New Strategies in the Development of Antimicrobial Coatings: The Example of Increasing Usage of Silver and Silver Nanoparticles
Abstract
: Bacterial infection from medical devices is a major problem and accounts for an increasing number of deaths as well as high medical costs. Many different strategies have been developed to decrease the incidence of medical device related infection. One way to prevent infection is by modifying the surface of the devices in such a way that no bacterial adhesion can occur. This requires modification of the complete surface with, mostly, hydrophilic polymeric surface coatings. These materials are designed to be non-fouling, meaning that protein adsorption and subsequent microbial adhesion are minimized. Incorporation of antimicrobial agents in the bulk material or as a surface coating has been considered a viable alternative for systemic application of antibiotics. However, the manifestation of more and more multi-drug resistant bacterial strains restrains the use of antibiotics in a preventive strategy. The application of silver nanoparticles on the surface of medical devices has been used to prevent bacterial adhesion and subsequent biofilm formation. The nanoparticles are either deposited directly on the device surface, or applied in a polymeric surface coating. The silver is slowly released from the surface, thereby killing the bacteria present near the surface. In the last decade there has been a surplus of studies applying the concept of silver nanoparticles as an antimicrobial agent on a range of different medical devices. The main problem however is that the exact antimicrobial mechanism of silver remains unclear. Additionally, the antimicrobial efficacy of silver on medical devices varies to a great extent. Here we will review existing antimicrobial coating strategies and discuss the use of silver or silver nanoparticles on surfaces that are designed to prevent medical device related infections.1. Introduction
It is acknowledged that medical device related infections account for a substantial morbidity as well as causing a sharp increase in health-care costs [1-4]. Especially, implanted synthetic medical devices demonstrate a significant number of infections. Although the rate of infection is relatively low, the sheer volume of medical devices accounts for a large number of infections. For instance, for orthopedic implants it has been reported that from the approximately 800,000 annually implanted devices in Europe, at least 1.5%, i.e., 12,000, peri-prosthetic infections, will occur [1]. When one also includes the steadily increasing number of revision operations that are associated with a much higher infection rate, a much higher real infection rate has to be considered. The infection will not only result in prolonged hospitalization and associated increased health care costs, but also in higher morbidity [1,4-6].
Infections do not only occur upon the implantation of a medical device, but also during “regular” interventions. However, implantation of a foreign body is associated with higher infection rates. For mastectomy, the removal of one or two breasts caused by breast cancer, the surgical site infection (SSI) was reported to be 2% overall by the Center for Disease Control [7]. However in individual reports the SSI rate varies between 1% and 28%. In a small study, an increase in SSI was observed for mastectomy with immediate placement of a breast implant (12.4%) when compared to more conventional mastectomy interventions (4.4% to 6.2%) [7]. It shows that SSI can vary considerably from study to study and that implantation of a synthetic device is associated with a higher rate of infection.
Another device that has been associated with a high number of bloodstream infections is the central venous catheter [8-10]. It is estimated that in the United States alone at least 80,000 catheter related bloodstream infections (CRBSI) occur annually in intensive care units. These CRBSIs are associated with 24,000 patient deaths and increased health care costs ranging from approximately $10,000 to $63,000 per case. Additionally, the mean hospital stay is prolonged by 12 days, putting a heavy burden on the health care system as well as on patients and their families [11,12].
Because the health insurance companies have enlisted medical device related infections as preventable, Medicare and Medicaid may no longer reimburse the costs associated with these infections in the U.S. in the near future [12,13]. At this moment there are no indications that a similar policy will be introduced in Europe, but it shows the need to combat medical device related infections. It also means that the complete responsibility for combating these infections is put on the hospitals. Much can be gained by education of the medical staff and also the patients, but the safety and efficiency of the medical devices will have to be improved to drastically decrease infection rate of synthetic implants and medical devices that contact human tissue and/or body fluids [12,14-16].
In this review we describe the main strategies that have been employed to prevent medical device related infection. In recent years the use of noble metals, in particular silver, has increased due to the evolution of antibiotic resistant bacteria. The use of silver in, and on, medical devices will be discussed as well as their clinical outcome. Finally an attempt will be made to describe a possible mode of action of silver as an antibiotic agent using the limited data available on this subject.
2. Infection and Biofilm Formation
Infection of medical implants and devices can be traced back to different sources of the infectious agent, such as: (i) a contaminated implant/device surface; (ii) the hands of the surgical staff during implantation/application; (iii) the patient's own skin or mucus membrane; (iv) distant local infections in the patient; (v) contaminated disinfectants; (vi) contact with other patients in the hospital, or family members after intervention [17,18]. Many of these risk factors can be easily avoided by stricter hygiene procedures in the hospitals. However, infections can never be completely avoided and therefore strategies to purposely avoid infection by either inhibiting adhesion of the pathogens or by killing adhesive microorganisms have to be pursued.
In order to design optimal strategies for the battle against medical device related infections, a good understanding of this bacterial infection is of critical importance. The microbial infection of foreign surfaces often progresses in a specific, defined order. The medical implant is delivered in an air-tight package completely clean and sterilized. Faulty sterilization procedures can lead to infection, but in practice this is rare because of the tight control mechanisms in place within the medical device industry [19].
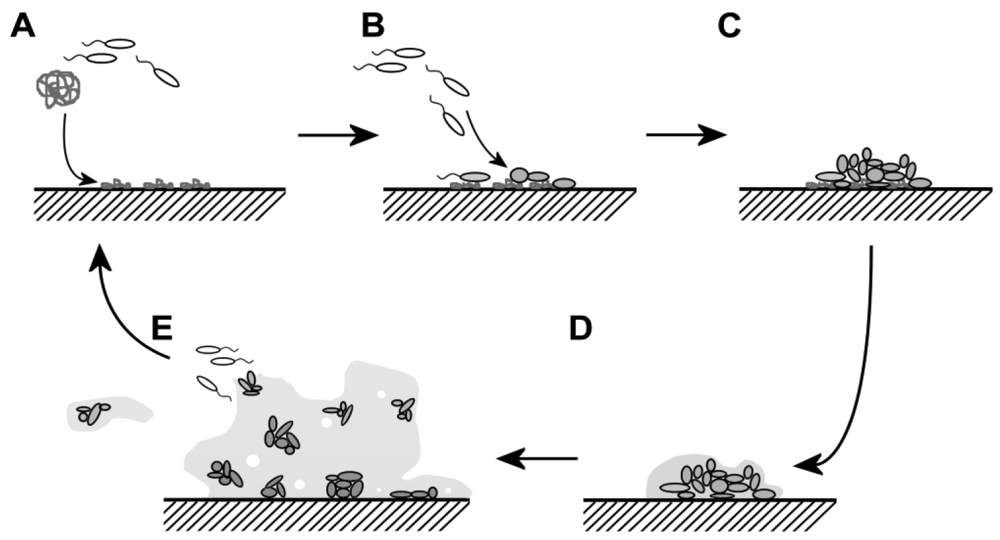
Upon implantation of the device, proteins from the blood or tissue directly adsorb onto the surface (Figure 1). This process of protein adsorption has been described extensively in the literature, and there are many parameters that will determine which proteins will eventually end up on the implant surface. Among others, protein adsorption is influenced by surface hydrophobicity, roughness, porosity, chemical composition, as well as composition and concentration of the protein solution, salt concentrations, pH, etcetera [20-23]. Although many studies have been performed on this interface phenomenon, a prediction of what proteins will adsorb to a synthetic surface has proven difficult if not impossible [23,24]. This layer of adsorbed proteins has been shown to be important for the adhesion of bacteria. Actually one could stipulate that the bacteria rarely encounter the “clean” surface of an implant. The free swimming bacteria, in the so-called planktonic state, will in vivo adsorb to these surface adsorbed proteins (Figure 1) [25,26]. The adhered bacteria will increase in numbers by proliferation and recruitment of other bacteria from the immediate environment. Once a good number of bacteria have formed a colony on the surface, these will change their gene expression pattern. Genes will be activated and expressed that are responsible for the production of extracellular polymeric substances, which are essential in the formation of biofilm [26,27]. This biofilm is a protective sheet around the sessile bacteria that will protect them from shear stress, attack by the host's immune system and (bad for the patient) against antibiotic substances. The morphology of the biofilm has been extensively studied and it turns out that this slime layer is mainly composed of extracellular polymeric substances (EPS). This EPS matrix can have varying composition and consists mainly of polysaccharides [25,28]. However, also non-cellular materials from the direct environment can be included like corrosion particles, wear debris particles, blood components, mineral crystals, etc. The biofilm also is highly hydrated and contains up to 95% water. Additionally, the layer is not solid, but has a more porous morphology with holes and tunnels [28,29]. The encasing of bacteria in the biofilm also has consequences for the bacteria. The biofilm matrix hampers proper transport of oxygen and nutrients to the bacteria. The emergence of anaerobic conditions in the biofilm leads to altered gene expression and metabolism in the bacteria. These new metabolic conditions also decrease sensitivity of bacteria to a number of antibiotics, which have been designed to interfere with the bacteria's metabolism.
Knowing the important steps in surface invasion and biofilm formation, the number of possible strategies to avoid these phenomena is limited. The post-biofilm formation treatment of the infection is very difficult because of the slimy nature of the biofilm. The systemically administered antibiotics will not penetrate and therefore the bacteria will not be killed [26]. The application of biofilm disturbing agents in combination with antibiotics seems a more efficient strategy, but in practice this has not been applied frequently because of the aggressive nature of the chemicals involved [26]. Therefore the modification of implant surfaces may be a more efficient strategy to combat the infection of biomedical implants. The inhibition of initial bacterial colonization of the surface is a prime subject of biomaterial science. This will avoid most implant related infections and diminish the chance of biofilm formation. This is also important so that the immune system of the patient has the possibility to reach the infectious agents and remove these from the implant surface and the surrounding tissues.
3. Anti-Microbial Coatings
3.1. Surface Modification to Prevent Microbial Population and Biofilm Formation
Biofilm formation on surfaces of medical implants is very difficult to prevent. There are many different reasons for implant-related infections of which hygienic handling, the nature of the implant, and proper application, are only a few. Hence, one has to realize that modification of the implant to create a surface that prevents microbial colonization and effectively kills microbes is only one part of the solution. In addition to material properties, breeches in aseptic technique and non-respecting infection control procedures are the most important risk factors for implant infections. In this review however we will focus on the possible surface modifications that will make implants less susceptible for infections.
It is clear that the topological and chemical characteristics of a medical device surface are important for the rate of microorganism adhesion. A perfectly smooth surface will be less likely to be populated than a rough surface, where more surface area is available as well as more adhesive force can be generated by the microorganism per surface area. Also the chemical characteristic is essential for the initial population of a surface by free-swimming pathogens. Hydrophilic surfaces have been shown to be less quickly populated by free-swimming bacteria than hydrophobic surfaces [25,30-33]. Although most microorganisms have a charged outer surface, they also contain hydrophobic patches and these may be involved in the adhesion to the hydrophobic surface of a medical implant. In reality however, the adhesion of microorganisms is almost always dependent on formation of a protein layer on the surface, possibly exposing high-affinity adhesion sites [25,26]. The proteins are present in the tissues of the patient and adsorb very rapidly upon implantation. Especially with blood contacting the surface, proteins like albumin, fibrinogen and fibronectin promptly adsorb onto the surface. This means that when designing an anti-microbial surface, the adhesion of proteins to that surface is an important parameter that has to be taken into account.
