The Quantification of Non-Action Costs as an Incentive to Address Water Pollution Problems
Abstract
1. Introduction
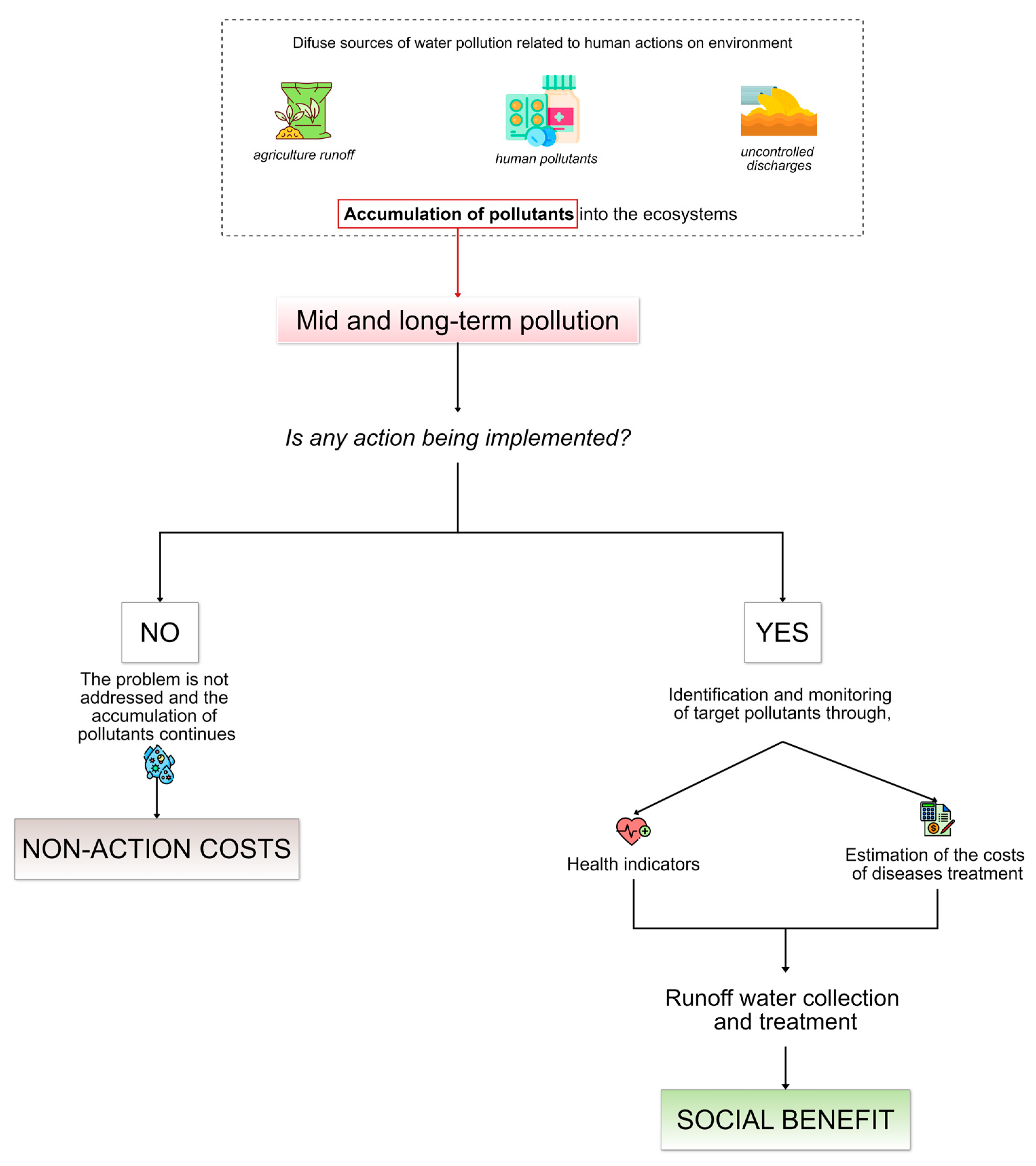
2. Non-Action Costs Considered as a Proxy for the Social Impact of Water Pollution
2.1. How Are Healthcare Costs Related to Non-Action Costs?
2.2. Methodologies for Monetary Valuation of Social Externalities and Healthcare Costs
2.2.1. Shadow Prices
2.2.2. Contingent Valuation
2.2.3. Choice Experiment
2.2.4. Benefit Transfer
2.3. Quantification of Healthcare Costs Caused by Polluted-Water Exposure and Consumption: Literature Studies
2.3.1. Nitrates
2.3.2. Pesticides
2.3.3. Metals
Cadmium
Chromium
Lead
2.4. Other Pollutants to Consider
2.4.1. Neurotoxicants Such as Lead, Methylmercury, and Polybrominated Diphenyl Ethers
2.4.2. Air Pollution
2.4.3. Endocrine Disruptors
3. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Xiao, S.; Hu, S.; Zhang, Y.; Zhao, X.; Pan, W. Influence of sewage treatment plant effluent discharge into multipurpose river on its water quality: A quantitative health risk assessment of Cryptosporidium and Giardia. Environ. Pollut. 2018, 233, 797–805. [Google Scholar] [CrossRef] [PubMed]
- UN. Informe Mundial de las Naciones Unidas Sobre el Desarrollo de los Recursos Hídricos 2021: El Valor del Agua; UNESCO: París, France, 2021. [Google Scholar]
- FAO. Progresos en el Nivel de Estrés Hídrico: Valores de Referencia Mundiales Para el Indicador 6.4.2 de los ODS; FAO and UN-WATER: Roma, Italy, 2018. [Google Scholar]
- UN-Agua. Progresos en los Ecosistemas Relacionados con el Agua. Prueba Piloto de la Metodología de Monitoreo y Primeras Constataciones Sobre el Indicador 6.6.1 de los ODS; UN-WATER: New York, NY, USA, 2018. [Google Scholar]
- Arauzo, M.; Valladolid, M.; García, G.; Andries, D.M. N and P behaviour in alluvial aquifers and in the soil solution of their catchment areas: How land use and the physical environment contribute to diffuse pollution. Sci. Total. Environ. 2022, 804, 150056. [Google Scholar] [CrossRef] [PubMed]
- Hernández-Sancho, F.; Lamizana-Diallo, B.; Mateo-Sagasta, J.; Qadir, M. Economic Valuation of Wastewater—The Cost of Action and the Cost of no Action; United Nations Environment Programme (UNEP): Nairobi, Kenya, 2015. [Google Scholar]
- Carvalho, D.J.; Costa, M.E.L.; Koide, S. Assessment of Diffuse Pollution Loads in Peri-Urban Rivers—Analysis of the Accuracy of Estimation Based on Monthly Monitoring Data. Water 2022, 14, 2354. [Google Scholar] [CrossRef]
- Bellver-Domingo, A.; Fuentes, R.; Hernández-Sancho, F. Shadow prices of emerging pollutants in wastewater treatment plants: Quantification of environmental externalities. J. Environ. Manag. 2017, 203, 439–447. [Google Scholar] [CrossRef] [PubMed]
- Lanrewaju, A.A.; Enitan-Folami, A.M.; Sabiu, S.; Edokpayi, J.N.; Swalaha, F.M. Global public health implications of human exposure to viral contaminated water. Front. Microbiol. 2022, 13, 981896. [Google Scholar] [CrossRef]
- CDC. National Health and Nutrition Examination Survey Data. Available online: https://www.cdc.gov/nchs/nhanes/index.htm (accessed on 10 January 2023).
- Zhang, Z.; Wang, S.; Li, L. Emerging investigator series: The role of chemical properties in human exposure to environmental chemicals. Environ. Sci. Process. Impacts 2021, 23, 1839–1862. [Google Scholar] [CrossRef]
