The Importance of the Nephrologist in the Treatment of the Diuretic-Resistant Heart Failure
Abstract
1. Introduction
2. Search Methods
3. Results
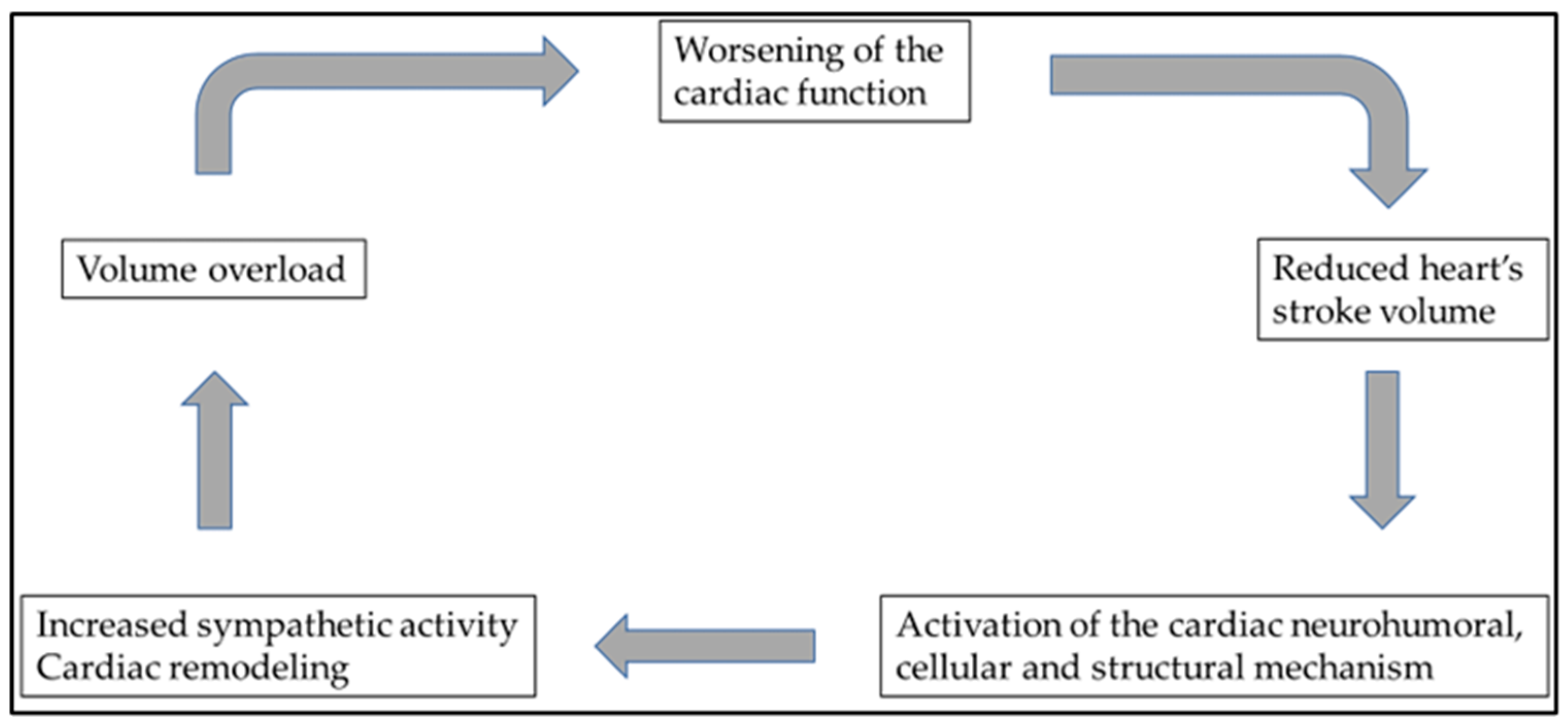
4. Diuretic Resistance to Heart Failure
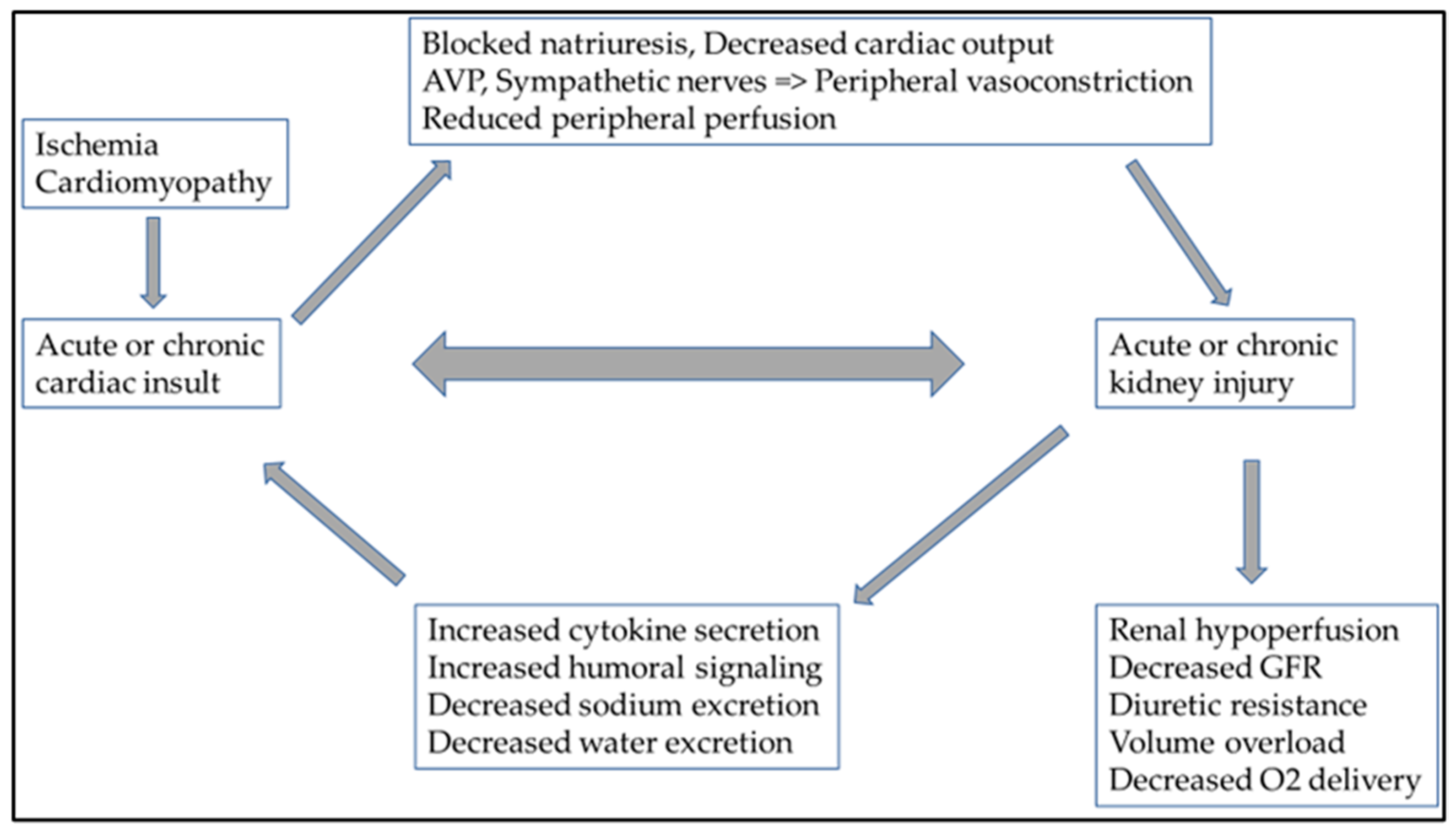
5. Cardiorenal Syndrome
6. Peritoneal Dialysis in Diuretic-Resistant Heart Failure
7. Urgent Start of the Peritoneal Dialysis in Diuretic Resistance Heart Failure
8. Other Specific Nephrology Treatments in Diuretic-Resistant Heart Failure
9. Discussion
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. Cardiovascular Diseases. 2023. Available online: https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds) (accessed on 20 April 2023).
- Back, M.; von Haehling, S.; Papp, Z.; Piepoli, M.F. A year in heart failure: Updates of clinical and preclinical findings. ESC Heart Fail 2023. [Google Scholar] [CrossRef] [PubMed]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Bohm, M.; Burri, H.; Butler, J.; Celutkiene, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef] [PubMed]
- Fitchett, D.; Inzucchi, S.E.; Cannon, C.P.; McGuire, D.K.; Scirica, B.M.; Johansen, O.E.; Sambevski, S.; Kaspers, S.; Pfarr, E.; George, J.T.; et al. Empagliflozin Reduced Mortality and Hospitalization for Heart Failure Across the Spectrum of Cardiovascular Risk in the EMPA-REG OUTCOME Trial. Circulation 2019, 139, 1384–1395. [Google Scholar] [CrossRef] [PubMed]
- McMurray, J.J.V.; Solomon, S.D.; Inzucchi, S.E.; Kober, L.; Kosiborod, M.N.; Martinez, F.A.; Ponikowski, P.; Sabatine, M.S.; Anand, I.S.; Belohlavek, J.; et al. Dapagliflozin in Patients with Heart Failure and Reduced Ejection Fraction. N. Engl. J. Med. 2019, 381, 1995–2008. [Google Scholar] [CrossRef]
- Dickstein, K.; Vardas, P.E.; Auricchio, A.; Daubert, J.C.; Linde, C.; McMurray, J.; Ponikowski, P.; Priori, S.G.; Sutton, R.; van Veldhuisen, D.J.; et al. 2010 Focused Update of ESC Guidelines on device therapy in heart failure: An update of the 2008 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure and the 2007 ESC guidelines for cardiac and resynchronization therapy. Developed with the special contribution of the Heart Failure Association and the European Heart Rhythm Association. Eur. Heart J. 2010, 31, 2677–2687. [Google Scholar] [CrossRef]
- Fudim, M.; Abraham, W.T.; von Bardeleben, R.S.; Lindenfeld, J.; Ponikowski, P.P.; Salah, H.M.; Khan, M.S.; Sievert, H.; Stone, G.W.; Anker, S.D.; et al. Device Therapy in Chronic Heart Failure: JACC State-of-the-Art Review. J. Am. Coll. Cardiol. 2021, 78, 931–956. [Google Scholar] [CrossRef]
- Templier, M.; Paré, G. Transparency in literature reviews: An assessment of reporting practices across review types and genres in top IS journals. Eur. J. Inf. Syst. 2017, 27, 503–550. [Google Scholar] [CrossRef]
- Guy Paré, S.K. Methods for Literature Reviews. In Handbook of eHealth Evaluation: An Evidence-Based Approach; Lau, F., Kuziemsky, C., Eds.; University of Victoria: Victoria, BC, Canada, 2017; pp. 157–179. [Google Scholar]
- Rahman, R.; Paz, P.; Elmassry, M.; Mantilla, B.; Dobbe, L.; Shurmur, S.; Nugent, K. Diuretic Resistance in Heart Failure. Cardiol. Rev. 2021, 29, 73–81. [Google Scholar] [CrossRef]
