Citicoline for the Management of Patients with Traumatic Brain Injury in the Acute Phase: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Selection Criteria
2.2. Search Methods
2.3. Study Selection and Data Extraction
2.4. Risk of Bias Assessment
2.5. Data Analysis
3. Results
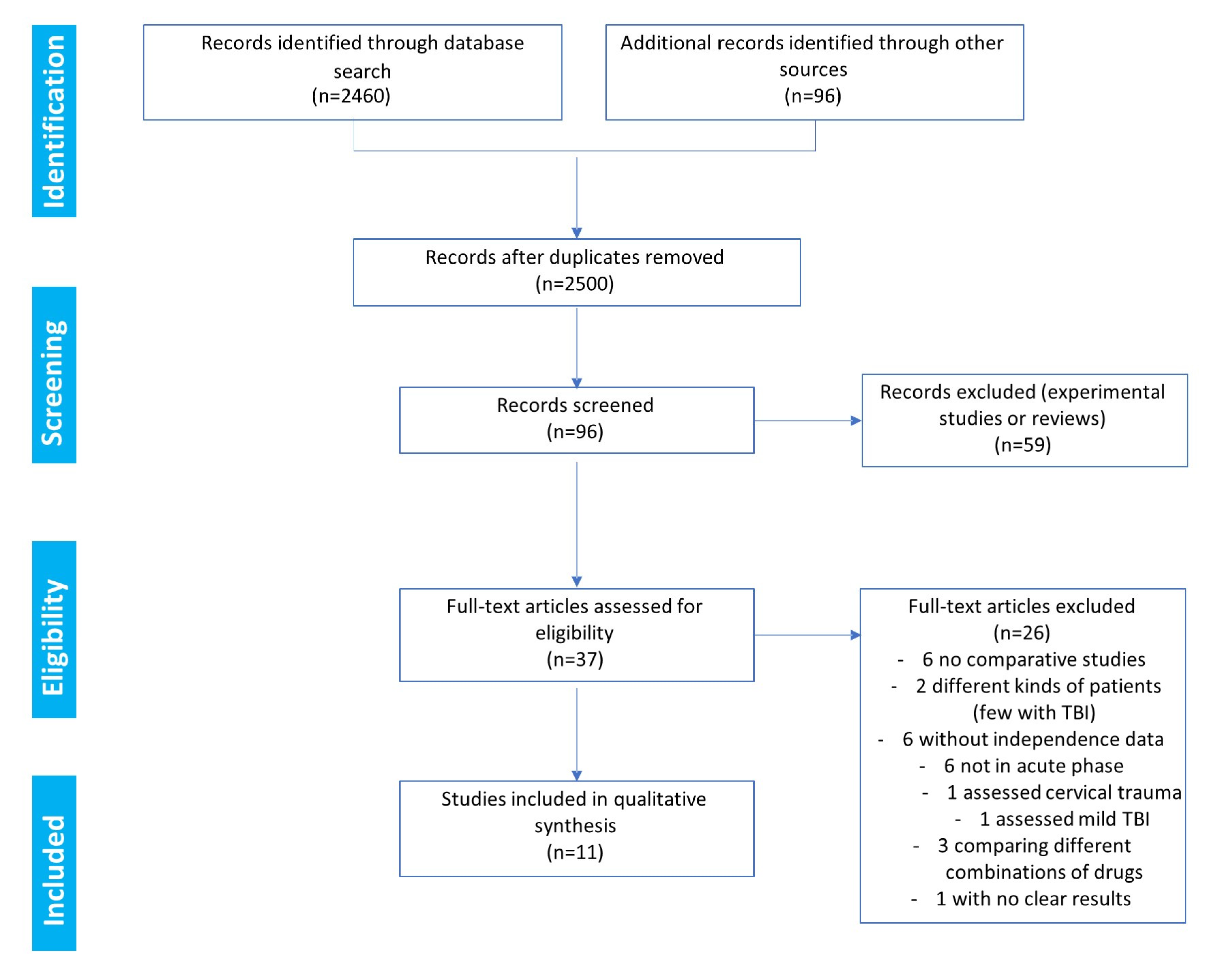
3.1. Study Selection
3.2. Study Characteristics
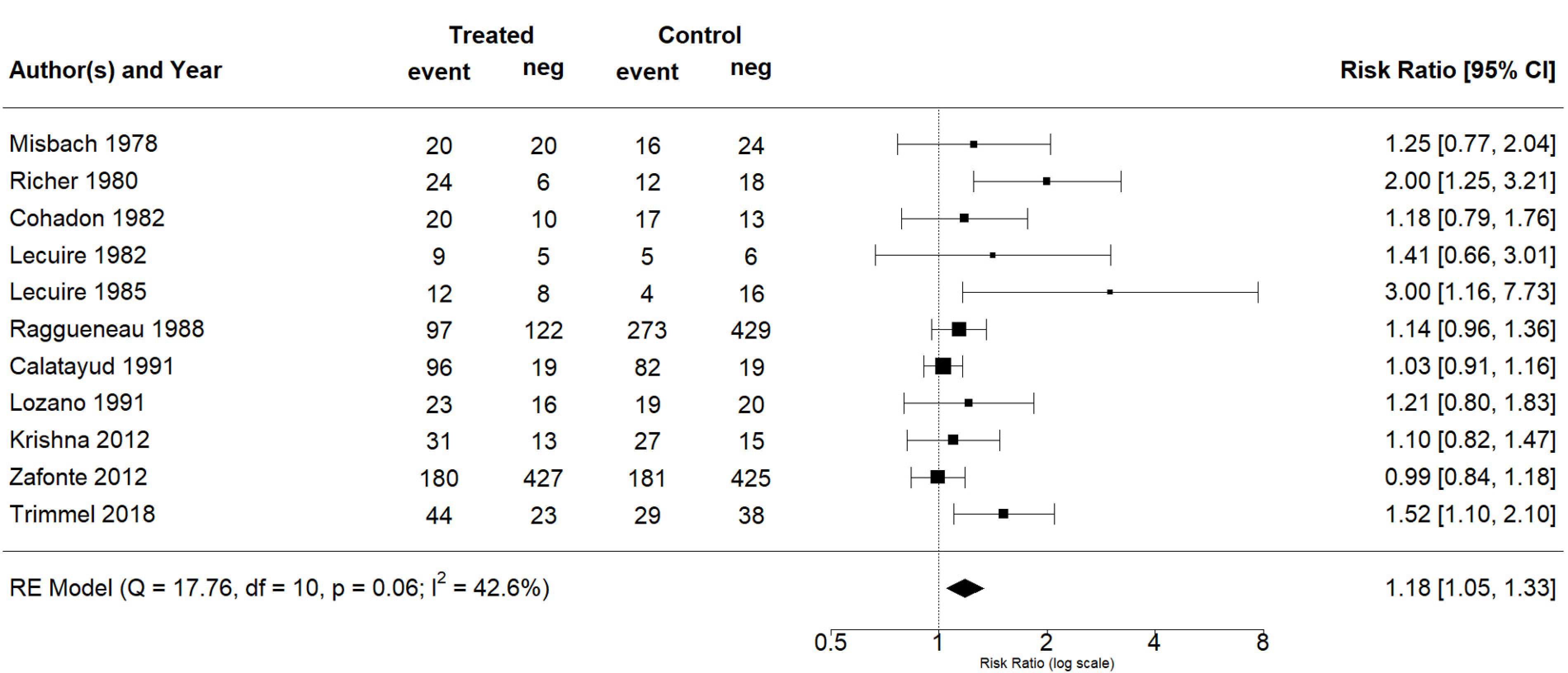
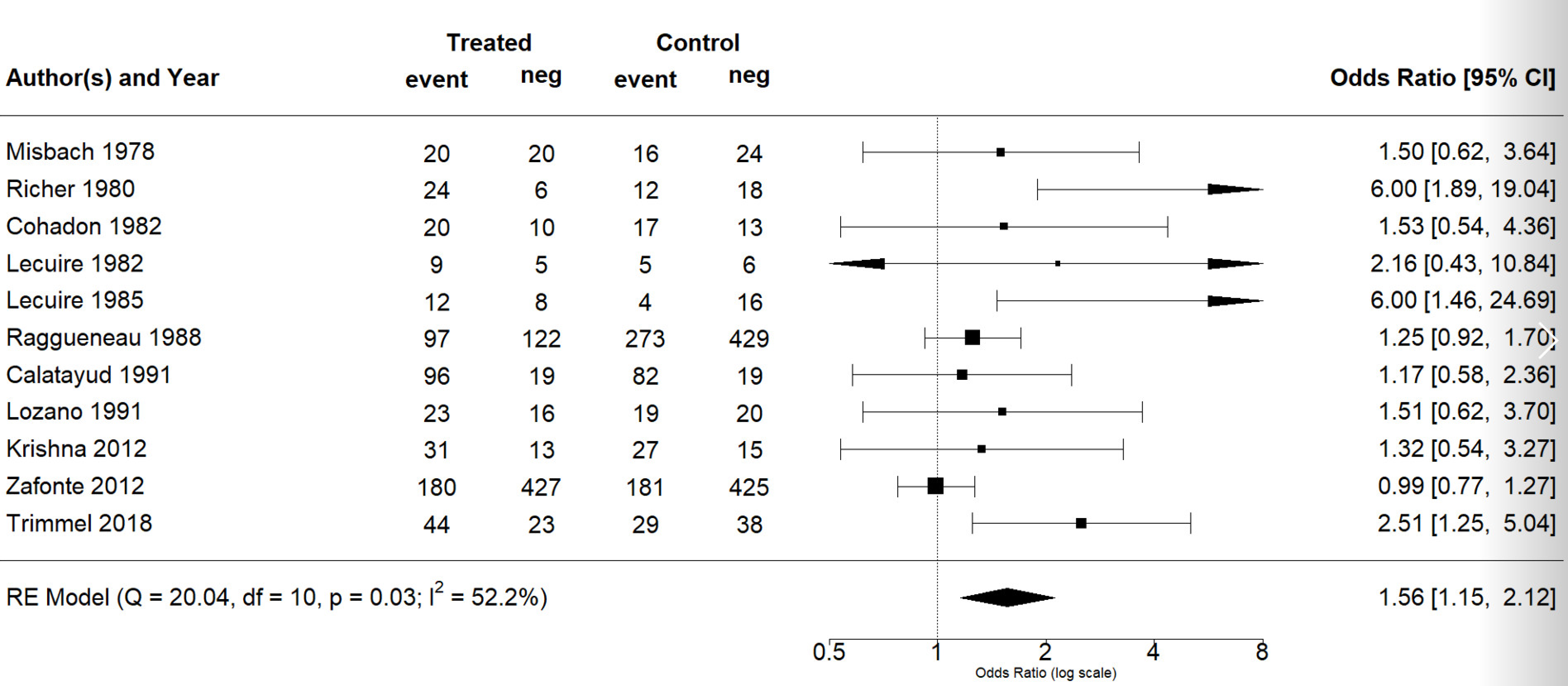
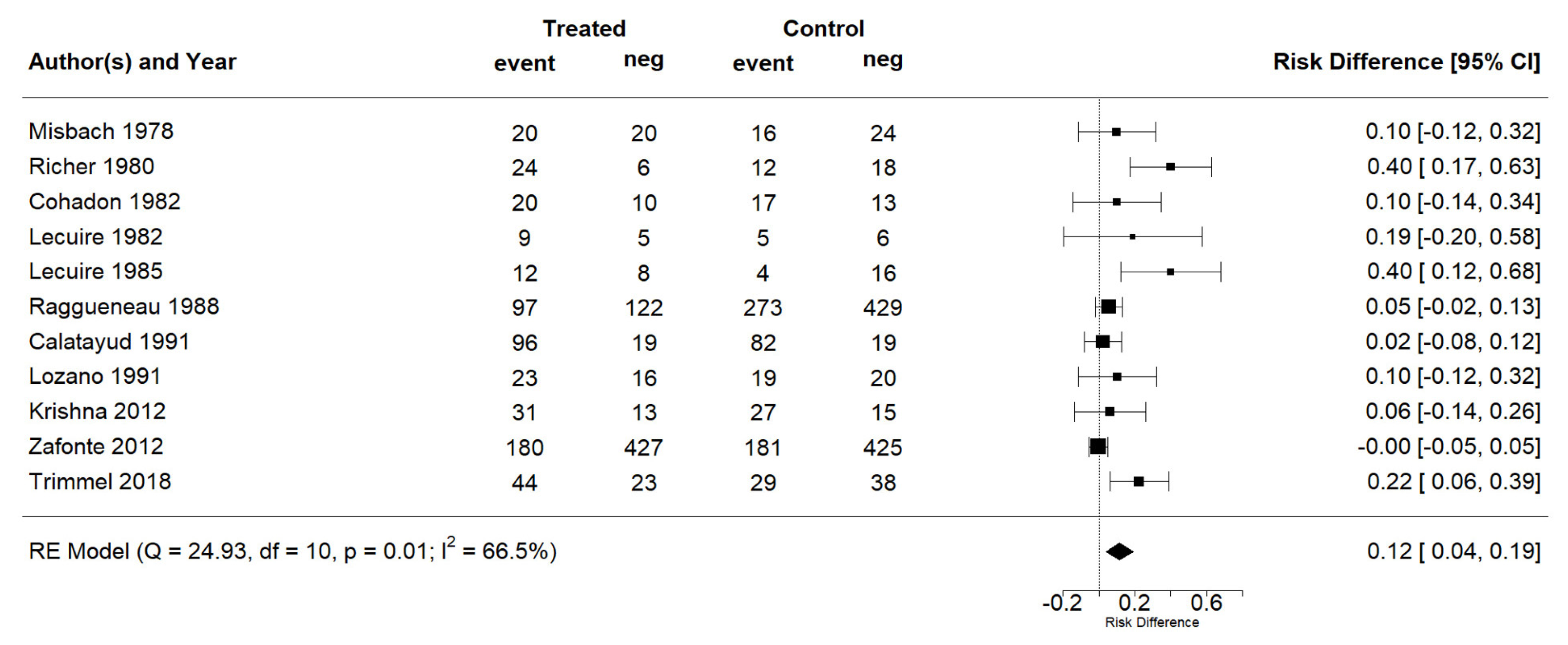
3.3. Synthesis of the Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Search Algorithms Used to Identify Studies in the Databases
| Database | Search Algorithm |
| OVID-Medline (PubMed) Up to January Week 3, 2021 | #1. exp CRANIOCEREBRAL TRAUMA/ #2. exp Cerebrovascular Trauma/ #3. exp BRAIN EDEMA/ #4. ((brain or cerebral or intracranial) adj3 (oedema or edema or swell$)).ab,ti. #5. exp GLASGOW COMA SCALE/ #6. exp GLASGOW OUTCOME SCALE/ #7. exp UNCONSCIOUSNESS/ #8. (Glasgow adj3 (coma or outcome) adj3 (scale$ or score$)).ab,ti. #9. (Unconscious$ or coma$ or concuss$ or ‘persistent vegetative state’).ab,ti. #10. “Rancho Los Amigos Scale”.ab,ti. #11. ((head or crani$ or cerebr$ or capitis or brain$ or forebrain$ or skull$ or hemispher$ or intra-cran$ or inter-cran$) adj3 (injur$ or trauma$ or damag$ or wound$ or fracture$ or contusion$)).ab,ti. #12. “Diffuse axonal injur$”.ab,ti. #13. ((head or crani$ or cerebr$ or brain$ or intra-cran$ or inter-cran$) adj3 (haematoma$ or hematoma$ or haemorrhag$ or hemorrhag$ or bleed$ or pressure)).ab,ti. #14. or/#1–13 #15. randomized.ab,ti. #16. randomized controlled trial.pt. #17. controlled clinical trial.pt. #18. placebo.ab. #19. clinical trials as topic.sh. #20. randomly.ab. #21. trial.ti. #22. Comparative Study/ #23. #15 or #16 or #17 or #18 or #19 or #20 or #21 or #22 #24. (animals not (humans and animals)).sh. #25. #23 not #24 #26. #14 and #25 #27. Cytidine Diphosphate Choline/ #28. citicoline.ab,ti. #29. cdp-choline.ab,ti. #30. cytidine-5-diphosphocholine.ab,ti. #31. (“cdp choline” or cdpcholine).ab,ti. #32. #27 or #28 or #29 or #30 or #31 #33. #26 and #32 |
