1. Introduction
Chronic obstructive pulmonary disease (COPD) remains among the foremost causes of global mortality and morbidity. The World Health Organization estimates that, in 2021, COPD was responsible for approximately 3.5 million deaths—around 5% of all deaths worldwide—ranking as the fourth leading cause of death [
1]. Beyond its epidemiological burden, COPD is increasingly conceptualized as a biologically heterogeneous, immune-mediated inflammatory disorder in which airway damage and systemic effects are shaped by complex crosstalk between epithelial injury, innate immune activation and vascular inflammation. Recent work has highlighted cigarette-smoke–driven epithelial–immune communication through extracellular vesicles; for example, exosomal signalling has been shown to promote macrophage M1 polarization and inflammatory cell death pathways via TREM-1–related mechanisms in experimental COPD models [
2]. In parallel, microRNA-regulated sirtuin axes have been implicated in cigarette smoke–induced lung injury and functional impairment (e.g., miR-132 targeting SIRT1/FoxO1) [
3], while activation of SIRT6 has been reported to suppress NF-κB–driven endothelial inflammatory responses relevant to pulmonary microvascular inflammation [
4]. Clinically, immune dysregulation may also translate into altered susceptibility to immune-related adverse events; notably, COPD has been associated with a higher risk of autoimmune thyroiditis during pembrolizumab therapy in non-small cell lung cancer [
5]. Together, these mechanistic and clinical data support the need for integrative severity approaches that go beyond spirometry alone and reflect the multidimensional burden of COPD. Independent analyses report over 212 million people affected and more than 3 million deaths annually, elevating COPD to third place in the global mortality hierarchy [
6,
7]. This burden is especially acute in low- and middle-income countries, where nearly 90% of premature deaths (<70 years) occur [
1].
Despite its clinical significance, commonly used composite indices—BODE, DOSE, ADO and B-AE-D—evaluate disease severity predominantly through somatic parameters, focusing on airflow limitation, exercise capacity, body mass index or exacerbation history. Yet, a substantial body of evidence demonstrates that anxiety and depressive disorders are not mere comorbidities but clinically consequential modifiers of COPD trajectories. Beyond symptom amplification, affective burden has been associated with higher healthcare utilization and poorer prognosis, including higher exacerbation risk and increased likelihood of hospital admission, and has been linked to adverse outcomes in longitudinal and registry-based studies [
8,
9,
10,
11,
12,
13].
From a mechanistic standpoint, anxiety intensifies the perception of dyspnoea through interoceptive hypersensitivity [
14] and heightened sympathetic activation, regardless of obstruction severity [
15,
16,
17,
18]. CAT scores are significantly higher in patients with anxiety or depression, even in the absence of objective FEV
1 deterioration [
19,
20,
21]. Clinically, this emotional influence has been associated with a markedly increased risk of subsequent exacerbation and a self-reinforcing cycle of functional decline, disproportionate symptom burden, and escalated care needs [
13,
22].
In a preliminary study, our team applied k-means clustering to a comprehensive set of cognitive, affective and respiratory variables in patients with chronic respiratory disorders (asthma or COPD), identifying three distinct clusters; one of these—corresponding to a “Severe Cognitive Respiratory” profile—was dominated by marked anxiety–depressive symptoms and cognitive impairment in the context of substantial respiratory limitation, i.e., a pronounced psycho-respiratory burden [
23]. These findings underscored the heterogeneity of COPD and highlighted the need for an index capable of quantifying both somatic and emotional dimensions concurrently.
On these grounds, the present study introduces the Integrated Pulmonary Severity Score (IPSS), a composite index combining airflow obstruction, symptomatic burden and anxiety–depressive load into a unified formula. Furthermore, we employ unsupervised spectral clustering—which has proven effective in delineating clinically meaningful phenotypes in asthma and sepsis [
24,
25]—to validate the existence of a discrete psycho-respiratory phenotype. The aim of this work is to propose and internally characterize IPSS as a pragmatic bedside tool for integrated severity assessment and risk stratification, while explicitly acknowledging the need for external, multi-ethnic and longitudinal validation before clinical implementation. Throughout the manuscript, “severity” refers to the integrated multidimensional burden quantified by the continuous IPSS, whereas “risk stratification” refers to the pragmatic assignment of patients into ordinal IPSS risk categories intended to guide clinical follow-up and management intensity.
2. Materials and Methods
This prospective observational study was conducted between October 2022 and September 2024 at two tertiary care centres in Romania: the Craiova Clinical Neuropsychiatry Hospital—Psychiatry Clinic (Park), which oversaw all psychiatric and cognitive evaluations, and Leamna Pulmonology Hospital, which performed respiratory function testing and symptom assessments. Adults (≥18 years) hospitalized with a spirometry-confirmed diagnosis of chronic obstructive pulmonary disease (COPD) were enrolled consecutively after providing written informed consent. Ethical approval was obtained from the Ethics Committee of the University of Medicine and Pharmacy Craiova (Protocol No. 196/17 February 2022) and from the local committees at both hospitals (Protocol No. 6190/14 October 2022), in accordance with the Declaration of Helsinki.
2.1. Inclusion and Exclusion Criteria
Eligible participants were adults (≥18 years) with a COPD diagnosis confirmed according to contemporary GOLD criteria who were able to provide informed consent and to complete study assessments during hospitalization. Exclusion criteria comprised major cardiometabolic comorbidities (e.g., heart failure, BMI > 35 kg/m
2, obstructive sleep apnoea), uncontrolled psychiatric disorders beyond anxiety and depression, major surgery within the previous six months, inability to perform valid spirometry or refusal to participate. Of 450 patients screened, 60 were excluded for these reasons, yielding a final cohort of 390 patients (
Figure 1).
These exclusions were applied to minimize major non-pulmonary confounding during exploratory score derivation, acknowledging that this may reduce generalizability to multimorbid real-world COPD populations.
2.2. Respiratory Assessment
At Leamna Pulmonology Hospital, respiratory evaluation included:
Spirometry (Spirolab IV): FEV1 and FVC were measured, and predicted FEV1% was calculated according to reference equations; airflow limitation was subsequently graded into GOLD I–IV categories.
mMRC Dyspnoea Scale: graded 0–4 according to dyspnoea severity during usual daily activities.
COPD Assessment Test (CAT): eight items scored 0–5 (total 0–40) covering cough, sputum, chest tightness, activity limitation, confidence, sleep and energy. In this study, values < 10 were considered low impact, 10–20 moderate, 21–30 high and >30 very high impact.
2.3. Psychiatric and Cognitive Evaluation
Within 48 h at Craiova Clinical Neuropsychiatry Hospital—Psychiatry Clinic (Park), participants completed:
Hospital Anxiety and Depression Scale (HADS): two subscales (0–21) for anxiety and depression (0–7 normal; 8–10 mild; 11–14 moderate; 15–21 severe).
Montreal Cognitive Assessment (MoCA): 0–30 scale (26–30 normal; 18–25 mild impairment; 10–17 moderate; <10 severe).
Mini–Mental State Examination (MMSE): 0–30 scale (25–30 normal; 21–24 mild; 10–20 moderate; <10 severe).
2.4. IPSS Construction and Clustering
The Integrated Pulmonary Severity Score (IPSS) was constructed in two steps. First, a pulmonary component (PulmoScore) was defined deterministically from CAT, mMRC (rescaled ×10 to harmonize with the CAT 0–40 range) and ventilatory deficit (100 − FEV
1%), yielding an explicit weighted combination of these three variables. Second, the PulmoScore was multiplied by a psychiatric amplification factor derived from HADS-Depression and HADS-Anxiety, yielding:
where α and β represent per-point fractional increases in the multiplier (cohort-derived coefficients). Coefficients and cut-offs are therefore subject to external recalibration in independent validation cohorts. Although cognitive assessments (MoCA and MMSE) were collected and analyzed to characterize phenotype burden, they were intentionally not incorporated into the final IPSS to preserve routine feasibility and portability across settings, given that cognitive testing is not universally performed at each visit and may be influenced by education, language/cultural factors and examiner variability.
