Simple Summary
Metastasis, the process by which cancer cells escape primary tumor site and colonize distant organs, is responsible for most cancer-related deaths. The tumor microenvironment (TME), comprises different cell types, including immune cells and cancer-associated fibroblasts, as well as structural elements, such as collagen and hyaluronan that constitute the extracellular matrix (ECM). Intratumoral interactions between the cellular and structural components of the TME regulate the aggressiveness, and dissemination of malignant cells and promote immune evasion. At the secondary site, the TME also facilitates escape from dormancy to enhance metastatic tumor outgrowth. Moreover, the ECM applies mechanical forces on tumors that contribute to hypoxia and cancer cell invasiveness whereas also hinders drug delivery and efficacy in both primary and metastatic sites. In this review, we summarize the latest developments regarding the role of the TME in cancer progression and discuss ongoing efforts to remodel the TME to stop metastasis in its tracks.
Abstract
The tumor microenvironment (TME) regulates essential tumor survival and promotion functions. Interactions between the cellular and structural components of the TME allow cancer cells to become invasive and disseminate from the primary site to distant locations, through a complex and multistep metastatic cascade. Tumor-associated M2-type macrophages have growth-promoting and immunosuppressive functions; mesenchymal cells mass produce exosomes that increase the migratory ability of cancer cells; cancer associated fibroblasts (CAFs) reorganize the surrounding matrix creating migration-guiding tracks for cancer cells. In addition, the tumor extracellular matrix (ECM) exerts determinant roles in disease progression and cancer cell migration and regulates therapeutic responses. The hypoxic conditions generated at the primary tumor force cancer cells to genetically and/or epigenetically adapt in order to survive and metastasize. In the circulation, cancer cells encounter platelets, immune cells, and cytokines in the blood microenvironment that facilitate their survival and transit. This review discusses the roles of different cellular and structural tumor components in regulating the metastatic process, targeting approaches using small molecule inhibitors, nanoparticles, manipulated exosomes, and miRNAs to inhibit tumor invasion as well as current and future strategies to remodel the TME and enhance treatment efficacy to block the detrimental process of metastasis.
1. Introduction
Metastasis is responsible for more than 90% of cancer mortality; however, the underlying mechanisms driving this multistep process, ranging from local invasion at the primary site to the outgrowth of metastatic cells at the secondary sites, remain elusive. The communication between the neoplastic cells and the adjacent stromal cells begins at the earliest stages of tumor formation and continues during primary growth, local invasion, intravasation and establishment at the secondary site. While it was initially established that genetic aberrations are predominantly responsible for tumor initiation and progression [1], it has become clear during the last two decades that the tumor microenvironment (TME) plays an equally important role in modulating the aggressiveness, motility, dissemination, and colonization of cancer cells to distal organs [2]. The TME comprises the extracellular matrix (ECM) and basement membrane (BM), endothelial cells, adipose cells, tumor-infiltrating immune cells, cancer-associated fibroblasts (CAFs), neuroendocrine cells, pericytes, as well as a plethora of signalling molecules that regulate tumor progression. Cancer cells secrete growth factors and cytokines (including IL-6, IL-1β, TGF-β1, TGF-β2, FGF-2, and PDGF) that recruit and reprogram stromal cells, such as immune cells and fibroblasts, as well as enzymes that degrade and remodel the surrounding ECM and BM, such as matrix metalloproteinases (MMPs). In this review, we summarize the latest findings in the efforts for understanding the complex roles of TME constituents in various stages of metastatic progression and discuss about strategies as well as future challenges for targeting TME components to battle the most aggressive forms of the disease.
2. Roles of Cellular TME Components in Regulating the Metastatic Cascade
2.1. Role of Immune Cells in Modulating Cancer Metastasis
It is unambiguously accepted that immune cells exert pivotal effects in the properties of cancer cells at different stages of the invasion-metastasis cascade, either by infiltrating the tumor or by affecting the systemic environment [3]. During every step of this lethal process, cancer cells are being exposed to the immune system which attacks them to restrain their growth [4]. These anti-tumor effects are primarily mediated by CD8+ T cells as well as natural killer (NK) cells, which have been shown to restrict metastatic outgrowth of tumor cells, whereas their depletion enhances metastasis without affecting primary tumor growth [5,6,7]. However, during tumor evolution, cancer cells develop strategies not only to avoid immune surveillance but also to induce systemic responses by exploiting types of immune cells, such as myeloid cells, in order to enhance their metastatic efficiency [8].
The main type of myeloid cells implicated in regulating metastasis are macrophages, which are derived by hematopoietic stem cells (HSC) in the bone marrow and considered “professional” antigen presenting cells (APCs) [9]. They present foreign antigens to helper T cells and can prime naïve T cells. Macrophages are recruited to the tumor site via chemokines produced from cancer and stromal cells and are, thus, referred to as tumor-associated macrophages (TAMs). TAMs can act in two opposing functions depending on their polarization subtype: M1-type TAMs have pro-inflammatory and anti-tumoral properties and activate the immune system by releasing interferon (IFN)-γ and IL-12. On the other hand, M2-type TAMs are pro-tumorigenic, and exert immunosuppressive functions by producing IL-10, induce angiogenesis and stimulate tumor cells to release MMPs that favor cancer progression by disrupting the ECM and BM [10,11].
TAMs enable metastasis at various stages of the process, including activation of epithelial-to-mesenchymal transition (EMT), local invasion, and intravasation into the blood stream, transfer of cancer cells through the circulation, extravasation, and seeding at the secondary site, and finally promotion of survival and outgrowth of cancer cells at distant organs [12,13]. They achieve this by secreting numerous chemokines, inflammatory molecules, and growth factors that promote metastatic progression.
At the primary tumor site, TAMs help create a suitable microenvironment that allows tumor invasion [14]. The term “tumor microenvironment of metastasis” (TMEM) is proposed to describe the close arrangement of cancer cells, perivascular TAMs, and endothelial cells often located at sites of intravasation. Increased TMEM density in breast carcinoma patient samples positively correlates with increased risk of distant organ metastases [15]. During EMT, growth factors and cytokines, including TGF-β, Wnt, and EGF, can lead to the activation of an orchestrated transcriptional program during which tumor cells lose epithelial characteristics and gain mesenchymal features leading to increased capacity for invasion and metastasis [16,17]. Inflammation-induced EMT has also been reported and TAMs appear to play an important role in this transition. In hepatocellular carcinoma (HCC), TAMs are recruited by cancer cells by expressing glypican and secrete TGF-β, PDGF, VEGF, chemokine (C-C motif) ligand 2 (CCL2), and M-CSF [18,19]. In the tumor microenvironment, TAMs secrete many cytokines such as TGF-β and IL-6 that can induce EMT [20]. In pancreatic cancer, M2-polarized TAMs expressing Toll-like receptor 4 (TLR4) promoted EMT via TLR4/IL-10 signaling. Specifically, TAMs upregulated mesenchymal markers vimentin and snail, induced MMP-2 and MMP-9 proteolytic activity and diminished E-cadherin levels, leading to increased fibroblastic morphology, proliferation, and migration of pancreatic cancer cells [21]. TAMs exhibiting a CD68+HLA−DR+ surface marker phenotype can induce migration of HCC cells via the NF-κB/FAK pathway [22]. TAMs can further facilitate the invasiveness of cancer cells induced by phosphatase of regenerating liver (PRL-3), a marker of colorectal cancer (CRC) liver metastasis. CRC cells also produce PRL-3 and tumor necrosis factor-α (TNF-α) that increase the expression of intermediate-conductance Ca2+-activated potassium (KCNN4) channels in TAMs [23]; KCNN4 induce the secretion of IL-6 and IL-8 by TAMs and improve CRC cell invasiveness [24]. In addition, TAMs can release CCL18 chemokine that can stimulate angiogenesis and promote tumor progression in breast cancer [25]. In addition to their role in regulating migration and invasion of primary tumor cells, TAMs also mediate crucial functions on cancer cells disseminated at secondary tissues [26].
The term “metastasis-associated macrophages” (MAMs) is proposed to describe the role of macrophages that have infiltrated at the metastatic site. MAMs are essential for the extravasation of circulating tumor cells (CTCs) and their successful outgrowth at the secondary site, partly through VEGF expression [27]. The expression of CCL2 and the infiltration of the tumor site by macrophages have been correlated with metastatic disease in breast cancer [28,29]. MAMs that originate from inflammatory monocytes (IMs), are recruited to secondary sites along with monocytes expressing the CCR2 receptor. The stroma, as well as the tumor itself, are responsible for attracting these cells at the metastatic site by expressing CCL2 [30]. CCR2 activation following binding to CCL2 in MAMs, induces the secretion of the chemokine ligand CCL3 by macrophages at the metastatic site; this enables the retention of macrophages at the lung and increases the number of lung metastatic foci, whereas inhibition of CCR1, the receptor of CCL3, may have therapeutic implications in breast cancer lung metastasis [31]. Moreover, vascular cell adhesion molecule-1 (VCAM-1) expressed in breast cancer cells has been associated with lung metastasis relapse [32]. Following infiltration of breast cancer cells to the leukocyte-rich microenvironment of the lung, VCAM-1 provides a survival advantage by tethering MAMs to cancer cells via counter-receptor α4 integrins [32].
2.2. Role of Mesenchymal Stem Cells in Regulating Metastasis
Mesenchymal stem (or stromal) cells (MSCs) are multipotent stem cells that reside in many adult tissues, such as the bone marrow, adipose tissue, liver, lung, periosteum, muscle connective tissue, and spleen. They are important for generating and repairing skeletal tissues, such as cartilage and bone [33]. MSCs reside in most tumors and significantly influence the development and function of the TME. These cancer-associated MSC (CA-MSC) are reprogrammed by the tumor to exert pro-tumorigenic functions, such as enhancing EMT, promoting angiogenesis and metastasis.
Importantly, MSCs facilitate metastases by secreting exosomes which interact with cancer cells to affect their proliferation and migration [34,35]. They are the only type of cells that can mass produce exosomes [36]. Exosomes derived from MSCs are microvesicles (60–200 nm size) that have a phospholipid bilayer carrying proteins, lipids, miRNAs and mRNA [37]. They act in a paracrine fashion and can be detected in various body fluids [38]. In a breast cancer model, treatment with MSC-exosomes led to an enhanced migratory ability, through increased β-catenin levels and activation of WNT pathway target genes, Axin2 and Dkk1 [39]. Gastric cancer tissue-related mesenchymal stem cells (GC-MSCs), excrete exosomes carrying miRNAs that following delivery into gastric cancer cells can promote gastric cancer metastasis [40]. Particularly, the expression of miR-221 was significantly increased and correlated with enhanced local invasion, advanced tumor-node-metastasis stage, and lymphatic metastasis [41]. Overall, the presence of MSC-derived exosomes induced an EMT program and promoted migration and invasion of HGC-27 gastric cancer cells [42]. Bone marrow-derived mesenchymal stem cells (BM-MSCs), can also promote the migration of multiple myeloma cells by producing exosomes which selectively carry cytokines, such as chemotactic proteins MCP-1, MCP-2, MCP-3, 40 SDF-1, 41,42, and IGF-1 [43].
Contradicting to these reports, MSCs were also found to suppress metastatic tumor growth through their excreted exosomes carrying different strands of miRNAs. MSCs that interact with disseminated breast cancer cells in the bone marrow during the early stages of dissemination, promote cancer cell dormancy and enable an extended period of cycling quiescence in which cancer cells are maintained in G0/G1 phase of the cell cycle [44,45]. MSCs that produce exosomes with increased miR-23b and decreased MARCKS expression suppress cell cycle and promote dormancy of metastatic breast cancer cells [46,47].
2.3. Cancer-Associated Fibroblasts in Promoting Metastasis
CAFs constitute one of the most abundant stromal components in solid tumors. CAFs are distinguished from different cell subtypes based on the presence of several stromal markers, including integrin β1 (CD29), fibroblast activation protein (FAP), and α-smooth muscle actin (α-SMA) [48,49]. CAFs can be derived from different cell types of the TME: local fibroblasts that undergo mesenchymal–mesenchymal transition (MMT), epithelial cells via epithelial-to-mesenchymal transition (EMT), endothelial cells following endothelial-to-mesenchymal transition (endMT), bone marrow originated from hematopoietic stem cells or mesenchymal stem cells and adipocytes [50]. Cancer cells can activate fibroblasts in a three-step process: recruitment, transformation to CAFs, and maintenance in the TME. Following their activation, CAFs release signaling molecules to favor the survival of cancer cells and promote the recruitment and transformation of other cell types within the TME [51]. CAFs facilitate remodelling of the ECM by releasing collagen and fibronectin, producing MMPs, and increasing VEGF levels. This leads to the re-organization of the matrix, creating tracks which neoplastic cells exploit to directionally migrate, accompanied by CAFs [52,53,54,55,56,57].
The presence of a specific subset of CAFs in the microenvironment, CAF-S1, was recently shown to suppress the immune system by attracting and promoting the survival, differentiation, and activation of CD4+CD25+ T lymphocytes [49]. In addition, in women with primary tumors smaller than 2 cm without lymph node metastasis, the presence of CAF-S1 cells favors breast cancer metastasis to the bone via CDH11/osteoblast cadherin [58].
2.4. Endothelial Cells Attract Cancer Cells to the Metastatic Site
The lymphatic vessels that support the tumor at the secondary site are lined with loosely-connected lymphatic endothelial cells (LECs) that may also promote metastasis [59,60]. LECs recruit tumor cells by producing chemoattractants, such as CCL21 and SDF-1, which bind to CCR7 and CXCR4 receptors expressed in cancer cells, respectively [61]. Tumors developing at secondary organs produce factors that condition LECs to facilitate with cancer cell recruitment, extravasation, and outgrowth [62]. One example is the secretion of IL-6 by tumor cells that leads to STAT3 activation in LECs and subsequently high VEGF expression [62]. The expression of VEGF induced by tumor cells has been associated with the activation of HIF-1 in LECs, suggesting that tumor-secreted factors may support and direct lymphatic metastasis.
2.5. Components in the Blood Microenvironment That Facilitate Metastasis
During their dissemination throughout the body, circulating tumor cells (CTCs) encounter other cell types and factors in the peripheral blood that facilitate not only their survival but also their metastatic ability. These include various components, such as platelets, immune cells, cytokines, and circulating tumor microemboli (CTMs), which interact with CTCs and promote their survival [63]. Metastatic tumor cells can induce platelet adhesion and aggregation through the production of platelet activators such as ADP, thrombin, thromboxane, and von Willebrand factor [64]. Platelets enable the survival of cancer cells during their transit within the blood circulation and their colonization at the secondary site [65]. Platelets are a major source of lysophosphatidic acid (LPA), a natural lysophospholipid, which can bind to six different G-protein coupled receptors (GPCRs—LPA1-6 receptors) expressed on eukaryotic cells and activate multiple intracellular signaling pathways involved in cell survival, proliferation, differentiation, motility, cytoskeleton rearrangement and cytokine secretion [66]. Tumor cells induce platelet aggregation and production of LPA. Autotaxin (ATX), a lysophospholipase D also produced and released in platelet α-granules, is responsible for the basal concentration of LPA in blood. LPA interacts with different GPCRs found on cancer cells and promotes metastasis. The presence of certain cytokines in serum, including IL-17A, has also been correlated with increased number of CTCs and metastatic burden [67,68].
