Abstract
Hepatocellular carcinoma (HCC) is a common complication of chronic liver diseases and remains a relevant cause of cancer-related mortality worldwide. The global prevalence of metabolic dysfunction-associated steatotic liver disease (MASLD) as a risk factor for hepatocarcinogenesis is on the rise. Early detection of HCC has been crucial in improving the survival outcomes of patients with metabolic dysfunction-associated steatohepatitis (MASH), even in the absence of cirrhosis. Understanding how hepatocarcinogenesis develops in MASH is increasingly becoming a current research focus. Additive risk factors such as type 2 diabetes mellitus (T2DM), genetic polymorphisms, and intestinal microbiota may have specific impacts. Pathophysiological and epidemiological associations between MASH and HCC will be discussed in this review. We will additionally review the available tumor therapies concerning their efficacy in MASH-associated HCC treatment.
1. Introduction
Hepatocellular carcinoma (HCC) is one of the leading causes of cancer-related deaths worldwide [1]. Hepatocarcinogenesis is predisposed by liver cirrhosis of any etiology. However, chronic viral hepatitis B and metabolic dysfunction-associated steatohepatitis (MASH), formerly known as non-alcoholic steatohepatitis (NASH) [2], already significantly increase the risk of developing HCC, even in the absence of cirrhosis [3,4,5].
The increasing prevalence of metabolic dysfunction-associated steatotic liver disease (MASLD), previously known as non-alcoholic fatty liver disease (NAFLD) [2], and its progression to MASH raise the incidence of progressive liver fibrosis, cirrhosis, and HCC. Current data support the notion that MASH is the leading cause of the predicted increase in HCC incidence in the next decades [6].
Causal therapeutic approaches to HCC-predisposing MASH are taking place in the context of clinical trials, which is why weight normalization, exercise, and optimization of concomitant diseases such as diabetes mellitus are still the current focus. Understanding how hepatocarcinogenesis develops in MASH is increasingly becoming a key research focus. Here, the roles of additive risks such as type 2 diabetes mellitus (T2DM), genetic polymorphisms, and the intestinal microbiome are of particular interest.
The importance of HCC surveillance in the MASH population is controversial. On the one hand, there is a lack of international consensus regarding the risk population to be defined. On the other hand, it has not been clarified whether standard screening methods using sonography in patients with MASH have sufficient sensitivity in early HCC detection [7,8].
In recent years, there has finally been a breakthrough in the systemic therapy of HCC, so several therapeutic options are now available in addition to current locoregional procedures. Since MASH is associated with a multitude of comorbidities, it remains challenging to extract the individual impact of MASH on the efficacy of available treatment options. This is particularly important when comparing MASH-related HCC with the HCC of other etiologies.
2. Epidemiology of HCC in MASH
Primary liver carcinomas represent the sixth most common cancer worldwide and the third leading cause of cancer-related death [1]. Approximately 75–90% of these tumors are classified as primary HCC, and only 10–15% of cases are classified as cholangiocarcinoma (CCA) [9]. The annual HCC incidence is almost identical to its annual mortality, illustrating the high mortality of this disease [10,11].
In the Western world, chronic viral hepatitis C is currently shown to be responsible for the majority of all new HCC cases. However, a gradual decline is expected in the coming years due to the success of direct antiviral therapies (DAAs) [12]. Alcohol-induced liver disease also accounts for 10–20% of relevant HCC predisposing factors, and chronic viral hepatitis B accounts for 10–15% of cases. In older epidemiological analyses, a large proportion of patients with MASH were not recorded separately and were, thus, incorrectly assigned to the cohort of “cryptogenic” cirrhosis. This can partly explain divergent data on the frequency of cryptogenic liver disease (15–50%) as an HCC risk factor [13].
According to the most recent epidemiological studies, hepatic steatosis is the leading cause of the increasing incidence of HCC in Western industrialized nations. An analysis of the US Liver Transplant Registry between 2002 and 2017 found that the prevalence of patients with MASLD awaiting liver transplantation increased by 16% over the past 15 years, from 6% in 2002 to 22% in 2017, with MASH emerging as the fastest growing cause. The proportion of MASH as a cause of HCC increased 8.5-fold during the study period, from 2% in 2002 to 18% in 2017 [14]. It should be noted here that a high number of HCC cases arise against a background of MASH in the absence of cirrhosis [3]. This population has not been subject to international consensus screening for early HCC detection.
Another analysis of patients transplanted for end-stage liver disease between January 2002 and December 2016 using the European Liver Transplant Registry database showed a greater proportion of patients transplanted for MASH-associated HCC (39.1%) than non-MASH patients (28.9%, p < 0.001) [15].
A US cohort study of over 500,000 participants, published in 2018, showed a cumulative 5- (or 10)-year HCC risk of 0.8 (or 1.7) per 1000 patients in the MASLD cohort. Compared with healthy controls, patients with MASLD had an 8.6-fold increase in HCC risk. Patients with MASLD-associated cirrhosis showed a further marked increase in HCC risk, with an annual incidence of 0.8–2.3% per year. Approximately 20% of all hepatic steatosis-associated HCC cases occurred without predisposing cirrhosis [11].
A large German monocentric study with 1119 HCC patients, in 2015, demonstrated epidemiological differences between patients with MASH-related HCC and those with other HCC-predisposing liver diseases. For instance, patients with MASH-related HCC were older at initial diagnosis than others (68 vs. 65 years). The MASH-HCC cohort showed a higher prevalence of obesity (31.1% vs. 14.7%) and T2DM (66.7% vs. 37.85%), with higher body mass index (BMI) correlating with worse overall survival. In MASH patients, there was a trend toward multifocality (80% vs. 70%) with larger lesions overall (6.0 cm vs. 4.8 cm). In addition, there was a tendency toward an increased extrahepatic metastasis rate at the initial diagnosis. Interestingly, liver function was preserved to a greater extent than in other etiologies of HCC patients. Therefore, it can be postulated that the potential diagnosis of MASH-associated cirrhosis and its complications occurred later. As a result, HCC could only be detected at more advanced stages [16]. Consequently, optimization of current HCC screening algorithms and a more precise definition of the population to be screened seem all the more urgent.
Projections using dynamic Markov modeling for accounting for obesity and diabetes trends claim that the annual incidence of MASLD-related HCC in the USA would increase by 137% from 5160 cases in 2015 to 12,240 cases in 2030 [17].
3. Pathogenesis of HCC in MASH
Chronic hepatic inflammation in the setting of MASH represents a potential trigger of hepatocarcinogenesis even in the absence of predisposing cirrhosis. It is a complex, multifactorial process involving various risk factors (genomic instability, obesity, diabetes mellitus, and others) (Figure 1). Metabolic alterations (lipid and glucose metabolism) contribute to hepatic steatosis. However, additional factors such as genetic variants, oxidative/endoplasmic reticulum stress, mitochondrial dysfunction, altered immune response, and microbiome conditions fuel disease progression (hepatic inflammation, fibrogenesis, and carcinogenesis) [18]. For conciseness, we focus on the influence of genetics and polymorphisms. In addition, the microbiome’s impact on the progression from MASH to HCC will be considered separately.
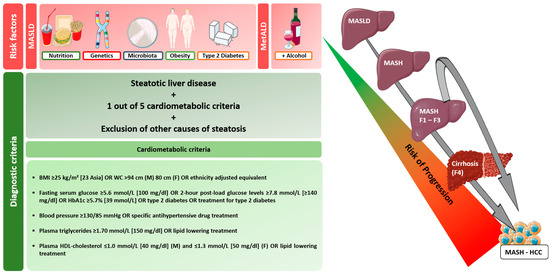
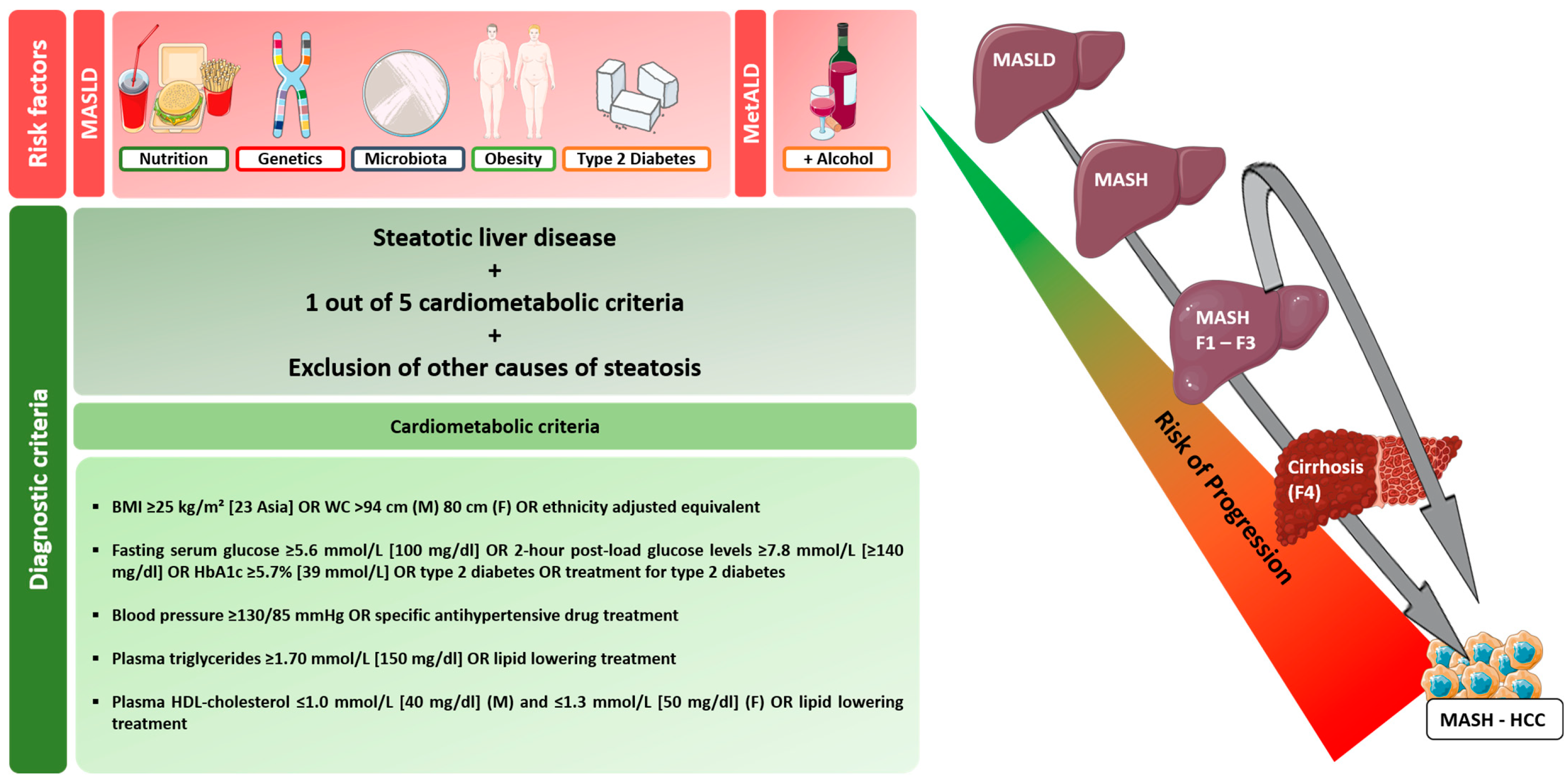
Figure 1.
