Regulatory Roles of Noncoding RNAs in the Progression of Gastrointestinal Cancers and Health Disparities
Abstract
:1. Introduction
2. ncRNA-Mediated Regulation of Cell Signaling Pathways in GI Cancer Progression
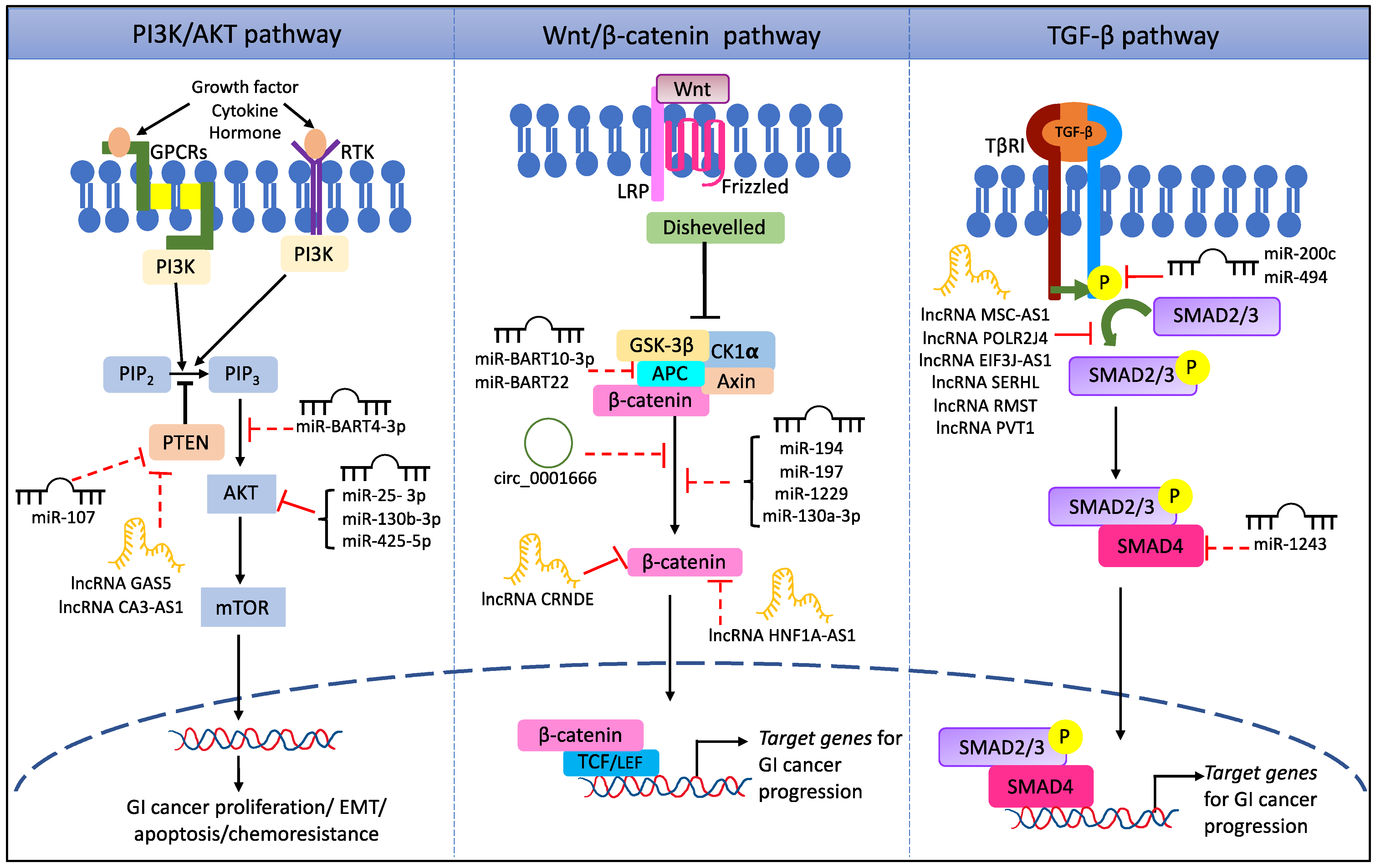
2.1. ncRNAs Regulate the PI3K/AKT Signaling Pathway
2.2. ncRNAs Regulate the Wnt/β-Catenin Signaling Pathway
2.3. ncRNAs and the Other Signaling Pathways
3. Role of ncRNAs in Chemoresistance in GI Cancers
4. Genome-Wide Profiling of ncRNAs in GI Cancers
5. ncRNAs as Potential Therapeutic Targets or Biomarkers for GI Cancer Progression
6. The Potential Role of ncRNAs to GI Cancer Disparities
7. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Mathers, C.; Parkin, D.M.; Piñeros, M.; Znaor, A.; Bray, F. Estimating the Global Cancer Incidence and Mortality in 2018: GLOBOCAN Sources and Methods. Int. J. Cancer 2019, 144, 1941–1953. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA A Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef] [PubMed]
- Peery, A.F.; Crockett, S.D.; Murphy, C.C.; Jensen, E.T.; Kim, H.P.; Egberg, M.D.; Lund, J.L.; Moon, A.M.; Pate, V.; Barnes, E.L.; et al. Burden and Cost of Gastrointestinal, Liver, and Pancreatic Diseases in the United States: Update 2021. Gastroenterology 2022, 162, 621–644. [Google Scholar] [CrossRef]
- Arnold, M.; Abnet, C.C.; Neale, R.E.; Vignat, J.; Giovannucci, E.L.; McGlynn, K.A.; Bray, F. Global Burden of 5 Major Types of Gastrointestinal Cancer. Gastroenterology 2020, 159, 335–349.e15. [Google Scholar] [CrossRef] [PubMed]
- Aznaourova, M.; Schmerer, N.; Schmeck, B.; Schulte, L.N. Disease-Causing Mutations and Rearrangements in Long Non-Coding RNA Gene Loci. Front. Genet. 2020, 11, 527484. [Google Scholar] [CrossRef] [PubMed]
- Guttman, M.; Rinn, J.L. Modular Regulatory Principles of Large Non-Coding RNAs. Nature 2012, 482, 339–346. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sanchez Calle, A.; Kawamura, Y.; Yamamoto, Y.; Takeshita, F.; Ochiya, T. Emerging Roles of Long Non-Coding RNA in Cancer. Cancer Sci. 2018, 109, 2093–2100. [Google Scholar] [CrossRef]
- Romano, G.; Veneziano, D.; Acunzo, M.; Croce, C.M. Small Non-Coding RNA and Cancer. Carcinogenesis 2017, 38, 485–491. [Google Scholar] [CrossRef] [Green Version]
- Esteller, M. Non-Coding RNAs in Human Disease. Nat. Rev. Genet. 2011, 12, 861–874. [Google Scholar] [CrossRef]
- Anastasiadou, E.; Jacob, L.S.; Slack, F.J. Non-Coding RNA Networks in Cancer. Nat. Rev. Cancer 2017, 18, 5–18. [Google Scholar] [CrossRef]
- Zhang, P.; Wu, W.; Chen, Q.; Chen, M. Non-Coding RNAs and Their Integrated Networks. J. Integr. Bioinform. 2019, 16, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Dai, X.; Kaushik, A.C.; Zhang, J. The Emerging Role of Major Regulatory RNAs in Cancer Control. Front. Oncol. 2019, 9, 920. [Google Scholar] [CrossRef] [PubMed]
- Derrien, T.; Johnson, R.; Bussotti, G.; Tanzer, A.; Djebali, S.; Tilgner, H.; Guernec, G.; Martin, D.; Merkel, A.; Knowles, D.G.; et al. The GENCODE v7 Catalog of Human Long Noncoding RNAs: Analysis of Their Gene Structure, Evolution, and Expression. Genome Res 2012, 22, 1775–1789. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Brien, J.O.; Hayder, H.; Zayed, Y.; Peng, C. Overview of MicroRNA Biogenesis, Mechanisms of Actions, and Circulation. Front. Endocrinol. 2018, 9, 402. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, J.; Liu, X.; Wu, H.; Ni, P.; Gu, Z.; Qiao, Y.; Chen, N.; Sun, F.; Fan, Q. CREB Up-Regulates Long Non-Coding RNA, HULC Expression through Interaction with MicroRNA-372 in Liver Cancer. Nucleic Acids Res. 2010, 38, 5366–5383. [Google Scholar] [CrossRef] [Green Version]
- Xiong, J.; Wang, D.; Wei, A.; Lu, H.; Tan, C.; Li, A.; Tang, J.; Wang, Y.; He, S.; Liu, X.; et al. Deregulated Expression of MiR-107 Inhibits Metastasis of PDAC through Inhibition PI3K/Akt Signaling via Caveolin-1 and PTEN. Exp. Cell Res. 2017, 361, 316–323. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.M.; Wu, Q.M.; Chang, L.Y.; Liu, J.C. MiR-34a and MiR-125a-5p Inhibit Proliferation and Metastasis but Induce Apoptosis in Hepatocellular Carcinoma Cells via Repressing the MACC1- Mediated PI3K/AKT/MTOR Pathway. Neoplasma 2020, 67, 1042–1053. [Google Scholar] [CrossRef]
- Zhao, M.H.; Liu, W.; Zhang, Y.; Liu, J.J.; Song, H.; Luo, B. Epstein–Barr Virus MiR-BART4-3p Regulates Cell Proliferation, Apoptosis, and Migration by Targeting AXL in Gastric Carcinoma. Virus Genes 2022, 58, 23–34. [Google Scholar] [CrossRef]
- Brown, J.M.; Recht, L.; Strober, S. The Promise of Targeting Macrophages in Cancer Therapy. Clin. Cancer Res. 2017, 23, 3241–3250. [Google Scholar] [CrossRef] [Green Version]
- Wang, D.; Wang, X.; Si, M.; Yang, J.; Sun, S.; Wu, H.; Cui, S.; Qu, X.; Yu, X. Exosome-Encapsulated MiRNAs Contribute to CXCL12/CXCR4-Induced Liver Metastasis of Colorectal Cancer by Enhancing M2 Polarization of Macrophages. Cancer Lett. 2020, 474, 36–52. [Google Scholar] [CrossRef]
- Zhong, M.E.; Chen, Y.; Zhang, G.; Xu, L.; Ge, W.; Wu, B. LncRNA H19 Regulates PI3K-Akt Signal Pathway by Functioning as a CeRNA and Predicts Poor Prognosis in Colorectal Cancer: Integrative Analysis of Dysregulated NcRNA-Associated CeRNA Network. Cancer Cell Int. 2019, 19, 1–13. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhou, S.; Guo, Z.; Zhou, C.; Zhang, Y.; Wang, S. Circ_NRIP1 Is Oncogenic in Malignant Development of Esophageal Squamous Cell Carcinoma (ESCC) via MiR-595/SEMA4D Axis and PI3K/AKT Pathway. Cancer Cell Int. 2021, 21, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Xiao, Z.; Qu, Z.; Chen, Z.; Fang, Z.; Zhou, K.; Huang, Z.; Guo, X.; Zhang, Y. LncRNA HOTAIR Is a Prognostic Biomarker for the Proliferation and Chemoresistance of Colorectal Cancer via MiR-203a-3p- Mediated Wnt/ß-Catenin Signaling Pathway. Cell Physiol. Biochem. 2018, 46, 1275–1285. [Google Scholar] [CrossRef] [PubMed]
- Han, P.; Li, J.; Zhang, B.; Lv, J.; Li, Y.; Gu, X.; Yu, Z.; Jia, Y.; Bai, X. The LncRNA CRNDE Promotes Colorectal Cancer Cell Proliferation and Chemoresistance via MiR-181a-5p-Mediated Regulation of Wnt/β-Catenin Signaling. Mol. Cancer 2017, 16, 9. [Google Scholar] [CrossRef] [Green Version]
- Zhang, J.; Zhang, K.; Hou, Y. Long Non-Coding RNA NNT-AS1 Knockdown Represses the Progression of Gastric Cancer via Modulating the MiR-142-5p/SOX4/Wnt/β-Catenin Signaling Pathway. Mol. Med. Rep. 2020, 22, 687–696. [Google Scholar] [CrossRef]
- Peng, Y.; Qin, Y.; Zhang, X.; Deng, S.; Yuan, Y.; Feng, X.; Chen, W.; Hu, F.; Gao, Y.; He, J.; et al. MiRNA-20b/SUFU/Wnt Axis Accelerates Gastric Cancer Cell Proliferation, Migration and EMT. Heliyon 2021, 7, e06695. [Google Scholar] [CrossRef]
- Dong, M.; Gong, L.-P.; Chen, J.-N.; Zhang, X.-F.; Zhang, Y.-W.; Hui, D.-Y.; Zhao, X.-X.; Wu, X.-Y.; Shao, C.-K. EBV-MiR-BART10-3p and EBV-MiR-BART22 Promote Metastasis of EBV-Associated Gastric Carcinoma by Activating the Canonical Wnt Signaling Pathway. Cell. Oncol. 2020, 43, 901–913. [Google Scholar] [CrossRef]
- Cao, X.; Zhang, J.; Apaer, S.; Yao, G.; Li, T. Microrna-19a-3p and Microrna-376c-3p Promote Hepatocellular Carcinoma Progression through Sox6-Mediated Wnt/β-Catenin Signaling Pathway. Int. J. Gen. Med. 2021, 14, 89–102. [Google Scholar] [CrossRef]
- Peng, Y.; Zhang, X.; Lin, H.; Deng, S.; Huang, Y.; Qin, Y.; Feng, X.; Yan, R.; Zhao, Y.; Cheng, Y.; et al. Inhibition of MiR-194 Suppresses the Wnt/β-Catenin Signalling Pathway in Gastric Cancer. Oncol. Rep. 2018, 40, 3323–3334. [Google Scholar] [CrossRef]
- Hu, Z.; Wang, P.; Lin, J.; Zheng, X.; Yang, F.; Zhang, G.; Chen, D.; Xie, J.; Gao, Z.; Peng, L.; et al. MicroRNA-197 Promotes Metastasis of Hepatocellular Carcinoma by Activating Wnt/β-Catenin Signaling. Cell. Physiol. Biochem. 2018, 51, 470–486. [Google Scholar] [CrossRef]
- Song, G.L.; Xiao, M.; Wan, X.Y.; Deng, J.; Ling, J.D.; Tian, Y.G.; Li, M.; Yin, J.; Zheng, R.Y.; Tang, Y.; et al. MiR-130a-3p Suppresses Colorectal Cancer Growth by Targeting Wnt Family Member 1 (WNT1). Bioengineered 2021, 12, 8407–8418. [Google Scholar] [CrossRef] [PubMed]
- Bai, F.; Zuo, C.; Ouyang, Y.; Xiao, K.; He, Z.; Yang, Z. Circular RNA 0001666 Inhibits Colorectal Cancer Cell Proliferation, Invasion and Stemness by Inactivating the Wnt/Β-catenin Signaling Pathway and Targeting MicroRNA-1229. Oncol. Lett. 2022, 23, 1–10. [Google Scholar] [CrossRef]
- Moustakas, A.; Pardali, K.; Gaal, A.; Heldin, C.-H. Mechanisms of TGF-β Signaling in Regulation of Cell Growth and Differentiation. Immunol. Lett. 2002, 82, 85–91. [Google Scholar] [CrossRef]
- Zhang, J.; Zhu, Y.; Hu, L.; Yan, F.; Chen, J. MiR-494 Induces EndMT and Promotes the Development of HCC (Hepatocellular Carcinoma) by Targeting SIRT3/TGF-β/SMAD Signaling Pathway. Sci. Rep. 2019, 9, 7213. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Cai, Q.Y.; Liu, J.; Peng, J.; Chen, Y.Q.; Sferra, T.J.; Lin, J.M. Ursolic Acid Suppresses the Invasive Potential of Colorectal Cancer Cells by Regulating the TGF-Β1/ZEB1/MiR-200c Signaling Pathway. Oncol. Lett. 2019, 18, 3274–3282. [Google Scholar] [CrossRef] [Green Version]
- Yu, D.; Liu, H.; Qin, J.; Huangfu, M.; Guan, X.; Li, X.; Zhou, L.; Dou, T.; Liu, Y.; Wang, L.; et al. Curcumol Inhibits the Viability and Invasion of Colorectal Cancer Cells via MiR-30a-5p and Hippo Signaling Pathway. Oncol. Lett. 2021, 21, 299. [Google Scholar] [CrossRef]
- Xu, X.; Chen, X.; Xu, M.; Liu, X.; Pan, B.; Qin, J.; Xu, T.; Zeng, K.; Pan, Y.; He, B.; et al. MiR-375-3p Suppresses Tumorigenesis and Partially Reverses Chemoresistance by Targeting YAP1 and SP1 in Colorectal Cancer Cells. Aging 2019, 11, 7357–7385. [Google Scholar] [CrossRef]
