Dual Targeting with Cell Surface Electrical Charge and Folic Acid via Superparamagnetic Fe3O4@Cu2–xS for Photothermal Cancer Cell Killing
Abstract
:Simple Summary
Abstract
1. Introduction
2. Materials and Methods
2.1. General
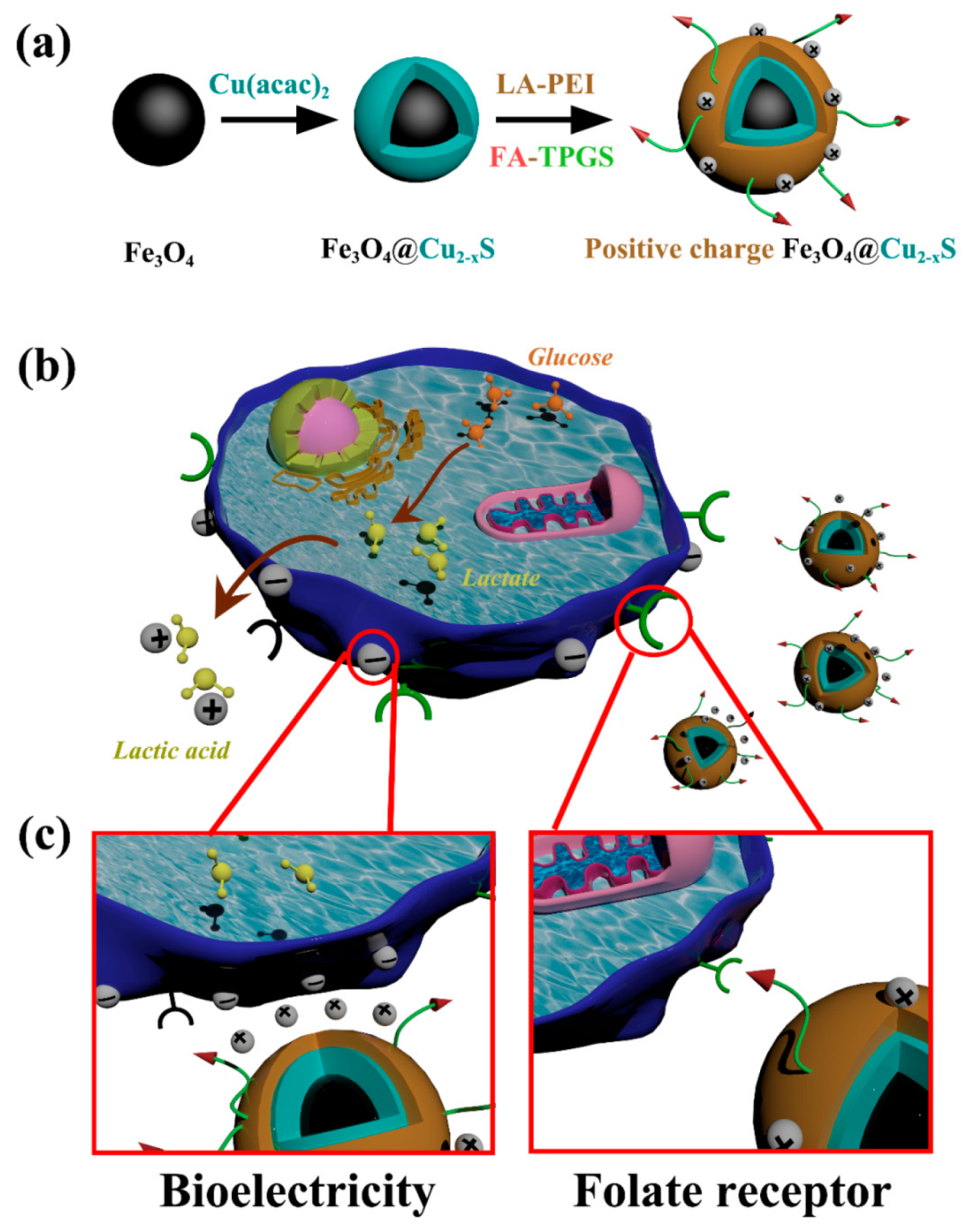
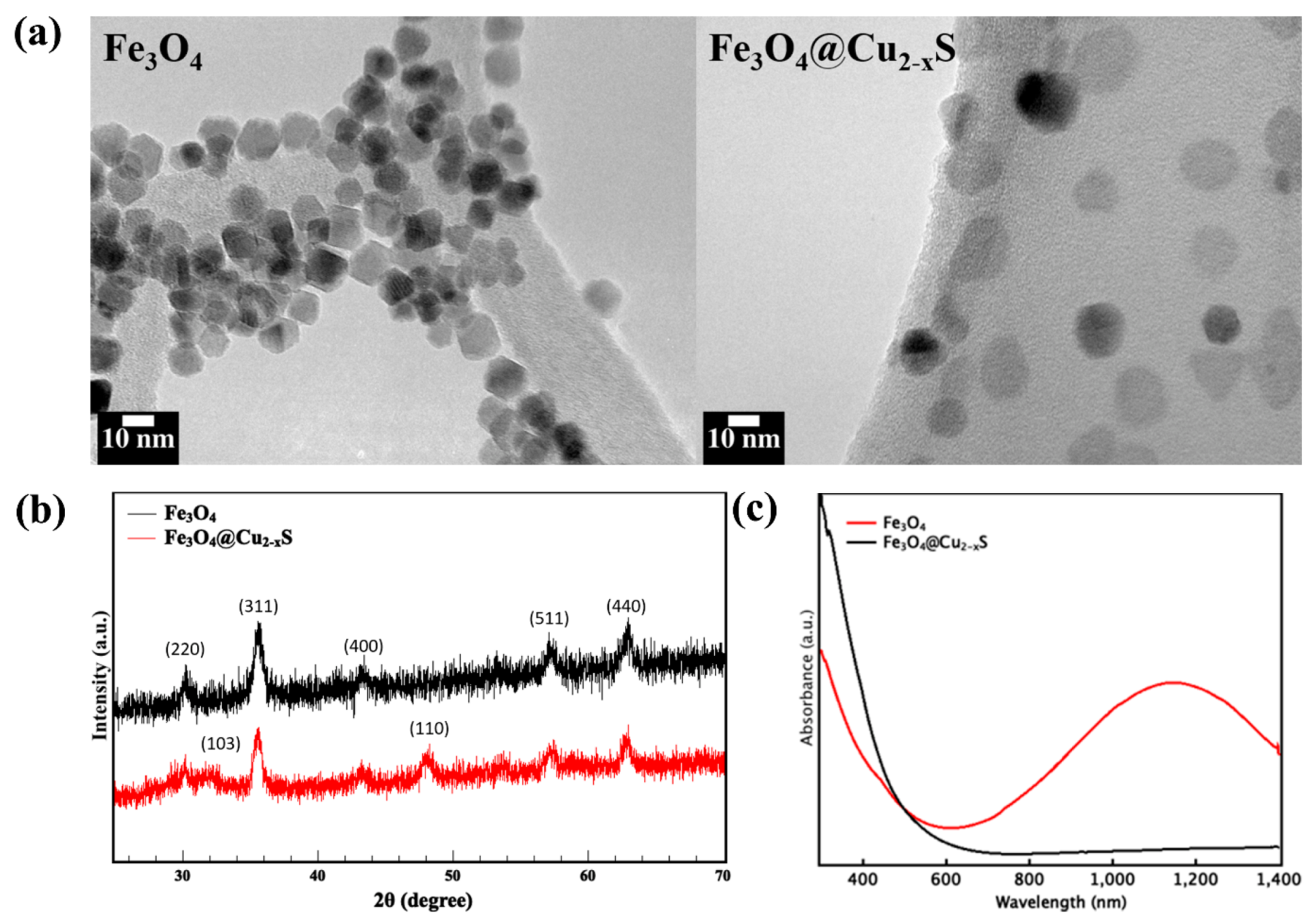
2.2. Synthesis of Fe3O4 and Fe3O4@Cu2–xS Nanoparticles
2.3. LA-PEI and Folate Modified TPGS Synthesis
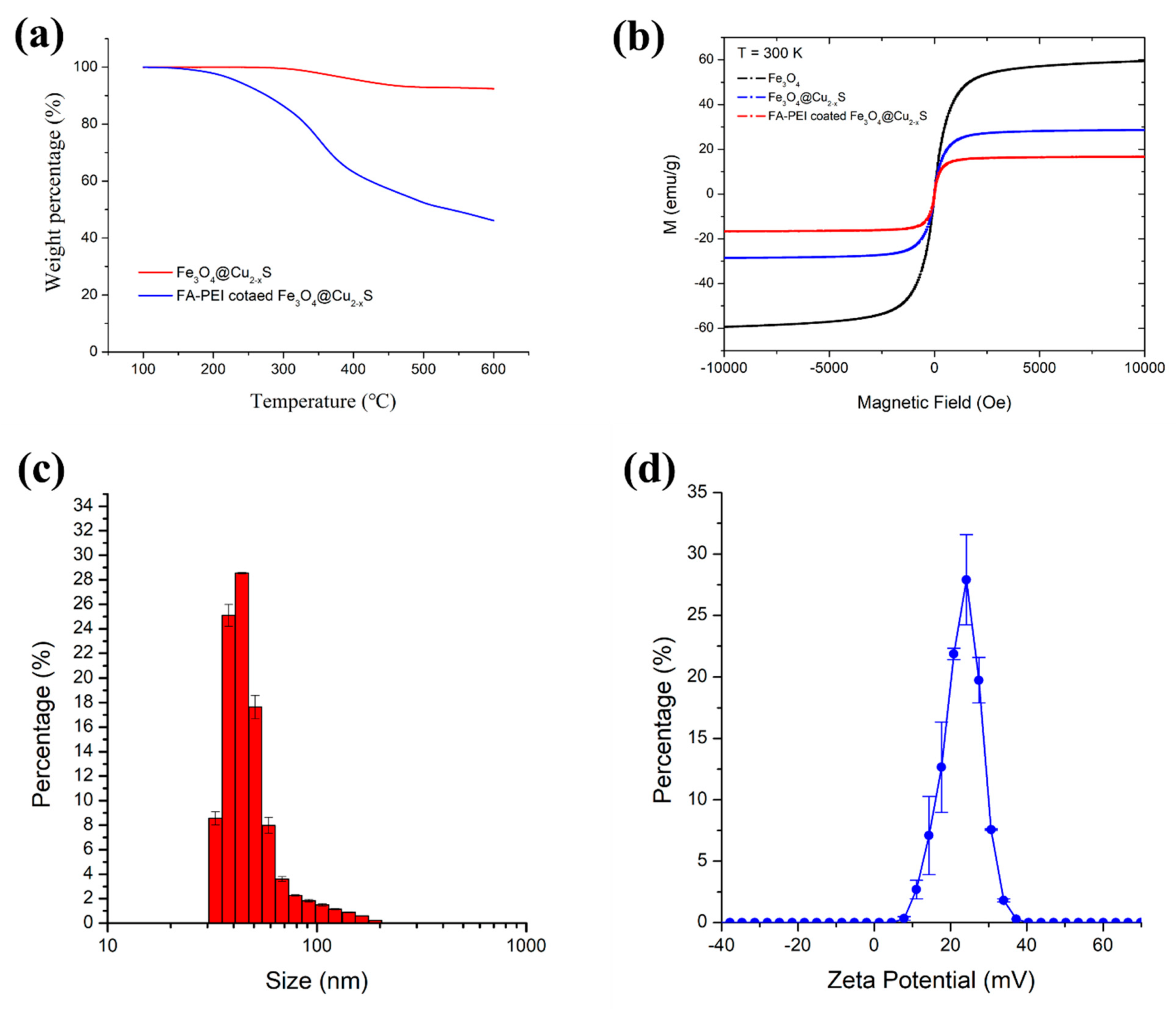
2.4. Polymer Coating of the Fe3O4 and Fe3O4@Cu2–xS Nanoparticles
2.5. Nanoparticle Characterizations
2.6. Cell Lines and Culture Conditions
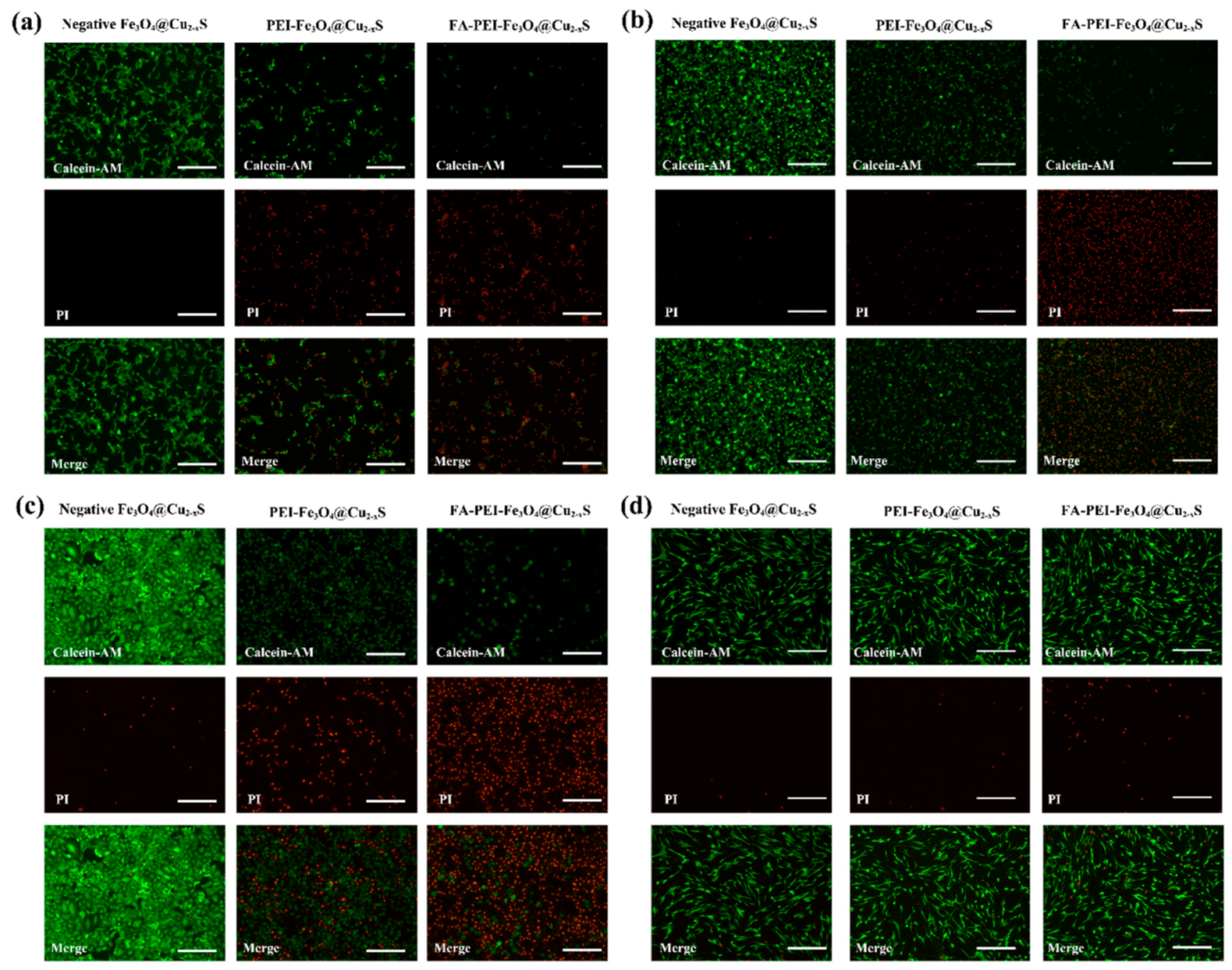
2.7. Calcein-AM/PI Assay
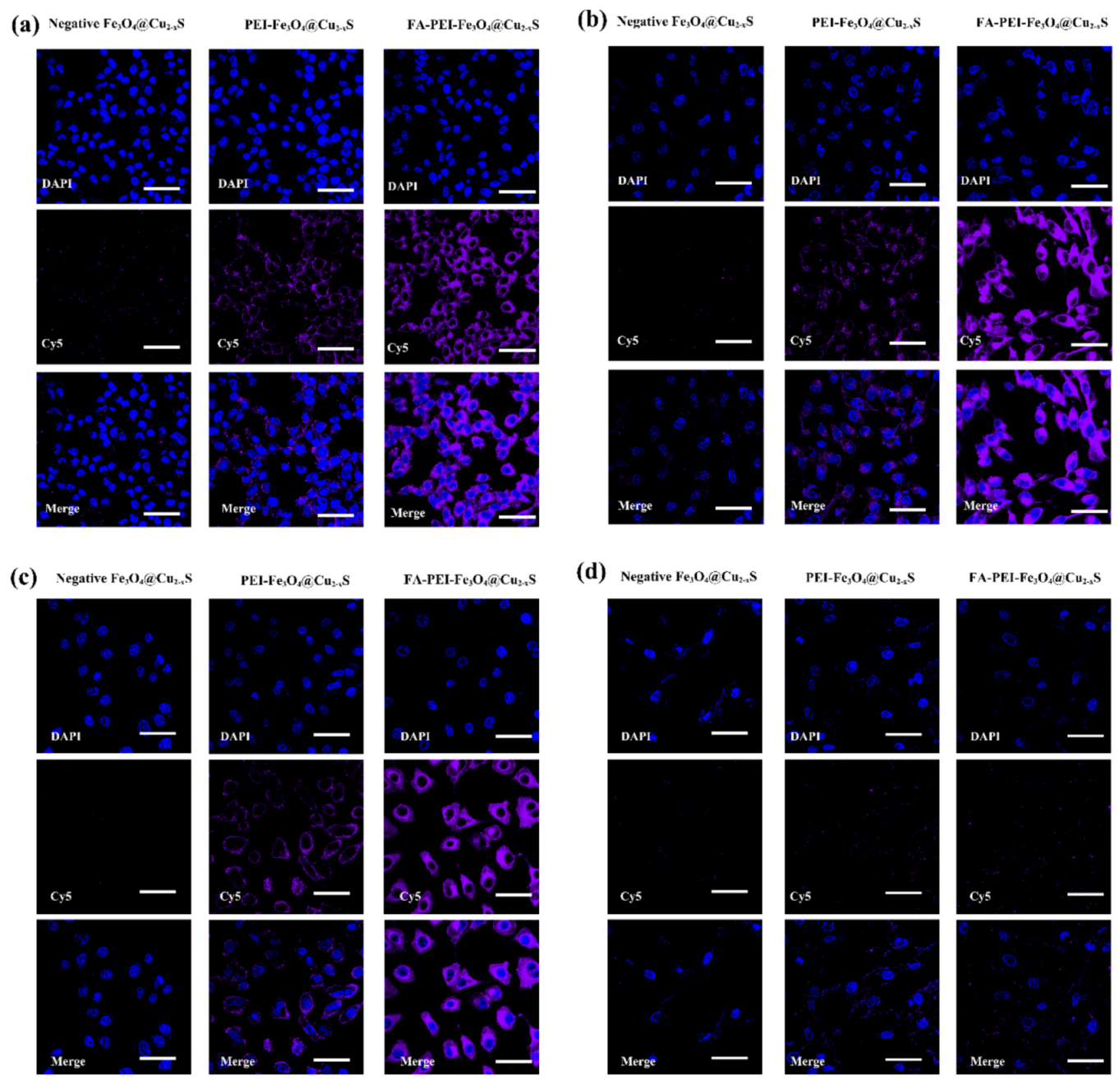
2.8. Confocal Microscopy Imaging
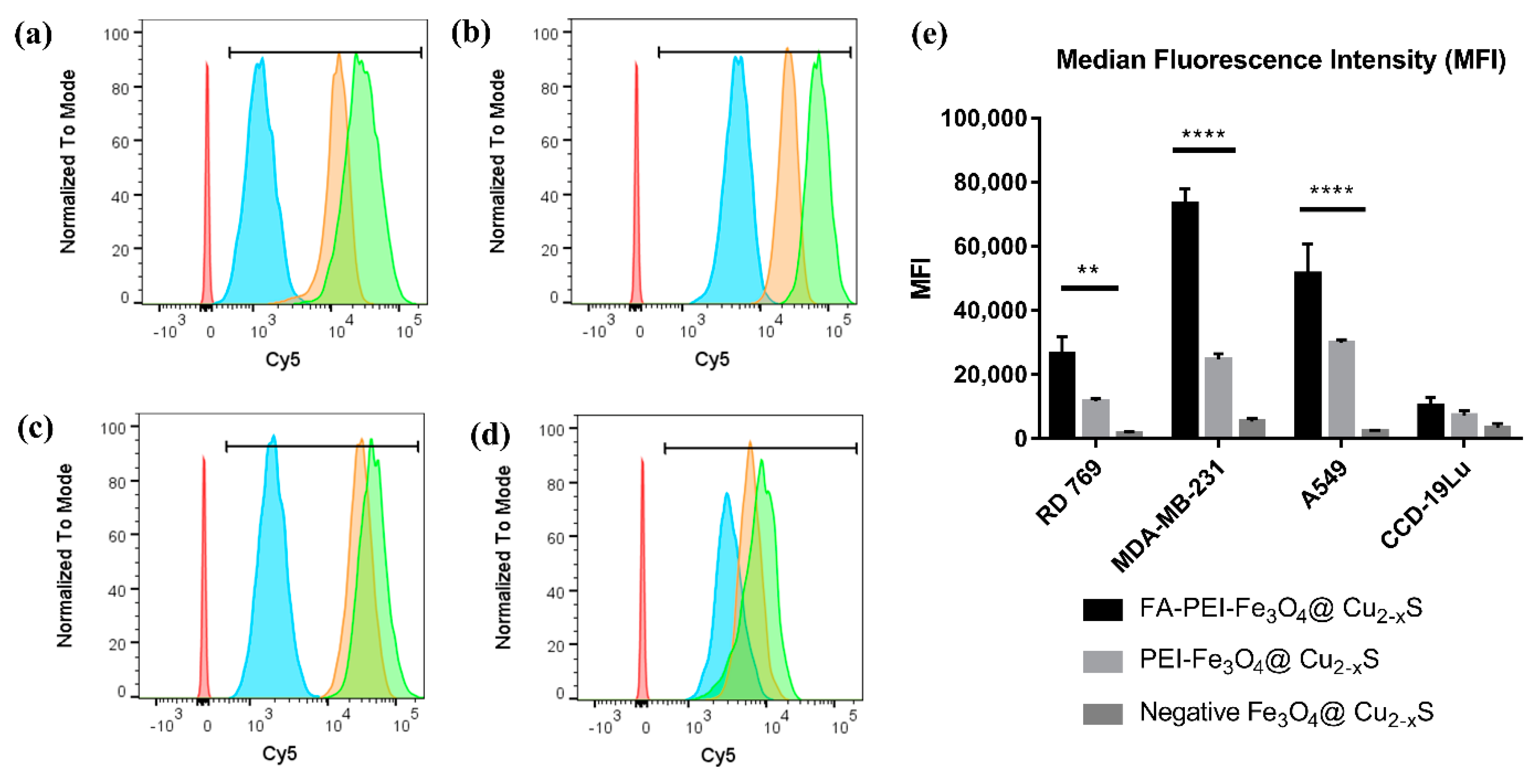
2.9. Flow Cytometry Analysis
2.10. Real-Time Quantitative RT-PCR (qRT-PCR)
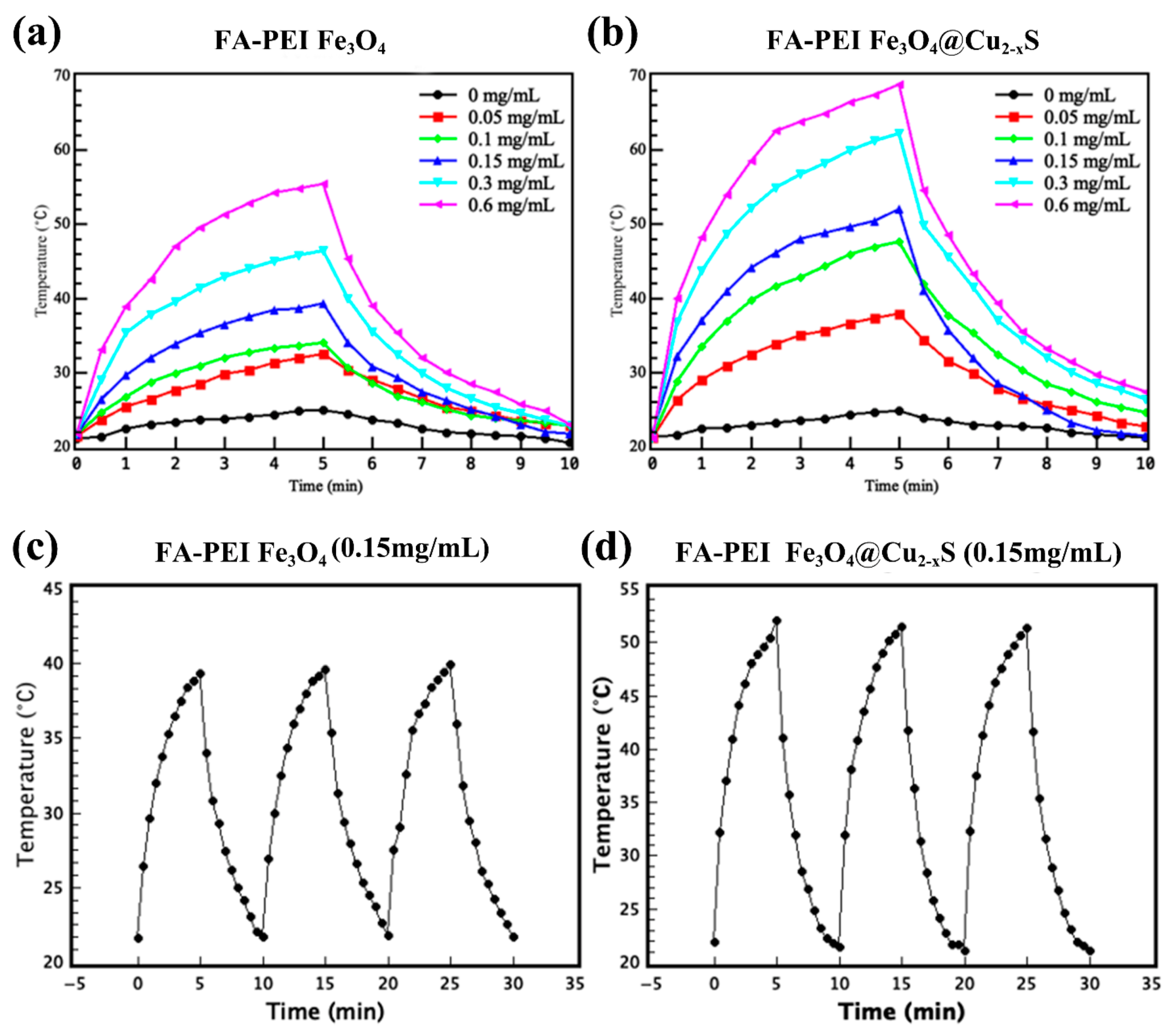
2.11. Photothermal Conversion Efficiency
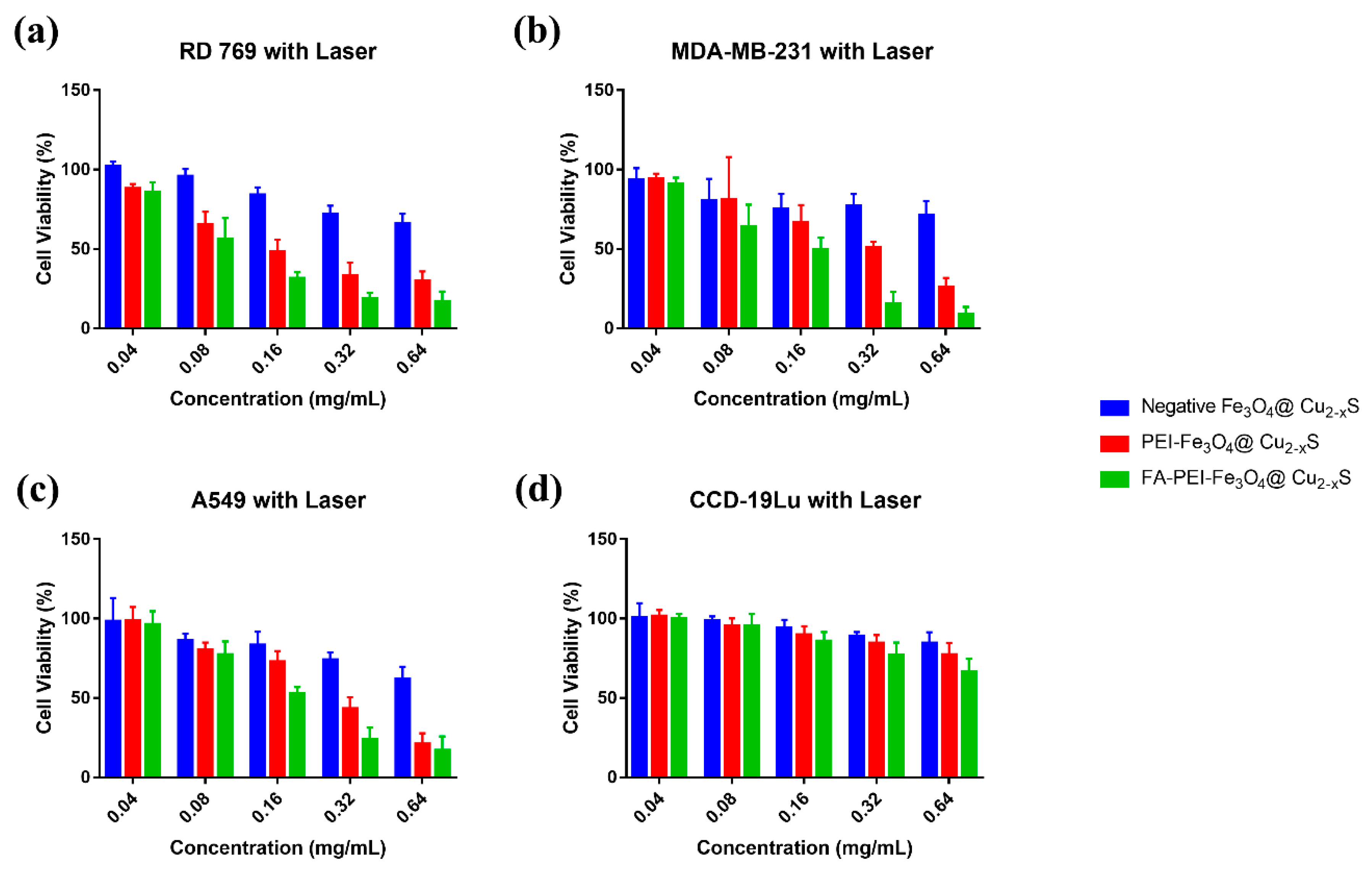
2.12. In Vitro Photothermal Cancer Killing Efficiency
- As = Absorbance of treated cell
- Ac = Absorbance of untreated cell
- Ab = Absorbance of blank background
3. Results and Discussion
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Crezee, J.; Franken, N.; Oei, A. Hyperthermia-based anti-cancer treatments. Cancers 2021, 13, 1240. [Google Scholar] [CrossRef]
- Dunn, A.W.; Zhang, Y.; Mast, D.; Pauletti, G.M.; Xu, H.; Zhang, J.; Ewing, R.C.; Shi, D. In-vitro depth-dependent hyperthermia of human mammary gland adenocarcinoma. Mater. Sci. Eng. C 2016, 69, 12–16. [Google Scholar] [CrossRef] [Green Version]
- Wang, R.; Yang, H.; Fu, R.; Su, Y.; Lin, X.; Jin, X.; Du, W.; Shan, X.; Huang, G. Biomimetic upconversion nanoparticles and gold nanoparticles for novel simultaneous dual-modal imaging-guided photothermal therapy of cancer. Cancers 2020, 12, 3136. [Google Scholar] [CrossRef] [PubMed]
- Qin, J.; Lian, J.; Wu, S.; Wang, Y.; Shi, D. Recent advances in nanotechnology for breast cancer therapy. Nano LIFE 2019, 9, 1940003. [Google Scholar] [CrossRef]
- Nicosia, A.; Cavallaro, G.; Costa, S.; Utzeri, M.A.; Cuttitta, A.; Giammona, G.; Mauro, N. Carbon nanodots for on demand chemophotothermal therapy combination to elicit necroptosis: Overcoming apoptosis resistance in breast cancer cell lines. Cancers 2020, 12, 3114. [Google Scholar] [CrossRef] [PubMed]
