Role of Basic Fibroblast Growth Factor in Cancer: Biological Activity, Targeted Therapies, and Prognostic Value
Abstract
1. Introduction
2. bFGF
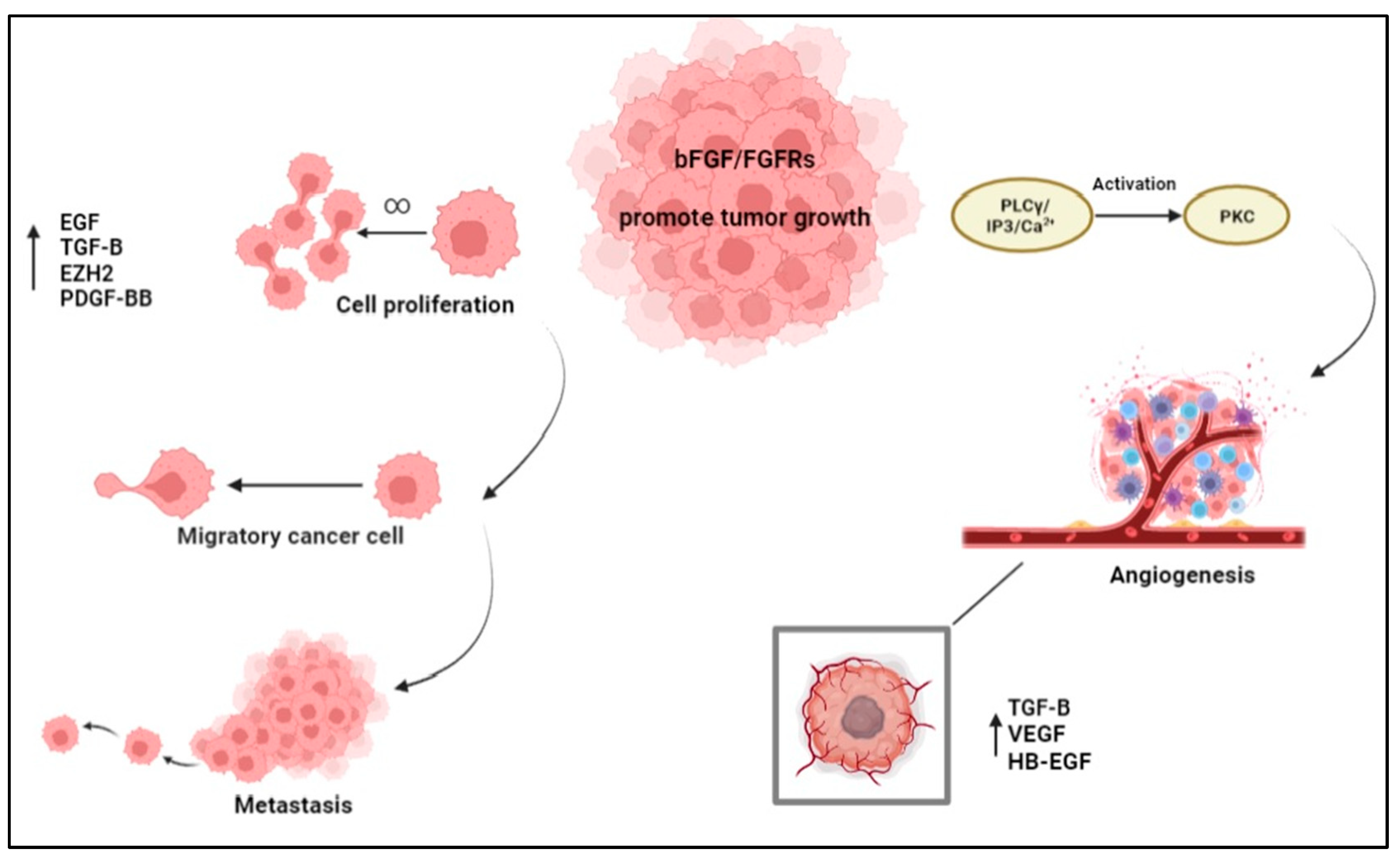
3. Function of bFGF in Tumor Microenvironment
3.1. bFGF and Angiogenesis
3.2. Role of bFGF in Cell Proliferation and Metastasis
3.3. bFGF and Chemoresistance
4. bFGF and Cancer
4.1. bFGF in Brain Tumors
4.2. bFGF in Gastrointestinal Cancers
4.3. bFGF in Liver Cancer
4.4. bFGF in Pancreatic Cancer
4.5. bFGF in Oral Cavity
4.6. bFGF in Lung Cancer
4.7. bFGF in Kidney Cancer
4.8. bFGF in Bone Tumors
4.9. bFGF in Thyroid Cancer
4.10. bFGF in Bladder Cancer
4.11. bFGF in Prostate Cancer
4.12. bFGF in Breast Cancer
4.13. bFGF in Ovarian and Cervical Cancer
4.14. Summary of Current Anticancer Therapies
4.15. Clinical Trials Evaluating FGFR Targeted Therapies
| Cancer Type | First Author | Title | Therapeutic Treatment | References |
|---|---|---|---|---|
| Gastric/Gastric-oesophageal | Wainberg et al. (2022) | Bemarituzumab in patients with FGFR2b-selected gastric or gastro-oesophageal junction adenocarcinoma (FIGHT): a randomised, double-blind, placebo-controlled, phase 2 study | Treatment with Bemarituzumab effectively inhibits the pathway of FGF and FGFR. | [218] |
| Bile ducts | Bibeau et al. (2022) | Progression-Free Survival in Patients with Cholangiocarcinoma with or Without FGF/FGFR Alterations: A FIGHT-202 Post Hoc Analysis of Prior Systemic Therapy Response | Patients with an alteration of FGFR showed a more prolonged progression-free survival during treatment with Pemigatinib and an association with second-line treatment. | [214] |
| Prostate | Liow et al. (2022) | Phase 2 Study of Neoadjuvant FGFR Inhibition and Androgen Deprivation Therapy Prior to Prostatectomy | The study showed the effects of FGF/FGFR-signaling inhibition and acute androgen deprivation. | [219] |
| Bile ducts, breast, colon, head and neck, other solid tumors | Subbiah et al. (2022) | FIGHT-101, a first-in-human study of potent and selective FGFR 1-3 inhibitor pemigatinib in pan-cancer patients with FGF/FGFR alterations and advanced malignancies | Pemigatinib has been shown to be clinically and pharmacodynamically safe; it is also safe towards tumors due to FGFR mutation. | [215] |
| Lung | Aggarwal et al. (2022) | SWOG S1400D (NCT02965378), a Phase II Study of the Fibroblast Growth Factor Receptor Inhibitor AZD4547 in Previously Treated Patients with Fibroblast Growth Factor Pathway-Activated Stage IV Squamous Cell Lung Cancer (Lung-MAP Substudy) | Treatment with AZD4547 showed a safe profile but unfortunately a modest improvement in patients with FGFR mutations. | [213] |
| Prostate | Choi et al. (2018) | Phase II Study of Dovitinib in Patients with Castration-Resistant Prostate Cancer (KCSG-GU11-05) | This study evaluated the progression-free survival and then the safety profile of dovitinib in patients who demonstrated different alterations of FGF and VEGF receptors. | [220] |
| Endometrial | Konecny et al. (2015) | Second-line dovitinib (TKI258) in patients with FGFR2-mutated or FGFR2-non-mutated advanced or metastatic endometrial cancer: a non-randomised, open-label, two-group, two-stage, phase 2 study | Evaluation of the safety and activity of dovitinib, FGFR, VEGFR, PDGFR-β, and c-KIT inhibitors in patients presenting and not presenting alterations of these receptors. | [217] |
| Renal | Kim et al. (2011) | Phase I/II and pharmacodynamic study of dovitinib (TKI258), an inhibitor of fibroblast growth factor receptors and VEGF receptors, in patients with advanced melanoma | The study reported that the tolerable dose of dovitinib effective in inhibiting the FGFR family was 400 mg/d. | [221] |
| Bile ducts | Goyal et al. (2023) | Futibatinib for FGFR2-Rearranged Intrahepatic Cholangiocarcinoma | Futibatinib has proven to be a valuable treatment for patients with FGFR2 abnormalities with cholangiocarcinoma. | [216] |
| Glioblastoma | Lee et al. (2019) | Phase II trial of ponatinib in patients with bevacizumab-refractory glioblastoma | The aim of the study was to evaluate patient 3-month progression-free survival, overall survival, and safety with bevacizumab-resistant GBM. | [222] |
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Beenken, A.; Mohammadi, M. The FGF family: Biology, pathophysiology and therapy. Nat. Rev. Drug Discov. 2009, 8, 235–253. [Google Scholar] [CrossRef] [PubMed]
- Raju, R.; Palapetta, S.M.; Sandhya, V.K.; Sahu, A.; Alipoor, A.; Balakrishnan, L.; Advani, J.; George, B.; Kini, K.R.; Geetha, N.P.; et al. A Network Map of FGF-1/FGFR Signaling System. J. Signal Transduct. 2014, 2014, 962962. [Google Scholar] [CrossRef] [PubMed]
- Fortin, D.; Rom, E.; Sun, H.; Yayon, A.; Bansal, R. Distinct fibroblast growth factor (FGF)/FGF receptor signaling pairs initiate diverse cellular responses in the oligodendrocyte lineage. J. Neurosci. 2005, 25, 7470–7479. [Google Scholar] [CrossRef]
- Akl, M.R.; Nagpal, P.; Ayoub, N.M.; Tai, B.; Prabhu, S.A.; Capac, C.M.; Gliksman, M.; Goy, A.; Suh, K.S. Molecular and clinical significance of fibroblast growth factor 2 (FGF2/bFGF) in malignancies of solid and hematological cancers for personalized therapies. Oncotarget 2016, 7, 44735–44762. [Google Scholar] [CrossRef]
- Noh, K.H.; Kim, S.-H.; Kim, J.H.; Song, K.-H.; Lee, Y.-H.; Kang, T.H.; Han, H.D.; Sood, A.K.; Ng, J.; Kim, K. API5 Confers Tumoral Immune Escape through FGF2-Dependent Cell Survival PathwayAPI5 Is a Novel Tumor Immune Escape Factor. Cancer Res. 2014, 74, 3556–3566. [Google Scholar] [CrossRef]
- Turner, N.; Grose, R. Fibroblast growth factor signalling: From development to cancer. Nat. Rev. Cancer 2010, 10, 116–129. [Google Scholar] [CrossRef] [PubMed]
- Gross, J.L.; Herblin, W.F.; Dusak, B.A.; Czerniak, P.; Diamond, M.D.; Sun, T.; Eidsvoog, K.; Dexter, D.L.; Yayon, A. Effects of modulation of basic fibroblast growth factor on tumor growth in vivo. J. Natl. Cancer Inst. 1993, 85, 121–131. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Hao, J.; Mao, Y.; Jin, Z.Q.; Cao, R.; Zhu, C.H.; Liu, X.H.; Liu, C.; Ding, X.L.; Wang, X.D.; et al. bFGF Promotes Migration and Induces Cancer-Associated Fibroblast Differentiation of Mouse Bone Mesenchymal Stem Cells to Promote Tumor Growth. Stem Cells Dev. 2016, 25, 1629–1639. [Google Scholar] [CrossRef]
- Parker, B.C.; Engels, M.; Annala, M.; Zhang, W. Emergence of FGFR family gene fusions as therapeutic targets in a wide spectrum of solid tumours. J. Pathol. 2014, 232, 4–15. [Google Scholar] [CrossRef] [PubMed]
- Daniele, G.; Corral, J.; Molife, L.R.; de Bono, J.S. FGF receptor inhibitors: Role in cancer therapy. Curr. Oncol. Rep. 2012, 14, 111–119. [Google Scholar] [CrossRef]
- Yun, Y.-R.; Won, J.E.; Jeon, E.; Lee, S.; Kang, W.; Jo, H.; Jang, J.-H.; Shin, U.S.; Kim, H.-W. Fibroblast growth factors: Biology, function, and application for tissue regeneration. J. Tissue Eng. 2010, 1, 218142. [Google Scholar] [CrossRef]
- Hassan, N.; Greve, B.; Espinoza-Sanchez, N.A.; Gotte, M. Cell-surface heparan sulfate proteoglycans as multifunctional integrators of signaling in cancer. Cell Signal. 2021, 77, 109822. [Google Scholar] [CrossRef]
- Babina, I.S.; Turner, N.C. Advances and challenges in targeting FGFR signalling in cancer. Nat. Rev. Cancer 2017, 17, 318–332. [Google Scholar] [CrossRef] [PubMed]
- Schlessinger, J.; Plotnikov, A.N.; Ibrahimi, O.A.; Eliseenkova, A.V.; Yeh, B.K.; Yayon, A.; Linhardt, R.J.; Mohammadi, M. Crystal structure of a ternary FGF-FGFR-heparin complex reveals a dual role for heparin in FGFR binding and dimerization. Mol. Cell 2000, 6, 743–750. [Google Scholar] [CrossRef] [PubMed]
- Parma, L.; Peters, H.A.B.; Sluiter, T.J.; Simons, K.H.; Lazzari, P.; de Vries, M.R.; Quax, P.H.A. bFGF blockade reduces intraplaque angiogenesis and macrophage infiltration in atherosclerotic vein graft lesions in ApoE3*Leiden mice. Sci. Rep. 2020, 10, 15968. [Google Scholar] [CrossRef] [PubMed]
- Steringer, J.P.; Lange, S.; Cujova, S.; Sachl, R.; Poojari, C.; Lolicato, F.; Beutel, O.; Muller, H.M.; Unger, S.; Coskun, U.; et al. Key steps in unconventional secretion of fibroblast growth factor 2 reconstituted with purified components. eLife 2017, 6, 28985. [Google Scholar] [CrossRef]
- Steringer, J.P.; Nickel, W. The molecular mechanism underlying unconventional secretion of Fibroblast Growth Factor 2 from tumour cells. Biol. Cell 2017, 109, 375–380. [Google Scholar] [CrossRef]
- Bikfalvi, A.; Klein, S.; Pintucci, G.; Rifkin, D.B. Biological roles of fibroblast growth factor-2. Endocr. Rev. 1997, 18, 26–45. [Google Scholar] [CrossRef] [PubMed]
- Sorensen, V.; Nilsen, T.; Wiedlocha, A. Functional diversity of FGF-2 isoforms by intracellular sorting. Bioessays 2006, 28, 504–514. [Google Scholar] [CrossRef]
- Touriol, C.; Bornes, S.; Bonnal, S.; Audigier, S.; Prats, H.; Prats, A.C.; Vagner, S. Generation of protein isoform diversity by alternative initiation of translation at non-AUG codons. Biol. Cell 2003, 95, 169–178. [Google Scholar] [CrossRef]
