Simple Summary
Hepatocellular carcinoma (HCC) constitutes a major health burden, accounting for >80% of primary liver cancers globally. Inflammation has come into the spotlight as a hallmark of cancer, and it is evident that tumor-associated inflammation drives the involvement of monocytes in tumor growth and metastasis. Tumor-associated macrophages (TAMs) actively participate in tumor-related inflammation, representing the main type of inflammatory cells in the tumor microenvironment, setting the crosstalk between tumor and stromal cells. Infiltrating TAMs exert either anti-tumorigenic (M1) or pro-tumorigenic (M2) functions. In most solid human tumors, increased TAM infiltration has been associated with enhanced tumor growth and metastasis, while other studies showcase that under certain conditions, TAMs exhibit cytotoxic and tumoricidal activity, inhibiting the progression of cancer. In this review, we summarize the current evidence on the role of macrophages in the pathogenesis and progression of HCC and we highlight their potential utilization in HCC prognosis and therapy.
Abstract
Hepatocellular carcinoma (HCC) constitutes a major health burden globally, and it is caused by intrinsic genetic mutations acting in concert with a multitude of epigenetic and extrinsic risk factors. Cancer induces myelopoiesis in the bone marrow, as well as the mobilization of hematopoietic stem and progenitor cells, which reside in the spleen. Monocytes produced in the bone marrow and the spleen further infiltrate tumors, where they differentiate into tumor-associated macrophages (TAMs). The relationship between chronic inflammation and hepatocarcinogenesis has been thoroughly investigated over the past decade; however, several aspects of the role of TAMs in HCC development are yet to be determined. In response to certain stimuli and signaling, monocytes differentiate into macrophages with antitumor properties, which are classified as M1-like. On the other hand, under different stimuli and signaling, the polarization of macrophages shifts towards an M2-like phenotype with a tumor promoting capacity. M2-like macrophages drive tumor growth both directly and indirectly, via the suppression of cytotoxic cell populations, including CD8+ T cells and NK cells. The tumor microenvironment affects the response to immunotherapies. Therefore, an enhanced understanding of its immunobiology is essential for the development of next-generation immunotherapies. The utilization of various monocyte-centered anticancer treatment modalities has been under clinical investigation, selectively targeting and modulating the processes of monocyte recruitment, activation and migration. This review summarizes the current evidence on the role of TAMs in HCC pathogenesis and progression, as well as in their potential involvement in tumor therapy, shedding light on emerging anticancer treatment methods targeting monocytes.
1. Introduction
Liver cancer is the sixth most commonly diagnosed cancer and the fourth leading cause of cancer-related death worldwide, while hepatocellular carcinoma (HCC) accounts for approximately 75–85% of primary liver cancers [1,2]. In the vast majority of cases, HCC arises as a result of sustained inflammatory damage, hepatocyte necrosis and regeneration in patients with liver cirrhosis [3]. The most common causes of liver cirrhosis that predispose patients to HCC are chronic hepatitis C virus (HCV), hepatitis B virus (HBV) and non-alcoholic fatty liver disease/non-alcoholic steatohepatitis (NAFLD/NASH) [4]. Despite major scientific advances, the majority of patients with HCC still face a dismal prognosis. Liver transplantation is only possible in patients with early HCC, whereas patients that undergo alternative treatment modalities—including liver resection or tumor ablation—develop recurrent disease in up to 70% of cases [5]. HCC prognosis fluctuates according to the stage at the time of diagnosis, with an overall 5-year survival rate of 20%. Patients who are not considered eligible for surgical or other curative procedures can receive palliative therapies, including tyrosine kinase inhibitors (TKI), such as sorafenib, lenvatinib, regorafenib or cabozantinib, or the VEGFR2-antibody ramucirumab [6,7,8,9]. However, these treatment options have minimal benefit in survival, increasing the necessity for novel therapeutic strategies for the treatment of HCC [10]. Recent evidence provided by Finn et al. showed that the use of the immune checkpoint inhibitor atezolizumab in combination with the antiangiogenic agent bevacizumab reduced mortality by 42% and decreased the risk of disease worsening or death by 41% compared to sorafenib alone, and it is currently accepted as the first-line systemic treatment of HCC [11]. Immunotherapies targeting the PD-1/PD-L1 axis, other than atezolizumab, have also been approved for the treatment of HCC without showing a major effect on patient survival [12]. Specifically, the efficacy of these agents is compromised in patients with NASH and this observation was linked to NASH-dependent altered immune cell function in TME [13].
Chronic liver inflammation drives a dysfunctional tissue repair process, leading to the formation of dysplastic nodules and, eventually, cancer [14,15]. The tumor microenvironment (TME) greatly contributes to the tolerogenic immune response towards HCC. It comprises myeloid-derived suppressor cells (MDSCs), tumor-associated macrophages (TAMs), tumor-associated neutrophils (TANs), cancer-associated fibroblasts (CAFs) and regulatory T cells (Tregs) [16,17,18]. MDSCs, either of monocytic or granulocytic origin, typically show immunosuppressive properties [19]. The liver bears the highest proportion of macrophages among all organs in the body [20], and in a healthy rodent liver, 20–40 macrophages accompany every 100 hepatocytes [21]. They are generally categorized into two distinct subsets that can be distinguished from each other based on their differential expression of cell surface markers. Kupffer cells (KCs) are the non-migratory tissue-resident macrophages of the liver, are located in the sinusoids and maintain homeostasis [22,23]. Monocyte-derived macrophages (MoMϕs) exert migratory capabilities and engraft liver tissue during inflammatory conditions or after KC depletion [24,25]. TAMs play an essential role in HCC pathogenesis, establishing a pro-inflammatory and pro-tumorigenic environment through the suppression of antitumor immune responses [26,27]. However, they can also participate in tumor immune surveillance and antitumor responses [28,29]. Given the major contribution of hepatic macrophages in normal tissue homeostasis, their pivotal role in liver inflammation and their dual promoting and inhibitory functions in tumor formation, hepatic macrophages have been at the forefront as potential therapeutic targets for various HCC treatment modalities [30].
This review summarizes the current state of knowledge regarding the involvement of TAMs in the pathogenesis and progression of HCC and the heterogeneity and plasticity that they exert in the cancer-associated microenvironment. We also highlight the principal future therapeutic options that target TAMs to treat HCC.
2. Monopoiesis and Tumor-Associated Monocytes
One of the main features of cancer is the tumor-associated chronic inflammation that results in the reprogramming of immune cells [31]. In addition to the immunomodulatory effect that this type of chronic inflammation elicits at the site of tumors, it has systemic effects, affecting cell populations in the bone marrow and spleen. One of these effects is the induction of emergency myelopoiesis, which results in the generation of mature cells of the myeloid lineage, including monocytes and neutrophils, that further infiltrate solid tumors and act mainly as immunosuppressive and tumor-promoting cells [32]. Hematopoietic stem and progenitor cells (HSPCs) and myeloid progenitors (MyP) can sense and are responsive to a variety of mediators that are released by tumor cells, such as granulocyte-colony stimulating factor (G-CSF), granulocyte macrophage (GM)-CSF or the chemokine CXCL-12 [33,34]. This results in their activation and differentiation towards a myeloid lineage, as well as in their mobilization and egress from the bone marrow and migration to extra medullary sites, such as the spleen [35].
Resident macrophages derive from the differentiation of progenitors in the yolk sack and fetal liver during early life, whereas bone marrow is the site of monocyte generation under steady state conditions [36]. Experiments in mice showed that monocytes derive from common myeloid progenitors, following two distinct differentiation pathways, giving rise to cells with different transcriptional programs and, probably, different functions [37]. Cancer-elicited inflammation promotes not only the generation of monocytes in the bone marrow in response to the myeloid-lineage growth factors GM-CSF, G-CSF and interleukin-6 (IL-6) [33], but also drives extramedullary monopoiesis in the spleen by mobilized HSPCs and MyP [38]. Indeed, both mice and patients with invasive cancer exhibited increased numbers of splenic granulocyte-macrophage progenitors (GMPs), which are able to generate monocytes, as well as neutrophils, that further infiltrate tumors and differentiate into TAMs and TANs, respectively [38]. The spleen is also a major site for the tumor-associated reprogramming of monocytes, which results in an accumulation of MDSCs, a monocytic cell population with potent immunosuppressive activity against CD8+ T cells [39]. For instance, a study by Jordan et al. showed that the accumulation of MDSCs of monocytic origin with T-cell-suppressive properties were observed in the spleens of patients with various types of cancer, including pancreatic and colorectal adenocarcinoma, pancreatic neuroendocrine tumors, melanoma or ovarian cancer [40]. Regarding HCC, increased numbers of hematopoietic progenitor cells, stained as CD133+, and CD11b+ myeloid cells were observed in the spleens of patients with HCC, as well as other tumors, compared to patients with cirrhosis, a condition that predisposes patients to HCC [41]. Interestingly, there was a positive correlation between the number of progenitor cells and mature myeloid cells, implying that extra medullary myelopoiesis was responsible for the generation of mature myeloid cells [41]. Taken together, enhanced myelopoiesis results in the generation of monocytic cells with immunosuppressive properties in the bone marrow and the spleen, which further migrate into tumors, where an additional step of reprogramming takes place during their differentiation to TAMs (Figure 1).
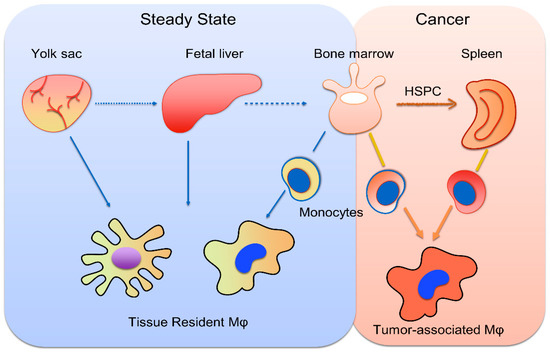
Figure 1.
Origins of tissue-resident and tumor-associated macrophages. Tissue-resident macrophages derive from the differentiation of yolk sac and fetal liver hematopoietic progenitors and, later in life, stem from the differentiation of monocytes, generated in the bone marrow. Cancer induces myelopoiesis in the bone marrow, as well as the mobilization of hematopoietic stem cells and progenitor cells (HSPCs), which reside in the spleen. Monocytes produced in the bone marrow and the spleen further infiltrate tumors, where they differentiate into tumor-associated macrophages.
3. Liver Macrophages and Their Plasticity in Response to the Tumor Microenvironment
Liver macrophages (Mϕs) are a heterogeneous cell population that includes resident Kupffer cells and MoMϕs. On histological examination, Kupffer cells share common morphological characteristics with the monocyte-derived cells, MoMϕs and dendritic cells, showing morphological variability in size and shape. Kupffer cells are identified on light microscopy by their location, as they are localized adjacent to sinusoids and play a crucial role in homeostasis. MoMϕs are observed in inflammatory sites, orchestrating the immune response to tissue injury or pathogens. Mϕs play a major role in the pathogenesis of inflammatory disorders, such as NASH, promoting liver inflammation and fibrosis [42,43], as discussed in elsewhere [43,44].