To explore whether IPSS components reflected clinically meaningful patterns, we applied spectral clustering to the matrix of respiratory, affective and cognitive variables. The number of clusters (k = 2–5) was examined, and the optimal solution was chosen based on the highest average silhouette coefficient and clinical interpretability, yielding two phenotypes: a psycho-respiratory and a predominantly respiratory profile.
2.5. Statistical Analysis
Classical statistical analyses were performed in SPSS 26.0 (IBM Corp., Armonk, NY, USA). Continuous variables were expressed as mean ± standard deviation or median (interquartile range) and compared using independent-samples t tests or non-parametric equivalents, as appropriate. Categorical variables were summarized as counts and percentages and compared with χ2 tests. Pearson correlation coefficients were computed to assess bivariate associations between FEV1%, CAT, mMRC, HADS, MoCA and MMSE. A two-tailed p < 0.05 was considered statistically significant.
Predictive modelling was conducted in Python 3.8 (Anaconda distribution; Anaconda, Inc., Austin, TX, USA)) using scikit-learn 1.2.2 (Python Software Foundation, Wilmington, DE, USA). Data were randomly split into a training set (70%) and a test set (30%), stratified by cluster membership. The following models were fitted:
Logistic regression: to estimate linear relationships between core predictors (respiratory, affective, cognitive variables and composite scores) and membership in the psycho-respiratory phenotype.
Multilayer perceptron (MLPClassifier): a feed-forward neural network with two hidden layers (50 and 25 neurons), rectified linear unit (ReLU) activation and Adam optimiser, to capture potential non-linear interactions.
Model performance was evaluated using accuracy, area under the receiver operating characteristic curve (AUC) and Cohen’s kappa (κ) on the test set. Local interpretability was obtained with the LIME package, which highlighted feature contributions—particularly FEV1% and HADS subscales—to individual predictions. Correlation networks and graphical representations (histograms, ROC curves, κ plots) were generated with matplotlib, seaborn and networkx.
3. Results
3.1. Descriptive Analysis of the Cohort
We first examined the clinical and demographic profile of the full cohort (n = 390) to establish a foundation for subsequent subgroup comparisons. Both continuous and categorical variables were catalogued to capture factors potentially influencing disease course, with particular attention to differences between patients with and without significant psychiatric symptoms.
3.1.1. Baseline Characteristics and Distribution of Continuous Variables
Continuous measures encompassed respiratory parameters and psychocognitive assessments. The mean age was 54.5 years (range 20–87), reflecting inclusion of both young adults and those with advanced disease. Sex distribution was balanced, and urban versus rural residence was nearly equal, ensuring broad socio-demographic representation.
Symptom severity by the COPD Assessment Test (CAT) averaged 17.3 (range 1–40), indicating the presence of both minimally and severely symptomatic subgroups. The mean Medical Research Council dyspnea grade (MRC) was 2.24 (0–4), suggesting that most patients experienced at least moderate exertional limitation. Objective obstruction, measured as percent-predicted FEV1, averaged 68.9% (range 28–99), with a subset demonstrating severe airflow limitation.
Psychiatric symptoms, assessed by HADS, showed mean depression and anxiety scores of 7.53 (1–20) and 8.04 (1–24), respectively. Although these averages are in the mild-to-moderate range, maximum scores indicate a subset with severe emotional disturbance. Cognitive function, measured by MoCA (mean 24.3, range 5–30) and MMSE (mean 23.8, range 6–30), was generally preserved; however, low-end scores reveal that a minority face substantial cognitive impairment. Together, these data underscore a highly heterogeneous cohort in terms of pulmonary obstruction severity, psychiatric burden and cognitive performance (
Table 1).
3.1.2. Subgroup Comparison: Impact of Psychiatric Symptoms
To assess how psychiatric symptoms influence respiratory impairment, patients were stratified into two groups based on HADS scores and affective history. Group 1 (n = 257) comprised individuals with combined psycho-respiratory involvement, while Group 2 (n = 133) included those with predominantly respiratory disease.
Marked differences emerged between groups. Mean percent-predicted FEV
1 in Group 1 was approximately 60%, versus over 85% in Group 2. CAT scores averaged 22.3 in Group 1—nearly threefold higher than the 7.7 observed in Group 2—reflecting significantly heightened symptom perception among those with psychiatric comorbidity. HADS depression and anxiety scores were also significantly elevated in Group 1, and cognitive testing yielded lower MoCA and MMSE scores. A
t test of the Integrated Pulmonary Severity Index (IPSS) produced a t-statistic of 18.33 (
p < 0.001), confirming highly significant intergroup differences (
Table 2).
3.1.3. Distribution of Categorical Variables and Between-Group Comparisons
We further examined categorical variables to complete the demographic and clinical picture. In the overall cohort, 207 patients were male (53%) and 183 were female (47%); 216 lived in urban areas (55%), 174 in rural (45%); occupational status was 42% unemployed, 53% employed and 5% retired; education level spanned 54% for lower secondary, 26% for high school and 19% for higher education; 18% presented via the emergency department versus 82% in outpatient settings; smoking status was 42% never-smokers, 28% ex-smokers and 30% current smokers; alcohol use was 52% abstinent, 39% occasional and 9% chronic.
Comparisons between Group 1 and Group 2 revealed significant differences in several categories (χ
2 test): sex distribution (
p = 0.050), urban versus rural residence (
p = 0.020), unemployment rate (
p = 0.010), education level (
p = 0.005), mode of presentation (
p = 0.030), smoking status (
p = 0.010) and alcohol consumption (
p = 0.020) (
Table 3).
These findings suggest that socio-demographic factors and health behaviours may modulate the interplay between psychiatric comorbidity and respiratory severity.
3.2. Analysis of Relationships Between Variables: Correlations and the Network of Interdependencies
We quantified pairwise associations among respiratory measures (percent-predicted FEV
1, CAT and mMRC scores), psychiatric indices (HADS-Depression and HADS-Anxiety) and cognitive assessments (MoCA and MMSE) using Pearson’s correlation coefficient. A very strong inverse correlation emerged between percent-predicted FEV
1 and CAT score (r = −0.82,
p < 0.001) and between FEV
1 and mMRC grade (r = −0.65,
p < 0.001), while CAT and mMRC were strongly interrelated (r = 0.71,
p < 0.001), confirming that declining lung function is tightly linked to worsening symptom burden and dyspnoea (
Figure 2).
MoCA and MMSE also showed an almost perfect positive correlation (r = 0.92, p < 0.001), supporting the consistency of the cognitive assessments.
HADS-Depression and HADS-Anxiety scores correlated moderately and positively with both CAT and mMRC (r ≈ 0.37–0.43, all
p < 0.001), indicating that affective burden contributes to, but does not fully explain, perceived respiratory symptoms. By contrast, HADS scores showed strong negative correlations with cognitive performance—for example, r = −0.76 between HADS-Depression and MoCA and r = −0.73 with MMSE—together with a strong positive correlation between HADS-Depression and HADS-Anxiety themselves (r = 0.79,
p < 0.001). These patterns suggest that elevated affective symptoms are accompanied by measurable cognitive decline, which may impede treatment self-management (
Table 3).
To illustrate these interdependencies, we constructed a correlation network in which each node represents one of the seven key variables and edges denote significant correlations (|r| > 0.30, p < 0.05). This network revealed a central hub linking FEV1%, CAT and mMRC directly to HADS-Depression and HADS-Anxiety, which in turn showed inverse ties to MoCA and MMSE. Clinically, this topology suggests that losses in FEV1 may be perceived as disproportionately severe in patients with concurrent anxiety or depression—driving up CAT and mMRC scores—while those psychiatric symptoms are themselves associated with reduced cognitive capacity, potentially complicating disease management.
