How to Measure Foot Self-Care? A Methodological Review of Instruments
Abstract
1. Introduction
- (1)
- What is the focus and content of the instruments that measure foot self-care?
- (2)
- What is the psychometric evidence for these foot self-care instruments?
2. Materials and Methods
2.1. Design
2.2. Eligibility Criteria
2.3. Information Sources and Search Strategy
2.4. Selection Process
2.5. Data Collection Process and Data Items
2.6. Quality Appraisal
2.7. Synthesis of Results
3. Results
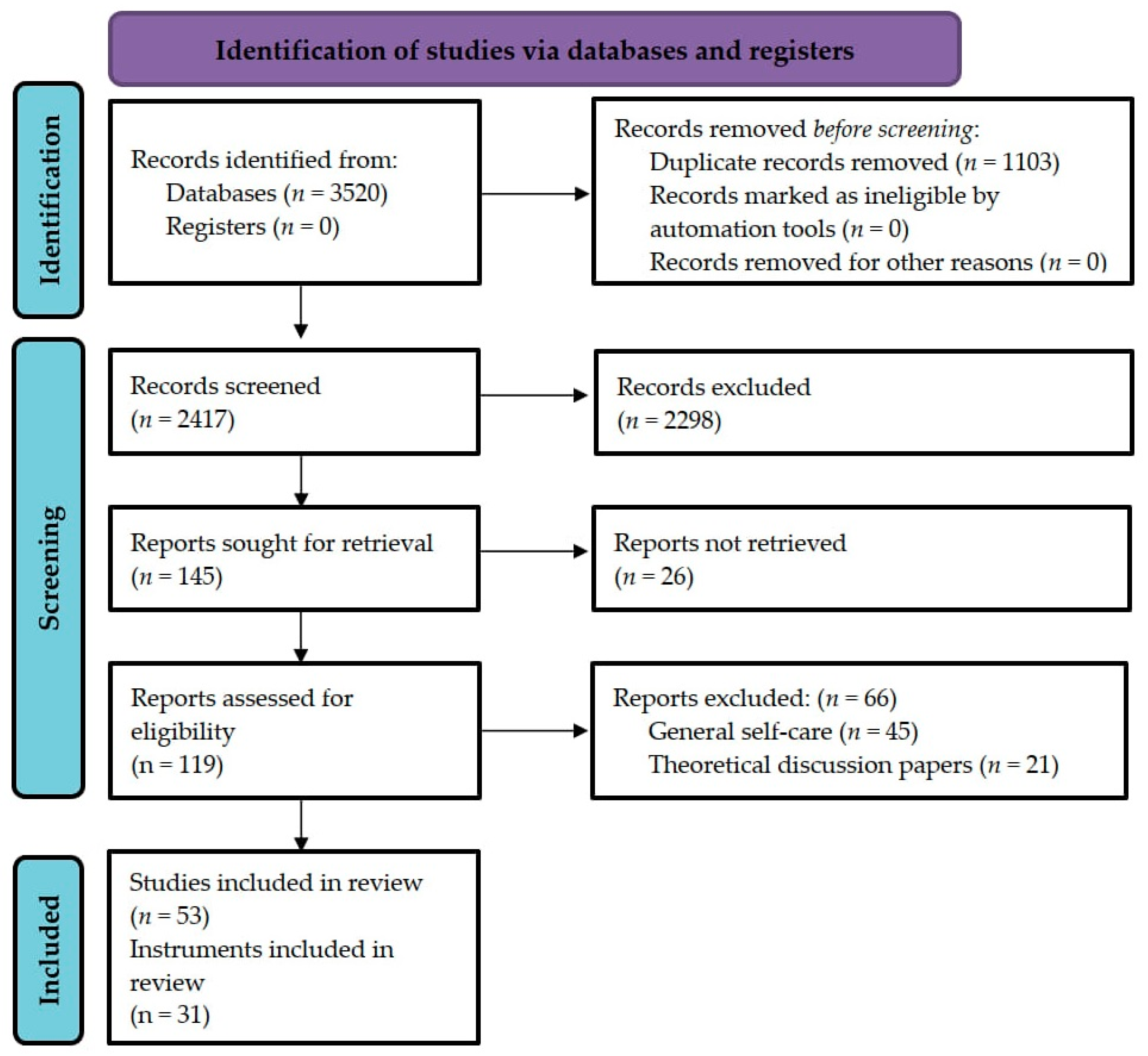
3.1. Study Selection
3.2. Study Characteristics
3.3. Description of the Analysed Instruments
3.4. Methodological Quality of the Included Studies
3.5. Focus and Content of the Instruments
3.6. Psychometric Evidence of the Instruments
3.7. Synthesis of the Results
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Muchna, A.; Najafi, B.B.; Wendel, C.S.; Schwenk, M.; Armstrong, D.G.; Mohler, J. Foot problems in older adults associations with incident falls, frailty syndrome, and sensor-derived gait, balance, and physical activity measures. J. Am. Podiatr. Med. Assoc. 2018, 108, 126–139. [Google Scholar] [CrossRef] [PubMed]
- Kunkel, D.; Mamode, L.; Burnett, M.; Pickering, R.; Bader, D.; Donovan-Hall, M.; Cole, M.; Ashburn, A.; Bowen, C. Footwear characteristics and foot problems in community dwelling people with stroke: A cross-sectional observational study. Disabil. Rehabil. 2022, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wilson, O.; Hewlett, S.; Woodburn, J.; Pollock, J.; Kirwan, J. Prevalence, impact and care of foot problems in people with rheumatoid arthritis: Results from a United Kingdom based cross-sectional survey. J. Foot Ankle Res. 2017, 10, 46. [Google Scholar] [CrossRef] [PubMed]
- Simonsen, M.B.; Hørslev-Petersen, K.; Cöster, M.C.; Jensen, C.; Bremander, A. Foot and ankle problems in patients with rheumatoid arthritis in 2019: Still an important issue. ACR Open Rheumatol. 2021, 3, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Tang, U.H.; Zügner, R.; Lisovskaja, V.; Karlsson, J.; Hagberg, K.; Tranberg, R. Foot deformities, function in the lower extremities, and plantar pressure in patients with diabetes at high risk to develop foot ulcers. Diabet. Foot Ankle 2015, 6, 27593. [Google Scholar] [CrossRef] [PubMed]
- Bundó, M.; Vlacho, B.; Llussà, J.; Puig-Treserra, R.; Mata-Cases, M.; Cos, X.; Jude, E.B.; Franch-Nadal, J.; Mauricio, D. Prevalence and risk factors of diabetic foot disease among the people with type 2 diabetes using real-world practice data from Catalonia during 2018. Front. Endocrinol. 2022, 13, 1024904. [Google Scholar] [CrossRef]
- WHO Regional Office for South-East Asia. Self Care for Health. Available online: https://apps.who.int/iris/handle/10665/205887 (accessed on 20 January 2022).
- Miikkola, M.; Lantta, T.; Suhonen, R.; Stolt, M. Challenges of foot self-care in older people: A qualitative focus-group study. J. Foot Ankle Res. 2019, 12, 5. [Google Scholar] [CrossRef]
- Omote, S.; Watanabe, A.; Hiramatsu, T.; Saito, E.; Yokogawa, M.; Okamoto, R.; Sakakibara, C.; Ichimori, A.; Kyota, K.; Tsukasaki, K. A foot-care program to facilitate self-care by the elderly: A non-randomized intervention study. BMC Res. Notes 2017, 10, 586. [Google Scholar] [CrossRef]
