Clinical Aspects of Genetic and Non-Genetic Cardiovascular Risk Factors in Familial Hypercholesterolemia
Abstract
1. Introduction
2. Familial Hypercholesterolemia as Cardiovascular Risk Factor
3. Genetic Causes of Familial Hypercholesterolemia
4. Concomitant Genetic Abnormalities
5. Genes Implicated in Lipoprotein Metabolism
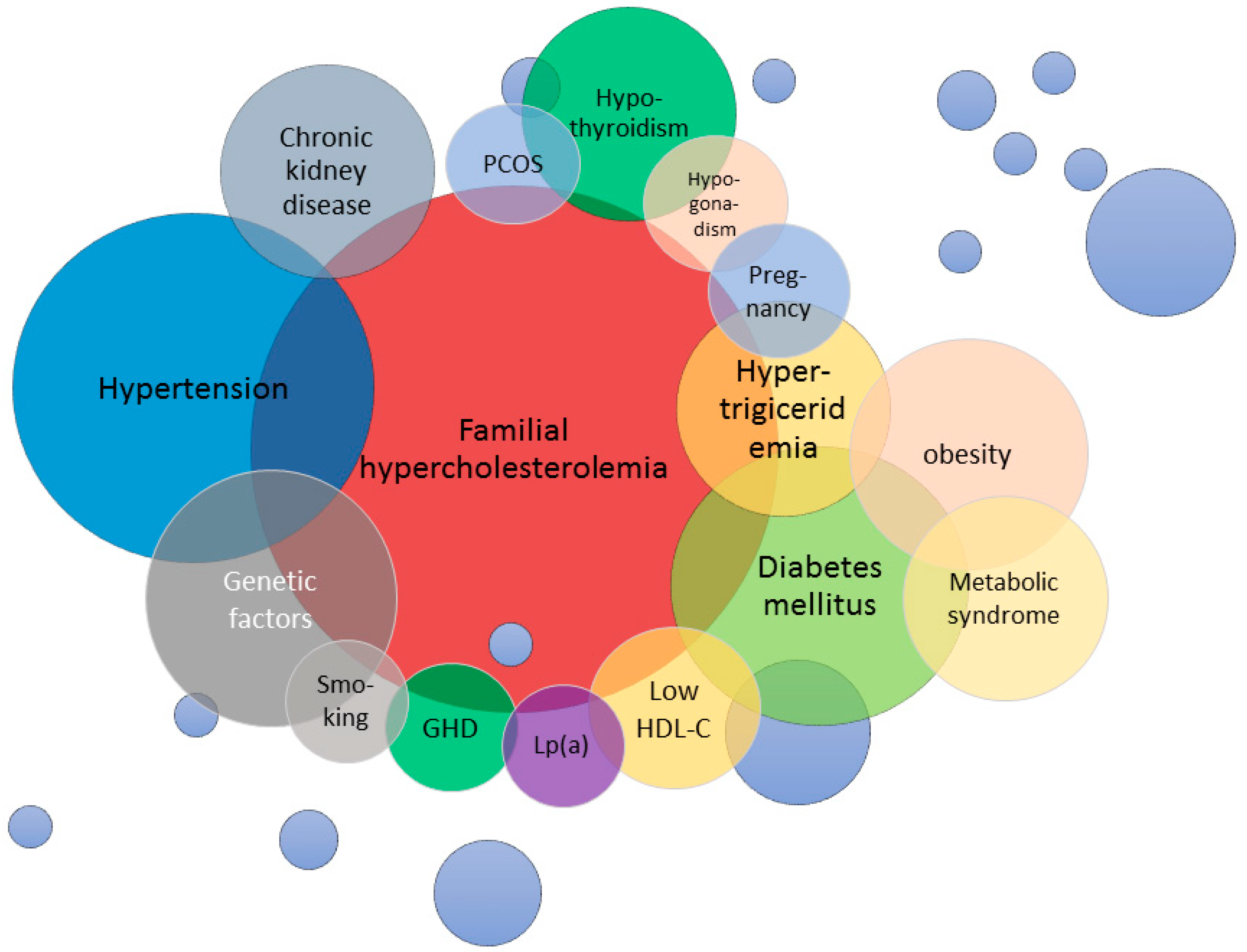
6. Concomitant Diseases
7. Coexisting Dyslipidemias with FH
7.1. Role of High-Density Cholesterol Levels
7.2. Lipoprotein (a)
7.3. The Role of Hypertriglyceridemias
8. Hypertension
9. Smoking
10. Endocrine Disorders
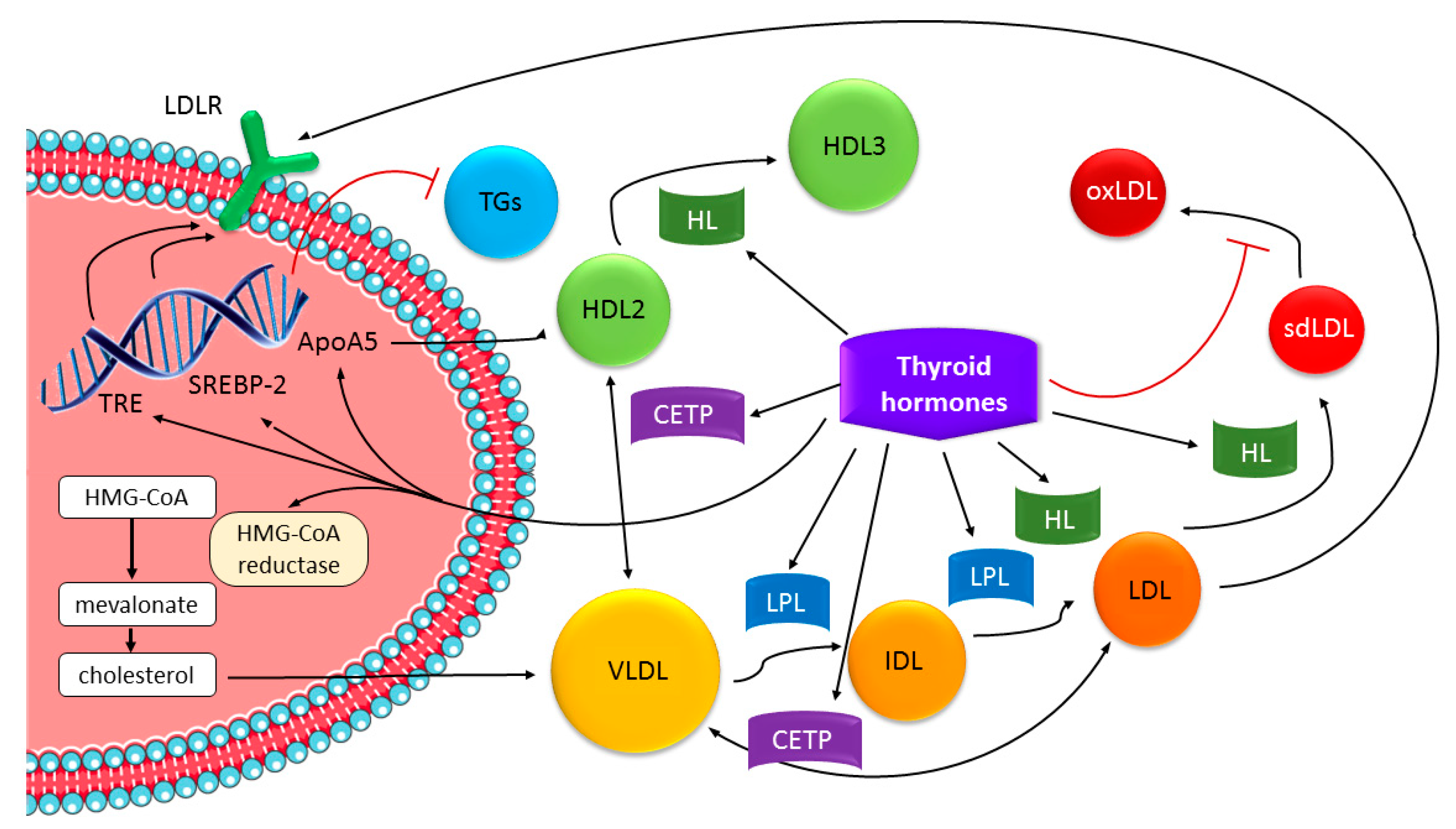
10.1. The Correlation between Thyroid Hormones and Lipid Homeostasis
10.2. Hypothyroidism
10.3. Diabetes Mellitus and Familial Hypercholesterolemia
10.4. Diabetic Dyslipidemia
10.5. Prevalence and Clinical Relevance of Diabetes in Familial Dyslipidemia
10.6. The Role of Obesity in FH Treatment
10.7. The Effect of Growth Hormone and Its Deficiency on Hypercholesterolemia
10.8. The Impact of Hypercholesterolemia on the Reproductive Hormones
10.9. The Association between Serum Testosterone and Lipids
10.10. Dyslipidemia in Polycystic Ovary Syndrome
10.11. Pregnancy in FH
11. Possibilities of Risk Stratification in Familial Hypercholesterolemia
Imaging
12. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Paragh, G.; Harangi, M.; Karányi, Z.; Daróczy, B.; Németh, Á.; Fülöp, P. Identifying patients with familial hypercholesterolemia using data mining methods in the Northern Great Plain region of Hungary. Atherosclerosis 2018, 277, 262–266. [Google Scholar] [CrossRef] [PubMed]
- Neefjes, L.A.; Ten Kate, G.J.; Alexia, R.; Nieman, K.; Galema-Boers, A.J.; Langendonk, J.G.; Weustink, A.C.; Mollet, N.R.; Sijbrands, E.J.; Krestin, G.P.; et al. Accelerated subclinical coronary atherosclerosis in patients with familial hypercholesterolemia. Atherosclerosis 2011, 219, 721–727. [Google Scholar] [CrossRef]
- Sijbrands, E.J.; Westendorp, R.G.; Defesche, J.C.; de Meier, P.H.; Smelt, A.H.; Kastelein, J.J. Mortality over two centuries in large pedigree with familial hypercholesterolaemia: Family tree mortality study. BMJ 2001, 322, 1019–1023. [Google Scholar] [CrossRef]
- Alonso, R.; Mata, N.; Castillo, S.; Fuentes, F.; Saenz, P.; Muñiz, O.; Galiana, J.; Figueras, R.; Diaz, J.L.; Gomez-Enterría, P.; et al. Cardiovascular disease in familial hypercholesterolaemia: Influence of low-density lipoprotein receptor mutation type and classic risk factors. Atherosclerosis 2008, 200, 315–321. [Google Scholar] [CrossRef] [PubMed]
- Marais, A.D. Familial hypercholesterolaemia. Clin. Biochem. Rev. 2004, 25, 49–68. [Google Scholar]
- Madar, L.; Juhász, L.; Szűcs, Z.; Kerkovits, L.; Harangi, M.; Balogh, I. Establishing the Mutational Spectrum of Hungarian Patients with Familial Hypercholesterolemia. Genes 2022, 13, 153. [Google Scholar] [CrossRef] [PubMed]
- Sturm, A.C.; Knowles, J.W.; Gidding, S.S.; Ahmad, Z.S.; Ahmed, C.D.; Ballantyne, C.M.; Baum, S.J.; Bourbon, M.; Carrié, A.; Cuchel, M.; et al. Clinical Genetic Testing for Familial Hypercholesterolemia: JACC Scientific Expert Panel. J. Am. Coll. Cardiol. 2018, 72, 662–680. [Google Scholar] [CrossRef]
- Vrablik, M.; Tichý, L.; Freiberger, T.; Blaha, V.; Satny, M.; Hubacek, J.A. Genetics of Familial Hypercholesterolemia: New Insights. Front. Genet. 2020, 11, 574474. [Google Scholar] [CrossRef]
- Di Taranto, M.D.; Giacobbe, C.; Fortunato, G. Familial hypercholesterolemia: A complex genetic disease with variable phenotypes. Eur. J. Med. Genet. 2020, 63, 103831. [Google Scholar] [CrossRef]
- Guay, S.P.; Brisson, D.; Lamarche, B.; Gaudet, D.; Bouchard, L. Epipolymorphisms within lipoprotein genes contribute independently to plasma lipid levels in familial hypercholesterolemia. Epigenetics 2014, 9, 718–729. [Google Scholar] [CrossRef]
- Vaseghi, G.; Javanmard, S.H.; Heshmat-Ghahdarijani, K.; Sarrafzadegan, N.; Amerizadeh, A. Comorbidities with Familial Hypercholesterolemia (FH): A Systematic Review. Curr. Probl. Cardiol. 2022, 101109. [Google Scholar] [CrossRef] [PubMed]
- Kinosian, B.; Glick, H.; Garland, G. Cholesterol and coronary heart disease: Predicting risks by levels and ratios. Ann. Intern. Med. 1994, 121, 641–647. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.D.; Chen, W.J.; Chien, K.L.; Seh-Yi Su, S.S.; Hsu, H.C.; Chen, M.F.; Liau, C.S.; Lee, Y.T. Efficacy of cholesterol levels and ratios in predicting future coronary heart disease in a Chinese population. Am. J. Cardiol. 2001, 88, 737–743. [Google Scholar] [CrossRef]
- Jansen, A.C.; van Aalst-Cohen, E.S.; Tanck, M.W.; Trip, M.D.; Lansberg, P.J.; Liem, A.H.; van Lennep, H.W.; Sijbrands, E.J.; Kastelein, J.J. The contribution of classical risk factors to cardiovascular disease in familial hypercholesterolaemia: Data in 2400 patients. J. Intern. Med. 2004, 256, 482–490. [Google Scholar] [CrossRef]
