Multimodal Surgical Management of Stage 1a/1b PCFD (Stage II AAFD): Early Outcomes of a Standardized Four-in-One Procedure Protocol
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Clinical Evaluation
2.2. Statistical Analysis
3. Results
3.1. Patient Demographics
3.2. Radiographic Outcomes
3.3. Clinical Outcomes
3.4. Arthroeresis Removal
3.5. Complications and Follow-Up
3.6. Representative Case
4. Discussion
4.1. The Shift from “2-in-1” to Multi-Component Reconstruction
4.2. Comparative Analysis of Surgical Protocols
4.3. The Paradox of Subtalar Arthroereisis in Adults
4.4. Clinical Significance and Global Context
4.5. Limitations and Future Directions
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AAFD | adult-acquired flatfoot deformity |
| AOFAS | American Orthopaedic Foot & Ankle Society |
| BMI | body mass index |
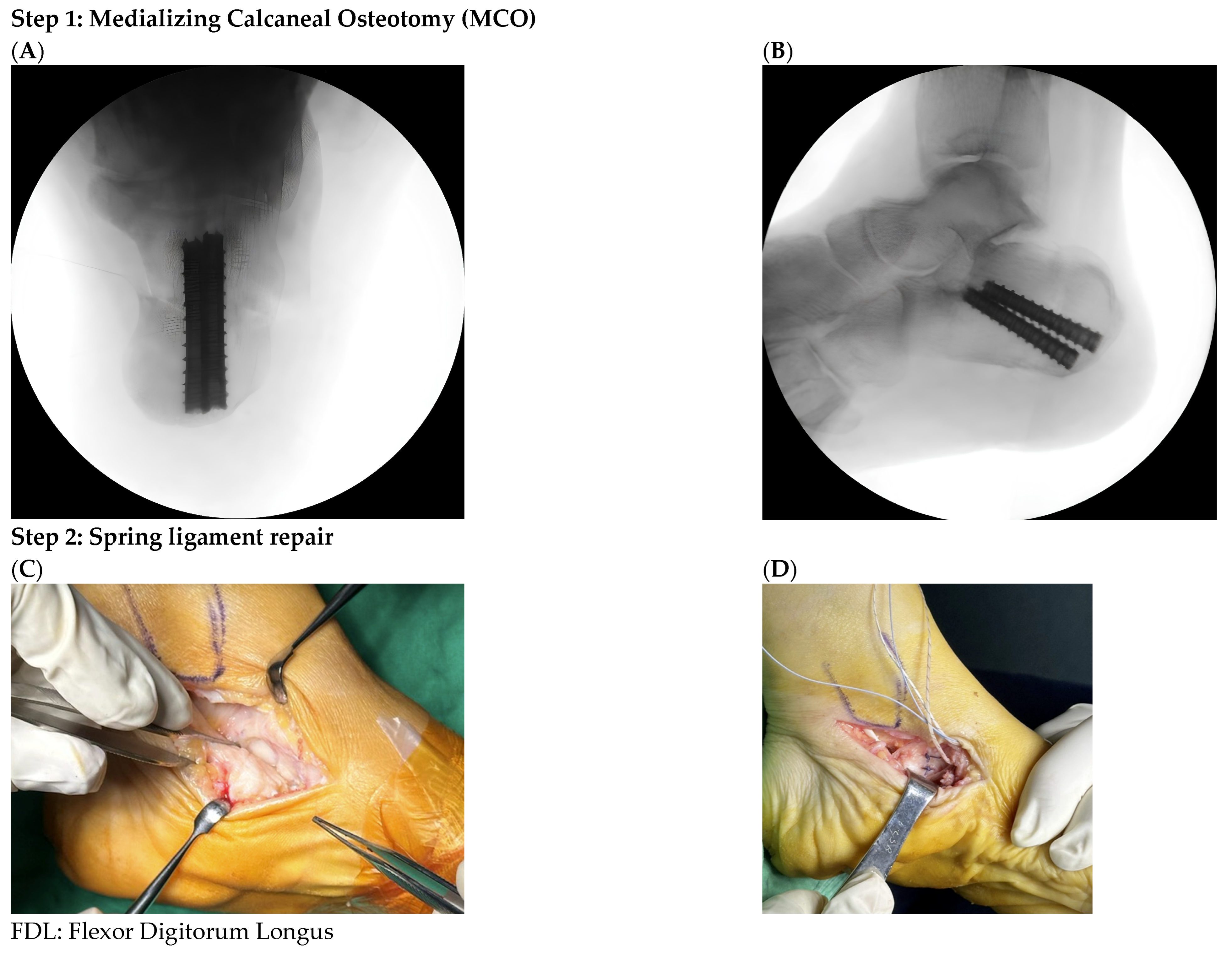
| FDL | flexor digitorum longus |
| GEE | generalized estimating equations |
| GLM | generalized linear model |
| IRB | institutional review board |
| MCO | medializing calcaneal osteotomy |
| PCFD | progressive collapsing foot deformity |
| SL | spring ligament |
| VAS | visual analog scale |
References
- Myerson, M.S.; Thordarson, D.B.; Johnson, J.E.; Hintermann, B.; Sangeorzan, B.J.; Deland, J.T.; Schon, L.C.; Ellis, S.J.; de Cesar Netto, C. Progressive collapsing foot deformity. Foot Ankle Int. 2020, 41, 1270–1276. [Google Scholar] [CrossRef]
- Pasapula, C.S.; Choudkhuri, M.R.; Monzó, E.R.G.; Dhukaram, V.; Shariff, S.; Pasterse, V.; Richie, D.; Kobezda, T.; Solomou, G.; Cutts, S. Review of classification systems for adult acquired flatfoot deformity/progressive collapsing foot deformity and development of a triple classification. J. Clin. Med. 2024, 13, 942. [Google Scholar] [CrossRef] [PubMed]
- Flores, D.V.; Mejía Gómez, C.; Fernández Hernando, M.; Davis, M.A.; Pathria, M.N. Adult acquired flatfoot deformity: Anatomy, biomechanics, staging, and imaging findings. Radiographics 2019, 39, 1437–1460. [Google Scholar] [CrossRef] [PubMed]
- Henry, J.K.; Shakked, R.; Ellis, S.J. Adult-acquired flatfoot deformity. Foot Ankle Orthop. 2019, 4, 247301141984865. [Google Scholar] [CrossRef] [PubMed]
- Krautmann, K.; Kadakia, A.R. Spring and deltoid ligament insufficiency in progressive collapsing foot deformity. Foot Ankle Clin. 2021, 26, 245–258. [Google Scholar] [CrossRef]
- Jackson, J.B., III. Adult acquired flatfoot deformity. J. Am. Acad. Orthop. Surg. 2022, 30, e553–e564. [Google Scholar] [CrossRef]