- Cowan, D.T.; Norman, I.; Coopamah, V.P. Competence in nursing practice: A controversial concept—A focused review of literature. Nurse Educ. Today 2005, 25, 355–362. [Google Scholar] [CrossRef]
- Matricciani, L.; Jones, S. Who cares about foot care? Barriers and enablers of foot self-care practices among non-institutionalized older adults diagnosed with diabetes: An integrative review. Diabetes Educ. 2015, 41, 106–117. [Google Scholar] [CrossRef]
- Chiwanga, F.S.; Njelekela, M.A. Diabetic foot: Prevalence, knowledge, and foot self-care practices among diabetic patients in Dar es Salaam, Tanzania—A cross-sectional study. J. Foot Ankle Res. 2015, 8, 20. [Google Scholar] [CrossRef] [PubMed]
- Hirpha, N.; Tatiparthi, R.; Mulugeta, T. Diabetic foot self-care practices among adult diabetic patients: A descriptive cross-sectional study. Diabetes Metab. Syndr. Obes. 2020, 13, 4779–4786. [Google Scholar] [CrossRef] [PubMed]
- Martin, R.L.; Irrgang, J.J. A survey of self-reported outcome instruments for the foot and ankle. J. Orthop. Sports Phys. Ther. 2007, 37, 72–84. [Google Scholar] [CrossRef] [PubMed]
- Sierevelt, I.N.; Zwiers, R.; Schats, W.; Haverkamp, D.; Terwee, C.B.; Nolte, P.A.; Kerkhoffs, G. Measurement properties of the most commonly used Foot- and Ankle-Specific Questionnaires: The FFI, FAOS and FAAM. A systematic review. Knee Surg. Sports Traumatol. Arthrosc. 2018, 26, 2059–2073. [Google Scholar] [CrossRef]
- Lakey, E.; Hunt, K.J. Patient-reported outcomes in foot and ankle orthopedics. Foot Ankle Orthop. 2019, 4, 2473011419852930. [Google Scholar] [CrossRef]
- Hijji, F.Y.; Schneider, A.D.; Pyper, M.; Laughlin, R.T. The popularity of outcome measures used in the foot and ankle literature. Foot Ankle Spec. 2020, 13, 58–68. [Google Scholar] [CrossRef]
- Jia, Y.; Huang, H.; Gagnier, J.J. A systematic review of measurement properties of patient-reported outcome measures for use in patients with foot or ankle diseases. Qual. Life Res. 2017, 26, 1969–2010. [Google Scholar] [CrossRef]
- Van der Leeden, M.; Steultjens, M.P.; Terwee, C.B.; Rosenbaum, D.; Turner, D.; Woodburn, J.; Dekker, J. A systematic review of instruments measuring foot function, foot pain, and foot-related disability in patients with rheumatoid arthritis. Arthritis Rheumatol. 2008, 59, 1257–1269. [Google Scholar] [CrossRef]
- Ortega-Avila, A.B.; Ramos-Petersen, L.; Cervera-Garvi, P.; Nester, C.J.; Morales-Asencio, J.M.; Gijon-Nogueron, G. Systematic review of the psychometric properties of patient-reported outcome measures for rheumatoid arthritis in the foot and ankle. Clin. Rehabil. 2019, 33, 1788–1799. [Google Scholar] [CrossRef]
- Fernández-Torres, R.; Ruiz-Muñoz, M.; Pérez-Panero, A.J.; García-Romero, J.; Gónzalez-Sánchez, M. Instruments of choice for assessment and monitoring diabetic foot: A systematic review. J. Clin. Med. 2020, 9, 602. [Google Scholar] [CrossRef]
- Goodall, R.J.; Ellauzi, J.; Tan, M.; Onida, S.; Davies, A.H.; Shalhoub, J. A systematic review of the impact of foot care education on self efficacy and self care in patients with diabetes. Eur. J. Vasc. Endovasc. Surg. 2020, 60, 282–292. [Google Scholar] [CrossRef] [PubMed]
- Paton, J.; Abey, S.; Hendy, P.; Williams, J.; Collings, R.; Callaghan, L. Behaviour change approaches for individuals with diabetes to improve foot self-management: A scoping review. J. Foot Ankle Res. 2021, 14, 1. [Google Scholar] [CrossRef] [PubMed]
