Therapeutic Management of Adults with Inflammatory Bowel Disease and Malignancies: A Clinical Challenge
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
3. Diagnosis of Cancer in IBD Patients: How to Manage IBD Therapies
4. Risk of New or Recurrent Cancer in IBD Patients with a Previous History of Cancer Treated with Immunosuppressants
4.1. Thiopurines
4.2. Anti-TNFα
4.3. Vedolizumab
4.4. Ustekinumab
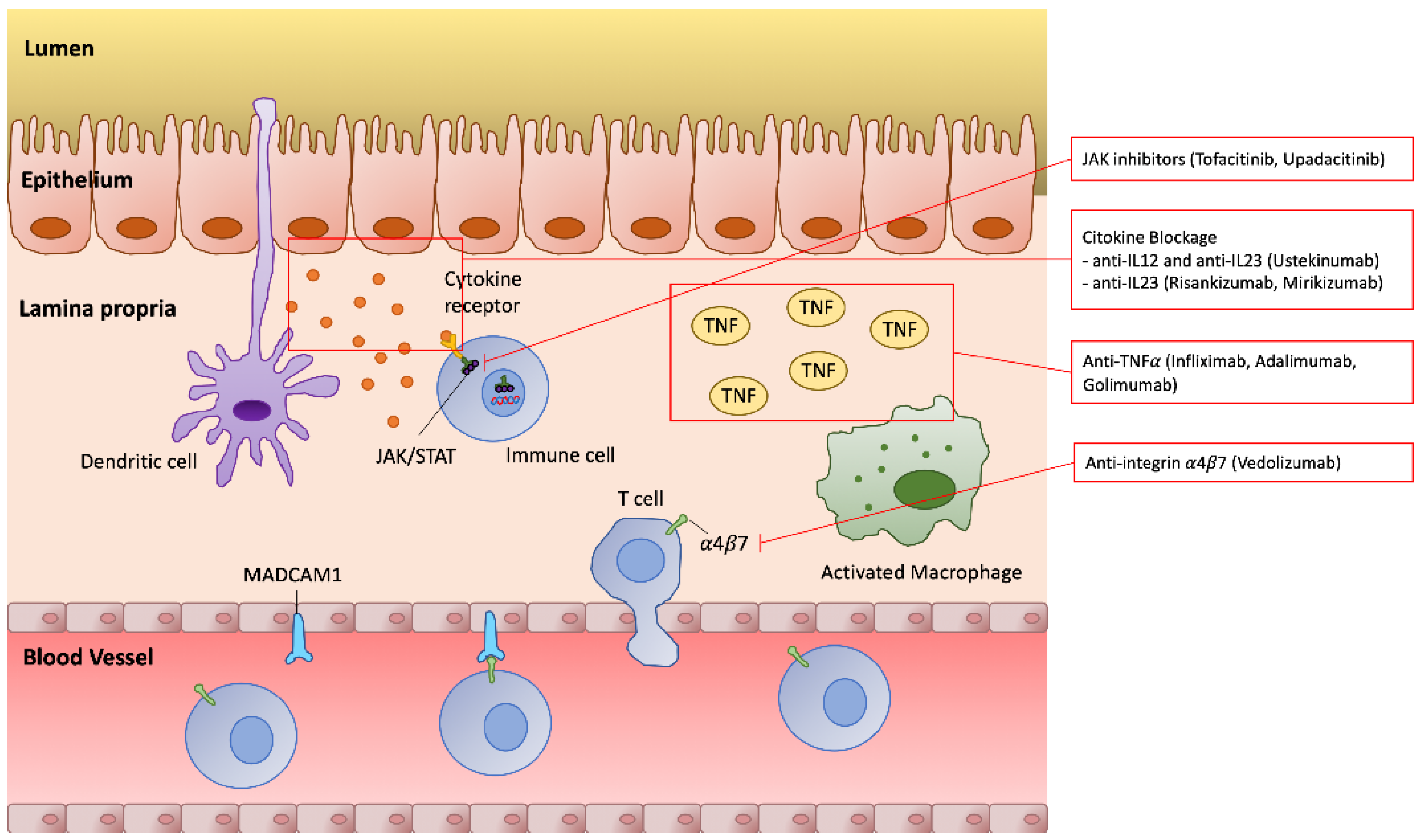
4.5. Novel Therapies
5. Risk of IBD Relapse in Patients with Cancer Who Discontinue Immunosuppressants
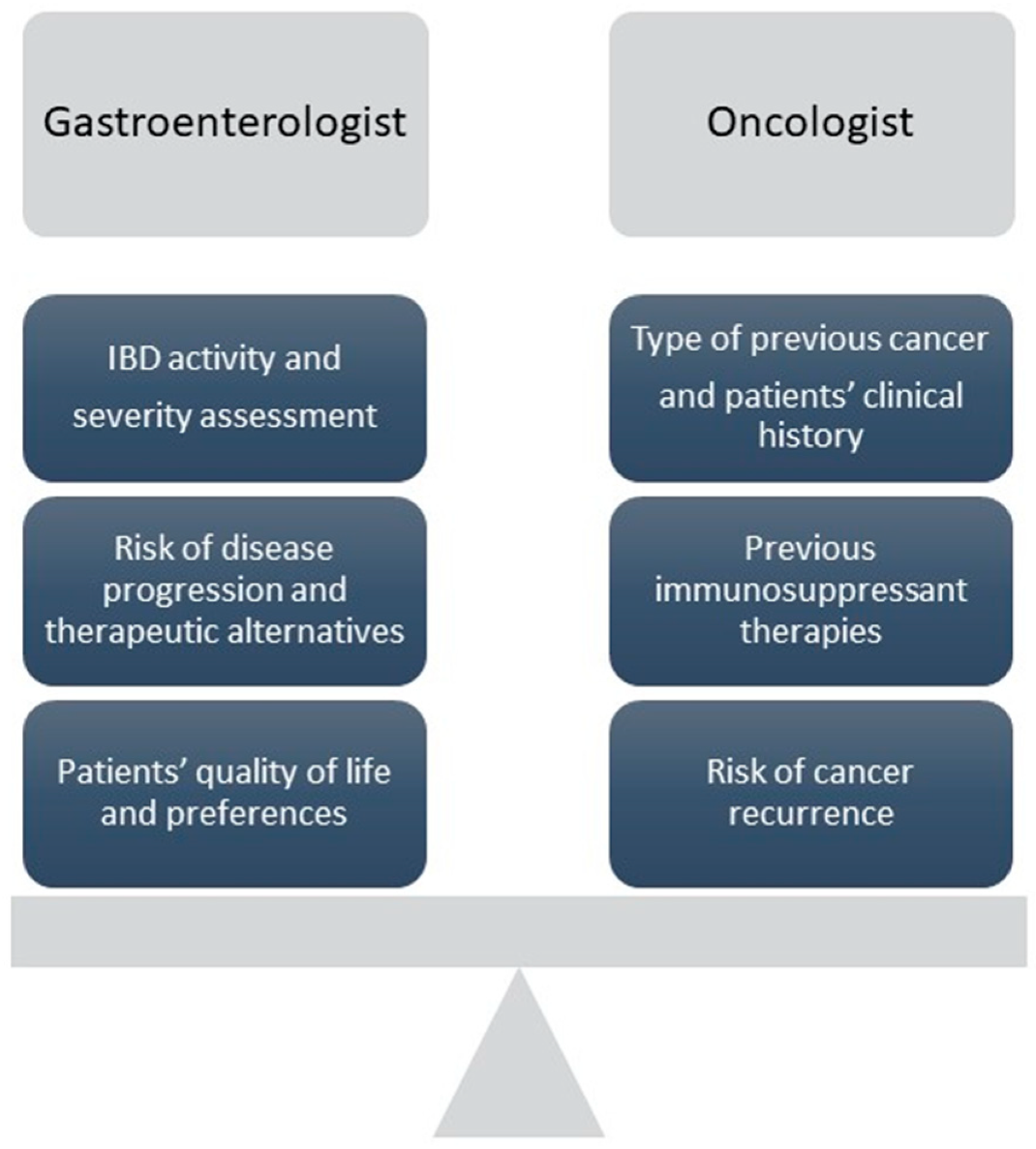
6. Discussion and Future Perspectives
- the ongoing immunosuppressants, if there was one, at the moment of previous cancer onset (i.e., melanoma under anti-TNF), in order to opt for another class of drug [51];
- the risk of cancer progression: in case of intermediated or high risk of recurrence, monotherapy with IMM or anti-TNF or VDZ should be adopted. Combo therapy should be used only in special and well-discussed situations.
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Hemminki, K.; Li, X.; Sundquist, J.; Sundquist, K. Cancer risks in Crohn disease patients. Ann. Oncol. 2009, 20, 574–580. [Google Scholar] [CrossRef] [PubMed]
- Ullman, T.A.; Itzkowitz, S.H. Intestinal inflammation and cancer. Gastroenterology 2011, 140, 1807–1816. [Google Scholar] [CrossRef] [PubMed]
- Pedersen, N.; Duricova, D.; Elkjaer, M.; Gamborg, M.; Munkholm, P.; Jess, T. Risk of extra-intestinal cancer in inflammatory bowel disease: Meta-analysis of population-based cohort studies. Am. J. Gastroenterol. 2010, 105, 1480–1487. [Google Scholar] [CrossRef] [PubMed]
- Biancone, L.; Armuzzi, A.; Scribano, M.L.; Castiglione, F.; D’Inca, R.; Orlando, A.; Papi, C.; Daperno, M.; Vecchi, M.; Riegler, G.; et al. Cancer Risk in Inflammatory Bowel Disease: A 6-Year Prospective Multicenter Nested Case-Control IG-IBD Study. Inflamm. Bowel Dis. 2020, 26, 450–459. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, R.G.; West, J.; Card, T.R. Risk of cancer in inflammatory bowel disease treated with azathioprine: A UK population-based case-control study. Am. J. Gastroenterol. 2010, 105, 1604–1609. [Google Scholar] [CrossRef]
- Lewis, J.D.; Bilker, W.B.; Brensinger, C.; Deren, J.J.; Vaughn, D.J.; Strom, B.L. Inflammatory bowel disease is not associated with an increased risk of lymphoma. Gastroenterology 2001, 121, 1080–1087. [Google Scholar] [CrossRef]
- Long, M.D.; Herfarth, H.H.; Pipkin, C.A.; Porter, C.Q.; Sandler, R.S.; Kappelman, M.D. Increased risk for non-melanoma skin cancer in patients with inflammatory bowel disease. Clin. Gastroenterol. Hepatol. 2010, 8, 268–274. [Google Scholar] [CrossRef]
- Long, M.D.; Martin, C.F.; Pipkin, C.A.; Herfarth, H.H.; Sandler, R.S.; Kappelman, M.D. Risk of melanoma and nonmelanoma skin cancer among patients with inflammatory bowel disease. Gastroenterology 2012, 143, 390–399.e391. [Google Scholar] [CrossRef]
- Peyrin-Biroulet, L.; Khosrotehrani, K.; Carrat, F.; Bouvier, A.M.; Chevaux, J.B.; Simon, T.; Carbonnel, F.; Colombel, J.F.; Dupas, J.L.; Godeberge, P.; et al. Increased risk for nonmelanoma skin cancers in patients who receive thiopurines for inflammatory bowel disease. Gastroenterology 2011, 141, 1621–1628.e5. [Google Scholar] [CrossRef]
