Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management
Abstract
1. Introduction
2. Etiologies and Classifications
3. Diagnostic Approach
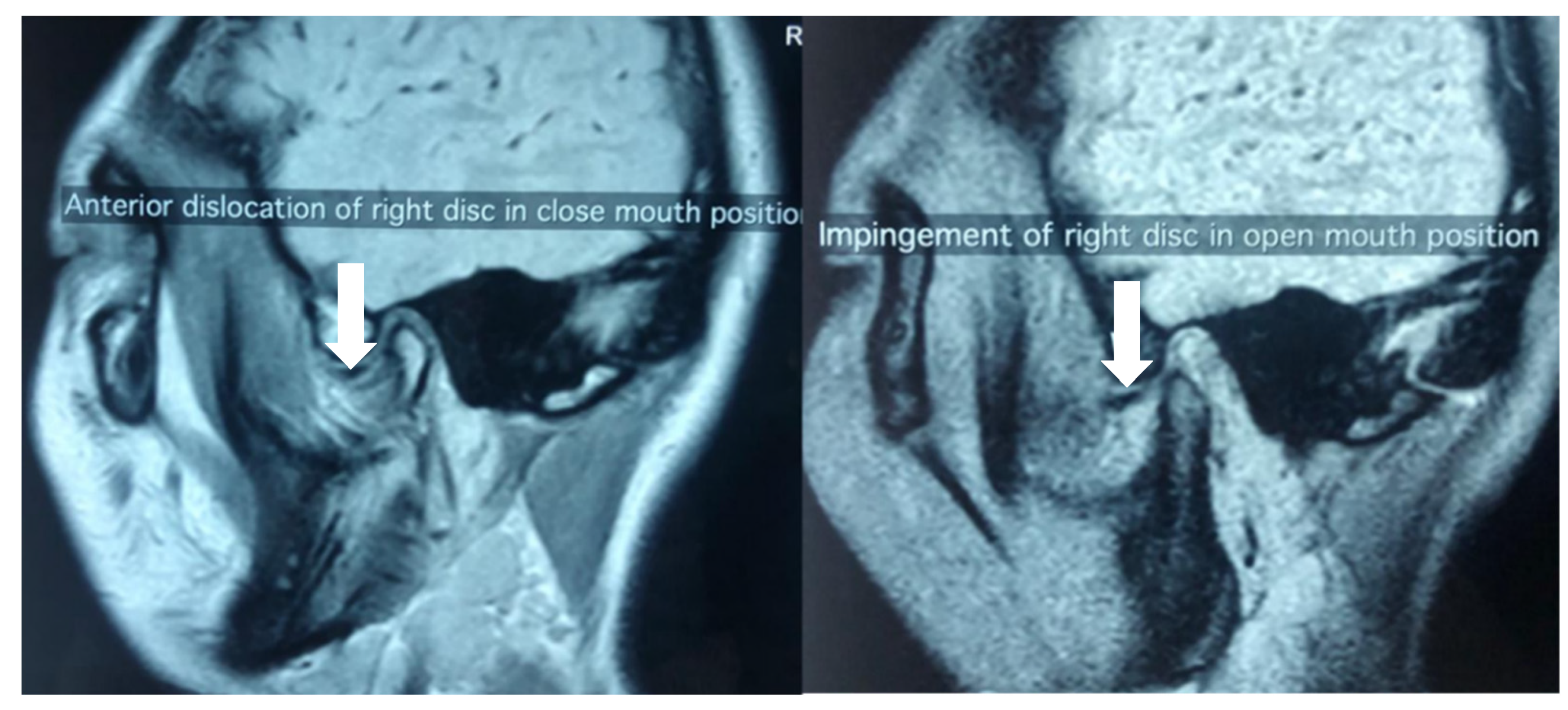
3.1. Imaging and Other Investigations
3.2. Diagnosis of TMD
4. Treatment Modalities—A Change in Paradigm?
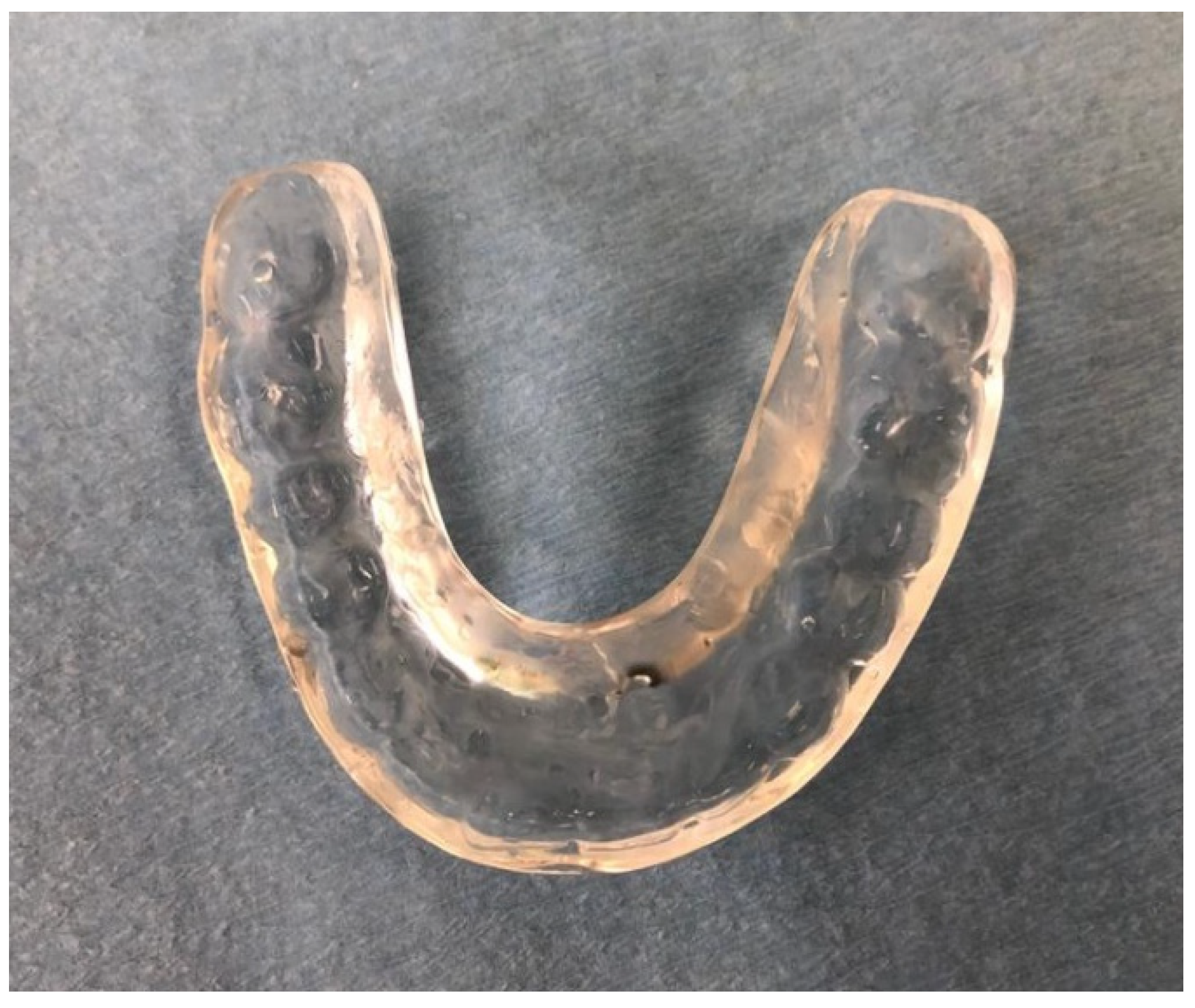
4.1. Conservative Options
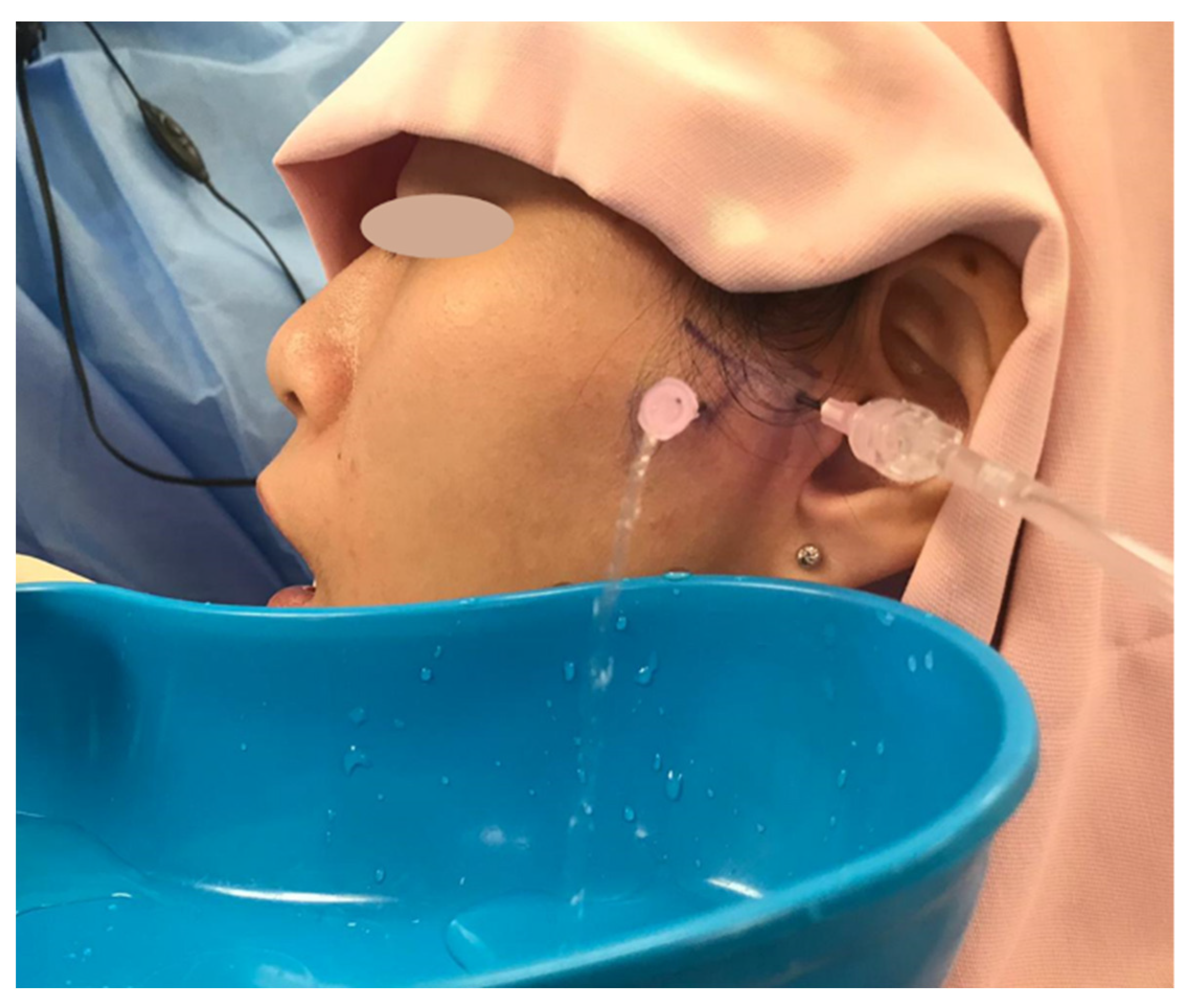
4.2. Minimally Invasive Options—Arthroscopy, Arthrocentesis and Intra-Articular Injections
4.3. Open Joint Surgery
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Von Korff, M.; Ormel, J.; Keefe, F.J.; Dworkin, S.F. Grading the severity of chronic pain. Pain 1992, 50, 133–149. [Google Scholar] [CrossRef]
- Ismail, F.; Eisenburger, M.; Lange, K.; Schneller, T.; Schwabe, L.; Strempel, J.; Stiesch, M. Identification of psychological comorbidity in TMD-patients. Cranio 2016, 34, 182–187. [Google Scholar] [CrossRef] [PubMed]
- List, T.; Jensen, R.H. Temporomandibular disorders: Old ideas and new concepts. Cephalalgia 2017, 37, 692–704. [Google Scholar] [CrossRef] [PubMed]
- Bitiniene, D.; Zamaliauskiene, R.; Kubilius, R.; Leketas, M.; Gailius, T.; Smirnovaite, K. Quality of life in patients with temporomandibular disorders. A systematic review. Stomatologija 2018, 20, 3–9. [Google Scholar] [PubMed]
