Prevalence and Characteristics of Psoriasis in Romania—First Study in Overall Population
Abstract
1. Introduction
2. Objectives
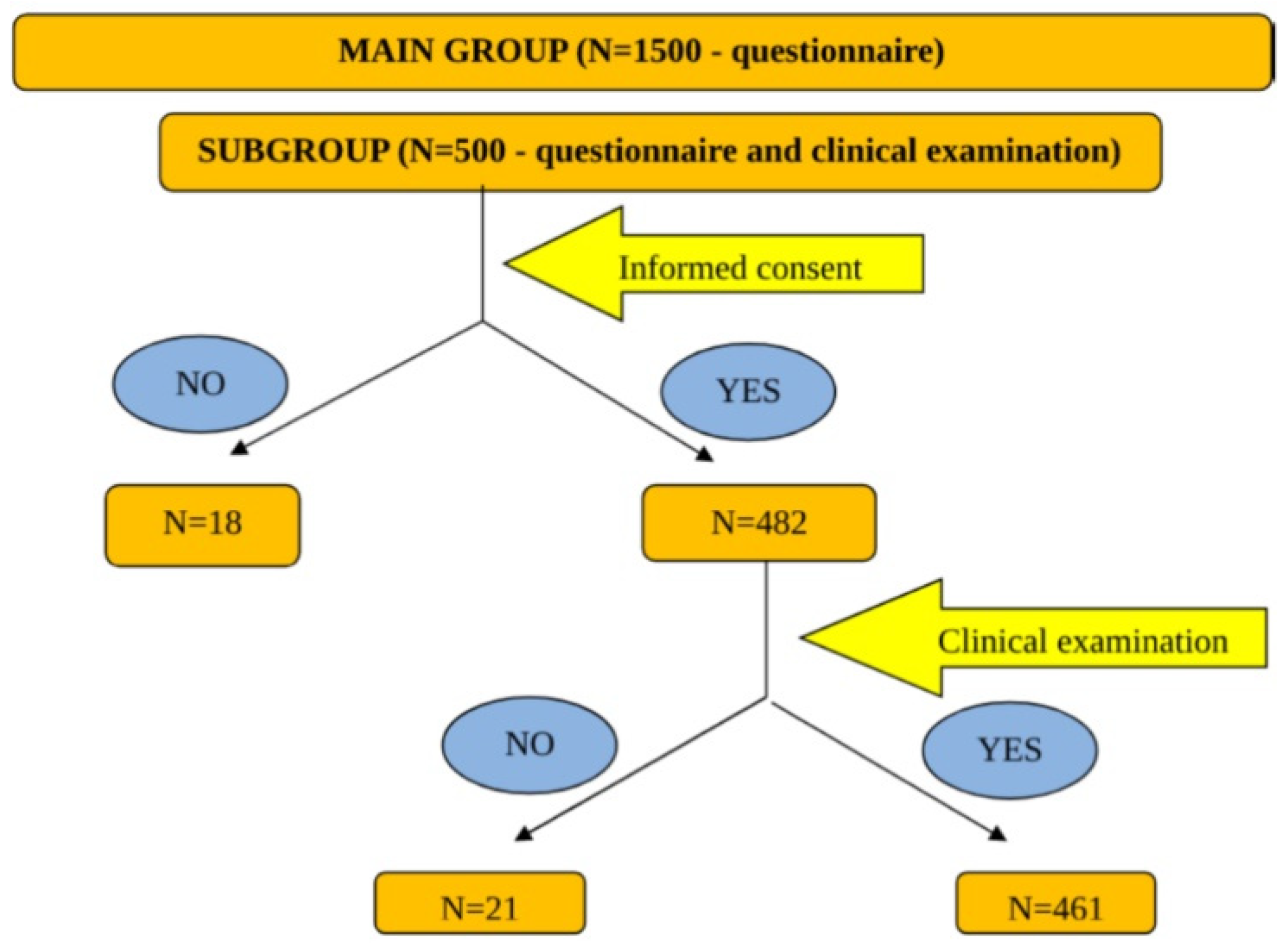
3. Materials and Methods
4. Results
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Fernández-Armenteros, J.M.; Gómez-Arbonés, X.; Buti-Solé, M.; Betriu-Bars, A.; Sanmartin-Novell, V.; Ortega-Bravo, M.; Martínez-Alonso, M.; Casanova-Seuma, J.M. Epidemiology of Psoriasis. A Population-Based Study. Actas Dermo-Sifiliogr. 2019, 110, 385–392. [Google Scholar] [CrossRef] [PubMed]
- Rapp, S.R.; Feldman, S.R.; Exum, M.; Fleischer, A.B.; Reboussin, D.M. Psoriasis causes as much disability as other major medical diseases. J. Am. Acad. Dermatol. 1999, 41, 401–407. [Google Scholar] [CrossRef]
- Plunkett, A.; Marks, R. A review of the epidemiology of psoriasis vulgaris in the community. Australas. J. Dermatol. 1998, 39, 225–232. [Google Scholar] [CrossRef]
- International Federation of Psoriasis Associations. World Psoriasis Day. Available online: https://ifpa-pso.com/our-actions/world-psoriasis-day (accessed on 6 May 2021).
