Polydioxanone Membrane Compared with Collagen Membrane for Bone Regeneration
Abstract
1. Introduction
2. Materials and Methods
2.1. Experimental Design
2.2. Animals and Ethics Committee
2.3. Collection and Histological Processing
2.4. Micro-Computed Tomography (micro-CT)
2.5. Real-Time PCR
2.6. Statistical Analysis
3. Results
3.1. Histometric Analysis
3.2. Immunolabeling Analysis
3.3. Real-Time PCR Analysis
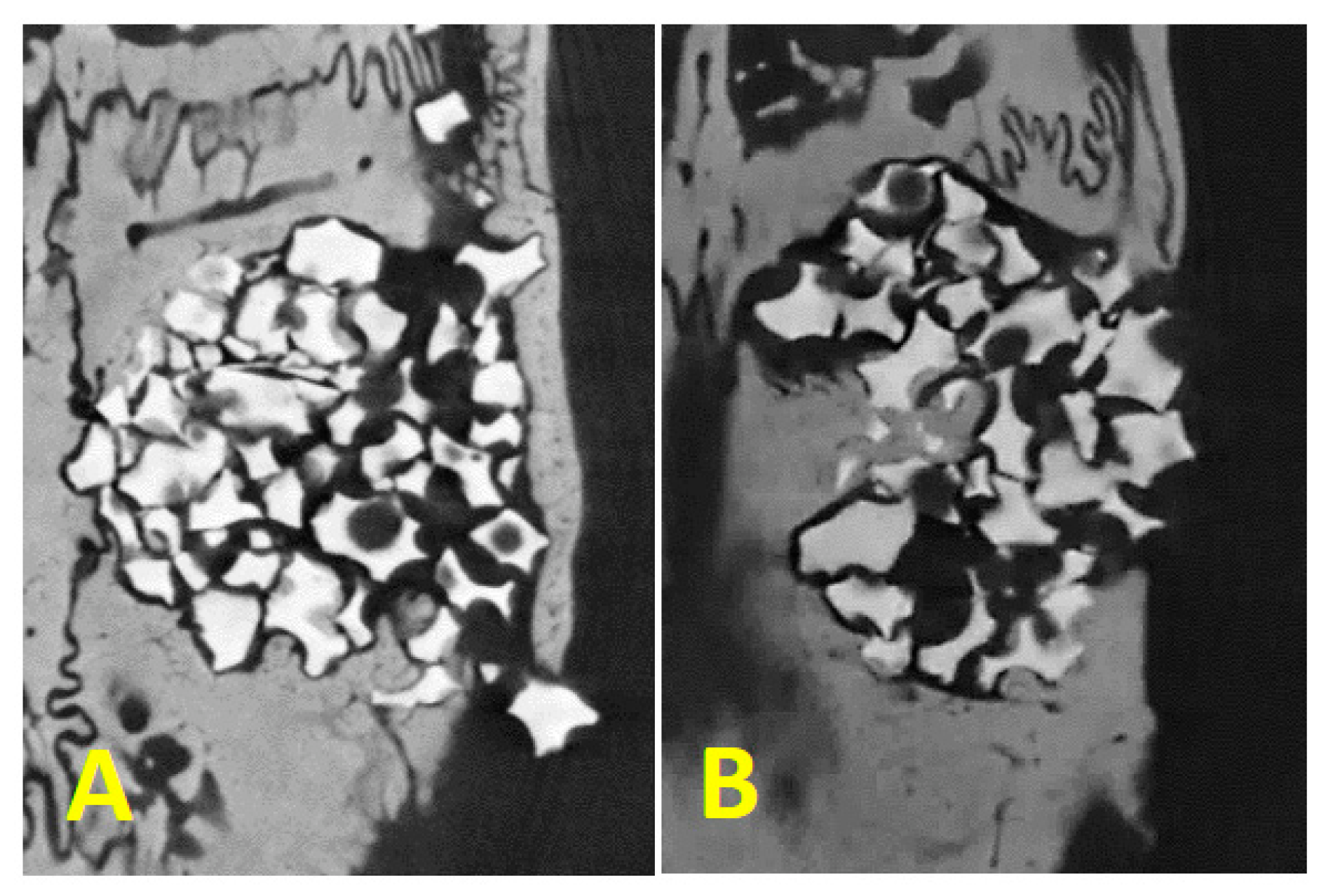
3.4. Micro-CT Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Nyman, S.; Lindhe, J.; Karring, T.; Rylander, H. New attachment following surgical treatment of human periodontal disease. J. Clin. Periodontol. 1982, 9, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Javed, F.; Ahmed, H.B.; Crespi, R.; Romanos, G.E. Role of primary stability for successful osseointegration of dental implants: Factors of influence and evaluation. Interv. Med. Appl. Sci. 2013, 5, 162–167. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.-l.; Boyapati, L. “PASS” Principles for Predictable Bone Regeneration. Implant Dent. 2006, 15, 8–17. [Google Scholar] [CrossRef] [PubMed]
- Juodžbalys, G.; Raustia, A.M.; Kubilius, R. A 5-year follow-up study on one-stage implants inserted concomitantly with localized alveolar ridge augmentation. J. Oral Rehabil. 2007, 34, 781–789. [Google Scholar] [CrossRef]
- Retzepi, M.; Donos, N. Guided Bone Regeneration: Biological principle and therapeutic applications. Clin. Oral Implants Res. 2010, 21, 567–576. [Google Scholar] [CrossRef]
- Elgali, I.; Omar, O.; Dahlin, C.; Thomsen, P. Guided bone regeneration: Materials and biological mechanisms revisited. Eur. J. Oral Sci. 2017, 125, 315–337. [Google Scholar] [CrossRef]
- Soldatos, N.; Stylianou, P.; Koidou, V.; Angelov, N.; Yukna, R.; Romanos, G. Limitations and options using resorbable versus nonresorbable membranes for successful guided bone regeneration. Quintessence Int. 2017, 48, 131–147. [Google Scholar]
- Laurell, L.; Gottlow, J.; Zybutz, M.; Persson, R. Treatment of Intrabony Defects by Different Surgical Procedures. A Literature Review. J. Periodontol. 1998, 69, 303–313. [Google Scholar] [CrossRef]
- Sculean, A.; Schwarz, F.; Chiantella, G.C.; Donos, N.; Arweiler, N.B.; Brecx, M.; Becker, J. Five-year results of a prospective, randomized, controlled study evaluating treatment of intra-bony defects with a natural bone mineral and GTR. J. Clin. Periodontol. 2007, 34, 72–77. [Google Scholar] [CrossRef]
