Nano Drug Delivery Platforms for Dental Application: Infection Control and TMJ Management—A Review
Abstract
1. Introduction
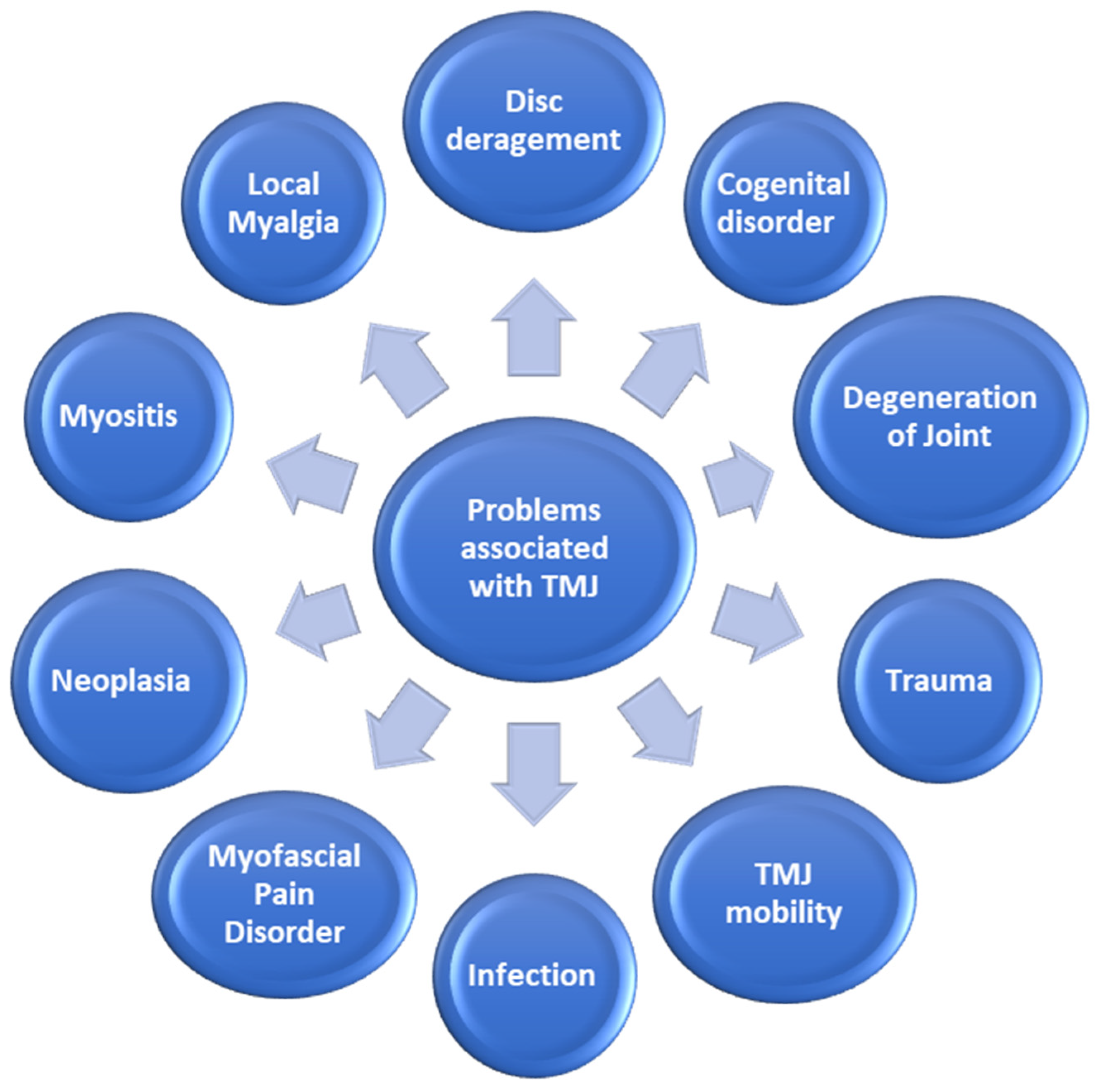
2. Temporomandibular Joint Disorders
2.1. Preventing Cartilage Degeneration of TMJ
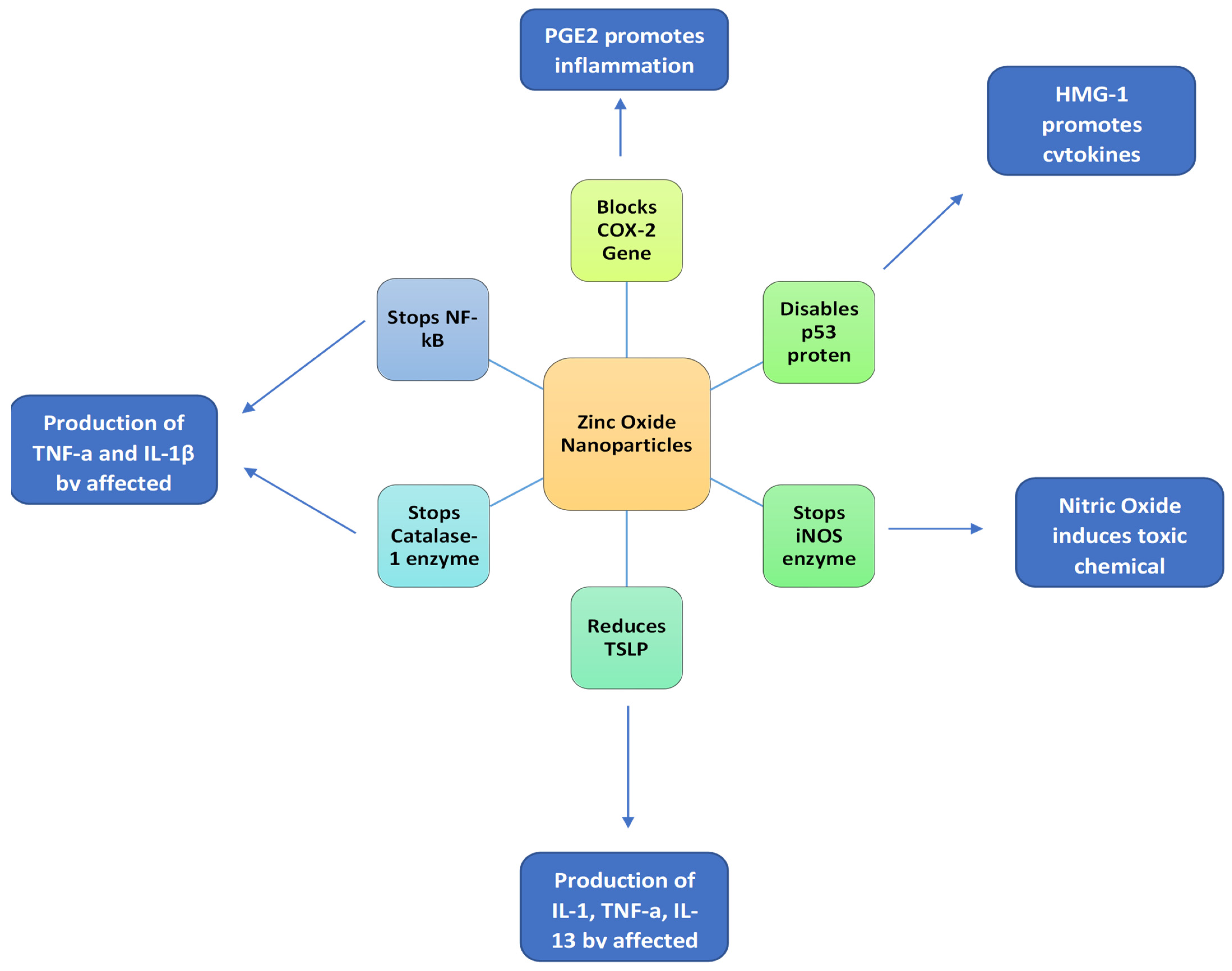
2.2. Anti-Inflammatory Effects
2.3. Anti-Arthritic Efficacy
3. Oral Infections Management
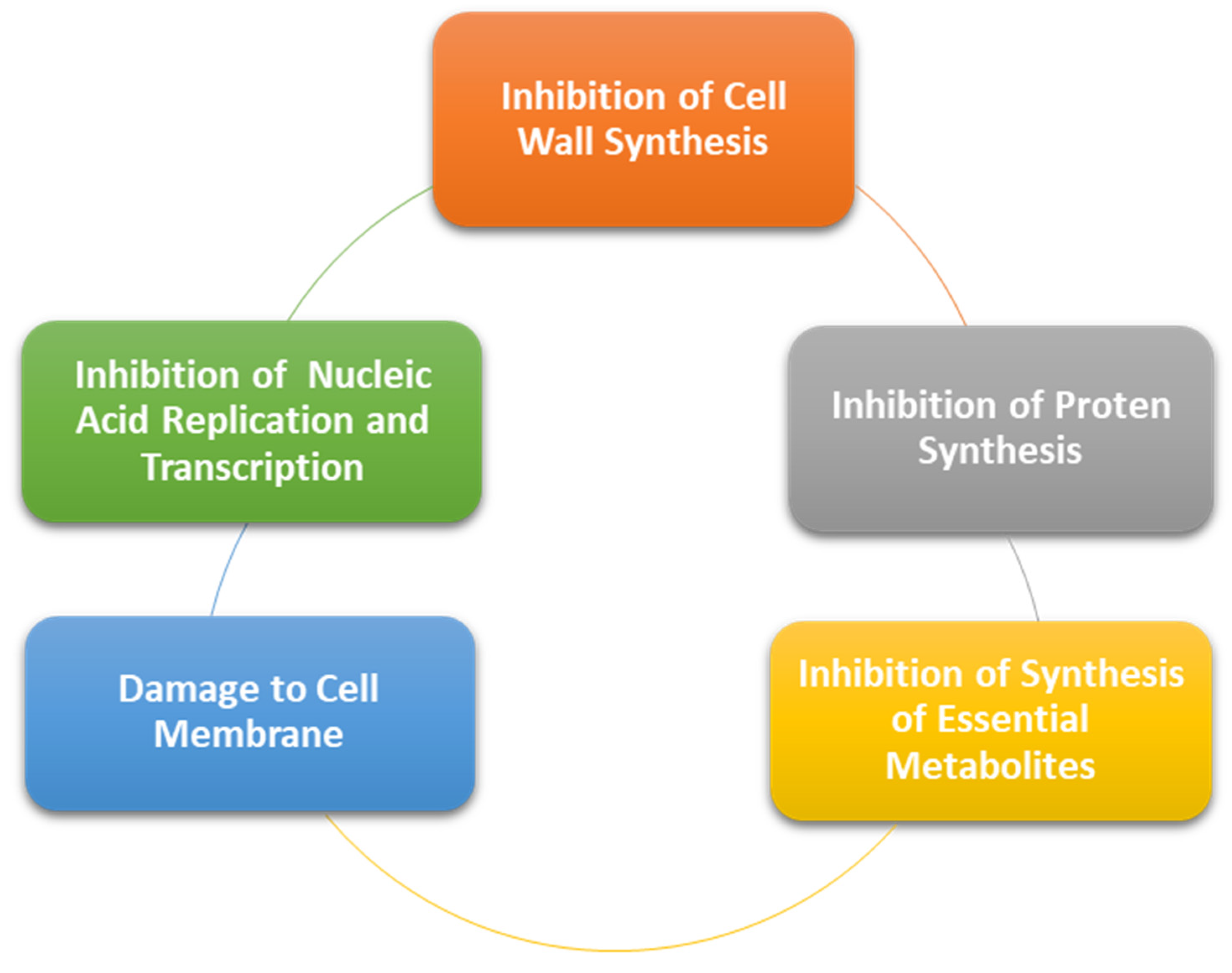
3.1. Antibacterial Effects
3.1.1. Dental Caries
3.1.2. Endodontic Diseases
3.1.3. Periodontal Diseases
3.2. Antifungal Effects
3.3. Anti-Viral Effects
3.3.1. Acyclovir Based Nanoparticles
3.3.2. Chitosan-Based Nanoparticles against Viral Infections
3.3.3. Chloroquine Based Nanoparticles against Viral Infections
3.3.4. Nanoparticles Drug Delivery System against SARS-CoV-2
4. Future Prospective
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Bandara, H.; Samaranayake, L.P. Viral, bacterial, and fungal infections of the oral mucosa: Types, incidence, predisposing factors, diagnostic algorithms, and management. Periodontology 2000 2019, 80, 148–176. [Google Scholar] [CrossRef] [PubMed]
- Maini, K.; Dua, A. Temporomandibular Joint Syndrome; StatPearls Publishing: London, UK, 2021. Available online: http://www.ncbi.nlm.nih.gov/pubmed/31869076 (accessed on 3 November 2021).
