Alcohol Consumption and the Risk of Incident Atrial Fibrillation: A Meta-Analysis
Abstract
:1. Introduction
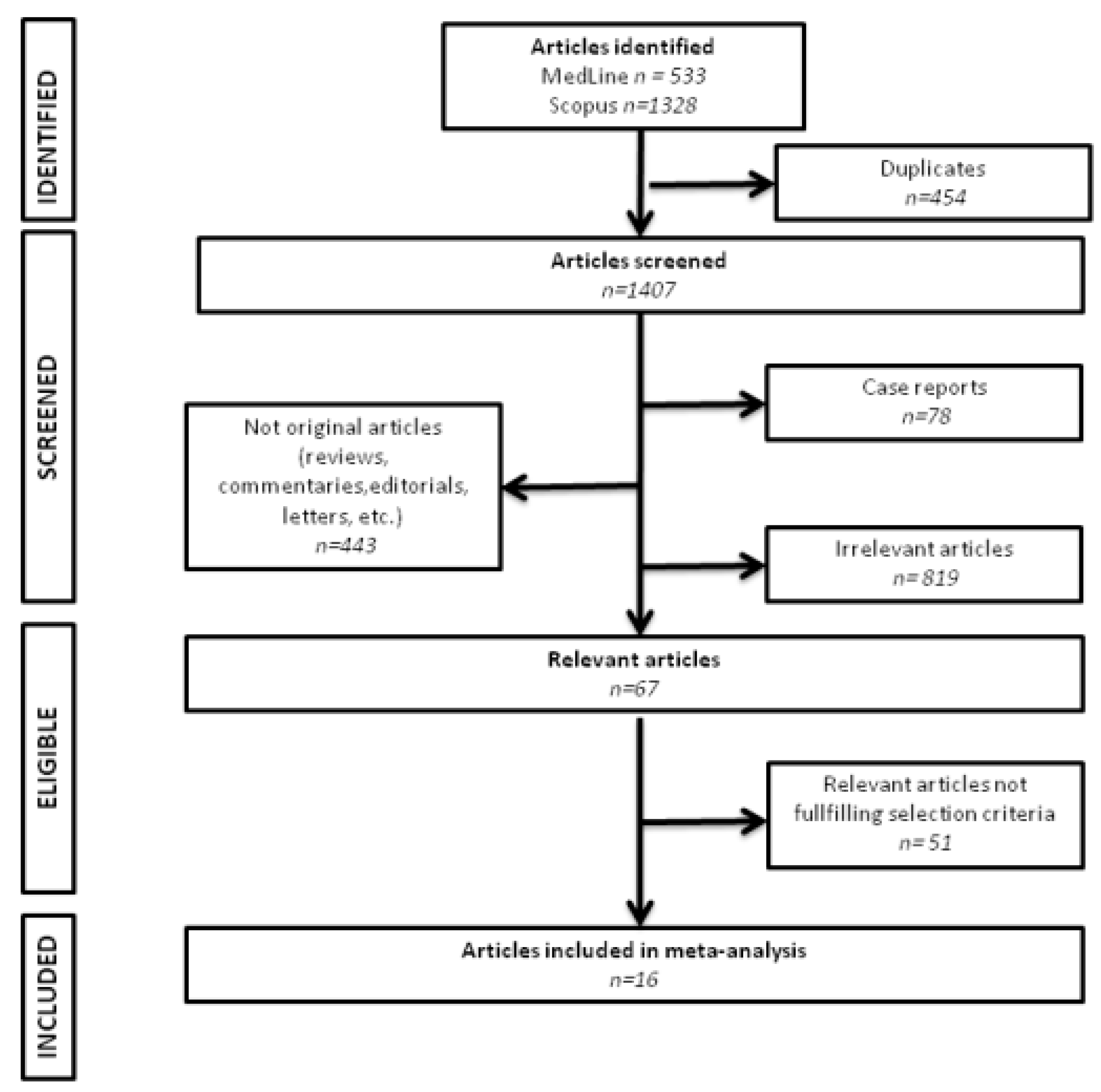
2. Materials and Methods
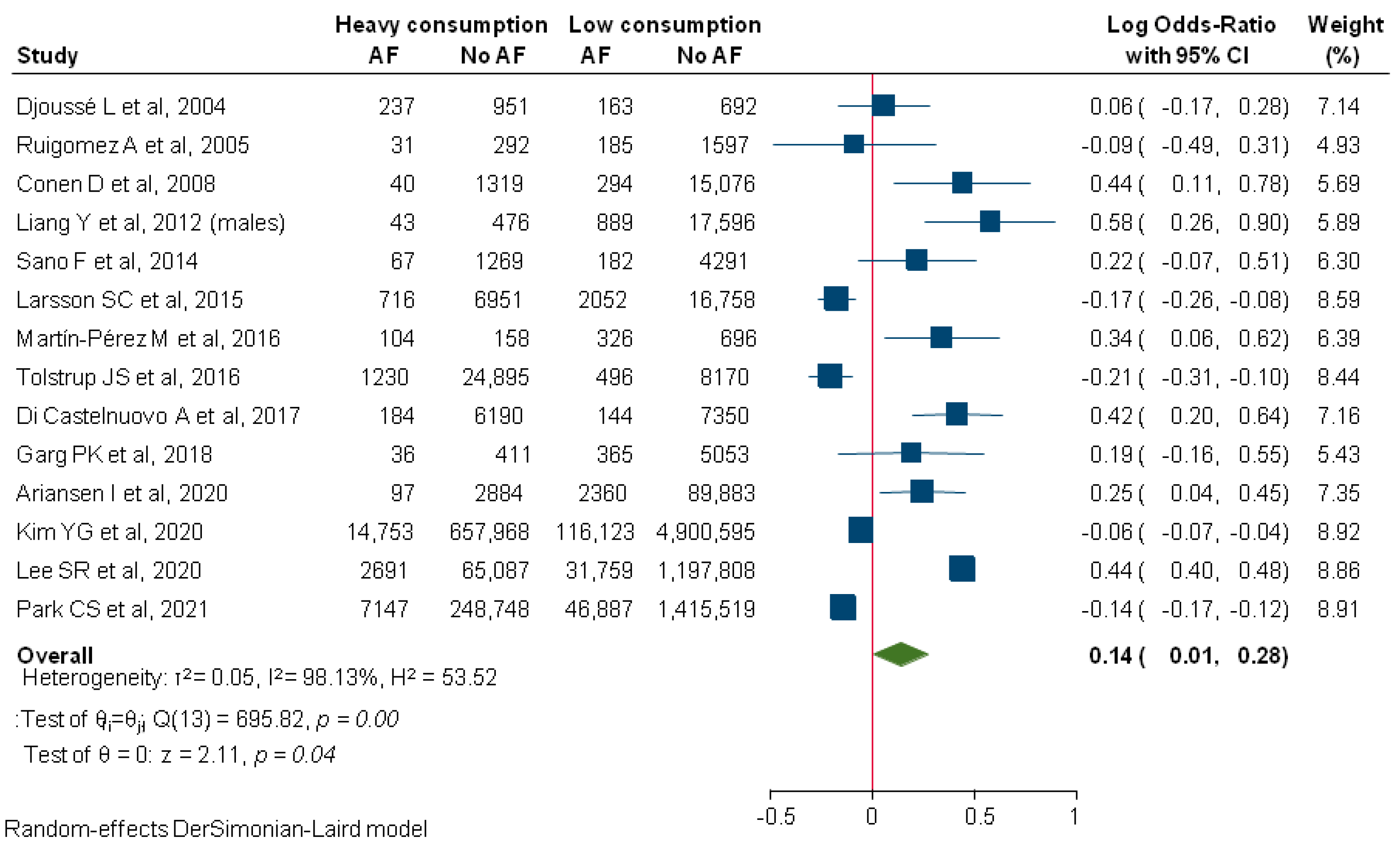
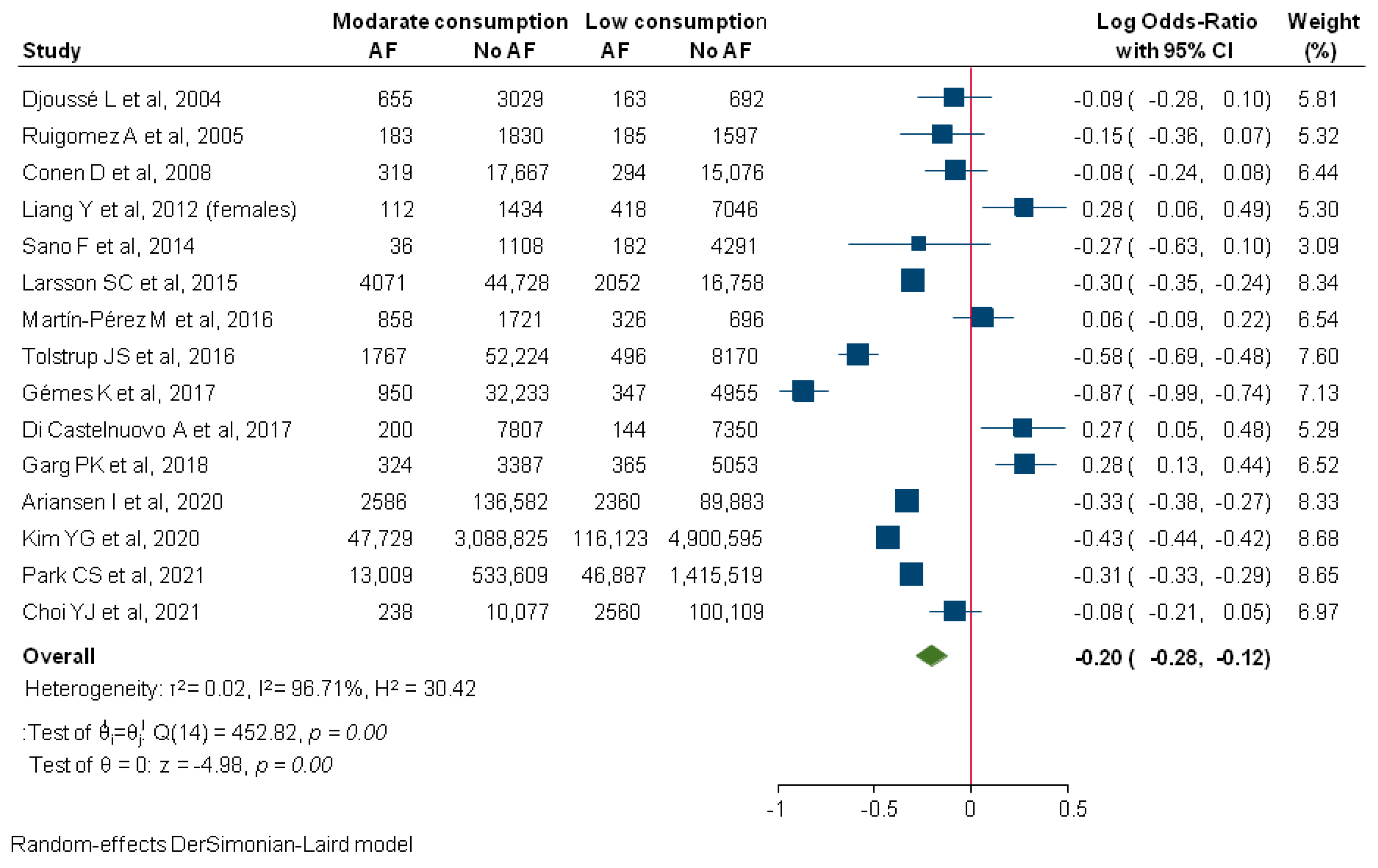
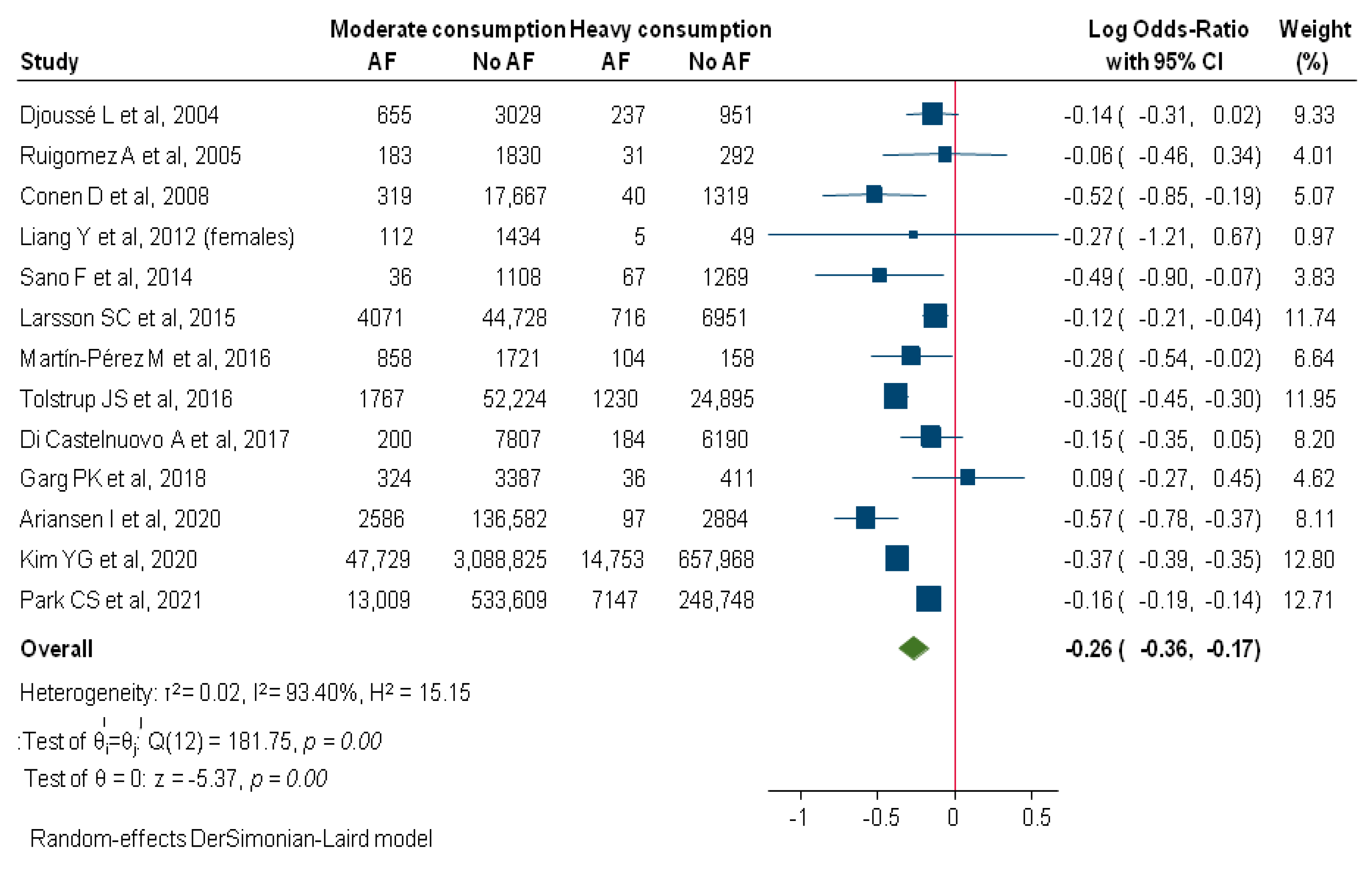
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Conen, D.; Chae, C.U.; Glynn, R.J.; Tedrow, U.B.; Everett, B.M.; Buring, J.E.; Albert, C.M. Risk of death and cardiovascular events in initially healthy women with new-onset atrial fibrillation. JAMA 2011, 305, 2080–2087. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Benjamin, E.J.; Muntner, P.; Alonso, A.; Bittencourt, M.S.; Callaway, C.W.; Carson, A.P.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Das, S.R.; et al. Heart Disease and Stroke Statistics-2019 Update: A Report From the American Heart Association. Circulation 2019, 139, e56–e528. [Google Scholar] [CrossRef] [PubMed]