- Kim, Y.-K.; Yun, P.-Y.; Lim, S.-C.; Kim, S.-G.; Lee, H.-J.; Ong, J.L. Clinical evaluations of OSTEON® as a new alloplastic material in sinus bone grafting and its effect on bone healing. J. Biomed. Mater. Res. Part B: Appl. Biomater. 2008, 86B, 270–277. [Google Scholar] [CrossRef]
- Cha, J.-K.; Park, J.-C.; Jung, U.-W.; Kim, C.-S.; Cho, K.-S.; Choi, S.-H. Case series of maxillary sinus augmentation with biphasic calcium phosphate: A clinical and radiographic study. J. Periodontal Implant Sci. 2011, 41, 98–104. [Google Scholar] [CrossRef]
- Güngörmüş, Z.; Güngörmüş, M. Effect of Religious Belief on Selecting of Graft Materials Used in Oral and Maxillofacial Surgery. J. Oral Maxillofac. Surg. 2017, 75, 2347–2353. [Google Scholar] [CrossRef]
- Motta, A.; Duek, E. Síntese, caracterização e degradação "in vitro" do poli(L-ácido láctico-co-ácido glicólico). Matéria. 2006, 11, 340–350. [Google Scholar] [CrossRef]
- Hoornaert, A.; D’Arros, C.; Heymann, M.-F.; Layrolle, P. Biocompatibility, resorption and biofunctionality of a new synthetic biodegradable membrane for guided bone regeneration. Biomed. Mater. 2016, 11, 045012. [Google Scholar] [CrossRef]
- Sabino, A.M.; González, S.; Márquez, L.; Feijoo, J.L. Study of the hydrolytic degradation of polydioxanone PPDX. Polym. Degrad. Stab. 2000, 69, 209–216. [Google Scholar] [CrossRef]
- Nair, L.S.; Laurencin, C.T. Biodegradable polymers as biomaterials. Prog. Polym. Sci. 2007, 32, 762–798. [Google Scholar] [CrossRef]
- Washington, M.A.; Swiner, D.J.; Bell, K.R.; Fedorchak, M.V.; Little, S.R.; Meyer, T.Y. The impact of monomer sequence and stereochemistry on the swelling and erosion of biodegradable poly(lactic-co-glycolic acid) matrices. Biomaterials 2017, 117, 66–76. [Google Scholar] [CrossRef]
- Goonoo, N.; Jeetah, R.; Bhaw-Luximon, A.; Jhurry, D. Polydioxanone-based bio-materials for tissue engineering and drug/gene delivery applications. Eur. J. Pharm. Biopharm. 2015, 97, 371–391. [Google Scholar] [CrossRef]
- Zhao, D.; Zhu, T.; Li, J.; Cui, L.; Zhang, Z.; Zhuang, X.; Ding, J. Poly(lactic-co-glycolic acid)-based composite bone-substitute materials. Bioact. Mater. 2020, 6, 346–360. [Google Scholar] [CrossRef]
- Boland, E.D.; Coleman, B.D.; Barnes, C.P.; Simpson, D.G.; Wnek, G.E.; Bowlin, G.L. Electrospinning polydioxanone for biomedical applications. Acta Biomater. 2005, 1, 115–123. [Google Scholar] [CrossRef]
