Fragile X-Associated Neuropsychiatric Disorders (FXAND) in Young Fragile X Premutation Carriers
Abstract
1. Background
2. Methods
2.1. Subjects
2.2. Study Measures
2.2.1. Clinical Phenotype-Related Measures
2.2.2. Molecular Data
2.2.3. Statistical Analysis
3. Results
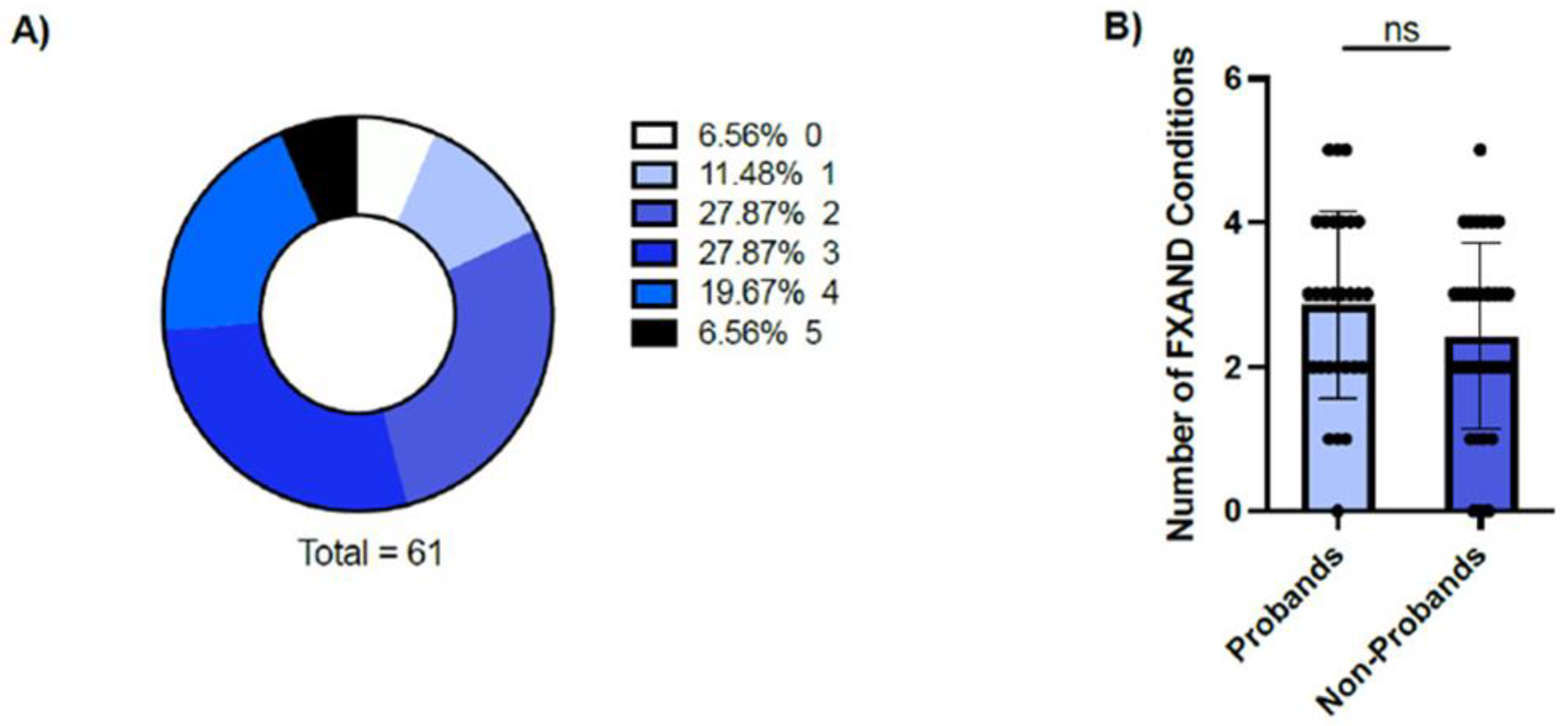
4. FXAND-Related Conditions
4.1. Factors Associated with Clinical Phenotype Features
4.2. Psychotropic Medication Intake
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| PM | Premutation carrier state |
| PM—FXPOI | fragile X-associated primary ovarian insufficiency |
| FXTAS | fragile X-associated tremor ataxia |
| FXAND | fragile X-associated neurodevelopmental disorders |
| ASD | autism spectrum disorder |
| ADHD | attention-deficit hyperactivity disorder |
References
- Hagerman, R.J.; Berry-Kravis, E.; Hazlett, H.C.; Bailey, D.B., Jr.; Moine, H.; Kooy, R.F.; Tassone, F.; Gantois, I.; Sonenberg, N.; Mandel, J.L.; et al. Fragile X syndrome. Nat. Rev. Dis. Prim. 2017, 3, 17065. [Google Scholar] [CrossRef] [PubMed]
- Tassone, F.; Iong, K.P.; Tong, T.H.; Lo, J.; Gane, L.W.; Berry-Kravis, E.; Nguyen, D.; Mu, L.Y.; Laffin, J.; Bailey, D.B.; et al. FMR1 CGG allele size and prevalence ascertained through newborn screening in the United States. Genome Med. 2012, 4, 100. [Google Scholar] [CrossRef] [PubMed]
- Saldarriaga, W.; Tassone, F.; Gonzalez-Teshima, L.Y.; Forero-Forero, J.V.; Ayala-Zapata, S.; Hagerman, R. Fragile X syndrome. Colomb. Med. 2014, 45, 190–198. [Google Scholar] [CrossRef]
- Bagni, C.; Tassone, F.; Neri, G.; Hagerman, R. Fragile X syndrome: Causes, diagnosis, mechanisms, and therapeutics. J. Clin. Investig. 2012, 122, 4314–4322. [Google Scholar] [CrossRef]
- Hagerman, R.J.H.; Paul, J. Fragile X Syndrome and Premutation Disorders; Mac Keith Press: London, UK, 2020. [Google Scholar]
- Cronister, A.; Schreiner, R.; Wittenberger, M.; Amiri, K.; Harris, K.; Hagerman, R.J. Heterozygous fragile X female: Historical, physical, cognitive, and cytogenetic features. Am. J. Med. Genet. 1991, 38, 269–274. [Google Scholar] [CrossRef]
- Sullivan, A.K.; Marcus, M.; Epstein, M.P.; Allen, E.G.; Anido, A.E.; Paquin, J.J.; Yadav-Shah, M.; Sherman, S.L. Association of FMR1 repeat size with ovarian dysfunction. Hum. Reprod. 2005, 20, 402–412. [Google Scholar] [CrossRef]
- Hagerman, R.J.; Leehey, M.; Heinrichs, W.; Tassone, F.; Wilson, R.; Hills, J.; Grigsby, J.; Gage, B.; Hagerman, P.J. Intention tremor, parkinsonism, and generalized brain atrophy in male carriers of fragile X. Neurology 2001, 57, 127–130. [Google Scholar] [CrossRef]