- Resende, C.; Rocha, L.; Paiva, R.P.; Cavalcanti, C.D.S.; Almeida, E.O.; Roncalli, A.G.; Barbosa, G.A.S. Relationship between anxiety, quality of life, and sociodemographic characteristics and temporomandibular disorder. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2020, 129, 125–132. [Google Scholar] [CrossRef] [PubMed]
- Dahlstrom, L.; Carlsson, G.E. Temporomandibular disorders and oral health-related quality of life. A systematic review. Acta Odontol. Scand. 2010, 68, 80–85. [Google Scholar] [CrossRef]
- Goncalves, D.A.; Camparis, C.M.; Speciali, J.G.; Franco, A.L.; Castanharo, S.M.; Bigal, M.E. Temporomandibular disorders are differentially associated with headache diagnoses: A controlled study. Clin. J. Pain 2011, 27, 611–615. [Google Scholar] [CrossRef]
- Lim, P.F.; Smith, S.; Bhalang, K.; Slade, G.D.; Maixner, W. Development of temporomandibular disorders is associated with greater bodily pain experience. Clin. J. Pain 2010, 26, 116–120. [Google Scholar] [CrossRef] [PubMed]
- Facial Pain. Available online: http://www.nidcr.nih.gov/DataStatistics/FindDataByTopic/FacialPain/ (accessed on 9 June 2019).