- Dörfer, C.E.; Kim, T.-S.; Steinbrenner, H.; Holle, R.; Eickholz, P. Regenerative periodontal surgery in interproximal intrabony defects with biodegradable barriers. J. Clin. Periodontol. 2000, 27, 162–168. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.S.; Knittel, M.; Dörfer, C.; Steinbrenner, H.; Holle, R.; Eickholz, P. Comparison of two types of synthetic biodegradable barriers for GTR in interproximal infrabony defects: Clinical and radiographic 24-month results. Int. J. Periodontics Restor. Dent. 2003, 23, 481–489. [Google Scholar] [PubMed]
- Pretzl, B.; Kim, T.-S.; Steinbrenner, H.; Dörfer, C.; Himmer, K.; Eickholz, P. Guided tissue regeneration with bioabsorbable barriers III 10-year results in infrabony defects. J. Clin. Periodontol. 2009, 36, 349–356. [Google Scholar] [CrossRef] [PubMed]
- Lizuka, T.; Mikkonen, P.; Paukku, P.; Lindqvist, C. Reconstruction of orbital floor with polydioxanone plate. Int. J. Oral Maxillofac. Surg. 1991, 20, 83–87. [Google Scholar] [CrossRef] [PubMed]
- Dietz, A.; Ziegler, C.M.; Dacho, A.; Althof, F.; Conradt, C.; Kolling, G.; Boehmer, H.v.; Steffen, H. Effectiveness of a new perforated 0.15 mm poly-p-dioxanon-foil versus titanium-dynamic mesh in reconstruction of the orbital floor. J. -Cranio-Maxillofac. Surg. 2001, 29, 82–88. [Google Scholar] [CrossRef]
- Becker, S.T.; Terheyden, H.; Fabel, M.; Kandzia, C.; Möller, B.; Wiltfang, J. Comparison of Collagen Membranes and Polydioxanone for Reconstruction of the Orbital Floor After Fractures. J. Craniofacial Surg. 2010, 21, 1066–1068. [Google Scholar] [CrossRef]
- Gierloff, M.; Seeck, N.G.K.; Springer, I.; Becker, S.; Kandzia, C.; Wiltfang, J. Orbital Floor Reconstruction With Resorbable Polydioxanone Implants. J. Craniofacial Surg. 2012, 23, 161–164. [Google Scholar] [CrossRef]
- Beck-Broichsitter, B.E.; Acar, C.; Kandzia, C.; Jochens, A.; Wiltfang, J.; Becker, S.T. Reconstruction of the orbital floor with polydioxanone: A long-term clinical survey of up to 12 years. Br. J. Oral Maxillofac. Surg. 2015, 53, 736–740. [Google Scholar] [CrossRef]
- Cohen, M.M., Jr. Perspectives on RUNX genes: An update. Am. J. Med. Genet. A. 2009, 149a, 2629–2646. [Google Scholar] [CrossRef]
- Goldberg, H.A.; Warner, K.J.; Li, M.C.; Hunter, G.K. Binding of Bone Sialoprotein, Osteopontin and Synthetic Polypeptides to Hydroxyapatite. Connect. Tissue Res. 2001, 42, 25–37. [Google Scholar] [CrossRef]