| EMBASE Up to January Week 3, 2021 | (‘acute brain injury’/exp OR ‘acute brain injury’ OR ‘brain injuries’/exp OR ‘brain injuries’ OR ‘brain injury’/exp OR ‘brain injury’ OR ‘brain injury, chronic’/exp OR ‘brain injury, chronic’ OR ‘cerebral injury’/exp OR ‘cerebral injury’ OR ‘cerebrum lesion’/exp OR ‘cerebrum lesion’ OR ‘chronic brain injury’/exp OR ‘chronic brain injury’ OR ‘injury, brain’/exp OR ‘injury, brain’ OR ‘left hemisphere injury’/exp OR ‘left hemisphere injury’ OR ‘right hemisphere injury’/exp OR ‘right hemisphere injury’ OR ‘brain injuries, traumatic’/exp OR ‘brain injuries, traumatic’ OR ‘brain lesion, traumatic’/exp OR ‘brain lesion, traumatic’ OR ‘brain system trauma’/exp OR ‘brain system trauma’ OR ‘brain trauma’/exp OR ‘brain trauma’ OR ‘cerebral trauma’/exp OR ‘cerebral trauma’ OR ‘cerebrovascular trauma’/exp OR ‘cerebrovascular trauma’ OR ‘encephalopathy, traumatic’/exp OR ‘encephalopathy, traumatic’ OR ‘mild traumatic brain injury’/exp OR ‘mild traumatic brain injury’ OR ‘organic cerebral trauma’/exp OR ‘organic cerebral trauma’ OR ‘posttraumatic encephalopathy’/exp OR ‘posttraumatic encephalopathy’ OR ‘traumatic brain injuries’/exp OR ‘traumatic brain injuries’ OR ‘traumatic brain injury’/exp OR ‘traumatic brain injury’ OR ‘traumatic brain lesion’/exp OR ‘traumatic brain lesion’ OR ‘traumatic cerebral lesion’/exp OR ‘traumatic cerebral lesion’ OR ‘traumatic encephalopathy’/exp OR ‘traumatic encephalopathy’ OR ‘brain edema’/exp OR ‘brain edema’ OR ‘brain oedema’/exp OR ‘brain oedema’ OR ‘cerebral edema’/exp OR ‘cerebral edema’ OR ‘cerebral oedema’/exp OR ‘cerebral oedema’ OR ‘edema, brain’/exp OR ‘edema, brain’ OR ‘oedema, brain’/exp OR ‘oedema, brain’ OR ‘cerebrocranial injury’/exp OR ‘cerebrocranial injury’ OR ‘cerebrocranial trauma’/exp OR ‘cerebrocranial trauma’ OR ‘closed head injuries’/exp OR ‘closed head injuries’ OR ‘cranial injury’/exp OR ‘cranial injury’ OR ‘cranial trauma’/exp OR ‘cranial trauma’ OR ‘craniocerebral injury’/exp OR ‘craniocerebral injury’ OR ‘craniocerebral lesion’/exp OR ‘craniocerebral lesion’ OR ‘craniocerebral trauma’/exp OR ‘craniocerebral trauma’ OR ‘craniocerebral wound’/exp OR ‘craniocerebral wound’ OR ‘head injuries’/exp OR ‘head injuries’ OR ‘head injuries, closed’/exp OR ‘head injuries, closed’ OR ‘head injuries, penetrating’/exp OR ‘head injuries, penetrating’ OR ‘head injury’/exp OR ‘head injury’ OR ‘head trauma’/exp OR ‘head