In this review we will discuss four different strategies to prevent and combat the adhesion and proliferation of microorganisms on a biomaterial surface. These include (i) the chemical modification of the surface with protein and bacteria-repellent coatings; (ii) surfaces with quaternary ammonium; (iii) the incorporation and release of antibiotics from the surface; and (iv) the use of noble metals and especially silver on the surface as anti-microbial coatings. These strategies will be discussed in this review and there will be a special focus on the use of silver as an antimicrobial agent in surface coatings of medical devices and implants.
3.2. Protein- and Microorganism-Repellent Coatings
The most common strategies for protein- or microbial-repellent coatings are polymer layers and brushes on surfaces. There are many different ways in which these polymers can be attached to the surface. Also the sort of polymers used can differ from linear to branched, like star-shaped, and from homo-polymers to block-copolymers [34-37]. These polymers all have in common that they are in most cases hydrophilic. The polymers are often kept on the surface by non-covalent tight interactions. A common technique is the tight interaction of sulfur atoms with a gold surface. Small linker molecules with thiol groups can be used to exploit this interaction. The desired polymers can be attached via the linking thiol-containing molecule to the gold surface, e.g., by grafting to an acrylate or methacrylate function in the linker [38,39]. Alternatively a polymer with a thiol end-group can be directly adsorbed onto the surface. A variation of this strategy was demonstrated by Hubbell and coworkers in which a block copolymer, poly(ethyleneglycol)-bl-poly(propylene sulphide)-bl-poly(ethyleneglycol), was shown to tightly and stably adsorb onto gold surfaces [40]. The advantage of this sulfur to gold strategy, is that the polymers will form a self-assembled monolayer on the surface. The method is easy to perform, however there are several disadvantages. The chemical stability is often relatively poor and the control over the quality of the monolayer is absent. Often imperfections appear and these are difficult to control [38,39]. Also there is a need to modify other surfaces than gold with polymer brushes. Recently Khoo and coworkers demonstrated the synthesis of a polymer brush on titanium via a peptide linked to PEG. The peptides contained several HKH motifs that show specific binding with high affinity to titanium surfaces. The resulting surfaces showed reduced protein and bacterial adhesion [41].
Polymeric surfaces are mostly modified with such brush layers via direct covalent coupling to reactive groups on the surface. These reactive groups can be designed into the original surface or generated by for instance plasma treatment of the surface. Glow discharge in the presence of amines can be used to introduce amine groups on PTFE surfaces [34]. These can then be used to link pre-synthesized polymers with carboxyl groups. Reactive surface exposed groups can also be used as an initiation site for polymerization in situ. An initiator is then first attached to the surface and used to graft polymers from this point of attachment [34].
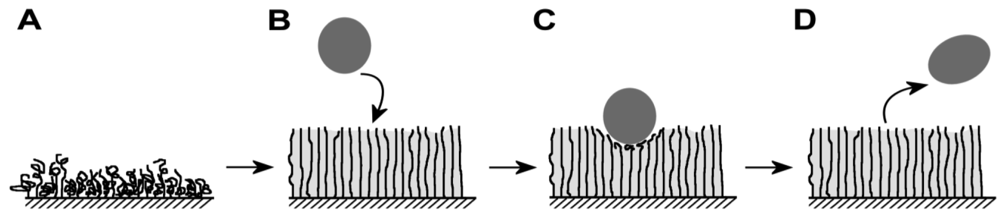
Since the polymers are applied to the surface in a high density, they are often called polymer brushes (Figure 2). The higher the surface density of the polymer chains on the surface, the better the anti-adhesive characteristics will be. Also the chain length of the polymers is of importance; longer chains are more effective in prevention of bacterial adhesion [42-44]. Because most of the polymers used for brushes are hydrophilic, water will be attracted into the brush layer and form a repellent layer close to the surface. The water is held in place via hydrogen bonding to the polymers. Consequently, there is steric hindrance for proteins or microorganisms to adsorb to the surface. The result is a reduction of protein adsorption by several orders of magnitude (Figure 2). Further details on the chemical synthesis and characterization of polymer brushes are not the focus of this review.
3.3. Surface Quaternary Ammonium Compounds
The presence of positive charge on a surface has been shown to have a negative effect on cell survival in general. Thus a number of anti-microbial surfaces and coatings have been developed that exploit the presence of quaternary ammonium (QA; Figure 3). In general quaternary ammonium compounds (QACs) are known and widely used as antimicrobial compounds [45,46]. These soluble QACs are employed in industrial applications, water treatment, in pharmaceutical and every day consumer products. These QACs are often employed as preserving agents in cosmetic products. QA also displays antimicrobial activity when exposed on a solid surface [47-50]. The QAs have a wide range of antimicrobial activity: vegetative bacteria, yeast, viruses, algae, and fungi. These compounds are however ineffective versus bacterial spores, mycobacteria and hydrophilic viruses [51-53]. The main antimicrobial activity of QAs is associated with their cationic, surfactant (in case of QACs), characteristics. The membranes of the contacting microbes will become distorted, leaky and consequently the microbe will die.
The use of quaternary ammonium has been popular since it is easy to manufacture in large quantities and modify large surface areas. Also the QAs and QACs have been found to be very stable, especially in the human body. These compounds are poorly metabolized and will be mainly excreted in non-metabolized form. The disadvantage of the quaternary ammonium surface coatings is that they are not cyto- and bio-compatible [53].
These surface coatings are more suited for use in contact with the skin or for materials that are being used in the hospital, like textiles, floors and ceilings in the operating theater, etc. Cells contacting a QA containing surface will show reduced cell viability and be killed. Another concern is the evolution of antimicrobial resistance to QA. The composition of the membrane may be altered after prolonged exposure to QACs, and thus the efficiency of the compound may decrease. Also altered gene expression has been linked to antimicrobial resistance concerning QA [53,54]. Hence the use of surfaces with QA for in vivo use is still limited although recently a number of different surfaces have been synthesized that carry various QA, and were shown to contain varying anti-microbial and cytotoxic effects. Future research will determine whether surfaces with QA can play a role as antimicrobial surface coatings for medical implants.
3.4. Antibiotic Releasing Coatings
Since the discovery of penicillin by Fleming in 1928 [55], the systemic application of a wide variety of antibiotics has been the treatment of choice for bacterial infections, also those associated with implanted medical devices. However it has been shown that a systemic approach to treatment of implant related infections is not optimal. Antibiotics have difficulty to penetrate the biofilm and reach the bacteria [26]. As a possible consequence to this, only subinhibitory concentrations of the antibiotic may be present in the biofilm and consequently lead to the development of resistance to the antibiotics used. In addition to this, altered metabolism of the bacteria in the biofilm diminishes the efficacy of many antibiotics. Hence, local application of antibiotics on the implant surface may be more efficient because the bacteria are killed locally directly upon binding, before the biofilm can be formed. Local delivery of antibiotics has been long applied in bone cements that are used to fix orthopedic and orthodontic implants [56,57]. Infection of the surface of the implant is a severe complication that may in the worst-case lead to implant failure and removal of the implant. For this, an antibiotic like gentamycin is mixed into the cement and subsequently slowly released after hardening in situ. The local delivery can prevent adhesion and growth of significant numbers of bacteria.
A similar strategy is based on the application of biodegradable surface coatings that contain antibiotics [58,59]. The surface layer would slowly degrade and cause antibiotic release directly at the surface-tissue interface. The kinetics of antibiotic release closely follows the degradation kinetics of the coating. Most examples of such antibiotic releasing coatings have been tested for orthopedic applications. For instance the application of poly(D,L-lactide) (PDLLA) containing gentamycin on the surface of orthopedic implants drastically decreased the infection rate and a better recovery after infection was observed when compared to systemic gentamycin treatment. The use of mixtures of antibiotics, like rifampicin and fusidic acid in PLLA coatings by Kalicke and coworkers, resulted in effective killing of Staphylococcus aureus infection in a rabbit tibia infection model [60]. Antibiotics have been incorporated in a variety of surface coatings like PVP, polyurethane, polyphosphoester (Politerefate), calcium phosphate (HA). A study by Harris et al. demonstrated that only when sufficiently fast release rates of chlorohexidine were obtained the coatings were effective in preventing and combating infection. The calcium phosphate and PVP coatings failed to release sufficiently high enough concentrations of antibiotics and therefore failed in preventing infection [61].
Hydroxyapatite (HA) coatings are frequently applied to orthopedic implants to stimulate osseointegration and accelerate bone formation. A variety of antibiotics was co-precipitated on titanium surfaces, resulting in drug-releasing surface coatings. It was found that the antibiotics that have the best calcium chelating properties showed the most optimal release kinetics and thus the best and longest lasting antimicrobial properties. The antibiotics that did not bind well to calcium, were washed rapidly out of the coating and the antimicrobial activity on the surface was quickly lost [62-64].
The direct coating of antibiotics, without a carrying coating, on implants has been shown in a study by Darouiche et al., to be a viable strategy. The antibiotics were dissolved in an organic solvent and after evaporation pure antibiotic was left on the implant surface. The coated implants showed promising antimicrobial activity, but the effect on the integration of the implant in the host tissue was not yet reported. High local concentrations of these antibiotics could be damaging to cells [65].
Antimicrobial coatings have also been applied to venous catheters. Coatings containing combinations of antibiotics and antiseptics like minocycline and rifampin or chlorohexidin and silver-sulfadiazine have been applied to the internal and external surface of catheters. In several studies these antimicrobial coated catheters were compared to non-coated catheters, and a reduction of catheter colonization and catheter related blood-stream infections were found [66-68]. The antimicrobial effect of antibiotics containing coatings was more pronounced than for the antiseptic coatings. Halton and Graves analyzed studies concerning economic aspects of catheter related bloodstream infections and concluded that the use of antibiotic coated catheters was clinically effective and cost-saving when compared to antiseptic-coated or standard catheters [11,69].
One of the disadvantages of local release of antibiotics is that the release is finite in case of permanent implants. For short-term implants, like the above mentioned catheters, this is not a major problem since the implant is removed before the antibiotic is fully released. However, for long-term use of catheters or for permanent implants, the concentration of the released antibiotic will eventually drop below the minimal inhibitory concentration [70]. The antibiotic cannot be replenished and thus the surface is now susceptible to infection by bacteria from distant sites. Alternatively, infection can be caused by bacteria that remained viable in close proximity of the implant, possibly even inside cells of the patient's immune system [71,72]. In the case of catheters, antibiotic lock solutions are applied to prevent or treat catheter-associated bloodstream infections. Another complication is that use of high doses of antibiotics leads to the generation of resistance in the bacteria. A large number of resistant bacterial strains have been described in clinical practice and simple general range antibiotics often fail to prevent infection by these multi-drug-resistant bacteria stains. The use of antibiotics for prevention of infection has thus become more controversial and may not be the best solution to surface associated infections [73,74].