- Srinath, K.M.; Basavegowda, M.; Tharuni, N.S. Diabetic self care practices in rural Mysuru, Southern Karnataka, India—A need for Diabetes Self Management Educational (DSME) program. Diabetes Metab. Syndr. 2017, 11, S181–S186. [Google Scholar] [CrossRef] [PubMed]
- Bonner, T.; Foster, M.; Spears-Lanoix, E. Type 2 Diabetes related foot care knowledge and foot self-care practice interventions in the United States: A systematic review of the literature. Diabet. Foot Ankle 2016, 7, 29758. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Hong, Q.N.; Pluye, P.; Fabregues, S.; Bartlett, G.; Boardman, F.; Cargo, M.; Dagenais, P.; Gagnon, M.-P.; Griffiths, F.; Nicolau, B.; et al. Mixed Methods Appraisal Tool (MMAT), Version 2018; Registration of Copyright (#1148552); Canadian Intellectual Property Office: Gatineau, QC, Canada, 2018. [Google Scholar]
- Zwakhalen, S.M.; Hamers, J.P.; Abu-Saad, H.H.; Berger, M.P. Pain in elderly people with severe dementia: A systematic review of behavioural pain assessment tools. BMC Geriatr. 2006, 6, 15. [Google Scholar] [CrossRef]
- Kielo, E.; Suhonen, R.; Ylönen, M.; Viljamaa, J.; Wahlroos, N.; Stolt, M. A systematic and psychometric review of tests measuring nurses’ wound care knowledge. Int. Wound J. 2020, 17, 1209–1224. [Google Scholar] [CrossRef]
- Chin, Y.F.; Huang, T.T. Development and validation of a diabetes foot self-care behavior scale. J. Nurs. Res. 2013, 21, 19–25. [Google Scholar] [CrossRef]
- Toobert, D.J.; Hampson, S.E.; Glasgow, R.E. The summary of diabetes self-care activities measure: Results from 7 studies and a revised scale. Diabetes Care 2000, 23, 943–950. [Google Scholar] [CrossRef]
- Lincoln, N.B.; Jeffcoate, W.J.; Ince, P.; Smith, M.; Radford, K.A. Validation of a new measure of protective footcare behaviour: The Nottingham Assessment of Functional Footcare (NAFF). Pract. Diabetes 2007, 24, 207–211. [Google Scholar] [CrossRef]
- Navarro-Flores, E.; Morales-Asencio, J.M.; Cervera-Marín, J.A.; Labajos-Manzanares, M.T.; Gijon-Nogueron, G. Development, validation and psychometric analysis of the diabetic foot self-care questionnaire of the University of Malaga, Spain (DFSQ-UMA). J. Tissue Viability 2015, 24, 24–34. [Google Scholar] [CrossRef]
- Vileikyte, L.; Gonzalez, J.S.; Leventhal, H.; Peyrot, M.F.; Rubin, R.R.; Garrow, A.; Ulbrecht, J.S.; Cavanagh, P.R.; Boulton, A.J. Patient Interpretation of Neuropathy (PIN) questionnaire: An instrument for assessment of cognitive and emotional factors associated with foot self-care. Diabetes Care 2006, 29, 2617–2624. [Google Scholar] [CrossRef] [PubMed]
- Borges, W.J.; Ostwald, S.K. Improving foot self-care behaviors with Pies Sanos. West. J. Nurs. Res. 2008, 30, 325–349. [Google Scholar] [CrossRef] [PubMed]
- Bahador, R.S.; Afrazandeh, S.S.; Ghanbarzehi, N.; Ebrahimi, M. The impact of three-month training programme on foot care and self-efficacy of patients with diabetic foot ulcers. J. Clin. Diagn. Res. 2017, 11, IC01–IC04. [Google Scholar] [CrossRef] [PubMed]
- Chin, Y.F.; Liang, J.; Wang, W.S.; Hsu, B.R.; Huang, T.T. The role of foot self-care behavior on developing foot ulcers in diabetic patients with peripheral neuropathy: A prospective study. Int. J. Nurs. Stud. 2014, 51, 1568–1574. [Google Scholar] [CrossRef]