- Lipton, J.A.; Ship, J.A.; Larach-Robinson, D. Estimated prevalence and distribution of reported orofacial pain in the United States. J. Am. Dental Assoc. 1993, 124, 115–121. [Google Scholar] [CrossRef] [PubMed]
- Locker, D.; Slade, G. Prevalence of symptoms associated with temporomandibular disorders in a Canadian population. Community Dent. Oral Epidemiol. 1988, 16, 310–313. [Google Scholar] [CrossRef]
- Magnusson, T.; Egermark, I.; Carlsson, G.E. A longitudinal epidemiologic study of signs and symptoms of temporomandibular disorders from 15 to 35 years of age. J. Orofac. Pain 2000, 14, 310–319. [Google Scholar]
- Ebrahimi, M.; Dashti, H.; Mehrabkhani, M.; Arghavani, M.; Daneshvar-Mozafari, A. Temporomandibular Disorders and Related Factors in a Group of Iranian Adolescents: A Cross-sectional Survey. J. Dent. Res. Dent. Clin. Dent. Prospect. 2011, 5, 123–127. [Google Scholar] [CrossRef]
- Manfredini, D.; Piccotti, F.; Ferronato, G.; Guarda-Nardini, L. Age peaks of different RDC/TMD diagnoses in a patient population. J. Dent. 2010, 38, 392–399. [Google Scholar] [CrossRef] [PubMed]
- Klatkiewicz, T.; Gawriolek, K.; Pobudek Radzikowska, M.; Czajka-Jakubowska, A. Ultrasonography in the Diagnosis of Temporomandibular Disorders: A Meta-Analysis. Med. Sci. Monit. 2018, 24, 812–817. [Google Scholar] [CrossRef] [PubMed]
- Sena, M.F.; Mesquita, K.S.; Santos, F.R.; Silva, F.W.; Serrano, K.V. Prevalence of temporomandibular dysfunction in children and adolescents. Rev. Paul. Pediatr. 2013, 31, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Valesan, L.F.; Da-Cas, C.D.; Reus, J.C.; Denardin, A.C.S.; Garanhani, R.R.; Bonotto, D.; Januzzi, E.; de Souza, B.D.M. Prevalence of temporomandibular joint disorders: A systematic review and meta-analysis. Clin. Oral Investig. 2021. [Google Scholar] [CrossRef] [PubMed]
- Rollman, G.B.; Gillespie, J.M. The role of psychosocial factors in temporomandibular disorders. Curr. Rev. Pain 2000, 4, 71–81. [Google Scholar] [CrossRef] [PubMed]
- Auerbach, S.M.; Laskin, D.M.; Frantsve, L.M.; Orr, T. Depression, pain, exposure to stressful life events, and long-term outcomes in temporomandibular disorder patients. J. Oral Maxillofac. Surg. 2001, 59, 628–633. [Google Scholar] [CrossRef]
- Toh, A.Q.J.; Chan, J.L.H.; Leung, Y.Y. Mandibular asymmetry as a possible etiopathologic factor in temporomandibular disorder: A prospective cohort of 134 patients. Clin. Oral Investig. 2021. [Google Scholar] [CrossRef] [PubMed]
- Wilkes, C.H. Internal Derangements of the Temporomandibular Joint: Pathological Variations. Arch. Otolaryngol. Head Neck Surg. 1989, 115, 469–477. [Google Scholar] [CrossRef]
- Mercuri, L.G. Osteoarthritis, osteoarthrosis, and idiopathic condylar resorption. Oral Maxillofac. Surg. Clin. N. Am. 2008, 20, 169–183. [Google Scholar] [CrossRef]
- Bertram, S.; Rudisch, A.; Innerhofer, K.; Pümpel, E.; Grubwieser, G.; Emshoff, R. Diagnosing TMJ internal derangement and osteoarthritis with magnetic resonance imaging. J. Am. Dent. Assoc. 2001, 132, 753–761. [Google Scholar] [CrossRef]
- Turk, D.C.; Gatchel, R.J. Psychological Approaches to Pain Management: A Practitioner’s Hand Book; The Gilford Press: New York, NY, USA, 2002. [Google Scholar]
- Dworkin, S.F.; Massoth, D.L. Temporomandibular disorders and chronic pain: Disease or illness? J. Prosthet. Dent. 1994, 72, 29–38. [Google Scholar] [CrossRef]
- Suvinen, T.I.; Reade, P.C. Temporomandibular disorders: A critical review of the nature of pain and its assessment. J. Orofac. Pain 1995, 9, 317–339. [Google Scholar] [PubMed]
- Yap, A.U.; Tan, K.B.; Chua, E.K.; Tan, H.H. Depression and somatization in patients with temporomandibular disorders. J. Prosthet. Dent. 2002, 88, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Saccomanno, S.; Bernabei, M.; Scoppa, F.; Pirino, A.; Mastrapasqua, R.; Visco, M.A. Coronavirus Lockdown as a Major Life Stressor: Does It Affect TMD Symptoms? Int. J. Environ. Res. Public Health 2020, 17, 8907. [Google Scholar] [CrossRef]
- Medeiros, R.A.; Vieira, D.L.; Silva, E.; Rezende, L.; Santos, R.W.D.; Tabata, L.F. Prevalence of symptoms of temporomandibular disorders, oral behaviors, anxiety, and depression in Dentistry students during the period of social isolation due to COVID-19. J. Appl. Oral Sci. 2020, 28, e20200445. [Google Scholar] [CrossRef]
- Fillingim, R.B.; Ohrbach, R.; Greenspan, J.D.; Knott, C.; Diatchenko, L.; Dubner, R.; Bair, E.; Baraian, C.; Mack, N.; Slade, G.D.; et al. Psychological factors associated with development of TMD: The OPPERA prospective cohort study. J. Pain Off. J. Am. Pain Soc. 2013, 14, T75–T90. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, E.; Ohrbach, R.; Truelove, E.; Look, J.; Anderson, G.; Goulet, J.P.; List, T.; Svensson, P.; Gonzalez, Y.; Lobbezoo, F.; et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: Recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Groupdagger. J. Oral Facial Pain Headache 2014, 28, 6–27. [Google Scholar] [CrossRef] [PubMed]