- Van Aalst-Cohen, E.S.; Jansen, A.C.; Boekholdt, S.M.; Tanck, M.W.; Fontecha, M.R.; Cheng, S.; Li, J.; Defesche, J.C.; Kuivenhoven, J.A.; Kastelein, J.J. Genetic determinants of plasma HDL-cholesterol levels in familial hypercholesterolemia. Eur. J. Hum. Genet. 2005, 13, 1137–1142. [Google Scholar] [CrossRef] [PubMed]
- Real, J.T.; Chaves, F.J.; Martínez-Usó, I.; García-García, A.B.; Ascaso, J.F.; Carmena, R. Importance of HDL cholesterol levels and the total/HDL cholesterol ratio as a risk factor for coronary heart disease in molecularly defined heterozygous familial hypercholesterolaemia. Eur. Heart J. 2001, 22, 465–471. [Google Scholar] [CrossRef]
- Ganjali, S.; Momtazi, A.A.; Banach, M.; Kovanen, P.T.; Stein, E.A.; Sahebkar, A. HDL abnormalities in familial hypercholesterolemia: Focus on biological functions. Prog. Lipid Res. 2017, 67, 16–26. [Google Scholar] [CrossRef]
- Pedro-Botet, J.; Climent, E.; Benaiges, D. Familial Hypercholesterolemia: Do HDL Play a Role? Biomedicines 2021, 9, 810. [Google Scholar] [CrossRef]
- Nordestgaard, B.G.; Chapman, M.J.; Ray, K.; Borén, J.; Andreotti, F.; Watts, G.F.; Ginsberg, H.; Amarenco, P.; Catapano, A.; Descamps, O.S.; et al. Lipoprotein(a) as a cardiovascular risk factor: Current status. Eur. Heart J. 2010, 31, 2844–2853. [Google Scholar] [CrossRef]
- Mach, F.; Baigent, C.; Catapano, A.L.; Koskinas, K.C.; Casula, M.; Badimon, L.; Chapman, M.J.; De Backer, G.G.; Delgado, V.; Ference, B.A.; et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. Eur. Heart J. 2019, 41, 111–188. [Google Scholar] [CrossRef]
- Watanabe, J.; Hamasaki, M.; Kotani, K. Risk of cardiovascular disease with lipoprotein(a) in familial hypercholesterolemia: A review. Arch. Med. Sci. Atheroscler. Dis. 2020, 5, e148–e152. [Google Scholar] [CrossRef] [PubMed]
- Friedlander, Y.; Leitersdorf, E. Segregation analysis of plasma lipoprotein(a) levels in pedigrees with molecularly defined familial hypercholesterolemia. Genet. Epidemiol. 1995, 12, 129–143. [Google Scholar] [CrossRef] [PubMed]
- Kraft, H.G.; Lingenhel, A.; Raal, F.J.; Hohenegger, M.; Utermann, G. Lipoprotein(a) in homozygous familial hypercholesterolemia. Arterioscler. Thromb. Vasc. Biol. 2000, 20, 522–528. [Google Scholar] [CrossRef]
- Németh, Á.; Daróczy, B.; Juhász, L.; Fülöp, P.; Harangi, M.; Paragh, G. Assessment of Associations Between Serum Lipoprotein (a) Levels and Atherosclerotic Vascular Diseases in Hungarian Patients with Familial Hypercholesterolemia Using Data Mining and Machine Learning. Front. Genet. 2022, 13, 849197. [Google Scholar] [CrossRef]
- Soutar, A.K.; McCarthy, S.N.; Seed, M.; Knight, B.L. Relationship between apolipoprotein(a) phenotype, lipoprotein(a) concentration in plasma, and low density lipoprotein receptor function in a large kindred with familial hypercholesterolemia due to the pro664----leu mutation in the LDL receptor gene. J. Clin. Investig. 1991, 88, 483–492. [Google Scholar] [CrossRef]
- Defesche, J.C.; van de Ree, M.A.; Kastelein, J.J.; van Diermen, D.E.; Janssens, N.W.; van Doormaal, J.J.; Hayden, M.R. Detection of the Pro664-Leu mutation in the low-density lipoprotein receptor and its relation to lipoprotein(a) levels in patients with familial hypercholesterolemia of Dutch ancestry from The Netherlands and Canada. Clin. Genet. 1992, 42, 273–280. [Google Scholar] [CrossRef] [PubMed]
- McCormick, S.P.A.; Schneider, W.J. Lipoprotein(a) catabolism: A case of multiple receptors. Pathology 2019, 51, 155–164. [Google Scholar] [CrossRef]
- Greco, M.F.; Sirtori, C.R.; Corsini, A.; Ezhov, M.; Sampietro, T.; Ruscica, M. Lipoprotein(a) Lowering-From Lipoprotein Apheresis to Antisense Oligonucleotide Approach. J. Clin. Med. 2020, 9, 2103. [Google Scholar] [CrossRef]
- Kayikcioglu, M.; Tokgozoglu, L.; Dogan, V.; Ceyhan, C.; Tuncez, A.; Kutlu, M.; Onrat, E.; Alici, G.; Akbulut, M.; Celik, A.; et al. What have we learned from Turkish familial hypercholesterolemia registries (A-HIT1 and A-HIT2)? Atherosclerosis 2018, 277, 341–346. [Google Scholar] [CrossRef]
- Waldmann, E.; Parhofer, K.G. Lipoprotein apheresis to treat elevated lipoprotein (a). J. Lipid Res. 2016, 57, 1751–1757. [Google Scholar] [CrossRef]
- Viney, N.J.; van Capelleveen, J.C.; Geary, R.S.; Xia, S.; Tami, J.A.; Yu, R.Z.; Marcovina, S.M.; Hughes, S.G.; Graham, M.J.; Crooke, R.M.; et al. Antisense oligonucleotides targeting apolipoprotein(a) in people with raised lipoprotein(a): Two randomised, double-blind, placebo-controlled, dose-ranging trials. Lancet 2016, 388, 2239–2253. [Google Scholar] [CrossRef]
- Nordestgaard, B.G. Triglyceride-Rich Lipoproteins and Atherosclerotic Cardiovascular Disease: New Insights from Epidemiology, Genetics, and Biology. Circ. Res. 2016, 118, 547–563. [Google Scholar] [CrossRef] [PubMed]