Taken together, these findings substantiate a shared core of physiological and psychological factors—where respiratory impairment, affective distress and cognitive decline are tightly interwoven—providing a robust multidimensional rationale for an integrated severity index such as IPSS.
3.3. Unsupervised Clustering and Natural Subgroup Separation
To explore whether the data naturally partition into two discrete subgroups—independently of the HADS-based classification—we applied spectral clustering to a set of standardized variables encompassing FEV1% predicted, CAT score, MRC dyspnoea grade, HADS depression and anxiety scores, and cognitive performance as assessed by MoCA and MMSE. Standardization ensured that each metric contributed equally to the multidimensional analysis, eliminating scale-related biases.
We assessed cluster validity using the Silhouette score, which identified an optimal solution at k = 2. In other words, the high-dimensional data define two well-separated regions, each corresponding to a cohort of patients with similar clinical profiles. Notably, the resulting clusters showed marked concordance with our pre-defined HADS groups: “Cluster 1” comprised predominantly patients with combined psychiatric and respiratory impairment, whereas “Cluster 2” aligned largely with those exhibiting primarily respiratory dysfunction.
This convergence between an unsupervised clustering approach and the HADS-driven classification further substantiates the hypothesis that psychiatric factors—particularly anxiety and depression—together with respiratory metrics (CAT, MRC, FEV1) constitute a core determinant of natural subgroup separation. Thus, beyond confirming the existence of two distinct phenotypic clusters, our analysis underscores the importance of integrating psychiatric assessment into the evaluation of pulmonary disease severity.
In summary, the intrinsic bifurcation of patient subgroups revealed by spectral clustering—and validated by the Silhouette Index—reinforces the notion that emotional symptoms can amplify both the perception and impact of respiratory impairment, providing a solid foundation for the future development of an integrated severity index.
3.4. Classification Models and Clinical Validation
To determine how well our predictors identify patients with combined psychiatric–respiratory impairment (Cohort 1), we compared two approaches: a logistic regression and a multi-layer perceptron (MLP) neural network. Both models were trained on the same feature set—HADS depression and anxiety scores, respiratory measures (CAT, FEV1%, MRC dyspnoea grade) and global cognition (MoCA, MMSE).
The logistic regression achieved 89% accuracy, an area under the ROC curve (AUC) of 0.95 (
Figure 3) and Cohen’s κ of 0.77 (
Figure 4).
Regression coefficients highlighted CAT score—and above all HADS-Anxiety—as the strongest positive predictors of Cohort 1 membership, indicating that rising anxiety and symptom burden dramatically increase the odds of dual impairment. By contrast, FEV1% exerted a protective effect (negative coefficient), implying that higher lung function attenuates the risk of psychiatric–respiratory comorbidity. Together, these coefficients frame a clear narrative: as psychiatric symptoms intensify and pulmonary function declines, clinical complexity escalates.
In parallel, an MLPClassifier with two hidden layers (50 and 25 neurons) yielded virtually identical performance—89% accuracy, AUC 0.95 and Cohen’s κ of 0.75 (
Figure 4).
To probe local decision drivers, we applied LIME, which consistently flagged low FEV
1% and elevated HADS-Anxiety as the dominant features (
Figure 5).
These findings reinforce the notion that, beyond isolated measurements, the interplay between psychiatric symptomatology and airflow obstruction constitutes a powerful predictor of clinical severity. A unified insight from both classification frameworks is that psychiatric manifestations—most notably anxiety—and declining pulmonary function (as reflected by a low FEV1%) operate in concert to define disease burden. As anxiety and depression worsen and lung function deteriorates, the risk of adverse outcomes rises, underscoring the imperative for a multidisciplinary approach in patients exhibiting dual impairment.
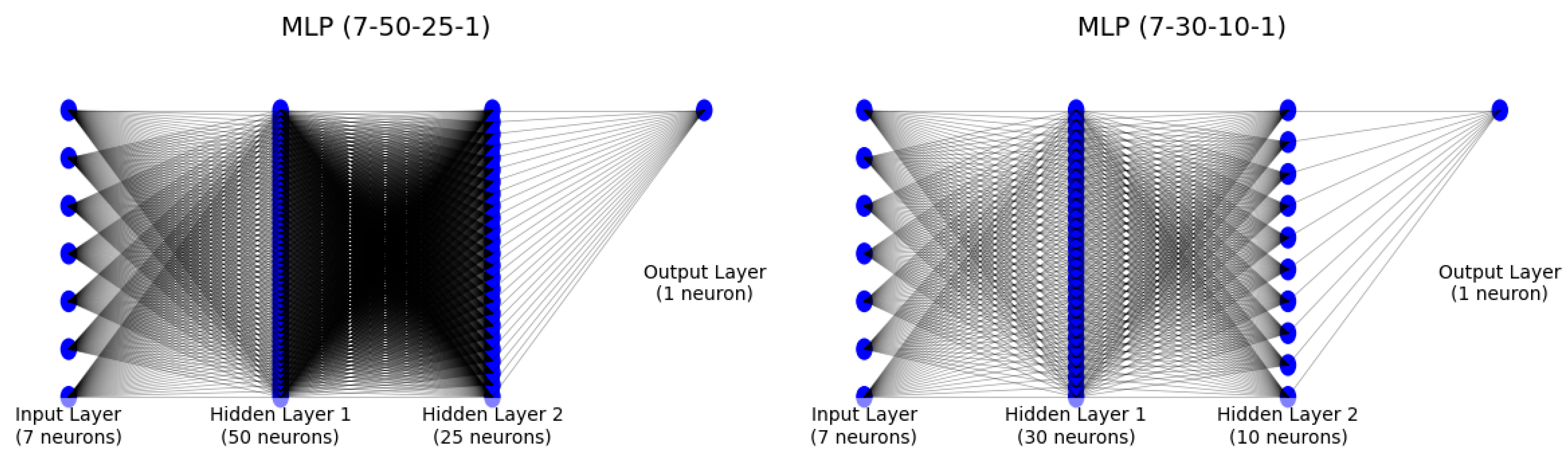
To offer further visual contrast between modelling strategies,
Figure 6 depicts the architecture of the MLPClassifier—highlighting its two hidden layers (50 and 25 neurons)—against the single-layer, unidirectional structure of logistic regression.
This schematic illustrates the added complexity of the neural network and its capacity to capture non-linear data relationships, which underpins its performance parity with the more interpretable regression model.
In sum, both logistic regression and neural-network approaches confirm that psychiatric distress and airflow limitation, particularly low FEV1%, are decisive in characterizing integrated disease severity. This underscores the value of integrating psychiatric evaluation into routine clinical assessment to support prognostic risk stratification and guide therapeutic decision-making.
3.5. Development and Implementation of the Integrated Pulmonary Severity Score (IPSS)
Given the strong correlations between FEV1%, symptom burden, dyspnoea, affective scores and cognition (e.g., r = −0.82 for FEV1% vs. CAT, r = −0.65 for FEV1% vs. mMRC, r = −0.43 and −0.37 for FEV1% vs. HADS-Anxiety and HADS-Depression, respectively, all p < 0.001), we sought to condense this multidimensional information into a single, clinically usable index. To this end, we constructed the Integrated Pulmonary Severity Score (IPSS) in two steps: first, by defining a pulmonary component that integrates obstruction and respiratory symptoms, and second, by applying a psychiatric multiplier reflecting the additional burden of anxiety and depression.