- Peck, C.C.; Goulet, J.P.; Lobbezoo, F.; Schiffman, E.L.; Alstergren, P.; Anderson, G.C.; de Leeuw, R.; Jensen, R.; Michelotti, A.; Ohrbach, R.; et al. Expanding the taxonomy of the diagnostic criteria for temporomandibular disorders. J. Oral Rehabil. 2014, 41, 2–23. [Google Scholar] [CrossRef] [PubMed]
- Al-Saleh, M.A.; Alsufyani, N.A.; Saltaji, H.; Jaremko, J.L.; Major, P.W. MRI and CBCT image registration of temporomandibular joint: A systematic review. J. Otolaryngol. Head Neck Surg. 2016, 45, 30. [Google Scholar] [CrossRef]
- Al-Saleh, M.A.; Jaremko, J.L.; Alsufyani, N.; Jibri, Z.; Lai, H.; Major, P.W. Assessing the reliability of MRI-CBCT image registration to visualize temporomandibular joints. Dentomaxillofac. Radiol. 2015, 44, 20140244. [Google Scholar] [CrossRef] [PubMed]
- Ladeira, D.B.; da Cruz, A.D.; de Almeida, S.M. Digital panoramic radiography for diagnosis of the temporomandibular joint: CBCT as the gold standard. Braz. Oral Res. 2015, 29, S1806-83242015000100303. [Google Scholar] [CrossRef]
- Larheim, T.A.; Abrahamsson, A.K.; Kristensen, M.; Arvidsson, L.Z. Temporomandibular joint diagnostics using CBCT. Dentomaxillofac. Radiol. 2015, 44, 20140235. [Google Scholar] [CrossRef]
- Su, N.; van Wijk, A.J.; Visscher, C.M.; Lobbezoo, F.; van der Heijden, G. Diagnostic value of ultrasonography for the detection of disc displacements in the temporomandibular joint: A systematic review and meta-analysis. Clin. Oral Investig. 2018, 22, 2599–2614. [Google Scholar] [CrossRef]
- Talmaceanu, D.; Lenghel, L.M.; Bolog, N.; Popa Stanila, R.; Buduru, S.; Leucuta, D.C.; Rotar, H.; Baciut, M.; Baciut, G. High-resolution ultrasonography in assessing temporomandibular joint disc position. Med. Ultrason. 2018, 1, 64–70. [Google Scholar] [CrossRef]
- Choi, B.H.; Yoon, S.H.; Song, S.I.; Yoon, J.K.; Lee, S.J.; An, Y.S. Comparison of Diagnostic Performance Between Visual and Quantitative Assessment of Bone Scintigraphy Results in Patients With Painful Temporomandibular Disorder. Medicine 2016, 95, e2485. [Google Scholar] [CrossRef]
- Epstein, J.B.; Rea, A.; Chahal, O. The use of bone scintigraphy in temporomandibular joint disorders. Oral Dis. 2002, 8, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.H.; An, Y.S.; Park, S.H.; Song, S.I. Influences of age and sex on the validity of bone scintigraphy for the diagnosis of temporomandibular joint osteoarthritis. Int. J. Oral Maxillofac. Surg. 2018, 47, 1445–1452. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.H.; Hong, I.K.; Chun, Y.H. Prediction of painful temporomandibular joint osteoarthritis in juvenile patients using bone scintigraphy. Clin. Exp. Dent. Res. 2019, 5, 225–235. [Google Scholar] [CrossRef] [PubMed]
- Park, K.S.; Song, H.C.; Cho, S.G.; Kang, S.R.; Kim, J.; Jun, H.M.; Song, M.; Jeong, G.C.; Park, H.J.; Kwon, S.Y.; et al. Open-Mouth Bone Scintigraphy Is Better than Closed-Mouth Bone Scintigraphy in the Diagnosis of Temporomandibular Osteoarthritis. Nucl. Med. Mol. Imaging 2016, 50, 213–218. [Google Scholar] [CrossRef][Green Version]
- Chan, B.H.; Leung, Y.Y. SPECT bone scintigraphy for the assessment of condylar growth activity in mandibular asymmetry: Is it accurate? Int. J. Oral Maxillofac. Surg. 2018, 47, 470–479. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.; Brennan, M.T. Differential diagnosis of orofacial pain and temporomandibular disorder. Dent. Clin. N. Am. 2013, 57, 419–428. [Google Scholar] [CrossRef]
- Alpaslan, G.H.; Alpaslan, C. Efficacy of temporomandibular joint arthrocentesis with and without injection of sodium hyaluronate in treatment of internal derangements. J. Oral Maxillofac. Surg. 2001, 59, 613–618. [Google Scholar] [CrossRef]
- Nitzan, D.W.; Dolwick, M.F.; Heft, M.W. Arthroscopic lavage and lysis of the temporomandibular joint: A change in perspective. J. Oral Maxillofac. Surg. 1990, 48, 798–801. [Google Scholar] [CrossRef]
- Zhang, C.; Wu, J.Y.; Deng, D.L.; He, B.Y.; Tao, Y.; Niu, Y.M.; Deng, M.H. Efficacy of splint therapy for the management of temporomandibular disorders: A meta-analysis. Oncotarget 2016, 7, 84043–84053. [Google Scholar] [CrossRef] [PubMed]
- Riley, P.; Glenny, A.M.; Worthington, H.V.; Jacobsen, E.; Robertson, C.; Durham, J.; Davies, S.; Petersen, H.; Boyers, D. Oral splints for temporomandibular disorder or bruxism: A systematic review. Br. Dent. J. 2020, 228, 191–197. [Google Scholar] [CrossRef]
- Al-Moraissi, E.A.; Farea, R.; Qasem, K.A.; Al-Wadeai, M.S.; Al-Sabahi, M.E.; Al-Iryani, G.M. Effectiveness of occlusal splint therapy in the management of temporomandibular disorders: Network meta-analysis of randomized controlled trials. Int. J. Oral Maxillofac. Surg. 2020, 49, 1042–1056. [Google Scholar] [CrossRef]
- Alkhutari, A.S.; Alyahya, A.; Rodrigues Conti, P.C.; Christidis, N.; Al-Moraissi, E.A. Is the therapeutic effect of occlusal stabilization appliances more than just placebo effect in the management of painful temporomandibular disorders? A network meta-analysis of randomized clinical trials. J. Prosthet. Dent. 2020. [Google Scholar] [CrossRef] [PubMed]
