Highly Efficient Conversion of Motor Neuron-Like NSC-34 Cells into Functional Motor Neurons by Prostaglandin E2
Abstract
1. Introduction
2. Materials and Methods
2.1. Reagents
2.2. Cell Culture
2.3. Neurite Outgrowth Assay
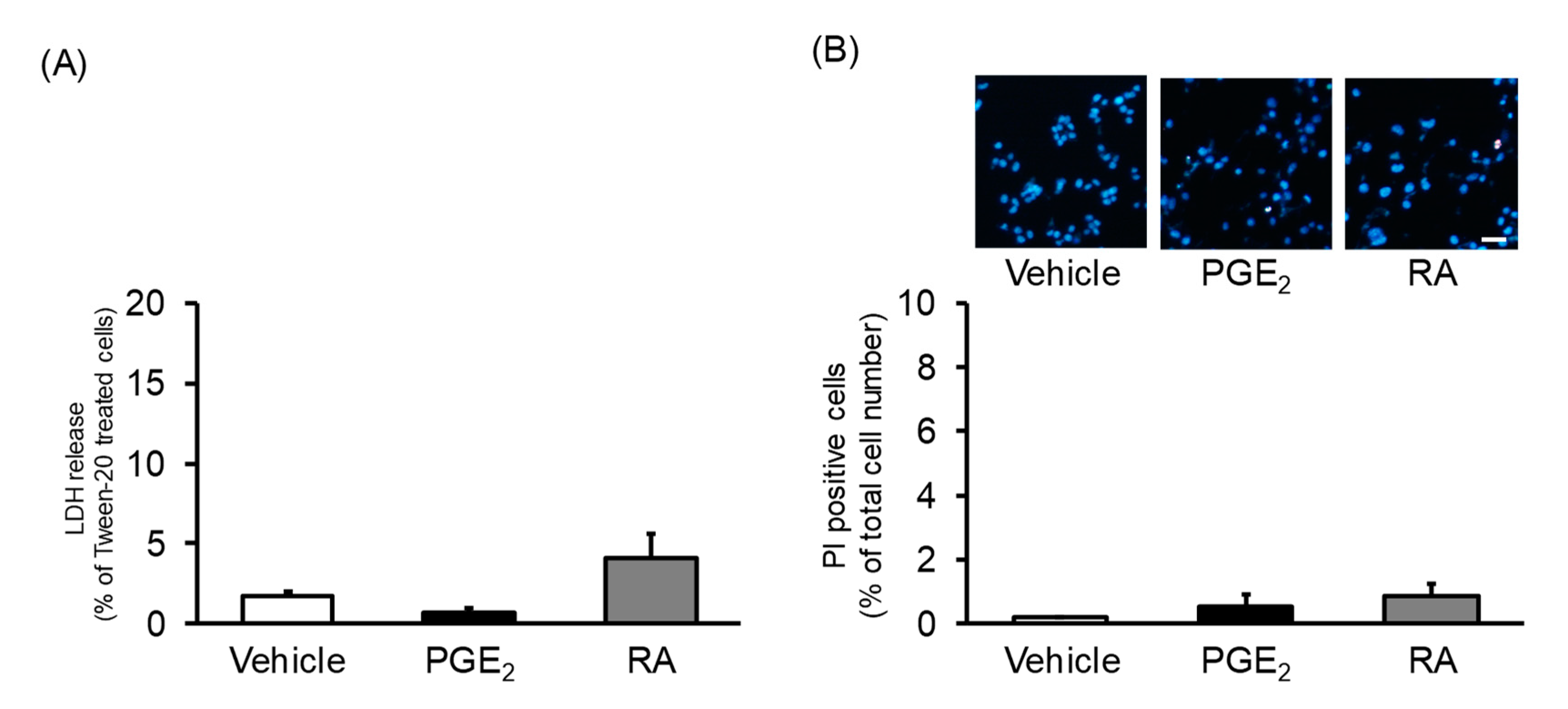
2.4. Cell Viability Assay
2.5. Nuclear Staining Assay
2.6. Whole-Cell Patch-Clamp Recording
2.7. Western Blotting
2.8. Acetylcholine Release and Quantification
2.9. Statistical Analysis
3. Results
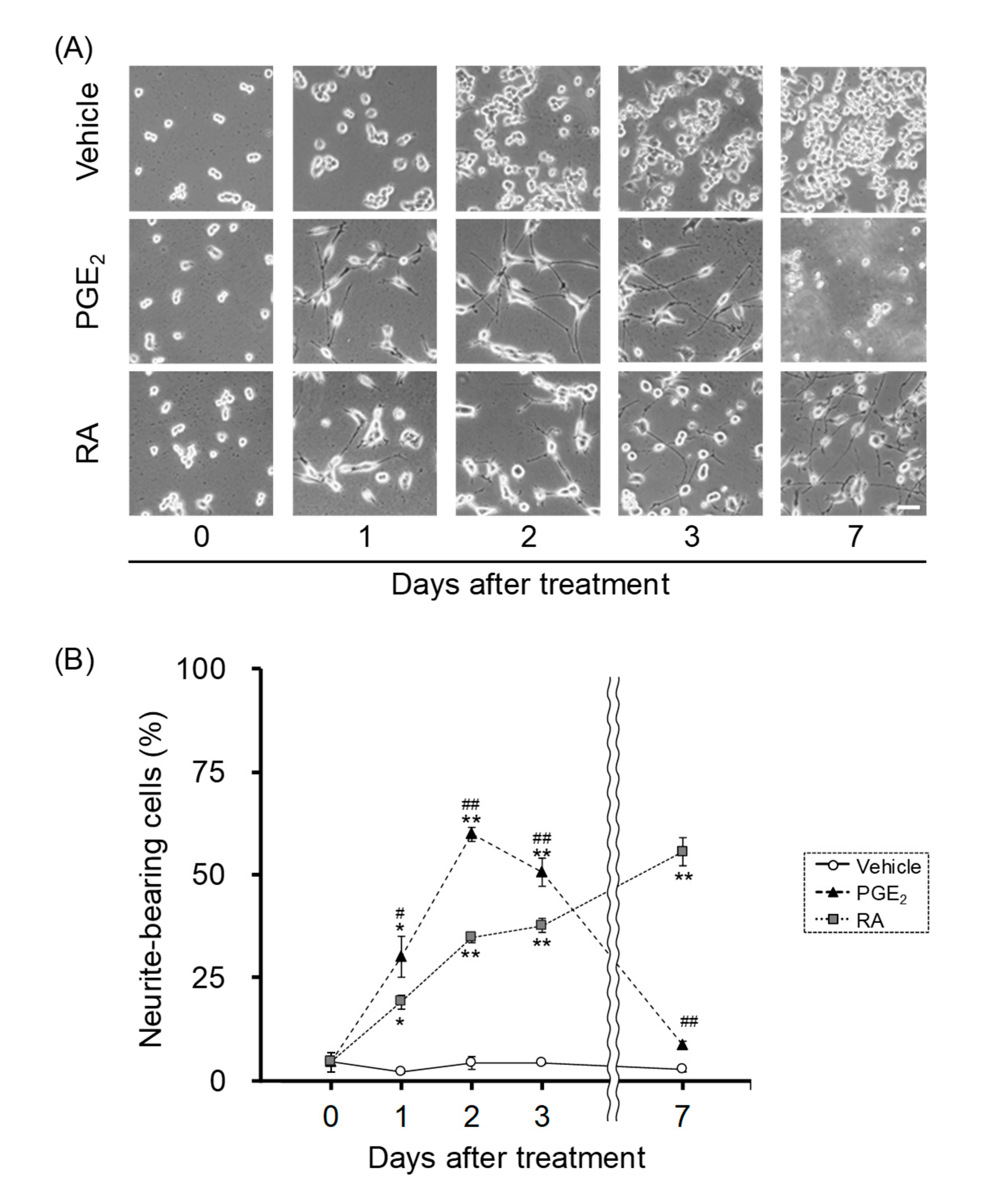
3.1. Effect of PGE2 and RA on Neurite Outgrowth
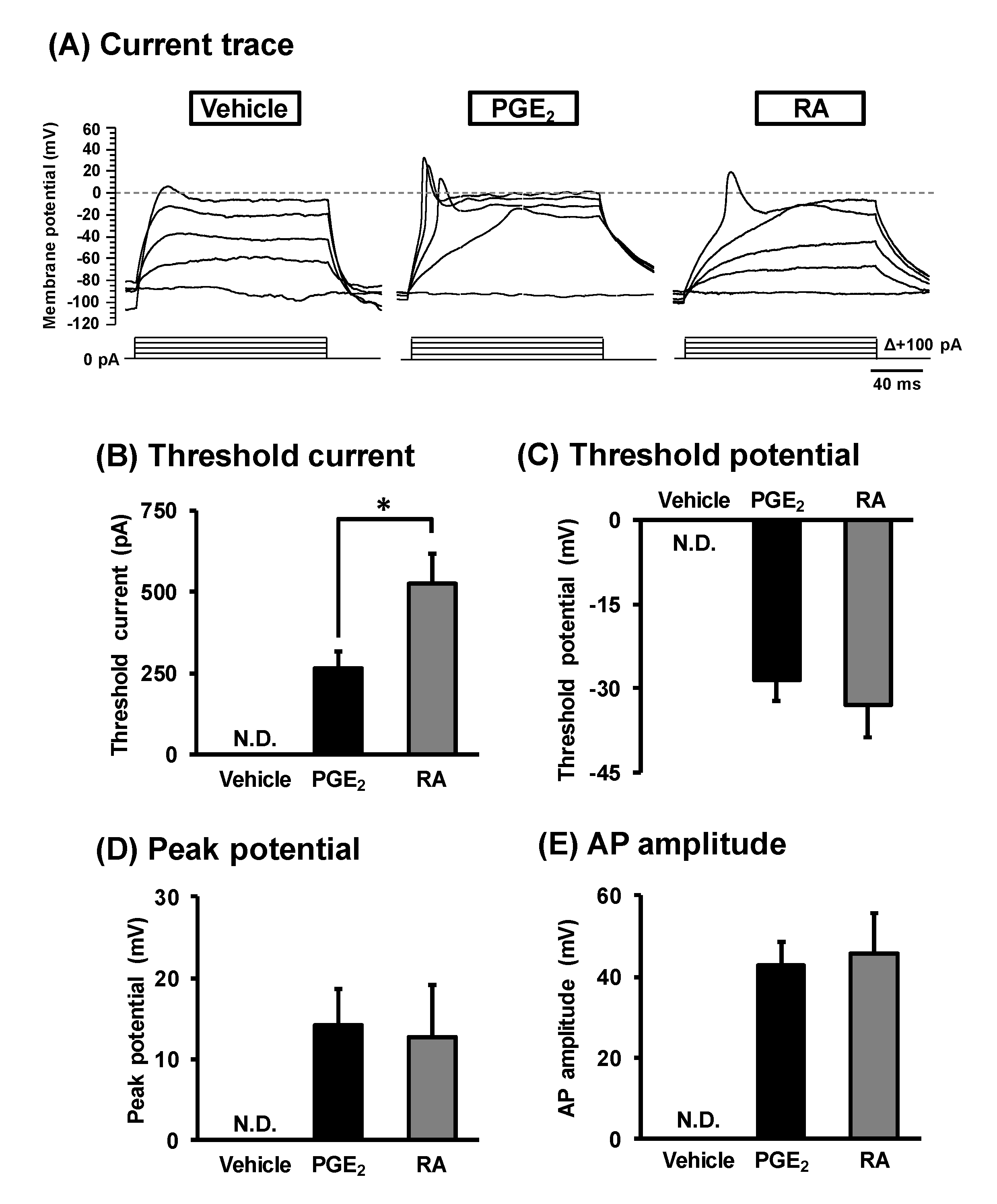
3.2. Action Potential Generation in Differentiated NSC-34 cells
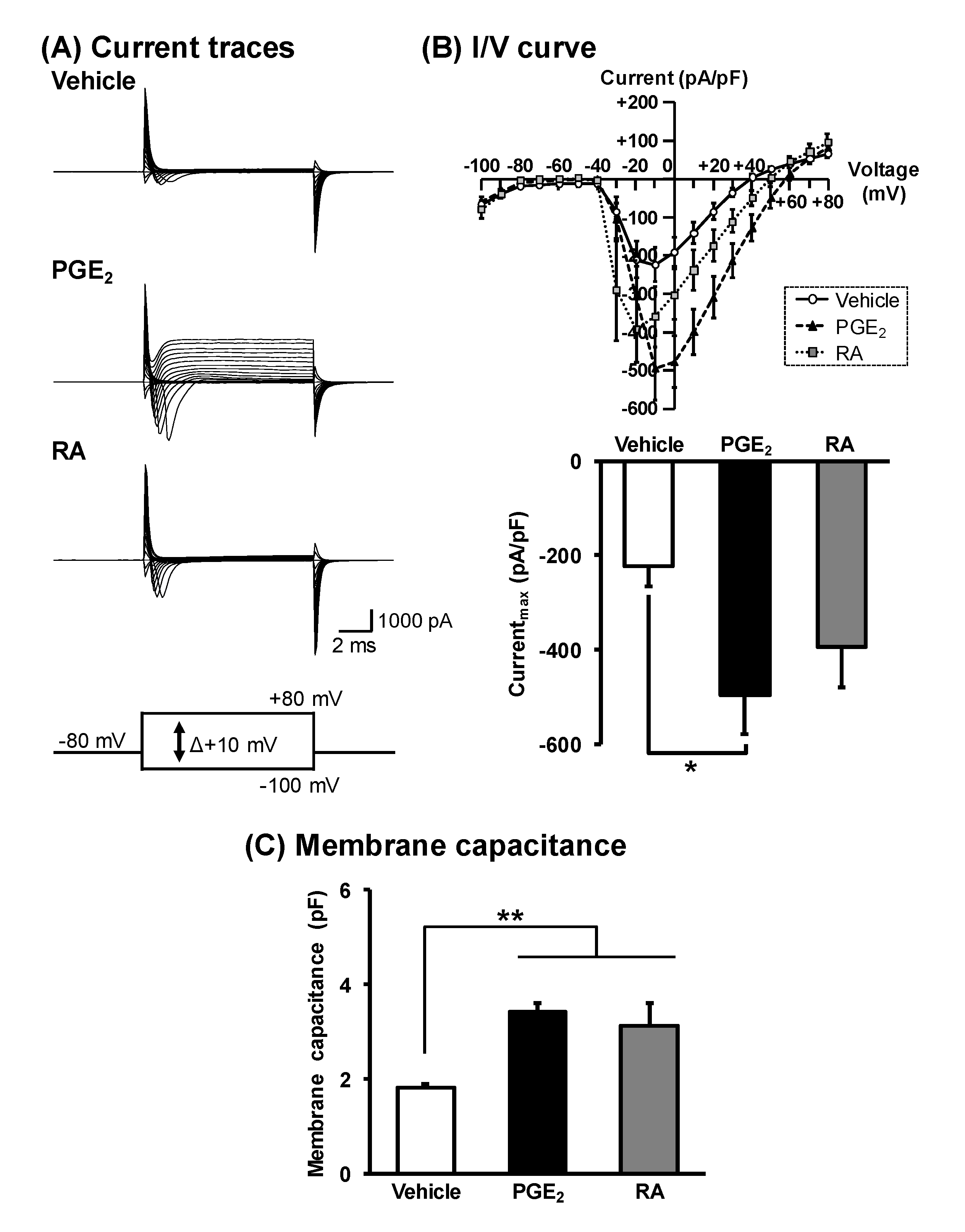
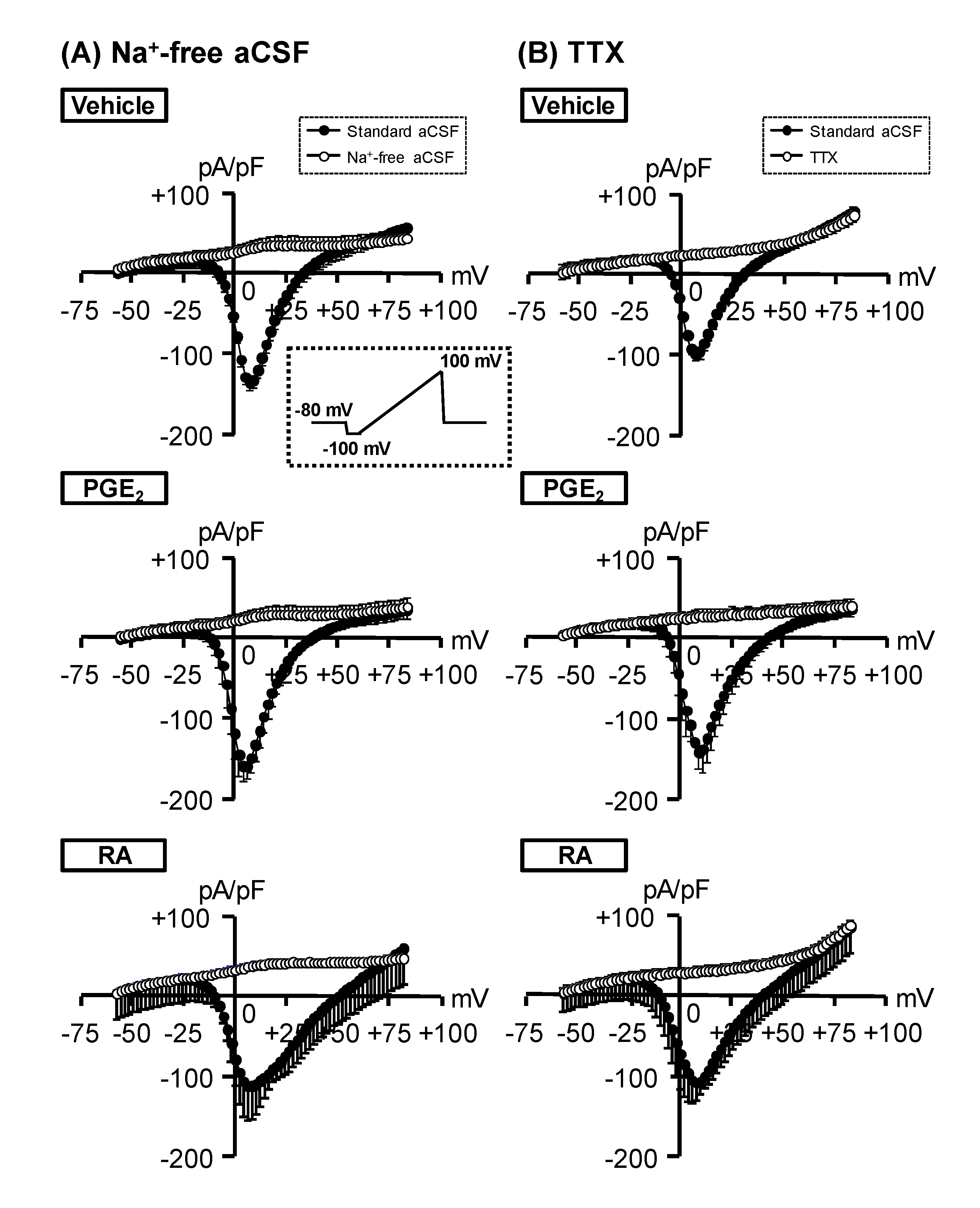
3.3. Characterization of Voltage-Dependent Inward Currents
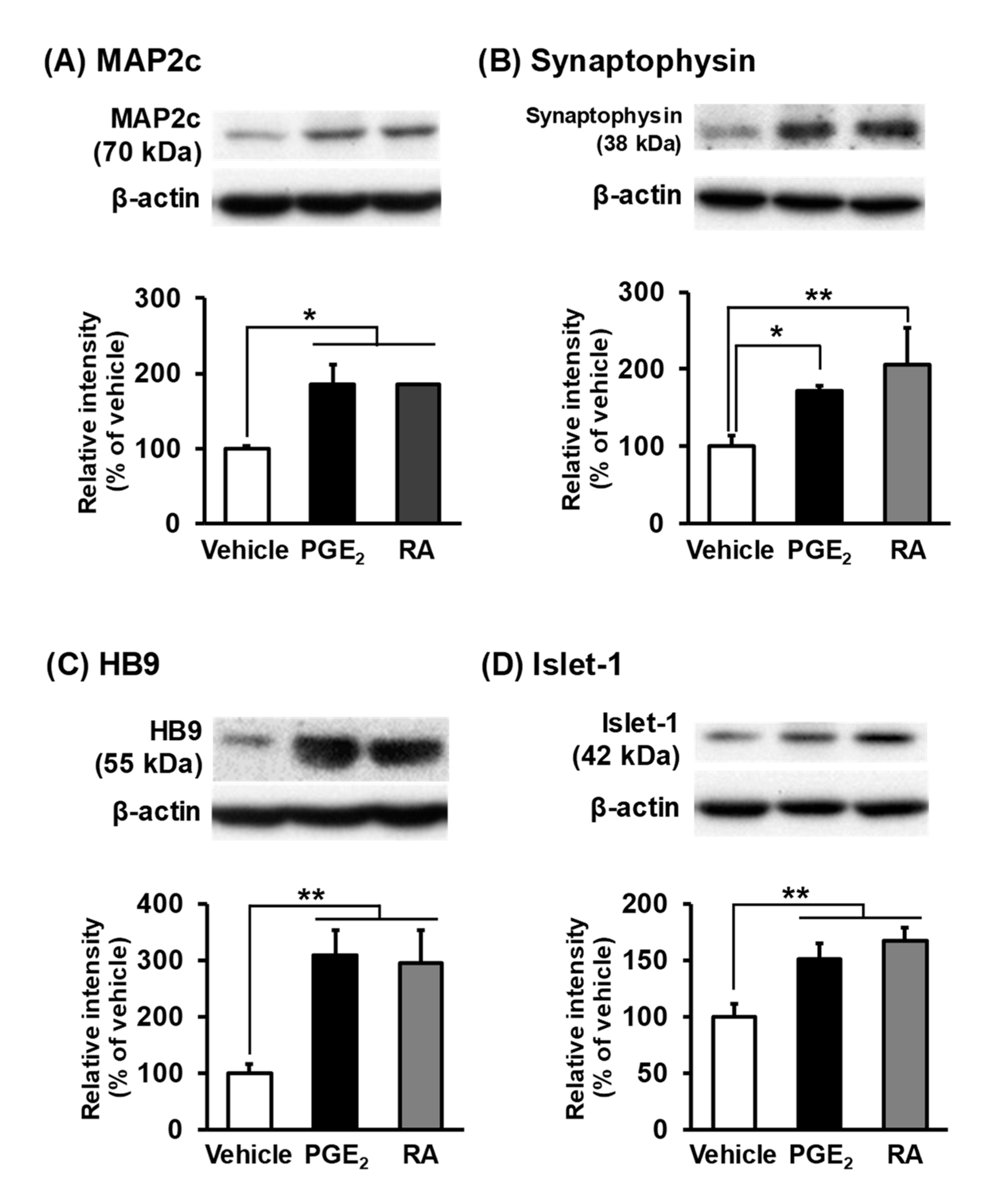
3.4. Expression of Neuronal Markers in PGE2- and RA-Differentiated cells
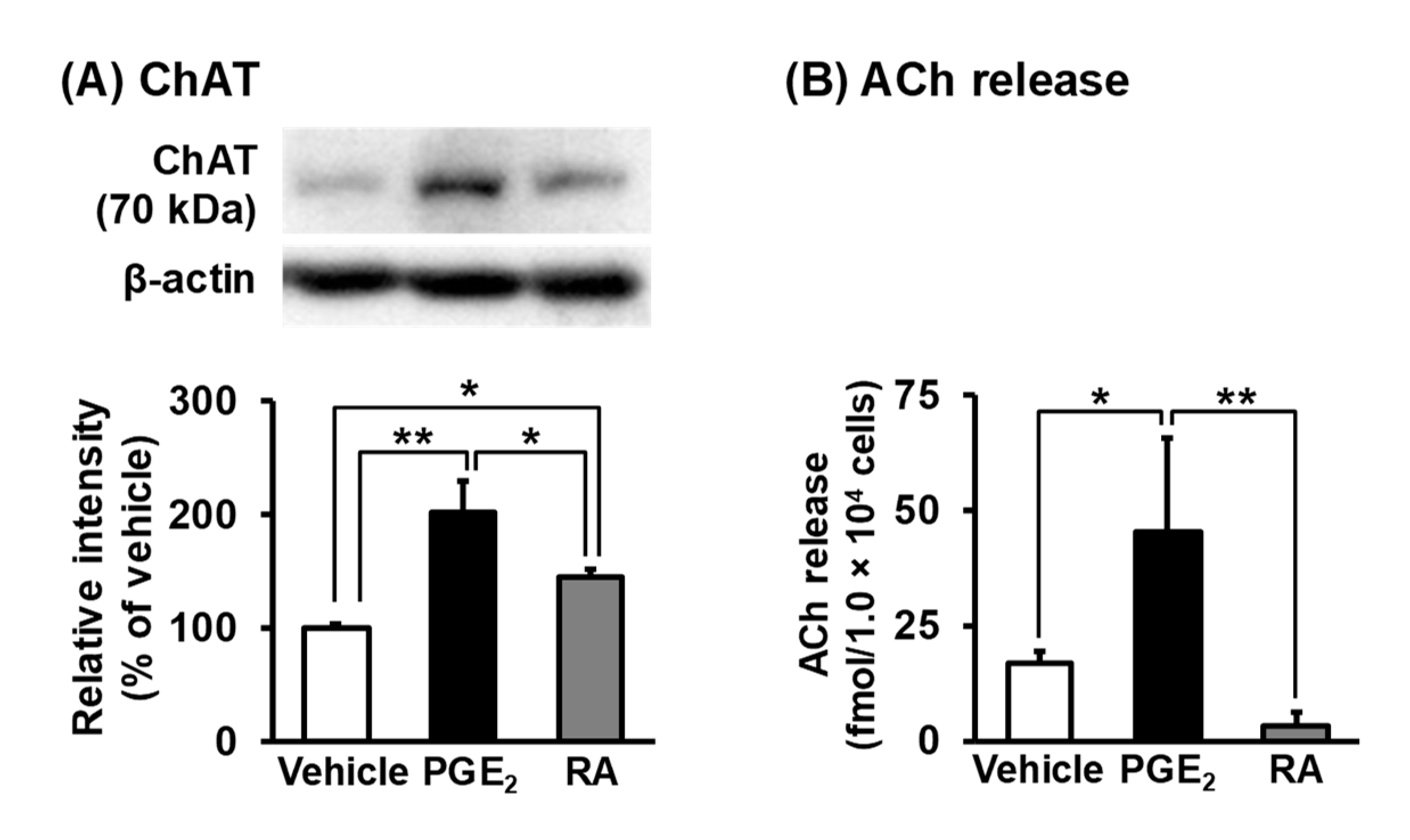
3.5. Synthesis and Release of ACh in NSC-34 Cells
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Stifani, N. Motor neurons and the generation of spinal motor neuron diversity. Front. Cell. Neurosci. 2014, 8, 1–22. [Google Scholar] [CrossRef] [PubMed]
- Tintignac, L.A.; Brenner, H.R.; Rüegg, M.A. Mechanisms regulating neuromuscular junction development and function and causes of muscle wasting. Physiol. Rev. 2015, 95, 809–852. [Google Scholar] [CrossRef] [PubMed]
- Beaudet, M.J.; Yang, Q.; Cadau, S.; Blais, M.; Bellenfant, S.; Gros-Louis, F.; Berthod, F. High yield extraction of pure spinal motor neurons, astrocytes and microglia from single embryo and adult mouse spinal cord. Sci. Rep. 2015, 5, 1–12. [Google Scholar] [CrossRef]
