning experience and acquired new knowledge. | Yes | Yes | Yes | No | Yes | Can’t tell | Yes | Yes | Yes |
| 23 | Kalet AL, Mukherjee D, Felix K, et al. Can a web-based curriculum improve students’ knowledge of, and attitudes about, the interpreted medical interview? J Gen Intern Med. 2005;20(10):929–934. | Web-based training/ pre-post test, 640 students, no control group | Aim: to develop and evaluate a web-based curriculum to introduce first-year students to the knowledge and attitudes necessary for working with LEP patients through interpreters. Key findings: Tested knowledge questions improved from 42% to 64% correct pre- to post- test. Pre- and post-module attitude and belief scores were considered statistically significantly improved | Yes | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes |
| 24 | Lie D, Bereknyei S, Kalet A, Braddock C 3rd. Learning outcomes of a web module for teaching interpreter interaction skills to pre-clerkship students. Fam Med. 2009;41(4):234–235. | Web-based module, pre-post test, control/intervention groups, 3 medical schools, 304 students | Aim: to evaluate the impact of training in working with LEP patients through interpreters. Key findings: Post-test MCQ test results are improved in those that took part in an online interpreter interaction skills module. However, clinical skills score did not correlate with the magnitude of knowledge gain. | Yes | Yes | Yes | No | Yes | Can’t tell | Yes | Yes | Yes |
| 25 | Fung CC, Lagha RR, Henderson P, Gomez AG. Working with interpreters: how student behavior affects quality of patient interaction when using interpreters. Med Educ Online. 2010;15:10.3402/meo.v15i0.511. | Workshop training, 152 students, OSCE examination, no control group | Aim: to evaluate the effectiveness of a workshop. Key findings: Students did well in managing the interpreted encounter, but had the biggest issue preparing the encounter in that the biggest failed items were arranging the patient and interpreter as they were taught and ensuring confidentiality. | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
| 26 | Lie DA, Bereknyei S, Vega CP. Longitudinal development of medical students’ communication skills in interpreted encounters. Educ Health (Abingdon). 2010;23(3):466. | One year training, clinical performance assessment and questionnaires, no control group, 192 students | Hypothesis: students will show improvement in objective ratings of communication skills in the interpreted encounter over one year of clinical training. Performance as rated by the patient did not change significantly (after a year of clinical training) for seven items. The ratings by the interpreter improved in two behaviors of setting the stage and introductions. However, performance was worse in some behaviors. | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
| 27 | Hasbún Avalos O, Pennington K, Osterberg L. Revolutionizing volunteer interpreter services: an evaluation of an innovative medical interpreter education program. J Gen Intern Med. 2013;28(12):1589–1595. | 6 months training, pre-post evaluation, written and oral assessment, 38 students, no control group | Aim: to evaluate the effectiveness of a training program. Key findings: Self-assessed knowledge, skills, and confidence were noted but the value of these changes was unclear. Written testing knowledge of the roles and skills of interpreters needed for proper medical interpretation improved. More students passed oral interpretation exams (a pass was being able to maintain the intended message) after training. This is the highest quality measurement of the program in the paper. | Yes | Yes | Yes | No | No | Yes | Yes | Yes | Yes |
| 28 | Bansal, A, Swann, J & Smithson, WH 2014, “Using professional interpreters in undergraduate medical consultation skills teaching”, Advances in medical education and practice, vol. 5, pp. 439–450. | Training, Survey, self-reported questionnaires completed by students and GP tutors, 274 students and 8 GP tutors | Aim: to evaluate the effectiveness of training. Key findings: Students’ perceived confidence in consulting increased with interpreter training. GP tutor explained that training helped themselves by filling a gap in their own skills to be used in practice, and the training was helpful and interactive for students | Yes | Yes | No | No | No | No | Can’t tell | Yes | No |
