The Art of Mast Cell Adhesion
Abstract
1. Introduction
2. Mast Cells
3. Mast Cell Adhesion Receptors
3.1. Immunoglobulin Superfamily Cell Adhesion Molecules (IgSF CAMs)
3.2. Integrins
3.3. Selectins
3.4. Cadherins
4. Mast Cells and Extracellular Matrix
5. Mast Cells and Intercellular Junctions
6. Adhesion Related Signaling Pathways
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Curtis, A.S.G. Cell adhesion. Prog. Biophys. Mol. Biol. 1973, 27, 315–385. [Google Scholar] [CrossRef]
- Horwitz, A.R. The origins of the molecular era of adhesion research. Nat. Rev. Mol. Cell Biol. 2012, 13, 805–811. [Google Scholar] [CrossRef] [PubMed]
- Okegawa, T.; Pong, R.-C.; Li, Y.; Hsieh, J.-T. The role of cell adhesion molecule in cancer progression and its application in cancer therapy. Acta Biochim. Pol. 2004, 51, 445–457. [Google Scholar] [CrossRef] [PubMed]
- Gumbiner, B.M. Cell Adhesion: The Molecular Basis of Tissue Architecture and Morphogenesis. Cell 1996, 84, 345–357. [Google Scholar] [CrossRef]
- Bendas, G.; Borsig, L. Cancer cell adhesion and metastasis: Selectins, integrins, and the inhibitory potential of heparins. Int. J. Cell Biol. 2012, 2012, 676731. [Google Scholar] [CrossRef] [PubMed]
- Pizarro-Cerdá, J.; Cossart, P. Bacterial Adhesion and Entry into Host Cells. Cell 2006, 124, 715–727. [Google Scholar] [CrossRef] [PubMed]
- Mateo, M.; Generous, A.; Sinn, P.L.; Cattaneo, R. Connections matter - How viruses use cell-cell adhesion components. J. Cell Sci. 2015, 128, 431–439. [Google Scholar] [CrossRef]
- Harris, E.S.; Weyrich, A.S.; Zimmerman, G.A. Lessons from rare maladies: Leukocyte adhesion deficiency syndromes. Curr. Opin. Hematol. 2013, 20, 16–25. [Google Scholar] [CrossRef]
- Hanna, S.; Etzioni, A. Leukocyte adhesion deficiencies. Ann. N. Y. Acad. Sci. 2012, 1250, 50–55. [Google Scholar] [CrossRef]
- Okayama, Y.; Kawakami, T. Development, Migration, and Survival of Mast Cells. Immunol. Res. 2006, 34, 97–116. [Google Scholar] [CrossRef]
- Krystel-Whittemore, M.; Dileepan, K.N.; Wood, J.G. Mast Cell: A Multi-Functional Master Cell. Front. Immunol. 2016, 6, 620. [Google Scholar] [CrossRef] [PubMed]
- Pastwińska, J.; Walczak-Drzewiecka, A.; Łukasiak, M.; Ratajewski, M.; Dastych, J. Hypoxia regulates human mast cell adhesion to fibronectin via the PI3K/AKT signaling pathway. Cell Adhes. Migr. 2020, 14, 106–117. [Google Scholar] [CrossRef] [PubMed]
- Dastych, J.; Metcalfe, D.D. Stem cell factor induces mast cell adhesion to fibronectin. J. Immunol. 1994, 152, 213–219. [Google Scholar] [PubMed]
- Abel, M.; Vliagoftis, H. Mast Cell-Fibroblast Interactions Induce Matrix Metalloproteinase-9 Release from Fibroblasts: Role for IgE-Mediated Mast Cell Activation. J. Immunol. 2008, 180, 3543–3550. [Google Scholar] [CrossRef] [PubMed]
- Gurish, M.F.; Tao, H.; Abonia, J.P.; Arya, A.; Friend, D.S.; Parker, C.M.; Austen, K.F. Intestinal Mast Cell Progenitors Require CD49dβ7 (α4β7 Integrin) for Tissue-specific Homing. J. Exp. Med. 2001, 194, 1243–1252. [Google Scholar] [CrossRef] [PubMed]
- Collington, S.J.; Williams, T.J.; Weller, C.L. Mechanisms underlying the localisation of mast cells in tissues. Trends Immunol. 2011, 32, 478–485. [Google Scholar] [CrossRef]
- Hamawy, M.M.; Oliver, C.; Mergenhagen, E.S.; Siraganian, R.P. Adherence of rat basophilic leukemia (RBL-2H3) cells to fibronectin-coated surfaces enhances secretion. J. Immunol. 1992, 149, 615–621. [Google Scholar]
- Hamawy, M.M.; Mergenhagen, S.E.; Siraganian, R.P. Adhesion molecules as regulators of mast-cell and basophil function. Immunol. Today 1994, 15, 62–66. [Google Scholar] [CrossRef]
- Valent, P.; Bevec, D.; Maurer, D.; Besemer, J.; Di Padova, F.; Butterfield, J.H.; Speiser, W.; Majdic, O.; Lechner, K.; Bettelheim, P. Interleukin 4 promotes expression of mast cell ICAM-1 antigen. Proc. Natl. Acad. Sci. USA 1991, 88, 3339–3342. [Google Scholar] [CrossRef]
- Toru, H.; Kinashi, T.; Ra, C.; Nonoyama, S.; Yata, J.-I.; Nakahata, T. Interleukin-4 Induces Homotypic Aggregation of Human Mast Cells by Promoting LFA-1/ICAM-1 Adhesion Molecules. Blood 1997, 89, 3296–3302. [Google Scholar] [CrossRef]
- Wedi, B.; Elsner, J.; Czech, W.; Butterfield, J.H.; Kapp, A. Modulation of intercellular adhesion molecule 1 (ICAM-1) expression on the human mast-cell line (HMC)-1 by inflammatory mediators. Allergy 1996, 51, 676–684. [Google Scholar] [CrossRef]
- Babina, M.; Mammeri, K.; Henz, B.M. ICAM-3 (CD50) is expressed by human mast cells: Induction of homotypic mast cell aggregation via ICAM-3. Cell Adhes. Commun. 1999, 7, 195–209. [Google Scholar] [CrossRef] [PubMed]
- Babina, M.; Krautheim, M.; Grützkau, A.; Henz, B.M. Human Leukemic (HMC-1) Mast Cells Are Responsive to 1α,25-Dihydroxyvitamin D3: Selective Promotion of ICAM-3 Expression and Constitutive Presence of Vitamin D3 Receptor. Biochem. Biophys. Res. Commun. 2000, 273, 1104–1110. [Google Scholar] [CrossRef] [PubMed]
- Boyce, J.A.; Mellor, E.A.; Perkins, B.; Lim, Y.-C.; Luscinskas, F.W. Human mast cell progenitors use α4-integrin, VCAM-1, and PSGL-1 E-selectin for adhesive interactions with human vascular endothelium under flow conditions. Blood 2002, 99, 2890–2896. [Google Scholar] [CrossRef]