- Pasumarthi, K.B.; Kardami, E.; Cattini, P.A. High and low molecular weight fibroblast growth factor-2 increase proliferation of neonatal rat cardiac myocytes but have differential effects on binucleation and nuclear morphology. Evidence for both paracrine and intracrine actions of fibroblast growth factor-2. Circ. Res. 1996, 78, 126–136. [Google Scholar] [CrossRef] [PubMed]
- Sherman, L.; Stocker, K.M.; Morrison, R.; Ciment, G. Basic fibroblast growth factor (bFGF) acts intracellularly to cause the transdifferentiation of avian neural crest-derived Schwann cell precursors into melanocytes. Development 1993, 118, 1313–1326. [Google Scholar] [CrossRef]
- Hu, M.; Hu, Y.; He, J.; Li, B. Prognostic Value of Basic Fibroblast Growth Factor (bFGF) in Lung Cancer: A Systematic Review with Meta-Analysis. PLoS ONE 2016, 11, e0147374. [Google Scholar] [CrossRef]
- Barrientos, S.; Brem, H.; Stojadinovic, O.; Tomic-Canic, M. Clinical application of growth factors and cytokines in wound healing. Wound Repair Regen. 2014, 22, 569–578. [Google Scholar] [CrossRef]
- Iwai-Kanai, E.; Hasegawa, K.; Fujita, M.; Araki, M.; Yanazume, T.; Adachi, S.; Sasayama, S. Basic fibroblast growth factor protects cardiac myocytes from iNOS-mediated apoptosis. J. Cell. Physiol. 2002, 190, 54–62. [Google Scholar] [CrossRef]
- Sun, D.; Wang, W.; Wang, X.; Wang, Y.; Xu, X.; Ping, F.; Du, Y.; Jiang, W.; Cui, D. bFGF plays a neuroprotective role by suppressing excessive autophagy and apoptosis after transient global cerebral ischemia in rats. Cell Death Dis. 2018, 9, 172. [Google Scholar] [CrossRef]
- Woodbury, M.E.; Ikezu, T. Fibroblast growth factor-2 signaling in neurogenesis and neurodegeneration. J. Neuroimmune Pharm. 2014, 9, 92–101. [Google Scholar] [CrossRef] [PubMed]
- Rabchevsky, A.; Fugaccia, I.; Turner, A.; Blades, D.; Mattson, M.; Scheff, S. Basic fibroblast growth factor (bFGF) enhances functional recovery following severe spinal cord injury to the rat. Exp. Neurol. 2000, 164, 280–291. [Google Scholar] [CrossRef]
- Sun, D.; Bullock, M.R.; McGinn, M.J.; Zhou, Z.; Altememi, N.; Hagood, S.; Hamm, R.; Colello, R.J. Basic fibroblast growth factor-enhanced neurogenesis contributes to cognitive recovery in rats following traumatic brain injury. Exp. Neurol. 2009, 216, 56–65. [Google Scholar] [CrossRef] [PubMed]
- Ogino, R.; Murayama, N.; Noshita, T.; Takemoto, N.; Toba, T.; Oka, T.; Narii, N.; Yoshida, S.; Ueno, N.; Inoue, T. SUN11602 has basic fibroblast growth factor-like activity and attenuates neuronal damage and cognitive deficits in a rat model of Alzheimer’s disease induced by amyloid beta and excitatory amino acids. Brain Res. 2014, 1585, 159–166. [Google Scholar] [CrossRef]
- Bogousslavsky, J.; Victor, S.J.; Salinas, E.O.; Pallay, A.; Donnan, G.A.; Fieschi, C.; Kaste, M.; Orgogozo, J.M.; Chamorro, A.; Desmet, A.; et al. Fiblast (trafermin) in acute stroke: Results of the European-Australian phase II/III safety and efficacy trial. Cereb. Dis. 2002, 14, 239–251. [Google Scholar] [CrossRef]
- Okada-Ban, M.; Thiery, J.P.; Jouanneau, J. Fibroblast growth factor-2. Int. J. Biochem. Cell Biol. 2000, 32, 263–267. [Google Scholar] [CrossRef] [PubMed]
- House, S.L.; Melhorn, S.J.; Newman, G.; Doetschman, T.; Schultz Jel, J. The protein kinase C pathway mediates cardioprotection induced by cardiac-specific overexpression of fibroblast growth factor-2. Am. J. Physiol. Heart Circ. Physiol. 2007, 293, H354–H365. [Google Scholar] [CrossRef] [PubMed]
- House, S.L.; House, B.E.; Glascock, B.; Kimball, T.; Nusayr, E.; Schultz, J.E.; Doetschman, T. Fibroblast Growth Factor 2 Mediates Isoproterenol-induced Cardiac Hypertrophy through Activation of the Extracellular Regulated Kinase. Mol. Cell Pharm. 2010, 2, 143–154. [Google Scholar]
- Ruel, M.; Laham, R.J.; Parker, J.A.; Post, M.J.; Ware, J.A.; Simons, M.; Sellke, F.W. Long-term effects of surgical angiogenic therapy with fibroblast growth factor 2 protein. J. Thorac. Cardiovasc. Surg. 2002, 124, 28–34. [Google Scholar] [CrossRef]
- Simons, M.; Annex, B.H.; Laham, R.J.; Kleiman, N.; Henry, T.; Dauerman, H.; Udelson, J.E.; Gervino, E.V.; Pike, M.; Whitehouse, M. Pharmacological treatment of coronary artery disease with recombinant fibroblast growth factor-2: Double-blind, randomized, controlled clinical trial. Circulation 2002, 105, 788–793. [Google Scholar] [CrossRef] [PubMed]
- Lederman, R.J.; Mendelsohn, F.O.; Anderson, R.D.; Saucedo, J.F.; Tenaglia, A.N.; Hermiller, J.B.; Hillegass, W.B.; Rocha-Singh, K.; Moon, T.E.; Whitehouse, M. Therapeutic angiogenesis with recombinant fibroblast growth factor-2 for intermittent claudication (the TRAFFIC study): A randomised trial. Lancet 2002, 359, 2053–2058. [Google Scholar] [CrossRef]
- Yonemitsu, Y.; Matsumoto, T.; Itoh, H.; Okazaki, J.; Uchiyama, M.; Yoshida, K.; Onimaru, M.; Onohara, T.; Inoguchi, H.; Kyuragi, R. DVC1-0101 to treat peripheral arterial disease: A Phase I/IIa open-label dose-escalation clinical trial. Mol. Ther. 2013, 21, 707–714. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Kuang, K.; Du, J.; Eymin, B.; Jia, T. Far beyond anti-angiogenesis: Benefits for anti-basicFGF therapy in cancer. Biochim. Biophys. Acta Mol. Cell Res. 2022, 1869, 119253. [Google Scholar] [CrossRef]
- Zahra, F.T.; Sajib, M.S.; Mikelis, C.M. Role of bFGF in Acquired Resistance upon Anti-VEGF Therapy in Cancer. Cancers 2021, 13, 1422. [Google Scholar] [CrossRef] [PubMed]
- Qing-Hua, L.; Wei, Q.; Jian, X.; Feng, F.; Ming-Fang, H. 1-Methoxycarbony-β-carboline from Picrasma quassioides exerts anti-angiogenic properties in HUVECs in vitro and zebrafish embryos in vivo. Chin. J. Nat. Med. 2018, 16, 599–609. [Google Scholar]
- Arunkumar, P.; Dougherty, J.A.; Weist, J.; Kumar, N.; Angelos, M.G.; Powell, H.M.; Khan, M. Sustained release of basic fibroblast growth factor (bFGF) encapsulated polycaprolactone (PCL) microspheres promote angiogenesis in vivo. Nanomaterials 2019, 9, 1037. [Google Scholar] [CrossRef]
- Sajib, S.; Zahra, F.T.; Lionakis, M.S.; German, N.A.; Mikelis, C.M. Mechanisms of angiogenesis in microbe-regulated inflammatory and neoplastic conditions. Angiogenesis 2018, 21, 1–14. [Google Scholar] [CrossRef]
- Akwii, R.G.; Sajib, M.S.; Zahra, F.T.; Mikelis, C.M. Role of Angiopoietin-2 in Vascular Physiology and Pathophysiology. Cells 2019, 8, 471. [Google Scholar] [CrossRef]
- Yu, P.; Wilhelm, K.; Dubrac, A.; Tung, J.K.; Alves, T.C.; Fang, J.S.; Xie, Y.; Zhu, J.; Chen, Z.; De Smet, F. FGF-dependent metabolic control of vascular development. Nature 2017, 545, 224–228. [Google Scholar] [CrossRef] [PubMed]
- Farhat, F.S.; Tfayli, A.; Fakhruddin, N.; Mahfouz, R.; Otrock, Z.K.; Alameddine, R.S.; Awada, A.H.; Shamseddine, A. Expression, prognostic and predictive impact of VEGF and bFGF in non-small cell lung cancer. Crit. Rev. Oncol. Hematol. 2012, 84, 149–160. [Google Scholar] [CrossRef] [PubMed]
- Le, T.B.U.; Vu, T.C.; Ho, R.Z.W.; Prawira, A.; Wang, L.; Goh, B.C.; Huynh, H. Bevacizumab augments the antitumor efficacy of infigratinib in hepatocellular carcinoma. Int. J. Mol. Sci. 2020, 21, 9405. [Google Scholar] [CrossRef]
- Salven, P.; Orpana, A.; Teerenhovi, L.; Joensuu, H. Simultaneous elevation in the serum concentrations of the angiogenic growth factors VEGF and bFGF is an independent predictor of poor prognosis in non-Hodgkin lymphoma: A single-institution study of 200 patients. Blood 2000, 96, 3712–3718. [Google Scholar] [CrossRef]
- Fujimoto, Y.; Yokozeki, T.; Yokoyama, A.; Tabata, Y. Basic fibroblast growth factor enhances proliferation and hepatocyte growth factor expression of feline mesenchymal stem cells. Regen. Ther. 2020, 15, 10–17. [Google Scholar] [CrossRef]
- Boilly, B.; Vercoutter-Edouart, A.S.; Hondermarck, H.; Nurcombe, V.; Le Bourhis, X. FGF signals for cell proliferation and migration through different pathways. Cytokine Growth Factor Rev. 2000, 11, 295–302. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Zhang, Y.; Tian, K.; Xun, C.; Wang, S.; Lv, D. Effects of nerve growth factor and basic fibroblast growth factor dual gene modification on rat bone marrow mesenchymal stem cell differentiation into neuron-like cells in vitro. Mol. Med. Rep. 2016, 13, 49–58. [Google Scholar] [CrossRef]
- Lu, C.; Han, H.D.; Mangala, L.S.; Ali-Fehmi, R.; Newton, C.S.; Ozbun, L.; Armaiz-Pena, G.N.; Hu, W.; Stone, R.L.; Munkarah, A.; et al. Regulation of tumor angiogenesis by EZH2. Cancer Cell 2010, 18, 185–197. [Google Scholar] [CrossRef] [PubMed]
- Hara, F.; Samuel, S.; Liu, J.; Rosen, D.; Langley, R.R.; Naora, H. A homeobox gene related to Drosophila distal-less promotes ovarian tumorigenicity by inducing expression of vascular endothelial growth factor and fibroblast growth factor-2. Am. J. Pathol. 2007, 170, 1594–1606. [Google Scholar] [CrossRef] [PubMed]
- Nissen, L.J.; Cao, R.; Hedlund, E.M.; Wang, Z.; Zhao, X.; Wetterskog, D.; Funa, K.; Brakenhielm, E.; Cao, Y. Angiogenic factors FGF2 and PDGF-BB synergistically promote murine tumor neovascularization and metastasis. J. Clin. Investig. 2007, 117, 2766–2777. [Google Scholar] [CrossRef]