- Seifeldin, S.A.; Elhayes, K.A. Soft versus hard occlusal splint therapy in the management of temporomandibular disorders (TMDs). Saudi Dent. J. 2015, 27, 208–214. [Google Scholar] [CrossRef]
- Incorvati, C.; Romeo, A.; Fabrizi, A.; Defila, L.; Vanti, C.; Gatto, M.R.A.; Marchetti, C.; Pillastrini, P. Effectiveness of physical therapy in addition to occlusal splint in myogenic temporomandibular disorders: Protocol of a randomised controlled trial. BMJ Open 2020, 10, e038438. [Google Scholar] [CrossRef]
- van der Meer, H.A.; Calixtre, L.B.; Engelbert, R.H.H.; Visscher, C.M.; Nijhuis-van der Sanden, M.W.; Speksnijder, C.M. Effects of physical therapy for temporomandibular disorders on headache pain intensity: A systematic review. Musculoskelet. Sci. Pract. 2020, 50, 102277. [Google Scholar] [CrossRef] [PubMed]
- Kutuk, S.G.; Ozkan, Y.; Kutuk, M.; Ozdas, T. Comparison of the Efficacies of Dry Needling and Botox Methods in the Treatment of Myofascial Pain Syndrome Affecting the Temporomandibular Joint. J. Craniofacial Surg. 2019, 30, 1556–1559. [Google Scholar] [CrossRef]
- Connelly, S.T.; Myung, J.; Gupta, R.; Tartaglia, G.M.; Gizdulich, A.; Yang, J.; Silva, R. Clinical outcomes of Botox injections for chronic temporomandibular disorders: Do we understand how Botox works on muscle, pain, and the brain? Int. J. Oral Maxillofac. Surg. 2017, 46, 322–327. [Google Scholar] [CrossRef]
- Kim, Y.H.; Bang, J.I.; Son, H.J.; Kim, Y.; Kim, J.H.; Bae, H.; Han, S.J.; Yoon, H.J.; Kim, B.S. Protective effects of extracorporeal shockwave on rat chondrocytes and temporomandibular joint osteoarthritis; preclinical evaluation with in vivo(99m)Tc-HDP SPECT and ex vivo micro-CT. Osteoarthr. Cartil. 2019, 27, 1692–1701. [Google Scholar] [CrossRef]
- Schenk, I.; Vesper, M.; Nam, V.C. Initial results using extracorporeal low energy shockwave therapy ESWT in muscle reflex-induced lock jaw. Mund Kiefer Gesichtschir. 2002, 6, 351–355. [Google Scholar] [CrossRef] [PubMed]
- Dworkin, S.F.; Turner, J.A.; Mancl, L.; Wilson, L.; Massoth, D.; Huggins, K.H.; LeResche, L.; Truelove, E. A randomized clinical trial of a tailored comprehensive care treatment program for temporomandibular disorders. J. Orofac. Pain 2002, 16, 259–276. [Google Scholar]
- Türp, J.C.; Jokstad, A.; Motschall, E.; Schindler, H.J.; Windecker-Gétaz, I.; Ettlin, D.A. Is there a superiority of multimodal as opposed to simple therapy in patients with temporomandibular disorders? A qualitative systematic review of the literature. Clin. Oral Implant. Res. 2007, 18 (Suppl. 3), 138–150. [Google Scholar] [CrossRef]
- Conti, P.C.; Correa, A.S.; Lauris, J.R.; Stuginski-Barbosa, J. Management of painful temporomandibular joint clicking with different intraoral devices and counseling: A controlled study. J. Appl. Oral Sci. 2015, 23, 529–535. [Google Scholar] [CrossRef]
- de Resende, C.; de Oliveira Medeiros, F.G.L.; de Figueiredo Rego, C.R.; Bispo, A.S.L.; Barbosa, G.A.S.; de Almeida, E.O. Short-term effectiveness of conservative therapies in pain, quality of life, and sleep in patients with temporomandibular disorders: A randomized clinical trial. Cranio 2019, 1–9. [Google Scholar] [CrossRef]
- de Barros Pascoal, A.L.; de Freitas, R.; da Silva, L.F.G.; Oliveira, A.; Dos Santos Calderon, P. Effectiveness of Counseling on Chronic Pain Management in Patients with Temporomandibular Disorders. J. Oral Facial Pain Headache 2020, 34, 77–82. [Google Scholar] [CrossRef]
- Delgado-Delgado, R.; Iriarte-Álvarez, N.; Valera-Calero, J.A.; Centenera-Centenera, M.B.; Garnacho-Garnacho, V.E.; Gallego-Sendarrubias, G.M. Association between temporomandibular disorders with clinical and sociodemographic features: An observational study. Int. J. Clin. Pract 2021, e13961. [Google Scholar] [CrossRef]
- Al-Ani, Z. Occlusion and Temporomandibular Disorders: A Long-Standing Controversy in Dentistry. Prim. Dent. J. 2020, 9, 43–48. [Google Scholar] [CrossRef]
- Manfredini, D.; Lombardo, L.; Siciliani, G. Temporomandibular disorders and dental occlusion. A systematic review of association studies: End of an era? J. Oral Rehabil. 2017, 44, 908–923. [Google Scholar] [CrossRef]
- Kakudate, N.; Yokoyama, Y.; Sumida, F.; Matsumoto, Y.; Gordan, V.V.; Gilbert, G.H.; Velly, A.M.; Schiffman, E.L. Dentist Practice Patterns and Therapeutic Confidence in the Treatment of Pain Related to Temporomandibular Disorders in a Dental Practice-Based Research Network. J. Oral Facial Pain Headache 2017, 31, 152–158. [Google Scholar] [CrossRef] [PubMed]
- Onishi, M. Arthroscopy of the temporomandibular joint (author’s transl). Kokubyo Gakkai Zasshi 1975, 42, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Murakami, K.; Ono, T. Temporomandibular joint arthroscopy by inferolateral approach. Int. J. Oral Maxillofac. Surg. 1986, 15, 410–417. [Google Scholar] [CrossRef]
- Sanders, B. Arthroscopic surgery of the temporomandibular joint: Treatment of internal derangement with persistent closed lock. Oral Surg. Oral Med. Oral Pathol. 1986, 62, 361–372. [Google Scholar] [CrossRef]