3. Role of Extracellular TME Components in Tumor Progression
3.1. Role of the ECM in Cancer Metastasis
Similar to stromal cells, the non-cellular component of the TME, the ECM, exerts determinant roles in tumor progression and metastasis. ECM is defined as a network of extracellular proteins and other macromolecules, including collagen, fibronectin, hyaluronan, elastin, integrins, microfibrillar proteins, and proteoglycans that provide structural and biochemical support to the tissue. ECM is present at the BM and interstitial space and regulates cell proliferation, differentiation, and tissue homeostasis [69]. Under pathological conditions like tumorigenesis, it functions as a biological barrier restraining tumor cells from proliferating and metastasizing. However, during tumor progression, ECM is remodeled and transformed into a metastasis-promoting microenvironment [70]. Such structural rearrangements involve the excessive production of collagen in the interstitial matrix and subsequent development of fibrosis, a hallmark of many desmoplastic tumors [71]. This fibrotic response predominantly occurs due to TGF-β-mediated activation of CAFs, which are the major drivers of collagen synthesis. Fibrosis involves not only upregulation of collagen but also Lysyl oxidase (LOX)-induced cross-linking of collagen fibers further causing tumor stiffening [72]. Individuals with high mammographic density (i.e., a greater accumulation of connective tissue to fat) are in greater risk for breast cancer development [73,74]. Furthermore, the differentially stiffened stroma combined with tumor cell overpopulation in a physically restricted area impose the development of compressive mechanical forces within the tumor, known as solid stress [75]. It has been estimated in humans that this growth-induced solid stress can be as high as 142.4 mmHg (19.0 kPa) [76]. Cancer cells respond to stiffness and mechanical compression by undergoing actomyosin and cytoskeleton contraction facilitating the formation of traction forces on their surroundings. Tumor cells become hyper-responsive to these matrix compliance cues, which are propagated intercellularly via mechanosensors, such as integrin-ECM complexes, growth factors and p130-associated proteins. Upon stimulation, mechanosensors transduce the signal to focal adhesion signaling molecules including small Rho-GTPases, FAK, SRC, paxillin, and RAS GTPase to activate downstream signaling cascades to promote malignancy [75,77,78,79,80,81,82,83]. In pancreatic cancer, solid stress can either activate fibroblasts or directly act on pancreatic cancer cells to promote migration via the GDF15-Akt pathway [84,85]. Moreover, mechanical compression facilitates migration of glioblastoma cells by inducing Mek1/Erk1 signaling [86]. Overall, tumors possessing a dynamic stiffened ECM are often highly metastatic and correlate with poorer patient outcome [72,78,87,88,89].
3.2. Hypoxic Microenvironment as a Major Driver of Cancer Metastasis
Solid stress and tumor stiffening contribute to metastasis not only by increasing directly the invasive and metastatic potential of cancer cells but also by inducing hypoxia. Specifically, the acquisition of solid stress can largely deform the surrounding tissue and compress or even collapse intratumoral lymphatic and blood vessels resulting in poor perfusion [90]. Tumor cells which have been deprived of oxygen and nutrients trigger the expression of pro-angiogenic factors such as VEGF, to induce the de novo formation of blood vessels ensuring the adequate supply of O2 and nutrients to the tumor. However, these “neovessels” are tortuous and leaky. The lack of intercellular junctions between endothelial cells and poor pericyte coverage foster an uneven distribution of blood flow. Consequently, in response to local hypoxia, the protein levels of hypoxia inducible factors (HIFs) increase and play a major role in regulating this process by promoting the survival of cancer cells under hypoxic conditions [91]. HIF is a heterodimeric transcription factor comprised of HIF-1α or HIF-2α and HIF-1β subunits. HIF interacts with its co-activator CBP/p300, and binds to hypoxia response elements located in target gene promoters to activate them [92].
During hypoxia, cancer cells change their metabolic activities by switching from oxidative phosphorylation to aerobic glycolysis which causes acidification of the extracellular space. Acidosis is a major physiological parameter of TME linked to hypoxia which allows the survival of selected cells that can adapt to these acidic conditions. As tumor cells undergo rapid rounds of proliferation, the energy consumption dramatically increases resulting in oxygen deprivation. To meet the biosynthetic requirements, tumors shift into aerobic glycolysis, known as Warburg effect, whereby glucose is converted into lactate, followed by lactic acid fermentation in the cytosol. The excess of lactate is then released in the TME along with other acidic materials, establishing an acidic environment. Importantly, the pH of tumors can decrease to 5.7 compared to the pH of healthy tissues which is 7.4. This pH reduction is even more striking in the lysosomes and endosomes, where it ranges from 4.5 to 5.5 and, thus, may interfere with the activity of therapeutic agents which utilize these structures for their intracellular transport [93,94,95].
Induction of hypoxia activates a vicious circle of downstream signaling cascades to promote responses that define cancer hallmarks, including metabolic reprogramming, mesenchymal transformation of cells, proliferation, survival, angiogenesis, migration, invasion, immunosuppression, and metastasis [96]. Approximately 50–60% of solid tumors exhibit hypoxic regions where O2 tension can be low (<10 mmHg) and heterogeneously distributed within the tumor. Hypoxia affects the TME and puts selective pressure on cancer cells that develop genetic and/or epigenetic adaptive changes in order to survive and in combination with the formation of new vessels, mainly at the tumor periphery, eventually metastasize to distant sites [97,98,99].
4. Targeting Cellular Constituents of the TME to Block Metastasis
4.1. TAMs as a Promising Target against Cancer Metastasis
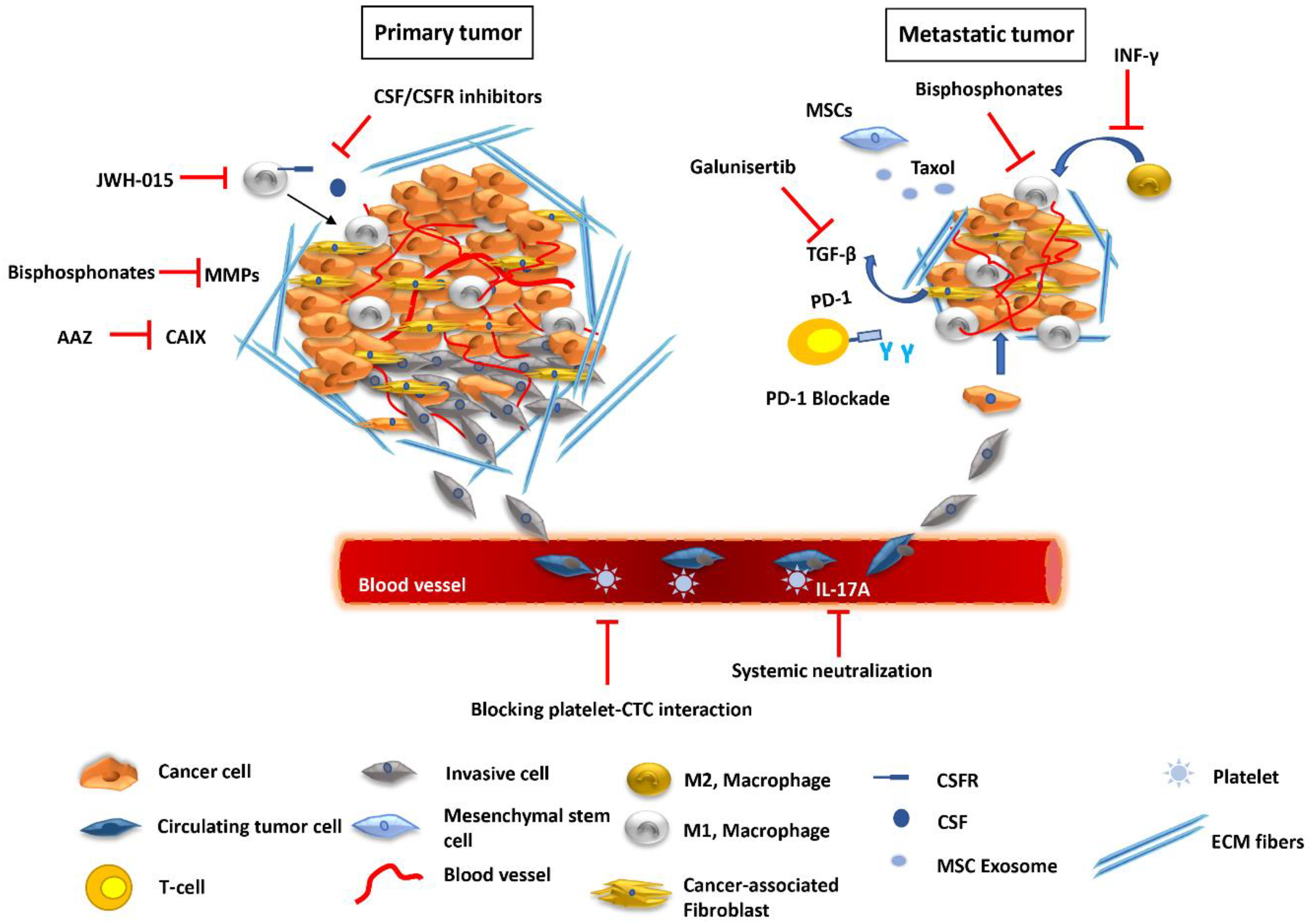
Targeting TAMs at the primary site has been a promising approach to combat metastatic disease. As described above, the presence of TAMs at the primary tumor site has been correlated with progressive disease and metastasis. Specifically, these cells enable EMT and help cancer cells escape towards the circulation. To block this metastasis enabling step, the role of JWH-015, a cannabinoid receptor 2 (CB2) agonist previously shown to suppress lung cancer progression [100], was investigated. JWH-105 inhibited EMT in non-small cell lung cancer cells (NSCLC) by suppressing ERK and STAT-3 activation and EGFR signaling; in addition, JWH-105 reduced invasiveness of A549 cells when co-cultured with M2 macrophages, by downregulating the expression of FAK, VCAM1, and MMP-2. The effects of the inhibitor were also confirmed using a syngeneic mouse model, where it blocked tumor growth in vivo and inhibited macrophage recruitment and EMT at the primary tumor [101]. TAMs are recruited to the tumor site by colony-stimulating factor-1 (CSF-1/M-CSF) to enhance their survival, differentiation and proliferation [102]. CSF-1 is a potent macrophage chemoattractant produced by cancer cells to recruit macrophages expressing the CSF-R1 receptor and polarizes them towards the M2-tumor promoting subtype [103]. Blocking CSF/CSFR interaction inhibits the pro-tumoral activities of TAMs and their ability to promote metastasis [104] (Figure 1).
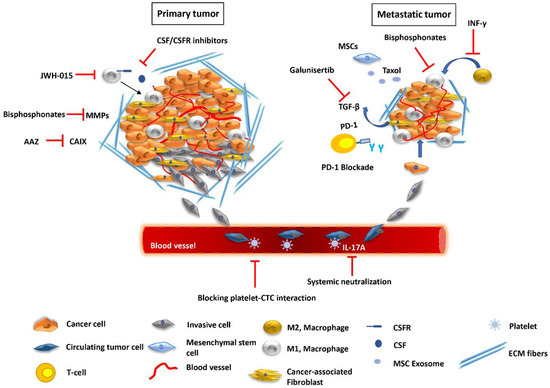
Figure 1.
Pharmaceutical regulation of the TME at various stages of the metastatic process. At the primary tumor site, JWH-015, a CB agonist, blocks macrophage recruitment, while other agents inhibit the interaction between CSFR and CSF produced by cancer cells. Bisphosphonates can block MMPs produced by CAFs and other types of cells and impair cancer cell invasion. CAIX produced under hypoxic conditions may be inhibited by small molecules, like AAZ. In the blood TME, blocking platelet interaction with CTCs as well as regulating cytokine content, such as of IL-17A, can effectively reduce metastatic burden. At the secondary site, bisphosphonates, including clodronate, can reduce the number of TAMs. Exosomes produced by manipulated MSCs can deliver anticancer therapeutics, such as Taxol, to inhibit distant metastases. INF-γ blocks the polarization of M1 macrophages to the M2-tumor promoting phenotype. Galunisertib can inhibit TGF-β signaling induced in the tumor by CAFs and is effective when combined with anti-PD-1 therapy, to promote T-cell activation.
Macrophages can also be targeted at the secondary metastatic site using chemical molecules. Liposomal encapsulation of clodronate (dichloromethylene diphosphonate), a bisphosphonate that acts by targeting osteoclasts and cancer cells, has been used to treat bone metastasis [105,106]. In addition, treatment with clodronate-liposomes is a well-established method for macrophage ablation [107]. The inhibition of metastasis by clodronate-liposomes may, therefore, be attributed to the depletion of osteoclasts precursors as well as TAMs. A distinct macrophage subpopulation (CD11b+Gr1−), was found to mediate extravasation and outgrowth of breast cancer cells to the lung. Treatment with liposomes bearing clodronate significantly reduced the number of tumor cells in murine lungs [27]. Using mice bearing lung tumors, liposomal delivery of clodronate was also shown to reduce the number of monocytes in peripheral blood and of macrophages in tumors, and to inhibit bone and muscle metastasis [108]. In a sorafenib-resistant tumor model, lung metastasis was inhibited following photoimmunotherapy targeting TAMs [109]. Moreover, dequalinium-14, an anti-tumor agent, was effective in reducing TAM motility and infiltration of irradiated tumors and blocked metastasis in a locally irradiated mouse model of CRC [110].
As previously mentioned, TAMs fuel cancer cells with pro-angiogenic factors within the TME to facilitate metastasis. One of the major factors that induce angiogenesis secreted by TAMs is MMP-9 that promotes the vascular development in avascular tumors and enables tumor cell intravasation [111,112]. However, targeting MMPs to reduce metastasis with the use of bisphosphonates has shown limited efficacy in pre-clinical and clinical studies [113,114,115]. The ability of TAMs to induce angiogenesis in tumors by secreting VEGF into the TME, was blocked in an in vivo model of gallbladder cancer, by intratumorally injecting IFN-γ. IFN-γ can inhibit the differentiation of monocytes to the tumor-promoting M2 macrophages in the TME, can switch TAMs from M2 into M1 subtype, blocking their ability to secrete VEGF [116]. The polarization of TAMs to the M2 phenotype can also be blocked by Luteolin which inhibits the IL4-mediated activation of STAT6, reduces the expression of M2-associated genes and suppresses TAM-secreted CCL2 to inhibit migration of Lewis lung carcinoma cells [117]. Finally, blocking the interaction of prostate cancer cells and TAMs, inhibited their proliferation, migration, and invasion as well as tumor growth in vivo [118].
4.2. Exploiting Cancer-Associated Mesenchymal Stroma/Stem-Like Cells to Control Metastasis
As discussed above, MSCs that associate with tumors excrete exosomes that carry components that affect the TME to promote or inhibit metastasis. MSCs can also be manipulated to deliver anti-cancer drugs to the tumor site [119]. In one study, several human MSC populations were treated with sub-lethal concentrations of taxol and exosomes carrying this drug were isolated. These taxol-loaded exosomes displayed enhanced cytotoxicity in cancer cell lines in vitro. Systemic intravenous administration of MSC-derived taxol-loaded exosomes in vivo significantly reduced the growth of subcutaneous primary highly metastatic MDA-hyb1 breast tumors. Importantly, the treatment also led to a significant reduction of distant metastases in the lung, liver, spleen, and kidney [120]. Moreover, MSCs loaded with paclitaxel strongly inhibited lung metastasis of murine melanoma [121].