- Ocampo D, V.; Gladman, D. Psoriatic arthritis. F1000Research 2019, 8, 1665. [Google Scholar] [CrossRef]
- Dinu, A.; Bucur, S.; Olteanu, R.; Constantin, T.; Raducan, A.; Baetu, M.; Constantin, M. Psoriatic arthritis: A permanent new challenge for dermatologists (Review). Exp. Ther. Med. 2019, 20, 47–51. [Google Scholar] [CrossRef] [PubMed]
- Barrea, L.; Nappi, F.; Di Somma, C.; Savanelli, M.C.; Falco, A.; Balato, A.; Balato, N.; Savastano, S. Environmental Risk Factors in Psoriasis: The Point of View of the Nutritionist. Int. J. Environ. Res. Public Health 2016, 13, 743. [Google Scholar] [CrossRef] [PubMed]
- Barrea, L.; Megna, M.; Cacciapuoti, S.; Frias-Toral, E.; Fabbrocini, G.; Savastano, S.; Colao, A.; Muscogiuri, G. Very low-calorie ketogenic diet (VLCKD) in patients with psoriasis and obesity: An update for dermatologists and nutritionists. Crit. Rev. Food Sci. Nutr. 2020, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Barrea, L.; Muscogiuri, G.; Di Somma, C.; Annunziata, G.; Megna, M.; Falco, A.; Balato, A.; Colao, A.; Savastano, S. Coffee consumption, metabolic syndrome and clinical severity of psoriasis: Good or bad stuff? Arch. Toxicol. 2018, 92, 1831–1845. [Google Scholar] [CrossRef]
- Barrea, L.; Savanelli, M.C.; Di Somma, C.; Napolitano, M.; Megna, M.; Colao, A.; Savastano, S. Vitamin D and its role in psoriasis: An overview of the dermatologist and nutritionist. Rev. Endocr. Metab. Disord. 2017, 18, 195–205. [Google Scholar] [CrossRef] [PubMed]
- National Institute of Statistics. Tempo Online Statistics. Available online: http://statistici.insse.ro:8077/tempo-online/#/pages/tables/insse-table (accessed on 13 April 2020).
- Raychaudhuri, S.P.; Farber, E.M. The prevalence of psoriasis in the world. J. Eur. Acad. Dermatol. Venereol. 2001, 15, 16–17. [Google Scholar] [CrossRef] [PubMed]
- Schonmann, Y.; Ashcroft, D.M.; Iskandar, I.Y.K.; Parisi, R.; Sde-Or, S.; Comaneshter, D.; Batat, E.; Shani, M.; Vinker, S.; Griffiths, C.E.; et al. Incidence and prevalence of psoriasis in Israel between 2011 and 2017. J. Eur. Acad. Dermatol. Venereol. 2019, 33, 2075–2081. [Google Scholar] [CrossRef]
- Finzi, A.F.; Benelli, C. A clinical survey of psoriasis in Italy: 1st AISP report. Interdisciplinary Association for the Study of Psoriasis. J. Eur. Acad. Dermatol. Venereol. 1998, 10, 125–129. [Google Scholar] [CrossRef] [PubMed]
- Ferrandiz, C.; Bordas, X.; García-Patos, V.; Puig, S.; Pujol, R.M.; Smandia, A. Prevalence of psoriasis in Spain (Epiderma Project: Phase I). J. Eur. Acad. Dermatol. Venereol. 2001, 15, 20–23. [Google Scholar] [CrossRef]
- Elewski, B.; Alexis, A.F.; Lebwohl, M.; Gold, L.S.; Pariser, D.; Del Rosso, J.; Yosipovitch, G. Itch: An under-recognized problem in psoriasis. J. Eur. Acad. Dermatol. Venereol. 2019, 33, 1465–1476. [Google Scholar] [CrossRef] [PubMed]
- Koo, J.; Marangell, L.; Nakamura, M.; Armstrong, A.; Jeon, C.; Bhutani, T.; Wu, J. Depression and suicidality in psoriasis: Review of the literature including the cytokine theory of depression. J. Eur. Acad. Dermatol. Venereol. 2017, 31, 1999–2009. [Google Scholar] [CrossRef]