- Sanders, B.; Buoncristiani, R. Diagnostic and surgical arthroscopy of the temporomandibular joint: Clinical experience with 137 procedures over a 2-year period. J. Craniomandib. Disord.: Facial Oral Pain 1987, 1, 202–213. [Google Scholar]
- McCain, J.P. Arthroscopy of the human temporomandibular joint. J. Oral Maxillofac. Surg. 1988, 46, 648–655. [Google Scholar] [CrossRef]
- McCain, J.P.; Sanders, B.; Koslin, M.G.; Quinn, J.H.; Peters, P.B.; Indresano, A.T. Temporomandibular joint arthroscopy: A 6-year multicenter retrospective study of 4,831 joints. J. Oral Maxillofac. Surg. 1992, 50, 926–930. [Google Scholar] [CrossRef]
- Reston, J.T.; Turkelson, C.M. Meta-analysis of surgical treatments for temporomandibular articular disorders. J. Oral Maxillofac. Surg. 2003, 61, 3–10. [Google Scholar] [CrossRef]
- Schiffman, E.L.; Velly, A.M.; Look, J.O.; Hodges, J.S.; Swift, J.Q.; Decker, K.L.; Anderson, Q.N.; Templeton, R.B.; Lenton, P.A.; Kang, W.; et al. Effects of four treatment strategies for temporomandibular joint closed lock. Int. J. Oral Maxillofac. Surg. 2014, 43, 217–226. [Google Scholar] [CrossRef]
- Dimitroulis, G. Outcomes of temporomandibular joint arthroscopy in patients with painful but otherwise normal joints. J. Craniomaxillofac. Surg. 2015, 43, 940–943. [Google Scholar] [CrossRef]
- McCain, J.P.; Hossameldin, R.H.; Srouji, S.; Maher, A. Arthroscopic discopexy is effective in managing temporomandibular joint internal derangement in patients with Wilkes stage II and III. J. Oral Maxillofac. Surg. 2015, 73, 391–401. [Google Scholar] [CrossRef]
- Al-Moraissi, E.A. Arthroscopy versus arthrocentesis in the management of internal derangement of the temporomandibular joint: A systematic review and meta-analysis. Int. J. Oral Maxillofac. Surg. 2015, 44, 104–112. [Google Scholar] [CrossRef]
- Liu, X.; Zheng, J.; Cai, X.; Abdelrehem, A.; Yang, C. Techniques of Yang’s arthroscopic discopexy for temporomandibular joint rotational anterior disc displacement. Int. J. Oral Maxillofac. Surg. 2019, 48, 769–778. [Google Scholar] [CrossRef]
- Machoň, V.; Levorová, J.; Hirjak, D.; Beňo, M.; Drahoš, M.; Foltán, R. Does arthroscopic lysis and lavage in subjects with Wilkes III internal derangement reduce pain? Oral Maxillofac. Surg. 2021. [Google Scholar] [CrossRef] [PubMed]
- Nitzan, D.W.; Dolwick, M.F.; Martinez, G.A. Temporomandibular joint arthrocentesis: A simplified treatment for severe, limited mouth opening. J. Oral Maxillofac. Surg. 1991, 49, 1163–1167. [Google Scholar] [CrossRef]
- Alpaslan, C.; Kahraman, S.; Guner, B.; Cula, S. Does the use of soft or hard splints affect the short-term outcome of temporomandibular joint arthrocentesis? Int J. Oral Maxillofac. Surg. 2008, 37, 424–427. [Google Scholar] [CrossRef] [PubMed]
- Bayramoglu, Z.; Tozoglu, S. Comparison of single- and double-puncture arthrocentesis for the treatment of temporomandibular joint disorders: A six-month, prospective study. Cranio 2019, 1–6. [Google Scholar] [CrossRef]
- Carvajal, W.A.; Laskin, D.M. Long-term evaluation of arthrocentesis for the treatment of internal derangements of the temporomandibular joint. J. Oral Maxillofac. Surg. 2000, 58, 852–855. [Google Scholar] [CrossRef]
- Diracoglu, D.; Saral, I.B.; Keklik, B.; Kurt, H.; Emekli, U.; Ozcakar, L.; Karan, A.; Aksoy, C. Arthrocentesis versus nonsurgical methods in the treatment of temporomandibular disc displacement without reduction. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2009, 108, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Emshoff, R.; Rudisch, A. Determining predictor variables for treatment outcomes of arthrocentesis and hydraulic distention of the temporomandibular joint. J. Oral Maxillofac. Surg. 2004, 62, 816–823. [Google Scholar] [CrossRef]
- Monje-Gil, F.; Nitzan, D.; Gonzalez-Garcia, R. Temporomandibular joint arthrocentesis. Review of the literature. Med. Oral Patol Oral Cir. Bucal 2012, 17, e575–e581. [Google Scholar] [CrossRef] [PubMed]
- Neeli, A.S.; Umarani, M.; Kotrashetti, S.M.; Baliga, S. Arthrocentesis for the treatment of internal derangement of the temporomandibular joint. J. Maxillofac. Oral Surg. 2010, 9, 350–354. [Google Scholar] [CrossRef] [PubMed]
- Nitzan, D.W.; Price, A. The use of arthrocentesis for the treatment of osteoarthritic temporomandibular joints. J. Oral Maxillofac. Surg. 2001, 59, 1154–1159. [Google Scholar] [CrossRef]
- Nitzan, D.W.; Samson, B.; Better, H. Long-term outcome of arthrocentesis for sudden-onset, persistent, severe closed lock of the temporomandibular joint. J. Oral Maxillofac. Surg. 1997, 55, 151–157. [Google Scholar] [CrossRef]
- Nitzan, D.W.; Svidovsky, J.; Zini, A.; Zadik, Y. Effect of Arthrocentesis on Symptomatic Osteoarthritis of the Temporomandibular Joint and Analysis of the Effect of Preoperative Clinical and Radiologic Features. J. Oral Maxillofac. Surg. 2017, 75, 260–267. [Google Scholar] [CrossRef]
- Polat, M.E.; Yanik, S. Efficiency of arthrocentesis treatment for different temporomandibular joint disorders. Int. J. Oral Maxillofac. Surg. 2020, 49, 621–627. [Google Scholar] [CrossRef]