- Raman, J.D.; Mongan, N.P.; Tickoo, S.K.; Boorjian, S.A.; Scherr, D.S.; Gudas, L.J. Increased expression of the polycomb group gene, EZH2, in transitional cell carcinoma of the bladder. Clin. Cancer Res. 2005, 11, 8570–8576. [Google Scholar] [CrossRef]
- Chengye, W.; Yu, T.; Ping, S.; Deguang, S.; Keyun, W.; Yan, W.; Rixin, Z.; Rui, L.; Zhenming, G.; Mingliang, Y.; et al. Metformin reverses bFGF-induced epithelial-mesenchymal transition in HCC cells. Oncotarget 2017, 8, 104247–104257. [Google Scholar] [CrossRef] [PubMed]
- Zheng, H.C. The molecular mechanisms of chemoresistance in cancers. Oncotarget 2017, 8, 59950–59964. [Google Scholar] [CrossRef]
- Pietras, K.; Pahler, J.; Bergers, G.; Hanahan, D. Functions of paracrine PDGF signaling in the proangiogenic tumor stroma revealed by pharmacological targeting. PLoS Med. 2008, 5, e19. [Google Scholar] [CrossRef]
- Carmo, C.R.; Lyons-Lewis, J.; Seckl, M.J.; Costa-Pereira, A.P. A novel requirement for Janus kinases as mediators of drug resistance induced by fibroblast growth factor-2 in human cancer cells. PLoS ONE 2011, 6, e19861. [Google Scholar] [CrossRef]
- Alavi, A.S.; Acevedo, L.; Min, W.; Cheresh, D.A. Chemoresistance of endothelial cells induced by basic fibroblast growth factor depends on Raf-1-mediated inhibition of the proapoptotic kinase, ASK1. Cancer Res. 2007, 67, 2766–2772. [Google Scholar] [CrossRef] [PubMed]
- Song, S.; Wientjes, M.G.; Gan, Y.; Au, J.L. Fibroblast growth factors: An epigenetic mechanism of broad spectrum resistance to anticancer drugs. Proc. Natl. Acad. Sci. USA 2000, 97, 8658–8663. [Google Scholar] [CrossRef]
- Kim, H.R.; Heo, Y.M.; Jeong, K.I.; Kim, Y.M.; Jang, H.L.; Lee, K.Y.; Yeo, C.Y.; Kim, S.H.; Lee, H.K.; Kim, S.R.; et al. FGF-2 inhibits TNF-alpha mediated apoptosis through upregulation of Bcl2-A1 and Bcl-xL in ATDC5 cells. BMB Rep. 2012, 45, 287–292. [Google Scholar] [CrossRef]
- Sie, M.; den Dunnen, W.F.; Lourens, H.J.; Meeuwsen-de Boer, T.G.; Scherpen, F.J.; Zomerman, W.W.; Kampen, K.R.; Hoving, E.W.; de Bont, E.S. Growth-factor-driven rescue to receptor tyrosine kinase (RTK) inhibitors through Akt and Erk phosphorylation in pediatric low grade astrocytoma and ependymoma. PLoS ONE 2015, 10, e0122555. [Google Scholar] [CrossRef]
- Trisolini, E.; Wardighi, D.E.; Giry, M.; Bernardi, P.; Boldorini, R.L.; Mokhtari, K.; Sanson, M. Actionable FGFR1 and BRAF mutations in adult circumscribed gliomas. J. Neurooncol. 2019, 145, 241–245. [Google Scholar] [CrossRef] [PubMed]
- Haley, E.M.; Kim, Y. The role of basic fibroblast growth factor in glioblastoma multiforme and glioblastoma stem cells and in their in vitro culture. Cancer Lett 2014, 346, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Toyoda, K.; Tanaka, K.; Nakagawa, S.; Thuy, D.H.; Ujifuku, K.; Kamada, K.; Hayashi, K.; Matsuo, T.; Nagata, I.; Niwa, M. Initial contact of glioblastoma cells with existing normal brain endothelial cells strengthen the barrier function via fibroblast growth factor 2 secretion: A new in vitro blood-brain barrier model. Cell Mol. Neurobiol. 2013, 33, 489–501. [Google Scholar] [CrossRef] [PubMed]
- Pollard, S.M.; Yoshikawa, K.; Clarke, I.D.; Danovi, D.; Stricker, S.; Russell, R.; Bayani, J.; Head, R.; Lee, M.; Bernstein, M.; et al. Glioma stem cell lines expanded in adherent culture have tumor-specific phenotypes and are suitable for chemical and genetic screens. Cell Stem Cell 2009, 4, 568–580. [Google Scholar] [CrossRef]
- Ronca, R.; Giacomini, A.; Di Salle, E.; Coltrini, D.; Pagano, K.; Ragona, L.; Matarazzo, S.; Rezzola, S.; Maiolo, D.; Torrella, R.; et al. Long-Pentraxin 3 Derivative as a Small-Molecule FGF Trap for Cancer Therapy. Cancer Cell 2015, 28, 225–239. [Google Scholar] [CrossRef] [PubMed]
- Ardizzone, A.; Scuderi, S.A.; Giuffrida, D.; Colarossi, C.; Puglisi, C.; Campolo, M.; Cuzzocrea, S.; Esposito, E.; Paterniti, I. Role of Fibroblast Growth Factors Receptors (FGFRs) in Brain Tumors, Focus on Astrocytoma and Glioblastoma. Cancers 2020, 12, 3825. [Google Scholar] [CrossRef]
- Hatlen, M.A.; Schmidt-Kittler, O.; Sherwin, C.A.; Rozsahegyi, E.; Rubin, N.; Sheets, M.P.; Kim, J.L.; Miduturu, C.; Bifulco, N.; Brooijmans, N.; et al. Acquired On-Target Clinical Resistance Validates FGFR4 as a Driver of Hepatocellular Carcinoma. Cancer Discov. 2019, 9, 1686–1695. [Google Scholar] [CrossRef]
- Kim, R.D.; Sarker, D.; Meyer, T.; Yau, T.; Macarulla, T.; Park, J.W.; Choo, S.P.; Hollebecque, A.; Sung, M.W.; Lim, H.Y.; et al. First-in-Human Phase I Study of Fisogatinib (BLU-554) Validates Aberrant FGF19 Signaling as a Driver Event in Hepatocellular Carcinoma. Cancer Discov. 2019, 9, 1696–1707. [Google Scholar] [CrossRef] [PubMed]
- Sootome, H.; Fujita, H.; Ito, K.; Ochiiwa, H.; Fujioka, Y.; Ito, K.; Miura, A.; Sagara, T.; Ito, S.; Ohsawa, H.; et al. Futibatinib Is a Novel Irreversible FGFR 1-4 Inhibitor That Shows Selective Antitumor Activity against FGFR-Deregulated Tumors. Cancer Res. 2020, 80, 4986–4997. [Google Scholar] [CrossRef]
- Kalyukina, M.; Yosaatmadja, Y.; Middleditch, M.J.; Patterson, A.V.; Smaill, J.B.; Squire, C.J. TAS-120 Cancer Target Binding: Defining Reactivity and Revealing the First Fibroblast Growth Factor Receptor 1 (FGFR1) Irreversible Structure. ChemMedChem 2019, 14, 494–500. [Google Scholar] [CrossRef] [PubMed]
- Meric-Bernstam, F.; Bahleda, R.; Hierro, C.; Sanson, M.; Bridgewater, J.; Arkenau, H.T.; Tran, B.; Kelley, R.K.; Park, J.O.; Javle, M.; et al. Futibatinib, an Irreversible FGFR1-4 Inhibitor, in Patients with Advanced Solid Tumors Harboring FGF/FGFR Aberrations: A Phase I Dose-Expansion Study. Cancer Discov. 2022, 12, 402–415. [Google Scholar] [CrossRef] [PubMed]
- Khabibov, M.; Garifullin, A.; Boumber, Y.; Khaddour, K.; Fernandez, M.; Khamitov, F.; Khalikova, L.; Kuznetsova, N.; Kit, O.; Kharin, L. Signaling pathways and therapeutic approaches in glioblastoma multiforme (Review). Int. J. Oncol. 2022, 60, 5359. [Google Scholar] [CrossRef] [PubMed]
- Kurimoto, M.; Endo, S.; Hirashima, Y.; Nishijima, M.; Takaku, A. Elevated plasma basic fibroblast growth factor in brain tumor patients. Neurol. Med. Chir. 1996, 36, 865–868; discussion 869. [Google Scholar] [CrossRef]
- Shi, H.; Xu, J.; Zhao, R.; Wu, H.; Gu, L.; Chen, Y. FGF2 regulates proliferation, migration, and invasion of ECA109 cells through PI3K/Akt signalling pathway in vitro. Cell Biol. Int. 2016, 40, 524–533. [Google Scholar] [CrossRef]
- Li, Z.; Shimada, Y.; Uchida, S.; Maeda, M.; Kawabe, A.; Mori, A.; Itami, A.; Kano, M.; Watanabe, G.; Imamura, M. TGF-alpha as well as VEGF, PD-ECGF and bFGF contribute to angiogenesis of esophageal squamous cell carcinoma. Int. J. Oncol. 2000, 17, 453–460. [Google Scholar] [CrossRef] [PubMed]
- Heeran, A.B.; McCready, J.; Dunne, M.R.; Donlon, N.E.; Nugent, T.S.; Bhardwaj, A.; Mitchelson, K.A.J.; Buckley, A.M.; Ravi, N.; Roche, H.M.; et al. Opposing Immune-Metabolic Signature in Visceral versus Subcutaneous Adipose Tissue in Patients with Adenocarcinoma of the Oesophagus and the Oesophagogastric Junction. Metabolites 2021, 11, 768. [Google Scholar] [CrossRef]
- Lord, R.V.; Park, J.M.; Wickramasinghe, K.; DeMeester, S.R.; Oberg, S.; Salonga, D.; Singer, J.; Peters, J.H.; Danenberg, K.D.; Demeester, T.R.; et al. Vascular endothelial growth factor and basic fibroblast growth factor expression in esophageal adenocarcinoma and Barrett esophagus. J. Thorac Cardiovasc. Surg. 2003, 125, 246–253. [Google Scholar] [CrossRef]
- Donlon, N.E.; Sheppard, A.; Davern, M.; O’Connell, F.; Phelan, J.J.; Power, R.; Nugent, T.; Dinneen, K.; Aird, J.; Greene, J.; et al. Linking Circulating Serum Proteins with Clinical Outcomes in Esophageal Adenocarcinoma—An Emerging Role for Chemokines. Cancers 2020, 12, 3356. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Zhou, Y.; Li, C.; Xu, S.; Li, M.; Liu, W.; Ma, Y.; Wang, H. The Expression and Prognostic Value of FGF2, FGFR3, and FGFBP1 in Esophageal Squamous Cell Carcinoma. Anal. Cell Pathol. 2020, 2020, 2872479. [Google Scholar] [CrossRef]
- Bilgic, I.; Ozalp, N.; Tez, M.; Koc, M. Serum bFGF concentrations in gastric cancer patients. Bratisl. Lek. Listy 2008, 109, 8–9. [Google Scholar]
- Guo, Z.Y.; Yao, G.D.; Fu, L.P.; Fu, Z.G.; Hou, B. Effect of recombinant human endostatin on the expression of c-Myc and bFGF in mouse gastric cancer cells. Genet. Mol. Res. 2015, 14, 5258–5265. [Google Scholar] [CrossRef] [PubMed]
- Fan, L.; Li, W.; Ying, S.; Shi, L.; Wang, Z.; Chen, G.; Ye, H.; Wu, X.; Wu, J.; Liang, G.; et al. A peptide derivative serves as a fibroblast growth factor 2 antagonist in human gastric cancer. Tumour Biol. 2015, 36, 7233–7241. [Google Scholar] [CrossRef]
- Li, W.; Du, X.; Chen, Q.; Kang, Y.; Xu, C.; Fan, L.; Ye, H.; Ying, S.; Shi, L.; Jin, R.; et al. Peptidomimetic suppresses proliferation and invasion of gastric cancer cells by fibroblast growth factor 2 signaling cascade blockage. Anticancer Drugs 2016, 27, 164–172. [Google Scholar] [CrossRef] [PubMed]