- Huxley, R.R.; Lopez, F.L.; Folsom, A.R.; Agarwal, S.K.; Loehr, L.R.; Soliman, E.Z.; Maclehose, R.; Konety, S.; Alonso, A. Absolute and attributable risks of atrial fibrillation in relation to optimal and borderline risk factors: The Atherosclerosis Risk in Communities (ARIC) study. Circulation 2011, 123, 1501–1508. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lip, G.Y.H. The ABC pathway: An integrated approach to improve AF management. Nat. Rev. Cardiol. 2017, 14, 627–628. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Lane, D.A.; Wang, L.; Zhang, H.; Wang, H.; Zhang, W.; Wen, J.; Xing, Y.; Wu, F.; Xia, Y.; et al. Mobile Health Technology to Improve Care for Patients With Atrial Fibrillation. J. Am. Coll. Cardiol. 2020, 75, 1523–1534. [Google Scholar] [CrossRef]
- Rienstra, M.; Hobbelt, A.H.; Alings, M.; Tijssen, J.G.P.; Smit, M.D.; Brügemann, J.; Geelhoed, B.; Tieleman, R.G.; Hillege, H.L.; Tukkie, R.; et al. Targeted therapy of underlying conditions improves sinus rhythm maintenance in patients with persistent atrial fibrillation: Results of the RACE 3 trial. Eur. Heart J. 2018, 39, 2987–2996. [Google Scholar] [CrossRef]
- Voskoboinik, A.; Prabhu, S.; Ling, L.H.; Kalman, J.M.; Kistler, P.M. Alcohol and Atrial Fibrillation: A Sobering Review. J. Am. Coll. Cardiol. 2016, 68, 2567–2576. [Google Scholar] [CrossRef] [PubMed]
- Conen, D.; Tedrow, U.B.; Cook, N.R.; Moorthy, M.V.; Buring, J.E.; Albert, C.M. Alcohol consumption and risk of incident atrial fibrillation in women. JAMA 2008, 300, 2489–2496. [Google Scholar] [CrossRef] [Green Version]
- Voskoboinik, A.; Kalman, J.M.; De Silva, A.; Nicholls, T.; Costello, B.; Nanayakkara, S.; Prabhu, S.; Stub, D.; Azzopardi, S.; Vizi, D.; et al. Alcohol Abstinence in Drinkers with Atrial Fibrillation. N. Engl. J. Med. 2020, 382, 20–28. [Google Scholar] [CrossRef]
- Ding, C.; O’Neill, D.; Bell, S.; Stamatakis, E.; Britton, A. Association of alcohol consumption with morbidity and mortality in patients with cardiovascular disease: Original data and meta-analysis of 48,423 men and women. BMC Med. 2021, 19, 167. [Google Scholar] [CrossRef]
- Marcus, G.M.; Vittinghoff, E.; Whitman, I.R.; Joyce, S.; Yang, V.; Nah, G.; Gerstenfeld, E.P.; Moss, J.D.; Lee, R.J.; Lee, B.K.; et al. Acute Consumption of Alcohol and Discrete Atrial Fibrillation Events. Ann. Intern. Med. 2021, 174, 1503–1509. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. J. Clin. Epidemiol. 2009, 62, e1–e34. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- National Institutes of Health. Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies. 2014. Available online: https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools (accessed on 19 December 2021).
