Figure 1.
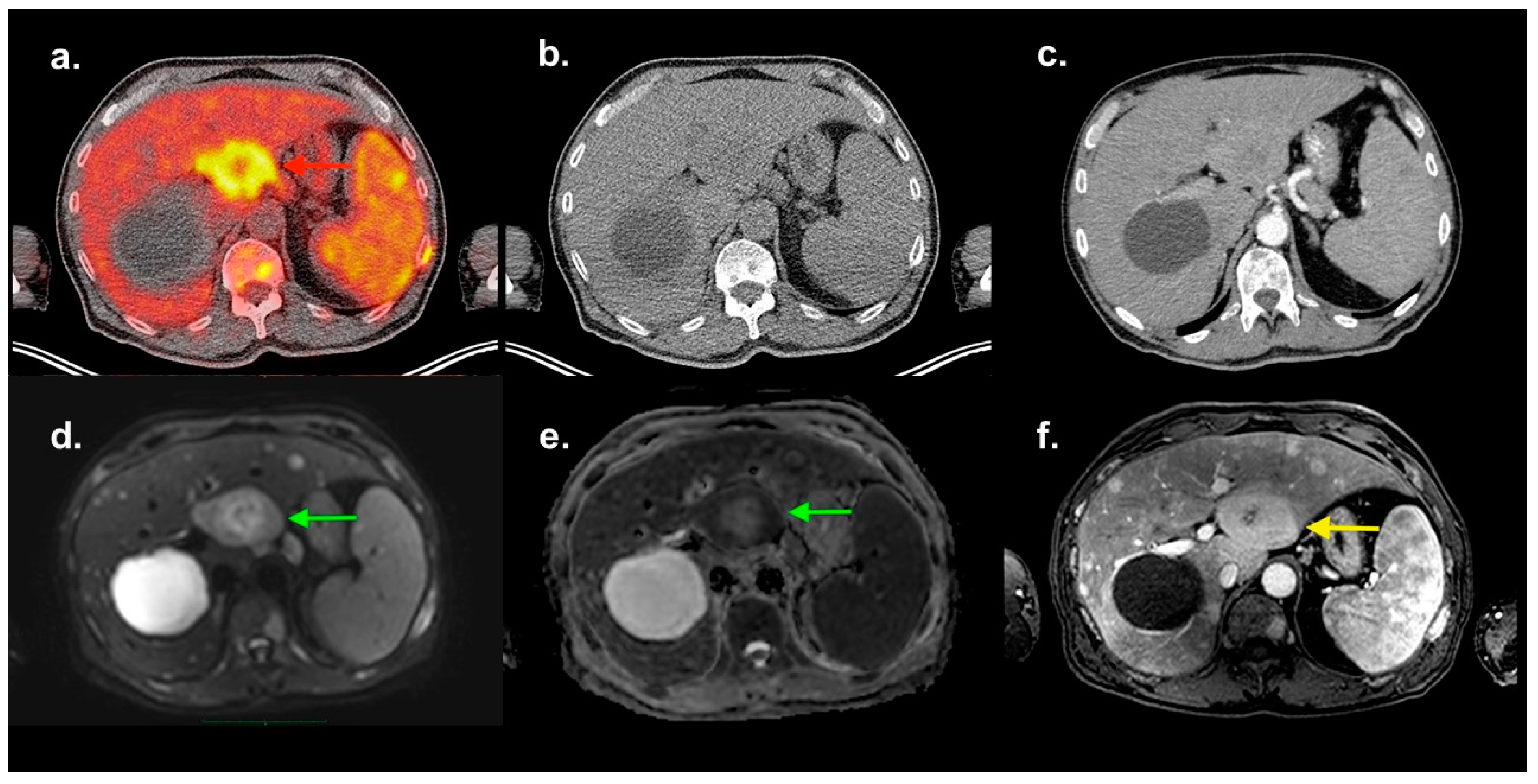
Newly diagnosed patient with multiple myeloma (MM, Typ IgA Kappa, Stage IIIA according to the Durie–Salmon staging system, ISS III), anemia and hepatosplenomegaly underwent an 18F-FDG PET/CT and a routine whole-body MRI investigation, as it is standard for all MM patients. The transaxial fused PET/CT image (
a) shows a circumscribed lesion in the IVb segment of the liver (red arrow) with an SUVmax of 10.1, a functional volume of approx. 90 ml and a hypometabolic center. At the same level, a cystic liver lesion of 9 cm in diameter is delineated (without FDG-uptake). The FDG-avid lesion is not distinguishable in the low-dose CT (
b). The contrast-enhanced diagnostic CT (
c) shows a contrast uptake in the arterial phase nearly similar to the liver parenchyma, and a hypodense core demarks itself as in the PET/CT-image. Diffusion-weighted (DW
d,
e) MRI demonstrates an inhomogeneous abnormal diffusion restriction in the same area (green arrows), which can be clearly distinguished, showing an intermediate T1-signal intensity and a hyperintense core (yellow arrow) in the contrast-enhanced MRI (
f). A biopsy of the lesion under sonographic control indicated plasma cell neoplasia. A diagnostic ultrasound of the liver was not performed before (no pre-described MM hepatic disease). The presence of extramedullary lesions at any time during the course of MM indicates a poor prognosis [
1], and these patients may need to follow additional treatment strategies [
2,
3].