trauma’ OR ‘head wound’/exp OR ‘head wound’ OR ‘injury, head’/exp OR ‘injury, head’ OR ‘penetrating head injuries’/exp OR ‘penetrating head injuries’ OR ‘trauma capitis’/exp OR ‘trauma capitis’ OR ‘trauma, cranial’/exp OR ‘trauma, cranial’ OR ‘trauma, head’/exp OR ‘trauma, head’) AND (‘cdp choline’/exp OR ‘cdp choline’ OR ‘brassel 1000’/exp OR ‘brassel 1000’ OR ‘ceraxon’/exp OR ‘ceraxon’ OR ‘cidifos’/exp OR ‘cidifos’ OR ‘cidiphos’/exp OR ‘cidiphos’ OR ‘citicholine’/exp OR ‘citicholine’ OR ‘citicolin’/exp OR ‘citicolin’ OR ‘citicolina’/exp OR ‘citicolina’ OR ‘citicoline’/exp OR ‘citicoline’ OR ‘cyticholine’/exp OR ‘cyticholine’ OR ‘cytidine 5 diphosphocholine’/exp OR ‘cytidine 5 diphosphocholine’ OR ‘cytidine 5‘ diphosphocholine’/exp OR ‘cytidine 5‘ diphosphocholine’ OR ‘cytidine 5‘ diphosphorylcholine’/exp OR ‘cytidine 5‘ diphosphorylcholine’ OR ‘cytidine diphosphate choline ester’/exp OR ‘cytidine diphosphate choline ester’ OR ‘cytidine diphosphocholine’/exp OR ‘cytidine diphosphocholine’ OR ‘cytocholine’/exp OR ‘cytocholine’ OR ‘nicholin’/exp OR ‘nicholin’ OR ‘rexort’/exp OR ‘rexort’ OR ‘sauran’/exp OR ‘sauran’ OR ‘sinkron’/exp OR ‘sinkron’ OR ‘sintoclar’/exp OR ‘sintoclar’ OR ‘somazina’/exp OR ‘somazina’ OR ‘cdp’/exp OR ‘cdp’ OR ‘cytidine 5‘ diphosphate’/exp OR ‘cytidine 5‘ diphosphate’ OR ‘cytidine diphosphate’/exp OR ‘cytidine diphosphate’ OR ‘cytosine diphosphate’/exp OR ‘cytosine diphosphate’ OR ‘cytidine diphosphate choline’/exp OR ‘cytidine diphosphate choline’) AND (‘clinical trial, controlled’/exp OR ‘clinical trial, controlled’ OR ‘controlled clinical comparison’/exp OR ‘controlled clinical comparison’ OR ‘controlled clinical drug trial’/exp OR ‘controlled clinical drug trial’ OR ‘controlled clinical experiment’/exp OR ‘controlled clinical experiment’ OR ‘controlled clinical study’/exp OR ‘controlled clinical study’ OR ‘controlled clinical test’/exp OR ‘controlled clinical test’ OR ‘controlled clinical trial’/exp OR ‘controlled clinical trial’ OR ‘review, systematic’/exp OR ‘review, systematic’ OR ‘systematic review’/exp OR ‘systematic review’ OR ‘meta analysis’/exp OR ‘meta analysis’) |
References