- Gao, X.; Liu, H.; Wu, Q.; Wang, R.; Huang, M.; Ma, Q.; Liu, Y. miRNA-381-3p Functions as a Tumor Suppressor to Inhibit Gastric Cancer by Targeting Fibroblast Growth Factor Receptor-2. Cancer Biother. Radiopharm. 2022. [Google Scholar] [CrossRef]
- Wang, J.; Li, L.; Jiang, M.; Li, Y. MicroRNA-195 inhibits human gastric cancer by directly targeting basic fibroblast growth factor. Clin. Transl. Oncol. 2017, 19, 1320–1328. [Google Scholar] [CrossRef]
- Guo, J.L.; Zheng, S.J.; Li, Y.N.; Jie, W.; Hao, X.B.; Li, T.F.; Xia, L.P.; Mei, W.L.; Huang, F.Y.; Kong, Y.Q.; et al. Toxicarioside A inhibits SGC-7901 proliferation, migration and invasion via NF-kappaB/bFGF signaling. World J. Gastroenterol. 2012, 18, 1602–1609. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Guo, X.B.; Wang, J.S.; Wang, H.C.; Li, L.P. Function of fibroblast growth factor 2 in gastric cancer occurrence and prognosis. Mol. Med. Rep. 2020, 21, 575–582. [Google Scholar] [CrossRef] [PubMed]
- Wang, N.; Chang, L.L. Maspin suppresses cell invasion and migration in gastric cancer through inhibiting EMT and angiogenesis via ITGB1/FAK pathway. Hum. Cell 2020, 33, 663–675. [Google Scholar] [CrossRef] [PubMed]
- Park, D.J.; Yoon, C.; Thomas, N.; Ku, G.Y.; Janjigian, Y.Y.; Kelsen, D.P.; Ilson, D.H.; Goodman, K.A.; Tang, L.H.; Strong, V.E.; et al. Prognostic significance of targetable angiogenic and growth factors in patients undergoing resection for gastric and gastroesophageal junction cancers. Ann. Surg. Oncol. 2014, 21, 1130–1137. [Google Scholar] [CrossRef] [PubMed]
- Yoshikawa, T.; Tsuburaya, A.; Kobayashi, O.; Sairenji, M.; Motohashi, H.; Yanoma, S.; Noguchi, Y. Plasma concentrations of VEGF and bFGF in patients with gastric carcinoma. Cancer Lett. 2000, 153, 7–12. [Google Scholar] [CrossRef] [PubMed]
- Caiado, H.; Conceicao, N.; Tiago, D.; Marreiros, A.; Vicente, S.; Enriquez, J.L.; Vaz, A.M.; Antunes, A.; Guerreiro, H.; Caldeira, P.; et al. Data on the evaluation of FGF2 gene expression in Colorectal Cancer. Data Brief 2020, 31, 105765. [Google Scholar] [CrossRef]
- Hernandez-Balmaseda, I.; Guerra, I.R.; Declerck, K.; Herrera Isidron, J.A.; Perez-Novo, C.; Van Camp, G.; De Wever, O.; Gonzalez, K.; Labrada, M.; Carr, A.; et al. Marine Seagrass Extract of Thalassia testudinum Suppresses Colorectal Tumor Growth, Motility and Angiogenesis by Autophagic Stress and Immunogenic Cell Death Pathways. Mar. Drugs 2021, 19, 52. [Google Scholar] [CrossRef]
- Delle Monache, S.; Cortellini, A.; Parisi, A.; Pulcini, F.; Martellucci, S.; Mei, C.; Danubio, M.E.; Mattei, V.; Angelucci, A.; Ficorella, C. Expression of pro-angiogenic factors as potential biomarkers in experimental models of colon cancer. J. Cancer Res. Clin. Oncol. 2020, 146, 1427–1440. [Google Scholar] [CrossRef]
- Zhu, P.; Wu, Y.; Yang, A.; Fu, X.; Mao, M.; Liu, Z. Catalpol suppressed proliferation, growth and invasion of CT26 colon cancer by inhibiting inflammation and tumor angiogenesis. Biomed Pharm. 2017, 95, 68–76. [Google Scholar] [CrossRef]
- Zhou, J.; Li, Y.; Shi, X.; Hao, S.; Zhang, F.; Guo, Z.; Gao, Y.; Guo, H.; Liu, L. Oridonin inhibits tumor angiogenesis and induces vessel normalization in experimental colon cancer. J. Cancer 2021, 12, 3257–3264. [Google Scholar] [CrossRef]
- Sudha, T.; Mousa, D.S.; El-Far, A.H.; Mousa, S.A. Pomegranate (Punica granatum) Fruit Extract Suppresses Cancer Progression and Tumor Angiogenesis of Pancreatic and Colon Cancer in Chick Chorioallantoic Membrane Model. Nutr. Cancer 2021, 73, 1350–1356. [Google Scholar] [CrossRef]
- Sharma, S.H.; Suresh Kumar, J.; Madhavan, S.; Nagarajan, S. Morin supplementation modulates PERK branch of UPR and mitigates 1,2-dimethylhydrazine-induced angiogenesis and oxidative stress in the colon of experimental rats. Toxicol. Mech. Methods 2020, 30, 306–315. [Google Scholar] [CrossRef]
- Samie, K.A.; Dayer, D.; Eshkiki, Z.S. Human Colon Cancer HT29 Cell Line Treatment with High-Dose L-Ascorbic Acid Results to Reduced Angiogenic Proteins Expression and Elevated Pro-apoptotic Proteins Expression. Curr. Mol. Med. 2022. [Google Scholar] [CrossRef]
- Luo, W.; Yu, Y.; Wang, R.; He, D.; Wang, C.; Zeng, X.; Chen, X.; Tan, X.; Huang, T.; Wu, X. P7 peptides targeting bFGF sensitize colorectal cancer cells to CPT-11. Int. J. Mol. Med. 2014, 33, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Jibiki, N.; Saito, N.; Kameoka, S.; Kobayashi, M. Clinical significance of fibroblast growth factor (FGF) expression in colorectal cancer. Int. Surg. 2014, 99, 493–499. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Xing, L.Q. Basic fibroblast growth factor as a potential biomarker for diagnosing malignant tumor metastasis in women. Oncol. Lett. 2017, 14, 1561–1567. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Yang, F.; Ren, X. Immunotherapy for hepatocellular carcinoma. Drug Discov. Ther. 2015, 9, 363–371. [Google Scholar] [CrossRef]
- Wang, H.; Yang, J.; Zhang, K.; Liu, J.; Li, Y.; Su, W.; Song, N. Advances of Fibroblast Growth Factor/Receptor Signaling Pathway in Hepatocellular Carcinoma and its Pharmacotherapeutic Targets. Front. Pharm. 2021, 12, 650388. [Google Scholar] [CrossRef]
- Li, X.M.; Chen, W.B.; Zhang, J.; Ma, L.F.; Li, Q.; Feng, C.; Yuan, X.H.; Kang, L.Q. Correlation of CT Perfusion Parameters and Vascular Endothelial Growth Factor (VEGF) and Basic Fibroblast Growth Factor (BFGF) in Patients with Primary Liver Cancer. Evid. Based Complement Altern. Med. 2022, 2022, 4548922. [Google Scholar] [CrossRef]
- Liu, D.; Zhang, T.; Chen, X.; Zhang, B.; Wang, Y.; Xie, M.; Ji, X.; Sun, M.; Huang, W.; Xia, L. ONECUT2 facilitates hepatocellular carcinoma metastasis by transcriptionally upregulating FGF2 and ACLY. Cell Death Dis. 2021, 12, 1113. [Google Scholar] [CrossRef]
- Deng, H.; Kan, A.; Lyu, N.; Mu, L.; Han, Y.; Liu, L.; Zhang, Y.; Duan, Y.; Liao, S.; Li, S.; et al. Dual Vascular Endothelial Growth Factor Receptor and Fibroblast Growth Factor Receptor Inhibition Elicits Antitumor Immunity and Enhances Programmed Cell Death-1 Checkpoint Blockade in Hepatocellular Carcinoma. Liver Cancer 2020, 9, 338–357. [Google Scholar] [CrossRef]
- Wei, Y.; Yang, Q.; Zhang, Y.; Zhao, T.; Liu, X.; Zhong, J.; Ma, J.; Chen, Y.; Zhao, C.; Li, J. Plumbagin restrains hepatocellular carcinoma angiogenesis by suppressing the migration and invasion of tumor-derived vascular endothelial cells. Oncotarget 2017, 8, 15230–15241. [Google Scholar] [CrossRef]
- Liu, Q.; Dai, Y. Sorafenib combined with transarterial chemoembolization prolongs survival of patients with advanced hepatocellular carcinoma. J. Buon 2020, 25, 945–951. [Google Scholar] [PubMed]
- Joo, Y.Y.; Jang, J.W.; Lee, S.W.; Yoo, S.H.; Kwon, J.H.; Nam, S.W.; Bae, S.H.; Choi, J.Y.; Yoon, S.K. Circulating pro- and anti-angiogenic factors in multi-stage liver disease and hepatocellular carcinoma progression. Sci. Rep. 2019, 9, 9137. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.S.; Eun, J.W.; Cho, H.J.; Lee, H.Y.; Seo, C.W.; Noh, C.K.; Shin, S.J.; Lee, K.M.; Cho, S.W.; Cheong, J.Y. Effect of Fibroblast Growth Factor-2 and its Receptor Gene Polymorphisms on the Survival of Patients with Hepatitis B Virus-associated Hepatocellular Carcinoma. Anticancer Res. 2019, 39, 2217–2226. [Google Scholar] [CrossRef] [PubMed]
- Tong, C.; Liu, H.; Chen, R.; Zhu, F. The effect of TACE in combination with thalidomide-mediated adjuvant therapy on the levels of VEGF and bFGF in patients with hepatocellular carcinoma. Am. J. Transl. Res. 2021, 13, 5575–5581. [Google Scholar]
- Wang, W.M.; Xu, Y.; Wang, Y.H.; Sun, H.X.; Sun, Y.F.; He, Y.F.; Zhu, Q.F.; Hu, B.; Zhang, X.; Xia, J.L.; et al. HOXB7 promotes tumor progression via bFGF-induced activation of MAPK/ERK pathway and indicated poor prognosis in hepatocellular carcinoma. Oncotarget 2017, 8, 47121–47135. [Google Scholar] [CrossRef]
- Soydal, C.; Araz, M.; Durmaz, M.; Ozkan, E.; Erguder, B.I.; Kucuk, N.O.; Bilgic, S.; Elhan, A.H.; Gecim, I.E. Elevated Angiogenic Factor Levels after Transarterial Radioembolization for Colorectal Cancer Liver Metastases May Predict a Poor Prognosis. Mol. Imaging Radionucl. Ther. 2022, 31, 114–122. [Google Scholar] [CrossRef] [PubMed]
- Lanfredini, S.; Thapa, A.; O’Neill, E. RAS in pancreatic cancer. Biochem. Soc. Trans. 2019, 47, 961–972. [Google Scholar] [CrossRef] [PubMed]
- Yan, C.; Wang, C.; Dong, M.; Liu, S.; Qi, C.; Zhao, Y. RNA interference-mediated silencing of VEGF and bFGF suppresses endostatin secretion in pancreatic carcinoma cells. Oncol. Lett. 2013, 5, 1031–1035. [Google Scholar] [CrossRef]
- Li, J.; Luo, M.; Wang, Y.; Shang, B.; Dong, L. Celecoxib suppresses fibroblast growth factor-2 expression in pancreatic ductal adenocarcinoma PANC-1 cells. Oncol. Rep. 2016, 36, 1345–1352. [Google Scholar] [CrossRef]
- Lee, J.; Lee, J.; Kim, S.J.; Kim, J.H. Quercetin-3-O-glucoside suppresses pancreatic cancer cell migration induced by tumor-deteriorated growth factors in vitro. Oncol. Rep. 2016, 35, 2473–2479. [Google Scholar] [CrossRef]
- Chen, X.; Zhao, H.; Chen, C.; Li, J.; He, J.; Fu, X.; Zhao, H. The HPA/SDC1 axis promotes invasion and metastasis of pancreatic cancer cells by activating EMT via FGF2 upregulation. Oncol. Lett. 2020, 19, 211–220. [Google Scholar] [CrossRef]