- Annese, V.; Beaugerie, L.; Egan, L.; Biancone, L.; Bolling, C.; Brandts, C.; Dierickx, D.; Dummer, R.; Fiorino, G.; Gornet, J.M.; et al. European Evidence-based Consensus: Inflammatory Bowel Disease and Malignancies. J. Crohn’s Colitis 2015, 9, 945–965. [Google Scholar] [CrossRef]
- Singh, H.; Demers, A.A.; Nugent, Z.; Mahmud, S.M.; Kliewer, E.V.; Bernstein, C.N. Risk of cervical abnormalities in women with inflammatory bowel disease: A population-based nested case-control study. Gastroenterology 2009, 136, 451–458. [Google Scholar] [CrossRef]
- Gutierrez-Dalmau, A.; Campistol, J.M. Immunosuppressive therapy and malignancy in organ transplant recipients. Drugs 2007, 67, 1167–1198. [Google Scholar] [CrossRef]
- Penn, I. The effect of immunosuppression on pre-existing cancers. Transplantation 1993, 55, 742–747. [Google Scholar] [CrossRef]
- Lamb, C.A.; Kennedy, N.A.; Raine, T.; Hendy, P.A.; Smith, P.J.; Limdi, J.K.; Hayee, B.H.; Lomer, M.C.E.; Parkes, G.C.; Selinger, C.; et al. British Society of Gastroenterology consensus guidelines on the management of inflammatory bowel disease in adults. Gut 2019, 68, s1–s106. [Google Scholar] [CrossRef]
- Offman, J.; Opelz, G.; Doehler, B.; Cummins, D.; Halil, O.; Banner, N.R.; Burke, M.M.; Sullivan, D.; Macpherson, P.; Karran, P. Defective DNA mismatch repair in acute myeloid leukemia/myelodysplastic syndrome after organ transplantation. Blood 2004, 104, 822–828. [Google Scholar] [CrossRef]
- Dixon, W.G.; Watson, K.D.; Lunt, M.; Mercer, L.K.; Hyrich, K.L.; Symmons, D.P.; British Society For Rheumatology Biologics Register Control Centre Consortium; British Society For Rheumatology Biologics Register. Influence of anti-tumor necrosis factor therapy on cancer incidence in patients with rheumatoid arthritis who have had a prior malignancy: Results from the British Society for Rheumatology Biologics Register. Arthritis Care Res. 2010, 62, 755–763. [Google Scholar] [CrossRef]
- Beaugerie, L. Management of inflammatory bowel disease patients with a cancer history. Curr. Drug Targets 2014, 15, 1042–1048. [Google Scholar] [CrossRef]
- Beaugerie, L.; Carrat, F.; Colombel, J.F.; Bouvier, A.M.; Sokol, H.; Babouri, A.; Carbonnel, F.; Laharie, D.; Faucheron, J.L.; Simon, T.; et al. Risk of new or recurrent cancer under immunosuppressive therapy in patients with IBD and previous cancer. Gut 2014, 63, 1416–1423. [Google Scholar] [CrossRef]
- Sandborn, W.J.; Rebuck, R.; Wang, Y.; Zou, B.; Adedokun, O.J.; Gasink, C.; Sands, B.E.; Hanauer, S.B.; Targan, S.; Ghosh, S.; et al. Five-Year Efficacy and Safety of Ustekinumab Treatment in Crohn’s Disease: The IM-UNITI Trial. Clin. Gastroenterol. Hepatol. 2022, 20, 578–590.e574. [Google Scholar] [CrossRef]
- Loftus, E.V., Jr.; Feagan, B.G.; Panaccione, R.; Colombel, J.F.; Sandborn, W.J.; Sands, B.E.; Danese, S.; D’Haens, G.; Rubin, D.T.; Shafran, I.; et al. Long-term safety of vedolizumab for inflammatory bowel disease. Aliment. Pharmacol. Ther. 2020, 52, 1353–1365. [Google Scholar] [CrossRef]
- Shelton, E.; Laharie, D.; Scott, F.I.; Mamtani, R.; Lewis, J.D.; Colombel, J.F.; Ananthakrishnan, A.N. Cancer Recurrence Following Immune-Suppressive Therapies in Patients with Immune-Mediated Diseases: A Systematic Review and Meta-analysis. Gastroenterology 2016, 151, 97–109.e104. [Google Scholar] [CrossRef] [PubMed]
- Swoger, J.M.; Regueiro, M. Stopping, continuing, or restarting immunomodulators and biologics when an infection or malignancy develops. Inflamm. Bowel Dis. 2014, 20, 926–935. [Google Scholar] [CrossRef] [PubMed]