Figure 1.
Newly diagnosed patient with multiple myeloma (MM, Typ IgA Kappa, Stage IIIA according to the Durie–Salmon staging system, ISS III), anemia and hepatosplenomegaly underwent an 18F-FDG PET/CT and a routine whole-body MRI investigation, as it is standard for all MM patients. The transaxial fused PET/CT image (
a) shows a circumscribed lesion in the IVb segment of the liver (red arrow) with an SUVmax of 10.1, a functional volume of approx. 90 ml and a hypometabolic center. At the same level, a cystic liver lesion of 9 cm in diameter is delineated (without FDG-uptake). The FDG-avid lesion is not distinguishable in the low-dose CT (
b). The contrast-enhanced diagnostic CT (
c) shows a contrast uptake in the arterial phase nearly similar to the liver parenchyma, and a hypodense core demarks itself as in the PET/CT-image. Diffusion-weighted (DW
d,
e) MRI demonstrates an inhomogeneous abnormal diffusion restriction in the same area (green arrows), which can be clearly distinguished, showing an intermediate T1-signal intensity and a hyperintense core (yellow arrow) in the contrast-enhanced MRI (
f). A biopsy of the lesion under sonographic control indicated plasma cell neoplasia. A diagnostic ultrasound of the liver was not performed before (no pre-described MM hepatic disease). The presence of extramedullary lesions at any time during the course of MM indicates a poor prognosis [
1], and these patients may need to follow additional treatment strategies [
2,
3].
![Diagnostics 09 00179 g001 Diagnostics 09 00179 g001]()
Figure 2.
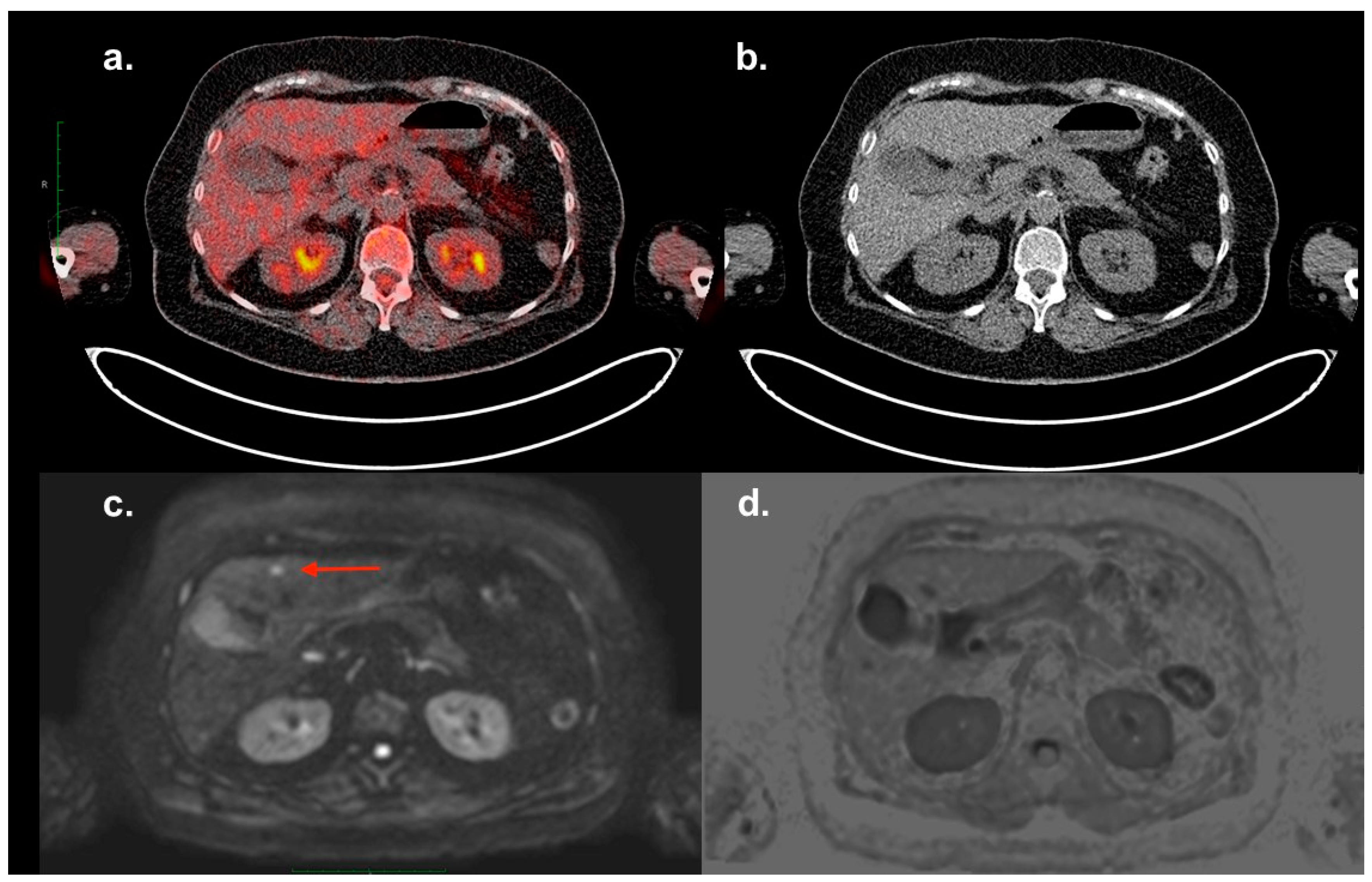
A patient with MM (Typ IgG lambda, Stage IA according to the Durie–Salmon staging system, ISS I) underwent an 18F-FDG PET/CT and a routine whole-body MRI investigation after radiation therapy of an extensive plasma cell infiltration in the sternum and three courses of induction therapy. No signs of further focal lesions were illustrated in previous CT and MRI investigations. A contrast-enhanced CT-scan was not performed in this case. The subsequent 18F-FDG PET/CT (
a,
b) did not demonstrate any focal lesion in the liver. A small lesion of 8 mm was delineated in Segment IVb, with an abnormal diffusion restriction in diffusion-weighted (DW,
c) MRI (red arrow). The same lesion could not be distinguished in the T1-VIBE or T2-weighted sequences (