The microenvironment of HCC, which consists of CAFs, hepatic stellate cells (HSCs), endothelial cells and immune cells, as well as extracellular matrix proteins [45], shapes Mϕs, altering their function. TAMs actively participate in tumor-related inflammation, setting the crosstalk between tumor and stromal cells [46,47]. TAMs are MoMϕs that are recruited into the TME, mostly by chemokine (C-C motif) ligand 2 (CCL2) and macrophage (M)-CSF, and eventually differentiate into mature macrophages. The plasticity of TAMs enables them to exert either anti- or pro-tumor activity, depending on the distinct micro-environmental signals originating from tumor cells, fibroblasts, stroma and immunocompetent cells [48]. TAMs show similar morphological features to their normal counterparts, despite their structural and functional diversity, which is controlled by the tumor microenvironment [49]. Similar to liver Mϕs, TAMs are functionally heterogeneous. However, in most human studies, TAMs are characterized based on the expression of polarization markers as classically activated (M1) and alternatively activated (M2). Classically activated M1 macrophages have pro-inflammatory activity and macrophages polarize to this direction in response to treatment with lipopolysaccharides (LPS) and interferon-gamma (IFN-γ). M1 macrophages produce proinflammatory cytokines, such as interleukin (IL)-12, and have the potential to stimulate effector T-cell proliferation and function. They also exhibit strong microbicidal and tumoricidal activity by the production of reactive oxygen species (ROS) and nitric oxide synthase (iNOS; NOS2) that promotes arginine metabolism into nitric oxide (NO) and citrulline [50,51]. Alternative activation by IL4, IL-10 and IL-13 in vitro results in the generation of macrophages with immunosuppressive properties that produce IL-10, transforming growth factor beta (TGF-β) and chemokine (C-C motif) ligand (CCL) family members, such as CCL17, CCL18, CCL22 and CCL24, and express high levels of PD-L1 [27,52]. M2 macrophages initiate the Th2 immune response, promoting angiogenesis, tissue remodeling and repair [53,54].
Histologically, the distinction between M1 and M2 macrophages is based on immunohistochemistry. CD68 is a common monocytic marker expressed by TAMs, of both M1 and M2 phenotypes, and dendritic cells. M1 macrophages are positive for several markers, such as iNOS, CD80 and CD86, whereas the M2 polarization markers are CD163, CD204 and CD206 [55,56]. CD163, in addition to being a marker for M2 macrophages, is also expressed by Kupffer cells. Moreover, a population of tolerogenic dendritic cells has been recently identified in peripheral blood, namely DC-10, which expresses CD163, releases IL-10 and induces type-1 T regulatory cells [57]. CD163 expression is upregulated by IL-10, and CD163-positive cells secrete IL-10.
The TME is the driving force behind macrophage polarization in HCC, leading to the generation of macrophages with immunosuppressive properties. For instance, the TME is characterized by an acidic pH, triggering regulatory macrophages and enhancing immune evasion [58]. Yang et al. demonstrated that Wnt/β-catenin signaling drives macrophage differentiation towards the M2 phenotype and was highly expressed in c-Myc-driven M2-polarized macrophages. Inhibition of Wnt protein secretion in HCC hindered hepatic tumor growth by regulating the tumor immune microenvironment in mice, whereas nuclear accumulation of β-catenin was observed in M2-like TAMs in human HCC biopsies [59]. Moreover, Chen et al. demonstrated that TLR4-elicited innate monocyte inflammation was necessary for IL21+ T follicular helper (Tfh)-like cell induction in HCC, and activation of STAT1 and STAT3 was critical for TFH-like cell polarization. Importantly, the TFH-like cells operated in IL21-IFNγ-dependent pathways to induce plasma cell differentiation and, thereby, create conditions for pro-tumorigenic M2 macrophage polarization and cancer progression [60]. Similarly, intratumoral macrophages were associated with increased intratumoral FoxP3+ regulatory T cells (Tregs) and poor prognosis in patients with HCC, while in vivo depletion of tissue macrophages decreased the frequency of intratumoral immunosuppressive FoxP3+ Tregs [61]. To underline the multitude and the complementarity of the mechanisms of local HCC immunosuppression, it was recently deduced that selectively increased intrahepatic Tregs can promote an immunosuppressive environment in NASH livers. Neutrophil extracellular traps link innate and adaptive immunity by promoting Treg differentiation via the metabolic reprogramming of naïve CD4+ T-cells. This mechanism may explain, at least partly, the relative resistance of NASH-related HCC to current first-line immunotherapies and could be targeted to prevent or treat liver cancer in patients with NASH etiology [62]. On the other hand, the extracellular matrix protein SPON2 and its integrin receptors α4β1 play significant roles in the recruitment of the M1-like TAM subtype in the HCC microenvironment, functioning as an opsonin for macrophage phagocytosis, resulting in anti-tumor immune responses [63]. Additionally, expression of MiR206 by Kupffer cells drives M1 polarization and the recruitment of CD8+ T cells through CCL2 production in mice with HCC [64]. In addition to T cells, Liu et al. reported that TAMs interact with B cells, since CXCR3+ B cells drive M2 polarization in HCC through IL-17 production [65]. The IL-6/STAT3 signaling pathway was shown to regulate M1/M2 macrophage polarization, as its inhibition, mediated by anti-IL6, reduced cell viability and drug resistance, suppressed cell invasion and migration and induced apoptosis of HCC cells co-cultured with M1- or M2-type macrophages, resulting in suppressed tumor formation and lung metastases [66]. In addition, TLR4 on macrophages promoted the growth of steatohepatitis-related HCC in mice, as the number of macrophages expressing Ly6C was increased and these cells were associated with inflammation and tumor progression, generating increased amounts of IL-6 and TNFα in response to LPS [67]. On the contrary, IL-12 inhibited HCC proliferation and invasiveness in vitro by the induction of M1-like polarization of macrophages through the downregulation of Stat-3 [68]. Furthermore, a study by Wang et al. demonstrated that TGF-β recruits M2 macrophages in HCC, which are in turn polarized by connective tissue growth factor (CTGF, CCN2), a protein expressed by mesenchymal-like HCC cells. TGF-β acts as a chemoattractant, recruiting monocytes from the peripheral blood, while CTGF acts as a transformant, polarizing monocytes to M2 macrophages, stimulating tumor growth. In turn, M2 macrophages secrete CCL18, promoting HCC cell migration [69]. Finally, the transition of the macrophage phenotype from antitumorigenic to protumorigenic, which has been proven to be mediated by c-Jun N-terminal phosphorylation in the liver microenvironment, occurs before overt tumorigenesis, resulting mostly in the production of CCL17 and CCL22, thus facilitating HCC growth [70,71].
Even though the aforementioned studies suggest that TAMs can be polarized between the two extremes of macrophage phenotypes, recent studies using single cell approaches demonstrated that TAMs in HCC are characterized by vast heterogeneity. A seminal study by Zhang et al. generated a large body of information regarding immune cell populations in HCC and ascites using single cell RNAseq of CD45+ cells [72]. Among others, six clusters of macrophages with distinct gene expression modules were identified [72]. Interestingly, they identified a cluster of macrophages that simultaneously expressed genes of both M1 and M2 polarization states [72]. Song et al. also engaged a similar experimental approach in HBV/HCV-related hepatocellular carcinoma and identified eight clusters of myeloid cells, showing that there is heterogeneity within macrophage populations, with a high number of macrophages sharing both M1 and M2 characteristics [73]. Among the different macrophage clusters, a cluster of CCL18-expressing macrophages with M2 features was identified that was associated with a worse clinical outcome [73]. In the same study, a population of XCL1+ CD8+ T cells was identified that was capable of recruiting dendritic cells, which resulted in an enhanced anti-tumor response, suggesting an interaction between T cells and myeloid cells [73]. In addition to the heterogenicity at the single cell level, it has been shown that immune cell infiltrates are distinct in intrahepatic metastatic lesions in multifocal HCC compared to multicentric occurrence, since more M2 macrophages and less T cells are observed in metastases [74] (Figure 2).
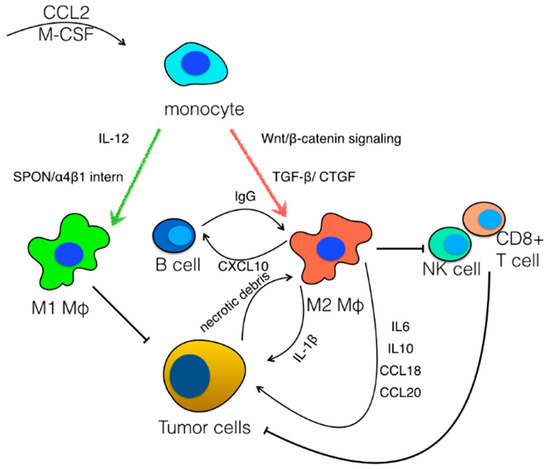
Figure 2.
Polarization of tumor-associated macrophages. Macrophage colony-stimulating factor (M-CSF) and C–C motif chemokine ligand 2 (CCL2) drive the generation of monocytes in cancer. In response to IL-12 and SPON/α4β1 signaling, monocytes differentiate into macrophages with antitumor properties, which are classified as M1-like. On the other hand, Wnt/β-catenin signaling, the TGF-β/CTGF pathway, necrotic debris from tumor cells and immunoglobulins released by B cells facilitate the polarization of macrophages towards a M2-like phenotype with tumor promoting properties. M2-like macrophages drive tumor growth directly, through the release of IL-1β, IL-6, IL-10, CCL18 and CCL20, and indirectly, via the suppression of cytotoxic cell populations, including CD8+ T cells and NK cells.
4. The Role of Macrophages in HCC Pathogenesis
The involvement of macrophages in the pathogenesis and development of HCC is crucial. Zhang et al. found that M2 macrophages increased the proliferation, migration and invasion of HCC cells through a fatty acid oxidation (FAO)-dependent process. Specifically, IL-1β instigated the pro-migratory effect of M2 cells, and FAO was responsible for the upregulated secretion of IL-1β, which depended on ROS and NLRP3 inflammasome [75]. A study on the diethylnitrosamine (DEN)-induced model of carcinogenesis engaged in transcriptomic analysis and demonstrated that MoMϕs acquire a proinflammatory phenotype during carcinogenesis in this model, which is, however, distinct from the mixed pro-inflammatory and immunosuppressive phenotype of cells from the NASH-induced carcinogenesis model [76]. This observation implies that there are diverse mechanisms in the response of immune cells to liver carcinogenesis in different animal models. Schneider et al. also demonstrated that DEN-induced hepatocarcinogenesis triggers liver inflammation with an intrahepatic accumulation of macrophages and cytotoxic T cells. Interestingly, the increased macrophage accumulation in chemokine scavenger receptor D6-deficient mice did not have an impact on HCC progression [77]. TAMs have also been linked to HCC growth stimulation via STAT3 signaling, while IL-6 release by macrophages was demonstrated to enhance HCC proliferation and migration [78]. Furthermore, evidence has been provided that chemokine CCL2/chemokine receptor CCR2-dependent signaling mechanisms participate in the process of HCC development. The levels of CCL2 are increased in patients with HCC and have been associated with poor prognosis [79]. In murine liver cancer models, CCR2+ myeloid cells exhibited dual functions. Before cancer initiation, CCR2+ myeloid cells suppressed tumorigenesis by removing senescent hepatocytes. However, when HCC was established, tumor cells inhibited the differentiation of infiltrating CCR2+ immature myeloid cells, which in turn promoted tumor growth, via the inhibition of NK cells. In a model of NASH-dependent HCC, CCR2 depletion had no distinct effect on HCC tumorigenesis, suggesting that the effect of CCR2 in hepatocarcinogenesis is dependent on disease etiology [80]. Guo et al. also provided evidence that infiltrating M2-TAMs were markedly elevated in the HCC TME, producing IL-17, a pro-inflammatory cytokine, and were augmented upon oxaliplatin treatment [81]. IL-17A, secreted in concert from lymphatic endothelial cells, promotes tumorigenesis by upregulation of PD-L1 in hepatoma stem cells [82]. Regarding HCC metastasis, it was demonstrated that the exosome-mediated transfer of the functional protein CD11b/CD18 (integrin αMβ2) from TAMs to tumor cells may have the potency to boost the migratory potential of HCC cells [83].