- Gaylord, A.; Osborne, G.; Ghassabian, A.; Malits, J.; Attina, T.; Trasande, L. Trends in neurodevelopmental disability burden due to early life chemical exposure in the USA from 2001 to 2016: A population-based disease burden and cost analysis. Mol. Cell. Endocrinol. 2020, 502, 110666. [Google Scholar] [CrossRef]
- Fiedler, B.A. 12—environmental perspectives from the ground up: The cost of poor environmental health on human health. In Three Facets of Public Health and Paths to Improvements; Fiedler, B.A., Ed.; Academic Press: Cambridge, MA, USA, 2020; Available online: https://www.sciencedirect.com/science/article/pii/B9780128190081000122 (accessed on 5 January 2023). [CrossRef]
- Norman, R.E.; Carpenter, D.O.; Scott, J.; Brune, M.N.; Sly, P. Environmental exposures: An underrecognized contribution to noncommunicable diseases. Rev. Environ. Health 2013, 28, 59–65. [Google Scholar] [CrossRef]
- Woodruff, T.J. Making It Real—The Environmental Burden of Disease. What Does It Take to Make People Pay Attention to the Environment and Health? J. Clin. Endocrinol. Metab. 2015, 100, 1241–1244. [Google Scholar] [CrossRef]
- Grandjean, P.; Bellanger, M. Calculation of the disease burden associated with environmental chemical exposures: Application of toxicological information in health economic estimation. Environ. Health 2017, 16, 123. [Google Scholar] [CrossRef]
- OECD. Costs of Inaction on Key Environmental Challenges; OECD: Paris, France, 2008. [Google Scholar]
- Bellver-Domingo, A.; Fuentes, R.; Hernández-Sancho, F. Reclaimed water and irrigation: A cost-benefit analysis for desalination of WWTPs effluents. Desalination Water Treat. 2019, 166, 193–201. [Google Scholar] [CrossRef]
- Bellver-Domingo, A.; Hernández-Sancho, F. Environmental Benefit of Improving Wastewater Quality: A Shadow Prices Approach for Sensitive Areas. Water Econ. Policy 2017, 4, 1750008. [Google Scholar] [CrossRef]
- Easter, K.W.; Konishi, Y. What Are the Economic Health Costs of Non-action in Controlling Toxic Water Pollution? Int. J. Water Resour. Dev. 2006, 22, 529–541. [Google Scholar] [CrossRef]
- Hernández-Sancho, F.; Bellver-Domingo, Á. Economics and innovative financing mechanisms in a circular economy. In Unconventional Water Resources; Qadir, M., Smakhtin, V., Koo-Oshima, S., Guenther, E., Eds.; Springer International Publishing: Cham, Switzerland, 2022. [Google Scholar] [CrossRef]
- Fare, R.; Grosskopf, S.; Lovell, C.A.K.; Yaisawarng, S. Derivation of Shadow Prices for Undesirable Outputs: A Distance Function Approach. Rev. Econ. Stat. 1993, 75, 374. [Google Scholar] [CrossRef]
- Hernández-Sancho, F.; Molinos-Senante, M.; Sala-Garrido, R. Economic valuation of environmental benefits from wastewater treatment processes: An empirical approach for Spain. Sci. Total. Environ. 2010, 408, 953–957. [Google Scholar] [CrossRef]
- Wei, C.; Löschel, A.; Liu, B. An empirical analysis of the CO2 shadow price in Chinese thermal power enterprises. Energy Econ. 2013, 40, 22–31. [Google Scholar] [CrossRef]
- Hernández-Sancho, F.; Bellver-Domingo, A. Environmentally adjusted efficiency of municipal water suppliers. In Environmentally Adjusted Efficiency of Municipal Water Suppliers; Edward Elgar Publishing: Cheltenham, UK, 2017. [Google Scholar]