- Casu, G.; Merella, P. Diuretic Therapy in Heart Failure—Current Approaches. Eur. Cardiol. 2015, 10, 42–47. [Google Scholar] [CrossRef]
- Palmer, L.G.; Schnermann, J. Integrated control of Na transport along the nephron. Clin. J. Am. Soc. Nephrol. 2015, 10, 676–687. [Google Scholar] [CrossRef]
- Oppermann, M.; Hansen, P.B.; Castrop, H.; Schnermann, J. Vasodilatation of afferent arterioles and paradoxical increase of renal vascular resistance by furosemide in mice. Am. J. Physiol.-Ren. Physiol. 2007, 293, F279–F287. [Google Scholar] [CrossRef]
- Francis, G.S.; Siegel, R.M.; Goldsmith, S.R.; Olivari, M.T.; Levine, T.B.; Cohn, J.N. Acute vasoconstrictor response to intravenous furosemide in patients with chronic congestive heart failure. Activation of the neurohumoral axis. Ann. Intern. Med. 1985, 103, 1–6. [Google Scholar] [CrossRef]
- Kaissling, B.; Stanton, B.A. Adaptation of distal tubule and collecting duct to increased sodium delivery. I. Ultrastructure. Am. J. Physiol. 1988, 255, F1256–F1268. [Google Scholar] [CrossRef]
- Pandey, A.K.; Dhingra, N.K.; Hibino, M.; Gupta, V.; Verma, S. Sodium-glucose cotransporter 2 inhibitors in heart failure with reduced or preserved ejection fraction: A meta-analysis. ESC Heart Fail. 2022, 9, 942–946. [Google Scholar] [CrossRef]
- Solomon, S.D.; McMurray, J.J.V.; Claggett, B.; de Boer, R.A.; DeMets, D.; Hernandez, A.F.; Inzucchi, S.E.; Kosiborod, M.N.; Lam, C.S.P.; Martinez, F.; et al. Dapagliflozin in Heart Failure with Mildly Reduced or Preserved Ejection Fraction. N. Engl. J. Med. 2022, 387, 1089–1098. [Google Scholar] [CrossRef]
- Voors, A.A.; Angermann, C.E.; Teerlink, J.R.; Collins, S.P.; Kosiborod, M.; Biegus, J.; Ferreira, J.P.; Nassif, M.E.; Psotka, M.A.; Tromp, J.; et al. The SGLT2 inhibitor empagliflozin in patients hospitalized for acute heart failure: A multinational randomized trial. Nat. Med. 2022, 28, 568–574. [Google Scholar] [CrossRef]
- Thomas, M.C.; Cherney, D.Z.I. The actions of SGLT2 inhibitors on metabolism, renal function and blood pressure. Diabetologia 2018, 61, 2098–2107. [Google Scholar] [CrossRef]
- Lytvyn, Y.; Bjornstad, P.; Udell, J.A.; Lovshin, J.A.; Cherney, D.Z.I. Sodium Glucose Cotransporter-2 Inhibition in Heart Failure: Potential Mechanisms, Clinical Applications, and Summary of Clinical Trials. Circulation 2017, 136, 1643–1658. [Google Scholar] [CrossRef]
- Nespoux, J.; Vallon, V. Renal effects of SGLT2 inhibitors: An update. Curr. Opin. Nephrol. Hypertens. 2020, 29, 190–198. [Google Scholar] [CrossRef]
- Griffin, M.; Riello, R.; Rao, V.S.; Ivey-Miranda, J.; Fleming, J.; Maulion, C.; McCallum, W.; Sarnak, M.; Collins, S.; Inzucchi, S.E.; et al. Sodium glucose cotransporter 2 inhibitors as diuretic adjuvants in acute decompensated heart failure: A case series. ESC Heart Fail. 2020, 7, 1966–1971. [Google Scholar] [CrossRef]
- De Vecchis, R.; Esposito, C.; Ariano, C.; Cantatrione, S. Hypertonic saline plus i.v. furosemide improve renal safety profile and clinical outcomes in acute decompensated heart failure: A meta-analysis of the literature. Herz 2015, 40, 423–435. [Google Scholar] [CrossRef] [PubMed]