In addition, inhibition of the CCL2/CCR2 axis resulted in the blockade of monocyte recruitment, M2 polarization and, as a result, inhibition of the CD8+ T-cell-mediated antitumor response [84]. Zhang et al. demonstrated that the hypoxia inducible factor (HIF)-1α /IL-1β feedback loop between tumor cells and TAMs in the hypoxic TME resulted in the epithelial–mesenchymal transition of cancer cells and metastasis in vitro. Specifically, they found that TAMs secreted increased amounts of IL-1β under moderate hypoxic conditions, due to the increased stability of HIF-1α, and that the necrotic debris of HCC cells increased IL-1β release by TAMs with an M2 phenotype, via TLR4/TRIF/NF-κB signaling [85]. Moreover, Zhao et al. observed a positive association between B7-H1+ monocyte/Mφ and IL-17-producing cell density in the peritumoral stroma of HCC patients and that the IL-17-exposed macrophages suppressed cytotoxic T-cell function through B7-H1/PD-1 interactions [86]. CD48/2B4 interactions mediated a high level of infiltration of peritumoral macrophages, which was correlated with the decreased activity of NK cells in HCC tissues [87]. Furthermore, IL-23 generation by liver CD14+ inflammatory macrophages in response to infected hepatocytes during chronic HBV was shown to alter macrophage function, favoring HCC growth [88] (Table 1).

Table 1.
Summary of studies evaluating the role of TAMs in HCC pathogenesis.
5. Macrophages in HCC Prognosis
The prognostic role of the proportion of M1 and M2 macrophages, as well as their ratio, have been reported in several tumors [91,92], including HCC [93]. M2 macrophages are implicated in the “exhausted immune response” subclass of HCC and are correlated with adverse prognosis [93,94]. The method for their quantification differs and is not comparable between studies. Density estimation, as reflected by the number/mm2, seems to be the most reliable method. Histologic distribution of TAMs and their subtypes, in the center of the tumor or the invasive front, has been proposed to have an independent prognostic value in several solid tumors [95,96]. Τhe histological evaluation of the invasive front is preferable to be performed in surgical specimens. Further research related to macrophage phenotypes and their ratios, in conjunction with their spatial location in the tumor specimens, can facilitate a better understanding of their biological behavior in HCC.
Recent evidence suggests that miR-148b deficiency promotes HCC growth and metastasis through colony-stimulating factor-1 (M-CSF)/CSF1 receptor (CSF1R)-mediated TAM infiltration, while HCC patients with decreased miR-148b levels and increased TAM infiltration were correlated with worse prognosis [97]. Moreover, Chen et al. reported that monocytes engage in glycolysis at the peritumoral region of human HCC, inducing PD-L1 expression and attenuating cytotoxic T lymphocyte responses in cancer. Tumor-derived soluble factors upregulated PFKFB3 expression in TAMs, which in turn mediated the increased expression of PD-L1 by the activation of the NF-kB signaling pathway. Interestingly, the degree of CD68 + PFKFB3 + PD-L1 + monocyte-macrophage infiltration in peritumoral tissues was negatively associated with the overall survival of HCC patients and could serve as an independent prognostic factor for patients with HCC [98]. In addition, Li et al. demonstrated that the downregulation of SIRT4 was correlated with increased macrophage infiltration and M2-like TAMs in HCC peritumoral tissues and, consequently, with poor survival of HCC patients. SIRT4 expression was decreased in macrophages in HCC, driving M2 polarization in a FAO-PPARδ-STAT3-dependent signaling pathway, while silencing SIRT4 increased IL-6 production in TAMs. Moreover, SIRT4 silencing also resulted in M1 macrophage apoptosis due to enhanced IL-10 production in HCC peritumoral tissues [99]. Along the same line, high-mobility group protein box1 (HMGB1) expression, which is linked to increased secretion of IL-1β, IFN-γ and TNF-α, was associated with peritumoral TAM infiltration and poor prognosis in patients with HCC. High peritumoral HMGB1 expression and TAM numbers were positively correlated with tumor size and BCLC stage and acted as independent prognostic factors for the overall survival (OS) and recurrence free survival (RFS) in patients with HCC [100]. Furthermore, Zhao et al. provided evidence that the expression of macrophage migration inhibitory factor (MIF) in tumors was positively correlated with plasma MIF levels, which had a higher value for the diagnosis of HCC compared to serum a-fetoprotein (AFP). In fact, plasma MIF levels demonstrated a significant correlation with the OS and disease-free survival (DFS) of HCC patients, even in those with normal serum AFP levels and tumor-node-metastasis (TNM) stage I. In addition, the plasma MIF levels were identified as an independent factor for OS and DFS and decreased significantly within 30 days after HCC resection [101]. Another study further reported that M-CSF density and the CD163 and CD31 indices in peritumoral tissues were predictable factors for time to recurrence, DFS and OS in patients with HCC, while M-CSF was involved in the progression of hepatocellular carcinoma after curative resection [102]. Moreover, hepatocellular tumors with increased intratumoral CD204, as well as monocarboxylate transporter-4 (MCT4)-positive macrophages and MCT4-postive expressing HCC cells, were associated with an unfavorable patient outcome [103].
Another study by Zhu et al. revealed that CD206 was highly expressed in the HCC tissues compared to its peri-carcinoma tissue levels, while GdCl3 treatment suppressed the malignant potential of HCC in vitro and in vivo, mainly by downregulating the expression of CD206 in M2 macrophages, indicating the potential significance of CD206 as a biomarker for HCC prognosis [104]. Similarly, high expression of peritumoral M-CSF and the density of macrophages, which correlated with a large tumor size, presence of intrahepatic metastasis and a high TNM stage, were associated with HCC progression, disease recurrence and poor survival after curative hepatectomy [105], while the combination of tumor-derived osteopontin (OPN) and peritumoral infiltrating macrophages was associated with a high incidence of early recurrence and poor survival for early-stage HCC, after curative resection [106]. A study by Zhou et al. demonstrated that Yes-Associated Protein (YAP) activation was critical for the recruitment of TAMs towards HCC cells, as IL-6 secreted by YAP-activated HCC cells induced TAM recruitment. Together with their findings that the expression levels of IL-6 in human HCC tumors were highly associated with the prognosis of HCC patients, they highlighted the possibility of improving HCC treatment by targeting YAP-IL-6-mediated TAM recruitment [107]. In addition, evidence has been provided that macrophages contribute to the decreased expression of E-cadherin in HCC via the NF–κB/Slug pathway, leading to increased tumor invasiveness and metastasis [108] (Table 2).

Table 2.
Summary of studies evaluating the role of TAMs in HCC prognosis.
6. The Potential Role of Macrophages in HCC Treatment
The implication of macrophages in various HCC treatment modalities has been at the forefront of clinical investigation, as various preclinical studies in animal models suggest that macrophages can play a pivotal role in HCC therapy. For instance, macrophage depletion by clodrolip or zoledronic acid, in combination with sorafenib, significantly inhibited HCC progression, tumor angiogenesis and lung metastasis in mice [109]. In addition, sorafenib administration at a subpharmacologic dose, augmented the antitumor effects of mouse chimeric antigen receptor CAR-T cells, partly by promoting IL12 secretion from TAMs [110]. Along the same line, there is evidence that sorafenib triggers the proinflammatory activity of TAMs, reverts their alternative polarization, enhancing IL12 secretion, and, as a result, induces antitumor NK cell responses in a cytokine- and NF-kB-dependent fashion [111]. This ability of sorafenib to partially inhibit M2-cell activation in vivo was shown by a study by Sprinzl et al. [112]. Another study by Yao et al. indicated that a natural CCR2 antagonist potentiated TAM-mediated tumor immunosuppression and enhanced the therapeutic effect of sorafenib, indicating that the combination of an immunomodulator with a chemotherapeutic drug could be a therapeutic approach for HCC [113]. Macrophage modulation could also potentiate the anti-cancer activity of sorafenib. In addition, it has been shown that sorafenib inhibits the macrophage-mediated epithelial–mesenchymal transition in HCC via the HGF-Met signaling pathway in vitro, while sorafenib therapy reduced plasma HGF and alpha-fetoprotein concentrations in patients with HCC [114]. Finally, it inhibited miR-101 expression and enhanced DUSP1 expression and downregulated the release of TGF-β and the expression of CD206 in M2 cells, suppressing the macrophage-mediated growth of HCC [115].
A study by Yang et al. identified that 17β-estradiol (E2) could suppress HCC growth via regulation of macrophage polarization, as E2 re-administration reduced tumor growth in orthotopic and ectopic mouse HCC models, functioning as an inhibitor of macrophage alternative activation and tumor progression, by keeping estrogen receptor-β (ERβ) away from interacting with ATP5J and hindering the JAK1-STAT6 signaling pathway [116]. Moreover, delivery of recombinant adenovirus vector (rAd) expressing monocyte chemoattractant protein-1 (MCP-1) was demonstrated to potentiate the antitumor effects of suicide gene therapy against HCC by M1 macrophage activation, suggesting its potential use as a method of cancer gene therapy against HCC progression and recurrence [117]. Guerra et al. also demonstrated that, in response to HCC cells, hydrogel-embedded M1 macrophages upregulated nitrite and TNF-α, activating caspase-3-induced apoptosis in the tumor cells, leading to tumor regression in vivo [118]. It is also worth mentioning that small interfering RNA (siRNA)-mediated knockdown of MIF suppressed cyclin D1 expression and HCC cell proliferation, inducing tumor-cell apoptosis [119], while antibody mediated therapy targeting CD47 inhibited HCC progression, promoting the migration of macrophages into the tumor mass and the subsequent phagocytosis of HCC cells [120]. Tan et al. provided evidence that IRE1α mediated the inhibition of TAM activation by genipin in HCC, suppressing its growth, while the reduced association of IRE1α-TRAF2-IKK might have been responsible for a genipin-regulated inactivation of NF-κB [121]. Furthermore, co-administration of glycyrrhizin and doxorubicin by alginate nanogel particles was demonstrated to diminish the activation of macrophages through the regulation of the apoptosis pathway, via altering the Bax/Bcl-2 ratio and caspase-3 activity, enhancing the therapeutic efficacy for HCC [122]. Moreover, nanoliposome C6-ceramide (LipC6) was demonstrated to enhance the anti-tumor immune response and hinder HCC growth in mice, reducing the number of TAMs and their ability to suppress the anti-tumor immune response, allowing LipC6, a potential chemotherapeutic agent, to increase the efficacy of immune therapy in patients with HCC [123]. An additional in vivo study provided evidence that the strategy of low doses and multiple treatments of nsPEF was superior to a high dose of a single treatment, as macrophage infiltration was markedly elevated in tumors that were treated by multiple low dose nsPEFs [124]. Finally, nanosecond pulsed electric field (nsPEF), a technology targeting tumor cells with a non-thermal high-voltage electric field using ultra-short pulses, increased HCC cell phagocytosis by human macrophage cells (THP1) in vitro [125] (Table 3).

Table 3.
Summary of studies evaluating the role of TAMs in HCC therapy.
Recent advances in tissue engineering research enabled the construction of three-dimensional (3D) in vitro tissue models, in order to recapitulate the TME without engaging in vivo animal models. In these 3D culture systems, different types of cancer cells and cells that form the TME, including CAFs and TAMs, are combined providing valuable tools for the discovery of new drugs [126,127]. This type of experimental approach has already been used in a model of lung carcinoma to test whether treatment can alter TAM density and spatial distribution and it revealed that the treatment had an important effect on the latter [128]. Regarding HCC, hydrogels loaded with M1-polarized macrophages had a tumor suppressing potential both in vitro and in vivo [118].
7. Critical Analysis of Data and Future Perspectives
The landscape and dynamics of macrophages have been studied alongside other cell populations in human HCC multiple tissue compartments using single cell-RNA sequencing analysis [72]. It was identified that the enrichment of TAM gene signatures was significantly associated with a survival disadvantage in HCC, rendering this type of tumor-infiltrating TAMs potential cellular candidates for therapeutic targeting in the TME. Importantly, two genes, SLC40A1, encoding ferroportin, and GPNMB, encoding type I transmembrane glycoprotein, were highly expressed as potential markers in these TAM-like cells. Furthermore, in a second human study of an early HCC relapse ecosystem, a different innate-like CD8+ T cell population was described by single-cell profiling in recurrent tumors. These T cells were overexpressing the CD161 surface marker and displaying an innate-like low cytotoxic state, with low clonal expansion, unlike the classical CD8+ T cell exhausted state observed in primary HCC. The selective relative enrichment of these cells in the TME was associated with a worse prognosis in patients [129]. These unique aspects of altered immune response associated with HCC relapse relative to the primary tumor underline the HCC immune micro-ecosystem complexity of heterogeneous spatiotemporal interactions between and within cell types, which may guide the development of rational precision oncology immune therapies, benefiting a wide range of patients.