- Toth, P.P. Triglyceride-rich lipoproteins as a causal factor for cardiovascular disease. Vasc. Health Risk Manag. 2016, 12, 171–183. [Google Scholar] [CrossRef] [PubMed]
- Degrace, P.; Moindrot, B.; Mohamed, I.; Gresti, J.; Du, Z.Y.; Chardigny, J.M.; Sébédio, J.L.; Clouet, P. Upregulation of liver VLDL receptor and FAT/CD36 expression in LDLR-/- apoB100/100 mice fed trans-10, cis-12 conjugated linoleic acid. J. Lipid Res. 2006, 47, 2647–2655. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, A.J.; Lamarche, B.; Ruel, I.L.; Hogue, J.C.; Bergeron, J.; Gagné, C.; Couture, P. Increased production of VLDL apoB-100 in subjects with familial hypercholesterolemia carrying the same null LDL receptor gene mutation. J. Lipid Res. 2004, 45, 866–872. [Google Scholar] [CrossRef]
- Cabezas, M.C.; de Bruin, T.W.; Westerveld, H.E.; Meijer, E.; Erkelens, D.W. Delayed chylomicron remnant clearance in subjects with heterozygous familial hypercholesterolaemia. J. Intern. Med. 1998, 244, 299–307. [Google Scholar] [CrossRef]
- Kolovou, G.D.; Anagnostopoulou, K.K.; Pilatis, N.D.; Iraklianou, S.; Hoursalas, I.S.; Liberi, S.; Pavlidis, A.N.; Dritsas, A.; Mikhailidis, D.P.; Cokkinos, D.V. Heterozygote men with familial hypercholesterolaemia may have an abnormal triglyceride response post-prandially. Evidence for another predictor of vascular risk in familial hypercholesterolaemia. Int. J. Clin. Pract. 2005, 59, 311–317. [Google Scholar] [CrossRef]
- Geisel, J.; Bunte, T.; Bodis, M.; Oette, K.; Herrmann, W. Apolipoprotein E2/E2 genotype in combination with mutations in the LDL receptor gene causes type III hyperlipoproteinemia. Clin. Chem. Lab. Med. 2002, 40, 475–479. [Google Scholar] [CrossRef]
- Rosenson, R.S.; Najera, S.D.; Hegele, R.A. Heterozygous familial hypercholesterolemia presenting as chylomicronemia syndrome. J. Clin. Lipidol. 2017, 11, 294–296. [Google Scholar] [CrossRef]
- Viñals, C.; Zambón, D.; Yago, G.; Domenech, M.; Ortega, E. Secondary hypertriglyceridemia. Clin. Investig. Arterioscler. 2021, 33 (Suppl. S2), 29–36. [Google Scholar] [CrossRef]
- Chan, D.C.; Pang, J.; Hooper, A.J.; Burnett, J.R.; Bell, D.A.; Bates, T.R.; van Bockxmeer, F.M.; Watts, G.F. Elevated lipoprotein(a), hypertension and renal insufficiency as predictors of coronary artery disease in patients with genetically confirmed heterozygous familial hypercholesterolemia. Int. J. Cardiol. 2015, 201, 633–638. [Google Scholar] [CrossRef] [PubMed]
- Dyrbuś, K.; Gąsior, M.; Desperak, P.; Osadnik, T.; Nowak, J.; Banach, M. The prevalence and management of familial hypercholesterolemia in patients with acute coronary syndrome in the Polish tertiary centre: Results from the TERCET registry with 19,781 individuals. Atherosclerosis 2019, 288, 33–41. [Google Scholar] [CrossRef] [PubMed]
- Korneva, V.; Kuznetsova, T.; Julius, U. Efficiency and problems of statin therapy in patients with heterozygous familial hypercholesterolemia. Atheroscler. Suppl. 2019, 40, 79–87. [Google Scholar] [CrossRef] [PubMed]
- Vlad, C.E.; Foia, L.; Florea, L.; Costache, I.I.; Covic, A.; Popescu, R.; Reurean-Pintilei, D. Evaluation of cardiovascular risk factors in patients with familial hypercholesterolemia from the North-Eastern area of Romania. Lipids Health Dis. 2021, 20, 4. [Google Scholar] [CrossRef] [PubMed]
- Oori, M.J.; Mohammadi, F.; Norozi, K.; Fallahi-Khoshknab, M.; Ebadi, A.; Gheshlagh, R.G. Prevalence of HTN in Iran: Meta-analysis of Published Studies in 2004–2018. Curr. Hypertens. Rev. 2019, 15, 113–122. [Google Scholar] [CrossRef] [PubMed]
- Bertolini, S.; Pisciotta, L.; Rabacchi, C.; Cefalù, A.B.; Noto, D.; Fasano, T.; Signori, A.; Fresa, R.; Averna, M.; Calandra, S. Spectrum of mutations and phenotypic expression in patients with autosomal dominant hypercholesterolemia identified in Italy. Atherosclerosis 2013, 227, 342–348. [Google Scholar] [CrossRef]
- Mehta, R.; Martagon, A.J.; Galan Ramirez, G.A.; Antonio-Villa, N.E.; Vargas-Vázquez, A.; Elias-Lopez, D.; Gonzalez-Retana, G.; Rodríguez-Encinas, B.; Ceballos-Macías, J.J.; Romero-Zazueta, A.; et al. Familial hypercholesterolemia in Mexico: Initial insights from the national registry. J. Clin. Lipidol. 2021, 15, 124–133. [Google Scholar] [CrossRef]
- Besseling, J.; Kindt, I.; Hof, M.; Kastelein, J.J.; Hutten, B.A.; Hovingh, G.K. Severe heterozygous familial hypercholesterolemia and risk for cardiovascular disease: A study of a cohort of 14,000 mutation carriers. Atherosclerosis 2014, 233, 219–223. [Google Scholar] [CrossRef]
- Wierzbicki, A.S.; Lambert-Hammill, M.; Lumb, P.J.; Crook, M.A. Renin-angiotensin system polymorphisms and coronary events in familial hypercholesterolemia. Hypertension 2000, 36, 808–812. [Google Scholar] [CrossRef][Green Version]
