The Impact of Ultraviolet Radiation on the Aetiology and Development of Uveal Melanoma
Abstract
Simple Summary
Abstract
1. Introduction
2. Interactions between UVR and the Eye
2.1. Overview of Radiation Spectrums
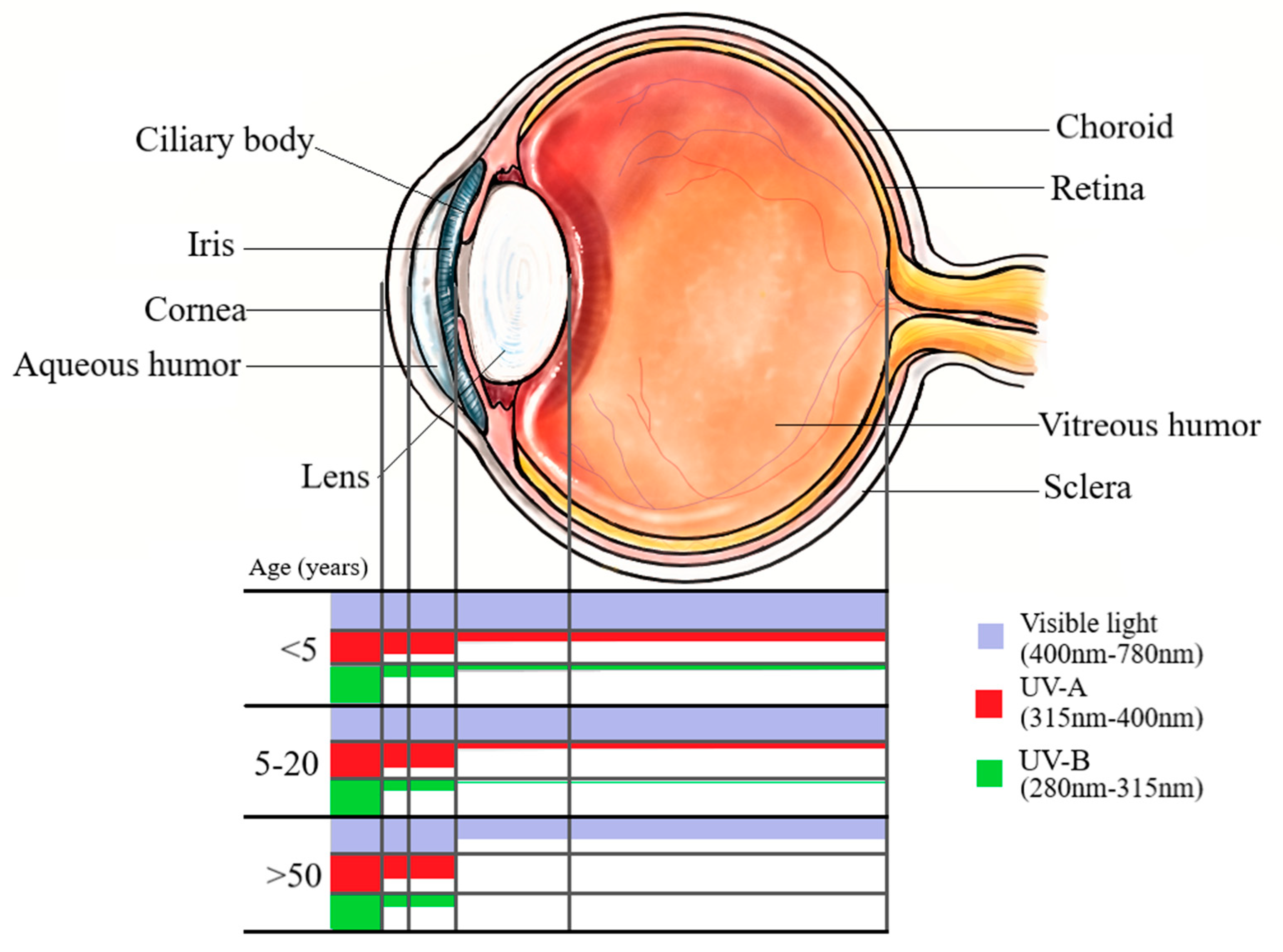
2.2. Transmission of Wavelengths through Ocular Structures
2.3. The Impact of Age on Transmission of UVR through Ocular Structures
2.4. Effect of Melanin on UVR Susceptibility in the Eye
3. Molecular Changes in UM in the Context of UVR Influence
3.1. Molecular Signatures of UVR Damage in UM
3.2. Common Genetic Mutations in UM are not Associated with UVR Exposure
4. UVR Susceptibility Relating to Environmental Factors
4.1. Differences in UVR at Different Latitudes
4.2. Changes in Global UVR Over Time
4.3. Differences in UVR Exposure between Urban and Rural Areas
5. The Relationship between UVR Exposure and UM in Australia
6. Risk Factors other than UVR Exposure that Influences UM Incidence
6.1. Wavelengths Other Than UVR That Could Cause Ocular Damage
6.2. Germline/Familial UM
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Damato, B.E.; Coupland, S.E. Ocular melanoma. Saudi J. Ophthalmol. 2012, 26, 137–144. [Google Scholar] [CrossRef] [PubMed]
- Cichorek, M.; Wachulska, M.; Stasiewicz, A.; Tymińska, A. Skin melanocytes: Biology and development. Adv. Dermatol. Allergol. 2013, 30, 30–41. [Google Scholar] [CrossRef] [PubMed]
- Van der Weyden, L.; Brenn, T.; Patton, E.E.; Wood, G.A.; Adams, D.J. Spontaneously occurring melanoma in animals and their relevance to human melanoma. J. Pathol. 2020, 252, 4–21. [Google Scholar] [CrossRef]
- White, D.; Rabago-Smith, M. Genotype–phenotype associations and human eye color. J. Hum. Genet. 2011, 56, 5–7. [Google Scholar] [CrossRef] [PubMed]
- Brenner, M.; Hearing, V.J. The protective role of melanin against UV damage in human skin. Photochem. Photobiol. 2008, 84, 539–549. [Google Scholar] [CrossRef]
- Goh, A.Y.; Ramlogan-Steel, C.A.; Jenkins, K.S.; Steel, J.C.; Layton, C.J. Presence and prevalence of UV related genetic mutations in uveal melanoma: Similarities with cutaneous melanoma. Neoplasma 2020, 67. [Google Scholar] [CrossRef]
- Johansson, P.A.; Brooks, K.; Newell, F.; Palmer, J.M.; Wilmott, J.S.; Pritchard, A.L.; Broit, N.; Wood, S.; Carlino, M.S.; Leonard, C.; et al. Whole genome landscapes of uveal melanoma show an ultraviolet radiation signature in iris tumours. Nat. Commun. 2020, 11, 2408. [Google Scholar] [CrossRef]
- Karlsson, J.; Nilsson, L.M.; Mitra, S.; Alsén, S.; Shelke, G.V.; Sah, V.R.; Forsberg, E.M.V.; Stierner, U.; All-Eriksson, C.; Einarsdottir, B.; et al. Molecular profiling of driver events in metastatic uveal melanoma. Nat. Commun. 2020, 11, 1894. [Google Scholar] [CrossRef]
- Cochran, A.J.; DE Elder, B.B. WHO Classification of Skin Tumors, 4th ed.; IARC: Lyon, France, 2018; Volume 11. [Google Scholar]
- Elder, D.E.; Bastian, B.C.; Cree, I.A.; Massi, D.; Scolyer, R.A. The 2018 World Health Organization Classification of Cutaneous, Mucosal, and Uveal Melanoma: Detailed Analysis of 9 Distinct Subtypes Defined by Their Evolutionary Pathway. Arch. Pathol. Lab. Med. 2020. [Google Scholar] [CrossRef]
- Logan, P.; Bernabeu, M.; Ferreira, A.; Burnier, M.N. Evidence for the Role of Blue Light in the Development of Uveal Melanoma. J. Ophthalmol. 2015, 2015, 386986. [Google Scholar] [CrossRef]
- Schwartz, L.H.; Ferrand, R.; Boelle, P.Y.; Maylin, C.; D’Hermies, F.; Virmont, J. Lack of Correlation between the Location of Choroidal Melanoma and Ultraviolet-Radiation Dose Distribution. Radiat. Res. 1997, 147, 451–456. [Google Scholar] [CrossRef]
- Krantz, B.A.; Dave, N.; Komatsubara, K.M.; Marr, B.P.; Carvajal, R.D. Uveal melanoma: Epidemiology, etiology, and treatment of primary disease. Clin. Ophthalmol. 2017, 11, 279–289. [Google Scholar] [CrossRef]
- McCarthy, W.H. The Australian experience in sun protection and screening for melanoma. J. Surg. Oncol 2004, 86, 236–245. [Google Scholar] [CrossRef]