- Nocito, G.; Calabrese, G.; Forte, S.; Petralia, S.; Puglisi, C.; Campolo, M.; Esposito, E.; Conoci, S. Carbon dots as promising tools for cancer diagnosis and therapy. Cancers 2021, 13, 1991. [Google Scholar] [CrossRef]
- Marcelo, G.; Lodeiro, C.; Capelo, J.L.; Lorenzo, J.; Oliveira, E. Magnetic, fluorescent and hybrid nanoparticles: From synthesis to application in biosystems. Mater. Sci. Eng. C 2020, 106, 110104. [Google Scholar] [CrossRef]
- Li, A.; Zuo, L. Construction of anti-EpCAM drug-loaded immunomagnetic balls and its application in diagnosis of breast cancer. Nano LIFE 2019, 9, 1940006. [Google Scholar] [CrossRef]
- Wang, Z.; Qiao, R.; Tang, N.; Lu, Z.; Wang, H.; Zhang, Z.; Xue, X.; Huang, Z.; Zhang, S.; Zhang, G.; et al. Active targeting theranostic iron oxide nanoparticles for MRI and magnetic resonance-guided focused ultrasound ablation of lung cancer. Biomaterials 2017, 127, 25–35. [Google Scholar] [CrossRef] [Green Version]
- Sun, S.; Wang, Y.; Zhou, R.; Deng, Z.; Han, Y.; Han, X.; Tao, W.; Yang, Z.; Shi, C.; Hong, D.; et al. Targeting and regulating of an oncogene via nanovector delivery of microRNA using patient-derived xenografts. Theranostics 2017, 7, 677–693. [Google Scholar] [CrossRef] [Green Version]
- Wang, Y.; Sun, S.; Zhang, Z.; Shi, D. Nanomaterials for cancer precision medicine. Adv. Mater. 2018, 30, e1705660. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Chang, Z.; Lu, M.; Shao, D.; Yue, J.; Yang, D.; Zheng, X.; Li, M.; He, K.; Zhang, M.; et al. Shape-controlled magnetic mesoporous silica nanoparticles for magnetically-mediated suicide gene therapy of hepatocellular carcinoma. Biomaterials 2018, 154, 147–157. [Google Scholar] [CrossRef] [PubMed]
- Giustini, A.J.; Petryk, A.A.; Cassim, S.M.; Tate, J.A.; Baker, I.; Hoopes, P.J. Magnetic nanoparticle hyperthermia in cancer treatment. Nano LIFE 2010, 1, 17–32. [Google Scholar] [CrossRef]
- Dunn, A.; Ehsan, S.M.; Mast, D.; Pauletti, G.M.; Xu, H.; Zhang, J.; Ewing, R.C.; Shi, D. Photothermal effects and toxicity of Fe3O4 nanoparticles via near infrared laser irradiation for cancer therapy. Mater. Sci. Eng. C 2015, 46, 97–102. [Google Scholar] [CrossRef]