- Wang, X.; Chen, Y.; Liu, W.; Liu, T.; Sun, D. Hsa_circ_0128846 Promotes Tumorigenesis of Colorectal Cancer by Sponging Hsa-MiR-1184 and Releasing AJUBA and Inactivating Hippo/YAP Signalling. J. Cell. Mol. Med. 2020, 24, 9908–9924. [Google Scholar] [CrossRef]
- Huang, F.-T.; Peng, J.-F.; Cheng, W.-J.; Zhuang, Y.-Y.; Li, C.-Q.; Tang, J.; Chen, W.-Y.; Li, Y.-H.; Zhang, S.-N. MiR-143 Targeting TAK1 Attenuates Pancreatic Ductal Adenocarcinoma Progression via MAPK and NF-JB Pathway In Vitro. Dig. Dis. Sci. 2017, 62, 944–957. [Google Scholar] [CrossRef]
- Li, Z.; Lu, J.; Zeng, G.; Pang, J.; Zheng, X.; Feng, J.; Zhang, J. MiR-129-5p Inhibits Liver Cancer Growth by Targeting Calcium Calmodulin-Dependent Protein Kinase IV (CAMK4). Cell Death Dis. 2019, 10, 1–14. [Google Scholar] [CrossRef] [Green Version]
- Li, Y.; Wu, D.; Wang, P.; Li, X.; Shi, G. MiR-195 Regulates Proliferation and Apoptosis through Inhibiting the MTOR/P70s6k Signaling Pathway by Targeting HMGA2 in Esophageal Carcinoma Cells. Dis. Markers 2017, 2017, 8317913. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhao, D.-W.; Hou, Y.-S.; Sun, F.-B.; Han, B.; Li, S.-J. Effects of MiR-132 on Proliferation and Apoptosis of Pancreatic Cancer Cells via Hedgehog Signaling Pathway. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 1978–1985. [Google Scholar] [PubMed]
- Chen, Y.; Zhang, R. Long Non-Coding RNA AL139002.1 Promotes Gastric Cancer Development by Sponging MicroRNA-490-3p to Regulate Hepatitis A Virus Cellular Receptor 1 Expression. Bioengineered 2021, 12, 1927–1938. [Google Scholar] [CrossRef] [PubMed]
- Bukowski, K.; Kciuk, M.; Kontek, R. Mechanisms of Multidrug Resistance in Cancer Chemotherapy1. Bukowski, K.; Kciuk, M.; Kontek, R. Mechanisms of Multidrug Resistance in Cancer Chemotherapy. Int. J. Mol. Sci. 2020, 21, 3233. [Google Scholar] [CrossRef]
- Zhang, F.; Wang, H.; Yu, J.; Yao, X.; Yang, S.; Li, W.; Xu, L.; Zhao, L. LncRNA CRNDE Attenuates Chemoresistance in Gastric Cancer via SRSF6-Regulated Alternative Splicing of PICALM. Mol. Cancer 2021, 20, 6. [Google Scholar] [CrossRef]
- Xie, S.; Zhang, J.; Jiang, X.; Hua, Y.; Xie, S.; Qin, Y.; Yang, Y. LncRNA CRNDE Facilitates Epigenetic Suppression of CELF2 and LATS2 to Promote Proliferation, Migration and Chemoresistance in Hepatocellular Carcinoma. Cell Death Dis. 2020, 11, 1–17. [Google Scholar] [CrossRef]
- Dong, B.; Li, S.; Zhu, S.; Yi, M.; Luo, S.; Wu, K. MiRNA-Mediated EMT and CSCs in Cancer Chemoresistance. Exp. Hematol. Oncol. 2021, 10, 12. [Google Scholar] [CrossRef]
- Wang, X.; Lan, Z.; He, J.; Lai, Q.; Yao, X.; Li, Q.; Liu, Y.; Lai, H.; Gu, C.; Yan, Q.; et al. LncRNA SNHG6 Promotes Chemoresistance through ULK1-Induced Autophagy by Sponging MiR-26a-5p in Colorectal Cancer Cells. Cancer Cell Int. 2019, 19, 234. [Google Scholar] [CrossRef] [Green Version]
- Wu, H.; Fan, D. Long Non-Coding RNA PCAT6 Targets MiR-204 to Modulate the Chemoresistance of Colorectal Cancer Cells to 5-Fluorouracil-Based Treatment through HMGA2 Signaling. Cancer Med. 2019, 8, 2484–2495. [Google Scholar] [CrossRef] [Green Version]
- Gao, R.; Fang, C.; Xu, J.; Tan, H.; Li, P.; Ma, L. LncRNA CACS15 Contributes to Oxaliplatin Resistance in Colorectal Cancer by Positively Regulating ABCC1 through Sponging MiR-145. Arch. Biochem. Biophys. 2019, 663, 183–191. [Google Scholar] [CrossRef]
- Wang, S.; Li, J.; Yang, X. Long Non-Coding RNA LINC00525 Promotes the Stemness and Chemoresistance of Colorectal Cancer by Targeting MiR-507 / ELK3 Axis. Int. J. Stem Cells 2019, 12, 347–359. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jiang, X.; Li, Q.; Zhang, S.; Song, C.; Zheng, P. Long Noncoding RNA GIHCG Induces Cancer Progression and Chemoresistance and Indicates Poor Prognosis in Colorectal Cancer. Onco Targets Ther. 2019, 12, 1059–1070. [Google Scholar] [CrossRef] [Green Version]
- Zhang, P.F.; Liu, M.; Wang, F. The LncRNA SCARNA2 Mediates Colorectal Cancer Chemoresistance through a Conserved MicroRNA-342-3p Target Sequence. J. Cell. Physiol. 2018, 234, 10157–10165. [Google Scholar] [CrossRef] [PubMed]
- Wu, J.; Wang, L.; Du, X.; Sun, Q.; Wang, Y.; Li, M.; Zang, W.; Liu, K.; Zhao, G. α-Solanine Enhances the Chemosensitivity of Esophageal Cancer Cells by Inducing MicroRNA-138 Expression. Oncol. Rep. 2018, 39, 1163–1172. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhang, S.; Zheng, F.; Zhang, L.; Huang, Z.; Huang, X.; Pan, Z. LncRNA HOTAIR-Mediated MTHFR Methylation Inhibits 5-Fluorouracil Sensitivity in Esophageal Cancer Cells. J. Exp. Clin. Cancer Res. 2020, 1, 131. [Google Scholar] [CrossRef]
- Li, B.; Hong, P.; Zheng, C.-C.; Dai, W.; Chen, W.-Y.; Yang, Q.-S.; Han, L.; Tsao, S.W.; Chan, K.T.; Lee, N.P.Y.; et al. Identification of MiR-29c and Its Target FBXO31 as a Key Regulatory Mechanism in Esophageal Cancer Chemoresistance: Functional Validation and Clinical Significance. Theranostics 2019, 9, 1599–1613. [Google Scholar] [CrossRef]
- Han, L.; Cui, D.; Li, B.; Xu, W.W.; Lam, A.K.Y.; Chan, K.T.; Zhu, Y.; Lee, N.P.Y.; Law, S.Y.K.; Guan, X.Y.; et al. MicroRNA-338-5p Reverses Chemoresistance and Inhibits Invasion of Esophageal Squamous Cell Carcinoma Cells by Targeting Id-1. Cancer Sci. 2019, 110, 3677–3688. [Google Scholar] [CrossRef]
- Hu, M.; Wang, J.L. LncRNA CCAT1 Is a Biomarker for the Proliferation and Drug Resistance of Esophageal Cancer via the MiR -143/PLK1/BUBR1 Axis. Mol. Carcinog. 2019, 58, 2207–2217. [Google Scholar] [CrossRef]
- Zhu, Z.; Pang, Y.; Jin, G.; Zhang, H.; Wang, W.; Liu, J.; Tuo, G.; Wu, P.; Yang, Y.; Wang, Z.; et al. Hypoxia Induces Chemoresistance of Esophageal Cancer Cells to Cisplatin through Regulating the LncRNA-EMS/MiR-758-3p/WTAP Axis. Aging 2021, 13, 17155–17176. [Google Scholar] [CrossRef]
- Yang, C.; Lu, Y. Long Non-Coding RNA LINC00337 Induces Autophagy and Chemoresistance to Cisplatin in Esophageal Squamous Cell Carcinoma Cells via Upregulation of TPX2 by Recruiting E2F4. FASEB J. 2020, 34, 6055–6069. [Google Scholar] [CrossRef] [Green Version]
- Zhang, Z.; Xiong, R.; Li, C.; Xu, M.; Guo, M. LncRNA TUG1 Promotes Cisplatin Resistance in Esophageal Squamous Cell Carcinoma Cells by Regulating Nrf2. Acta Biochim. Biophys. Sin. 2019, 51, 826–833. [Google Scholar] [CrossRef] [PubMed]
- Wu, K.; Hu, Y.; Yan, K.; Qi, Y.; Zhang, C.; Zhu, D.; Liu, D.; Zhao, S. MicroRNA-10b Confers Cisplatin Resistance by Activating AKT/MTOR/P70S6K Signaling via Targeting PPARγ in Esophageal Cancer. J. Cell. Physiol. 2020, 235, 1247–1258. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Chen, W.; Yu, H.; Song, Z.; Li, Q.; Shen, X.; Wu, Y.; Zhu, L.; Ma, Q.; Xing, D. LncRNA ROR Promotes Gastric Cancer Drug Resistance. Cancer Control 2020, 27, 1073274820904694. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.; Liu, B.; Chen, Z.; Li, G.; Zhang, Z. MSC-Induced LncRNA HCP5 Drove Fatty Acid Oxidation through MiR-3619-5p/AMPK/PGC1 α/CEBPB Axis to Promote Stemness and Chemo- Resistance of Gastric Cancer. Cell Death Dis. 2020, 11, 233. [Google Scholar] [CrossRef] [Green Version]
- Zhu, L.; Zhu, Y.; Han, S.; Chen, M.; Song, P.; Dai, D.; Xu, W.; Jiang, T.; Feng, L.; Shin, V.Y.; et al. Impaired Autophagic Degradation of LncRNA ARHGAP5-AS1 Promotes Chemoresistance in Gastric Cancer. Cell Death Dis. 2019, 10, 383. [Google Scholar] [CrossRef] [PubMed]
- Xu, F.; Zha, G.; Wu, Y.; Cai, W.; Ao, J. Overexpressing LncRNA SNHG16 Inhibited HCC Proliferation and Chemoresistance by Functionally Sponging Hsa-MiR-93. Onco Targets Ther. 2018, 11, 8855–8863. [Google Scholar] [CrossRef] [Green Version]
- Wang, C.; Ke, S.; Li, M.; Lin, C.; Liu, X.; Pan, Q. Downregulation of LncRNA GAS5 Promotes Liver Cancer Proliferation and Drug Resistance by Decreasing PTEN Expression. Mol. Genet. Genom. 2020, 295, 251–260. [Google Scholar] [CrossRef]
- Xiao, J.; Lv, Y.; Jin, F.; Liu, Y.; Ma, Y.; Xiong, Y.; Liu, L.; Zhang, S.; Sun, Y.; Tipoe, G.L.; et al. LncRNA HANR Promotes Tumorigenesis and Increase of Chemoresistance in Hepatocellular Carcinoma. Cell. Physiol. Biochem. 2017, 43, 1926–1938. [Google Scholar] [CrossRef]
- Fan, L.; Huang, X.; Chen, J.; Zhang, K.; Gu, Y.-H.; Sun, J.; Cui, S.-Y. Long Noncoding RNA MALAT1 Contributes to Sorafenib Resistance by Targeting MiR-140-5p/Aurora-A Signaling in Hepatocellular Carcinoma. Mol. Cancer Ther. 2020, 19, 1197–1209. [Google Scholar] [CrossRef] [Green Version]
- Schultheiss, C.S.; Laggai, S.; Czepukojc, B.; Hussein, U.K.; List, M.; Tierling, S.; Hosseini, K.; Golob-schwarzl, N.; Pokorny, J.; Hachenthal, N.; et al. The Long Non-Coding RNA H19 Suppresses Carcinogenesis and Chemoresistance in Hepatocellular Carcinoma. Cell Stress 2017, 1, 37–54. [Google Scholar] [CrossRef] [Green Version]
- Yang, Q.; Li, K.; Huang, X.; Zhao, C.; Mei, Y.; Li, X.; Jiao, L.; Yang, H. LncRNA SLC7A11-AS1 Promotes Chemoresistance by Blocking SCF b -TRCP -Mediated Degradation of NRF2 in Pancreatic Cancer. Mol. Ther. Nucleic Acid 2020, 19, 974–985. [Google Scholar] [CrossRef] [PubMed]
- Gao, Z.; Wang, J.; Chen, D.; Ma, X.; Yang, W.; Zhe, T.; Dang, X. Biomedicine & Pharmacotherapy Long Non-Coding RNA GAS5 Antagonizes the Chemoresistance of Pancreatic Cancer Cells through down-Regulation of MiR-181c-5p. Biomed. Pharmacother. 2018, 97, 809–817. [Google Scholar] [CrossRef] [PubMed]
- Shimura, T.; Toden, S.; Kandimalla, R.; Toiyama, Y.; Okugawa, Y.; Kanda, M.; Baba, H.; Kodera, Y.; Kusunoki, M.; Goel, A. Genomewide Expression Profiling Identifies a Novel MiRNA-Based Signature for the Detection of Peritoneal Metastasis in Patients with Gastric Cancer. Ann. Surg. 2021, 274, E425–E434. [Google Scholar] [CrossRef]