- Sneyd, M.J.; Cox, B. A comparison of trends in melanoma mortality in New Zealand and Australia: The two countries with the highest melanoma incidence and mortality in the world. BMC Cancer 2013, 13, 372. [Google Scholar] [CrossRef]
- Lemus-Deschamps, L.; Makin, J.K. Fifty years of changes in UV Index and implications for skin cancer in Australia. Int. J. Biometeorol. 2012, 56, 727–735. [Google Scholar] [CrossRef]
- Lemus-Deschamps, L.; Rikus, L.; Grainger, S.; Gies, P.; Sisson, J.; Li, Z. UV Index and UV dose distributions for Australia (1997–2001). Aust. Met. Mag. 2004, 53, 239–250. [Google Scholar]
- Apalla, Z.; Lallas, A.; Sotiriou, E.; Lazaridou, E.; Ioannides, D. Epidemiological trends in skin cancer. Dermatol. Pract. Concept. 2017, 7, 1–6. [Google Scholar] [CrossRef]
- Sample, A.; He, Y.-Y. Mechanisms and prevention of UV-induced melanoma. Photodermatol. Photoimmunol. Photomed. 2018, 34, 13–24. [Google Scholar] [CrossRef]
- Jovanovic, P.; Mihajlovic, M.; Djordjevic-Jocic, J.; Vlajkovic, S.; Cekic, S.; Stefanovic, V. Ocular melanoma: An overview of the current status. Int. J. Clin. Exp. Pathol. 2013, 6, 1230–1244. [Google Scholar] [PubMed]
- Vajdic, C.M.; Kricker, A.; Giblin, M.; McKenzie, J.; Aitken, J.; Giles, G.G.; Armstrong, B.K. Incidence of ocular melanoma in Australia from 1990 to 1998. Int. J. Cancer 2003, 105, 117–122. [Google Scholar] [CrossRef] [PubMed]
- Ghazawi, F.M.; Darwich, R.; Le, M.; Rahme, E.; Zubarev, A.; Moreau, L.; Burnier, J.V.; Sasseville, D.; Burnier, M.N.; Litvinov, I.V. Uveal melanoma incidence trends in Canada: A national comprehensive population-based study. Br. J. Ophthalmol. 2019, 103, 1872. [Google Scholar] [CrossRef] [PubMed]
- Mahendraraj, K.; Lau, C.S.; Lee, I.; Chamberlain, R.S. Trends in incidence, survival, and management of uveal melanoma: A population-based study of 7,516 patients from the Surveillance, Epidemiology, and End Results database (1973-2012). Clin. Ophthalmol. 2016, 10, 2113–2119. [Google Scholar] [CrossRef] [PubMed]
- Xu, Y.; Lou, L.; Wang, Y.; Miao, Q.; Jin, K.; Chen, M.; Ye, J. Epidemiological Study of Uveal Melanoma from US Surveillance, Epidemiology, and End Results Program (2010–2015). J. Ophthalmol. 2020, 2020, 3614039. [Google Scholar] [CrossRef] [PubMed]
- Virgili, G.; Gatta, G.; Ciccolallo, L.; Capocaccia, R.; Biggeri, A.; Crocetti, E.; Lutz, J.-M.; Paci, E. Incidence of Uveal Melanoma in Europe. Ophthalmology 2007, 114, 2309–2315.e2302. [Google Scholar] [CrossRef]
- Baily, C.; O’Neill, V.; Dunne, M.; Cunningham, M.; Gullo, G.; Kennedy, S.; Walsh, P.M.; Deady, S.; Horgan, N. Uveal Melanoma in Ireland. Ocul. Oncol. Pathol. 2019, 5, 195–204. [Google Scholar] [CrossRef]
- Carvajal, R.D.; Schwartz, G.K.; Tezel, T.; Marr, B.; Francis, J.H.; Nathan, P.D. Metastatic disease from uveal melanoma: Treatment options and future prospects. Br. J. Ophthalmol. 2017, 101, 38–44. [Google Scholar] [CrossRef]
- Jin, B.; Zhang, P.; Zou, H.; Ye, H.; Wang, Y.; Zhang, J.; Yang, H.; Pan, J. Verification of EZH2 as a druggable target in metastatic uveal melanoma. Mol. Cancer 2020, 19, 52. [Google Scholar] [CrossRef]
- Kujala, E.; Makitie, T.; Kivela, T. Very long-term prognosis of patients with malignant uveal melanoma. Investig. Opthalmology Vis. Sci. 2003, 44, 4651–4659. [Google Scholar] [CrossRef]
- Holly, E.A.; Aston, D.A.; Char, D.H.; Kristiansen, J.J.; Ahn, D.K. Uveal Melanoma in Relation to Ultraviolet Light Exposure and Host Factors. Cancer Res. 1990, 50, 5773. [Google Scholar]
- Schmidt-Pokrzywniak, A.; Jöckel, K.-H.; Bornfeld, N.; Sauerwein, W.; Stang, A.J.O. Positive interaction between light iris color and ultraviolet radiation in relation to the risk of uveal melanoma: A case-control study. Ophthalmology 2009, 116, 340–348. [Google Scholar] [CrossRef]
- Guénel, P.; Laforest, L.; Cyr, D.; Févotte, J.; Sabroe, S.; Dufour, C.; Lutz, J.M.; Lynge, E. Occupational risk factors, ultraviolet radiation, and ocular melanoma: A case-control study in France. Cancer Causes Control. 2001, 12, 451–459. [Google Scholar] [CrossRef]
- Pane, A.R.; Hirst, L.W. Ultraviolet light exposure as a risk factor for ocular melanoma in Queensland, Australia. Ophthalmic Epidemiol. 2000, 7, 159–167. [Google Scholar] [CrossRef]