- Bellver-Domingo, A.; Fuentes, R.; Hernández-Sancho, F.; Carmona, E.; Picó, Y.; Hernández-Chover, V. Monetary valuation of salicylic acid, methylparaben and THCOOH in a Mediterranean coastal wetland through the shadow prices methodology. Sci. Total. Environ. 2018, 627, 869–879. [Google Scholar] [CrossRef]
- Linares, P.; Romero, C. Economy and environmental: Tools for environmental valuation [in spanish]. In Tratado de Tributación Medioambiental 2008, 2, 1189–1225. [Google Scholar]
- Damigos, D.; Menegaki, M.; Kaliampakos, D. Monetizing the social benefits of landfill mining: Evidence from a Contingent Valuation survey in a rural area in Greece. Waste Manag. 2016, 51, 119–129. [Google Scholar] [CrossRef]
- Kuhfuss, L.; Hanley, N.; Whyte, R. Should historic sites protection be targeted at the most famous? Evidence from a contingent valuation in Scotland. J. Cult. Heritage 2016, 20, 682–685. [Google Scholar] [CrossRef]
- He, J.; Huang, A.; Xu, L. Spatial heterogeneity and transboundary pollution: A contingent valuation (CV) study on the Xijiang River drainage basin in south China. China Econ. Rev. 2015, 36, 101–130. [Google Scholar] [CrossRef]
- Desaigues, B.; Ami, D.; Bartczak, A.; Kohlová, M.B.; Chilton, S.; Czajkowski, M.; Farreras, V.; Hunt, A.; Hutchison, M.; Jeanrenaud, C.; et al. Economic valuation of air pollution mortality: A 9-country contingent valuation survey of value of a life year (VOLY). Ecol. Indic. 2011, 11, 902–910. [Google Scholar] [CrossRef]
- MacKerron, G.J.; Egerton, C.; Gaskell, C.; Parpia, A.; Mourato, S. Willingness to pay for carbon offset certification and co-benefits among (high-)flying young adults in the UK. Energy Policy 2009, 37, 1372–1381. [Google Scholar] [CrossRef]
- Perez-Verdin, G.; Sanjurjo-Rivera, E.; Galicia, L.; Hernandez-Diaz, J.C.; Hernandez-Trejo, V.; Marquez-Linares, M.A. Economic valuation of ecosystem services in Mexico: Current status and trends. Ecosyst. Serv. 2016, 21, 6–19. [Google Scholar] [CrossRef]
- Patenaude, B.N.; Semali, I.; Killewo, J.; Bärnighausen, T. The Value of a Statistical Life-Year in Sub-Saharan Africa: Evidence From a Large Population-Based Survey in Tanzania. Value Health Reg. Issues 2019, 19, 151–156. [Google Scholar] [CrossRef]
- Mussio, I.; Brandt, S.; Hanemann, M. Parental beliefs and willingness to pay for reduction in their child’s asthma symptoms: A joint estimation approach. Health Econ. 2021, 30, 129–143. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Jin, J.; He, R.; Gong, H.; Tian, Y. Farmers’ Willingness to Pay for Health Risk Reductions of Pesticide Use in China: A Contingent Valuation Study. Int. J. Environ. Res. Public Health 2018, 15, 625. [Google Scholar] [CrossRef]
- Mundaca, G. Economic valuation of environmental and health impacts from mining: The case of Peru. Environ. Dev. Sustain. 2022, 1–27. [Google Scholar] [CrossRef]
- Graham, H.; de Bell, S.; Hanley, N.; Jarvis, S.; White, P. Willingness to pay for policies to reduce future deaths from climate change: Evidence from a British survey. Public Health 2019, 174, 110–117. [Google Scholar] [CrossRef]
- Bai, R.; Lam, J.C.; Li, V.O. A review on health cost accounting of air pollution in China. Environ. Int. 2018, 120, 279–294. [Google Scholar] [CrossRef]
- Guerriero, C.; Chatzidiakou, L.; Cairns, J.; Mumovic, D. The economic benefits of reducing the levels of nitrogen dioxide (NO2) near primary schools: The case of London. J. Environ. Manag. 2016, 181, 615–622. [Google Scholar] [CrossRef] [PubMed]