- Yako, Y.Y.; Brand, M.; Smith, M.; Kruger, D. Inflammatory cytokines and angiogenic factors as potential biomarkers in South African pancreatic ductal adenocarcinoma patients: A preliminary report. Pancreatology 2017, 17, 438–444. [Google Scholar] [CrossRef]
- Cella, C.A.; Spada, F.; Berruti, A.; Bertolini, F.; Mancuso, P.; Barberis, M.; Pisa, E.; Rubino, M.; Gervaso, L.; Laffi, A.; et al. Addressing the Role of Angiogenesis in Patients with Advanced Pancreatic Neuroendocrine Tumors Treated with Everolimus: A Biological Prospective Analysis of Soluble Biomarkers and Clinical Outcomes. Cancers 2022, 14, 4471. [Google Scholar] [CrossRef] [PubMed]
- Ghaneh, P.; Kawesha, A.; Evans, J.D.; Neoptolemos, J.P. Molecular prognostic markers in pancreatic cancer. J. Hepatobiliary Pancreat. Surg. 2002, 9, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Sano, D.; Myers, J.N. Metastasis of squamous cell carcinoma of the oral tongue. Cancer Metastasis Rev. 2007, 26, 645–662. [Google Scholar] [CrossRef]
- Michi, Y.; Morita, I.; Amagasa, T.; Murota, S. Human oral squamous cell carcinoma cell lines promote angiogenesis via expression of vascular endothelial growth factor and upregulation of KDR/flk-1 expression in endothelial cells. Oral Oncol. 2000, 36, 81–88. [Google Scholar] [CrossRef] [PubMed]
- Forootan, S.S.; Ke, Y.; Jones, A.S.; Helliwell, T.R. Basic fibroblast growth factor and angiogenesis in squamous carcinoma of the tongue. Oral Oncol. 2000, 36, 437–443. [Google Scholar] [CrossRef]
- Mariz, B.; Soares, C.D.; de Carvalho, M.G.F.; Jorge-Junior, J. FGF-2 and FGFR-1 might be independent prognostic factors in oral tongue squamous cell carcinoma. Histopathology 2019, 74, 311–320. [Google Scholar] [CrossRef]
- Huber, L.; Birk, R.; Knuettel, M.; Rotter, N.; Aderhold, C.; Scherl, C.; Lammert, A.; Jungbauer, F.; Kramer, B. FGF Expression in HPV16-positive and -negative SCC after Treatment with Small-molecule Tyrosine Kinase Inhibitors and Everolimus. Anticancer Res. 2020, 40, 5621–5630. [Google Scholar] [CrossRef]
- Harada, K.; Ferdous, T.; Mishima, K. Efficacy of a Novel Oral Chemotherapeutic Agent, TAS-102, against Human Oral Squamous Cell Carcinoma Cells. Anticancer Res. 2021, 41, 6039–6049. [Google Scholar] [CrossRef]
- Khandelwal, A.R.; Moore-Medlin, T.; Ekshyyan, O.; Gu, X.; Abreo, F.; Nathan, C.O. Local and systemic Curcumin C3 complex inhibits 4NQO-induced oral tumorigenesis via modulating FGF-2/FGFR-2 activation. Am. J. Cancer Res. 2018, 8, 2538–2547. [Google Scholar] [PubMed]
- Aytatli, A.; Barlak, N.; Sanli, F.; Caglar, H.O.; Gundogdu, B.; Tatar, A.; Ittmann, M.; Karatas, O.F. AZD4547 targets the FGFR/Akt/SOX2 axis to overcome paclitaxel resistance in head and neck cancer. Cell Oncol. 2022, 45, 41–56. [Google Scholar] [CrossRef]
- Butkiewicz, D.; Gdowicz-Klosok, A.; Krzesniak, M.; Rutkowski, T.; Lasut-Szyszka, B.; Skladowski, K. Germline Variants in Angiogenesis-Related Genes Contribute to Clinical Outcome in Head and Neck Squamous Cell Carcinoma. Cancers 2022, 14, 1844. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Luo, Z.; Qin, Y.; Zhou, Y.; Gong, L.; Huang, J.; Wang, H. Production of bFGF monoclonal antibody and its inhibition of metastasis in Lewis lung carcinoma. Mol. Med. Rep. 2017, 16, 4015–4021. [Google Scholar] [CrossRef]
- Hirsch, F.R.; Scagliotti, G.V.; Mulshine, J.L.; Kwon, R.; Curran, W.J., Jr.; Wu, Y.L.; Paz-Ares, L. Lung cancer: Current therapies and new targeted treatments. Lancet 2017, 389, 299–311. [Google Scholar] [CrossRef]
- Azuma, K.; Kawahara, A.; Sonoda, K.; Nakashima, K.; Tashiro, K.; Watari, K.; Izumi, H.; Kage, M.; Kuwano, M.; Ono, M.; et al. FGFR1 activation is an escape mechanism in human lung cancer cells resistant to afatinib, a pan-EGFR family kinase inhibitor. Oncotarget 2014, 5, 5908–5919. [Google Scholar] [CrossRef]
- Ornitz, D.M.; Itoh, N. The Fibroblast Growth Factor signaling pathway. Wiley Interdiscip. Rev. Dev. Biol. 2015, 4, 215–266. [Google Scholar] [CrossRef] [PubMed]
- Lamouille, S.; Xu, J.; Derynck, R. Molecular mechanisms of epithelial-mesenchymal transition. Nat. Rev. Mol. Cell Biol. 2014, 15, 178–196. [Google Scholar] [CrossRef]
- Preusser, M.; Berghoff, A.S.; Berger, W.; Ilhan-Mutlu, A.; Dinhof, C.; Widhalm, G.; Dieckmann, K.; Wohrer, A.; Hackl, M.; von Deimling, A.; et al. High rate of FGFR1 amplifications in brain metastases of squamous and non-squamous lung cancer. Lung Cancer 2014, 83, 83–89. [Google Scholar] [CrossRef] [PubMed]
- Shirakihara, T.; Horiguchi, K.; Miyazawa, K.; Ehata, S.; Shibata, T.; Morita, I.; Miyazono, K.; Saitoh, M. TGF-beta regulates isoform switching of FGF receptors and epithelial-mesenchymal transition. EMBO J. 2011, 30, 783–795. [Google Scholar] [CrossRef]
- Chaffer, C.L.; Weinberg, R.A. A perspective on cancer cell metastasis. Science 2011, 331, 1559–1564. [Google Scholar] [CrossRef]
- Ciruna, B.; Rossant, J. FGF signaling regulates mesoderm cell fate specification and morphogenetic movement at the primitive streak. Dev. Cell 2001, 1, 37–49. [Google Scholar] [CrossRef]
- Behrens, C.; Lin, H.Y.; Lee, J.J.; Raso, M.G.; Hong, W.K.; Wistuba, I.I.; Lotan, R. Immunohistochemical expression of basic fibroblast growth factor and fibroblast growth factor receptors 1 and 2 in the pathogenesis of lung cancer. Clin. Cancer Res. 2008, 14, 6014–6022. [Google Scholar] [CrossRef]
- Zhang, H.; Ye, Q.; Du, Z.; Huang, M.; Zhang, M.; Tan, H. MiR-148b-3p inhibits renal carcinoma cell growth and pro-angiogenic phenotype of endothelial cell potentially by modulating FGF2. Biomed Pharm. 2018, 107, 359–367. [Google Scholar] [CrossRef]
- Xu, M.; Gu, M.; Zhang, K.; Zhou, J.; Wang, Z.; Da, J. miR-203 inhibition of renal cancer cell proliferation, migration and invasion by targeting of FGF2. Diagn. Pathol. 2015, 10, 24. [Google Scholar] [CrossRef] [PubMed]
- Matsuki, M.; Adachi, Y.; Ozawa, Y.; Kimura, T.; Hoshi, T.; Okamoto, K.; Tohyama, O.; Mitsuhashi, K.; Yamaguchi, A.; Matsui, J.; et al. Targeting of tumor growth and angiogenesis underlies the enhanced antitumor activity of lenvatinib in combination with everolimus. Cancer Sci. 2017, 108, 763–771. [Google Scholar] [CrossRef] [PubMed]
- Horstmann, M.; Merseburger, A.S.; von der Heyde, E.; Serth, J.; Wegener, G.; Mengel, M.; Feil, G.; Hennenlotter, J.; Nagele, U.; Anastasiadis, A.; et al. Correlation of bFGF expression in renal cell cancer with clinical and histopathological features by tissue microarray analysis and measurement of serum levels. J. Cancer Res. Clin. Oncol. 2005, 131, 715–722. [Google Scholar] [CrossRef] [PubMed]
- Su, N.; Jin, M.; Chen, L. Role of FGF/FGFR signaling in skeletal development and homeostasis: Learning from mouse models. Bone Res. 2014, 2, 14003. [Google Scholar] [CrossRef] [PubMed]
- Ornitz, D.M.; Marie, P.J. Fibroblast growth factor signaling in skeletal development and disease. Genes Dev. 2015, 29, 1463–1486. [Google Scholar] [CrossRef]
- Labanca, E.; Vazquez, E.S.; Corn, P.G.; Roberts, J.M.; Wang, F.; Logothetis, C.J.; Navone, N.M. Fibroblast growth factors signaling in bone metastasis. Endocr. Relat. Cancer 2020, 27, R255–R265. [Google Scholar] [CrossRef]
- Xiao, L.; Liu, P.; Li, X.; Doetschman, T.; Coffin, J.D.; Drissi, H.; Hurley, M.M. Exported 18-kDa isoform of fibroblast growth factor-2 is a critical determinant of bone mass in mice. J. Biol. Chem. 2009, 284, 3170–3182. [Google Scholar] [CrossRef]
- Homer-Bouthiette, C.; Doetschman, T.; Xiao, L.; Hurley, M.M. Knockout of nuclear high molecular weight FGF2 isoforms in mice modulates bone and phosphate homeostasis. J. Biol. Chem. 2014, 289, 36303–36314. [Google Scholar] [CrossRef] [PubMed]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer Statistics, 2017. CA Cancer J. Clin. 2017, 67, 7–30. [Google Scholar] [CrossRef]
- Tsubaki, M.; Yamazoe, Y.; Yanae, M.; Satou, T.; Itoh, T.; Kaneko, J.; Kidera, Y.; Moriyama, K.; Nishida, S. Blockade of the Ras/MEK/ERK and Ras/PI3K/Akt pathways by statins reduces the expression of bFGF, HGF, and TGF-beta as angiogenic factors in mouse osteosarcoma. Cytokine 2011, 54, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Soriano, O.; Alcon-Perez, M.; Vicente-Manzanares, M.; Castellano, E. The Crossroads between RAS and RHO Signaling Pathways in Cellular Transformation, Motility and Contraction. Genes 2021, 12, 819. [Google Scholar] [CrossRef] [PubMed]
- Hatton, J.P.; Pooran, M.; Li, C.F.; Luzzio, C.; Hughes-Fulford, M. A short pulse of mechanical force induces gene expression and growth in MC3T3-E1 osteoblasts via an ERK 1/2 pathway. J. Bone Min. Res. 2003, 18, 58–66. [Google Scholar] [CrossRef]
- Chattopadhyay, N.; MacLeod, R.J.; Tfelt-Hansen, J.; Brown, E.M. 1alpha,25(OH)2-vitamin D3 inhibits HGF synthesis and secretion from MG-63 human osteosarcoma cells. Am. J. Physiol. Endocrinol. Metab. 2003, 284, E219–E227. [Google Scholar] [CrossRef]