- Hintermann, B. Biomechanics of medial ankle and peritalar instability. Foot Ankle Clin. 2021, 26, 219–233. [Google Scholar] [CrossRef]
- de Cesar Netto, C.; Silva, T.; Li, S.; Mansur, N.S.; Auch, E.; Dibbern, K.; Femino, J.E.; Baumfeld, D. Assessment of Posterior and Middle Facet Subluxation of the Subtalar Joint in Progressive Flatfoot Deformity. Foot Ankle Int. 2020, 41, 1190–1197. [Google Scholar] [CrossRef]
- de Cesar Netto, C.; Myerson, M.S.; Day, J.; Ellis, S.J.; Hintermann, B.; Johnson, J.E.; Sangeorzan, B.J.; Schon, L.C.; Thordarson, D.B.; Deland, J.T. Consensus for the Use of Weightbearing CT in the Assessment of Progressive Collapsing Foot Deformity. Foot Ankle Int. 2020, 41, 1277–1282. [Google Scholar] [CrossRef]
- Polichetti, C.; De Filippo, M.; Sverzellati, N. Imaging of adult acquired flatfoot deformity. Diagnostics 2023, 13, 225. [Google Scholar] [CrossRef]
- Chien, B.Y.; Greisberg, J.K.; Arciero, E. Spring ligament reconstruction for progressive collapsing foot deformity: Contemporary review. Foot Ankle Int. 2023, 44, 796–809. [Google Scholar] [CrossRef] [PubMed]
- Nery, C.; Lemos, A.V.K.C.; Raduan, F.; Mansur, N.S.B.; Baumfeld, D. Combined spring and deltoid ligament repair in adult-acquired flatfoot deformity. Foot Ankle Int. 2018, 39, 782–789. [Google Scholar] [CrossRef] [PubMed]
- Brodell, J.D., Jr.; MacDonald, A.; Perkins, J.A.; Deland, J.T.; Oh, I. Deltoid-Spring Ligament Reconstruction in Adult Acquired Flatfoot Deformity With Medial Peritalar Instability. Foot Ankle Int. 2019, 40, 753–761. [Google Scholar] [CrossRef]
- Osbeck, I.; Cöster, M.; Montgomery, F.; Atroshi, I. Surgically treated adult acquired flatfoot deformity: Register-based study. Foot Ankle Surg. 2023, 29, 367–372. [Google Scholar] [CrossRef]
- Conti, M.S.; Jones, M.T.; Savenkov, O.; Deland, J.T.; Ellis, S.J. Outcomes of reconstruction of stage II adult-acquired flatfoot deformity in older patients. Foot Ankle Int. 2018, 39, 389–397. [Google Scholar] [CrossRef]
- Bastias, G.F.; Dalmau-Pastor, M.; Astudillo, C.; Pellegrini, M.J. Spring ligament instability. Foot Ankle Clin. 2018, 23, 659–678. [Google Scholar] [CrossRef]
- Tang, C.Y.K.; Ng, K.H. Clinical and radiological outcomes of braided suture tape system augmentation for spring ligament repair in flexible flatfoot. Foot 2020, 45, 101685. [Google Scholar] [CrossRef]
- Mattesi, L.; Ancelin, D.; Severyns, M.P. Is subtalar arthroereisis a good procedure in adult acquired flatfoot? A systematic review. Orthop. Traumatol. Surg. Res. 2021, 107, 103002. [Google Scholar] [CrossRef]