- Masella, C.; Viggiano, D.; Molfino, I.; Zacchia, M.; Capolongo, G.; Anastasio, P.; Simeoni, M. Diuretic Resistance in Cardio-Nephrology: Role of Pharmacokinetics, Hypochloremia, and Kidney Remodeling. Kidney Blood Press. Res. 2019, 44, 915–927. [Google Scholar] [CrossRef]
- Ljungman, S.; Laragh, J.H.; Cody, R.J. Role of the kidney in congestive heart failure. Relationship of cardiac index to kidney function. Drugs 1990, 39 (Suppl. 4), 10–21; discussion 22–14. [Google Scholar] [CrossRef] [PubMed]
- Verbrugge, F.H.; Dupont, M.; Steels, P.; Grieten, L.; Malbrain, M.; Tang, W.H.; Mullens, W. Abdominal contributions to cardiorenal dysfunction in congestive heart failure. J. Am. Coll. Cardiol. 2013, 62, 485–495. [Google Scholar] [CrossRef] [PubMed]
- Licata, G.; Di Pasquale, P.; Parrinello, G.; Cardinale, A.; Scandurra, A.; Follone, G.; Argano, C.; Tuttolomondo, A.; Paterna, S. Effects of high-dose furosemide and small-volume hypertonic saline solution infusion in comparison with a high dose of furosemide as bolus in refractory congestive heart failure: Long-term effects. Am. Heart J. 2003, 145, 459–466. [Google Scholar] [CrossRef] [PubMed]
- Paterna, S.; Gaspare, P.; Fasullo, S.; Sarullo, F.M.; Di Pasquale, P. Normal-sodium diet compared with low-sodium diet in compensated congestive heart failure: Is sodium an old enemy or a new friend? Clin. Sci. 2008, 114, 221–230. [Google Scholar] [CrossRef]
- Ichikawa, I.; Pfeffer, J.M.; Pfeffer, M.A.; Hostetter, T.H.; Brenner, B.M. Role of angiotensin II in the altered renal function of congestive heart failure. Circ. Res. 1984, 55, 669–675. [Google Scholar] [CrossRef]
- Haase, M.; Muller, C.; Damman, K.; Murray, P.T.; Kellum, J.A.; Ronco, C.; McCullough, P.A. Pathogenesis of cardiorenal syndrome type 1 in acute decompensated heart failure: Workgroup statements from the eleventh consensus conference of the Acute Dialysis Quality Initiative (ADQI). Contrib. Nephrol. 2013, 182, 99–116. [Google Scholar] [CrossRef]
- Kopitko, C.; Medve, L.; Gondos, T.; Soliman, K.M.M.; Fulop, T. Mediators of Regional Kidney Perfusion during Surgical Pneumo-Peritoneum Creation and the Risk of Acute Kidney Injury-A Review of Basic Physiology. J. Clin. Med. 2022, 11, 2728. [Google Scholar] [CrossRef]
- Faul, C.; Amaral, A.P.; Oskouei, B.; Hu, M.C.; Sloan, A.; Isakova, T.; Gutierrez, O.M.; Aguillon-Prada, R.; Lincoln, J.; Hare, J.M.; et al. FGF23 induces left ventricular hypertrophy. J. Clin. Investig. 2011, 121, 4393–4408. [Google Scholar] [CrossRef]
- Ganda, A.; Onat, D.; Demmer, R.T.; Wan, E.; Vittorio, T.J.; Sabbah, H.N.; Colombo, P.C. Venous congestion and endothelial cell activation in acute decompensated heart failure. Curr. Heart Fail. Rep. 2010, 7, 66–74. [Google Scholar] [CrossRef]
- Nguyen, V.Q.; Gadiraju, T.V.; Patel, H.; Park, M.; Le Jemtel, T.H.; Jaiswal, A. Intra-abdominal Hypertension: An Important Consideration for Diuretic Resistance in Acute Decompensated Heart Failure. Clin. Cardiol. 2016, 39, 37–40. [Google Scholar] [CrossRef]