- Ria, R.; Prete, F.; Melaccio, A.; Di Meo, G.; Saltarella, I.; Solimando, A.G.; Gurrado, A.; Ferraro, V.; Pasculli, A.; Sgaramella, L.I.; et al. Effect of thyroidectomy on circulating angiogenic cytokines in papillary thyroid carcinoma and benign goiter: Potential for new biomarkers? Surgery 2021, 169, 27–33. [Google Scholar] [CrossRef]
- Xu, Y.; Han, Y.F.; Ye, B.; Zhang, Y.L.; Dong, J.D.; Zhu, S.J.; Chen, J. miR-27b-3p is Involved in Doxorubicin Resistance of Human Anaplastic Thyroid Cancer Cells via Targeting Peroxisome Proliferator-Activated Receptor Gamma. Basic Clin. Pharm. Toxicol. 2018, 123, 670–677. [Google Scholar] [CrossRef]
- Yin, Y.; Hong, S.; Yu, S.; Huang, Y.; Chen, S.; Liu, Y.; Zhang, Q.; Li, Y.; Xiao, H. MiR-195 Inhibits Tumor Growth and Metastasis in Papillary Thyroid Carcinoma Cell Lines by Targeting CCND1 and FGF2. Int. J. Endocrinol. 2017, 2017, 6180425. [Google Scholar] [CrossRef]
- Wu, D.; Tian, W.; Li, J.; Zhang, Q.; Wang, H.; Zhang, L.; Xie, Z.; Ji, A.; Li, Y. Peptide P11 suppresses the growth of human thyroid carcinoma by inhibiting the PI3K/AKT/mTOR signaling pathway. Mol. Biol. Rep. 2019, 46, 2665–2678. [Google Scholar] [CrossRef] [PubMed]
- Rudzinska, M.; Mikula, M.; Arczewska, K.D.; Gajda, E.; Sabalinska, S.; Stepien, T.; Ostrowski, J.; Czarnocka, B. Transcription Factor Prospero Homeobox 1 (PROX1) as a Potential Angiogenic Regulator of Follicular Thyroid Cancer Dissemination. Int. J. Mol. Sci. 2019, 20, 5619. [Google Scholar] [CrossRef] [PubMed]
- Jia, Z.Y.; Wu, X.L.; Zhang, Y.H.; Ma, B.L.; Ma, F.C. The correlation between ultrasonographic features, bFGF, and the local invasiveness of thyroid papillary carcinoma. Medicine 2020, 99, e20644. [Google Scholar] [CrossRef]
- Chikazawa, M.; Inoue, K.; Fukata, S.; Karashima, T.; Shuin, T. Expression of angiogenesis-related genes regulates different steps in the process of tumor growth and metastasis in human urothelial cell carcinoma of the urinary bladder. Pathobiology 2008, 75, 335–345. [Google Scholar] [CrossRef]
- Gazzaniga, P.; Gradilone, A.; de Berardinis, E.; Sciarra, A.; Cristini, C.; Naso, G.; di Silverio, F.; Frati, L.; Agliano, A.M. A chemosensitivity test to individualize intravesical treatment for non-muscle-invasive bladder cancer. BJU Int. 2009, 104, 184–188. [Google Scholar] [CrossRef] [PubMed]
- Inoue, K.; Slaton, J.W.; Karashima, T.; Yoshikawa, C.; Shuin, T.; Sweeney, P.; Millikan, R.; Dinney, C.P. The prognostic value of angiogenesis factor expression for predicting recurrence and metastasis of bladder cancer after neoadjuvant chemotherapy and radical cystectomy. Clin. Cancer Res. 2000, 6, 4866–4873. [Google Scholar]
- Chen, Y.; Zhu, G.; Wu, K.; Gao, Y.; Zeng, J.; Shi, Q.; Guo, P.; Wang, X.; Chang, L.S.; Li, L.; et al. FGF2-mediated reciprocal tumor cell-endothelial cell interplay contributes to the growth of chemoresistant cells: A potential mechanism for superficial bladder cancer recurrence. Tumour Biol. 2016, 37, 4313–4321. [Google Scholar] [CrossRef]
- Tanaka, N.; Miyajima, A.; Kosaka, T.; Miyazaki, Y.; Shirotake, S.; Shirakawa, H.; Kikuchi, E.; Oya, M. Acquired platinum resistance enhances tumour angiogenesis through angiotensin II type 1 receptor in bladder cancer. Br. J. Cancer 2011, 105, 1331–1337. [Google Scholar] [CrossRef]
- Youssef, R.F.; Kapur, P.; Mosbah, A.; Abol-Enein, H.; Ghoneim, M.; Lotan, Y. Role of fibroblast growth factor in squamous cell carcinoma of the bladder: Prognostic biomarker and potential therapeutic target. Urol. Oncol. 2015, 33, 111.e1–111.e17. [Google Scholar] [CrossRef]
- Szarvas, T.; Jager, T.; Laszlo, V.; Kramer, G.; Klingler, H.C.; vom Dorp, F.; Romics, I.; Ergun, S.; Rubben, H. Circulating angiostatin, bFGF, and Tie2/TEK levels and their prognostic impact in bladder cancer. Urology 2012, 80, 737.e13–737.e18. [Google Scholar] [CrossRef]
- El-Mouallem, N.; Paul, A.K. Immune Checkpoint Inhibitors for Urothelial Cancer: An Update on New Therapies. Fed. Pract. 2018, 35, S62–S64. [Google Scholar]
- Tomlinson, D.C.; L’Hote, C.G.; Kennedy, W.; Pitt, E.; Knowles, M.A. Alternative splicing of fibroblast growth factor receptor 3 produces a secreted isoform that inhibits fibroblast growth factor-induced proliferation and is repressed in urothelial carcinoma cell lines. Cancer Res. 2005, 65, 10441–10449. [Google Scholar] [CrossRef]
- Knowles, M.A. Novel therapeutic targets in bladder cancer: Mutation and expression of FGF receptors. Future Oncol. 2008, 4, 71–83. [Google Scholar] [CrossRef] [PubMed]
- Van Rhijn, B.W.; Montironi, R.; Zwarthoff, E.C.; Jobsis, A.C.; van der Kwast, T.H. Frequent FGFR3 mutations in urothelial papilloma. J. Pathol. 2002, 198, 245–251. [Google Scholar] [CrossRef]
- Gravas, S.; Bosinakou, I.; Kehayas, P.; Giannopoulos, A. Urinary basic fibroblast growth factor in bladder cancer patients. Histopathological correlation and clinical potential. Urol. Int. 2004, 73, 173–177. [Google Scholar] [CrossRef] [PubMed]
- Veltman, J.A.; Fridlyand, J.; Pejavar, S.; Olshen, A.B.; Korkola, J.E.; DeVries, S.; Carroll, P.; Kuo, W.L.; Pinkel, D.; Albertson, D.; et al. Array-based comparative genomic hybridization for genome-wide screening of DNA copy number in bladder tumors. Cancer Res. 2003, 63, 2872–2880. [Google Scholar]
- Perez-Jacoiste Asin, M.A.; Fernandez-Ruiz, M.; Lopez-Medrano, F.; Lumbreras, C.; Tejido, A.; San Juan, R.; Arrebola-Pajares, A.; Lizasoain, M.; Prieto, S.; Aguado, J.M. Bacillus Calmette-Guerin (BCG) infection following intravesical BCG administration as adjunctive therapy for bladder cancer: Incidence, risk factors, and outcome in a single-institution series and review of the literature. Medicine 2014, 93, 236–254. [Google Scholar] [CrossRef] [PubMed]
- Sylvester, R.J.; van der Meijden, A.P.; Witjes, J.A.; Kurth, K. Bacillus calmette-guerin versus chemotherapy for the intravesical treatment of patients with carcinoma in situ of the bladder: A meta-analysis of the published results of randomized clinical trials. J. Urol. 2005, 174, 86–91. [Google Scholar] [CrossRef]
- Gregg, J.R.; McCormick, B.; Wang, L.; Cohen, P.; Sun, D.; Penson, D.F.; Smith, J.A.; Clark, P.E.; Cookson, M.S.; Barocas, D.A.; et al. Short term complications from transurethral resection of bladder tumor. Can. J. Urol. 2016, 23, 8198–8203. [Google Scholar]
- Serretta, V.; Pavone, C.; Allegro, R.; Vella, M.; Sanguedolce, R.; Porcasi, R.; Morello, V.; Tomasino, R.M.; Pavone-Macaluso, M. Correlation between GP-170 expression, prognosis, and chemoresistance of superficial bladder carcinoma. J. Cancer Res. Clin. Oncol. 2003, 129, 472–476. [Google Scholar] [CrossRef]
- Martinez-Torrecuadrada, J.; Cifuentes, G.; Lopez-Serra, P.; Saenz, P.; Martinez, A.; Casal, J.I. Targeting the extracellular domain of fibroblast growth factor receptor 3 with human single-chain Fv antibodies inhibits bladder carcinoma cell line proliferation. Clin. Cancer Res. 2005, 11, 6280–6290. [Google Scholar] [CrossRef]
- Nakamoto, T.; Chang, C.S.; Li, A.K.; Chodak, G.W. Basic fibroblast growth factor in human prostate cancer cells. Cancer Res. 1992, 52, 571–577. [Google Scholar]
- Sinowatz, F.; Schams, D.; Einspanier, R.; Arnold, G.; Pfeffer, M.; Temmim-Baker, L.; Amselgruber, W.; Plendl, J. Cellular localization of fibroblast growth factor 2 (FGF-2) in benign prostatic hyperplasia. Histol. Histopathol. 2000, 15, 475–481. [Google Scholar] [CrossRef] [PubMed]
- Giri, D.; Ittmann, M. Interleukin-8 is a paracrine inducer of fibroblast growth factor 2, a stromal and epithelial growth factor in benign prostatic hyperplasia. Am. J. Pathol. 2001, 159, 139–147. [Google Scholar] [CrossRef] [PubMed]
- Pecqueux, C.; Arslan, A.; Heller, M.; Falkenstein, M.; Kaczorowski, A.; Tolstov, Y.; Sultmann, H.; Grullich, C.; Herpel, E.; Duensing, A.; et al. FGF-2 is a driving force for chromosomal instability and a stromal factor associated with adverse clinico-pathological features in prostate cancer. Urol. Oncol. 2018, 36, 365.e15–365.e26. [Google Scholar] [CrossRef]
- Teishima, J.; Hayashi, T.; Nagamatsu, H.; Shoji, K.; Shikuma, H.; Yamanaka, R.; Sekino, Y.; Goto, K.; Inoue, S.; Matsubara, A. Fibroblast Growth Factor Family in the Progression of Prostate Cancer. J. Clin. Med. 2019, 8, 183. [Google Scholar] [CrossRef] [PubMed]
- Strohmeyer, D.; Strauss, F.; Rossing, C.; Roberts, C.; Kaufmann, O.; Bartsch, G.; Effert, P. Expression of bFGF, VEGF and c-met and their correlation with microvessel density and progression in prostate carcinoma. Anticancer Res. 2004, 24, 1797–1804. [Google Scholar]
- Gravdal, K.; Halvorsen, O.J.; Haukaas, S.A.; Akslen, L.A. Expression of bFGF/FGFR-1 and vascular proliferation related to clinicopathologic features and tumor progress in localized prostate cancer. Virchows Arch. 2006, 448, 68–74. [Google Scholar] [CrossRef]
- Thomson, A.A.; Marker, P.C. Branching morphogenesis in the prostate gland and seminal vesicles. Differentiation 2006, 74, 382–392. [Google Scholar] [CrossRef]
- Giacomini, A.; Chiodelli, P.; Matarazzo, S.; Rusnati, M.; Presta, M.; Ronca, R. Blocking the FGF/FGFR system as a “two-compartment” antiangiogenic/antitumor approach in cancer therapy. Pharm. Res. 2016, 107, 172–185. [Google Scholar] [CrossRef] [PubMed]