- Capizzi, A.; Woo, J.; Verduzco-Gutierrez, M. Traumatic Brain Injury: An Overview of Epidemiology, Pathophysiology, and Medical Management. Med. Clin. N. Am. 2020, 104, 213–238. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.K.; Yang, Z.; Zhu, T.; Shi, Y.; Rubenstein, R.; Tyndall, J.A.; Manley, G.T. An update on diagnostic and prognostic biomarkers for traumatic brain injury. Expert Rev. Mol. Diagn. 2018, 18, 165–180. [Google Scholar] [CrossRef] [PubMed]
- GBD 2016 Traumatic Brain Injury and Spinal Cord Injury Collaborators. Global, regional, and national burden of traumatic brain injury and spinal cord injury, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2019, 18, 56–87. [Google Scholar] [CrossRef] [PubMed]
- James, S.L.; Lucchesi, L.R.; Bisignano, C.; Castle, C.D.; Dingels, Z.V.; Fox, J.T.; Hamilton, E.B.; Liu, Z.; McCracken, D.; Nixon, M.R.; et al. Morbidity and mortality from road injuries: Results from the Global Burden of Disease Study 2017. Inj. Prev. 2020, 26 (Suppl. S1), i46–i56. [Google Scholar] [CrossRef] [PubMed]
- Secades, J.J. Role of Citicoline in the Management of Traumatic Brain Injury. Pharmaceuticals 2021, 14, 410. [Google Scholar] [CrossRef] [PubMed]
- Lorenz, L.S.; Doonan, M. Value and Cost Savings from Access to Multi-disciplinary Rehabilitation Services After Severe Acquired Brain Injury. Front. Public Health 2021, 9, 753447. [Google Scholar] [CrossRef]
- Fu, T.S.; Jing, R.; McFaull, S.R.; Cusimano, M.D. Health & Economic Burden of Traumatic Brain Injury in the Emergency Department. Can. J. Neurol. Sci. 2016, 43, 238–247. [Google Scholar] [CrossRef]
- Adibhatla, R.M.; Hatcher, J.F. Role of Lipids in Brain Injury and Diseases. Future Lipidol. 2007, 2, 403–422. [Google Scholar] [CrossRef]
- Javaid, S.; Farooq, T.; Rehman, Z.; Afzal, A.; Ashraf, W.; Rasool, M.F.; Alqahtani, F.; Alsanea, S.; Alasmari, F.; Alanazi, M.M.; et al. Dynamics of Choline-Containing Phospholipids in Traumatic Brain Injury and Associated Comorbidities. Int. J. Mol. Sci. 2021, 22, 11313. [Google Scholar] [CrossRef]
- Maas, A.I.; Stocchetti, N.; Bullock, R. Moderate and severe traumatic brain injury in adults. Lancet Neurol. 2008, 7, 728–741. [Google Scholar] [CrossRef]
- Carney, N.; Totten, A.M.; O’Reilly, C.; Ullman, J.S.; Hawryluk, G.W.; Bell, M.J.; Bratton, S.L.; Chesnut, R.; Harris, O.A.; Kissoon, N.; et al. Guidelines for the Management of Severe Traumatic Brain Injury, Fourth Edition. Neurosurgery 2017, 80, 6–15. [Google Scholar] [CrossRef]