- Kopitko, C.; Gondos, T.; Fulop, T.; Medve, L. Reinterpreting Renal Hemodynamics: The Importance of Venous Congestion and Effective Organ Perfusion in Acute Kidney Injury. Am. J. Med. Sci. 2020, 359, 193–205. [Google Scholar] [CrossRef]
- Ronco, C.; McCullough, P.; Anker, S.D.; Anand, I.; Aspromonte, N.; Bagshaw, S.M.; Bellomo, R.; Berl, T.; Bobek, I.; Cruz, D.N.; et al. Cardio-renal syndromes: Report from the consensus conference of the acute dialysis quality initiative. Eur. Heart J. 2010, 31, 703–711. [Google Scholar] [CrossRef]
- Wojtaszek, E.; Grzejszczak, A.; Niemczyk, S.; Malyszko, J.; Matuszkiewicz-Rowinska, J. Peritoneal Ultrafiltration in the Long-Term Treatment of Chronic Heart Failure Refractory to Pharmacological Therapy. Front. Physiol. 2019, 10, 310. [Google Scholar] [CrossRef]
- Stegmayr, B.G.; Banga, R.; Lundberg, L.; Wikdahl, A.M.; Plum-Wirell, M. PD treatment for severe congestive heart failure. Perit. Dial. Int. 1996, 16 (Suppl. 1), S231–S235. [Google Scholar] [CrossRef]
- Bertoli, S.V.; Musetti, C.; Ciurlino, D.; Basile, C.; Galli, E.; Gambaro, G.; Iadarola, G.; Guastoni, C.; Carlini, A.; Fasciolo, F.; et al. Peritoneal ultrafiltration in refractory heart failure: A cohort study. Perit. Dial. Int. 2014, 34, 64–70. [Google Scholar] [CrossRef]
- Husain-Syed, F.; Grone, H.J.; Assmus, B.; Bauer, P.; Gall, H.; Seeger, W.; Ghofrani, A.; Ronco, C.; Birk, H.W. Congestive nephropathy: A neglected entity? Proposal for diagnostic criteria and future perspectives. ESC Heart Fail. 2021, 8, 183–203. [Google Scholar] [CrossRef]
- Courivaud, C.; Kazory, A.; Crepin, T.; Azar, R.; Bresson-Vautrin, C.; Chalopin, J.M.; Ducloux, D. Peritoneal dialysis reduces the number of hospitalization days in heart failure patients refractory to diuretics. Perit. Dial. Int. 2014, 34, 100–108. [Google Scholar] [CrossRef]
- Scurt, F.G.; Kuczera, T.; Mertens, P.R.; Chatzikyrkou, C. The Cardiorenal Syndrome. Dtsch. Med. Wochenschr. 2019, 144, 910–916. [Google Scholar] [CrossRef]
- Sugiura, E.; Dohi, K.; Tanimura, M.; Kumagai, N.; Ishikawa, E.; Ito, M. Successful Peritoneal Dialysis for the Treatment of Inotrope-Dependent End-Stage Heart Failure. Int. Heart J. 2019, 60, 1211–1218. [Google Scholar] [CrossRef] [PubMed]
- Szabó, R.P.; Pethő, Á.; Fedor, R.; Kertész, A.; Bódi, A.; Szegedi, A.; Balla, J. A diuretikum-refrakter szívelégtelen betegek körében alkalmazott peritonealis dialízissel szerzett tapasztalataink. Cardiol. Hung. 2018, 48, 179–183. [Google Scholar] [CrossRef]
- Sun, C.Y.; Sung, J.M.; Wang, J.D.; Li, C.Y.; Kuo, Y.T.; Lee, C.C.; Wu, J.L.; Chang, Y.T. A comparison of the risk of congestive heart failure-related hospitalizations in patients receiving hemodialysis and peritoneal dialysis—A retrospective propensity score-matched study. PLoS ONE 2019, 14, e0223336. [Google Scholar] [CrossRef]
- Puttagunta, H.; Holt, S.G. Peritoneal Dialysis for Heart Failure. Perit. Dial. Int. 2015, 35, 645–649. [Google Scholar] [CrossRef] [PubMed]
- Karopadi, A.N.; Mason, G.; Rettore, E.; Ronco, C. Cost of peritoneal dialysis and haemodialysis across the world. Nephrol. Dial. Transplant. 2013, 28, 2553–2569. [Google Scholar] [CrossRef]