- Hotchkiss, K.A.; Ashton, A.W.; Mahmood, R.; Russell, R.G.; Sparano, J.A.; Schwartz, E.L. Inhibition of endothelial cell function in vitro and angiogenesis in vivo by docetaxel (Taxotere): Association with impaired repositioning of the microtubule organizing center. Mol Cancer Ther. 2002, 1, 1191–1200. [Google Scholar] [PubMed]
- Corn, P.G. The tumor microenvironment in prostate cancer: Elucidating molecular pathways for therapy development. Cancer Manag. Res. 2012, 4, 183–193. [Google Scholar] [CrossRef]
- Dubrovska, A.; Elliott, J.; Salamone, R.J.; Kim, S.; Aimone, L.J.; Walker, J.R.; Watson, J.; Sauveur-Michel, M.; Garcia-Echeverria, C.; Cho, C.Y.; et al. Combination therapy targeting both tumor-initiating and differentiated cell populations in prostate carcinoma. Clin. Cancer Res. 2010, 16, 5692–5702. [Google Scholar] [CrossRef]
- Cenni, E.; Perut, F.; Granchi, D.; Avnet, S.; Amato, I.; Brandi, M.L.; Giunti, A.; Baldini, N. Inhibition of angiogenesis via FGF-2 blockage in primitive and bone metastatic renal cell carcinoma. Anticancer Res. 2007, 27, 315–319. [Google Scholar]
- Rusnati, M.; Presta, M. Fibroblast growth factors/fibroblast growth factor receptors as targets for the development of anti-angiogenesis strategies. Curr. Pharm. Des. 2007, 13, 2025–2044. [Google Scholar] [CrossRef]
- Meyer, G.E.; Yu, E.; Siegal, J.A.; Petteway, J.C.; Blumenstein, B.A.; Brawer, M.K. Serum basic fibroblast growth factor in men with and without prostate carcinoma. Cancer 1995, 76, 2304–2311. [Google Scholar] [CrossRef] [PubMed]
- Dumas, A.; Vaz Luis, I.; Bovagnet, T.; El Mouhebb, M.; Di Meglio, A.; Pinto, S.; Charles, C.; Dauchy, S.; Delaloge, S.; Arveux, P.; et al. Impact of Breast Cancer Treatment on Employment: Results of a Multicenter Prospective Cohort Study (CANTO). J. Clin. Oncol. 2020, 38, 734–743. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Tang, P.M.K.; Zhou, Y.; Cheng, A.S.L.; Yu, J.; Kang, W.; To, K.F. Targeting the Oncogenic FGF-FGFR Axis in Gastric Carcinogenesis. Cells 2019, 8, 637. [Google Scholar] [CrossRef]
- Gartside, M.G.; Chen, H.; Ibrahimi, O.A.; Byron, S.A.; Curtis, A.V.; Wellens, C.L.; Bengston, A.; Yudt, L.M.; Eliseenkova, A.V.; Ma, J.; et al. Loss-of-function fibroblast growth factor receptor-2 mutations in melanoma. Mol. Cancer Res. 2009, 7, 41–54. [Google Scholar] [CrossRef] [PubMed]
- Parish, A.; Schwaederle, M.; Daniels, G.; Piccioni, D.; Fanta, P.; Schwab, R.; Shimabukuro, K.; Parker, B.A.; Helsten, T.; Kurzrock, R. Fibroblast growth factor family aberrations in cancers: Clinical and molecular characteristics. Cell Cycle 2015, 14, 2121–2128. [Google Scholar] [CrossRef] [PubMed]
- DiGiacomo, J.W.; Godet, I.; Trautmann-Rodriguez, M.; Gilkes, D.M. Extracellular Matrix-Bound FGF2 Mediates Estrogen Receptor Signaling and Therapeutic Response in Breast Cancer. Mol. Cancer Res. 2021, 19, 136–149. [Google Scholar] [CrossRef]
- Roberts, P.J.; Der, C.J. Targeting the Raf-MEK-ERK mitogen-activated protein kinase cascade for the treatment of cancer. Oncogene 2007, 26, 3291–3310. [Google Scholar] [CrossRef]
- Shee, K.; Yang, W.; Hinds, J.W.; Hampsch, R.A.; Varn, F.S.; Traphagen, N.A.; Patel, K.; Cheng, C.; Jenkins, N.P.; Kettenbach, A.N.; et al. Therapeutically targeting tumor microenvironment-mediated drug resistance in estrogen receptor-positive breast cancer. J. Exp. Med. 2018, 215, 895–910. [Google Scholar] [CrossRef] [PubMed]
- Faridi, A.; Rudlowski, C.; Biesterfeld, S.; Schuh, S.; Rath, W.; Schroder, W. Long-term follow-up and prognostic significance of angiogenic basic fibroblast growth factor (bFGF) expression in patients with breast cancer. Pathol. Res. Pr. 2002, 198, 1–5. [Google Scholar] [CrossRef]
- Jemal, A.; Siegel, R.; Ward, E.; Murray, T.; Xu, J.; Thun, M.J. Cancer statistics, 2007. CA Cancer J. Clin. 2007, 57, 43–66. [Google Scholar] [CrossRef]
- Wang, J.; Zhao, H.; Zheng, L.; Zhou, Y.; Wu, L.; Xu, Y.; Zhang, X.; Yan, G.; Sheng, H.; Xin, R.; et al. FGF19/SOCE/NFATc2 signaling circuit facilitates the self-renewal of liver cancer stem cells. Theranostics 2021, 11, 5045–5060. [Google Scholar] [CrossRef]
- Mateus, D.; Wiedlocha, A. FGF-FGFR signaling promotes the development of invasive cervical cancer. FEBS J. 2022, 289, 3419–3421. [Google Scholar] [CrossRef]
- Servetto, A.; Kollipara, R.; Formisano, L.; Lin, C.C.; Lee, K.M.; Sudhan, D.R.; Gonzalez-Ericsson, P.I.; Chatterjee, S.; Guerrero-Zotano, A.; Mendiratta, S.; et al. Nuclear FGFR1 Regulates Gene Transcription and Promotes Antiestrogen Resistance in ER(+) Breast Cancer. Clin. Cancer Res. 2021, 27, 4379–4396. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Fan, X.; Zhang, Q.; Shi, X.; Xu, G.; Zou, C. Cancer-associated fibroblasts secrete FGF-1 to promote ovarian proliferation, migration, and invasion through the activation of FGF-1/FGFR4 signaling. Tumor Biol. 2017, 39, 1010428317712592. [Google Scholar] [CrossRef]
- Narla, S.T.; Lee, Y.W.; Benson, C.A.; Sarder, P.; Brennand, K.J.; Stachowiak, E.K.; Stachowiak, M.K. Common developmental genome deprogramming in schizophrenia—Role of Integrative Nuclear FGFR1 Signaling (INFS). Schizophr. Res. 2017, 185, 17–32. [Google Scholar] [CrossRef] [PubMed]
- Terranova, C.; Narla, S.T.; Lee, Y.W.; Bard, J.; Parikh, A.; Stachowiak, E.K.; Tzanakakis, E.S.; Buck, M.J.; Birkaya, B.; Stachowiak, M.K. Global Developmental Gene Programing Involves a Nuclear Form of Fibroblast Growth Factor Receptor-1 (FGFR1). PLoS ONE 2015, 10, e0123380. [Google Scholar] [CrossRef] [PubMed]
- Li, T.; Jiang, S. Effect of bFGF on invasion of ovarian cancer cells through the regulation of Ets-1 and urokinase-type plasminogen activator. Pharm. Biol. 2010, 48, 161–165. [Google Scholar] [CrossRef]
- Aggarwal, C.; Redman, M.W.; Lara, P.N., Jr.; Borghaei, H.; Hoffman, P.; Bradley, J.D.; Newman, A.J., III; Feldman, M.J.; Minichiello, K.; Miao, J.; et al. SWOG S1400D (NCT02965378), a Phase II Study of the Fibroblast Growth Factor Receptor Inhibitor AZD4547 in Previously Treated Patients with Fibroblast Growth Factor Pathway-Activated Stage IV Squamous Cell Lung Cancer (Lung-MAP Substudy). J. Thorac. Oncol. 2019, 14, 1847–1852. [Google Scholar] [CrossRef]
- Bibeau, K.; Feliz, L.; Lihou, C.F.; Ren, H.; Abou-Alfa, G.K. Progression-Free Survival in Patients with Cholangiocarcinoma with or without FGF/FGFR Alterations: A FIGHT-202 Post Hoc Analysis of Prior Systemic Therapy Response. JCO Precis. Oncol. 2022, 6, e2100414. [Google Scholar] [CrossRef] [PubMed]
- Subbiah, V.; Iannotti, N.O.; Gutierrez, M.; Smith, D.C.; Feliz, L.; Lihou, C.F.; Tian, C.; Silverman, I.M.; Ji, T.; Saleh, M. FIGHT-101, a first-in-human study of potent and selective FGFR 1-3 inhibitor pemigatinib in pan-cancer patients with FGF/FGFR alterations and advanced malignancies. Ann. Oncol. 2022, 33, 522–533. [Google Scholar] [CrossRef]
- Goyal, L.; Meric-Bernstam, F.; Hollebecque, A.; Valle, J.W.; Morizane, C.; Karasic, T.B.; Abrams, T.A.; Furuse, J.; Kelley, R.K.; Cassier, P.A.; et al. Futibatinib for FGFR2-Rearranged Intrahepatic Cholangiocarcinoma. N. Engl. J. Med. 2023, 388, 228–239. [Google Scholar] [CrossRef] [PubMed]
- Konecny, G.E.; Finkler, N.; Garcia, A.A.; Lorusso, D.; Lee, P.S.; Rocconi, R.P.; Fong, P.C.; Squires, M.; Mishra, K.; Upalawanna, A.; et al. Second-line dovitinib (TKI258) in patients with FGFR2-mutated or FGFR2-non-mutated advanced or metastatic endometrial cancer: A non-randomised, open-label, two-group, two-stage, phase 2 study. Lancet Oncol. 2015, 16, 686–694. [Google Scholar] [CrossRef]
- Wainberg, Z.A.; Enzinger, P.C.; Kang, Y.K.; Qin, S.; Yamaguchi, K.; Kim, I.H.; Saeed, A.; Oh, S.C.; Li, J.; Turk, H.M.; et al. Bemarituzumab in patients with FGFR2b-selected gastric or gastro-oesophageal junction adenocarcinoma (FIGHT): A randomised, double-blind, placebo-controlled, phase 2 study. Lancet Oncol. 2022, 23, 1430–1440. [Google Scholar] [CrossRef] [PubMed]
- Liow, E.; Howard, N.; Jung, C.H.; Pope, B.; Campbell, B.K.; Nguyen, A.; Kerger, M.; Ruddle, J.B.; Anton, A.; Thomas, B.; et al. Phase 2 Study of Neoadjuvant FGFR Inhibition and Androgen Deprivation Therapy Prior to Prostatectomy. Clin. Genitourin Cancer 2022, 20, 452–458. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.J.; Kim, H.S.; Park, S.H.; Kim, B.S.; Kim, K.H.; Lee, H.J.; Song, H.S.; Shin, D.Y.; Lee, H.Y.; Kim, H.G.; et al. Phase II Study of Dovitinib in Patients with Castration-Resistant Prostate Cancer (KCSG-GU11-05). Cancer Res. Treat. 2018, 50, 1252–1259. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.B.; Chesney, J.; Robinson, D.; Gardner, H.; Shi, M.M.; Kirkwood, J.M. Phase I/II and pharmacodynamic study of dovitinib (TKI258), an inhibitor of fibroblast growth factor receptors and VEGF receptors, in patients with advanced melanoma. Clin. Cancer Res. 2011, 17, 7451–7461. [Google Scholar] [CrossRef] [PubMed]
- Lee, E.Q.; Muzikansky, A.; Duda, D.G.; Gaffey, S.; Dietrich, J.; Nayak, L.; Chukwueke, U.N.; Beroukhim, R.; Doherty, L.; Laub, C.K.; et al. Phase II trial of ponatinib in patients with bevacizumab-refractory glioblastoma. Cancer Med. 2019, 8, 5988–5994. [Google Scholar] [CrossRef] [PubMed]