In accordance with the above, the HCC microenvironment in human patients and mice is characterized by functionally distinct macrophage populations. There are four possible main interventions for TAM-based antitumor therapy: inhibition of macrophage recruitment, induction of TAM death or apoptosis, enhancement of M1 antitumoral activity of TAMs and, last but not least, inhibition of the functional axes of M2 tumor-promoting activity of TAMs. In addition, functional subsets of TAMs were analyzed in human HCC samples and, in a combined fibrosis–HCC mouse model, demonstrated that human CCR2+ TAMs accumulated at the highly vascularized HCC border and expressed the inflammatory marker S100A9, whereas a second subset of CD163+ immune-suppressive TAMs accumulated in the HCC epicenter. Inhibition of CCR2+ TAM infiltration using a CCL2 antagonist in the fibrosis–HCC model significantly reduced pathogenic angiogenesis alongside tumor growth [90]. Moreover, the dual CCR2/CCR5 inhibitor cenicriviroc is currently under phase 3 clinical trial evaluation in patients with NASH and advanced fibrosis, representing a high-risk group for liver cancer [130]. However, the exact role of CCR2 and CCR5 in macrophage function in the liver is rather obscure. Recently, it was demonstrated that both CCR2 and CCR5 deficiency/inhibition led to reduced fibrosis, and sole CCR5 deficiency increased steatosis and the incidence of HCC in the model of NEMO LPC-KO mice. While CCR2 controlled the recruitment of monocytes to injured livers, CCR5+ macrophages limited liver injury in NEMOLPC-KO mice (CCR5-dependent differential function), thereby reducing steatosis and hepatocarcinogenesis [131]. In the hypoxic environment of HCC, HIF-1a enhanced the expression of triggering receptor expressed on myeloid cells-1 (TREM-1) in TAMs, leading to immunosuppression through the impairment of the cytotoxic functions of CD8+ T cells. Mechanistically, TREM-1+ TAMs increased the expression of CCL20 via the extracellular signal-regulated kinase/NF-κβ pathway in response to hypoxia and tumor metabolites leading to CCR6+ Foxp3+ Treg accumulation. Inhibition of the TREM-1 pathway could hinder tumor progression, reduce CCR6+ Foxp3+ Treg recruitment and improve the therapeutic efficacy of PD-L1 blockade [132].
It has been also indicated that the function of CCR2+ myeloid cells depends on the developmental stage of liver tumors. Precancerous senescent hepatocytes produce CCL2, which attracts macrophages, eliminating precancerous lesions (antitumoral effect), while established HCCs can also attract monocytic macrophages, which can, in turn, block the antitumor activity of NK cells (tumor-promoting effect) [79]. It has also been shown that selective blocking of CCR5 induces antitumoral macrophage polarization, and anti-CCR5 therapy was reported to be efficient in treating metastases [133]. Therefore, a critical review of the aforementioned data indicates that not all patients with HCC might eventually benefit from a selective CCR2- or CCR5-directed axis-inhibiting tumor therapy, while combined CCR2 and CCR5 inhibition is only beneficial for certain subgroups of patients with HCC. Due to the complicated nature of myeloid inflammation, multiple target inhibition might be necessary in order to overcome myeloid-mediated immune suppression. In this context, it was found that GM-CSF- and TNFa-producing CD206+ macrophages accumulated in human fibrotic liver. GM-CSF potentiated monocytes to CD206+ macrophage conversion, while anti-GM-CSF therapy suppressed liver fibrosis and CD206+ macrophage accumulation [134]. Furthermore, it was identified that tumor-derived GM-CSF was the primary regulator of myeloid cell ARG1 expression and local immune suppression. STAT3, p38 mitogen-activated protein kinases and acid signaling through cAMP were required to activate myeloid cell ARG1 expression in a STAT6-independent manner. A blockade of the tumor-derived GM-CSF enhanced the efficacy of tumor-specific adaptive T-cell therapy and immune checkpoint blockade [135]. Taken together, it seems that either monocyte or tumor cell–derived GM-CSF significantly contributed to the development of the immunosuppressive TME by regulating myeloid cell ARG1 expression and could serve as a target in order to enhance the efficacy of cancer immunotherapy.
There are currently several clinical trials investigating the use of monoclonal antibodies to inhibit GM-CSF or GM-CSFR in patients with various diseases. In a completed phase IIb study, a 24-week treatment with mavrilimumab, a human monoclonal antibody targeting the GM-CSFR a-chain, significantly reduced rheumatoid arthritis disease activity compared to placebo [136]. Moreover, GSK3196165, a human monoclonal antibody inhibiting GM-CSF, has also shown evidence of rapid favorable clinical responses in a phase Ib/IIa trial of patients with moderate RA [137]. In addition, it was demonstrated that GM-CSF neutralization with lenzilumab results in the reduction of neuro-inflammation and cytokine release syndrome in a primary acute lymphoblastic leukemia patient-derived xenograft model following chimeric antigen receptor T-cell therapy [138]. Furthermore, a phase ΙΙΙ trial is underway, investigating the potential use of lenzilumab to improve the likelihood of ventilator-free survival beyond standard supportive care, in hospitalized patients with severe SARS-CoV-2 [139]. Along the same line, recent evidence from studies of human and transplant mouse melanomas implicate CSF1 induction as a CD8+ T-cell–dependent adaptive resistance mechanism and demonstrate that simultaneous CSF1R targeting might be beneficial in melanomas refractory to immune checkpoint blockade and potentially, in other T-cell–based therapies [140]. Future findings from those ongoing trials and studies could provide insight into the potential use of GM-CSF-targeted therapies for the treatment of patients with HCC. Finally, subsets of tumor-associated innate immune cells, macrophages and neutrophils in particular, suppress the cytotoxic activity of innate and adaptive immune cells and interact with tumor cells to promote tumor growth and metastasis, suggesting that selectively targeting these sub-populations of TAMs and TANs holds therapeutic promise in treating metastatic disease [141].
8. Conclusions
Monocytes are highly adaptive cells that are influenced by the cytokine-chemokine milieu and are subsequently transformed by signals encountered upon entry into a tissue niche. Due to myeloid cell complexity and diversity, we are still far from understanding the complete set of internal and external signals that are sufficient to establish any particular monocyte-macrophage phenotype in the TME. Given the pro-metastatic role of monocytes in HCC, these shifts seem to have functional outcomes influencing disease state, rather than being simply epiphenomenal markers of the tumor and systemic environment.
Broadening our knowledge on how different signaling pathways regarding the recruitment and differentiation of monocytes interact with lineage-determining transcription factors, and how these factors interact with the overlaid differentiation factors within blood and tissue in cancer, might potentially enable us to intervene and define cell fate or phenotype for therapeutic purposes. Thus, insight into intra- and inter-cellular crosstalk may better showcase the role of monocytes and macrophages in tumor immunity. Some of these cells hinder tumor growth and are essential in effective tumor therapies, particularly immunotherapy. Such a delicate balance argues against systemic elimination of cells using a generic cell-type marker. It should also be emphasized that myeloid cells crosstalk with each other, and in many instances when one cell-type is removed (TAMs), there may be a subsequent increase of another (TANs). These complex cellular interactions within the TME, as well as those between the acquired and innate immune systems, although incompletely understood, should be at the forefront of future investigation, as immunotherapy is undoubtedly promising. A better understanding of the mechanisms and axes controlling tumor context-specific monocytes and tissue-resident macrophage phenotypes, is essential for the rational development of methods that can favorably alter their functions in HCC.
Author Contributions
Conceptualization, G.G. and I.M.; investigation, K.A. and I.M.; resources, K.A. and T.K.; data curation, K.A. and I.M.; writing—original draft preparation, K.A., T.K. and I.M.; writing—review and editing, K.A., I.M., T.K. and G.G.; visualization, G.G.; supervision, I.M. and G.G.; project administration, I.M. and G.G. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef] [PubMed]
- Global Burden of Disease Liver Cancer Collaboration; Akinyemiju, T.; Abera, S.F.; Ahmed, M.B.; Alam, N.; Alemayohu, M.A.; Allen, C.; Alraddadi, R.; Alvisguzman, N.; Amoako, Y.; et al. The Burden of Primary Liver Cancer and Underlying Etiologies From 1990 to 2015 at the Global, Regional, and National Level: Results From the Global Burden of Disease Study 2015. JAMA Oncol. 2017, 3, 1683–1691. [Google Scholar] [PubMed]
- Fattovich, G.; Stroffolini, T.; Zagni, I.; Donato, F. Hepatocellular carcinoma in cirrhosis: Incidence and risk factors. Gastroenterology 2004, 127, S35–S50. [Google Scholar] [CrossRef]
