Adherence to Long-Acting Inhaler Use for Initial Treatment and Acute Exacerbation of Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Dataset and Study Population
2.2. Medication Adherence and Comorbidities
2.3. Outcome Variables
2.4. Statistical Analyses
3. Results
3.1. Study Population Baseline Characteristics according to Medication Adherence
3.2. Differences in Clinical Characteristics and Adherence to Long-Acting Inhalers according to COPD Exacerbation Incidence
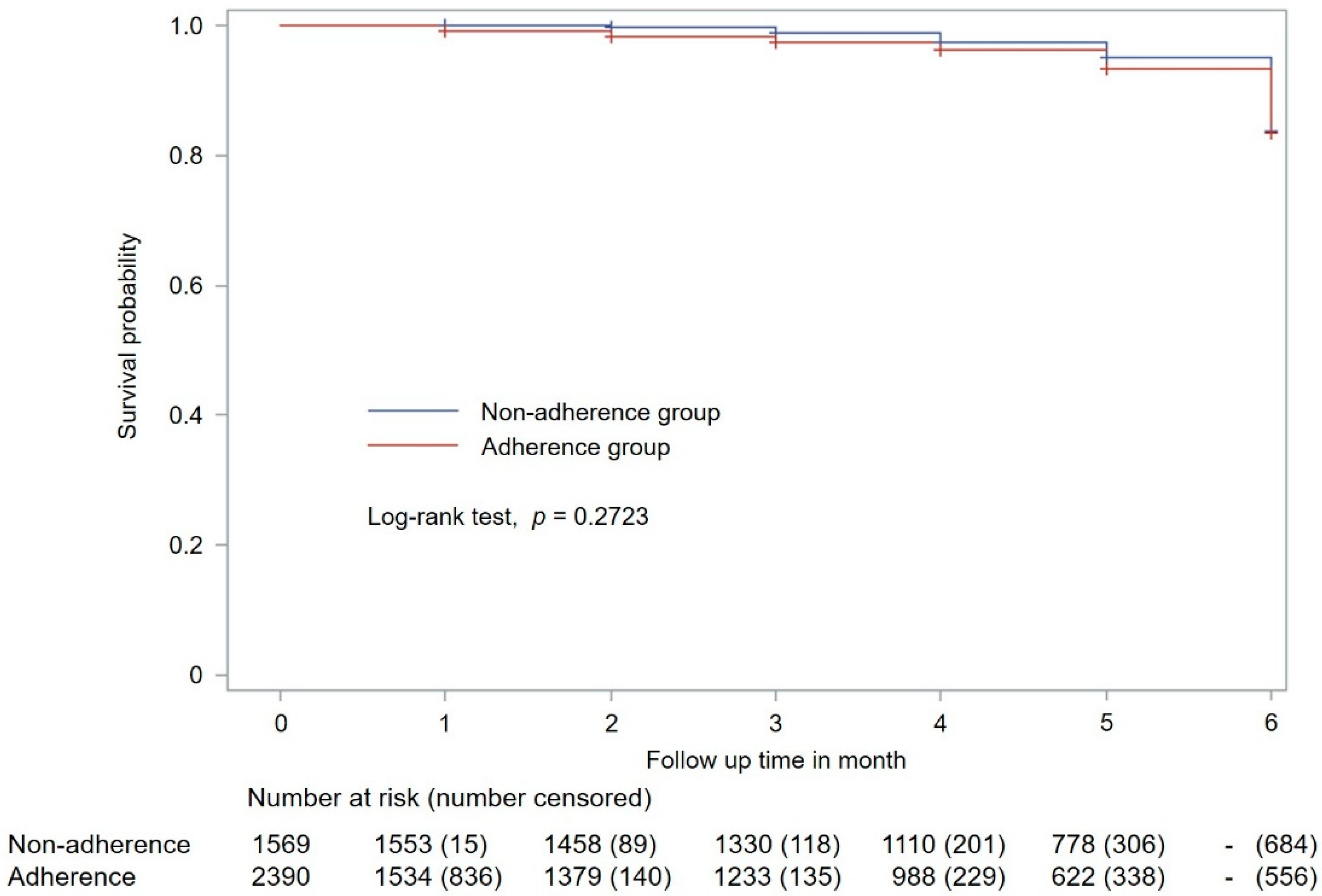
3.3. Impact of Medication Adherence to Long-Acting Inhalers on COPD Exacerbation
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Singh, D.; Agusti, A.; Anzueto, A.; Barnes, P.J.; Bourbeau, J.; Celli, B.R.; Criner, G.J.; Frith, P.; Halpin, D.M.G.; Han, M.; et al. Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Lung Disease: The Gold Science Committee Report 2019. Eur. Respir. J. 2019, 53, 1900164. [Google Scholar] [CrossRef] [PubMed]
- Rolnick, S.J.; Pawloski, P.A.; Hedblom, B.D.; Asche, S.E.; Bruzek, R.J. Patient Characteristics Associated With Medication Adherence. Clin. Med. Res. 2013, 11, 54–65. [Google Scholar] [CrossRef] [PubMed]
- Vestbo, J.; Anderson, J.A.; Calverley, P.M.; Celli, B.; Ferguson, G.T.; Jenkins, C.; Knobil, K.; Willits, L.R.; Yates, J.C.; Jones, P.W. Adherence to Inhaled Therapy, Mortality and Hospital Admission in COPD. Thorax 2009, 64, 939–943. [Google Scholar] [CrossRef] [PubMed]
- Restrepo, R.D.; Alvarez, M.T.; Wittnebel, L.D.; Sorenson, H.; Wettstein, R.; Vines, D.L.; Sikkema-Ortiz, J.; Gardner, D.D.; Wilkins, R.L. Medication Adherence Issues in Patients Treated for COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 2008, 3, 371–384. [Google Scholar] [CrossRef] [PubMed]
- Toy, E.L.; Beaulieu, N.U.; McHale, J.M.; Welland, T.R.; Plauschinat, C.A.; Swensen, A.; Duh, M.S. Treatment of COPD: Relationships Between Daily Dosing Frequency, Adherence, Resource Use, and Costs. Respir. Med. 2011, 105, 435–441. [Google Scholar] [CrossRef]
- Vogelmeier, C.F.; Criner, G.J.; Martinez, F.J.; Anzueto, A.; Barnes, P.J.; Bourbeau, J.; Celli, B.R.; Chen, R.; Decramer, M.; Fabbri, L.M.; et al. Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Lung Disease 2017 Report. Gold Executive Summary. Am. J. Respir. Crit. Care Med. 2017, 195, 557–582. [Google Scholar] [CrossRef]