- Algaba, A.; Guerra, I.; Marin-Jimenez, I.; Quintanilla, E.; Lopez-Serrano, P.; Garcia-Sanchez, M.C.; Casis, B.; Taxonera, C.; Moral, I.; Chaparro, M.; et al. Incidence, management, and course of cancer in patients with inflammatory bowel disease. J. Crohn’s Colitis 2015, 9, 326–333. [Google Scholar] [CrossRef] [PubMed]
- Axelrad, J.E.; Fowler, S.A.; Friedman, S.; Ananthakrishnan, A.N.; Yajnik, V. Effects of cancer treatment on inflammatory bowel disease remission and reactivation. Clin. Gastroenterol. Hepatol. 2012, 10, 1021–1027.e1021. [Google Scholar] [CrossRef] [PubMed]
- Rajca, S.; Seksik, P.; Bourrier, A.; Sokol, H.; Nion-Larmurier, I.; Beaugerie, L.; Cosnes, J. Impact of the diagnosis and treatment of cancer on the course of inflammatory bowel disease. J. Crohn’s Colitis 2014, 8, 819–824. [Google Scholar] [CrossRef]
- Vedamurthy, A.; Gangasani, N.; Ananthakrishnan, A.N. Vedolizumab or Tumor Necrosis Factor Antagonist Use and Risk of New or Recurrent Cancer in Patients with Inflammatory Bowel Disease with Prior Malignancy: A Retrospective Cohort Study. Clin. Gastroenterol. Hepatol. 2022, 20, 88–95. [Google Scholar] [CrossRef]
- Hasan, B.; Tandon, K.S.; Miret, R.; Khan, S.; Riaz, A.; Gonzalez, A.; Rahman, A.U.; Charles, R.; Narula, N.; Castro, F.J. Ustekinumab does not increase risk of new or recurrent cancer in inflammatory bowel disease patients with prior malignancy. J. Gastroenterol. Hepatol. 2022, 37, 1016–1021. [Google Scholar] [CrossRef]
- Poullenot, F.; Amiot, A.; Nachury, M.; Viennot, S.; Altwegg, R.; Bouhnik, Y.; Abitbol, V.; Nancey, S.; Vuitton, L.; Peyrin-Biroulet, L.; et al. Comparative Risk of Incident Cancer in Patients with Inflammatory Bowel Disease with Prior Non-digestive Malignancy According to Immunomodulator: A Multicentre Cohort Study. J. Crohn’s Colitis 2022, 16, 1523–1530. [Google Scholar] [CrossRef]
- Axelrad, J.; Bernheim, O.; Colombel, J.F.; Malerba, S.; Ananthakrishnan, A.; Yajnik, V.; Hoffman, G.; Agrawal, M.; Lukin, D.; Desai, A.; et al. Risk of New or Recurrent Cancer in Patients with Inflammatory Bowel Disease and Previous Cancer Exposed to Immunosuppressive and Anti-Tumor Necrosis Factor Agents. Clin. Gastroenterol. Hepatol. 2016, 14, 58–64. [Google Scholar] [CrossRef]
- Poullenot, F.; Seksik, P.; Beaugerie, L.; Amiot, A.; Nachury, M.; Abitbol, V.; Stefanescu, C.; Reenaers, C.; Fumery, M.; Pelletier, A.L.; et al. Risk of Incident Cancer in Inflammatory Bowel Disease Patients Starting Anti-TNF Therapy While Having Recent Malignancy. Inflamm. Bowel Dis. 2016, 22, 1362–1369. [Google Scholar] [CrossRef]
- Hong, S.J.; Zenger, C.; Pecoriello, J.; Pang, A.; Vallely, M.; Hudesman, D.P.; Chang, S.; Axelrad, J.E. Ustekinumab and Vedolizumab Are Not Associated with Subsequent Cancer in IBD Patients with Prior Malignancy. Inflamm. Bowel Dis. 2022, 28, 1826–1832. [Google Scholar] [CrossRef]
- Ferretti, F.; Cannatelli, R.; Monico, M.C.; Maconi, G.; Ardizzone, S. An Update on Current Pharmacotherapeutic Options for the Treatment of Ulcerative Colitis. J. Clin. Med. 2022, 11, 2302. [Google Scholar] [CrossRef]
- Huang, S.Z.; Liu, Z.C.; Liao, W.X.; Wei, J.X.; Huang, X.W.; Yang, C.; Xia, Y.H.; Li, L.; Ye, C.; Dai, S.X. Risk of skin cancers in thiopurines-treated and thiopurines-untreated patients with inflammatory bowel disease: A systematic review and meta-analysis. J. Gastroenterol. Hepatol. 2019, 34, 507–516. [Google Scholar] [CrossRef]