- Kew, M. Hepatocellular carcinoma: Epidemiology and risk factors. J. Hepatocell. Carcinoma 2014, 1, 115–125. [Google Scholar] [CrossRef]
- Bruix, J.; Takayama, T.; Mazzaferro, V.; Chau, G.-Y.; Yang, J.; Kudo, M.; Cai, J.; Poon, R.T.; Han, K.-H.; Tak, W.Y.; et al. Adjuvant sorafenib for hepatocellular carcinoma after resection or ablation (STORM): A phase 3, randomised, double-blind, placebo-controlled trial. Lancet Oncol. 2015, 16, 1344–1354. [Google Scholar] [CrossRef]
- Abou-Alfa, G.K.; Meyer, T.; Cheng, A.-L.; El-Khoueiry, A.B.; Rimassa, L.; Ryoo, B.-Y.; Cicin, I.; Merle, P.; Chen, Y.; Park, J.-W.; et al. Cabozantinib in Patients with Advanced and Progressing Hepatocellular Carcinoma. N. Engl. J. Med. 2018, 379, 54–63. [Google Scholar] [CrossRef]
- Bruix, J.; Qin, S.; Merle, P.; Granito, A.; Huang, Y.-H.; Bodoky, G.; Pracht, M.; Yokosuka, O.; Rosmorduc, O.; Breder, V.; et al. Regorafenib for patients with hepatocellular carcinoma who progressed on sorafenib treatment (RESORCE): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 2017, 389, 56–66. [Google Scholar] [CrossRef]
- Kudo, M.; Finn, R.S.; Qin, S.; Han, K.-H.; Ikeda, K.; Piscaglia, F.; Baron, A.; Park, J.-W.; Han, G.; Jassem, J.; et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: A randomised phase 3 non-inferiority trial. Lancet 2018, 391, 1163–1173. [Google Scholar] [CrossRef]
- Llovet, J.M.; Ricci, S.; Mazzaferro, V.; Hilgard, P.; Gane, E.; Blanc, J.-F.; De Oliveira, A.C.; Santoro, A.; Raoul, J.-L.; Forner, A.; et al. Sorafenib in Advanced Hepatocellular Carcinoma. N. Engl. J. Med. 2008, 359, 378–390. [Google Scholar] [CrossRef] [PubMed]
- Parikh, N.D.; Singal, A.G.; Hutton, D.W. Cost effectiveness of regorafenib as second-line therapy for patients with advanced hepatocellular carcinoma. Cancer 2017, 123, 3725–3731. [Google Scholar] [CrossRef]
- Finn, R.S.; Qin, S.; Ikeda, M.; Galle, P.R.; Ducreux, M.; Kim, T.-Y.; Kudo, M.; Breder, V.; Merle, P.; Kaseb, A.O.; et al. Atezolizumab plus Bevacizumab in Unresectable Hepatocellular Carcinoma. N. Engl. J. Med. 2020, 382, 1894–1905. [Google Scholar] [CrossRef]
- Pinter, M.; Scheiner, B.; Peck-Radosavljevic, M. Immunotherapy for advanced hepatocellular carcinoma: A focus on special subgroups. Gut 2021, 70, 204–214. [Google Scholar] [CrossRef] [PubMed]
- Pfister, D.; Núñez, N.G.; Pinyol, R.; Govaere, O.; Pinter, M.; Szydlowska, M.; Gupta, R.; Qiu, M.; Deczkowska, A.; Weiner, A.; et al. NASH limits anti-tumour surveillance in immunotherapy-treated HCC. Nature 2021, 592, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Albillos, A.; Lario, M.; Álvarez-Mon, M. Cirrhosis-associated immune dysfunction: Distinctive features and clinical relevance. J. Hepatol. 2014, 61, 1385–1396. [Google Scholar] [CrossRef] [PubMed]
- Aravalli, R.N. Role of innate immunity in the development of hepatocellular carcinoma. World J. Gastroenterol. 2013, 19, 7500–7514. [Google Scholar] [CrossRef]
- Binnewies, M.; Roberts, E.W.; Kersten, K.; Chan, V.; Fearon, D.F.; Merad, M.; Coussens, L.M.; Gabrilovich, D.I.; Ostrand-Rosenberg, S.; Hedrick, C.C.; et al. Understanding the tumor immune microenvironment (TIME) for effective therapy. Nat. Med. 2018, 24, 541–550. [Google Scholar] [CrossRef]
- Li, X.-F.; Chen, D.-P.; Ouyang, F.-Z.; Chen, M.-M.; Wu, Y.; Kuang, D.-M.; Zheng, L. Increased autophagy sustains the survival and pro-tumourigenic effects of neutrophils in human hepatocellular carcinoma. J. Hepatol. 2015, 62, 131–139. [Google Scholar] [CrossRef]
- Rizvi, S.; Wang, J.; El-Khoueiry, A.B. Liver Cancer Immunity. Hepatology 2021, 73 (Suppl. S1), 86–103. [Google Scholar] [CrossRef]
- Veglia, F.; Perego, M.; Gabrilovich, D. Myeloid-derived suppressor cells coming of age. Nat. Immunol. 2018, 19, 108–119. [Google Scholar] [CrossRef]
- Guilliams, M.; Dutertre, C.-A.; Scott, C.L.; McGovern, N.; Sichien, D.; Chakarov, S.; Van Gassen, S.; Chen, J.; Poidinger, M.; De Prijck, S.; et al. Unsupervised High-Dimensional Analysis Aligns Dendritic Cells across Tissues and Species. Immunity 2016, 45, 669–684. [Google Scholar] [CrossRef]
- Lopez, B.G.; Tsai, M.S.; Baratta, J.L.; Longmuir, K.J.; Robertson, R.T. Characterization of Kupffer cells in livers of developing mice. Comp. Hepatol. 2011, 10, 2. [Google Scholar] [CrossRef] [PubMed]
- David, B.A.; Rezende, R.M.; Antunes, M.; Santos, M.M.; Lopes, M.A.F.; Diniz, A.B.; Pereira, R.V.S.; Marchesi, S.C.; Alvarenga, D.M.; Nakagaki, B.N.; et al. Combination of Mass Cytometry and Imaging Analysis Reveals Origin, Location, and Functional Repopulation of Liver Myeloid Cells in Mice. Gastroenterology 2016, 151, 1176–1191. [Google Scholar] [CrossRef] [PubMed]
- Surewaard, B.G.; Kubes, P. Measurement of bacterial capture and phagosome maturation of Kupffer cells by intravital microscopy. Methods 2017, 128, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Mossanen, J.C.; Krenkel, O.; Ergen, C.; Govaere, O.; Liepelt, A.; Puengel, T.; Heymann, F.; Kalthoff, S.; Lefebvre, E.; Eulberg, D.; et al. Chemokine (C-C motif) receptor 2-positive monocytes aggravate the early phase of acetaminophen-induced acute liver injury. Hepatology 2016, 64, 1667–1682. [Google Scholar] [CrossRef]
- Scott, C.; Zheng, F.; De Baetselier, P.; Martens, L.; Saeys, Y.; De Prijck, S.; Lippens, S.; Abels, C.; Schoonooghe, S.; Raes, G.; et al. Bone marrow-derived monocytes give rise to self-renewing and fully differentiated Kupffer cells. Nat. Commun. 2016, 7, 10321. [Google Scholar] [CrossRef]
- Ritz, T.; Krenkel, O.; Tacke, F. Dynamic plasticity of macrophage functions in diseased liver. Cell. Immunol. 2018, 330, 175–182. [Google Scholar] [CrossRef]
- Wan, S.; Kuo, N.; Kryczek, I.; Zou, W.; Welling, T.H. Myeloid cells in hepatocellular carcinoma. Hepatology 2015, 62, 1304–1312. [Google Scholar] [CrossRef]
- Kang, T.-W.; Yevsa, T.; Woller, N.; Hoenicke, L.; Wuestefeld, T.; Dauch, D.; Hohmeyer, A.; Gereke, M.; Rudalska, R.; Potapova, A.; et al. Senescence surveillance of pre-malignant hepatocytes limits liver cancer development. Nature 2011, 479, 547–551. [Google Scholar] [CrossRef]
- Mossanen, J.C.; Tacke, F. Role of lymphocytes in liver cancer. OncoImmunology 2013, 2, e26468. [Google Scholar] [CrossRef]
- Man, K.; Ng, K.T.; Xu, A.; Cheng, Q.; Lo, C.M.; Xiao, J.W.; Sun, B.S.; Lim, Z.X.; Cheung, J.S.; Wu, E.X.; et al. Suppression of Liver Tumor Growth and Metastasis by Adiponectin in Nude Mice through Inhibition of Tumor Angiogenesis and Downregulation of Rho Kinase/IFN-Inducible Protein 10/Matrix Metalloproteinase 9 Signaling. Clin. Cancer Res. 2010, 16, 967–977. [Google Scholar] [CrossRef]
- Coussens, L.M.; Zitvogel, L.; Palucka, A.K. Neutralizing Tumor-Promoting Chronic Inflammation: A Magic Bullet? Science 2013, 339, 286–291. [Google Scholar] [CrossRef]
- Gabrilovich, D.I.; Ostrand-Rosenberg, S.; Bronte, V. Coordinated regulation of myeloid cells by tumours. Nat. Rev. Immunol. 2012, 12, 253–268. [Google Scholar] [CrossRef] [PubMed]
- Marigo, I.; Bosio, E.; Solito, S.; Mesa, C.; Fernandez, A.; Dolcetti, L.; Ugel, S.; Sonda, N.; Bicciato, S.; Falisi, E.; et al. Tumor-Induced Tolerance and Immune Suppression Depend on the C/EBPβ Transcription Factor. Immunity 2010, 32, 790–802. [Google Scholar] [CrossRef]
- McAllister, S.S.; Weinberg, R.A. The tumour-induced systemic environment as a critical regulator of cancer progression and metastasis. Nat. Cell Biol. 2014, 16, 717–727. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.-C.; Sun, H.-W.; Chen, H.-T.; Liang, J.; Yu, X.-J.; Wu, C.; Wang, Z.; Zheng, L. Circulating hematopoietic stem and progenitor cells are myeloid-biased in cancer patients. Proc. Natl. Acad. Sci. USA 2014, 111, 4221–4226. [Google Scholar] [CrossRef] [PubMed]
- Geissmann, F.; Manz, M.G.; Jung, S.; Sieweke, M.H.; Merad, M.; Ley, K. Development of Monocytes, Macrophages, and Dendritic Cells. Science 2010, 327, 656–661. [Google Scholar] [CrossRef] [PubMed]
- Yáñez, A.; Coetzee, S.; Olsson, A.; Muench, D.; Berman, B.P.; Hazelett, D.J.; Salomonis, N.; Grimes, H.L.; Goodridge, H.S. Granulocyte-Monocyte Progenitors and Monocyte-Dendritic Cell Progenitors Independently Produce Functionally Distinct Monocytes. Immunity 2017, 47, 890–902.e4. [Google Scholar] [CrossRef]
- Cortez-Retamozo, V.; Etzrodt, M.; Newton, A.; Rauch, P.; Chudnovskiy, A.; Berger, C.; Ryan, R.; Iwamoto, Y.; Marinelli, B.; Gorbatov, R.; et al. Origins of tumor-associated macrophages and neutrophils. Proc. Natl. Acad. Sci. USA 2012, 109, 2491–2496. [Google Scholar] [CrossRef]
- Yousif, A.S.; Ronsard, L.; Shah, P.; Omatsu, T.; Sangesland, M.; Moreno, T.B.; Lam, E.C.; Vrbanac, V.D.; Balazs, A.B.; Reinecker, H.-C.; et al. The persistence of interleukin-6 is regulated by a blood buffer system derived from dendritic cells. Immunity 2021, 54, 235–246.e5. [Google Scholar] [CrossRef]
- Jordan, K.R.; Kapoor, P.; Spongberg, E.; Tobin, R.P.; Gao, D.; Borges, V.F.; McCarter, M.D. Immunosuppressive myeloid-derived suppressor cells are increased in splenocytes from cancer patients. Cancer Immunol. Immunother. 2017, 66, 503–513. [Google Scholar] [CrossRef]
- Wu, C.; Ning, H.; Liu, M.; Lin, J.; Luo, S.; Zhu, W.; Xu, J.; Wu, W.-C.; Liang, J.; Shao, C.-K.; et al. Spleen mediates a distinct hematopoietic progenitor response supporting tumor-promoting myelopoiesis. J. Clin. Investig. 2018, 128, 3425–3438. [Google Scholar] [CrossRef]
- Li, H.; Zhou, Y.; Wang, H.; Zhang, M.; Qiu, P.; Zhang, R.; Zhao, Q.; Liu, J. Crosstalk Between Liver Macrophages and Surrounding Cells in Nonalcoholic Steatohepatitis. Front. Immunol. 2020, 11, 1169. [Google Scholar] [CrossRef] [PubMed]