- Kalmár, A.; Nagy, Z.B.; Galamb, O.; Csabai, I.; Bodor, A.; Wichmann, B.; Valcz, G.; Barták, B.K.; Tulassay, Z.; Igaz, P.; et al. Genome-Wide Expression Profiling in Colorectal Cancer Focusing on LncRNAs in the Adenoma-Carcinoma Transition. BMC Cancer 2019, 19, 1059. [Google Scholar] [CrossRef] [PubMed]
- Chen, D.; Sun, Q.; Cheng, X.; Zhang, L.; Song, W.; Zhou, D.; Lin, J.; Wang, W. Genome-Wide Analysis of Long Noncoding RNA (LncRNA) Expression in Colorectal Cancer Tissues from Patients with Liver Metastasis. Cancer Med. 2016, 5, 1629–1639. [Google Scholar] [CrossRef] [Green Version]
- Yao, J.; Wu, L.; Meng, X.; Yang, H.; Ni, S.; Wang, Q.; Zhou, J.; Zhang, Q.; Su, K.; Shao, L.; et al. Profiling, Clinicopathological Correlation and Functional Validation of Specific Long Non-Coding RNAs for Hepatocellular Carcinoma. Mol. Cancer 2017, 16, 164. [Google Scholar] [CrossRef] [Green Version]
- Xue, J.; Jia, E.; Ren, N.; Xin, H. Identification of Prognostic MiRNA Biomarkers for Esophageal Cancer Based on The Cancer Genome Atlas and Gene Expression Omnibus. Medicine 2021, 100, e24832. [Google Scholar] [CrossRef]
- Chen, F.; Zhou, H.; Wu, C.; Yan, H. Identification of MiRNA Profiling in Prediction of Tumor Recurrence and Progress and Bioinformatics Analysis for Patients with Primary Esophageal Cancer: Study Based on TCGA Database. Pathol. Res. Pract. 2018, 214, 2081–2086. [Google Scholar] [CrossRef]
- Ma, J.; Xiao, Y.; Tian, B.; Chen, S.; Zhang, B.; Wu, J.; Wu, Z.; Li, X.; Tang, J.; Yang, D.; et al. Genome-Wide Analyses of Long Non-Coding RNA Expression Profiles and Functional Network Analysis in Esophageal Squamous Cell Carcinoma. Sci. Rep. 2019, 9, 9162. [Google Scholar] [CrossRef]
- Cui, H.; Zhang, Y.; Zhang, Q.; Chen, W.; Zhao, H.; Liang, J. A Comprehensive Genome-Wide Analysis of Long Noncoding RNA Expression Profile in Hepatocellular Carcinoma. Cancer Med. 2017, 6, 2932–2941. [Google Scholar] [CrossRef]
- Zheng, R.; Liang, J.; Lu, J.; Li, S.; Zhang, G.; Wang, X.; Liu, M.; Wang, W.; Chu, H.; Tao, G.; et al. Genome-Wide Long Non-Coding RNAs Identified a Panel of Novel Plasma Biomarkers for Gastric Cancer Diagnosis. Gastric Cancer 2019, 22, 731–741. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zhang, K.; Shi, H.; Xi, H.; Wu, X.; Cui, J.; Gao, Y.; Liang, W.; Hu, C.; Liu, Y.; Li, J.; et al. Genome-Wide LncRNA Microarray Profiling Identifies Novel Circulating LncRNAs for Detection of Gastric Cancer. Theranostics 2017, 7, 213–227. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.; Wen, D.Y.; Li, Q.; He, Y.; Yang, H.; Chen, G. Genome-Wide Analysis of Prognostic LncRNAs, MiRNAs, and MRNAs Forming a Competing Endogenous RNA Network in Hepatocellular Carcinoma. Cell. Physiol. Biochem. 2018, 530021, 1953–1967. [Google Scholar] [CrossRef] [PubMed]
- Xie, J.; Chen, L.; Sun, Q.; Li, H.; Wei, W.; Wu, D.; Hu, Y.; Zhu, Z.; Shi, J.; Wang, M. An Immune Subtype-Related Prognostic Signature of Hepatocellular Carcinoma Based on Single-Cell Sequencing Analysis. Aging 2022, 14, 3276–3292. [Google Scholar] [CrossRef]
- Pavlova, N.N.; Thompson, C.B. The Emerging Hallmarks of Cancer Metabolism. Cell Metab. 2016, 23, 27–47. [Google Scholar] [CrossRef] [Green Version]
- Mujica, M.L.; Gallay, P.A.; Perrachione, F.; Montemerlo, A.E.; Tamborelli, L.A.; Vaschetti, V.M.; Reartes, D.F.; Bollo, S.; Rodríguez, M.C.; Dalmasso, P.R.; et al. New Trends in the Development of Electrochemical Biosensors for the Quantification of MicroRNAs. J. Pharm. Biomed. Anal. 2020, 189, 113478. [Google Scholar] [CrossRef]
- Zhou, X.; Yin, C.; Dang, Y.; Ye, F.; Zhang, G. Identification of the Long Non-Coding RNA H19 in Plasma as a Novel Biomarker for Diagnosis of Gastric Cancer. Sci. Rep. 2015, 5, 11516. [Google Scholar] [CrossRef]
- Toden, S.; Zumwalt, T.J.; Goel, A. Non-Coding RNAs and Potential Therapeutic Targeting in Cancer. Biochim. Biophys. Acta-Rev. Cancer 2021, 1875, 188491. [Google Scholar] [CrossRef]
- Chandra Gupta, S.; Nandan Tripathi, Y. Potential of Long Non-Coding RNAs in Cancer Patients: From Biomarkers to Therapeutic Targets. Int. J. Cancer 2017, 140, 1955–1967. [Google Scholar] [CrossRef]
- Cai, Y.; Yan, P.; Zhang, G.; Yang, W.; Wang, H.; Cheng, X. Long Non-Coding RNA TP73-AS1 Sponges MiR-194 to Promote Colorectal Cancer Cell Proliferation, Migration and Invasion via up-Regulating TGFα. Cancer Biomark. 2018, 23, 145–156. [Google Scholar] [CrossRef]
- Ma, Z.; Peng, P.; Zhou, J.; Hui, B.; Ji, H.; Wang, J.; Wang, K. Long Non-Coding RNA SH3PXD2A-AS1 Promotes Cell Progression Partly through Epigenetic Silencing P57 and KLF2 in Colorectal Cancer. Cell. Physiol. Biochem. 2018, 46, 2197–2214. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.; Chen, Y.; Lin, C.; Hu, G. Biological Functions and Clinical Significance of the Newly Identified Long Non-coding RNA RP1-85F18.6 in Colorectal Cancer. Oncol. Rep. 2018, 40, 2648–2658. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.-B.; Han, C.; Sun, C.-Z. Long Non-Coding RNA DLEU7-AS1 Promotes the Occurrence and Development of Colorectal Cancer via Wnt/β-Catenin Pathway. Eur. Rev. Med. Pharmacol. Sci. 2018, 22, 110–117. [Google Scholar] [PubMed]
- Shen, X.; Bai, Y.; Luo, B.; Zhou, X. Upregulation of LncRNA BANCR Associated with the Lymph Node Metastasis and Poor Prognosis in Colorectal Cancer. Biol. Res. 2017, 50, 32. [Google Scholar] [CrossRef] [Green Version]
- Zhang, X.; Xiong, Y.; Tang, F.; Bian, Y.; Chen, Y.; Zhang, F. Long Noncoding RNA HNF1A-AS1 Indicates a Poor Prognosis of Colorectal Cancer and Promotes Carcinogenesis via Activation of the Wnt/β-Catenin Signaling Pathway. Biomed. Pharmacother. 2017, 96, 877–883. [Google Scholar] [CrossRef]
- Zhang, X.F.; Zhang, Y.; Shen, Z.; Yang, G.G.; Wang, H.D.; Li, L.F.; Liu, D.C.; Qiu, J.M. LncRNALUADT1 Is Overexpressed in Colorectal Cancer and Its Expression Level Is Related to Clinicopathology. Eur. Rev. Med. Pharm. Sci. 2018, 22, 2282–2286. [Google Scholar] [CrossRef]
- Li, X.; Wang, F.; Sun, Y.; Fan, Q.; Cui, G. Expression of Long Non-Coding RNA PANDAR and Its Prognostic Value in Colorectal Cancer Patients. Int. J. Biol. Markers 2017, 32, e218–e223. [Google Scholar] [CrossRef]
- Sun, L.; Jiang, C.; Xu, C.; Xue, H.; Zhou, H.; Gu, L.; Liu, Y.; Xu, Q. Down-Regulation of Long Non-Coding RNA RP11-708H21.4 Is Associated with Poor Prognosis for Colorectal Cancer and Promotes Tumorigenesis through Regulating AKT/MTOR Pathway. Oncotarget 2017, 8, 27929–27942. [Google Scholar] [CrossRef] [Green Version]
- Zhou, H.-B.; Li, Q.; Liu, M.; Cao, Y.-Q.; Xu, J.-Y. Increased Expression of Long Non-Coding RNA SBDSP1 Correlates with Poor Survival in Colorectal Cancer. Eur. Rev. Med. Pharmacol. Sci. 2017, 21, 3837–3841. [Google Scholar]
- Li, M.; Bian, Z.; Yao, S.; Zhang, J.; Jin, G.; Wang, X.; Yin, Y.; Huang, Z. Up-Regulated Expression of SNHG6 Predicts Poor Prognosis in Colorectal Cancer. Pathol. Res. Pract. 2018, 214, 784–789. [Google Scholar] [CrossRef]
- Fu, J.; Cui, Y. Long Noncoding RNA ZEB1-AS1 Expression Predicts Progression and Poor Prognosis of Colorectal Cancer. Int. J. Biol. Markers 2017, 32, e428–e433. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Luo, J.; Xu, L.-N.; Zhang, S.-J.; Jiang, Y.-G.; Zhuo, D.-X.; Wu, L.-H.; Jiang, X.; Huang, Y. Downregulation of LncRNA-RP11-317J10.2 Promotes Cell Proliferation and Invasion and Predicts Poor Prognosis in Colorectal Cancer. Scand. J. Gastroenterol. 2018, 53, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Fan, Q.; Liu, B. Discovery of a Novel Six-Long Non-Coding RNA Signature Predicting Survival of Colorectal Cancer Patients. J. Cell. Biochem. 2018, 119, 3574–3585. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Kuang, H.; Xue, J.; Liao, L.; Yin, F.; Zhou, X. LncRNA AB073614 Regulates Proliferation and Metastasis of Colorectal Cancer Cells via the PI3K/AKT Signaling Pathway. Biomed. Pharmacother. 2017, 93, 1230–1237. [Google Scholar] [CrossRef] [PubMed]
- Sha, Q.-K.; Chen, L.; Xi, J.-Z.; Song, H. Long Non-Coding RNA LINC00858 Promotes Cells Proliferation, Migration and Invasion by Acting as a CeRNA of MiR-22-3p in Colorectal Cancer. Artif. Cells Nanomed. Biotechnol. 2019, 47, 1057–1066. [Google Scholar] [CrossRef] [Green Version]
- Wang, X.; Lai, Q.; He, J.; Li, Q.; Ding, J.; Lan, Z.; Gu, C.; Yan, Q.; Fang, Y.; Zhao, X.; et al. LncRNA SNHG6 Promotes Proliferation, Invasion and Migration in Colorectal Cancer Cells by Activating TGF-β/Smad Signaling Pathway via Targeting UPF1 and Inducing EMT via Regulation of ZEB1. Int. J. Med. Sci. 2019, 16, 51–59. [Google Scholar] [CrossRef] [Green Version]
- Wei, H.; Yang, Z.; Lin, B. Overexpression of Long Non Coding RNA CA3-AS1 Suppresses Proliferation, Invasion and Promotes Apoptosis via MiRNA-93/PTEN Axis in Colorectal Cancer. Gene 2019, 687, 9–15. [Google Scholar] [CrossRef]
- Tsai, K.-W.; Lo, Y.-H.; Liu, H.; Yeh, C.-Y.; Chen, Y.-Z.; Hsu, C.-W.; Chen, W.-S.; Wang, J.-H. Linc00659, a Long Noncoding RNA, Acts as Novel Oncogene in Regulating Cancer Cell Growth in Colorectal Cancer. Mol. Cancer 2018, 17, 72. [Google Scholar] [CrossRef]
- Lin, K.; Jiang, H.; Zhang, L.-L.; Jiang, Y.; Yang, Y.-X.; Qiu, G.-D.; She, Y.-Q.; Zheng, J.-T.; Chen, C.; Fang, L.; et al. Down-Regulated LncRNA-HOTAIR Suppressed Colorectal Cancer Cell Proliferation, Invasion, and Migration by Mediating P21. Dig. Dis. Sci. 2018, 63, 2320–2331. [Google Scholar] [CrossRef]
- American Cancer Society. Colorectal Cancer Facts & Figures; 2020–2022; American Cancer Society: Atlanta, GA, USA, 2020; Available online: https://www.cancer.org/research/cancer-facts-statistics/colorectal-cancer-facts-figures.html (accessed on 6 July 2022).