Diagnostic criteria and risk factors for MASLD and progression of MASLD to MASH-HCC [19]. In the progression from MASLD to MASH, MASH fibrosis, and finally cirrhosis, a variety of factors (type 2 diabetes mellitus, obesity, microbiome, genetic and epigenetic factors, lifestyle) have a similar effect on hepatocarcinogenesis. HCC risk appears to correlate with the extent of fibrosis, but MASH-associated HCC may develop even without cirrhosis. The time to which the above factors, particularly type 2 diabetes, have direct carcinogenic potential has not been conclusively determined. Abbreviations: MetALD: metabolic dysfunction and alcohol-associated steatotic liver disease, BMI: body mass index; WC: waist circumference.
3.1. Genetic Factors
Several gene polymorphisms have demonstrated an association between the prevalence of MASLD per se and the risk of progression to advanced MASH fibrosis [20]. The best known is the polymorphism of the PNPLA3 (patatin-like phospholipase domain containing 3) gene (variant rs738409 c.444 C>G, p.I148M) on chromosome 22. This PNPLA3 variant leads to impaired triglyceride mobilization of hepatic lipid droplets with increased hepatic lipid accumulation, but also the alteration of retinol storage in the liver, and altered retinol serum levels, especially in obese patients. Of note, the PNPLA3 polymorphism is associated with a 3-fold increased risk of HCC in its carriers, independent of other risk factors such as BMI, diabetes, and advanced fibrosis [21].
The TM6SF2 (transmembrane 6 superfamily member 2) gene polymorphism (variant rs58542926, c.449 C>T, p.E167K) on chromosome 19 manifests as a transport disorder of pre-VLDL particles. It correlates with the extent of steatosis and progression of fibrosis in MASH, independent of obesity, diabetes, and the PNPLA3 genotype. However, the direct role of this TM6SF2 variant in hepatocarcinogenesis is controversial; the profibrogenic effect might indirectly promote progression to HCC [22,23].
Recent data also suggest that a loss-of-function variant in the 17-beta hydroxysteroid dehydrogenase 13 gene (HSD17B13) is associated with a reduced risk of chronic liver disease and of progression from steatosis to steatohepatitis and, thus, may represent another factor in HCC development [24,25,26].
In addition, individual studies of different mutations have demonstrated an unfavorable influence on the course of MASH. Mutations of the hereditary hemochromatosis protein-encoding gene (HFE) on chromosome 6 are associated with a complicated course of MASH, potentially favoring the development of HCC [27].
In conclusion, it is important to note that both hepatocarcinogenic single mutations and the increased genetic instability in patients with MASH, compared to those with MASLD, favor the development of HCC. Other mechanisms promoting the progression of MASH to HCC include epigenetic alterations causing aberrant DNA methylation and the expression of diverse microRNAs (miR-21, miR-23, miR-29, miR-93, miR-106, miR-155, miR-221, miR-222, and miR-519). Mechanisms and pathways involved are the major tumor-associated signaling cascades (transforming growth factor (TGF-), Wingless and INT-1 (Wnt)/catenin, mitogen-activated protein kinase (MAPK), Hedgehog, NF-κB, phosphatidylinositol 3-kinase (PI3K)/AKT/Mechanical (mammalian) target of rapamycin (mTOR)) [28], and CD44 [29].
3.2. Intestinal Microbiome
The gut microbiome is considered a key modulator of metabolism. It not only facilitates the extraction of nutrients and energy from food but is also essential for producing numerous metabolites, including bile acids, regulating various metabolic pathways. The gut microbiome outnumbers the human genome many times over. It plays a vital role in metabolism, immune system formation, health maintenance, tolerance development, and the prevention of colonization by pathogens. Its alteration, called dysbiosis, has been described for different intestinal metabolic and inflammatory diseases, including MASLD/MASH, alcoholic liver disease, cirrhosis, and complications [30,31,32,33].
Shifts of specific bacterial strains affect the production of bacterial-derived metabolic active components, including bile acids, ethanol, cytokines, short-chain fatty acids, or other inflammatory metabolites. Those may affect the host and possibly promote cancer-related risk factors or diseases [34]. In rodent studies, fecal microbiota transplantation increased the abundance of beneficial bacterial groups and alleviated the progression of MASH development [35].
Modulating the gut microbiota, e.g., with antibiotic treatment, may reduce the risk of hepatic carcinogenesis [36,37]. After antibiotic treatment, mice fed a high-fat diet showed reduced toxic secondary bile acids [38]. In MASLD and especially MASH, nutrition, metabolic disturbances, and related comorbidities such as diabetes may influence gut microbiota composition. Changes in the abundances of different bacterial groups have been described within other patient groups. The metabolism of specific bacterial groups affects the mucosal barrier, hepatic inflammation, fibrogenesis, and tumorigenesis [39]. The gut microbiota impacts energy balance, altering the uptake of calories derived from food and alcohol [40]. Emerging data indicate that specific characteristic changes in the gut microbiome are associated with MASLD and even cirrhosis, which is the primary driver of HCC development [31,41,42]. In MASLD-related HCC and viral hepatitis-related HCC (hepatitis B), specific modification of gut microbiota may represent a potential therapeutic option for HCC treatment [43]. A study comparing MASH and MASH-HCC patients with or without cirrhosis showed that changes in bacterial groups regulating bile acid metabolism affected hepatic fibrogenesis and liver injury. The changes in the bile acid pool were associated with an increased abundance of several bacterial strains, particularly Lactobacilli and Bacteroides, which were related to altered liver injury and liver stiffness [44]. In patients with MASH, the abundance of bile salt hydrolase-expressing bacteria is shifted, resulting in increased bile acid levels and the altered composition of the bile acid pool, which tends to increase the amount of secondary conjugated bile acids [45]. Alterations in bile acid composition may be associated with advanced fibrosis in MASH-HCC, suggesting an essential role in fibrosis-related tumorigenesis [46,47].
4. HCC Surveillance in MASLD/MASH
It is well established that patients participating in surveillance programs are diagnosed with HCC at less advanced stages, resulting in a survival advantage. Successful screening, however, requires reliable screening methods, on the one hand, and a definition of the population at risk, on the other hand.
In the context of a steady worldwide increase in HCC incidence on the background of MASH, there is a compelling need for a clear recommendation regarding HCC surveillance for this patient population. While the risk of HCC in MASH cirrhosis is sufficiently high to warrant surveillance, there is still no clear consensus among international guidelines for patients with MASH without cirrhosis. The German HCC S3 guideline provides sonographic screening with or without additional AFP determination every six months in MASH patients, even in non-cirrhotic livers. The current AASLD (American Association for the Study of Liver Diseases) HCC guidelines do not recommend surveillance in MASLD alone; only in MASH cirrhosis should sonography (±AFP determination) be offered every six months [48]. The 2018 EASL (European Association for the Study of the Liver) HCC guidelines also do not recommend general HCC surveillance in MASH; however, surveillance may be considered across etiologies in patients with advanced fibrosis (F3) without cirrhosis based on the individual risk profile. The EASL guidelines only recommend sonographic controls every six months without additional determination of AFP (European Association for the Study of the Liver).
As early as 2011, Ertle et al., in a retrospective epidemiological HCC monocenter study, described that 42% of patients in the MASLD/MASH-HCC group did not have cirrhosis at the time of HCC diagnosis [3]. Later publications showed a slightly lower proportion of non-cirrhotic MASH-HCC patients ranging from 23% to 37% [49,50].