- Krigsman, K.; Moen, J.; Nilsson, J.L.; Ring, L. Refill Adherence by the Elderly for Asthma/Chronic Obstructive Pulmonary Disease Drugs Dispensed Over a 10-Year Period. J. Clin. Pharm. Ther. 2007, 32, 603–611. [Google Scholar] [CrossRef]
- Kim, J.A.; Lim, M.K.; Kim, K.; Park, J.; Rhee, C.K. Adherence to Inhaled Medications and Its Effect on Healthcare Utilization and Costs Among High-Grade Chronic Obstructive Pulmonary Disease Patients. Clin. Drug Investig. 2018, 38, 333–340. [Google Scholar] [CrossRef]
- Cushen, B.; Sulaiman, I.; Greene, G.; MacHale, E.; Mokoka, M.; Reilly, R.B.; Bennett, K.; Doyle, F.; van Boven, J.F.M.; Costello, R.W. The Clinical Impact of Different Adherence Behaviors in Patients With Severe Chronic Obstructive Pulmonary Disease. Am. J. Respir. Crit. Care Med. 2018, 197, 1630–1633. [Google Scholar] [CrossRef]
- Montes de Oca, M.; Menezes, A.; Wehrmeister, F.C.; Lopez Varela, M.V.; Casas, A.; Ugalde, L.; Ramirez-Venegas, A.; Mendoza, L.; López, A.; Surmont, F.; et al. Adherence to Inhaled Therapies of COPD Patients From Seven Latin American Countries: The LASSYC Study. PLoS ONE 2017, 12, e0186777. [Google Scholar] [CrossRef]
- Simoni-Wastila, L.; Wei, Y.J.; Qian, J.; Zuckerman, I.H.; Stuart, B.; Shaffer, T.; Dalal, A.A.; Bryant-Comstock, L. Association of Chronic Obstructive Pulmonary Disease Maintenance Medication Adherence With All-Cause Hospitalization and Spending in a Medicare Population. Am. J. Geriatr. Pharmacother. 2012, 10, 201–210. [Google Scholar] [CrossRef]
- Kim, J.; Rhee, C.K.; Yoo, K.H.; Kim, Y.S.; Lee, S.W.; Park, Y.B.; Lee, J.H.; Oh, Y.; Lee, S.D.; Kim, Y.; et al. The Health Care Burden of High Grade Chronic Obstructive Pulmonary Disease in Korea: Analysis of the Korean Health Insurance Review and Assessment Service Data. Int. J. Chron. Obstruct. Pulmon. Dis. 2013, 8, 561–568. [Google Scholar] [CrossRef]
- Kim, C.; Yoo, K.H.; Rhee, C.K.; Yoon, H.K.; Kim, Y.S.; Lee, S.W.; Oh, Y.M.; Lee, S.D.; Lee, J.H.; Kim, K.J.; et al. Health Care Use and Economic Burden of Patients With Diagnosed Chronic Obstructive Pulmonary Disease in Korea. Int. J. Tuberc. Lung Dis. 2014, 18, 737–743. [Google Scholar] [CrossRef]