- Istamto, T.; Houthuijs, D.; Lebret, E. Willingness to pay to avoid health risks from road-traffic-related air pollution and noise across five countries. Sci. Total. Environ. 2014, 497, 420–429. [Google Scholar] [CrossRef] [PubMed]
- Deh-Haghi, Z.; Bagheri, A.; Damalas, C.A.; Fotourehchi, Z. Horticultural products irrigated with treated sewage: Are they acceptable? Environ. Sci. Pollut. Res. 2021, 28, 54057–54068. [Google Scholar] [CrossRef]
- Gerard, K.; Mandy, R.; Amaya-Amaya, M. Using Discrete Choice Experiments to Value Health and Health Care. 2008. Available online: https://link.springer.com/content/pdf/bfm:978-1-4020-5753-3/1 (accessed on 15 January 2023). [CrossRef]
- Rolfe, J.; Rajapaksa, D.; De Valck, J.; Star, M. Will greenhouse concerns impact meat consumption? Best-worst scaling analysis of Australian consumers. Food Qual. Prefer. 2023, 104, 104755. [Google Scholar] [CrossRef]
- Mazzocchi, C.; Orsi, L.; Zilia, F.; Costantini, M.; Bacenetti, J. Consumer awareness of sustainable supply chains: A choice experiment on Parma ham PDO. Sci. Total. Environ. 2022, 836, 155602. [Google Scholar] [CrossRef]
- Bruzzese, S.; Blanc, S.; Merlino, V.M.; Massaglia, S.; Brun, F. Civil society’s perception of forest ecosystem services. A case study in the Western Alps. Front. Psychol. 2022, 13, 1000043. [Google Scholar] [CrossRef]
- Castillo-Eguskitza, N.; Hoyos, D.; Onaindia, M.; Czajkowski, M. Unraveling local preferences and willingness to pay for different management scenarios: A choice experiment to biosphere reserve management. Land Use Policy 2019, 88, 104200. [Google Scholar] [CrossRef]
- Badura, T.; Lorencová, E.K.; Ferrini, S.; Vačkářová, D. Public support for urban climate adaptation policy through nature-based solutions in Prague. Landsc. Urban Plan. 2021, 215, 104215. [Google Scholar] [CrossRef]
- L’Ecuyer-Sauvageau, C.; Kermagoret, C.; Dupras, J.; He, J.; Leroux, J.; Schinck, M.-P.; Poder, T.G. Understanding the preferences of water users in a context of cyanobacterial blooms in Quebec. J. Environ. Manag. 2019, 248, 109271. [Google Scholar] [CrossRef]
- Markandya, A.; Ortiz, R.A.; Chiabai, A. Estimating environmental health costs: General introduction to valuation of human health risks. In Encyclopedia of Environmental Health, 2nd ed.; Nriagu, J., Ed.; Elsevier: Oxford, UK, 2019; pp. 719–727. [Google Scholar]
- Herrera-Araujo, D.; Mikecz, O.; Pica-Ciamarra, U. Placing a monetary value on the human health component of zoonotic diseases: A methodological note with an application to cysticercosis in Africa. Prev. Veter Med. 2020, 175, 104862. [Google Scholar] [CrossRef]
- Schaider, L.A.; Swetschinski, L.; Campbell, C.; Rudel, R.A. Environmental justice and drinking water quality: Are there socioeconomic disparities in nitrate levels in U.S. drinking water? Environ. Health 2019, 18, 3. [Google Scholar] [CrossRef] [PubMed]
- Espejo-Herrera, N.; Gràcia-Lavedan, E.; Boldo, E.; Aragones, N.; Pérez-Gómez, B.; Pollan, M.; Molina, A.J.; Fernández, T.; Martín, V.; La Vecchia, C.; et al. Colorectal cancer risk and nitrate exposure through drinking water and diet. Int. J. Cancer 2016, 139, 334–346. [Google Scholar] [CrossRef]
- Temkin, A.; Evans, S.; Manidis, T.; Campbell, C.; Naidenko, O.V. Exposure-based assessment and economic valuation of adverse birth outcomes and cancer risk due to nitrate in United States drinking water. Environ. Res. 2019, 176, 108442. [Google Scholar] [CrossRef]