- Wen, H.; Jung, H.; Li, X. Drug Delivery Approaches in Addressing Clinical Pharmacology-Related Issues: Opportunities and Challenges. AAPS J. 2015, 17, 1327–1340. [Google Scholar] [CrossRef]
- Wang, L.; Yang, J.; Li, S.; Li, Q.; Liu, S.; Zheng, W.; Jiang, X. Oral Administration of Starting Materials for In Vivo Synthesis of Antibacterial Gold Nanoparticles for Curing Remote Infections. Nano Lett. 2021, 21, 1124–1131. [Google Scholar] [CrossRef]
- Ochubiojo, M.; Chinwude, I.; Ibanga, E.; Ifianyi, S. Nanotechnology in Drug Delivery. In Recent Advances in Novel Drug Carrier Systems; InTech: London, UK, 2012; Available online: http://www.intechopen.com/books/recent-advances-in-novel-drug-carrier-systems/nanotechnology-in-drug-delivery (accessed on 1 November 2021).
- Kothamasu, P.; Kanumur, H.; Ravur, N.; Maddu, C.; Parasuramrajam, R.; Thangavel, S. Nanocapsules: The Weapons for Novel Drug Delivery Systems. BioImpacts 2012, 2, 71–81. [Google Scholar] [CrossRef]
- McMillan, J.; Batrakova, E.; Gendelman, H.E. Cell Delivery of Therapeutic Nanoparticles. Prog. Mol. Biol. Transl. Sci. 2011, 104, 563–601. [Google Scholar] [CrossRef] [PubMed]
- Bharti, C.; Gulati, N.; Nagaich, U.; Pal, A. Mesoporous silica nanoparticles in target drug delivery system: A review. Int. J. Pharm. Investig. 2015, 5, 124–133. [Google Scholar] [CrossRef]
- Nomoev, A.V.; Bardakhanov, S.P.; Schreiber, M.; Bazarova, D.G.; Romanov, N.A.; Baldanov, B.B.; Radnaev, B.R.; Syzrantsev, V.V. Structure and mechanism of the formation of core–shell nanoparticles obtained through a one-step gas-phase synthesis by electron beam evaporation. Beilstein J. Nanotechnol. 2015, 6, 874–880. Available online: https://www.beilstein-journals.org/bjnano/articles/6/89 (accessed on 16 October 2021). [CrossRef]
- Khan, I.; Saeed, K.; Khan, I. Nanoparticles: Properties, applications and toxicities. Arab. J. Chem. 2019, 12, 908–931. Available online: https://linkinghub.elsevier.com/retrieve/pii/S1878535217300990 (accessed on 25 October 2021). [CrossRef]
- Rokaya, D.; Srimaneepong, V.; Sapkota, J.; Qin, J.; Siraleartmukul, K.; Siriwongrungson, V. Polymeric materials and films in dentistry: An overview. J. Adv. Res. 2018, 14, 25–34. [Google Scholar] [CrossRef]
- Dannert, C.; Stokke, B.T.; Dias, R.S. Nanoparticle-Hydrogel Composites: From Molecular Interactions to Macroscopic Behavior. Polymers 2019, 11, 275. Available online: https://www.mdpi.com/2073-4360/11/2/275 (accessed on 23 October 2021). [CrossRef]
- Shan, X.; Liu, C.; Li, F.; Ouyang, C.; Gao, Q.; Zheng, K. Nanoparticles vs. nanofibers: A comparison of two drug delivery systems on assessing drug release performance in vitro. Des. Monomers Polym. 2015, 18, 678–689. [Google Scholar] [CrossRef]
- Thomas, R.; Snigdha, S.; Bhavitha, K.B.; Babu, S.; Ajith, A.; Radhakrishnan, E.K. Biofabricated silver nanoparticles incorporated polymethyl methacrylate as a dental adhesive material with antibacterial and antibiofilm activity against Streptococcus mutans. Biotech 2018, 8, 404. [Google Scholar] [CrossRef] [PubMed]
- Commisso, M.S.; Ojeda, J.; Mayo, J.; Martínez-Reina, J. Influence of the Temporomandibular Joint in the Estimation of Bone Density in the Mandible through a Bone Remodelling Model. Math. Probl. Eng. 2018, 2018, 1–14. [Google Scholar] [CrossRef]
- Bordoni, B.; Varacallo, M. Anatomy, Head and Neck, Temporomandibular Joint; StatPearls Publishing: Treasure Island, FL, USA, 2021. Available online: http://www.ncbi.nlm.nih.gov/pubmed/30860721 (accessed on 16 October 2021).