3.5.1. Construction of the Pulmonary Component (PulmoScore)
The pulmonary component, termed the PulmoScore, was defined a priori from three clinically interpretable variables: CAT, mMRC and ventilatory deficit expressed as (100 − FEV
1%). To harmonize scales, mMRC (0–4) was rescaled by multiplying by 10 to align with the CAT 0–40 range. The PulmoScore was then computed deterministically as:
A slightly higher weight was assigned to ventilatory deficit to anchor the score to objective obstruction, while CAT and rescaled mMRC contribute equally to capture patient-reported symptom burden and dyspnoea-related functional limitation. Under this formulation, a 10-point decrease in FEV1% increases the PulmoScore by 4 points, whereas a 10-point increase in CAT or a 1-grade increase in mMRC (i.e., +10 after rescaling) increases the PulmoScore by 3 points.
3.5.2. Addition of the Psychiatric Multiplier and Definition of IPSS
To capture the contribution of affective symptoms to overall disease severity, the PulmoScore was extended with a psychiatric multiplier based on HADS-Depression and HADS-Anxiety. The final index was defined as:
Using ordinary least squares regression with the global psycho-respiratory index (SGPI) as the dependent variable, the coefficients were estimated as α = 0.0231 and β = 0.0423 (per-point fractional increases in the multiplier), while the intercept was small and not retained for bedside computation. Visual inspection of the final IPSS distribution (
Figure 7) did not suggest marked score inflation or extreme outliers in this cohort. Thus, each additional HADS-Depression point increases the multiplier by 2.31%, and each additional HADS-Anxiety point increases the multiplier by 4.23%, holding other components constant. The larger coefficient for HADS-Anxiety should be interpreted cautiously: it is cohort-derived and may reflect stronger coupling between anxiety, dyspnoea perception and patient-reported symptom burden in this sample rather than a universal hierarchy of affective domains. Accordingly, these coefficients require external validation and may need recalibration across populations and care settings. In the cohort, this formulation produced IPSS values ranging from very low scores in patients with preserved lung function, minimal symptoms and normal HADS values to triple-digit scores in individuals with combined severe obstruction, high CAT and mMRC grades and marked anxiety–depression.
3.5.3. Interpretation of the IPSS Formula
The IPSS is obtained in two conceptually simple steps. First, the PulmoScore aggregates objective and subjective respiratory information into a single pulmonary severity index. Second, this PulmoScore is multiplied by a factor that increases with HADS-Depression and HADS-Anxiety scores, thereby “amplifying” the respiratory burden in the presence of affective comorbidity.
Clinically, this behaviour is intuitive:
Patients with relatively preserved FEV1%, low CAT and mMRC scores and normal HADS values tend to have low PulmoScores and remain in the lower IPSS range, corresponding to a predominantly somatic but mild overall burden.
Patients with comparable spirometric impairment but elevated HADS-Anxiety and/or HADS-Depression exhibit substantially higher IPSS values, shifting them into higher risk strata despite similar obstruction.
This mechanism formally explains the frequent discrepancy between spirometry and perceived health status in COPD: the psychiatric multiplier captures the additional psycho-emotional load that is invisible to FEV1% alone. In line with this, the psycho-respiratory cluster (Group 1) was characterized by lower FEV1%, higher CAT and mMRC scores and markedly higher HADS values, while the predominantly respiratory cluster (Group 2) had better lung function, lower symptom burden and near-normal affective scores.
3.5.4. Distribution of IPSS Values and Risk Categories
To render the IPSS interpretable at the bedside, we grouped the continuous score into four ordinal risk categories that balance the empirical score distribution with clinically intuitive cut-points:
Low risk: IPSS < 30 points
Moderate risk: IPSS 30–69 points
High risk: IPSS 70–119 points
Very high risk: IPSS ≥ 120 points.
To provide an explicit empirical reference for stratification, we also report the distribution-based cut-points of IPSS in this cohort. The IPSS quartiles were Q1 = 17.79, Q2 (median) = 35.91 and Q3 = 54.77. Accordingly, a quartile-based stratification would define four groups as IPSS ≤ 17.79, 17.79 < IPSS ≤ 35.91, 35.91 < IPSS ≤ 54.77, and IPSS > 54.77. We emphasize that both the pragmatic thresholds and the quantile-based cut-points are cohort-dependent and should be recalibrated and/or outcome-optimized in future external validation studies.
These bands were not optimized against hard endpoints (e.g., exacerbations, hospitalisations, mortality) in this cross-sectional derivation cohort. Instead, they were selected as pragmatic, distribution-informed thresholds approximating the sample quartiles and then rounded to improve bedside usability. Accordingly, these cut-offs should be recalibrated and/or outcome-optimized in external longitudinal validation cohorts before being used for prognostic decision-making. Patients were represented in all four strata, with a progressive gradient in respiratory impairment, symptom burden and affective distress from the low to the very-high IPSS category (
Table 4).
Descriptively, individuals with preserved lung function, low CAT and mMRC scores and normal or near-normal HADS values were concentrated in the low and moderate IPSS categories. By contrast, those combining severe obstruction, marked dyspnoea, high CAT scores and significant anxiety–depression predominantly occupied the high and very-high bands. This gradient closely mirrored the distribution of the two spectral-clustering phenotypes: the psycho-respiratory Group 1 showed a marked right-shift in the IPSS distribution, with a higher proportion of high and very-high scores compared with Group 2, whereas Group 2 was concentrated almost entirely in the low and moderate IPSS range (
Figure 7).
From a practical standpoint, these categories offer a simple decision-making framework. Low-IPSS patients are typically candidates for routine follow-up and standard pharmacological management. Moderate IPSS values signal the need to optimize inhaled therapy and initiate structured psychological support. High and very-high IPSS identify a subset requiring intensified and often multidisciplinary care, potentially including psychiatric consultation, pulmonary rehabilitation and closer monitoring.
3.5.5. Relationship Between IPSS-Based Profiles and Predictive Models
The clinical relevance of this integrated construct was further supported by the performance of supervised models trained to distinguish the two spectral-clustering phenotypes. Because the clustering procedure and IPSS construction relied on overlapping core variables, these supervised results should be interpreted as convergent internal validity (consistency with the latent structure captured by clustering) rather than as an independent external validation. A logistic regression model using the core IPSS components (FEV1%, CAT, mMRC, HADS-Depression, HADS-Anxiety, MoCA and MMSE) as predictors correctly classified 89% of patients (accuracy 0.89), with an area under the ROC curve (AUC) of 0.95 and a Cohen’s κ of 0.77, indicating almost perfect agreement beyond chance. A multilayer perceptron (MLP) neural network trained on the same variables and evaluated on an independent test set yielded a similar accuracy of 0.89, an AUC of 0.95 and a Cohen’s κ of 0.75.
LIME explanations for the MLP underscored that low FEV1% and elevated HADS-Anxiety scores were the most influential features for predicting assignment to the psycho-respiratory group, followed by intermediate levels of HADS-Depression, mMRC and CAT. These findings are consistent with the design of IPSS and reinforce the notion that integrating pulmonary function, symptom burden and affective status captures a clinically meaningful psycho-respiratory phenotype rather than a purely statistical construct.
4. Discussion
In contemporary pulmonology practice, there is broad consensus that disease severity assessment cannot be confined to the predicted percentage of FEV1, although this remains an essential physiological pillar. Established instruments—BODE, DOSE, ADO and B-AE-D—have successfully correlated spirometric values with mortality, exacerbation frequency or healthcare utilization; nevertheless, they almost exclusively describe the somatic dimension and systematically omit psycho-emotional factors. The Integrated Pulmonary Severity Score (IPSS) provides a coherent conceptual extension by explicitly incorporating anxiety–depressive symptomatology as a variable with its own numerical weight, thus allowing it to enter severity models on an equal footing with spirometry and dyspnoea.