- Kolosnjaj-Tabi, J.; Kralj, S.; Griseti, E.; Nemec, S.; Wilhelm, C.; Sangnier, A.P.; Bellard, E.; Fourquaux, I.; Golzio, M.; Rols, M.-P. Magnetic silica-coated iron oxide nanochains as photothermal agents, disrupting the extracellular matrix, and eradicating cancer cells. Cancers 2019, 11, 2040. [Google Scholar] [CrossRef] [Green Version]
- Tian, Q.; Hu, J.; Zhu, Y.; Zou, R.; Chen, Z.; Yang, S.; Li, R.; Su, Q.; Han, Y.; Liu, X. Sub-10 nm Fe3O4@Cu2–xS core–shell nanoparticles for dual-modal imaging and photothermal therapy. J. Am. Chem. Soc. 2013, 135, 8571–8577. [Google Scholar] [CrossRef]
- Lin, J.; Zhao, Y.; Shi, D. Optical thermal insulation via the photothermal effects of Fe3O4 and Fe3O4@Cu2–xS thin films for energy-efficient single-pane windows. MRS Commun. 2020, 10, 155–163. [Google Scholar] [CrossRef]
- Chen, B.; Le, W.; Wang, Y.; Li, Z.; Wang, D.; Lin, L.; Cui, S.; Hu, J.J.; Hu, Y.; Yang, P.; et al. Targeting negative surface charges of cancer cells by multifunctional nanoprobes. Theranostics 2016, 6, 1887–1898. [Google Scholar] [CrossRef]
- Han, X.; Deng, Z.; Yang, Z.; Wang, Y.; Zhu, H.; Chen, B.; Cui, Z.; Ewing, R.C.; Shi, D. Biomarkerless targeting and photothermal cancer cell killing by surface-electrically-charged superparamagnetic Fe3O4 composite nanoparticles. Nanoscale 2017, 9, 1457–1465. [Google Scholar] [CrossRef]
- Shi, D. Cancer cell surface negative charges: A bio-physical manifestation of the warburg effect. Nano LIFE 2017, 7, 1771001. [Google Scholar] [CrossRef]
- Wang, Y.; Han, X.; Cui, Z.; Shi, D. Bioelectricity, its fundamentals, characterization methodology, and applications in nano-bioprobing and cancer diagnosis. Adv. Biosyst. 2019, 3, e1900101. [Google Scholar] [CrossRef] [PubMed]
- Zhao, J.; Wu, S.; Qin, J.; Shi, D.; Wang, Y. Electrical-charge-mediated cancer cell targeting via protein corona-decorated superparamagnetic nanoparticles in a simulated physiological environment. ACS Appl. Mater. Interfaces 2018, 10, 41986–41998. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.; Wang, Y.; Shi, D. Positively charged magnetic nanoparticles for capture of circulating tumor cells from clinical blood samples. Nano LIFE 2020, 10, 1971001. [Google Scholar] [CrossRef]
- Wu, S.; Gu, L.; Qin, J.; Zhang, L.; Sun, F.; Liu, Z.; Wang, Y.; Shi, D. Rapid label-free isolation of circulating tumor cells from patients’ peripheral blood using electrically charged Fe3O4 nanoparticles. ACS Appl. Mater. Interfaces 2020, 12, 4193–4203. [Google Scholar] [CrossRef] [PubMed]