- Salameh, B.S.; Abdallah, J.; Naerat, E.O. Case-control study of risk factors and self-care behaviors of foot ulceration in diabetic patients attending primary healthcare services in Palestine. J. Diabetes Res. 2020, 2020, 7624267. [Google Scholar] [CrossRef]
- Ahmad Sharoni, S.K.; Mohd Razi, M.N.; Abdul Rashid, N.F.; Mahmood, Y.E. Self-efficacy of foot care behaviour of elderly patients with diabetes. Malays. Fam. Physician 2017, 12, 2–8. [Google Scholar]
- Şahin, S.; Cingil, D. Evaluation of the relationship among foot wound risk, foot self-care behaviors, and illness acceptance in patients with type 2 diabetes mellitus. Prim. Care Diabetes 2020, 14, 469–475. [Google Scholar] [CrossRef]
- Ahmad Sharoni, S.; Abdul Rahman, H.; Minhat, H.S.; Shariff Ghazali, S.; Azman Ong, M.H. A self-efficacy education programme on foot self-care behaviour among older patients with diabetes in a public long-term care institution, Malaysia: A quasi-experimental pilot study. BMJ Open 2017, 7, e014393. [Google Scholar] [CrossRef]
- Bell, R.A.; Arcury, T.A.; Snively, B.M.; Smith, S.L.; Stafford, J.M.; Dohanish, R.; Quandt, S.A. Diabetes foot self-care practices in a rural triethnic population. Diabetes Educ. 2005, 31, 75–83. [Google Scholar] [CrossRef]
- Rezende Neta, D.S.; da Silva, A.R.; da Silva, G.R. Adherence to foot self-care in diabetes mellitus patients. Rev. Bras. Enferm. 2015, 68, 103–116. [Google Scholar] [PubMed]
- Jordan, D.N.; Jordan, J.L. Foot self-care practices among Filipino American women with Type 2 Diabetes mellitus. Diabetes Ther. 2011, 2, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Dikeukwu, R.A.; Omole, O.B. Awareness and practices of foot self-care in patients with diabetes at Dr Yusuf Dadoo District Hospital, Johannesburg. J. Clin. Endocrinol. Metab. 2013, 18, 112–118. [Google Scholar] [CrossRef]
- Batista, I.B.; Pascoal, L.M.; Gontijo, P.; Brito, P.; Sousa, M.A.; Santos Neto, M.; Sousa, M.S. Association between knowledge and adherence to foot self-care practices performed by diabetics. Rev. Bras. Enferm. 2020, 73, e20190430. [Google Scholar] [CrossRef] [PubMed]
- Senussi, M.; Lincoln, N.; Jeffcoate, W. Psychometric properties of the Nottingham Assessment of Functional Footcare (NAFF). Int. J. Ther. Rehabil. 2011, 18, 330–334. [Google Scholar] [CrossRef]
- Wendling, S.; Beadle, V. The relationship between self-efficacy and diabetic foot self-care. J. Clin. Transl. Endocrinol. 2015, 2, 37–41. [Google Scholar] [CrossRef] [PubMed]
- Abdelhamid, F.M.; Taha, N.M.; Mohamed, E.H.; El-Khashab, M.N. Effect of self-management support program on improving diabetic foot care behaviors. Int. J. Pharm. Sci. Rev. Res. 2018, 7, 67–76. [Google Scholar]
- González-de la Torre, H.; Quintana-Lorenzo, M.L.; Lorenzo-Navarro, A.; Suárez-Sánchez, J.J.; Berenguer-Pérez, M.; Verdú-Soriano, J. Diabetic foot self-care and concordance of 3 diabetic foot risk stratification systems in a basic health area of Gran Canaria. Enferm. Clin. 2020, 30, 72–81. [Google Scholar] [CrossRef]
- Nguyen, T.; Edwards, H.; Do, T.; Finlayson, K. Effectiveness of a theory-based foot care education program (3STEPFUN) in improving foot self-care behaviours and foot risk factors for ulceration in people with type 2 diabetes. Diabetes Res. Clin. Pract. 2019, 152, 29–38. [Google Scholar] [CrossRef]