- Bellver-Domingo, Á.; Hernández-Sancho, F. Circular economy and payment for ecosystem services: A framework proposal based on water reuse. J. Environ. Manag. 2022, 305, 114416. [Google Scholar] [CrossRef]
- Pimentel, D.; Burgess, M. Environmental and Economic Costs of the Application of Pesticides Primarily in the United States. In Integrated Pest Management: Pesticide Problems; Pimentel, D., Peshin, R., Eds.; Springer: Dordrecht, The Netherlands, 2014; Volume 3, pp. 47–71. [Google Scholar] [CrossRef]
- Bourguet, D.; Guillemaud, T. The hidden and external costs of pesticide use. In Sustainable Agriculture Reviews, 1st ed.; Lichtfouse, E., Ed.; Springer: Cham, Switzerland, 2016; Volume 19, pp. 35–120. [Google Scholar]
- Ngowi, A.; Mbise, T.; Ijani, A.; London, L.; Ajayi, O. Pesticides use by smallholder farmers in vegetable production in Northern Tanzania. Crop. Prot. 2007, 26, 1617–1624. [Google Scholar] [CrossRef] [PubMed]
- Pretty, J.N.; Brett, C.; Gee, D.; Hine, R.E.; Mason, C.F.; Morison, J.I.L.; Raven, H.; Rayment, M.D.; Van Der Bijl, G. An assessment of the total external costs of UK agriculture. Agric. Syst. 2000, 65, 113–136. [Google Scholar] [CrossRef]
- Alexakis, D.E.; Kiskira, K.; Gamvroula, D.; Emmanouil, C.; Psomopoulos, C.S. Evaluating toxic element contamination sources in groundwater bodies of two Mediterranean sites. Environ. Sci. Pollut. Res. 2021, 28, 34400–34409. [Google Scholar] [CrossRef]
- Khafouri, A.; Talbi, E.H.; Abdelouas, A.; Benjmel, K.; Antunes, I.M.H.R.; Abioui, M. Groundwater Vulnerability and Potentially Toxic Elements Associated with the Iron Mining District of Ouixane (Northeast of Morocco). Water 2023, 15, 118. [Google Scholar] [CrossRef]
- Maruzeni, S.; Nishijo, M.; Nakamura, K.; Morikawa, Y.; Sakurai, M.; Nakashima, M.; Kido, T.; Okamoto, R.; Nogawa, K.; Suwazono, Y.; et al. Mortality and causes of deaths of inhabitants with renal dysfunction induced by cadmium exposure of the polluted Jinzu River basin, Toyama, Japan; a 26-year follow-up. Environ. Health 2014, 13, 18. [Google Scholar] [CrossRef]
- Bharagava, R.N.; Mishra, S. Hexavalent chromium reduction potential of Cellulosimicrobium sp. isolated from common effluent treatment plant of tannery industries. Ecotoxicol. Environ. Saf. 2018, 147, 102–109. [Google Scholar] [CrossRef]
- Yoshinaga, M.; Ninomiya, H.; Al Hossain, M.A.; Sudo, M.; Akhand, A.A.; Ahsan, N.; Alim, A.; Khalequzzaman; Iida, M.; Yajima, I.; et al. A comprehensive study including monitoring, assessment of health effects and development of a remediation method for chromium pollution. Chemosphere 2018, 201, 667–675. [Google Scholar] [CrossRef] [PubMed]
- Tseng, C.-H.; Lei, C.; Chen, Y.-C. Evaluating the health costs of oral hexavalent chromium exposure from water pollution: A case study in Taiwan. J. Clean. Prod. 2018, 172, 819–826. [Google Scholar] [CrossRef]
- Hanna-Attisha, M.; Lachance, J.; Sadler, R.C.; Schnepp, A.C. Elevated Blood Lead Levels in Children Associated with the Flint Drinking Water Crisis: A Spatial Analysis of Risk and Public Health Response. Am. J. Public Health 2016, 106, 283–290. [Google Scholar] [CrossRef]
- Agency for Toxic Substances and Disease Registry (ATSDR). Toxicological Profile for LEAD; U.S. Department of Health and Human Services, Public Health Service: Atlanta, GA, USA, 2020.