- Deng, Z.; Kalin, G.T.; Shi, D.; Kalinichenko, V.V. Nanoparticle delivery systems with cell-specific targeting for pulmonary diseases. Am. J. Respir. Cell Mol. Biol. 2021, 64, 292–307. [Google Scholar] [CrossRef] [PubMed]
- Yoo, J.; Park, C.; Yi, G.; Lee, D.; Koo, H. Active targeting strategies using biological ligands for nanoparticle drug delivery systems. Cancers 2019, 11, 640. [Google Scholar] [CrossRef] [Green Version]
- Frigerio, B.; Bizzoni, C.; Jansen, G.; Leamon, C.P.; Peters, G.J.; Low, P.S.; Matherly, L.H.; Figini, M. Folate receptors and transporters: Biological role and diagnostic/therapeutic targets in cancer and other diseases. J. Exp. Clin. Cancer Res. 2019, 38, 1–12. [Google Scholar] [CrossRef] [Green Version]
- Yu, J.; He, X.; Wang, Z.; Wang, Y.; Liu, S.; Li, X.; Huang, Y. Combining PD-L1 inhibitors with immunogenic cell death triggered by chemo-photothermal therapy via a thermosensitive liposome system to stimulate tumor-specific immunological response. Nanoscale 2021, 13, 12966–12978. [Google Scholar] [CrossRef]
- Nam, K.C.; Han, Y.S.; Lee, J.-M.; Kim, S.C.; Cho, G.; Park, B.J. Photo-functionalized magnetic nanoparticles as a nanocarrier of photodynamic anticancer agent for biomedical theragnostics. Cancers 2020, 12, 571. [Google Scholar] [CrossRef] [Green Version]
- Nejadshafiee, V.; Naeimi, H.; Goliaei, B.; Bigdeli, B.; Sadighi, A.; Dehghani, S.; Lotfabadi, A.; Hosseini, M.; Nezamtaheri, M.S.; Amanlou, M.; et al. Magnetic bio-metal–organic framework nanocomposites decorated with folic acid conjugated chitosan as a promising biocompatible targeted theranostic system for cancer treatment. Mater. Sci. Eng. C 2019, 99, 805–815. [Google Scholar] [CrossRef]
- Moradi, R.; Mohammadzadeh, R.; Akbari, A. Kappa-carrageenan crosslinked magnetic folic acid-conjugated chitosan nanocomposites for arginase encapsulation, delivery and cancer therapy. Nano LIFE 2021, 11, 2140005. [Google Scholar] [CrossRef]
- Wang, F.; Pauletti, G.M.; Wang, J.; Zhang, J.; Ewing, R.C.; Wang, Y.; Shi, D. Dual surface-functionalized janus nanocomposites of polystyrene/Fe3O4@SiO2 for simultaneous tumor cell targeting and stimulus-induced drug release. Adv. Mater. 2013, 25, 3485–3489. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jin, Z.; Nguyen, K.T.; Go, G.; Kang, B.; Min, H.-K.; Kim, S.-J.; Kim, Y.; Li, H.; Kim, C.-S.; Lee, S.; et al. Multifunctional nanorobot system for active therapeutic delivery and synergistic chemo-photothermal therapy. Nano Lett. 2019, 19, 8550–8564. [Google Scholar] [CrossRef] [PubMed]
