The Performance of HE4 Alone and in Combination with CA125 for the Detection of Ovarian Cancer in an Enriched Primary Care Population
Abstract
:Simple Summary
Abstract
1. Introduction
2. Materials and Methods
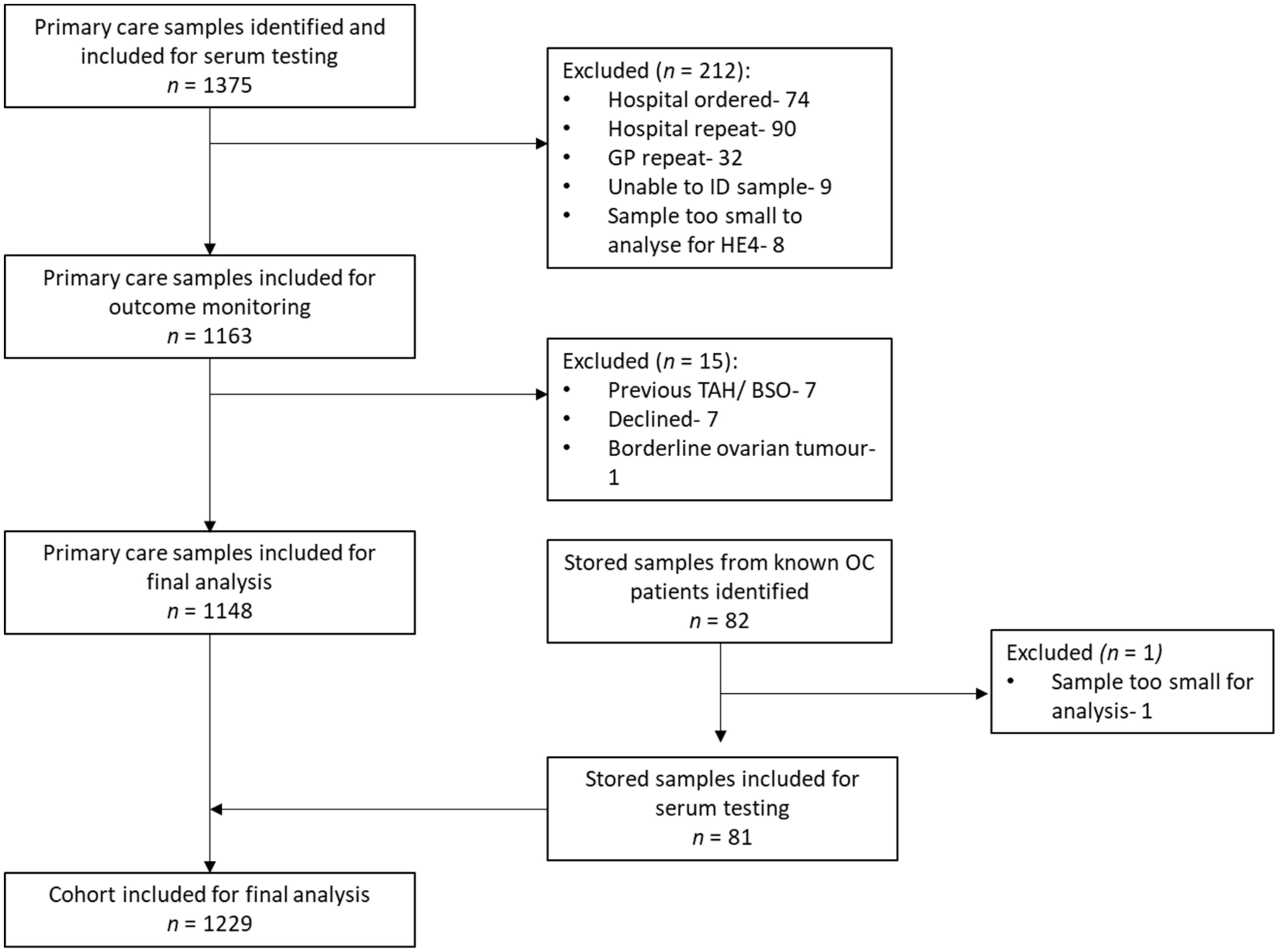
2.1. Study Population
2.2. Laboratory Assays
2.3. Statistical Analysis
3. Results
3.1. Study Population
3.1.1. Clinico-Pathological Features of Malignancies
3.1.2. Clinical Follow-Up
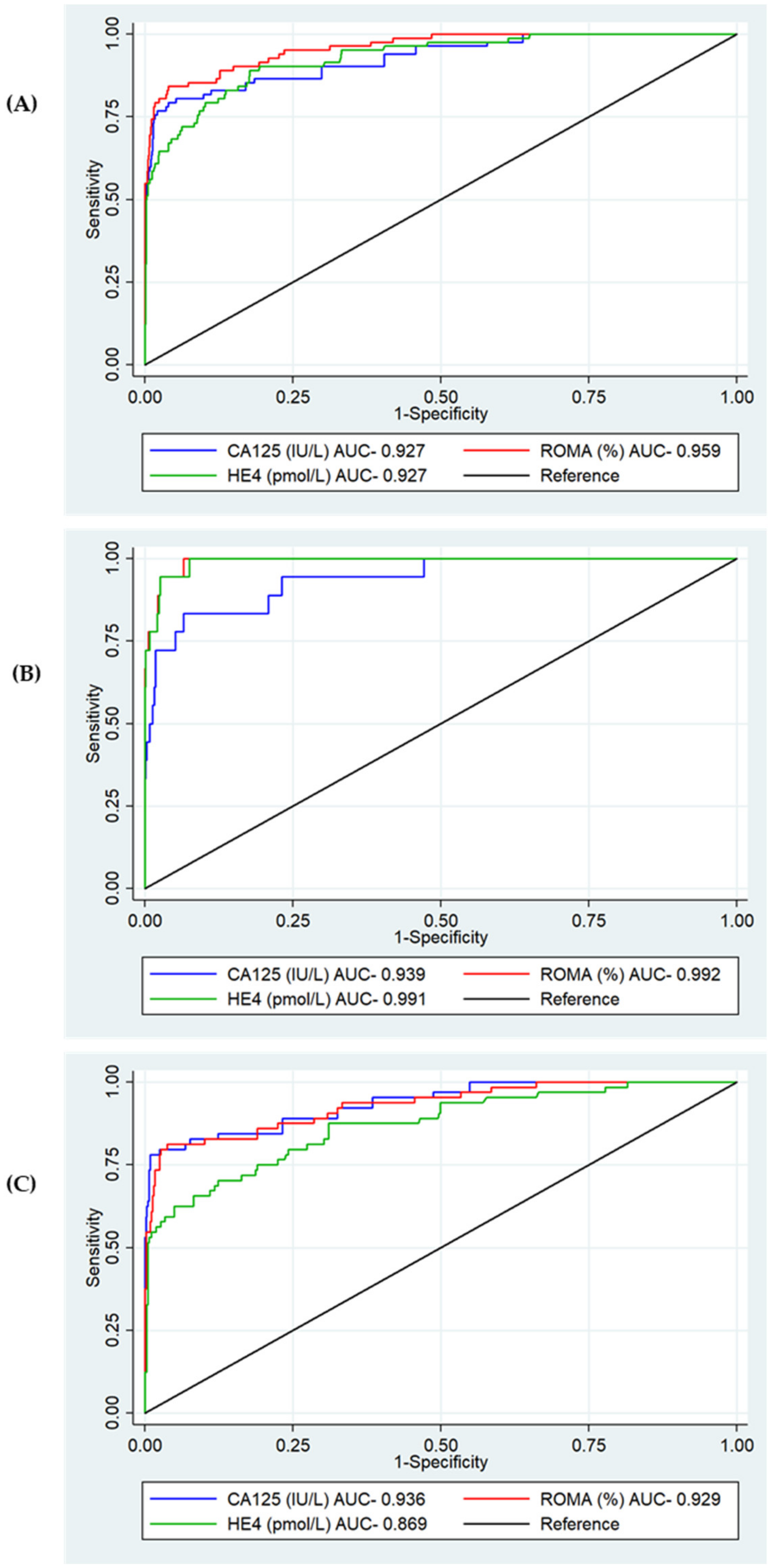
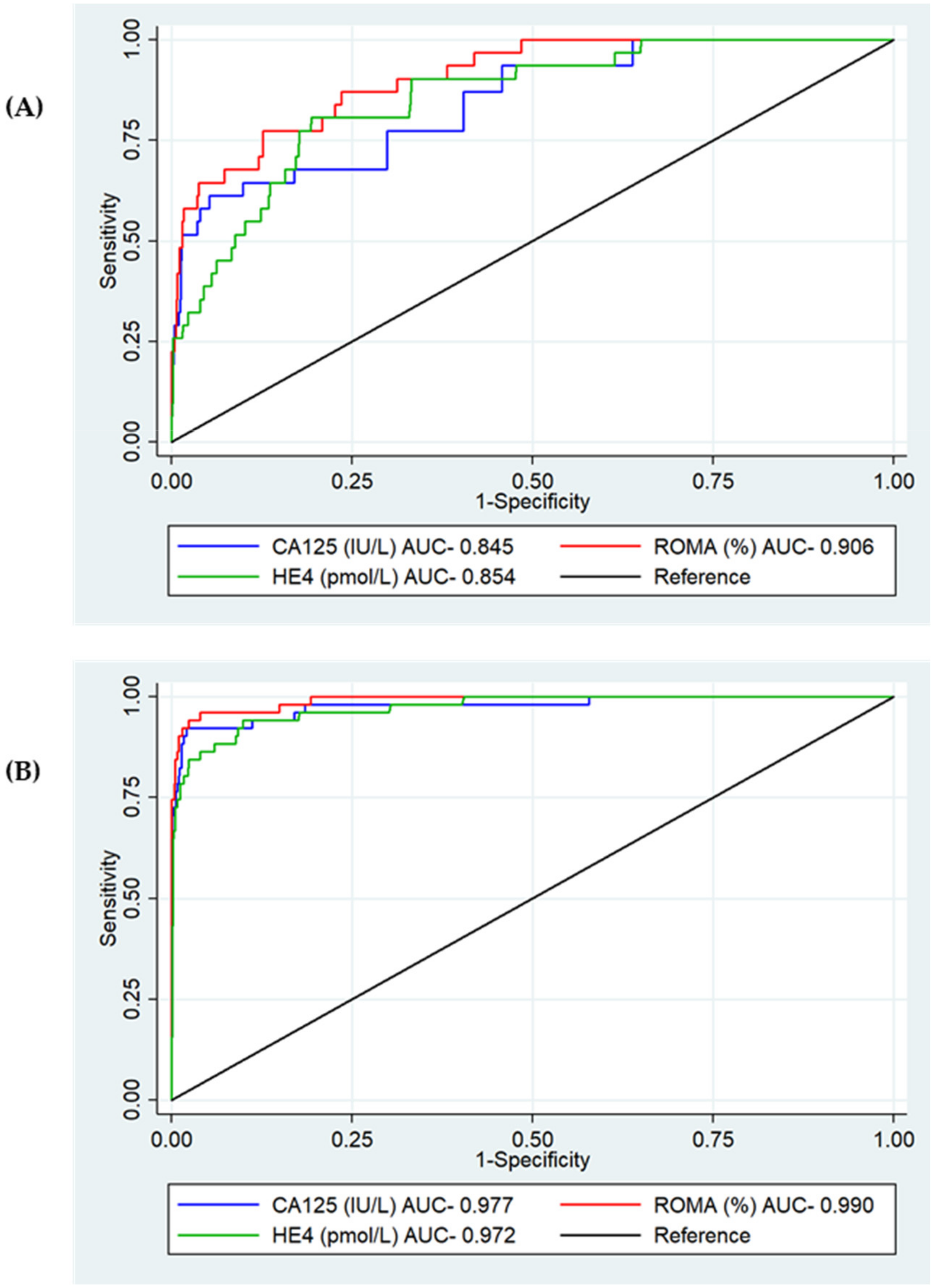
3.2. Test Diagnostic Accuracy
3.2.1. Age and Adjusted Serum HE4 Thresholds
3.2.2. Test Diagnostic Accuracy by Stage at Diagnosis
4. Discussion
4.1. Summary
4.2. Strengths and Limitations
4.3. Comparison with Existing Literature