The sensitivity of ultrasound-based surveillance in MASH patients is limited by investigator dependence, frequent concomitant obesity, and by MASH itself. A recent US meta-analysis examined the sensitivity of sonography in HCC detection, with or without concurrent AFP determination, in a cohort of 13,367 high-risk HCC patients of any etiology. Ultrasound alone showed a sensitivity of only 45%, which significantly increased to 63% with the addition of AFP. Thus, whether sonography alone can reduce HCC-associated mortality remains inconclusive and urgently requires data from prospective studies [51].
To address the unsatisfactory performance of sonography-based HCC surveillance, the GALAD score was developed, which includes age, sex, and the biomarkers AFP, AFP isoform L3 (AFP-L3), and Des-γ-Carboxy-Prothrombin (DCP), also known as protein induced by vitamin K absence or antagonist-II (PIVKA-II). In a recent Japanese–German multicenter study, it was shown in MASH patient collectives that the GALAD score can detect HCC with high sensitivity while comprising reasonable specificity in these patients in the presence and absence of cirrhosis. Even early-stage HCC could be detected with high reliability [52]. However, a limitation of this multicenter study is the lack of a direct comparison with an ultrasound-based surveillance strategy in the populations studied. A future prospective study should, therefore, investigate the performance of ultrasound alone and in combination with the GALAD score in NASH patients. A retrospective American multicenter study shows that this approach may be promising, with the combination of GALAD and ultrasound achieving an AUC of 0.98 (US alone AUC 0.82 vs. GALAD alone AUC 0.95) [53].
Recent data show that hepatocarcinogenesis is accompanied by epigenetic changes and mutations in various genes. These molecular changes, which have so far been described using tissue biopsies and cell models, can also be detected in circulating fragmented DNA (cfDNA) in the blood. As with other tumor entities, the molecular cfDNA can be used to analyze the molecular changes [54]. In this context, it would be all the more obvious to establish the use of liquid biopsy (LB) in HCC on a larger scale in order to be able to do justice to the still insufficient early diagnosis. The use of LB appears to be particularly useful in HCC, as the arterial hyperperfusion of tumor tissue means that there is a particularly high probability of circulating tumor cells (CTCs) and cfDNA being distributed in the peripheral blood.
5. Therapeutical Challenges in Patients with MASH-Related HCC
In unifocal HCC (Barcelona Clinic Liver Cancer (BCLC) stage 0/A), therapy of smaller lesions with curative intent is possible by radiofrequency ablation (RFA) or microwave ablation (MWA). For larger lesions, liver resection is indicated, assuming there is preserved liver synthesis function in the absence of portal hypertension. A large US monocenter study demonstrated that patients with HCC and MASH had better liver function at the time of resection and showed a lower rate of cirrhosis than patients with hepatitis C or alcohol-related liver disease. As a result, a more significant proportion of patients could be resected in MASH-associated HCC compared with the other etiologies. In addition, improved overall survival (OS) has been detected compared with the HCV/alcohol cohort [55].
For functionally irresectable HCC with a single lesion <5 cm or a maximum of 3 lesions <3 cm (Milan criteria), evaluation for liver transplantation (LT) is recommended. It should be emphasized at this point that, as mentioned at the outset, MASH is primarily responsible for the sharp increase in HCC-related transplant listings in the United States.
The resulting increase in demand for donor organs requires more optimized allocation of organs. However, current data suggest that the Milan criteria, which are still considered the standard, could deny many potential organ recipients suffering from MASLD-associated HCC from receiving a donor organ due to the more advanced tumor stages at initial diagnosis. In recent years, several different approaches have been taken to extend these current criteria. Among the best known are the UCSF criteria, defined as a single tumor that is less than or equal to 6.5 cm, or up to 3 lesions with the largest lesion less than or equal to 4.5 cm, with a total tumor diameter no greater than 8 cm. Here, patients transplanted within these criteria had a 5-year survival rate of 75.2% [56]. In contrast, the Up-to-Seven criteria propose that for HCC, with 7 as the total of the size of the largest lesion in cm and the number of lesions, and without vascular invasion, could have survival outcomes as good as those within the Milan criteria. In the patient cohort without microvascular invasion but within the Up-to-Seven criteria, 5-year overall survival was 71.2% [57]. Later, Mazzaferro et al. developed the Metroticket 2.0 model, incorporating the size of the largest HCC lesion, the total number of nodules, and the AFP level in 2018. According to this model, the overall 5-year survival rate reached 79.7%, and tumor recurrence could be more accurately estimated than with the Milan, UCSF, or Up-to-7 criteria [58].
The additional use of biomarkers in decision algorithms for LT is a matter of debate. However, there is a correlation between microvascular invasion (MVI) [59], histological differentiation, and the risk of post-LT HCC recurrence, as reported in several publications. AFP and DCP levels are reliable surrogate markers of the biological behavior of HCC due to their strong correlation with MVI and degree of differentiation [60] and micro-intrahepatic metastasis. The inclusion of these markers in the development of criteria has become widely accepted in the last decade.
Even at the listing stage, MASH presents unique features compared to other etiologies. It is well known that metabolic syndrome (especially T2DM and obesity), related coronary artery disease, and chronic renal failure are predictors of worse postoperative and long-term outcomes. On the LT waiting list, patients with MASH frequently exhibit numerous metabolically related risk factors simultaneously. This results in several potential pitfalls for LT-listed patients with MASH: an overall older patient age at the time of listing for liver transplantation, comorbidities, and a lower model for end-stage liver disease (MELD) score than other etiologies. In the context of obesity and transplantation, the results of different meta-analyses are wildly divergent. Some studies report worse post-LT survival in patients with high BMI, whereas other papers report similar long-term outcomes as in normal-weight patients. The postoperative complication rate is higher in obese patients. Whether combining bariatric surgery with LT may improve overall survival needs to be investigated using more extensive randomized trials. However, T2DM should be emphasized as a predictor of poor graft and long-term patient survival. In the future, the integrated weighting of MASH-associated comorbidities in selecting MASH-HCC patients for potential LT listing will be a significant challenge [61].
5.1. Treatment of Intermediate-Stage HCC
For patients presenting non-diffuse, multifocal tumor nodules without extrahepatic tumor manifestations or macrovascular invasion and compensated liver function (BCLC stage B), a transarterial chemoembolization (TACE) treatment is recommended, according to the EASL guidelines [62]. A survival benefit from TACE was first demonstrated in 2002 in a randomized controlled trial comparing TACE to symptomatic treatment [63]. Since then, the technique has undergone several improvements, e.g., super-selective chemoembolization of the target volume can facilitate optimal sparing of healthy liver tissue surrounding the tumor and, thus, help preserve liver function. As a different concept for locoregional therapy, transarterial radioembolization (TARE) is an alternative treatment option for patients with locally advanced HCC who are not eligible for TACE [62]. To the best of our knowledge, little evidence exists regarding MASLD’s influence on the efficacy and safety of locoregional therapies.
In a retrospective study comparing the outcome of TACE in cirrhotic patients with MASH-related HCC to patients with HCV- or alcohol-related HCC, no significant differences in OS, response rate, or time to progression (TTP) could be identified. Apart from adverse events, no significant differences between the groups were also observable [64]. Concerning MASLD-related comorbidities, another retrospective study could identify obesity (BMI ≥ 25 kg/m2) as a risk factor for worse tumor response after TACE [65]. Furthermore, T2DM could be identified as an independent predictor for worse OS in patients with non-viral HCC undergoing TACE [66]. The negative influence of T2DM could be demonstrated in a further retrospective study. Patients suffering from liver cirrhosis and concomitant T2DM had a worse long-term prognosis after TACE [67]. Interestingly, the drug Metformin, frequently prescribed for T2DM, seems to have beneficial effects on the outcomes after TACE in patients with T2DM and early-stage HCC [68]. Regarding TARE, a retrospective study conducted by Schotten and colleagues found MASLD-related comorbidities not to influence the critical outcomes of TARE [69].
5.2. The Treatment Landscape for Advanced-Stage HCC
Over the past few years, the landscape of systemic therapy options for patients with advanced-stage HCC and compensated liver function has significantly expanded. In 2008, for the first time, two independently conducted studies (SHARP trial and Asia-Pacific trial) demonstrated a survival benefit for HCC patients treated with systemic therapy, leading to the approval of the tyrosine kinase inhibitor (TKI) sorafenib [70,71]. Based on the results of the REFLECT trial, lenvatinib was approved in 2018 as a further first-line treatment option. Although lenvatinib did not achieve superior OS (OS lenvatinib: 13.6 months vs. OS sorafenib: 12.3 months, hazard ratio (HR) 0.92, 95% confidence interval (CI) 0.79–1.06), progression-free survival (PFS), time to progression (TTP), as well as the objective response rate (ORR) significantly improved in the lenvatinib group compared to sorafenib [72]. Further, two more TKIs, regorafenib and cabozantinib, have been approved as second (or third) line therapies after pretreatment with sorafenib [73,74]. With the introduction of ramucirumab, therapy options in second-line treatment further expanded to include a monoclonal antibody directed against vascular endothelial growth factor receptor type 2 (VEGFR2). Ramucirumab, the only drug that has to be guided by a biomarker, has been approved for patients with tumor progression on sorafenib and an alpha fetoprotein (AFP) value of at least 400 ng/mL [75]. Developing the aforementioned new TKIs and monoclonal antibodies has significantly improved the OS of HCC patients eligible for systemic therapy. However, the improved OS is not consistently matched by an improved ORR. Furthermore, in HCC patients with MASH, TKI treatment approaches are potentially limited by extrahepatic manifestations of the metabolic syndrome such as obesity, diabetes, hyperlipidemia, and arterial hypertension, frequently accompanied by chronic kidney and cardiovascular disease. Here, TKIs may aggravate arterial hypertension and increase the risk of myocardial infarction, potentially necessitating treatment de-escalation or discontinuation. Therefore, in this patient cohort, alternative treatment approaches with more favorable safety profiles are required.