- Cheddani, H.; Dauchet, L.; Fumery, M.; Charpentier, C.; Marie Bouvier, A.; Dupas, J.L.; Pariente, B.; Peyrin-Biroulet, L.; Savoye, G.; Gower-Rousseau, C. Cancer in Elderly Onset Inflammatory Bowel Disease: A Population-Based Study. Am. J. Gastroenterol. 2016, 111, 1428–1436. [Google Scholar] [CrossRef]
- Zheng, K.Y.C.; Guo, C.G.; Wong, I.O.L.; Chen, L.; Chung, H.Y.; Cheung, K.S.; Leung, W.K. Risk of malignancies in patients with inflammatory bowel disease who used thiopurines as compared with other indications: A territory-wide study. Ther. Adv. Gastroenterol. 2020, 13, 1756284820967275. [Google Scholar] [CrossRef]
- Kotlyar, D.S.; Lewis, J.D.; Beaugerie, L.; Tierney, A.; Brensinger, C.M.; Gisbert, J.P.; Loftus, E.V., Jr.; Peyrin-Biroulet, L.; Blonski, W.C.; Van Domselaar, M.; et al. Risk of lymphoma in patients with inflammatory bowel disease treated with azathioprine and 6-mercaptopurine: A meta-analysis. Clin. Gastroenterol. Hepatol. 2015, 13, 847–858.e844, quiz e848–e850. [Google Scholar] [CrossRef]
- Beaugerie, L.; Brousse, N.; Bouvier, A.M.; Colombel, J.F.; Lemann, M.; Cosnes, J.; Hebuterne, X.; Cortot, A.; Bouhnik, Y.; Gendre, J.P.; et al. Lymphoproliferative disorders in patients receiving thiopurines for inflammatory bowel disease: A prospective observational cohort study. Lancet 2009, 374, 1617–1625. [Google Scholar] [CrossRef]
- Sokol, H.; Beaugerie, L. Inflammatory bowel disease and lymphoproliferative disorders: The dust is starting to settle. Gut 2009, 58, 1427–1436. [Google Scholar] [CrossRef]
- Abbas, A.M.; Almukhtar, R.M.; Loftus, E.V., Jr.; Lichtenstein, G.R.; Khan, N. Risk of melanoma and non-melanoma skin cancer in ulcerative colitis patients treated with thiopurines: A nationwide retrospective cohort. Am. J. Gastroenterol. 2014, 109, 1781–1793. [Google Scholar] [CrossRef]
- Scott, F.I.; Mamtani, R.; Brensinger, C.M.; Haynes, K.; Chiesa-Fuxench, Z.C.; Zhang, J.; Chen, L.; Xie, F.; Yun, H.; Osterman, M.T.; et al. Risk of Nonmelanoma Skin Cancer Associated with the Use of Immunosuppressant and Biologic Agents in Patients with a History of Autoimmune Disease and Nonmelanoma Skin Cancer. JAMA Dermatol. 2016, 152, 164–172. [Google Scholar] [CrossRef]
- Khan, N.; Lee, H.; Trivedi, C.; Kavani, H.; Medvedeva, E.; Xie, D.; Lewis, J.D.; Yang, Y.X. Mortality Associated with Development of Squamous Cell Cancer in Patients with Inflammatory Bowel Diseases Receiving Treatment with Thiopurines. Clin. Gastroenterol. Hepatol. 2019, 17, 2262–2268. [Google Scholar] [CrossRef] [PubMed]
- Khan, N.; Patel, D.; Trivedi, C.; Kavani, H.; Medvedeva, E.; Pernes, T.; Xie, D.; Lewis, J.; Yang, Y.X. Repeated Occurrences of Basal Cell Cancer in Patients with Inflammatory Bowel Disease Treated with Immunosuppressive Medications. Am. J. Gastroenterol. 2020, 115, 1246–1252. [Google Scholar] [CrossRef]
- Raine, T.; Bonovas, S.; Burisch, J.; Kucharzik, T.; Adamina, M.; Annese, V.; Bachmann, O.; Bettenworth, D.; Chaparro, M.; Czuber-Dochan, W.; et al. ECCO Guidelines on Therapeutics in Ulcerative Colitis: Medical Treatment. J. Crohn’s Colitis 2022, 16, 2–17. [Google Scholar] [CrossRef] [PubMed]
- Torres, J.; Bonovas, S.; Doherty, G.; Kucharzik, T.; Gisbert, J.P.; Raine, T.; Adamina, M.; Armuzzi, A.; Bachmann, O.; Bager, P.; et al. ECCO Guidelines on Therapeutics in Crohn’s Disease: Medical Treatment. J. Crohn’s Colitis 2020, 14, 4–22. [Google Scholar] [CrossRef] [PubMed]