The premise for this integration arises from a robust convergence of evidence: anxiety amplifies the perception of breathlessness and dyspnoea-related fear in COPD [
26,
27], elevates CAT scores irrespective of the obstruction degree [
19,
20] and—when co-existing with depression—more than doubles the risk of future exacerbations [
13]. Depression, in turn, overlaps with those neurocognitive and functional domains that drive prognosis: COPD-related cognitive impairment, frequently accompanied by depressive symptoms, has been linked to frontal lobe hypoperfusion on SPECT imaging [
28] and to poorer performance on both MoCA and MMSE [
29,
30]. At the same time, dyspnoea severity itself—strongly intertwined with affective burden—independently predicts in-hospital mortality during acute exacerbations [
31]. In light of these observations, the direct inclusion of HADS scores in a composite severity index is not merely optional but appears methodologically necessary to reflect the true impact of the disease on the patient.
4.1. Rationale for the IPSS Structure
The PulmoScore—the core respiratory component—aggregates the CAT, mMRC and ventilatory deficit, with a weight of 0.40 assigned to (100 − FEV
1%). This higher weighting for obstruction derives from the observation that, in our cohort, the FEV
1–symptom relationship (r = −0.82 for FEV
1% vs. CAT) was considerably tighter than the modest correlations reported in multicentre CAT validation studies [
32,
33]. Similar observations have emerged from the COSYCONET registry, where longitudinal declines in FEV
1 tracked worsening SGRQ scores over time [
34].
A relatively greater weight for FEV
1 is also justified by data on early-onset COPD: younger adults can exhibit marked airflow limitation and unfavourable trajectories despite relatively preserved multidimensional scores, challenging the traditional Fletcher–Peto paradigm [
35,
36]. Large cohort analyses show that “young COPD” patients carry a substantial burden of comorbidities and an excess mortality risk compared with age-matched ever-smoker controls [
37]. In such individuals, indices that strongly weight chronological age—such as ADO—may yield deceptively low risk estimates despite clinically significant impairment. By contrast, including both FEV
1 and patient-reported measures (CAT and mMRC) within the PulmoScore preserves the subjective dimension of symptom burden while anchoring it to the objective severity of obstruction, thus offering an immediate and clinically interpretable snapshot without requiring elaborate exercise testing.
4.2. Detailed Comparison with Established Indices
BODE remains a robust predictor of mortality in COPD, but it relies on the six-minute walk test (6MWT), which is difficult to standardize and is not routinely available in many outpatient clinics, limiting its practicality in everyday practice [
38,
39]. DOSE prioritizes exacerbation history and current smoking status, variables that can be collected rapidly in primary care and that have demonstrated prognostic value for mortality and healthcare utilization [
39]. However, active smokers often underestimate or normalize respiratory symptoms and therefore underreport them, which may attenuate the sensitivity of DOSE to detect clinically relevant risk [
40,
41].
ADO introduces chronological age as an essential variable alongside dyspnoea and FEV
1, yet early-onset and rapidly progressive COPD have been described in younger adults, indicating that a strong age component can still underestimate risk in susceptible individuals [
35,
36,
37]. B-AE-D incorporates body mass index, prior severe exacerbations and mMRC dyspnoea grade, and its extended version (B-AE-D-C) adds the biomarker copeptin, whose measurement requires laboratory infrastructure that is not universally accessible [
42]. By contrast, IPSS relies exclusively on spirometry and brief questionnaires, allowing calculation in 3–5 min and facilitating inter-centre comparability without additional investment. Importantly, IPSS is not proposed as a replacement for these established indices but as a complementary tool that explicitly integrates psycho-emotional burden into severity assessment. From the standpoint of everyday implementation, these instruments differ markedly in the time, infrastructure and data completeness they require. BODE offers strong prognostic performance, but its dependence on a standardized 6MWT introduces logistical barriers (space, staffing, protocol consistency) and limits rapid use in busy outpatient clinics and in telemedicine workflows. DOSE is well suited to primary care because its components can be collected quickly, yet it depends on accurate exacerbation history and current smoking status; both can be incompletely documented or variably reported, which may reduce sensitivity for clinically meaningful risk in routine practice. ADO improves prognostic discrimination by incorporating age, but a strong age component can yield deceptively low risk estimates in younger patients with marked airflow limitation or rapidly progressive disease. In contrast, IPSS was designed for maximal feasibility: it uses spirometry plus short questionnaires (CAT, mMRC, HADS) that are routinely obtainable in most settings, enabling computation within minutes and supporting digital capture in registries, spirometry software, and remote monitoring platforms. Practically, IPSS therefore complements established indices by offering a rapid, reproducible multidimensional snapshot that makes psycho-emotional burden quantitatively visible alongside obstruction and symptom severity.
4.3. Convergence with Unsupervised Phenotyping and Network Analysis
Applying spectral clustering to the clinical variable matrix yielded two clinically coherent clusters that showed substantial overlap with groups defined by HADS scores, suggesting that anxiety, depression, CAT, mMRC and FEV
1 constitute a major axis of variability in this dataset [
24,
25]. Network-based analyses placed affective variables among high-centrality nodes [
43,
44], indicating not merely passive association but a potential generative role in clinical distress and functional limitation. This unsupervised convergence supports the notion that the IPSS formula approximates the latent structure of the data rather than merely modelling relationships imposed a priori. Nevertheless, because the same feature set underlies both clustering and score construction, this convergence should be viewed as supportive internal evidence, and independent validation against external cohorts and longitudinal outcomes remains required.
4.4. Clinical Implementation and Pragmatic Benefits
IPSS uses five routinely available variables (FEV
1%, CAT, mMRC, HADS-Anxiety and HADS-Depression) and can be embedded into spirometry software, outpatient workflows, and telemonitoring platforms. In practice, IPSS can function as a triage and personalization aid: (i) it can flag patients who may benefit from earlier multidisciplinary review (pulmonology + psychiatry/psychology), (ii) it can serve as a structured trigger for psychological referral (including telepsychiatry in low-access regions), and (iii) it can support prioritization for pulmonary rehabilitation and structured behavioural interventions (e.g., CBT-informed programmes) aimed at reducing affective distress and improving function [
45,
46,
47,
48]. Importantly, while higher IPSS plausibly indicates increased vulnerability to exacerbation and healthcare utilization, prospective longitudinal validation against hard endpoints is required before IPSS is used as an outcome-prediction tool in routine care. Moreover, the structure of IPSS is amenable to explainable-AI pipelines: in our cohort, LIME highlighted HADS-Anxiety and FEV
1 as leading contributors to the model output, consistent with comparative evaluations showing the usefulness of local interpretability techniques such as LIME and SHAP for distinguishing clinically meaningful classes [
49,
50]. These characteristics suggest that IPSS can act as a bridge between traditional bedside assessment and algorithm-assisted decision support systems.
4.5. Relevance to Public Health Policy
Our analysis revealed significantly higher IPSSs among patients with lower educational attainment, precarious occupational status and rural residence—findings that mirror research on the social determinants of health and on COPD-related disparities in access and outcomes [
51,
52]. Integrating IPSS into a national electronic registry could enable continuous monitoring of such inequalities and support dynamic resource reallocation, in line with Frohlich and Potvin’s ecosocial perspective on the “determinants of determinants” [
53] and with evidence of rural disadvantage in quality of life and service availability for patients with COPD [
45,
54].
In summary, IPSS addresses important gaps left by traditional composite indices by offering a patient-centred tool that simultaneously quantifies ventilatory impairment and emotional burden. Its internal validation through unsupervised clustering and supervised models, its feasibility in everyday clinical workflows and its compatibility with digital infrastructure recommend IPSS as a promising candidate for individualized clinical decision-making and for health policies adapted to the current socio-epidemiological context. At the same time, external validation in independent cohorts and prospective evaluation against hard clinical outcomes (exacerbations, hospitalizations, mortality) remain essential before IPSS can be adopted as a definitive standard in COPD severity assessment.