- Vajdic, C.M.; Kricker, A.; Giblin, M.; McKenzie, J.; Aitken, J.; Giles, G.G.; Armstrong, B.K. Eye color and cutaneous nevi predict risk of ocular melanoma in Australia. Int. J. Cancer 2001, 92, 906–912. [Google Scholar] [CrossRef]
- Houtzagers, L.E.; Wierenga, A.P.A.; Ruys, A.A.M.; Luyten, G.P.M.; Jager, M.J. Iris Colour and the Risk of Developing Uveal Melanoma. Int. J. Mol. Sci. 2020, 21, 7172. [Google Scholar] [CrossRef]
- Tucker, M.A.; Shields, J.A.; Hartge, P.; Augsburger, J.; Hoover, R.N.; Fraumeni, J.F. Sunlight Exposure as Risk Factor for Intraocular Malignant Melanoma. N. Engl. J. Med. 1985, 313, 789–792. [Google Scholar] [CrossRef]
- Vajdic, C.M.; Kricker, A.; Giblin, M.; McKenzie, J.; Aitken, J.; Giles, G.G.; Armstrong, B.K. Sun exposure predicts risk of ocular melanoma in Australia. Int. J. Cancer 2002, 101, 175–182. [Google Scholar] [CrossRef] [PubMed]
- Vajdic, C.M.; Kricker, A.; Giblin, M.; Mckenzie, J.; Aitken, J.F.; Giles, G.G.; Armstrong, B.K. Artificial ultraviolet radiation and ocular melanoma in Australia. Int. J. Cancer 2004, 112, 896–900. [Google Scholar] [CrossRef] [PubMed]
- Seddon, J.M.; Gragoudas, E.S.; Glynn, R.J.; Egan, K.M.; Albert, D.M.; Blitzer, P.H. Host Factors, UV Radiation, and Risk of Uveal Melanoma: A Case-Control Study. Arch. Ophthalmol. 1990, 108, 1274–1280. [Google Scholar] [CrossRef]
- Modenese, A.; Korpinen, L.; Gobba, F. Solar Radiation Exposure and Outdoor Work: An Underestimated Occupational Risk. Int. J. Environ. Res. Public Health 2018, 15, 2063. [Google Scholar] [CrossRef]
- Behar-Cohen, F.; Baillet, G.; de Ayguavives, T.; Garcia, P.O.; Krutmann, J.; Peña-García, P.; Reme, C.; Wolffsohn, J.S. Ultraviolet damage to the eye revisited: Eye-sun protection factor (E-SPF®), a new ultraviolet protection label for eyewear. Clin. Ophthalmol. 2014, 8, 87–104. [Google Scholar] [CrossRef] [PubMed]
- Mainster, M.A.; Turner, P.L. Ultraviolet-B Phototoxicity and Hypothetical Photomelanomagenesis: Intraocular and Crystalline Lens Photoprotection. Am. J. Ophthalmol. 2010, 149, 543–549. [Google Scholar] [CrossRef] [PubMed]
- Mallet, J.D.; Gendron, S.P.; Drigeard Desgarnier, M.-C.; Rochette, P.J. Implication of ultraviolet light in the etiology of uveal melanoma: A review. Photochem. Photobiol. 2014, 90, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Hu, D.-N.; McCormick, S.A.; Yu, G.-P. Latitude and Uveal Melanoma. Ophthalmology 2008, 115, 757. [Google Scholar] [CrossRef] [PubMed]
- Sasaki, H.; Sakamoto, Y.; Schnider, C.; Fujita, N.; Hatsusaka, N.; Sliney, D.H.; Sasaki, K. UV-B exposure to the eye depending on solar altitude. Eye Contact Lens 2011, 37, 191–195. [Google Scholar] [CrossRef] [PubMed]
- Ivanov, I.V.; Mappes, T.; Schaupp, P.; Lappe, C.; Wahl, S. Ultraviolet radiation oxidative stress affects eye health. J. Biophotonics 2018, 11, e201700377. [Google Scholar] [CrossRef] [PubMed]
- Boettner, E. Spectral Transmission of the Eye; Michigan Univ Ann Arbor: San Antonio, TA, USA, 1967. [Google Scholar]
- Boettner, E.A.; Wolter, J.R. Transmission of the Ocular Media. Invest. Ophth. Vis. Sci. 1962, 1, 776–783. [Google Scholar]
- Dillon, J.; Wang, R.H.; Atherton, S.J. Photochemical and photophysical studies on human lens constituents. Photochem. Photobiol. 1990, 52, 849–854. [Google Scholar] [CrossRef]
- Dillon, J.; Zheng, L.; Merriam, J.C.; Gaillard, E.R. The optical properties of the anterior segment of the eye: Implications for cortical cataract. Exp. Eye Res. 1999, 68, 785–795. [Google Scholar] [CrossRef]
- Kolozsvári, L.; Nógrádi, A.; Hopp, B.; Bor, Z. UV Absorbance of the Human Cornea in the 240- to 400-nm Range. Investig. Ophthalmol. Vis. Sci. 2002, 43, 2165–2168. [Google Scholar]
- Pajer, V.; Rárosi, F.; Kolozsvári, L.; Hopp, B.; Nógrádi, A. Age-Related Absorption of the Human Lens in the Near-Ultraviolet Range. Photochem. Photobiol. 2020, 96, 826–833. [Google Scholar] [CrossRef]
- Doutch, J.J.; Quantock, A.J.; Joyce, N.C.; Meek, K.M. Ultraviolet light transmission through the human corneal stroma is reduced in the periphery. Biophys. J. 2012, 102, 1258–1264. [Google Scholar] [CrossRef]