- Katner, A.L.; Brown, K.; Pieper, K.; Edwards, M.; Lambrinidou, Y.; Subra, W. America’s path to drinking water infrastructure inequality and environmental injustice: The case of flint, Michigan. In The Palgrave Handbook of Sustainability: Case Studies and Practical Solutions; Brinkmann, R., Garren, S.J., Eds.; Springer: Berlin/Heidelberg, Germany, 2018. [Google Scholar] [CrossRef]
- Sorensen, L.C.; Fox, A.M.; Jung, H.; Martin, E.G. Lead exposure and academic achievement: Evidence from childhood lead poisoning prevention efforts. J. Popul. Econ. 2019, 32, 179–218. [Google Scholar] [CrossRef]
- AWWA. Buried No Longer: Confronting America’s Water Infrastructure Challenge; American Water Works Association: Boulder, Colorado, 2013. [Google Scholar]
- Gould, E. Childhood Lead Poisoning: Conservative Estimates of the Social and Economic Benefits of Lead Hazard Control. Environ. Health Perspect. 2009, 117, 1162–1167. [Google Scholar] [CrossRef]
- Landrigan, P.J.; Schechter, C.B.; Lipton, J.M.; Fahs, M.C.; Schwartz, J. Environmental pollutants and disease in American children: Estimates of morbidity, mortality, and costs for lead poisoning, asthma, cancer, and developmental disabilities. Environ. Cite hHealth Perspect. 2002, 110, 721–728. [Google Scholar] [CrossRef] [PubMed]
- Trasande, L.; Liu, B.; Bao, W. Phthalates and attributable mortality: A population-based longitudinal cohort study and cost analysis. Environ. Pollut. 2022, 292, 118021. [Google Scholar] [CrossRef]
- Lu, W.; Levin, R.; Schwartz, J. Lead contamination of public drinking water and academic achievements among children in Massachusetts: A panel study. BMC Public Health 2022, 22, 107. [Google Scholar] [CrossRef]
- Bartlett, E.S.; Trasande, L. Economic impacts of environmentally attributable childhood health outcomes in the European Union. Eur. J. Public Health 2013, 24, 21–26. [Google Scholar] [CrossRef]
- Grosse, S.D.; Matte, T.D.; Schwartz, J.; Jackson, R.J. Economic gains resulting from the reduction in children’s exposure to lead in the United States. Environ. Health Perspect. 2002, 110, 563–569. [Google Scholar] [CrossRef]
- Pichery, C.; Bellanger, M.; Zmirou-Navier, D.; Fréry, N.; Cordier, S.; Roue-LeGall, A.; Hartemann, P.; Grandjean, P. Economic evaluation of health consequences of prenatal methylmercury exposure in France. Environ. Health 2012, 11, 53. [Google Scholar] [CrossRef] [PubMed]
- Brumberg, H.L.; Karr, C.J.; Bole, A.; Ahdoot, S.; Balk, S.J.; Bernstein, A.S.; Byron, L.G.; Landrigan, P.J.; Marcus, S.M.; Nerlinger, A.L.; et al. Ambient Air Pollution: Health Hazards to Children. Pediatrics 2021, 147, e2021051484. [Google Scholar] [CrossRef] [PubMed]
- WHO. WHO Air Quality Guidelines for Particulate Matter, Ozone, Nitrogen Dioxide and Sulfur Dioxide (WHO/SDE/PHE/OEH/06.02); World Health Organization: Geneva, Switzerland, 2005.
- Garrett, P.; Casimiro, E. Short-term effect of fine particulate matter (PM2.5) and ozone on daily mortality in Lisbon, Portugal. Environ. Sci. Pollut. Res. 2011, 18, 1585–1592. [Google Scholar] [CrossRef] [PubMed]
- Faustini, A.; Stafoggia, M.; Berti, G.; Bisanti, L.; Chiusolo, M.; Cernigliaro, A.; Mallone, S.; Primerano, R.; Scarnato, C.; Simonato, L.; et al. The relationship between ambient particulate matter and respiratory mortality: A multi-city study in Italy. Eur. Respir. J. 2011, 38, 538–547. [Google Scholar] [CrossRef]
- Brook, R.D.; Rajagopalan, S.; Pope, C.A., 3rd; Brook, J.R.; Bhatnagar, A.; Diez-Roux, A.V.; Holguin, F.; Hong, Y.; Luepker, R.V.; Mittleman, M.A.; et al. Particulate Matter Air Pollution and Cardiovascular Disease: An update to the scientific statement from the american heart association. Circulation 2010, 121, 2331–2378. [Google Scholar] [CrossRef]
- Woodruff, T.J.; Parker, J.D.; Darrow, L.A.; Slama, R.; Bell, M.L.; Choi, H.; Glinianaia, S.; Hoggatt, K.J.; Karr, C.J.; Lobdell, D.T.; et al. Methodological issues in studies of air pollution and reproductive health. Environ. Res. 2009, 109, 311–320. [Google Scholar] [CrossRef]
- Li, R.; Hopke, P.K.; Dozier, A.; Thurston, S.W.; Thevenet-Morrison, K.; Croft, D.; Masiol, M.; Squizzato, S.; Chalupa, D.; Rich, D.Q. Term birth weight and ambient air pollutant concentrations during pregnancy, among women living in Monroe County, New York. J. Expo. Sci. Environ. Epidemiol. 2019, 29, 500–509. [Google Scholar] [CrossRef]