- Egger, M.; Smith, G.D.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. Br. Med. J. 1997, 315, 629–634. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ryan, R.; Cochrane Consumers and Communication Review Group. Heterogeneity and subgroup analyses in Cochrane Consumers and Communication Group Reviews: Planning the Analysis at Protocol Stage. Available online: https://cccrg.cochrane.org/sites/cccrg.cochrane.org/files/public/uploads/heterogeneity_subgroup_analyses_revising_december_1st_2016.pdf (accessed on 19 December 2021).
- Harrell, F.E., Jr.; Lee, K.L.; Pollock, B.G. Regression models in clinical studies: Determining relationships between predictors and response. J. Natl. Cancer Inst. 1988, 80, 1198–1202. [Google Scholar] [CrossRef]
- Djoussé, L.; Levy, D.; Benjamin, E.J.; Blease, S.J.; Russ, A.; Larson, M.G.; Massaro, J.M.; D’Agostino, R.B.; Wolf, P.A.; Ellison, R.C. Long-term alcohol consumption and the risk of atrial fibrillation in the Framingham Study. Am. J. Cardiol. 2004, 93, 710–713. [Google Scholar] [CrossRef]
- Ruigómez, A.; Johansson, S.; Wallander, M.A.; García Rodríguez, L.A. Predictors and prognosis of paroxysmal atrial fibrillation in general practice in the UK. BMC Cardiovasc. Disord. 2005, 5, 20. [Google Scholar] [CrossRef] [Green Version]
- Liang, Y.; Mente, A.; Yusuf, S.; Gao, P.; Sleight, P.; Zhu, J.; Fagard, R.; Lonn, E.; Teo, K.K.; ONTARGET and TRANSCEND Investigators. Alcohol consumption and the risk of incident atrial fibrillation among people with cardiovascular disease. CMAJ 2012, 184, E857–E866. [Google Scholar] [CrossRef] [Green Version]
- Sano, F.; Ohira, T.; Kitamura, A.; Imano, H.; Cui, R.; Kiyama, M.; Okada, T.; Yamagishi, K.; Sankai, T.; Tanigawa, T.; et al. Heavy alcohol consumption and risk of atrial fibrillation. The Circulatory Risk in Communities Study (CIRCS). Circ. J. 2014, 78, 955–961. [Google Scholar] [CrossRef] [Green Version]
- Larsson, S.C.; Drca, N.; Wolk, A. Alcohol consumption and risk of atrial fibrillation: A prospective study and dose-response meta-analysis. J. Am. Coll. Cardiol. 2014, 64, 281–289. [Google Scholar] [CrossRef]
- Martín-Pérez, M.; Ruigómez, A.; Michel, A.; García Rodríguez, L.A. Incidence and risk factors for atrial fibrillation in patients with newly diagnosed heart failure. J. Cardiovasc. Med. (Hagerstown) 2016, 17, 608–615. [Google Scholar] [CrossRef]
- Tolstrup, J.S.; Wium-Andersen, M.K.; Ørsted, D.D.; Nordestgaard, B.G. Alcohol consumption and risk of atrial fibrillation: Observational and genetic estimates of association. Eur. J. Prev. Cardiol. 2016, 23, 1514–1523. [Google Scholar] [CrossRef] [PubMed]
- Gémes, K.; Malmo, V.; Laugsand, L.E.; Loennechen, J.P.; Ellekjaer, H.; László, K.D.; Ahnve, S.; Vatten, L.J.; Mukamal, K.J.; Janszky, I. Does Moderate Drinking Increase the Risk of Atrial Fibrillation? The Norwegian HUNT (Nord-Trøndelag Health) Study. J. Am. Heart Assoc. 2017, 6, e007094. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Di Castelnuovo, A.; Costanzo, S.; Bonaccio, M.; Rago, L.; De Curtis, A.; Persichillo, M.; Bracone, F.; Olivieri, M.; Cerletti, C.; Donati, M.B.; et al. Moderate Alcohol Consumption Is Associated with Lower Risk for Heart Failure But Not Atrial Fibrillation. JACC Heart Fail. 2017, 5, 837–844. [Google Scholar] [CrossRef] [PubMed]