- Van Boven, J.F.; Chavannes, N.H.; van der Molen, T.; Rutten-van Mölken, M.P.; Postma, M.J.; Vegter, S. Clinical and Economic Impact of Non-adherence in COPD: A Systematic Review. Respir. Med. 2014, 108, 103–113. [Google Scholar] [CrossRef]
- Mueller, S.; Wilke, T.; Bechtel, B.; Punekar, Y.S.; Mitzner, K.; Virchow, J.C. Non-persistence and Non-adherence to Long-Acting COPD Medication Therapy: A Retrospective Cohort Study Based on a Large German Claims Dataset. Respir. Med. 2017, 122, 1–11. [Google Scholar] [CrossRef]
- Punekar, Y.S.; Landis, S.H.; Wurst, K.; Le, H. Characteristics, Disease Burden and Costs of COPD Patients in the Two Years Following Initiation of Long-Acting Bronchodilators in UK Primary Care. Respir. Res. 2015, 16, 141. [Google Scholar] [CrossRef]
- Chen, R.; Gao, Y.; Wang, H.; Shang, H.; Xuan, J. Association Between Adherence to Maintenance Medication in Patients With COPD and Acute Exacerbation Occurrence and Cost in China: A Retrospective Cohort Database Study. Int. J. Chron. Obstruct. Pulmon. Dis. 2020, 15, 963–971. [Google Scholar] [CrossRef]
- Hurst, J.R.; Vestbo, J.; Anzueto, A.; Locantore, N.; Müllerova, H.; Tal-Singer, R.; Miller, B.; Lomas, D.A.; Agusti, A.; Macnee, W.; et al. Susceptibility to Exacerbation in Chronic Obstructive Pulmonary Disease. N. Engl. J. Med. 2010, 363, 1128–1138. [Google Scholar] [CrossRef]
- Han, M.K.; Quibrera, P.M.; Carretta, E.E.; Barr, R.G.; Bleecker, E.R.; Bowler, R.P.; Cooper, C.B.; Comellas, A.; Couper, D.J.; Curtis, J.L.; et al. Frequency of Exacerbations in Patients With Chronic Obstructive Pulmonary Disease: An Analysis of the SPIROMICS Cohort. Lancet Respir. Med. 2017, 5, 619–626. [Google Scholar] [CrossRef]
- Ierodiakonou, D.; Sifaki-Pistolla, D.; Kampouraki, M.; Poulorinakis, I.; Papadokostakis, P.; Gialamas, I.; Athanasiou, P.; Bempi, V.; Lampraki, I.; Tsiligianni, I.; et al. Adherence to Inhalers and Comorbidities in COPD Patients. A Cross-Sectional Primary Care Study From Greece. BMC Pulm. Med. 2020, 20, 253. [Google Scholar] [CrossRef]
- Zhang, S.; King, D.; Rosen, V.M.; Ismaila, A.S. Impact of Single Combination Inhaler Versus Multiple Inhalers to Deliver the Same Medications for Patients With Asthma or COPD: A Systematic Literature Review. Int. J. Chron. Obstruct. Pulmon. Dis. 2020, 15, 417–438. [Google Scholar] [CrossRef] [PubMed]