- Polfus, L.M.; Smith, J.A.; Shimmin, L.C.; Bielak, L.F.; Morrison, A.C.; Kardia, S.L.; Peyser, P.A.; Hixson, J.E. Genome-wide association study of gene by smoking interactions in coronary artery calcification. PLoS ONE 2013, 8, e74642. [Google Scholar] [CrossRef]
- Bentley, A.R.; Sung, Y.J.; Brown, M.R.; Winkler, T.W.; Kraja, A.T.; Ntalla, I.; Schwander, K.; Chasman, D.I.; Lim, E.; Deng, X.; et al. Multi-ancestry genome-wide gene-smoking interaction study of 387,272 individuals identifies new loci associated with serum lipids. Nat. Genet. 2019, 51, 636–648. [Google Scholar] [CrossRef] [PubMed]
- Roy, N.; Gaudet, D.; Tremblay, G.; Brisson, D. Association of common gene-smoking interactions with elevated plasma apolipoprotein B concentration. Lipids Health Dis. 2020, 19, 98. [Google Scholar] [CrossRef] [PubMed]
- Mytilinaiou, M.; Kyrou, I.; Khan, M.; Grammatopoulos, D.K.; Randeva, H.S. Familial Hypercholesterolemia: New Horizons for Diagnosis and Effective Management. Front. Pharmacol. 2018, 9, 707. [Google Scholar] [CrossRef] [PubMed]
- Duntas, L.H.; Brenta, G. A Renewed Focus on the Association Between Thyroid Hormones and Lipid Metabolism. Front. Endocrinol. 2018, 9, 511. [Google Scholar] [CrossRef]
- Duntas, L.H. Thyroid disease and lipids. Thyroid 2002, 12, 287–293. [Google Scholar] [CrossRef] [PubMed]
- Biondi, B.; Kahaly, G.J.; Robertson, R.P. Thyroid Dysfunction and Diabetes Mellitus: Two Closely Associated Disorders. Endocr. Rev. 2019, 40, 789–824. [Google Scholar] [CrossRef]
- Rizos, C.V.; Elisaf, M.S.; Liberopoulos, E.N. Effects of thyroid dysfunction on lipid profile. Open Cardiovasc. Med. J. 2011, 5, 76–84. [Google Scholar] [CrossRef]
- Damiano, F.; Rochira, A.; Gnoni, A.; Siculella, L. Action of Thyroid Hormones, T3 and T2, on Hepatic Fatty Acids: Differences in Metabolic Effects and Molecular Mechanisms. Int. J. Mol. Sci. 2017, 18, 744. [Google Scholar] [CrossRef]
- Lithell, H.; Boberg, J.; Hellsing, K.; Ljunghall, S.; Lundqvist, G.; Vessby, B.; Wide, L. Serum lipoprotein and apolipoprotein concentrations and tissue lipoprotein-lipase activity in overt and subclinical hypothyroidism: The effect of substitution therapy. Eur. J. Clin. Investig. 1981, 11, 3–10. [Google Scholar] [CrossRef]
- Duntas, L.H.; Brenta, G. Thyroid hormones: A potential ally to LDL-cholesterol-lowering agents. Hormones 2016, 15, 500–510. [Google Scholar] [CrossRef]
- Canaris, G.J.; Manowitz, N.R.; Mayor, G.; Ridgway, E.C. The Colorado thyroid disease prevalence study. Arch. Intern. Med. 2000, 160, 526–534. [Google Scholar] [CrossRef] [PubMed]
- Wiseman, S.A.; Powell, J.T.; Humphries, S.E.; Press, M. The magnitude of the hypercholesterolemia of hypothyroidism is associated with variation in the low density lipoprotein receptor gene. J. Clin. Endocrinol. Metab. 1993, 77, 108–112. [Google Scholar] [CrossRef] [PubMed]
- Erdogan, M.; Canataroglu, A.; Ganidagli, S.; Kulaksızoglu, M. Metabolic syndrome prevalence in subclinic and overt hypothyroid patients and the relation among metabolic syndrome parameters. J. Endocrinol. Investig. 2011, 34, 488–492. [Google Scholar] [CrossRef]
- Cappola, A.R.; Ladenson, P.W. Hypothyroidism and atherosclerosis. J. Clin. Endocrinol. Metab. 2003, 88, 2438–2444. [Google Scholar] [CrossRef]
- Prisant, L.M.; Gujral, J.S.; Mulloy, A.L. Hyperthyroidism: A secondary cause of isolated systolic hypertension. J. Clin. Hypertens. 2006, 8, 596–599. [Google Scholar] [CrossRef] [PubMed]
- Berta, E.; Lengyel, I.; Halmi, S.; Zrínyi, M.; Erdei, A.; Harangi, M.; Páll, D.; Nagy, E.V.; Bodor, M. Hypertension in Thyroid Disorders. Front. Endocrinol. 2019, 10, 482. [Google Scholar] [CrossRef]
- Palmieri, E.A.; Fazio, S.; Lombardi, G.; Biondi, B. Subclinical hypothyroidism and cardiovascular risk: A reason to treat? Treat. Endocrinol. 2004, 3, 233–244. [Google Scholar] [CrossRef]
- Vargas, F.; Moreno, J.M.; Rodríguez-Gómez, I.; Wangensteen, R.; Osuna, A.; Alvarez-Guerra, M.; García-Estañ, J. Vascular and renal function in experimental thyroid disorders. Eur. J. Endocrinol. 2006, 154, 197–212. [Google Scholar] [CrossRef]
- Pykälistö, O.; Goldberg, A.P.; Brunzell, J.D. Reversal of decreased human adipose tissue lipoprotein lipase and hypertriglyceridemia after treatment of hypothyroidism. J. Clin. Endocrinol. Metab. 1976, 43, 591–600. [Google Scholar] [CrossRef]
- Paquette, M.; Bernard, S.; Ruel, I.; Blank, D.W.; Genest, J.; Baass, A. Diabetes is associated with an increased risk of cardiovascular disease in patients with familial hypercholesterolemia. J. Clin. Lipidol. 2019, 13, 123–128. [Google Scholar] [CrossRef]