- Hounoum, B.M.; Vourc’h, P.; Felix, R.; Corcia, P.; Patin, F.; Guéguinou, M.; Potier-Cartereau, M.; Vandier, C.; Raoul, C.; Andres, C.R.; et al. NSC-34 motor neuron-like cells are unsuitable as experimental model for glutamate-mediated excitotoxicity. Front. Cell. Neurosci. 2016, 10, 1–9. [Google Scholar] [CrossRef]
- Mitra, P.; Brownstone, R.M. An in vitro spinal cord slice preparation for recording from lumbar motoneurons of the adult mouse. J. Neurophysiol. 2012, 107, 728–741. [Google Scholar] [CrossRef]
- Qu, Q.; Li, D.; Louis, K.R.; Li, X.; Yang, H.; Sun, Q.; Crandall, S.R.; Tsang, S.; Zhou, J.; Cox, C.L.; et al. High-efficiency motor neuron differentiation from human pluripotent stem cells and the function of Islet-1. Nat. Commun. 2014, 5, 3449. [Google Scholar] [CrossRef] [PubMed]
- Cashman, N.R.; Durham, H.D.; Blusztajn, J.K.; Oda, K.; Tabira, T.; Shaw, I.T.; Dahrouge, S.; Antel, J.P.; Durham, H.D.; Tabira, T.; et al. Neuroblastoma × spinal cord (NSC) hybrid cell lines resemble developing motor neurons. Dev. Dyn. 1992, 194, 209–221. [Google Scholar] [CrossRef]
- Jiang, J.X.S.; Choi, R.C.Y.; Siow, N.L.; Lee, H.H.C.; Wan, D.C.C.; Tsim, K.W.K. Muscle induces neuronal expression of acetylcholinesterase in neuron-muscle co-culture: Transcriptional regulation mediated by camp-dependent signaling. J. Biol. Chem. 2003, 278, 45435–45444. [Google Scholar] [CrossRef] [PubMed]
- Smith, R.G.; Alexianu, M.E.; Crawford, G.; Nyormoi, O.; Stefani, E.; Appel, S.H. Cytotoxicity of immunoglobulins from amyotrophic lateral sclerosis patients on a hybrid motoneuron cell line. Proc. Natl. Acad. Sci. USA 1994, 91, 3393–3397. [Google Scholar] [CrossRef] [PubMed]