Regarding the critical endpoint of ORR, a clear improvement was achieved with the combination of the programmed death-ligand 1 (PD-L1) inhibitor atezolizumab and the VEGF inhibitor bevacizumab tested against sorafenib as first-line therapy (IMbrave 150 trial) [76]. In addition to a survival benefit of nearly six months (OS atezolizumab plus bevacizumab: 19.2 months vs. OS sorafenib 13.4 months), this new combination therapy induced an ORR in 30% of all participants, and 25 patients (8%) even showed a complete response. As a result, the combination of atezolizumab and bevacizumab became the new standard of care for first-line systemic treatment in 2020. Supported by the results of the above-mentioned IMbrave150 study, an immune checkpoint inhibitor (ICI)-based combination therapy is seen as having great potential in treating liver cancer. Based on the positive results of the phase III HIMALAYA trial, the dual immune checkpoint blockade consisting of the cytotoxic T-lymphocyte-associated Protein 4 (CTLA-4) antibody tremelimumab and the PD-1 inhibitor durvalumab was recently approved as an additional first-line therapy [77]. The so-called STRIDE regimen (single tremelimumab regular interval durvalumab) showed both an OS benefit (OS STRIDE 16.4 months vs. OS sorafenib 13.8 months, HR 0.78, 96% CI 0.65–0.92, p = 0.0035) and an improved treatment response rate (ORR STRIDE 20.1% vs. sorafenib 5.1%). In addition to combination therapy, durvalumab was also tested as a monotherapy and was found to be non-inferior to sorafenib [77].
Apart from the dual ICI blockade, the combination of an ICI with TKIs has also been tested. Recently, the results of LEAP-002, a phase III study evaluating the combination of pembrolizumab plus lenvatinib versus lenvatinib as monotherapy, were reported. Although the combination therapy did not reach the pre-specified statistical significance for OS, it achieved the longest OS among systemic treatments for advanced HCC to date (OS lenvatinib plus pembrolizumab: 21.2 months vs. OS lenvatinib: 19 months, HR 0.84, 95% CI 0.708–0.997, p = 0.0227) [78]. The combination of atezolizumab and cabozantinib investigated in the COSMIC 312 trial only improved PFS, but not OS [79]. In addition to their use in the first-line setting, ICIs have also been investigated in the second-line setting. For example, the CheckMate 040 phase I/II trial found that the combination of ipilimumab and nivolumab induced a durable response in a subset of patients with HCC who had previously received sorafenib treatment [34].
5.3. Immunotherapy and Targeted Therapies in Non-Viral HCC
Regarding the expanding therapeutic armamentarium, a new challenge arises—namely, to identify the most suitable treatment sequence for each patient as systemic treatment has been conducted in a “one-size-fits-all” fashion for many years. To what extent the etiology of the underlying chronic liver disease contributes to therapy success or failure is currently gaining increased attention. In light of the rapidly increasing incidence, patients with MASLD-associated HCC are of particular interest. A closer look into the patient cohorts of the above-mentioned phase III trials reveals that only small subgroups had non-viral HCC. Furthermore, only a few studies reported a precise number of MASLD-related etiology (Table 1) [70,71,72,73,74,75,76,80]. Interestingly, to our knowledge, only the CELESTIAL trial considered MASLD as a stratification parameter. The current knowledge regarding therapy implications for non-viral HCC is primarily based on findings from retrospective cohorts, potentially biased subgroup analyses, and meta-analyses, but no specific RCTs have been conducted assessing this issue.

Table 1.
Role of HCC etiologies in selected clinical trials on systemic therapy with subsequent approval of the therapy regimen by the EMA.
It was hypothesized that patients with non-viral HCC may benefit less from ICI-based immunotherapy. Subgroup analyses of the IMbrave150 trial indicate a clear survival benefit for viral HCC, but the HR for non-viral HCC was not statistically significant (HR 1.05, 95% CI 0.68–1.63) [76]. These findings are further supported by two meta-analyses that merged data from the three large ICI phase III trials (IMbrave 150, Checkmate 459, and Keynote 240). The analyses showed that ICI-based therapies seemed to be less effective in patients with non-viral HCC [81,82]. The possible underlying mechanisms of resistance against immunotherapy in MASLD-associated HCC are not fully understood. It seems that CD8 + PD1 + -T-cells contribute to the pathophysiology of MASLD, and interestingly, anti-PD1 therapy promotes adverse tumor necrosis factor-alpha (TNFα)-secretion by these cells in the MASLD setting [81]. However, in contrast to the aforementioned studies, newer trials reported more promising results, questioning the assumption that ICI-based therapy is not the optimal choice for patients with non-viral HCC. The recently published HIMALAYA trial demonstrated a significant survival benefit for patients with non-viral HCC receiving the STRIDE regime (HR 0.74, 95% CI 0.57–0.95) [77]. Another meta-analysis did not demonstrate a notable difference in treatment efficacy associated with the underlying HCC etiology [83].
Regarding TKI-based therapy, the role of the etiology of the underlying chronic liver disease is also not fully understood. A recent meta-analysis as well as a real-world study, which included patients treated with lenvatinib from German tertiary cancer centers, did not identify any differences in HCC treatment success according to the etiology of chronic liver disease [82,84]. In the SHARP trial, the survival benefit of sorafenib over the placebo was consistent for the different etiologies HBV, HCV, and alcohol. However, the effect seemed more pronounced in patients suffering from HCC due to HCV infection [85]. In a multicentric retrospective study conducted in a Japanese cohort investigating the impact of lenvatinib in accordance with the HCC etiology (MASLD/MASH group vs. Viral/Alcohol group), OS and PFS tended to be even better in the MASLD/MASH group [86]. Another retrospective study featuring a European cohort of HCC patients receiving lenvatinib treatment, conducted by Sacco and colleagues, also found that patients with non-viral HCC had longer OS compared to patients with viral-related HCC [87]. In further retrospective studies, two other working groups investigated the effect of lenvatinib compared to the combination therapy of atezolizumab and bevacizumab in patients with non-viral HCC and were able to identify a favorable effect for lenvatinib in this patient group [88,89]. In summary, etiology cannot currently serve as a selection criterion for the preferred therapy due to insufficient high-quality data from prospective studies using MASLD as a stratification criterion or even considering MASLD as a distinct subgroup. It is important to note that MASLD has also not been considered as a separate patient group in phase III studies to date and it can also be challenging to identify MASH as the sole risk factor for the development of HCC. Therefore, the combination of atezolizumab and bevacizumab remains the recommended first-line therapy for all patients.
6. Future Directions
The relationship between obesity and type II diabetes mellitus in the progression of MASLD to fibrosis, cirrhosis, and HCC is well-established. Adipokines and insulin resistance are among the factors that orchestrate this progression. By effectively treating the additive risk factors of obesity and diabetes, the risk of progression to HCC can be mitigated.
Drug therapy for morbid obesity remains a clinical challenge, which is why bariatric surgery continues to play an important role here. According to a recent large meta-analysis by Ramai and colleagues (9 studies, 18,423,546 controls vs. 1,091,204 bariatric patients), surgical treatment of obesity can significantly reduce the risk of concomitant progression from MASLD to HCC. The pooled rate per 1000 person-years was 0.05 (95% CI: 0.02–0.07) in bariatric surgery patients versus 0.34 (95% CI: 0.20–0.49) in the control group with an incidence rate ratio of 0.28 (95% CI: 0.18–0.42). Bariatric weight reduction reduces the risk of HCC in obese patients, as indicated by the data [90].
The efficacy of glucagon-like peptide-1 (GLP-1) receptor agonists such as liraglutide in the treatment of MASLD/MASH remains unclear. In an animal study, mice with streptozotocin- and high-fat diet-induced diabetes with MASH were treated with liraglutide or saline for 14 days in the control arm. The two groups were compared in terms of glycemic control: liver histology and hepato-carcinogenesis. While fasting plasma glucose was significantly lower in the liraglutide group than in the control group, fasting insulin levels were significantly higher in the test group than in the control group. Impressively, in contrast to the control group, liraglutide completely suppressed the development of HCC and also significantly attenuated steatosis and inflammation [91].
Another treatment option for the effective management of T2DM, one of the major risk factors for MASLD, is sodium-glucose co-transporter (SGLT2) inhibitors. Experimental studies in animal models have suggested that SGLT2 inhibitors may have beneficial modulatory effects on MASLD, and several studies in patients have demonstrated their beneficial effects on liver enzymes, BMI, hyperlipidemia, hyperglycemia, and insulin resistance in MASLD patients, potentially inhibiting the progression of liver damage to HCC in these patients [92]. In the future, effective control of predisposing factors for HCC will undoubtedly be an essential preventive component in reducing the increasing incidence of HCC worldwide.