- Humenberger, M.; Horner, A.; Labek, A.; Kaiser, B.; Frechinger, R.; Brock, C.; Lichtenberger, P.; Lamprecht, B. Adherence to Inhaled Therapy and Its Impact on Chronic Obstructive Pulmonary Disease (COPD). BMC Pulm. Med. 2018, 18, 163. [Google Scholar] [CrossRef] [PubMed]
- Deniz, S.; Şengül, A.; Aydemir, Y.; Çeldir Emre, J.; Özhan, M.H. Clinical Factors and Comorbidities Affecting the Cost of Hospital-Treated COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 2016, 11, 3023–3030. [Google Scholar] [CrossRef] [PubMed]
- Dong, H.; Hao, Y.; Li, D.; Su, Z.; Li, W.; Shi, B.; Gao, P. Risk Factors for Acute Exacerbation of Chronic Obstructive Pulmonary Disease in Industrial Regions of China: A Multicenter Cross-Sectional Study. Int. J. Chron. Obstruct. Pulmon. Dis. 2020, 15, 2249–2256. [Google Scholar] [CrossRef]
- Divo, M.; Cote, C.; de Torres, J.P.; Casanova, C.; Marin, J.M.; Pinto-Plata, V.; Zulueta, J.; Cabrera, C.; Zagaceta, J.; Hunninghake, G.; et al. Comorbidities and Risk of Mortality in Patients With Chronic Obstructive Pulmonary Disease. Am. J. Respir. Crit. Care Med. 2012, 186, 155–161. [Google Scholar] [CrossRef]
- Ngo, C.Q.; Phan, D.M.; Vu, G.V.; Dao, P.N.; Phan, P.T.; Chu, H.T.; Nguyen, L.H.; Vu, G.T.; Ha, G.H.; Tran, T.H.; et al. Inhaler Technique and Adherence to Inhaled Medications among Patients with Acute Exacerbation of Chronic Obstructive Pulmonary Disease in Vietnam. Int. J. Environ. Res. Public Health. 2019, 16, 185. [Google Scholar] [CrossRef]
- Gregoriano, C.; Dieterle, T.; Breitenstein, A.L.; Dürr, S.; Baum, A.; Giezendanner, S.; Maier, S.; Leuppi-Taegtmeyer, A.; Arnet, I.; Hersberger, K.E.; et al. Does a Tailored Intervention to Promote Adherence in Patients With Chronic Lung Disease Affect Exacerbations? A Randomized Controlled Trial. Respir. Res. 2019, 20, 273. [Google Scholar] [CrossRef]

| Characteristics | All Patients (n = 3959) | MPR ≥ 80% (n = 2390) | MPR < 80% (n = 1569) | p-Value |
|---|---|---|---|---|
| Sex | 0.0025 | |||
| Women | 925 (23.4) | 519 (21.7) | 406 (25.9) | |
| Men | 3034 (76.6) | 1871 (78.3) | 1163 (74.1) | |
| Age, years | 0.0003 | |||
| 40–49 | 111 (2.8) | 78 (3.3) | 33 (2.1) | |
| 50–59 | 457 (11.5) | 284 (11.9) | 173 (11.0) | |
| 60–69 | 1093 (27.6) | 706 (29.6) | 387 (24.7) | |
| 70–79 | 1598 (40.4) | 918 (38.4) | 680 (43.3) | |
| 80 or more | 700 (17.7) | 404 (16.9) | 296 (18.9) | |
| Type of coverage | 0.5307 | |||