- Toameh, M.H.; Alkhouri, I.; Karman, M.A. Management of patients with disk displacement without reduction of the temporomandibular joint by arthrocentesis alone, plus hyaluronic acid or plus platelet-rich plasma. Dent. Med. Probl. 2019, 56, 265–272. [Google Scholar] [CrossRef]
- Yilmaz, O.; Korkmaz, Y.T.; Tuzuner, T. Comparison of treatment efficacy between hyaluronic acid and arthrocentesis plus hyaluronic acid in internal derangements of temporomandibular joint. J. Craniomaxillofac. Surg. 2019, 47, 1720–1727. [Google Scholar] [CrossRef]
- Vos, L.M.; Huddleston Slater, J.J.; Stegenga, B. Arthrocentesis as initial treatment for temporomandibular joint arthropathy: A randomized controlled trial. J. Craniomaxillofac. Surg. 2014, 42, e134–e139. [Google Scholar] [CrossRef] [PubMed]
- Al-Moraissi, E.A.; Wolford, L.M.; Ellis, E., 3rd; Neff, A. The hierarchy of different treatments for arthrogenous temporomandibular disorders: A network meta-analysis of randomized clinical trials. J. Craniomaxillofac. Surg. 2020, 48, 9–23. [Google Scholar] [CrossRef] [PubMed]
- Li, D.T.S.; Wong, N.S.M.; Li, S.K.Y.; McGrath, C.P.; Leung, Y.Y. Timing of Arthrocentesis in the Management of Temporomandibular Disorders: An Integrative Review and Meta-analysis. Int. J. Oral Maxillofac. Surg. 2021. [Google Scholar] [CrossRef]
- Hobeich, J.B.; Salameh, Z.A.; Ismail, E.; Sadig, W.M.; Hokayem, N.E.; Almas, K. Arthroscopy versus arthrocentesis. A retrospective study of disc displacement management without reduction. Saudi Med. J. 2007, 28, 1541–1544. [Google Scholar] [PubMed]
- Laskin, D.M. Arthroscopy Versus Arthrocentesis for Treating Internal Derangements of the Temporomandibular Joint. Oral Maxillofac. Surg. Clin. N. Am. 2018, 30, 325–328. [Google Scholar] [CrossRef]
- Monteiro, J.; de Arruda, J.A.A.; Silva, E.; Vasconcelos, B. Is Single-Puncture TMJ Arthrocentesis Superior to the Double-Puncture Technique for the Improvement of Outcomes in Patients With TMDs? J. Oral Maxillofac. Surg. 2020, 78, 1319.e1311–1319.e1315. [Google Scholar] [CrossRef] [PubMed]
- Nagori, S.A.; Roy Chowdhury, S.K.; Thukral, H.; Jose, A.; Roychoudhury, A. Single puncture versus standard double needle arthrocentesis for the management of temporomandibular joint disorders: A systematic review. J. Oral Rehabil. 2018, 45, 810–818. [Google Scholar] [CrossRef]
- Folle, F.S.; Poluha, R.L.; Setogutti, E.T.; Grossmann, E. Double puncture versus single puncture arthrocentesis for the management of unilateral temporomandibular joint disc displacement without reduction: A randomized controlled trial. J. Craniomaxillofac. Surg. 2018, 46, 2003–2007. [Google Scholar] [CrossRef] [PubMed]
- Bhargava, D.; Thomas, S.; Pawar, P.; Jain, M.; Pathak, P. Ultrasound-guided arthrocentesis using single-puncture, double-lumen, single-barrel needle for patients with temporomandibular joint acute closed lock internal derangement. Oral Maxillofac. Surg. 2019, 23, 159–165. [Google Scholar] [CrossRef]
- Antony, P.G.; Sebastian, A.; Annapoorani, D.; Varghese, K.G.; Mohan, S.; Jayakumar, N.; Dominic, S.; John, B. Comparison of clinical outcomes of treatment of dysfunction of the temporomandibular joint between conventional and ultrasound-guided arthrocentesis. Br. J. Oral Maxillofac. Surg. 2019, 57, 62–66. [Google Scholar] [CrossRef]
- Bilgir, E.; Yildirim, D.; Senturk, M.F.; Orhan, H. Clinical and ultrasonographic evaluation of ultrasound-guided single puncture temporomandibular joint arthrocentesis. Cranio 2020, 1–10. [Google Scholar] [CrossRef]
- Hu, Y.; Zhang, X.; Liu, S.; Xu, F. Ultrasound-guided vs conventional arthrocentesis for management of temporomandibular joint disorders: A systematic review and meta-analysis. Cranio 2020. [Google Scholar] [CrossRef]
- Leung, Y.Y.; Wu, F.H.W.; Chan, H.H. Ultrasonography-guided arthrocentesis versus conventional arthrocentesis in treating internal derangement of temporomandibular joint: A systematic review. Clin. Oral Investig. 2020, 24, 3771–3780. [Google Scholar] [CrossRef]
- Haigler, M.C.; Abdulrehman, E.; Siddappa, S.; Kishore, R.; Padilla, M.; Enciso, R. Use of platelet-rich plasma, platelet-rich growth factor with arthrocentesis or arthroscopy to treat temporomandibular joint osteoarthritis: Systematic review with meta-analyses. J. Am. Dent. Assoc. 2018, 149, 940–952.e942. [Google Scholar] [CrossRef]
- Liu, Y.; Wu, J.S.; Tang, Y.L.; Tang, Y.J.; Fei, W.; Liang, X.H. Multiple Treatment Meta-Analysis of Intra-Articular Injection for Temporomandibular Osteoarthritis. J. Oral Maxillofac. Surg. 2020, 78, 373.e371–373.e318. [Google Scholar] [CrossRef]
- Chowdhury, S.K.R.; Saxena, V.; Rajkumar, K.; Shadamarshan, R.A. Evaluation of Total Alloplastic Temporomandibular Joint Replacement in TMJ Ankylosis. J. Maxillofac. Oral Surg. 2019, 18, 293–298. [Google Scholar] [CrossRef]
- Bhargava, D.; Neelakandan, R.S.; Dalsingh, V.; Sharma, Y.; Pandey, A.; Pandey, A.; Beena, S.; Koneru, G. A three dimensional (3D) musculoskeletal finite element analysis of DARSN temporomandibular joint (TMJ) prosthesis for total unilateral alloplastic joint replacement. J. Stomatol. Oral Maxillofac. Surg. 2019, 120, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Mercuri, L.G. Costochondral Graft Versus Total Alloplastic Joint for Temporomandibular Joint Reconstruction. Oral Maxillofac. Surg. Clin. N. Am. 2018, 30, 335–342. [Google Scholar] [CrossRef]