- Schwabe, R.F.; Tabas, I.; Pajvani, U.B. Mechanisms of Fibrosis Development in Nonalcoholic Steatohepatitis. Gastroenterology 2020, 158, 1913–1928. [Google Scholar] [CrossRef]
- Guillot, A.; Tacke, F. Liver Macrophages: Old Dogmas and New Insights. Hepatol. Commun. 2019, 3, 730–743. [Google Scholar] [CrossRef]
- Yang, J.D.; Nakamura, I.; Roberts, L.R. The tumor microenvironment in hepatocellular carcinoma: Current status and therapeutic targets. Semin. Cancer Biol. 2011, 21, 35–43. [Google Scholar] [CrossRef] [PubMed]
- Mantovani, A.; Germano, G.; Marchesi, F.; Locatelli, M.; Biswas, S.K. Cancer-promoting tumor-associated macrophages: New vistas and open questions. Eur. J. Immunol. 2011, 41, 2522–2525. [Google Scholar] [CrossRef] [PubMed]
- Solinas, G.; Germano, G.; Mantovani, A.; Allavena, P. Tumor-associated macrophages (TAM) as major players of the cancer-related inflammation. J. Leukoc. Biol. 2009, 86, 1065–1073. [Google Scholar] [CrossRef] [PubMed]
- Mantovani, A.; Garlanda, C.; Allavena, P. Molecular pathways and targets in cancer-related inflammation. Ann. Med. 2010, 42, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Robinson, A.; Han, C.Z.; Glass, C.K.; Pollard, J.W. Monocyte Regulation in Homeostasis and Malignancy. Trends Immunol. 2021, 42, 104–119. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, S.R.; Schmid, M.C. Macrophages as Key Drivers of Cancer Progression and Metastasis. Mediat. Inflamm. 2017, 2017, 9624760. [Google Scholar] [CrossRef] [PubMed]
- Sica, A.; Mantovani, A. Macrophage plasticity and polarization: In vivo veritas. J. Clin. Investig. 2012, 122, 787–795. [Google Scholar] [CrossRef]
- Locati, M.; Curtale, G.; Mantovani, A. Diversity, Mechanisms, and Significance of Macrophage Plasticity. Annu. Rev. Pathol. Mech. Dis. 2020, 15, 123–147. [Google Scholar] [CrossRef]
- Gordon, S.; Martinez, F.O. Alternative Activation of Macrophages: Mechanism and Functions. Immunity 2010, 32, 593–604. [Google Scholar] [CrossRef]
- Hao, N.-B.; Lü, M.-H.; Fan, Y.-H.; Cao, Y.-L.; Zhang, Z.-R.; Yang, S.-M. Macrophages in Tumor Microenvironments and the Progression of Tumors. Clin. Dev. Immunol. 2012, 2012, 948098. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.; Ge, W.; Zhou, J.; Gao, B.; Qian, X.; Wang, W. The Role of Tumor Associated Macrophages in Hepatocellular Carcinoma. J. Cancer 2021, 12, 1284–1294. [Google Scholar] [CrossRef] [PubMed]
- Jayasingam, S.D.; Citartan, M.; Thang, T.H.; Mat Zin, A.A.; Ang, K.C.; Ch’ng, E.S. Evaluating the Polarization of Tumor-Associated Macrophages Into M1 and M2 Phenotypes in Human Cancer Tissue: Technicalities and Challenges in Routine Clinical Practice. Front. Oncol. 2020, 9, 1512. [Google Scholar] [CrossRef] [PubMed]
- Comi, M.; Avancini, D.; De Sio, F.S.; Villa, M.; Uyeda, M.J.; Floris, M.; Tomasoni, D.; Bulfone, A.; Roncarolo, M.G.; Gregori, S. Coexpression of CD163 and CD141 identifies human circulating IL-10-producing dendritic cells (DC-10). Cell. Mol. Immunol. 2020, 17, 95–107. [Google Scholar] [CrossRef]
- Bohn, T.; Rapp, S.; Luther, N.; Klein, M.; Bruehl, T.-J.; Kojima, N.; Lopez, P.A.; Hahlbrock, J.; Muth, S.; Endo, S.; et al. Tumor immunoevasion via acidosis-dependent induction of regulatory tumor-associated macrophages. Nat. Immunol. 2018, 19, 1319–1329. [Google Scholar] [CrossRef]
- Yang, Y.; Ye, Y.-C.; Chen, Y.; Zhao, J.-L.; Gao, C.-C.; Han, H.; Liu, W.-C.; Qin, H.-Y. Crosstalk between hepatic tumor cells and macrophages via Wnt/β-catenin signaling promotes M2-like macrophage polarization and reinforces tumor malignant behaviors. Cell Death Dis. 2018, 9, 793. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.-M.; Xiao, X.; Lao, X.-M.; Wei, Y.; Liu, R.-X.; Zeng, Q.-H.; Wang, J.-C.; Ouyang, F.-Z.; Chen, D.-P.; Chan, K.-W.; et al. Polarization of Tissue-Resident TFH-Like Cells in Human Hepatoma Bridges Innate Monocyte Inflammation and M2b Macrophage Polarization. Cancer Discov. 2016, 6, 1182–1195. [Google Scholar] [CrossRef]
- Zhou, J.; Ding, T.; Pan, W.; Zhu, L.-Y.; Li, L.; Zheng, L. Increased intratumoral regulatory T cells are related to intratumoral macrophages and poor prognosis in hepatocellular carcinoma patients. Int. J. Cancer 2009, 125, 1640–1648. [Google Scholar] [CrossRef]
- Wang, H.; Zhang, H.; Wang, Y.; Brown, Z.J.; Xia, Y.; Huang, Z.; Shen, C.; Hu, Z.; Beane, J.; Ansa-Addo, E.A.; et al. Regulatory T-cell and neutrophil extracellular trap interaction contributes to carcinogenesis in non-alcoholic steatohepatitis. J. Hepatol. 2021, 75, 1271–1283. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.-L.; Li, Q.; Yang, X.-M.; Fang, F.; Li, J.; Wang, Y.-H.; Yang, Q.; Zhu, L.; Nie, H.-Z.; Zhang, X.; et al. SPON2 Promotes M1-like Macrophage Recruitment and Inhibits Hepatocellular Carcinoma Metastasis by Distinct Integrin–Rho GTPase–Hippo Pathways. Cancer Res. 2018, 78, 2305–2317. [Google Scholar] [CrossRef] [PubMed]
- Liu, N.; Wang, X.; Steer, C.J.; Song, G. MicroRNA-206 promotes the recruitment of CD8+ T cells by driving M1 polarisation of Kupffer cells. Gut 2021. [Google Scholar] [CrossRef] [PubMed]
- Liu, R.-X.; Wei, Y.; Zeng, Q.-H.; Chan, K.-W.; Xiao, X.; Zhao, X.; Chen, M.-M.; Ouyang, F.-Z.; Chen, D.-P.; Zheng, L.; et al. Chemokine (C-X-C motif) receptor 3-positive B cells link interleukin-17 inflammation to protumorigenic macrophage polarization in human hepatocellular carcinoma. Hepatology 2015, 62, 1779–1790. [Google Scholar] [CrossRef]
- Zhao, Q.; Kuang, D.-M.; Wu, Y.; Xiao, X.; Li, X.-F.; Li, T.-J.; Zheng, L. Activated CD69+ T Cells Foster Immune Privilege by Regulating IDO Expression in Tumor-Associated Macrophages. J. Immunol. 2012, 188, 1117–1124. [Google Scholar] [CrossRef] [PubMed]
- Miura, K.; Ishioka, M.; Minami, S.; Horie, Y.; Ohshima, S.; Goto, T.; Ohnishi, H. Toll-like Receptor 4 on Macrophage Promotes the Development of Steatohepatitis-related Hepatocellular Carcinoma in Mice. J. Biol. Chem. 2016, 291, 11504–11517. [Google Scholar] [CrossRef]
- Wang, Q.; Cheng, F.; Ma, T.-T.; Xiong, H.-Y.; Li, Z.-W.; Xie, C.-L.; Liu, C.-Y.; Tu, Z.-G. Interleukin-12 inhibits the hepatocellular carcinoma growth by inducing macrophage polarization to the M1-like phenotype through downregulation of Stat-3. Mol. Cell. Biochem. 2016, 415, 157–168. [Google Scholar] [CrossRef]
- Wang, T.-T.; Yuan, J.-H.; Ma, J.-Z.; Yang, W.-J.; Liu, X.-N.; Yin, Y.-P.; Liu, Y.; Pan, W.; Sun, S.-H. CTGF secreted by mesenchymal-like hepatocellular carcinoma cells plays a role in the polarization of macrophages in hepatocellular carcinoma progression. Biomed. Pharmacother. 2017, 95, 111–119. [Google Scholar] [CrossRef] [PubMed]
- Curiel, T.J.; Coukos, G.; Zou, L.; Alvarez, X.; Cheng, P.; Mottram, P.; Evdemon-Hogan, M.; Conejo-Garcia, J.R.; Zhang, L.; Burow, M.; et al. Specific recruitment of regulatory T cells in ovarian carcinoma fosters immune privilege and predicts reduced survival. Nat. Med. 2004, 10, 942–949. [Google Scholar] [CrossRef] [PubMed]
- Hefetz-Sela, S.; Stein, I.; Klieger, Y.; Porat, R.; Sade-Feldman, M.; Zreik, F.; Nagler, A.; Pappo, O.; Quagliata, L.; Dazert, E.; et al. Acquisition of an immunosuppressive protumorigenic macrophage phenotype depending on c-Jun phosphorylation. Proc. Natl. Acad. Sci. USA 2014, 111, 17582–17587. [Google Scholar] [CrossRef]
- Zhang, Q.; He, Y.; Luo, N.; Patel, S.J.; Han, Y.; Gao, R.; Modak, M.; Carotta, S.; Haslinger, C.; Kind, D.; et al. Landscape and Dynamics of Single Immune Cells in Hepatocellular Carcinoma. Cell 2019, 179, 829–845.e20. [Google Scholar] [CrossRef] [PubMed]
- Song, G.; Shi, Y.; Zhang, M.; Goswami, S.; Afridi, S.; Meng, L.; Ma, J.; Chen, Y.; Lin, Y.; Zhang, J.; et al. Global immune characterization of HBV/HCV-related hepatocellular carcinoma identifies macrophage and T-cell subsets associated with disease progression. Cell Discov. 2020, 6, 90. [Google Scholar] [CrossRef]
- Dong, L.-Q.; Peng, L.-H.; Ma, L.-J.; Liu, D.-B.; Zhang, S.; Luo, S.-Z.; Rao, J.-H.; Zhu, H.-W.; Yang, S.-X.; Xi, S.-J.; et al. Heterogeneous immunogenomic features and distinct escape mechanisms in multifocal hepatocellular carcinoma. J. Hepatol. 2020, 72, 896–908. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Wang, H.; Mao, C.; Sun, M.; Dominah, G.; Chen, L.; Zhuang, Z. Fatty acid oxidation contributes to IL-1β secretion in M2 macrophages and promotes macrophage-mediated tumor cell migration. Mol. Immunol. 2018, 94, 27–35. [Google Scholar] [CrossRef]
- Degroote, H.; Lefere, S.; Vandierendonck, A.; Vanderborght, B.; Meese, T.; Van Nieuwerburgh, F.; Verhelst, X.; Geerts, A.; Van Vlierberghe, H.; Devisscher, L. Characterization of the inflammatory microenvironment and hepatic macrophage subsets in experimental hepatocellular carcinoma models. Oncotarget 2021, 12, 562–577. [Google Scholar] [CrossRef] [PubMed]
- Schneider, C.; Teufel, A.; Yevsa, T.; Staib, F.; Hohmeyer, A.; Walenda, G.; Zimmermann, H.W.; Vucur, M.; Huss, S.; Gassler, N.; et al. Adaptive immunity suppresses formation and progression of diethylnitrosamine-induced liver cancer. Gut 2012, 61, 1733–1743. [Google Scholar] [CrossRef]
- Mano, Y.; Aishima, S.; Fujita, N.; Tanaka, Y.; Kubo, Y.; Motomura, T.; Taketomi, A.; Shirabe, K.; Maehara, Y.; Oda, Y. Tumor-Associated Macrophage Promotes Tumor Progression via STAT3 Signaling in Hepatocellular Carcinoma. Pathobiology 2013, 80, 146–154. [Google Scholar] [CrossRef]