In addition, MSCs delivering miR-124 and miR-145 synthetic mimics to co-cultured glioma cells significantly decreased their migration by targeting SCP-1 and Sox2 genes, respectively [122]. MSCs producing exosomes that deliver the synthetic miR-143 to osteosarcoma cells can significantly reduce their migration [123]. Manipulated therapeutic stem cells encapsulated in biodegradable, synthetic extracellular matrix (sECM) that could release tumor-selective S-TRAIL, eliminated tumor cells in a glioblastoma mouse model and significantly prolonged animal survival [124].
4.3. Targeting the Blood Microenvironment
Functional blocking of platelet activity leads to inhibition of cancer cell metastasis. Anti-platelet drugs have been explored in cancer treatment. Resting platelets are activated by ADP produced by cancer cells. APT102, an ADPase that can block platelet function, was able to disrupt bone metastasis in mice when combined with aspirin [125]. In addition, blocking the LPA/ATX signaling axis has been shown to be effective against metastasis. Treatment of animals with the BMP22 ATX inhibitor, inhibited cancer cell colonization to the bone [126]. In addition, taking advantage of the interaction of platelets with CTCs may be a promising therapeutic approach against metastasis. Genetically modified platelets that express TRAIL can significantly eliminate the tumor cells in vitro and suppress metastasis in a prostate cancer mouse model [127].
Regulating the cytokine content of peripheral blood may also help reduce tumor burden. IL-17A, a pro-inflammatory cytokine, has emerged as a critical factor in enhancing breast cancer metastasis. The systemic neutralization of IL-17A significantly reduces breast cancer metastasis in mice by reducing expression of CXCL12/SDF-1 in the metastatic niches [128]. When cancer cells pass through organs with high levels of the chemokine SDF-1/CXCL12, they exit circulation and extravasate [129]. The ablation of IL-17A and treatment with granulocyte-macrophage colony-stimulating factor (GM-CSF) causes a decline in the number of CTCs and decreased metastasis in mice (Figure 1). GM-CSF administration polarized the TAMs toward the M1 phenotype, elevated the number of CD4+ and CD8+ T lymphocytes and NK cells and eliminated CTCs [67].
5. Strategies to Improve Tumor Oxygenation and Therapeutic Efficacy
As described above, the dense ECM and the solid stress applied in desmoplastic tumors contribute to metastasis not only by increasing directly the invasive and metastatic potential of cancer cells but also by inducing hypoxia and hindering drug delivery owing to hypo-perfusion caused by vessel compression [130,131]. There are two main strategies to overcome these physiological abnormalities of the TME: (i) the vascular remodeling and (ii) the stroma normalization strategy.
5.1. Remodeling the Tumor Vasculature
In contrast to vascular disruption, the vascular normalization strategy involves the restoration of a functional vasculature that closely resembles the normal and is mediated by increasing the pericyte coverage of endothelial cells, limiting leakiness of blood vessels and, thus, increasing tumor perfusion and oxygenation. This approach alleviates the geometric obstruction against blood flow and re-establishes the balance between pro- and anti-angiogenic signaling [132,133]. A classical therapeutic target of vascular normalization is VEGF signaling, which is upregulated in most tumors. Bevacizumab, the first approved anti-angiogenic drug, and its derivatives are currently used for the treatment of metastatic CRC [134]. Bevacizumab interacts with soluble VEGF preventing receptor binding. To avoid tumor acquired resistance, these anti-angiogenic drugs are used in combination with tyrosine receptor kinases inhibitors (e.g., sorafenib, and sunatinib) acting downstream in the signaling cascade or as cocktail (e.g., with Herceptin) [135,136,137,138]. An alternative therapeutic approach is the application of anti-angiogenic peptides like thrombospondin (TSP), endostatin, coagulation peptides, growth factors and chemokines, all having a high success rate in clinical trials due to their low toxicity and high specificity for their receptors [139]. Many studies have demonstrated that pre-treatment of tumors with VEGF signaling inhibitors improves delivery of both intermediate and large-size nanoparticles (NPs) by inducing vascular normalization, increasing the expression of MMPs and degradation of collagen fibers and, thus, potentiating drug penetration [140,141,142,143]. However, not all cancer types are benefited by the vascular normalization strategy. For instance, the less permeable and compressed vasculature of desmoplastic tumors may not exhibit the expected normalization phenotype [136]. Vessel density, anti-angiogenic drug dose, and treatment intervals are important factors influencing therapeutic outcome [144]. Additionally, reduction in vessel pore size may hamper large NPs from entering the tumor stroma [145,146,147]. Therefore, alternative strategies applied alone or in combination with vascular normalization should be considered to improve treatment outcomes.
5.2. Stroma Normalization Strategy to Target Hypoxia
Apart from promoting metastasis, the dense ECM can act as a physical barrier to the penetration of immune cells within the TME, creating an immune-excluded phenotype. Furthermore, the compression of intratumoral vessels owing to tumor stiffening and solid stress elevation can cause an inefficient and heterogeneous distribution of blood flow in the tumor resulting in insufficient and non-uniform delivery of drugs and immune cells to the tumor and hypoxia, which can further support tumor progression and metastasis [148]. Importantly, increased ECM density and vessel compression have been recently observed not only in the primary tumors but also in breast cancer metastasis in the lungs and has been related to compromised therapeutic efficacy in lung metastatic lesions [149]. Therefore, the stroma normalization strategy aims to restore vessel functionality by alleviating intratumoral solid stresses and reducing tumor stiffness [146,147], which allows for increased tumor perfusion and suppresses invasion and metastasis [150,151]. There are two routes to stroma normalization by: (a) CAF reprogramming and (b) ECM remodeling [152,153].
Targeting CAFs as an intratumoral solid stress alleviation approach, has yielded promising results. Although highly heterogenic, CAFs are generally divided into myofibroblastic and non-myofibroblastic populations across different cancer types. Myofibroblastic CAFs are responsible for ECM deposition contributing to tissue stiffness directly through the production of collagen and proteoglycans, while non-myofibroblasts are implicated in inflammatory signaling. Importantly, targeting CAFs and associated responses by sonic hedgehog signaling inhibition has shown to reduce solid stress and IFP in tumor models, enhancing the activity of cytotoxic agents like taxol and 5′-fluorouracil (5′-FU) [146,154,155,156]. However, this strategy has failed in clinical trials and preclinical studies have shown that excessive depletion of CAFs might fuel tumor progression [157,158,159]. In addition to their role in solid stress accumulation, CAFs along with other stromal components promote the establishment of an immunosuppressive TME via the release of various immunosuppressive ligands such as TGF-β, CXCL12, IL-6, CXCL-1, G-SCF, and others which can impede intratumoral cytotoxic T cell infiltration and activity and enhance the recruitment of MDSCs, neutrophils and M2-like TAMs [160]. The production of TGF-β by CAFs, allows invasive cancers to evade immune system surveillance by excluding T-cells from the microenvironment [161]. Concurrent treatment with therapeutic antibodies that inhibit the programmed death-1 (PD-1)–programmed death-ligand 1 (PD-L1) pathway and TGFβR1 kinase inhibitor, galunisertib, led to increased recruitment of CD8+ T cells to the liver colonized with CRC cells and reduced metastatic burden. In addition, combined targeting of TGF-β and PD-1/PD-L1 blockade reduced overall metastatic burden and caused complete tumor eradication in the majority of treated animals [162]. Similarly, in patients with metastatic urothelial cancer, concurrent targeting of the TGF-β and PD-1/PD-L1 axis led to increased T cell infiltration and significant anti-tumor response [163].
Regarding ECM remodeling, several studies have focused on modifying the two most abundant ECM components of desmoplastic tumors, collagen, and hyaluronan [148]. Targeting the ECM using monoclonal antibodies against TGF-β (ID11) as well as known antihypertensive drugs have been found to potentiate the distribution and efficacy of therapeutics [164]. A well-characterized example is the angiotensin II type I receptor inhibitor, losartan. Preclinical studies evaluating the effect of losartan in pancreatic and breast tumor models have demonstrated that losartan suppresses TGF-β signaling resulting in a subsequent downregulation of collagen I and hyaluronan synthesis and other downstream fibrotic factors, alleviating solid stress and IFP, all of which leading to enhanced vascular perfusion, improved efficacy of drugs and reduced metastasis [165,166,167,168,169] (Figure 2). The potential of losartan to modulate the tumor microenvironment and improve cancer therapy has been already shown in clinical trials in combination with chemoradiation in locally advanced pancreatic tumors [170,171,172,173]. Safety concerns have been raised, though, regarding the use of antihypertensive agents in cancer patients experiencing normal blood pressure or hypotension. Hence, additional approved agents have been repurposed for priming the TME including antihistamine drugs (e.g., tranilast) [149,174,175], corticosteroids (e.g., dexamethasone) [176], anti-inflammatory (e.g., pirfenidone) [177], anti-diabetic drugs (e.g., metformin) [178], and other agents possessing anti-fibrotic effects (e.g., pentoxifylline) [179], vitamin D [180], and relaxin [181,182,183,184].
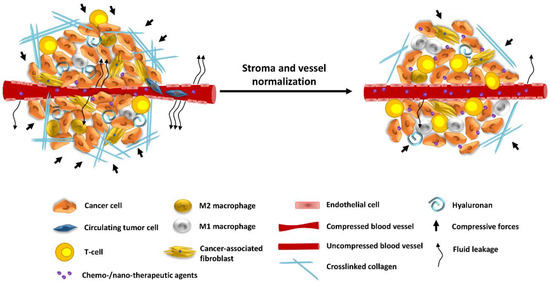
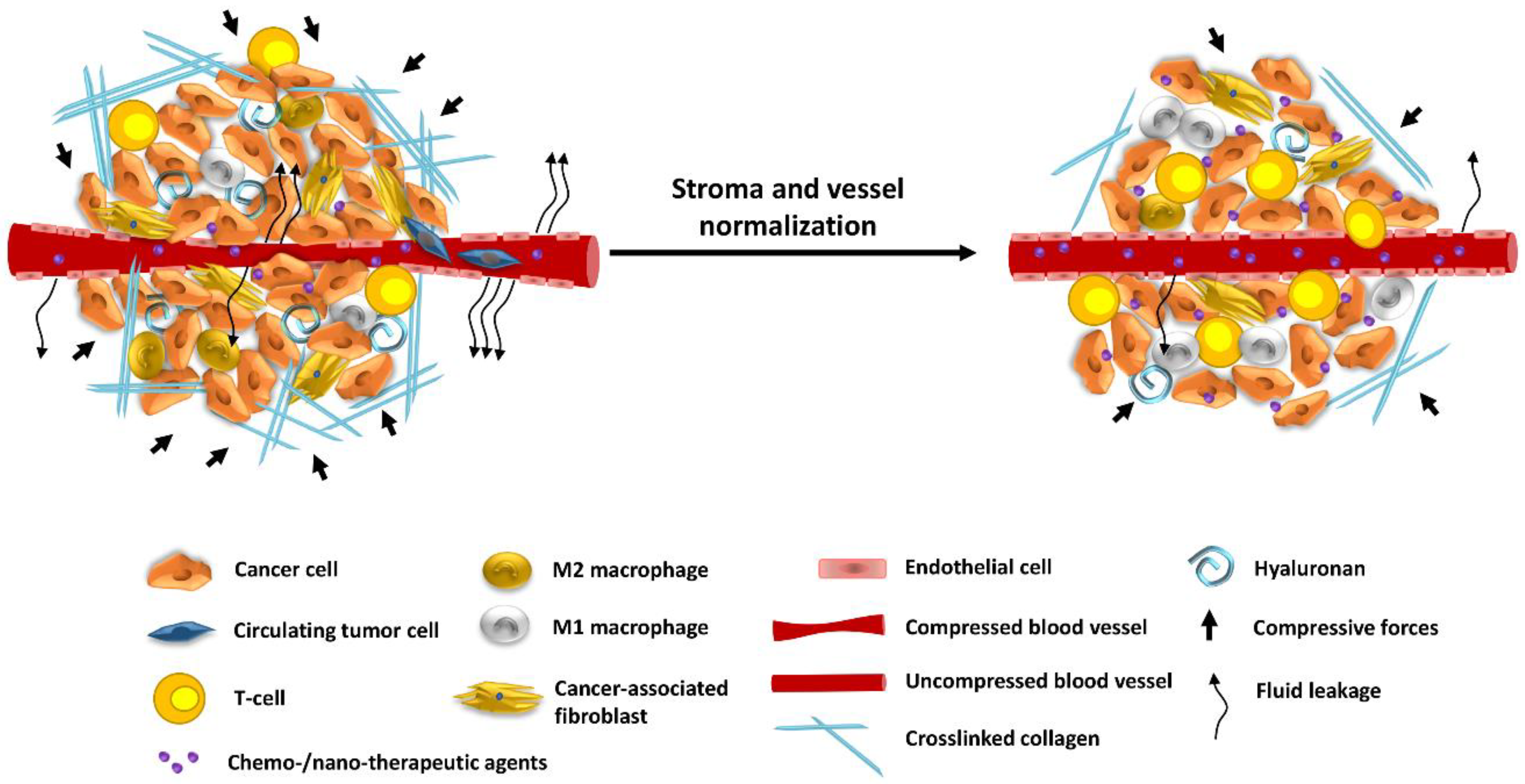
Figure 2.
Strategies to improve tumor oxygenation and therapeutic efficacy in primary and metastatic tumors. A desmoplastic TME is defined by excess ECM and dysfunctional vasculature. Abundantly found stromal structures, like collagen and hyaluronan, promote the development of compressive forces leading to blood vessel collapse, which in turn causes hypo-perfusion and hypoxia. In addition, the abnormally large vessel pores of some tumor vessels enhance fluid leakage to the interstitial space that further contributes to hypo-perfusion and hypoxia. Hypoxia recruits immunosuppressive immune cells, such as M2-macrophages, which in combination with T-cell exclusion and CAFs activation promote metastasis. Stroma and vessel normalization strategies aim to alleviate intratumoral forces and stiffness, decompress vessels, improve perfusion and heterogeneous delivery of chemo- and nano-therapeutic agents. Re-establishment of adequate oxygenation within the TME potentiates T cell infiltration, immunostimulation and suppresses metastasis.
6. Discussion—Future Perspectives
Currently, the development of novel therapeutic approaches for treating metastatic tumors specifically by remodeling the TME, is focused on combination studies, as monotherapies have had limited success in the clinic. Special attention is given on the concurrent modulation of the immune system. One example is anti-CD40 agonistic antibody therapy that involves CD8+ T cell-priming and T cell-mediated anti-tumor responses [185]. CD40 agonists bind to the CD40 receptor, a cell-surface member of the TNF receptor superfamily, expressed by APCs, including dendritic cells; once activated, dendritic cells activate T cells and prime them against tumors. Even though local or systemic administration of anti-CD40 treatment was shown to slow post-surgical metastatic growth in mice, it has performed moderately in pre-clinical studies [186]. In the TME, tumors and tumor-associated macrophages (TAMs) secrete immunosuppressive factors, such as the checkpoint modulator PD-L1, which diminish the cytotoxic functions of tumor-specific CD8+ T cells [187]. A recent study showed that in metastatic ductal pancreatic adenocarcinoma (PDAC) patients, the concurrent treatment with agonistic CD40 antibodies and anti-PD-1 treatment, can trigger effective T cell immunity [188]. In addition, the presence of Toll-like Receptors (TLRs) expressed in macrophages and other cells in the TME can provide immunosuppressive tumor protection. Treatment with TLR agonists, in combination with anti-PD-1 therapy, suppresses the growth of primary and metastatic tumors. Treatment with the TLR7 agonist increases the M1/M2 TAMs ratio and increases recruitment of activated CD8+ T cells in the TME in a mouse model of metastatic head and neck squamous cell carcinoma (HNSCC) [189].