7. Conclusions
MASH is considered to be a significant cause of the increasing incidence of HCC worldwide. Chronic hepatic inflammation in MASH triggers hepatocarcinogenesis even without predisposing cirrhosis. It is a complex, multifactorial process involving various risk factors (genomic instability, obesity, diabetes mellitus, etc.). The heterogeneity of HCCs resulting from this multitude of MASH-associated risks makes it difficult to define a risk population to be screened clearly. In consequence, MASLD is associated with lower HCC surveillance receipt, lower early-stage cancer detection, and modestly worse OS. Furthermore, previous approaches to ultrasound-based HCC surveillance show clear limitations.
Therefore, the evaluation of alternative, e.g., biomarker-based, screening methods is mandatory. The selection of appropriate HCC treatment options for MASH patients must also consider MASH-associated and potentially therapy-limiting comorbidities, as non-cancer mortality significantly impacts OS even in curatively treated patients. Here future systemic therapy trials urgently need to address MASLD as a separate subgroup to avoid underrepresentation of this worldwide epidemic disease.
Author Contributions
Conceptualization, J.B., P.P.M. and C.L.; investigation, J.B., P.P.M. and C.L.; performed the literature review, J.B., P.P.M. and C.L. writing—original draft preparation, J.B., P.P.M. and C.L.; writing—review and editing, J.B., P.P.M., C.L. and J.D.C.; designed the project, J.B., P.P.M. and C.L. All authors provided intellectual input. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Acknowledgments
Figures were created with “Biological illustration” (http://smart.servier.com, accessed on 10 February 2024) by Servier, used under Creative Commons Attribution 3.0 Unported License/modified by Paul Manka.
Conflicts of Interest
C.L. and J.D.C. certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or nonfinancial interest (such as personal or professional relationships, affiliations, knowledge, or beliefs) in the subject matter or materials discussed in this manuscript. P.P.M. reports personal fees and non-financial support from Intercept Pharmaceuticals. J.B. reports personal fees and non-financial support from Roche, BMS, Novartis, EISAI, Falk, Ipsen, MSD, Boston Scientific. No other potential conflict of interest relevant to this article was reported.
References
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Mathers, C.; Parkin, D.M.; Piñeros, M.; Znaor, A.; Bray, F. Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int. J. Cancer 2019, 144, 1941–1953. [Google Scholar] [CrossRef] [PubMed]
- Rinella, M.E. Examining the Nomenclature Change from NAFLD and NASH to MASLD and MASH. Gastroenterol. Hepatol. 2023, 19, 697–699. [Google Scholar]
- Ertle, J.; Dechêne, A.; Sowa, J.-P.; Penndorf, V.; Herzer, K.; Kaiser, G.; Schlaak, J.F.; Gerken, G.; Syn, W.-K.; Canbay, A. Non-alcoholic fatty liver disease progresses to hepatocellular carcinoma in the absence of apparent cirrhosis. Int. J. Cancer 2011, 128, 2436–2443. [Google Scholar] [CrossRef] [PubMed]
- Stine, J.G.; Wentworth, B.J.; Zimmet, A.; Rinella, M.E.; Loomba, R.; Caldwell, S.H.; Argo, C.K. Systematic review with meta-analysis: Risk of hepatocellular carcinoma in non-alcoholic steatohepatitis without cirrhosis compared to other liver diseases. Aliment. Pharmacol. Ther. 2018, 48, 696–703. [Google Scholar] [CrossRef] [PubMed]
- Desai, A.; Sandhu, S.; Lai, J.-P.; Sandhu, D.S. Hepatocellular carcinoma in non-cirrhotic liver: A comprehensive review. World J. Hepatol. 2019, 11, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Balakrishnan, M.; El-Serag, H.B. Editorial: NAFLD-related hepatocellular carcinoma—Increasing or not? With or without cirrhosis? Aliment. Pharmacol. Ther. 2018, 47, 437–438. [Google Scholar] [CrossRef] [PubMed]
- Loomba, R.; Lim, J.K.; Patton, H.; El-Serag, H.B. AGA Clinical Practice Update on Screening and Surveillance for Hepatocellular Carcinoma in Patients with Nonalcoholic Fatty Liver Disease: Expert Review. Gastroenterology 2020, 158, 1822–1830. [Google Scholar] [CrossRef] [PubMed]
- Singal, A.G.; El-Serag, H.B. Rational HCC screening approaches for patients with NAFLD. J. Hepatol. 2022, 76, 195–201. [Google Scholar] [CrossRef]
- Center, M.M.; Jemal, A. International trends in liver cancer incidence rates. Cancer Epidemiol. Biomark. Prev. 2011, 20, 2362–2368. [Google Scholar] [CrossRef]
- Ascha, M.S.; Hanouneh, I.A.; Lopez, R.; Tamimi, T.A.; Feldstein, A.F.; Zein, N.N. The incidence and risk factors of hepatocellular carcinoma in patients with nonalcoholic steatohepatitis. Hepatology 2010, 51, 1972–1978. [Google Scholar] [CrossRef]
- Kanwal, F.; Kramer, J.R.; Mapakshi, S.; Natarajan, Y.; Chayanupatkul, M.; Richardson, P.A.; Li, L.; Desiderio, R.; Thrift, A.P.; Asch, S.M.; et al. Risk of Hepatocellular Cancer in Patients with Non-Alcoholic Fatty Liver Disease. Gastroenterology 2018, 155, 1828–1837. [Google Scholar] [CrossRef]
- Sayiner, M.; Golabi, P.; Younossi, Z.M. Disease Burden of Hepatocellular Carcinoma: A Global Perspective. Dig. Dis. Sci. 2019, 64, 910–917. [Google Scholar] [CrossRef]
- White, D.L.; Kanwal, F.; El–Serag, H.B. Association Between Nonalcoholic Fatty Liver Disease and Risk for Hepatocellular Cancer, Based on Systematic Review. Clin. Gastroenterol. Hepatol. 2012, 10, 1342–1359.e2. [Google Scholar] [CrossRef] [PubMed]
- Younossi, Z.; Stepanova, M.; Ong, J.P.; Jacobson, I.M.; Bugianesi, E.; Duseja, A.; Eguchi, Y.; Wong, V.W.; Negro, F.; Yilmaz, Y.; et al. Nonalcoholic Steatohepatitis Is the Fastest Growing Cause of Hepatocellular Carcinoma in Liver Transplant Candidates. Clin. Gastroenterol. Hepatol. 2019, 17, 748–755. [Google Scholar] [CrossRef] [PubMed]
- Haldar, D.; Kern, B.; Hodson, J.; Armstrong, M.J.; Adam, R.; Berlakovich, G.; Fritz, J.; Feurstein, B.; Popp, W.; Karam, V.; et al. Outcomes of liver transplantation for non-alcoholic steatohepatitis: A European Liver Transplant Registry study. J. Hepatol. 2019, 71, 313–322. [Google Scholar] [CrossRef] [PubMed]
- Weinmann, A.; Koch, S.; Niederle, I.M.; Schulze-Bergkamen, H.; König, J.; Hoppe-Lotichius, M.; Hansen, T.; Pitton, M.B.; Düber, C.; Otto, G.; et al. Trends in epidemiology, treatment, and survival of hepatocellular carcinoma patients between 1998 and 2009: An analysis of 1066 cases of a German HCC Registry. J. Clin. Gastroenterol. 2014, 48, 279–289. [Google Scholar] [CrossRef] [PubMed]
- Estes, C.; Anstee, Q.M.; Arias-Loste, M.T.; Bantel, H.; Bellentani, S.; Caballeria, J.; Colombo, M.; Craxi, A.; Crespo, J.; Day, C.P.; et al. Modeling NAFLD disease burden in China, France, Germany, Italy, Japan, Spain, United Kingdom, and United States for the period 2016–2030. J. Hepatol. 2018, 69, 896–904. [Google Scholar] [CrossRef] [PubMed]
- Anstee, Q.M.; Reeves, H.L.; Kotsiliti, E.; Govaere, O.; Heikenwalder, M. From NASH to HCC: Current concepts and future challenges. Nat. Rev. Gastroenterol. Hepatol. 2019, 16, 411–428. [Google Scholar] [CrossRef] [PubMed]
- Rinella, M.E.; Lazarus, J.V.; Ratziu, V.; Francque, S.M.; Sanyal, A.J.; Kanwal, F.; Romero, D.; Abdelmalek, M.F.; Anstee, Q.M.; Arab, J.P.; et al. A multisociety Delphi consensus statement on new fatty liver disease nomenclature. Hepatology 2023, 78, 1966–1986. [Google Scholar] [CrossRef]