- Dal Canto, E.; Ceriello, A.; Rydén, L.; Ferrini, M.; Hansen, T.B.; Schnell, O.; Standl, E.; Beulens, J.W. Diabetes as a cardiovascular risk factor: An overview of global trends of macro and micro vascular complications. Eur. J. Prev. Cardiol. 2019, 26, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Damaskos, C.; Garmpis, N.; Kollia, P.; Mitsiopoulos, G.; Barlampa, D.; Drosos, A.; Patsouras, A.; Gravvanis, N.; Antoniou, V.; Litos, A.; et al. Assessing Cardiovascular Risk in Patients with Diabetes: An Update. Curr. Cardiol. Rev. 2020, 16, 266–274. [Google Scholar] [CrossRef] [PubMed]
- Sarwar, N.; Gao, P.; Seshasai, S.R.; Gobin, R.; Kaptoge, S.; Di Angelantonio, E.; Ingelsson, E.; Lawlor, D.A.; Selvin, E.; Stampfer, M.; et al. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: A collaborative meta-analysis of 102 prospective studies. Lancet 2010, 375, 2215–2222. [Google Scholar] [CrossRef] [PubMed]
- Nikkilä, E.A.; Kekki, M. Plasma triglyceride transport kinetics in diabetes mellitus. Metabolism 1973, 22, 1–22. [Google Scholar] [CrossRef]
- Warraich, H.J.; Wong, N.D.; Rana, J.S. Role for combination therapy in diabetic dyslipidemia. Curr. Cardiol. Rep. 2015, 17, 32. [Google Scholar] [CrossRef] [PubMed]
- McEneny, J.; O’Kane, M.J.; Moles, K.W.; McMaster, C.; McMaster, D.; Mercer, C.; Trimble, E.R.; Young, I.S. Very low density lipoprotein subfractions in Type II diabetes mellitus: Alterations in composition and susceptibility to oxidation. Diabetologia 2000, 43, 485–493. [Google Scholar] [CrossRef]
- Malmström, R.; Packard, C.J.; Caslake, M.; Bedford, D.; Stewart, P.; Yki-Järvinen, H.; Shepherd, J.; Taskinen, M.R. Defective regulation of triglyceride metabolism by insulin in the liver in NIDDM. Diabetologia 1997, 40, 454–462. [Google Scholar] [CrossRef]
- Cummings, M.H.; Watts, G.F.; Umpleby, A.M.; Hennessy, T.R.; Kelly, J.M.; Jackson, N.C.; Sönksen, P.H. Acute hyperinsulinemia decreases the hepatic secretion of very-low-density lipoprotein apolipoprotein B-100 in NIDDM. Diabetes 1995, 44, 1059–1065. [Google Scholar] [CrossRef]
- Chen, Y.D.; Swami, S.; Skowronski, R.; Coulston, A.; Reaven, G.M. Differences in postprandial lipemia between patients with normal glucose tolerance and noninsulin-dependent diabetes mellitus. J. Clin. Endocrinol. Metab. 1993, 76, 172–177. [Google Scholar] [CrossRef]
- Schofield, J.D.; Liu, Y.; Rao-Balakrishna, P.; Malik, R.A.; Soran, H. Diabetes Dyslipidemia. Diabetes Ther. 2016, 7, 203–219. [Google Scholar] [CrossRef]
- Hermans, M.P.; Amoussou-Guenou, K.D.; Bouenizabila, E.; Sadikot, S.S.; Ahn, S.A.; Rousseau, M.F. Size, density and cholesterol load of HDL predict microangiopathy, coronary artery disease and β-cell function in men with T2DM. Diabetes Metab. Syndr. 2017, 11, 125–131. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.T.; Liu, Y.; Lu, L.; Liu, H.J.; Shen, W.F.; Yang, K.; Zhang, R.Y. Diabetes-Invoked High-Density Lipoprotein and Its Association with Coronary Artery Disease in Patients with Type 2 Diabetes Mellitus. Am. J. Cardiol. 2016, 118, 1674–1679. [Google Scholar] [CrossRef] [PubMed]
- Russo, G.T.; De Cosmo, S.; Viazzi, F.; Pacilli, A.; Ceriello, A.; Genovese, S.; Guida, P.; Giorda, C.; Cucinotta, D.; Pontremoli, R.; et al. Plasma Triglycerides and HDL-C Levels Predict the Development of Diabetic Kidney Disease in Subjects with Type 2 Diabetes: The AMD Annals Initiative. Diabetes Care 2016, 39, 2278–2287. [Google Scholar] [CrossRef] [PubMed]
- Gomez Rosso, L.; Lhomme, M.; Meroño, T.; Dellepiane, A.; Sorroche, P.; Hedjazi, L.; Zakiev, E.; Sukhorukov, V.; Orekhov, A.; Gasparri, J.; et al. Poor glycemic control in type 2 diabetes enhances functional and compositional alterations of small, dense HDL3c. Biochim. Biophys. Acta Mol. Cell. Biol. Lipids 2017, 1862, 188–195. [Google Scholar] [CrossRef]
- Varga, T.V.; Winters, A.H.; Jablonski, K.A.; Horton, E.S.; Khare-Ranade, P.; Knowler, W.C.; Marcovina, S.M.; Renström, F.; Watson, K.E.; Goldberg, R.; et al. Comprehensive Analysis of Established Dyslipidemia-Associated Loci in the Diabetes Prevention Program. Circ. Cardiovasc. Genet. 2016, 9, 495–503. [Google Scholar] [CrossRef]
- Tomkin, G.H.; Owens, D. Diabetes and dyslipidemia: Characterizing lipoprotein metabolism. Diabetes Metab. Syndr. Obes. 2017, 10, 333–343. [Google Scholar] [CrossRef]
- Galvan, A.Q.; Santoro, D.; Natali, A.; Sampietro, T.; Boni, C.; Masoni, A.; Buzzigoli, G.; Ferrannini, E. Insulin sensitivity in familial hypercholesterolemia. Metabolism 1993, 42, 1359–1364. [Google Scholar] [CrossRef]
- Preiss, D.; Seshasai, S.R.; Welsh, P.; Murphy, S.A.; Ho, J.E.; Waters, D.D.; DeMicco, D.A.; Barter, P.; Cannon, C.P.; Sabatine, M.S.; et al. Risk of incident diabetes with intensive-dose compared with moderate-dose statin therapy: A meta-analysis. JAMA 2011, 305, 2556–2564. [Google Scholar] [CrossRef]