4.4. Clinical and Research Implications
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cancer Research UK. Ovarian Cancer Mortality Statistics. Available online: https://cancerresearchuk.org/health-professional/cancer-statistics/cancer-by-type/ovarian-cancer/mortality (accessed on 22 October 2021).
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef] [PubMed]
- Reid, B.M.; Permuth, J.B.; Sellers, T.A. Epidemiology of ovarian cancer: A review. Cancer Biol. Med. 2017, 14, 9–32. [Google Scholar] [CrossRef] [Green Version]
- Cancer Research UK. Ovarian Cancer Survival Statistics. Available online: https://cancerresearchuk.org/health-professional/cancer-statistics/cancer-by-type/ovarian-cancer/survival#heading-Three (accessed on 20 December 2021).
- Quaye, L.; Gayther, S.A.; Ramus, S.; di Cioccio, R.A.; McGuire, V.; Høgdall, E.; Høgdall, C.; Blaakr, J.; Easton, D.F.; Ponder, B.A.; et al. The Effects of Common Genetic Variants in Oncogenes on Ovarian Cancer Survival. Clin. Cancer Res. 2008, 14, 5833–5839. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barrett, J.; Sharp, D.; Stapley, S.; Stabb, C.; Hamilton, W. Pathways to the diagnosis of ovarian cancer in the UK: A cohort study in primary care. BJOG: Int. J. Obstet. Gynaecol. 2010, 117, 610–614. [Google Scholar] [CrossRef] [PubMed]
- National Cancer Intelligence Network Routes to Diagnosis 2006–2016 by Year, V2.1a. Available online: http://www.ncin.org.uk/publications/routes_to_diagnosis (accessed on 21 May 2020).