- Ioannou, G.N. Epidemiology and risk-stratification of NAFLD-associated HCC. J. Hepatol. 2021, 75, 1476–1484. [Google Scholar] [CrossRef]
- Liu, Y.L.; Patman, G.L.; Leathart, J.B.; Piguet, A.C.; Burt, A.D.; Dufour, J.F.; Day, C.P.; Daly, A.K.; Reeves, H.L.; Anstee, Q.M. Carriage of the PNPLA3 rs738409 C > G polymorphism confers an increased risk of non-alcoholic fatty liver disease associated hepatocellular carcinoma. J. Hepatol. 2014, 61, 75–81. [Google Scholar] [CrossRef] [PubMed]
- Stickel, F.; Buch, S.; Nischalke, H.D.; Weiss, K.H.; Gotthardt, D.; Fischer, J.; Rosendahl, J.; Marot, A.; Elamly, M.; Casper, M.; et al. Correction: Genetic Variants in PNPLA3 and TM6SF2 Predispose to the Development of Hepatocellular Carcinoma in Individuals with Alcohol-Related Cirrhosis. Am. J. Gastroenterol. 2018, 113, 1099. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; Trépo, E.; Nahon, P.; Cao, Q.; Moreno, C.; Letouzé, E.; Imbeaud, S.; Gustot, T.; Deviere, J.; Debette, S.; et al. PNPLA3 and TM6SF2 variants as risk factors of hepatocellular carcinoma across various etiologies and severity of underlying liver diseases. Int. J. Cancer 2019, 144, 533–544. [Google Scholar] [CrossRef] [PubMed]
- Gellert-Kristensen, H.; Nordestgaard, B.G.; Tybjaerg-Hansen, A.; Stender, S. High Risk of Fatty Liver Disease Amplifies the Alanine Transaminase-Lowering Effect of a HSD17B13 Variant. Hepatology 2020, 71, 56–66. [Google Scholar] [CrossRef] [PubMed]
- Abul-Husn, N.S.; Cheng, X.; Li, A.H.; Xin, Y.; Schurmann, C.; Stevis, P.; Liu, Y.; Kozlitina, J.; Stender, S.; Wood, G.C.; et al. A Protein-Truncating HSD17B13 Variant and Protection from Chronic Liver Disease. N. Engl. J. Med. 2018, 378, 1096–1106. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Belyaeva, O.V.; Brown, P.M.; Fujita, K.; Valles, K.; Karki, S.; de Boer, Y.S.; Koh, C.; Chen, Y.; Du, X.; et al. 17-Beta Hydroxysteroid Dehydrogenase 13 Is a Hepatic Retinol Dehydrogenase Associated with Histological Features of Nonalcoholic Fatty Liver Disease. Hepatology 2019, 69, 1504–1519. [Google Scholar] [CrossRef] [PubMed]
- Pietrangelo, A. Iron in NASH, chronic liver diseases and HCC: How much iron is too much? J. Hepatol. 2009, 50, 249–251. [Google Scholar] [CrossRef] [PubMed]
- Kutlu, O.; Kaleli, H.N.; Ozer, E. Molecular Pathogenesis of Nonalcoholic Steatohepatitis- (NASH-) Related Hepatocellular Carcinoma. Can. J. Gastroenterol. Hepatol. 2018, 2018, 8543763. [Google Scholar] [CrossRef] [PubMed]
- Dhar, D.; Antonucci, L.; Nakagawa, H.; Kim, J.Y.; Glitzner, E.; Caruso, S.; Shalapour, S.; Yang, L.; Valasek, M.A.; Lee, S.; et al. Liver Cancer Initiation Requires p53 Inhibition by CD44-Enhanced Growth Factor Signaling. Cancer Cell 2018, 33, 1061–1077.e1066. [Google Scholar] [CrossRef]
- Brenner, D.A.; Paik, Y.-H.; Schnabl, B. Role of Gut Microbiota in Liver Disease. J. Clin. Gastroenterol. 2015, 49, S25–S27. [Google Scholar] [CrossRef]
- Etienne-Mesmin, L.; Chassaing, B.; Gewirtz, A.T. Tryptophan: A gut microbiota-derived metabolites regulating inflammation. World J. Gastrointest. Pharmacol. Ther. 2017, 8, 7–9. [Google Scholar] [CrossRef] [PubMed]
- Konturek, P.C.; Harsch, I.A.; Konturek, K.; Schink, M.; Konturek, T.; Neurath, M.F.; Zopf, Y. Gut⁻Liver Axis: How Do Gut Bacteria Influence the Liver? Med. Sci. 2018, 6, 79. [Google Scholar] [CrossRef] [PubMed]
- Kostic, A.D.; Xavier, R.J.; Gevers, D. The microbiome in inflammatory bowel disease: Current status and the future ahead. Gastroenterology 2014, 146, 1489–1499. [Google Scholar] [CrossRef]
- Kudo, M.; Matilla, A.; Santoro, A.; Melero, I.; Gracian, A.C.; Acosta-Rivera, M.; Choo, S.P.; El-Khoueiry, A.B.; Kuromatsu, R.; El-Rayes, B.; et al. CheckMate 040 cohort 5: A phase I/II study of nivolumab in patients with advanced hepatocellular carcinoma and Child-Pugh B cirrhosis. J. Hepatol. 2021, 75, 600–609. [Google Scholar] [CrossRef]
- Zhou, D.; Pan, Q.; Shen, F.; Cao, H.X.; Ding, W.J.; Chen, Y.W.; Fan, J.G. Total fecal microbiota transplantation alleviates high-fat diet-induced steatohepatitis in mice via beneficial regulation of gut microbiota. Sci. Rep. 2017, 7, 1529. [Google Scholar] [CrossRef]
- Dapito, D.H.; Mencin, A.; Gwak, G.Y.; Pradere, J.P.; Jang, M.K.; Mederacke, I.; Caviglia, J.M.; Khiabanian, H.; Adeyemi, A.; Bataller, R.; et al. Promotion of hepatocellular carcinoma by the intestinal microbiota and TLR4. Cancer Cell 2012, 21, 504–516. [Google Scholar] [CrossRef]
- Nowak, A.; Paliwoda, A.; Błasiak, J. Anti-proliferative, pro-apoptotic and anti-oxidative activity of Lactobacillus and Bifidobacterium strains: A review of mechanisms and therapeutic perspectives. Crit. Rev. Food Sci. Nutr. 2019, 59, 3456–3467. [Google Scholar] [CrossRef]
- Yoshimoto, S.; Loo, T.M.; Atarashi, K.; Kanda, H.; Sato, S.; Oyadomari, S.; Iwakura, Y.; Oshima, K.; Morita, H.; Hattori, M.; et al. Obesity-induced gut microbial metabolite promotes liver cancer through senescence secretome. Nature 2013, 499, 97–101. [Google Scholar] [CrossRef] [PubMed]
- Ponziani, F.R.; Bhoori, S.; Castelli, C.; Putignani, L.; Rivoltini, L.; Del Chierico, F.; Sanguinetti, M.; Morelli, D.; Paroni Sterbini, F.; Petito, V.; et al. Hepatocellular Carcinoma Is Associated with Gut Microbiota Profile and Inflammation in Nonalcoholic Fatty Liver Disease. Hepatology 2019, 69, 107–120. [Google Scholar] [CrossRef]
- Schonewille, M.; de Boer, J.F.; Groen, A.K. Bile salts in control of lipid metabolism. Curr. Opin. Lipidol. 2016, 27, 295–301. [Google Scholar] [CrossRef]
- Mouzaki, M.; Wang, A.Y.; Bandsma, R.; Comelli, E.M.; Arendt, B.M.; Zhang, L.; Fung, S.; Fischer, S.E.; McGilvray, I.G.; Allard, J.P. Bile Acids and Dysbiosis in Non-Alcoholic Fatty Liver Disease. PLoS ONE 2016, 11, e0151829. [Google Scholar] [CrossRef] [PubMed]
- Neuschwander-Tetri, B.A.; Van Natta, M.L.; Tonascia, J.; Brunt, E.M.; Kleiner, D.E. Trials of obeticholic acid for non-alcoholic steatohepatitis—Authors’ reply. Lancet 2015, 386, 28–29. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Li, F.; Zhuang, Y.; Xu, J.; Wang, J.; Mao, X.; Zhang, Y.; Liu, X. Alteration in gut microbiota associated with hepatitis B and non-hepatitis virus related hepatocellular carcinoma. Gut Pathog. 2019, 11, 1. [Google Scholar] [CrossRef] [PubMed]
- Sydor, S.; Best, J.; Messerschmidt, I.; Manka, P.; Vilchez-Vargas, R.; Brodesser, S.; Lucas, C.; Wegehaupt, A.; Wenning, C.; Aßmuth, S.; et al. Altered Microbiota Diversity and Bile Acid Signaling in Cirrhotic and Noncirrhotic NASH-HCC. Clin. Transl. Gastroenterol. 2020, 11, e00131. [Google Scholar] [CrossRef] [PubMed]
- Jiao, N.; Baker, S.S.; Chapa-Rodriguez, A.; Liu, W.; Nugent, C.A.; Tsompana, M.; Mastrandrea, L.; Buck, M.J.; Baker, R.D.; Genco, R.J.; et al. Suppressed hepatic bile acid signalling despite elevated production of primary and secondary bile acids in NAFLD. Gut 2018, 67, 1881–1891. [Google Scholar] [CrossRef] [PubMed]
- Bechmann, L.P.; Kocabayoglu, P.; Sowa, J.P.; Sydor, S.; Best, J.; Schlattjan, M.; Beilfuss, A.; Schmitt, J.; Hannivoort, R.A.; Kilicarslan, A.; et al. Free fatty acids repress small heterodimer partner (SHP) activation and adiponectin counteracts bile acid-induced liver injury in superobese patients with nonalcoholic steatohepatitis. Hepatology 2013, 57, 1394–1406. [Google Scholar] [CrossRef] [PubMed]