- Dudeck, A.; Leist, M.; Rubant, S.; Zimmermann, A.; Dudeck, J.; Boehncke, W.H.; Maurer, M. Immature mast cells exhibit rolling and adhesion to endothelial cells and subsequent diapedesis triggered by E- and P-selectin, VCAM-1 and PECAM-1. Exp. Dermatol. 2010, 19, 424–434. [Google Scholar] [CrossRef]
- Krüger-Krasagakes, S.; Grützkau, A.; Baghramian, R.; Henz, B.M. Interactions of Immature Human Mast Cells with Extracellular Matrix: Expression of Specific Adhesion Receptors and Their Role in Cell Binding to Matrix Proteins. J. Investig. Dermatol. 1996, 106, 538–543. [Google Scholar] [CrossRef][Green Version]
- Rosbottom, A.; Scudamore, C.L.; Von Der Mark, H.; Thornton, E.M.; Wright, S.H.; Miller, H.R.P. TGF-β1 Regulates Adhesion of Mucosal Mast Cell Homologues to Laminin-1 Through Expression of Integrin α7. J. Immunol. 2002, 169, 5689–5695. [Google Scholar] [CrossRef]
- Columbo, M.; Bochner, B.S.; Marone, G. Human skin mast cells express functional beta 1 integrins that mediate adhesion to extracellular matrix proteins. J. Immunol. 1995, 154, 6058–6064. [Google Scholar]
- Abonia, J.P.; Hallgren, J.; Jones, T.; Shi, T.; Xu, Y.; Koni, P.; Flavell, R.A.; Boyce, J.A.; Austen, K.F.; Gurish, M.F. Alpha-4 integrins and VCAM-1, but not MAdCAM-1, are essential for recruitment of mast cell progenitors to the inflamed lung. Blood 2006, 108, 1588–1594. [Google Scholar] [CrossRef]
- Ra, C.; Yasuda, M.; Yagita, H.; Okumura, K. Fibronectin receptor integrins are involved in mast cell activation. J. Allergy Clin. Immunol. 1994, 94, 625–628. [Google Scholar] [CrossRef]
- Artis, D.; Humphreys, N.E.; Potten, C.S.; Wagner, N.; Müller, W.; McDermott, J.R.; Grencis, R.K.; Else, K.J. Beta7 integrin-deficient mice: Delayed leukocyte recruitment and attenuated protective immunity in the small intestine during enteric helminth infection. Eur. J. Immunol. 2000, 30, 1656–1664. [Google Scholar] [CrossRef]
- Fehlner-Gardiner, C.C.; Uniyal, S.; Chan, B.M.C. Integrin VLA-6 (alpha6beta1) is transiently expressed during the development of mouse bone marrow-derived mast cells. Dev. Growth Differ. 1996, 38, 673–686. [Google Scholar] [CrossRef]
- Berlanga, O.; Emambokus, N.; Frampton, J. GPIIb (CD41) integrin is expressed on mast cells and influences their adhesion properties. Exp. Hematol. 2005, 33, 403–412. [Google Scholar] [CrossRef] [PubMed]
- Oki, T.; Kitaura, J.; Eto, K.; Lu, Y.; Maeda-Yamamoto, M.; Inagaki, N.; Nagai, H.; Yamanishi, Y.; Nakajina, H.; Kumagai, H.; et al. Integrin αIIbβ3 Induces the Adhesion and Activation of Mast Cells through Interaction with Fibrinogen. J. Immunol. 2005, 176, 52–60. [Google Scholar] [CrossRef]
- Tegoshi, T.; Nishida, M.; Arizono, N. Expression and role of E-cadherin and CD103beta7 (alphaEbeta7 integrin) on cultured mucosal-type mast cells. APMIS 2005, 113, 91–98. [Google Scholar] [CrossRef]
- Weber, S.; Babina, M.; Feller, G.; Henz, B.M. Human Leukaemic (HMC-1) and Normal Skin Mast Cells Express β2-Integrins: Characterization of β2-Integrins and ICAM-1 on HMC-1 Cells. Scand. J. Immunol. 1997, 45, 471–481. [Google Scholar] [CrossRef]
- Küchler, J.; Grützkau, A.; Henz, B.M.; Krüger-Krasagakis, S. Morphological analysis of integrin-mediated adhesion of immature human mast cells to extracellular matrix proteins. Arch. Dermatol. Res. 2006, 298, 153–161. [Google Scholar] [CrossRef]
- Sugimoto, K.; Kudo, M.; Sundaram, A.; Ren, X.; Huang, K.; Bernstein, X.; Wang, Y.; Raymond, W.W.; Erle, D.J.; Åbrink, M.; et al. The αvβ6 integrin modulates airway hyperresponsiveness in mice by regulating intraepithelial mast cells. J. Clin. Investig. 2012, 122, 748–758. [Google Scholar] [CrossRef]
- Kaburagi, Y.; Hasegawa, M.; Nagaoka, T.; Shimada, Y.; Hamaguchi, Y.; Komura, K.; Saito, E.; Yanaba, K.; Takehara, K.; Kadono, T.; et al. The cutaneous reverse Arthus reaction requires intercellular adhesion molecule 1 and L-selectin expression. J. Immunol. 2002, 168, 2970–2978. [Google Scholar] [CrossRef]
- Nishida, M.; Kawai, K.; Tanaka, M.; Tegoshi, T.; Arizono, N. Expression of E-cadherin in human mast cell line HMC-1. APMIS 2003, 111, 1067–1074. [Google Scholar] [CrossRef]
- Tegoshi, T.; Nishida, M.; Ishiwata, K.; Kobayashi, T.; Uchiyama, F.; Nabeshima, K.; Nawa, Y.; Arizono, N. E-cadherin and cadherin-associated cytoplasmic proteins are expressed in murine mast cells. Lab. Invest. 2000, 80, 1571–1581. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Moon, T.C.; Befus, A.D.; Kulka, M. Mast Cell Mediators: Their Differential Release and the Secretory Pathways Involved. Front. Immunol. 2014, 5, 569. [Google Scholar] [CrossRef] [PubMed]
- Mukai, K.; Tsai, M.; Saito, H.; Galli, S.J. Mast cells as sources of cytokines, chemokines, and growth factors. Immunol. Rev. 2018, 282, 121–150. [Google Scholar] [CrossRef] [PubMed]
- Olivera, A.; Beaven, M.A.; Metcalfe, D.D. Mast cells signal their importance in health and disease. J. Allergy Clin. Immunol. 2018, 142, 381–393. [Google Scholar] [CrossRef] [PubMed]
- Dawicki, W.; Marshall, J.S. New and emerging roles for mast cells in host defence. Curr. Opin. Immunol. 2007, 19, 31–38. [Google Scholar] [CrossRef]
- Gilfillan, A.M.; Beaven, M.A. Regulation of Mast Cell Responses in Health and Disease. Crit. Rev. Immunol. 2011, 31, 475–530. [Google Scholar] [CrossRef]