- Grossekettler, L.; Schmack, B.; Schwenger, V. Cardiorenal syndrome: Limits of heart failure therapy. Herz 2013, 38, 569–577. [Google Scholar] [CrossRef]
- Francois, K.; Ronco, C.; Bargman, J.M. Peritoneal Dialysis for Chronic Congestive Heart Failure. Blood Purif. 2015, 40, 45–52. [Google Scholar] [CrossRef]
- Sahlie, A.; Jaar, B.G.; Paez, L.G.; Masud, T.; Lea, J.P.; Burkart, J.M.; Plantinga, L.C. Burden and Correlates of Hospital Readmissions among U.S. Peritoneal Dialysis Patients. Perit. Dial. Int. 2019, 39, 261–267. [Google Scholar] [CrossRef]
- Chionh, C.Y.; Clementi, A.; Poh, C.B.; Finkelstein, F.O.; Cruz, D.N. The use of peritoneal dialysis in heart failure: A systematic review. Perit. Dial. Int. 2020, 40, 527–539. [Google Scholar] [CrossRef]
- van der Meer, P.; Gaggin, H.K.; Dec, G.W. ACC/AHA Versus ESC Guidelines on Heart Failure: JACC Guideline Comparison. J. Am. Coll. Cardiol. 2019, 73, 2756–2768. [Google Scholar] [CrossRef]
- Schalk, E.; Tolle, D.; Schulz, S.; Teschner, D.; Hentrich, M.; Fischer, T. Risk of central venous catheter (CVC)-related bloodstream infections (CRBSI) in cancer patients (pts) with or without neutropenia at time of CVC insertion. Oncol. Res. Treat. 2018, 41, 145. [Google Scholar]
- Hickson, L.J.; Gooden, J.Y.; Le, K.Y.; Baddour, L.M.; Friedman, P.A.; Hayes, D.L.; Wilson, W.R.; Steckelberg, J.M.; Sohail, M.R. Clinical presentation and outcomes of cardiovascular implantable electronic device infections in hemodialysis patients. Am. J. Kidney Dis. 2014, 64, 104–110. [Google Scholar] [CrossRef]
- Carrillo, R.G.; Garisto, J.D.; Salman, L.; Merrill, D.; Asif, A. Contamination of transvenous pacemaker leads due to tunneled hemodialysis catheter infection: A report of 2 cases. Am. J. Kidney Dis. 2010, 55, 1097–1101. [Google Scholar] [CrossRef]
- Thomas, B.A.; Logar, C.M.; Anderson, A.E. Renal replacement therapy in congestive heart failure requiring left ventricular assist device augmentation. Perit. Dial. Int. 2012, 32, 386–392. [Google Scholar] [CrossRef]
- Dukka, H.; Kalra, P.A.; Wilkie, M.; Bhandari, S.; Davies, S.J.; Barratt, J.; Squire, I.; Odudu, A.; Selby, N.M.; McIntyre, C.; et al. Peritoneal Ultrafiltration for Heart Failure: Lessons from a Randomized Controlled Trial. Perit. Dial. Int. 2019, 39, 486–489. [Google Scholar] [CrossRef]
- Verger, C. Peritoneal dialysis solution and nutrition. Contrib. Nephrol. 2012, 178, 6–10. [Google Scholar] [CrossRef]
- Gotloib, L.; Fudin, R.; Yakubovich, M.; Vienken, J. Peritoneal dialysis in refractory end-stage congestive heart failure: A challenge facing a no-win situation. Nephrol. Dial. Transplant. 2005, 20 (Suppl. 7), vii32–vii36. [Google Scholar] [CrossRef]
- Wojtaszek, E.; Malyszko, J.; Matuszkiewicz-Rowinska, J. Peritoneal ultrafiltration in end-stage congestive heart failure. Cardiol. J. 2014, 21, 115–120. [Google Scholar] [CrossRef][Green Version]
- Akula, Y.V.; Fulop, T.; Dixit, M.P. Peritoneal Dialysis in Class 2-3 Obesity-A Single-Center Experience. Am. J. Med. Sci. 2017, 353, 70–75. [Google Scholar] [CrossRef]