- Xing, J.; Wan, S.; Zhou, F.; Qu, F.; Li, B.; Myers, R.E.; Fu, X.; Palazzo, J.P.; He, X.; Chen, Z.; et al. Genetic Polymorphisms in Pre-MicroRNA Genes as Prognostic Markers of Colorectal Cancer. Cancer Epidemiol. Biomark. Prev. 2012, 21, 217–227. [Google Scholar] [CrossRef] [Green Version]
- Ryan, B.M.; McClary, A.C.; Valeri, N.; Robinson, D.; Paone, A.; Bowman, E.D.; Robles, A.I.; Croce, C.; Harris, C.C. Rs4919510 in Hsa-Mir-608 Is Associated with Outcome but Not Risk of Colorectal Cancer. PLoS ONE 2012, 7, e0036306. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wei, J.; Zheng, L.; Liu, S.; Yin, J.; Wang, L.; Wang, X.; Shi, Y.; Shao, A.; Tang, W.; Ding, G.; et al. MiR-196a2 Rs11614913 T>C Polymorphism and Risk of Esophageal Cancer in a Chinese Population. Hum. Immunol. 2013, 74, 1199–1205. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Du, M.; Chen, W.; Zhu, L.; Wu, C.; Zhang, Z.; Wang, M.; Chu, H.; Gu, D.; Chen, J. Polymorphism Rs2682818 in MiR-618 Is Associated with Colorectal Cancer Susceptibility in a Han Chinese Population. Cancer Med. 2018, 7, 1194–1200. [Google Scholar] [CrossRef]
- Li, S.; Hua, Y.; Jin, J.; Wang, H.; Du, M.; Zhu, L.; Chu, H.; Zhang, Z.; Wang, M. Association of Genetic Variants in LncRNA H19 with Risk of Colorectal Cancer in a Chinese Population. Oncotarget 2016, 7, 25470–25477. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chao, X.; Feng, X.; Shi, H.; Wang, Y.; Wang, L.; Shen, H.; Zha, Q.; Chen, Y.; Jiang, C. MIR17HG Polymorphism (Rs7318578) Is Associated with Liver Cancer Risk in the Chinese Han Population. Biosci. Rep. 2020, 40, 1–8. [Google Scholar] [CrossRef]
- Wu, H.; He, G.; Han, H.; Xiong, W.; Song, T.; Chen, H.; Chen, X.; Wu, X.; Huang, G.; Zhang, Y.; et al. Analysis of MIR155HG Variants and Colorectal Cancer Susceptibility in Han Chinese Population. Mol. Genet. Genom. Med. 2019, 7, e778. [Google Scholar] [CrossRef] [Green Version]
- Chen, P.; Bai, Y.; Li, Y.; Yuan, Y.; Cheng, Y.; Pang, J.; Zhu, H.; Chen, C. Association between Polymorphisms of MIR17HG and Risk of Colorectal Cancer in the Chinese Han Population. Mol. Genet. Genom. Med. 2019, 7, e667. [Google Scholar] [CrossRef] [Green Version]
- Yu, Z.; Rong, Z.Y.; Sheng, J.; Luo, Z.; Zhang, J.; Li, T.; Zhu, Z.; Fu, Z.; Qiu, Z.; Huang, C. Aberrant Non-Coding RNA Expressed in Gastric Cancer and Its Diagnostic Value. Front. Oncol. 2021, 11, 2584. [Google Scholar] [CrossRef]
- Wang, Q.; Yu, X.; Yang, N.; Xu, L.; Zhou, Y. LncRNA AC007255.1, an Immune-Related Prognostic Enhancer RNA in Esophageal Cancer. PeerJ 2021, 9, e11698. [Google Scholar] [CrossRef]
- Bovell, L.C.; Shanmugam, C.; Putcha, B.D.K.; Katkoori, V.R.; Zhang, B.; Bae, S.; Singh, K.P.; Grizzle, W.E.; Manne, U. The Prognostic Value of MicroRNAs Varies with Patient Race/Ethnicity and Stage of Colorectal Cancer. Clin. Cancer Res. 2013, 19, 3955–3965. [Google Scholar] [CrossRef] [Green Version]
- Tu, M.J.; Pan, Y.Z.; Qiu, J.X.; Kim, E.J.; Yu, A.M. MicroRNA-1291 Targets the FOXA2-AGR2 Pathway to Suppress Pancreatic Cancer Cell Proliferation and Tumorigenesis. Oncotarget 2016, 7, 45547–45561. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Paredes, J.; Ji, P.; Lacomb, J.F.; Shroyer, K.R.; Martello, L.A.; Williams, J.L. Establishment of Three Novel Cell Lines Derived from African American Patients with Colorectal Carcinoma: A Unique Tool for Assessing Racial Health Disparity. Int. J. Oncol. 2018, 53, 1516–1528. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Alidoust, M.; Hamzehzadeh, L.; Rivandi, M.; Pasdar, A. Polymorphisms in Non-Coding RNAs and Risk of Colorectal Cancer: A Systematic Review and Meta-Analysis. Crit. Rev. Oncol./Hematol. 2018, 132, 100–110. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, A.; Azim, S.; Zubair, H.; Khan, M.A.; Singh, S.; Carter, J.E.; Rocconi, R.P.; Singh, A.P. Epigenetic Basis of Cancer Health Disparities: Looking beyond Genetic Differences. Biochim. Biophys. Acta-Rev. Cancer 2017, 1868, 16–28. [Google Scholar] [CrossRef]
- Li, E.; Ji, P.; Ouyang, N.; Zhang, Y.; Wang, X.Y.; Rubin, D.C.; Davidson, N.O.; Bergamaschi, R.; Shroyer, K.R.; Burke, S.; et al. Differential Expression of MiRNAs in Colon Cancer between African and Caucasian Americans: Implications for Cancer Racial Health Disparities. Int. J. Oncol. 2014, 45, 587–594. [Google Scholar] [CrossRef] [Green Version]
- Farhana, L.; Antaki, F.; Anees, M.R.; Nangia-Makker, P.; Judd, S.; Hadden, T.; Levi, E.; Murshed, F.; Yu, Y.; van Buren, E.; et al. Role of Cancer Stem Cells in Racial Disparity in Colorectal Cancer. Cancer Med. 2016, 5, 1268–1278. [Google Scholar] [CrossRef]
- Wang, X.; Ji, P.; Zhang, Y.; LaComb, J.F.; Tian, X.; Li, E.; Williams, J.L. Aberrant DNA Methylation: Implications in Racial Health Disparity. PLoS ONE 2016, 11, e0153125. [Google Scholar] [CrossRef]
- Augustus, G.J.; Ellis, N.A. Colorectal Cancer Disparity in African Americans: Risk Factors and Carcinogenic Mechanisms. Am. J. Pathol. 2018, 188, 291–303. [Google Scholar] [CrossRef]
- Jackson, C.S.; Oman, M.; Patel, A.M.; Vega, K.J. Health Disparities in Colorectal Cancer among Racial and Ethnic Minorities in the United States. J. Gastrointest. Oncol. 2016, 7, S32–S43. [Google Scholar] [CrossRef]
- Goyal, A.; Myacheva, K.; Groß, M.; Klingenberg, M.; Duran Arqué, B.; Diederichs, S. Challenges of CRISPR/Cas9 Applications for Long Non-Coding RNA Genes. Nucleic Acids Res. 2017, 45, e12. [Google Scholar] [CrossRef] [Green Version]
- Said, H.; Sameh, M.; Shawky, M.; Meteini, E. Genomics LncRNA- RP11-156p1.3, Novel Diagnostic and Therapeutic Targeting via CRISPR / Cas9 Editing in Hepatocellular Carcinoma. Genomics 2020, 112, 3306–3314. [Google Scholar] [CrossRef]
- Wang, J.-J.; Yang, Y.-C.; Song, Y.-X.; Peng, G.; Sun, J.-X.; Chen, X.-W.; Ma, B.; Wang, Z.-N. Long Non-Coding RNA AB007962 Is Downregulated in Gastric Cancer and Associated with Poor Prognosis. Oncol. Lett. 2018, 16, 4621–4627. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sun, Y.-Y.; Zhang, H.; Ma, R.-R.; Zhang, G.-H.; Tian, Y.-R.; Liu, L.; Liu, L.; Gao, P. Long Non-Coding RNA AK025387 Promotes Cell Migration and Invasion of Gastric Cancer. Front. Oncol. 2020, 10, 633. [Google Scholar] [CrossRef] [PubMed]
- Luo, X.; Wang, G.-H.; Bian, Z.-L.; Li, X.-W.; Zhu, B.-Y.; Jin, C.-J.; Ju, S.-Q. Long Non-Coding RNA CCAL/MiR-149/FOXM1 Axis Promotes Metastasis in Gastric Cancer. Cell Death Dis. 2018, 9, 993. [Google Scholar] [CrossRef]
- Xiao, K.; Dong, Z.; Wang, D.; Liu, M.; Ding, J.; Chen, W.; Shang, Z.; Yue, C.; Zhang, Y. Clinical Value of LncRNA CCAT1 in Serum Extracellular Vesicles as a Potential Biomarker for Gastric Cancer. Oncol. Lett. 2021, 21, 447. [Google Scholar] [CrossRef]
- Hao, Y.-P.; Qiu, J.-H.; Zhang, D.-B.; Yu, C.-G. Long Non-Coding RNA DANCR, a Prognostic Indicator, Promotes Cell Growth and Tumorigenicity in Gastric Cancer. Tumour Biol. 2017, 39, 1010428317699798. [Google Scholar] [CrossRef] [Green Version]
- Song, W.; Qian, Y.; Zhang, M.-H.; Wang, H.; Wen, X.; Yang, X.-Z.; Dai, W.-J. The Long Non-Coding RNA DDX11-AS1 Facilitates Cell Progression and Oxaliplatin Resistance via Regulating MiR-326/IRS1 Axis in Gastric Cancer. Eur. Rev. Med. Pharmacol. Sci. 2020, 24, 3049–3061. [Google Scholar]
- Liang, Y.; Zhang, C.-D.; Zhang, C.; Dai, D.-Q. DLX6-AS1/MiR-204-5p/OCT1 Positive Feedback Loop Promotes Tumor Progression and Epithelial-Mesenchymal Transition in Gastric Cancer. Gastric Cancer 2020, 23, 212–227. [Google Scholar] [CrossRef]
- Luo, Y.; Zheng, S.; Wu, Q.; Wu, J.; Zhou, R.; Wu, Z.; Rong, X.; Huang, N.; Sun, L.; Bin, J.; et al. Long Noncoding RNA (LncRNA) EIF3J-DT Induces Chemoresistance of Gastric Cancer via Autophagy Activation. Autophagy 2021, 17, 4083–4101. [Google Scholar] [CrossRef]
- Zhang, G.; Wang, Q.; Lu, J.; Ma, G.; Ge, Y.; Chu, H.; Du, M.; Wang, M.; Zhang, Z. Long Non-Coding RNA FLJ22763 Is Involved in the Progression and Prognosis of Gastric Cancer. Gene 2019, 693, 84–91. [Google Scholar] [CrossRef]
- Bo, G.; Liu, Y.; Li, W.; Wang, L.; Zhao, L.; Tong, D.; Ni, L.; Liu, L.; Qin, Y.; Wang, W.; et al. The Novel LncRNA GPC5-AS1 Stabilizes GPC5 MRNA by Competitively Binding with MiR-93/106a to Suppress Gastric Cancer Cell Proliferation. Aging 2022, 14, 1767–1781. [Google Scholar] [CrossRef] [PubMed]
- Yörüker, E.E.; Keskin, M.; Kulle, C.B.; Holdenrieder, S.; Gezer, U. Diagnostic and Prognostic Value of Circulating LncRNA H19 in Gastric Cancer. Biomed. Rep. 2018, 9, 181–186. [Google Scholar]
- Da, M.; Ma, J.; Zhang, Y.; Yang, J.; Yao, J.; Huang, B.; Ma, H.; Ge, L. High Expression Level of Long Non-Coding RNA HOTAIR Is Associated with Poor Overall Survival in Gastric Cancer Patients: Evidence from Meta-Analysis. J. BUON 2017, 22, 911–918. [Google Scholar] [PubMed]
- Yao, L.; Ye, P.-C.; Tan, W.; Luo, Y.-J.; Xiang, W.-P.; Liu, Z.-L.; Fu, Z.-M.; Lu, F.; Tang, L.-H.; Xiao, J.-W. Decreased Expression of the Long Non-Coding RNA HOXD-AS2 Promotes Gastric Cancer Progression by Targeting HOXD8 and Activating PI3K/Akt Signaling Pathway. World J. Gastrointest. Oncol. 2020, 12, 1237–1254. [Google Scholar] [CrossRef] [PubMed]
- Hu, Z.; Yang, D.; Tang, Y.; Zhang, X.; Wei, Z.; Fu, H.; Xu, J.; Zhu, Z.; Cai, Q. Five-Long Non-Coding RNA Risk Score System for the Effective Prediction of Gastric Cancer Patient Survival. Oncol. Lett. 2019, 17, 4474–4486. [Google Scholar] [CrossRef] [PubMed]
- Zhong, X.; Wen, X.; Chen, L.; Gu, N.; Yu, X.; Sui, K. Long Non-Coding RNA KCNQ1OT1 Promotes the Progression of Gastric Cancer via the MiR-145-5p/ARF6 Axis. J. Gene Med. 2021, 23, e3330. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Chen, W.; Yang, P.; Jun, Z.; Wang, K.; Tao, Q. Knockdown of Linc00152 Inhibits the Progression of Gastric Cancer by Regulating MicroRNA-193b-3p/ETS1 Axis. Cancer Biol. Ther. 2019, 20, 461–473. [Google Scholar] [CrossRef] [Green Version]
- He, W.; Zhang, D.; Li, D.; Zhu, D.; Geng, Y.; Wang, Q.; He, J.; Wu, J. Knockdown of Long Non-Coding RNA LINC00200 Inhibits Gastric Cancer Progression by Regulating MiR-143-3p/SERPINE1 Axis. Dig. Dis. Sci. 2021, 66, 3404–3414. [Google Scholar] [CrossRef]
- Li, D.; Yang, M.; Liao, A.; Zeng, B.; Liu, D.; Yao, Y.; Hu, G.; Xuanmin, Z.C.; Feng, Z.; Du, Y.; et al. Linc00483 as CeRNA Regulates Proliferation and Apoptosis through Activating MAPKs in Gastric Cancer. J. Cell. Mol. Med. 2018, 22, 3875–3886. [Google Scholar] [CrossRef]
- Pang, K.; Ran, M.-J.; Zou, F.-W.; Yang, T.-W.; He, F. Long Non-Coding RNA LINC00857 Promotes Gastric Cancer Cell Proliferation and Predicts Poor Patient Survival. Oncol. Lett. 2018, 16, 2119–2124. [Google Scholar] [CrossRef] [Green Version]