- Burmester, G.R.; Gordon, K.B.; Rosenbaum, J.T.; Arikan, D.; Lau, W.L.; Li, P.; Faccin, F.; Panaccione, R. Long-Term Safety of Adalimumab in 29,967 Adult Patients From Global Clinical Trials Across Multiple Indications: An Updated Analysis. Adv. Ther. 2020, 37, 364–380. [Google Scholar] [CrossRef]
- Bonovas, S.; Pantavou, K.; Evripidou, D.; Bastiampillai, A.J.; Nikolopoulos, G.K.; Peyrin-Biroulet, L.; Danese, S. Safety of biological therapies in ulcerative colitis: An umbrella review of meta-analyses. Best Pract. Res. Clin. Gastroenterol. 2018, 32–33, 43–47. [Google Scholar] [CrossRef]
- Nardone, B.; Hammel, J.A.; Raisch, D.W.; Weaver, L.L.; Schneider, D.; West, D.P. Melanoma associated with tumour necrosis factor-alpha inhibitors: A Research on Adverse Drug events And Reports (RADAR) project. Br. J. Dermatol. 2014, 170, 1170–1172. [Google Scholar] [CrossRef]
- Raaschou, P.; Simard, J.F.; Holmqvist, M.; Askling, J.; Group, A.S. Rheumatoid arthritis, anti-tumour necrosis factor therapy, and risk of malignant melanoma: Nationwide population based prospective cohort study from Sweden. BMJ 2013, 346, f1939. [Google Scholar] [CrossRef]
- Singh, S.; Nagpal, S.J.; Murad, M.H.; Yadav, S.; Kane, S.V.; Pardi, D.S.; Talwalkar, J.A.; Loftus, E.V., Jr. Inflammatory bowel disease is associated with an increased risk of melanoma: A systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 2014, 12, 210–218. [Google Scholar] [CrossRef]
- Nyboe Andersen, N.; Pasternak, B.; Basit, S.; Andersson, M.; Svanstrom, H.; Caspersen, S.; Munkholm, P.; Hviid, A.; Jess, T. Association between tumor necrosis factor-alpha antagonists and risk of cancer in patients with inflammatory bowel disease. JAMA 2014, 311, 2406–2413. [Google Scholar] [CrossRef]
- Lee, J.; Clarke, K. Anti-TNF agents in patients with inflammatory bowel disease and malignant melanoma—Challenges in management. Int. J. Color. Dis. 2015, 30, 1595–1602. [Google Scholar] [CrossRef]
- Strangfeld, A.; Hierse, F.; Rau, R.; Burmester, G.R.; Krummel-Lorenz, B.; Demary, W.; Listing, J.; Zink, A. Risk of incident or recurrent malignancies among patients with rheumatoid arthritis exposed to biologic therapy in the German biologics register RABBIT. Arthritis Res. Ther. 2010, 12, R5. [Google Scholar] [CrossRef]
- Sandborn, W.J.; Feagan, B.G.; Rutgeerts, P.; Hanauer, S.; Colombel, J.F.; Sands, B.E.; Lukas, M.; Fedorak, R.N.; Lee, S.; Bressler, B.; et al. Vedolizumab as induction and maintenance therapy for Crohn’s disease. N. Engl. J. Med. 2013, 369, 711–721. [Google Scholar] [CrossRef]
- Feagan, B.G.; Rutgeerts, P.; Sands, B.E.; Hanauer, S.; Colombel, J.F.; Sandborn, W.J.; Van Assche, G.; Axler, J.; Kim, H.J.; Danese, S.; et al. Vedolizumab as induction and maintenance therapy for ulcerative colitis. N. Engl. J. Med. 2013, 369, 699–710. [Google Scholar] [CrossRef]
- Card, T.; Ungaro, R.; Bhayat, F.; Blake, A.; Hantsbarger, G.; Travis, S. Vedolizumab use is not associated with increased malignancy incidence: GEMINI LTS study results and post-marketing data. Aliment. Pharmacol. Ther. 2020, 51, 149–157. [Google Scholar] [CrossRef]
- Amiot, A.; Serrero, M.; Peyrin-Biroulet, L.; Filippi, J.; Pariente, B.; Roblin, X.; Buisson, A.; Stefanescu, C.; Trang-Poisson, C.; Altwegg, R.; et al. Three-year effectiveness and safety of vedolizumab therapy for inflammatory bowel disease: A prospective multi-centre cohort study. Aliment. Pharmacol. Ther. 2019, 50, 40–53. [Google Scholar] [CrossRef]