- Garg, P.K.; O’Neal, W.T.; Ogunsua, A.; Thacker, E.L.; Howard, G.; Soliman, E.Z.; Cushman, M. Usefulness of the American Heart Association’s Life Simple 7 to Predict the Risk of Atrial Fibrillation (from the REasons for Geographic And Racial Differences in Stroke [REGARDS] Study). Am. J. Cardiol. 2018, 121, 199–204. [Google Scholar] [CrossRef] [PubMed]
- Ariansen, I.; Degerud, E.; Gjesdal, K.; Tell, G.S.; Næss, Ø. Examining the lower range of the association between alcohol intake and risk of incident hospitalization with atrial fibrillation. Int. J. Cardiol. Heart Vasc. 2020, 31, 100679. [Google Scholar] [CrossRef]
- Kim, Y.G.; Han, K.D.; Choi, J.I.; Boo, K.Y.; Kim, D.Y.; Lee, K.N.; Shim, J.; Kim, J.S.; Kim, Y.H. Frequent drinking is a more important risk factor for new-onset atrial fibrillation than binge drinking: A nationwide population-based study. Europace 2020, 22, 216–224. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.R.; Choi, E.K.; Ahn, H.J.; Han, K.D.; Oh, S.; Lip, G.Y.H. Association between clustering of unhealthy lifestyle factors and risk of new-onset atrial fibrillation: A nationwide population-based study. Sci. Rep. 2020, 10, 19224. [Google Scholar] [CrossRef]
- Park, C.S.; Han, K.D.; Choi, E.K.; Kim, D.H.; Lee, H.J.; Lee, S.R.; Oh, S. Lifestyle is associated with atrial fibrillation development in patients with type 2 diabetes mellitus. Sci. Rep. 2021, 11, 4676. [Google Scholar] [CrossRef]
- Choi, Y.J.; Han, K.D.; Choi, E.K.; Jung, J.H.; Lee, S.R.; Oh, S.; Lip, G.Y.H. Alcohol Abstinence and the Risk of Atrial Fibrillation in Patients With Newly Diagnosed Type 2 Diabetes Mellitus: A Nationwide Population-Based Study. Diabetes Care 2021, 44, 1393–1401. [Google Scholar] [CrossRef]
- Gallagher, C.; Hendriks, J.M.L.; Elliott, A.D.; Wong, C.X.; Rangnekar, G.; Middeldorp, M.E.; Mahajan, R.; Lau, D.H.; Sanders, P. Alcohol and incident atrial fibrillation—A systematic review and meta-analysis. Int. J.Cardiol. 2017, 246, 46–52. [Google Scholar] [CrossRef]
- Kodama, S.; Saito, K.; Tanaka, S.; Horikawa, C.; Saito, A.; Heianza, Y.; Anasako, Y.; Nishigaki, Y.; Yachi, Y.; Iida, K.T.; et al. Alcohol consumption and risk of atrial fibrillation: A meta-analysis. J. Am. Coll. Cardiol. 2011, 57, 427–436. [Google Scholar] [CrossRef] [Green Version]
- Samokhvalov, A.V.; Irving, H.M.; Rehm, J. Alcohol consumption as a risk factor for atrial fibrillation: A systematic review and meta-analysis. Eur. J. Cardiovasc. Prev. Rehabil. 2010, 17, 706–712. [Google Scholar] [CrossRef] [Green Version]
- Yoon, S.J.; Jung, J.G.; Lee, S.; Kim, J.S.; Ahn, S.K.; Shin, E.S.; Jang, J.E.; Lim, S.H. The protective effect of alcohol consumption on the incidence of cardiovascular diseases: Is it real? A systematic review and meta-analysis of studies conducted in community settings. BMC Public Health 2020, 20, 90. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Li, X.H.; Yu, F.F.; Zhou, Y.H.; He, J. Association between alcohol consumption and the risk of incident type 2 diabetes: A systematic review and dose-response meta-analysis. Am. J. Clin. Nutr. 2016, 103, 818–829. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Larsson, S.C.; Wallin, A.; Wolk, A. Alcohol consumption and risk of heart failure: Meta-analysis of 13 prospective studies. Clin. Nutr. 2018, 37, 1247–1251. [Google Scholar] [CrossRef]