- Crabtree, J.H.; Shrestha, B.M.; Chow, K.M.; Figueiredo, A.E.; Povlsen, J.V.; Wilkie, M.; Abdel-Aal, A.; Cullis, B.; Goh, B.L.; Briggs, V.R.; et al. Creating and Maintaining Optimal Peritoneal Dialysis Access in the Adult Patient: 2019 Update. Perit. Dial. Int. 2019, 39, 414–436. [Google Scholar] [CrossRef]
- Yeter, H.H.; Izgi, A.; Yildirim, S.; Akcay, O.F.; Derici, U. Outcomes of early-start peritoneal dialysis (PD) and the comparison with urgent-start hemodialysis and conventional-start PD. Ther. Apher. Dial. 2023, 27, 480–487. [Google Scholar] [CrossRef] [PubMed]
- Cheng, S.; Yang, L.; Sun, Z.; Zhang, X.; Zhu, X.; Meng, L.; Guo, S.; Zhuang, X.; Luo, P.; Cui, W. Safety of a 24-h-or-less break-in period in elderly patients undergoing urgent-start peritoneal dialysis: A multicenter retrospective cohort study. Ther. Apher. Dial. 2023, 27, 304–313. [Google Scholar] [CrossRef] [PubMed]
- Karpinski, S.; Sibbel, S.; Cohen, D.E.; Colson, C.; Van Wyck, D.B.; Ghaffari, A.; Schreiber, M.J.; Brunelli, S.M.; Tentori, F. Urgent-start peritoneal dialysis: Association with outcomes. Perit. Dial. Int. 2023, 43, 186–189. [Google Scholar] [CrossRef] [PubMed]
- Wen, X.; Yang, L.; Sun, Z.; Zhang, X.; Zhu, X.; Zhou, W.; Hu, X.; Liu, S.; Luo, P.; Cui, W. Feasibility of a break-in period of less than 24 hours for urgent start peritoneal dialysis: A multicenter study. Ren. Fail. 2022, 44, 450–460. [Google Scholar] [CrossRef]
- Nagatomo, M.; Yamada, H.; Shinozuka, K.; Shimoto, M.; Yunoki, T.; Ohtsuru, S. Peritoneal dialysis for COVID-19-associated acute kidney injury. Crit. Care 2020, 24, 309. [Google Scholar] [CrossRef]
- Parapiboon, W.; Ponce, D.; Cullis, B. Acute peritoneal dialysis in COVID-19. Perit. Dial. Int. 2020, 40, 359–362. [Google Scholar] [CrossRef]
- El Shamy, O.; Patel, N.; Abdelbaset, M.H.; Chenet, L.; Tokita, J.; Lookstein, R.; Lee, D.S.; Cohen, N.A.; Sharma, S.; Uribarri, J. Acute Start Peritoneal Dialysis during the COVID-19 Pandemic: Outcomes and Experiences. J. Am. Soc. Nephrol. 2020, 31, 1680–1682. [Google Scholar] [CrossRef]
- Bowes, E.; Joslin, J.; Braide-Azikiwe, D.C.B.; Tulley, C.; Bramham, K.; Saha, S.; Jayawardene, S.; Shakoane, B.; Wilkins, C.J.; Hutchings, S.; et al. Acute Peritoneal Dialysis With Percutaneous Catheter Insertion for COVID-19-Associated Acute Kidney Injury in Intensive Care: Experience From a UK Tertiary Center. Kidney Int. Rep. 2021, 6, 265–271. [Google Scholar] [CrossRef]
- Ponce, D.; Banin, V.B.; Bueloni, T.N.; Barretti, P.; Caramori, J.; Balbi, A.L. Different outcomes of peritoneal catheter percutaneous placement by nephrologists using a trocar versus the Seldinger technique: The experience of two Brazilian centers. Int. Urol. Nephrol. 2014, 46, 2029–2034. [Google Scholar] [CrossRef]
- Boujelbane, L.; Fu, N.; Chapla, K.; Melnick, D.; Redfield, R.R.; Waheed, S.; Yevzlin, A.S.; Shin, J.I.; Astor, B.C.; Chan, M.R. Percutaneous versus surgical insertion of PD catheters in dialysis patients: A meta-analysis. J. Vasc. Access 2015, 16, 498–505. [Google Scholar] [CrossRef]
- Medani, S.; Hussein, W.; Shantier, M.; Flynn, R.; Wall, C.; Mellotte, G. Comparison of Percutaneous and Open Surgical Techniques for First-Time Peritoneal Dialysis Catheter Placement in the Unbreached Peritoneum. Perit. Dial. Int. 2015, 35, 576–585. [Google Scholar] [CrossRef]