| Health insurance | 3449 (87.1) | 2093 (87.6) | 1356 (86.4) | |
| Medical care | 502 (12.7) | 292 (12.2) | 210 (13.4) | |
| Veteran welfare | 8 (0.2) | 5 (0.2) | 3 (0.2) | |
| Number of outpatient clinics used | 0.9219 | |||
| 1 | 3007 (76.0) | 1814 (75.9) | 1193 (76.0) | |
| 2 | 952 (24.0) | 576 (24.1) | 376 (24.0) | |
| Number of comorbid diseases | 0.4360 | |||
| 0 | 2171 (54.8) | 1333 (55.8) | 838 (53.4) | |
| 1 | 1196 (30.2) | 706 (29.5) | 490 (31.2) | |
| 2 | 476 (12.0) | 283 (11.8) | 193 (12.3) | |
| 3 | 104 (2.6) | 63 (2.6) | 41 (2.6) | |
| 4 | 12 (0.3) | 5 (0.2) | 7 (0.5) | |
| Number of inhalers used | <0.0001 | |||
| 1 | 3239 (81.8) | 1909 (79.9) | 1330 (84.8) | |
| 2 or more | 720 (18.2) | 481 (20.1) | 239 (15.2) | |
| Acute exacerbation | <0.0001 | |||
| Incident | 312 (7.9) | 156 (6.5) | 156 (9.9) | |
| Non-incident | 3647 (92.1) | 2234 (93.5) | 1413 (90.1) |
| Characteristics | Acute Exacerbation of COPD | p-Value | |
|---|---|---|---|
| Presence (n = 312) | Absence (n = 3647) | ||
| Sex | 0.0084 | ||
| Women | 54 (17.3) | 871 (23.9) | |
| Men | 258 (82.7) | 2776 (76.1) | |
| Age, years | <0.0001 | ||
| 40–49 | 1 (0.3) | 110 (3.0) | |
| 50–59 | 25 (8.0) | 432 (11.9) | |
| 60–69 | 61 (19.6) | 1032 (28.3) | |
| 70–79 | 144 (46.2) | 1454 (39.9) | |
| 80 or more | 81 (26.0) | 619 (17.0) | |
| Type of coverage | 0.4520 | ||
| Health insurance | 267 (85.6) | 3182 (87.3) | |
| Medical care | 45 (14.4) | 457 (12.5) | |
| Veteran welfare | 0 (0.0) | 8 (0.2) | |
| Number of outpatient clinics used | <0.0001 | ||
| 1 | 194 (62.2) | 2813 (77.1) | |
| 2 or more | 118 (37.8) | 834 (22.9) | |
| Number of comorbid diseases | <0.0001 | ||
| 0 | 130 (41.7) | 2041 (56.0) | |
| 1 | 95 (30.5) | 1101 (30.2) | |
| 2 | 60 (19.2) | 416 (11.4) | |
| 3 | 24 (7.7) | 80 (2.2) | |
| 4 | 3 (1.0) | 9 (0.3) | |
| Number of inhalers used | <0.0001 | ||
| 1 | 207 (66.4) | 3032 (83.1) | |
| 2 or more | 105 (33.7) | 615 (16.9) | |
| Medication adherence | <0.0001 | ||
| MPR ≥ 80% | 156 (50.0) | 2234 (61.3) | |
| MPR < 80% | 156 (50.0) | 1413 (38.7) | |
| Variables | Number (%) | Univariable Analysis | p-Value | |
|---|---|---|---|---|
| Odds Ratio | 95% CI | |||
| Medication adherence | <0.0001 | |||
| MPR ≥ 80% | 2390 (60.4) | 1 | ||
| MPR < 80% | 1569 (39.6) | 1.58 | 1.25–1.99 | |