- Pastwińska, J.; Agier, J.; Dastych, J.; Brzezińska-Błaszczyk, E. Mast cells as the strength of the inflammatory process. Pol. J. Pathol. 2017, 68, 187–196. [Google Scholar] [CrossRef]
- Żelechowska, P.; Agier, J.; Kozłowska, E.; Brzezińska-Błaszczyk, E. Mast cells participate in chronic low-grade inflammation within adipose tissue. Obes. Rev. 2018, 19, 686–697. [Google Scholar] [CrossRef]
- Sismanopoulos, N.; Delivanis, D.-A.; Alysandratos, K.-D.; Angelidou, A.; Therianou, A.; Kalogeromitros, D.; Theoharides, T.C. Mast cells in allergic and inflammatory diseases. Curr. Pharm. Des. 2012, 18, 2261–2277. [Google Scholar] [CrossRef]
- Malbec, O.; Daëron, M. The mast cell IgG receptors and their roles in tissue inflammation. Immunol. Rev. 2007, 217, 206–221. [Google Scholar] [CrossRef]
- Migalovich-Sheikhet, H.; Friedman, S.; Mankuta, D.; Levi-Schaffer, F. Novel Identified Receptors on Mast Cells. Front. Immunol. 2012, 3, 238. [Google Scholar] [CrossRef] [PubMed]
- Agier, J.; Różalska, S.; Wódz, K.; Brzezińska-Błaszczyk, E. Leukotriene receptor expression in mast cells is affected by their agonists. Cell. Immunol. 2017, 317, 37–47. [Google Scholar] [CrossRef] [PubMed]
- Thangam, E.B.; Jemima, E.A.; Singh, H.; Baig, M.S.; Khan, M.; Mathias, C.B.; Church, M.K.; Saluja, R. The Role of Histamine and Histamine Receptors in Mast Cell-Mediated Allergy and Inflammation: The Hunt for New Therapeutic Targets. Front. Immunol. 2018, 9, 1873. [Google Scholar] [CrossRef] [PubMed]
- Agier, J.; Żelechowska, P.; Kozłowska, E.; Brzezińska-Błaszczyk, E. Expression of surface and intracellular Toll-like receptors by mature mast cells. Central Eur. J. Immunol. 2016, 41, 333–338. [Google Scholar] [CrossRef]
- Bąbolewska, E.; Brzezińska-Błaszczyk, E. [Mast cell inhibitory receptors]. Postępy Hig. Med. Dośw. 2012, 66, 739–751. [Google Scholar] [CrossRef]
- Ramos, T.N.; Bullard, D.C.; Barnum, S.R. ICAM-1: Isoforms and Phenotypes. J. Immunol. 2014, 192, 4469–4474. [Google Scholar] [CrossRef]
- Zhong, X.; Drgonova, J.; Li, C.-Y.; Uhl, G.R. Human cell adhesion molecules: Annotated functional subtypes and overrepresentation of addiction-associated genes. Ann. N. Y. Acad. Sci. 2015, 1349, 83–95. [Google Scholar] [CrossRef]
- Kong, D.-H.; Kim, Y.K.; Kim, M.R.; Jang, J.H.; Lee, S. Emerging Roles of Vascular Cell Adhesion Molecule-1 (VCAM-1) in Immunological Disorders and Cancer. Int. J. Mol. Sci. 2018, 19, 1057. [Google Scholar] [CrossRef]
- Fong, S.; Jones, S.; Renz, M.E.; Chiu, H.H.; Ryan, A.M.; Presta, L.G.; Jackson, D. Mucosal addressin cell adhesion molecule-1 (MAdCAM-1). Immunol. Res. 1997, 16, 299–311. [Google Scholar] [CrossRef]
- Ghannadan, M.; Baghestanian, M.; Wimazal, F.; Eisenmenger, M.; Latal, D.; Kargül, G.; Walchshofer, S.; Sillaber, C.; Lechner, K.; Valent, P. Phenotypic Characterization of Human Skin Mast Cells by Combined Staining with Toluidine Blue and CD Antibodies. J. Investig. Dermatol. 1998, 111, 689–695. [Google Scholar] [CrossRef]
- Wong, M.-X.; Roberts, D.; Bartley, P.A.; Jackson, D.E. Absence of Platelet Endothelial Cell Adhesion Molecule-1 (CD31) Leads to Increased Severity of Local and Systemic IgE-Mediated Anaphylaxis and Modulation of Mast Cell Activation. J. Immunol. 2002, 168, 6455–6462. [Google Scholar] [CrossRef] [PubMed]
- Numata, T.; Ito, T.; Maeda, T.; Egusa, C.; Tsuboi, R. IL-33 promotes ICAM-1 expression via NF-kB in murine mast cells. Allergol. Int. 2016, 65, 158–165. [Google Scholar] [CrossRef]
- Babina, M.; Mammeri, K.; Henz, B.M. Retinoic acid up-regulates myeloid ICAM-3 expression and function in a cell-specific fashion–evidence for retinoid signaling pathways in the mast cell lineage. J. Leukoc. Biol. 2001, 69, 361–372. [Google Scholar] [CrossRef] [PubMed]
- Hallgren, J.; Jones, T.G.; Abonia, J.P.; Xing, W.; Humbles, A.; Austen, K.F.; Gurish, M.F. Pulmonary CXCR2 regulates VCAM-1 and antigen-induced recruitment of mast cell progenitors. Proc. Natl. Acad. Sci. USA 2007, 104, 20478–20483. [Google Scholar] [CrossRef] [PubMed]
- Van Haaster, C.M.C.J.; Derhaag, J.G.; Engels, W.; Lemmens, P.J.M.R.; Gijsen, A.P.; Hornstra, G.; Van Der Vusse, G.J.; Duijvestijn, A.M. Mast cell-mediated induction of ICAM-1, VCAM-1 and E-selectin in endothelial cells in vitro: Constitutive release of inducing mediators but no effect of degranulation. Pflügers Arch. 1997, 435, 137–144. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Tonnesen, M.G.; Marchese, M.J.; Clark, R.A.F.; Bahou, W.F.; Gruber, B.L. Mast cells are potent regulators of endothelial cell adhesion molecule ICAM-1 and VCAM-1 expression. J. Cell. Physiol. 1995, 165, 40–53. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Marchese, M.J.; Garlick, J.A.; Jelaska, A.; Korn, J.H.; Gailit, J.; Clark, R.A.; Gruber, B.L. Mast Cells Induce T-Cell Adhesion to Human Fibroblasts by Regulating Intercellular Adhesion Molecule-1 and Vascular Cell Adhesion with Expression. J. Invest. Dermatol. 1995, 105, 789–796. [Google Scholar] [CrossRef]
- Barczyk, M.; Carracedo, S.; Gullberg, D. Integrins. Cell Tissue Res. 2010, 339, 269–280. [Google Scholar] [CrossRef]
- Takada, Y.; Ye, X.; Simon, S. The integrins. Genome Biol. 2007, 8, 215. [Google Scholar] [CrossRef]