| 29 | Quick KK, Selameab T, Woll A, Mazzei C, Miller JL. Creating and Evaluating Skills-Based Training in Working with Spoken-Language Interpreters for Oral Health Professions Students. J Dent Educ. 2019;83(6):645–653. | Workshop training, pre-post test, 294 students, intervention and control groups, 1 focus group with 11 students | Aim: to evaluate the effectiveness of a training program in terms of trainees’ familiarity and confidence. Both familiarity and confidence in working with LEP patients increased significantly after the training. | Yes | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes |
| 30 | McEvoy M, Santos MT, Marzan M, Green EH, Milan FB. Teaching medical students how to use interpreters: a three year experience. Med Educ Online. 2009;14:12. | Training, pre-post test and feedback, 110 students, no control group | Aim: to evaluate the effectiveness of training. Key findings: The study showed that the session was effective in increasing students’ perceived efficacy for using the skills to communicate with a patient with LEP, give instructions to an untrained interpreter, and access a telephone interpreter. | Yes | Yes | Yes | No | No | Can’t tell | No | Yes | Yes |
| 31 | Ikram UZ, Essink-Bot ML, Suurmond J. How we developed an effective e-learning module for medical students on using professional interpreters. Med Teach. 2015;37(5):422–427. | E-learning training module, pre-post test, 281 students, no control group | Aim: to develop an effective e-learning module for medical students on using professional interpreters. Key findings: Professional interpreter use knowledge and self-efficacy increased after completing a teaching e-module. | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
| 32 | Marion GS, Hildebrandt CA, Davis SW, Marín AJ, Crandall SJ. Working effectively with interpreters: a model curriculum for physician assistant students. Med Teach. 2008;30(6):612–617. | Training, 12-item check list and student feedback, 96 students, no control group, no pre-post test | Aim: to see if physician assistant students could effectively use interpreters to communicate with Spanish-speaking patients after implementation of a cultural competency and medical Spanish curriculum. Key findings: Based on anevaluation of student performance using a 12-item checklist and student feedback on the curriculum, the enhancements were proven successful and feasible | Yes | No | Yes | No | No | Yes | Yes | Yes | No |
| 33 | Jacobs EA, Diamond LC, Stevak L. The importance of teaching clinicians when and how to work with interpreters. Patient Educ Couns. 2010;78(2):149–153. | Training, 72 students, pre-post test, no control group | Aim: to describe the importance of teaching students when and how to overcome language barriers in clinical practice, provide an example of a curriculum for teaching on this topic, and outline the critical issues that must be addressed in this type of teaching. Key findings: Students improved in working with an interpreter, were significantly more likely to endorse that it is easy to work with interpreters, that cultural competency is necessary to provide high quality health care, that the information obtained through interpreters is accurate, and that they will not find it frustrating and more rewarding to care for limited English proficient (LEP) patients. | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
| 34 | Aitken, G 2019, “Medical Students as Certified Interpreters”, AMA journal of ethics, vol. 21, no. 3, pp. E232–E238. | Descriptive paper | Aim: to look at the interpreter certification program created at a US University to certify medical students as interpreters themselves. Students serving as interpreters gained more experience/exposure, and built cultural competency. On the other hand, they found it hard to separate roles as clinicians vs interpreters. | Yes | Yes | Yes | N/A | N/A | N/A | Yes | Yes | Yes |