5. Limitations of the Study
This study has several limitations. First, its bi-institutional design (psychiatric vs. pulmonology recruitment) may introduce selection/spectrum bias due to differences in referral patterns and the routine use of psychocognitive assessment. Second, major cardiometabolic comorbidities (e.g., heart failure, sleep apnoea, severe obesity) were excluded to reduce confounding during score derivation; however, this limits generalizability to real-world multimorbid COPD, and future studies should validate and, if needed, recalibrate IPSS in broader cohorts, ideally including sensitivity analyses with relaxed exclusions and/or comorbidity-stratified models. Third, IPSS coefficients and cut-offs were derived and internally evaluated in the same dataset; thus, discrimination of cluster membership should be interpreted as internal separability rather than independent validation, and external validation in independent, multi-ethnic cohorts is required. Fourth, the cross-sectional design precludes causal inference and does not allow assessment of longitudinal predictive accuracy against hard endpoints (exacerbations, hospitalisations, mortality or healthcare costs). Fifth, CAT, mMRC and HADS are self-reported measures and are susceptible to measurement error and interviewer/context effects, including cultural and educational influences. Finally, the absence of continuous telemonitoring data (nocturnal SpO2, physical activity) and biological markers limits comparisons with biomarker-enriched indices and the ability to capture rapid clinical changes; additionally, the multiplicative formulation may be sensitive to distributional shifts and should be re-assessed for skewness/outliers during external validation, while the exclusion of cognitive scales from IPSS reflects a feasibility–comprehensiveness trade-off that should be revisited in settings where standardized cognitive testing is systematically available.
6. Conclusions
This study demonstrates that incorporating anxiety and depression into COPD assessment adds clinically relevant information beyond spirometry and dyspnoea scales alone. By combining FEV1%, mMRC, CAT and HADS-based affective scores, the Integrated Pulmonary Severity Score (IPSS) captures a psycho-respiratory phenotype characterized by more severe airflow limitation, higher symptom perception and poorer cognitive performance than that seen in predominantly respiratory profiles.
In our cohort, IPSS showed good internal validity and clearly separated patients into four severity strata (<30, 30–69, 70–119, ≥120 points), which may support graded clinical decisions ranging from routine follow-up to intensified multidisciplinary management. Both logistic regression and a multilayer perceptron achieved high discrimination (AUC 0.95, Cohen’s κ ≥ 0.75) when using the same core variables that informed the clustering and IPSS construction to classify membership in the psycho-respiratory phenotype; therefore, this agreement supports internal (convergent) validity rather than independent validation, while explainable-AI analyses (LIME) consistently highlighted HADS-Anxiety and FEV1% as dominant contributors. These findings suggest that IPSS can complement existing indices by making the emotional burden of COPD quantitatively visible in everyday practice.
At the same time, the score was derived and tested in two tertiary centres, excluded major cardiometabolic comorbidities and lacked longitudinal endpoints such as exacerbations, hospitalisations and mortality. Before routine clinical adoption, IPSS therefore requires external validation in independent populations, potential recalibration of cut-off values and prospective evaluation of its impact on outcomes and resource allocation. If these steps confirm its performance, IPSS could help bridge the gap between physiological impairment and emotional distress in COPD and serve as a template for future multidimensional, explainable prediction models and patient-centred, interdisciplinary care strategies.
Author Contributions
Conceptualization, I.-L.B., D.R. and C.-T.S.; methodology, I.-L.B. and C.-T.S.; software, D.-M.C.; validation, I.-L.B., D.R. and C.-T.S.; formal analysis, I.-L.B., D.R. and D.-M.C.; investigation, I.-L.B., A.-C.B.-C., I.U. and V.G.; resources, I.U., V.G. and C.-T.S.; data curation, A.-C.B.-C. and D.R.; writing—original draft preparation, I.-L.B.; writing—review and editing, D.R., C.-T.S. and A.-C.B.-C.; visualization, I.-L.B. and D.-M.C.; supervision, D.R. and C.-T.S.; project administration, C.-T.S.; funding acquisition, C.-T.S. All authors have read and agreed to the published version of the manuscript.
Funding
The article processing charges were funded by the University of Medicine and Pharmacy of Craiova, Romania.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the University of Medicine and Pharmacy in Craiova (approval number: 196/17 February 2022) and Leamna Pulmonology Hospital (approval number: 6189/13 October 2022).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Data is contained within the article. The original contributions presented in the study are included in the article; further inquiries can be directed to the corresponding authors.
Conflicts of Interest
The author Dragoș-Mihai Cojocaru is affiliated with Sanacare AG. The company had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results. The authors declare no conflicts of interest.
References
- World Health Organization. Chronic Obstructive Pulmonary Disease (COPD). Available online: https://www.who.int/news-room/fact-sheets/detail/chronic-obstructive-pulmonary-disease-(copd) (accessed on 6 November 2024).
- Wang, L.; Yu, Q.; Xiao, J.; Chen, Q.; Fang, M.; Zhao, H. Cigarette Smoke Extract-Treated Mouse Airway Epithelial Cells-Derived Exosomal LncRNA MEG3 Promotes M1 Macrophage Polarization and Pyroptosis in Chronic Obstructive Pulmonary Disease by Upregulating TREM-1 via m6A Methylation. Immune Netw. 2024, 24, e3. [Google Scholar] [CrossRef]
- Shen, Q.; Chen, J.; Yang, S.; Zhang, H.; Yu, H.; Wang, S.; Li, J. Protection against cigarette smoke-induced chronic obstructive pulmonary disease via activation of the SIRT1/FoxO1 axis by targeting microRNA-132. Am. J. Transl. Res. 2024, 16, 5516–5524. [Google Scholar] [CrossRef]
- Wang, J.; Luo, J.; Rotili, D.; Mai, A.; Steegborn, C.; Xu, S.; Jin, Z.G. SIRT6 Protects Against Lipopolysaccharide-Induced Inflammation in Human Pulmonary Lung Microvascular Endothelial Cells. Inflammation 2024, 47, 323–332. [Google Scholar] [CrossRef]