- Caussy, C.; Tripathi, A.; Humphrey, G.; Bassirian, S.; Singh, S.; Faulkner, C.; Bettencourt, R.; Rizo, E.; Richards, L.; Xu, Z.Z.; et al. A gut microbiome signature for cirrhosis due to nonalcoholic fatty liver disease. Nat. Commun. 2019, 10, 1406. [Google Scholar] [CrossRef] [PubMed]
- Heimbach, J.K.; Kulik, L.M.; Finn, R.S.; Sirlin, C.B.; Abecassis, M.M.; Roberts, L.R.; Zhu, A.X.; Murad, M.H.; Marrero, J.A. AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 2018, 67, 358–380. [Google Scholar] [CrossRef] [PubMed]
- Dyson, J.; Jaques, B.; Chattopadyhay, D.; Lochan, R.; Graham, J.; Das, D.; Aslam, T.; Patanwala, I.; Gaggar, S.; Cole, M.; et al. Hepatocellular cancer: The impact of obesity, type 2 diabetes and a multidisciplinary team. J. Hepatol. 2014, 60, 110–117. [Google Scholar] [CrossRef]
- van Meer, S.; van Erpecum, K.J.; Sprengers, D.; Coenraad, M.J.; Klümpen, H.J.; Jansen, P.L.; Ijzermans, J.N.; Verheij, J.; van Nieuwkerk, C.M.; Siersema, P.D.; et al. Hepatocellular carcinoma in cirrhotic versus noncirrhotic livers: Results from a large cohort in the Netherlands. Eur. J. Gastroenterol. Hepatol. 2016, 28, 352–359. [Google Scholar] [CrossRef]
- Tzartzeva, K.; Obi, J.; Rich, N.E.; Parikh, N.D.; Marrero, J.A.; Yopp, A.; Waljee, A.K.; Singal, A.G. Surveillance Imaging and Alpha Fetoprotein for Early Detection of Hepatocellular Carcinoma in Patients with Cirrhosis: A Meta-analysis. Gastroenterology 2018, 154, 1706–1718.e1. [Google Scholar] [CrossRef] [PubMed]
- Best, J.; Bechmann, L.P.; Sowa, J.P.; Sydor, S.; Dechêne, A.; Pflanz, K.; Bedreli, S.; Schotten, C.; Geier, A.; Berg, T.; et al. GALAD Score Detects Early Hepatocellular Carcinoma in an International Cohort of Patients with Nonalcoholic Steatohepatitis. Clin. Gastroenterol. Hepatol. 2020, 18, 728–735.e4. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.D.; Addissie, B.D.; Mara, K.C.; Harmsen, W.S.; Dai, J.; Zhang, N.; Wongjarupong, N.; Ali, H.M.; Ali, H.A.; Hassan, F.A.; et al. GALAD Score for Hepatocellular Carcinoma Detection in Comparison with Liver Ultrasound and Proposal of GALADUS Score. Cancer Epidemiol. Biomark. Prev. 2019, 28, 531–538. [Google Scholar] [CrossRef] [PubMed]
- Okajima, W.; Komatsu, S.; Ichikawa, D.; Miyamae, M.; Ohashi, T.; Imamura, T.; Kiuchi, J.; Nishibeppu, K.; Arita, T.; Konishi, H.; et al. Liquid biopsy in patients with hepatocellular carcinoma: Circulating tumor cells and cell-free nucleic acids. World J. Gastroenterol. 2017, 23, 5650–5668. [Google Scholar] [CrossRef] [PubMed]
- Reddy, S.K.; Steel, J.L.; Chen, H.W.; DeMateo, D.J.; Cardinal, J.; Behari, J.; Humar, A.; Marsh, J.W.; Geller, D.A.; Tsung, A. Outcomes of curative treatment for hepatocellular cancer in nonalcoholic steatohepatitis versus hepatitis C and alcoholic liver disease. Hepatology 2012, 55, 1809–1819. [Google Scholar] [CrossRef] [PubMed]
- Yao, F.Y.; Ferrell, L.; Bass, N.M.; Watson, J.J.; Bacchetti, P.; Venook, A.; Ascher, N.L.; Roberts, J.P. Liver transplantation for hepatocellular carcinoma: Expansion of the tumor size limits does not adversely impact survival. Hepatology 2001, 33, 1394–1403. [Google Scholar] [CrossRef] [PubMed]
- Mazzaferro, V.; Llovet, J.M.; Miceli, R.; Bhoori, S.; Schiavo, M.; Mariani, L.; Camerini, T.; Roayaie, S.; Schwartz, M.E.; Grazi, G.L.; et al. Predicting survival after liver transplantation in patients with hepatocellular carcinoma beyond the Milan criteria: A retrospective, exploratory analysis. Lancet Oncol. 2009, 10, 35–43. [Google Scholar] [CrossRef] [PubMed]
- Mazzaferro, V.; Sposito, C.; Zhou, J.; Pinna, A.D.; De Carlis, L.; Fan, J.; Cescon, M.; Di Sandro, S.; Yi-Feng, H.; Lauterio, A.; et al. Metroticket 2.0 Model for Analysis of Competing Risks of Death after Liver Transplantation for Hepatocellular Carcinoma. Gastroenterology 2018, 154, 128–139. [Google Scholar] [CrossRef]
- Shirabe, K.; Itoh, S.; Yoshizumi, T.; Soejima, Y.; Taketomi, A.; Aishima, S.; Maehara, Y. The predictors of microvascular invasion in candidates for liver transplantation with hepatocellular carcinoma-with special reference to the serum levels of des-gamma-carboxy prothrombin. J. Surg. Oncol. 2007, 95, 235–240. [Google Scholar] [CrossRef]
- Duvoux, C.; Roudot-Thoraval, F.; Decaens, T.; Pessione, F.; Badran, H.; Piardi, T.; Francoz, C.; Compagnon, P.; Vanlemmens, C.; Dumortier, J.; et al. Liver transplantation for hepatocellular carcinoma: A model including alpha-fetoprotein improves the performance of Milan criteria. Gastroenterology 2012, 143, 986–994. [Google Scholar] [CrossRef]
- Mikolasevic, I.; Filipec-Kanizaj, T.; Mijic, M.; Jakopcic, I.; Milic, S.; Hrstic, I.; Sobocan, N.; Stimac, D.; Burra, P. Nonalcoholic fatty liver disease and liver transplantation—Where do we stand? World J. Gastroenterol. 2018, 24, 1491–1506. [Google Scholar] [CrossRef] [PubMed]
- Reig, M.; Forner, A.; Rimola, J.; Ferrer-Fàbrega, J.; Burrel, M.; Garcia-Criado, Á.; Kelley, R.K.; Galle, P.R.; Mazzaferro, V.; Salem, R.; et al. BCLC strategy for prognosis prediction and treatment recommendation: The 2022 update. J. Hepatol. 2022, 76, 681–693. [Google Scholar] [CrossRef]
- Llovet, J.M.; Real, M.I.; Montaña, X.; Planas, R.; Coll, S.; Aponte, J.; Ayuso, C.; Sala, M.; Muchart, J.; Solà, R.; et al. Arterial embolisation or chemoembolisation versus symptomatic treatment in patients with unresectable hepatocellular carcinoma: A randomised controlled trial. Lancet 2002, 359, 1734–1739. [Google Scholar] [CrossRef] [PubMed]
- Young, S.; Sanghvi, T.; Rubin, N.; Hall, D.; Roller, L.; Charaf, Y.; Golzarian, J. Transarterial Chemoembolization of Hepatocellular Carcinoma: Propensity Score Matching Study Comparing Survival and Complications in Patients with Nonalcoholic Steatohepatitis Versus Other Causes Cirrhosis. Cardiovasc. Interv. Radiol. 2020, 43, 65–75. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.E.; Charles, H.W.; Park, J.S.; Goldenberg, A.S.; Deipolyi, A.R. Obesity conveys poor outcome in patients with hepatocellular carcinoma treated by transarterial chemoembolization. Diagn. Interv. Imaging 2017, 98, 37–42. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Gong, F.; Li, L.; Zhao, M.; Song, J. Diabetes mellitus and the neutrophil to lymphocyte ratio predict overall survival in non-viral hepatocellular carcinoma treated with transarterial chemoembolization. Oncol. Lett. 2014, 7, 1704–1710. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.; Xia, F.; Fan, G.; Yu, J.; Bao, L.; Zhang, C.; Chi, R.; Zhang, T.; Wang, L.; Shen, F.; et al. Type 2 diabetes mellitus worsens the prognosis of intermediate-stage hepatocellular carcinoma after transarterial chemoembolization. Diabetes Res. Clin. Pract. 2020, 169, 108375. [Google Scholar] [CrossRef]
- Jung, W.J.; Jang, S.; Choi, W.J.; Park, J.; Choi, G.H.; Jang, E.S.; Jeong, S.H.; Choi, W.S.; Lee, J.H.; Yoon, C.J.; et al. Metformin administration is associated with enhanced response to transarterial chemoembolization for hepatocellular carcinoma in type 2 diabetes patients. Sci. Rep. 2022, 12, 14482. [Google Scholar] [CrossRef] [PubMed]
- Schotten, C.; Bechmann, L.P.; Manka, P.; Theysohn, J.; Dechêne, A.; EI Fouly, A.; Barbato, F.; Neumann, U.; Radünz, S.; Sydor, S.; et al. NAFLD-Associated Comorbidities in Advanced Stage HCC Do Not Alter the Safety and Efficacy of Yttrium-90 Radioembolization. Liver Cancer 2019, 8, 491–504. [Google Scholar] [CrossRef]