- Shim, J.S.; Kim, C.; Ryu, J.J.; Choi, S.J. Correlation between TM joint disease and rheumatic diseases detected on bone scintigra-phy and clinical factors. Sci. Rep. 2020, 10, 4547. [Google Scholar] [CrossRef]
- Kalladka, M.; Quek, S.; Heir, G.; Eliav, E.; Mupparapu, M.; Viswanath, A. Temporomandibular Joint Osteoarthritis: Diagnosis and Long-Term Conservative Management: A Topic Review. J. Indian Prosthodont. Soc. 2014, 14, 6–15. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, E.; Detamore, M.; Mercuri, L. Degenerative Disorders of the Temporomandibular Joint: Etiology, Diagnosis, and Treatment. J. Dent. Res. 2008, 87, 296–307. [Google Scholar] [CrossRef]
- Srivastava, K.C.; Shrivastava, D.; Khan, Z.A.; Nagarajappa, A.K.; Mousa, M.A.; Hamza, M.O.; Al-Johani, K.; Alam, M.K. Evaluation of temporomandibular disorders among dental students of Saudi Arabia using Diagnostic Criteria for Temporomandibular Disorders (DC/TMD): A cross-sectional study. BMC Oral Health. 2021, 21, 211. [Google Scholar] [CrossRef]
- Wang, X.; Zhang, J.; Gan, Y.; Zhou, Y. Current Understanding of Pathogenesis and Treatment of TMJ Osteoarthritis. J. Dent. Res. 2015, 94, 666–673. [Google Scholar] [CrossRef]
- Cui, D.; Li, H.; Xu, X.; Zheng, L.; Zhou, Y. Mesenchymal Stem Cells for Cartilage Regeneration of TMJ Osteoarthri-tis. Stem Cells Int. 2017, 2017, 1–11. Available online: https://www.hindawi.com/journals/sci/2017/5979741/ (accessed on 29 October 2021). [CrossRef]
- Makadia, H.K.; Siegel, S.J. Poly lactic-co-glycolic acid (PLGA) As biodegradable controlled drug delivery carrier. Polymers 2011, 3, 1377–1397. [Google Scholar] [CrossRef]
- Zille, H.; Paquet, J.; Henrionnet, C.; Scala-Bertola, J.; Leonard, M.; Six, J.L.; Deschamp, F.; Netter, P.; Vergès, J.; Gillet, P.; et al. Evaluation of intra-articular delivery of hyaluronic acid functionalized biopolymeric nanoparticles in healthy rat knees. Bio-Medical Mater. Eng. 2010, 20, 235–242. [Google Scholar] [CrossRef]
- Lu, H.-D.; Zhao, H.-Q.; Wang, K.; Lv, L.-L. Novel hyaluronic acid–chitosan nanoparticles as non-viral gene delivery vectors tar-geting osteoarthritis. Int. J. Pharm. 2011, 420, 358–365. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0378517311008179 (accessed on 16 October 2021). [CrossRef]
- Ponnurangam, S.; O’Connell, G.D.; Chernyshova, I.V.; Wood, K.; Hung, C.T.-H.; Somasundaran, P. Beneficial Effects of Cerium Oxide Nanoparticles in Development of Chondrocyte-Seeded Hydrogel Constructs and Cellular Response to Interleukin Insults. Tissue Eng. Part A 2014, 20, 2908–2919. [Google Scholar] [CrossRef]
- Ong, C.; Lirk, P.; Tan, C.; Seymour, R. An Evidence-Based Update on Nonsteroidal Anti-Inflammatory Drugs. Clin. Med. Res. 2007, 5, 19–34. [Google Scholar] [CrossRef]
- Barry, F.; Chai, F.; Chijcheapaza-Flores, H.; Garcia-Fernandez, M.J.; Blanchemain, N.; Nicot, R. Systematic review of studies on drug-delivery systems for management of temporomandibular-joint osteoarthritis. J. Stomatol. Oral Maxillofac. Surg. 2021. [Google Scholar] [CrossRef] [PubMed]
- Iannitti, T.; Lodi, D.; Palmieri, B. Intra-Articular Injections for the Treatment of Osteoarthritis. Drugs 2011, 11, 13–27. [Google Scholar] [CrossRef] [PubMed]
- De Jong, W.; Borm, P.J.A. Drug delivery and nanoparticles: Applications and hazards. Int. J. Nanomed. 2008, 2008, 133. Available online: http://www.dovepress.com/drug-delivery-and-nanoparticles-applications-and-hazards-peer-reviewed-article-IJN (accessed on 23 October 2021). [CrossRef] [PubMed]
- Shinde, C.G.; Kumar, T.M.P.; Venkatesh, M.P.; Rajesh, K.S.; Srivastava, A.; Osmani, R.A.M.; Sonawane, Y.H. Intra-articular delivery of a methotrexate loaded nanostructured lipid carrier based smart gel for effective treatment of rheumatic diseases. RSC Adv. 2016, 6, 12913–12924. [Google Scholar] [CrossRef]
- Dyondi, D.; Sarkar, A.; Banerjee, R. Joint Surface-Active Phospholipid-Mimetic Liposomes for Intra-Articular Delivery of Paclitaxel. J. Biomed. Nanotechnol. 2015, 11, 1225–1235. [Google Scholar] [CrossRef]
- Pivetta, T.P.; Simões, S.; Araújo, M.M.; Carvalho, T.; Arruda, C.; Marcato, P.D. Development of nanoparticles from natural lipids for topical delivery of thymol: Investigation of its anti-inflammatory properties. Colloids Surf. B Biointerfaces 2018, 164, 281–290. [Google Scholar] [CrossRef]
- Guilherme, V.A.; Ribeiro, L.N.M.; Bonfante, R.; Cereda, C.M.S.; de Paula, E.; Alcântara, A.C.S.; Castro, S.R.; da Silva, G.H.R.; Da Silva, C.G.; Breitkreitz, M.C.; et al. Improved efficacy of naproxen-loaded NLC for temporomandibular joint administration. Sci. Rep. 2019, 9, 11160. [Google Scholar] [CrossRef]
- Hoscheid, J.; Outuki, P.M.; Kleinubing, S.A.; Silva, M.F.; Bruschi, M.L.; Cardoso, M.L.C. Development and characterization of Pterodon pubescens oil nanoemulsions as a possible delivery system for the treatment of rheumatoid arthritis. Colloids Surf. A Physicochem. Eng. Asp. 2015, 484, 19–27. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0927775715301199 (accessed on 26 October 2021). [CrossRef]
- Rao, K.; Aziz, S.; Roome, T.; Razzak, A.; Sikandar, B.; Jamali, K.S.; Imran, M.; Jabri, T.; Shah, M.R. Gum acacia stabilized silver nanoparticles based nano-cargo for enhanced anti-arthritic potentials of hesperidin in adjuvant induced arthritic rats. Artif. Cells Nanomed. Biotechnol. 2018, 46, 597–607. [Google Scholar] [CrossRef]
- Cui, P.; Qu, F.; Sreeharsha, N.; Sharma, S.; Mishra, A.; Gubbiyappa, S.K. Antiarthritic effect of chitosan nanoparticle loaded with embelin against adjuvant-induced arthritis in Wistar rats. IUBMB Life 2020, 72, 1054–1064. [Google Scholar] [CrossRef] [PubMed]
- Shrivastava, D.; Natoli, V.; Srivastava, K.C.; Alzoubi, I.A.; Nagy, A.I.; Hamza, M.O.; Al-Johani, K.; Alam, M.K.; Khurshid, Z. Novel Approach to Dental Biofilm Management through Guided Biofilm Therapy (GBT): A Review. Microorganisms 2021, 9, 1966. [Google Scholar] [CrossRef] [PubMed]
- Rathee, M.; Sapra, A. Dental Caries; StatPearls Publishing: Treasure Island, FL, USA, 2021. Available online: http://www.ncbi.nlm.nih.gov/pubmed/31869163 (accessed on 26 October 2021).