- Gilbert, L.; Basso, O.; Sampalis, J.; Karp, I.; Martins, C.; Feng, J.; Piedimonte, S.; Quintal, L.; Ramanakumar, A.V.; Takefman, J.; et al. Assessment of symptomatic women for early diagnosis of ovarian cancer: Results from the prospective DOvE pilot project. Lancet Oncol. 2012, 13, 285–291. [Google Scholar] [CrossRef]
- National Institute for Health and Care Excellence. Ovarian Cancer: Recognition and Initial Management CG122. Available online: https://www.nice.org.uk/guidance/cg122 (accessed on 18 June 2018).
- Funston, G.; Hamilton, W.; Abel, G.; Crosbie, E.J.; Rous, B.; Walter, F.M. The diagnostic performance of CA125 for the detection of ovarian and non-ovarian cancer in primary care: A population-based cohort study. PLOS Med. 2020, 17, e1003295. [Google Scholar] [CrossRef]
- Urban, N.; Thorpe, J.; Karlan, B.Y.; McIntosh, M.W.; Palomares, M.R.; Daly, M.B.; Paley, P.; Drescher, C.W. Interpretation of Single and Serial Measures of HE4 and CA125 in Asymptomatic Women at High Risk for Ovarian Cancer. Cancer Epidemiol. Biomark. Prev. 2012, 21, 2087–2094. [Google Scholar] [CrossRef] [Green Version]
- Moore, R.G.; McMeekin, D.S.; Brown, A.K.; DiSilvestro, P.; Miller, M.C.; Allard, W.J.; Gajewski, W.; Kurman, R.; Bast, R.C., Jr.; Skates, S.J. A novel multiple marker bioassay utilizing HE4 and CA125 for the prediction of ovarian cancer in patients with a pelvic mass. Gynecol. Oncol. 2009, 112, 40–46. [Google Scholar] [CrossRef] [Green Version]
- Dayyani, F.; Uhlig, S.; Colson, B.; Simon, K.; Rolny, V.; Morgenstern, D.; Schlumbrecht, M. Diagnostic Performance of Risk of Ovarian Malignancy Algorithm Against CA125 and HE4 in Connection with Ovarian Cancer: A Meta-analysis. Int. J. Gynecol. Cancer 2016, 26, 1586–1593. [Google Scholar] [CrossRef]
- Scaletta, G.; Plotti, F.; Luvero, D.; Capriglione, S.; Montera, R.; Miranda, A.; Lopez, S.; Terranova, C.; Nardone, C.D.C.; Angioli, R. The role of novel biomarker HE4 in the diagnosis, prognosis and follow-up of ovarian cancer: A systematic review. Expert Rev. Anticancer Ther. 2017, 17, 827–839. [Google Scholar] [CrossRef]
- Yu, S.; Yang, H.-J.; Xie, S.-Q.; Bao, Y.-X. Diagnostic value of HE4 for ovarian cancer: A meta-analysis. Clin. Chem. Lab. Med. (CCLM) 2012, 50, 1439–1446. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.; Dai, Z.-Y.; Qian, Y.-H.; Shi, Y.; Liu, F.-J.; Yang, C. Diagnostic Value of Serum Human Epididymis Protein 4 (HE4) in Ovarian Carcinoma: A Systematic Review and Meta-Analysis. Int. J. Gynecol. Cancer 2012, 22, 1106–1112. [Google Scholar] [CrossRef] [PubMed]
- Huhtinen, K.; Suvitie, P.; Hiissa, J.; Junnila, J.; Huvila, J.; Kujari, H.; Setala, M.; Härkki, P.; Jalkanen, J.; Fraser, J.K.; et al. Serum HE4 concentration differentiates malignant ovarian tumours from ovarian endometriotic cysts. Br. J. Cancer 2009, 100, 1315–1319. [Google Scholar] [CrossRef]
- Usher-Smith, J.A.; Sharp, S.J.; Griffin, S.J. The spectrum effect in tests for risk prediction, screening, and diagnosis. BMJ 2016, 353, i3139. [Google Scholar] [CrossRef] [Green Version]
- Ferraro, S.; Borille, S.; Carnevale, A.; Frusciante, E.; Bassani, N.; Panteghini, M. Verification of the harmonization of human epididymis protein 4 assays. Clin. Chem. Lab. Med. 2016, 54, 1635. [Google Scholar] [CrossRef]
- Bast, R.C., Jr.; Klug, T.L.; St. John, E.; Jenison, E.; Niloff, J.M.; Lazarus, H.; Berkowitz, R.S.; Leavitt, T.; Griffiths, C.T.; Parker, L.; et al. A Radioimmunoassay Using a Monoclonal Antibody to Monitor the Course of Epithelial Ovarian Cancer. N. Engl. J. Med. 1983, 309, 883–887. [Google Scholar] [CrossRef] [PubMed]
- Moore, R.G.; Brown, A.K.; Miller, M.C.; Skates, S.; Allard, W.J.; Verch, T.; Steinhoff, M.; Messerlian, G.; DiSilvestro, P.; Granai, C.; et al. The use of multiple novel tumor biomarkers for the detection of ovarian carcinoma in patients with a pelvic mass. Gynecol. Oncol. 2008, 108, 402–408. [Google Scholar] [CrossRef] [PubMed]
- Barr, C.E.; Funston, G.; Mounce, L.T.; Pemberton, P.W.; Howe, J.D.; Crosbie, E.J. Comparison of two immunoassays for the measurement of serum HE4 for ovarian cancer. Pract. Lab. Med. 2021, 26, e00235. [Google Scholar] [CrossRef]
- NHS. Menopause. Available online: www.nhs.uk/conditions/menopause/ (accessed on 11 January 2022).