- Baryeh, K.W.; Ismail, H.; Sobti, A.; Harb, Z. Outcomes following subtalar arthroereisis in adult acquired flatfoot. Foot Ankle Spec. 2022, 15, 384–393. [Google Scholar] [CrossRef] [PubMed]
- Saxena, A.; Via, A.G.; Maffulli, N.; Chiu, H. Subtalar arthroereisis implant removal in adults. J. Foot Ankle Surg. 2016, 55, 500–503. [Google Scholar] [CrossRef]
- Mueller, G.; Frosch, K.-H.; Barg, A.; Schlickewei, C.; Weel, H.; Krähenbühl, N.; Priemel, M. Impact of medial displacement calcaneal osteotomy on foot biomechanics. Arch. Orthop. Trauma Surg. 2024, 144, 1955–1967. [Google Scholar] [CrossRef] [PubMed]
- Arangio, G.A.; Salathe, E.P. A biomechanical analysis of posterior tibial tendon dysfunction, medial displacement calcaneal osteotomy and flexor digitorum longus transfer in adult acquired flat foot. Clin. Biomech. 2009, 24, 385–390. [Google Scholar] [CrossRef] [PubMed]
- Krautmann, K.; Kadakia, A.R. Spring and deltoid ligament insufficiency in the setting of progressive collapsing foot deformity: An update on diagnosis and management. Foot Ankle Clin. 2021, 26, 577–590. [Google Scholar] [CrossRef]
- Marsland, D.; Morris, A.M.; Gould, A.E.R.; Calder, J.D.F.; Amis, A.A. Systematic review of tendon transfers in the foot and ankle using interference screw fixation: Outcomes and safety of early versus standard postoperative rehabilitation. Foot Ankle Surg. 2022, 28, 166–175. [Google Scholar] [CrossRef]
- Cruz-Jentoft, A.J.; Bahat, G.; Bauer, J.; Boirie, Y.; Bruyère, O.; Cederholm, T.; Cooper, C.; Landi, F.; Rolland, Y.; Sayer, A.A.; et al. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing 2019, 48, 16–31. [Google Scholar] [CrossRef] [PubMed]
- Hintermann, B.; Knupp, M.; Pagenstert, G. Surgical treatment of the adult acquired flexible flatfoot. Foot Ankle Clin. 2007, 12, 277–296. [Google Scholar]
- Niki, H.; Hirano, T.; Okada, H.; Beppu, M. Outcome of medial displacement calcaneal osteotomy for correction of adult-acquired flatfoot. Foot Ankle Int. 2012, 33, 900–908. [Google Scholar] [CrossRef]
- Hintermann, B.; Valderrabano, V.; Nigg, B.M. Correction of moderate and severe acquired flexible flatfoot with medializing calcaneal osteotomy and flexor digitorum longus transfer. J. Bone Joint Surg. Am. 2006, 88, 1726–1734. [Google Scholar]
- Maskill, J.D.; Bohay, D.R.; Anderson, J.G. Radiographic correction following reconstruction of adult acquired flatfoot deformity. Foot Ankle Int. 2010, 31, 749–756. [Google Scholar]