- Jacquemont, S.; Hagerman, R.J.; Leehey, M.; Grigsby, J.; Zhang, L.; Brunberg, J.A.; Greco, C.; Des Portes, V.; Jardini, T.; Levine, R.; et al. Fragile X premutation tremor/ataxia syndrome: Molecular, clinical, and neuroimaging correlates. Am. J. Hum. Genet. 2003, 72, 869–878. [Google Scholar] [CrossRef]
- Jacquemont, S.; Hagerman, R.J.; Leehey, M.A.; Hall, D.A.; Levine, R.A.; Brunberg, J.A.; Zhang, L.; Jardini, T.; Gane, L.W.; Harris, S.W.; et al. Penetrance of the fragile X-associated tremor/ataxia syndrome in a premutation carrier population. JAMA 2004, 291, 460–469. [Google Scholar] [CrossRef]
- Hagerman, R.J.; Hagerman, P. Fragile X-associated tremor/ataxia syndrome—Features, mechanisms and management. Nat. Rev. Neurol. 2016, 12, 403–412. [Google Scholar] [CrossRef]
- Tassone, F.; Hagerman, R.J.; Taylor, A.K.; Gane, L.W.; Godfrey, T.E.; Hagerman, P.J. Elevated levels of FMR1 mRNA in carrier males: A new mechanism of involvement in the fragile-X syndrome. Am. J. Hum. Genet. 2000, 66, 6–15. [Google Scholar] [CrossRef] [PubMed]
- Hagerman, R.J.; Protic, D.; Rajaratnam, A.; Salcedo-Arellano, M.J.; Aydin, E.Y.; Schneider, A. Fragile X-Associated Neuropsychiatric Disorders (FXAND). Front. Psychiatry 2018, 9, 564. [Google Scholar] [CrossRef] [PubMed]
- Roberts, J.E.; Bailey, D.B., Jr.; Mankowski, J.; Ford, A.; Sideris, J.; Weisenfeld, L.A.; Heath, T.M.; Golden, R.N. Mood and anxiety disorders in females with the FMR1 premutation. Am. J. Med. Genet. B Neuropsychiatr. Genet. 2009, 150, 130–139. [Google Scholar] [CrossRef] [PubMed]
- Roberts, J.E.; Tonnsen, B.L.; McCary, L.M.; Ford, A.L.; Golden, R.N.; Bailey, D.B., Jr. Trajectory and Predictors of Depression and Anxiety Disorders in Mothers with the FMR1 Premutation. Biol. Psychiatry 2016, 79, 850–857. [Google Scholar] [CrossRef] [PubMed]
- Sobesky, W.E.; Pennington, B.F.; Porter, D.; Hull, C.E.; Hagerman, R.J. Emotional and neurocognitive deficits in fragile X. Am. J. Med. Genet. 1994, 51, 378–385. [Google Scholar] [CrossRef] [PubMed]
- Bailey, D.B., Jr.; Raspa, M.; Olmsted, M.; Holiday, D.B. Co-occurring conditions associated with FMR1 gene variations: Findings from a national parent survey. Am. J. Med. Genet. A 2008, 146, 2060–2069. [Google Scholar] [CrossRef]
- Farzin, F.; Perry, H.; Hessl, D.; Loesch, D.; Cohen, J.; Bacalman, S.; Gane, L.; Tassone, F.; Hagerman, P.; Hagerman, R. Autism spectrum disorders and attention-deficit/hyperactivity disorder in boys with the fragile X premutation. J. Dev. Behav. Pediatr. 2006, 27 (Suppl. 2), S137–S144. [Google Scholar] [CrossRef]