- Maier, O.; Dahm, M.; Brück, S.; Johann, S.; Böhm, J.; Beyer, C.; Dahm, M.; Brück, S.; Beyer, C.; Johann, S.; et al. Differentiated NSC-34 motoneuron-like cells as experimental model for cholinergic neurodegeneration. Neurochem. Int. 2013, 62, 1029–1038. [Google Scholar] [CrossRef]
- Liu, X.; Xu, S.; Wang, P.; Wang, W. Transient mitochondrial permeability transition mediates excitotoxicity in glutamate-sensitive NSC34 D motor neuron-like cells. Exp. Neurol. 2015, 271, 122–130. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.H.; Choi, N.Y.; Yu, H.J.; Park, J.; Choi, H.; Lee, K.Y.; Huh, Y.M.; Lee, Y.J.; Koh, S.H. Atorvastatin protects NSC-34 motor neurons against oxidative stress by activating PI3K, ERK and free radical scavenging. Mol. Neurobiol. 2016, 53, 695–705. [Google Scholar] [CrossRef] [PubMed]
- Miyagishi, H.; Kosuge, Y.; Yoneoka, Y.; Ozone, M.; Endo, M.; Osada, N.; Ishige, K.; Kusama-Eguchi, K.; Ito, Y. Prostaglandin E2-Induced cell death is mediated by activation of EP2 receptors in motor neuron-like NSC-34 cells. J. Pharmacol. Sci. 2013, 121, 347–350. [Google Scholar] [CrossRef] [PubMed]
- Kosuge, Y.; Miyagishi, H.; Yoneoka, Y.; Yoneda, K.; Nango, H. Neurochemistry international pathophysiological role of prostaglandin E2-induced up-regulation of the EP2 receptor in motor neuron-like NSC-34 cells and lumbar motor neurons in ALS model mice. Neurochem. Int. 2017, 2–9. [Google Scholar] [CrossRef]
- Zhang, Y.; Desai, A.; Yang, S.Y.; Bae, K.B.; Antczak, M.I.; Fink, S.P.; Tiwari, S.; Willis, J.E.; Williams, N.S.; Dawson, D.M.; et al. Inhibition of the prostaglandin-degrading enzyme 15-PGDH potentiates tissue regeneration. Science 2015, 348, aaa2340. [Google Scholar] [CrossRef]