- National Institute for Health and Care Excellence. Tests in Secondary Care to Identify People at High Risk of Ovarian Cancer dg31. Available online: https://www.nice.org.uk/guidance/dg31/ (accessed on 12 January 2021).
- Ratnavelu, N.; Founta, C.; Addison, C.; Bradbury, M.; Handley, G.; Das, M.; Kucukmetin, A.; Naik, R. The diagnostic value of adding he4 to ca125 for women investigated for ovarian cancer in primary care: A prospective pilot study. Int. J. Gynecol. Cancer 2014, 24, 18–19. [Google Scholar]
- Liu, X. Classification accuracy and cut point selection. Stat. Med. 2012, 31, 2676–2686. [Google Scholar] [CrossRef]
- Li, F.; Tie, R.; Chang, K.; Wang, F.; Deng, S.; Lu, W.; Yu, L.; Chen, M. Does risk for ovarian malignancy algorithm excel human epididymis protein 4 and ca125 in predicting epithelial ovarian cancer: A meta-analysis. BMC Cancer 2012, 12, 258. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sundar, S.; Rick, C.; Dowling, F.; Au, P.; Snell, K.; Rai, N.; Champaneria, R.; Stobart, H.; Neal, R.; Davenport, C.; et al. Refining Ovarian Cancer Test Accuracy Scores (ROCkeTS): Protocol for a prospective longitudinal test accuracy study to validate new risk scores in women with symptoms of suspected ovarian cancer. BMJ Open 2016, 6, e010333. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rai, N.; Champaneria, R.; Snell, K.; Mallett, S.; Bayliss, S.E.; Neal, R.D.; Balogun, M.; Kehoe, S.; Deeks, J.J.; Sundar, S.; et al. Symptoms, ultrasound imaging and biochemical markers alone or in combination for the diagnosis of ovarian cancer in women with symptoms suspicious of ovarian cancer. Cochrane Database Syst. Rev. 2015, 2015, 011964. [Google Scholar] [CrossRef]
- Lin, J.; Qin, J.; Sangvatanakul, V. Human epididymis protein 4 for differential diagnosis between benign gynecologic disease and ovarian cancer: A systematic review and meta-analysis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 167, 81–85. [Google Scholar] [CrossRef] [PubMed]
- Qu, W.; Li, J.; Duan, P.; Tang, Z.; Guo, F.; Chen, H.; Zhu, X.; Jiang, S.-W. Physiopathological factors affecting the diagnostic value of serum HE4-test for gynecologic malignancies. Expert Rev. Mol. Diagn. 2016, 16, 1271–1282. [Google Scholar] [CrossRef] [Green Version]
- Moore, R.G.; Miller, M.C.; Steinhoff, M.M.; Skates, S.J.; Lu, K.H.; Lambert-Messerlian, G.; Bast, R.C. Serum HE4 levels are less frequently elevated than CA125 in women with benign gynecologic disorders. Am. J. Obstet. Gynecol. 2012, 206, 351.e1–351.e8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cornish, D.B.A.; Horton, M.; Scanlon, S.; Adult Smoking Habits in the UK: 2018. Office of National Statistics. Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/healthandlifeexpectancies/bulletins/adultsmokinghabitsgreatbritatin/2018 (accessed on 11 January 2021).
- Ferraro, S.; Schiumarini, D.; Panteghini, M. Human epididymis protein 4: Factors of variation. Clin. Chim. Acta 2015, 438, 171–177. [Google Scholar] [CrossRef]
- British Lung Foundation. Chronic Obstructive Pulmonary Disease (COPD) Statistics. Available online: https://statistics.blf.org.uk/copd (accessed on 11 January 2021).