- Tachimoto, H.; Hudson, S.A.; Bochner, B.S. Acquisition and alteration of adhesion molecules during cultured human mast cell differentiation. J. Allergy Clin. Immunol. 2001, 107, 302–309. [Google Scholar] [CrossRef]
- Sime, W.; Lunderius-Andersson, C.; Enoksson, M.; Rousselle, P.; Tryggvason, K.; Nilsson, G.; Harvima, I.; Patarroyo, M. Human Mast Cells Adhere to and Migrate on Epithelial and Vascular Basement Membrane Laminins LM-332 and LM-511 via α3β1 Integrin. J. Immunol. 2009, 183, 4657–4665. [Google Scholar] [CrossRef] [PubMed]
- Fowlkes, V.; Wilson, C.G.; Carver, W.; Goldsmith, E.C. Mechanical loading promotes mast cell degranulation via RGD-integrin dependent pathways. J. Biomech. 2013, 46, 788–795. [Google Scholar] [CrossRef] [PubMed]
- Inamura, N.; Mekori, Y.A.; Bhattacharyya, S.P.; Bianchine, P.J.; Metcalfe, D.D. Induction and enhancement of Fc(epsilon)RI-dependent mast cell degranulation following coculture with activated T cells: Dependency on ICAM-1- and leukocyte function-associated antigen (LFA)-1-mediated heterotypic aggregation. J. Immunol. 1998, 160, 4026–4033. [Google Scholar] [PubMed]
- Mekori, Y.A.; Baram, D. Heterotypic adhesion-induced mast cell activation: Biologic relevance in the inflammatory context. Mol. Immunol. 2002, 38, 1363–1367. [Google Scholar] [CrossRef]
- Carroll-Portillo, A.; Cannon, J.L.; Riet, J.T.; Holmes, A.M.; Kawakami, Y.; Kawakami, T.; Cambi, A.; Lidke, D.S. Mast cells and dendritic cells form synapses that facilitate antigen transfer for T cell activation. J. Cell Biol. 2015, 210, 851–864. [Google Scholar] [CrossRef]
- Ioffreda, M.D.; Whitaker, D.; Murphy, G.F. Mast Cell Degranulation Upregulates ∝6 Integrins on Epidermal Langerhans Cells. J. Investig. Dermatol. 1993, 101, 150–154. [Google Scholar] [CrossRef]
- Koch, A.E.; Halloran, M.M.; Haskell, C.J.; Shah, M.R.; Polverini, P.J. Angiogenesis mediated by soluble forms of E-selectin and vascular cell adhesion molecule-1. Nature 1995, 376, 517–519. [Google Scholar] [CrossRef]
- Frenette, P.S.; Subbarao, S.; Mazo, I.B.; Von Andrian, U.H.; Wagner, D.D. Endothelial selectins and vascular cell adhesion molecule-1 promote hematopoietic progenitor homing to bone marrow. Proc. Natl. Acad. Sci. USA 1998, 95, 14423–14428. [Google Scholar] [CrossRef]
- Natoni, A.; Macauley, M.S.; O’Dwyer, M.E. Targeting Selectins and Their Ligands in Cancer. Front. Oncol. 2016, 6, 93. [Google Scholar] [CrossRef]
- Gotsch, U.; Jäger, U.; Dominis, M.; Vestweber, D. Expression of P-selectin on Endothelial Cells is Upregulated by LPS and TNF-α in Vivo. Cell Adhes. Commun. 1994, 2, 7–14. [Google Scholar] [CrossRef]
- Merten, M.; Thiagarajan, P. P-Selectin Expression on Platelets Determines Size and Stability of Platelet Aggregates. Circulation 2000, 102, 1931–1936. [Google Scholar] [CrossRef]
- Tchernychev, B.; Furie, B.; Furie, B.C. Peritoneal macrophages express both P-selectin and PSGL-1. J. Cell Biol. 2003, 163, 1145–1155. [Google Scholar] [CrossRef] [PubMed]
- Wyble, C.W.; Hynes, K.L.; Kuchibhotla, J.; Marcus, B.C.; Hallahan, D.; Gewertz, B.L. TNF-α and IL-1 Upregulate Membrane-Bound and Soluble E-Selectin through a Common Pathway. J. Surg. Res. 1997, 73, 107–112. [Google Scholar] [CrossRef] [PubMed]
- Steegmaier, M.; Blanks, J.E.; Borges, E.; Vestweber, D. P-selectin glycoprotein ligand-1 mediates rolling of mouse bone marrow-derived mast cells on P-selectin but not efficiently on E-selectin. Eur. J. Immunol. 1997, 27, 1339–1345. [Google Scholar] [CrossRef] [PubMed]
- Thorlacius, H.; Raud, J.; Rosengrenbeezley, S.; Forrest, M.; Hedqvist, P.; Lindbom, L. Mast Cell Activation Induces P-Selectin-Dependent Leukocyte Rolling and Adhesion in Postcapillary Venules in Vivo. Biochem. Biophys. Res. Commun. 1994, 203, 1043–1049. [Google Scholar] [CrossRef] [PubMed]
- Christofidou-Solomidou, M.; Murphy, G.F.; Albelda, S.M. Induction of E-selectin-dependent leukocyte recruitment by mast cell degranulation in human skin grafts transplanted on SCID mice. Am. J. Pathol. 1996, 148, 177–188. [Google Scholar]
- Zhang, J.; Alcaide, P.; Liu, L.; Sun, J.; He, A.; Luscinskas, F.W.; Shi, G.-P. Regulation of Endothelial Cell Adhesion Molecule Expression by Mast Cells, Macrophages, and Neutrophils. PLoS ONE 2011, 6, e14525. [Google Scholar] [CrossRef]
- Palm, A.-K.E.; Garcia-Faroldi, G.; Lundberg, M.; Pejler, G.; Kleinau, S. Activated mast cells promote differentiation of B cells into effector cells. Sci. Rep. 2016, 6, 20531. [Google Scholar] [CrossRef]
- Zhao, X.; Dib, M.; Wang, X.; Widegren, B.; Andersson, R. Influence of Mast Cells on the Expression of Adhesion Molecules on Circulating and Migrating Leukocytes in Acute Pancreatitis-Associated Lung Injury. Lung 2005, 183, 253–264. [Google Scholar] [CrossRef]
- Saito, M.; Tucker, D.K.; Kohlhorst, D.; Niessen, C.M.; Kowalczyk, A.P. Classical and desmosomal cadherins at a glance. J. Cell Sci. 2012, 125, 2547–2552. [Google Scholar] [CrossRef]
- Frank, M.; Kemler, R. Protocadherins. Curr. Opin. Cell Biol. 2002, 14, 557–562. [Google Scholar] [CrossRef]