- Goncalves, M.B.; Williams, E.J.; Yip, P.; Yáñez-Muñoz, R.J.; Williams, G.; Doherty, P. The COX-2 inhibitors, meloxicam and nimesulide, suppress neurogenesis in the adult mouse brain. Br. J. Pharmacol. 2010, 159, 1118–1125. [Google Scholar] [CrossRef]
- Zaccai, T.C.F.; Savitzki, D.; Zivony-Elboum, Y.; Vilboux, T.; Fitts, E.C.; Shoval, Y.; Kalfon, L.; Samra, N.; Keren, Z.; Gross, B.; et al. Phospholipase A2-activating protein is associated with a novel form of leukoencephalopathy. Brain 2017, 140, 370–386. [Google Scholar] [CrossRef][Green Version]
- Kim, H.S.; Song, M.; Kim, E.; Ryu, S.H.; Suh, P.-G. Dexamethasone differentiates NG108-15 cells through cyclooxygenase 1 induction. Exp. Mol. Med. 2003, 35, 203–210. [Google Scholar] [CrossRef][Green Version]
- Mitani, K.; Sekiguchi, F.; Maeda, T.; Tanaka, Y.; Yoshida, S.; Kawabata, A. The prostaglandin E2/EP4 receptor/cyclic AMP/T-type Ca2+ channel pathway mediates neuritogenesis in sensory neuron-like ND7/23 cells. J. Pharmacol. Sci. 2016, 130, 177–180. [Google Scholar] [CrossRef]
- Nango, H.; Kosuge, Y.; Miyagishi, H.; Sugawa, K.; Ito, Y.; Ishige, K. Prostaglandin E2 facilitates neurite outgrowth in a motor neuron-like cell line, NSC-34. J. Pharmacol. Sci. 2017, 135, 64–71. [Google Scholar] [CrossRef]
- Johann, S.; Dahm, M.; Kipp, M.; Zahn, U.; Beyer, C. Regulation of choline acetyltransferase expression by 17β-oestradiol in NSC-34 cells and in the spinal cord. J. Neuroendocrinol. 2011, 23, 839–848. [Google Scholar] [CrossRef] [PubMed]
- Nango, H.; Kosuge, Y.; Yoshimura, N.; Miyagishi, H.; Kanazawa, T.; Hashizaki, K.; Suzuki, T.; Ishige, K. The molecular mechanisms underlying prostaglandin D2-Induced neuritogenesis in motor neuron-like NSC-34 cells. Cells 2020, 9, 934. [Google Scholar] [CrossRef] [PubMed]