- Yan, L.; Hu, Z.-D. Diagnostic accuracy of human epididymis secretory protein 4 for lung cancer: A systematic review and meta-analysis. J. Thorac. Dis. 2019, 11, 2737–2744. [Google Scholar] [CrossRef]
- Behrouzi, R.; Barr, C.E.; Crosbie, E.J. HE4 as a Biomarker for Endometrial Cancer. Cancers 2021, 13, 4764. [Google Scholar] [CrossRef]
- Kemal, Y.; Demïrag, G.; Bedïr, A.; Tomak, L.; Derebey, M.; Erdem, D.; Gör, U.; Yücel, I. Serum human epididymis protein 4 levels in colorectal cancer patients. Mol. Clin. Oncol. 2017, 7, 481–485. [Google Scholar] [CrossRef] [Green Version]
- Bolstad, N.; Øijordsbakken, M.; Nustad, K.; Bjerner, J. Human epididymis protein 4 reference limits and natural variation in a Nordic reference population. Tumor Biol. 2011, 33, 141–148. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gasiorowska, E.; Kluz, T.; Lipski, D.; Warchoł, W.; Tykarski, A.; Nowak-Markwitz, E.; Nowak-Markwiz, E. Human Epididymis Protein 4 (HE4) Reference Limits in Polish Population of Healthy Women, Pregnant Women, and Women with Benign Ovarian Tumors. Dis. Markers 2019, 2019, 3890906. [Google Scholar] [CrossRef] [Green Version]
- Tian, Y.; Wang, C.; Cheng, L.; Zhang, A.; Liu, W.; Guo, L.; Ye, H.; Huang, Y.; Chen, J.; Wen, X.; et al. Determination of reference intervals of serum levels of human epididymis protein 4 (HE4) in Chinese women. J. Ovarian Res. 2015, 8, 72. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Funston, G.; Mounce, L.T.A.; Price, S.; Rous, B.; Crosbie, E.J.; Hamilton, W.; Walter, F.M. Variation in the initial assessment and investigation for ovarian cancer in symptomatic women: A systematic review of international guidelines. BMC Cancer 2019, 19, 1028. [Google Scholar] [CrossRef] [Green Version]
- Funston, G.; Mounce, L.T.A.; Price, S.; Rous, B.; Crosbie, E.J.; Hamilton, W.; Walter, F.M. CA125 test result, test-to-diagnosis interval, and stage in ovarian cancer at diagnosis: A retrospective cohort study using electronic health records. Br. J. Gen. Pract. 2021, 71, e465–e472. [Google Scholar] [CrossRef]
- Badrick, E.; Cresswell, K.; Ellis, P.; Detecting Cancer Early Priority Setting Partnership Steering Group (Appendix); Renehan, A.G.; Crosbie, E.J. Top ten research priorities for detecting cancer early. Lancet Public Health 2019, 4, e551. [Google Scholar] [CrossRef] [Green Version]
- Crafton, S.M.; Cohn, D.E.; Llamocca, E.N.; Louden, E.; Rhoades, J.; Felix, A.S. Fertility-sparing surgery and survival among reproductive-age women with epithelial ovarian cancer in 2 cancer registries. Cancer 2019, 126, 1217–1224. [Google Scholar] [CrossRef]
- Wright, J.D.; Shah, M.; Mathew, L.; Burke, W.M.; Culhane, J.; Goldman, N.; Schiff, P.B.; Herzog, T.J. Fertility preservation in young women with epithelial ovarian cancer. Cancer 2009, 115, 4118–4126. [Google Scholar] [CrossRef]
- Cancer Research UK. Ovarian Cancer Incidence-Age. Available online: https://cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/ovarian-cancer/incidence#heading-One (accessed on 10 February 2022).