Novel combination studies also include nanotherapeutics against metastasis. Current strategies developed to modulate the TME using NPs, include modifying tumor vasculature permeability, polarizing macrophages towards the M1 phenotype, affecting CAFs and stromal components modulating tumor hypoxia [94]. Gold nanoparticles (AuNPs), exhibiting low toxicity, can remodel the TME and may be used either with targeted therapeutics or conventional chemotherapy drugs [190]. AuNPs induce tumor vasculature normalization, increase blood perfusion, minimize hypoxia in melanoma tumors, and suppress lung metastasis [191].
In addition to manipulating the tumor vasculature and stroma to improve oxygenation, targeting other factors that contribute to the development of hypoxia in the TME were also found to effectively block metastasis [192]. In most solid tumors, hypoxia causes the production of carbonic anhydrase (CAIX). CAIX is involved in pH regulation, causes acidification of the tumor microenvironment leading to reduced cell adhesion, increased motility and migration, induction of neovascularization, and activation of proteases. Expression of CAIX is a poor prognostic marker in patients with metastatic cancer [193]. Since CAIX is implicated in regulating both extracellular and intracellular pH, targeting its enzymatic activity with specific pharmacological inhibitors is a logical approach against metastasis [194]. The efficacy of sulfamate CAIX inhibitors has been shown in in vitro and in vivo models of breast metastasis as well as in clinical Phase I/II trials [195,196,197]. Inhibition of CAIX using small molecule inhibitor AAZ can slow tumor growth, inhibit metastasis, and eliminate tumor stem cells in mice [198]. Therefore, combination strategies targeting cancer cell-derived molecules under hypoxic conditions along with TME remodeling agents which promote tumor oxygenation could be exploited as promising therapeutic approaches.
The experimental models utilized to study anti-metastatic therapy should also be revisited to include important TME components that seem to affect patient therapeutic outcomes. Metastasis-on-a-chip devices that house multiple bioengineered three-dimensional (3D) organoids can be used for the evaluation of therapeutic approaches against metastatic potential of cancer cells. A recent study showed that CRC cells specifically homed to liver and lung constructs, similarly to the clinical setting [199]. Moreover, novel 3D metastasis-on-a-chip model, which includes organ-specific extracellular microenvironment mimicking the progression of kidney cancer cells metastasizing to the liver, can be used to compare the efficacy of various therapeutic strategies [200].
In vivo metastasis models using immunosuppressed mice lack the important component of the immune system needed to fully characterize the therapeutic efficacy of a potential TME-modulating drug. Currently, substantial effort is being made to create humanized patient-derived xenograft (PDX) mouse models, for example using CD34+ HSCs, which more accurately recapitulate human immune responses [201]. The next generation of PDX mice will involve engraftment with a human immune system and are expected to be a valuable tool for assessing therapeutic approaches for metastatic tumors [202,203,204,205].
While developing therapeutics to target the metastatic process by modulating the TME, considerations should also be taken regarding the differences between the microenvironment at the primary and secondary tumor sites. In a recent paper discussing the differences between the TME at the breast and following metastasis to the brain, it was highlighted that the tissue of origin, such as lung, breast, or melanoma, determines the type of TME to be developed at the secondary site and how this will regulate metastatic outgrowth [206]. Evidence suggests that malignant cells facilitate metastasis by bringing their own soil from the primary site. The resident ECM composition, however, is also partially responsible for shaping the pre-metastatic niche environment [207,208,209]. Therefore, modulating one facet of the TME may not yield to the desirable anti-tumor effects, while the simultaneous targeting of multiple aspects could be a promising strategy. Conclusively, a thorough characterization of TME constituents must be taken prior to any rational design of combinatorial approaches to optimize drug delivery and assure optimal therapeutic responses against metastatic cancer.
Author Contributions
Conceptualization, C.M.N. and P.P.; writing—original draft preparation, C.M.N., M.P., T.S., and P.P.; writing—review and editing, C.M.N., M.P., T.S., and P.P.; visualization, C.M.N., M.P., T.S., and P.P.; funding acquisition, C.M.N. and P.P. All authors have read and agreed to the published version of the manuscript.
Funding
This work was co-funded by the European Regional Development Fund and the Republic of Cyprus through the Research and Innovation Foundation (Project: POST-DOC/0916/0044). T.S.’s research is supported by the European Research Council (ERC-2019-CoG-863955) and the Cyprus Research and Innovation Foundation (Grant INFRASTRUCTURE/1216/0052).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
| 5′-FU | 5′-fluorouracil |
| APCs | antigen presenting cells |
| ATX | autotaxin |
| BM | basement membrane |
| BM-MSCs | bone marrow-derived mesenchymal stem cells |
| CAFs | cancer associated fibroblasts |
| CA-MSC | cancer-associated MSC |
| CB2 | cannabinoid receptor 2 |
| CAIX | carbonic anhydrase |
| CCL2 | chemokine (C-C motif) ligand 2 |
| CTCs | circulating tumor cells |
| CTMs | circulating tumor microemboli |
| CSF-1 | colony-stimulating factor-1 |
| CRC | colorectal cancer |
| PDAC | pancreatic ductal adenocarcinoma |
| endMT | endothelial-to-mesenchymal transition |
| EMT | epithelial-to-mesenchymal transition |
| ECM | extracellular matrix |
| FAP | fibroblast activation protein |
| GC-MSCs | gastric cancer tissue-related mesenchymal stem cells |
| AuNPs | gold nanoparticles |
| GPCRs | G-protein coupled receptors |
| GM-CSF | granulocyte-macrophage colony-stimulating factor |
| HNSCC | head and neck squamous cell carcinoma |
| HSC | hematopoietic stem cells |
| HCC | hepatocellular carcinoma |
| IMs | inflammatory monocytes |
| IFN-γ | interferon-γ |
| KCNN4 | intermediate-conductance Ca2+-activated potassium channels |
| LECs | lymphatic endothelial cells |
| LPA | lysophosphatidic acid |
| LOX | lysyl oxidase |
| MMPs | matrix metalloproteinases |
| MSCs | mesenchymal stem cells |
| MMT | mesenchymal-mesenchymal transition |
| MAMs | metastasis-associated macrophages |
| NPs | nanoparticles |
| NK | natural killer cells |
| NSCLC | non-small cell lung cancer cells |
| PDX | patient-derived xenograft mouse |
| PD-L1 | programmed death-ligand 1 |
| PRL-3 | phosphatase of regenerating liver |
| S-TRAIL | secretable tumor necrosis factor apoptosis inducing ligand |
| sECM | synthetic extracellular matrix |
| TSP | thrombospondin |
| TLRs | toll-like Receptors |
| TME | tumor microenvironment |
| TMEM | tumor microenvironment of metastasis |
| TNF-α | tumor necrosis factor-α |
| TAMs | tumor-associated macrophages |
| VCAM-1 | vascular cell adhesion molecule-1 |
| α-SMA | α-smooth muscle actin |
References
- Fearon, E.R.; Vogelstein, B. A genetic model for colorectal tumorigenesis. Cell 1990, 61, 759–767. [Google Scholar] [CrossRef]
- Kurose, K.; Hoshaw-Woodard, S.; Adeyinka, A.; Lemeshow, S.; Watson, P.H.; Eng, C. Genetic model of multi-step breast carcino-genesis involving the epithelium and stroma: Clues to tumour-microenvironment interactions. Hum. Mol. Genet. 2001, 10, 1907–1913. [Google Scholar] [CrossRef]
- Kitamura, T.; Qian, B.-Z.; Pollard, J.W. Immune cell promotion of metastasis. Nat. Rev. Immunol. 2015, 15, 73–86. [Google Scholar] [CrossRef] [PubMed]
- Dunn, G.P.; Old, L.J.; Schreiber, R.D. The Immunobiology of Cancer Immunosurveillance and Immunoediting. Immunity 2004, 21, 137–148. [Google Scholar] [CrossRef]
- Eyles, J.; Puaux, A.-L.; Wang, X.; Toh, B.; Prakash, C.; Hong, M.; Tan, T.G.; Zheng, L.; Ong, L.C.; Jin, Y.; et al. Tumor cells disseminate early, but immunosurveillance limits metastatic outgrowth, in a mouse model of melanoma. J. Clin. Investig. 2010, 120, 2030–2039. [Google Scholar] [CrossRef]
- Paolino, M.; Choidas, A.; Wallner, S.; Pranjic, B.; Uribesalgo, I.; Loeser, S.; Jamieson, A.M.; Langdon, W.Y.; Ikeda, F.; Fededa, J.P.; et al. The E3 ligase Cbl-b and TAM receptors regulate cancer metastasis via natural killer cells. Nat. Cell Biol. 2014, 507, 508–512. [Google Scholar] [CrossRef]
- Bidwell, B.N.; Slaney, C.Y.; Withana, N.P.; Forster, S.; Cao, Y.; Loi, S.; Andrews, D.; Mikeska, T.; Mangan, N.E.; Samarajiwa, S.A.; et al. Silencing of Irf7 pathways in breast cancer cells promotes bone metastasis through immune escape. Nat. Med. 2012, 18, 1224–1231. [Google Scholar] [CrossRef]
- McAllister, S.S.; Weinberg, R.A. The tumour-induced systemic environment as a critical regulator of cancer progression and metastasis. Nat. Cell Biol. 2014, 16, 717–727. [Google Scholar] [CrossRef]
- Neophytou, C.M.; Pierides, C.; Christodoulou, M.I.; Costeas, P.; Kyriakou, T.C.; Papageorgis, P. The Role of Tumor-Associated My-eloid Cells in Modulating Cancer Therapy. Front. Oncol. 2020, 10, 899. [Google Scholar] [CrossRef]
- Whipple, C.A. Tumor talk: Understanding the conversation between the tumor and its microenvironment. Cancer Cell Microenviron. 2015, 2, e773. [Google Scholar] [PubMed]
- Singh, S.; Mehta, N.; Lilan, J.; Budhthoki, M.B.; Chao, F.; Yong, L. Initiative action of tumor-associated macrophage during tumor metastasis. Biochim. Open 2017, 4, 8–18. [Google Scholar] [CrossRef]
- Smith, H.A.; Kang, Y. The metastasis-promoting roles of tumor-associated immune cells. J. Mol. Med. 2013, 91, 411–429. [Google Scholar] [CrossRef]
- Sanchez, L.R.; Borriello, L.; Entenberg, D.; Condeelis, J.S.; Oktay, M.H.; Karagiannis, G.S. The emerging roles of macrophages in cancer metastasis and response to chemotherapy. J. Leukoc. Biol. 2019, 106, 259–274. [Google Scholar] [CrossRef]
- Wang, R.; Zhang, J.; Chen, S.; Lu, M.; Luo, X.; Yao, S.; Liu, S.; Qin, Y.; Chen, H. Tumor-associated macrophages provide a suitable microenvironment for non-small lung cancer invasion and progression. Lung Cancer 2011, 74, 188–196. [Google Scholar] [CrossRef]
- Robinson, B.D.; Sica, G.L.; Liu, Y.-F.; Rohan, T.E.; Gertler, F.B.; Condeelis, J.S.; Jones, J.G. Tumor Microenvironment of Metastasis in Human Breast Carcinoma: A Potential Prognostic Marker Linked to Hematogenous Dissemination. Clin. Cancer Res. 2009, 15, 2433–2441. [Google Scholar] [CrossRef] [PubMed]
- Thiery, J.P.; Acloque, H.; Huang, R.Y.; Nieto, M.A. Epithelial-Mesenchymal Transitions in Development and Disease. Cell 2009, 139, 871–890. [Google Scholar] [CrossRef]
- Papageorgis, P. TGFbeta Signaling in Tumor Initiation, Epithelial-to-Mesenchymal Transition, and Metastasis. J. Oncol. 2015, 2015, 587193. [Google Scholar] [CrossRef]
- Gupta, D.K.; Singh, N.; Sahu, D.K. TGF-beta Mediated Crosstalk Between Malignant Hepatocyte and Tumor Microenvironment in Hepatocellular Carcinoma. Cancer Growth Metastasis 2014, 7, 1–8. [Google Scholar] [CrossRef]
- Zhu, X.-D.; Zhang, J.-B.; Zhuang, P.-Y.; Zhu, H.-G.; Zhang, W.; Xiong, Y.-Q.; Wu, W.-Z.; Wang, L.; Tang, Z.-Y.; Sun, H.-C. High Expression of Macrophage Colony-Stimulating Factor in Peritumoral Liver Tissue Is Associated with Poor Survival After Curative Resection of Hepatocellular Carcinoma. J. Clin. Oncol. 2008, 26, 2707–2716. [Google Scholar] [CrossRef]
- Lewis, C.E.; Pollard, J.W. Distinct Role of Macrophages in Different Tumor Microenvironments. Cancer Res. 2006, 66, 605–612. [Google Scholar] [CrossRef]
