Endoscopic Ultrasound View of Pneumatosis Cystoides Intestinalis
Abstract
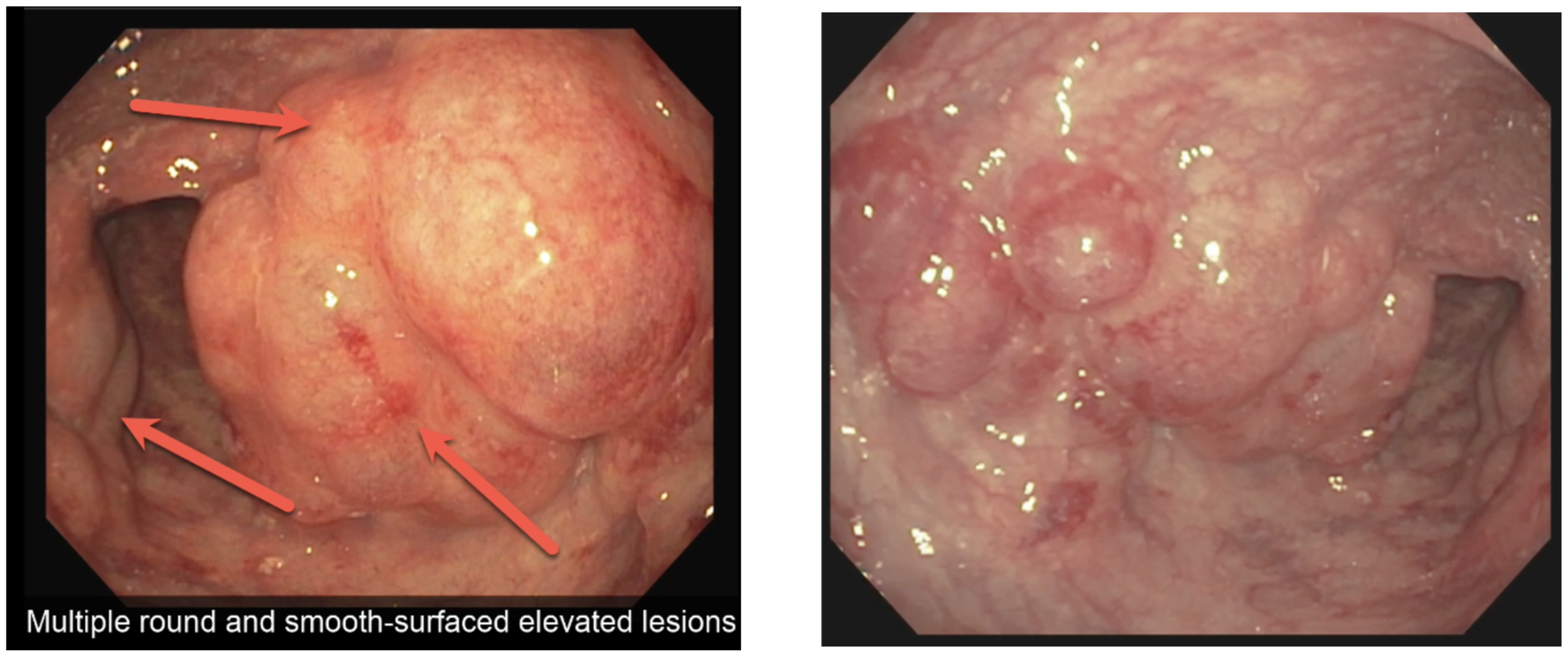
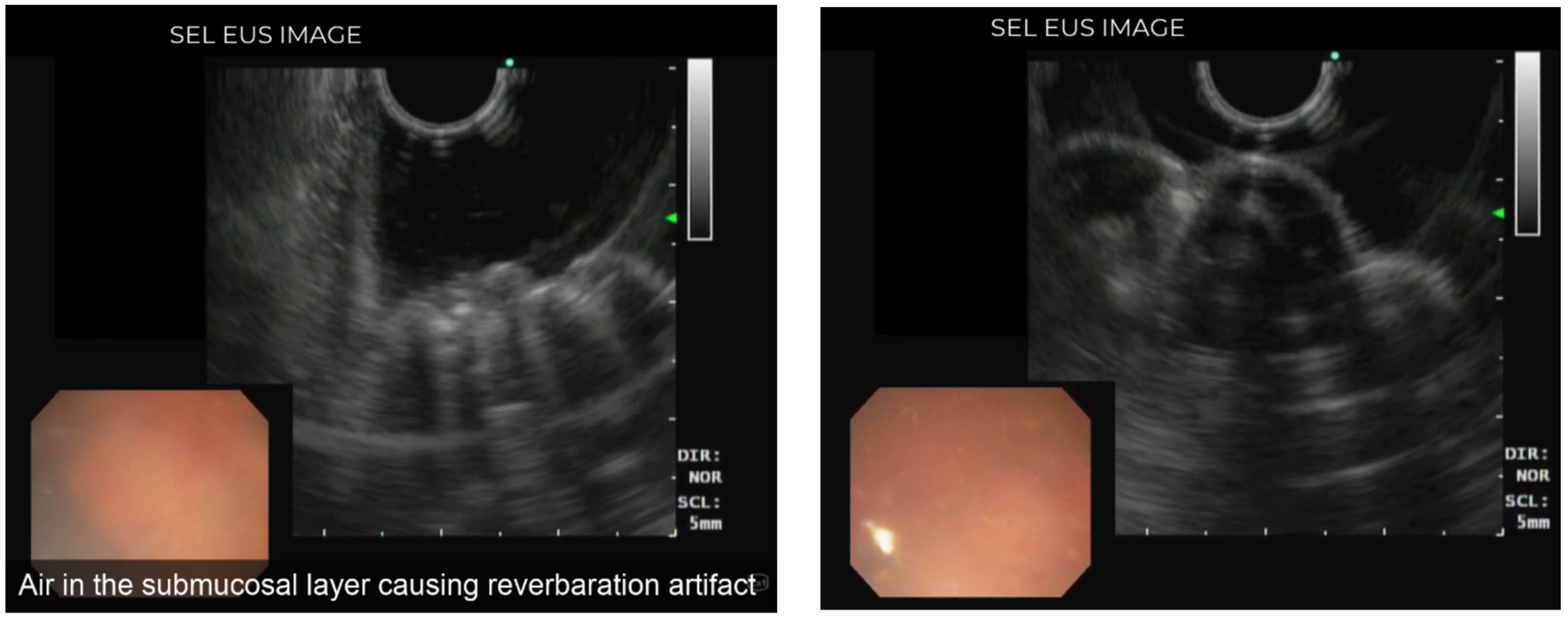
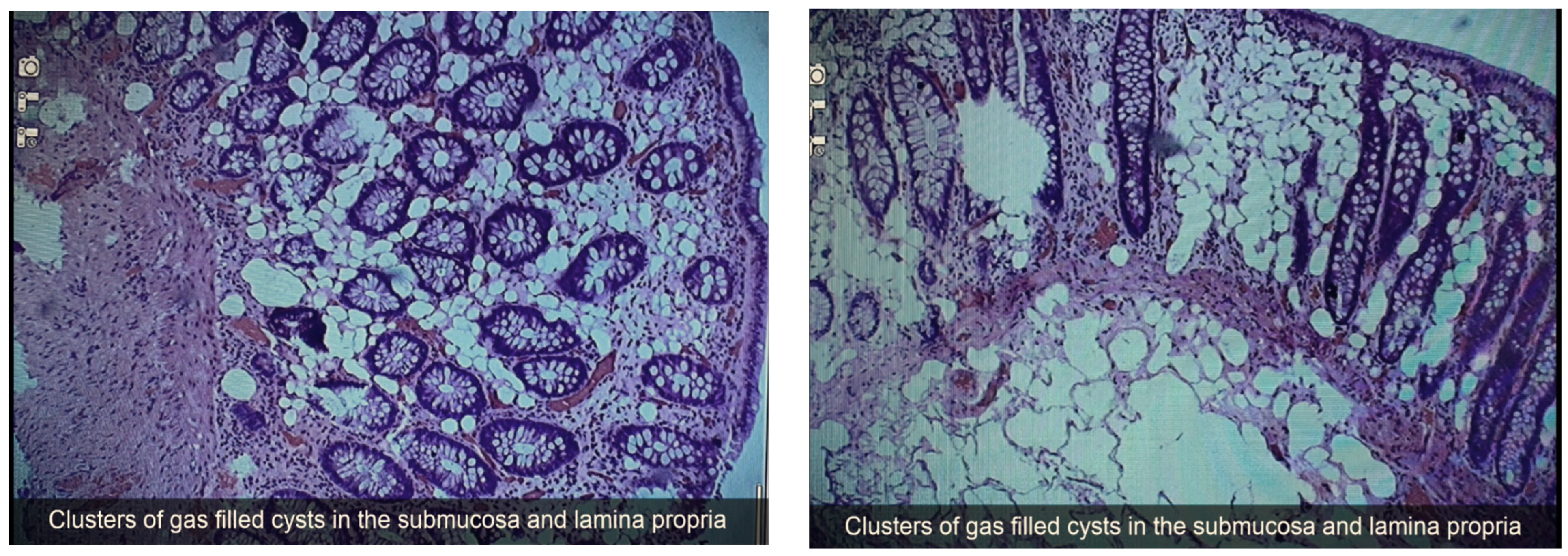
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Piltcher-da-Silva, R.; Sasaki, V.L.; Zangari, M.A.C.; Gallotti, F.M.; Saenger, B.F.; Piltcher-Recuero, M.; de Melo Rocha, G.; da Costa, M.R.; Coelho, J.C.U. Pneumatosis cystoides intestinalis with pneumoperitoneum in an 87-years-old male patient: A case report. J. Surg. Case Rep. 2022, 2022, rjac103. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.L.; Yang, Y.S.; Dou, Y.; Liu, Q.S. A systematic analysis of pneumatosis cystoids intestinalis. World J. Gastroenterol. 2013, 19, 4973–4978. [Google Scholar] [CrossRef] [PubMed]
- Cheng, S.P.; Matuguma, S.E.M.; de Oliveira, G.H.P.M.; Silva, G.L.M.; Cheng, H.P.; Sánchez-Luna, S.A.M.; Minata, M.K.M. Colonoscopic Ultrasound-Guided Fine-Needle Aspiration Using a Curvilinear Array Transducer: A Single-Center Retrospective Cohort Study. Dis. Colon. Rectum. 2022, 65, e80–e84. [Google Scholar] [CrossRef] [PubMed]