- Fleischer, N.L.; Merialdi, M.; Van Donkelaar, A.; Vadillo-Ortega, F.; Martin, R.; Betran, A.P.; Souza, J.P.; O’neill, M.S. Outdoor Air Pollution, Preterm Birth, and Low Birth Weight: Analysis of the World Health Organization Global Survey on Maternal and Perinatal Health. Environ. Health Perspect. 2014, 122, 425–430. [Google Scholar] [CrossRef]
- Sunyer, J.; Esnaola, M.; Alvarez-Pedrerol, M.; Forns, J.; Rivas, I.; López-Vicente, M.; Suades-González, E.; Foraster, M.; Garcia-Esteban, R.; Basagaña, X.; et al. Association between Traffic-Related Air Pollution in Schools and Cognitive Development in Primary School Children: A Prospective Cohort Study. PLOS Med. 2015, 12, e1001792. [Google Scholar] [CrossRef]
- Pascal, M.; Corso, M.; Chanel, O.; Declercq, C.; Badaloni, C.; Cesaroni, G.; Henschel, S.; Meister, K.; Haluza, D.; Martin-Olmedo, P.; et al. Assessing the public health impacts of urban air pollution in 25 European cities: Results of the Aphekom project. Sci. Total. Environ. 2013, 449, 390–400. [Google Scholar] [CrossRef]
- Marle, M.V.D.A.-V.; Bruil, J.; Detmar, S. Evaluation of cost of disease: Assessing the burden to society of asthma in children in the European Union. Allergy 2005, 60, 140–149. [Google Scholar] [CrossRef] [PubMed]
- Trasande, L.; Wong, K.; Roy, A.; Savitz, D.A.; Thurston, G. Exploring prenatal outdoor air pollution, birth outcomes and neonatal health care utilization in a nationally representative sample. J. Expo. Sci. Environ. Epidemiol. 2013, 23, 315–321. [Google Scholar] [CrossRef] [PubMed]
- Rocha, C.A.; Lima, J.L.; Mendonça, K.V.; Marques, E.V.; Zanella, M.E.; Ribeiro, J.P.; Bertoncini, B.V.; Branco, V.T.C.; Cavalcante, R.M. Health impact assessment of air pollution in the metropolitan region of Fortaleza, Ceará, Brazil. Atmos. Environ. 2020, 241, 117751. [Google Scholar] [CrossRef]
- Trasande, L.; Zoeller, R.T.; Hass, U.; Kortenkamp, A.; Grandjean, P.; Myers, J.P.; DiGangi, J.; Bellanger, M.; Hauser, R.; Legler, J.; et al. Estimating Burden and Disease Costs of Exposure to Endocrine-Disrupting Chemicals in the European Union. J. Clin. Endocrinol. Metab. 2015, 100, 1245–1255. [Google Scholar] [CrossRef]
- Malits, J.; Naidu, M.; Trasande, L. Exposure to Endocrine Disrupting Chemicals in Canada: Population-Based Estimates of Disease Burden and Economic Costs. Toxics 2022, 10, 146. [Google Scholar] [CrossRef]
- Trasande, L.; Zoeller, R.T.; Hass, U.; Kortenkamp, A.; Grandjean, P.; Myers, J.P.; DiGangi, J.; Hunt, P.M.; Rudel, R.; Sathyanarayana, S.; et al. Burden of disease and costs of exposure to endocrine disrupting chemicals in the European Union: An updated analysis. Andrology 2016, 4, 565–572. [Google Scholar] [CrossRef]
- Attina, T.M.; Hauser, R.; Sathyanarayana, S.; Hunt, P.A.; Bourguignon, J.-P.; Myers, J.P.; DiGangi, J.; Zoeller, R.T.; Trasande, L. Exposure to endocrine-disrupting chemicals in the USA: A population-based disease burden and cost analysis. Lancet Diabetes Endocrinol. 2016, 4, 996–1003. [Google Scholar] [CrossRef]
- Das, A.M.; Gogia, A.; Janardhanan, R.; Babu-Rajendran, R.; Das, B.C. Environmental Contamination and Chronic Exposure to Endocrine-Disrupting Phthalates: An Overlooked and Emerging Determinant for Hormone-Sensitive Cancers. J. Indian Inst. Sci. 2022, 102, 731–742. [Google Scholar] [CrossRef]
- Pérez-Carrascosa, F.M.; Barrios-Rodríguez, R.; Gómez-Peña, C.; Salcedo-Bellido, I.; Velasco-García, M.E.; Moleón, J.J.J.; García-Ruiz, A.; Navarro-Espigares, J.L.; Requena, P.; Muñoz-Sánchez, C.; et al. Public healthcare costs associated with long-term exposure to mixtures of persistent organic pollutants in two areas of Southern Spain: A longitudinal analysis. Environ. Res. 2022, 213, 113609. [Google Scholar] [CrossRef]
- Gibson, J.M.; Fisher, M.; Clonch, A.; MacDonald, J.M.; Cook, P.J. Children drinking private well water have higher blood lead than those with city water. Proc. Natl. Acad. Sci. USA 2020, 117, 16898–16907. [Google Scholar] [CrossRef]