- Liu, C.Y.; Xu, J.Y.; Shi, X.Y.; Huang, W.; Ruan, T.Y.; Xie, P.; Ding, J.L. M2-polarized tumor-associated macrophages promoted epitheli-al-mesenchymal transition in pancreatic cancer cells, partially through TLR4/IL-10 signaling pathway. Lab. Investig. 2013, 93, 844–854. [Google Scholar] [CrossRef]
- Wang, H.; Wang, X.; Li, X.; Fan, Y.; Li, G.; Guo, C.; Zhu, F.; Zhang, L.; Shi, Y. CD68(+)HLA-DR(+) M1-like macrophages promote motility of HCC cells via NF-kappaB/FAK pathway. Cancer Lett. 2014, 345, 91–99. [Google Scholar] [CrossRef]
- Chu, Z.; Lai, W.; Chen, S.; Wu, H.; Guan, Y.; Liu, L.; Zeng, Y.; Zhao, H.; Jiang, J. PRL-3 promotes the proliferation of LoVo cells via the upregulation of KCNN4 channels. Oncol. Rep. 2011, 26, 909–917. [Google Scholar] [CrossRef][Green Version]
- Xu, H.; Lai, W.; Zhang, Y.; Liu, L.; Luo, X.; Zeng, Y.; Wu, H.; Lan, Q.; Chu, Z. Tumor-associated macrophage-derived IL-6 and IL-8 enhance invasive activity of LoVo cells induced by PRL-3 in a KCNN4 channel-dependent manner. BMC Cancer 2014, 14, 330. [Google Scholar] [CrossRef]
- Lin, L.; Chen, Y.S.; Yao, Y.D.; Chen, J.Q.; Chen, J.N.; Huang, S.Y.; Zeng, Y.J.; Yao, H.R.; Zeng, S.H.; Fu, Y.S.; et al. CCL18 from tumor-associated macrophages promotes angio-genesis in breast cancer. Oncotarget 2015, 6, 34758–34773. [Google Scholar] [CrossRef]
- Lin, Y.; Xu, J.; Lan, H. Tumor-associated macrophages in tumor metastasis: Biological roles and clinical therapeutic applica-tions. J. Hematol. Oncol. 2019, 12, 76. [Google Scholar] [CrossRef]
- Qian, B.; Deng, Y.; Im, J.H.; Muschel, R.J.; Zou, Y.; Li, J.; Lang, R.A.; Pollard, J.W. A Distinct Macrophage Population Mediates Metastatic Breast Cancer Cell Extravasation, Establishment and Growth. PLoS ONE 2009, 4, e6562. [Google Scholar] [CrossRef]
- Ueno, T.; Toi, M.; Saji, H.; Muta, M.; Bando, H.; Kuroi, K.; Koike, M.; Inadera, H.; Matsushima, K. Significance of macrophage chemoattractant protein-1 in macrophage recruitment, angiogenesis, and survival in human breast cancer. Clin. Cancer Res. 2000, 6, 3282–3289. [Google Scholar]
- Saji, H.; Koike, M.; Yamori, T.; Saji, S.; Seiki, M.; Matsushima, K.; Toi, M. Significant correlation of monocyte chemoattractant protein-1 expression with neovascularization and progression of breast carcinoma. Cancer 2001, 92, 1085–1091. [Google Scholar] [CrossRef]
- Qian, B.-Z.; Li, J.; Zhang, H.; Kitamura, T.; Zhang, J.; Campion, L.R.; Kaiser, E.A.; Snyder, L.A.; Pollard, J.W. CCL2 recruits inflammatory monocytes to facilitate breast-tumour metastasis. Nature 2011, 475, 222–225. [Google Scholar] [CrossRef]
- Kitamura, T.; Qian, B.-Z.; Soong, D.; Cassetta, L.; Noy, R.; Sugano, G.; Kato, Y.; Li, J.; Pollard, J.W. CCL2-induced chemokine cascade promotes breast cancer metastasis by enhancing retention of metastasis-associated macrophages. J. Exp. Med. 2015, 212, 1043–1059. [Google Scholar] [CrossRef] [PubMed]
- Chen, Q.; Zhang, X.H.-F.; Massagué, J. Macrophage Binding to Receptor VCAM-1 Transmits Survival Signals in Breast Cancer Cells that Invade the Lungs. Cancer Cell 2011, 20, 538–549. [Google Scholar] [CrossRef] [PubMed]
- Ding, D.-C.; Shyu, W.-C.; Lin, S.-Z. Mesenchymal Stem Cells. Cell Transplant. 2011, 20, 5–14. [Google Scholar] [CrossRef]
- Zhou, J.; Tan, X.; Tan, Y.; Li, Q.; Ma, J.; Wang, G. Mesenchymal Stem Cell Derived Exosomes in Cancer Progression, Metastasis and Drug Delivery: A Comprehensive Review. J. Cancer 2018, 9, 3129–3137. [Google Scholar] [CrossRef]
- Atiya, H.; Frisbie, L.; Pressimone, C.; Coffman, L. Mesenchymal Stem Cells in the Tumor Microenvironment. Adv. Exp. Med. Biol. 2020, 1234, 31–42. [Google Scholar] [CrossRef]
- Yeo, R.W.Y.; Lai, R.C.; Zhang, B.; Tan, S.S.; Yin, Y.; Teh, B.J.; Lim, S.K. Mesenchymal stem cell: An efficient mass producer of exosomes for drug delivery. Adv. Drug Deliv. Rev. 2013, 65, 336–341. [Google Scholar] [CrossRef] [PubMed]
- Simpson, R.J.; Lim, J.W.; Moritz, R.L.; Mathivanan, S. Exosomes: Proteomic insights and diagnostic potential. Expert Rev. Proteom. 2009, 6, 267–283. [Google Scholar] [CrossRef] [PubMed]
- Mathivanan, S.; Fahner, C.J.; Reid, G.E.; Simpson, R.J. ExoCarta 2012: Database of exosomal proteins, RNA and lipids. Nucleic Acids Res. 2011, 40, D1241–D1244. [Google Scholar] [CrossRef]
- Lin, R.; Wang, S.; Zhao, R.C. Exosomes from human adipose-derived mesenchymal stem cells promote migration through Wnt signaling pathway in a breast cancer cell model. Mol. Cell. Biochem. 2013, 383, 13–20. [Google Scholar] [CrossRef]
- Wang, M.; Zhao, C.; Shi, H.; Zhang, B.; Zhang, L.; Zhang, X.; Wang, S.; Wu, X.; Yang, T.; Huang, F.; et al. Deregulated microRNAs in gastric cancer tissue-derived mesen-chymal stem cells: Novel biomarkers and a mechanism for gastric cancer. Br. J. Cancer. 2014, 110, 1199–1210. [Google Scholar] [CrossRef]
- Liu, K.; Li, G.; Fan, C.; Diao, Y.; Wu, B.; Li, J. Increased Expression of MicroRNA-221 in gastric cancer and its clinical significance. J. Int. Med. Res. 2012, 40, 467–474. [Google Scholar] [CrossRef] [PubMed]
- Gu, H.; Ji, R.; Zhang, X.; Wang, M.; Zhu, W.; Qian, H.; Chen, Y.; Jiang, P.; Xu, W. Exosomes derived from human mesenchymal stem cells promote gastric cancer cell growth and migration via the activation of the Akt pathway. Mol. Med. Rep. 2016, 14, 3452–3458. [Google Scholar] [CrossRef]
- Wang, J.; Hendrix, A.; Hernot, S.; Lemaire, M.; De Bruyne, E.; Van Valckenborgh, E.; Lahoutte, T.; De Wever, O.; Vanderkerken, K.; Menu, E.; et al. Bone marrow stromal cell-derived ex-osomes as communicators in drug resistance in multiple myeloma cells. Blood 2014, 124, 555–566. [Google Scholar] [CrossRef] [PubMed]
- Casson, J.; Davies, O.G.; Smith, C.-A.; Dalby, M.J.; Berry, C.C. Mesenchymal stem cell-derived extracellular vesicles may promote breast cancer cell dormancy. J. Tissue Eng. 2018, 9. [Google Scholar] [CrossRef]
- Neophytou, C.M.; Kyriakou, T.-C.; Papageorgis, P. Mechanisms of Metastatic Tumor Dormancy and Implications for Cancer Therapy. Int. J. Mol. Sci. 2019, 20, 6158. [Google Scholar] [CrossRef] [PubMed]
- Ono, M.; Kosaka, N.; Tominaga, N.; Yoshioka, Y.; Takeshita, F.; Takahashi, R.-U.; Yoshida, M.; Tsuda, H.; Tamura, K.; Ochiya, T. Exosomes from bone marrow mesenchymal stem cells contain a microRNA that promotes dormancy in metastatic breast cancer cells. Sci. Signal. 2014, 7, ra63. [Google Scholar] [CrossRef]
- Bliss, S.A.; Sinha, G.; Sandiford, O.A.; Williams, L.M.; Engelberth, D.J.; Guiro, K.; Isenalumhe, L.L.; Greco, S.J.; Ayer, S.; Bryan, M.; et al. Mesenchymal stem cell–derived exosomes stimulate cycling quiescence and early breast cancer dormancy in bone marrow. Cancer Res. 2016, 76, 5832–5844. [Google Scholar] [CrossRef]
- Puré, E.; Blomberg, R. Pro-tumorigenic roles of fibroblast activation protein in cancer: Back to the basics. Oncogene 2018, 37, 4343–4357. [Google Scholar] [CrossRef]
- Costa, A.; Kieffer, Y.; Scholer-Dahirel, A.; Pelon, F.; Bourachot, B.; Cardon, M.; Sirven, P.; Magagna, I.; Fuhrmann, L.; Bernard, C.; et al. Fibroblast Heterogeneity and Immunosup-pressive Environment in Human Breast Cancer. Cancer Cell 2018, 33, 463–479.e10. [Google Scholar] [CrossRef]
- Shiga, K.; Hara, M.; Nagasaki, T.; Sato, T.; Takahashi, H.; Takeyama, H. Cancer-Associated Fibroblasts: Their Characteristics and Their Roles in Tumor Growth. Cancers 2015, 7, 2443–2458. [Google Scholar] [CrossRef] [PubMed]
- Heneberg, P. Paracrine tumor signaling induces transdifferentiation of surrounding fibroblasts. Crit. Rev. Oncol. 2016, 97, 303–311. [Google Scholar] [CrossRef]
- Räsänen, K.; Vaheri, A. Activation of fibroblasts in cancer stroma. Exp. Cell Res. 2010, 316, 2713–2722. [Google Scholar] [CrossRef]
- Gaggioli, C.; Hooper, S.; Hidalgo-Carcedo, C.; Grosse, R.; Marshall, J.F.; Harrington, K.; Sahai, E. Fibroblast-led collective invasion of carcinoma cells with differing roles for RhoGTPases in leading and following cells. Nat. Cell Biol. 2007, 9, 1392–1400. [Google Scholar] [CrossRef] [PubMed]
- Eck, S.M.; Cote, A.L.; Winkelman, W.D.; Brinckerhoff, C.E. CXCR4 and matrix metalloproteinase-1 are elevated in breast carcino-ma-associated fibroblasts and in normal mammary fibroblasts exposed to factors secreted by breast cancer cells. Mol. Cancer Res. 2009, 7, 1033–1044. [Google Scholar] [CrossRef] [PubMed]
- Murphy, G.; Nagase, H. Progress in matrix metalloproteinase research. Mol. Asp. Med. 2008, 29, 290–308. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Avila, G.; Sommer, B.; Mendoza-Posada, D.A.; Ramos, C.; Garcia-Hernandez, A.A.; Falfan-Valencia, R. Matrix metallo-proteinases participation in the metastatic process and their diagnostic and therapeutic applications in cancer. Crit. Rev. Oncol. Hematol. 2019, 137, 57–83. [Google Scholar] [CrossRef]
- Erdogan, B.; Ao, M.; White, L.M.; Means, A.L.; Brewer, B.M.; Yang, L.; Washington, M.K.; Shi, C.; Franco, O.E.; Weaver, A.M.; et al. Cancer-associated fibroblasts promote directional cancer cell migration by aligning fibronectin. J. Cell Biol. 2017, 216, 3799–3816. [Google Scholar] [CrossRef] [PubMed]
- Bonneau, C.; Eliès, A.; Kieffer, Y.; Bourachot, B.; Ladoire, S.; Pelon, F.; Hequet, D.; Guinebretière, J.-M.; Blanchet, C.; Vincent-Salomon, A.; et al. A subset of activated fibroblasts is associated with distant relapse in early luminal breast cancer. Breast Cancer Res. 2020, 22, 1–22. [Google Scholar] [CrossRef]
- Rankin, E.B.; Giaccia, A.J. Hypoxic control of metastasis. Science 2016, 352, 175–180. [Google Scholar] [CrossRef]
- Smolarczyk, R.; Czapla, J.; Jarosz-Biej, M.; Czerwinski, K.; Cichoń, T. Vascular disrupting agents in cancer therapy. Eur. J. Pharmacol. 2021, 891, 173692. [Google Scholar] [CrossRef]
- Albrecht, I.; Christofori, G. Molecular mechanisms of lymphangiogenesis in development and cancer. Int. J. Dev. Biol. 2011, 55, 483–494. [Google Scholar] [CrossRef]
- Lee, E.; Fertig, E.J.; Jin, K.; Sukumar, S.; Pandey, N.B.; Popel, A.S. Breast cancer cells condition lymphatic endothelial cells within pre-metastatic niches to promote metastasis. Nat. Commun. 2014, 5, 1–16. [Google Scholar] [CrossRef]
- Wang, W.-C.; Zhang, X.-F.; Peng, J.; Li, X.-F.; Wang, A.-L.; Bie, Y.-Q.; Shi, L.-H.; Lin, M.-B. Survival Mechanisms and Influence Factors of Circulating Tumor Cells. BioMed Res. Int. 2018, 2018, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Camerer, E.; Qazi, A.A.; Duong, D.N.; Cornelissen, I.; Advincula, R.; Coughlin, S.R. Platelets, protease-activated receptors, and fi-brinogen in hematogenous metastasis. Blood 2004, 104, 397–401. [Google Scholar] [CrossRef] [PubMed]
- Gay, L.J.; Felding-Habermann, B. Contribution of platelets to tumour metastasis. Nat. Rev. Cancer 2011, 11, 123–134. [Google Scholar] [CrossRef]
- Mutoh, T.; Rivera, R.; Chun, J. Insights into the pharmacological relevance of lysophospholipid receptors. Br. J. Pharmacol. 2012, 165, 829–844. [Google Scholar] [CrossRef] [PubMed]
- Tseng, J.Y.; Yang, C.Y.; Liang, S.C.; Liu, R.S.; Yang, S.H.; Lin, J.K.; Chen, Y.M.; Wu, Y.C.; Jiang, J.K.; Lin, C.H. Interleukin-17A modulates circulating tumor cells in tumor draining vein of colorectal cancers and affects metastases. Clin. Cancer Res. 2014, 20, 2885–2897. [Google Scholar] [CrossRef] [PubMed]
- Leblanc, R.; Houssin, A.; Peyruchaud, O. Platelets, autotaxin and lysophosphatidic acid signalling: Win-win factors for cancer metastasis. Br. J. Pharmacol. 2018, 175, 3100–3110. [Google Scholar] [CrossRef] [PubMed]
- Frantz, C.; Stewart, K.M.; Weaver, V.M. The extracellular matrix at a glance. J. Cell Sci. 2010, 123 Pt 24, 4195–4200. [Google Scholar] [CrossRef]
- Khawar, I.A.; Kim, J.H.; Kuh, H.-J. Improving drug delivery to solid tumors: Priming the tumor microenvironment. J. Control. Release 2015, 201, 78–89. [Google Scholar] [CrossRef]
- Egeblad, M.; Rasch, M.G.; Weaver, V.M. Dynamic interplay between the collagen scaffold and tumor evolution. Curr. Opin. Cell Biol. 2010, 22, 697–706. [Google Scholar] [CrossRef] [PubMed]