- Li, X.; Chen, S.-L.; Zhu, S.-X.; Zha, G.-Q. Guided bone regeneration using collagen membranes for sinus augmentation. Br. J. Oral Maxillofac. Surg. 2012, 50, 69–73. [Google Scholar] [CrossRef]
- Kämmerer, P.; Palarie, V.; Schiegnitz, E.; Nacu, V.; Draenert, F.; Al-Nawas, B. Influence of a collagen membrane and recombinant platelet-derived growth factor on vertical bone augmentation in implant-fixed deproteinized bovine bone-animal pilot study. Clin. Oral Implants Res. 2013, 24, 1222–1230. [Google Scholar] [CrossRef]
- Stricker, A.; Fleiner, J.; Stübinger, S.; Fleiner, H.; Buser, D.; Bosshardt, D.D. Ridge preservation after ridge expansion with simultaneous guided bone regeneration: A preclinical study. Clin. Oral Implants Res. 2016, 27, e116–e124. [Google Scholar] [CrossRef]
- Izu, Y.; Sun, M.; Zwolanek, D.; Veit, G.; Williams, V.; Cha, B.; Jepsen, K.J.; Koch, M.; Birk, D.E. Type XII collagen regulates osteoblast polarity and communication during bone formation. J. Cell Biol. 2011, 193, 1115–1130. [Google Scholar] [CrossRef]
- Tal, H.; Kozlovsky, A.; Artzi, Z.; Nemcovsky, C.E.; Moses, O. Long-term bio-degradation of cross-linked and non-cross-linked collagen barriers in human guided bone regeneration. Clin. Oral Implants Res. 2008, 19, 295–302. [Google Scholar] [CrossRef]
- Gielkens, P.F.; Schortinghuis, J.; de Jong, J.R.; Raghoebar, G.M.; Stegenga, B.; Bos, R.R. Vivosorb, Bio-Gide, and Gore-Tex as barrier membranes in rat mandibular defects: An evaluation by microradiography and micro-CT. Clin. Oral Implants Res. 2008, 19, 516–521. [Google Scholar] [CrossRef]
- Ferreira, A.M.; Gentile, P.; Chiono, V.; Ciardelli, G. Collagen for bone tissue regeneration. Acta Biomater. 2012, 8, 3191–3200. [Google Scholar] [CrossRef]
- Hu, K.; Olsen, B.R. Osteoblast-derived VEGF regulates osteoblast differentiation and bone formation during bone repair. J. Clin. Investig. 2016, 126, 509–526. [Google Scholar] [CrossRef] [PubMed]
- Mizuno, M.; Imai, T.; Fujisawa, R.; Tani, H.; Kuboki, Y. Bone Sialoprotein (BSP) is a Crucial Factor for the Expression of Osteoblastic Phenotypes of Bone Marrow Cells Cultured on Type I Collagen Matrix. Calcif. Tissue Int. 2000, 66, 388–396. [Google Scholar] [CrossRef]