- Fang, Y.; Huang, S.; Han, L.; Wang, S.; Xiong, B. Comprehensive Analysis of Peritoneal Metastasis Sequencing Data to Identify LINC00924 as a Prognostic Biomarker in Gastric Cancer. Cancer Manag. Res. 2021, 13, 5599–5611. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Wu, N.; Zhang, Z.; Zhong, X.; Zhang, H.; Guo, H.; Nie, Y.; Liu, Y. Long Non-Coding RNA LINC00941 as a Potential Biomarker Promotes the Proliferation and Metastasis of Gastric Cancer. Front. Genet. 2019, 10, 5. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yang, X.-Z.; Cheng, T.-T.; He, Q.-J.; Lei, Z.-Y.; Chi, J.; Tang, Z.; Liao, Q.-X.; Zhang, H.; Zeng, L.-S.; Cui, S.-Z. LINC01133 as CeRNA Inhibits Gastric Cancer Progression by Sponging MiR-106a-3p to Regulate APC Expression and the Wnt/β-Catenin Pathway. Mol. Cancer 2018, 17, 126. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.; Dolo, P.R.; Guo, P.; Hong, J.; Li, C.; Zhu, X.; Zhou, D. The Expression of Long Non-Coding RNA LINC01279 in Gastric Adenocarcinoma and Its Clinical Significance. Asian J. Surg. 2022, 45, 1231–1236. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Wu, Z.; Yuan, J.; Sun, L.; Lin, L.; Huang, N.; Bin, J.; Liao, Y.; Liao, W. Long Non-Coding RNA MALAT1 Promotes Gastric Cancer Tumorigenicity and Metastasis by Regulating Vasculogenic Mimicry and Angiogenesis. Cancer Lett. 2017, 395, 31–44. [Google Scholar] [CrossRef]
- Luo, T.; Zhao, J.; Lu, Z.; Bi, J.; Pang, T.; Cui, H.; Yang, B.; Li, W.; Wang, Y.; Wu, S.; et al. Characterization of Long Non-Coding RNAs and MEF2C-AS1 Identified as a Novel Biomarker in Diffuse Gastric Cancer. Transl. Oncol. 2018, 11, 1080–1089. [Google Scholar] [CrossRef]
- Zhong, F.; Zhu, M.; Gao, K.; Xu, P.; Yang, H.; Hu, D.; Cui, D.; Wang, M.; Xie, X.; Wei, Y.; et al. Low Expression of the Long Non-Coding RNA NR_026827 in Gastric Cancer. Am. J. Transl. Res. 2018, 10, 2706–2711. [Google Scholar]
- Li, J.-F.; Li, W.-H.; Xue, L.-L.; Zhang, Y. Long Non-Coding RNA PICART1 Inhibits Cell Proliferation by Regulating the PI3K/AKT and MAPK/ERK Signaling Pathways in Gastric Cancer. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 588–597. [Google Scholar]
- Chen, H.; Xu, Z.; Liu, X.; Gao, Y.; Wang, J.; Qian, P.; Yang, B. Increased Expression of LncRNA RP11-397A15.4 in Gastric Cancer and Its Clinical Significance. Ann. Clin. Lab. Sci. 2018, 48, 707–711. [Google Scholar]
- Wu, Q.; Ma, J.; Wei, J.; Meng, W.; Wang, Y.; Shi, M. LncRNA SNHG11 Promotes Gastric Cancer Progression by Activating the Wnt/β-Catenin Pathway and Oncogenic Autophagy. Mol. Ther. 2021, 29, 1258–1278. [Google Scholar] [CrossRef]
- Liu, Y.-Y.; Chen, Z.-H.; Peng, J.-J.; Wu, J.-L.; Yuan, Y.-J.; Zhai, E.-T.; Cai, S.-R.; He, Y.-L.; Song, W. Up-Regulation of Long Non-Coding RNA XLOC_010235 Regulates Epithelial-to-Mesenchymal Transition to Promote Metastasis by Associating with Snail1 in Gastric Cancer. Sci. Rep. 2017, 7, 2461. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chai, H.; Sun, C.; Liu, J.; Sheng, H.; Zhao, R.; Feng, Z. The Relationship between ZEB1-AS1 Expression and the Prognosis of Patients with Advanced Gastric Cancer Receiving Chemotherapy. Technol. Cancer Res. Treat. 2019, 18, 1533033819849069. [Google Scholar] [CrossRef]
- Wang, F.; Li, X.; Zhao, X.; Xue, Y. Detection of a 5-CircRNA Signature to Improve Prognostic Prediction in Gastric Cancer. J. Investig. Med. 2020, 68, 762–769. [Google Scholar] [CrossRef] [PubMed]
- Xian, H.-P.; Zhuo, Z.-L.; Sun, Y.-J.; Liang, B.; Zhao, X.-T. Circulating Long Non-Coding RNAs HULC and ZNFX1-AS1 Are Potential Biomarkers in Patients with Gastric Cancer. Oncol. Lett. 2018, 16, 4689–4698. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jiao, Y.; Zhang, L.; Li, J.; He, Y.; Zhang, X.; Li, J. Exosomal MiR-122-5p Inhibits Tumorigenicity of Gastric Cancer by Downregulating GIT1. Int. J. Biol. Mark. 2021, 36, 36–46. [Google Scholar] [CrossRef]
- Sui, M.; Jiao, A.; Zhai, H.; Wang, Y.; Wang, Y.; Sun, D.; Li, P. Upregulation of MiR-125b Is Associated with Poor Prognosis and Trastuzumab Resistance in HER2-Positive Gastric Cancer. Exp. Ther. Med. 2017, 14, 657–663. [Google Scholar] [CrossRef] [Green Version]
- Azarbarzin, S.; Feizi, M.A.H.; Safaralizadeh, R.; Kazemzadeh, M.; Fateh, A. The Value of MiR-383, an Intronic MiRNA, as a Diagnostic and Prognostic Biomarker in Intestinal-Type Gastric Cancer. Biochem. Genet. 2017, 55, 244–252. [Google Scholar] [CrossRef]
- Schaalan, M.; Mohamed, W.; Fathy, S. MiRNA-200c, MiRNA-139 and Ln RNA H19; New Predictors of Treatment Response in H-Pylori- Induced Gastric Ulcer or Progression to Gastric Cancer. Microb. Pathog. 2020, 149, 104442. [Google Scholar] [CrossRef]
- Liu, L.; Liu, F.-B.; Huang, M.; Xie, K.; Xie, Q.-S.; Liu, C.-H.; Shen, M.-J.; Huang, Q. Circular RNA CiRS-7 Promotes the Proliferation and Metastasis of Pancreatic Cancer by Regulating MiR-7-Mediated EGFR/STAT3 Signaling Pathway. Hepatobiliary Pancreat. Dis. Int. 2019, 18, 580–586. [Google Scholar] [CrossRef]
- Wong, C.H.; Lou, U.K.; Fung, F.K.-C.; Tong, J.H.M.; Zhang, C.-H.; To, K.-F.; Chan, S.L.; Chen, Y. CircRTN4 Promotes Pancreatic Cancer Progression through a Novel CircRNA-MiRNA-LncRNA Pathway and Stabilizing Epithelial-Mesenchymal Transition Protein. Mol. Cancer 2022, 21, 10. [Google Scholar] [CrossRef]
- Ma, L.; Tian, X.; Guo, H.; Zhang, Z.; Du, C.; Wang, F.; Xie, X.; Gao, H.; Zhuang, Y.; Kornmann, M.; et al. Long Noncoding RNA H19 Derived MiR-675 Regulates Cell Proliferation by down-Regulating E2F-1 in Human Pancreatic Ductal Adenocarcinoma. J. Cancer 2018, 9, 389–399. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fu, Z.; Li, G.; Li, Z.; Wang, Y.; Zhao, Y.; Zheng, S.; Ye, H.; Luo, Y.; Zhao, X.; Wei, L.; et al. Endogenous MiRNA Sponge LincRNA-ROR Promotes Proliferation, Invasion and Stem Cell-like Phenotype of Pancreatic Cancer Cells. Cell Death Discov. 2017, 3, 17004. [Google Scholar] [CrossRef] [Green Version]
- Wang, L.; Wang, F.; Na, L.; Yu, J.; Huang, L.; Meng, Z.-Q.; Chen, Z.; Chen, H.; Ming, L.-L.; Hua, Y.-Q. LncRNA AB209630 Inhibits Gemcitabine Resistance Cell Proliferation by Regulating PI3K/AKT Signaling in Pancreatic Ductal Adenocarcinoma. Cancer Biomark. 2018, 22, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Yun, Z.; Meng, F.; Li, S.; Zhang, P. Long Non-Coding RNA CERS6-AS1 Facilitates the Oncogenicity of Pancreatic Ductal Adenocarcinoma by Regulating the MicroRNA-15a-5p/FGFR1 Axis. Aging 2021, 13, 6041–6054. [Google Scholar] [CrossRef]
- Yong, S.; Yabin, Y.; Bing, Z.; Chuanrong, Z.; Dianhua, G.; Jianhuai, Z.; Weidong, Y.; Shuming, W.; Ling, L. Reciprocal Regulation of DGCR5 and MiR-320a Affects the Cellular Malignant Phenotype and 5-FU Response in Pancreatic Ductal Adenocarcinoma. Oncotarget 2017, 8, 90868–90878. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gao, S.; Cai, Y.; Zhang, H.; Hu, F.; Hou, L.; Xu, Q. Long Noncoding RNA DLEU1 Aggravates Pancreatic Ductal Adenocarcinoma Carcinogenesis via the MiR-381/CXCR4 Axis. J. Cell. Physiol. 2019, 234, 6746–6757. [Google Scholar] [CrossRef]
- Ye, H.; Zhou, Q.; Zheng, S.; Li, G.; Lin, Q.; Ye, L.; Wang, Y.; Wei, L.; Zhao, X.; Li, W.; et al. FEZF1-AS1/MiR-107/ZNF312B Axis Facilitates Progression and Warburg Effect in Pancreatic Ductal Adenocarcinoma. Cell Death Dis. 2018, 9, 34. [Google Scholar] [CrossRef]
- Sun, Y.; Zhu, Q.; Yang, W.; Shan, Y.; Yu, Z.; Zhang, Q.; Wu, H. LncRNA H19/MiR-194/PFTK1 Axis Modulates the Cell Proliferation and Migration of Pancreatic Cancer. J. Cell. Biochem. 2019, 120, 3874–3886. [Google Scholar] [CrossRef]
- Fu, Z.; Chen, C.; Zhou, Q.; Wang, Y.; Zhao, Y.; Zhao, X.; Li, W.; Zheng, S.; Ye, H.; Wang, L.; et al. LncRNA HOTTIP Modulates Cancer Stem Cell Properties in Human Pancreatic Cancer by Regulating HOXA9. Cancer Lett. 2017, 410, 68–81. [Google Scholar] [CrossRef]
- Yang, M.; Qin, Q.; Zhu, J.; Guo, Y.; Yin, T.; Wu, H.; Wang, C. Long Noncoding RNA ITGB2-AS1 Promotes Growth and Metastasis through MiR-4319/RAF1 Axis in Pancreatic Ductal Adenocarcinoma. J. Cell. Physiol. 2020, 1–14. [Google Scholar] [CrossRef]
- Wu, J.; Sun, S.; Liao, W.; Chen, E.; Wang, X.; Song, Y.; Duan, F.; Deng, W.; Li, S. LINC00460 Promotes Pancreatic Cancer Progression by Sponging MiR-491-5p. J. Gene Med. 2021, 23, e3333. [Google Scholar] [CrossRef] [PubMed]
- Ni, C.; Zheng, K.; Liu, W.; Ou, Y.; Li, G.; Jin, G. LINC00483 Promotes Proliferation and Metastasis through the MiR-19a-3p/TBK1/MAPK Axis in Pancreatic Ductal Adenocarcinoma (PDAC). Ann. Transl. Med. 2022, 10, 317. [Google Scholar] [CrossRef] [PubMed]
- Bi, S.; Wang, Y.; Feng, H.; Li, Q. Long Noncoding RNA LINC00657 Enhances the Malignancy of Pancreatic Ductal Adenocarcinoma by Acting as a Competing Endogenous RNA on MicroRNA-433 to Increase PAK4 Expression. Cell Cycle 2020, 19, 801–816. [Google Scholar] [CrossRef] [PubMed]
- Lu, W.; Zhang, H.; Niu, Y.; Wu, Y.; Sun, W.; Li, H.; Kong, J.; Ding, K.; Shen, H.-M.; Wu, H.; et al. Long Non-Coding RNA Linc00673 Regulated Non-Small Cell Lung Cancer Proliferation, Migration, Invasion and Epithelial Mesenchymal Transition by Sponging MiR-150-5p. Mol. Cancer 2017, 16, 118. [Google Scholar]
- Xu, M.; Cui, R.; Ye, L.; Wang, Y.; Wang, X.; Zhang, Q.; Wang, K.; Dong, C.; Le, W.; Chen, B. LINC00941 Promotes Glycolysis in Pancreatic Cancer by Modulating the Hippo Pathway. Mol. Ther. Nucleic Acids 2021, 26, 280–294. [Google Scholar] [CrossRef]
- Chen, M.; Zhang, C.; Liu, W.; Du, X.; Liu, X.; Xing, B. Long Noncoding RNA LINC01234 Promotes Hepatocellular Carcinoma Progression through Orchestrating Aspartate Metabolic Reprogramming. Mol. Ther. 2022, 30, 2354–2369. [Google Scholar] [CrossRef]
- Nai, Y.; Pan, C.; Hu, X.; Ma, Y. LncRNA LUCAT1 Contributes to Cell Proliferation and Migration in Human Pancreatic Ductal Adenocarcinoma via Sponging MiR-539. Cancer Med. 2020, 9, 757–767. [Google Scholar] [CrossRef] [Green Version]
- Liu, P.; Yang, H.; Zhang, J.; Peng, X.; Lu, Z.; Tong, W.; Chen, J. The LncRNA MALAT1 Acts as a Competing Endogenous RNA to Regulate KRAS Expression by Sponging MiR-217 in Pancreatic Ductal Adenocarcinoma. Sci. Rep. 2017, 7, 5186. [Google Scholar] [CrossRef] [Green Version]
- Zhuo, M.; Yuan, C.; Han, T.; Cui, J.; Jiao, F.; Wang, L. A Novel Feedback Loop between High MALAT-1 and Low MiR-200c-3p Promotes Cell Migration and Invasion in Pancreatic Ductal Adenocarcinoma and Is Predictive of Poor Prognosis. BMC Cancer 2018, 18, 1032. [Google Scholar] [CrossRef] [Green Version]
- Sun, Y.; Wang, P.; Yang, W.; Shan, Y.; Zhang, Q.; Wu, H. The Role of LncRNA MSC-AS1/MiR-29b-3p Axis-Mediated CDK14 Modulation in Pancreatic Cancer Proliferation and Gemcitabine-Induced Apoptosis. Cancer Biol. Ther. 2019, 20, 729–739. [Google Scholar] [CrossRef]
- Luo, Z.; Yi, Z.-J.; Ou, Z.-L.; Han, T.; Wan, T.; Tang, Y.-C.; Wang, Z.-C.; Huang, F.-Z. RELA/NEAT1/MiR-302a-3p/RELA Feedback Loop Modulates Pancreatic Ductal Adenocarcinoma Cell Proliferation and Migration. J. Cell. Physiol. 2019, 234, 3583–3597. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Li, H.; Lu, X.; Wen, C.; Huo, Z.; Shi, M.; Tang, X.; Chen, H.; Peng, C.; Fang, Y.; et al. Melittin-Induced Long Non-Coding RNA NONHSAT105177 Inhibits Proliferation and Migration of Pancreatic Ductal Adenocarcinoma. Cell Death Dis. 2018, 9, 940. [Google Scholar] [CrossRef] [Green Version]