- Meserve, J.; Aniwan, S.; Koliani-Pace, J.L.; Shashi, P.; Weiss, A.; Faleck, D.; Winters, A.; Chablaney, S.; Kochhar, G.; Boland, B.S.; et al. Retrospective Analysis of Safety of Vedolizumab in Patients with Inflammatory Bowel Diseases. Clin. Gastroenterol. Hepatol. 2019, 17, 1533–1540.e1532. [Google Scholar] [CrossRef]
- Colombel, J.F.; Sands, B.E.; Rutgeerts, P.; Sandborn, W.; Danese, S.; D’Haens, G.; Panaccione, R.; Loftus, E.V., Jr.; Sankoh, S.; Fox, I.; et al. The safety of vedolizumab for ulcerative colitis and Crohn’s disease. Gut 2017, 66, 839–851. [Google Scholar] [CrossRef]
- Feagan, B.G.; Sandborn, W.J.; Gasink, C.; Jacobstein, D.; Lang, Y.; Friedman, J.R.; Blank, M.A.; Johanns, J.; Gao, L.L.; Miao, Y.; et al. Ustekinumab as Induction and Maintenance Therapy for Crohn’s Disease. N. Engl. J. Med. 2016, 375, 1946–1960. [Google Scholar] [CrossRef]
- Sands, B.E.; Sandborn, W.J.; Panaccione, R.; O’Brien, C.D.; Zhang, H.; Johanns, J.; Adedokun, O.J.; Li, K.; Peyrin-Biroulet, L.; Van Assche, G.; et al. Ustekinumab as Induction and Maintenance Therapy for Ulcerative Colitis. N. Engl. J. Med. 2019, 381, 1201–1214. [Google Scholar] [CrossRef]
- Sandborn, W.J.; Su, C.; Sands, B.E.; D’Haens, G.R.; Vermeire, S.; Schreiber, S.; Danese, S.; Feagan, B.G.; Reinisch, W.; Niezychowski, W.; et al. Tofacitinib as Induction and Maintenance Therapy for Ulcerative Colitis. N. Engl. J. Med. 2017, 376, 1723–1736. [Google Scholar] [CrossRef] [PubMed]
- Lichtenstein, G.R.; Rogler, G.; Ciorba, M.A.; Su, C.; Chan, G.; Pedersen, R.D.; Lawendy, N.; Quirk, D.; Nduaka, C.I.; Thorpe, A.J.; et al. Tofacitinib, an Oral Janus Kinase Inhibitor: Analysis of Malignancy (Excluding Nonmelanoma Skin Cancer) Events Across the Ulcerative Colitis Clinical Program. Inflamm. Bowel Ddiseases 2021, 27, 816–825. [Google Scholar] [CrossRef] [PubMed]
- Sandborn, W.J.; Feagan, B.G.; D’Haens, G.; Wolf, D.C.; Jovanovic, I.; Hanauer, S.B.; Ghosh, S.; Petersen, A.; Hua, S.Y.; Lee, J.H.; et al. Ozanimod as Induction and Maintenance Therapy for Ulcerative Colitis. N. Engl. J. Med. 2021, 385, 1280–1291. [Google Scholar] [CrossRef]
- Sandborn, W.J.; Ghosh, S.; Panes, J.; Schreiber, S.; D’Haens, G.; Tanida, S.; Siffledeen, J.; Enejosa, J.; Zhou, W.; Othman, A.A.; et al. Efficacy of Upadacitinib in a Randomized Trial of Patients with Active Ulcerative Colitis. Gastroenterology 2020, 158, 2139–2149.e2114. [Google Scholar] [CrossRef] [PubMed]
- Smith, S.C.L.; Zardo, D.; Cannatelli, R.; Stevens, N.; Iacucci, M. Endoscopic findings of checkpoint inhibitor-induced ileitis with use of the latest advanced endoscopic optical diagnosis: Near-focus narrow-band imaging. VideoGIE 2019, 4, 133–135. [Google Scholar] [CrossRef]
- Prieux-Klotz, C.; Dior, M.; Damotte, D.; Dreanic, J.; Brieau, B.; Brezault, C.; Abitbol, V.; Chaussade, S.; Coriat, R. Immune Checkpoint Inhibitor-Induced Colitis: Diagnosis and Management. Target. Oncol. 2017, 12, 301–308. [Google Scholar] [CrossRef]
- Johnston, R.L.; Lutzky, J.; Chodhry, A.; Barkin, J.S. Cytotoxic T-lymphocyte-associated antigen 4 antibody-induced colitis and its management with infliximab. Dig. Ddiseases Sci. 2009, 54, 2538–2540. [Google Scholar] [CrossRef]