- Maître, J.-L.; Heisenberg, C.-P. Three Functions of Cadherins in Cell Adhesion. Curr. Biol. 2013, 23, R626–R633. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, A.; Suzuki, R.; Furuno, T.; Teshima, R.; Nakanishi, M. N-Cadherin Plays a Role in the Synapse-Like Structures between Mast Cells and Neurites. Biol. Pharm. Bull. 2004, 27, 1891–1894. [Google Scholar] [CrossRef] [PubMed]
- Sendo, T.; Sumimura, T.; Itoh, Y.; Goromaru, T.; Aki, K.; Yano, T.; Oike, M.; Ito, Y.; Mori, S.; Nishibori, M.; et al. Involvement of proteinase-activated receptor-2 in mast cell tryptase-induced barrier dysfunction in bovine aortic endothelial cells. Cell. Signal. 2003, 15, 773–781. [Google Scholar] [CrossRef]
- Ashina, K.; Tsubosaka, Y.; Nakamura, T.; Omori, K.; Kobayashi, K.; Hori, M.; Ozaki, H.; Murata, T. Histamine Induces Vascular Hyperpermeability by Increasing Blood Flow and Endothelial Barrier Disruption In Vivo. PLoS ONE 2015, 10, e0132367. [Google Scholar] [CrossRef] [PubMed]
- Fu, Z.; Thorpe, M.; Hellman, L. rMCP-2, the Major Rat Mucosal Mast Cell Protease, an Analysis of Its Extended Cleavage Specificity and Its Potential Role in Regulating Intestinal Permeability by the Cleavage of Cell Adhesion and Junction Proteins. PLoS ONE 2015, 10, e0131720. [Google Scholar] [CrossRef] [PubMed]
- Frantz, C.; Stewart, K.M.; Weaver, V.M. The extracellular matrix at a glance. J. Cell Sci. 2010, 123, 4195–4200. [Google Scholar] [CrossRef]
- Bonnans, C.; Chou, J.; Werb, Z. Remodelling the extracellular matrix in development and disease. Nat. Rev. Mol. Cell Biol. 2014, 15, 786–801. [Google Scholar] [CrossRef]
- Theocharis, A.D.; Skandalis, S.S.; Gialeli, C.; Karamanos, N.K. Extracellular matrix structure. Adv. Drug Deliv. Rev. 2016, 97, 4–27. [Google Scholar] [CrossRef]
- Preissner, K.T.; Reuning, U. Vitronectin in Vascular Context: Facets of a Multitalented Matricellular Protein. Semin. Thromb. Hemost. 2011, 37, 408–424. [Google Scholar] [CrossRef] [PubMed]
- Moiseeva, E.P.; Straatman, K.R.; Leyland, M.L.; Bradding, P. CADM1 Controls Actin Cytoskeleton Assembly and Regulates Extracellular Matrix Adhesion in Human Mast Cells. PLoS ONE 2014, 9, e85980. [Google Scholar] [CrossRef] [PubMed]
- Vliagoftis, H.; Metcalfe, D.D. Characterization of adhesive interactions between mast cells and laminin isoforms: Evidence of a principal role for α6 integrin. Immunology 1997, 92, 553–560. [Google Scholar] [CrossRef] [PubMed]
- Fukui, M.; Whittlesey, K.; Metcalfe, D.D.; Dastych, J. Human Mast Cells Express the Hyaluronic-Acid-Binding Isoform of CD44 and Adhere to Hyaluronic Acid. Clin. Immunol. 2000, 94, 173–178. [Google Scholar] [CrossRef] [PubMed]
- Ch’Ng, S.; Wallis, R.A.; Yuan, L.; Davis, P.F.; Tan, S.T. Mast cells and cutaneous malignancies. Mod. Pathol. 2006, 19, 149–159. [Google Scholar] [CrossRef]
- Kovanen, P.T. Mast cells and degradation of pericellular and extracellular matrices: Potential contributions to erosion, rupture and intraplaque haemorrhage of atherosclerotic plaques. Biochem. Soc. Trans. 2007, 35, 857–861. [Google Scholar] [CrossRef]
- Xiang, M.; Gu, Y.; Zhao, F.; Lu, H.; Chen, S.; Yin, L. Mast cell tryptase promotes breast cancer migration and invasion. Oncol. Rep. 2010, 23, 615–619. [Google Scholar] [CrossRef]
- Brower, G.L.; Janicki, J.S. Pharmacologic Inhibition of Mast Cell Degranulation Prevents Left Ventricular Remodeling Induced by Chronic Volume Overload in Rats. J. Card. Fail. 2005, 11, 548–556. [Google Scholar] [CrossRef]
- Okayama, Y.; Ra, C.; Saito, H. Role of mast cells in airway remodeling. Curr. Opin. Immunol. 2007, 19, 687–693. [Google Scholar] [CrossRef]
- Cavey, M.; Lecuit, T. Molecular Bases of Cell-Cell Junctions Stability and Dynamics. Cold Spring Harb. Perspect. Biol. 2009, 1, a002998. [Google Scholar] [CrossRef]
- Sumigray, K.D.; Lechler, T. Cell adhesion in epidermal development and barrier formation. Curr. Top. Dev. Biol. 2015, 112, 383–414. [Google Scholar] [CrossRef]
- Kempuraj, D.; Mentor, S.; Thangavel, R.; Ahmed, M.E.; Selvakumar, G.P.; Raikwar, S.P.; Dubova, I.; Zaheer, S.; Iyer, S.S.; Zaheer, A. Mast Cells in Stress, Pain, Blood-Brain Barrier, Neuroinflammation and Alzheimer’s Disease. Front. Cell. Neurosci. 2019, 13, 54. [Google Scholar] [CrossRef] [PubMed]
- Potts, R.A.; Tiffany, C.M.; Pakpour, N.; Lokken, K.L.; Tiffany, C.R.; Cheung, K.; Tsolis, R.M.; Luckhart, S. Mast cells and histamine alter intestinal permeability during malaria parasite infection. Immunobiol. 2016, 221, 468–474. [Google Scholar] [CrossRef] [PubMed]
- Zhou, X.; Wei, T.; Cox, C.W.; Jiang, Y.; Roche, W.R.; Walls, A.F. Mast cell chymase impairs bronchial epithelium integrity by degrading cell junction molecules of epithelial cells. Allergy 2019, 74, 1266–1276. [Google Scholar] [CrossRef] [PubMed]
- Johnson, J.L.; Najor, N.A.; Green, K.J. Desmosomes: Regulators of Cellular Signaling and Adhesion in Epidermal Health and Disease. Cold Spring Harb. Perspect. Med. 2014, 4, a015297. [Google Scholar] [CrossRef]
- Vodenicharov, A.; Chouchkov, C. Morphological study of mast cell localization in the wall of the proximal tubule in the domestic swine kidney. Anat. Histol. Embryol. 1999, 28, 85–88. [Google Scholar] [CrossRef]
- Niessen, C.M. Tight junctions/adherens junctions: Basic structure and function. J. Invest. Dermatol. 2007, 127, 2525–2532. [Google Scholar] [CrossRef]