| 35 | Mihalic AP, Morrow JB, Long RB & Dobbie AE 2010, “A validated cultural competence curriculum for US pediatric clerkships”, Patient Education & Counseling, vol. 79, no. 1, pp. 77–82. | Survey, self-reported, 149 students, 1 focus group | Aim: to evaluate curriculum in cultural competence. Key findings: improved skills in working with interpreters (90%), improved skills in cross-cultural communication (82%), increased knowledge of racial and ethnic disparities (89%), increased their knowledge of core cultural issues and their impact on health care (91%), and increased their level of awareness and understanding of the culture of medicine (91%). Cultural knowledge test became validated in achieving target reliability of 0.7 for combined pre- and post-tests. Score gain of 17% considered significant | Yes | Yes | Yes | No | No | Yes | Yes | Yes | Yes |
| 36 | Pelaez AF, Ramirez SI, Valdes Sanchez C, et al. Implementing a medical student interpreter training program as a strategy to developing humanism. BMC Med Educ. 2018;18(1):141. | Training, no control, pre-post surveys, 80 students. | Aim: to address issues by implementing a medical interpretation training program with bilingual medical students with the goal of creating a sustainable language access program and increasing students’ communication skills and empathy, potentially resulting in more humanistic medical professionals. Key findings: After training, 98% felt more confident about interpreting, 87.5% felt more empathy for LEP patients. Program well received by students since 100% recommended training | Yes | Yes | Yes | No | No | Can’t tell | Yes | Yes | Yes |
References
- Alizadeh, S.; Chavan, M. Cultural competence dimensions and outcomes: A systematic review of the literature. Health Soc. Care Community 2016, 24, 117–130. [Google Scholar] [CrossRef]
- Betancourt, J.; Green, A.R.; Carrillo, J.E.; Ananeh-Firempong, O. Defining cultural competence: A practical framework for addressing racial/ethnic disparities in health and health care. Public Health Rep. 2003, 118, 293–302. [Google Scholar] [CrossRef]
- Constantinou, C.S.; Papageorgiou, A.; Andreou, P.; McCrorie, P. How to integrate cultural competence in medical curricula: Learning from a new medical programme. MedEdPublish 2020, 9. [Google Scholar] [CrossRef]
- Constantinou, C.S.; Papageorgiou, A.; Samoutis, G.; McCrorie, P. Acquire, apply, and activate knowledge: A pyramid model for teaching and integrating cultural competence in medical curricula. Patient Educ. Couns. 2018, 101, 1147–1151. [Google Scholar] [CrossRef] [PubMed]
- Borrell-Carrió, F.; Suchman, A.L.; Epstein, R.M. The Biopsychosocial Model 25 Years Later: Principles, Practice, and Scientific Inquiry. Ann. Fam. Med. 2004, 2, 576–582. [Google Scholar] [CrossRef]
- Horvat, L.; Horey, D.; Romios, P.; Kis-Rigo, J. Cultural competence education for health professionals. Cochrane Database Syst. Rev. 2014, CD009405. [Google Scholar] [CrossRef]
- Renzaho, A.M.N.; Romios, P.; Crock, C.; Sonderlund, A.L. The effectiveness of cultural competence programs in ethnic minority patient-centered health care--a systematic review of the literature. Int. J. Qual. Health Care 2013, 25, 261–269. [Google Scholar] [CrossRef] [PubMed]
- Hudelson, P.; Dogra, N.; Hendrickx, K.; Verdonk, P.; Essink-Bot, M.-L.; Suurmond, J. The challenges of integrating cultural competence into undergraduate medical curricula across Europe: Experience from the C2ME “Culturally competent in medical education” project. MedEdPublish 2016, 5. [Google Scholar] [CrossRef]
- Sorensen, J.; Jervelund, S.S.; Norredam, M.; Kristiansen, M.; Krasnik, A. Cultural competence in medical education: A questionnaire study of Danish medical teachers’ perceptions of and preparedness to teach cultural competence. Scand. J. Public Health 2017, 45, 153–160. [Google Scholar] [CrossRef] [PubMed]
- White, J.; Plompen, T.; Tao, L.; Micallef, E.; Haines, T. What is needed in culturally competent healthcare systems? A qualitative exploration of culturally diverse patients and professional interpreters in an Australian healthcare setting. BMC Public Health 2019, 19, 1096. [Google Scholar] [CrossRef] [PubMed]