- Perrin, B.M.; Swerissen, H.; Payne, C. The association between foot-care self efficacy beliefs and actual foot-care behaviour in people with peripheral neuropathy: A cross-sectional study. J. Foot Ankle Res. 2009, 2, 3. [Google Scholar] [CrossRef]
- Gökdeniz, D.; Akgün Şahin, Z. Evaluation of knowledge levels about diabetes foot care and self-care activities in diabetic individuals. Int. J. Low. Extrem. Wounds 2022, 21, 65–74. [Google Scholar] [CrossRef] [PubMed]
- Terwee, C.B.; Prinsen, C.; Chiarotto, A.; Westerman, M.J.; Patrick, D.L.; Alonso, J.; Bouter, L.M.; de Vet, H.; Mokkink, L.B. COSMIN methodology for evaluating the content validity of patient-reported outcome measures: A Delphi study. Qual. Life Res. 2018, 27, 1159–1170. [Google Scholar] [CrossRef] [PubMed]
- Li, R.; Yuan, L.; Guo, X.-H.; Lou, Q.-Q.; Zhao, F.; Shen, L.; Zhang, M.-X.; Sun, Z.-L. The current status of foot self-care knowledge, behaviours, and analysis of influencing factors in patients with type 2 diabetes mellitus in China. Int. J. Nurs. Sci. 2014, 1, 266–271. [Google Scholar] [CrossRef]
- Al Sayah, F.; Soprovich, A.; Qiu, W.; Edwards, A.L.; Johnson, J.A. Diabetic foot disease, Self-care and clinical monitoring in adults with Type 2 Diabetes: The Alberta's Caring for Diabetes (ABCD) cohort study. Can. J. Diabetes 2015, 39, S120–S126. [Google Scholar] [CrossRef] [PubMed]
- Magbanua, E.; Lim-Alba, R. Knowledge and practice of diabetic foot care in patients with diabetes at Chinese General Hospital and Medical Center. J. ASEAN Fed. Endocr. Soc. 2017, 32, 123–131. [Google Scholar] [CrossRef]
- Kurup, R.; Ansari, A.A.; Singh, J.; Raja, A.V. Wound care knowledge, attitudes and practice among people with and without diabetes presenting with foot ulcers in Guyana. Diabet. Foot 2019, 22, 24–31. [Google Scholar]
- Perrin, B.M.; Swerissen, H.; Payne, C.B.; Skinner, T.C. Cognitive representations of peripheral neuropathy and self-reported foot-care behaviour of people at high risk of diabetes-related foot complications. Diabet. Med. 2014, 31, 102–106. [Google Scholar] [CrossRef]
- Bohorquez Robles, R.; Compeán Ortiz, L.G.; González Quirarte, N.H.; Berry, D.C.; Aguilera Pérez, P.; Piñones Martínez, S. Knowledge and Practices of Diabetes Foot Care and Risk of Developing Foot Ulcers in México May Have Implications for Patients of Méxican Heritage Living in the US. Diabetes Educ. 2017, 43, 297–303. [Google Scholar] [CrossRef]
- Sari, Y.; Upoyo, A.S.; Isworo, A.; Taufik, A.; Sumeru, A.; Anandari, D.; Sutrisna, E. Foot self-care behavior and its predictors in diabetic patients in Indonesia. BMC Res. Notes 2020, 13, 38. [Google Scholar] [CrossRef]
- Schmidt, S.; Mayer, H.; Panfil, E.M. Diabetes foot self-care practices in the German population. J. Clin. Nurs. 2008, 17, 2920–2926. [Google Scholar] [CrossRef]
- Ahmad Sharoni, S.K.; Abdul Rahman, H.; Minhat, H.S.; Shariff-Ghazali, S.; Azman Ong, M.H. The effects of self-efficacy enhancing program on foot self-care behaviour of older adults with diabetes: A randomised controlled trial in elderly care facility, Peninsular Malaysia. PLoS ONE 2018, 13, e0192417. [Google Scholar] [CrossRef] [PubMed]