4. Silver as Antimicrobial Additive to Coatings
4.1. Silver as Antimicrobial Agent
The application of silver as a preserving and antimicrobial agent goes back to 4000 BC. Silver vessels were used to transport water during military campaigns, and also silver salts were used to preserve water and food. A similar method was employed by the early pioneers traveling over long distances across the North American continent. They would drop a silver coin in their water or milk as a preservation method [75,76]. From a medical point of view, silver also has a long history of use. The ancient Egyptians, Greeks and Romans used metal salts (zinc, copper, silver, mercury) to clean wounds and silver threads were used as sutures. The use of silver and silver salts to clean wounds and promote healing remained even into the 20th century. Silver was (and still is) used in wound dressings and successfully applied on open infected wounds, skin ulcers, compound fractures, and burn injuries [77,78]. The closure of wounds and fistulas using silver sutures was shown to be very successful in preventing infections. Also solutions of silver nitrate were used to prevent infections, for instance in eye drops to combat eye infections. In the late 19th century the first use of colloidal silver was reported for wound antisepsis. The use of silver solutions (mostly silver nitrate) became a wide-spread therapy until the discovery and introduction of antibiotics in the 20th century [75].
The exact mechanism by which silver exerts its antimicrobial activity still remains unclear today and a possible explanation will be discussed later in this review. Silver can be applied in different forms, namely as the metal, as a compound or as the free dissolved ion. The ancient users of silver had no idea what form of silver worked best, but they just observed the positive effects of silver and silver salts. They also realized that silver worked best when some moisture was present [76]. It was only relatively recently discovered that the silver ion (Ag+) was responsible for the antimicrobial activity of silver [79]. After the introduction of antibiotics like penicillin in the 1940s, the use of silver declined. In the 1960s however, silver nitrate solutions were reintroduced to treat burns, and this treatment was improved by the introduction of silver sulfadiazine cream. This compound did decrease infection rate but was found to delay healing, so is no longer recommended [80].
The introduction of silver nanoparticles has a profound impact on silver use [81]. There is circumstantial evidence that these particles have good antimicrobial activity. The exact way in which silver nanoparticles exert anti-microbial activity is still speculative. What is clear is that proper use and application of this form of silver can reduce microbial infection. However there is some doubt on the safety on such particles. Due to the small size in combination with varying properties it has been suggested that these small particles might show nano-toxicity. In vitro studies have indeed demonstrated that high concentrations of silver nanoparticles have damaging effects on cells that can lead to cell death. It remains to be determined if silver nanoparticles will be safe in patients in the long run. In the mean time, silver nanoparticles remain a hot item and these are incorporated in a number of products ranging from device coatings and wound dressings to commercially available deodorants and cosmetics [81,82].
4.2. Silver Nanoparticles: an Alternative for Metallic Silver and Silver-Salts?
The evolution of bacteria strains, resistant against multiple antibiotics, prompted scientists and medical experts to look for antimicrobial alternatives [80]. Thus silver resurfaced, since it is considered to be a broad-spectrum antimicrobial agent. Especially the use of silver nanoparticles was explored as a constituent of coatings on medical devices and implants. The use of such small particles was investigated because of the disappointing results of metallic silver in contact with blood or tissues. The metallic silver did not show enough antimicrobial activity and also deteriorated fast [77,81]. Metallic silver in a moist environment will react and results in the formation and release of silver ions. These ions are highly potent as antimicrobial agent. It was already known that ionic silver is the most potent antimicrobial form of silver, but it is difficult to use in combination with medical devices [81,83]. The mixing of silver salts into surface coatings does not result in efficient antimicrobial activity because of the poor solubility of most silver salts.
In the meantime, Furno and coworkers had demonstrated the potential of silver nanoparticles as antimicrobial agent [84]. They showed that silicon discs impregnated with silver nanoparticles efficiently prevented bacterial adhesion and growth, although the particles were washed out of the elastomer. This meant that silver nanoparticles showed promise as antimicrobial agent, but that keeping this effect up for longer times is dependent on the way the silver particles are fixed to the surface layer. One problem of silver nanoparticles is their biosafety. For the moment the biocompatibility of silver containing coatings in vivo is not clear. There have been several reports showing that silver nanoparticles are not specific in killing (or damaging) cells [85]. Apparently some of the mechanism by which cells are killed by Ag-nanoparticles is not specific for bacteria and fungi, but conserved among many organisms. As a result, the patients' tissues are at risk when exposed to high concentrations of Ag-nanoparticles. The tight incorporation of silver nanoparticles in coatings could circumvent part of this toxicity problem by avoiding extensive release of free nanoparticles. Essentially the Ag nanoparticles are then used as a reservoir of silver ions, being released from the coating. Efficiency and longevity of the antimicrobial surface are increased, because the nanoparticles are not flushed away. Additionally, the silver is needed close to the surface, since bacterial adhesion and proliferation are observed there. The highest concentration of silver ions can be expected close to the surface, i.e., the place they are needed. How exactly the surface bound nanoparticles would exert antimicrobial activity is still unclear. What is clear is that the large surface-to-volume ratio is important for antimicrobial efficiency [85].
4.3. Medical Coatings Containing Silver or Silver Nanoparticles
Nano-silver coatings have been applied to several medical devices of which catheters, drains, and wound dressings are the most prominent. These are studied in clinical experiments in order to demonstrate if the addition of silver nanoparticles to the coating of the device reduces colonization, infection rate, hospitalization days, wound healing, and shows economical benefit. The efficacy of silver to improve clinical outcome is dependent on the application and device. Additionally, for some applications, the number of well controlled, randomized and double-blind trials is limited. Hence a definite answer concerning the positive effects of silver impregnation or silver coatings is difficult because of the lack of proper statistics.
Wound dressings used for treatment of burns and non-healing wounds can be impregnated with silver sulfadiazine crème or with other silver compounds or salts [86,87]. The wound dressings are applied to the wounds and compared to non-silver dressings. The outcome concerning wound healing or reduction in wound area and depth, infection, odor, wound exudates, pain, and quality of life [88-91]. Some of these criteria are subjective (arbitrary scale) and it is hard to imagine how these measurements can be used to analyze the efficiency of silver dressings. The final data on silver containing dressings are variable, because in the different studies different silver products are investigated. Verdu-Soriano et al., for instance, using a silver-charcoal dressing, did not show significant advantages when compared to the control dressing [92]. The rate of wound infection was not found to be significantly reduced. Silver hydroalginate and hydrophilic silver foam dressing had clear significant effects on wound area reduction and wound healing, also wound infection was reduced when using these silver dressings in a number of studies [87]. In a study by Miller and coworkers, the effect of nano-crystalline silver on the healing of leg-ulcers was studied. The silver-dressing did not increase the overall healing rate, but was associated with quicker healing in the larger and older ulcers [93]. An extensive meta study from Storm-Versloot confirmed these findings in that most studies on silver dressings for non-healing wounds did not show significant reduction of infection when using silver sulfadiazine cream or silver dressings. Wound healing was found to be varied in the different studies, depending on the type of wounds included in the study and exact dressing used [87].
For burns, the results are also varied; some studies showed that topical silver reduced infection while in others a higher rate of infection was detected for the silver containing treatment. The rate of healing was also not significantly increased in all studies for the silver dependent treatment. Interestingly, in a recent analysis Gravante and colleagues showed that nano-silver showed improved prevention of burn wound infections when compared to other silver formulations (silver-sulfadiazine and silver nitrate) [91]. They also described faster healing of deep burns was associated with the use of nanocrystalline silver impregnated dressings [94]. This means that the full potential of silver antimicrobial activity is not being used, and that new dressings using nano-silver particles may improve the efficiency of wound dressings even further in the near future.
External ventricular drains (EVD) are frequently used in neurosurgery to treat acute hydrocephalus. A common complication is colonization of the EVC and subsequent infection resulting in ventriculomeningitis. Therefore anti-microbial coating strategies can be of vital importance for the treatment of these patients. In recent years, some drains with coatings containing silver nano-particles have been tested in patients. In a study by Fichtner and coworkers, the colonization of the drains was reduced by a factor of four, and the infection of the central-spinal fluid by a factor of two [95]. In a small scale analysis performed by Lackner, non-coated EVDs (20 patients) were compared to nanosilver impregnated drains (20 patients). The control groups showed five cases of infection leading to ventriculitis. The group of patients treated with the silver-nanoparticle coated drains had no occurrence of infection [96]. Although the sample size in both cases was small, the positive effects of the silver nanoparticle coatings were clear and significant. These two studies showed the feasibility of silver nano-coatings. The results now need to be confirmed in larger, well-controlled studies.
In the case of catheters, no comprehensive studies in patients on the effects of silver-nanoparticle impregnated coatings on colonization and infection-rate of these devices are available. The reports that have been published compare silver-coatings with their control counterparts. There are studies that show the feasibility of nanosilver coatings on catheter-materials like poly(urethane), but these have only been studied in detail in animal experiments [97,98]. The application of silver-nanoparticle coated venous catheters in patients remains to be reported. In animal studies however, the efficacy of silver nanoparticles in reducing or preventing biofilm formation was demonstrated [97].
For venous catheters, the rate of infection varies in different publications because different parameters are applied: surface colonization can go up to 80%, while the resulting catheter related bloodstream infections (CBSI) have a frequency which is much lower (average of 3–5%) [70,99]. Because these devices are used in large numbers, the total number of catheter related infections is a major economical factor (vide supra) [1,8-10]. Infection is often caused by poor hygiene or wrong application of the catheter. One should not forget that significant improvement can be gained from proper training of medical personnel using and placing catheters [5,12]. Especially catheters that remain in the patient for prolonged times are susceptible to infection. The central venous catheters are an example of such long-term catheters. These are used for easy access to the bloodstream of the patient to apply drugs or collect blood samples. Failure of this device is very often caused by the formation of a biofilm or of thrombus on the surface. The catheter will adsorb proteins upon contact with the blood, and this may be a breeding ground for bacteria and microbes. The strategies to prevent catheter failure have focused on development of surface coatings that prevent thrombus formation or infection [100]. It is very difficult to imagine that a surface which only prevents one complication can be effective in preventing failure. The formation of a thrombus can stimulate infection and vice versa. But it has proven very hard to combine both antithrombotic and antimicrobial characteristics in one coating. Again there are a number of studies in which the silver coated catheters are compared to their antibiotic-loaded or non-coated counterparts. However, there are many studies that confirm the antibiotic effect of catheter silver coatings, which reduce surface colonization and CBSI [100-102]. However some studies report the reduction of surface colonization without a direct significant effect on CBSI [103]. In addition to this, in a recent study, Kalfon and coworkers analyzed 617 catheters from 577 patients in a multicenter prospective randomized controlled clinical study. Although they found a reduction in colonization (14.7 vs. 12.1%) and a reduced incidence (11.2 vs. 9.4 per 1,000 catheter days), this reduction of surface colonization was not significant and the clinically more important CBSI was not reduced in this study [104]. There are more studies that dampen the initial enthusiasm about silver-impregnated central venous catheters. These data show that there is a need for large-scale well designed randomized trials.