- Jacob, C.; Yang, P.-C.; Darmoul, D.; Amadesi, S.; Saito, T.; Cottrell, G.S.; Coelho, A.-M.; Singh, P.; Grady, E.F.; Perdue, M.H.; et al. Mast Cell Tryptase Controls Paracellular Permeability of the Intestine. Role of protease-activated receptor 2 and beta-arrestins. J. Biol. Chem. 2005, 280, 31936–31948. [Google Scholar] [CrossRef]
- Goodenough, D.A.; Paul, D.L. Gap Junctions. Cold Spring Harb. Perspect. Biol. 2009, 1, a002576. [Google Scholar] [CrossRef]
- Vliagoftis, H.; Hutson, A.M.; Mahmudi-Azer, S.; Kim, H.; Rumsaeng, V.; Oh, C.K.; Moqbel, R.; Metcalfe, D.D. Mast cells express connexins on their cytoplasmic membrane. J. Allergy Clin. Immunol. 1999, 103, 656–662. [Google Scholar] [CrossRef]
- Oliani, S.M.; Girol, A.P.; Smith, R.L. Gap Junctions between Mast Cells and Fibroblasts in the Developing Avian Eye. Acta Anat. 1995, 154, 267–271. [Google Scholar] [CrossRef]
- Foley, T.T.; Ehrlich, H.P. Through Gap Junction Communications, Co-Cultured Mast Cells and Fibroblasts Generate Fibroblast Activities Allied with Hypertrophic Scarring. Plast. Reconstr. Surg. 2013, 131, 1036–1044. [Google Scholar] [CrossRef] [PubMed]
- De Souza Junior, D.A.; Mazucato, V.M.; Santana, A.C.; Oliver, C.; Jamur, M.C. Mast Cells Interact with Endothelial Cells to Accelerate In Vitro Angiogenesis. Int. J. Mol. Sci. 2017, 18, 2674. [Google Scholar] [CrossRef]
- Litjens, S.H.M.; De Pereda, J.M.; Sonnenberg, A. Current insights into the formation and breakdown of hemidesmosomes. Trends Cell Biol. 2006, 16, 376–383. [Google Scholar] [CrossRef] [PubMed]
- Lo, S.H. Focal adhesions: What’s new inside. Dev. Biol. 2006, 294, 280–291. [Google Scholar] [CrossRef]
- Kawasugi, K.; French, P.W.; Penny, R.; Ludowyke, R.I. Focal adhesion formation is associated with secretion of allergic mediators. Cell Motil. Cytoskelet. 1995, 31, 215–224. [Google Scholar] [CrossRef]
- Leskinen, M.J.; Lindstedt, K.A.; Wang, Y.; Kovanen, P.T. Mast Cell Chymase Induces Smooth Muscle Cell Apoptosis by a Mechanism Involving Fibronectin Degradation and Disruption of Focal Adhesions. Arter. Thromb. Vasc. Biol. 2003, 23, 238–243. [Google Scholar] [CrossRef]
- Ginsberg, M.H.; Partridge, A.; Shattil, S.J. Integrin regulation. Curr. Opin. Cell Biol. 2005, 17, 509–516. [Google Scholar] [CrossRef]
- Abram, C.L.; Lowell, C.A. The Ins and Outs of Leukocyte Integrin Signaling. Annu. Rev. Immunol. 2009, 27, 339–362. [Google Scholar] [CrossRef]
- Ye, F.; Kim, C.; Ginsberg, M.H. Molecular mechanism of inside-out integrin regulation. J. Thromb. Haemost. 2011, 9, 20–25. [Google Scholar] [CrossRef]
- Legate, K.R.; Wickström, S.A.; Fässler, R. Genetic and cell biological analysis of integrin outside-in signaling. Genes Dev. 2009, 23, 397–418. [Google Scholar] [CrossRef]
- Huveneers, S.; Danen, E.H. Adhesion signaling—Crosstalk between integrins, Src and Rho. J. Cell Sci. 2009, 122, 1059–1069. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, S.; Friedl, P. Interstitial cell migration: Integrin-dependent and alternative adhesion mechanisms. Cell Tissue Res. 2010, 339, 83–92. [Google Scholar] [CrossRef] [PubMed]
- McEver, R.P. Selectins: Initiators of leucocyte adhesion and signalling at the vascular wall. Cardiovasc. Res. 2015, 107, 331–339. [Google Scholar] [CrossRef] [PubMed]
- Wyczółkowska, J.; Dastych, J.; Ślusarczyk, A.; Kolago, B. Relations between Fc epsilon RI crosslinking-induced mast cell activation and adhesion to fibronectin. J. Physiol. Pharmacol. 1994, 45, 501–516. [Google Scholar]
- Kitaura, J.; Eto, K.; Kinoshita, T.; Kawakami, Y.; Leitges, M.; Lowell, C.A.; Kawakami, T. Regulation of Highly Cytokinergic IgE-Induced Mast Cell Adhesion by Src, Syk, Tec, and Protein Kinase C Family Kinases. J. Immunol. 2005, 174, 4495–4504. [Google Scholar] [CrossRef] [PubMed]
- Smith, J.A.; Samayawardhena, L.A.; Craig, A.W.B. Fps/Fes protein-tyrosine kinase regulates mast cell adhesion and migration downstream of Kit and β1 integrin receptors. Cell. Signal. 2010, 22, 427–436. [Google Scholar] [CrossRef]
- Dastych, J.; Taub, D.; Hardison, M.C.; Metcalfe, D.D. Tyrosine kinase-deficient Wv c-kit induces mast cell adhesion and chemotaxis. Am. J. Physiol. 1998, 275, C1291–C1299. [Google Scholar] [CrossRef]
- Dastych, J.; Hardison, M.C.; Metcalfe, D.D. Aggregation of low affinity IgG receptors induces mast cell adherence to fibronectin: Requirement for the common FcR gamma-chain. J. Immunol. 1997, 158, 1803–1809. [Google Scholar]
- Hershkoviz, R.; Preciado-Patt, L.; Lider, O.; Fridkin, M.; Dastych, J.; Metcalfe, D.D.; Mekori, Y.A. Extracellular matrix-anchored serum amyloid A preferentially induces mast cell adhesion. Am. J. Physiol. 1997, 273, C179–C187. [Google Scholar] [CrossRef]
- Vliagoftis, H. Thrombin Induces Mast Cell Adhesion to Fibronectin: Evidence for Involvement of Protease-Activated Receptor-1. J. Immunol. 2002, 169, 4551–4558. [Google Scholar] [CrossRef]
- Sivalenka, R.R.; Jessberger, R. SWAP-70 Regulates c-kit-Induced Mast Cell Activation, Cell-Cell Adhesion, and Migration. Mol. Cell. Biol. 2004, 24, 10277–10288. [Google Scholar] [CrossRef] [PubMed]
- Yoshikawa, H.; Nakajima, Y.; Tasaka, K. Glucocorticoid suppresses autocrine survival of mast cells by inhibiting IL-4 production and ICAM-1 expression. J. Immunol. 1999, 162, 6162–6170. [Google Scholar] [PubMed]