- Zecevic, A.; Blanka-Protic, A.; Jandric, A.; Adzic-Vukicevic, T. Are patients with chronic obstructive pulmonary disease at a greater risk for the development of autoimmune thyroiditis as an adverse event of immunotherapy in non-small cell lung cancer treatment? Pathol. Oncol. Res. 2025, 31, 1612022. [Google Scholar] [CrossRef]
- Bracke, K.R.; Mestdagh, P. MicroRNAs as future therapeutic targets in COPD? Eur. Respir. J. 2017, 49, 1700431. [Google Scholar] [CrossRef] [PubMed]
- Rabe, K.F.; Watz, H. Chronic obstructive pulmonary disease. Lancet 2017, 389, 1931–1940. [Google Scholar] [CrossRef]
- Strollo, H.C.; Nouraie, S.M.; Hoth, K.F.; Riley, C.M.; Karoleski, C.; Zhang, Y.; Hanania, N.A.; Bowler, R.P.; Bon, J.; Sciurba, F.C. Association of systemic inflammation with depressive symptoms in individuals with COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 2021, 16, 2515–2522. [Google Scholar] [CrossRef] [PubMed]
- Donaldson, G.C.; Seemungal, T.A.; Patel, I.S.; Bhowmik, A.; Wilkinson, T.M.; Hurst, J.R.; Maccallum, P.K.; Wedzicha, J.A. Airway and systemic inflammation and decline in lung function in patients with COPD. Chest 2005, 128, 1995–2004. [Google Scholar] [CrossRef]
- Kim, V.; Zhao, H.; Armstrong, H.F.; O’Neal, W.K.; Bailey, K.L.; Rennard, S.I.; Barr, R.G.; Criner, G.J.; Lovasi, G.S.; Morrison, M.F. Elevated systemic biomarkers and persistent anxiety and depression in smokers with and without COPD: An analysis of the SPIROMICS cohort. Eur. Respir. J. 2017, 50, PA4967. [Google Scholar]
- Mobeen, F.; Edgar, R.; Pye, A.; Stockley, R.; Turner, A.M. Effect of depression and anxiety on health status and lung function in patients with alpha 1 antitrypsin deficiency. Thorax 2018, 73, A171. [Google Scholar] [CrossRef]
- Bratek, A.; Zawada, K.; Beil-Gawełczyk, J.; Beil, S.; Sozańska, E.; Krysta, K.; Barczyk, A.; Krupka-Matuszczyk, I.; Pierzchała, W. Depressiveness, symptoms of anxiety and cognitive dysfunctions in patients with asthma and chronic obstructive pulmonary disease (COPD): Possible associations with inflammation markers: A pilot study. J. Neural Transm. 2015, 122, 83–91. [Google Scholar] [CrossRef]
- Wu, K.; Lu, L.; Chen, Y.; Peng, J.; Wu, X.; Tang, G.; Ma, T.; Cheng, J.; Ran, P.; Zhou, Y. Associations of anxiety and depression with prognosis in chronic obstructive pulmonary disease: A systematic review and meta-analysis. Pulmonology 2025, 31, 2438553. [Google Scholar] [CrossRef]
- Giardino, N.D.; Curtis, J.L.; Abelson, J.L.; King, A.P.; Pamp, B.; Liberzon, I.; Martinez, F.J. The impact of panic disorder on interoception and dyspnea reports in chronic obstructive pulmonary disease. Biol. Psychol. 2010, 84, 142–146. [Google Scholar] [CrossRef] [PubMed]
- Mansukhani, M.P.; Kara, T.; Caples, S.M.; Somers, V.K. Chemoreflexes, sleep apnea, and sympathetic dysregulation. Curr. Hypertens. Rep. 2014, 16, 476. [Google Scholar] [CrossRef]
- Ziegler, M.G.; Mills, P.J.; Loredo, J.S.; Ancoli-Israel, S.; Dimsdale, J.E. Effect of continuous positive airway pressure and placebo treatment on sympathetic nervous activity in patients with obstructive sleep apnea. Chest 2001, 120, 887–893. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, C.B.; Schoorlemmer, G.H.; Rocha, A.A.; Cravo, S.L. Increased sympathetic responses induced by chronic obstructive sleep apnea are caused by sleep fragmentation. J. Appl. Physiol. 2020, 129, 163–172. [Google Scholar] [CrossRef] [PubMed]
- Harrison, O.K.; Köchli, L.; Marino, S.; Luechinger, R.; Hennel, F.; Brand, K.; Hess, A.J.; Frässle, S.; Iglesias, S.; Vinckier, F.; et al. Interoception of breathing and its relationship with anxiety. Neuron 2021, 109, 4080–4093.e8. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Zhao, X.; Huang, D.; Dai, Z.; Chen, M.; Li, D.; Wu, B. Outcomes associated with comorbid anxiety and depression among patients with stable COPD: A patient registry study in China. J. Affect. Disord. 2022, 313, 77–83. [Google Scholar] [CrossRef]
- Coelho, R.; Santos, A.S.; Maia, D.; Rosa, R.; Caldeira, V.; Sá, T.; Semedo, L.; Cardoso, J. Symptoms of anxiety and depression in COPD patients. Eur. Respir. J. 2014, 44, P981. [Google Scholar]
- Janssen, D.J.; Spruit, M.A.; Leue, C.; Gijsen, C.; Hameleers, H.; Schols, J.M.; Wouters, E.F. Symptoms of anxiety and depression in COPD patients entering pulmonary rehabilitation. Chron. Respir. Dis. 2010, 7, 147–157. [Google Scholar] [CrossRef]
- Karloh, M.; Pizzichinni, M.M.; Pizzichini, E. Effects of comorbidities on the CAT score: A population-based study. Eur. Respir. J. 2016, 48, PA3705. [Google Scholar]
- Buican, I.L.; Gheorman, V.; Udriştoiu, I.; Olteanu, M.; Rădulescu, D.; Calafeteanu, D.M.; Nemeş, A.F.; Călăraşu, C.; Rădulescu, P.M.; Streba, C.T. Interactions between cognitive, affective, and respiratory profiles in chronic respiratory disorders: A cluster analysis approach. Diagnostics 2024, 14, 1153. [Google Scholar] [CrossRef] [PubMed]
- Howrylak, J.A.; Fuhlbrigge, A.L.; Strunk, R.C.; Zeiger, R.S.; Weiss, S.T.; Raby, B.A. Classification of Childhood Asthma Phenotypes and Long-Term Clinical Responses to Inhaled Anti-inflammatory Medications. J. Allergy Clin. Immunol. 2014, 133, 1289–1300.e12. [Google Scholar] [CrossRef] [PubMed]
- Boussina, A.; Wardi, G.; Shashikumar, S.P.; Malhotra, A.; Zheng, K.; Nemati, S. Representation Learning and Spectral Clustering for the Development and External Validation of Dynamic Sepsis Phenotypes: Observational Cohort Study. J. Med. Internet Res. 2023, 25, e45614. [Google Scholar] [CrossRef] [PubMed]
- Janssens, T.; De Peuter, S.; Stans, L.; Verleden, G.; Troosters, T.; Decramer, M.; Van den Bergh, O. Dyspnea perception in COPD: Association between anxiety, dyspnea-related fear and dyspnea in a pulmonary rehabilitation program. Chest 2011, 140, 618–625. [Google Scholar] [CrossRef]
- Di Marco, F.; Verga, M.; Reggente, M.; Casanova, F.M.; Santus, P.; Blasi, F.; Allegra, L.; Centanni, S. Anxiety and depression in COPD patients: The roles of gender and disease severity. Respir. Med. 2006, 100, 1767–1774. [Google Scholar] [CrossRef]
- Antonelli Incalzi, R.; Marra, C.; Giordano, A.; Calcagni, M.L.; Cappa, A.; Basso, S.; Pagliari, G.; Fuso, L. Cognitive impairment in chronic obstructive pulmonary disease—A neuropsychological and SPECT study. J. Neurol. 2003, 250, 325–332. [Google Scholar] [CrossRef]
- Xu, C.; He, Y.; Zheng, Y.; Zhou, L.; Liu, S.; Wan, Y. Correlation of depression and cognitive function in patients with chronic obstructive pulmonary disease. Chin. J. Gen. Pract. 2013, 12, 59–61. [Google Scholar]
- Uryasev, O.M.; Sidorova, I.V.; Shakhanov, A.V. The cognitive impairment in patients with chronic obstructive pulmonary disease. Pak. J. Med. Health Sci. 2019, 13, 276–279. [Google Scholar]