- Abousayed, M.M.; Alley, M.C.; Shakked, R.; Rosenbaum, A.J. Adult-acquired flatfoot deformity: Etiology, diagnosis, and management. JBJS Rev. 2017, 5, e7. [Google Scholar] [CrossRef]
- De Pellegrin, M.; Moharamzadeh, D. Subtalar arthroereisis for surgical treatment of flexible flatfoot. Foot Ankle Clin. 2021, 26, 765–805. [Google Scholar] [CrossRef] [PubMed]
- Walley, K.C.; Greene, G.; Hallam, J.; Juliano, P.J.; Aynardi, M.C. Short- to mid-term outcomes following the use of an arthroereisis implant as an adjunct for correction of flexible, acquired flatfoot deformity in adults. Foot Ankle Spec. 2019, 12, 122–130. [Google Scholar] [CrossRef] [PubMed]
- de Cesar Netto, C.; Saito, G.H.; Roney, A.; Day, J.; Greditzer, H.; Sofka, C.; Ellis, S.J.; Richter, M.; Barg, A.; Lintz, F.; et al. Combined weightbearing CT and MRI assessment of flexible progressive collapsing foot deformity. Foot Ankle Surg. 2021, 27, 884–891. [Google Scholar] [CrossRef]
- Poutoglidou, F.; Marsland, D.; Elliot, R. Does foot shape really matter? Correlation of patient-reported outcomes with radiographic assessment in progressive collapsing foot deformity reconstruction: A systematic review. Foot Ankle Surg. 2024, 30, 441–449. [Google Scholar] [CrossRef] [PubMed]




| Variable | Value |
|---|---|
| Total patients (n) | 20 |
| Female:Male | 19:1 |
| Mean age (years) | 61.0 ± 8.3 |
| BMI (kg/m2) | 26.9 ± 8.25 |
| Affected side (Right:Left) | 8:12 |
| Parameter | Preoperative | Postoperative | 24 Months of Follow-Up | p-Value |
|---|---|---|---|---|
| Meary angle (AP, °) | 24.2 ± 7.4 | 9.2 ± 4.1 | 8.6 ± 4.1 | <0.001 |
| Meary angle (Lateral, °) | 9.96 ± 2.3 | 1.92 ± 1.4 | 2.05 ± 1.6 | <0.012 |
| Calcaneal pitch (°) | 10.64 ± 4.87 | 15.78 ± 3.33 | 15.55 ± 4.25 | <0.01 |
| Talonavicular coverage angle (°) | 14.53 ± 6.67 | 3.46 ± 1.56 | 3.58 ± 0.78 | <0.024 |
| VAS pain score | 7.2 ± 1.2 | 2.6 ± 1.1 | 1.9 ± 1.1 | <0.001 |
| AOFAS hindfoot score | 48.5 ± 10.3 | 78.4 ± 8.9 | 84.7 ± 7.6 | <0.001 |
| Variable | Removed (n = 9) | Retention (n = 11) | p-Value |
|---|---|---|---|
| Age (years) | 60.1 ± 7.9 | 60.9 ± 8.6 | 0.833 |
| BMI (kg/m2) | 27.8 ± 3.5 | 26.1 ± 4.1 | 0.332 |
| Side (Right) | 5 (55.6%) | 6 (54.5%) | 0.999 |
| Radiographic Parameter | Group | Preoperative | Final Follow-Up | p-Value (Final) | p-Value (Interaction) |
|---|---|---|---|---|---|
| Meary angle (AP, °) | Removed | 24.2 ± 7.4 | 8.6 ± 4.1 | 0.912 | 0.884 |
| Retention | 23.8 ± 6.9 | 8.8 ± 3.9 | |||