- Nimbulkar, G.; Garacha, v.; Shetty, V.; Bhor, K.; Srivastava, K.C.; Shrivastava, D.; Sghaireen, M.G. Microbiological and Clinical evaluation of Neem gel and Chlorhexidine gel on dental plaque and gingivitis in 20–30 years old adults: A Randomized Parallel-Armed, Double-blinded Controlled Trial. J. Pharm. Bioallied Sci. 2020, 12 (Suppl. 1), S345. [Google Scholar]
- Shrivastava, D.; Srivastava, K.C.; Ganji, K.K.; Alam, M.K.; Al Zoubi, I.; Sghaireen, M.G. Quantitative Assessment of Gingival Inflammation in Patients Undergoing Nonsurgical Periodontal Therapy Using Photometric CIELab Analysis. BioMed Res. International 2021, 2021, 6615603. [Google Scholar] [CrossRef]
- Horst, J.A.; Tanzer, J.M.; Milgrom, P.M. Fluorides and Other Preventive Strategies for Tooth Decay. Dent. Clin. N. Am. 2018, 62, 207–234. [Google Scholar] [CrossRef] [PubMed]
- Sondi, I.; Salopek-Sondi, B. Silver nanoparticles as antimicrobial agent: A case study on E. coli as a model for Gram-negative bacteria. J. Colloid Interface Sci. 2004, 275, 177–182. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0021979704001638 (accessed on 3 November 2021). [CrossRef]
- Cioffi, N.; Torsi, L.; Ditaranto, N.; Tantillo, G.; Ghibelli, L.; Sabbatini, L.; Bleve-Zacheo, T.; D’Alessio, M.; Zambonin, A.P.G.; Travers, E. Copper Nanoparticle/Polymer Composites with Antifungal and Bacteriostatic Properties. Chem. Mater. 2005, 17, 5255–5262. [Google Scholar] [CrossRef]
- Wang, L.; Hu, C.; Shao, L. The antimicrobial activity of nanoparticles: Present situation and prospects for the future. Int. J. Nanomed. 2017, 12, 1227–1249. Available online: https://www.dovepress.com/the-antimicrobial-activity-of-nanoparticles-present-situation-and-pros-peer-reviewed-article-IJN (accessed on 26 October 2021). [CrossRef] [PubMed]
- Park, H.-J.; Park, S.; Roh, J.; Kim, S.; Choi, K.; Yi, J.; Kim, Y.; Yoon, J. Biofilm-inactivating activity of silver nanoparticles: A comparison with silver ions. J. Ind. Eng. Chem. 2012, 19, 614–619. [Google Scholar] [CrossRef]
- Sotiriou, G.A.; Pratsinis, S.E. Antibacterial Activity of Nanosilver Ions and Particles. Environ. Sci. Technol. 2010, 44, 5649–5654. [Google Scholar] [CrossRef]
- Peng, J.J.-Y.; Botelho, M.G.; Matinlinna, J. Silver compounds used in dentistry for caries management: A review. J. Dent. 2012, 40, 531–541. [Google Scholar] [CrossRef]
- Durner, J.; Stojanovic, M.; Urcan, E.; Hickel, R.; Reichl, F.-X. Influence of silver nano-particles on monomer elution from light-cured composites. Dent. Mater. 2011, 27, 631–636. [Google Scholar] [CrossRef] [PubMed]
- Boldyryeva, H.; Umeda, N.; Plaksin, O.; Takeda, Y.; Kishimoto, N. High-fluence implantation of negative metal ions into polymers for surface modification and nanoparticle formation. Surf. Coatings Technol. 2005, 196, 373–377. [Google Scholar] [CrossRef]
- Ren, G.; Hu, D.; Cheng, E.W.C.; Vargas-Reus, M.A.; Reip, P.; Allaker, R.P. Characterisation of copper oxide nanoparticles for anti-microbial applications. Int. J. Antimicrob. Agents 2009, 33, 587–590. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0924857909000041 (accessed on 16 October 2021). [CrossRef]
- Cheng, L.; Weir, M.D.; Xu, H.H.K.; Antonucci, J.M.; Kraigsley, A.M.; Lin, N.J.; Lin-Gibson, S.; Zhou, X. Antibacterial amorphous calcium phosphate nano-composites with a quaternary ammonium dimethacrylate and silver nanoparticles. Dent. Mater. 2012, 28, 561–572. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0109564112000176 (accessed on 16 October 2021). [CrossRef]
- Cheng, L.; Weir, M.D.; Xu, H.H.K.; Antonucci, J.M.; Lin, N.J.; Lin-Gibson, S.; Xu, S.M.; Zhou, X. Effect of amorphous calcium phosphate and silver nanocomposites on dental plaque microcosm biofilms. J. Biomed. Mater. Res. Part B Appl. Biomater. 2012, 100B, 1378–1386. [Google Scholar] [CrossRef]
- Damm, C.; Münstedt, H.; Rösch, A. Long-term antimicrobial polyamide 6/silver-nanocomposites. J. Mater. Sci. 2007, 42, 6067–6073. [Google Scholar] [CrossRef]