- Besseling, J.; Kastelein, J.J.; Defesche, J.C.; Hutten, B.A.; Hovingh, G.K. Association between familial hypercholesterolemia and prevalence of type 2 diabetes mellitus. JAMA 2015, 313, 1029–1036. [Google Scholar] [CrossRef]
- Climent, E.; Pérez-Calahorra, S.; Marco-Benedí, V.; Plana, N.; Sánchez, R.; Ros, E.; Ascaso, J.F.; Puzo, J.; Almagro, F.; Lahoz, C.; et al. Effect of LDL cholesterol, statins and presence of mutations on the prevalence of type 2 diabetes in heterozygous familial hypercholesterolemia. Sci. Rep. 2017, 7, 5596. [Google Scholar] [CrossRef]
- Skoumas, J.; Liontou, C.; Chrysohoou, C.; Masoura, C.; Aznaouridis, K.; Pitsavos, C.; Stefanadis, C. Statin therapy and risk of diabetes in patients with heterozygous familial hypercholesterolemia or familial combined hyperlipidemia. Atherosclerosis 2014, 237, 140–145. [Google Scholar] [CrossRef] [PubMed]
- Khera, A.V.; Won, H.H.; Peloso, G.M.; Lawson, K.S.; Bartz, T.M.; Deng, X.; van Leeuwen, E.M.; Natarajan, P.; Emdin, C.A.; Bick, A.G.; et al. Diagnostic Yield and Clinical Utility of Sequencing Familial Hypercholesterolemia Genes in Patients with Severe Hypercholesterolemia. J. Am. Coll. Cardiol. 2016, 67, 2578–2589. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Ryan, K.A.; Jaworek, T.J.; Southam, L.; Reid, J.G.; Overton, J.D.; Baras, A.; Puurunen, M.K.; Zeggini, E.; Taylor, S.I.; et al. Familial Hypercholesterolemia and Type 2 Diabetes in the Old Order Amish. Diabetes 2017, 66, 2054–2058. [Google Scholar] [CrossRef]
- Jermendy, G.; Kiss, Z.; Rokszin, G.; Abonyi-Tóth, Z.; Wittmann, I.; Kempler, P. Decreasing incidence of pharmacologically treated Type 2 diabetes in Hungary from 2001 to 2016: A nationwide cohort study. Diabetes Res. Clin. Pract. 2019, 155, 107788. [Google Scholar] [CrossRef]
- Vohnout, B.; Fábryová, Ľ.; Klabník, A.; Kadurová, M.; Bálinth, K.; Kozárová, M.; Bugáňová, I.; Sirotiaková, J.; Rašlová, K. Treatment pattern of familial hypercholesterolemia in Slovakia: Targets, treatment and obstacles in common practice. Atherosclerosis 2018, 277, 323–326. [Google Scholar] [CrossRef] [PubMed]
- Tankova, T.; Elenkova, A.; Robeva, R.; Dimova, R.; Borissova, A.M.; Olszewski, A.; Lachev, V.; Petkova, R. Familial Hypercholesterolaemia in a Bulgarian Population of Patients with Dyslipidaemia and Diabetes: An Observational Study. Diabetes Ther. 2020, 11, 453–465. [Google Scholar] [CrossRef] [PubMed]
- Moller, D.E.; Kaufman, K.D. Metabolic syndrome: A clinical and molecular perspective. Annu. Rev. Med. 2005, 56, 45–62. [Google Scholar] [CrossRef]
- Csige, I.; Ujvárosy, D.; Szabó, Z.; Lőrincz, I.; Paragh, G.; Harangi, M.; Somodi, S. The Impact of Obesity on the Cardiovascular System. J. Diabetes Res. 2018, 2018, 3407306. [Google Scholar] [CrossRef]
- Jung, U.J.; Choi, M.S. Obesity and its metabolic complications: The role of adipokines and the relationship between obesity, inflammation, insulin resistance, dyslipidemia and nonalcoholic fatty liver disease. Int. J. Mol. Sci. 2014, 15, 6184–6223. [Google Scholar] [CrossRef]
- Dönmez, Y.; Bulut, A. Epicardial fat thickness is significantly increased and related to LDL cholesterol level in patients with familial hypercholesterolemia. J. Ultrasound 2019, 22, 309–314. [Google Scholar] [CrossRef]
- Apovian, C.M. Obesity: Definition, comorbidities, causes, and burden. Am. J. Manag. Care 2016, 22, s176–s185. [Google Scholar] [PubMed]
- Baggio, L.L.; Drucker, D.J. Glucagon-like peptide-1 receptor co-agonists for treating metabolic disease. Mol. Metab. 2021, 46, 101090. [Google Scholar] [CrossRef]
- Mateo-Gallego, R.; Perez-Calahorra, S.; Cofán, M.; Baila-Rueda, L.; Cenarro, A.; Ros, E.; Puzo, J.; Civeira, F. Serum lipid responses to weight loss differ between overweight adults with familial hypercholesterolemia and those with familial combined hyperlipidemia. J. Nutr. 2014, 144, 1219–1226. [Google Scholar] [CrossRef] [PubMed]
- Isgaard, J.; Arcopinto, M.; Karason, K.; Cittadini, A. GH and the cardiovascular system: An update on a topic at heart. Endocrine 2015, 48, 25–35. [Google Scholar] [CrossRef] [PubMed]
- Metwalley, K.A.; Farghaly, H.S.; Abd El-Hafeez, H.A. Evaluation of left ventricular mass and function, lipid profile, and insulin resistance in Egyptian children with growth hormone deficiency: A single-center prospective case-control study. Indian J. Endocrinol. Metab. 2013, 17, 876–882. [Google Scholar] [CrossRef] [PubMed]
- Lanes, R.; Gunczler, P.; Lopez, E.; Esaa, S.; Villaroel, O.; Revel-Chion, R. Cardiac mass and function, carotid artery intima-media thickness, and lipoprotein levels in growth hormone-deficient adolescents. J. Clin. Endocrinol. Metab. 2001, 86, 1061–1065. [Google Scholar] [CrossRef]
- De Leonibus, C.; De Marco, S.; Stevens, A.; Clayton, P.; Chiarelli, F.; Mohn, A. Growth Hormone Deficiency in Prepubertal Children: Predictive Markers of Cardiovascular Disease. Horm. Res. Paediatr. 2016, 85, 363–371. [Google Scholar] [CrossRef]