For urinary catheters the situation is somewhat different, in that it has become clear that silver coated catheters do have a beneficial clinical outcome. The rate of catheter-associated urinary tract infections is significantly lower in almost all studies, although the specific characteristics of the study determined the risk reduction which varies between 2 and 32% [105,106]. Recent studies by Seymour in the United Kingdom have shown that silver-coated catheters have a clear effect in reducing urinary tract infection (UTI) by up to 20% [107]. Also Parker and coworkers produced an evidence based report that supports the conclusion that silver alloy-coated catheters reduce the risk of UTI significantly [108]. Overall there seems to be a consensus that silver-coated urinary catheters are beneficial and will eventually lower the burden on the health systems.
In the end, the inclusion of silver nanoparticles, metallic silver, silver salts, or silver sulfadiazine in the coatings of catheters all aim at releasing silver ions close to the surface. These ions can then reduce or even prevent colonization and subsequent biofilm formation on the surface. In this way the number of catheter associated infections can be reduced. The use of nanosilver may improve this strategy since the release of silver ions from these nanoparticles can be precisely controlled [109,110]. Therefore in the next few years, more and more studies will emerge in which the efficacy of silver nanoparticles in the coatings of medical devices will be studied in patients. It has already been shown that the use of nanosilver in the coating of drains and for wound dressings has, in general, a beneficial effect. The rate of infection of the silver-modified surfaces and dressings is reduced. However, the initial hooray concerning silver coatings has to be restrained until solid, well-designed clinical trials show the real benefits of the use of silver and in particular silver nanoparticles in medical devices. Care should be taken in defining proper endpoints which may include bloodstream infection, urinary tract infection, ventriculomeningitis, morbidity, hospitalization time, economic costs. Improved methodology to detect real catheter related infections may have to be designed to get an objective measure of the beneficial effect of silver coatings [106,111].
5. Mechanism of Antibacterial Action of Silver
It is absolutely unclear how silver actually kills bacteria. In a number of studies on this topic, several possibilities and theories have been proposed. Here, different studies into the mechanism of the antimicrobial activity of nano-silver will be discussed. When these fragments of evidence are combined, more light is shed on the mode of action of silver nanoparticles.
Over the past decades a number of possible targets for silver inside the (bacterial) cell have been identified [112]. These targets are diverse and this may be the basis of the success of silver. Since many different processes are affected by silver, resistance to silver is not wide-spread and has not been a major concern in clinical practice. This may also be the reason for the broad range of silvers' antimicrobial activity; not only bacteria but also fungi and yeasts are inhibited and killed.
The bactericidal activity of silver is dependent on the form in which it is applied. Metallic silver has been shown to possess only weak antimicrobial activity which deteriorates fast, and is strongly inhibited by protein adsorption to the silver [77,81]. However, almost all studied silver nanoparticles have very strong bactericidal activity. This activity has been shown to be dependent on the size and shape of the particles [113-115]. Smaller sized silver nanoparticles (<10 nm) were demonstrated to have higher antibiotic activity than larger particles. In addition to the size, the shape of the nanoparticles was also shown to be of influence. In a study by Pal et al., triangular shaped particles of silver were shown to have more bacterial killing activity than rods and spherical particles [113]. In a study by Lok et al. oxidized and reduced nanoparticles were produced under careful controlled conditions. The oxidized particles were shown to contain the antibiotic properties while the reduced ones were ineffective in killing or inhibiting bacterial growth [116]. The authors calculated that approximately 12% of the silver is present in ionic, Ag+ form, tightly associated in the oxidation layer. The release of the Ag+ ions is very slow and hardly ever reaches the concentrations needed to kill bacteria. The silver ions are too tightly bound in the oxidation layer and thus free Ag+ released from the nanoparticles cannot solely be responsible for the antibiotic action.
An often observed problem of commercially available nanoparticles is that these have a tendency to form large aggregates in solutions with physiological salt concentrations [116]. This means that when performing in vitro assays with suspension of such particles, the conditions are not ideal because: (i) the nanoparticles aggregate or (ii) the solvent does not reflect the physiological conditions. The fact that smaller and irregular nanoparticles show the highest antibiotic activity indicates that the surface area of the particles is important. The rate at which Ag+ can be released is dependent on the surface area, and can thus be the determining factor for antibiotic activity [117,118]. The formation of a surface layer of oxidized Ag during production and storage might occur, and this may be a reservoir for the antimicrobial ions. As the nanoparticles are only precisely analyzed in a few studies, this remains speculation.
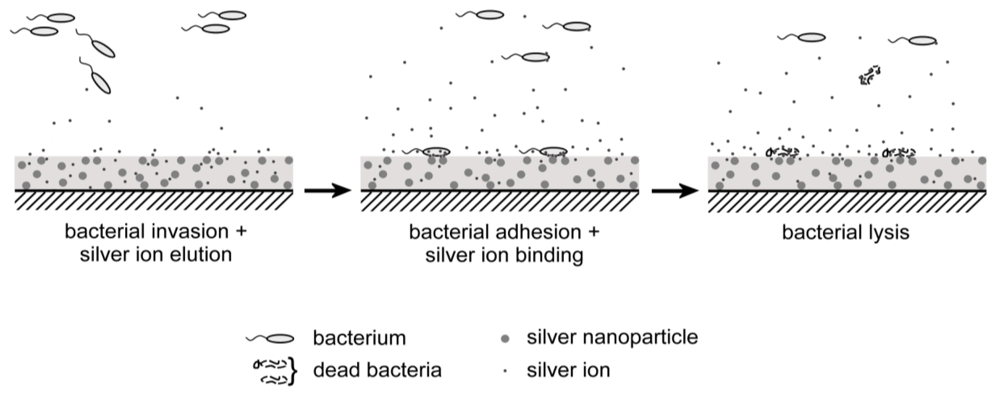
Additionally, nanoparticles themselves have been shown to bind to and migrate into cells, damaging proteins, genetic material and the membranes, leading to cell-death [119-121]. One can never exclude the fact that the silver nanoparticles are the interacting and bioactive components. The release of silver ions will of course continue after uptake of the Ag-nanoparticles. A possible explanation for the bactericidal activity of silver particles comprises the direct transfer of silver ions, from oxidized nanoparticles to biological targets as proteins or the cell membrane. This would then mean a direct interaction with the silver particles and a solvent-free transfer of silver ions. This process is demonstrated in Figure 4.
As previously stated, silver ions have been shown to bind to sulfhydryl and phosphoryl groups of proteins, rendering these inactive and causing aggregations of these proteins [112]. In addition, intracellular silver nanoparticles cause damage to proteins and nucleic acids inside bacteria. The clearest effect of silver nanoparticles and silver ions is direct binding to the cell membrane. Accumulation of silver on negatively charged parts of the cellular membrane leads to perforation of the membrane, leakage of the cellular compounds, and cell death. In a study by Danilczuk and coworkers, the generation of reactive oxygen species (e.g., oxygen radicals like O2− or hydroxyl radicals) on silver nanoparticles was demonstrated [122,112]. The addition of the anti-oxidant N-acetylcysteine to solutions of Ag nanoparticles or Ag ions inhibited the antibiotic activity [123]. This result indicates that oxygen species generated by silver, play a role in the killing activity of gram-negative bacteria in that study. It remains to be determined whether this mechanism is uniformly responsible for the antibiotic activity of silver. Another possibility is that the anti-oxidant prevents the formation of a silver oxide layer on the nanoparticle surface and consequently formation of the Ag+ reservoir. Therefore, the physico-chemical nature of silver particles, used in studies to analyze the mechanism of action of antimicrobial silver nanoparticles, should be carefully determined.
The concentration of silver ions needed for an optimal antibiotic effect ranges between 10 nM and 10 μM [123]. However the release of soluble silver ions from nanoparticles alone is unlikely to lead to sufficiently high enough concentrations in vivo. This means that silver transfer directly from the particles in the coating to the microbes may occur.
The long-term use of silver has been associated with the development of bacterial resistance to silver [124,125]. A number of resistant bacterial strains have been isolated that show a decreased sensitivity to silver nanoparticles and silver ions. The broad range of silver targets in the cell makes evolution of silver resistance slow. The appearance of silver resistance is a matter of concern although at this moment this resistance does not seem to spread as for antibiotics. This may be based on the fact that silver affects a number of cellular processes as well as the membrane integrity, while antibiotics specifically target one process. The bacteria mutate in such a way that the antibiotic is metabolized or removed from the cell. Also the specific target enzyme can be mutated, so that the sensitivity for the antibiotic decreases. In the case of silver, some of the resistance genes that have been identified seem to be involved in pumping silver out of the cell [126]. Also the composition of the membrane can be changed so that silver affinity is lowered and antimicrobial activity is abolished.
6. Side Effects of Silver and Silver Coatings
6.1. Effects of Silver on Human Physiology
The extended use of silver and silver solutions can lead to a number of disorders [127]. These can also be unintentional due to long-term occupational exposure to high doses of silver particles, vapors or solutions. The most common condition is argyria in which silver is stored under the skin, leaving it with a grayish tinge [128-130]. Argyria is considered a harmless condition other than the cosmetic consequences it has for the patient which are irreversible. Not only the skin can become discolored, but also the eyes can suffer this fate upon long-term silver exposure. This ophthalmological condition is called argyrosis and is mostly caused by prolonged (voluntary) intake of silver nitrate or silver colloid solutions [125]. Argyrosis was also reported to be caused by silver-nitrate coated soft contact lenses, which were used for cosmetic purposes [131]. The leached silver apparently accumulated in the eye to leave a blue-gray deposit. A cosmetic consequence of the medicinal use of silver was observed in the discoloration of scars of burns treated with silver containing dressings. This phenomenon was studied in detail in a pig model, but represents a real possibility in human patients as the use of silver-impregnated dressings is increasing [132]. Besides these cosmetic disorders, reports on silver induced organ toxicity or organ damage are rare [127]. Silver has been shown to accumulate in the liver and kidney upon prolonged silver intake. The high level of thiol-rich proteins like glutathione in the liver is a possible reservoir for silver. Also silver has a tendency to be accumulated in the glomerulus of the kidney. Recently Mayr and coworkers studied the kidney of a patient with severe organ agyrosis [118]. They could demonstrate the presence of a high number of diffuse silver deposits, but no toxicity to the kidney was observed. This is in line with the fact there are very few reports showing silver-mediated organ toxicity.