- Clifford, S.; Dissanayake, C.; Bui, Q.M.; Huggins, R.; Taylor, A.K.; Loesch, D.Z. Autism spectrum phenotype in males and females with fragile X full mutation and premutation. J. Autism. Dev. Disord. 2007, 37, 738–747. [Google Scholar] [CrossRef]
- Chonchaiya, W.; Au, J.; Schneider, A.; Hessl, D.; Harris, S.W.; Laird, M.; Mu, Y.; Tassone, F.; Nguyen, D.V.; Hagerman, R.J. Increased prevalence of seizures in boys who were probands with the FMR1 premutation and co-morbid autism spectrum disorder. Hum. Genet. 2012, 131, 581–589. [Google Scholar] [CrossRef][Green Version]
- Lord, C.; Rutter, M.; DiLavore, P.; Risi, S.; Gotham, K.; Bishop, S. Autism Diagnostic Observation Schedule, 2nd ed.; Manual (Part 1): Modules 1–4; Western Psychological Services: Torrance, CA, USA, 2012. [Google Scholar]
- Wechsler, D. Wechsler Abbreviated Scale of Intelligence; Psychological Corporation: Tokyo, Japan, 1999. [Google Scholar]
- Roid, G.H.; Pomplun, M. The Stanford-Binet Intelligence Scales; The Guilford Press: New York, NY, USA, 2012. [Google Scholar]
- Wechsler, D. Wechsler adult intelligence scale. Arch. Clin. Neuropsychol. 1955. [Google Scholar] [CrossRef]
- Sparrow, S.S.; Balla, D.A.; Cicchetti, D.V.; Doll, E.A. Vineland Adaptive Behavior Scales Interview Edition Expanded Form Manual; American Guidance Services, Inc.: Circle Pines, MN, USA, 1984. [Google Scholar]
- First, M.B.; Gibbon, M.; Spitzer, R.L.; Williams, J.B.; Benjamin, L.S. Structured Clinical Interview for DSM-IV® Axis II Personality Disorders SCID-II.; American Psychiatric Pub.: Washington, DC, USA, 1997. [Google Scholar]
- Tassone, F.; Pan, R.; Amiri, K.; Taylor, A.K.; Hagerman, P.J. A rapid polymerase chain reaction-based screening method for identification of all expanded alleles of the fragile X (FMR1) gene in newborn and high-risk populations. J. Mol. Diagn. 2008, 10, 43–49. [Google Scholar] [CrossRef]
- Filipovic-Sadic, S.; Sah, S.; Chen, L.; Krosting, J.; Sekinger, E.; Zhang, W.; Hagerman, P.J.; Stenzel, T.T.; Hadd, A.G.; Latham, C.J.; et al. A novel FMR1 PCR method for the routine detection of low abundance expanded alleles and full mutations in fragile X syndrome. Clin. Chem. 2010, 56, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Corp, I. IBM SPSS Statistics for Windows; Version 22.0; IBM Corp.: Armonk, NY, USA, 2011. [Google Scholar]
- Cordeiro, L.; Abucayan, F.; Hagerman, R.; Tassone, F.; Hessl, D. Anxiety disorders in fragile X premutation carriers: Preliminary characterization of probands and non-probands. Intractable Rare Dis. Res. 2015, 4, 123–130. [Google Scholar] [CrossRef] [PubMed]
- Costello, E.J.; Egger, H.L.; Angold, A. The developmental epidemiology of anxiety disorders: Phenomenology, prevalence, and comorbidity. Child Adolesc. Psychiatr. Clin. N. Am. 2005, 14, 631–648. [Google Scholar] [CrossRef] [PubMed]
- Bitsko, R.H.; Claussen, A.H.; Lichstein, J.; Black, L.I.; Jones, S.E.; Danielson, M.L.; Hoenig, J.M.; Davis Jack, S.P.; Brody, D.J.; Gyawali, S.; et al. Mental Health Surveillance Among Children—United States, 2013–2019. MMWR Suppl. 2022, 71, 1–42. [Google Scholar] [CrossRef]
- Ghandour, R.M.; Sherman, L.J.; Vladutiu, C.J.; Ali, M.M.; Lynch, S.E.; Bitsko, R.H.; Blumberg, S.J. Prevalence and Treatment of Depression, Anxiety, and Conduct Problems in US Children. J. Pediatr. 2019, 206, 256–267.e3. [Google Scholar] [CrossRef]
- Maenner, M.J.; Shaw, K.A.; Bakian, A.V.; Bilder, D.A.; Durkin, M.S.; Esler, A.; Furnier, S.M.; Hallas, L.; Hall-Lande, J.; Hudson, A.; et al. Prevalence and Characteristics of Autism Spectrum Disorder Among Children Aged 8 Years—Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2018. MMWR Surveill. Summ. 2021, 70, 1–16. [Google Scholar] [CrossRef]
- Baxter, A.J.; Brugha, T.S.; Erskine, H.E.; Scheurer, R.W.; Vos, T.; Scott, J.G. The epidemiology and global burden of autism spectrum disorders. Psychol. Med. 2015, 45, 601–613. [Google Scholar] [CrossRef]
- White, S.J.; Gerber, D.; Sanchez Hernandez, R.D.; Efiannayi, A.; Chowdhury, I.; Partington, H.; Moss, J.F. Autistic traits and mental health in women with the fragile-X premutation: Maternal status versus genetic risk. Br. J. Psychiatry 2021, 218, 28–34. [Google Scholar] [CrossRef]
- Coury, D.L.; Anagnostou, E.; Manning-Courtney, P.; Reynolds, A.; Cole, L.; McCoy, R.; Whitaker, A.; Perrin, J.M. Use of psychotropic medication in children and adolescents with autism spectrum disorders. Pediatrics 2012, 130 (Suppl. 2), S69–S76. [Google Scholar] [CrossRef]
- Spencer, D.; Marshall, J.; Post, B.; Kulakodlu, M.; Newschaffer, C.; Dennen, T.; Azocar, F.; Jain, A. Psychotropic medication use and polypharmacy in children with autism spectrum disorders. Pediatrics 2013, 132, 833–840. [Google Scholar] [CrossRef] [PubMed]
- Lozano, R.; Hagerman, R.J.; Duyzend, M.; Budimirovic, D.B.; Eichler, E.E.; Tassone, F. Genomic studies in fragile X premutation carriers. J. Neurodev. Disord. 2014, 6, 27. [Google Scholar] [CrossRef] [PubMed]
- Aishworiya, R.; Protic, D.; Hagerman, R. Autism spectrum disorder in the Fragile X premutation state: Possible mechanisms and implications. J. Neurol. 2022, 269, 4676–4683. [Google Scholar] [CrossRef]
- Chen, Y.; Tassone, F.; Berman, R.F.; Hagerman, P.J.; Hagerman, R.J.; Willemsen, R.; Pessah, I.N. Murine hippocampal neurons expressing Fmr1 gene premutations show early developmental deficits and late degeneration. Hum. Mol. Genet. 2010, 19, 196–208. [Google Scholar] [CrossRef]
- Robin, G.; Lopez, J.R.; Espinal, G.M.; Hulsizer, S.; Hagerman, P.J.; Pessah, N. Calcium dysregulation and Cdk5-ATM pathway involved in a mouse model of fragile X-associated tremor/ataxia syndrome. Hum. Mol. Genet. 2017, 26, 2649–2666. [Google Scholar] [CrossRef] [PubMed]
- Napoli, E.; Ross-Inta, C.; Wong, S.; Omanska-Klusek, A.; Barrow, C.; Iwahashi, C.; Garcia-Arocena, D.; Sakaguchi, D.; Berry-Kravis, E.; Hagerman, R.; et al. Altered zinc transport disrupts mitochondrial protein processing/import in fragile X-associated tremor/ataxia syndrome. Hum. Mol. Genet. 2011, 20, 3079–3092. [Google Scholar] [CrossRef] [PubMed]
- Berman, R.F.; Buijsen, R.A.; Usdin, K.; Pintado, E.; Kooy, F.; Pretto, D.; Pessah, L.N.; Nelson, D.L.; Zalewski, Z.; Charlet-Bergeurand, N.; et al. Mouse models of the fragile X premutation and fragile X-associated tremor/ataxia syndrome. J. Neurodev. Disord. 2014, 6, 25. [Google Scholar] [CrossRef]
- Hagerman, R.; Hagerman, P. Fragile X-associated tremor/ataxia syndrome: Pathophysiology and management. Curr. Opin. Neurol. 2021, 34, 541–546. [Google Scholar] [CrossRef]
- Napoli, E.; Schneider, A.; Hagerman, R.; Song, G.; Wong, S.; Tassone, F.; Giulivi, C. Impact of FMR1 Premutation on Neurobehavior and Bioenergetics in Young Monozygotic Twins. Front. Genet. 2018, 9, 338. [Google Scholar] [CrossRef]
- Iossifov, I.; Ronemus, M.; Levy, D.; Wang, Z.; Hakker, I.; Rosenbaum, J.; Yamrom, B.; Lee, Y.H.; Narzisi, G.; Leotta, A.; et al. De novo gene disruptions in children on the autistic spectrum. Neuron 2012, 74, 285–299. [Google Scholar] [CrossRef]
- Baio, J.; Wiggins, L.; Christensen, D.L.; Maenner, M.J.; Daniels, J.; Warren, Z.; Kurzius-Spencer, M.; Zahorodny, W.; Rosenberg, C.R.; White, T. Prevalence of autism spectrum disorder among children aged 8 years—Autism and developmental disabilities monitoring network, 11 sites, United States, 2014. MMWR Surveill. Summ. 2018, 67, 1. [Google Scholar] [CrossRef] [PubMed]
- Charman, T.; Pickles, A.; Simonoff, E.; Chandler, S.; Loucas, T.; Baird, G. IQ in children with autism spectrum disorders: Data from the Special Needs and Autism Project (SNAP). Psychol. Med. 2011, 41, 619–627. [Google Scholar] [CrossRef] [PubMed]
| Variable | All | Males | Females | p-Value | Probands | Non-Probands | p-Value |
|---|---|---|---|---|---|---|---|
| N (%) | 61 | 52 (85.2) | 9 (14.5) | / | 28 | 33 | / |
| Males (%) | / | / | / | / | 24 (86) | 28 (85) | 1.0 |
| Age range (years) | 7.8–20.0 | 8–20 | 9–19 | / | 8–19 | 8–20 | / |
| Mean age (years) | 12.6 ± 3.4 | 12.2 ± 3.3 | 14.7 ± 3.5 | 0.04 | 12.8 ± 3.6 | 12.2 ± 3.2 | 0.47 |
| Mean (SD) | |||||||
| CGG repeat size | 96.7 ± 41.2 | 101.0 ± 42.4 | 73.0 ± 24.0 | 0.01 | 98.5 ± 46.3 | 95.0 ± 36.9 | 0.75 |
| Mean mRNA level (AU) | 2.8 ± 1.1 † | 2.9 ± 1.1 † | 1.6 ± 0 | NA | 2.9 ± 1.2 | 2.8 ± 1.1 | 0.76 |
| Mean FMRP level (AU) | 1.1 ± 0.4 | 0.9 ± 0.4 ‡ | 1.3 ± 0.3 ‡ | 0.04 | 1.1 ± 0.3 | 1.1 ± 0.4 | 1.00 |
| FSIQ | 90.9 ± 22.7 | 91.2 ± 21.8 | 89.3 ± 28.1 | 0.83 | 79.0 ± 25.0 | 99.3 ± 16.6 | 0.001 |
| PIQ | 93.0 ± 20.9 | 91.1 ± 20.9 | 98.6 ± 21.5 | 0.42 | 78.6 ± 21.1 | 101.5 ± 16.0 | 0.004 |
| VIQ | 96.5 ± 25.2 | 95.7 ± 27.1 | 98.7 ± 20.4 | 0.79 | 83.3 ± 32.5 | 103.8 ± 17.1 | 0.04 |
| VABS ABC | 81.8 ± 14.7 | 81.1 ± 15.4 | 88.0 ± 3.6 | 0.54 | 71.9 ± 14.7 | 89.8 ± 9.1 | 0.004 |
| VABS Communication | 79.5.5 ± 15.7 | 79.4 ± 16.1 | 81.0 ± 17.0 | 0.89 | 72.8 ± 11.8 | 85.6 ± 16.9 | 0.0750 |
| VABS Socialization | 86.1 ± 16.3 | 84.1 ± 16.1 | 102.0 ± 2.8 | 0.15 | 75.0 ± 17.6 | 94.9 ± 7.9 | 0.005 |
| VABS Daily living | 85.8 ± 17.8 | 85.1 ± 18.7 | 91.5 ± 6.4 | 0.64 | 74.8 ± 18.1 | 95.7 ± 10.6 | 0.006 |
| Condition | All (N = 61) | Male (N = 52) | Female (N = 9) | p-Value | Probands (N = 28) | Non-Probands (N = 33) | p-Value |
|---|---|---|---|---|---|---|---|
| ASD (N, %) | 20 (32.8) | 17 (32.7) | 3 (33.3) | 1 | 15 (53.6) | 5 (15.2) | 0.04 |
| ADHD (N, %) | 40 (65.6) | 39 (97.5) | 1 (11.1) | 0.0004 | 18 (64.3) | 22 (66.7) | 0.37 |
| OCD (N, %) | 20 (32.8) | 19 (36.5) | 1 (11.1) | 0.24 | 11 (39.3) | 9 (27.3) | 0.27 |
| Anxiety (N, %) | 50 (82.0) | 43 (82.7) | 7 (77.8) | 1 | 23 (82.1) | 27 (81.2) | 0.38 |
| Social Phobia (N, %) | 14 (23.0) | 13 (25.0) | 1 (11.1) | 0.44 | 6 (21.4) | 8 (24.2) | 0.86 |
| Depression (N, %) | 12 (19.7) | 10 (19.2) | 2 (22.2) | 1 | 5 (17.9) | 7 (21.2) | 0.85 |
| Variables | ASD Present (N = 20) | ASD Absent (N = 30) | p-Value | Probands with ASD (N = 15) | Non-Probands with ASD (N = 5) | p-Value |
|---|---|---|---|---|---|---|
| Mean (SD) | ||||||
| Age in years | 12.7 (+3.5) | 12.3 (3.2) | 0.60 | 14.0 (3.2) | 9.2 (1.34) | 0.005 |
| CGG repeat size | 95.9 (46.4) | 96.1 (39.3) | 0.99 | 100 (47.8) | 81.5 (44.0) | 0.50 |
| mRNA level (AU) | 2.8 (1.3) | 2.8 (1.1) | 0.87 | 3.1 (1.4) | 2.1 (0.4) | 0.19 |
| FSIQ | 73.5 (21.7) | 98.0 (20.0) | 0.001 | 62.1 (14.6) | 94.0 (16.8) | 0.003 |
| VIQ | 75.1 (20.4) | 102.9 (23.2) | 0.009 | 64.2 (11.3) | 93.3 (20.1) | 0.04 |
| PIQ | 77.6 (16.3) | 101.0 (20.2) | 0.01 | 70.2 (11.3) | 96.0 (11.3) | 0.04 |
| VABS ABC | 76.8 (15.0) | 86.7 (13.4) | 0.14 | 69.7 (14.3) | 87.5 (9.0) | 0.06 |