- Hammond, B.R., Jr.; Renzi-Hammond, L. Individual variation in the transmission of UVB radiation in the young adult eye. PLoS ONE 2018, 13, e0199940. [Google Scholar] [CrossRef]
- Artigas, J.M.; Felipe, A.; Navea, A.; Fandiño, A.; Artigas, C. Spectral transmission of the human crystalline lens in adult and elderly persons: Color and total transmission of visible light. Investig. Opthalmol. Vis. Sci. 2012, 53, 4076–4084. [Google Scholar] [CrossRef]
- Kaliki, S.; Shields, C.L. Uveal melanoma: Relatively rare but deadly cancer. Eye 2017, 31, 241–257. [Google Scholar] [CrossRef]
- Chew, A.L.; Spilsbury, K.; Isaacs, T.W. Survival from uveal melanoma in Western Australia 1981-2005. Clin. Exp. Ophthalmol. 2015, 43, 422–428. [Google Scholar] [CrossRef]
- Kessel, L.; Lundeman, J.H.; Herbst, K.; Andersen, T.V.; Larsen, M. Age-related changes in the transmission properties of the human lens and their relevance to circadian entrainment. J. Cataract. Refract. Surg. 2010, 36, 308–312. [Google Scholar] [CrossRef]
- Weale, R.A. Age and the transmittance of the human crystalline lens. J. Physiol. 1988, 395, 577–587. [Google Scholar] [CrossRef] [PubMed]
- Korlimbinis, A.; Aquilina, J.A.; Truscott, R.J. Protein-bound UV filters in normal human lenses: The concentration of bound UV filters equals that of free UV filters in the center of older lenses. Investig. Opthalmology Vis. Sci. 2007, 48, 1718–1723. [Google Scholar] [CrossRef] [PubMed]
- Pogrzebielski, A.; Orłowska-Heitzman, J.; Romanowska-Dixon, B. Uveal melanoma in young patients. Graefes Arch. Clin. Exp. Ophthalmol. 2006, 244, 1646–1649. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.D.; Shields, C.L.; Shields, J.A.; Sato, T. Uveal Melanoma in Young Patients. Arch. Ophthalmol. 2000, 118, 918–923. [Google Scholar]
- Shields, C.L.; Kaliki, S.; Furuta, M.; Mashayekhi, A.; Shields, J.A. Clinical spectrum and prognosis of uveal melanoma based on age at presentation in 8,033 cases. Retina 2012, 32, 1363–1372. [Google Scholar] [CrossRef]
- Young, R.W. Sunlight and age-related eye disease. J. Natl. Med. Assoc. 1992, 84, 353–358. [Google Scholar] [PubMed]
- Whiteman, D.C.; Whiteman, C.A.; Green, A.C. Childhood sun exposure as a risk factor for melanoma: A systematic review of epidemiologic studies. Cancer Causes Control. 2001, 12, 69–82. [Google Scholar] [CrossRef] [PubMed]
- Imesch, P.D.; Wallow, I.H.; Albert, D.M. The color of the human eye: A review of morphologic correlates and of some conditions that affect iridial pigmentation. Surv. Ophthalmol. 1997, 41 (Suppl. 2), S117–S123. [Google Scholar] [CrossRef]
- Wakamatsu, K.; Hu, D.N.; McCormick, S.A.; Ito, S. Characterization of melanin in human iridal and choroidal melanocytes from eyes with various colored irides. Pigment. Cell Melanoma Res. 2008, 21, 97–105. [Google Scholar] [CrossRef]
- Hu, D.-N.; Wakamatsu, K.; Ito, S.; McCormick, S.A. Comparison of eumelanin and pheomelanin content between cultured uveal melanoma cells and normal uveal melanocytes. Melanoma Res. 2009, 19, 75–79. [Google Scholar] [CrossRef] [PubMed]
- de Lange, M.J.; Razzaq, L.; Versluis, M.; Verlinde, S.; Dogrusöz, M.; Böhringer, S.; Marinkovic, M.; Luyten, G.P.; de Keizer, R.J.; de Gruijl, F.R.; et al. Distribution of GNAQ and GNA11 Mutation Signatures in Uveal Melanoma Points to a Light Dependent Mutation Mechanism. PLoS ONE 2015, 10, e0138002. [Google Scholar] [CrossRef][Green Version]
- Mar, V.J.; Wong, S.Q.; Li, J.; Scolyer, R.A.; McLean, C.; Papenfuss, A.T.; Tothill, R.W.; Kakavand, H.; Mann, G.J.; Thompson, J.F.; et al. Wild-Type Melanomas Have a High Mutation Load Correlating with Histologic and Molecular Signatures of UV Damage. Clin. Cancer Res. 2013, 19, 4589. [Google Scholar] [CrossRef]
- Furney, S.J.; Pedersen, M.; Gentien, D.; Dumont, A.G.; Rapinat, A.; Desjardins, L.; Turajlic, S.; Piperno-Neumann, S.; de la Grange, P.; Roman-Roman, S.; et al. SF3B1 mutations are associated with alternative splicing in uveal melanoma. Cancer Discov. 2013, 3, 1122–1129. [Google Scholar] [CrossRef]