- Kosuge, Y.; Nango, H.; Kasai, H.; Yanagi, T.; Mawatari, T.; Nishiyama, K.; Miyagishi, H.; Ishige, K.; Ito, Y.; Fischer, R. Generation of cellular reactive oxygen species by activation of the EP2 receptor contributes to prostaglandin E2-induced cytotoxicity in motor neuron-like NSC-34 cells. Oxid. Med. Cell. Longev. 2020, 2020. [Google Scholar] [CrossRef] [PubMed]
- Shiozaki, Y.; Sato, M.; Kimura, M.; Sato, T.; Tazaki, M.; Shibukawa, Y. Ionotropic P2X ATP receptor channels mediate purinergic signaling in mouse odontoblasts. Front. Physiol. 2017, 8, 1–10. [Google Scholar] [CrossRef]
- Auld, D.S.; Day, J.C.; Mennicken, F.; Quirion, R. Pharmacological characterization of endogenous acetylcholine release from primary septal cultures. J. Pharmacol. Exp. Ther. 2000, 292, 692–697. [Google Scholar]
- Kiguchi, Y.; Aono, Y.; Watanabe, Y.; Yamamoto-Nemoto, S.; Shimizu, K.; Shimizu, T.; Kosuge, Y.; Waddington, J.L.; Ishige, K.; Ito, Y.; et al. In vivo neurochemical evidence that delta1-, delta2- and mu2-opioid receptors, but not mu1-opioid receptors, inhibit acetylcholine efflux in the nucleus accumbens of freely moving rats. Eur. J. Pharmacol. 2016, 789, 402–410. [Google Scholar] [CrossRef]
- Castro-Obregón, S.; Covarrubias, L. Role of retinoic acid and oxidative stress in embryonic stem cell death and neuronal differentiation. FEBS Lett. 1996, 381, 93–97. [Google Scholar] [CrossRef]
- Cunningham, T.J.; Duester, G. Mechanisms of retinoic acid signalling and its roles in organ and limb development. Nat. Rev. Mol. Cell Biol. 2015, 16, 110–123. [Google Scholar] [CrossRef]
- Liu, J.; Tu, H.; Zhang, D.; Zheng, H.; Li, Y.L. Voltage-gated sodium channel expression and action potential generation in differentiated NG108-15 cells. BMC Neurosci. 2012, 13. [Google Scholar] [CrossRef]