Recently an animal study was performed to assess the in vivo tissue reaction to urinary catheter materials impregnated with noble metals (Ag, Au, Pd) or a mixture thereof [133]. It was found that the coatings with silver alone and silver with medium amounts of gold and low-medium palladium content performed best. These coatings showed the lowest inflammatory response and induced the thinnest fibrous capsule after three weeks implantation. Additionally, there was little lactate dehydrogenase (LDH) release in the exudate around the implants in the rats, demonstrating the in vivo biocompatibility of silver containing coatings. These data support earlier observations that silver has low toxicity and silver coated materials display good biocompatibility.
6.2. Silver Induced Cytotoxicity and Genotoxicity
From the information above it is clear that silver ions and silver salts have limited systemic toxicity in vivo. The solubility of silver is low in a physiological setting where the most common anion is chloride, and silver chloride is relatively insoluble. However, the increase in use of small silver particles and silver nanoparticles requires new evaluation of silver toxicity [121]. This necessity is increased by the non-regulated growth in silver nanoparticles use in cosmetic products. In recent studies silver nanoparticles were added to cell cultures and the effects on cell viability and metabolism were assessed [134]. Several cell types like lung fibroblasts, glioblastoma cells, and keratinocytes ingest the nanoparticles by clathrin-mediated endocytosis. The nanoparticles were distributed evenly throughout the cells and caused the instability of chromosomes in the nucleus. The particles also caused the change of cell morphology by down-regulating a number of proteins, under which the cytoskeletal protein filamin. In addition, upon treatment with silver, cells demonstrated a transient increase in cytosolic calcium which mediated cytotoxicity. The authors proposed that a disruption of the respiratory chain in the mitochondria will lead to the production of reactive oxygen species and disruption of adenosine-triphosphate (ATP) synthesis, which can lead to DNA damage. This DNA damage may lead to cell cycle arrest and eventually to the complete cessation in proliferation. This anti-proliferative effect can also be used to treat cancers or maybe prevent neointimal hyperplasia in stents.
6.3. Blood Compatibility of Silver Coatings
Silver coatings have been applied to central venous catheters that are intended to function in contact with blood for a prolonged time. The interaction of these coatings with blood is therefore of critical importance for the function of the device. Studies with central venous catheter (CVC) carrying patients showed varying results: Some have shown that silver coatings did not increase the rate of catheter induced thrombosis, while others implicate a rise in thrombus formation [135-137]. One has to keep in mind that the rate of thrombus formation on CVCs in general is high (up to 40%), especially in catheters that are in place for a long period of time, like for oncology patients. When CVCs are removed after a short time, the number of catheters carrying thrombi is much lower (<<10%). In case a catheter associated thrombus does occur, systemic anticoagulation is the treatment of choice [138]. The application of heparin was demonstrated not to influence the thrombus formation in and on the catheter, but administration of low-dose warfarin was effective in decreasing the thrombus formation. This treatment however is reserved for patients with normal liver function and good health. The modification of the catheter surfaces with anticoagulant molecules may be a more effective and safe strategy to prevent catheter-induced thrombus formation. Over the years a number of heparin coatings have been introduced. The effect of surface coatings containing heparin on bacterial adhesion and biofilm formation is unclear. Some reports show a decreased rate of infection while other reports show no antibiotic effect of surface attached heparin [139-142]. The mechanism, by which heparin coatings decrease bacterial colonization, may be indirect. Proteins that bind specifically to heparin may possess antibactericidal activity and in this way reduce microbial adhesion and biofilm formation [143,144]. Peptides derived from several plasma proteins like fibronectin, vitronectin, protein-C inhibitor, von Willebrand factor, were demonstrated to have antimicrobial activity. These proteins will bind to surface bound heparin on the catheters directly upon blood contact. This layer of proteins will then exert its bactericidal activity and reduce bacterial adhesion. For coatings with non-covalent heparin this layer of proteins with antimicrobial activity will eventually be washed away and therefore in some studies no effect of heparin coatings was observed.
In a recent study by Stevens, a surface coating containing both heparin and silver nanoparticles was studied in vitro [145]. The coatings were demonstrated to have silver dependent antimicrobial activity, but also the coatings with only heparin demonstrated bactericidal activity after incubation in human plasma (vide supra). The blood compatibility of the coatings was studied by determining platelet adhesion and thrombin generation. The coatings containing heparin showed excellent blood compatibility with no thrombin generation found in the time-course of the experiments. Inclusion of silver nanoparticles in the heparin coatings did not influence thrombin generation. Also in the coatings containing only silver particles, the thrombin generation was not altered when compared to the control. However a clear effect was found on platelet adhesion and activation. The number of adhered platelets was strongly reduced on the coatings containing silver and/or heparin. Upon a more careful examination of the adhered platelets, their morphology appeared distorted which indicated activation and disruption. This was in accordance with an earlier report by the same authors that described activation and disruption of platelets on surfaces containing AgBr nanoparticles [146]. The authors proposed that platelets may get activated and disrupted by mechanisms similar to the bactericidal effect of the silver nanoparticles. However the activation of the platelets did not reflect in thrombin generation and thrombus formation. These results indicate that catheters containing coatings with both heparin and silver nanoparticles may be a real option to reduce infection rate and thrombosis risk.
All in all silver containing coatings may prove to be a real asset for hospitals in decreasing the number of medical device related infection. However, the nature of the silver particles as well as how these are incorporated in the coating will determine the efficacy of such modified medical devices.

References
- Gradinger, R.; Graf, R.; Grifka, J.; Löhr, J. Das infizierte implantat. Der. Orthopäde 2008, 3, 257–269. [Google Scholar]
- Hellmann, M.; Mehta, S.D.; Bishai, D.M.; Mears, S.C.; Zenilman, J.M. The estimated magnitude and direct hospital costs of prosthetic joint infections in the United States, 1997 to 2004. J. Athroplasty 2010, 25, 766–771. [Google Scholar]
- Sampredo, M.F.; Patel, R. Infections associated with long-term prosthetic devices. Infect. Dis. Clin. N. Am. 2007, 21, 785–819. [Google Scholar]
- Tokarczyk, A.J.; Greenberg, S.B.; Vender, J.S. Death, dollars, and diligence: Prevention of catheter-related bloodstream infections must persist. Crit. Care Med. 2009, 37, 2320–2321. [Google Scholar]
- Von eiff, C.; jansen, B.; Kohnen, W.; Becker, K. Infections associated with medical devices. Drugs 2005, 65, 179–214. [Google Scholar]
- Turnidge, J.D.; Kotsanas, D.; Munckhof, W.; Roberts, S.; Bennett, C.M.; Nimmo, G.R.; Coombs, G.W.; Murray, R.J.; Howden, B.; Johnson, P.D.R.; Dowling, K. Staphylococcus aureus bacterimia: A major cause of mortality in Australia and New Zealand. Med. J. Aust. 2009, 191, 368–373. [Google Scholar]
- Olsen, M.A.; Chu-Ongsakul, S.; Brandt, K.E.; Dietz, J.R.; Mayfeld, J.; Fraser, V.J. Horpital-associated costs due to surgical site infection after breast surgery. Arch. Surg. 2008, 143, 53–60. [Google Scholar]
- Noimark, S.; Dunnill, C.W.; Wilson, M.; Parkin, I.P. The role of surfaces in catheter-associated infections. Chem. Soc. Rev. 2009, 38, 3435–3448. [Google Scholar]
- Trautner, B.W.; Darouiche, R.O. Catheter-associated infections. Arch. Intern. Med. 2004, 164, 842–850. [Google Scholar]
- David, A.; Risitano, D.C.; Mazzeo, G.; Sinardi, L.; Venuti, F.S.; Sinardi, A.U. Central venous catheters and infections. Minerva Anestesiol. 2005, 71, 561–564. [Google Scholar]
- Halton, K.; Graves, N. Economic evaluation and catheter-related bloodstream infections. Emerg. Infect. Dis. 2007, 13, 815–823. [Google Scholar]
- Prencevich, E.N.; Pittet, D. Preventing catheter-related bloodstream infections. J. Am. Med. Assoc. 2009, 301, 1285–1287. [Google Scholar]
- Moureau, N.L. Reducing the costs of catheter-related bloodstream infections. Nursing 2009, 39, 14–15. [Google Scholar]
- Zingg, W.; Imhof, A.; Maggiorini, M.; Stocker, R.; Keller, E.; Ruef, C. Impact of a prevention strategy targeting hand hygiene and catheter care on the incidence of catheter-related bloodstream infections. Crit. Care Med. 2009, 37, 2167–2173. [Google Scholar]