- Zhou, M.; Li, J.; Liang, S.; Sood, A.K.; Liang, D.; Li, C. CuS nanodots with ultrahigh efficient renal clearance for positron emission tomography imaging and image-guided photothermal therapy. ACS Nano 2015, 9, 7085–7096. [Google Scholar] [CrossRef] [Green Version]
- Cheng, G.; Zong, W.; Guo, H.; Li, F.; Zhang, X.; Yu, P.; Ren, F.; Zhang, X.; Shi, X.; Gao, F.; et al. Programmed size-changeable nanotheranostic agents for enhanced imaging-guided chemo/photodynamic combination therapy and fast elimination. Adv. Mater. 2021, 33, 2100398. [Google Scholar] [CrossRef]
- Wang, S.; Lin, J.; Wang, Z.; Zhou, Z.; Bai, R.; Lu, N.; Liu, Y.; Fu, X.; Jacobson, O.; Fan, W.; et al. Core-satellite polydopamine-gadolinium-metallofullerene nanotheranostics for multimodal imaging guided combination cancer therapy. Adv. Mater. 2017, 29, 1701013. [Google Scholar] [CrossRef]
- Liu, Y.; Bhattarai, P.; Dai, Z.; Chen, X. Photothermal therapy and photoacoustic imaging via nanotheranostics in fighting cancer. Chem. Soc. Rev. 2019, 48, 2053–2108. [Google Scholar] [CrossRef]
- Yang, C.; Wu, T.; Qi, Y.; Zhang, Z. Recent advances in the application of vitamin E TPGS for drug delivery. Theranostics 2018, 8, 464–485. [Google Scholar] [CrossRef]
- Cheng, X.; Zeng, X.; Li, D.; Wang, X.; Sun, M.; He, L.; Tang, R. TPGS-grafted and acid-responsive soy protein nanogels for efficient intracellular drug release, accumulation, penetration in 3D tumor spheroids of drug-resistant cancer cells. Mater. Sci. Eng. C 2019, 102, 863–875. [Google Scholar] [CrossRef]
- Cheng, W.; Liang, C.; Xu, L.; Liu, G.; Gao, N.; Tao, W.; Luo, L.; Zuo, Y.; Wang, X.; Zhang, X.; et al. TPGS-functionalized polydopamine-modified mesoporous silica as drug nanocarriers for enhanced lung cancer chemotherapy against multidrug resistance. Small 2017, 13, 1–12. [Google Scholar] [CrossRef]
- Bolte, C.; Ustiyan, V.; Ren, X.; Dunn, A.W.; Pradhan, A.; Wang, G.; Kolesnichenko, O.A.; Deng, Z.; Zhang, Y.; Shi, D.; et al. Nanoparticle delivery of proangiogenic transcription factors into the neonatal circulation inhibits alveolar simplification caused by hyperoxia. Am. J. Respir. Crit. Care Med. 2020, 202, 100–111. [Google Scholar] [CrossRef] [PubMed]