- Hu, R.; Cao, Q.; Sun, Z.; Chen, J.; Zheng, Q.; Xiao, F. A novel method of neural differentiation of PC12 cells by using Opti-MEM as a basic induction medium. Int. J. Mol. Med. 2018, 41, 195–201. [Google Scholar] [CrossRef] [PubMed]
- Catterall, W.A.; Goldin, A.L.; Waxman, S.G. International Union of Pharmacology. XLVII. Nomenclature and structure-function relationships of voltage-gated sodium channels. Pharmacol. Rev. 2005, 57, 397–409. [Google Scholar] [CrossRef] [PubMed]
- Kole, M.H.P.P.; Ilschner, S.U.; Kampa, B.M.; Williams, S.R.; Ruben, P.C.; Stuart, G.J. Action potential generation requires a high sodium channel density in the axon initial segment. Nat. Neurosci. 2008, 11, 178–186. [Google Scholar] [CrossRef]
- Novitch, B.G.; Wichterle, H.; Jessell, T.M.; Sockanathan, S. A requirement for retinoic acid-mediated transcriptional activation in ventral neural patterning and motor neuron specification. Neuron 2003, 40, 81–95. [Google Scholar] [CrossRef]
- Shimojo, D.; Onodera, K.; Doi-Torii, Y.; Ishihara, Y.; Hattori, C.; Miwa, Y.; Tanaka, S.; Okada, R.; Ohyama, M.; Shoji, M.; et al. Rapid, efficient, and simple motor neuron differentiation from human pluripotent stem cells. Mol. Brain 2015, 8, 1–15. [Google Scholar] [CrossRef]
- Petrozziello, T.; Secondo, A.; Tedeschi, V.; Esposito, A.; Sisalli, M.J.; Scorziello, A.; Di Renzo, G.; Annunziato, L. ApoSOD1 lacking dismutase activity neuroprotects motor neurons exposed to beta-methylamino-L-alanine through the Ca2+/Akt/ERK1/2 prosurvival pathway. Cell Death Differ. 2017, 24, 511–522. [Google Scholar] [CrossRef] [PubMed]