- Merriel, S.W.D.; Funston, G.; Hamilton, W. Prostate Cancer in Primary Care. Adv. Ther. 2018, 35, 1285–1294. [Google Scholar] [CrossRef] [Green Version]

| Variable | No Ovarian Cancer | Ovarian Cancer | ||
|---|---|---|---|---|
| N = 1147 | N = 82 | |||
| Age < 50 Years | Age ≥ 50 Years | Age < 50 Years | Age ≥ 50 Years | |
| N = 622 | N = 525 | N = 18 | N = 64 | |
| Age (years) | ||||
| Mean (SD) | 37 (8.6) | 63 (10.1) | 44 (4.0) | 65 (9.5) |
| Serum CA125 (U/mL) | ||||
| Median (IQR) | 14 (10–21) | 11 (8–17) | 167 (50–2352) | 257 (85–961) |
| Negative result (n, %) | 562 (90) | 495 (94) | 3 (17) | 13 (20) |
| Positive result (n, %) | 60 (10) | 30 (6) | 15 (83) | 51 (80) |
| Serum HE4 (pmol/L) | ||||
| Median (IQR) | 53 (45–65) | 68 (55–96) | 284 (150–534) | 314 (107–742) |
| Negative result (n, %) | 550 (88) | 317 (60) | 0 (0) | 8 (12) |
| Positive result (n, %) | 72 (12) | 208 (40) | 18 (100) | 56 (88) |
| Combined results (n, %) | ||||
| Negative CA125 + HE4 | 498 (80) | 305 (59) | 0 (0) | 6 (9) |
| Positive CA125, negative HE4 | 51 (8) | 12 (2) | 0 (0) | 2 (3) |
| Positive HE4, negative CA125 | 65 (11) | 190 (36) | 3 (17) | 7 (11) |
| Positive CA125 + HE4 | 8 (1) | 18 (3) | 15 (83) | 49 (77) |
| Variable | Number (%) | Median CA125 (IQR), U/mL | Median HE4 (IQR), pmol/L |
|---|---|---|---|
| Histological Classification | |||
| Serous | 47 (57) | 708 (97–2352) | 411 (186–830) |
| Clear cell | 8 (10) | 206 (21–5488) | 135 (88–344) |
| Mucinous | 8 (10) | 100 (40–210) | 90 (74–134) |
| Endometrioid | 8 (10) | 169 (22–468) | 404 (88–4049) |
| Mixed | 4 (5) | 132 (62–216) | 311 (124–441) |
| Carcinosarcoma | 7 (8) | 279 (80–978) | 280 (112–804) |
| Tumour Grade | |||
| 1 | 15 (18) | 105 (24–219) | 139 (69–207) |
| 2 | 4 (5) | 374 (69–2209) | 422 (100–25617) |
| 3 | 63 (77) | 526 (92–2315) | 377 (137–804) |
| FIGO 2014 Stage | |||
| 1 | 25 (30) | 90 (17–185) | 117 (89–197) |
| 2 | 6 (8) | 193 (13–3435) | 257 (58–2695) |
| 3 | 33 (40) | 746 (162–2546) | 418 (186–828) |
| 4 | 18 (22) | 806 (174–2948) | 518 (281–981) |
| N = 1229 OC = 82 (7%) | Sensitivity % (95%CI) | Specificity % (95%CI) | True Positive | False Positive |
|---|---|---|---|---|
| CA125 (≥35 U/mL) | 80.5 (70.3–88.4) | 92.2 (90.4–93.6) | 66 | 90 |
| HE4 (≥77pmol/L) | 90.2 (81.7–95.7) | (73.0–78.0) | 74 | 280 |
| Combination, either positive | 92.7 (84.8–97.3) | (67.3–72.6) | 76 | 344 |
| Combination, both positive | 78.0 (67.5–86.4) | 97.7 (96.7–98.5) | 64 | 26 |
| ROMA | 87.8 (78.7–94) | 80.8 (78.4–83.1) | 72 | 220 |
| Sensitivity % (95%CI) | Specificity % (95%CI) | True Positive | False Positive | |
|---|---|---|---|---|
| a. Under 50 years of age (n = 640, OC = 18) | ||||
| CA125 (≥35U/mL) | 83.3 (58.6–96.4) | 90.4 (87.8–92.6) | 15 | 60 |
| HE4 (≥77pmol/L) | 100.0 (81.5–100.0) | 88.4 (85.6–90.8) | 18 | 72 |
| Combined, either positive | 100.0 (81.5–100.0) | 80.1 (76.7–83.1) | 18 | 124 |
| Combined, both positive | 83.3 (58.6–96.4) | 98.7 (97.5–99.4) | 15 | 8 |
| ROMA | 100.0 (81.5–100.0) | 75.4 (71.8–78.7) | 18 | 153 |
| b. Over 50 years of age (n = 589, OC = 64) | ||||
| CA125 (≥35U/mL) | 79.7 (67.8–88.7) | 94.3 (91.9–96.1) | 51 | 30 |
| HE4 (≥77pmol/L) | 87.5 (76.8–94.4) | 60.4 (56.1–64.6) | 56 | 208 |
| Combined, either positive | 90.6 (80.7–96.5) | 58.1 (53.7–62.4) | 58 | 220 |