- Steer, J.; Norman, E.; Afolabi, G.; Gibson, G.J.; Bourke, S.C. Evaluation of the MRC dyspnoea scale and a novel extended version in prediction of in-hospital death and early readmission in acute exacerbations of COPD. Thorax 2010, 65, A76. [Google Scholar] [CrossRef]
- Kwon, N.; Amin, M.; Hui, D.S.; Jung, K.S.; Lim, S.Y.; Ta, H.D.; Thai, T.T.L.; Yunus, F.; Jones, P.W. Validity of the COPD assessment test translated into local languages for Asian patients. Chest 2013, 143, 703–710. [Google Scholar] [CrossRef]
- De Castro, R.A.S.; Zanatta, D.J.M.; Rached, S.Z.; Athanazio, R.A.; de Camargo, A.A.; Cukier, A.; Stelmach, R.; Dal Corso, S.; Lanza, F.C. COPD Assessment Test (CAT): Validity and reproducibility in patients with non-cystic fibrosis bronchiectasis. Eur. Respir. J. 2015, 46, PA2791. [Google Scholar] [CrossRef]
- Lutter, J.I.; Jörres, R.A.; Kahnert, K.; Schwarzkopf, L.; Studnicka, M.; Karrasch, S.; Schulz, H.; Vogelmeier, C.F.; Holle, R.; COSYCONET Study Group. Health-related quality of life associates with change in FEV1 in COPD: Results from the COSYCONET cohort. BMC Pulm. Med. 2020, 20, 148. [Google Scholar] [CrossRef]
- Sanchez-Salcedo, P.; Divo, M.; Casanova, C.; Pinto-Plata, V.; de-Torres, J.P.; Cote, C.; Cabrera, C.; Zagaceta, J.; Rodriguez-Roisin, R.; Zulueta, J.J.; et al. Disease progression in young patients with COPD: Rethinking the Fletcher and Peto model. Eur. Respir. J. 2014, 44, 324–331. [Google Scholar] [CrossRef]
- Bakke, P.S. Forløp av obstruktive lungesykdommer [Course of obstructive lung diseases]. Tidsskr. Nor. Laegeforen. 1993, 113, 177–181. [Google Scholar] [PubMed]
- Divo, M.J.; Marin, J.M.; Casanova, C.; Cabrera Lopez, C.; Pinto-Plata, V.M.; Marin-Oto, M.; Polverino, F.; de-Torres, J.P.; Billheimer, D.; Celli, B.R.; et al. Comorbidities and mortality risk in adults younger than 50 years of age with chronic obstructive pulmonary disease. Respir. Res. 2022, 23, 267. [Google Scholar] [CrossRef]
- Celli, B.R.; Cote, C.G.; Marín, J.M.; Casanova, C.; Montes de Oca, M.; Méndez, R.A.; Pinto-Plata, V.; Cabral, H.J. The body-mass index, airflow obstruction, dyspnea, and exercise capacity index in chronic obstructive pulmonary disease. N. Engl. J. Med. 2004, 350, 1005–1012. [Google Scholar] [CrossRef]
- Espantoso-Romero, M.; Román Rodríguez, M.; Duarte-Pérez, A.; Gonzálvez-Rey, J.; Callejas-Cabanillas, P.A.; Kasuba Lazic, D.; Anta-Agudo, B.; Torán Monserrat, P.; Magallon-Botaya, R.; Gerasimovska Kitanovska, B.; et al. External validation of multidimensional prognostic indices (ADO, BODEx and DOSE) in a primary care international cohort (PROEPOC/COPD cohort). BMC Pulm. Med. 2016, 16, 143. [Google Scholar] [CrossRef]
- Woodruff, P.G.; Barr, R.G.; Bleecker, E.; Christenson, S.A.; Couper, D.; Curtis, J.L.; Gouskova, N.A.; Hansel, N.N.; Hoffman, E.A.; Kanner, R.E.; et al. Clinical significance of symptoms in smokers with preserved pulmonary function. N. Engl. J. Med. 2016, 374, 1811–1821. [Google Scholar] [CrossRef]
- Gogou, E.; Kotsiou, O.S.; Siachpazidou, D.S.; Pinaka, M.; Varsamas, C.; Bardaka, F.; Gerogianni, I.; Hatzoglou, C.; Gourgoulianis, K.I. Underestimation of respiratory symptoms by smokers: A thorn in chronic obstructive pulmonary disease diagnosis. npj Prim. Care Respir. Med. 2021, 31, 14. [Google Scholar] [CrossRef] [PubMed]
- Boeck, L.; Soriano, J.B.; Brusse-Keizer, M.; Blasi, F.; Kostikas, K.; Boersma, W.G.; Milenkovic, B.; Louis, R.; Lacoma, A.; Djamin, R.; et al. Prognostic assessment in COPD without lung function: The B-AE-D indices. Eur. Respir. J. 2016, 47, 1635–1644. [Google Scholar] [CrossRef]
- Ashtiani, M.; Mirzaie, M.; Jafari, M. CINNA: An R/CRAN package to decipher central informative nodes in network analysis. Bioinformatics 2019, 35, 1436–1437. [Google Scholar] [CrossRef] [PubMed]
- Kaur, S.; Gupta, A.; Saxena, R. Identifying central nodes in directed and weighted networks. Int. J. Adv. Comput. Sci. Appl. 2021, 12, 905–914. [Google Scholar] [CrossRef]
- Burkes, R.M.; Gassett, A.J.; Ceppe, A.S.; Anderson, W.; O’Neal, W.K.; Woodruff, P.G.; Krishnan, J.A.; Barr, R.G.; Han, M.K.; Martinez, F.J.; et al. Rural residence and chronic obstructive pulmonary disease exacerbations: Analysis of the SPIROMICS cohort. Ann. Am. Thorac. Soc. 2018, 15, 808–816. [Google Scholar] [CrossRef] [PubMed]
- Picazo, F.; Duan, K.I.; Hee Wai, T.; Hayes, S.; Leonhard, A.G.; Fonseca, G.A.; Plumley, R.; Beaver, K.A.; Donovan, L.M.; Au, D.H.; et al. Rural residence associated with receipt of recommended postdischarge chronic obstructive pulmonary disease care among a cohort of U.S. veterans. Ann. Am. Thorac. Soc. 2025, 22, 515–522. [Google Scholar] [CrossRef]
- Farver Vestergaard, I.; Danielsen, J.T.T.; Løkke, A.; Zachariae, R. Psychosocial intervention in chronic obstructive pulmonary disease: Meta-analysis of randomized controlled trials. Psychosom. Med. 2022, 84, 347–358. [Google Scholar] [CrossRef]
- Zhang, J.H.; Zhang, L.Q.; Yang, Y.P.; Li, X.; Zhang, Y.; Wang, L.Y.; Shi, H.; Jiang, H.; Guo, W.; Mu, L.; et al. Clinical effect of nutritional and psychological intervention combined with pulmonary rehabilitation exercise on patients with chronic obstructive pulmonary disease. Zhonghua Yi Xue Za Zhi 2020, 100, 110–115. [Google Scholar]
- ElShawi, R.; Sherif, Y.; Al-Mallah, M.; Sakr, S. Interpretability in healthcare: A comparative study of local machine learning interpretability techniques. Comput. Intell. 2020, 37, 1633–1650. [Google Scholar] [CrossRef]
- Soujanya, K.J.; Kodipalli, A.; Gosai, S.; Sneha, B.J.; Rao, T. Symptoms-based classification of disease using various ML algorithms and interpretation using LIME and SHAP kernels. In 2024 4th Asian Conference on Innovation in Technology (ASIANCON); IEEE: Piscataway, NJ, USA, 2025; pp. 1–6. [Google Scholar]
- Neadley, K.E.; McMichael, G.; Freeman, T.; Browne Yung, K.; Baum, F.; Pretorius, E.; Taylor, K.; Boyd, M.A. Capturing the social determinants of health at the individual level: A pilot study. Public Health Res. Pract. 2021, 31, 30232008. [Google Scholar] [CrossRef]
- Gaffney, A.W.; Hawks, L.; White, A.C.; Woolhandler, S.; Himmelstein, D.U.; Christiani, D.C.; McCormick, D. Health care disparities across the urban–rural divide: A national study of COPD. J. Rural Health 2019, 35, 449–458. [Google Scholar] [CrossRef]
- Frohlich, K.L.; Potvin, L. Commentary: Structure or agency? The importance of both for addressing social inequalities in health. Int. J. Epidemiol. 2010, 39, 378–379. [Google Scholar] [CrossRef] [PubMed]
- Jackson, B.E.; Coultas, D.B.; Suzuki, S.; Singh, K.P.; Bae, S. Rural–urban disparities in quality of life among patients with COPD. J. Rural Health 2013, 29, S62–S69. [Google Scholar] [CrossRef] [PubMed]
| Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |