In Vitro Fertilisation (IVF) Associated with Preimplantation Genetic Testing for Monogenic Diseases (PGT-M) in a Romanian Carrier Couple for Congenital Disorder of Glycosylation Type Ia (CDG-Ia): A Case Report
Abstract
1. Introduction
2. Case Presentation
3. Discussion
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A


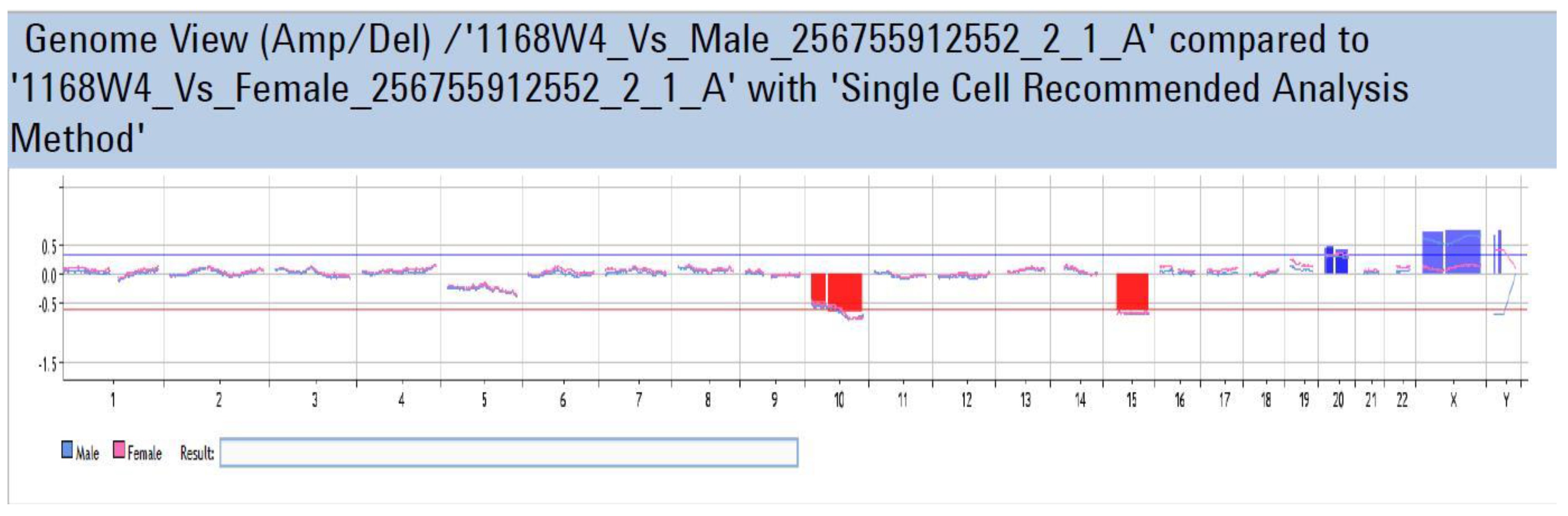
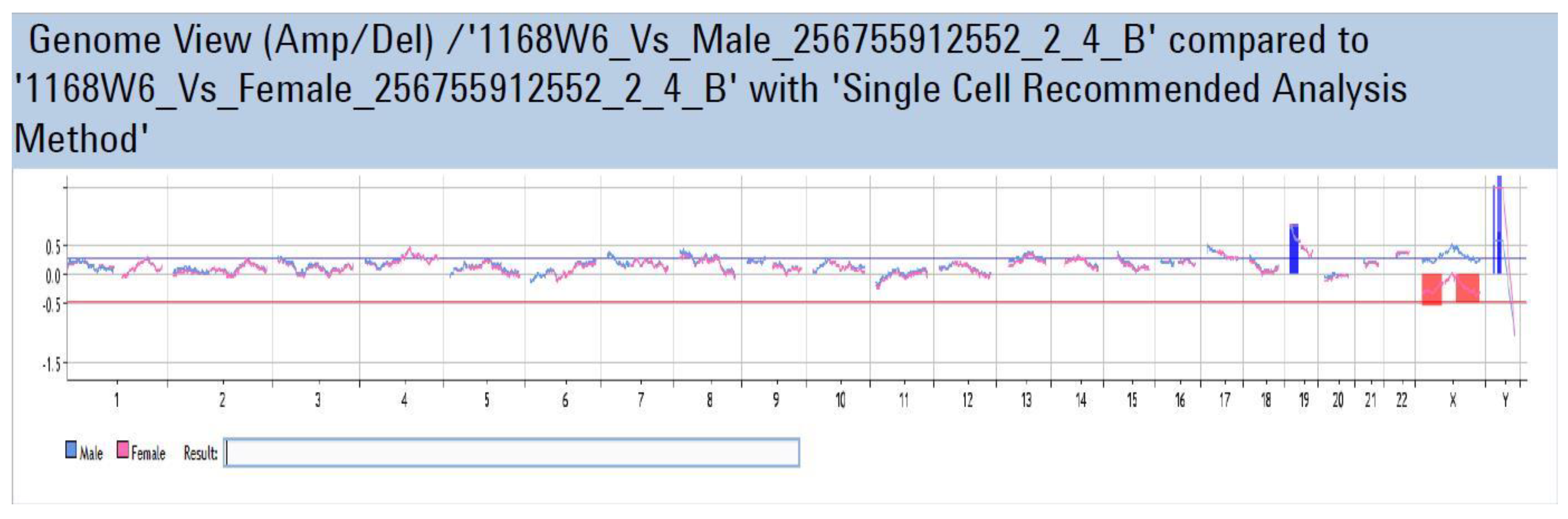
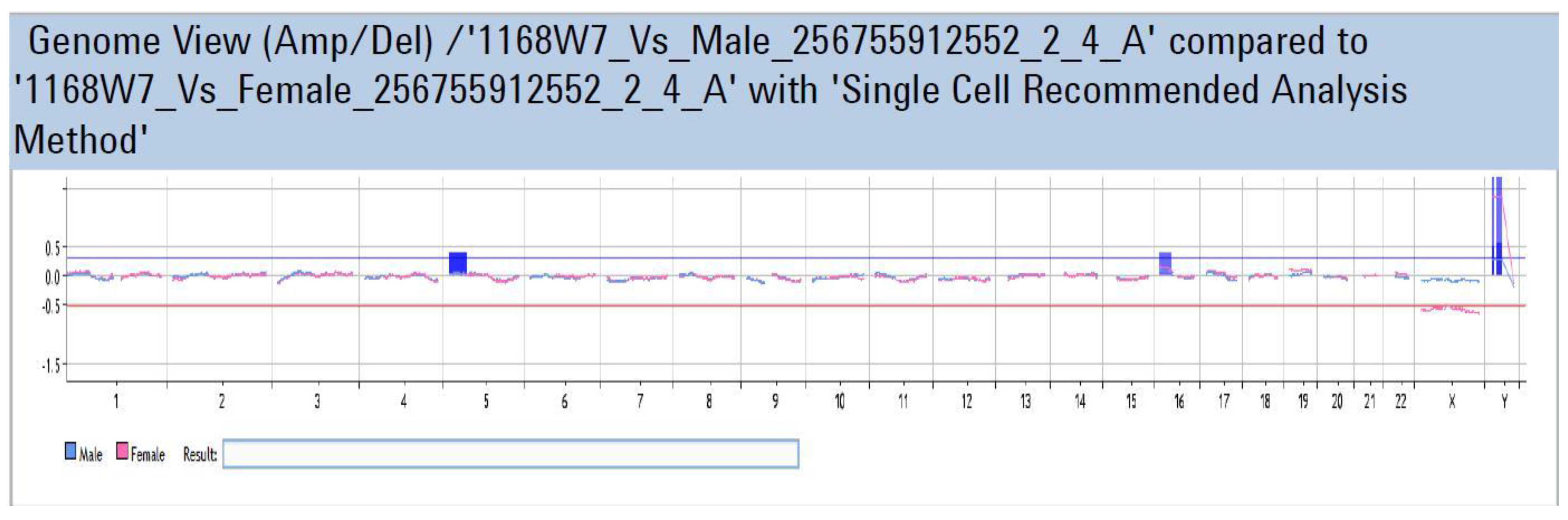

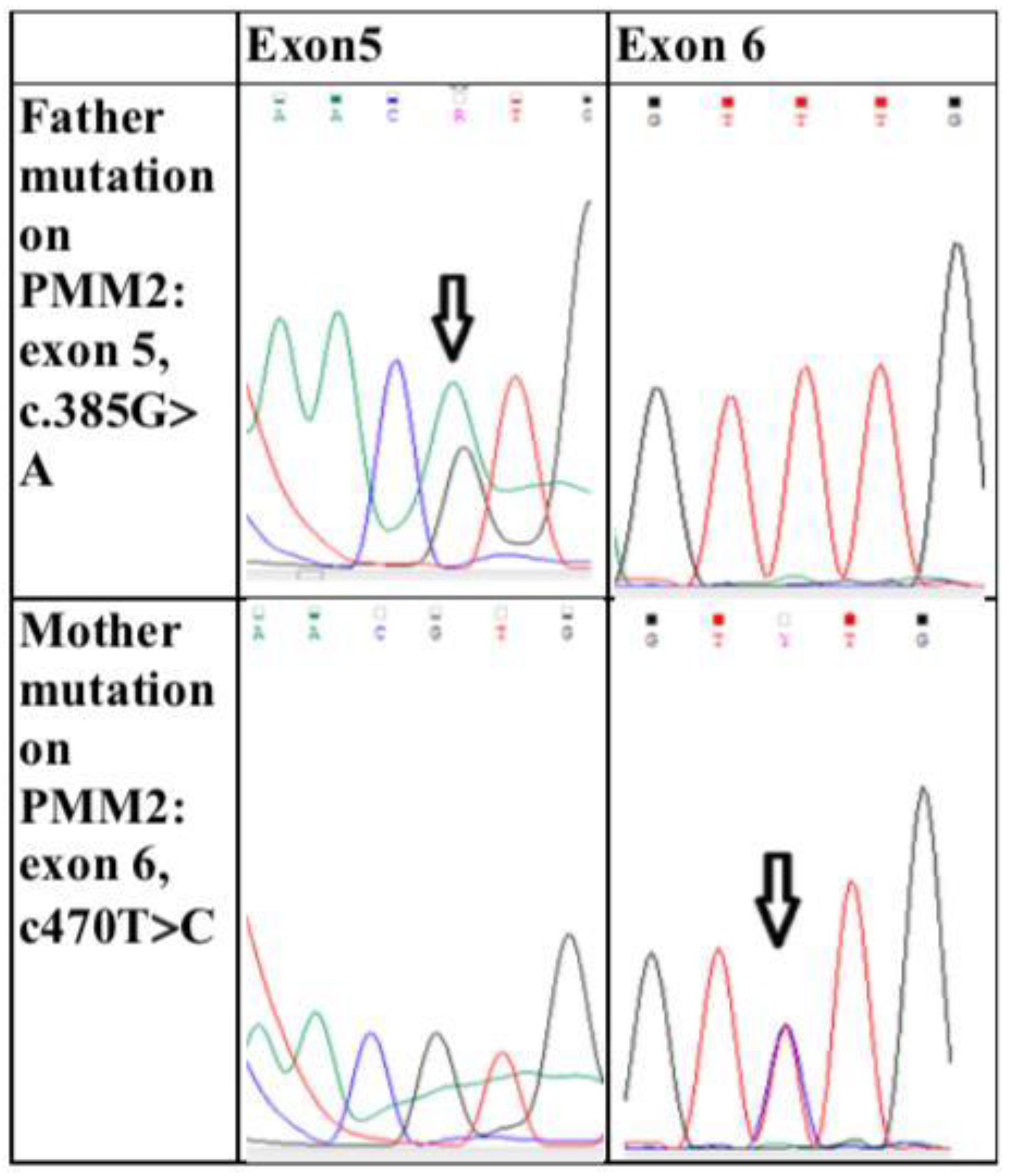
References
- Grünewald, S.; Matthijs, G.; Jaeken, J. Congenital Disorders of Glycosylation: A Review. Pediatr. Res. 2002, 52, 618–624. [Google Scholar] [CrossRef] [PubMed]
- Freeze, H.H.; Eklund, E. Introduction to Human Glycosylation Disorders. In Handbook of Glycomics; Cummings, R.D., Pierce, J.M., Eds.; Academic Press: Waltham, MA, USA, 2010; pp. 431–464. [Google Scholar]
- Jaeken, J.; Vanderschueren-Lodeweyckx, M.; Casaer, P.; Snoeck, L.; Corbeel, L.; Eggermont, E. Familial psychomotor retardation with markedly fluctuating serum prolactin, FSH and GH levels, partial TBG-deficiency, increased serum arylsulphatase A and increased CSF protein: A new syndrome?: 90. Pediatr. Res. 1980, 14, 179. [Google Scholar] [CrossRef]
- Ganetzky, R.; Reynoso, F.J.; He, M. Congenital disorders of glycosylation. In Biomarkers in Inborn Errors of Metabolism; Garg, U., Smith, L.D., Eds.; Elsevier: Amsterdam, The Netherlands, 2017; pp. 343–360. [Google Scholar]
- Jaeken, J. Glycosylation and its Disorders: General Overview. Ref. Modul. Biomed. Sci. 2016. [Google Scholar] [CrossRef]
- Scott, K.; Gadomski, T.; Kozicz, T.; Morava, E. Congenital disorders of glycosylation: New defects and still counting. J. Inherit. Metab. Dis. 2014, 37, 609–617. [Google Scholar] [CrossRef] [PubMed]
- Van Schaftingen, E.; Jaeken, J. Phosphomannomutase deficiency is a cause of carbohydrate-deficient glycoprotein syndrome type I. FEBS Lett. 1995, 377, 318–320. [Google Scholar]
- Goreta, S.S.; Dabelic, S.; Dumic, J. Insights into complexity of congenital disorders of glycosylation. Biochem. Med. 2012, 22, 156–170. [Google Scholar] [CrossRef]
- Ohtsubo, K.; Marth, J.D. Glycosylation in Cellular Mechanisms of Health and Disease. Cell 2006, 126, 855–867. [Google Scholar] [CrossRef]
- Vega, A.I.; Pérez-Cerdá, C.; Abia, D.; Gámez, A.; Briones, P.; Artuch, R.; Desviat, L.R.; Ugarte, M.; Pérez, B. Expression analysis revealing destabilizing mutations in phosphomannomutase 2 deficiency (PMM2-CDG). J. Inherit. Metab. Dis. 2011, 34, 929–939. [Google Scholar] [CrossRef]
- Haeuptle, M.A.; Hennet, T. Congenital disorders of glycosylation: An update on defects affecting the biosynthesis of dolichol-linked oligosaccharides. Hum. Mutat. 2009, 30, 1628–1641. [Google Scholar] [CrossRef]
- Jaeken, J. Congenital disorders of glycosylation. Ann. N. Y. Acad. Sci. 2010, 1214, 190–198. [Google Scholar] [CrossRef]
- Erlandson, A.; Bjursell, C.; Stibler, H.; Kristiansson, B.; Wahlström, J.; Martinsson, T. Scandinavian CDG-Ia patients: Genotype/phenotype correlation and geographic origin of founder mutations. Hum. Genet. 2001, 108, 359–367. [Google Scholar] [CrossRef] [PubMed]
- Imtiaz, F.; Worthington, V.; Champion, M.; Beesley, C.; Charlwood, J.; Clayton, P.; Keir, G.; Mian, N.; Winchester, B. Genotypes and phenotypes of patients in the UK with carbohydrate-deficient glycoprotein syndrome type 1. J. Inherit. Metab. Dis. 2000, 23, 162–174. [Google Scholar] [CrossRef] [PubMed]
- Enns, G.M.; Steiner, R.D.; Buist, N.; Cowan, C.; Leppig, K.A.; McCracken, M.F.; Westphal, V.; Freeze, H.H.; O’Brien, J.F.; Jaeken, J.; et al. Clinical and molecular features of congenital disorder of glycosylation in patients with type 1 sialotransferrin pattern and diverse ethnic origins. J. Pediatr. 2002, 141, 695–700. [Google Scholar] [CrossRef]
- Ohno, K.; Yuasa, I.; Akaboshi, S.; Itoh, M.; Yoshida, K.; Ehara, H.; Ochiai, Y.; Takeshita, K. The carbohydrate deficient glycoprotein syndrome in three Japanese children. Brain Dev. 1992, 14, 30–35. [Google Scholar] [CrossRef]
- Briones, P.; Vilaseca, M.A.; Schollen, E.; Ferrer, I.; Maties, M.; Busquets, C.; Artuch, R.; Gort, L.; Marco, M.; van Schaftingen, E.; et al. Biochemical and molecular studies in 26 Spanish patients with congenital disorder of glycosylation type Ia. J. Inherit. Metab. Dis. 2003, 25, 635–646. [Google Scholar] [CrossRef] [PubMed]
- De Lonlay, P.; Seta, N.; Barrot, S.; Chabrol, B.; Drouin, V.; Gabriel, B.M.; Journelf, H.; Kretzg, M.; Laurenta, J.; le Merrer, M.; et al. A broad spectrum of clinical presentations in congenital disorders of glycosylation I: A series of 26 cases. J. Med. Genet. 2001, 38, 14–19. [Google Scholar] [CrossRef]
- Pérez-Dueñas, B.; García-Cazorla, A.; Pineda, M.; Poo, P.; Campistol, J.; Cusí, V.; Schollenf, E.; Matthijsf, G.; Grunewalde, S.; Briones, P.; et al. Long-term evolution of eight Spanish patients with CDG type Ia: Typical and atypical manifestations. Eur. J. Paediatr. Neurol. 2009, 13, 444–451. [Google Scholar] [CrossRef]
- Monin, M.-L.; Mignot, C.; de Lonlay, P.; Héron, B.; Masurel, A.; Mathieu-Dramard, M.; Lenaerts, C.; Thauvin, C.; Gérard, M.; Roze, E.; et al. 29 French adult patients with PMM2-congenital disorder of glycosylation: Outcome of the classical pediatric phenotype and depiction of a late-onset phenotype. Orphanet J. Rare Dis. 2014, 9, 207. [Google Scholar] [CrossRef]
- Vals, M.-A.; Pajusalu, S.; Kals, M.; Mägi, R.; Õunap, K. The Prevalence of PMM2-CDG in Estonia Based on Population Carrier Frequencies and Diagnosed Patients. JIMD Rep. 2018, 39, 13–17. [Google Scholar]
- Krasnewich, D.; O’Brien, K.; Sparks, S. Clinical features in adults with congenital disorders of glycosylation type Ia (CDG-Ia). Am. J. Med. Genet. Part C Semin. Med. Genet. 2007, 145, 302–306. [Google Scholar] [CrossRef]
- Le Bizec, C.; Vuillaumier-Barrot, S.; Barnier, A.; Dupré, T.; Durand, G.; Seta, N. A new insight into PMM2 mutations in the French population. Hum. Mutat. 2005, 25, 504–505. [Google Scholar] [CrossRef] [PubMed]
- Stefanits, H.; Konstantopoulou, V.; Kuess, M.; Milenkovic, I.; Matula, C. Initial diagnosis of the congenital disorder of glycosylation PMM2-CDG (CDG1a) in a 4-year-old girl after neurosurgical intervention for cerebral hemorrhage. J. Neurosurg. Pediatr. Ped. 2014, 14, 546–549. [Google Scholar] [CrossRef]
- Miossec-Chauvet, E.; Mikaeloff, Y.; Heron, D.; Merzoug, V.; Cormier-Daire, V.; Lonlay, P.; Matthijs, G.; van Hulle, C.; Ponsot, G.; Seta, N. Neurological Presentation in Pediatric Patients with Congenital Disorders of Glycosylation Type Ia. Neuropediatrics 2003, 34, 1–6. [Google Scholar] [CrossRef] [PubMed]
- McKenzie, F.A.; Fietz, M.; Fletcher, J.; Smith, R.L.L.; Wright, I.M.R.; Jaeken, J. A previously undescribed form of congenital disorder of glycosylation with variable presentation in siblings: Early fetal loss with hydrops fetalis, and infant death with hypoproteinemia. Am. J. Med. Genet. Part A 2007, 143, 2029–2034. [Google Scholar] [CrossRef] [PubMed]
- Wolthuis, D.F.G.J.; Janssen, M.C.; Cassiman, D.; Lefeber, D.J.; Morava-Kozicz, E. Defining the phenotype and diagnostic considerations in adults with congenital disorders of N-linked glycosylation. Expert Rev. Mol. Diagn. 2014, 14, 217–224. [Google Scholar] [CrossRef]
- Stibler, H.; Blennow, G.; Kristiansson, B.; Lindehammer, H.; Hagberg, B. Carbohydrate-deficient glycoprotein syndrome: Clinical expression in adults with a new metabolic disease. J. Neurol. Neurosurg. Psychiatry 1994, 57, 552–556. [Google Scholar] [CrossRef]
- Kjaergaard, S.; Schwartz, M.; Skovby, F. Congenital disorder of glycosylation type Ia (CDG-Ia): Phenotypic spectrum of the R141H/F119L genotype. Arch. Dis. Child. 2001, 85, 236–239. [Google Scholar] [CrossRef]
- Coman, D.; McGill, J.; MacDonald, R.; Morris, D.; Klingberg, S.; Jaeken, J.; Appleton, D. Congenital disorder of glycosylation type 1a: Three siblings with a mild neurological phenotype. J. Clin. Neurosci. 2007, 14, 668–672. [Google Scholar] [CrossRef]
- Bortot, B.; Cosentini, D.; Faletra, F.; Biffi, S.; De Martino, E.; Carrozzi, M.; Severini, M.G. PMM2-CDG: Phenotype and genotype in four affected family members. Gene 2013, 531, 506–509. [Google Scholar] [CrossRef]
- Grünewald, S. The clinical spectrum of phosphomannomutase 2 deficiency (CDG-Ia). Biochim. Biophys. Acta Mol. Basis Dis. 2009, 1792, 827–834. [Google Scholar] [CrossRef]
- Grünewald, S.; Schollen, E.; Van Schaftingen, E.; Jaeken, J.; Matthijs, G. High residual activity of PMM2 in patients’ fibroblasts: Possible pitfall in the diagnosis of CDG-Ia (phosphomannomutase deficiency). Am. J. Hum. Genet. 2001, 68, 347–354. [Google Scholar] [CrossRef] [PubMed]
- Citro, V.; Cimmaruta, C.; Monticelli, M.; Riccio, G.; Hay Mele, B.; Cubellis, M.V.; Andreotti, G. The Analysis of Variants in the General Population Reveals That PMM2 Is Extremely Tolerant to Missense Mutations and That Diagnosis of PMM2-CDG Can Benefit from the Identification of Modifiers. Int. J. Mol. Sci. 2018, 19, 2218. [Google Scholar] [CrossRef] [PubMed]
- Thirumal Kumar, D.; Jain, N.; Udhaya Kumar, S.; George Priya Doss, C.; Zayed, H. Identification of potential inhibitors against pathogenic missense mutations of PMM2 using a structure-based virtual screening approach. J. Biomol. Struct. Dyn. 2019, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Casado, M.; O’Callaghan, M.M.; Montero, R.; Pérez-Cerda, C.; Pérez, B.; Briones, P.; Quintana, E.; Muchart, J.; Aracil, A.; Pineda, M.; et al. Mild Clinical and Biochemical Phenotype in Two Patients with PMM2-CDG (Congenital Disorder of Glycosylation Ia). Cerebellum 2012, 11, 557–563. [Google Scholar] [CrossRef] [PubMed]
- Jaeken, J.; Lefeber, D.; Matthijs, G. Clinical utility gene card for: Phosphomannomutase 2 deficiency. Eur. J. Hum. Genet. 2014, 22, 1054. [Google Scholar] [CrossRef][Green Version]
- De Koning, T.J.; Toet, M.; Dorland, L.; de Vries, L.S.; van den Berg, I.E.T.; Duran, M.; Poll-The, B.T. Recurrent nonimmune hydrops fetalis associated with carbohydrate-deficient glycoprotein syndrome. J. Inherit. Metab. Dis. 1998, 21, 681–682. [Google Scholar] [CrossRef]
- Schwarz, M.; Thiel, C.; Lübbehusen, J.; Dorland, B.; de Koning, T.; von Figura, K.; Lehle, L.; Körner, C. Deficiency of GDP-Man:GlcNAc2-PP-dolichol mannosyltransferase causes congenital disorder of glycosylation type Ik. Am. J. Hum. Genet. 2004, 74, 472–481. [Google Scholar] [CrossRef][Green Version]
- Vesela, K.; Honzik, T.; Hansikova, H.; Haeuptle, M.A.; Semberova, J.; Stranak, Z.; Hennet, T.; Zeman, J. A new case of ALG8 deficiency (CDG Ih). J. Inherit. Metab. Dis. 2009, 32, 259–264. [Google Scholar] [CrossRef]
- Aronica, E.; van Kempen, A.A.M.W.; van der Heide, M.; Poll-The, B.T.; van Slooten, H.J.; Troost, D.; Rozemuller-Kwakkel, J.M. Congenital disorder of glycosylation type Ia: A clinicopathological report of a newborn infant with cerebellar pathology. Acta Neuropathol. 2005, 109, 433–442. [Google Scholar] [CrossRef]
- Noelle, V.; Knuepfer, M.; Pulzer, F.; Schuster, V.; Siekmeyer, W.; Matthijs, G.; Vogtmann, C. Unusual presentation of congenital disorder of glycosylation type 1a: Congenital persistent thrombocytopenia, hypertrophic cardiomyopathy and hydrops-like aspect due to marked peripheral oedema. Eur. J. Pediatr. 2005, 164, 223–226. [Google Scholar] [CrossRef]
- Van de Kamp, J.M.; Lefeber, D.J.; Ruijter, G.J.G.; Steggerda, S.J.; den Hollander, N.S.; Willems, S.M.; Matthijs, G.; Poorthuis, B.J.H.M.; Wevers, R.A. Congenital disorder of glycosylation type Ia presenting with hydrops fetalis. J. Med. Genet. 2007, 44, 277–280. [Google Scholar] [CrossRef] [PubMed]
- Wurm, D.; Löffler, G.; Lindinger, A.; Gortner, L. Congenital disorders of glycosylation type Ia as a cause of mirror syndrome. J. Perinatol. 2007, 27, 802–804. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Truin, G.; Guillard, M.; Lefeber, D.J.; Sykut-Cegielska, J.; Adamowicz, M.; Hoppenreijs, E.; Sengersa, R.C.A.; Weversb, R.A.; Moravaa, E. Pericardial and abdominal fluid accumulation in Congenital Disorder of Glycosylation type Ia. Mol. Genet. Metab. 2008, 94, 481–484. [Google Scholar] [CrossRef] [PubMed]
- Schollen, E.; Kjaergaard, S.; Martinsson, T.; Vuillaumier-Barrot, S.; Dunoe, M.; Keldermans, L.; Seta, N.; Matthijs, G. Increased recurrence risk in congenital disorders of glycosylation type Ia (CDG-Ia) due to a transmission ratio distortion. J. Med. Genet. 2004, 41, 877–880. [Google Scholar] [CrossRef] [PubMed]
- McAllister, M.; Moldovan, R.; Paneque, M.; Skirton, H. The need to develop an evidence base for genetic counselling in Europe. Eur. J. Hum. Genet. 2016, 24, 504–505. [Google Scholar] [CrossRef] [PubMed]
- Nahman, M. Romanian IVF: A brief history through the ‘lens’ of labour, migration and global egg donation markets. Reprod. Biomed. Soc. Online 2016, 2, 79–87. [Google Scholar] [CrossRef] [PubMed]
| PMM2-CDG Phenotype | Pregnancy Status | Molecular Analysis | Reference |
|---|---|---|---|
| Postnatal | Full-term (death at four weeks) and ultrasound echography at twenty gestational weeks | c.691G>A p.Val231Met c.710C>G p.Thr237Arg | [41] |
| At fifty days | Full-term (death at eight weeks) and ultrasound echography at birth | c.357CNA p.Phe119Leu c.470 TNC p.Phe157Ser | [42] |
| Both in day two | Births at thirty-two and thirty-six gestational weeks, respectively, through Caesarean section. Death at day 7 and an ultrasound echography was carried out at twenty-nine gestational weeks. Death in week eight and an ultrasound echography was carried out at thirty-five gestational weeks | c.160_161insG c.357CNA p.Phe119Leu c.357CNA p.Phe119Leu c.470 TNC p.Phe157Ser | [43] |
| After birth, before week eight | Siblings—Both births at thirty-six gestational weeks through Caesarean section and have died at three and eight weeks, respectively. Only one ultrasound echography was carried out at thirty-one gestational weeks. Not specified for the other one. | c.161_162insG c.385GNT p.Val129L | [44] |