- Wu, L.; Liu, Y.; Guo, C.; Shao, Y. LncRNA OIP5-AS1 Promotes the Malignancy of Pancreatic Ductal Adenocarcinoma via Regulating MiR-429/FOXD1/ERK Pathway. Cancer Cell Int. 2020, 20, 296. [Google Scholar] [CrossRef]
- Zhang, Y.; Ma, H.; Chen, C. Long Non-coding RNA PCED1B-AS1 Promotes Pancreatic Ductal Adenocarcinoma Progression by Regulating the MiR-411-3p/HIF-1α Axis. Oncol. Rep. 2021, 46, 134. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Tang, J.; Zhang, H.; Kong, F.; Zhu, H.; Li, P.; Li, Z.; Kong, X.; Wang, K. A Novel LncRNA PTTG3P/MiR-132/212-3p/FoxM1 Feedback Loop Facilitates Tumorigenesis and Metastasis of Pancreatic Cancer. Cell Death Discov. 2020, 6, 136. [Google Scholar] [CrossRef] [PubMed]
- Sun, J.; Zhang, P.; Yin, T.; Zhang, F.; Wang, W. Upregulation of LncRNA PVT1 Facilitates Pancreatic Ductal Adenocarcinoma Cell Progression and Glycolysis by Regulating MiR-519d-3p and HIF-1A. J. Cancer 2020, 11, 2572–2579. [Google Scholar] [CrossRef]
- Huang, S.; Li, Y.; Hu, J.; Li, L.; Liu, Z.; Guo, H.; Jiang, B.; Chen, J.; Junhe, X.L.; Xiang, X.; et al. LncRNA PWAR6 Regulates Proliferation and Migration by Epigenetically Silencing YAP1 in Tumorigenesis of Pancreatic Ductal Adenocarcinoma. J. Cell. Mol. Med. 2021, 25, 4275–4286. [Google Scholar] [CrossRef]
- Li, N.; Yang, G.; Luo, L.; Ling, L.; Wang, X.; Shi, L.; Lan, J.; Jia, X.; Zhang, Q.; Long, Z.; et al. LncRNA THAP9-AS1 Promotes Pancreatic Ductal Adenocarcinoma Growth and Leads to a Poor Clinical Outcome via Sponging MiR-484 and Interacting with YAP. Clin. Cancer Res. 2020, 26, 1736–1748. [Google Scholar] [CrossRef] [Green Version]
- Miao, H.; Lu, J.; Guo, Y.; Qiu, H..; Zhang, Y.; Yao, X.; Li, X.; Lu, Y. LncRNA TP73-AS1 Enhances the Malignant Properties of Pancreatic Ductal Adenocarcinoma by Increasing MMP14 Expression through MiRNA -200a Sponging. J. Cell. Mol. Med. 2021, 25, 3654–3664. [Google Scholar] [CrossRef]
- Bai, J.; Yao, B.; Wang, L.; Sun, L.; Chen, T.; Liu, R.; Yin, G.; Qiuran, X.; Yang, W. LncRNA A1BG-AS1 Suppresses Proliferation and Invasion of Hepatocellular Carcinoma Cells by Targeting MiR-216a-5p. J. Cell. Biochem. 2019, 120, 10310–10322. [Google Scholar] [CrossRef]
- Zeng, T.; Wang, D.; Chen, J.; Tian, Y.; Cai, X.; Peng, H.; Zhu, L.; Huang, A.; Tang, H. LncRNA-AF113014 Promotes the Expression of Egr2 by Interaction with MiR-20a to Inhibit Proliferation of Hepatocellular Carcinoma Cells. PLoS ONE 2017, 12, e0177843. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Zhu, L.; Xue, Q.; Tang, C.; Tang, W.; Zhang, N.; Dai, C.; Chen, Z. Novel LncRNA AL033381.2 Promotes Hepatocellular Carcinoma Progression by Upregulating PRKRA Expression. Oxid. Med. Cell. Longev. 2022, 2022, 1125932. [Google Scholar] [CrossRef]
- Zhao, X.; Liu, Y.; Yu, S. Long Noncoding RNA AWPPH Promotes Hepatocellular Carcinoma Progression through YBX1 and Serves as a Prognostic Biomarker. Biochim. Biophys. Acta 2017, 1863, 1805–1816. [Google Scholar] [CrossRef] [PubMed]
- Chen, F.; Bai, G.; Li, Y.; Feng, Y.; Wang, L. A Positive Feedback Loop of Long Noncoding RNA CCAT2 and FOXM1 Promotes Hepatocellular Carcinoma Growth. Am. J. Cancer Res. 2017, 7, 1423–1434. [Google Scholar]
- Zhuang, H.; Cao, G.; Kou, C.; Li, D. Overexpressed LncRNA CDKN2B-AS1 Is an Independent Prognostic Factor for Liver Cancer and Promotes Its Proliferation. J. BUON 2019, 24, 1441–1448. [Google Scholar] [PubMed]
- Chao, Y.; Zhou, D. LncRNA-D16366 Is a Potential Biomarker for Diagnosis and Prognosis of Hepatocellular Carcinoma. Med. Sci. Monit. 2019, 25, 6581–6586. [Google Scholar] [CrossRef]
- Li, B.; Mao, R.; Liu, C.; Zhang, W.; Tang, Y.; Guo, Z. LncRNA FAL1 Promotes Cell Proliferation and Migration by Acting as a CeRNA of MiR-1236 in Hepatocellular Carcinoma Cells. Life Sci. 2018, 197, 122–129. [Google Scholar] [CrossRef]
- Chen, F.; Li, Y.; Li, M.; Wang, L. Long Noncoding RNA GAS5 Inhibits Metastasis by Targeting MiR-182/ANGPTL1 in Hepatocellular Carcinoma. Am. J. Cancer Res. 2019, 9, 108–121. [Google Scholar]
- Yu, J.; Hong, J.-F.; Kang, J.; Liao, L.-H.; Li, C.-D. Promotion of LncRNA HOXA11-AS on the Proliferation of Hepatocellular Carcinoma by Regulating the Expression of LATS1. Eur. Rev. Med. Pharmacol. Sci. 2017, 21, 3402–3411. [Google Scholar]
- Zhou, J.-F.; Shi, Y.-T.; Wang, H.-G.; Yang, X.-Z.; Wu, S.-N. Overexpression of Long Noncoding RNA HOXC13-AS and Its Prognostic Significance in Hepatocellular Carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 7369–7374. [Google Scholar]
- Xiong, H.; Ni, Z.; He, J.; Jiang, S.; Li, X.; He, J.; Gong, W.; Zheng, L.; Chen, S.; Li, B.; et al. LncRNA HULC Triggers Autophagy via Stabilizing Sirt1 and Attenuates the Chemosensitivity of HCC Cells. Oncogene 2017, 36, 3528–3540. [Google Scholar] [CrossRef] [PubMed]
- Xiong, H.; Li, B.; He, J.; Zeng, Y.; Zhang, Y.; He, F. LncRNA HULC Promotes the Growth of Hepatocellular Carcinoma Cells via Stabilizing COX-2 Protein. Biochem. Biophys. Res. Commun. 2017, 490, 693–699. [Google Scholar] [CrossRef] [PubMed]
- Xu, L.-C.; Chen, Q.-N.; Liu, X.-Q.; Wang, X.-M.; Chang, Q.-M.; Pan, Q.; Wang, L.; Wang, Y.-L. Up-Regulation of LINC00161 Correlates with Tumor Migration and Invasion and Poor Prognosis of Patients with Hepatocellular Carcinoma. Oncotarget 2017, 8, 56168–56173. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gao, J.; Dai, C.; Yu, X.; Yin, X.-B.; Zhou, F. Long Noncoding RNA LINC00324 Exerts Protumorigenic Effects on Liver Cancer Stem Cells by Upregulating Fas Ligand via PU Box Binding Protein. FASEB J. 2020, 34, 5800–5817. [Google Scholar] [CrossRef]
- Yin, Y.-Z.; Zheng, W.-H.; Zhang, X.; Chen, Y.-H.; Tuo, Y.-H. LINC00346 Promotes Hepatocellular Carcinoma Progression via Activating the JAK-STAT3 Signaling Pathway. J. Cell. Biochem. 2020, 121, 735–742. [Google Scholar] [CrossRef]
- Wu, J.-H.; Tian, X.-Y.; An, Q.-M.; Guan, X.-Y.; Hao, C.-Y. LINC00963 Promotes Hepatocellular Carcinoma Progression by Activating PI3K/AKT Pathway. Eur. Rev. Med. Pharmacol. Sci. 2018, 22, 1645–1652. [Google Scholar]
- Zheng, Y.-L.; Li, L.; Jia, Y.-X.; Zhang, B.-Z.; Li, J.-C.; Zhu, Y.-H.; Li, M.-Q.; He, J.-Z.; Zeng, T.-T.; Ban, X.-J.; et al. LINC01554-Mediated Glucose Metabolism Reprogramming Suppresses Tumorigenicity in Hepatocellular Carcinoma via Downregulating PKM2 Expression and Inhibiting Akt/MTOR Signaling Pathway. Theranostics 2019, 9, 796–810. [Google Scholar] [CrossRef]
- Chen, M.H.; Qi, B.; Cai, Q.Q.; Sun, J.W.; Fu, L.S.; Kang, C.L.; Fan, F.; Ma, M.Z.; Wu, X.Z. LncRNA LncAY Is Upregulated by Sulfatide via Myb/MEF2C Acetylation to Promote the Tumorigenicity of Hepatocellular Carcinoma Cells. Biochim. Biophys. Acta Gene Regul. Mech. 2022, 1865, 194777. [Google Scholar] [CrossRef]
- Dong, H.; Zhang, Y.; Xu, Y.; Ma, R.; Liu, L.; Luo, C.; Jiang, W. Downregulation of Long Non-Coding RNA MEG3 Promotes Proliferation, Migration, and Invasion of Human Hepatocellular Carcinoma Cells by Upregulating TGF-Β1. Acta Biochim. Biophys. Sin. 2019, 51, 645–652. [Google Scholar] [CrossRef]
- Shen, X.; Ding, Y.; Lu, F.; Yuan, H.; Luan, W. Long Noncoding RNA MIR4435-2HG Promotes Hepatocellular Carcinoma Proliferation and Metastasis through the MiR-22-3p/YWHAZ Axis. Am. J. Transl. Res. 2020, 12, 6381–6394. [Google Scholar]
- Kong, Q.; Liang, C.; Jin, Y.; Pan, Y.; Tong, D.; Kong, Q.; Zhou, J. The LncRNA MIR4435-2HG Is Upregulated in Hepatocellular Carcinoma and Promotes Cancer Cell Proliferation by Upregulating MiRNA-487a. Cell. Mol. Biol. Lett. 2019, 24, 26. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wang, H.; Liang, L.; Dong, Q.; Huan, L.; He, J.; Li, B.; Yang, C.; Jin, H.; Lin, C.W.; Yu, C.; et al. Long Noncoding RNA MiR503HG, a Prognostic Indicator, Inhibits Tumor Metastasis by Regulating the HNRNPA2B1/NF-ΚB Pathway in Hepatocellular Carcinoma. Theranostics 2018, 8, 2814–2829. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Zhao, S.-Y.; Jiang, Q.; Qu, Y.; Huang, X.; Du, J.; Sun, W.; Ye, Q. Long Noncoding RNA MYLK-AS1 Promotes Growth and Invasion of Hepatocellular Carcinoma through the EGFR/HER2-ERK1/2 Signaling Pathway. Int. J. Biol. Sci. 2020, 16, 1989–2000. [Google Scholar] [CrossRef] [PubMed]
- Ling, Z.-A.; Xiong, D.-D.; Meng, R.-M.; Cen, J.-M.; Zhao, N.; Chen, G.; Li, R.-L.; Dang, Y.-W. LncRNA NEAT1 Promotes Deterioration of Hepatocellular Carcinoma Based on in Vitro Experiments, Data Mining, and RT-QPCR Analysis. Cell. Physiol. Biochem. 2018, 48, 540–555. [Google Scholar] [CrossRef]
- Fang, L.; Sun, J.; Pan, Z.; Song, Y.; Zhong, L.; Zhang, Y.; Liu, Y.; Zheng, X.; Huang, P. Long Non-Coding RNA NEAT1 Promotes Hepatocellular Carcinoma Cell Proliferation through the Regulation of MiR-129-5p-VCP-IκB. Am. J. Physiol. Gastrointest. Liver Physiol. 2017, 313, G150–G156. [Google Scholar] [CrossRef]
- Li, W.; Fu, Q.; Man, W.; Guo, H.; Yang, P. LncRNA OR3A4 Participates in the Angiogenesis of Hepatocellular Carcinoma through Modulating AGGF1/Akt/MTOR Pathway. Eur. J. Pharmacol. 2019, 849, 106–114. [Google Scholar] [CrossRef]
- Qi, H.; Lu, Y.; Lv, J.; Wu, H.; Jing, C.L.; Zhang, C.; Zhang, S.; Bao, Q.; Zhang, X.; Xie, C.; et al. The Long Noncoding RNA LncPARP1 Contributes to Progression of Hepatocellular Carcinoma through Up-Regulation of PARP1. Biosci. Rep. 2018, 38, 1–38. [Google Scholar] [CrossRef] [Green Version]
- Yu, A.T.; Berasain, C.; Bhatia, S.; Rivera, K.; Liu, B.; Rigo, F.; Pappin, D.J.; Spector, D.L. PHAROH LncRNA Regulates Myc Translation in Hepatocellular Carcinoma via Sequestering TIAR. Elife 2021, 10, 1–34. [Google Scholar] [CrossRef]
- Xiang, X.; Fu, Y.; Zhao, K.; Miao, R.; Zhang, X.; Ma, X.; Liu, C.; Zhang, N.; Qu, K. Cellular Senescence in Hepatocellular Carcinoma Induced by a Long Non-Coding RNA-Encoded Peptide PINT87aa by Blocking FOXM1-Mediated PHB2. Theranostics 2021, 11, 4929–4944. [Google Scholar] [CrossRef]
- Zhang, Y.; Wen, D.-Y.; Zhang, R.; Huang, J.; Lin, P.; Ren, F.-H.; Wang, X.; He, Y.; Yang, H.; Chen, G.; et al. A Preliminary Investigation of PVT1 on the Effect and Mechanisms of Hepatocellular Carcinoma: Evidence from Clinical Data, a Meta-Analysis of 840 Cases, and in Vivo Validation. Cell. Physiol. Biochem. 2018, 47, 2216–2232. [Google Scholar] [CrossRef]
- Hongfeng, Z.; Andong, J.; Liwen, S.; Minping, B.; Xiaowei, Y.; Mingyong, L.; Aimin, Y. LncRNA RMRP Knockdown Suppress Hepatocellular Carcinoma Biological Activities via Regulation MiRNA-206/TACR1. J. Cell. Biochem. 2020, 121, 1690–1702. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Lu, L.; Feng, B.; Zhang, K.; Han, S.; Hou, D.; Chen, L.; Chu, X.; Wang, R. The LincRNA-ROR/MiR-145 Axis Promotes Invasion and Metastasis in Hepatocellular Carcinoma via Induction of Epithelial-Mesenchymal Transition by Targeting ZEB2. Sci. Rep. 2017, 7, 4637. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Wang, S.; Yang, F.; Meng, Z.; Liu, Y. LncRNA ROR1-AS1 High Expression and Its Prognostic Significance in Liver Cancer. Oncol. Rep. 2020, 43, 55–74. [Google Scholar] [CrossRef]