- Marehbian, J.; Muehlschlegel, S.; Edlow, B.L.; Hinson, H.E.; Hwang, D.Y. Medical Management of the Severe Traumatic Brain Injury Patient. Neurocrit. Care 2017, 27, 430–446. [Google Scholar] [CrossRef] [PubMed]
- Grieb, P. Neuroprotective properties of citicoline: Facts, doubts and unresolved issues. CNS Drugs 2014, 28, 185–193. [Google Scholar] [CrossRef] [PubMed]
- Secades, J.J.; Gareri, P. Citicoline: Pharmacological and clinical review, 2022 update. Rev. Neurol. 2022, 75, S1–S89. [Google Scholar] [CrossRef]
- Zafonte, R.D.; Bagiella, E.; Ansel, B.M.; Novack, T.A.; Friedewald, W.T.; Hesdorffer, D.C.; Timmons, S.D.; Jallo, J.; Eisenberg, H.; Hart, T.; et al. Effect of citicoline on functional and cognitive status among patients with traumatic brain injury: Citicoline Brain Injury Treatment Trial (COBRIT). JAMA 2012, 308, 1993–2000. [Google Scholar] [CrossRef]
- Adibhatla, R.M. Citicoline in stroke and TBI clinical trials. Nat. Rev. Neurol. 2013, 9, 173. [Google Scholar] [CrossRef] [PubMed]
- Secades, J.J. Citicoline for the treatment of head injury: A systematic review and meta-analysis of controlled clinical trials. J. Trauma Treat. 2014, 4, 227. [Google Scholar] [CrossRef]
- El Sayed, I.; Zaki, A.; Fayed, A.M.; Shehata, G.M.; Abdelmonem, S. A meta-analysis of the effect of different neuroprotective drugs in management of patients with traumatic brain injury. Neurosurg. Rev. 2018, 41, 427–438. [Google Scholar] [CrossRef]
- Higgins, J.P.T.; Lasserson, T.; Chandler, J.; Tovey, D.; Thomas, J.; Flemyng, E.; Churchill, R. Methodological Expectations of Cochrane Intervention Reviews; Cochrane: London, UK, 2022. [Google Scholar]
- Booth, A.; Clarke, M.; Dooley, G.; Ghersi, D.; Moher, D.; Petticrew, M.; Stewart, L. The nuts and bolts of PROSPERO: An international prospective register of systematic reviews. Syst. Rev. 2012, 1, 2. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Higgins, J.P.T.; Savović, J.; Page, M.J.; Sterne, J.A.C.; on behalf of the RoB2 Development Group. Revised Cochrane Risk-of-Bias Tool for Randomized Trials (RoB 2). Available online: https://www.riskofbias.info/welcome/rob-2-0-tool/current-version-of-rob-2 (accessed on 26 January 2022).