d). A diagnostic ultrasound of the liver was not performed before (no pre-described hepatic disease), while the biopsy of the lesion under sonographic control indicated plasma cell neoplasia. Chen et al. reported a sensitivity of PET/CT nearly equivalent to that of MRI for the detection of extramedullary lesions; however, they added that in some areas, the use of both techniques could offer complementary information [
4]. It must be noted that small lesions with a subcentimeter size may not be detectable on 18F-FDG PET, due to volume averaging in relation to the limited spatial resolution of the PET scanner [
5]. This case report confirms the presumption of Chen et al. and reflects the high disease heterogeneity in patients with MM.
Figure 2.
A patient with MM (Typ IgG lambda, Stage IA according to the Durie–Salmon staging system, ISS I) underwent an 18F-FDG PET/CT and a routine whole-body MRI investigation after radiation therapy of an extensive plasma cell infiltration in the sternum and three courses of induction therapy. No signs of further focal lesions were illustrated in previous CT and MRI investigations. A contrast-enhanced CT-scan was not performed in this case. The subsequent 18F-FDG PET/CT (
a,
b) did not demonstrate any focal lesion in the liver. A small lesion of 8 mm was delineated in Segment IVb, with an abnormal diffusion restriction in diffusion-weighted (DW,
c) MRI (red arrow). The same lesion could not be distinguished in the T1-VIBE or T2-weighted sequences (
d). A diagnostic ultrasound of the liver was not performed before (no pre-described hepatic disease), while the biopsy of the lesion under sonographic control indicated plasma cell neoplasia. Chen et al. reported a sensitivity of PET/CT nearly equivalent to that of MRI for the detection of extramedullary lesions; however, they added that in some areas, the use of both techniques could offer complementary information [
4]. It must be noted that small lesions with a subcentimeter size may not be detectable on 18F-FDG PET, due to volume averaging in relation to the limited spatial resolution of the PET scanner [
5]. This case report confirms the presumption of Chen et al. and reflects the high disease heterogeneity in patients with MM.
![Diagnostics 09 00179 g002 Diagnostics 09 00179 g002]()