| Meary angle (Lat, °) | Removed | 10.9 ± 2.1 | 2.0 ± 0.3 | 0.724 | 0.920 |
| Retention | 8.8 ± 1.9 | 2.0 ± 0.5 | |||
| Calcaneal Pitch (°) | Removed | 12.9 ± 2.3 | 15.5 ± 2.1 | <0.01 * | 0.752 |
| Retention | 12.4 ± 6.3 | 16.2 ± 4.3 | |||
| Talonavicular coverage angle (°) | Removed | 11.0 ± 2.2 | 3.8 ± 1.8 | 0.024 * | 0.814 |
| Retention | 17.1 ± 7.9 | 3.3 ± 1.5 | |||
| Clinical Outcome | Group | Preoperative | Final Follow-Up | p-Value (Final) | p-Value (Interaction) |
| VAS Score | Removed | 7.8 ± 0.4 | 2.0 ± 0.7 | 0.57 | 0.002 * |
| Retention | 6.7 ± 0.8 | 2.2 ± 0.8 | |||
| AOFAS Score | Removed | 52.2 ± 5.7 | 91.1 ± 3.3 | 0.125 | 0.041 * |
| Retention | 57.5 ± 6.3 | 88.1 ± 4.8 |
| Protocol | Components | 10-Year Literature Trend | Clinical Utility vs. Risks |
|---|---|---|---|
| 2-in-1 | MCO + FDL | Risk of residual transverse-plane deformity in selected patterns [4,5]. | Lower surgical time; higher risk of recurrent midfoot abduction. |
| 3-in-1 | MCO + FDL + SL Repair | Recognition of the Spring Ligament (SL) as the primary stabilizer [11]. | Improved arch height; potential for soft-tissue stretching over time. |
| 4-in-1 (Current) | MCO + FDL + SL/IB + Arthroereisis | Focus on “Internal Splinting” and immediate stabilization [12,18]. | Protocolized multiplanar correction; high hardware removal rate (45%). |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Chen, Y.T.; Lin, C.S.; Cheng, S.E.; Lin, S.M.; Lan, T.Y. Multimodal Surgical Management of Stage 1a/1b PCFD (Stage II AAFD): Early Outcomes of a Standardized Four-in-One Procedure Protocol. Diagnostics 2026, 16, 1124. https://doi.org/10.3390/diagnostics16081124
Chen YT, Lin CS, Cheng SE, Lin SM, Lan TY. Multimodal Surgical Management of Stage 1a/1b PCFD (Stage II AAFD): Early Outcomes of a Standardized Four-in-One Procedure Protocol. Diagnostics. 2026; 16(8):1124. https://doi.org/10.3390/diagnostics16081124
Chicago/Turabian StyleChen, Yu Ting, Cing Syue Lin, Shou En Cheng, Shang Ming Lin, and Tsung Yu Lan. 2026. "Multimodal Surgical Management of Stage 1a/1b PCFD (Stage II AAFD): Early Outcomes of a Standardized Four-in-One Procedure Protocol" Diagnostics 16, no. 8: 1124. https://doi.org/10.3390/diagnostics16081124
APA StyleChen, Y. T., Lin, C. S., Cheng, S. E., Lin, S. M., & Lan, T. Y. (2026). Multimodal Surgical Management of Stage 1a/1b PCFD (Stage II AAFD): Early Outcomes of a Standardized Four-in-One Procedure Protocol. Diagnostics, 16(8), 1124. https://doi.org/10.3390/diagnostics16081124