- Ronksley, P.E.; Brien, S.E.; Turner, B.J.; Mukamal, K.J.; Ghali, W.A. Association of alcohol consumption with selected cardiovascular disease outcomes: A systematic review and meta-analysis. BMJ 2011, 342, d671. [Google Scholar] [CrossRef] [Green Version]
- Yuan, H.C.; Yu, Q.T.; Bai, H.; Xu, H.Z.; Gu, P.; Chen, L.Y. Alcohol intake and the risk of chronic kidney disease: Results from a systematic review and dose-response meta-analysis. Eur. J. Clin. Nutr. 2021, 75, 1555–1567. [Google Scholar] [CrossRef] [PubMed]
- Kaluza, J.; Harris, H.R.; Linden, A.; Wolk, A. Alcohol Consumption and Risk of Chronic Obstructive Pulmonary Disease: A Prospective Cohort Study of Men. Am. J. Epidemiol. 2019, 188, 907–916. [Google Scholar] [CrossRef]
- Mezue, K.; Abbas, T.; Radfar, A.; Zureigat, H.; Abohashem, S.; Shin, L.; Pitman, R.; Osborne, M.; Tawakol, A. Alcohol’s Beneficial Effect on Cardiovascular Disease Is Partially Mediated through Modulation of Stress-Associated Brain Activity. J. Am. Coll. Cardiol. 2021, 77 (Suppl. 2), 6. [Google Scholar] [CrossRef]
- Briasoulis, A.; Agarwal, V.; Messerli, F.H. Alcohol consumption and the risk of hypertension in men and women: A systematic review and meta-analysis. J. Clin. Hypertens. (Greenwich) 2012, 14, 792–798. [Google Scholar] [CrossRef]
- Roerecke, M.; Tobe, S.W.; Kaczorowski, J.; Bacon, S.L.; Vafaei, A.; Hasan, O.S.M.; Krishnan, R.J.; Raifu, A.O.; Rehm, J. Sex-Specific Associations Between Alcohol Consumption and Incidence of Hypertension: A Systematic Review and Meta-Analysis of Cohort Studies. J. Am. Heart Assoc. 2018, 7, e008202. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Voskoboinik, A.; Wong, G.; Lee, G.; Nalliah, C.; Hawson, J.; Prabhu, S.; Sugumar, H.; Ling, L.H.; McLellan, A.; Morton, J.; et al. Moderate alcohol consumption is associated with atrial electrical and structural changes: Insights from high-density left atrial electroanatomic mapping. Heart Rhythm 2019, 16, 251–259. [Google Scholar] [CrossRef] [PubMed]
- Hung, C.L.; Gonçalves, A.; Lai, Y.J.; Lai, Y.H.; Sung, K.T.; Lo, C.I.; Liu, C.C.; Kuo, J.Y.; Hou, C.J.; Chao, T.F.; et al. Light to Moderate Habitual Alcohol Consumption Is Associated with Subclinical Ventricular and Left Atrial Mechanical Dysfunction in an Asymptomatic Population: Dose-Response and Propensity Analysis. J. Am. Soc. Echocardiogr. 2016, 29, 1043–1051. [Google Scholar] [CrossRef] [PubMed]
- Djoussé, L.; Hunt, S.C.; Eckfeldt, J.H.; Arnett, D.K.; Province, M.A.; Ellison, R.C. Alcohol consumption and plasma atrial natriuretic peptide (from the HyperGEN study). Am. J. Cardiol. 2006, 98, 628–632. [Google Scholar] [CrossRef] [PubMed]
- Voskoboinik, A.; Costello, B.T.; Kalman, E.; Prabhu, S.; Sugumar, H.; Wong, G.; Nalliah, C.; Ling, L.H.; McLellan, A.; Hettige, T.; et al. Regular Alcohol Consumption Is Associated With Impaired Atrial Mechanical Function in the Atrial Fibrillation Population: A Cross-Sectional MRI-Based Study. JACC Clin. Electrophysiol. 2018, 4, 1451–1459. [Google Scholar] [CrossRef] [PubMed]