- Teja, K.V.; Janani, K.; Srivastava, K.C.; Shrivastava, D.; Jose, J.; Marya, A.; Karobari, M.I. Comparison of Herbal Agents with Sodium Hypochlorite as Root Canal Irrigant: A Systematic Review of In Vitro Studies. Evid. Based Complementary Altern. Med. 2021, 2021, 8967219. [Google Scholar] [CrossRef]
- Raura, N.; Garg, A.; Arora, A.; Roma, M. Nanoparticle technology and its implications in endodontics: A review. Biomater. Res. 2020, 24, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Afkhami, F.; Akbari, S.; Chiniforush, N. Entrococcus faecalis Elimination in Root Canals Using Silver Nanoparticles, Photodynamic Therapy, Diode Laser, or Laser-activated Nanoparticles: An In Vitro Study. J. Endod. 2017, 43, 279–282. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.-K.; Kim, S.V.; Limansubroto, A.N.; Yen, A.; Soundia, A.; Wang, C.-Y.; Shi, W.; Hong, C.; Tetradis, S.; Kim, Y.; et al. Nanodiamond–Gutta Percha Composite Biomaterials for Root Canal Therapy. ACS Nano 2015, 9, 11490–11501. [Google Scholar] [CrossRef]
- Kishen, A.; Shi, Z.; Shrestha, A.; Neoh, K.G. An Investigation on the Antibacterial and Antibiofilm Efficacy of Cationic Nanopar-ticulates for Root Canal Disinfection. J. Endod. 2008, 34, 1515–1520. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0099239908007991 (accessed on 16 October 2021). [CrossRef]
- Del Carpio-Perochena, A.; Kishen, A.; Shrestha, A.; Bramante, C.M. Antibacterial Properties Associated with Chitosan Nanopar-ticle Treatment on Root Dentin and 2 Types of Endodontic Sealers. J. Endod. 2015, 41, 1353–1358. Available online: https://linkinghub.elsevier.com/retrieve/pii/S0099239915003015 (accessed on 28 October 2021). [CrossRef]
- Pagonis, T.C.; Chen, J.; Fontana, C.R.; Devalapally, H.; Ruggiero, K.; Song, X.; Foschi, F.; Dunham, J.; Skobe, Z.; Yamazaki, H. Nanoparticle-based Endodontic Antimicrobial Photodynamic Therapy. J. Endod. 2010, 36, 322–328. [Google Scholar] [CrossRef]
- Pramod, K.; Alex, M.R.A.; Singh, M.; Dang, S.; Ansari, S.H.; Ali, J. Eugenol nanocapsule for enhanced therapeutic activity against periodontal infections. J. Drug Target. 2016, 24, 24–33. [Google Scholar] [CrossRef]
- Takahashi, C.; Hattori, Y.; Yagi, S.; Murai, T.; Tanemura, M.; Kawashima, Y.; Yamamoto, H. Ionic liquid-incorporated polymeric nanoparti-cles as carriers for prevention and at an earlier stage of periodontal disease. Materialia 2019, 8, 100395. Available online: https://linkinghub.elsevier.com/retrieve/pii/S2589152919301917 (accessed on 16 October 2021). [CrossRef]
- Pang, Z.; Xu, P.; Zhao, J.; Cheng, N.; Chai, Z.; Yang, Z.; Li, H.; Jiang, M.; Zhang, B.; Cheng, H.; et al. Local delivery of minocycline-loaded PEG-PLA nanoparticles for the enhanced treatment of periodontitis in dogs. Int. J. Nanomed. 2014, 9, 3963–3970. [Google Scholar] [CrossRef]
- Hayakumo, S.; Arakawa, S.; Mano, Y.; Izumi, Y. Clinical and microbiological effects of ozone nano-bubble water irrigation as an adjunct to mechanical subgingival debridement in periodontitis patients in a randomized controlled trial. Clin. Oral Investig. 2013, 17, 379–388. [Google Scholar] [CrossRef]
- Shinwari, M.S.; Tanwir, F.; Hyder, P.R.; Bin Saeed, M.H. Host modulation therapeutics in periodontics: Role as an adjunctive periodontal therapy. J. Coll. Phys. Surg. Pak. 2014, 24, 676–684. Available online: http://www.ncbi.nlm.nih.gov/pubmed/25233975 (accessed on 16 October 2021).
- Cafferata, E.A.; Alvarez, C.; Diaz, K.T.; Maureira, M.; Monasterio, G.; González, F.E.; Covarrubias, C.; Vernal, R. Multifunctional nanocarriers for the treatment of periodontitis: Immunomodulatory, antimicrobial, and regenerative strategies. Oral Dis. 2019, 25, 1866–1878. [Google Scholar] [CrossRef] [PubMed]
- Amelia Piñón Castillo, H.; Nayzzel Muñoz Castellanos, L.; Martínez Chamorro, R.; Reyes Martínez, R.; Orrantia Borunda, E. Nanoparticles as New Therapeutic Agents against Candida albicans. In Candida Albicans; InTech: London, UK, 2019; Available online: https://www.intechopen.com/books/candida-albicans/nanoparticles-as-new-therapeutic-agents-against-candida-albicans (accessed on 23 October 2021).