- Alexandrov, L.B.; Nik-Zainal, S.; Wedge, D.C.; Aparicio, S.A.; Behjati, S.; Biankin, A.V.; Bignell, G.R.; Bolli, N.; Borg, A.; Børresen-Dale, A.L.; et al. Signatures of mutational processes in human cancer. Nature 2013, 500, 415–421. [Google Scholar] [CrossRef]
- Greenman, C.; Stephens, P.; Smith, R.; Dalgliesh, G.L.; Hunter, C.; Bignell, G.; Davies, H.; Teague, J.; Butler, A.; Stevens, C.; et al. Patterns of somatic mutation in human cancer genomes. Nature 2007, 446, 153–158. [Google Scholar] [CrossRef] [PubMed]
- Carlino, M.S.; Long, G.V.; Kefford, R.F.; Rizos, H. Targeting oncogenic BRAF and aberrant MAPK activation in the treatment of cutaneous melanoma. Crit. Rev. Oncol. 2015, 96, 385–398. [Google Scholar] [CrossRef] [PubMed]
- Thomas, N.E.; Berwick, M.; Cordeiro-Stone, M. Could BRAF mutations in melanocytic lesions arise from DNA damage induced by ultraviolet radiation? J. Investig. Dermatol. 2006, 126, 1693–1696. [Google Scholar] [CrossRef]
- Henriquez, F.; Janssen, C.; Kemp, E.G.; Roberts, F. The T1799A BRAF Mutation Is Present in Iris Melanoma. Investig. Opthalmol. Vis. Sci. 2007, 48, 4897–4900. [Google Scholar] [CrossRef] [PubMed]
- Janssen, C.S.; Sibbett, R.; Henriquez, F.L.; McKay, I.C.; Kemp, E.G.; Roberts, F. The T1799A point mutation is present in posterior uveal melanoma. Br. J. Cancer 2008, 99, 1673–1677. [Google Scholar] [CrossRef]
- Chen, X.; Wu, Q.; Tan, L.; Porter, D.; Jager, M.J.; Emery, C.; Bastian, B.C. Combined PKC and MEK inhibition in uveal melanoma with GNAQ and GNA11 mutations. Oncogene 2014, 33, 4724–4734. [Google Scholar] [CrossRef]
- Gaffal, E. Research in practice: Therapeutic targeting of oncogenic GNAQ mutations in uveal melanoma. J. Dtsch. Dermatol. Ges. 2020, 18, 1245–1248. [Google Scholar] [CrossRef]
- Moore, A.R.; Ran, L.; Guan, Y.; Sher, J.J.; Hitchman, T.D.; Zhang, J.Q.; Hwang, C.; Walzak, E.G.; Shoushtari, A.N.; Monette, S.; et al. GNA11 Q209L mouse model reveals RasGRP3 as an essential signaling node in uveal melanoma. Cell Rep. 2018, 22, 2455–2468. [Google Scholar] [CrossRef]
- Van Raamsdonk, C.D.; Griewank, K.G.; Crosby, M.B.; Garrido, M.C.; Vemula, S.; Wiesner, T.; Obenauf, A.C.; Wackernagel, W.; Green, G.; Bouvier, N.; et al. Mutations in GNA11 in uveal melanoma. N. Engl. J. Med 2010, 363, 2191–2199. [Google Scholar] [CrossRef]
- Zhang, Q.; Lin, Z.-N.; Chen, J.; Zheng, W.-X. A multi-omics study on cutaneous and uveal melanoma. Int. J. Ophthalmol. 2021, 14, 32–41. [Google Scholar] [CrossRef]
- Goh, A.Y.; Layton, C.J. Evolving systemic targeted therapy strategies in uveal melanoma and implications for ophthalmic management: A review. Clin. Exp. Ophthalmol. 2016, 44, 509–519. [Google Scholar] [CrossRef] [PubMed]
- Fallico, M.; Raciti, G.; Longo, A.; Reibaldi, M.; Bonfiglio, V.; Russo, A.; Caltabiano, R.; Gattuso, G.; Falzone, L.; Avitabile, T. Current molecular and clinical insights into uveal melanoma (Review). Int. J. Oncol. 2021, 58, 1. [Google Scholar] [CrossRef] [PubMed]
- Croce, M.; Ferrini, S.; Pfeffer, U.; Gangemi, R. Targeted Therapy of Uveal Melanoma: Recent Failures and New Perspectives. Cancers 2019, 11, 846. [Google Scholar] [CrossRef] [PubMed]
- Masclef, L.; Ahmed, O.; Estavoyer, B.; Larrivée, B.; Labrecque, N.; Nijnik, A.; Affar, E.B. Roles and mechanisms of BAP1 deubiquitinase in tumor suppression. Cell Death Differ. 2021, 28, 606–625. [Google Scholar] [CrossRef]
- O’Shea, S.J.; Robles-Espinoza, C.D.; McLellan, L.; Harrigan, J.; Jacq, X.; Hewinson, J.; Iyer, V.; Merchant, W.; Elliott, F.; Harland, M.; et al. A population-based analysis of germline BAP1 mutations in melanoma. Hum. Mol. Genet. 2017, 26, 717–728. [Google Scholar] [CrossRef]
- Hacker, E.; Irwin, N.; Muller, H.K.; Powell, M.B.; Kay, G.; Hayward, N.; Walker, G. Neonatal ultraviolet radiation exposure is critical for malignant melanoma induction in pigmented Tpras transgenic mice. J. Investig. Dermatol. 2005, 125, 1074–1077. [Google Scholar] [CrossRef]