- Jiang, X.; Wang, G.; Liu, Y.; Mei, C.; Yao, Y.; Wu, X.; Chen, X.; Ma, W.; Li, K.; Zhang, Z.; et al. A Novel Long Non-Coding RNA RP11-286H15.1 Represses Hepatocellular Carcinoma Progression by Promoting Ubiquitination of PABPC4. Cancer Lett. 2021, 499, 109–121. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.-M.; Li, L.; Ren, L.-L.; Du, L.; Wang, Y.-M. LncRNA SNHG17 Predicts Poor Prognosis and Promotes Cell Proliferation and Migration in Hepatocellular Carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 4219–4227. [Google Scholar] [PubMed]
- Liu, J.; Lu, C.; Xiao, M.; Jiang, F.; Qu, L.; Ni, R. Long Non-Coding RNA SNHG20 Predicts a Poor Prognosis for HCC and Promotes Cell Invasion by Regulating the Epithelial-to-Mesenchymal Transition. Biomed. Pharmacother. 2017, 89, 857–863. [Google Scholar] [CrossRef]
- Shen, A.; Ma, J.; Hu, X.; Cui, X. High Expression of LncRNA-SNHG7 Is Associated with Poor Prognosis in Hepatocellular Carcinoma. Oncol. Lett. 2020, 19, 3959–3963. [Google Scholar] [CrossRef] [Green Version]
- Dong, J.; Teng, F.; Guo, W.; Yang, J.; Ding, G.; Fu, Z. LncRNA SNHG8 Promotes the Tumorigenesis and Metastasis by Sponging MiR-149-5p and Predicts Tumor Recurrence in Hepatocellular Carcinoma. Cell. Physiol. Biochem. 2018, 51, 2262–2274. [Google Scholar] [CrossRef]
- Ye, S.; Ni, Y. LncRNA SNHG9 Promotes Cell Proliferation, Migration, and Invasion in Human Hepatocellular Carcinoma Cells by Increasing GSTP1 Methylation, as Revealed by CRISPR-DCas9. Front. Mol. Biosci. 2021, 8, 649976. [Google Scholar] [CrossRef]
- Hu, S.; Liu, J.; Feng, S.; Wang, Y.; Liu, H. LncRNA SUMO1P3 Acts as a Prognostic Biomarker and Promotes Hepatocellular Carcinoma Growth and Metastasis. Aging 2021, 13, 12479–12492. [Google Scholar] [CrossRef]
- Liu, W.; Huai, R.; Zhang, Y.; Rao, S.; Xiong, L.; Ding, R.; Mao, C.; Zhao, W.; Hao, T.; Huang, Q.; et al. Down-Regulation Expression of TGFB2-AS1 Inhibits the Proliferation, Migration, Invasion and Induces Apoptosis in HepG2 Cells. Genes Genom. 2019, 41, 951–959. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Huang, F.; Deng, L.; Tang, Y.; Li, D.; Wang, T.; Fan, Y.; Tao, Q.; Tang, D. Long Non-Coding RNA TGLC15 Advances Hepatocellular Carcinoma by Stabilizing Sox4. J. Clin. Lab. Anal. 2020, 34, e23009. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yao, J.; Hua, X.; Shi, J.; Hu, X.; Lui, K.; He, K.; Mai, J.; Lan, T.; Lu, M. LncRNA THEMIS2-211, a Tumor-Originated Circulating Exosomal Biomarker, Promotes the Growth and Metastasis of Hepatocellular Carcinoma by Functioning as a Competing Endogenous RNA. FASEB J. 2022, 36, e22238. [Google Scholar] [CrossRef] [PubMed]
- Xu, C.; Huang, Q.; Zhang, C.; Xu, W.; Xu, G.; Zhao, X.; Liu, X.; Du, Y. Long Non-Coding RNA TRPM2-AS as a Potential Biomarker for Hepatocellular Carcinoma. Ir. J. Med. Sci. 2018, 187, 621–628. [Google Scholar] [CrossRef] [Green Version]
- Lu, J.; Li, B.; Xiong, X.; Cheng, N. RNA Sequencing Reveals the Long Noncoding RNA and MRNA Profiles and Identifies Long Non-Coding RNA TSPAN12 as a Potential Microvascular Invasion-Related Biomarker in Hepatocellular Carcinoma. Biomed. Pharmacother. 2020, 126, 110111. [Google Scholar] [CrossRef]
- Yan, J.; Zhou, C.; Guo, K.; Li, Q.; Wang, Z. A Novel Seven-LncRNA Signature for Prognosis Prediction in Hepatocellular Carcinoma. J. Cell. Biochem. 2019, 120, 213–223. [Google Scholar] [CrossRef] [Green Version]
- Gu, J.-X.; Zhang, X.; Miao, R.-C.; Xiang, X.-H.; Fu, Y.-N.; Zhang, J.-Y.; Liu, C.; Qu, K. Six-Long Non-Coding RNA Signature Predicts Recurrence-Free Survival in Hepatocellular Carcinoma. World J. Gastroenterol. 2019, 25, 220–232. [Google Scholar] [CrossRef]
- Zhao, X.; Bai, Z.; Li, C.; Sheng, C.; Li, H. Identification of a Novel Eight-LncRNA Prognostic Signature for HBV-HCC and Analysis of Their Functions Based on Coexpression and CeRNA Networks. Biomed Res. Int. 2020, 2020, 8765461. [Google Scholar] [CrossRef] [Green Version]
- Bao, L.; Zhang, M.; Han, S.; Zhan, Y.; Guo, W.; Teng, F.; Liu, F.; Guo, M.; Zhang, L.; Ding, G.; et al. MicroRNA-500a Promotes the Progression of Hepatocellular Carcinoma by Post-Transcriptionally Targeting BID. Cell. Physiol. Biochem. 2018, 47, 2046–2055. [Google Scholar] [CrossRef]
- Sadeghpour, S.; Ghorbian, S. Evaluation of the Potential Clinical Prognostic Value of LncRNA-BANCR Gene in Esophageal Squamous Cell Carcinoma. Mol. Biol. Rep. 2019, 46, 991–995. [Google Scholar] [CrossRef]
- Bahramian, S.; Sahebi, R.; Roohinejad, Z.; Delshad, E.; Javid, N.; Amini, A.; Razavi, A.E.; Shafiee, M.; Shamsabadi, F.T. Low Expression of LncRNA-CAF Attributed to the High Expression of HIF1A in Esophageal Squamous Cell Carcinoma and Gastric Cancer Patients. Mol. Biol. Rep. 2022, 49, 895–905. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Hu, L.; Liang, Y.; Li, J.; Wang, K.; Chen, X.; Meng, H.; Guan, X.; Yang, K.; Bai, Y. Up-Regulation of LncRNA CASC9 Promotes Esophageal Squamous Cell Carcinoma Growth by Negatively Regulating PDCD4 Expression through EZH2. Mol. Cancer 2017, 16, 150. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Liu, H.; Zhen, Q.; Fan, Y. LncRNA GHET1 Promotes Esophageal Squamous Cell Carcinoma Cells Proliferation and Invasion via Induction of EMT. Int. J. Biol. Markers 2017, 32, e403–e408. [Google Scholar] [CrossRef] [Green Version]
- Li, X.; Yang, H.; Wang, J.; Li, X.; Fan, Z.; Zhao, J.; Liu, L.; Zang, M.; Goscinski, M.A.; Wang, J.; et al. High Level of LncRNA H19 Expression Is Associated with Shorter Survival in Esophageal Squamous Cell Cancer Patients. Pathol. Res. Pract. 2019, 215, 152638. [Google Scholar] [CrossRef] [PubMed]
- Liang, Y.; Wu, Y.; Chen, X.; Zhang, S.; Wang, K.; Guan, X.; Yang, K.; Li, J.; Bai, Y. A Novel Long Noncoding RNA Linc00460 Up-Regulated by CBP/P300 Promotes Carcinogenesis in Esophageal Squamous Cell Carcinoma. Biosci. Rep. 2017, 37, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Liang, Y.; Wu, Y.; Chen, X.; Wang, K.; Li, J.; Guan, X.; Gang, X.; Yang, K.; Bai, Y. Upregulation of a Novel LncRNA LINC01980 Promotes Tumor Growth of Esophageal Squamous Cell Carcinoma. Biochem. Biophys. Res. Commun. 2019, 513, 73–80. [Google Scholar] [CrossRef]
- Zang, B.; Zhao, J.; Chen, C. LncRNA PCAT-1 Promoted ESCC Progression via Regulating ANXA10 Expression by Sponging MiR-508-3p. Cancer Manag. Res. 2019, 11, 10841–10849. [Google Scholar] [CrossRef]
- Dong, Z.; Liang, X.; Wu, X.; Kang, X.; Guo, Y.; Shen, S.; Liang, J.; Guo, W. Promoter Hypermethylation-Mediated Downregulation of Tumor Suppressor Gene SEMA3B and LncRNA SEMA3B-AS1 Correlates with Progression and Prognosis of Esophageal Squamous Cell Carcinoma. Clin. Exp. Metastasis 2019, 36, 225–241. [Google Scholar] [CrossRef]
- Han, G.-H.; Lu, K.-J.; Wang, P.; Ye, J.; Ye, Y.-Y.; Huang, J.-X. LncRNA SNHG16 Predicts Poor Prognosis in ESCC and Promotes Cell Proliferation and Invasion by Regulating Wnt/β-Catenin Signaling Pathway. Eur. Rev. Med. Pharmacol. Sci. 2018, 22, 3795–3803. [Google Scholar]
- Weng, N.-Q.; Chi, J.; Wen, J.; Mai, S.-J.; Zhang, M.-Y.; Huang, L.; Liu, J.; Yang, X.-Z.; Xu, G.-L.; Fu, J.-H.; et al. The Prognostic Value of a Seven-LncRNA Signature in Patients with Esophageal Squamous Cell Carcinoma: A LncRNA Expression Analysis. J. Transl. Med. 2020, 18, 47. [Google Scholar] [CrossRef] [Green Version]
- Chen, J.; Shen, Z.; Deng, H.; Zhou, W.; Liao, Q.; Mu, Y. Long Non-Coding RNA Biomarker for Human Laryngeal Squamous Cell Carcinoma Prognosis. Gene 2018, 671, 96–102. [Google Scholar] [CrossRef] [PubMed]
- Zong, M.-Z.; Shao, Q.; An, X.-S. Expression and Prognostic Significance of Long Noncoding RNA AK001796 in Esophageal Squamous Cell Carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 181–186. [Google Scholar] [PubMed]
- Cao, T.; Shen, J.; Pan, W.; Li, C.; Qiao, Z. Upregulation of Long Noncoding RNA ANRIL Correlates with Tumor Progression and Poor Prognosis in Esophageal Squamous Cell Carcinoma. J. BUON 2018, 23, 1862–1866. [Google Scholar] [PubMed]
- Wang, M.; Li, Y.; Yang, Y.; Liu, X.; Zang, M.; Li, Y.; Yang, K.; Yang, W.; Zhang, S. Long Non-coding RNA DLX6-AS1 Is Associated with Malignant Progression and Promotes Proliferation and Invasion in Esophageal Squamous Cell Carcinoma. Mol. Med. Rep. 2019, 19, 1942–1950. [Google Scholar] [CrossRef] [Green Version]
- Bao, J.; Zhou, C.; Zhang, J.; Mo, J.; Ye, Q.; He, J.; Diao, J. Upregulation of the Long Noncoding RNA FOXD2-AS1 Predicts Poor Prognosis in Esophageal Squamous Cell Carcinoma. Cancer Biomark. 2018, 21, 527–533. [Google Scholar] [CrossRef]
- Zong, M.-Z.; Feng, W.-T.; Du, N.; Yu, X.-J.; Yu, W.-Y. Upregulation of Long Noncoding RNA LEF1-AS1 Predicts a Poor Prognosis in Patients with Esophageal Squamous Cell Carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 7929–7934. [Google Scholar]
- Liu, D.; Gao, M.; Wu, K.; Zhu, D.; Yang, Y.; Zhao, S. LINC00152 Facilitates Tumorigenesis in Esophageal Squamous Cell Carcinoma via MiR-153-3p/FYN Axis. Biomed. Pharmacother. 2019, 112, 108654. [Google Scholar] [CrossRef]
- Sharma, U.; Barwal, T.S.; Khandelwal, A.; Rana, M.K.; Rana, A.P.S.; Singh, K.; Jain, A. Circulating Long Non-Coding RNAs LINC00324 and LOC100507053 as Potential Liquid Biopsy Markers for Esophageal Squamous Cell Carcinoma: A Pilot Study. Front. Oncol. 2022, 12, 397. [Google Scholar] [CrossRef]
- Zhang, X.; Feng, Y.; Gao, Y.; Hu, J. Long Noncoding RNA LINC00634 Functions as an Oncogene in Esophageal Squamous Cell Carcinoma Through the MiR-342-3p/Bcl2L1 Axis. Technol Cancer Res Treat 2020, 19, 1533033820928508. [Google Scholar] [CrossRef]
- Yang, X.-Z.; He, Q.-J.; Cheng, T.-T.; Chi, J.; Lei, Z.-Y.; Tang, Z.; Liao, Q.-X.; Zhang, H.; Zeng, L.-S.; Cui, S.-Z. Predictive Value of LINC01133 for Unfavorable Prognosis Was Impacted by Alcohol in Esophageal Squamous Cell Carcinoma. Cell. Physiol. Biochem. 2018, 48, 251–262. [Google Scholar] [CrossRef]
- Sun, K.; Zhao, X.; Wan, J.; Yang, L.; Chu, J.; Dong, S.; Yin, H.; Ming, L.; He, F. The Diagnostic Value of Long Non-Coding RNA MIR31HG and Its Role in Esophageal Squamous Cell Carcinoma. Life Sci. 2018, 202, 124–130. [Google Scholar] [CrossRef] [PubMed]
- Jiao, Z.; Yu, A.; Rong, W.; He, X.; Zen, K.; Shi, M.; Wang, T. Five-LncRNA Signature in Plasma Exosomes Serves as Diagnostic Biomarker for Esophageal Squamous Cell Carcinoma. Aging 2020, 12, 15002–15010. [Google Scholar] [CrossRef] [PubMed]
- Shi, W.; Wang, Q.; Bian, Y.; Fan, Y.; Zhou, Y.; Feng, T.; Li, Z.; Cao, X. Long Noncoding RNA PANDA Promotes Esophageal Squamous Carcinoma Cell Progress by Dissociating from NF-YA but Interact with SAFA. Pathol. Res. Pract. 2019, 215, 152604. [Google Scholar] [CrossRef] [PubMed]