- Flores, G. The Impact of Medical Interpreter Services on the Quality of Health Care: A Systematic Review. Med. Care Res. Rev. 2005, 62, 255–299. [Google Scholar] [CrossRef] [PubMed]
- Brandl, E.J.; Schreiter, S.; Schouler-Ocak, M. Are Trained Medical Interpreters Worth the Cost? A Review of the Current Literature on Cost and Cost-Effectiveness. J. Immigr. Minor. Health 2020, 22, 175–181. [Google Scholar] [CrossRef]
- Himmelstein, J.; Wright, W.S.; Wiederman, M.W. U.S. medical school curricula on working with medical interpreters and/or patients with limited English proficiency. Adv. Med. Educ. Pract. 2018, 9, 729–733. [Google Scholar] [CrossRef] [PubMed]
- Ferrari, R. Writing narrative style literature reviews. Med. Writ. 2015, 24, 230–235. [Google Scholar] [CrossRef]
- Baethge, C.; Goldbeck-Wood, S.; Mertens, S. SANRA—A scale for the quality assessment of narrative review articles. Res. Integr. Peer Rev. 2019, 4, 5. [Google Scholar] [CrossRef]
- Thomas, J.; Harden, A. Methods for the thematic synthesis of qualitative research in systematic reviews. BMC Med. Res. Methodol. 2008, 8, 45. [Google Scholar] [CrossRef]
- Critical Appraisal Skills Programme. CASP (Systematic Review, Qualitative Studies) Checklist. Available at: CASP CHECKLISTS—CASP—Critical Appraisal Skills Programme (casp-uk.net); CASP: Oxford, UK, 2019. [Google Scholar]
- Itaya, L.E.; Glassman, P.; Gregorczyk, S.; Bailit, H.L. Dental School Patients with Limited English Proficiency: The California Experience. J. Dent. Educ. 2009, 73, 1055–1064. [Google Scholar] [CrossRef]
- Simon, L.; Hum, L.; Nalliah, R. Training to care for limited English proficient patients and provision of interpreter services at US dental school clinics. J. Dent. Educ. 2017, 81, 169–177. [Google Scholar] [CrossRef]
- Omoruyi, E.A.; Dunkle, J.; Dendy, C.; McHugh, E.; Barratt, M.S. Cross Talk: Evaluation of a Curriculum to Teach Medical Students How to Use Telephone Interpreter Services. Acad. Pediatr. 2018, 18, 214–219. [Google Scholar] [CrossRef]
- Mazori, A.; Maron, M.; Osterbur, M.; Santos, D.; Marco, V.; Lin, J.; Cortijo, A.; Nosal, S.; Schoenbaum, E. Enhancing Medical Stu-dent-Interpreter Collaboration in an Urban Free Clinic. Fam. Med. 2019, 51, 593–597. [Google Scholar] [CrossRef]
- Kalet, A.; Gany, F.; Senter, L. Working with interpreters: An interactive Web-based learning module. Acad. Med. 2002, 77, 927. [Google Scholar] [CrossRef]
- Kalet, A.L.; Mukherjee, D.; Felix, K.; Steinberg, S.E.; Nachbar, M.; Lee, A.; Changrani, J.; Gany, F. Can a web-based curriculum improve students’ knowledge of, and attitudes about, the interpreted medical interview? J. Gen. Intern. Med. 2005, 20, 929–934. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Lie, D.; Bereknyei, S.; Kalet, A.; Braddock, C., 3rd. Learning outcomes of a web module for teaching interpreter interaction skills to pre-clerkship students. Fam. Med. 2009, 41, 234–235. [Google Scholar] [PubMed]
- Fung, C.-C.; Lagha, R.R.; Henderson, P.; Gomez, A.G. Working with interpreters: How student behavior affects quality of patient interaction when using interpreters. Med. Educ. Online 2010, 15, 5151. [Google Scholar] [CrossRef]
- Lie, D.A.; Bereknyei, S.; Vega, C.P. Longitudinal development of medical students’ communication skills in interpreted en-counters. Educ. Health 2010, 23, 466. [Google Scholar]
- Avalos, O.H.; Pennington, K.; Osterberg, L. Revolutionizing Volunteer Interpreter Services: An Evaluation of an Innovative Medical Interpreter Education Program. J. Gen. Intern. Med. 2013, 28, 1589–1595. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bansal, A.; Swann, J.; Smithson, W. Using professional interpreters in undergraduate medical consultation skills teaching. Adv. Med. Educ. Pract. 2014, 5, 439–450. [Google Scholar] [CrossRef]
- Quick, K.K.; Selameab, T.; Woll, A.; Mazzei, C.; Miller, J.L. Creating and Evaluating Skills-Based Training in Working with Spoken-Language Interpreters for Oral Health Professions Students. J. Dent. Educ. 2019, 83, 645–653. [Google Scholar] [CrossRef] [PubMed]