- Klein-Szanto, A.J.P.; Silvers, W.K.; Mintz, B. Ultraviolet Radiation-induced Malignant Skin Melanoma in Melanoma-susceptible Transgenic Mice. Cancer Res. 1994, 54, 4569. [Google Scholar]
- Kuzu, O.F.; Nguyen, F.D.; Noory, M.A.; Sharma, A. Current State of Animal (Mouse) Modeling in Melanoma Research. Cancer Growth Metastasis 2015, 8, 81–94. [Google Scholar] [CrossRef]
- Huang, J.L.; Urtatiz, O.; Van Raamsdonk, C.D. Oncogenic G Protein GNAQ Induces Uveal Melanoma and Intravasation in Mice. Cancer Res. 2015, 75, 3384–3397. [Google Scholar] [CrossRef] [PubMed]
- Mouti, M.A.; Dee, C.; Coupland, S.E.; Hurlstone, A.F. Minimal contribution of ERK1/2-MAPK signalling towards the maintenance of oncogenic GNAQQ209P-driven uveal melanomas in zebrafish. Oncotarget 2016, 7, 39654–39670. [Google Scholar] [CrossRef]
- Singh, A.D.; Rennie, I.G.; Seregard, S.; Giblin, M.; McKenzie, J. Sunlight exposure and pathogenesis of uveal melanoma. Surv. Ophthalmol. 2004, 49, 419–428. [Google Scholar] [CrossRef]
- Yu, G.-P.; Hu, D.-N.; McCormick, S.A. Latitude and Incidence of Ocular Melanoma. Photochem. Photobiol. 2006, 82, 1621–1626. [Google Scholar] [CrossRef] [PubMed]
- Bais, A.F.; Lucas, R.M.; Bornman, J.F.; Williamson, C.E.; Sulzberger, B.; Austin, A.T.; Wilson, S.R.; Andrady, A.L.; Bernhard, G.; McKenzie, R.L.; et al. Environmental effects of ozone depletion, UV radiation and interactions with climate change: UNEP Environmental Effects Assessment Panel, update 2017. Photochem. Photobiol. Sci. 2018, 17, 127–179. [Google Scholar] [CrossRef] [PubMed]
- Dolin, P.J.; Foss, A.J.E.; Hungerford, J.L. Uveal melanoma: Is solar ultraviolet radiation a risk factor? Ophthalmic Epidemiol. 1994, 1, 27–30. [Google Scholar] [CrossRef] [PubMed]
- Weis, E.; Vrouwe, S.Q.; LeBaron, D.B.; Parliament, M.B.; Shields, J.; Shields, C.L. Changes in Ultraviolet Radiation Exposure to the Ocular Region: A Population-Based Study. Cancers 2019, 11, 719. [Google Scholar] [CrossRef] [PubMed]
- Ajani, U.A.; Seddon, J.M.; Hsieh, C.C.; Egan, K.M.; Albert, D.M.; Gragoudas, E.S. Occupation and risk of uveal melanoma. An exploratory study. Cancer 1992, 70, 2891–2900. [Google Scholar] [CrossRef]
- Andersen, P.A.; Buller, D.B.; Walkosz, B.J.; Scott, M.D.; Maloy, J.A.; Cutter, G.R.; Dignan, M.D. Environmental cues to UV radiation and personal sun protection in outdoor winter recreation. Arch. Dermatol. 2010, 146, 1241–1247. [Google Scholar] [CrossRef]
- Whiteman, D.C.; Bray, C.A.; Siskind, V.; Green, A.C.; Hole, D.J.; Mackie, R.M. Changes in the incidence of cutaneous melanoma in the west of Scotland and Queensland, Australia: Hope for health promotion? Eur. J. Cancer Prev. 2008, 17, 243–250. [Google Scholar] [CrossRef]
- Rahman, A.M.; Selva, D.; Davis, G. Choroidal melanoma with extrascleral extension in an Australian Aboriginal man. Clin Exp Ophthalmol. 2007, 35, 187–189. [Google Scholar] [CrossRef]
- Aoude, L.G.; Vajdic, C.M.; Kricker, A.; Armstrong, B.; Hayward, N.K. Prevalence of germline BAP1 mutation in a population-based sample of uveal melanoma cases. Pigment. Cell Melanoma Res. 2013, 26, 278–279. [Google Scholar] [CrossRef]
- Manning, W.S., Jr.; Greenlee, P.G.; Norton, J.N. Ocular melanoma in a Long Evans rat. Contemp. Top. Lab. Anim. Sci. 2004, 43, 44–46. [Google Scholar]
- Fernandes, B.F.; Marshall, J.-C.A.; Burnier, M.N., Jr. Blue Light Exposure and Uveal Melanoma. Ophthalmology 2006, 113, 1062.e1. [Google Scholar] [CrossRef] [PubMed]
- Marshall, J.-C.A.; Gordon, K.D.; McCauley, C.S.; de Souza Filho, J.P.; Burnier, M.N. The effect of blue light exposure and use of intraocular lenses on human uveal melanoma cell lines. Melanoma Res. 2006, 16, 537–541. [Google Scholar] [CrossRef] [PubMed]
- Di Cesare, S.; Maloney, S.; Fernandes, B.F.; Martins, C.; Marshall, J.-C.; Antecka, E.; Odashiro, A.N.; Dawson, W.W.; Burnier, J.M.N. The effect of blue light exposure in an ocular melanoma animal model. J. Exp. Clin. Cancer Res. 2009, 28, 48. [Google Scholar] [CrossRef]
- Zhao, Z.-C.; Zhou, Y.; Tan, G.; Li, J. Research progress about the effect and prevention of blue light on eyes. Int. J. Ophthalmol. 2018, 11, 1999–2003. [Google Scholar] [CrossRef]