- Shen, Z.; Wu, L.; Hao, W.; Li, Q.; Zhou, C. Expression of the Long Noncoding RNA RP11-169D4.1-001 in Hypopharyngeal Squamous Cell Carcinoma Tissue and Its Clinical Significance. J. Clin. Lab. Anal. 2020, 34, e23019. [Google Scholar] [CrossRef] [PubMed]
- Liang, M.; Pan, Z.; Yu, F.; Chen, C. Long Noncoding RNA SNHG12 Suppresses Esophageal Squamous Cell Carcinoma Progression through Competing Endogenous RNA Networks. Clin. Transl. Oncol. 2020, 22, 1786–1795. [Google Scholar] [CrossRef]
- Zhang, Y.; Li, R.; Ding, X.; Zhang, K.; Qin, W. Upregulation of Long Non-Coding RNA SNHG6 Promote Esophageal Squamous Cell Carcinoma Cell Malignancy and Its Diagnostic Value. Am. J. Transl. Res. 2019, 11, 1084. [Google Scholar]
- Wang, J.; Yang, X.; Li, R.; Zhang, R.; Hu, D.; Zhang, Y.; Gao, L. LncRNA SNHG6 Inhibits Apoptosis by Regulating EZH2 Expression via the Sponging of MiR-101-3p in Esophageal Squamous-Cell Carcinoma. Onco Targets 2020, 13, 11411–11420. [Google Scholar] [CrossRef]
- Qie, P.; Yin, Q.; Xun, X.; Song, Y.; Zhou, S.; Liu, H.; Feng, J.; Tian, Z. Long Non-Coding RNA SPRY4-IT1 as a Promising Indicator for Three Field Lymph-Node Dissection of Thoracic Esophageal Carcinoma. J. Cardiothorac. Surg. 2021, 16, 48. [Google Scholar] [CrossRef]
- Wang, Y.; Zhang, W.; Liu, W.; Huang, L.; Wang, Y.; Li, D.; Wang, G.; Zhao, Z.; Chi, X.; Xue, Y.; et al. Long Noncoding RNA VESTAR Regulates Lymphangiogenesis and Lymph Node Metastasis of Esophageal Squamous Cell Carcinoma by Enhancing VEGFC MRNA Stability. Cancer Res. 2021, 81, 3187–3199. [Google Scholar] [CrossRef]
- Huang, G.-W.; Xue, Y.-J.; Wu, Z.-Y.; Xu, X.-E.; Wu, J.-Y.; Cao, H.-H.; Zhu, Y.; He, J.-Z.; Li, C.-Q.; Li, E.-M.; et al. A Three-LncRNA Signature Predicts Overall Survival and Disease-Free Survival in Patients with Esophageal Squamous Cell Carcinoma. BMC Cancer 2018, 18, 147. [Google Scholar] [CrossRef] [Green Version]
- Xie, R.; Wu, S.-N.; Gao, C.-C.; Yang, X.-Z.; Wang, H.-G.; Zhang, J.-L.; Wei, Y.; Ma, T.-H. Prognostic Value of Combined and Individual Expression of MicroRNA-1290 and Its Target Gene Nuclear Factor I/X in Human Esophageal Squamous Cell Carcinoma. Cancer Biomark. 2017, 20, 325–331. [Google Scholar] [CrossRef] [PubMed]
- Zheng, S.; Zhang, X.; Wang, X.; Li, J. Downregulation of MiR-138 Predicts Poor Prognosis in Patients with Esophageal Squamous Cell Carcinoma. Cancer Biomark. 2017, 20, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Jin, W.; Luo, W.; Fang, W.; Wang, Y.; Wang, L.; Shen, Q.; Liu, W.; Zhang, H. MiR-145 Expression Level in Tissue Predicts Prognosis of Patients with Esophageal Squamous Cell Carcinoma. Pathol. Res. Pract. 2019, 215, 152401. [Google Scholar] [CrossRef] [PubMed]
- Gao, X.; Xie, Z.; Wang, Z.; Cheng, K.; Liang, K.; Song, Z. Overexpression of MiR-191 Predicts Poor Prognosis and Promotes Proliferation and Invasion in Esophageal Squamous Cell Carcinoma. Yonsei Med. J. 2017, 58, 1101–1110. [Google Scholar] [CrossRef]
- Liu, Z.; Huang, Y.; Han, Z.; Shen, Z.; Yu, S.; Wang, T.; Dong, Z.; Kang, M. Exosome-Mediated MiR-25/MiR-203 as a Potential Biomarker for Esophageal Squamous Cell Carcinoma: Improving Early Diagnosis and Revealing Malignancy. Transl. Cancer Res 2021, 10, 5174–5182. [Google Scholar] [CrossRef]
- Yang, H.; Wei, Y.-N.; Zhou, J.; Hao, T.-T.; Liu, X.-L. MiR-455-3p Acts as a Prognostic Marker and Inhibits the Proliferation and Invasion of Esophageal Squamous Cell Carcinoma by Targeting FAM83F. Eur. Rev. Med. Pharmacol. Sci. 2017, 21, 3200–3206. [Google Scholar]
- Liu, Z.H.; Chen, L.D.; He, Y.B.; Xu, B.; Wang, K.B.; Sun, G.X.; Zhang, Z.H. Study of Expression Levels and Clinical Significance of MiR-503 and MiR-375 in Patients with Esophageal Squamous Cell Carcinoma. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 3799–3805. [Google Scholar] [CrossRef]
- Guo, Y.; Wang, C.; Miao, X.; Chen, S.; Qian, Y.; Li, G.; Jiang, Y. Upregulation of Uc.189 in Patients with Esophageal Squamous Cell Carcinoma and Its Clinicopathologic Value. Pathol. Res. Pract. 2017, 213, 1400–1403. [Google Scholar] [CrossRef]
| ncRNA | GI Cancer Type | Expression | Drug(s) | Molecular Target(s) | Reference |
|---|---|---|---|---|---|
| lncRNA CRNDE | Colorectal cancer | Upregulated | 5FU | β-catenin and TCF4 | [24] |
| lncRNA PCAT6 | Colorectal cancer | Upregulated | 5FU | HMGA2 | [49] |
| lncRNA SNHG6 | Colorectal cancer | Upregulated | 5FU | ULK1 | [48] |
| miR-125b | Colorectal cancer | Downregulated | 5FU | APC | [47] |
| miR-26a-5p | Colorectal cancer | Downregulated | 5FU | ULK1 | [48] |
| miR-328 | Colorectal cancer | Upregulated | 5FU and HCPT | ABCG2 | [47] |
| miR-532-3p | Colorectal cancer | Upregulated | 5FU, cisplatin | ETS1 and TGM2 | [47] |
| lncRNA HOTAIR | Colorectal cancer | Upregulated | cisplatin | β-catenin, GRG5 | [23] |
| lncRNA CACS15 | Colorectal cancer | Upregulated | oxaliplatin | ABCC1 | [50] |
| lncRNA LINC00525 | Colorectal cancer | Upregulated | oxaliplatin | ELK3 | [51] |
| miR-128-3p | Colorectal cancer | Upregulated | oxaliplatin | Bmi and MRP5 | [47] |
| lncRNA GIHCG | Colorectal cancer | Upregulated | oxaliplatin and 5FU | unknown | [52] |
| lncRNA SCARNA2 | Colorectal cancer | Upregulated | oxaliplatin and 5FU | WGFR and BCL-2 | [53] |
| miR-451 | Colorectal cancer | Upregulated | SN38 | ABCB1 | [47] |
| miR-514b-3p | Colorectal cancer | Upregulated | cisplatin and irinotecan | FZD4, NTN1 | [47] |
| miR-514b-5p | Colorectal cancer | Downregulated | cisplatin and irinotecan | CDH1, CLDN1 | [47] |
| miR-138 | Esophageal cancer | Downregulated | 5FU and cisplatin | Survivin | [54] |
| lncRNA HOTAIR | Esophageal cancer | Upregulated | 5FU | MTHFR | [55] |
| miR-221 | Esophageal cancer | Downregulated | 5FU | DKK2 | [47] |
| miR-29c | Esophageal cancer | Downregulated | 5FU | FBXO3I | [56] |
| miR-338-5p | Esophageal cancer | Downregulated | 5FU | ID-1 | [57] |
| lncRNA CCAT1 | Esophageal cancer | Upregulated | cisplatin | PLK1 and BURB1 | [58] |
| lncRNA EMS | Esophageal cancer | Upregulated | cisplatin | WTAP | [59] |
| lncRNA LINC00337 | Esophageal cancer | Upregulated | cisplatin | TPX2 | [60] |
| lncRNA TUG1 | Esophageal cancer | Upregulated | cisplatin | NRF2 | [61] |
| miR-10b | Esophageal cancer | Downregulated | cisplatin | PPARɣ | [62] |
| lncRNA ROR | Gastric cancer | Upregulated | adriamycin and vincristine | MRP1 | [63] |
| lncRNA HCP5 | Gastric cancer | Upregulated | oxaliplatin and 5FU | AMPK, PGC1α, CEBPB | [64] |
| lncRNA ARHGAP5-AS1 | Gastric cancer | Upregulated | cisplatin, actinomycin, and 5FU | METTL3 | [65] |
| lncRNA SNHG16 | Hepatocarcinoma | Downregulated | 5FU | unknown | [66] |
| lncRNA CRNDE | Hepatocarcinoma | Upregulated | adriamycin | CELF2 and LATS2 | [46] |
| lncRNA GAS5 | Hepatocarcinoma | Upregulated | doxorubicin | PTEN | [67] |
| lncRNA HANR | Hepatocarcinoma | Upregulated | doxorubicin | GSKIP | [68] |
| lncRNA MALAT1 | Hepatocarcinoma | Upregulated | sorafenib | miR-140-5p | [69] |
| lncRNA H19 | Hepatocarcinoma | Downregulated | sorafenib or doxorubicin | ELAVL1 | [70] |
| miR-138-5p | Pancreatic cancer | Upregulated | 5FU | Vimentin | [47] |
| miR-27b | Pancreatic cancer | Upregulated | docetaxel | ZEB1 | [47] |
| miR-34a | Pancreatic cancer | Upregulated | docetaxel | ZEB1 | [47] |
| lncRNA SLC7A11-AS1 | Pancreatic cancer | Upregulated | gemcitabine | NRF2 | [71] |
| miR-1243 | Pancreatic cancer | Upregulated | gemcitabine | SMAD4 | [47] |
| miR-153 | Pancreatic cancer | Upregulated | gemcitabine | Snail | [47] |
| miR-30a | Pancreatic cancer | Upregulated | gemcitabine | Snail | [47] |
| miR-34 | Pancreatic cancer | Upregulated | gemcitabine | Slug | [47] |
| miR-509-5p | Pancreatic cancer | Upregulated | gemcitabine | Vimentin | [47] |
| lncRNA GAS5 | Pancreatic cancer | Upregulated | gemcitabine and 5FU | MST-1 | [72] |
| ncRNA | Expression | Clinical Significance | Molecular Target(s) | Reference |
|---|---|---|---|---|
| lncRNA TP73-AS1 | Upregulated | Biomarker | TGF-α | [90] |
| lncRNA SH3PXD2A-AS1 | Upregulated | Biomarker and therapeutic target | P57 and KLF2 | [91] |
| lncRNA RP1-85F18.6 | Upregulated | Diagnostic or prognostic biomarker | cell proliferation, cell cycle progression, and apoptosis | [92] |
| lncRNA DLEU7-AS1 | Upregulated | Prognostic biomarker | Wnt/β-Catenin signaling pathway | [93] |
| lncRNA BANCR | Upregulated | Prognostic biomarker | unknown | [94] |
| lncRNA HNF1A-AS1 | Upregulated | Prognostic biomarker | Wnt/β-Catenin signaling pathway | [95] |
| lncRNA LUADT1 | Upregulated | Prognostic biomarker | unknown | [96] |
| lncRNA PANDAR | Upregulated | Prognostic biomarker | unknown | [97] |
| lncRNA RP11-708H21.4 | Downregulated | Prognostic biomarker | AKT/MTOR pathway | [98] |
| lncRNA SBDSP1 | Upregulated | Prognostic biomarker | unknown | [99] |
| lncRNA SNHG6 | Upregulated | Prognostic biomarker | cell proliferation, cell cycle progression, and apoptosis | [100] |
| lncRNA ZEB1-AS1 | Upregulated | Prognostic biomarker | P15, ZEB1 | [101] |
| lncRNA-RP11-317J10.2 | Downregulated | Prognostic biomarker | Cyclin D1 | [102] |
| lncRNAs (RP1-170O19.17, RP11-785D18.3, RP11-798K3.2, XXbac-B476C20.9, RP11-481J13.1, and RP11-167H9.4) | Upregulated | Prognostic biomarkers | cGMP-PKG signaling pathway and cAMP signaling pathway | [103] |
| lncRNA AB073614 | Upregulated | Prognostic marker and therapeutic target | PI3K/AKT signaling pathway | [104] |
| lncRNA LINC00858 | Upregulated | Prognostic marker and therapeutic target | miR-22-3p | [105] |
| lncRNA SNHG6 | Upregulated | Prognostic marker and therapeutic target | Upf1 and ZEB1 | [106] |
| lncRNA CA3-AS1 | Upregulated | Therapeutic target | miRNA-93/PTEN Axis | [107] |
| lncRNA Linc00659 | Upregulated | Therapeutic target | PI3K/AKT signaling pathway | [108] |
| lncRNA-HOTAIR | Upregulated | Therapeutic target | P21 | [109] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kulkarni, A.; Gayathrinathan, S.; Nair, S.; Basu, A.; Al-Hilal, T.A.; Roy, S. Regulatory Roles of Noncoding RNAs in the Progression of Gastrointestinal Cancers and Health Disparities. Cells 2022, 11, 2448. https://doi.org/10.3390/cells11152448
Kulkarni A, Gayathrinathan S, Nair S, Basu A, Al-Hilal TA, Roy S. Regulatory Roles of Noncoding RNAs in the Progression of Gastrointestinal Cancers and Health Disparities. Cells. 2022; 11(15):2448. https://doi.org/10.3390/cells11152448
Chicago/Turabian StyleKulkarni, Aditi, Sharan Gayathrinathan, Soumya Nair, Anamika Basu, Taslim A. Al-Hilal, and Sourav Roy. 2022. "Regulatory Roles of Noncoding RNAs in the Progression of Gastrointestinal Cancers and Health Disparities" Cells 11, no. 15: 2448. https://doi.org/10.3390/cells11152448
APA StyleKulkarni, A., Gayathrinathan, S., Nair, S., Basu, A., Al-Hilal, T. A., & Roy, S. (2022). Regulatory Roles of Noncoding RNAs in the Progression of Gastrointestinal Cancers and Health Disparities. Cells, 11(15), 2448. https://doi.org/10.3390/cells11152448