- Lind, S.; Rudling, M.; Ericsson, S.; Olivecrona, H.; Eriksson, M.; Borgström, B.; Eggertsen, G.; Berglund, L.; Angelin, B. Growth hormone induces low-density lipoprotein clearance but not bile acid synthesis in humans. Arterioscler. Thromb. Vasc. Biol. 2004, 24, 349–356. [Google Scholar] [CrossRef]
- Yang, S.; Ke, X.; Liang, H.; Li, R.; Zhu, H. Case Report: A Clinical and Genetic Analysis of Childhood Growth Hormone Deficiency with Familial Hypercholesterolemia. Front. Endocrinol. 2021, 12, 691490. [Google Scholar] [CrossRef]
- Stanley, T. Diagnosis of growth hormone deficiency in childhood. Curr. Opin. Endocrinol. Diabetes Obes. 2012, 19, 47–52. [Google Scholar] [CrossRef]
- Braamskamp, M.J.; Kusters, D.M.; Wiegman, A.; Avis, H.J.; Wijburg, F.A.; Kastelein, J.J.; van Trotsenburg, A.S.; Hutten, B.A. Gonadal steroids, gonadotropins and DHEAS in young adults with familial hypercholesterolemia who had initiated statin therapy in childhood. Atherosclerosis 2015, 241, 427–432. [Google Scholar] [CrossRef] [PubMed]
- Smals, A.G.; Weusten, J.J.; Benraad, T.J.; Kloppenborg, P.W. The HMG-CoA reductase inhibitor simvastatin suppresses human testicular testosterone synthesis in vitro by a selective inhibitory effect on 17-ketosteroid-oxidoreductase enzyme activity. J. Steroid. Biochem. Mol. Biol. 1991, 38, 465–468. [Google Scholar] [CrossRef]
- Rezanezhad, B.; Borgquist, R.; Willenheimer, R.; Elzanaty, S. The Association between Serum Testosterone and Risk Factors for Atherosclerosis. Curr. Urol. 2019, 13, 101–106. [Google Scholar] [CrossRef] [PubMed]
- Tajar, A.; Huhtaniemi, I.T.; O’Neill, T.W.; Finn, J.D.; Pye, S.R.; Lee, D.M.; Bartfai, G.; Boonen, S.; Casanueva, F.F.; Forti, G.; et al. Characteristics of androgen deficiency in late-onset hypogonadism: Results from the European Male Aging Study (EMAS). J. Clin. Endocrinol. Metab. 2012, 97, 1508–1516. [Google Scholar] [CrossRef]
- Jones, T.H.; Arver, S.; Behre, H.M.; Buvat, J.; Meuleman, E.; Moncada, I.; Morales, A.M.; Volterrani, M.; Yellowlees, A.; Howell, J.D.; et al. Testosterone replacement in hypogonadal men with type 2 diabetes and/or metabolic syndrome (the TIMES2 study). Diabetes Care 2011, 34, 828–837. [Google Scholar] [CrossRef]
- Rastrelli, G.; Filippi, S.; Sforza, A.; Maggi, M.; Corona, G. Metabolic Syndrome in Male Hypogonadism. Front. Horm. Res. 2018, 49, 131–155. [Google Scholar] [CrossRef]
- Popovic, V.; Korbonits, M. Metabolic Syndrome Consequent to Endocrine Disorders; Karger: Basel, Switzerland, 2018; Volume 49. [Google Scholar]
- Saad, F. Androgen therapy in men with testosterone deficiency: Can testosterone reduce the risk of cardiovascular disease? Diabetes Metab. Res. Rev. 2012, 28 (Suppl. S2), 52–59. [Google Scholar] [CrossRef]
- Aversa, A.; Bruzziches, R.; Francomano, D.; Rosano, G.; Isidori, A.M.; Lenzi, A.; Spera, G. Effects of testosterone undecanoate on cardiovascular risk factors and atherosclerosis in middle-aged men with late-onset hypogonadism and metabolic syndrome: Results from a 24-month, randomized, double-blind, placebo-controlled study. J. Sex. Med. 2010, 7, 3495–3503. [Google Scholar] [CrossRef]
- Kalyani, R.R.; Dobs, A.S. Androgen deficiency, diabetes, and the metabolic syndrome in men. Curr. Opin. Endocrinol. Diabetes Obes. 2007, 14, 226–234. [Google Scholar] [CrossRef]
- Kim, J.J.; Choi, Y.M. Dyslipidemia in women with polycystic ovary syndrome. Obstet. Gynecol. Sci. 2013, 56, 137–142. [Google Scholar] [CrossRef] [PubMed]
- Luo, X.; Cai, W.Y.; Wu, X.K. Prevalence, Pattern and Predictors for Dyslipidemia of Chinese Women with Polycystic Ovary Syndrome. Front. Cardiovasc. Med. 2021, 8, 790454. [Google Scholar] [CrossRef] [PubMed]
- Liu, Q.; Xie, Y.J.; Qu, L.H.; Zhang, M.X.; Mo, Z.C. Dyslipidemia involvement in the development of polycystic ovary syndrome. Taiwan. J. Obstet. Gynecol. 2019, 58, 447–453. [Google Scholar] [CrossRef]
- Yilmaz, B.; Vellanki, P.; Ata, B.; Yildiz, B.O. Metabolic syndrome, hypertension, and hyperlipidemia in mothers, fathers, sisters, and brothers of women with polycystic ovary syndrome: A systematic review and meta-analysis. Fertil. Steril. 2018, 109, 356–364. [Google Scholar] [CrossRef]
- Toleikyte, I.; Retterstøl, K.; Leren, T.P.; Iversen, P.O. Pregnancy outcomes in familial hypercholesterolemia: A registry-based study. Circulation 2011, 124, 1606–1614. [Google Scholar] [CrossRef] [PubMed]
- Hyánek, J.; Pehal, F.; Dryahina, K.; Dubská, L.; Míková, B.; Gombíková, L.; Průcha, M.; Kubů, S.; Haláčková, P.; Feyreisl, J. Gestational hypercholesterolemia helps detect familial hypercholesterolemia and prevent late pregnancy complications. Clin. J. Obstet. Gynecol. 2019, 2, 079–089. [Google Scholar] [CrossRef]
