HER3 PET Imaging: 68Ga-Labeled Affibody Molecules Provide Superior HER3 Contrast to 89Zr-Labeled Antibody and Antibody-Fragment-Based Tracers
Abstract
Simple Summary
Abstract
1. Introduction
2. Materials and Methods
2.1. General
2.2. Generation of Seribantumab-F(ab’)2 and DFO Conjugation
2.3. Conjugation of DFO to Seribantumab and Seribantumab-F(ab’)2
2.4. Kinetic Evaluation of Seribantumab and Seribantumab-F(ab’)2
2.5. Radiolabeling of DFO-Seribantumab and DFO-Seribantumab-F(ab’)2 with 89Zr and 68Ga
2.6. Stability of [89Zr]Zr-DFO-Seribantumab, [89Zr]Zr-DFO-Seribantumab-F(ab’)2, and [68Ga]Ga-DFO-Seribantumab-F(ab’)2
2.7. Production and Radiolabeling of [68Ga]Ga-ZHER3
2.8. In Vitro Characterization of [89Zr]Zr-DFO-Seribantumab, [89Zr]Zr-DFO-Seribantumab-F(ab’)2, and [68Ga]Ga-DFO-Seribantumab-F(ab’)2
2.9. Biodistribution and In Vivo Specificity of [68Ga]Ga-DFO-Seribantumab-F(ab’)2, [89Zr]Zr-DFO-Seribantumab-F(ab’)2, and [89Zr]Zr-DFO-Seribantumab
2.10. Ex Vivo Autoradiography and Hematoxylin and Eosin Staining of BxPC-3 Xenografts
2.11. nanoPET/CT Imaging
3. Results
3.1. Generation of Seribantumab-F(ab’)2 and DFO Conjugation
3.2. Kinetic Evaluation of Seribantumab-F(ab’)2 and Seribantumab
3.3. Radiolabeling and Stability