- Stolt, M.; Suhonen, R.; Puukka, P.; Viitanen, M.; Voutilainen, P.; Leino-Kilpi, H. Foot health and self-care activities of older people in home care. J. Clin. Nurs. 2012, 21, 3082–3095. [Google Scholar] [CrossRef]
- Świątoniowska, N.; Chabowski, M.; Jankowska-Polańska, B. Quality of foot care among patients with diabetes: A study using a Polish version of the diabetes foot disease and foot care questionnaire. J. Foot Ankle Surg. 2020, 59, 231–238. [Google Scholar] [CrossRef] [PubMed]
- Thomas, S.M.; Nitin, I.G.; Reddy, M.U.K.; Devi, S.H. A prospective study: Knowledge assessment and patient care of diabetic foot ulcer patients in tertiary care hospital. Int. J. Pharm. Pharm. Sci. 2017, 9, 104–110. [Google Scholar] [CrossRef]
- Vatankhah, N.; Khamseh, M.E.; Noudeh, Y.J.; Aghili, R.; Baradaran, H.R.; Haeri, N.S. The effectiveness of foot care education on people with Type 2 Diabetes in Tehran, Iran. Prim. Care Diabetes 2009, 3, 73–77. [Google Scholar] [CrossRef] [PubMed]
- Kruger, S.; Guthrie, D. Foot care: Knowledge retention and self-care practices. Diabetes Educ. 1992, 18, 487–490. [Google Scholar] [CrossRef] [PubMed]
- Lael-Monfared, E.; Tehrani, H.; Moghaddam, Z.E.; Ferns, G.A.; Tatari, M.; Jafari, A. Health literacy, knowledge and self-care behaviors to take care of diabetic foot in low-income individuals: Application of extended parallel process model. Diabetes Metab. Syndr. 2019, 13, 1535–1541. [Google Scholar] [CrossRef]
- Corbett, C.F. A randomized pilot study of improving foot care in home health patients with diabetes. Diabetes Educ. 2003, 29, 273–282. [Google Scholar] [CrossRef]
- Fan, L.; Sidani, S.; Cooper-Brathwaite, A.; Metcalfe, K. Improving foot self-care knowledge, self-efficacy, and behaviors in patients with Type 2 Diabetes at low risk for foot ulceration: A pilot study. Clin. Nurs. Res. 2014, 23, 627–643. [Google Scholar] [CrossRef]
- Li, J.; Gu, L.; Guo, Y. An educational intervention on foot self-care behaviour among diabetic retinopathy patients with visual disability and their primary caregivers. J. Clin. Nurs. 2019, 28, 2506–2516. [Google Scholar] [CrossRef]
- Liang, R.; Dai, X.; Zuojie, L.; Zhou, A.; Meijuan, C. Two-year foot care program for minority patients with Type 2 Diabetes Mellitus of Zhuang Tribe in Guangxi, China. Can. J. Diabetes 2012, 36, 15–18. [Google Scholar] [CrossRef]
- Makiling, M.; Smart, H. Patient-centered health education intervention to empower preventive diabetic foot self-care. Adv. Skin Wound Care 2020, 33, 360–365. [Google Scholar] [CrossRef] [PubMed]
- Olson, J.M.; Hogan, M.T.; Pogach, L.M.; Rajan, M.; Raugi, G.J.; Reiber, G.E. Foot care education and self management behaviors in diverse veterans with diabetes. Patient Prefer. Adherence 2009, 3, 45–50. [Google Scholar] [CrossRef] [PubMed]
- Sable-Morita, S.; Arai, Y.; Takanashi, S.; Aimoto, K.; Okura, M.; Tanikawa, T.; Maeda, K.; Tokuda, H.; Arai, H. Development and Testing of the Foot Care Scale for Older Japanese Diabetic Patients. Int. J. Low. Extrem. Wounds 2021, 15347346211045033. [Google Scholar] [CrossRef] [PubMed]
- Hanley, G.; Chiou, P.Y.; Liu, C.Y.; Chen, H.M.; Pfeiffer, S. Foot care knowledge, attitudes and practices among patients with diabetic foot and amputation in St. Kitts and Nevis. Int. Wound J. 2020, 17, 1142–1152. [Google Scholar] [CrossRef] [PubMed]