- Davis-Dusenbery, B.N.; Williams, L.A.; Klim, J.R.; Eggan, K. How to make spinal motor neurons. Development 2014, 141, 491–501. [Google Scholar] [CrossRef]
- Arumugam, S.; Garcera, A.; Soler, R.M.; Tabares, L. Smn-deficiency increases the intrinsic excitability of motoneurons. Front. Cell. Neurosci. 2017, 11, 1–13. [Google Scholar] [CrossRef] [PubMed]
- VanderWall, K.B.; Vij, R.; Ohlemacher, S.K.; Sridhar, A.; Fligor, C.M.; Feder, E.M.; Edler, M.C.; Baucum, A.J.; Cummins, T.R.; Meyer, J.S. Astrocytes regulate the development and maturation of retinal ganglion cells derived from human pluripotent stem cells. Stem Cell Rep. 2019, 12, 201–212. [Google Scholar] [CrossRef]
- Calder, E.L.; Tchieu, J.; Steinbeck, J.A.; Tu, E.; Keros, S.; Ying, S.W.; Jaiswal, M.K.; Cornacchia, D.; Goldstein, P.A.; Tabar, V.; et al. Retinoic acid-mediated regulation of GLI3 enables efficient motoneuron derivation from human ESCs in the absence of extrinsic SHH activation. J. Neurosci. 2015, 35, 11462–11481. [Google Scholar] [CrossRef]
- Dehmelt, L.; Smart, F.M.; Ozer, R.S.; Halpain, S. The role of microtubule-associated protein 2c in the reorganization of microtubules and lamellipodia during neurite initiation. J. Neurosci. 2003, 23, 9479–9490. [Google Scholar] [CrossRef]
- Lieven, C.J.; Millet, L.E.; Hoegger, M.J.; Levin, L.A. Induction of axon and dendrite formation during early RGC-5 cell differentiation. Exp. Eye Res. 2007, 85, 678–683. [Google Scholar] [CrossRef] [PubMed]
- Valtorta, F.; Tarelli, F.T.; Campanati, L.; Villa, A.; Greengard, P. Synaptophysin and synapsin I as tools for the study of the exo-endocytotic cycle. Cell Biol. Int. Rep. 1989, 13, 1023–1038. [Google Scholar] [CrossRef]