- Weber, J.S.; Dummer, R.; de Pril, V.; Lebbe, C.; Hodi, F.S.; Investigators, M.D.X. Patterns of onset and resolution of immune-related adverse events of special interest with ipilimumab: Detailed safety analysis from a phase 3 trial in patients with advanced melanoma. Cancer 2013, 119, 1675–1682. [Google Scholar] [CrossRef]
- Weber, J. Ipilimumab: Controversies in its development, utility and autoimmune adverse events. Cancer Immunol. Immunother. 2009, 58, 823–830. [Google Scholar] [CrossRef]
- Johnson, D.B.; Sullivan, R.J.; Ott, P.A.; Carlino, M.S.; Khushalani, N.I.; Ye, F.; Guminski, A.; Puzanov, I.; Lawrence, D.P.; Buchbinder, E.I.; et al. Ipilimumab Therapy in Patients with Advanced Melanoma and Preexisting Autoimmune Disorders. JAMA Oncol. 2016, 2, 234–240. [Google Scholar] [CrossRef]
- Wiedenmann, B.; Malfertheiner, P.; Friess, H.; Ritch, P.; Arseneau, J.; Mantovani, G.; Caprioni, F.; Van Cutsem, E.; Richel, D.; DeWitte, M.; et al. A multicenter, phase II study of infliximab plus gemcitabine in pancreatic cancer cachexia. J. Support. Oncol. 2008, 6, 18–25. [Google Scholar]
- Jatoi, A.; Ritter, H.L.; Dueck, A.; Nguyen, P.L.; Nikcevich, D.A.; Luyun, R.F.; Mattar, B.I.; Loprinzi, C.L. A placebo-controlled, double-blind trial of infliximab for cancer-associated weight loss in elderly and/or poor performance non-small cell lung cancer patients (N01C9). Lung Cancer 2010, 68, 234–239. [Google Scholar] [CrossRef]
- Harrison, M.L.; Obermueller, E.; Maisey, N.R.; Hoare, S.; Edmonds, K.; Li, N.F.; Chao, D.; Hall, K.; Lee, C.; Timotheadou, E.; et al. Tumor necrosis factor alpha as a new target for renal cell carcinoma: Two sequential phase II trials of infliximab at standard and high dose. J. Clin. Oncol. 2007, 25, 4542–4549. [Google Scholar] [CrossRef]
- Raaschou, P.; Simard, J.F.; Neovius, M.; Askling, J.; Anti-Rheumatic Therapy in Sweden Study Group. Does cancer that occurs during or after anti-tumor necrosis factor therapy have a worse prognosis? A national assessment of overall and site-specific cancer survival in rheumatoid arthritis patients treated with biologic agents. Arthritis Rheum. 2011, 63, 1812–1822. [Google Scholar] [CrossRef]
- Lin, S.C.; Goldowsky, A.; Papamichael, K.; Cheifetz, A.S. The Treatment of Inflammatory Bowel Disease in Patients with a History of Malignancy. Inflamm. Bowel Dis. 2019, 25, 998–1005. [Google Scholar] [CrossRef]
- Beaugerie, L. Lymphoma: The bete noire of the long-term use of thiopurines in adult and elderly patients with inflammatory bowel disease. Gastroenterology 2013, 145, 927–930. [Google Scholar] [CrossRef]
- Bourrier, A.; Carrat, F.; Colombel, J.F.; Bouvier, A.M.; Abitbol, V.; Marteau, P.; Cosnes, J.; Simon, T.; Peyrin-Biroulet, L.; Beaugerie, L.; et al. Excess risk of urinary tract cancers in patients receiving thiopurines for inflammatory bowel disease: A prospective observational cohort study. Aliment. Pharmacol. Ther. 2016, 43, 252–261. [Google Scholar] [CrossRef]
- Lemaitre, M.; Kirchgesner, J.; Rudnichi, A.; Carrat, F.; Zureik, M.; Carbonnel, F.; Dray-Spira, R. Association Between Use of Thiopurines or Tumor Necrosis Factor Antagonists Alone or in Combination and Risk of Lymphoma in Patients with Inflammatory Bowel Disease. JAMA 2017, 318, 1679–1686. [Google Scholar] [CrossRef]
- Biancone, L.; Armuzzi, A.; Scribano, M.L.; D’Inca, R.; Castiglione, F.; Papi, C.; Angelucci, E.; Daperno, M.; Mocciaro, F.; Riegler, G.; et al. Inflammatory Bowel Disease Phenotype as Risk Factor for Cancer in a Prospective Multicentre Nested Case-Control IG-IBD Study. J. Crohn’s Colitis 2016, 10, 913–924. [Google Scholar] [CrossRef]