| Sex | 0.009 | |||
| Women | 925 (23.4) | 1 | ||
| Men | 3034 (76.6) | 1.50 | 1.11–2.03 | |
| Age, years | <0.0001 | |||
| 40–49 | 111 (2.8) | 1 | ||
| 50–59 | 457 (11.5) | 6.37 | 0.85–47.50 | |
| 60–69 | 1093 (27.6) | 6.50 | 0.89–47.36 | |
| 70–79 | 1598 (40.4) | 10.89 | 1.51–78.61 | |
| 80 or more | 700 (17.7) | 14.39 | 1.98–104.51 | |
| Number of comorbid diseases | <0.0001 | |||
| 0 | 2171 (54.8) | 1 | ||
| 1 | 1196 (30.2) | 1.35 | 1.03–1.78 | |
| 2 | 476 (12.0) | 2.26 | 1.64–3.13 | |
| 3 | 104 (2.6) | 4.71 | 2.89–7.68 | |
| 4 | 12 (0.3) | 5.23 | 1.40–19.56 | |
| Number of inhalers used | <0.0001 | |||
| 1 | 3239 (81.8) | 1 | ||
| 2 or more | 720 (18.2) | 2.50 | 1.95–3.21 | |
| Model 1 | Model 2 | Model 3 | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| Medication Adherence | ||||||
| MPR ≥ 80% | 1 | 1 | 1 | |||
| MPR < 80% | 1.55 | 1.22–1.95 | 1.57 | 1.24–1.99 | 1.68 | 1.33–2.14 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Suh, H.-S.; Chang, M.-S.; Yu, I.; Park, S.; Lee, J.-H.; Lee, S.J.; Lee, W.-Y.; Yong, S.J.; Kim, S.-H. Adherence to Long-Acting Inhaler Use for Initial Treatment and Acute Exacerbation of Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study. J. Pers. Med. 2022, 12, 2073. https://doi.org/10.3390/jpm12122073
Suh H-S, Chang M-S, Yu I, Park S, Lee J-H, Lee SJ, Lee W-Y, Yong SJ, Kim S-H. Adherence to Long-Acting Inhaler Use for Initial Treatment and Acute Exacerbation of Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study. Journal of Personalized Medicine. 2022; 12(12):2073. https://doi.org/10.3390/jpm12122073
Chicago/Turabian StyleSuh, Hee-Sook, Min-Seok Chang, Iseul Yu, Sunmin Park, Ji-Ho Lee, Seok Jeong Lee, Won-Yeon Lee, Suk Joong Yong, and Sang-Ha Kim. 2022. "Adherence to Long-Acting Inhaler Use for Initial Treatment and Acute Exacerbation of Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study" Journal of Personalized Medicine 12, no. 12: 2073. https://doi.org/10.3390/jpm12122073
APA StyleSuh, H.-S., Chang, M.-S., Yu, I., Park, S., Lee, J.-H., Lee, S. J., Lee, W.-Y., Yong, S. J., & Kim, S.-H. (2022). Adherence to Long-Acting Inhaler Use for Initial Treatment and Acute Exacerbation of Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study. Journal of Personalized Medicine, 12(12), 2073. https://doi.org/10.3390/jpm12122073