- Petho, A.; Szabo, R.P.; Tapolyai, M.; Rosivall, L. Bedside placement of peritoneal dialysis catheters—A single-center experience from Hungary. Ren. Fail. 2019, 41, 434–438. [Google Scholar] [CrossRef]
- Veress, J. Neues Instrument zur Ausführung von Brust- oder Bauchpunktionen und Pneumothoraxbehandlung. DMW—Dtsch. Med. Wochenschr. 2009, 64, 1480–1481. [Google Scholar] [CrossRef]
- Szabó Réka, S.A.P.; Attila, K.; Ákos, P.; Attila, S.; Zoltán, S.; József, B. Peritoneális dialízis-hídterápia a szívtranszplantációig. In Barna István (Szerk.) Orvosi Esettanulmányok-Hypertonai és Nephrológia Budapest; SpringMed Kiadó: Budapest, Hungary, 2016; pp. 198–204. [Google Scholar]
- Szegedi, A.; Pszabó, R.; Pethő, Á.G.; Kertész, A.B.; Maros, T.M.; Borbély, A.; Édes, I.; Csanádi, Z. Peritonealis dialízis, mint “bridge” terápia a szívtranszplantációig. Cardiol. Hung. 2018, 48, 184–186. [Google Scholar] [CrossRef]
- Tominaga, M.; Kawai, M.; Minai, K.; Ogawa, K.; Inoue, Y.; Morimoto, S.; Tanaka, T.; Nagoshi, T.; Ogawa, T.; Yoshimura, M. Association between plasma B-type natriuretic peptide and anaemia in heart failure with or without ischaemic heart disease: A retrospective study. BMJ Open 2019, 9, e024194. [Google Scholar] [CrossRef]
- Sharma, R.; Francis, D.P.; Pitt, B.; Poole-Wilson, P.A.; Coats, A.J.; Anker, S.D. Haemoglobin predicts survival in patients with chronic heart failure: A substudy of the ELITE II trial. Eur. Heart J. 2004, 25, 1021–1028. [Google Scholar] [CrossRef]
- Loncar, G.; Obradovic, D.; Thiele, H.; von Haehling, S.; Lainscak, M. Iron deficiency in heart failure. ESC Heart Fail. 2021, 8, 2368–2379. [Google Scholar] [CrossRef]
- Anker, S.D.; Comin Colet, J.; Filippatos, G.; Willenheimer, R.; Dickstein, K.; Drexler, H.; Luscher, T.F.; Bart, B.; Banasiak, W.; Niegowska, J.; et al. Ferric carboxymaltose in patients with heart failure and iron deficiency. N. Engl. J. Med. 2009, 361, 2436–2448. [Google Scholar] [CrossRef]
- Sindone, A.; Doehner, W.; Comin-Colet, J. Systematic review and meta-analysis of intravenous iron-carbohydrate complexes in HFrEF patients with iron deficiency. ESC Heart Fail. 2023, 10, 44–56. [Google Scholar] [CrossRef]
- Kalra, P.R.; Cleland, J.G.F.; Petrie, M.C.; Thomson, E.A.; Kalra, P.A.; Squire, I.B.; Ahmed, F.Z.; Al-Mohammad, A.; Cowburn, P.J.; Foley, P.W.X.; et al. Intravenous ferric derisomaltose in patients with heart failure and iron deficiency in the UK (IRONMAN): An investigator-initiated, prospective, randomised, open-label, blinded-endpoint trial. Lancet 2022, 400, 2199–2209. [Google Scholar] [CrossRef]
- Lopez-Vilella, R.; Lozano-Edo, S.; Arenas Martin, P.; Jover-Pastor, P.; Ezzitouny, M.; Sorolla Romero, J.; Calvo Asensio, M.; Martinez-Sole, J.; Guerrero Cervera, B.; Sanchez Martinez, J.C.; et al. Impact of intravenous ferric carboxymaltose on heart failure with preserved and reduced ejection fraction. ESC Heart Fail. 2022, 9, 133–145. [Google Scholar] [CrossRef] [PubMed]
| Searching Keywords | Number of Publications until 1 April 2023 | First Publication in This Field |
|---|---|---|
| “heart failure” | 309,020 | 1879 |