- Llovet, J.M.; Ricci, S.; Mazzaferro, V.; Hilgard, P.; Gane, E.; Blanc, J.F.; de Oliveira, A.C.; Santoro, A.; Raoul, J.L.; Forner, A.; et al. Sorafenib in advanced hepatocellular carcinoma. N. Engl. J. Med. 2008, 359, 378–390. [Google Scholar] [CrossRef]
- Cheng, A.L.; Kang, Y.K.; Chen, Z.; Tsao, C.J.; Qin, S.; Kim, J.S.; Luo, R.; Feng, J.; Ye, S.; Yang, T.S.; et al. Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: A phase III randomised, double-blind, placebo-controlled trial. Lancet Oncol. 2009, 10, 25–34. [Google Scholar] [CrossRef] [PubMed]
- Kudo, M.; Finn, R.S.; Qin, S.; Han, K.H.; Ikeda, K.; Piscaglia, F.; Baron, A.; Park, J.W.; Han, G.; Jassem, J.; et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: A randomised phase 3 non-inferiority trial. Lancet 2018, 391, 1163–1173. [Google Scholar] [CrossRef] [PubMed]
- Bruix, J.; Qin, S.; Merle, P.; Granito, A.; Huang, Y.H.; Bodoky, G.; Pracht, M.; Yokosuka, O.; Rosmorduc, O.; Breder, V.; et al. Regorafenib for patients with hepatocellular carcinoma who progressed on sorafenib treatment (RESORCE): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 2017, 389, 56–66. [Google Scholar] [CrossRef] [PubMed]
- Abou-Alfa, G.K.; Meyer, T.; Cheng, A.L.; El-Khoueiry, A.B.; Rimassa, L.; Ryoo, B.Y.; Cicin, I.; Merle, P.; Chen, Y.; Park, J.W.; et al. Cabozantinib in Patients with Advanced and Progressing Hepatocellular Carcinoma. N. Engl. J. Med. 2018, 379, 54–63. [Google Scholar] [CrossRef] [PubMed]
- Zhu, A.X.; Kang, Y.K.; Yen, C.J.; Finn, R.S.; Galle, P.R.; Llovet, J.M.; Assenat, E.; Brandi, G.; Pracht, M.; Lim, H.Y.; et al. Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased α-fetoprotein concentrations (REACH-2): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2019, 20, 282–296. [Google Scholar] [CrossRef] [PubMed]
- Cheng, A.L.; Qin, S.; Ikeda, M.; Galle, P.R.; Ducreux, M.; Kim, T.Y.; Lim, H.Y.; Kudo, M.; Breder, V.; Merle, P.; et al. Updated efficacy and safety data from IMbrave150: Atezolizumab plus bevacizumab vs. sorafenib for unresectable hepatocellular carcinoma. J. Hepatol. 2022, 76, 862–873. [Google Scholar] [CrossRef] [PubMed]
- Abou-Alfa, G.K.; Lau, G.; Kudo, M.; Chan, S.L.; Kelley, R.K.; Furuse, J.; Sukeepaisarnjaroen, W.; Kang, Y.-K.; Dao, T.V.; Toni, E.N.D.; et al. Tremelimumab plus Durvalumab in Unresectable Hepatocellular Carcinoma. NEJM Evid. 2022, 1, EVIDoa2100070. [Google Scholar] [CrossRef] [PubMed]
- Finn, R.S.; Kudo, M.; Merle, P.; Meyer, T.; Qin, S.; Ikeda, M.; Xu, R.; Edeline, J.; Ryoo, B.Y.; Ren, Z.; et al. LBA34 Primary results from the phase III LEAP-002 study: Lenvatinib plus pembrolizumab versus lenvatinib as first-line (1L) therapy for advanced hepatocellular carcinoma (aHCC). Ann. Oncol. 2022, 33, S1401. [Google Scholar] [CrossRef]
- Kelley, R.K.; Rimassa, L.; Cheng, A.L.; Kaseb, A.; Qin, S.; Zhu, A.X.; Chan, S.L.; Melkadze, T.; Sukeepaisarnjaroen, W.; Breder, V.; et al. Cabozantinib plus atezolizumab versus sorafenib for advanced hepatocellular carcinoma (COSMIC-312): A multicentre, open-label, randomised, phase 3 trial. Lancet Oncol. 2022, 23, 995–1008. [Google Scholar] [CrossRef]
- Finn, R.S.; Qin, S.; Ikeda, M.; Galle, P.R.; Ducreux, M.; Kim, T.Y.; Kudo, M.; Breder, V.; Merle, P.; Kaseb, A.O.; et al. Atezolizumab plus Bevacizumab in Unresectable Hepatocellular Carcinoma. N. Engl. J. Med. 2020, 382, 1894–1905. [Google Scholar] [CrossRef]
- Pfister, D.; Núñez, N.G.; Pinyol, R.; Govaere, O.; Pinter, M.; Szydlowska, M.; Gupta, R.; Qiu, M.; Deczkowska, A.; Weiner, A.; et al. NASH limits anti-tumour surveillance in immunotherapy-treated HCC. Nature 2021, 592, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Haber, P.K.; Puigvehí, M.; Castet, F.; Lourdusamy, V.; Montal, R.; Tabrizian, P.; Buckstein, M.; Kim, E.; Villanueva, A.; Schwartz, M.; et al. Evidence-Based Management of Hepatocellular Carcinoma: Systematic Review and Meta-analysis of Randomized Controlled Trials (2002–2020). Gastroenterology 2021, 161, 879–898. [Google Scholar] [CrossRef] [PubMed]
- Meyer, T.; Galani, S.; Lopes, A.; Vogel, A. Aetiology of liver disease and response to immune checkpoint inhibitors: An updated meta-analysis confirms benefit in those with non-viral liver disease. J. Hepatol. 2023, 79, e73–e76. [Google Scholar] [CrossRef] [PubMed]
- Welland, S.; Leyh, C.; Finkelmeier, F.; Jefremow, A.; Shmanko, K.; Gonzalez-Carmona, M.A.; Kandulski, A.; Jeliazkova, P.; Best, J.; Fründt, T.W.; et al. Real-World Data for Lenvatinib in Hepatocellular Carcinoma (ELEVATOR): A Retrospective Multicenter Study. Liver Cancer 2022, 11, 219–232. [Google Scholar] [CrossRef] [PubMed]
- Bruix, J.; Raoul, J.L.; Sherman, M.; Mazzaferro, V.; Bolondi, L.; Craxi, A.; Galle, P.R.; Santoro, A.; Beaugrand, M.; Sangiovanni, A.; et al. Efficacy and safety of sorafenib in patients with advanced hepatocellular carcinoma: Subanalyses of a phase III trial. J. Hepatol. 2012, 57, 821–829. [Google Scholar] [CrossRef] [PubMed]
- Hiraoka, A.; Kumada, T.; Tada, T.; Tani, J.; Kariyama, K.; Fukunishi, S.; Atsukawa, M.; Hirooka, M.; Tsuji, K.; Ishikawa, T.; et al. Efficacy of lenvatinib for unresectable hepatocellular carcinoma based on background liver disease etiology: Multi-center retrospective study. Sci. Rep. 2021, 11, 16663. [Google Scholar] [CrossRef] [PubMed]
- Sacco, R.; Ramai, D.; Tortora, R.; di Costanzo, G.G.; Burlone, M.E.; Pirisi, M.; Federico, P.; Daniele, B.; Silletta, M.; Gallo, P.; et al. Role of Etiology in Hepatocellular Carcinoma Patients Treated with Lenvatinib: A Counterfactual Event-Based Mediation Analysis. Cancers 2023, 15, 381. [Google Scholar] [CrossRef] [PubMed]
- Casadei-Gardini, A.; Rimini, M.; Tada, T.; Suda, G.; Shimose, S.; Kudo, M.; Cheon, J.; Finkelmeier, F.; Lim, H.Y.; Rimassa, L.; et al. Atezolizumab plus bevacizumab versus lenvatinib for unresectable hepatocellular carcinoma: A large real-life worldwide population. Eur. J. Cancer 2023, 180, 9–20. [Google Scholar] [CrossRef]
- Rimini, M.; Rimassa, L.; Ueshima, K.; Burgio, V.; Shigeo, S.; Tada, T.; Suda, G.; Yoo, C.; Cheon, J.; Pinato, D.J.; et al. Atezolizumab plus bevacizumab versus lenvatinib or sorafenib in non-viral unresectable hepatocellular carcinoma: An international propensity score matching analysis. ESMO Open 2022, 7, 100591. [Google Scholar] [CrossRef]
- Ramai, D.; Singh, J.; Lester, J.; Khan, S.R.; Chandan, S.; Tartaglia, N.; Ambrosi, A.; Serviddio, G.; Facciorusso, A. Systematic review with meta-analysis: Bariatric surgery reduces the incidence of hepatocellular carcinoma. Aliment. Pharmacol. Ther. 2021, 53, 977–984. [Google Scholar] [CrossRef]
- Kojima, M.; Takahashi, H.; Kuwashiro, T.; Tanaka, K.; Mori, H.; Ozaki, I.; Kitajima, Y.; Matsuda, Y.; Ashida, K.; Eguchi, Y.; et al. Glucagon-Like Peptide-1 Receptor Agonist Prevented the Progression of Hepatocellular Carcinoma in a Mouse Model of Nonalcoholic Steatohepatitis. Int. J. Mol. Sci. 2020, 21, 5722. [Google Scholar] [CrossRef] [PubMed]
- Mirarchi, L.; Amodeo, S.; Citarrella, R.; Licata, A.; Soresi, M.; Giannitrapani, L. SGLT2 Inhibitors as the Most Promising Influencers on the Outcome of Non-Alcoholic Fatty Liver Disease. Int. J. Mol. Sci. 2022, 23, 3668. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).