- Fox, C.C.; Jewell, S.D.; Whitacre, C.C. Rat Peritoneal Mast Cells Present Antigen to a PPD-Specific T Cell Line. Cell. Immunol. 1994, 158, 253–264. [Google Scholar] [CrossRef] [PubMed]
- Ryu, S.Y.; Hong, G.U.; Kim, D.Y.; Ro, J.Y. Enolase 1 and calreticulin regulate the differentiation and function of mouse mast cells. Cell. Signal. 2012, 24, 60–70. [Google Scholar] [CrossRef] [PubMed]
- Sagawa, K.; Swaim, W.; Zhang, J.; Unsworth, E.; Siraganian, R.P. Aggregation of the High Affinity IgE Receptor Results in the Tyrosine Phosphorylation of the Surface Adhesion Protein PECAM-1 (CD31). J. Biol. Chem. 1997, 272, 13412–13418. [Google Scholar] [CrossRef] [PubMed]
- Grodzki, A.C.G.; Pástor, M.V.D.; Sousa, J.F.; Oliver, C.; Jamur, M.C. Differential expression of integrin subunits on adherent and nonadherent mast cells. Braz. J. Med Biol. Res. 2003, 36, 1101–1109. [Google Scholar] [CrossRef] [PubMed]
- Akula, S.; Paivandy, A.; Fu, Z.; Thorpe, M.; Pejler, G.; Hellman, L. Quantitative In-Depth Analysis of the Mouse Mast Cell Transcriptome Reveals Organ-Specific Mast Cell Heterogeneity. Cells 2020, 9, 211. [Google Scholar] [CrossRef]
- Fehlner-Gardiner, C.; Uniyal, S.; Von Ballestrem, C.; Dougherty, G.J.; Chan, B.M.C. Integrin VLA-6 (α6β1) mediates adhesion of mouse bone marrow-derived mast cells to laminin. Allergy 1996, 51, 650–656. [Google Scholar] [CrossRef]
- Honjo, A.; Nakano, N.; Yamazaki, S.; Hara, M.; Uchida, K.; Kitaura, J.; Nishiyama, C.; Yagita, H.; Ohtsuka, Y.; Ogawa, H.; et al. Pharmacologic inhibition of Notch signaling suppresses food antigen–induced mucosal mast cell hyperplasia. J. Allergy Clin. Immunol. 2017, 139, 987–996e10. [Google Scholar] [CrossRef]
- Bankova, L.G.; Dwyer, D.F.; Liu, A.Y.; Austen, K.F.; Gurish, M.F. Maturation of mast cell progenitors to mucosal mast cells during allergic pulmonary inflammation in mice. Mucosal Immunol. 2015, 8, 596–606. [Google Scholar] [CrossRef]
- Trautmann, A.; Feuerstein, B.; Ernst, N.; Bröcker, E.-B.; Klein, C.E. Heterotypic cell-cell adhesion of human mast cells to fibroblasts. Arch. Dermatol. Res. 1997, 289, 194–203. [Google Scholar] [CrossRef] [PubMed]
- Sanmugalingam, D.; Wardlaw, A.J.; Bradding, P. Adhesion of human lung mast cells to bronchial epithelium: Evidence for a novel carbohydrate-mediated mechanism. J. Leukoc. Biol. 2000, 68, 38–46. [Google Scholar] [CrossRef] [PubMed]
- Nakashima, K.; Sakurai, F.; Kawabata, K.; Mizuguchi, H. Efficient gene delivery in human and rodent mast cells using adenovirus vectors. J. Control. Release 2008, 129, 215–222. [Google Scholar] [CrossRef] [PubMed]
- Powner, D.J.; Payne, R.M.; Pettitt, T.R.; Giudici, M.L.; Irvine, R.F.; Wakelam, M.J.O. Phospholipase D2 stimulates integrin-mediated adhesion via phosphatidylinositol 4-phosphate 5-kinase Iγb. J. Cell Sci. 2005, 118, 2975–2986. [Google Scholar] [CrossRef] [PubMed]
- Yamada, D.; Kadono, T.; Masui, Y.; Yanaba, K.; Sato, S. β7 Integrin Controls Mast Cell Recruitment, whereas αE Integrin Modulates the Number and Function of CD8+ T Cells in Immune Complex–Mediated Tissue Injury. J. Immunol. 2014, 192, 4112–4121. [Google Scholar] [CrossRef]
- Chen, Y.; Garrison, S.; Weis, J.J.; Weis, J.H. Identification of Pactolus, an Integrin β Subunit-like Cell-surface Protein Preferentially Expressed by Cells of the Bone Marrow. J. Biol. Chem. 1998, 273, 8711–8718. [Google Scholar] [CrossRef]
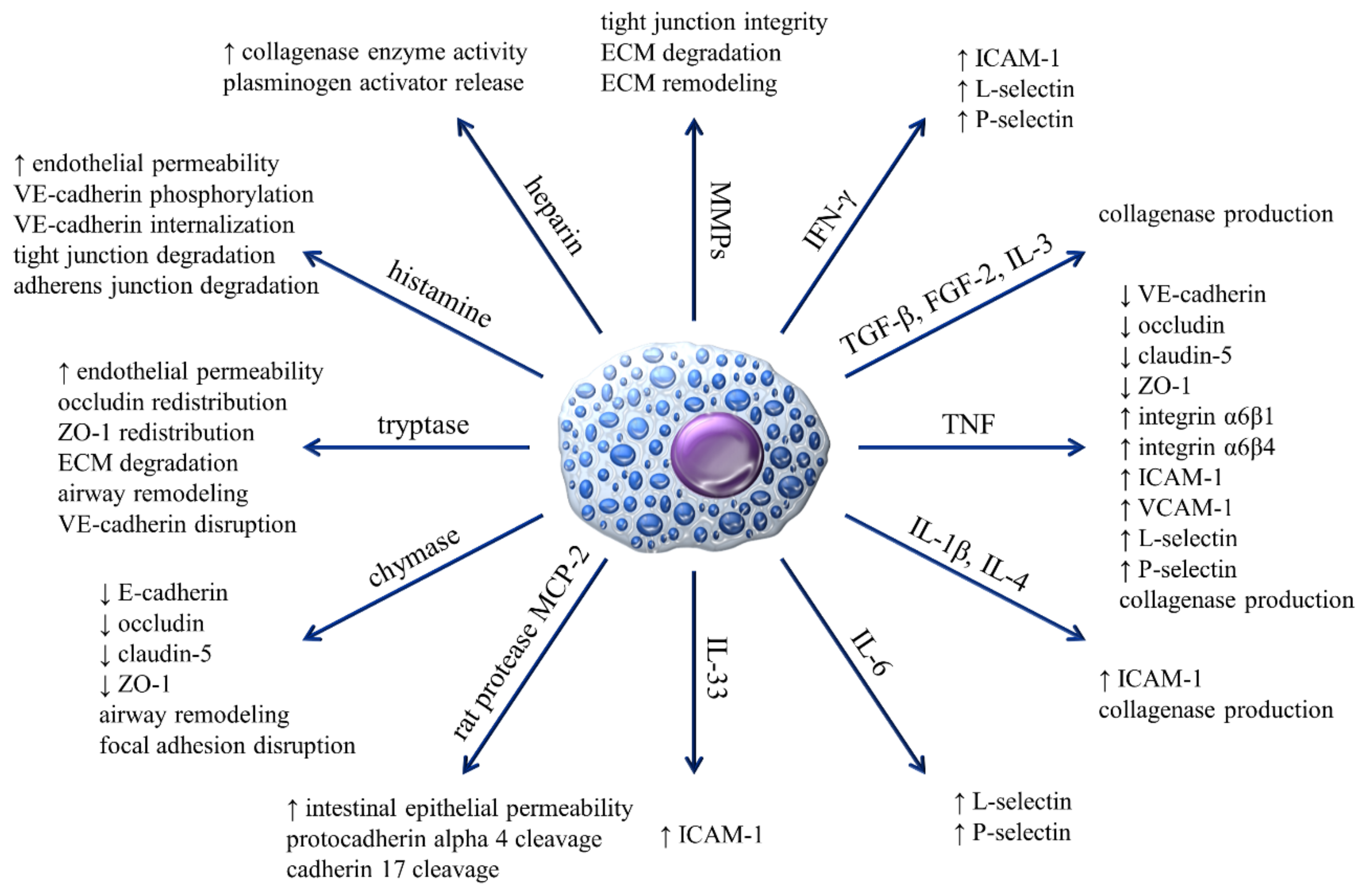
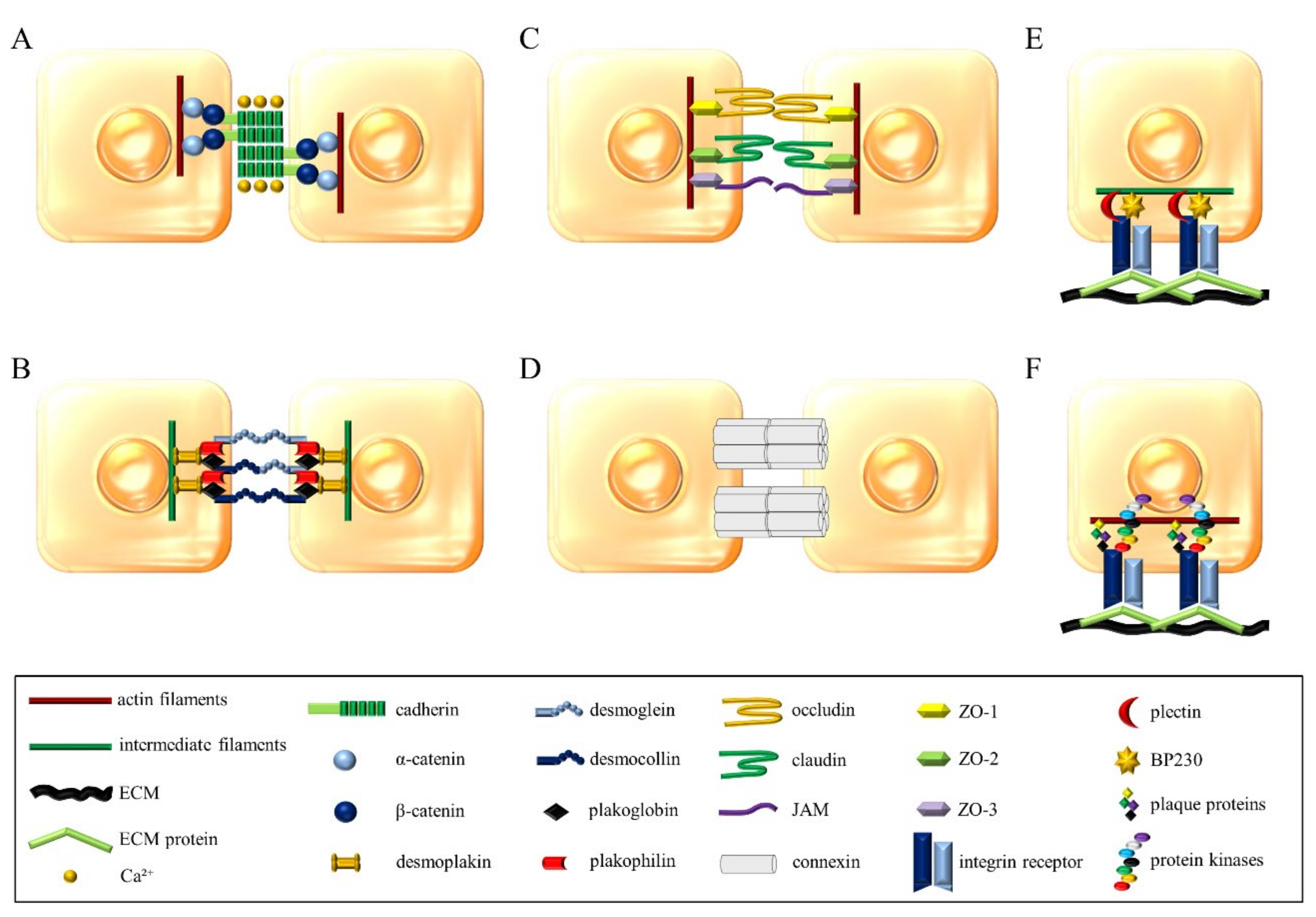
| CAMs | Functions in MCs | References | |
|---|---|---|---|
| Ligand/-s | Action | ||
| IgSF CAMs | |||
| ICAM-1 | LFA-1 (αLβ2) | Migration of MCs to inflamed tissues. Interaction with stroma cells, cytotoxic or helper T cells, Langerhans’ cells, monocytes, and granulocytes. Activation of lymphocytes. | [19,20,21] |
| ICAM-3 | αDβ2 LFA-1 (αLβ2) | Regulation of proliferation, apoptosis, spreading, and cytokine production. Cross-linking leads to homotypic/heterotypic aggregation and MC adhesion to ECM. | [22,23] |
| VCAM-1 | VLA-4 (α4β1) α4β7 | Scarce data. | [24] |
| PECAM-1 | αVβ3 | Cross-talk with PECAM-1 expressed on endothelial cells leads to transmigration of BMMCs through skin endothelial cell barrier. | [25] |
| Integrins | |||
| α2β1 | collagen laminin | Scarce data. | [26] |
| α3β1 | laminin fibronectin | Interaction with ECM. Contribution to human MC migration. | [27,28] |
| VLA-4 (α4β1) | VCAM-1 MAdCAM-1 fibronectin | Recruitment of MC progenitors in allergic inflammation. Recruitment of mouse MC progenitors to inflamed lungs. Interaction with ECM proteins. Mouse and rat MC activation and degranulation associated with the high-affinity IgE receptor cross-linking. | [24,28,29,30] |
| α4β7 | VCAM-1 MAdCAM-1 | Recruitment of MC progenitors in allergic inflammation. Homing of MC progenitors to small intestine. Recruitment of mouse MC progenitors to inflamed lungs. | [24,25,29,31] |
| α5β1 | fibronectin | Interaction with ECM proteins. Mouse and rat MC activation and degranulation associated with the high-affinity IgE receptor cross-linking. | [28,30] |
| α6β1 | laminin | Presence on BMMC and their mature form – CTMC, thus, may be related to MC heterogeneity and involved in MC development. | [32] |