- Arzate-Quintana, C.; Sánchez-Ramírez, B.; Infante-Ramírez, R.; Pinon-Castillo, H.; Duarte-Moller, J.A.; Luna, A.; Erasmo, O.-B.; Montes-Fonseca, S.K.; Javier Solis-Martinez, F. Toxicity Effects in Pathogen Microorganisms Exposed to Silver Nanoparticles. Nanosci. Nanotechnol. Lett. 2017, 9, 165–173. [Google Scholar] [CrossRef]
- Corrêa, J.M.; Mori, M.; Sanches, H.L.; Cruz, A.; Poiate, E.; Poiate, I.A.V.P. Silver Nanoparticles in Dental Biomaterials. Int. J. Biomater. 2015, 2015, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Khatoon, N.; Sharma, Y.; Sardar, M.; Manzoor, N. Mode of action and anti-Candida activity of Artemisia annua mediated-synthesized silver nanoparticles. J. De Mycol. Med. 2019, 29, 201–209. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, M.A.; Ebrahim, M.I. Effect of Zirconium Oxide Nano-Fillers Addition on the Flexural Strength, Fracture Toughness, and Hardness of Heat-Polymerized Acrylic Resin. World J. Nano Sci. Eng. 2014, 04, 50–57. [Google Scholar] [CrossRef]
- Gowri, S.; Rajiv Gandhi, R.; Sundrarajan, M. Structural, Optical, Antibacterial and Antifungal Properties of Zirconia Nanopar-ticles by Biobased Protocol. J. Mater. Sci. Technol. 2014, 30, 782–790. Available online: https://linkinghub.elsevier.com/retrieve/pii/S1005030214000292 (accessed on 16 October 2021). [CrossRef]
- Al, H.M. Fluconazole Nanoparticles Loaded Gel for Improved Efficacy in Treatment of Oral Candidiasis. Int. J. Pharmacol. 2019, 15, 436–440. [Google Scholar] [CrossRef]
- Roque, L.; Castro, P.; Molpeceres, J.; Viana, A.S.; Roberto, A.; Reis, C.; Rijo, P.; Tho, I.; Sarmento, B.; Reis, C. Bioadhesive polymeric nanoparticles as strategy to improve the treatment of yeast infections in oral cavity: In vitro and ex vivo studies. Eur. Polym. J. 2018, 104, 19–31. [Google Scholar] [CrossRef]
- Hassan, H.; Adam, S.K.; Othman, F.; Shamsuddin, A.F.; Basir, R. Antiviral Nanodelivery Systems: Current Trends in Acyclovir Administration. J. Nanomater. 2016, 2016, 1–8. [Google Scholar] [CrossRef]
- Patel, D.; Sawant, K.K. Oral Bioavailability Enhancement of Acyclovir by Self-Microemulsifying Drug Delivery Systems (SMEDDS). Drug Dev. Ind. Pharm. 2007, 33, 1318–1326. [Google Scholar] [CrossRef] [PubMed]
- Tang, X.C.; Nail, S.L.; Pikal, M.J. Evaluation of manometric temperature measurement, a process analytical technology tool for freeze-drying: Part II: Measurement of dry-layer resistance. AAPS PharmSciTech 2006, 7, E77–E84. [Google Scholar] [CrossRef] [PubMed]
- Gandhi, A.; Jana, S.; Sen, K.K. In-vitro release of acyclovir loaded Eudragit RLPO® nanoparticles for sustained drug delivery. Int. J. Biol. Macromol. 2014, 67, 478–482. [Google Scholar] [CrossRef]
- Senel, S.; Gurkan, A.; Erkek, N. Localized bullous eruptions away from infusion site due to intravenous acyclovir admin-istration in a child. Indian J. Pharmacol. 2012, 44, 126. Available online: http://www.ijp-online.com/text.asp?2012/44/1/126/91885 (accessed on 16 October 2021). [CrossRef] [PubMed]
- Fleischer, R.; Johnson, M. Acyclovir Nephrotoxicity: A Case Report Highlighting the Importance of Prevention, Detection, and Treatment of Acyclovir-Induced Nephropathy. Case Rep. Med. 2010, 2010, 1–3. [Google Scholar] [CrossRef]
- Kamel, A.O.; Awad, G.A.S.; Geneidi, A.S.; Mortada, N.D. Preparation of Intravenous Stealthy Acyclovir Nanoparticles with Increased Mean Residence Time. AAPS Pharm. Sci. Tech. 2009, 10, 1427–1436. [Google Scholar] [CrossRef][Green Version]
- Gupta, S.; Agarwal, A.; Gupta, N.K.; Saraogi, G.; Agrawal, H.; Agrawal, G.P. Galactose decorated PLGA nanoparticles for hepatic delivery of acyclovir. Drug Dev. Ind. Pharm. 2013, 39, 1866–1873. [Google Scholar] [CrossRef]
- Illum, L. Chitosan and its use as a pharmaceutical excipient. Pharm. Res. 1998, 15, 1326–1331. Available online: http://www.ncbi.nlm.nih.gov/pubmed/9755881 (accessed on 16 October 2021). [CrossRef]
- Hu, L.; Sun, Y.; Wu, Y. Advances in chitosan-based drug delivery vehicles. Nanoscale 2013, 5, 3103–3111. [Google Scholar] [CrossRef]
- Donalisio, M.; Leone, F.; Civra, A.; Spagnolo, R.; Özer, Ö.; Lembo, D.; Cavalli, R. Acyclovir-Loaded Chitosan Nanospheres from Nano-Emulsion Templating for the Topical Treatment of Herpesviruses Infections. Pharmaceutics 2018, 10, 46. [Google Scholar] [CrossRef] [PubMed]
- Shibata, Y.; A. Foster, L.; Metzger, W.J.; Myrvik, Q.N. Alveolar macrophage priming by intravenous administration of chitin particles, polymers of N-acetyl-D-glucosamine, in mice. Infect. Immun. 1997, 65, 1734–1741. [Google Scholar] [CrossRef] [PubMed]
- Chirkov, S.N. The Antiviral Activity of Chitosan (Review). Appl. Biochem. Microbiol. 2002, 38, 1–8. [Google Scholar] [CrossRef]
- Ahmad, M.Z.; Akhter, S.; Jain, G.K.; Rahman, M.; Pathan, S.A.; Ahmad, F.J.; Khar, R.K. Metallic nanoparticles: Technology overview & drug delivery applications in oncology. Expert Opin. Drug Deliv. 2010, 7, 927–942. [Google Scholar] [CrossRef]