- Singh, K.J.; Cohen, B.E.; Na, B.; Regan, M.; Schiller, N.B.; Whooley, M.A. Alcohol consumption and 5-year change in left atrial volume among patients with coronary heart disease: Results from the Heart and Soul study. J. Card. Fail. 2013, 19, 183–189. [Google Scholar] [CrossRef]
| Study | Region | Follow-Up (Years) | Method of AF Diagnosis | N | Males (%) | Age | BMI | HT (%) | DM (%) | Sm (%) |
|---|---|---|---|---|---|---|---|---|---|---|
| Djoussé L et al., 2004 | US | >50 | ECG | 5727 | 51 | 45.8 8.04 | NA | NA | 12 | NA |
| Ruigómez A et al., 2005 | UK | 2.7 | ICD | 5525 | 47.2 | NA | NA | 19.1 | 4.2 | 29.7 |
| Conen D et al., 2008 | U.S. | 12.4 | ECG. medical records | 34.715 | 0 | 53.1 7.1 | 24.9 4.5 | 25.3 | 2.4 | 48.5 |
| Liang Y et al., 2012 | Multi-center | 4.6 | ECG | 30.433 | 70 | 66.4 7.2 | NA | 70 | 37.2 | 62.3 |
| Sano F et al., 2014 | Japan | 6.4 | ECG. medical records | 8284 | 35.7 | 56 | NA | 30.2 | NA | 18.6 |
| Larsson SC et al., 2015 | Sweden | 12 | ICD. ECG | 75.276 | 58.2 | 60.5 | 25.4 | 22.3 | 7 | 23.9 |
| Martín-Pérez M et al., 2016 | UK | 2.7 | medical records | 4489 | 55 | NA | NA | NA | NA | 58.7 |
| Tolstrup JS et al., 2016 | Denmark | 6.1 | ICD | 88.782 | 45.1 | 57.4 14.5 | 25.4 4.1 | 18.1 | 3.7 | 22.3 |
| Gémes K et al., 2017 | Norway | 8 | ECG | 47.002 | 44.9 | 52.3 15.7 | 27.1 4.4 | NA | NA | 55.9 |
| Di Castelnuovo A et al., 2017 | Italy | 8.2 | medical records | 22.065 | 48.6 | 55.3 11.9 | 28 4.6 | 55.7 | 9.2 | 23.6 |
| Garg PK et al., 2018 | U.S. | 9.4 | ECG. self-reports | 9576 | 42.6 | 63.3 8.1 | 29 6 | NA | NA | 12.6 |
| Ariansen I et al., 2020 (males) | Norway | 9 | hospital discharge diagnosis | 234.392 | 48.4 | 43.5 10 | 25.6 3.8 | NA | 1.2 | 63.4 |
| Kim YG et al., 2020 | Korea | NA | ICD | 9.776.956 | 54.7 | 47 14.1 | 23.7 3.2 | 25.4 | 8.6 | 40.4 |
| Lee SR et al., 2020 | Korea | 5 | ICD | 1.719.401 | 46 | 66 0 | 24.3 3 | 53 | 20.5 | 30.6 |
| Park CS et al., 2021 | Korea | 7.1 | ICD | 2.551.036 | 59.9 | 57.7 11.9 | NA | 56.8 | 100 | 44.1 |
| Choi YJ et al., 2021 | Korea | 4 | ICD | 112.984 | 35 | 63.3 10.6 | 25.1 3.3 | 21.7 | 100 | 23.8 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Giannopoulos, G.; Anagnostopoulos, I.; Kousta, M.; Vergopoulos, S.; Deftereos, S.; Vassilikos, V. Alcohol Consumption and the Risk of Incident Atrial Fibrillation: A Meta-Analysis. Diagnostics 2022, 12, 479. https://doi.org/10.3390/diagnostics12020479
Giannopoulos G, Anagnostopoulos I, Kousta M, Vergopoulos S, Deftereos S, Vassilikos V. Alcohol Consumption and the Risk of Incident Atrial Fibrillation: A Meta-Analysis. Diagnostics. 2022; 12(2):479. https://doi.org/10.3390/diagnostics12020479
Chicago/Turabian StyleGiannopoulos, Georgios, Ioannis Anagnostopoulos, Maria Kousta, Stavros Vergopoulos, Spyridon Deftereos, and Vassilios Vassilikos. 2022. "Alcohol Consumption and the Risk of Incident Atrial Fibrillation: A Meta-Analysis" Diagnostics 12, no. 2: 479. https://doi.org/10.3390/diagnostics12020479
APA StyleGiannopoulos, G., Anagnostopoulos, I., Kousta, M., Vergopoulos, S., Deftereos, S., & Vassilikos, V. (2022). Alcohol Consumption and the Risk of Incident Atrial Fibrillation: A Meta-Analysis. Diagnostics, 12(2), 479. https://doi.org/10.3390/diagnostics12020479