- Dunn, A.W.; Kalinichenko, V.V.; Shi, D. Highly efficient in vivo targeting of the pulmonary endothelium using novel modifications of polyethylenimine: An importance of charge. Adv. Health Mater. 2018, 7, e1800876. [Google Scholar] [CrossRef]
- Sun, F.; Wang, G.; Pradhan, A.; Xu, K.; Gomez-Arroyo, J.; Zhang, Y.; Kalin, G.T.; Deng, Z.; Vagnozzi, R.J.; He, H.; et al. Nanoparticle delivery of STAT3 alleviates pulmonary hypertension in a mouse model of alveolar capillary dysplasia. Circulation 2021, 144, 539–555. [Google Scholar] [CrossRef] [PubMed]
- Pradhan, A.; Dunn, A.; Ustiyan, V.; Bolte, C.; Wang, G.; Whitsett, J.A.; Zhang, Y.; Porollo, A.; Hu, Y.-C.; Xiao, R.; et al. The S52F FOXF1 mutation inhibits STAT3 signaling and causes alveolar capillary dysplasia. Am. J. Respir. Crit. Care Med. 2019, 200, 1045–1056. [Google Scholar] [CrossRef] [PubMed]
- Luiz, M.T.; Viegas, J.S.R.; Abriata, J.P.; Tofani, L.B.; Vaidergorn, M.D.M.; Emery, F.D.S.; Chorilli, M.; Marchetti, J.M. Docetaxel-loaded folate-modified TPGS-transfersomes for glioblastoma multiforme treatment. Mater. Sci. Eng. C 2021, 124, 112033. [Google Scholar] [CrossRef] [PubMed]
- Xiang, H.; Xue, F.; Yi, T.; Tham, H.P.; Liu, J.-G.; Zhao, Y. Cu2–xS nanocrystals cross-linked with chlorin e6-functionalized polyethylenimine for synergistic photodynamic and photothermal therapy of cancer. ACS Appl. Mater. Interfaces 2018, 10, 16344–16351. [Google Scholar] [CrossRef]
- Xu, Y.; Qin, Y.; Palchoudhury, S.; Bao, Y. Water-soluble iron oxide nanoparticles with high stability and selective surface functionality. Langmuir 2011, 27, 8990–8997. [Google Scholar] [CrossRef]
- Lin, C.-A.J.; Sperling, R.A.; Li, J.K.; Yang, T.-Y.; Li, P.-Y.; Zanella, M.; Chang, W.H.; Parak, W.J. Design of an amphiphilic polymer for nanoparticle coating and functionalization. Small 2008, 4, 334–341. [Google Scholar] [CrossRef]
- Wang, X.; Bhattacharyya, D.; Dennewitz, M.B.; Kalinichenko, V.V.; Zhou, Y.; Lepe, R.; Costa, R.H. Rapid hepatocyte nuclear translocation of the Forkhead Box M1B (FoxM1B) transcription factor caused a transient increase in size of regenerating transgenic hepatocytes. Gene Expr. 2003, 11, 149–162. [Google Scholar] [CrossRef]