- Edison, R.J.; Muenke, M. Central nervous system and limb anomalies in case reports of first-trimester statin exposure. N. Engl. J. Med. 2004, 350, 1579–1582. [Google Scholar] [CrossRef]
- Klevmoen, M.; Bogsrud, M.P.; Retterstøl, K.; Svilaas, T.; Vesterbekkmo, E.K.; Hovland, A.; Berge, C.; Roeters van Lennep, J.; Holven, K.B. Loss of statin treatment years during pregnancy and breastfeeding periods in women with familial hypercholesterolemia. Atherosclerosis 2021, 335, 8–15. [Google Scholar] [CrossRef]
- Wiegman, A.; de Groot, E.; Hutten, B.A.; Rodenburg, J.; Gort, J.; Bakker, H.D.; Sijbrands, E.J.; Kastelein, J.J. Arterial intima-media thickness in children heterozygous for familial hypercholesterolaemia. Lancet 2004, 363, 369–370. [Google Scholar] [CrossRef]
- Martinez, L.R.; Miname, M.H.; Bortolotto, L.A.; Chacra, A.P.; Rochitte, C.E.; Sposito, A.C.; Santos, R.D. No correlation and low agreement of imaging and inflammatory atherosclerosis’ markers in familial hypercholesterolemia. Atherosclerosis 2008, 200, 83–88. [Google Scholar] [CrossRef]
- Miname, M.H.; Bittencourt, M.S.; Moraes, S.R.; Alves, R.I.M.; Silva, P.R.S.; Jannes, C.E.; Pereira, A.C.; Krieger, J.E.; Nasir, K.; Santos, R.D. Coronary Artery Calcium and Cardiovascular Events in Patients with Familial Hypercholesterolemia Receiving Standard Lipid-Lowering Therapy. JACC Cardiovasc. Imaging 2019, 12, 1797–1804. [Google Scholar] [CrossRef]
- Okada, H.; Tada, H.; Hayashi, K.; Kawashima, H.; Takata, T.; Sakata, K.; Nohara, A.; Mabuchi, H.; Yamagishi, M.; Kawashiri, M.A. Aortic Root Calcification Score as an Independent Factor for Predicting Major Adverse Cardiac Events in Familial Hypercholesterolemia. J. Atheroscler. Thromb. 2018, 25, 634–642. [Google Scholar] [CrossRef] [PubMed]
| Condition | Clinical Presentation | Underlying Pathophysiology | Clinical Relevance |
|---|---|---|---|
| Hypothyroidism | Elevated triglycerides (TGs) and LDL intermediate-density lipoproteins, apoA and apoB | Increased cholesterol synthesis to degradation rate | After 4–6 weeks of thyroxin replacement therapy corrects dyslipidemia |
| Diabetic dyslipidemia | Elevated TGs Low HDL-C Small-dense LDL particles | Due to inflammation and increased availability of glucose and/or free fatty acids Increased production of TG-rich lipoproteins | Fundamental compound of elevated cardiovascular risk in diabetes Primary goal: treat to LDL-C to target |
| Diabetes | Decreased risk for diabetes (especially in patients with LDLR mutations) | Lower intracellular cholesterol levels have a protective effect | Statin therapy does not increase diabetes risk in FH patients Screen FH patients for diabetes with FPG and HgbA1C; weight control |
| Growth hormone deficiency | Elevated TGs and LDL Low HDL-C | GH decreases lipogenesis, stimulates lipolysis and LDL clearance through LDL-receptor stimulation | rhGH therapy in GHD reduces dyslipidemia and cardiovascular risk |
| Male hypogonadism | Elevated TGs and LDL Low HDL-C Oxidized LDL | Complex, poorly understood mechanism | Androgen treatment results in a favorable lipid profile |
| Polycystic ovarian syndrome | Elevated TGs and LDL Low HDL-C Small-dense LDL particles Elevated lipoprotein (a) Decreased ApoA1 Elevated ApoC1 | Abdominal obesity, increased lipolysis | Statins improve lipid abnormalities, insulin sensitivity, inflammation, oxidative stress and hyperandrogenism |
| Obesity | Elevated TGs Low HDL-C Small-dense LDL particles | Postprandial hyperlipidemia, inhibition of hormone sensitive lipase | Lifestyle modification, statins lower TG only marginally, combination with ezetimibe and fibrates to reduce hypertriglyceridemia |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Berta, E.; Zsíros, N.; Bodor, M.; Balogh, I.; Lőrincz, H.; Paragh, G.; Harangi, M. Clinical Aspects of Genetic and Non-Genetic Cardiovascular Risk Factors in Familial Hypercholesterolemia. Genes 2022, 13, 1158. https://doi.org/10.3390/genes13071158
Berta E, Zsíros N, Bodor M, Balogh I, Lőrincz H, Paragh G, Harangi M. Clinical Aspects of Genetic and Non-Genetic Cardiovascular Risk Factors in Familial Hypercholesterolemia. Genes. 2022; 13(7):1158. https://doi.org/10.3390/genes13071158
Chicago/Turabian StyleBerta, Eszter, Noémi Zsíros, Miklós Bodor, István Balogh, Hajnalka Lőrincz, György Paragh, and Mariann Harangi. 2022. "Clinical Aspects of Genetic and Non-Genetic Cardiovascular Risk Factors in Familial Hypercholesterolemia" Genes 13, no. 7: 1158. https://doi.org/10.3390/genes13071158
APA StyleBerta, E., Zsíros, N., Bodor, M., Balogh, I., Lőrincz, H., Paragh, G., & Harangi, M. (2022). Clinical Aspects of Genetic and Non-Genetic Cardiovascular Risk Factors in Familial Hypercholesterolemia. Genes, 13(7), 1158. https://doi.org/10.3390/genes13071158