- Castro-Poças, F.; Araújo, T.; Pedroto, I. Endoscopic ultrasound of pneumatosis cystoides intestinalis. Endoscopy 2015, 47 (Suppl 1), E274. [Google Scholar] [CrossRef] [PubMed]
- Ling, F.; Guo, D.; Zhu, L. Pneumatosis cystoides intestinalis: A case report and literature review. BMC Gastroenterol. 2019, 19, 176. [Google Scholar] [CrossRef] [PubMed]
- Shimada, M.; Ina, K.; Takahashi, H.; Horiuchi, Y.; Imada, A.; Nishio, Y.; Ando, T.; Kusugami, K. Pneumatosis cystoides intestinalis treated with hyperbaric oxygen therapy: Usefulness of an endoscopic ultrasonic catheter probe for diagnosis. Intern Med. 2001, 40, 896–900. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yvamoto, E.Y.; Cheng, S.; de Oliveira, G.H.P.; Sasso, J.G.R.J.; Boghossian, M.B.; Minata, M.K.; Ribeiro, I.B.; de Moura, E.G.H. Endoscopic Ultrasound View of Pneumatosis Cystoides Intestinalis. Diagnostics 2023, 13, 1424. https://doi.org/10.3390/diagnostics13081424
Yvamoto EY, Cheng S, de Oliveira GHP, Sasso JGRJ, Boghossian MB, Minata MK, Ribeiro IB, de Moura EGH. Endoscopic Ultrasound View of Pneumatosis Cystoides Intestinalis. Diagnostics. 2023; 13(8):1424. https://doi.org/10.3390/diagnostics13081424
Chicago/Turabian StyleYvamoto, Erika Yuki, Spencer Cheng, Guilherme Henrique Peixoto de Oliveira, João Guilherme Ribeiro Jordão Sasso, Mateus Bond Boghossian, Mauricio Kazuyoshi Minata, Igor Braga Ribeiro, and Eduardo Guimarães Hourneaux de Moura. 2023. "Endoscopic Ultrasound View of Pneumatosis Cystoides Intestinalis" Diagnostics 13, no. 8: 1424. https://doi.org/10.3390/diagnostics13081424
APA StyleYvamoto, E. Y., Cheng, S., de Oliveira, G. H. P., Sasso, J. G. R. J., Boghossian, M. B., Minata, M. K., Ribeiro, I. B., & de Moura, E. G. H. (2023). Endoscopic Ultrasound View of Pneumatosis Cystoides Intestinalis. Diagnostics, 13(8), 1424. https://doi.org/10.3390/diagnostics13081424