- Levental, K.R.; Yu, H.; Kass, L.; Lakins, J.N.; Egeblad, M.; Erler, J.T.; Fong, S.F.; Csiszar, K.; Giaccia, A.; Weninger, W.; et al. Matrix Crosslinking Forces Tumor Progression by Enhancing Integrin Signaling. Cell 2009, 139, 891–906. [Google Scholar] [CrossRef] [PubMed]
- Byrne, C.; Schairer, C.; Wolfe, J.; Parekh, N.; Salane, M.; Brinton, L.A.; Hoover, R.; Haile, R. Mammographic Features and Breast Cancer Risk: Effects with Time, Age, and Menopause Status. J. Natl. Cancer Inst. 1995, 87, 1622–1629. [Google Scholar] [CrossRef] [PubMed]
- Boyd, N.F.; Guo, H.; Martin, L.J.; Sun, L.; Stone, J.; Fishell, E.; Jong, R.A.; Hislop, G.; Chiarelli, A.; Minkin, S.; et al. Mammographic Density and the Risk and Detection of Breast Cancer. N. Engl. J. Med. 2007, 356, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Kalli, M.; Stylianopoulos, T. Defining the Role of Solid Stress and Matrix Stiffness in Cancer Cell Proliferation and Metastasis. Front. Oncol. 2018, 8, 55. [Google Scholar] [CrossRef] [PubMed]
- Cheng, G.; Tse, J.; Jain, R.K.; Munn, L.L. Micro-Environmental Mechanical Stress Controls Tumor Spheroid Size and Morphology by Suppressing Proliferation and Inducing Apoptosis in Cancer Cells. PLoS ONE 2009, 4, e4632. [Google Scholar] [CrossRef]
- Butcher, D.T.; Alliston, T.; Weaver, V.M. A tense situation: Forcing tumour progression. Nat. Rev. Cancer 2009, 9, 108–122. [Google Scholar] [CrossRef] [PubMed]
- Northey, J.J.; Przybyla, L.; Weaver, V.M. Tissue Force Programs Cell Fate and Tumor Aggression. Cancer Discov. 2017, 7, 1224–1237. [Google Scholar] [CrossRef]
- Samuel, M.S.; Lopez, J.I.; McGhee, E.J.; Croft, D.R.; Strachan, D.; Timpson, P.; Munro, J.; Schröder, E.; Zhou, J.; Brunton, V.G.; et al. Actomyosin-mediated cellular tension drives increased tissue stiffness and beta-catenin activation to induce epidermal hyperplasia and tumor growth. Cancer Cell 2011, 19, 776–791. [Google Scholar] [CrossRef]
- Lawson, C.D.; Burridge, K. The on-off relationship of Rho and Rac during integrin-mediated adhesion and cell migration. Small GTPases 2014, 5, e27958. [Google Scholar] [CrossRef]
- Polacheck, W.J.; Zervantonakis, I.K.; Kamm, R.D. Tumor cell migration in complex microenvironments. Cell. Mol. Life Sci. 2012, 70, 1335–1356. [Google Scholar] [CrossRef]
- Katsumi, A.; Orr, A.W.; Tzima, E.; Schwartz, M.A. Integrins in Mechanotransduction. J. Biol. Chem. 2004, 279, 12001–12004. [Google Scholar] [CrossRef]
- Shi, Q.; Boettiger, D. A Novel Mode for Integrin-mediated Signaling: Tethering Is Required for Phosphorylation of FAK Y397. Mol. Biol. Cell 2003, 14, 4306–4315. [Google Scholar] [CrossRef] [PubMed]
- Kalli, M.; Papageorgis, P.; Gkretsi, V.; Stylianopoulos, T. Solid Stress Facilitates Fibroblasts Activation to Promote Pancreatic Cancer Cell Migration. Ann. Biomed. Eng. 2018, 46, 657–669. [Google Scholar] [CrossRef]
- Kalli, M.; Minia, A.; Pliaka, V.; Fotis, C.; Alexopoulos, L.G.; Stylianopoulos, T. Solid stress-induced migration is mediated by GDF15 through Akt pathway activation in pancreatic cancer cells. Sci. Rep. 2019, 9, 1–12. [Google Scholar] [CrossRef]
- Kalli, M.; Voutouri, C.; Minia, A.; Pliaka, V.; Fotis, C.; Alexopoulos, L.G.; Stylianopoulos, T. Mechanical Compression Regulates Brain Cancer Cell Migration Through MEK1/Erk1 Pathway Activation and GDF15 Expression. Front. Oncol. 2019, 9, 992. [Google Scholar] [CrossRef]
- Naba, A.; Clauser, K.R.; Lamar, J.M.; Carr, S.A.; Hynes, R.O. Extracellular matrix signatures of human mammary carcinoma identify novel metastasis promoters. eLife 2014, 3, e01308. [Google Scholar] [CrossRef]
- Laklai, H.; Miroshnikova, Y.A.; Pickup, M.W.; Collisson, E.A.; Kim, G.E.; Barrett, A.S.; Hill, R.C.; Lakins, J.N.; Schlaepfer, D.D.; Mouw, J.K.; et al. Genotype tunes pancreatic ductal adeno-carcinoma tissue tension to induce matricellular fibrosis and tumor progression. Nat. Med. 2016, 22, 497–505. [Google Scholar] [CrossRef]
- Jiang, H.; Hegde, S.; Knolhoff, B.L.; Zhu, Y.; Herndon, J.M.; Meyer, M.A.; Nywening, T.M.; Hawkins, T.M.N.W.G.; Shapiro, I.M.; Weaver, D.T.; et al. Targeting focal adhesion kinase renders pancreatic cancers responsive to checkpoint immunotherapy. Nat. Med. 2016, 22, 851–860. [Google Scholar] [CrossRef] [PubMed]
- Stylianopoulos, T.; Martin, J.D.; Snuderl, M.; Mpekris, F.; Jain, S.R.; Jain, R.K. Coevolution of Solid Stress and Interstitial Fluid Pressure in Tumors during Progression: Implications for Vascular Collapse. Cancer Res. 2013, 73, 3833–3841. [Google Scholar] [CrossRef] [PubMed]
- Lu, X.; Kang, Y. Hypoxia and Hypoxia-Inducible Factors: Master Regulators of Metastasis. Clin. Cancer Res. 2010, 16, 5928–5935. [Google Scholar] [CrossRef] [PubMed]
- Tsai, Y.-P.; Wu, K.-J. Hypoxia-regulated target genes implicated in tumor metastasis. J. Biomed. Sci. 2012, 19, 102. [Google Scholar] [CrossRef] [PubMed]
- Stubbs, M.; McSheehy, P.M.J.; Griffiths, J.R.; Bashford, C.L. Causes and consequences of tumour acidity and implications for treat-ment. Mol. Med. Today 2000, 6, 15–19. [Google Scholar] [CrossRef]
- Yang, S.; Gao, H. Nanoparticles for modulating tumor microenvironment to improve drug delivery and tumor therapy. Pharmacol. Res. 2017, 126, 97–108. [Google Scholar] [CrossRef]
- Romero-Garcia, S.; Lopez-Gonzalez, J.S.; B´ez-Viveros, J.L.; Aguilar-Cazares, D.; Prado-Garcia, H. Tumor cell metabolism: An integral view. Cancer Biol. Ther. 2011, 12, 939–948. [Google Scholar] [CrossRef] [PubMed]
- Schito, L.; Semenza, G.L. Hypoxia-inducible factors: Master regulators of cancer progression. Trends Cancer 2016, 2, 758–770. [Google Scholar] [CrossRef]
- Dhani, N.; Fyles, A.; Hedley, D.; Milosevic, M. The Clinical Significance of Hypoxia in Human Cancers. Semin. Nucl. Med. 2015, 45, 110–121. [Google Scholar] [CrossRef]
- Sullivan, R.; Graham, C.H. Hypoxia-driven selection of the metastatic phenotype. Cancer Metastasis Rev. 2007, 26, 319–331. [Google Scholar] [CrossRef]
- Vaupel, P.; Mayer, A. Hypoxia in cancer: Significance and impact on clinical outcome. Cancer Metastasis Rev. 2007, 26, 225–239. [Google Scholar] [CrossRef]
- Preet, A.; Qamri, Z.; Nasser, M.W.; Prasad, A.; Shilo, K.; Zou, X.; Groopman, J.E.; Ganju, R.K. Cannabinoid Receptors, CB1 and CB2, as Novel Targets for Inhibition of Non–Small Cell Lung Cancer Growth and Metastasis. Cancer Prev. Res. 2011, 4, 65–75. [Google Scholar] [CrossRef]
- Ravi, J.; Elbaz, M.; Wani, N.A.; Nasser, M.W.; Ganju, R.K. Cannabinoid receptor-2 agonist inhibits macrophage induced EMT in non-small cell lung cancer by downregulation of EGFR pathway. Mol. Carcinog. 2016, 55, 2063–2076. [Google Scholar] [CrossRef]
- Pixley, F.J.; Stanley, E.R. CSF-1 regulation of the wandering macrophage: Complexity in action. Trends Cell Biol. 2004, 14, 628–638. [Google Scholar] [CrossRef] [PubMed]
- Mantovani, A.; Sozzani, S.; Locati, M.; Allavena, P.; Sica, A. Macrophage polarization: Tumor-associated macrophages as a para-digm for polarized M2 mononuclear phagocytes. Trends Immunol. 2002, 23, 549–555. [Google Scholar] [CrossRef]
- Ries, C.H.; Hoves, S.; Cannarile, M.A.; Rüttinger, D. CSF-1/CSF-1R targeting agents in clinical development for cancer therapy. Curr. Opin. Pharmacol. 2015, 23, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Green, J.R.; Clezardin, P. Mechanisms of bisphosphonate effects on osteoclasts, tumor cell growth, and metastasis. Am. J. Clin. Oncol. 2002, 25 (Suppl. 1), S3–S9. [Google Scholar] [CrossRef] [PubMed]
- Green, J.R. Bisphosphonates: Preclinical review. Oncologist 2004, 9 (Suppl. 4), 3–13. [Google Scholar] [CrossRef] [PubMed]
- Zeisberger, S.M.; Odermatt, B.; Marty, C.; Zehnder-Fjallman, A.H.; Ballmer-Hofer, K.; Schwendener, R.A. Clodro-nate-liposome-mediated depletion of tumour-associated macrophages: A new and highly effective antiangiogenic therapy approach. Br. J. Cancer 2006, 95, 272–281. [Google Scholar] [CrossRef]
- Hiraoka, K.; Zenmyo, M.; Watari, K.; Iguchi, H.; Fotovati, A.; Kimura, Y.N.; Hosoi, F.; Shoda, T.; Nagata, K.; Osada, H.; et al. Inhibition of bone and muscle metastases of lung cancer cells by a decrease in the number of monocytes/macrophages. Cancer Sci. 2008, 99, 1595–1602. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Gao, L.; Cai, Y.; Liu, H.; Gao, D.; Lai, J.; Jia, B.; Wang, F.; Liu, Z. Inhibition of tumor growth and metastasis by photoimmunotherapy targeting tumor-associated macrophage in a sorafenib-resistant tumor model. Biomaterials 2016, 84, 1–12. [Google Scholar] [CrossRef]
- Timaner, M.; Bril, R.; Kaidar-Person, O.; Rachman-Tzemah, C.; Alishekevitz, D.; Kotsofruk, R.; Miller, V.; Nevelsky, A.; Daniel, S.; Raviv, Z.; et al. Dequalinium blocks mac-rophage-induced metastasis following local radiation. Oncotarget 2015, 6, 27537–27554. [Google Scholar] [CrossRef]
- Deryugina, E.I.; Zajac, E.; Juncker-Jensen, A.; Kupriyanova, T.A.; Welter, L.; Quigley, J.P. Tissue-Infiltrating Neutrophils Constitute the Major In Vivo Source of Angiogenesis-Inducing MMP-9 in the Tumor Microenvironment. Neoplasia 2014, 16, 771–788. [Google Scholar] [CrossRef]
- Deryugina, E.I.; Quigley, J.P. Pleiotropic roles of matrix metalloproteinases in tumor angiogenesis: Contrasting, overlapping and compensatory functions. Biochim. Biophys. Acta 2010, 1803, 103–120. [Google Scholar] [CrossRef] [PubMed]
- Li, X.-Y.; Lin, Y.-C.; Huang, W.-L.; Hong, C.-Q.; Chen, J.-Y.; You, Y.-J.; Li, W.-B. Zoledronic acid inhibits proliferation and impairs migration and invasion through downregulating VEGF and MMPs expression in human nasopharyngeal carcinoma cells. Med. Oncol. 2011, 29, 714–720. [Google Scholar] [CrossRef]
- Dedes, P.; Kanakis, I.; Gialeli, C.; Theocharis, A.; Tsegenidis, T.; Kletsas, D.; Tzanakakis, G.; Karamanos, N. Preclinical evaluation of zoledronate using an in vitro mimetic cellular model for breast cancer metastatic bone disease. Biochim. Biophys. Acta (BBA) Gen. Subj. 2013, 1830, 3625–3634. [Google Scholar] [CrossRef]
- Coleman, R.; Cook, R.; Hirsh, V.; Major, P.; Lipton, A. Zoledronic acid use in cancer patients: More than just supportive care? Cancer 2011, 117, 11–23. [Google Scholar] [CrossRef] [PubMed]
- Sun, T.; Yang, Y.; Luo, X.; Cheng, Y.; Zhang, M.; Wang, K.; Ge, C. Inhibition of tumor angiogenesis by interferon-gamma by suppression of tumor-associated macrophage differentiation. Oncol. Res. 2014, 21, 227–235. [Google Scholar] [CrossRef] [PubMed]
- Choi, H.-J.; Chung, T.-W.; Ha, K.-T. Luteolin inhibits recruitment of monocytes and migration of Lewis lung carcinoma cells by suppressing chemokine (C–C motif) ligand 2 expression in tumor-associated macrophage. Biochem. Biophys. Res. Commun. 2016, 470, 101–106. [Google Scholar] [CrossRef]
- Guo, Z.; Xing, Z.; Cheng, X.; Fang, Z.; Jiang, C.; Su, J.; Zhou, Z.; Xu, Z.; Holmberg, A.; Nilsson, S.; et al. Somatostatin Derivate (smsDX) Attenuates the TAM-Stimulated Prolif-eration, Migration and Invasion of Prostate Cancer via NF-kappaB Regulation. PLoS ONE 2015, 10, e0124292. [Google Scholar]
- Babajani, A.; Soltani, P.; Jamshidi, E.; Farjoo, M.H.; Niknejad, H. Recent Advances on Drug-Loaded Mesenchymal Stem Cells with Anti-neoplastic Agents for Targeted Treatment of Cancer. Front. Bioeng. Biotechnol. 2020, 8, 748. [Google Scholar] [CrossRef] [PubMed]
- Melzer, C.; Rehn, V.; Yang, Y.; Bähre, H.; Von Der Ohe, J.; Hass, R. Taxol-Loaded MSC-Derived Exosomes Provide a Therapeutic Vehicle to Target Metastatic Breast Cancer and Other Carcinoma Cells. Cancers 2019, 11, 798. [Google Scholar] [CrossRef] [PubMed]
- Nicolay, N.H.; Rühle, A.; Perez, R.L.; Trinh, T.; Sisombath, S.; Weber, K.J.; Ho, A.D.; Debus, J.; Saffrich, R.; Huber, P.E. Mesenchymal stem cells are sensitive to bleomycin treatment. Sci. Rep. 2016, 6, 26645. [Google Scholar] [CrossRef]