- Misopoulos, F.; Argyropoulou, R.; Manthou, V.; Kelmendi, I.; Argyropoulou, M. Carbon emissions of bottled water sector supply chains: A multiple case-study approach. Int. J. Logist. Res. Appl. 2019, 23, 178–194. [Google Scholar] [CrossRef]
- Botto, S.; Niccolucci, V.; Rugani, B.; Nicolardi, V.; Bastianoni, S.; Gaggi, C. Towards lower carbon footprint patterns of consumption: The case of drinking water in Italy. Environ. Sci. Policy 2011, 14, 388–395. [Google Scholar] [CrossRef]

| Health | Environment | Productive Activities |
|---|---|---|
| Increased risk of diseases caused by loss of quality in drinking and bathing water and unsafe food (polluted water used to produce vegetables or fish). Increased financial costs of healthcare | Loss of biodiversity. Unsuitable quality of ecosystems. Greenhouse gas emissions. Loss of recreational value of ecosystems. | Loss of productivity in the agricultural and industrial sectors. Reduced market value of unsafe products. Loss of earnings from tourism activities. |
| Oral Ingestion | Nasal Absorption | Dermal Contact |
|---|---|---|
| Bioaccumulation in food | Chemicals in gas phase (vapor) | Cosmetics |
| Drinking water | Chemicals in particulate phase (aerosols, suspended dust) | Personal care products |
| Step 1—Identification | Step 2—Methodology Selection | Step 3—Valorization | |||
|---|---|---|---|---|---|
| Identifying goods and services (social and environmental) affected by pollution | Section 2.1. | Applying the appropriate methodology to assess short-, medium-, and long-term effects of pollution exposure | Section 2.2. | Assessing the results of the methodology applied to establish the baseline scenario | Section 2.3 and Section 2.4. |
| Pollutant | Shadow Price | Units | Source |
|---|---|---|---|
| Nitrogen | 66 | EUR /kg | [19] |
| Phosphorus | 264 | ||
| Salts (conductivity) | 62 | [18] | |
| Trimethoprim | 0.4 | EUR /mg | [8] |
| Acetaminophen | 128.2 | ||
| Ibuprofen | 11 | ||
| Naproxen | 3.4 | ||
| Carbamazepine | 0.6 | ||
| Salicylic acid | 33.5 | EUR /µg | [26] |
| Methylparaben | 24.6 | ||
| THCOOH | 30.8 |
| Cancer Type | Cancer Cases Attributable to Consumption of Water with Nitrates | Economic Losses Due to Loss of Productive Activity (Billions of Dollars) | Medical Costs of Healthcare Treatment (Billions of Dollars) |
|---|---|---|---|
| Colorectal | 24,479 | 11.56 | 3.13 |
| Ovaries | 690 | 0.56 | 0.13 |
| Thyroid | 1416 | 1.15 | N/A |
| Kidney | 454 | 0.25 | 0.06 |
| Bladder | 134 | 0.03 | 0.01 |
| Type | Pollutant | Disease | Economic Cost ($billion/Year) |
|---|---|---|---|
| Neurotoxicants | Lead exposure | Cognitive deficits | 876.7–1373.5 |
| Methylmercury a | 13.8–16.9 | ||
| Polybrominated diphenyl ethers b | 135.08–396.4 | ||
| Air pollutants | N/A | Asthma in European Union | 0.568–1.98 |
| Cardiovascular problems | 24.47–49.83 | ||
| Endocrine disruptors | Aldrin c, bisphenols d, dichlorodiphenyltrichloroethane (DDE) e, lindane c, organic and inorganic mercury, organophosphates f, polybrominated diphenyl ethers b, and phthalates d | Childhood and adult obesity, testicular cancer, male infertility, and mortality associated with reduced testosterone, fibroids, and endometriosis | 110–359 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bellver-Domingo, Á.; Castellet-Viciano, L.; Hernández-Chover, V.; Hernández-Sancho, F. The Quantification of Non-Action Costs as an Incentive to Address Water Pollution Problems. Water 2023, 15, 582. https://doi.org/10.3390/w15030582
Bellver-Domingo Á, Castellet-Viciano L, Hernández-Chover V, Hernández-Sancho F. The Quantification of Non-Action Costs as an Incentive to Address Water Pollution Problems. Water. 2023; 15(3):582. https://doi.org/10.3390/w15030582
Chicago/Turabian StyleBellver-Domingo, Águeda, Lledó Castellet-Viciano, Vicent Hernández-Chover, and Francesc Hernández-Sancho. 2023. "The Quantification of Non-Action Costs as an Incentive to Address Water Pollution Problems" Water 15, no. 3: 582. https://doi.org/10.3390/w15030582
APA StyleBellver-Domingo, Á., Castellet-Viciano, L., Hernández-Chover, V., & Hernández-Sancho, F. (2023). The Quantification of Non-Action Costs as an Incentive to Address Water Pollution Problems. Water, 15(3), 582. https://doi.org/10.3390/w15030582