- Kalinichenko, V.V.; Gusarova, G.A.; Shin, B.; Costa, R.H. The Forkhead Box F1 transcription factor is expressed in brain and head mesenchyme during mouse embryonic development. Gene Expr. Patterns 2003, 3, 153–158. [Google Scholar] [CrossRef]
- Ren, X.; Zhang, Y.; Snyder, J.; Cross, E.R.; Shah, T.A.; Kalin, T.V.; Kalinichenko, V.V. Forkhead Box M1 transcription factor is required for macrophage recruitment during liver repair. Mol. Cell. Biol. 2010, 30, 5381–5393. [Google Scholar] [CrossRef] [Green Version]
- Cai, Y.; Bolte, C.; Le, T.; Goda, C.; Xu, Y.; Kalin, T.V.; Kalinichenko, V.V. FOXF1 maintains endothelial barrier function and prevents edema after lung injury. Sci. Signal. 2016, 9, ra40. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, I.-M.; Zhou, Y.; Ramakrishna, S.; Hughes, D.E.; Solway, J.; Costa, R.H.; Kalinichenko, V.V. Functional characterization of evolutionarily conserved DNA regions in Forkhead Box F1 gene locus. J. Biol. Chem. 2005, 280, 37908–37916. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kalin, T.V.; Meliton, L.; Meliton, A.Y.; Zhu, X.; Whitsett, J.A.; Kalinichenko, V.V. Pulmonary mastocytosis and enhanced lung inflammation in mice heterozygous null for the Foxf1 gene. Am. J. Respir. Cell Mol. Biol. 2008, 39, 390–399. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bolte, C.; Zhang, Y.; Wang, I.-C.; Kalin, T.V.; Molkentin, J.D.; Kalinichenko, V.V. Expression of Foxm1 transcription factor in cardiomyocytes is required for myocardial development. PLoS ONE 2011, 6, e22217. [Google Scholar] [CrossRef] [Green Version]
- Ustiyan, V.; Wert, S.E.; Ikegami, M.; Wang, I.-C.; Kalin, T.V.; Whitsett, J.A.; Kalinichenko, V.V. Foxm1 transcription factor is critical for proliferation and differentiation of Clara cells during development of conducting airways. Dev. Biol. 2012, 370, 198–212. [Google Scholar] [CrossRef] [Green Version]
- Roper, D.K.; Ahn, W.; Hoepfner, M. Microscale heat transfer transduced by surface plasmon resonant gold nanoparticles. J. Phys. Chem. C 2007, 111, 3636–3641. [Google Scholar] [CrossRef] [Green Version]
- Chen, H.-A.; Ma, Y.-H.; Hsu, T.-Y.; Chen, J.-P. Preparation of peptide and recombinant tissue plasminogen activator conjugated poly (lactic-Co-glycolic acid) (PLGA) magnetic nanoparticles for dual targeted thrombolytic therapy. Int. J. Mol. Sci. 2020, 21, 2690. [Google Scholar] [CrossRef] [Green Version]