- Eggert, T.; Wolter, K.; Ji, J.; Ma, C.; Yevsa, T.; Klotz, S.; Medina-Echeverz, J.; Longerich, T.; Forgues, M.; Reisinger, F.; et al. Distinct Functions of Senescence-Associated Immune Responses in Liver Tumor Surveillance and Tumor Progression. Cancer Cell 2016, 30, 533–547. [Google Scholar] [CrossRef]
- Wolf, M.J.; Adili, A.; Piotrowitz, K.; Abdullah, Z.; Boege, Y.; Stemmer, K.; Ringelhan, M.; Simonavicius, N.; Egger, M.; Wohlleber, D.; et al. Metabolic Activation of Intrahepatic CD8+ T Cells and NKT Cells Causes Nonalcoholic Steatohepatitis and Liver Cancer via Cross-Talk with Hepatocytes. Cancer Cell 2014, 26, 549–564. [Google Scholar] [CrossRef]
- Guo, B.; Li, L.; Guo, J.; Liu, A.; Wu, J.; Wang, H.; Shi, J.; Pang, D.; Cao, Q. M2 tumor-associated macrophages produce interleukin-17 to suppress oxaliplatin-induced apoptosis in hepatocellular carcinoma. Oncotarget 2017, 8, 44465–44476. [Google Scholar] [CrossRef]
- Wei, Y.; Shi, D.; Liang, Z.; Liu, Y.; Li, Y.; Xing, Y.; Liu, W.; Ai, Z.; Zhuang, J.; Chen, X.; et al. IL-17A secreted from lymphatic endothelial cells promotes tumorigenesis by upregulation of PD-L1 in hepatoma stem cells. J. Hepatol. 2019, 71, 1206–1215. [Google Scholar] [CrossRef]
- Wu, J.; Gao, W.; Zuo, X.; Zhang, Y.; Chen, Z.; Ding, W.; Li, X.; Lin, F.; Shen, H.; Tang, J.; et al. M2 Macrophage–Derived Exosomes Facilitate HCC Metastasis by Transferring αMβ2 Integrin to Tumor Cells. Hepatology 2020, 73, 1365–1380. [Google Scholar] [CrossRef]
- Li, X.; Yao, W.; Yuan, Y.; Chen, P.; Li, B.; Li, J.; Chu, R.; Song, H.; Xie, D.; Jiang, X.; et al. Targeting of tumour-infiltrating macrophages via CCL2/CCR2 signalling as a therapeutic strategy against hepatocellular carcinoma. Gut 2015, 66, 157–167. [Google Scholar] [CrossRef]
- Zhang, J.; Zhang, Q.; Lou, Y.; Fu, Q.; Chen, Q.; Wei, T.; Yang, J.; Tang, J.; Wang, J.; Chen, Y.; et al. Hypoxia-inducible factor-1α/interleukin-1β signaling enhances hepatoma epithelial-mesenchymal transition through macrophages in a hypoxic-inflammatory microenvironment. Hepatology 2018, 67, 1872–1889. [Google Scholar] [CrossRef]
- Zhao, Q.; Xiao, X.; Wu, Y.; Wei, Y.; Zhu, L.-Y.; Zhou, J.; Kuang, D.-M. Interleukin-17-educated monocytes suppress cytotoxic T-cell function through B7-H1 in hepatocellular carcinoma patients. Eur. J. Immunol. 2011, 41, 2314–2322. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Kuang, D.-M.; Pan, W.-D.; Wan, Y.-L.; Lao, X.-M.; Wang, D.; Li, X.-F.; Zheng, L. Monocyte/macrophage-elicited natural killer cell dysfunction in hepatocellular carcinoma is mediated by CD48/2B4 interactions. Hepatology 2013, 57, 1107–1116. [Google Scholar] [CrossRef]
- Zang, M.; Li, Y.; He, H.; Ding, H.; Chen, K.; Du, J.; Chen, T.; Wu, Z.; Liu, H.; Wang, D.; et al. IL-23 production of liver inflammatory macrophages to damaged hepatocytes promotes hepatocellular carcinoma development after chronic hepatitis B virus infection. Biochim. Biophys. Acta (BBA)-Mol. Basis Dis. 2018, 1864, 3759–3770. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Li, J.-Q.; Jiang, Z.-Z.; Li, L.; Wu, Y.; Zheng, L. CD169 identifies an anti-tumour macrophage subpopulation in human hepatocellular carcinoma. J. Pathol. 2016, 239, 231–241. [Google Scholar] [CrossRef]
- Bartneck, M.; Schrammen, P.L.; Möckel, D.; Govaere, O.; Liepelt, A.; Krenkel, O.; Ergen, C.; McCain, M.V.; Eulberg, D.; Luedde, T.; et al. The CCR2+ Macrophage Subset Promotes Pathogenic Angiogenesis for Tumor Vascularization in Fibrotic Livers. Cell. Mol. Gastroenterol. Hepatol. 2019, 7, 371–390. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Wang, X.; Shen, Z.; Xu, J.; Qin, J.; Sun, Y. Infiltration of diametrically polarized macrophages predicts overall survival of patients with gastric cancer after surgical resection. Gastric Cancer 2015, 18, 740–750. [Google Scholar] [CrossRef]
- Zhang, M.; He, Y.; Sun, X.; Li, Q.; Wang, W.; Zhao, A.; Di, W. A high M1/M2 ratio of tumor-associated macrophages is associated with extended survival in ovarian cancer patients. J. Ovarian Res. 2014, 7, 19. [Google Scholar] [CrossRef]
- Dong, P.; Ma, L.; Liu, L.; Zhao, G.; Zhang, S.; Dong, L.; Xue, R.; Chen, S. CD86+/CD206+, Diametrically Polarized Tumor-Associated Macrophages, Predict Hepatocellular Carcinoma Patient Prognosis. Int. J. Mol. Sci. 2016, 17, 320. [Google Scholar] [CrossRef]
- Sia, D.; Jiao, Y.; Martinez-Quetglas, I.; Kuchuk, O.; Villacorta-Martin, C.; de Moura, M.C.; Putra, J.; Campreciós, G.; Bassaganyas, L.; Akers, N.; et al. Identification of an Immune-specific Class of Hepatocellular Carcinoma, Based on Molecular Features. Gastroenterology 2017, 153, 812–826. [Google Scholar] [CrossRef]
- Liu, J.-Y.; Peng, C.-W.; Yang, G.-F.; Hu, W.-Q.; Yang, X.-J.; Huang, C.-Q.; Xiong, B.; Li, Y. Distribution pattern of tumor associated macrophages predicts the prognosis of gastric cancer. Oncotarget 2017, 8, 92757–92769. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.; Wei, C.; Wang, S.; Shi, D.; Zhang, C.; Lin, X.; Dou, R.; Xiong, B. Elevated CD163+/CD68+ Ratio at Tumor Invasive Front is Closely Associated with Aggressive Phenotype and Poor Prognosis in Colorectal Cancer. Int. J. Biol. Sci. 2019, 15, 984–998. [Google Scholar] [CrossRef] [PubMed]
- Ke, M.; Zhang, Z.; Cong, L.; Zhao, S.; Li, Y.; Wang, X.; Lv, Y.; Zhu, Y.; Dong, J. MicroRNA-148b-colony-stimulating factor-1 signaling-induced tumor-associated macrophage infiltration promotes hepatocellular carcinoma metastasis. Biomed. Pharmacother. 2019, 120, 109523. [Google Scholar] [CrossRef] [PubMed]
- Chen, D.-P.; Ning, W.-R.; Jiang, Z.-Z.; Peng, Z.-P.; Zhu, L.-Y.; Zhuang, S.-M.; Kuang, D.-M.; Zheng, L.; Wu, Y. Glycolytic activation of peritumoral monocytes fosters immune privilege via the PFKFB3-PD-L1 axis in human hepatocellular carcinoma. J. Hepatol. 2019, 71, 333–343. [Google Scholar] [CrossRef]
- Li, Z.; Li, H.; Zhao, Z.-B.; Zhu, W.; Feng, P.-P.; Zhu, X.-W.; Gong, J.-P. SIRT4 silencing in tumor-associated macrophages promotes HCC development via PPARδ signalling-mediated alternative activation of macrophages. J. Exp. Clin. Cancer Res. 2019, 38, 469. [Google Scholar] [CrossRef]
- Zhang, Q.-B.; Jia, Q.-A.; Wang, H.; Hu, C.-X.; Sun, D.; Jiang, R.-D.; Zhang, Z.-L. High-mobility group protein box1 expression correlates with peritumoral macrophage infiltration and unfavorable prognosis in patients with hepatocellular carcinoma and cirrhosis. BMC Cancer 2016, 16, 880. [Google Scholar] [CrossRef]
- Zhao, Y.-M.; Wang, L.; Dai, Z.; Wang, D.-D.; Hei, Z.-Y.; Zhang, N.; Fu, X.-T.; Wang, X.-L.; Zhang, S.-C.; Qin, L.-X.; et al. Validity of plasma macrophage migration inhibitory factor for diagnosis and prognosis of hepatocellular carcinoma. Int. J. Cancer 2011, 129, 2463–2472. [Google Scholar] [CrossRef]
- Kono, H.; Fujii, H.; Furuya, S.; Hara, M.; Hirayama, K.; Akazawa, Y.; Nakata, Y.; Tsuchiya, M.; Hosomura, N.; Sun, C. Macrophage colony-stimulating factor expressed in non-cancer tissues provides predictive powers for recurrence in hepatocellular carcinoma. World J. Gastroenterol. 2016, 22, 8779–8789. [Google Scholar] [CrossRef]
- Ohno, A.; Yorita, K.; Haruyama, Y.; Kondo, K.; Kato, A.; Ohtomo, T.; Kawaguchi, M.; Marutuska, K.; Chijiiwa, K.; Kataoka, H. Aberrant expression of monocarboxylate transporter 4 in tumour cells predicts an unfavourable outcome in patients with hepatocellular carcinoma. Liver Int. 2014, 34, 942–952. [Google Scholar] [CrossRef] [PubMed]
- Zhu, F.; Li, X.; Jiang, Y.; Zhu, H.; Zhang, H.; Zhang, C.; Zhao, Y.; Luo, F. GdCl3 suppresses the malignant potential of hepatocellular carcinoma by inhibiting the expression of CD206 in tumor-associated macrophages. Oncol. Rep. 2015, 34, 2643–2655. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Zhu, X.-D.; Zhang, J.-B.; Zhuang, P.-Y.; Zhu, H.-G.; Zhang, W.; Xiong, Y.-Q.; Wu, W.-Z.; Wang, L.; Tang, Z.-Y.; Sun, H.-C. High Expression of Macrophage Colony-Stimulating Factor in Peritumoral Liver Tissue Is Associated With Poor Survival After Curative Resection of Hepatocellular Carcinoma. J. Clin. Oncol. 2008, 26, 2707–2716. [Google Scholar] [CrossRef] [PubMed]
- Zhu, W.; Guo, L.; Zhang, B.; Lou, L.; Lin, Z.; Zhu, X.; Ren, N.; Dong, Q.; Ye, Q.; Qin, L. Combination of Osteopontin with Peritumoral Infiltrating Macrophages is Associated with Poor Prognosis of Early-Stage Hepatocellular Carcinoma after Curative Resection. Ann. Surg. Oncol. 2013, 21, 1304–1313. [Google Scholar] [CrossRef]
- Zhou, T.-Y.; Zhou, Y.-L.; Qian, M.-J.; Fang, Y.-Z.; Ye, S.; Xin, W.-X.; Yang, X.-C.; Wu, H.-H. Interleukin-6 induced by YAP in hepatocellular carcinoma cells recruits tumor-associated macrophages. J. Pharmacol. Sci. 2018, 138, 89–95. [Google Scholar] [CrossRef]
- Wang, X.; Wang, H.; Li, G.; Song, Y.; Wang, S.; Zhu, F.; Guo, C.; Zhang, L.; Shi, Y. Activated macrophages down-regulate expression of E-cadherin in hepatocellular carcinoma cells via NF–κB/Slug pathway. Tumor Biol. 2014, 35, 8893–8901. [Google Scholar] [CrossRef]
- Zhang, W.; Zhu, X.-D.; Sun, H.-C.; Xiong, Y.-Q.; Zhuang, P.-Y.; Xu, H.-X.; Kong, L.-Q.; Wang, L.; Wu, W.-Z.; Tang, Z.-Y. Depletion of Tumor-Associated Macrophages Enhances the Effect of Sorafenib in Metastatic Liver Cancer Models by Antimetastatic and Antiangiogenic Effects. Clin. Cancer Res. 2010, 16, 3420–3430. [Google Scholar] [CrossRef]