| Combined, both positive | 76.7 (64.3–86.2) | 96.6 (94.6–98.0) | 49 | 18 |
| ROMA | 84.4 (73.1–92.2) | 87.2 (84.1–90) | 54 | 67 |
| Predicted Median HE4 (95%CI) pmol/L | |
|---|---|
| Age at the following years | |
| 20 | 47.2 (43.6–50.8) |
| 30 | 52.1 (49.5–54.8) |
| 40 | 57.0 (55.2–58.9) |
| 50 | 62.0 (60.5–63.5) |
| 60 | 66.9 (65.0–68.8) |
| 70 | 71.8 (69.1–74.6) |
| 80 | 76.8 (73.0–80.5) |
| Age in bands (years) | |
| <30 | 53.4 (48.8–58.0) |
| 30–39 | 55.4 (51.4–59.5) |
| 40–49 | 55.4 (52.4–58.5) |
| 50–59 | 60.8 (57.6–64.0) |
| 60–69 | 69.5 (65.0–74.1) |
| ≥70 | 88.5 (83.5–93.5) |
| Sensitivity % (95%CI) | Specificity % (95%CI) | True Positive | False Positive | |
|---|---|---|---|---|
| a. Under 50 years of age (n = 640, OC = 18) | ||||
| CA125 (≥35 U/mL) | 83.3 (58.6–96.4) | 90.4 (87.8–92.6) | 15 | 60 |
| HE4 (≥68 pmol/L) | 100 (81.5–100) | 80.4 (77.0–83.4) | 18 | 122 |
| Combined, either positive | 100 (81.5–100) | 73.5 (69.8–76.9) | 18 | 165 |
| Combined, both positive | 83.3 (58.6–96.4) | 97.3 (95.7–98.4) | 15 | 17 |
| b. Over 50 years of age (n = 589, OC= 64) | ||||
| CA125 (≥35 U/mL) | 79.7 (67.8–88.7) | 94.3 (91.9–96.1) | 51 | 30 |
| HE4 (≥96 pmol/L) | 79.7 (67.8–88.7) | 74.7 (70.7–78.3) | 51 | 133 |
| Combined, either positive | 87.5 (76.8–94.4) | 71.8 (67.8–75.6) | 56 | 148 |
| Combined, both positive | 71.9 (59.2–82.4) | 97.1 (95.3–98.4) | 46 | 15 |
| Early Stage (I + II) n = 31 | Late Stage (III + IV) n = 51 | |||
|---|---|---|---|---|
| Sensitivity % (95%CI) | Specificity % (95%CI) | Sensitivity % (95%CI) | Specificity % (95%CI) | |
| CA125 (≥35 U/mL) | 61.3 (42.2–78.2) | 92.2 (90.4–93.6) | 92.2 (81.1–97.8) | 92.2 (90.4- 93.6) |
| HE4 (≥77 pmol/L) | 80.6 (62.5–92.5) | 75.6 (73.0–78.0) | 96.1 (86.5–99.5) | 75.6 (73.0–78.0) |
| Combined, either positive | 83.9 (66.3–94.5) | 70.0 (67.3–72.6) | 98.0 (89.6–100.0) | 70.0 (67.3–72.6) |
| Combined, both positive | 58.1 (39.1–75.5) | 97.7 (96.7–98.5) | 90.2 (78.6–96.7) | 97.7 (96.7–98.5) |
| ROMA | 74.3 (55.4–88.1) | 80.8 (78.4–83.1) | 96.1 (86.5–99.5) | 80.8 (78.4–83.1) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barr, C.E.; Funston, G.; Jeevan, D.; Sundar, S.; Mounce, L.T.A.; Crosbie, E.J. The Performance of HE4 Alone and in Combination with CA125 for the Detection of Ovarian Cancer in an Enriched Primary Care Population. Cancers 2022, 14, 2124. https://doi.org/10.3390/cancers14092124
Barr CE, Funston G, Jeevan D, Sundar S, Mounce LTA, Crosbie EJ. The Performance of HE4 Alone and in Combination with CA125 for the Detection of Ovarian Cancer in an Enriched Primary Care Population. Cancers. 2022; 14(9):2124. https://doi.org/10.3390/cancers14092124
Chicago/Turabian StyleBarr, Chloe E., Garth Funston, David Jeevan, Sudha Sundar, Luke T. A. Mounce, and Emma J. Crosbie. 2022. "The Performance of HE4 Alone and in Combination with CA125 for the Detection of Ovarian Cancer in an Enriched Primary Care Population" Cancers 14, no. 9: 2124. https://doi.org/10.3390/cancers14092124
APA StyleBarr, C. E., Funston, G., Jeevan, D., Sundar, S., Mounce, L. T. A., & Crosbie, E. J. (2022). The Performance of HE4 Alone and in Combination with CA125 for the Detection of Ovarian Cancer in an Enriched Primary Care Population. Cancers, 14(9), 2124. https://doi.org/10.3390/cancers14092124