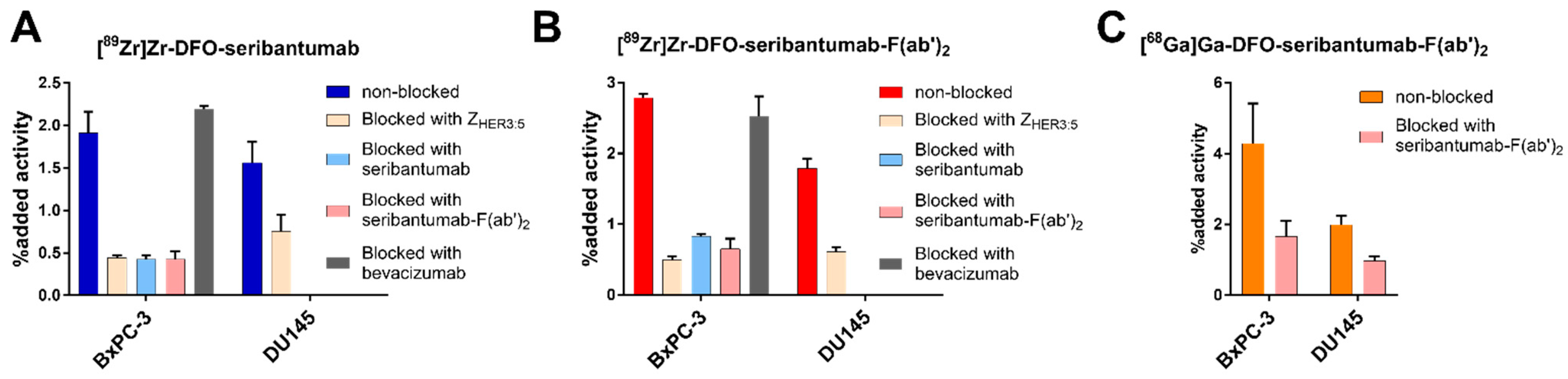
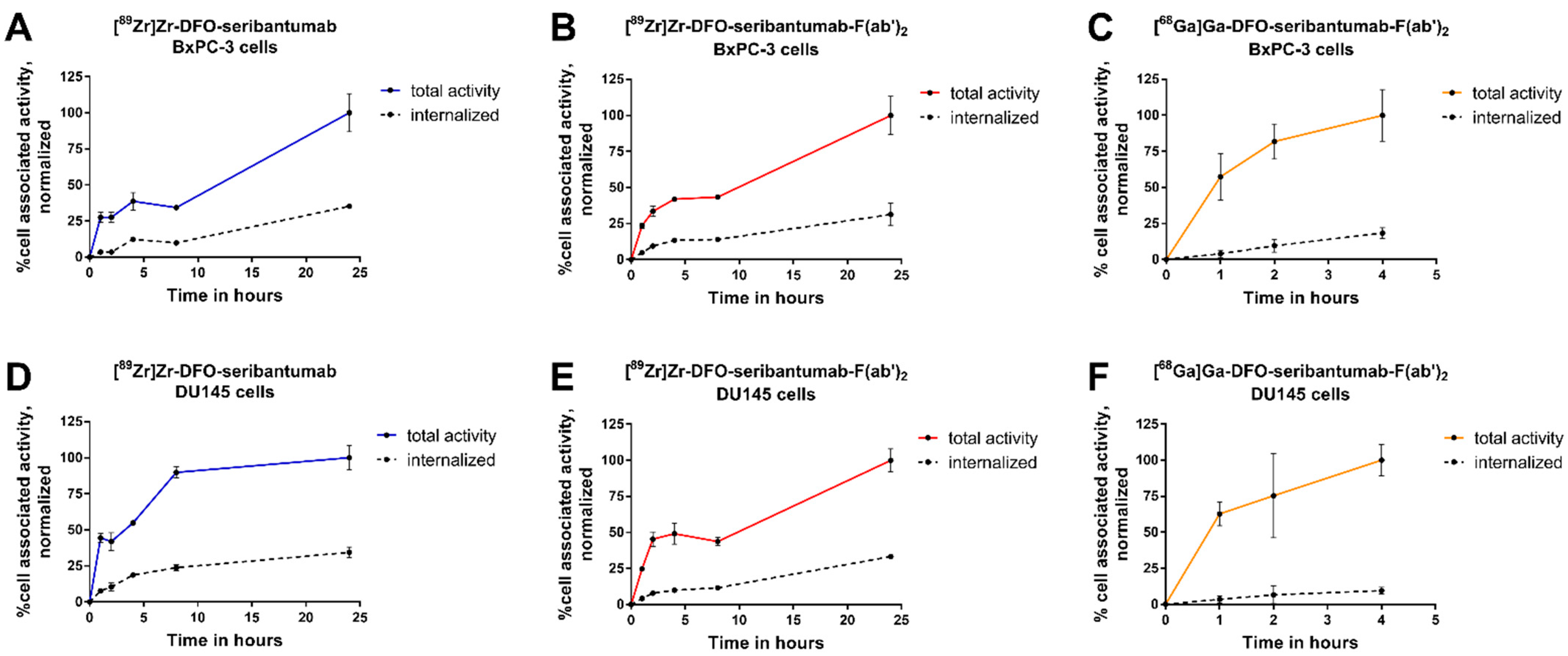
3.4. In Vitro Characterization of [89Zr]Zr-DFO-Seribantumab, [89Zr]Zr-DFO-Seribantumab-F(ab’)2, and [68Ga]Ga-DFO-Seribantumab-F(ab’)2
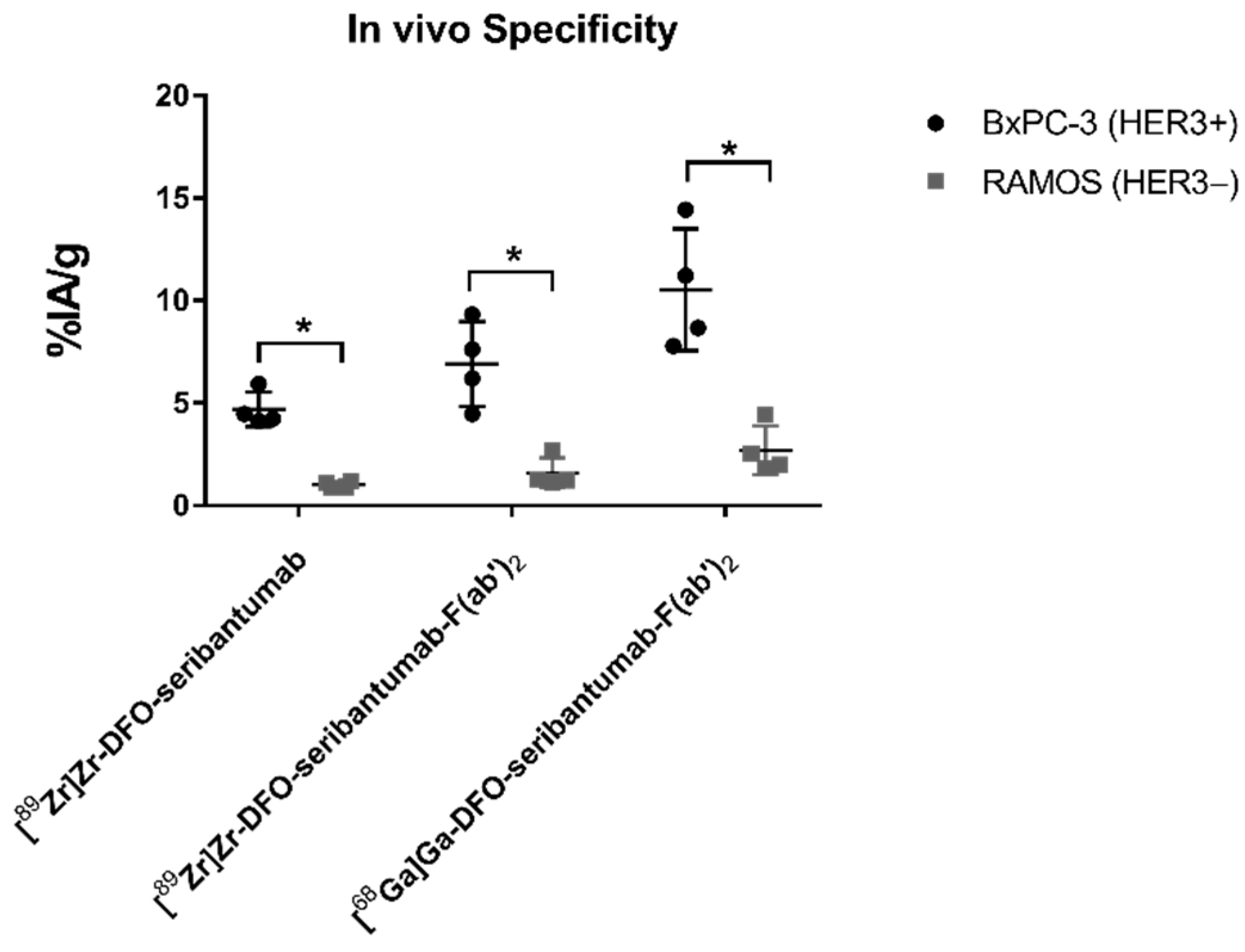
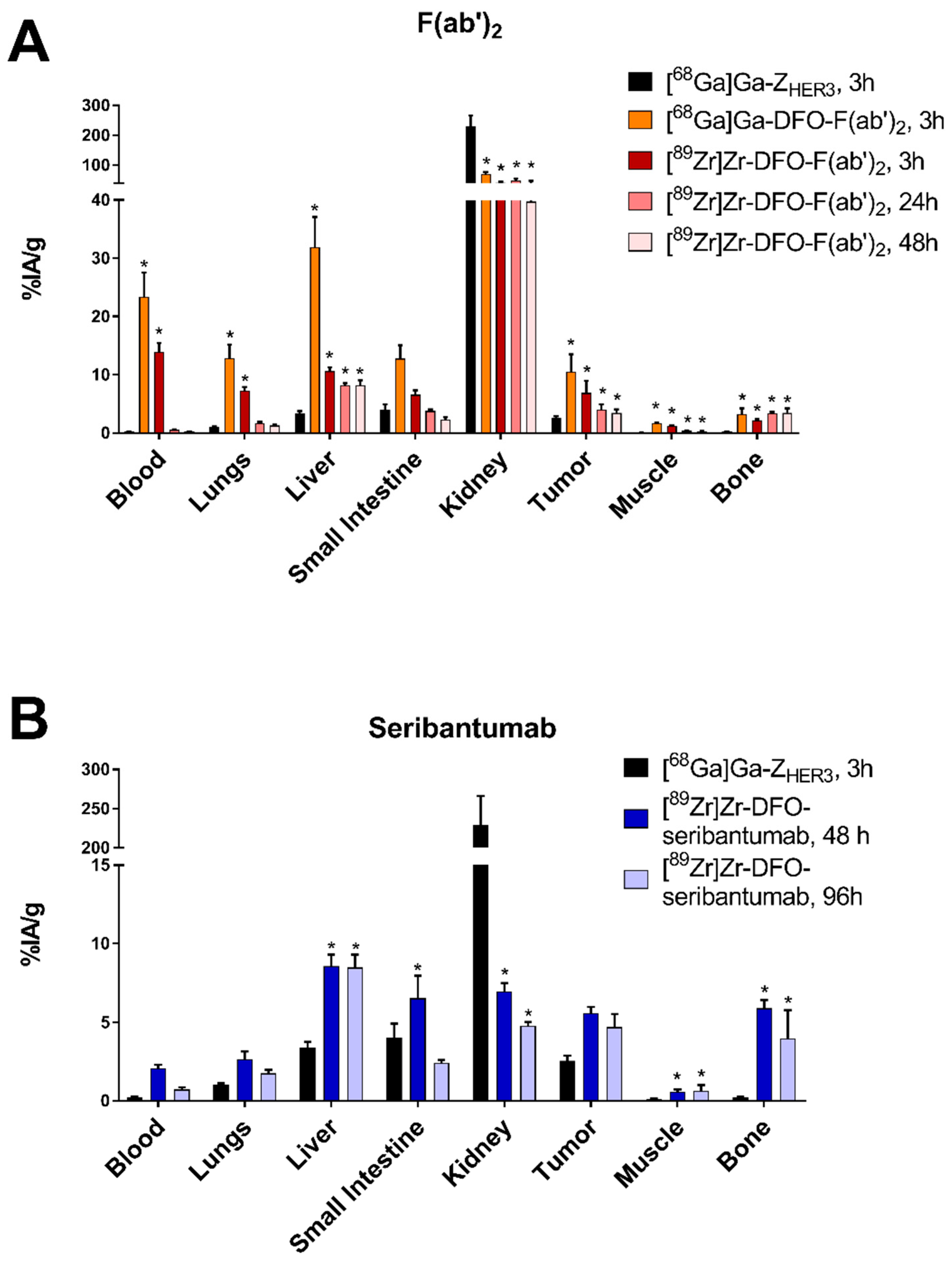
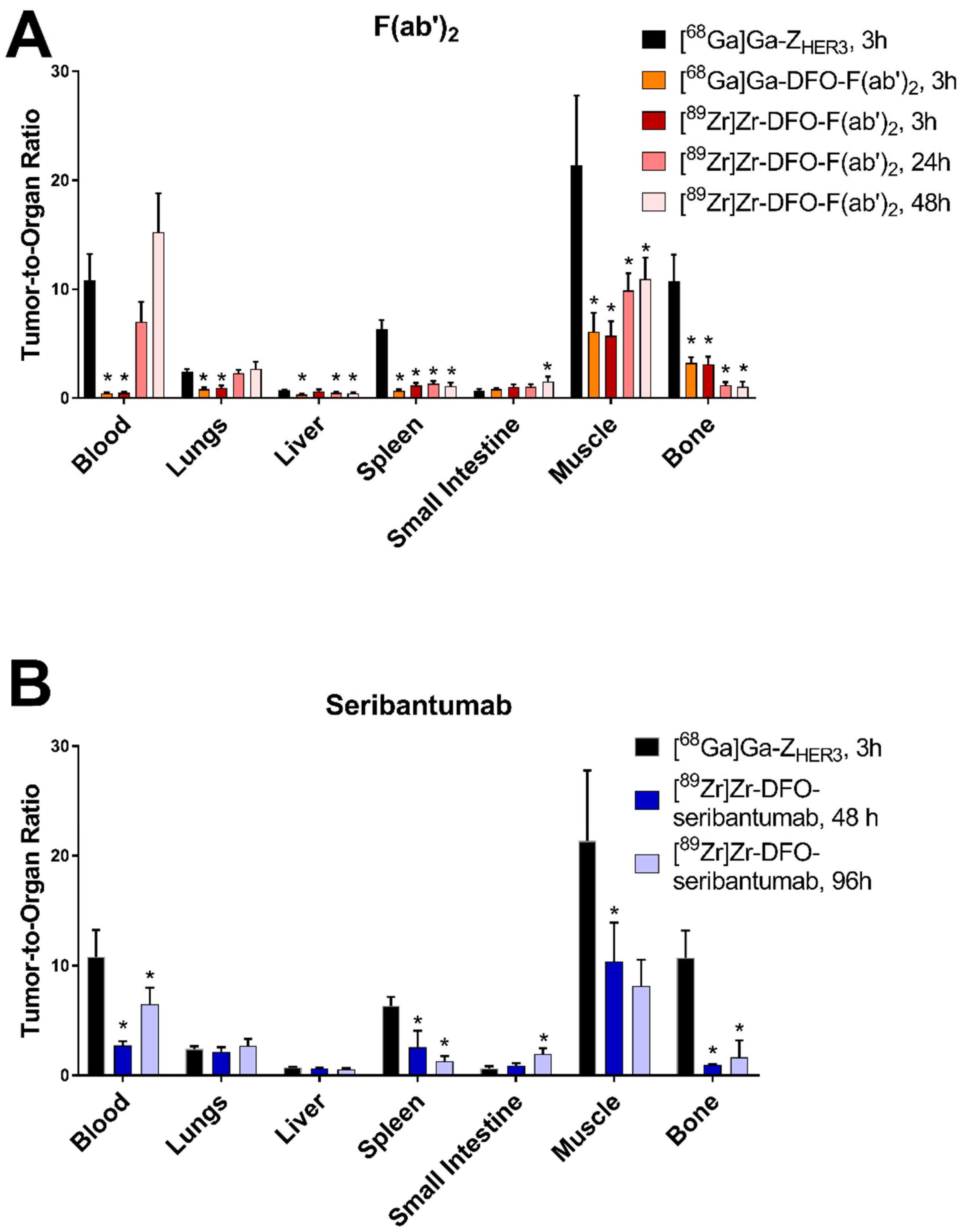
3.5. In Vivo Biodistribution and Specificity