- Lee, H.K.; Finniss, S.; Cazacu, S.; Bucris, E.; Ziv-Av, A.; Xiang, C.; Bobbitt, K.; Rempel, S.A.; Hasselbach, L.; Mikkelsen, T.; et al. Mesenchymal stem cells deliver synthetic microRNA mimics to glioma cells and glioma stem cells and inhibit their cell migration and self-renewal. Oncotarget 2013, 4, 346–361. [Google Scholar] [CrossRef]
- Shimbo, K.; Miyaki, S.; Ishitobi, H.; Kato, Y.; Kubo, T.; Shimose, S.; Ochi, M. Exosome-formed synthetic microRNA-143 is transferred to osteosarcoma cells and inhibits their migration. Biochem. Biophys. Res. Commun. 2014, 445, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Kauer, T.M.; Figueiredo, J.-L.; Hingtgen, S.; Shah, K. Encapsulated therapeutic stem cells implanted in the tumor resection cavity induce cell death in gliomas. Nat. Neurosci. 2011, 15, 197–204. [Google Scholar] [CrossRef]
- Uluçkan, Ö.; Eagleton, M.C.; Floyd, D.H.; Morgan, E.A.; Hirbe, A.C.; Kramer, M.; Dowland, N.; Prior, J.L.; Piwnica-Worms, D.; Jeong, S.S.; et al. APT102, a novel adpase, cooperates with aspirin to disrupt bone metastasis in mice. J. Cell. Biochem. 2008, 104, 1311–1323. [Google Scholar] [CrossRef] [PubMed]
- Leblanc, R.; Lee, S.C.; David, M.; Bordet, J.C.; Norman, D.D.; Patil, R.; Miller, D.; Sahay, D.; Ribeiro, J.; Ribeiro, P.; et al. Interaction of platelet-derived autotaxin with tumor integrin alphaVbeta3 controls metastasis of breast cancer cells to bone. Blood 2014, 124, 3141–3150. [Google Scholar] [CrossRef]
- Li, J.; Sharkey, C.C.; Wun, B.; Liesveld, J.L.; King, M.R. Genetic engineering of platelets to neutralize circulating tumor cells. J. Control. Release 2016, 228, 38–47. [Google Scholar] [CrossRef] [PubMed]
- Roy, L.D.; Sahraei, M.; Schettini, J.L.; Gruber, H.E.; Besmer, D.M.; Mukherjee, P. Systemic neutralization of IL-17A significantly reduces breast cancer associated metastasis in arthritic mice by reducing CXCL12/SDF-1 expression in the metastatic niches. BMC Cancer 2014, 14, 225. [Google Scholar] [CrossRef] [PubMed]
- Muller, A.; Homey, B.; Soto, H.; Ge, N.; Catron, D.; Buchanan, M.E.; McClanahan, T.; Murphy, E.; Yuan, W.; Wagner, S.N.; et al. Involvement of chemokine receptors in breast cancer me-tastasis. Nature 2001, 410, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Hobbs, S.K.; Monsky, W.L.; Yuan, F.; Roberts, W.G.; Griffith, L.; Torchilin, V.P.; Jain, R.K. Regulation of transport pathways in tumor vessels: Role of tumor type and microenvironment. Proc. Natl. Acad. Sci. USA 1998, 95, 4607–4612. [Google Scholar] [CrossRef]
- Stylianopoulos, T.; Jain, R.K. Design considerations for nanotherapeutics in oncology. Nanomedicine 2015, 11, 1893–1907. [Google Scholar] [CrossRef] [PubMed]
- Jain, R.K.; Martin, J.D.; Stylianopoulos, T. The Role of Mechanical Forces in Tumor Growth and Therapy. Annu. Rev. Biomed. Eng. 2014, 16, 321–346. [Google Scholar] [CrossRef]
- Huang, Y.; Goel, S.; Duda, D.G.; Fukumura, D.; Jain, R.K. Vascular normalization as an emerging strategy to enhance cancer im-munotherapy. Cancer Res. 2013, 73, 2943–2948. [Google Scholar] [CrossRef] [PubMed]
- Salgaller, M.L. Technology evaluation: Bevacizumab, Genentech/Roche. Curr. Opin. Mol. Ther. 2003, 5, 657–667. [Google Scholar] [PubMed]
- Chauhan, V.P.; Stylianopoulos, T.; Martin, J.D.; Popović, Z.; Chen, O.; Kamoun, W.S.; Bawendi, M.G.; Fukumura, D.; Jain, R.K. Normalization of tumour blood vessels improves the delivery of nanomedicines in a size-dependent manner. Nat. Nanotechnol. 2012, 7, 383–388. [Google Scholar] [CrossRef]
- Stylianopoulos, T.; Jain, R.K. Combining two strategies to improve perfusion and drug delivery in solid tumors. Proc. Natl. Acad. Sci. USA 2013, 110, 18632–18637. [Google Scholar] [CrossRef]
- Heist, R.S.; Duda, D.G.; Sahani, D.V.; Ancukiewicz, M.; Fidias, P.; Sequist, L.V.; Temel, J.S.; Shaw, A.T.; Pennell, N.A.; Neal, J.W.; et al. Improved tumor vascularization after anti-VEGF therapy with carboplatin and nab-paclitaxel associates with survival in lung cancer. Proc. Natl. Acad. Sci. USA 2015, 112, 1547–1552. [Google Scholar] [CrossRef]
- Izumi, Y.; Xu, L.; Di Tomaso, E.; Fukumura, D.; Jain, R.K. Herceptin acts as an anti-angiogenic cocktail. Nat. Cell Biol. 2002, 416, 279–280. [Google Scholar] [CrossRef]
- Rosca, E.V.; Koskimaki, J.E.; Rivera, C.G.; Pandey, N.B.; Tamiz, A.P.; Popel, A.S. Anti-angiogenic peptides for cancer therapeutics. Curr. Pharm. Biotechnol. 2011, 12, 1101–1116. [Google Scholar] [CrossRef]
- Zhang, B.; Shi, W.; Jiang, T.; Wang, L.; Mei, H.; Lu, H.; Hu, Y.; Pang, Z. Optimization of the tumor microenvironment and nanomedicine properties simultaneously to improve tumor therapy. Oncotarget 2016, 7, 62607–62618. [Google Scholar] [CrossRef]
- Jiang, W.; Huang, Y.; An, Y.; Kim, B.Y.S. Remodeling Tumor Vasculature to Enhance Delivery of Intermediate-Sized Nanoparticles. ACS Nano 2015, 9, 8689–8696. [Google Scholar] [CrossRef]
- Sakurai, Y.; Hada, T.; Yamamoto, S.; Kato, A.; Mizumura, W.; Harashima, H. Remodeling of the Extracellular Matrix by Endothelial Cell-Targeting siRNA Improves the EPR-Based Delivery of 100 nm Particles. Mol. Ther. 2016, 24, 2090–2099. [Google Scholar] [CrossRef] [PubMed]
- Smith, N.R.; Baker, D.; Farren, M.; Pommier, A.; Swann, R.; Wang, X.; Mistry, S.; McDaid, K.; Kendrew, J.; Womack, C.; et al. Tumor Stromal Architecture Can Define the Intrinsic Tumor Response to VEGF-Targeted Therapy. Clin. Cancer Res. 2013, 19, 6943–6956. [Google Scholar] [CrossRef]
- Tolaney, S.M.; Boucher, Y.; Duda, D.G.; Martin, J.D.; Seano, G.; Ancukiewicz, M.; Barry, W.T.; Goel, S.; Lahdenrata, J.; Isakoff, S.J.; et al. Role of vascular density and normalization in response to neoadjuvant bevacizumab and chemotherapy in breast cancer patients. Proc. Natl. Acad. Sci. USA 2015, 112, 14325–14330. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.; Liu, R.; Zhou, Y.; Gao, H. Size-Tunable Strategies for a Tumor Targeted Drug Delivery System. ACS Central Sci. 2020, 6, 100–116. [Google Scholar] [CrossRef]
- Stylianopoulos, T.; Martin, J.D.; Chauhan, V.P.; Jain, S.R.; Diop-Frimpong, B.; Bardeesy, N.; Smith, B.L.; Ferrone, C.R.; Hornicek, F.J.; Boucher, Y.; et al. Causes, consequences, and remedies for growth-induced solid stress in murine and human tumors. Proc. Natl. Acad. Sci. USA 2012, 109, 15101–15108. [Google Scholar] [CrossRef] [PubMed]
- Stylianopoulos, T. The Solid Mechanics of Cancer and Strategies for Improved Therapy. J. Biomech. Eng. 2017, 139. [Google Scholar] [CrossRef] [PubMed]
- Stylianopoulos, T.; Munn, L.L.; Jain, R.K. Reengineering the Tumor Vasculature: Improving Drug Delivery and Efficacy. Trends Cancer 2018, 4, 258–259. [Google Scholar] [CrossRef]
- Mpekris, F.; Panagi, M.; Voutouri, C.; Martin, J.D.; Samuel, R.; Takahashi, S.; Gotohda, N.; Suzuki, T.; Papageorgis, P.; Demetriou, P.; et al. Normalizing the Microenvironment Overcomes Vessel Compression and Resistance to Nano-immunotherapy in Breast Cancer Lung Metastasis. Adv. Sci. 2021, 8. [Google Scholar] [CrossRef]
- Chen, I.X.; Chauhan, V.P.; Posada, J.; Ng, M.R.; Wu, M.W.; Adstamongkonkul, P.; Huang, P.; Lindeman, N.; Langer, R.; Jain, R.K. Blocking CXCR4 alleviates desmoplasia, increases T-lymphocyte infiltration, and improves immunotherapy in metastatic breast cancer. Proc. Natl. Acad. Sci. USA 2019, 116, 4558–4566. [Google Scholar] [CrossRef]
- Mpekris, F.; Voutouri, C.; Baish, J.W.; Duda, D.G.; Munn, L.L.; Stylianopoulos, T.; Jain, R.K. Combining microenvironment normalization strategies to improve cancer immunotherapy. Proc. Natl. Acad. Sci. USA 2020, 117, 3728–3737. [Google Scholar] [CrossRef]
- Tsai, M.; Lu, Z.; Wientjes, M.G.; Au, J.L.-S. Paclitaxel-loaded polymeric microparticles: Quantitative relationships between in vitro drug release rate and in vivo pharmacodynamics. J. Control. Release 2013, 172, 737–744. [Google Scholar] [CrossRef] [PubMed]
- Tong, R.; Chiang, H.H.; Kohane, D.S. Photoswitchable nanoparticles for in vivo cancer chemotherapy. Proc. Natl. Acad. Sci. USA 2013, 110, 19048–19053. [Google Scholar] [CrossRef] [PubMed]
- Pietras, K.; Rubin, K.; Sjöblom, T.; Buchdunger, E.; Sjöquist, M.; Heldin, C.-H.; Ostman, A. Inhibition of PDGF receptor signaling in tumor stroma enhances antitumor effect of chemotherapy. Cancer Res. 2002, 62, 5476–5484. [Google Scholar] [PubMed]
- Mpekris, F.; Papageorgis, P.; Polydorou, C.; Voutouri, C.; Kalli, M.; Pirentis, A.P.; Stylianopoulos, T. Sonic-hedgehog pathway inhibition nor-malizes desmoplastic tumor microenvironment to improve chemo-and nanotherapy. J. Control. Release 2017, 261, 105–112. [Google Scholar] [CrossRef]
- Olive, K.P.; Jacobetz, M.A.; Davidson, C.J.; Gopinathan, A.; McIntyre, D.; Honess, D.; Madhu, B.; Goldgraben, M.A.; Caldwell, M.E.; Allard, D.; et al. Inhibition of Hedgehog Signaling Enhances Delivery of Chemotherapy in a Mouse Model of Pancreatic Cancer. Science 2009, 324, 1457–1461. [Google Scholar] [CrossRef]
- Rhim, A.D.; Oberstein, P.E.; Thomas, D.H.; Mirek, E.T.; Palermo, C.F.; Sastra, S.A.; Dekleva, E.N.; Saunders, T.; Becerra, C.P.; Tattersall, I.W.; et al. Stromal Elements Act to Restrain, Rather Than Support, Pancreatic Ductal Adenocarcinoma. Cancer Cell 2014, 25, 735–747. [Google Scholar] [CrossRef]
- Ozdemir, B.C.; Pentcheva-Hoang, T.; Carstens, J.L.; Zheng, X.; Wu, C.C.; Simpson, T.R.; Laklai, H.; Sugimoto, H.; Kahlert, C.; Novitskiy, S.V.; et al. Depletion of carcinoma-associated fi-broblasts and fibrosis induces immunosuppression and accelerates pancreas cancer with reduced survival. Cancer Cell 2014, 25, 719–734. [Google Scholar] [CrossRef]
- Chen, Y.; Kim, J.; Yang, S.; Wang, H.; Wu, C.-J.; Sugimoto, H.; LeBleu, V.S.; Kalluri, R. Type I collagen deletion in αSMA+ myofibroblasts augments immune suppression and accelerates progression of pancreatic cancer. Cancer Cell 2021, 39, 548–565.e6. [Google Scholar] [CrossRef]
- Monteran, L.; Erez, N. The Dark Side of Fibroblasts: Cancer-Associated Fibroblasts as Mediators of Immunosuppression in the Tumor Microenvironment. Front. Immunol. 2019, 10, 1835. [Google Scholar] [CrossRef]
- Tauriello, D.V.F.; Palomo-Ponce, S.; Stork, D.; Berenguer-Llergo, A.; Badia-Ramentol, J.; Iglesias, M.; Sevillano, M.; Ibiza, S.; Cañellas, A.; Hernando-Momblona, X.; et al. TGFbeta drives immune evasion in genetically reconstituted colon cancer metastasis. Nature 2018, 554, 538–543. [Google Scholar] [CrossRef] [PubMed]
- Holmgaard, R.B.; Schaer, D.A.; Li, Y.; Castaneda, S.P.; Murphy, M.Y.; Xu, X.; Inigo, I.; Dobkin, J.; Manro, J.R.; Iversen, P.W.; et al. Targeting the TGFβ pathway with galunisertib, a TGFβRI small molecule inhibitor, promotes anti-tumor immunity leading to durable, complete responses, as monotherapy and in combination with checkpoint blockade. J. Immunother. Cancer 2018, 6, 47. [Google Scholar] [CrossRef] [PubMed]
- Mariathasan, S.; Turley, S.J.; Nickles, D.; Castiglioni, A.; Yuen, K.; Wang, Y.; Kadel III, E.E.; Koeppen, H.; Astarita, J.L.; Cubas, R.; et al. TGFbeta attenuates tumour response to PD-L1 blockade by contributing to exclusion of T cells. Nature 2018, 554, 544–548. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Liao, S.; Diop-Frimpong, B.; Chen, W.; Goel, S.; Naxerova, K.; Huang, Y.; Boucher, Y.; Xu, L. TGF-beta blockade improves the distribution and efficacy of therapeutics in breast carcinoma by normalizing the tumor stroma. Proc. Natl. Acad. Sci. USA 2012, 109, 16618–16623. [Google Scholar] [CrossRef]
- De Caestecker, M.P.; Piek, E.; Roberts, A.B. Role of transforming growth factor-beta signaling in cancer. J. Nat. Cancer Inst. 2000, 92, 1388–1402. [Google Scholar] [CrossRef]
- Chauhan, V.P.; Martin, J.D.; Liu, H.; Lacorre, D.A.; Jain, S.R.; Kozin, S.V.; Stylianopoulos, T.; Mousa, A.S.; Han, X.; Adstamongkonkul, P.; et al. Angiotensin inhibition enhances drug delivery and potentiates chemotherapy by decompressing tumour blood vessels. Nat. Commun. 2013, 4, 2516. [Google Scholar] [CrossRef]