- McEvoy, M.; Santos, M.T.; Marzan, M.; Green, E.H.; Milan, F.B. Teaching medical students how to use interpreters: A three year experience. Med. Educ. Online 2009, 14, 4507. [Google Scholar] [CrossRef]
- Ikram, U.Z.; Essink-Bot, M.-L.; Suurmond, J. How we developed an effective e-learning module for medical students on using professional interpreters. Med. Teach. 2014, 37, 422–427. [Google Scholar] [CrossRef]
- Marion, G.S.; Hildebrandt, C.A.; Davis, S.W.; Marín, A.J.; Crandall, S.J. Working effectively with interpreters: A model curriculum for physician assistant students. Med. Teach. 2008, 30, 612–617. [Google Scholar] [CrossRef] [PubMed]
- Jacobs, E.A.; Diamond, L.C.; Stevak, L. The importance of teaching clinicians when and how to work with interpreters. Patient Educ. Couns. 2010, 78, 149–153. [Google Scholar] [CrossRef] [PubMed]
- Aitken, G. Medical Students as Certified Interpreters. AMA J. Ethics 2019, 21, 232–238. [Google Scholar]
- Mihalic, A.P.; Morrow, J.B.; Long, R.B.; Dobbie, A.E. A validated cultural competence curriculum for US pediatric clerkships. Patient Educ. Couns. 2010, 79, 77–82. [Google Scholar] [CrossRef]
- Pelaez, A.F.V.; Ramirez, S.I.; Sanchez, C.V.; Abusharar, S.P.; Romeu, J.C.; Carmichael, C.; Bascoy, S.; Baron, R.; Pichardo-Lowden, A.; Albarracin, N.; et al. Implementing a medical student interpreter training program as a strategy to developing humanism. BMC Med. Educ. 2018, 18, 141. [Google Scholar]
| Inclusion | Peer-reviewed articles or chapters Theses and dissertations Literature reviews Conference papers Editorials Books or textbooks All of the above, which include or discuss medical students, medical or health care curricula Published in English Period of publication: 2000–2020 |
| Exclusion | Peer review articles, chapters, thesis dissertations, conference papers, editorials, books and textbooks which do not include or discuss medical students, medical or health care curricula Any of the above publications published before 2000 Published in languages other than English |
| Utilization | Are interpreters used in medical education as part of the curriculum? If yes how, where, and when are they used? What is the effect of the use of interpreters on the quality of medical education? How confident are medical students in using interpreters in medical education? |
| Perspectives | What are the patients’ perspectives when they see medical students and interpreters? What are the students’ feelings when being in clinical placements where they do not speak the language of their patients? What are the perspectives of students, interpreters, health care providers (e.g., clinics, hospitals, health care facilities, etc.), and medical educators? |
| Impact | Is there any research done looking at patient outcomes when medical students use interpreters in their clinical placements? What are students learning from the use of interpreters during their medical education? What is the impact of using interpreters in clinical placements/medical education on patients? |
| Barriers/Enablers | What are the facilitators and challenges for using interpreters in medical education for medical students, their supervisors, and the patients? |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Constantinou, C.S.; Ng, A.T.; Becker, C.B.; Zadeh, P.E.; Papageorgiou, A. The Use of Interpreters in Medical Education: A Narrative Literature Review. Societies 2021, 11, 70. https://doi.org/10.3390/soc11030070
Constantinou CS, Ng AT, Becker CB, Zadeh PE, Papageorgiou A. The Use of Interpreters in Medical Education: A Narrative Literature Review. Societies. 2021; 11(3):70. https://doi.org/10.3390/soc11030070
Chicago/Turabian StyleConstantinou, Costas S., Andrew Timothy Ng, Chase Beverley Becker, Parmida Enayati Zadeh, and Alexia Papageorgiou. 2021. "The Use of Interpreters in Medical Education: A Narrative Literature Review" Societies 11, no. 3: 70. https://doi.org/10.3390/soc11030070
APA StyleConstantinou, C. S., Ng, A. T., Becker, C. B., Zadeh, P. E., & Papageorgiou, A. (2021). The Use of Interpreters in Medical Education: A Narrative Literature Review. Societies, 11(3), 70. https://doi.org/10.3390/soc11030070