- Lotesto, A.; Miloro, M.; Mercuri, L.G.; Sukotjo, C. Status of alloplastic total temporomandibular joint replacement procedures performed by members of the American Society of Temporomandibular Joint Surgeons. Int. J. Oral Maxillofac. Surg. 2017, 46, 93–96. [Google Scholar] [CrossRef] [PubMed]
- Ramos, A.; Mesnard, M. Christensen vs Biomet Microfixation alloplastic TMJ implant: Are there improvements? A numerical study. J. Craniomaxillofac. Surg. 2015, 43, 1398–1403. [Google Scholar] [CrossRef]
- Neelakandan, R.S.; Raja, A.V.; Krishnan, A.M. Total Alloplastic Temporomandibular Joint Reconstruction for Management of TMJ Ankylosis. J. Maxillofac. Oral Surg. 2014, 13, 575–582. [Google Scholar] [CrossRef]
- Burgess, M.; Bowler, M.; Jones, R.; Hase, M.; Murdoch, B. Improved outcomes after alloplastic TMJ replacement: Analysis of a multicenter study from Australia and New Zealand. J. Oral Maxillofac. Surg. 2014, 72, 1251–1257. [Google Scholar] [CrossRef] [PubMed]
| Painful Conditions | Clinical Findings |
| Myalgia | Familiar pain in the masseter or temporalis upon palpation or mouth opening |
| Local Myalgia | Familiar pain in the masseter or temporalis localized to the site of palpation |
| Myofascial pain | Pain in the masseter or temporalis spreading beyond the site of palpation but within the confines of the muscle |
| Myofascial pain with referral | Pain in the masseter or temporalis beyond the confines of the muscle being palpated |
| Arthralgia | Familiar pain in the TMJ upon palpation or during function |
| Headache attributed to TMD | Headache in the temple upon palpation of the temporalis muscle or during function |
| Non-Painful Conditions | Clinical Findings |
| Disc displacement with reduction | Clicking in the TMJ upon function |
| Disc displacement with reduction with intermittent locking | Clicking in the TMJ with reported episodes of limited mouth opening |
| Disc displacement without reduction with limited opening | Limited mouth opening affecting function, with maximum assisted opening < 40mm |
| Disc displacement without reduction without limited opening | Limited mouth opening affecting function, with maximum assisted opening of ≥ 40mm |
| Degenerative joint disease | Crepitus of the TMJ upon function |
| Subluxation | History of jaw locking in an open mouth position, cannot close without a self-maneuver |
| I. TMJ |
| A. Joint pain |
| 1. Arthritis |
| B. Joint disorders |
| 1. Hypomobility disorders other than disc disorders |
| a. Adhesions/Adherence |
| b. Ankylosis (Fibrous or Osseous) |
| 2. TMJ dislocations |
| C. Joint diseases |
| 1. Systemic arthritides |
| 2. Condylysis/Idiopathic condylar resorption |
| 3. Osteochondritis dissecans |
| 4. Osteonecrosis |
| 5. Neoplasm |
| 6. Synovial Chondromatosis |
| D. Fractures |
| E. Congenital/Developmental disorders |
| 1. Aplasia |
| 2. Hypoplasia |
| 3. Hyperplasia |
| II. Masticatory Muscles |
| A. Muscle pain |
| 1. Tendonitis |
| 2. Myositis |
| 3. Spasm |
| B. Contracture |
| C. Hypertrophy |
| D. Neoplasm |
| E. Movement Disorders |
| 1. Orofacial dyskinesia |
| 2. Oromandibular dystonia |
| F. Masticatory muscle pain related to central/systemic pain disorder |
| 1. Fibromyalgia/widespread pain |
| III. Associated Structures |
| A. Coronoid hyperplasia |
| Neuropathic Pain |
| Trigeminal neuralgia |
| Glossopharyngeal neuralgia |
| Postherpetic neuralgia |
| Traumatic neuralgia |
| Burning mouth syndrome |
| Atypical odontalgia |
| Atypical facial pain |
| Odontogenic Pain |
| Dental caries |
| Periodontal disease |
| Dental abscess |
| Dental sensitivity |
| Cracked tooth syndrome |
| Periocoronitis |
| Intracranial Pain |
| Tumours |
| Aneurysms |
| Bleeding |
| Infection |
| Pain from Other Adjacent Structures |
| Ear |
| Nose |
| Throat |
| Eyes |
| Sinus |
| Salivary glands |
| Lymph nodes |
| Vasculature |
| Cervical region |
| Headaches not Attributed to TMD |
| Migraine |
| Cluster headache |
| Tension-type headache |
| Temporal arteritis |
| Referred Pain |
| Psychogenic Pain |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Li, D.T.S.; Leung, Y.Y. Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management. Diagnostics 2021, 11, 459. https://doi.org/10.3390/diagnostics11030459
Li DTS, Leung YY. Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management. Diagnostics. 2021; 11(3):459. https://doi.org/10.3390/diagnostics11030459
Chicago/Turabian StyleLi, Dion Tik Shun, and Yiu Yan Leung. 2021. "Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management" Diagnostics 11, no. 3: 459. https://doi.org/10.3390/diagnostics11030459
APA StyleLi, D. T. S., & Leung, Y. Y. (2021). Temporomandibular Disorders: Current Concepts and Controversies in Diagnosis and Management. Diagnostics, 11(3), 459. https://doi.org/10.3390/diagnostics11030459