- Abramovits, W.; Stevenson, L.C. A comparison of biologic therapies for psoriasis. J. Am. Acad. Dermatol. 2004, 50, P142. [Google Scholar] [CrossRef]
- Olteanu, R.; Constantin, M.M.; Zota, A.; Dorobanțu, D.; Constantin, T.; Serban, E.D.; Bălănescu, P.; Mihele, D.; Solovastru, L. Original clinical experience and approach to treatment study with interleukine 12/23 inhibitor in moderate-to-severe psoriasis patients. Farmacia 2016, 64, 918–921. [Google Scholar]
- Constantin, M.M.; Cristea, C.M.; Taranu, T. Biosimilars in dermatology: The wind of change. Exp. Ther. Med. 2019, 18, 911–915. [Google Scholar]
- Olteanu, R.; Zota, A.; Constantin, M. Biosimilars: An Update on Clinical Trials (Review of Published and Ongoing Studies). Acta Dermatovenerol. Croat. ADC 2017, 25, 57–66. [Google Scholar]
- Dattola, A.; Silvestri, M.; Tamburi, F.; Amoruso, G.F.; Bennardo, L.; Nisticò, S.P. Emerging role of anti-IL23 in the treatment of psoriasis: When humanized is very promising. Dermatol. Ther. 2020, 33, e14504. [Google Scholar] [CrossRef] [PubMed]
- Iannone, L.F.; Bennardo, L.; Palleria, C.; Roberti, R.; De Sarro, C.; Naturale, M.D.; Dastoli, S.; Donato, L.; Manti, A.; Valenti, G.; et al. Safety profile of biologic drugs for psoriasis in clinical practice: An Italian prospective pharmacovigilance study. PLoS ONE 2020, 15, e0241575. [Google Scholar] [CrossRef] [PubMed]
- Raducan, A.; Bucur, S.; Caruntu, C.; Constantin, T.; Nita, I.E.; Manolache, N.; Constantin, M.-M. Therapeutic management with biological anti-TNF-α agent in severe psoriasis associated with chronic hepatitis B: A case report. Exp. Ther. Med. 2019, 18, 895–899. [Google Scholar] [CrossRef] [PubMed]
- Noe, M.H.; Grewal, S.K.; Shin, D.B.; Ogdie, A.; Takeshita, J.; Gelfand, J.M. Increased prevalence of HCV and hepatic decompensation in adults with psoriasis: A population-based study in the United Kingdom. J. Eur. Acad. Dermatol. Venereol. 2017, 31, 1674–1680. [Google Scholar] [CrossRef] [PubMed]
- Sondermann, W.; Deudjui, D.D.; Körber, A.; Slomiany, U.; Brinker, T.; Erbel, R.; Moebus, S. Psoriasis, cardiovascular risk factors and metabolic disorders: Sex-specific findings of a population-based study. J. Eur. Acad. Dermatol. Venereol. 2019, 34, 779–786. [Google Scholar] [CrossRef] [PubMed]
- Stewart, T.J.; Tong, W.; Whitfeld, M. The associations between psychological stress and psoriasis: A systematic review. Int. J. Dermatol. 2018, 57. [Google Scholar] [CrossRef] [PubMed]
| Criteria | No. | % | No. | % | p-Value * |
|---|---|---|---|---|---|
| Region | |||||
| Bucharest-Ilfov | 173 | 11.5% | 58 | 11.6% | |
| Center | 176 | 11.7% | 59 | 11.8% | |
| Northeast | 261 | 17.4% | 87 | 17.4% | |
| Northwest | 191 | 12.7% | 63 | 12.6% | |
| South | 220 | 14.7% | 73 | 14.6% | |
| Southeast | 193 | 12.9% | 64 | 12.8% | |
| Southwest | 146 | 9.7% | 50 | 10.0% | |
| West | 140 | 9.3% | 46 | 9.2% | |
| Total | 1500 | 100.0% | 500 | 100.0% | >0.99 |
| Environment | |||||
| Rural | 638 | 42.5% | 210 | 42.0% | |
| Urban | 862 | 57.5% | 290 | 58.0% | |
| Total | 1500 | 100.0% | 500 | 100.0% | 0.834 |