- Uthaman, S.; Pillarisetti, S.; Hwang, H.S.; Mathew, A.P.; Huh, K.M.; Rhee, J.H.; Park, I.-K. Tumor microenvironment-regulating immunosenescence-independent nanostimulant synergizing with near-infrared light irradiation for antitumor immunity. ACS Appl. Mater. Interfaces 2021, 13, 4844–4852. [Google Scholar] [CrossRef] [PubMed]
- Gibori, H.; Eliyahu, S.; Krivitsky, A.; Ben-Shushan, D.; Epshtein, Y.; Tiram, G.; Blau, R.; Ofek, P.; Lee, J.S.; Ruppin, E.; et al. Amphiphilic nanocarrier-induced modulation of PLK1 and miR-34a leads to improved therapeutic response in pancreatic cancer. Nat. Commun. 2018, 9, 1–18. [Google Scholar] [CrossRef] [Green Version]
- Zheng, X.; Pan, D.; Chen, M.; Dai, X.; Cai, H.; Zhang, H.; Gong, Q.; Gu, Z.; Luo, K. Tunable hydrophile–lipophile balance for manipulating structural stability and tumor retention of amphiphilic nanoparticles. Adv. Mater. 2019, 31, e1901586. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Deng, Z.; Lin, J.; Bud’ko, S.L.; Webster, B.; Kalin, T.V.; Kalinichenko, V.V.; Shi, D. Dual Targeting with Cell Surface Electrical Charge and Folic Acid via Superparamagnetic Fe3O4@Cu2–xS for Photothermal Cancer Cell Killing. Cancers 2021, 13, 5275. https://doi.org/10.3390/cancers13215275
Deng Z, Lin J, Bud’ko SL, Webster B, Kalin TV, Kalinichenko VV, Shi D. Dual Targeting with Cell Surface Electrical Charge and Folic Acid via Superparamagnetic Fe3O4@Cu2–xS for Photothermal Cancer Cell Killing. Cancers. 2021; 13(21):5275. https://doi.org/10.3390/cancers13215275
Chicago/Turabian StyleDeng, Zicheng, Jou Lin, Sergey L. Bud’ko, Brent Webster, Tanya V. Kalin, Vladimir V. Kalinichenko, and Donglu Shi. 2021. "Dual Targeting with Cell Surface Electrical Charge and Folic Acid via Superparamagnetic Fe3O4@Cu2–xS for Photothermal Cancer Cell Killing" Cancers 13, no. 21: 5275. https://doi.org/10.3390/cancers13215275
APA StyleDeng, Z., Lin, J., Bud’ko, S. L., Webster, B., Kalin, T. V., Kalinichenko, V. V., & Shi, D. (2021). Dual Targeting with Cell Surface Electrical Charge and Folic Acid via Superparamagnetic Fe3O4@Cu2–xS for Photothermal Cancer Cell Killing. Cancers, 13(21), 5275. https://doi.org/10.3390/cancers13215275