- Kallen, A.J.; Patel, P.R.; O'Grady, N.P. Preventing catheter-related bloodstream infections outside the intensive care unit: Expanding to new settings. Healthcare Epidem. 2010, 51, 335–341. [Google Scholar]
- Walz, J.M.; Memtsoudis, S.G.; Heard, S.O. Prevention of central venous catheter bloodstream infections. J. Intensive Care Med. 1997, 25, 131–138. [Google Scholar]
- Rosenthal, V.D.; Maki, D.G.; Graves, N. The international nosocomical infection control consortium (INICC): Goals and objectives, description of surveillance methods, and operational activities. Am. J. Infect. Control 2008, 36, e1–e12. [Google Scholar]
- Bearman, G.M.L.; Munro, C.; Sessler, C.N.; Wenzel, R.P. Infection control and the prevention of nosocomical infections in the intensive care unit. Sem. Resp. Crit. Care Med. 2006, 27, 310–324. [Google Scholar]
- Youg, W.T. How to respond to changes in the regulation of the ethylene-oxide sterilization process. Med. Dev. Technol. 2006, 17, 12–15. [Google Scholar]
- Thevenot, P.; Hu, W.; Tang, L. Surface chemistry influences implant biocompatibility. Curr. Top. Med. Chem. 2008, 8, 270–280. [Google Scholar]
- Vroman, L. Methods of investigating protein interactions on artificial and natural surfaces. Ann. N. Y. Acad. Sci. 1987, 516, 300–305. [Google Scholar]
- Stutz, H. Protein attachment onto silica surfaces—A survey of molecular fundamentals, resulting effects and novel preventive strategies in CE. Electrophoresis 2009, 30, 2032–2061. [Google Scholar]
- Fang, F.; Szleifer, I. Kinetics and thermodynamics of protein adsorption: A generalized molecular theoretical approach. Biophys. J. 2001, 80, 2568–2589. [Google Scholar]
- Ganazzoli, F.; Raffaini, G. Computer simulation of polypeptide adsorption on model biomaterials. Phys. Chem. Chem. Phys. 2005, 7, 365–3663. [Google Scholar]
- Pavithra, D.; Doble, M. Biofilm formation, bacterial adhesion and host response on polymeric implants—issues and prevention. Biomed. Mater. 2008, 3, 1–13. [Google Scholar]
- Hoiby, N.; Bjarnsholt, T.; Givskov, M.; Molin, S.; Ciofy, O. Antibiotic resistance of bacterial biofilms. Int. J. Antimicrob. Agents 2010, 35, 322–332. [Google Scholar]
- Hall-Stoodley, L.; Stoodley, P. Evolving concepts in biofilm infections. Cell. Microbiol. 2009, 11, 1034–1043. [Google Scholar]
- Donlan, R.M. Biofilms: Microbial life on surfaces. Emerg. Infect. Dis. 2002, 9, 891–890. [Google Scholar]
- Sutherland, I.W. The biofilm matrix—an immobilized but dynamic microbial environment. Trends Microbiol. 2001, 9, 222–227. [Google Scholar]
- Sousa, C.; Teixeira, P.; Oliveira, R. Influence of surface properties on the adhesion of Staphylococcus epidemidis to acrylic and silicone. Int. J. Biomater. 2009. [Google Scholar] [CrossRef]
- van Hoogmoed, C.G.; van der Mei, H.C.; Busscher, H.J. The influence of calcium on the initial adhesion of S. thermophilus to stainless steel under flow studied by metallurgical microscopy. Biofouling 1997, 11, 167–176. [Google Scholar]
- Katsikogianni, M.; Spiliopoulou, I.; Dowling, D.P.; Missirlis, Y.F. Adhseion of slime producing Staphylococcus epidermidis strains to PVC and diamond-like carbon/silver/fluorinated coatings. J. Mater. Sci. 2006, 17, 679–689. [Google Scholar]
- Almaguer-Flores, A.; Ximenez-Fyvie, L.A.; Rodil, S.E. Oral bacterial adhesion on amorphous carbon and titanium films: Effect of surface roughness and culture media. J. Biomed. Mater. Sci. B Appl. Biomater. 2010, 92B, 196–204. [Google Scholar]
- Zhao, B.; Brittain, W.J. Polymeric brushes: Surface-immobilized macromolecules. Prog. Polym. Sci. 2000, 25, 677–710. [Google Scholar]
- Hoffmann, J.; Groll, J.; Heuts, J.; Rong, H.; Klee, D.; Ziemer, G.; Moeller, M.; Wendel, H.P. Blood cell and plasma protein repellent properties of star-PEG-modified surfaces. J. Biomater. Sci. Polym. Ed. 2006, 17, 985–996. [Google Scholar]
- Fundeanu, I.; Klee, D.; Schouten, A.J.; Busscher, H.J.; van der Mei, H.C. Solvent-free functionalization of silicone rubber and efficacy of PAAm brushes grafted from an amino-PPX layer against bacterial adhesion. Acta Biomater. 2010, 6, 4271–4276. [Google Scholar]
- Cheng, G.; Xue, H.; Zhang, Z.; Chen, S.; Jiang, S. A switchable biocompatible polymer surface with self-sterilizing and nonfouling capabilities. Angew. Chem. Int. Ed. 2008, 47, 8831–8834. [Google Scholar]
- Senaratne, W.; Andruzzi, L.; Ober, C.K. Self-assembled monolayers and polymer brushes in biotechnology: Current applications and future perspectives. Biomacromolecules 2005, 6, 2427–2448. [Google Scholar]
- Schreiber, F. Structure and growth of self-assembling monolayers. Prog. Surf. Sci. 2000, 65, 151–256. [Google Scholar]
- Bearinger, J.P.; Terrettaz, S.; Michel, R.; Tirelli, N.; Vogel, H.; Textor, M.; Hubbell, J.A. Chemiadsorbed poly(propylene sulphide)-based copolymers resist biomolecular interactions. Nat. Mater. 2003, 2, 259–264. [Google Scholar]
- Khoo, X.; Hamilton, P.; O'Toole, G.A.; Snyder, B.D.; Kenan, D.J.; Grinstaff, M.W. Directed assembly of PEGylated-peptide coatings for infection-resistant titanium metal. J. Am. Chem. Soc. 2009, 131, 10992–10997. [Google Scholar]
- Heijkants, R.G.J.C. Nanotechnology delivers microcoatings. Med. Device Technol. 2006, 17, 14–16. [Google Scholar]
- Bridges, A.W.; Garcia, A.J. Anti-inflammatory polymeric coatings for implantable biomaterials and devices. J. Diabet. Sci. Technol. 2008, 2, 984–994. [Google Scholar]
- Roosjen, A.; van der Mei, H.C.; Busscher, H.J.; Norde, W. Microbial adhesion to poly(ethyle oxide) brushes: Influence of polymer chain length and temperature. Langmuir 2004, 20, 10949–10955. [Google Scholar]
- Nohr, R.S.; MacDonald, J.G. New biomaterials through surface segregation phenomenon: New quaternary ammonium compounds as antibacterial agents. J. Bioamter. Sci. Polym. Ed. 1994, 5, 607–619. [Google Scholar]
- Thorsteinsson, T.; Loftsson, T.; Masson, M. Soft antibacterial agents. Curr. Med. Chem. 2003, 10, 1129–1136. [Google Scholar]
- Murata, H.; Koepsel, R.R.; Matyjaszewski, K.; Russell, A.J. Permanent, non-leaching antibacterial surfaces-2: How high density cationic surfaces kill bacterial cells. Biomaterials 2007, 28, 4870–4879. [Google Scholar]
- Cheng, G.; Xue, H.; Li, G.; Jiang, S. Integrated antimicrobial and nonfouling hydrogels to inhibit the growth of planktonic bacterial cells and keep the surface clean. Langmuir 2010, 26, 10425–10428. [Google Scholar]
- Rawlinson, L.B.; O'Brien, P.J.; Brayden, D.J. High content analysis of cytotoxic effects of pDMAEMA on human intestinal epithelial and monocytes cultures. J. Contr. Rel. 2010, 146, 84–92. [Google Scholar]
- Venkataraman, S.; Zhang, Y.; Liu, L.; Yang, Y. Design, synthesis and evaluation of hemocompatible pegylated-antimcrobial polymers with well-controlled molecular structures. Biomaterials 2010, 31, 1751–1756. [Google Scholar]
- Fredell, D.L. Biological properties and applications of cationic surfactants. In Cationic Surfactants, 1st ed.; Cross, J., Singer, E.J., Eds.; Marcel Dekker Inc: New York, NY, USA, 1990; pp. 31–60. [Google Scholar]
- Ravikumar, T.; Murata, H.; Koepsel, R.R.; Russell, A.J. Surface-active antifungal polyqyaternary amine. Biomacromolecules 2006, 7, 2762–2769. [Google Scholar]
- Hegstad, K.; Langsrud, S.; Lunestad, B.T.; Scheie, A.A.; Sunce, M.; Yazdankhah, S.P. Does the wide use of quaternary ammonium compounds enhance the selection and spread of antimicrobial resistance and thus threaten our health? Microb. Drug Resist. 2010, 16, 91–104. [Google Scholar]
- Russell, A.D. Introduction of biocides into clinical practice and the impact on antibiotic-resistant bacteria. J. Appl. Microbiol. 2002, 92, 121S–135S. [Google Scholar]
- Fleming, A. On the antibacterial action of cultures of a Penicilium, with special reference to their use in the isolation of B. influenzae. Br. J. Exp. Pathol. 1929, 10, 226–236. [Google Scholar]
- Jaeblon, T. Polymethylmethacrylate: Properties and contemporary uses in orhtopaedics. J. Am. Acad. Otrhop. Surg. 2010, 18, 297–305. [Google Scholar]
- Webb, J.C.J.; Spencer, R.F. The role of polymethylmethacrylate bone cement in modern orthopaedic surgery. J. Bone Joint Surg. 2007, 89-B, 851–857. [Google Scholar]
- Norowski, P.A.; Bumgardner, J.D. Biomaterial and antibiotic strategies for peri-implants. J. Biomed. Mater. Res. B Appl. Biomater. 2009, 88B, 530–543. [Google Scholar]
- Zhao, L.; Chu, P.K.; Zhang, Y.; Wu, Z. Antibacterial coatings on titanium implants. J. Biomed. Mater. Res. B Appl. Biomater. 2009, 91B, 470–480. [Google Scholar]
- Kälicke, T.; Schierholz, J.; Schlegel, U.; Frangen, T.M.; Köller, M.; Printzen, G.; Seybold, D.; Klöckner, S.; Muhr, G.; Arens, S. Effect on infection resistance of a local antiseptic and antibiotic coating on osteosynthesis implants: An in vitro and in vivo study. J. Orthop. Res. 2006, 24, 1622–1640. [Google Scholar]
- Harris, L.G.; Mead, L.; Müller-Oberländer, E.; Richards, R.G. Bacteria and cell cytocompatibility studies on coated medical grade titanium surfaces. J. Biomed. Mater. Res. 2006, 78A, 50–58. [Google Scholar]
- Oosterbos, G.J.; Vogely, H.C.; Nijhof, M.W.; Fleer, A.; Verbout, A.J.; Tonino, A.J.; Dhert, W.J. Osseointegration of hydroxyapatite-coated and noncoated Ti6Al4V implants in the presence of local infection: A comparative histomorphometrical study in rabbits. J. Biomed. Mater. Res. 2002, 60, 339–347. [Google Scholar]
- Stigter, M.; de Groot, K.; Layrolle, P. Incorporation of tobramycin into biomimetic hydroxyapatite coating on titanium. Biomaterials 2002, 23, 4143–4153. [Google Scholar]