- Sterne, J.A.; Hernán, M.A.; Reeves, B.C.; Savović, J.; Berkman, N.D.; Viswanathan, M.; Henry, D.; Altman, D.G.; Ansari, M.T.; Boutron, I.; et al. ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ 2016, 355, i4919. [Google Scholar] [CrossRef] [PubMed]
- Viechtbauer, W. Conducting meta-analyses in R with the metafor package. J. Stat. Softw. 2010, 36, 1–48. Available online: https://wwwjstatsoftorg/v36/i03/ (accessed on 20 July 2021). [CrossRef]
- Guyatt, G.H.; Oxman, A.D.; Vist, G.E.; Kunz, R.; Falck-Ytter, Y.; Alonso-Coello, P.; Schünemann, H.J.; GRADE Working Group. GRADE: An emerging consensus on rating quality of evidence and strength of recommendations. BMJ 2008, 336, 924–926. [Google Scholar] [CrossRef] [PubMed]
- Misbach, J.; Andradi, S.; Harahap, T.P.; Soemargo, S.; Markam, S. Double blind trial of Nicholin (CDP-choline) on the patients with severe head injury. In Proceedings of the Biannual Meeting of Neurology, Psychiatry and Neurosurgery, Surabaya, Indonesia, 6–8 November 1978. [Google Scholar]
- Richer, E.; Cohadon, F. Therapeutic trial of a precursor phospholipids on the treatment of severe traumatic comas. In Proceedings of the International Symposium: Suffering and Cerebral Phospholipid Precursors; Laboratoires Cassenne-Takeda: Paris, France, 1980. [Google Scholar]
- Cohadon, F.; Richer, E.; Poletto, B. Etude d’un precurseur des phospholipides dans le traitement des comas traumatiques graves [A precursor of phospholipids in the treatment of severe traumatic comas]. Neurochirurgie 1982, 28, 287–290. [Google Scholar]
- Lecuire, J.; Duplay, J. Double-blind trial of citicoline versus meclofenossato in patients with head injury. G. Ital. Ric. Clin Ter. 1982, 3, 51–55. [Google Scholar]
- Lecuire, J. Traumatismes craniens: Etude comparative Piracetam- CDPcholine. CR Ther. Pharmacol. Clin. 1985, 3, 3–7. [Google Scholar]
- Raggueneau, J.L.; Jarrige, B. National Survey result in serious head injuries: Analysis of 219 injuries treated with CDP-choline [National inquiry on the outcome of severe head injuries: Analysis of 921 Injured Patients Treated with CDP-choline]. Agressologie 1988, 29, 439–443. [Google Scholar]
- Calatayud Maldonado, V.; Calatayud Pérez, J.B.; Aso Escario, J. Effects of CDP-choline on the recovery of patients with head injury. J. Neurol. Sci. 1991, 103 Suppl, S15–S18. [Google Scholar] [CrossRef]
- Lozano, R. CDP-choline in the treatment of cranio-encephalic traumata. J. Neurol. Sci. 1991, 103, S43–S47. [Google Scholar] [CrossRef]
- Krishna, D.; Chaurasia, I.D.; Jethwani, U. Role of citicoline in traumatic brain injury: A randomized controlled study. IJPMR 2012, 2, 1–5. [Google Scholar]
- Trimmel, H.; Majdan, M.; Wodak, A.; Herzer, G.; Csomor, D.; Brazinova, A. Citicoline in severe traumatic brain injury: Indications for improved outcome: A retrospective matched pair analysis from 14 Austrian trauma centers. Wien. Klin. Wochenschr. 2018, 130, 37–44. [Google Scholar] [CrossRef] [PubMed]
- Moriyama, M.; Tsukumo, T.; Nakagawa, Y. Effects of CDP-choline on head trauma. Gendai Rinsho 1967, 1, 114–120. [Google Scholar]
- Oka, M.; Oku, N.; Kujiraoka, Y.; Yoshida, S.; Higashiguchi, H. The effects of cytidine diphosphate choline (CDP-choline) on patients with head injury. Shinryo Shinyaku 1968, 3, 1101–1104. [Google Scholar]
- Miyazaki, M. Evaluation of the effectiveness of citicoline (CDP-choline) on motor paralysis as a sequela of cerebral apoplexy. Jpn. J. Geriatr. 1969, 6, 245–252. [Google Scholar] [CrossRef]
- Miyake, H.; Hayakawa, I.; Takakura, K. Treatment of head injuries with intermediate substances of the metabolic cycle of the brain. 1. The use of CDP-choline]. No To Shinkei 1964, 16, 873–878. [Google Scholar] [PubMed]
- Lecuire, J.; Duplay, J. Sperimentazione della citicolina in un campione di 154 traumatizzati cranici [Trial of citicoline in a sample of 154 head injuries]. G. Ital. Ric. Clin Ter. 1982, 3, 61–67. [Google Scholar]
- Hinev, S.; Tzoneva, D.; Ljubenova, K.; Tzvetkov, V.; Dimitrov, G.; Stefanov, I. Neuroprotection as component of complex therapy in patients with severe head trauma and cerebrovascular diseases. Anaesthesiol. Intensive Care 2007, 34, 19–24. [Google Scholar]
- Kumoi, T.; Hosomi, H.; Amatsu, M.; Shita, E.; Inokuchi, J.; Kokan, T.; et al. Recognition of the pharmacological effect of cdp-choline (nicholin) on vertigo caused by the sequelae of head trauma, whiplash injury and by alterations in cerebral circulation. A double blind trial. Data on file (Ferrer database).
- Miyashita, E. Clinical treatment with Audes (CDP-choline). Data on file (Ferrer database).
- Levin, H.S. Treatment of postconcussional symptoms with CDP-choline. J. Neurol. Sci. 1991, 103, S39–S42. [Google Scholar] [CrossRef]
- Carrion, J.L.; Dominguez-Roldán, J.M.; Cabezas, F.M.; Dominguez-Morales, M.R.; Munoz-Sánchez, M.A. Normalization of memory-related cerebral blood flow in severe traumatic brain injury patients and improvements of memory induced by citicholine (CDP-choline): The role of a pro-cognitive drug. In Proceedings of the ICRAN’99, Taipei, Taiwan, 20–23 November 1999. [Google Scholar]
- Leon-Carrion, J.; Dominguez-Roldan, J.M.; Murillo-Cabezas, F.; del Rosario Dominguez-Morales, M.; Munoz-Sanchez, M.A. The role of citicholine in neuropsychological training after traumatic brain injury. NeuroRehabilitation 2000, 14, 33–40. [Google Scholar] [CrossRef]
- Arenth, P. CDP-Choline and Working Memory After TBI: A Neuroimaging Study. Available online: https://clinicaltrials.gov/ct2/show/NCT00727246 (accessed on 26 January 2022).