| Study | Year | Type of Study | IBD Patients (n) | Therapies | Follow-Up | Results |
|---|---|---|---|---|---|---|
| Beaugerie et al. [18] | 2014 | Prospective | 405 | 91 IMM 7 anti-TNF | Median 36 months (IQR 32–43) 1091 p-y | There was no significant difference in the incidence of new or recurrent cancers between patients exposed or not exposed to any immunosuppressant. |
| Axelrad et al. [29] | 2016 | Retrospective | 333 | 55 anti-TNF 51 anti-TNF + IMM 78 IMM 149 no IS | NA | No statistical difference in type (p = 0.61) or time (p = 0.14) of incident cancer. No statistical difference in risk of incident cancer or time of subsequent cancer (p = 0.22) between 4 groups. |
| Poullenot et al. [30] | 2016 | Retrospective and prospective | 79 | 61 anti-TNF 18 anti-TNF+IMM | Median 21 months (1–119) | Crude incidence rate of cancer was 84.5 per 1000 p-y. It was 74.8 per 1000 p-y in pts with IMM and 87.3 per 1000 p-y in pts without IMM. |
| Shelton et al. [21] | 2016 | Systematic review and meta-analysis | 3706 | N/A | 10,332 p-y | There was no statistical difference in pooled incidence rate per 1000 p-y between anti-TNF (48.5), IMM (37.9), and none (35.7), p > 0.30. |
| Vedamurthy et al. [26] | 2020 | Retrospective | 463 | 184 anti-TNF 96 VDZ 183 no IS | Median 6.2 p-y | No increase in the risk of new or recurrent cancer in pts under anti-TNF (HR 1.03) and VDZ (HR 1.38) compared to pts without IS treatment, after adjusting for confounders. |
| Hasan et al. [27] | 2022 | Retrospective | 341 | 99 anti-TNF 34 VDZ 27 USK 181 no IS | Median 5.2 p-y | No increased risk of incident cancer in patients receiving USK (HR 0.88), VDZ (HR 0.18), or anti-TNF (HR 0.47). |
| Hong et al. [31] | 2022 | Retrospective | 390 | 41 anti-TNF 37 VDZ 14 USK 31 IMM 267 no IS | Median 52 months | No increase in subsequent cancer with VDZ (adjusted HR 1.36) or USK (adjusted HR 0.96). No increased risk in subsequent cancer in patients with more than 1 biologic exposure. |
| Poullenot et al. [28] | 2022 | Retrospective | 538 | 112 anti-TNF 48 VDZ 4 USK (excluded) 143 IMM 231 no IS | Median 55 months (IQR 23–100) | Crude incidence rates for cancer were not different in patients under anti-TNF (36.6), VDZ (33.6), or no treatment (47.0), p = 0.23. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ferretti, F.; Cannatelli, R.; Maconi, G.; Ardizzone, S. Therapeutic Management of Adults with Inflammatory Bowel Disease and Malignancies: A Clinical Challenge. Cancers 2023, 15, 542. https://doi.org/10.3390/cancers15020542
Ferretti F, Cannatelli R, Maconi G, Ardizzone S. Therapeutic Management of Adults with Inflammatory Bowel Disease and Malignancies: A Clinical Challenge. Cancers. 2023; 15(2):542. https://doi.org/10.3390/cancers15020542
Chicago/Turabian StyleFerretti, Francesca, Rosanna Cannatelli, Giovanni Maconi, and Sandro Ardizzone. 2023. "Therapeutic Management of Adults with Inflammatory Bowel Disease and Malignancies: A Clinical Challenge" Cancers 15, no. 2: 542. https://doi.org/10.3390/cancers15020542
APA StyleFerretti, F., Cannatelli, R., Maconi, G., & Ardizzone, S. (2023). Therapeutic Management of Adults with Inflammatory Bowel Disease and Malignancies: A Clinical Challenge. Cancers, 15(2), 542. https://doi.org/10.3390/cancers15020542