- Aronow, M.E.; Topham, A.K.; Singh, A.D. Uveal Melanoma: 5-Year Update on Incidence, Treatment, and Survival (SEER 1973-2013). Ocul. Oncol. Pathol. 2018, 4, 145–151. [Google Scholar] [CrossRef]
- Broadway, D.; Lang, S.; Harper, J.; Madanat, F.; Pritchard, J.; Tarawneh, M.; Taylor, D. Congenital malignant melanoma of the eye. Cancer 1991, 67, 2642–2652. [Google Scholar] [CrossRef]
- Greer, C.H. Congenital Melanoma of the Anterior Uvea. Arch. Ophthalmol. 1966, 76, 77–78. [Google Scholar] [CrossRef]
- Palazzi, M.A.; Ober, M.D.; Abreu, H.F.; Cardinalli, I.A.; Isaac, C.R.; Odashiro, A.N.; Burnier, M.N., Jr. Congenital uveal malignant melanoma: A case report. Can. J. Ophthalmol. 2005, 40, 611–615. [Google Scholar] [CrossRef]
- Helgadottir, H.; Höiom, V. The genetics of uveal melanoma: Current insights. Appl. Clin. Genet. 2016, 9, 147–155. [Google Scholar] [CrossRef] [PubMed]
- Van Poppelen, N.M.; de Bruyn, D.P.; Bicer, T.; Verdijk, R.; Naus, N.; Mensink, H.; Paridaens, D.; de Klein, A.; Brosens, E.; Kiliҫ, E. Genetics of Ocular Melanoma: Insights into Genetics, Inheritance and Testing. Int. J. Mol. Sci. 2021, 22, 336. [Google Scholar] [CrossRef] [PubMed]
- Turunen, J.A.; Markkinen, S.; Wilska, R.; Saarinen, S.; Raivio, V.; Täll, M.; Lehesjoki, A.E.; Kivelä, T.T. BAP1 Germline Mutations in Finnish Patients with Uveal Melanoma. Ophthalmology 2016, 123, 1112–1117. [Google Scholar] [CrossRef] [PubMed]
- Gupta, M.P.; Lane, A.M.; DeAngelis, M.M.; Mayne, K.; Crabtree, M.; Gragoudas, E.S.; Kim, I.K. Clinical Characteristics of Uveal Melanoma in Patients With Germline BAP1 Mutations. JAMA Ophthalmol. 2015, 133, 881–887. [Google Scholar] [CrossRef] [PubMed]
- Njauw, C.N.; Kim, I.; Piris, A.; Gabree, M.; Taylor, M.; Lane, A.M.; DeAngelis, M.M.; Gragoudas, E.; Duncan, L.M.; Tsao, H. Germline BAP1 inactivation is preferentially associated with metastatic ocular melanoma and cutaneous-ocular melanoma families. PLoS ONE 2012, 7, e35295. [Google Scholar] [CrossRef] [PubMed]
| Risk Factor Relating to UVR Susceptibility | Risk for UM Incidence | Reference |
|---|---|---|
| Light (blonde or red) hair colour | - | [30] |
| - to + | [31] | |
| + | [32] | |
| - | [33] | |
| - | [34] | |
| Light (Green/gray/hazel/blue) eye colour | + | [30] |
| - to ++ | [31] | |
| + to ++ | [32] | |
| + to ++ | [35] | |
| - to + | [33] | |
| ++ | [34] | |
| Light skin colour | ++ | [32] |
| + to ++ | [31] | |
| - to + | [33] | |
| + to ++ | [34] | |
| Burns easily (with little to no tanning) | ++ | [30] |
| + | [32] | |
| - to + | [33] | |
| - to + | [34] | |
| ≥1 welding burn, sunburn to eye, or snow blindness | ++ | [30] |
| - | [32] | |
| ≥5 eye burns | ++ | [32] |
| Freckles | - | [30] |
| + | [36] | |
| - to + | [33] | |
| + | [34] | |
| Takes outdoor sunny vacations | - | [30] |
| ++ | [36] | |
| Leisure time spent mostly outdoors | - | [30] |
| + | [36] | |
| - to + | [37] | |
| High cumulative occupational sun exposure | ++ | [37] |
| Large nevi ≥ 1 | + | [30] |
| + to ++ | [34] | |
| High cumulative exposure to artificial UVR | ++ | [30] |
| ++ | [32] | |
| ++ | [36] | |
| + to ++ | [31] | |
| + to ++ | [38] | |
| High cumulative exposure to solar UVR | + | [32] |
| + to ++ | [37] | |
| Freckling in childhood | + to ++ | [31] |
| - to + 1 | [33] | |
| + | [34] | |
| First use of sunlamp (artificial UVR) at <20 years old | ++ | [31] |
| Personal history of CM | ++ | [33] |
| Family history of UM | ++ | [33] |
| Ancestry from more northern latitudes (Northern Hemisphere) | ++ | [39] |
| Southern residence below latitude 40° N for >5 years (Northern Hemisphere) | ++ | [39] |
| Northern residence above latitude 36° S (Southern Hemisphere) | - | [37] |
| Northern residence above latitude 30° S for most of life (Southern Hemisphere) | - to ++ 2 | [33] |
| Wearing sunglasses more than half to all the time | - | [33] |
| Wearing prescription glasses or contact lenses | - | [30] |
| - | [33] |
| Title | Year | Data set | Type of Study | Conclusions | Reference |
|---|---|---|---|---|---|