| Not specified | Full-term from which one died at six years and the third at four months. Not specified for the second infant. An ultrasound echography was carried out at birth for all three | c.357CNA p.Phe119Leu c.422GNA p.Arg141His c.691GNA p.Val231Met c.640-15479CNT c.563ANG p.Asp188Gly c.104 T>A p.Leu35 | [45] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Doroftei, B.; Nemtanu, L.; Ilie, O.-D.; Simionescu, G.; Ivanov, I.; Anton, E.; Puiu, M.; Maftei, R. In Vitro Fertilisation (IVF) Associated with Preimplantation Genetic Testing for Monogenic Diseases (PGT-M) in a Romanian Carrier Couple for Congenital Disorder of Glycosylation Type Ia (CDG-Ia): A Case Report. Genes 2020, 11, 697. https://doi.org/10.3390/genes11060697
Doroftei B, Nemtanu L, Ilie O-D, Simionescu G, Ivanov I, Anton E, Puiu M, Maftei R. In Vitro Fertilisation (IVF) Associated with Preimplantation Genetic Testing for Monogenic Diseases (PGT-M) in a Romanian Carrier Couple for Congenital Disorder of Glycosylation Type Ia (CDG-Ia): A Case Report. Genes. 2020; 11(6):697. https://doi.org/10.3390/genes11060697
Chicago/Turabian StyleDoroftei, Bogdan, Loredana Nemtanu, Ovidiu-Dumitru Ilie, Gabriela Simionescu, Iuliu Ivanov, Emil Anton, Maria Puiu, and Radu Maftei. 2020. "In Vitro Fertilisation (IVF) Associated with Preimplantation Genetic Testing for Monogenic Diseases (PGT-M) in a Romanian Carrier Couple for Congenital Disorder of Glycosylation Type Ia (CDG-Ia): A Case Report" Genes 11, no. 6: 697. https://doi.org/10.3390/genes11060697
APA StyleDoroftei, B., Nemtanu, L., Ilie, O.-D., Simionescu, G., Ivanov, I., Anton, E., Puiu, M., & Maftei, R. (2020). In Vitro Fertilisation (IVF) Associated with Preimplantation Genetic Testing for Monogenic Diseases (PGT-M) in a Romanian Carrier Couple for Congenital Disorder of Glycosylation Type Ia (CDG-Ia): A Case Report. Genes, 11(6), 697. https://doi.org/10.3390/genes11060697