- Wu, X.; Luo, H.; Shi, B.; Di, S.; Sun, R.; Su, J.; Liu, Y.; Li, H.; Jiang, H.; Li, Z. Combined Antitumor Effects of Sorafenib and GPC3-CAR T Cells in Mouse Models of Hepatocellular Carcinoma. Mol. Ther. 2019, 27, 1483–1494. [Google Scholar] [CrossRef]
- Sprinzl, M.F.; Reisinger, F.; Puschnik, A.; Ringelhan, M.; Ackermann, K.; Hartmann, D.; Schiemann, M.; Weinmann, A.; Galle, P.R.; Schuchmann, M.; et al. Sorafenib perpetuates cellular anticancer effector functions by modulating the crosstalk between macrophages and natural killer cells. Hepatology 2013, 57, 2358–2368. [Google Scholar] [CrossRef]
- Sprinzl, M.F.; Puschnik, A.; Schlitter, A.M.; Schad, A.; Ackermann, K.; Esposito, I.; Lang, H.; Galle, P.R.; Weinmann, A.; Heikenwälder, M.; et al. Sorafenib inhibits macrophage-induced growth of hepatoma cells by interference with insulin-like growth factor-1 secretion. J. Hepatol. 2015, 62, 863–870. [Google Scholar] [CrossRef]
- Yao, W.; Ba, Q.; Li, X.; Li, H.; Zhang, S.; Yuan, Y.; Wang, F.; Duan, X.; Li, J.; Zhang, W.; et al. A Natural CCR2 Antagonist Relieves Tumor-associated Macrophage-mediated Immunosuppression to Produce a Therapeutic Effect for Liver Cancer. EBioMedicine 2017, 22, 58–67. [Google Scholar] [CrossRef] [PubMed]
- Deng, Y.-R.; Liu, W.-B.; Lian, Z.-X.; Li, X.; Hou, X. Sorafenib inhibits macrophage-mediated epithelial-mesenchymal transition in hepatocellular carcinoma. Oncotarget 2016, 7, 38292–38305. [Google Scholar] [CrossRef] [PubMed]
- Wei, X.; Tang, C.; Lu, X.; Liu, R.; Zhou, M.; He, D.; Zheng, D.; Sun, C.; Wu, Z. MiR-101 targets DUSP1 to regulate the TGF-β secretion in sorafenib inhibits macrophage-induced growth of hepatocarcinoma. Oncotarget 2015, 6, 18389–18405. [Google Scholar] [CrossRef]
- Yang, W.; Lu, Y.; Xu, Y.; Xu, L.; Zheng, W.; Wu, Y.; Li, L.; Shen, P. Estrogen Represses Hepatocellular Carcinoma (HCC) Growth via Inhibiting Alternative Activation of Tumor-associated Macrophages (TAMs)*. J. Biol. Chem. 2012, 287, 40140–40149. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiyama, T.; Nakamoto, Y.; Sakai, Y.; Mukaida, N.; Kaneko, S. Optimal amount of monocyte chemoattractant protein-1 enhances antitumor effects of suicide gene therapy against hepatocellular carcinoma by M1 macrophage activation. Cancer Sci. 2008, 99, 2075–2082. [Google Scholar] [CrossRef]
- Guerra, A.D.; Yeung, O.W.; Qi, X.; Kao, W.J.; Man, K. The Anti-Tumor Effects of M1 Macrophage-Loaded Poly (ethylene glycol) and Gelatin-Based Hydrogels on Hepatocellular Carcinoma. Theranostics 2017, 7, 3732–3744. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.-H.; Jian, W.-H.; Wu, Z.-F.; Zhao, J.; Wang, H.; Li, W.; Xia, J.-T. Small interfering RNA (siRNA)-mediated knockdown of macrophage migration inhibitory factor (MIF) suppressed cyclin D1 expression and hepatocellular carcinoma cell proliferation. Oncotarget 2014, 5, 5570–5580. [Google Scholar] [CrossRef]
- Xiao, Z.; Chung, H.; Banan, B.; Manning, P.T.; Ott, K.C.; Lin, S.; Capoccia, B.J.; Subramanian, V.; Hiebsch, R.R.; Upadhya, G.A.; et al. Antibody mediated therapy targeting CD47 inhibits tumor progression of hepatocellular carcinoma. Cancer Lett. 2015, 360, 302–309. [Google Scholar] [CrossRef]
- Tan, H.-Y.; Wang, N.; Tsao, S.-W.; Che, C.-M.; Yuen, M.-F.; Feng, Y. IRE1α inhibition by natural compound genipin on tumour associated macrophages reduces growth of hepatocellular carcinoma. Oncotarget 2016, 7, 43792–43804. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.-S.; Gao, L.-N.; Zhu, X.-N.; Zhang, Y.; Zhang, C.-N.; Xu, D.; Cui, Y.-L. Co-delivery of glycyrrhizin and doxorubicin by alginate nanogel particles attenuates the activation of macrophage and enhances the therapeutic efficacy for hepatocellular carcinoma. Theranostics 2019, 9, 6239–6255. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Liu, D.; Kimchi, E.T.; Kaifi, J.T.; Qi, X.; Manjunath, Y.; Liu, X.; Deering, T.; Avella, D.M.; Fox, T.; et al. Nanoliposome C6-Ceramide Increases the Anti-tumor Immune Response and Slows Growth of Liver Tumors in Mice. Gastroenterology 2018, 154, 1024–1036.e9. [Google Scholar] [CrossRef]
- Chen, X.; Yin, S.; Hu, C.; Chen, X.; Jiang, K.; Ye, S.; Feng, X.; Fan, S.; Xie, H.; Zhou, L.; et al. Comparative Study of Nanosecond Electric Fields In Vitro and In Vivo on Hepatocellular Carcinoma Indicate Macrophage Infiltration Contribute to Tumor Ablation In Vivo. PLoS ONE 2014, 9, e86421. [Google Scholar] [CrossRef] [PubMed]
- Yin, S.; Chen, X.; Hu, C.; Zhang, X.; Hu, Z.; Yu, J.; Feng, X.; Jiang, K.; Ye, S.; Shen, K.; et al. Nanosecond pulsed electric field (nsPEF) treatment for hepatocellular carcinoma: A novel locoregional ablation decreasing lung metastasis. Cancer Lett. 2014, 346, 285–291. [Google Scholar] [CrossRef]
- Nii, T.; Kuwahara, T.; Makino, K.; Tabata, P.Y. A Co-Culture System of Three-Dimensional Tumor-Associated Macrophages and Three-Dimensional Cancer-Associated Fibroblasts Combined with Biomolecule Release for Cancer Cell Migration. Tissue Eng. Part A 2020, 26, 1272–1282. [Google Scholar] [CrossRef] [PubMed]
- Nii, T.; Makino, K.; Tabata, Y. Three-Dimensional Culture System of Cancer Cells Combined with Biomaterials for Drug Screening. Cancers 2020, 12, 2754. [Google Scholar] [CrossRef]
- Cuccarese, M.F.; Dubach, J.M.; Pfirschke, C.; Engblom, C.; Garris, C.; Miller, M.; Pittet, M.J.; Weissleder, R. Heterogeneity of macrophage infiltration and therapeutic response in lung carcinoma revealed by 3D organ imaging. Nat. Commun. 2017, 8, 14293. [Google Scholar] [CrossRef]
- Sun, Y.; Wu, L.; Zhong, Y.; Zhou, K.; Hou, Y.; Wang, Z.; Zhang, Z.; Xie, J.; Wang, C.; Chen, D.; et al. Single-cell landscape of the ecosystem in early-relapse hepatocellular carcinoma. Cell 2021, 184, 404–421.e16. [Google Scholar] [CrossRef]
- Tacke, F. Cenicriviroc for the treatment of non-alcoholic steatohepatitis and liver fibrosis. Expert Opin. Investig. Drugs 2018, 27, 301–311. [Google Scholar] [CrossRef]
- Bartneck, M.; Koppe, C.; Fech, V.; Warzecha, K.T.; Kohlhepp, M.; Huss, S.; Weiskirchen, R.; Trautwein, C.; Luedde, T.; Tacke, F. Roles of CCR2 and CCR5 for Hepatic Macrophage Polarization in Mice With Liver Parenchymal Cell-Specific NEMO Deletion. Cell. Mol. Gastroenterol. Hepatol. 2021, 11, 327–347. [Google Scholar] [CrossRef] [PubMed]
- Wu, Q.; Zhou, W.; Yin, S.; Zhou, Y.; Chen, T.; Qian, J.; Su, R.; Hong, L.; Lu, H.; Zhang, F.; et al. Blocking Triggering Receptor Expressed on Myeloid Cells-1-Positive Tumor-Associated Macrophages Induced by Hypoxia Reverses Immunosuppression and Anti-Programmed Cell Death Ligand 1 Resistance in Liver Cancer. Hepatology 2019, 70, 198–214. [Google Scholar] [CrossRef] [PubMed]
- Halama, N.; Zoernig, I.; Berthel, A.; Kahlert, C.; Klupp, F.; Suarez-Carmona, M.; Suetterlin, T.; Brand, K.; Krauss, J.; Lasitschka, F.; et al. Tumoral Immune Cell Exploitation in Colorectal Cancer Metastases Can Be Targeted Effectively by Anti-CCR5 Therapy in Cancer Patients. Cancer Cell 2016, 29, 587–601. [Google Scholar] [CrossRef] [PubMed]
- Tan-Garcia, A.; Lai, F.; Yeong, J.P.S.; Irac, S.E.; Ng, P.Y.; Msallam, R.; Lim, J.C.T.; Wai, L.-E.; Tham, C.Y.; Choo, S.P.; et al. Liver fibrosis and CD206+ macrophage accumulation are suppressed by anti-GM-CSF therapy. JHEP Rep. 2020, 2, 100062. [Google Scholar] [CrossRef]
- Su, X.; Xu, Y.; Fox, G.C.; Xiang, J.; Kwakwa, K.A.; Davis, J.L.; Belle, J.I.; Lee, W.-C.; Wong, W.H.; Fontana, F.; et al. Breast cancer–derived GM-CSF regulates arginase 1 in myeloid cells to promote an immunosuppressive microenvironment. J. Clin. Investig. 2021, 131. [Google Scholar] [CrossRef]
- Burmester, G.R.; McInnes, I.B.; Kremer, J.; Miranda, P.; Korkosz, M.; Vencovsky, J.; Rubbert-Roth, A.; Mysler, E.; Sleeman, M.A.; Godwood, A.; et al. A randomised phase IIb study of mavrilimumab, a novel GM–CSF receptor alpha monoclonal antibody, in the treatment of rheumatoid arthritis. Ann. Rheum. Dis. 2017, 76, 1020–1030. [Google Scholar] [CrossRef]
- Behrens, F.; Tak, P.P.; Østergaard, M.; Stoilov, R.; Wiland, P.; Huizinga, T.W.; Berenfus, V.; Vladeva, S.; Rech, J.; Rubbert-Roth, A.; et al. MOR103, a human monoclonal antibody to granulocyte–macrophage colony-stimulating factor, in the treatment of patients with moderate rheumatoid arthritis: Results of a phase Ib/IIa randomised, double-blind, placebo-controlled, dose-escalation trial. Ann. Rheum. Dis. 2014, 74, 1058–1064. [Google Scholar] [CrossRef]
- Sterner, R.M.; Sakemura, R.; Cox, M.J.; Yang, N.; Khadka, R.H.; Forsman, C.L.; Hansen, M.J.; Jin, F.; Ayasoufi, K.; Hefazi, M.; et al. GM-CSF inhibition reduces cytokine release syndrome and neuroinflammation but enhances CAR-T cell function in xenografts. Blood 2019, 133, 697–709. [Google Scholar] [CrossRef]
- Temesgen, Z.; Burger, C.D.; Baker, J.; Polk, C.; Libertin, C.; Kelley, C.; Marconi, V.C.; Orenstein, R.; Durrant, C.; Chappell, D.; et al. Lenzilumab Efficacy and Safety in Newly Hospitalized COVID-19 Subjects: Results from the Live-Air Phase 3 Randomized Double-Blind Placebo-Controlled Trial. medRxiv 2021. [Google Scholar] [CrossRef]
- Neubert, N.J.; Schmittnaegel, M.; Bordry, N.; Nassiri, S.; Wald, N.; Martignier, C.; Tillé, L.; Homicsko, K.; Damsky, W.; Hajjami, H.M.-E.; et al. T cell–induced CSF1 promotes melanoma resistance to PD1 blockade. Sci. Transl. Med. 2018, 10. [Google Scholar] [CrossRef]
- Güç, E.; Pollard, J.W. Redefining macrophage and neutrophil biology in the metastatic cascade. Immunity 2021, 54, 885–902. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).