| Gender | |||||
| Men | 726 | 48.4% | 241 | 48.2% | |
| Women | 774 | 51.6% | 259 | 51.8% | |
| Total | 1500 | 100.0% | 500 | 100.0% | 0.938 |
| Age groups | |||||
| 18–29 | 264 | 17.6% | 92 | 18.4% | |
| 30–49 | 611 | 40.7% | 202 | 40.4% | |
| 50+ | 625 | 41.7% | 206 | 41.2% | |
| Total | 1500 | 100.0% | 500 | 100.0% | 0.921 |
| Education | |||||
| No studies | 2 | 0.1% | 1 | 0.2% | |
| Primary | 102 | 6.8% | 35 | 7.0% | |
| Secondary | 650 | 43.3% | 222 | 44.4% | |
| Tertiary | 746 | 49.7% | 242 | 48.4% | |
| Total | 1500 | 100.0% | 500 | 100.0% | 0.947 |
| Declared diagnostic history | |||||
| Yes | 63 | 4.2% | 21 | 4.2% | |
| No | 1437 | 95.8% | 479 | 95.8% | |
| Total | 1500 | 100.0% | 500 | 100.0% | >0.99 |
| Variable | No. | % | p-Value–Nonhealthy-Healthy |
|---|---|---|---|
| Region | |||
| Bucharest-Ilfov | 56 | 12% | 0.089 |
| Center | 40 | 9% | |
| Northeast | 87 | 19% | |
| Northwest | 55 | 12% | |
| South | 69 | 15% | |
| Southeast | 59 | 13% | |
| Southwest | 49 | 11% | |
| West | 46 | 10% | |
| Total | 461 | 100% | |
| Environment | |||
| Rural | 194 | 42% | 0.251 |
| Urban | 267 | 58% | |
| Total | 461 | 100% | |
| Gender | |||
| Men | 221 | 48% | 0.104 |
| Women | 240 | 52% | |
| Total | 461 | 100% | |
| Age groups | |||
| 18–29 | 81 | 18% | 0.188 |
| 30–49 | 189 | 41% | |
| 50+ | 191 | 41% | |
| Total | 461 | 100% | |
| Education | |||
| No studies | 1 | 0% | 0.76 |
| Primary | 34 | 7% | |
| Secondary | 201 | 44% | |
| Tertiary | 225 | 49% | |
| Total | 461 | 100% | |
| Monitored by a Doctor | Local Treatment | Family Member with Psoriasis | Skin Lesions 25% | Types of Lesions 26% | Characteristics of the Lesions | Nail Changes | |
|---|---|---|---|---|---|---|---|
| 47.9% | 44% | A form of psoriasis9% | Hands 48% | Elbows 19% | Erythema 82% | Disappear spontaneously 52% | Nail yellowing 19% |
| 75.8%— by a dermatologist | Only on lesions 88% | Psoriatic arthritis 2% | Feet 46% | Knees 17% | Pruritus 69% | Disappear and reappear depending on the local treatment 52% | Nail stains 19% |
| 15.2%—by a family doctor | Phototherapy 17% | Face 30% | Nails 15% | Scales 33% | In correlation with stress 39% | Onychomadesis/nail loss 6% | |
| 6.1%—other doctors | NSAIDs 13% | Back 25% | Genitals 13% | Pigmentation disorders 29% | Persistent without improvement 36% | ||
| Other 4% | Abdomen 24% | Ears 9% | Papules/Pustules18% | ||||
| Thorax 20% | All over the body 6% | Hemorrhagic areas 17% | |||||
| Scalp 19% | Other areas 6% | Other 8% | |||||
| Comorbidities and Related Conditions | |||||
|---|---|---|---|---|---|
| Arterial hypertension | 31% | Following a treatment 82% | |||
| Dyslipidemia | 22% | Following a treatment 42% | |||
| Diabetes mellitus | 10% | Following a treatment 85% | |||
| Depression/Anxiety | 10% | Following a treatment 45% | |||
| Infections | 30% pharyngitis and tonsillitis during childhood | 12% hospitalized for these diseases | |||
| Obesity | 17% yes, 3% from childhood | 1 out of 5 was diagnosed with obesity at some point in life | |||