- Hoogeveen, E.J.; Gielkens, P.F.; Schortinghuis, J.; Ruben, J.L.; Huysmans, M.C.; Stegenga, B. Vivosorb as a barrier membrane in rat mandibular defects. An evaluation with transversal microradiography. Int. J. Oral Maxillofac. Surg. 2009, 38, 870–875. [Google Scholar] [CrossRef]
- Zhang, Y.Y.; Mao, W.J.; Wang, J.; Li, Q.L.; Mei, M.L.; Chu, C.H.; Xia, R.; Zhang, Z.H. Antibacterial Membrane with a Bone-Like Structure for Guided Bone Regeneration. J. Nanomater. 2015, 2015. [Google Scholar] [CrossRef]






| Gene | Gene Name | Identification |
|---|---|---|
| B2M | B2M | Rn00560865_m1 |
| RUNX-2 | RUNX2 | Rn01512298_m1 |
| VEGF | VEGFA | Rn01511602_m1 |
| IBSP | IBSP | Rn00561414_m1 |
| Period (days) | Plenum® Guide + Plenum® Osshp | Bio Gide® + Plenum® Osshp | |
|---|---|---|---|
| Connective Tissue | 15 | 1.63 (0.36)a | 0.86 (0.17)b |
| 30 | 1.32 (0.53)ab | 0.81 (0.2)b | |
| 60 | 0.83 (0.45)b | 0.70 (0.34)b | |
| Newly formed bone tissue | 15 | 0.38 (0.26)a | 0.21 (0.11)a |
| 30 | 0.40 (0.23)a | 0.68 (0.21)a | |
| 60 | 0.60 (0.24)a | 0.65 (0.51)a | |
| Bone graft remaining | 15 | 1.07 (0.4)a | 0.51 (0.08)b |
| 30 | 0.87 (0.36)a | 0.78 (0.26)a | |
| 60 | 0.84 (0.31)a | 0.91 (0.33)a |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Quirino, L.C.; de Azambuja Carvalho, P.H.; Neto, R.T.A.; Comachio, C.A.; Monteiro, N.G.; Ervolino-Silva, A.C.; Okamoto, R.; Pereira-Filho, V.A. Polydioxanone Membrane Compared with Collagen Membrane for Bone Regeneration. Polymers 2023, 15, 868. https://doi.org/10.3390/polym15040868
Quirino LC, de Azambuja Carvalho PH, Neto RTA, Comachio CA, Monteiro NG, Ervolino-Silva AC, Okamoto R, Pereira-Filho VA. Polydioxanone Membrane Compared with Collagen Membrane for Bone Regeneration. Polymers. 2023; 15(4):868. https://doi.org/10.3390/polym15040868
Chicago/Turabian StyleQuirino, Lilian Caldas, Pedro Henrique de Azambuja Carvalho, Renato Torres Augusto Neto, Cássio Amaro Comachio, Naara Gabriela Monteiro, Ana Cláudia Ervolino-Silva, Roberta Okamoto, and Valfrido Antonio Pereira-Filho. 2023. "Polydioxanone Membrane Compared with Collagen Membrane for Bone Regeneration" Polymers 15, no. 4: 868. https://doi.org/10.3390/polym15040868
APA StyleQuirino, L. C., de Azambuja Carvalho, P. H., Neto, R. T. A., Comachio, C. A., Monteiro, N. G., Ervolino-Silva, A. C., Okamoto, R., & Pereira-Filho, V. A. (2023). Polydioxanone Membrane Compared with Collagen Membrane for Bone Regeneration. Polymers, 15(4), 868. https://doi.org/10.3390/polym15040868