- Ghasemi, Z.; Yousefi, H.; Torabikhah, M. The Effect of Peer Support on Foot Care in Patients with Type 2 Diabetes. Iran. J. Nurs. Midwifery Res. 2021, 26, 303–309. [Google Scholar]
- Rossaneis, M.A.; Haddad, M.; Mathias, T.A.; Marcon, S.S. Differences in foot self-care and lifestyle between men and women with diabetes mellitus. Rev. Lat. Am. Enfermagem. 2016, 24, e2761. [Google Scholar] [CrossRef]
- Bonner, T.; Guidry, J.; Jackson, Z. Association between foot care knowledge and practices among African Americans with Type 2 diabetes: An exploratory pilot study. J. Natl. Med. Assoc. 2019, 111, 256–261. [Google Scholar] [CrossRef]
- Madarshahian, F.; Hassanabadi, M.; Koshniat Nikoo, M. Cognitive status and foot self care practice in overweight diabetics, engaged in different levels of physical activity. J. Diabetes Metab. Disord. 2014, 13, 31. [Google Scholar] [CrossRef]
- Tuha, A.; Getie Faris, A.; Andualem, A.; Ahmed Mohammed, S. Knowledge and practice on diabetic foot self-care and associated factors among diabetic patients at Dessie Referral Hospital, Northeast Ethiopia: Mixed Method. Diabetes Metab. Syndr. Obes. 2021, 14, 1203–1214. [Google Scholar] [CrossRef]
- Qasim, M.; Rashid, M.U.; Islam, H.; Amjad, D.; Ehsan, S.B. Knowledge, attitude, and practice of diabetic patients regarding foot care: Experience from a single tertiary care outpatient clinic. Foot 2021, 49, 101843. [Google Scholar] [CrossRef] [PubMed]
- Ong, J.J.; Azmil, S.S.; Kang, C.S.; Lim, S.F.; Ooi, G.C.; Patel, A.; Mawardi, M. Foot care knowledge and self-care practices among diabetic patients in Penang: A primary care study. Med. J. Malays. 2022, 77, 224–231. [Google Scholar]
| Name of Instrument, Reference | Number of Items | Instrument Content | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Foot Inspection | Foot Wash | Foot Soaking | Drying the Feet | Skin Care | Skin Moisturization | Nail Cutting | Foot Warming | Footwear Assessment | Selection and Type of Footwear | Socks | Walking Barefoot | Attitude toward Foot Self-Care | ||
| Diabetes Foot Self-Care Behavior Scale (DFSBS) [30] | 7 | 2 | 1 | 1 | 1 | 2 | ||||||||
| Summary of Diabetes Self e Care Activities (SDSCA) [31] | 4 | 1 | 1 | 1 | 1 | |||||||||
| Nottingham Assessment of Functional Footcare (NAFF) [32] | 29 | 1 | 1 | 2 | 3 | 2 | 1 | 4 | 2 | 7 | 4 | 2 | ||
| Diabetic foot self-care questionnaire of the University of Malaga, Spain (DFSQ-UMA) [33] | 15 | 2 | 2 | 1 | 1 | 1 | 4 | 2 | 2 | |||||
| Foot Self-Care Behaviour (FSCB) questionnaire [34] | 17 | 1 | 1 | 2 | 1 | 1 | 2 | 1 | 4 | 2 | 2 | |||
| The Foot Self-Care Observation Guide (FSCOG) [35] | 16 | 3 | 1 | 1 | 3 | 1 | 1 | 2 | 1 | 3 | 1 | |||
| number of items/content | 10 | 4 | 1 | 7 | 9 | 5 | 4 | 7 | 8 | 16 | 11 | 5 | 2 | |
| Instrument | Origin of Items | Number of Participants | Validity | Reliability | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Content | Criterion | Construct I: in Relation to Other Tests | Construct II: Differentiates | Homogeneity | Intra-Rater | Test-Retest | Feasibility | Total Score | |||
| Diabetes foot self-care behavior scale (DFSBS) | |||||||||||
| Diabetes foot self-care behavior scale (DFSBS) [30] | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 0 | 0 | 2 | 16 |