- Stigter, M.; Bezemer, J.; de Groot, K.; Layrolle, P. Incorporation of different antibiotics into carbonated hydrozyapatite coatings on titanium implants, release and antibiotic effect. J. Contr. Rel. 2004, 99, 127–137. [Google Scholar]
- Darouiche, R.O.; Mansouri, M.D.; Zakarevicz, D.; Alsharif, A.; Landon, G.C. In vivo efficacy of antimicrobial-coated devices. J. Bone Joint Surg. Am. 2007, 89, 792–797. [Google Scholar]
- Darouiche, R.O.; Raad, I.I.; Heard, S.O.; Thornby, J.I.; Wenker, O.C.; Gabrielli, A.; Berg, J.; Khardori, N.; Hanna, H.; Hachem, R.; Harris, R.L.; Mayhall, G. A comparison of two anti-microbial-impregnated central venous catheters. New Eng. J. Med. 1999, 340, 1–8. [Google Scholar]
- Falagas, M.E.; Fragoulis, K.; Bliziotis, I.A.; Chatzinikolaou, I. Rifampicin-impregnated central venous catheters: A meta-analysis of randomized controlled trials. J. Antimicrob. Chemother. 2007, 59, 359–369. [Google Scholar]
- Hernandez-Richter, T.; Schardey, H.M.; Wittmann, F.; Mayr, S.; Schmitt-Sody, M.; Blasenbrue, S.; Heiss, M.M.; Gabka, C.; Angele, M.K. Rifampicin and triclosan but not silver is effective in preventing bacterial infection of vascular Dacron graft material. Eur. J. Vasc. Endovasc. Surg. 2003, 26, 550–557. [Google Scholar]
- Halton, K.A.; Cook, D.; Paterson, D.L.; Safdar, N.; Graves, N. Cost-effectiveness of a central venous catheter care bundle. PloS ONE 2010, 5, e12815. [Google Scholar]
- Walder, B.; Pittet, D.; Tramer, M.R. Prevention of bloodstream infections with central venous catheters treated with anti-infective agents depends on catheter type and insertion time: Evidence from a meta-analysis. Infect. Control Hosp. Epidemiol. 2002, 23, 748–756. [Google Scholar]
- Boelens, J.J.; Dankert, J.; Murk, J.L.; Weening, J.J.; van der Poll, T.; Dingemans, K.P.; Koole, L.; Laman, J.D.; Zaat, S.A.J. Biomaterial-associated persistence of Staphylococcus epidermidis in pericatheter macrophages. J. Infect. Dis. 2000, 181, 1337–1349. [Google Scholar]
- Broekhuizen, C.A.N.; de Boer, L.; Schipper, K.; Jones, C.D.; Quadir, S.; Feldman, R.G.; Dankert, J.; Vandenbroucke-Grauls, C.M.J.E.; Weening, J.J.; Zaat, S.A.J. Peri-implant tissue is an important niche for Staphylococcus epidermidis in experimental biomaterial-associated infection in mice. Infect. Immun. 2007, 75, 1129–1136. [Google Scholar]
- Ceri, H.; Olson, M.E.; Turner, R.J. Needed, new paradigms in antibiotic development. Expert Opin. Pharmacother. 2010, 11, 1233–1237. [Google Scholar]
- Lohda, A.; Furlan, A.D.; Whyte, H.; Moore, A.M. Prophylactic antibiotics in the prevention of catheter-associated bloodstream bacterial infection in preterm neonates: A systematic review. J. Perionatol. 2008, 28, 526–533. [Google Scholar]
- Alexander, J.W. History of the medical use of silver. Surg. Infect. 2009, 10, 289–292. [Google Scholar]
- Spear, M. Silver: An age-old treatment modality in modern times. Plast. Surg. Nurs. 2010, 30, 90–93. [Google Scholar]
- Atiyeh, B.S.; Costagliola, M.; Hayek, S.N.; Dibo, S.A. Effect of silver on burn wound infection and healing: Review of the literature. Burns 2007, 33, 139–148. [Google Scholar]
- Silver, S.; Phung, L.T.; Silver, G. Silver as biocides in burn and wound dressings and bacterial resistance to silver compounds. J. Ind. Microbiol. Biotechnol. 2006, 33, 627–634. [Google Scholar]
- Klasen, H.J. Historical review of the use of silver in the treatment of burns. I. Early uses. Burns 2000, 26, 117–130. [Google Scholar]
- Klasen, H.J. A historical review of the use of silver in the treatment o burns. II. Renewed interest for silver. Burns 2000, 26, 131–138. [Google Scholar]
- Rai, M.; Yadav, A.; Gade, A. Silver nanoparticles as a new generation of antimicrobials. Biotechnology Advances 2009, 27, 76–83. [Google Scholar]
- Nakane, T.; Gomyo, H.; Sasaki, I.; Kimoto, Y.; Hanzawa, N.; Teshima, Y.; Namba, T. New antiaxillary odour deodorant made with antimicrobial Ag-eolite (silver-exchanged zeolite). Int. J. Cosmet. Sci. 2006, 28, 299–309. [Google Scholar]
- Meakins, J.L. Silver and new technology: Dressings and devices. Surg. Infect. 2009, 10, 293–296. [Google Scholar]
- Furno, F.; Morley, K.S.; Wong, B.; Sharp, B.L.; Arnold, P.L.; Howdle, S.M.; Bayston, R.; Brown, P.D.; Winship, P.D.; Reid, H.J. Silver nanoparticles and polymeric medical devices: A new approach to prevention of infection? J. Antimicrob. Chemother. 2004, 54, 1019–1024. [Google Scholar]
- Johnston, H.J.; Hutchison, G.; Christensen, F.M.; Peters, S.; Hankin, S.; Stone, V. A review of the in vivo and in vitro toxicity of silver and gold particulates: Particle attributes and biological mechanisms responsible for the observed toxicity. Crit. Rev. Toxicol. 2010, 40, 328–346. [Google Scholar]
- Dowsett, C. The use of silver-based dressing in wound care. Nurs. Stand. 2004, 19, 56–60. [Google Scholar]
- Strom-Versloot, M.N.; Vos, C.G.; Ubbink, D.T.; Vermeulen, H. Topical silver for preventing wound infection. Cochrane Database Syst. Rev. 2010, 3, CD006478. [Google Scholar]
- Carter, M.J.; Tingley-Kelley, K.; Warriner, R.A., III. Silver treatments and silver-impregnated dressings for the healing of leg wounds and ulcers: A systematic review and meta-analysis. J. Am. Acad. Dermatol. 2010, 63, 668–679. [Google Scholar]
- Lo, S.; Chang, C.; Hu, W.; Hayter, M.; Change, Y. The effectiveness of silver-releasing dressing in the management of non-healing wounds: A meta-analysis. J. Clin. Nurs. 2009, 18, 716–728. [Google Scholar]
- Woo, K.Y. Review: Silver-releasing dressings improve healing and quality of life in patients with non-healing chronic wounds. Evid. Based Nurs. 2009, 12, 117. [Google Scholar]
- Gravante, G.; Caruso, R.; Sorge, R.; Nicoli, F.; Gentile, P.; Cervelli, V. Nanocrystalline silver. Reconstr. Surg. Burns 2009, 63, 201–205. [Google Scholar]
- Verdu-Soriano, J.; Rueda-Lopez, J.; Martinez-Cuervo, F.; Soldevilla-Agreda, J. Effects of an activated charcoal solver dressing on chronic wounds with no clinical signs of infection. J. Wound Care 2004, 13, 419–423. [Google Scholar]
- Miller, C.N.; Newall, N.; Kapp, S.E.; Lewin, G.; Karimi, L.; Carville, K.; Gliddon, T.; Santamaria, N.M. A randomized-controlled trial comparing cadexomer iodine and nanocrystalline silver on the healing of leg ulcers. Wound Repair Regen. 2010, 18, 359–367. [Google Scholar]
- Gravante, G.; Montone, A. A retrospective analysis of ambulatory burn patients: Focus on wound dressings and healing times. Ann. Rev. Coll. Surg. Engl. 2010, 92, 118–123. [Google Scholar]
- Fichtner, J.; Güresir, E.; Seifert, V.; Raabe, A. Efficacy of silver-bearing external ventricular drainage catheters: A retrospective analysis. J. Neurosurg. 2010, 112, 840–846. [Google Scholar]
- Lackner, P.; Beer, R.; Broessner, G.; Helbok, R.; Galiano, K.; Pleifer, C.; Pfausler, B.; Brenneis, C.; Huck, C.; Engelhardt, K.; Obwegeser, A.A.; Schmutzhard, E. Efficacy of silver-nanoparticles-impregnated external ventricular drain catheters in patients with acute occlusive hydrocephalus. Neurocrit. Care. 2008, 8, 360–365. [Google Scholar]
- Roe, D.; Karandikar, B.; Bonn-Savage, N.; Gibbins, B.; Roullet, J.B. Antimicrobial surface functionalization of plastic catheters by silver nanoparticles. J. Antimicrob. Chemther. 2008, 61, 869–876. [Google Scholar]
- Hsu, S.H.; Tseng, H.J.; Lin, Y.C. The biocompatibility and antibacterial properties of waterborne polyurethane-silver nanocomposites. Biomaterials 2010, 31, 6796–6808. [Google Scholar]
- McCann, M.; Moore, Z.E.H. Interventions for preventing infectious complications in haemodialysis patients with central venous catheters. Cochrane Database Syst. Rev. 2010, 1, CD006894. [Google Scholar]
- Gilbert, R.E.; Harden, M. Effectiveness of impregnated central venous catheters for catheter related blood stream infection: A systematic review. Curr. Opin. Infect. Dis. 2008, 21, 325–245. [Google Scholar]
- Jaeger, K.; Zenz, S.; Jüttner, B.; Ruschulte, H.; Kuse, E.; Heie, J.; Piepenbrock, S.; Ganser, A.; Karthaus, M. Reduction of catheter-related infections in neutropenic patients: A prospective controlled randomized trial using chlorohexidine and silver sulfadiazine-impregnated central venous catheter. Ann. Hematol. 2005, 84, 258–262. [Google Scholar]
- Rupp, M.E.; Lisco, S.J.; Lipsett, P.A.; Perl, T.M.; Keating, K.; Civetta, J.M.; Mermel, L.A.; Lee, D.; Dellinger, P.; Donahoe, M.; Giles, D.; Pfaller, M.A.; Maki, D.G.; Sheretz, R. Effect of a second-generation venous catheter impregnated with chlorohexidine and silver sulfadiazine on central catheter-related infections. Ann. Intern. Med. 2005, 143, 570–580. [Google Scholar]
- Khare, M.D.; Bukhari, S.S.; Swann, A.; Spiers, P.; McLaren, I.; Myers, J. Reduction of catheter-related colonisation by the use of a silver zeolite-impregnated central venous catheter in adult critical care. J. Infect. 2007, 54, 146–150. [Google Scholar]
- Kaflon, P.; de Vaumas, C.; Samba, D.; Boulet, E.; Lefrant, J.; Eyraud, D.; Lherm, T.; Santoli, F.; Naija, W.; Riou, B. Comparison of silver-impregnated with standard multi-lumen central venous catheters in critically ill patients. Crit. Care Med. 2007, 35, 1032–1039. [Google Scholar]
- Johnson, J.R.; Kuskowski, M.A.; de Wilt, T.J. Systematic review: Antimicrobial urinary catheters to prevent catheter-associated urinary tract infection in hospitalized patients. Ann. Intern. Med. 2006, 144, 116–126. [Google Scholar]
- Trautner, B. Management of catheter-associated urinary tract infection. Curr. Opin. Infect. Dis. 2010, 23, 76–82. [Google Scholar]