| Cancer Type | First Author | Title | Therapeutic Treatment | References |
|---|---|---|---|---|
| Brain | Meric-Bernstam et al. (2022) | “Futibatinib, an Irreversible FGFR1–4 Inhibitor, in Patients with Advanced Solid Tumors Harboring FGF/FGFR Aberrations: A Phase I Dose-Expansion Study.” | Fisogatinib and Futibatinib could be two effective and safe compounds capable of improving the CNS neoplastic conditions. | [74] |
| Khabibov et al. (2022) | “Signaling pathways and therapeutic approaches in glioblastoma multiforme.” | [75] | ||
| Esophageal | Shi et al. (2016) | “FGF2 regulates proliferation, migration, and invasion of ECA109 cells through PI3K/Akt signalling pathway in vitro.” | LY294002, a PI3K inhibitor, as a therapeutic strategy for alleviating the tumorigenic effects of bFGF. | [77] |
| Gastrointestinal | Fan et al. (2015) | “A peptide derivative serves as a fibroblast growth factor 2 antagonist in human gastric cancer.” | P29 and P32 suppressed the bFGF-induced proliferation of GC cells and inhibited the activation of AKT and Erk1/2 cascades. | [85] |
| Li et al. (2016) | “Peptidomimetic suppresses proliferation and invasion of gastric cancer cells by fibroblast growth factor 2 signaling cascade blockage.” | [86] | ||
| Gao et al. (2022) | “miRNA-381-3p Functions as a Tumor Suppressor to Inhibit Gastric Cancer by Targeting Fibroblast Growth Factor Receptor-2.” | MiR-381-3p and miR-195 target bFGF, decreasing tumorigenesis of GC. | [87] | |
| Wang et al. (2020) | “MicroRNA-195 inhibits human gastric cancer by directly targeting basic fibroblast growth factor.” | [88] | ||
| Guo et al. (2012) | “Toxicarioside A inhibits SGC-7901 proliferation, migration and invasion via NF-kappaB/bFGF signaling.” | Toxicarioside A reduced cell viability, cell growth, cell migration, and invasion in SGC-7901 GC cells by NF-κB/bFGF/FGFR1 signaling. | [89] | |
| Zhu et. al. (2017) | “Catalpol suppressed proliferation, growth and invasion of CT26 colon cancer by inhibiting inflammation and tumor angiogenesis.” | Catalpol blocked cell proliferation, growth, and invasion of CT26 lines. | [97] | |
| Zhou et al. (2021) | “Oridonin inhibits tumor angiogenesis and induces vessel normalization in experimental colon cancer.” | Oridonin controlled JAK2/STAT3 signaling and angiogenesis-related factors, including bFGF. | [98] | |
| CRC | Sudha et al. (2021) | “Pomegranate (Punica granatum) Fruit Extract Suppresses Cancer Progression and Tumor Angiogenesis of Pancreatic and Colon Cancer in Chick Chorioallantoic Membrane Model.” | Morin and pomegranate, respectively, decreased bFGF levels in vivo and in colo205 cell lines. | [99] |
| Sharma et al. (2020) | “Morin supplementation modulates PERK branch of UPR and mitigates 1,2-dimethylhydrazine-induced angiogenesis and oxidative stress in the colon of experimental rats.” | [100] | ||
| Liver | Wei et al. (2017) | “Plumbagin restrains hepatocellular carcinoma angiogenesis by suppressing the migration and invasion of tumor-derived vascular endothelial cells.” | Plumbagin suppresses angiogenesis pathways such as PI3K-Akt, VEGF/KDR, and Angiopoietins/Tie2, as well as angiogenic factors such as bFGF. | [110] |
| Liu et al. (2020) | “Sorafenib combined with transarterial chemoembolization prolongs survival of patients with advanced hepatocellular carcinoma.” | Sorafenib-treated HCC patients evidently revealed lower levels of VEGF, bFGF, and AFP in serum. | [111] | |
| Tong et al. (2021) | “The effect of TACE in combination with thalidomide-mediated adjuvant therapy on the levels of VEGF and bFGF in patients with hepatocellular carcinoma.” | Combined therapies of TACE with thalidomide downregulated VEGF and bFGF levels. | [114] | |
| Pancreatic | Li et al. (2016) | “Celecoxib suppresses fibroblast growth factor-2 expression in pancreatic ductal adenocarcinoma PANC-1 cells.” | Quercetin-3-O-glucoside and Celecoxib acted as bFGF inhibitors, avoiding the expansion of local metastasis. | [119] |
| Lee et al. (2016) | “Quercetin-3-O-glucoside suppresses pancreatic cancer cell migration induced by tumor-deteriorated growth factors in vitro.” | [120] | ||
| Oral cavity | Khandelwal et al. (2018) | “Local and systemic Curcumin C3 complex inhibits 4NQO-induced oral tumorigenesis via modulating FGF-2/FGFR-2 activation.” | Curcumin inhibited 4NQO-induced tumorigenesis via modulation of the bFGF/FGFR-2 axis. | [131] |
| Aytatli et al. (2022) | “AZD4547 targets the FGFR/Akt/SOX2 axis to overcome paclitaxel resistance in head and neck cancer.” | AZD4547 targeted the FGFR/Akt/SOX2 axis to overcome paclitaxel resistance in HNSCC. | [132] | |
| Lung | Yang et al. (2017) | “Production of bFGF monoclonal antibody and its inhibition of metastasis in Lewis lung carcinoma.” | mAb-E12 inhibited CLL metastasis spreading. | [134] |
| Kidney | Zhang et al. (2018) | “MiR-148b-3p inhibits renal carcinoma cell growth and pro-angiogenic phenotype of endothelial cell potentially by modulating FGF2.” | miR-148b-3p stimulated renal carcinoma cell apoptosis and migration growth via the FGF2-FGFR2 pathway. | [144] |
| Xu et al. (2015) | “miR-203 inhibition of renal cancer cell proliferation, migration and invasion by targeting of FGF2.” | miR-203 targeted bFGF, limiting renal cancer cell growth and metastases. | [145] | |
| Bone | Tsubaki et al. (2011) | “Blockade of the Ras/MEK/ERK and Ras/PI3K/Akt pathways by statins reduces the expression of bFGF, HGF, and TGF-beta as angiogenic factors in mouse osteosarcoma.” | Inhibition of growth factors such as bFGF, HGF, and TGF- β with Statins. | [154] |
| Thyroid | Xu et al. (2017) | “miR-27b-3p is Involved in Doxorubicin Resistance of Human Anaplastic Thyroid Cancer Cells via Targeting Peroxisome Proliferator-Activated Receptor Gamma.” | miR-195 overexpression limited bFGF and, consequently, the proliferation, migration, and invasion of PTC cell lines. | [159] |
| Wu et al. (2019) | “Peptide P11 suppresses the growth of human thyroid carcinoma by inhibiting the PI3K/AKT/mTOR signaling pathway.” | P11 peptide inhibited the PI3K/Akt/mTOR signaling pathway. | ||
| Bladder | Chen et al. (2016) | “FGF2-mediated reciprocal tumor cell-endothelial cell interplay contributes to the growth of chemoresistant cells: a potential mechanism for superficial bladder cancer recurrence.” | Evaluation of the antagonism against bFGF using the neutralizing antibody, which, however, did not affect the growth of 253J/DOX cells. | [167] |
| Prostate | Hotchkiss et al. (2002) | “Inhibition of endothelial cell function in vitro and angiogenesis in vivo by docetaxel (Taxotere): association with impaired repositioning of the microtubule organizing center.” | Taxane and Docetaxel effectively downregulated bFGF expression. | [191] |
| Cenni et al. (2007) | “Inhibition of angiogenesis via FGF-2 blockage in primitive and bone metastatic renal cell carcinoma.” | Antisense bFGF oligonucleotide blocked the production of FGF by both tumor and endothelial cells. | [194] | |
| Breast | Shee et al. (2018) | “Therapeutically targeting tumor microenvironment-mediated drug resistance in estrogen receptor-positive breast cancer.” | PD170374 inhibiting bFGF stopped ECM/FGF-mediated regulation of ER breast cancer. | [203] |
| Ovarian | Wang et al. (2021) | “Cancer-associated fibroblasts secrete FGF-1 to promote ovarian proliferation, migration, and invasion through the activation of FGF-1/FGFR4 signaling.” | PD173074 terminated cellular proliferation, migration, and invasion. | [209] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ardizzone, A.; Bova, V.; Casili, G.; Repici, A.; Lanza, M.; Giuffrida, R.; Colarossi, C.; Mare, M.; Cuzzocrea, S.; Esposito, E.; et al. Role of Basic Fibroblast Growth Factor in Cancer: Biological Activity, Targeted Therapies, and Prognostic Value. Cells 2023, 12, 1002. https://doi.org/10.3390/cells12071002
Ardizzone A, Bova V, Casili G, Repici A, Lanza M, Giuffrida R, Colarossi C, Mare M, Cuzzocrea S, Esposito E, et al. Role of Basic Fibroblast Growth Factor in Cancer: Biological Activity, Targeted Therapies, and Prognostic Value. Cells. 2023; 12(7):1002. https://doi.org/10.3390/cells12071002
Chicago/Turabian StyleArdizzone, Alessio, Valentina Bova, Giovanna Casili, Alberto Repici, Marika Lanza, Raffaella Giuffrida, Cristina Colarossi, Marzia Mare, Salvatore Cuzzocrea, Emanuela Esposito, and et al. 2023. "Role of Basic Fibroblast Growth Factor in Cancer: Biological Activity, Targeted Therapies, and Prognostic Value" Cells 12, no. 7: 1002. https://doi.org/10.3390/cells12071002
APA StyleArdizzone, A., Bova, V., Casili, G., Repici, A., Lanza, M., Giuffrida, R., Colarossi, C., Mare, M., Cuzzocrea, S., Esposito, E., & Paterniti, I. (2023). Role of Basic Fibroblast Growth Factor in Cancer: Biological Activity, Targeted Therapies, and Prognostic Value. Cells, 12(7), 1002. https://doi.org/10.3390/cells12071002