- Alder, J.; Kanki, H.; Valtorta, F.; Greengard, P.; Poo, M.M. Overexpression of synaptophysin enhances neurotransmitter secretion at Xenopus neuromuscular synapses. J. Neurosci. 1995, 15, 511–519. [Google Scholar] [CrossRef]
- Ericson, J.; Thor, S.; Edlund, T.; Jessell, T.M.; Yamada, T. Early stages of motor neuron differentiation revealed by expression of homeobox gene Islet-1. Science 1992, 256, 1555–1560. [Google Scholar] [CrossRef] [PubMed]
- Arber, S.; Han, B.; Mendelsohn, M.; Smith, M.; Jessell, T.M.; Sockanathan, S. Requirement for the homeobox gene Hb9 in the consolidation of motor neuron identity. Neuron 1999, 23, 659–674. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nango, H.; Kosuge, Y.; Sato, M.; Shibukawa, Y.; Aono, Y.; Saigusa, T.; Ito, Y.; Ishige, K. Highly Efficient Conversion of Motor Neuron-Like NSC-34 Cells into Functional Motor Neurons by Prostaglandin E2. Cells 2020, 9, 1741. https://doi.org/10.3390/cells9071741
Nango H, Kosuge Y, Sato M, Shibukawa Y, Aono Y, Saigusa T, Ito Y, Ishige K. Highly Efficient Conversion of Motor Neuron-Like NSC-34 Cells into Functional Motor Neurons by Prostaglandin E2. Cells. 2020; 9(7):1741. https://doi.org/10.3390/cells9071741
Chicago/Turabian StyleNango, Hiroshi, Yasuhiro Kosuge, Masaki Sato, Yoshiyuki Shibukawa, Yuri Aono, Tadashi Saigusa, Yoshihisa Ito, and Kumiko Ishige. 2020. "Highly Efficient Conversion of Motor Neuron-Like NSC-34 Cells into Functional Motor Neurons by Prostaglandin E2" Cells 9, no. 7: 1741. https://doi.org/10.3390/cells9071741
APA StyleNango, H., Kosuge, Y., Sato, M., Shibukawa, Y., Aono, Y., Saigusa, T., Ito, Y., & Ishige, K. (2020). Highly Efficient Conversion of Motor Neuron-Like NSC-34 Cells into Functional Motor Neurons by Prostaglandin E2. Cells, 9(7), 1741. https://doi.org/10.3390/cells9071741