- Seymour, C. Audit of catheter-associated UTI using silver alloy-coated Foley catheters. Br. J. Nurs. 2006, 15, 598–603. [Google Scholar]
- Parker, D.; Callan, L.; Harwood, J.; Thompson, D.L.; Wilde, M.; Gray, M. Nursing interventions to reduce the risk of catheter-associated urinary tract infection. J. Wound Ostomy Cont. Nurs. 2009, 36, 23–34. [Google Scholar]
- Liu, J.; Sonshine, D.A.; Shervani, S.; Hurt, R.H. Controlled release of biologically active silver from nanosilver surfaces. ACS Nano 2010, 4, 6903–6913. [Google Scholar]
- Pallavicini, P.; Taglietti, A.; Dacarro, G.; Diaz-Fernandez, Y.A.; Galli, M.; Grisoli, P.; Patrini, M.; De Magistris, G.S.; Zanoni, R. Self-assembled monolayers of silver nanoparticles firmly grafted on glass surfaces: Low Ag+ release for an efficient antibacterial activity. J. Colloid Interface Sci. 2010, 350, 110–116. [Google Scholar]
- Safdar, N.; Kluger, D.M.; Maki, D.G. A review of risk factors for catheter-related bloodstream infection caused by percutaenously inserted, noncuffed central venous catheters. Medicine 2002, 81, 466–479. [Google Scholar]
- Gordon, O.; Slenters, T.V.; Brunetto, P.S.; Villaruz, A.E.; Sturdevant, D.E.; Otto, M.; Landmann, R.; Fromm, K.M. Silver coordination polymers for the prevention of implant infection: Thiol interaction, impact on respiratory chain enzymes and hydroxyl radical induction. Antimicrob. Agents Chemother. 2010, 54, 4208–4218. [Google Scholar]
- Pal, S.; Tak, Y.K.; Song, J.M. Does the antibacterial activity of silver nanoparticles depend on the shape of the nanoparticles? A study of the gram-negative bacterium Eschericia coli. Appl. Environ. Microbiol. 2007, 73, 1712–1720. [Google Scholar]
- Panacek, A.; Kvitek, L.; Prucek, R.; Kolar, M.; Vecerova, R.; Pizurove, N.; Sharma, V.K.; Nevecna, T.; Zboril, R. Silver colloid nanoparticles: Synthesis, characterization, and their antibacterial activity. J. Phys. Chem. B 2006, 110, 16248–16253. [Google Scholar]
- Sotiriou, G.A.; Pratsinis, S.E. Antibacterial activity of nanosilver ions and particles. Environ. Sci. Technol. 2010, 44, 5649–5654. [Google Scholar]
- Lok, C.; Ho, C.; Chen, R.; He, Q.; Yu, W.; Sun, H.; Tam, P.K.; Chiu, J.; Che, C. Silver nanoparticles: Partical oxidation and antibacterial activities. J. Biol. Inorg. Chem. 2007, 12, 527–534. [Google Scholar]
- Danscher, G.; Jansons-Locht, L. In vivo liberation of silver ions from metallic silver surfaces. Histochem. Cell. Biol. 2010, 133, 359–366. [Google Scholar]
- Ho, C.; Yau, S.K.; Lok, C.; So, M.; Che, C. Oxidative dissolution of silver nanoparticles by biologically relevant oxidants: A kinetic and mechanistic study. Chem. Asian J. 2010, 5, 285–293. [Google Scholar]
- Sondi, I.; Salopek-Sondi, B. Silver nanoparticles as antimicrobial agent: A case on E. coli as a model for gram-negative bacteria. J. Colloid Interface Sci. 2004, 275, 177–182. [Google Scholar]
- Mayr, M.; Kim, M.J.; Warner, D.; Hopfer, H.; Schroeder, J.; Mihatsch, M.J. Argyria and decreased kidney function: Are silver compounds toxic to the kidney? Am. J. Kidney Dis. 2009, 53, 890–894. [Google Scholar]
- Asharani, P.V.; Mun, G.L.K.; Hande, M.P.; Valiyaveettil, S. Cytotoxicity and genotoxicity of silver nanoparticles in human cells. ACS Nano 2009, 3, 279–290. [Google Scholar]
- Danilczuk, M.; Lund, A.; Saldo, J.; Yamada, H.; Michalik, J. Conduction electron spin resonance of small silver particles. Spectrochim. Acta A 2006, 63, 189–191. [Google Scholar]
- Kim, J.S.; Kuk, E.; Yu, K.N.; Kim, J.; Park, S.J.; Lee, H.J.; Kim, S.H.; Park, Y.K.; Park, Y.H.; Hwang, C.; Kim, Y.; Lee, Y.; Jeong, D.H.; Cho, M. Antimicrobial effects of silver nanoparticles. Nanomed. Nanotechnol. Biol. Med. 2007, 3, 95–101. [Google Scholar]
- Silver, S. Bacterial silver resistance: Molecular biology and uses and misuses of silver compounds. FEMS Microbiol. Rev. 2003, 27, 341–353. [Google Scholar]
- Percival, S.L.; Bowler, P.G.; Russell, D. Bacterial resistance to silver in wound care. J. Hosp. Infect. 2005, 60, 1–7. [Google Scholar]
- Cuin, A.; Massabni, A.C.; Leite, C.Q.F.; Sato, D.N.; Neves, A.; Szpoganicz, B.; Silve, M.S.; Bortoluzzi, A.J. Synthesis, X-ray structure and antimycobacterial activity of silver complexes with α-hydroxycarboxylic acids. J. Inorg. Biochem. 2007, 101, 291–296. [Google Scholar]
- Drake, P.L.; Hazelwood, K.J. Exposure-related health effects of silver and silver compounds: A review. Ann. Occup. Hyg. 2005, 49, 575–585. [Google Scholar]
- Ah, E.; Lee, W.S.; Kim, K.M.; Kim, S.Y. Occupational generalized argyria after exposure to aerosolized silver. J. Dermatol. 2008, 35, 759–760. [Google Scholar]
- Kwon, H.B.; Lee, J.H.; Lee, S.H.; Lee, A.Y.; Choi, J.S.; Ahn, Y.S. A case of argyria following colloidal silver ingestion. Ann. Dermatol. 2009, 21, 308–310. [Google Scholar]
- Tomi, N.S.; Kränke, B.; Aberer, W. A silver man. Lancet 2004, 363, 532. [Google Scholar]
- Hau, S.C.; Tuft, S.J. Presumed corneal argyrosis from occlusive soft contact lenses: A case report. Cornea 2009, 28, 703–705. [Google Scholar]
- Wang, X.; Chang, H.; Francis, R.; Olszowy, H.; Liu, P.; Kempf, M.; Cuttle, L.; Kravchuk, O.; Phillips, G.E.; Kimble, R.M. Silver deposits in cutaenous burn scar tissue is a common phenomenon following application of a silver dressing. J. Cutan. Pathol. 2009, 36, 788–792. [Google Scholar]
- Suska, F.; Svensson, S.; Johansson, A.; Emanuelsson, L.; Karholm, H.; Ohrlander, M.; Thomsen, P. In vivo evaluation of noble metal coatings. J. Biomed. Mater. Res. B Appl. Biomater. 2010, 92B, 86–94. [Google Scholar]
- Asharani, P.V.; Hande, M.P.; Valiyaveettil, S. Anti-proliferative activity of silver nanoparticles. BMC Cell Biol. 2009, 10, 65–79. [Google Scholar]
- Harter, C.; Salwender, H.J.; Bach, A.; Egerer, G.; Goldschmidt, H.; Ho, A.H. Catheter-related infection and thrombosis of the internal jugular vein in hematologic-oncologic patients undergoing chemotherapy. Cancer 2002, 94, 245–251. [Google Scholar]
- Kakkos, S.K.; Haddad, G.K.; Haddad, R.K.; Scully, M.M. Effectiveness of a new tunneled catheter in preventing catheter malfunction: A comparative study. J. Vasc. Interv. Radiol. 2008, 19, 1018–1026. [Google Scholar]
- Jansen, B.; Rinck, M.; Wolbring, P.; Strohmeier, A.; Jahns, T. In vitro evaluation of the antimicrobial efficacy and biocomaptibility of a silver-coated central venous catheter. J. Biomater. Appl. 1994, 9, 55–70. [Google Scholar]
- Kuter, D.J. Thrombotic complications of central venous catheters in cancer patients. Oncologist 2004, 9, 207–216. [Google Scholar]
- Tenke, P.; Riedl, C.R.; Jones, G.L.; Williams, G.J.; Stickler, D.; Nagy, E. Bacterial biofilm formation on urological devices and heparin coating as preventive strategy. Int. J. Antimicrob. Agents 2004, 23, S67–S74. [Google Scholar]
- Cauda, F.; Cauda, V.; Fiori, C.; Onida, B.; Garrone, E. Heparin coating on uretral double J stents prevents encrustations: An in vivo case study. J. Endourol. 2008, 22, 465–472. [Google Scholar]
- Zdanowski, Z.; Koul, B.; Hallberg, E.; Schalen, C. Influence of heparin coating on in vitro bacterial adherence to poly(vinyl chloride) segments. J. Biomater. Sci. Polym. Ed. 1997, 8, 825–832. [Google Scholar]
- Tang, H.; Cao, T.; Wang, A.; Liang, X.; Salley, S.O.; McAllister, J.P., II; Ng, K.Y.S. Effect of surface modification of silicone on Staphylococcus epidermidis adhesion and colonization. J. Biomed. Mater. Res. 2007, 80A, 885–894. [Google Scholar]
- Andersson, E.; Rydengard, V.; Sonesson, A.; Mörgelin, M.; Björck, L.; Schmidtchen, A. Antimicrobial activities of heparin-binding peptides. Eur. J. Biochem. 2004, 271, 1219–1226. [Google Scholar]
- Malmsten, M.; Davoudi, M.; Schmidtchen, A. Bacterial killing by heparin-binding peptides from PRELP and thrombospondin. Matrix Biol. 2006, 25, 294–300. [Google Scholar]
- Stevens, K.N.J.; Crespo-Biel, O.; van den Bosch, E.E.M.; Dias, A.A.; Knetsch, M.L.W.; Aldenhoff, Y.B.J.; van der Veen, F.H.; maessen, J.G.; Stobberingh, E.E.; Koole, L.H. The relationship between the antimicrobial effect of catheter coatings containing silver nanoparticles and the coagulation of contacting blood. Biomaterials 2009, 30, 3682–3690. [Google Scholar]
- Stevens, K.N.; Knetsch, M.L.; Sen, A.; Sambhy, V.; Koole, L.H. Disruption and activation of blood platelets in contact with an antimicrobial composite coating consisting of a pyridinium polymer and AgBr nanoparticles. ACS Appl. Mater. Interfaces 2009, 1, 2049–2054. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Knetsch, M.L.W.; Koole, L.H. New Strategies in the Development of Antimicrobial Coatings: The Example of Increasing Usage of Silver and Silver Nanoparticles. Polymers 2011, 3, 340-366. https://doi.org/10.3390/polym3010340
Knetsch MLW, Koole LH. New Strategies in the Development of Antimicrobial Coatings: The Example of Increasing Usage of Silver and Silver Nanoparticles. Polymers. 2011; 3(1):340-366. https://doi.org/10.3390/polym3010340
Chicago/Turabian StyleKnetsch, Menno L. W., and Leo H. Koole. 2011. "New Strategies in the Development of Antimicrobial Coatings: The Example of Increasing Usage of Silver and Silver Nanoparticles" Polymers 3, no. 1: 340-366. https://doi.org/10.3390/polym3010340
APA StyleKnetsch, M. L. W., & Koole, L. H. (2011). New Strategies in the Development of Antimicrobial Coatings: The Example of Increasing Usage of Silver and Silver Nanoparticles. Polymers, 3(1), 340-366. https://doi.org/10.3390/polym3010340