- Pelt, J.; Busatto, S.; Ferrari, M.; Thompson, E.A.; Mody, K.; Wolfram, J. Chloroquine and nanoparticle drug delivery: A promising combination. Pharmacol. Ther. 2018, 191, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Lima, T.; Feitosa, R.; dos Santos-Silva, E.; dos Santos-Silva, A.; Siqueira, E.; Machado, P.; Maira Cornelio, A.; Socrates Tabosa Do Egito, E.; de Freitas Fernandes-Pedrosa, M.; Juvenal Silva Farias, K.; et al. Improving Encapsulation of Hy-drophilic Chloroquine Diphosphate into Biodegradable Nanoparticles: A Promising Approach against Herpes Virus Simplex-1 Infection. Pharmaceutics 2018, 10, 255. Available online: https://www.mdpi.com/1999-4923/10/4/255 (accessed on 16 October 2021). [CrossRef]
- Chakravarty, M.; Vora, A. Nanotechnology-based antiviral therapeutics. Drug Deliv. Transl. Res. 2021, 11, 748–787. [Google Scholar] [CrossRef]
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A Novel Coronavirus from Patients with Pneumonia in China, 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef]
- Pandey, P.; Gulati, N.; Makhija, M.; Purohit, D.; Dureja, H. Nanoemulsion: A Novel Drug Delivery Approach for Enhancement of Bioavailability. Recent Patents Nanotechnol. 2020, 14, 276–293. [Google Scholar] [CrossRef]
- Franklyne, J.S.; Gopinath, P.M.; Mukherjee, A.; Chandrasekaran, N. Nanoemulsions: The rising star of antiviral therapeutics and nanodelivery system—Current status and prospects. Curr. Opin. Colloid Interface Sci. 2021, 54, 101458. [Google Scholar] [CrossRef]
- Khatir, N.M.; Abdul-Malek, Z.; Zak, A.K.; Akbari, A.; Sabbagh, F. Sol–gel grown Fe-doped ZnO nanoparticles: An-tibacterial and structural behaviors. J. Sol Gel Sci. Technol. 2016, 78, 91–98. [Google Scholar] [CrossRef]
- Astani, A.; Reichling, J.; Schnitzler, P. Comparative study on the antiviral activity of selected monoterpenes derived from essential oils. Phytotherapy Res. 2010, 24, 673–679. [Google Scholar] [CrossRef] [PubMed]
- Pandita, D.; Poonia, N.; Kumar, S.; Lather, V.; Madaan, K. Dendrimers in drug delivery and targeting: Drug-dendrimer interactions and toxicity issues. J. Pharm. Bioallied Sci. 2014, 6, 139–150. [Google Scholar] [CrossRef] [PubMed]
- Wang, F.; Cai, X.; Su, Y.; Hu, J.; Wu, Q.; Zhang, H.; Xiao, J.; Cheng, Y. Reducing cytotoxicity while improving anti-cancer drug loading capaci-ty of polypropylenimine dendrimers by surface acetylation. Acta Biomater. 2012, 8, 4304–4313. Available online: https://linkinghub.elsevier.com/retrieve/pii/S1742706112003509 (accessed on 16 October 2021). [CrossRef]
- Itani, R.; Tobaiqy, M.; Al Faraj, A. Optimizing use of theranostic nanoparticles as a life-saving strategy for treating COVID-19 patients. Theranostics 2020, 10, 5932–5942. [Google Scholar] [CrossRef]
- Kim, Y.; Park, E.J.; Na, D.H. Recent progress in dendrimer-based nanomedicine development. Arch. Pharmacal Res. 2018, 41, 571–582. [Google Scholar] [CrossRef] [PubMed]
- Chahal, J.S.; Khan, O.F.; Cooper, C.L.; McPartlan, J.S.; Tsosie, J.K.; Tilley, L.D.; Sidik, S.M.; Lourido, S.; Langer, R.; Bavari, S.; et al. Dendrimer-RNA nanoparticles generate protective immunity against lethal Ebola, H1N1 influenza, and Toxoplasma gondii challenges with a single dose. Proc. Natl. Acad. Sci. USA 2016, 113, E4133–E4142. [Google Scholar] [CrossRef]


| Types of Nanoparticles | Action Against the Bacteria | Reference |
|---|---|---|
| Silver nanoparticles (AgNP) | Bactericidal against Escherichia coli, Porphyromonas gingivalis, Aggregatibacter actinomycetememcomitans | [43] |
| Copper nanoparticles | Bacteriostatic | [44] |
| Copper oxide nanoparticles | Bactericidal against methicillin-resistant Staphylococcus aureus (MRSA) and Escherichia coli | [51] |
| Poly lactic-co-glycolic acid (PGLA) with photosensitizer Methylene Blue | Bactericidal against Enterococcus faecalis | [60] |
| Chitosan nanoparticles | Bactericidal against Enterococcus faecalis | [61] |
| Minocycline loaded polyethylene glycol and polylactic acid | Bactericidal against Aggregatibacter actinomycetememcomitans | [64] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lal, A.; Alam, M.K.; Ahmed, N.; Maqsood, A.; Al-Qaisi, R.K.; Shrivastava, D.; Alkhalaf, Z.A.; Alanazi, A.M.; Alshubrmi, H.R.; Sghaireen, M.G.; et al. Nano Drug Delivery Platforms for Dental Application: Infection Control and TMJ Management—A Review. Polymers 2021, 13, 4175. https://doi.org/10.3390/polym13234175
Lal A, Alam MK, Ahmed N, Maqsood A, Al-Qaisi RK, Shrivastava D, Alkhalaf ZA, Alanazi AM, Alshubrmi HR, Sghaireen MG, et al. Nano Drug Delivery Platforms for Dental Application: Infection Control and TMJ Management—A Review. Polymers. 2021; 13(23):4175. https://doi.org/10.3390/polym13234175
Chicago/Turabian StyleLal, Abhishek, Mohammad Khursheed Alam, Naseer Ahmed, Afsheen Maqsood, Ruba K. Al-Qaisi, Deepti Shrivastava, Zainab Ali Alkhalaf, Amal Mohamed Alanazi, Hasna Rasheed Alshubrmi, Mohammed G. Sghaireen, and et al. 2021. "Nano Drug Delivery Platforms for Dental Application: Infection Control and TMJ Management—A Review" Polymers 13, no. 23: 4175. https://doi.org/10.3390/polym13234175
APA StyleLal, A., Alam, M. K., Ahmed, N., Maqsood, A., Al-Qaisi, R. K., Shrivastava, D., Alkhalaf, Z. A., Alanazi, A. M., Alshubrmi, H. R., Sghaireen, M. G., & Srivastava, K. C. (2021). Nano Drug Delivery Platforms for Dental Application: Infection Control and TMJ Management—A Review. Polymers, 13(23), 4175. https://doi.org/10.3390/polym13234175