| Use of DFSBS in Iran [36] | 2 | 2 | 2 | 0 | 0 | 0 | 2 | 0 | 0 | 0 | 8 |
| Use of DFSCBS in Taiwan [37] | 2 | 2 | 0 | 0 | 0 | 0 | 2 | 0 | 0 | 0 | 6 |
| Use of DFSBS in State of Palestine [38] | 2 | 2 | 2 | 0 | 0 | 0 | 2 | 0 | 2 | 0 | 10 |
| Use of DFSBS in Malaysia [39] | 2 | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 6 |
| Use of DFSBS in Turkey [40] | 2 | 2 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 5 |
| Use of DFSBS in Malaysia [41] | 2 | 2 | 2 | 0 | 0 | 0 | 1 | 0 | 0 | 2 | 9 |
| The Summary of Diabetes Self-Care Activities (SDSCA): foot care | |||||||||||
| Use of SDSCA in United States [42] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| Use of SDSCA in Tanzania [12] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| Use of SDSCA in Brazil [43] | 0 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 2 |
| Use of SDSCA in Filippines [44] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| Use of SDSCA in South Africa [45] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 2 | 6 |
| The Diabetes Self-Care Activities Questionnaire (DSQ) [46] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| Nottingham Assessment of Functional Foot-Care questionnaire (NAFF) | |||||||||||
| The Nottingham Assessment of Functional Footcare, original study [32] | 2 | 2 | 0 | 0 | 0 | 2 | 1 | 0 | 2 | 2 | 11 |
| The use of NAFF in United Kingdom [47] | 2 | 2 | 0 | 0 | 0 | 2 | 1 | 0 | 2 | 0 | 9 |
| The use of NAFF in United Kingdom [48] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| The use of NAFF in United Kingdom [49] | 2 | 2 | 2 | 0 | 0 | 0 | 2 | 0 | 0 | 0 | 8 |
| Diabetic foot self-care questionnaire of the University of Malaga, Spain (DFSQ-UMA) | |||||||||||
| Diabetic foot self-care questionnaire of the University of Malaga, Spain (DFSQ-UMA) [33] | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 0 | 2 | 2 | 18 |
| The use of DFSQ-UMA in Spain [50] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| Foot Self-Care Behaviour (FSCB) questionnaire | |||||||||||
| The use of FSCB in Australia [51] | 2 | 2 | 2 | 0 | 0 | 0 | 2 | 0 | 0 | 0 | 8 |
| The use of FSCB in Australia [52] | 2 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 4 |
| The Foot Self-Care Observation Guide | |||||||||||
| Original study [35] | 2 | 2 | 1 | 0 | 0 | 0 | 1 | 0 | 2 | 2 | 10 |
| Gökdeniz & Sahin 2020 [53] | 2 | 2 | 0 | 0 | 0 | 0 | 2 | 0 | 0 | 0 | 6 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sipilä, J.; Mäkelä, A.-M.; Hyytiä, S.; Stolt, M. How to Measure Foot Self-Care? A Methodological Review of Instruments. J. Pers. Med. 2023, 13, 434. https://doi.org/10.3390/jpm13030434
Sipilä J, Mäkelä A-M, Hyytiä S, Stolt M. How to Measure Foot Self-Care? A Methodological Review of Instruments. Journal of Personalized Medicine. 2023; 13(3):434. https://doi.org/10.3390/jpm13030434
Chicago/Turabian StyleSipilä, Jenni, Anne-Marie Mäkelä, Sasu Hyytiä, and Minna Stolt. 2023. "How to Measure Foot Self-Care? A Methodological Review of Instruments" Journal of Personalized Medicine 13, no. 3: 434. https://doi.org/10.3390/jpm13030434
APA StyleSipilä, J., Mäkelä, A.-M., Hyytiä, S., & Stolt, M. (2023). How to Measure Foot Self-Care? A Methodological Review of Instruments. Journal of Personalized Medicine, 13(3), 434. https://doi.org/10.3390/jpm13030434