| VABS Communication | 76.6 (15.1) | 82.8 (16.7) | 0.41 | 71.2 (12.3) | 84.8 (16.8) | 0.17 |
| VABS Socialization | 81.0 (17.2) | 91.1 (14.4) | 0.12 | 73.0 (19.1) | 91.0 (7.8) | 0.12 |
| VABS Daily living | 82.0 (19.9) | 90.0 (15.0) | 0.34 | 72.3 (17.0) | 96.5 (15.7) | 0.05 |
| Number of prescribed medications | 2.32 (1.0) | 1.3 (1.11) | 0.002 | 2.3 (1.1) | 2.4 (0.9) | 0.83 |
| Number of Males (%) | 17 (85.0) | 27 (90.0) | 0.59 | 12 (80) | 5 (100) | 0.54 |
| Number with ADHD (%) | 14 (70.0) | 19 (63.3) | 0.15 | 9 (60) | 5 (100) | 0.26 |
| Number with Depression (%) | 1 (5.0) | 9 (30.0) | 0.17 | 1 (7) | 0 (0) | >0.99 |
| Number with Anxiety (%) | 16 (80.0) | 24 (80.0) | 0.89 | 12 (80) | 4 (80) | >0.99 |
| Intake of Medications (Yes/No) | All (N = 61) | Males (N = 52) | Female (N = 9) | p-Value | Probands (N = 28) | Non-Probands (N = 33) | p-Value |
|---|---|---|---|---|---|---|---|
| N (%) | |||||||
| Antipsychotics | 12 (19.7) | 12 (23.1) | 0 (0) | NA | 10 (35.7) | 2 (6.1) | 0.005 |
| Antidepressants (All) | 45 (75.0) | 40 (76.9) | 5 (55.5) | 0.57 | 20 (71.4) | 25 (75.7) | 0.69 |
| SSRIs | 42 (68.9) | 36 (69.2) | 6 (66.7) | 0.55 | 18 (64.28) | 24 (72.7) | 0.48 |
| Stimulants | 20 (32.8) | 19 (36.5) | 1 (11.1) | NA | 8 (28.57) | 12 (36.4) | 0.52 |
| α agonists | 5 (8.2) | 4 (7.7) | 1 (11.1) | NA | 2 (7.14) | 3 (9.1) | 1 † |
| Melatonin | 2 (3.3) | 2 (3.8) | 0 (0) | NA | 0 (0) | 2 (6.1) | 0.49 † |
| Other Medications | 10 (16.4) | 6 (11.5) | 4 (44.4) | 0.60 | 8 (28.57) | 2 (6.1) | 0.03 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aishworiya, R.; Protic, D.; Tang, S.J.; Schneider, A.; Tassone, F.; Hagerman, R. Fragile X-Associated Neuropsychiatric Disorders (FXAND) in Young Fragile X Premutation Carriers. Genes 2022, 13, 2399. https://doi.org/10.3390/genes13122399
Aishworiya R, Protic D, Tang SJ, Schneider A, Tassone F, Hagerman R. Fragile X-Associated Neuropsychiatric Disorders (FXAND) in Young Fragile X Premutation Carriers. Genes. 2022; 13(12):2399. https://doi.org/10.3390/genes13122399
Chicago/Turabian StyleAishworiya, Ramkumar, Dragana Protic, Si Jie Tang, Andrea Schneider, Flora Tassone, and Randi Hagerman. 2022. "Fragile X-Associated Neuropsychiatric Disorders (FXAND) in Young Fragile X Premutation Carriers" Genes 13, no. 12: 2399. https://doi.org/10.3390/genes13122399
APA StyleAishworiya, R., Protic, D., Tang, S. J., Schneider, A., Tassone, F., & Hagerman, R. (2022). Fragile X-Associated Neuropsychiatric Disorders (FXAND) in Young Fragile X Premutation Carriers. Genes, 13(12), 2399. https://doi.org/10.3390/genes13122399