| α7β1 | laminin | Interaction with ECM proteins. Present mainly in mouse. | [27] |
| α9β1 | Scarce data. | ||
| αIIbβ3 | fibronectin vitronectin, fibrinogen | Possible role in differentiation and homing of human and mouse tissue MCs. Activation of MCs. | [33,34] |
| αEβ7 | E-cadherin | Heterophilic adhesion of BMMCs to epithelial cells. Possible contribution to allergic inflammation and removal of nematodes. | [31,35] |
| LFA-1 (αLβ2) | Function not clear. Possible role in MC-other inflammatory cell interaction and immature MC homing. | [24,36] | |
| αMβ2 | Function not clear. Possible role in MC-other inflammatory cell interaction and immature MC homing. | [24,36] | |
| αVβ1 | vitronectin | Clustering of the receptor on filopodia during cell spreading. | [37] |
| αVβ3 | PECAM-1 | Rolling of immature MCs during inflammation. Transmigration of BMMCs through skin endothelial cell barrier. Mouse and rat MC activation and degranulation associated with the high-affinity IgE receptor cross-linking. | [25,30] |
| αVβ5 | vitronectin | Clustering of the receptor on filopodia during cell spreading. | [37] |
| αVβ6 | Participation in MC protease expression regulation, thus, may regulate airway responsiveness in allergic asthma. | [38] | |
| αXβ2 | Function not clear in the context of MC adhesion. Possible role in MC-other inflammatory cell interaction and immature MC homing. | [24,36] | |
| Selectins | |||
| L-selectin | Recruitment of mouse MCs during cutaneous Arthus reaction. | [39] | |
| Cadherins | |||
| E-cadherin | E-cadherin | Homophilic adhesion of BMMCs and HMC-1 to E-cadherin on epithelial cells. Possible contribution to allergic inflammation and removal of nematodes. Possible role in differentiation, proliferation and cell recognition. | [35,40] |
| N-cadherin | Present in BMMC. Exact role not clear. | [41] | |
| CAMs | Expression in MCs | References | ||
|---|---|---|---|---|
| Primary and In Vitro Differentiated Cells | Cell Lines | |||
| Mature | Immature | (Immature) | ||
| IgSF CAMs | ||||
| ICAM-1 | LMCs (h), SMCs (h), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), MC-9 (m) | [20,62,142,143] |
| ICAM-3 | LMCs (h), SMCs (h) | HMC-1 (h) | [22] | |
| VCAM-1 | BMMCs (m) | [144] | ||
| PECAM-1 | mPMCs (m) | BMMCs (m) | RBL-2H3 (r) | [61,145] |
| Integrins | ||||
| α2 | mPMCs (m) | CBMCs (h), BMMCs (m) | HMC-1 (h), RBL-2H3 (r) | [26,34,71,102,146] |
| α3 | SMCs (h) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h) | [12,26,28,71,102] |
| α4 | LMCs (h), SMCs (h), mPMCs (m), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h), RBL-2H3 (r) | [12,18,26,28,30,34,70,147] |
| α5 | LMCs (h), SMCs (h), mPMCs (m), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h), MC-9 (m), RBL-2H3 (r) | [12,18,26,27,28,30,70,147] |
| α6 | SMCs (h), mPMCs (m), rPMCs (r) | BMMCs (m) | HMC-1 (h), MC-9 (m), RBL-2H3 (r) | [18,26,27,32,146,148] |
| α7 | BMMCs (m) | LAD2 (h) | [12,27] | |
| α9 | mPMCs (m) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h) | [12,71,147,149] |
| αIIb | mPMCs (m) | CBMCs (h), BMMCs (m) | [33,34] | |
| αE | mPMCs (m) | BMMCs (m) | [35,150] | |
| αL | SMCs (h) | CBMCs (m), BMMCs (m) | HMC-1 (h), LAD2 (h), MC-9 (m) | [12,34,36,70,142,151] |
| αM | LMCs (h), mPMCs (m) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h) | [12,36,70,147,149,152] |
| αV | LMCs (h), SMCs (h), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h), RBL-2H3 (r) | [18,26,30,38,71,153] |
| αX | LMCs (h), SMCs (h) | CBMCs (h) | HMC-1 (h), LAD2 (h) | [12,36,70,152] |
| β1 | LMCs (h), SMCs (h), mPMCs (m), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h), MC-9 (m), RBL-2H3 (r) | [12,18,26,34,71,146,148] |
| β2 | LMCs (h), SMCs (h), mPMCs (m), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), RBL-2H3 (r) | [34,36,39,70,143,151,152,154] |
| β3 | LMCs (h), SMCs (h), mPMCs (m), rPMCs (r) | CBMCs (h), BMMCs (m) | HMC-1 (h), LAD2 (h), RBL-2H3 (r) | [18,30,34,71,153] |
| β5 | HMC-1 (h), LAD2 (h) | [26,153] | ||
| β6 | BMMCs (m) | [38] | ||
| β7 | mPMCs (m), rPMCs (r) | BMMCs (m) | LAD2 (h), RBL-2H3 (r) | [12,35,146,155] |
| Selectins | ||||
| L-selectin | mPMCs (m) | BMMCs (m) | [39,156] | |
| Cadherins | ||||
| E-cadherin | mPMCs (m) | BMMCs (m) | HMC-1 (h) | [35,40,41] |
| N-cadherin | BMMCs (m) | [41] | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pastwińska, J.; Żelechowska, P.; Walczak-Drzewiecka, A.; Brzezińska-Błaszczyk, E.; Dastych, J. The Art of Mast Cell Adhesion. Cells 2020, 9, 2664. https://doi.org/10.3390/cells9122664
Pastwińska J, Żelechowska P, Walczak-Drzewiecka A, Brzezińska-Błaszczyk E, Dastych J. The Art of Mast Cell Adhesion. Cells. 2020; 9(12):2664. https://doi.org/10.3390/cells9122664
Chicago/Turabian StylePastwińska, Joanna, Paulina Żelechowska, Aurelia Walczak-Drzewiecka, Ewa Brzezińska-Błaszczyk, and Jarosław Dastych. 2020. "The Art of Mast Cell Adhesion" Cells 9, no. 12: 2664. https://doi.org/10.3390/cells9122664
APA StylePastwińska, J., Żelechowska, P., Walczak-Drzewiecka, A., Brzezińska-Błaszczyk, E., & Dastych, J. (2020). The Art of Mast Cell Adhesion. Cells, 9(12), 2664. https://doi.org/10.3390/cells9122664