| “heart failure” and “nephrologist” | 352 | 1983 |
| “diuretic resistance” | 7087 | 1952 |
| “diuretic resistance” and “nephrologist” | 22 | 1976 |
| “diuretic-resistant heart failure” | 1361 | 1952 |
| “diuretic-resistant heart failure” and “nephrologist” | 15 | 1996 |
| “diuretic-resistant heart failure treatment” | 2 | 1994 |
| “diuretic-resistant heart failure treatment” and “nephrologist” | 0 | - |
| “cardiorenal syndrome” | 2322 | 1946 |
| “cardiorenal syndrome” and “nephrologist” | 66 | 2002 |
| Diuretics | Name | Effect on Nephron | Dose | Mechanism of Action | Overall Outcome |
|---|---|---|---|---|---|
| Loop diuretics | Furosemide, bumetanide, torsemide | Henle loop | 40 mg furosemide is equivalent to 1 mg bumetanide and 20 mg torsemide | Na+–K+–2Cl− symporter | Decreasing hypertonic renal medulla |
| Thiazides | Hydrochlorothiazide, chlortalidone | Distal convoluted tubule | 1−2 × 50 mg/day | Na+–Cl− transporter | Releasing NaCl and water |
| Aldosterone antagonist | Spironolactone | Distal tubule | 100 mg/day | Na+/K+ ATPase | Increasing sodium excretion |
| Carboanhyd-rase inhibitor | Acetazolamide, methazolamide | Proximal convoluted tubules | Typically, 250 mg/day | Causing the accumulation of carbonic acid | Increasing urinary Na+ and bicarbonate (HCO3−) |
| SGLT2 inhibitors | Dapagliflozin, empagliflozin | Proximal tubules | Typically, 10 mg/day | Sodium–glucose transport proteins | Glucosuria and natriuresis |
| CRS Type | Nomenclature | Description | Clinical Examples |
|---|---|---|---|
| CRS 1 | Acute CRS | HF resulting in AKI | ACS resulting in cardiogenic shock and AKI; AHF resulting in AKI |
| CRS 2 | Chronic CRS | Chronic HF resulting in CKD | Chronic HF |
| CRS 3 | Acute renocardiac syndrome | AKI resulting in AHF | HF in the setting of AKI from volume overload, inflammatory surge, and metabolic disturbances in uremia |
| CRS 4 | Chronic renocardiac syndrome | CKD resulting in chronic HF | LVH and HF from CKD-associated cardiomyopathy |
| CRS 5 | Secondary CRS | The systemic process resulting in HF and kidney failure | Sepsis, liver cirrhosis, and amyloidosis |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pethő, Á.G.; Tapolyai, M.; Browne, M.; Fülöp, T.; Orosz, P.; Szabó, R.P. The Importance of the Nephrologist in the Treatment of the Diuretic-Resistant Heart Failure. Life 2023, 13, 1328. https://doi.org/10.3390/life13061328
Pethő ÁG, Tapolyai M, Browne M, Fülöp T, Orosz P, Szabó RP. The Importance of the Nephrologist in the Treatment of the Diuretic-Resistant Heart Failure. Life. 2023; 13(6):1328. https://doi.org/10.3390/life13061328
Chicago/Turabian StylePethő, Ákos Géza, Mihály Tapolyai, Maria Browne, Tibor Fülöp, Petronella Orosz, and Réka P. Szabó. 2023. "The Importance of the Nephrologist in the Treatment of the Diuretic-Resistant Heart Failure" Life 13, no. 6: 1328. https://doi.org/10.3390/life13061328
APA StylePethő, Á. G., Tapolyai, M., Browne, M., Fülöp, T., Orosz, P., & Szabó, R. P. (2023). The Importance of the Nephrologist in the Treatment of the Diuretic-Resistant Heart Failure. Life, 13(6), 1328. https://doi.org/10.3390/life13061328