| UV light exposure as a risk factor for ocular melanoma in QLD, Australia | 1972 to 1996 | QLD cases from the QLD Cancer Registry and from pathology laboratory ocular specimens in QLD 216 choroidal 35 ciliary body 27 iris 35 conjunctival | Determining risk factors using case-control study (125 patients, 375 controls), questionnaire without disclosing study hypotheses OR and 95% CI | No correlation between estimated lifetime cumulative solar radiation exposure and ocular melanoma in QLD from 1972 to 1996 but a protective effect of dark skin, brown eyes, and resistance to sunburn. A family history of ocular melanoma was a strong risk factor. | [33] |
| Eye colour and cutaneous nevi predict risk of ocular melanoma in Australia | 1996 to 1998 | NSW, VIC, QLD and Other from “all ophthalmologists and population-based cancer registries in Australia” 222 choroid 22 ciliary body 1 ciliochoroidal 25 iris 19 conjunctival | Determining risk factors using case-control study (290 patients, 914 controls), questionnaire without disclosing study hypotheses OR and 95% CI using STATA and Mantel-Haenszel | Light eyes, cutaneous nevi and inability to tan were found to be risk factors for UM. | [34] |
| Sun exposure predicts risk of ocular melanoma in Australia | As above | Same dataset as above | Same model as above | Long hours outdoors increase risk of UM. | [37] |
| Artificial UV light radiation and ocular melanoma in Australia | As above | Same dataset as above | Same model as above, but with 290 patients and 893 controls | Risk of ciliary body and choroidal (but not iris or conjunctival) melanomas increased with exposure to sunlamps or welding independent of personal sun exposure. | [38] |
| Incidence of ocular melanoma in Australia from 1990 to 1998 | 1990 to 1998 | From Australian population-based cancer registries and all practising ophthalmologists 1990 to 1995 = 768 1996 to 1998 = 539 (choroid or ciliary body 459, iris 42, conjunctiva 37) | Determine the incidence and incidence trends of ocular melanoma based on distribution, latitude and in subpopulations. Incidence trends only used cancer registry-reported cases and excluded QLD | Incidence increased weakly across latitude bands from <30°S to >36°S. Rural residence increased incidence by 50%. | [21] |
| Survival from UM in WA 1981–2005 | 1981 to 2005 | WA Cancer Registry 229 Choroid 33 Ciliary 46 Iris or Unknown | Determining relative survival estimation and proportional hazards regression models using STATA Eerer II methodology(308 patients) | When life tables were used to account for the baseline death rates in the general population, the relative survival rates at 3, 5 and 10 years were 88% (95% CI: 83–92%), 81% (95% CI: 76–87%) and 71% (95% CI: 63–78%), respectively | [57] |
| Prevalence of germline BAP1 mutation in a population-based sample of UM cases | (Not specified) 2012 or earlier based on publication date | NSW Patients diagnosed at ≤50 years old (n = 66) | Sanger sequencing to determine BAP1 mutations | 2/66 possessed BAP1 mutations | [102] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chalada, M.; Ramlogan-Steel, C.A.; Dhungel, B.P.; Layton, C.J.; Steel, J.C. The Impact of Ultraviolet Radiation on the Aetiology and Development of Uveal Melanoma. Cancers 2021, 13, 1700. https://doi.org/10.3390/cancers13071700
Chalada M, Ramlogan-Steel CA, Dhungel BP, Layton CJ, Steel JC. The Impact of Ultraviolet Radiation on the Aetiology and Development of Uveal Melanoma. Cancers. 2021; 13(7):1700. https://doi.org/10.3390/cancers13071700
Chicago/Turabian StyleChalada, Melissa, Charmaine A. Ramlogan-Steel, Bijay P. Dhungel, Christopher J. Layton, and Jason C. Steel. 2021. "The Impact of Ultraviolet Radiation on the Aetiology and Development of Uveal Melanoma" Cancers 13, no. 7: 1700. https://doi.org/10.3390/cancers13071700
APA StyleChalada, M., Ramlogan-Steel, C. A., Dhungel, B. P., Layton, C. J., & Steel, J. C. (2021). The Impact of Ultraviolet Radiation on the Aetiology and Development of Uveal Melanoma. Cancers, 13(7), 1700. https://doi.org/10.3390/cancers13071700