- De Blas, A.; Martinez Cubells, J.; Hernando, C. Assessment of the effectiveness of citicoline in the treatment of traumatic brain injury. Med. Clin. 1986, 87, 41–44. [Google Scholar]
- El Reweny, E.M.; Okasha, A.; Hafez, A. The neuroprotective effect of citicholine (CDP choline) in patients with traumatic brain injury. In Proceedings of the 25th ESICM Annual Congress, Lisbon, Portugal, 13–17 October 2012. [Google Scholar]
- Salehpour, F.; Aghazade, J.; Mirzaee, F.; Mahdkhah, A. Citicoline in patients with traumatic brain injuries. EC Neurol. 2015, 2, 87–93. [Google Scholar]
- Shokouhi, G.; Haghjoo, A.G.; Sattarnezhad, N.; Asghari, M.; Sattarnezhad, A.; Asghari, A.; Pezeshki, A. Effects of citicoline on level of consciousness, serum level of fetuin-A and matrix Gla-protein (MGP) in trauma patients with diffuse axonal injury (DAI) and GCS ≤ 8. Ulus. Travma Acil Cerrahi Derg. 2014, 20, 410–416. [Google Scholar] [CrossRef] [PubMed]
- Espagno, J.; Trémoulet, M.; Gigaud, M.; Espagno, C. Étude de l’action de la CDP-choline dans les troubles de la vigilance posttraumatique. Vie Méd. 1979, 3, 95–196. [Google Scholar]
- Carcassonne, M.; Letourneau, J. Double-blind study of Rexort in childhood neurotrauma. Life Med. 1979, 12, 1007. [Google Scholar]
- Varadaraju, D.N.; Ananthakishan, A. Effect of cerebroprotein hydrolysate with citicoline versus citicoline alone in the initial management of head injury and its clinical outcome a prospective randomised comparative study. J. Evid. Based Med. Healthc. 2017, 4, 2835–2837. [Google Scholar]
- Titov, I.I.; Voloshinsky, O.V.; Martin, A.Y.; Vintonyak, I.V.; Nestor, I.I. Evaluation of neuroprotectoral therapy efficiency in TBI. Pain Anesth. Intensive Care 2018, 3, 61–68. [Google Scholar]
- Geng, H.J.; Xie, Y.M.; Zhang, M. Tabu search algorithm analysis on effect of Xingnaojing Injection in treatment of craniocerebral injury and complications in real world. Zhongguo Zhong Yao Za Zhi 2020, 45, 3324–3330. [Google Scholar] [CrossRef]
- Araki, O.; Ishii, S.; Kondo, Y. Biochemical studies of head injury and brain edema. Jpn. J. Med. Prog. 1961, 48, 519–539. [Google Scholar]
- Ogashiwa, M.; Sano, K.; Manaka, S.; Kitamura, K.; Kagawa, M.; Takeuchi, K. Effectiveness of CDP-choline on disturbance of consciousness (DOC): 1. An experimental study of concussive head injury in mice. 2. A controlled trial in patients with DOC. In Novel Biochemical, Pharmacological and Clinical Aspects of Cytidinediphosphocholine; Zappia, V., Kennedy, E.P., Nilsson, B.I., Galletti, P., Eds.; Elsevier Science Publishing: Amsterdam, The Netherlands, 1985; pp. 317–327. [Google Scholar]
- Uyama, T.; Shigemoto, K.; Yanagisawa, T. Therapeutic effect of CDP-choline on sequelae of head injury on cervical injury in particular. Comparison with analgesics by the doble blind method. In Proceedings of the Symposium on the Chemotherapies on the Sequelae of Head Injuries-—The 27th Annual Meeting of Japan Neurosurgical Society, Tokyo, Japan; 1968. [Google Scholar]
- Aniruddha, T.J.; Pillai, S.; Devi, B.I.; Sampath, S.; Chandramouli, B.A. Role of citicoline in the management of mild head injury. Indian J. Neurotrauma 2009, 6, 49–52. [Google Scholar]
- Ahmadi, J.; Hoseinzadeh-Chahkandak, F.; Roobiyat, M.Y.; Pourbagher-Shahri, A.M.; Irankhah, S.; Rajabpour-Sanati, A. Comparison of two different doses of citicoline in patients with traumatic brain injury. J. Surg. Trauma 2020, 8, 8–15. [Google Scholar]
- Maher, C.G.; Sherrington, C.; Herbert, R.D.; Moseley, A.M.; Elkins, M. Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys. Ther. 2003, 83, 713–721. [Google Scholar] [CrossRef] [PubMed]
- Wurtman, R.J.; Ulus, I.H.; Cansev, M.; Watkins, C.J.; Wang, L.; Marzloff, G. Synaptic proteins and phospholipids are increased in gerbil brain by administering uridine plus docosahexaenoic acid orally. Brain Res. 2006, 1088, 83–92. [Google Scholar] [CrossRef] [PubMed]
- Hurtado, O.; Cardenas, A.; Pradillo, J.M.; Morales, J.R.; Ortego, F.; Sobrino, T.; Castillo, J.; Moro, M.A.; Lizasoain, I. A chronic treatment with CDP-choline improves functional recovery and increases neuronal plasticity after experimental stroke. Neurobiol. Dis. 2007, 26, 105–111. [Google Scholar] [CrossRef]
- Diederich, K.; Frauenknecht, K.; Minnerup, J.; Schneider, B.K.; Schmidt, A.; Altach, E.; Eggert, V.; Sommer, C.J.; Schäbitz, W.R. Citicoline Enhances Neuroregenerative Processes After Experimental Stroke in Rats. Stroke 2012, 43, 1931–1940. [Google Scholar] [CrossRef]