- Diop-Frimpong, B.; Chauhan, V.P.; Krane, S.; Boucher, Y.; Jain, R.K. Losartan inhibits collagen I synthesis and improves the dis-tribution and efficacy of nanotherapeutics in tumors. Proc. Natl. Acad. Sci. USA 2011, 108, 2909–2914. [Google Scholar] [CrossRef]
- Zhao, Y.; Cao, J.; Melamed, A.; Worley, M.; Gockley, A.; Jones, D.; Nia, H.T.; Zhang, Y.; Stylianopoulos, T.; Kumar, A.S.; et al. Losartan treatment enhances chemotherapy efficacy and reduces ascites in ovarian cancer models by normalizing the tumor stroma. Proc. Natl. Acad. Sci. USA 2019, 116, 2210–2219. [Google Scholar] [CrossRef]
- Li, W.; Li, S.; Chen, I.X.; Liu, Y.; Ramjiawan, R.R.; Leung, C.H.; Gerweck, L.E.; Fukumura, D.; Loeffler, J.S.; Jain, R.K.; et al. Combining losartan with radiotherapy increases tumor control and inhibits lung metastases from a HER2/neu-positive orthotopic breast cancer model. Radiat. Oncol. 2021, 16, 48. [Google Scholar] [CrossRef]
- Wilop, S.; von Hobe, S.; Crysandt, M.; Esser, A.; Osieka, R.; Jost, E. Impact of angiotensin I converting enzyme inhibitors and an-giotensin II type 1 receptor blockers on survival in patients with advanced non-small-cell lung cancer undergoing first-line platinum-based chemotherapy. J. Cancer Res. Clin. Oncol. 2009, 135, 1429–1435. [Google Scholar] [CrossRef]
- Keizman, D.; Huang, P.; Eisenberger, M.A.; Pili, R.; Kim, J.J.; Antonarakis, E.S.; Hammers, H.; Carducci, M.A. Angiotensin system inhibitors and outcome of sunitinib treatment in patients with metastatic renal cell carcinoma: A retrospective examination. Eur. J. Cancer 2011, 47, 1955–1961. [Google Scholar] [CrossRef]
- Nakai, Y.; Isayama, H.; Ijichi, H.; Sasaki, T.; Takahara, N.; Ito, Y.; Matsubara, S.; Uchino, R.; Yagioka, H.; Arizumi, T.; et al. A multicenter phase II trial of gemcitabine and candesartan combination therapy in patients with advanced pancreatic cancer: GECA2. Investig. New Drugs 2013, 31, 1294–1299. [Google Scholar] [CrossRef] [PubMed]
- Murphy, J.E.; Wo, J.Y.; Ryan, D.P.; Clark, J.W.; Jiang, W.; Yeap, B.Y.; Drapek, L.C.; Ly, L.; Baglini, C.V.; Blaszkowsky, L.S.; et al. Total neoadjuvant therapy with FOLFIRINOX in combination with losartan followed by chemoradiotherapy for locally advanced pancreatic cancer: A phase 2 clinical trial. JAMA Oncol. 2019, 5, 1020–1027. [Google Scholar] [CrossRef]
- Papageorgis, P.; Polydorou, C.; Mpekris, F.; Voutouri, C.; Agathokleous, E.; Kapnissi-Christodoulou, C.P.; Stylianopoulos, T. Tranilast-induced stress alleviation in solid tumors improves the efficacy of chemo- and nanotherapeutics in a size-independent manner. Sci. Rep. 2017, 7, 46140. [Google Scholar] [CrossRef] [PubMed]
- Panagi, M.; Voutouri, C.; Mpekris, F.; Papageorgis, P.; Martin, M.R.; Martin, J.D.; Demetriou, P.; Pierides, C.; Polydorou, C.; Stylianou, A.; et al. TGF-β inhibition combined with cytotoxic nanomedicine normalizes triple negative breast cancer microenvironment towards anti-tumor immunity. Theranostics 2020, 10, 1910–1922. [Google Scholar] [CrossRef] [PubMed]
- Martin, J.D.; Panagi, M.; Wang, C.; Khan, T.T.; Martin, M.R.; Voutouri, C.; Toh, K.; Papageorgis, P.; Mpekris, F.; Polydorou, C.; et al. Dexamethasone Increases Cisplatin-Loaded Nanocarrier Delivery and Efficacy in Metastatic Breast Cancer by Normalizing the Tumor Microenvironment. ACS Nano 2019, 13, 6396–6408. [Google Scholar] [CrossRef] [PubMed]
- Polydorou, C.; Mpekris, F.; Papageorgis, P.; Voutouri, C.; Stylianopoulos, T. Pirfenidone normalizes the tumor microenvironment to improve chemotherapy. Oncotarget 2017, 8, 24506–24517. [Google Scholar] [CrossRef]
- Incio, J.; Suboj, P.; Chin, S.M.; Vardam-Kaur, T.; Liu, H.; Hato, T.; Babykutty, S.; Chen, I.; Deshpande, V.; Jain, R.K.; et al. Metformin reduces desmoplasia in pancreatic cancer by re-programming stellate cells and tumor-associated macrophages. PLoS ONE 2015, 10, e0141392. [Google Scholar] [CrossRef]
- Kim, J.H.; Shin, B.C.; Park, W.S.; Lee, J.; Kuh, H. Antifibrotic effects of pentoxifylline improve the efficacy of gemcitabine in human pancreatic tumor xenografts. Cancer Sci. 2017, 108, 2470–2477. [Google Scholar] [CrossRef] [PubMed]
- Sherman, M.H.; Yu, R.T.; Engle, D.D.; Ding, N.; Atkins, A.R.; Tiriac, H.; Collisson, E.A.; Connor, F.; Van Dyke, T.; Kozlov, S.; et al. Vitamin D Receptor-Mediated Stromal Reprogramming Suppresses Pancreatitis and Enhances Pancreatic Cancer Therapy. Cell 2014, 159, 80–93. [Google Scholar] [CrossRef]
- Masterson, R.; Hewitson, T.D.; Kelynack, K.; Martic, M.; Parry, L.; Bathgate, R.; Darby, I.; Becker, G. Relaxin down-regulates renal fibroblast function and promotes matrix remodelling in vitro. Nephrol. Dial. Transplant. 2004, 19, 544–552. [Google Scholar] [CrossRef]
- Brown, E.; McKee, T.; diTomaso, E.; Pluen, A.; Seed, B.; Boucher, Y.; Jain, R.K. Dynamic imaging of collagen and its modulation in tumors in vivo using second-harmonic generation. Nat. Med. 2003, 9, 796–800. [Google Scholar] [CrossRef] [PubMed]
- Unemori, E.N.; Amento, E.P. Relaxin modulates synthesis and secretion of procollagenase and collagen by human dermal fi-broblasts. J. Biol. Chem. 1990, 265, 10681–10685. [Google Scholar] [CrossRef]
- Feng, S.; Agoulnik, I.U.; Bogatcheva, N.V.; Kamat, A.A.; Kwabi-Addo, B.; Li, R.; Ayala, G.; Ittmann, M.M.; Agoulnik, A.I. Relaxin Promotes Prostate Cancer Progression. Clin. Cancer Res. 2007, 13, 1695–1702. [Google Scholar] [CrossRef] [PubMed]
- Eltahir, M.; Persson, H.; Mangsbo, S. Tumor localized agonistic anti-CD40 therapy and beyond. Expert Opin. Biol. Ther. 2020, 20, 215–217. [Google Scholar] [CrossRef]
- Khong, A.; Brown, M.D.; Vivian, J.B.; Robinson, B.W.; Currie, A.J. Agonistic anti-CD40 antibody therapy is effective against post-operative cancer recurrence and metastasis in a murine tumor model. J. Immunother. 2013, 36, 365–372. [Google Scholar] [CrossRef]
- Gajewski, T.F.; Schreiber, H.; Fu, Y.-X. Innate and adaptive immune cells in the tumor microenvironment. Nat. Immunol. 2013, 14, 1014–1022. [Google Scholar] [CrossRef]
- O’Hara, M.H.; O’Reilly, E.M.; Varadhachary, G.; Wolff, R.A.; Wainberg, Z.A.; Ko, A.H.; Fisher, G.; Rahma, O.; Lyman, J.P.; Cabanski, C.R.; et al. CD40 agonistic monoclonal antibody APX005M (sotigalimab) and chemotherapy, with or without nivolumab, for the treatment of metastatic pancreatic adenocarcinoma: An open-label, multicentre, phase 1b study. Lancet Oncol. 2021, 22, 118–131. [Google Scholar] [CrossRef]
- Sato-Kaneko, F.; Yao, S.; Ahmadi, A.; Zhang, S.S.; Hosoya, T.; Kaneda, M.M.; Varner, J.A.; Pu, M.; Messer, K.S.; Guiducci, C.; et al. Combination immunotherapy with TLR agonists and checkpoint inhibitors suppresses head and neck cancer. JCI Insight 2017, 2. [Google Scholar] [CrossRef]
- Roma-Rodrigues, C.; Pombo, I.; Raposo, L.; Pedrosa, P.; Fernandes, A.R.; Baptista, P.V. Nanotheranostics Targeting the Tumor Mi-croenvironment. Front. Bioeng. Biotechnol. 2019, 7, 197. [Google Scholar] [CrossRef] [PubMed]
- Ali, A.; Kataoka, N.; Ranneh, A.-H.; Iwao, Y.; Noguchi, S.; Oka, T.; Itai, S. Enhancing the Solubility and Oral Bioavailability of Poorly Water-Soluble Drugs Using Monoolein Cubosomes. Chem. Pharm. Bull. 2017, 65, 42–48. [Google Scholar] [CrossRef] [PubMed]
- Pettersen, E.O.; Ebbesen, P.; Gieling, R.G.; Williams, K.J.; Dubois, L.; Lambin, P.; Ward, C.; Meehan, J.; Kunkler, I.H.; Langdon, S.P.; et al. Targeting tumour hypoxia to prevent cancer metastasis. From biology, biosensing and technology to drug development: The METOXIA consortium. J. Enzym. Inhib. Med. Chem. 2015, 30, 689–721. [Google Scholar] [CrossRef] [PubMed]
- Potter, C.P.S.; Harris, A.L. Diagnostic, prognostic and therapeutic implications of carbonic anhydrases in cancer. Br. J. Cancer 2003, 89, 2–7. [Google Scholar] [CrossRef]
- Neri, D.; Supuran, C.T. Interfering with pH regulation in tumours as a therapeutic strategy. Nat. Rev. Drug Discov. 2011, 10, 767–777. [Google Scholar] [CrossRef] [PubMed]
- Williams, K.J.; Gieling, R.G. Preclinical Evaluation of Ureidosulfamate Carbonic Anhydrase IX/XII Inhibitors in the Treatment of Cancers. Int. J. Mol. Sci. 2019, 20, 6080. [Google Scholar] [CrossRef]
- Ward, C.; Meehan, J.; Mullen, P.; Supuran, C.; Dixon, J.M.; Thomas, J.S.; Winum, J.-Y.; Lambin, P.; Dubois, L.; Pavathaneni, N.-K.; et al. Evaluation of carbonic anhydrase IX as a therapeutic target for inhibition of breast cancer invasion and metastasis using a series of in vitro breast cancer models. Oncotarget 2015, 6, 24856–24870. [Google Scholar] [CrossRef] [PubMed]
- Lou, Y.; McDonald, P.C.; Oloumi, A.; Chia, S.; Ostlund, C.; Ahmadi, A.; Kyle, A.; Keller, U.A.D.; Leung, S.; Huntsman, D.; et al. Targeting Tumor Hypoxia: Suppression of Breast Tumor Growth and Metastasis by Novel Carbonic Anhydrase IX Inhibitors. Cancer Res. 2011, 71, 3364–3376. [Google Scholar] [CrossRef]
- Wichert, M.; Krall, N. Targeting carbonic anhydrase IX with small organic ligands. Curr. Opin. Chem. Biol. 2015, 26, 48–54. [Google Scholar] [CrossRef]
- Aleman, J.; Skardal, A. A multi-site metastasis-on-a-chip microphysiological system for assessing metastatic preference of cancer cells. Biotechnol. Bioeng. 2019, 116, 936–944. [Google Scholar] [CrossRef]
- Wang, Y.; Wu, D.; Wu, G.; Wu, J.; Lu, S.; Lo, J.; He, Y.; Zhao, C.; Zhao, X.; Zhang, H.; et al. Metastasis-on-a-chip mimicking the progression of kidney cancer in the liver for predicting treatment efficacy. Theranostics 2020, 10, 300–311. [Google Scholar] [CrossRef]
- Walsh, N.C.; Kenney, L.L.; Jangalwe, S.; Aryee, K.-E.; Greiner, D.L.; Brehm, M.A.; Shultz, L.D. Humanized Mouse Models of Clinical Disease. Annu. Rev. Pathol. Mech. Dis. 2017, 12, 187–215. [Google Scholar] [CrossRef]
- Shi, C.; Chen, X.; Tan, D. Development of patient-derived xenograft models of prostate cancer for maintaining tumor het-erogeneity. Trans. Androl. Urol. 2019, 8, 519–528. [Google Scholar] [CrossRef]
- Morton, J.J.; Bird, G.; Refaeli, Y.; Jimeno, A. Humanized Mouse Xenograft Models: Narrowing the Tumor–Microenvironment Gap. Cancer Res. 2016, 76, 6153–6158. [Google Scholar] [CrossRef]
- Pearson, T.; Greiner, D.L.; Shultz, L.D. Creation of “humanized” mice to study human immunity. Curr. Protocols Immunol. 2008, 15, 15–21. [Google Scholar] [CrossRef]
- Lefley, D.; Howard, F.; Arshad, F.; Bradbury, S.; Brown, H.; Tulotta, C.; Eyre, R.; Alférez, D.; Wilkinson, J.M.; Holen, I.; et al. Development of clinically relevant in vivo metastasis models using human bone discs and breast cancer patient-derived xenografts. Breast Cancer Res. 2019, 21, 130. [Google Scholar] [CrossRef] [PubMed]
- Cacho-Diaz, B.; Garcia-Botello, D.R.; Wegman-Ostrosky, T.; Reyes-Soto, G.; Ortiz-Sanchez, E.; Herrera-Montalvo, L.A. Tumor mi-croenvironment differences between primary tumor and brain metastases. J. Trans. Med. 2020, 18, 1. [Google Scholar] [CrossRef] [PubMed]
- O’Connell, J.T.; Sugimoto, H.; Cooke, V.G.; Macdonald, B.A.; Mehta, A.I.; LeBleu, V.S.; Dewar, R.; Rocha, R.M.; Brentani, R.R.; Resnick, M.B.; et al. VEGF-A and Tenascin-C produced by S100A4+ stromal cells are important for metastatic colonization. Proc. Natl. Acad. Sci. USA 2011, 108, 16002–16007. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, R.N.; Riba, R.D.; Zacharoulis, S.; Bramley, A.H.; Vincent, L.; Costa, C.; Macdonald, D.D.; Jin, D.K.; Shido, K.; Kerns, S.A.; et al. VEGFR1-positive haematopoietic bone marrow progenitors initiate the pre-metastatic niche. Nature 2005, 438, 820–827. [Google Scholar] [CrossRef]
- Duda, D.G.; Duyverman, A.M.M.J.; Kohno, M.; Snuderl, M.; Steller, E.J.A.; Fukumura, D.; Jain, R.K. Malignant cells facilitate lung metastasis by bringing their own soil. Proc. Natl. Acad. Sci. USA 2010, 107, 21677–21682. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).