| Stress, life style | 1 out of 3 cannot cope with the important things in life | 2 out of 5 sometimes feel that the difficulties have accumulated to such an extent that they can no longer control them | |||
| Alcohol | Never 23% | 1 time/month 36% | 2–4 times/month 29% | >4 times /month 12% | |
| Smoking | Average age of onset—20 years 45% | Currently smokers 51% | Average smoking period—15 years | Passive smoking 25% | Exposure to smoke during childhood 74% |
| Nonhealthy | Healthy | p-Value | |||
|---|---|---|---|---|---|
| Number | % | Number | % | ||
| Hereditary factors | |||||
| Relative with psoriasis | 17 | 70.8% | 32 | 7.3% | <0.001 |
| Skin and nail lesions | |||||
| Skin lesions | 8 | 33.3% | 118 | 27.0% | 0.54 |
| Nail lesions | 4 | 16.7% | 79 | 18.1% | 0.58 |
| Nail yellowing | 4 | 16.7% | 88 | 20.1% | 0.46 |
| Onychomadesis | 2 | 8.3% | 23 | 5.3% | 0.38 |
| Smoking | |||||
| Ever smoked for at least 2 years | 11 | 45.8% | 165 | 37.8% | 0.279 |
| Currently smoker | 3 | 12.5% | 82 | 18.8% | 0.248 |
| Former smoker | 8 | 33.3% | 80 | 18.3% | 0.179 |
| Exposure in the last 12 months | 0 | 0.0% | 92 | 21.1% | 0.004 |
| Exposure in childhood | 18 | 75.0% | 325 | 74.4% | 0.581 |
| Alcohol | |||||
| Alcohol consumption ever in the last year | 16 | 66.7% | 332 | 76.0% | 0.303 |
| Infections | |||||
| Pharyngitis/tonsillitis during childhood | 11 | 45.8% | 102 | 23.3% | 0.028 |
| Hospitalization | 6 | 25.0% | 57 | 13.0% | 0.009 |
| Obesity | |||||
| BMI > 25 | 18 | 75.0% | 224 | 51.3% | 0.216 |
| Ever been obese | 8 | 33.3% | 74 | 16.9% | 0.053 |
| Obesity during childhood | 0 | 0.0% | 18 | 4.1% | 0.375 |
| Arterial hypertension | 9 | 37.5% | 146 | 33.4% | 0.663 |
| Diabetes mellitus | 4 | 16.7% | 45 | 10.3% | 0.307 |
| Depression/Anxiety | 5 | 20.8% | 40 | 9.2% | 0.073 |
| Dyslipidemia | 10 | 41.7% | 115 | 26.3% | 0.104 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nicolescu, A.C.; Bucur, Ș.; Giurcăneanu, C.; Gheucă-Solovăstru, L.; Constantin, T.; Furtunescu, F.; Ancuța, I.; Constantin, M.M. Prevalence and Characteristics of Psoriasis in Romania—First Study in Overall Population. J. Pers. Med. 2021, 11, 523. https://doi.org/10.3390/jpm11060523
Nicolescu AC, Bucur Ș, Giurcăneanu C, Gheucă-Solovăstru L, Constantin T, Furtunescu F, Ancuța I, Constantin MM. Prevalence and Characteristics of Psoriasis in Romania—First Study in Overall Population. Journal of Personalized Medicine. 2021; 11(6):523. https://doi.org/10.3390/jpm11060523
Chicago/Turabian StyleNicolescu, Alin Codruț, Ștefana Bucur, Călin Giurcăneanu, Laura Gheucă-Solovăstru, Traian Constantin, Florentina Furtunescu, Ioan Ancuța, and Maria Magdalena Constantin. 2021. "Prevalence and Characteristics of Psoriasis in Romania—First Study in Overall Population" Journal of Personalized Medicine 11, no. 6: 523. https://doi.org/10.3390/jpm11060523
APA StyleNicolescu, A. C., Bucur, Ș., Giurcăneanu, C., Gheucă-Solovăstru, L., Constantin, T., Furtunescu, F., Ancuța, I., & Constantin, M. M. (2021). Prevalence and Characteristics of Psoriasis in Romania—First Study in Overall Population. Journal of Personalized Medicine, 11(6), 523. https://doi.org/10.3390/jpm11060523