- Krupinski, J.; Abudawood, M.; Matou-Nasri, S.; Al-Baradie, R.; Petcu, E.; Justicia, C.; Planas, A.; Liu, D.; Rovira, N.; Grau-Slevin, M.; et al. Citicoline induces angiogenesis improving survival of vascular/human brain microvessel endothelial cells through pathways involving ERK1/2 and insulin receptor substrate-1. Vasc. Cell 2012, 4, 20. [Google Scholar] [CrossRef] [PubMed]
- Turana, Y.; Nathaniel, M.; Shen, R.; Ali, S.; Aparasu, R.R. Citicoline and COVID-19-Related Cognitive and Other Neurologic Complications. Brain Sci. 2021, 12, 59. [Google Scholar] [CrossRef]
- Grieb, P.; Świątkiewicz, M.; Kamińska, A.; Jünemann, A.; Rejdak, R.; Rejdak, K. Citicoline: A Candidate for Adjunct Treatment of Multiple Sclerosis. Pharmaceuticals 2021, 14, 326. [Google Scholar] [CrossRef]
- Gareri, P.; Veronese, N.; Cotroneo, A.M. An Overview of Combination Treatment with Citicoline in Dementia. Rev. Recent Clin. Trials 2022, 17, 4–8. [Google Scholar] [CrossRef]


| Study | Year | n | Severity | Control | Doses | Outcome |
|---|---|---|---|---|---|---|
| Misbach et al. [26] | 1978 | 80 | Moderate to severe | Placebo | 300 mg IV × 14 d | Recovery rate at 14 d |
| Richer et al. [27] | 1980 | 60 | Severe | Placebo | 750 mg IV or IM × 20 d | GOS (like) at 3 m |
| Cohadon et al. [28] | 1982 | 60 | Severe | Placebo | 750 mg IV or IM × 20 d | GOS (like) at 2 m |
| Lecuire et al. [29] | 1982 | 25 | Moderate to severe | Meclofenoxate | 750 mg IV × 10 d | Global recovery at 10 d |
| Lecuire [30] | 1985 | 40 | Moderate to severe | Piracetam | 750 mg IV × 10 d | Global recovery at 1 m |
| Raggueneau et al. [31] | 1988 | 921 | Severe | Control | 500–750 mg IV × 20 d | GOS at 1 m |
| Calatayud et al. [32] | 1991 | 216 | Moderate to severe | Control | 3–4 g IV × 4 d 2 g po × 26 d | GOS at 3 m |
| Lozano [33] | 1991 | 78 | Moderate to severe | Control | 3–6 g IV × 1 | GOS at 1 m |
| Zafonte et al. [15] | 2012 | 1070 | Mild complicated, moderate, and severe | Placebo | 2 g po × 90 d | GOSe at 6 m |
| Krishna et al. [34] | 2012 | 87 | Moderate to severe | Placebo | 2 g po × 60 d | GOS at 90 d |
| Trimmel et al. [35] | 2018 | 134 | Severe | Control | 3 g IV × 21 d | GOSe at 6 m |
| Study | C1 | C2 | C3 | C4 | C5 | C6 | C7 | C8 | C9 | C10 | C11 | TOTAL |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Misbach et al. [26] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | 10 |
| Richer et al. [27] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 11 |
| Cohadon et al. [28] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 11 |
| Lecuire et al. [29] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 11 |
| Lecuire [30] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 11 |
| Raggueneau et al. [31] | Y | N | N | Y | Y | N | N | Y | Y | Y | Y | 7 |
| Calatayud et al. [32] | Y | Y | Y | Y | Y | N | N | Y | Y | Y | Y | 9 |
| Lozano [33] | Y | Y | Y | Y | Y | N | N | Y | Y | Y | Y | 9 |
| Zafonte et al. [15] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | 11 |
| Krishna et al. [34] | Y | Y | Y | Y | Y | Y | N | Y | Y | Y | N | 9 |
| Trimmel et al. [35] | Y | N | N | Y | Y | N | N | Y | Y | Y | Y | 7 |
| Model | No. of Studies | RR | 95% IC | I2 | τ2 |
|---|---|---|---|---|---|
| Main analysis | 11 | 1.18 | 1.05, 1.33 | 42.6% | 0.014 |
| Fixed effects | 11 | 1.11 | 1.03, 1.20 | 43.7% | - |
| Only RCT | 9 | 1.16 | 1.01, 1.33 | 39.4% | 0.015 |
| With route as moderator | Parenteral 9 Oro-enteral 2 | 1.25 1.03 | 1.08, 1.45 0.81, 1.31 | 42.8% | 0.017 |
| With dose as moderator | <2gr. 8 >2 gr. 3 | 1.21 1.18 | 1.02, 1.43 0.94, 1.49 | 47.4% | 0.022 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Secades, J.J.; Trimmel, H.; Salazar, B.; González, J.A. Citicoline for the Management of Patients with Traumatic Brain Injury in the Acute Phase: A Systematic Review and Meta-Analysis. Life 2023, 13, 369. https://doi.org/10.3390/life13020369
Secades JJ, Trimmel H, Salazar B, González JA. Citicoline for the Management of Patients with Traumatic Brain Injury in the Acute Phase: A Systematic Review and Meta-Analysis. Life. 2023; 13(2):369. https://doi.org/10.3390/life13020369
Chicago/Turabian StyleSecades, Julio José, Helmut Trimmel, Byron Salazar, and José Antonio González. 2023. "Citicoline for the Management of Patients with Traumatic Brain Injury in the Acute Phase: A Systematic Review and Meta-Analysis" Life 13, no. 2: 369. https://doi.org/10.3390/life13020369
APA StyleSecades, J. J., Trimmel, H., Salazar, B., & González, J. A. (2023). Citicoline for the Management of Patients with Traumatic Brain Injury in the Acute Phase: A Systematic Review and Meta-Analysis. Life, 13(2), 369. https://doi.org/10.3390/life13020369