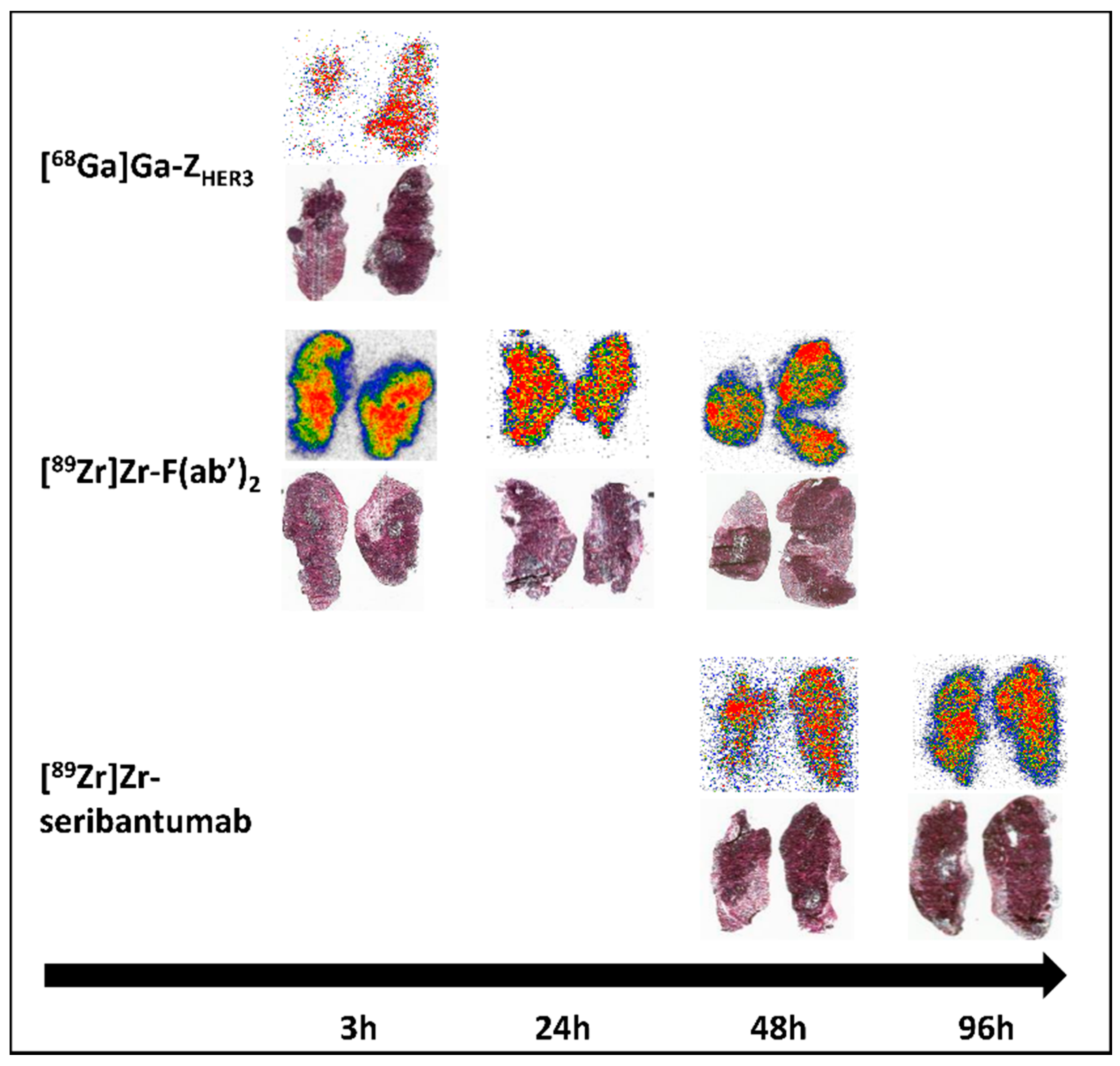
3.6. Ex Vivo Autoradiography of BxPC-3 Xenografts
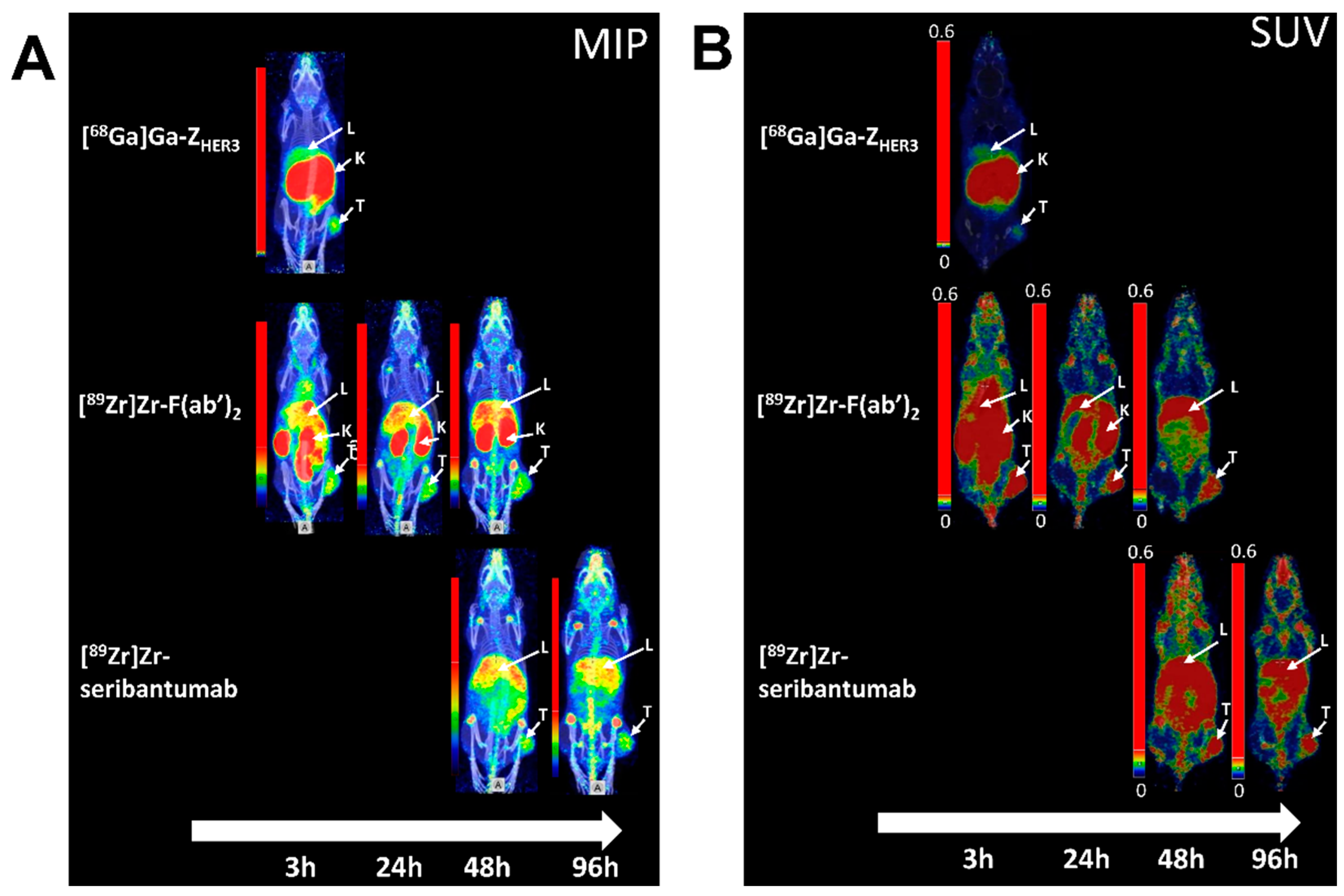
3.7. nanoPET/CT Imaging
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lee, Y.; Ma, J.; Lyu, H.; Huang, J.; Kim, A.; Liu, B. Role of ErbB3 receptors in cancer therapeutic resistance. Acta Biochim. Biophys. Sin. 2014, 46, 190–198. [Google Scholar] [CrossRef]
- Li, Q.; Zhang, R.; Yan, H.; Zhao, P.; Wu, L.; Wang, H.; Li, T.; Cao, B. Prognostic significance of HER3 in Patients with malignant solid tumors. Oncotarget 2017, 8, 67140–67151. [Google Scholar] [CrossRef] [PubMed]
- Mishra, R.; Patel, H.; Alanazi, S.; Yuan, L.; Garrett, J.T. HER3 signaling and targeted therapy in cancer. Oncol. Rev. 2018, 12, 355. [Google Scholar] [CrossRef] [PubMed]
- Robinson, M.K.; Hodge, K.M.; Horak, E.; Sundberg, Å.L.; Russeva, M.; Shaller, C.C.; von Mehren, M.; Shchaveleva, I.; Simmons, H.H.; Marks, J.D.; et al. Targeting ErbB2 and ErbB3 with a bispecific single-chain fv enhances targeting selectivity and induces a therapeutic effect in vitro. Br. J. Cancer 2008, 99, 1415–1425. [Google Scholar] [CrossRef] [PubMed]
- Ross, J.S.; Fletcher, J.A.; Bloom, K.J.; Linette, G.P.; Stec, J.; Symmans, W.F.; Pusztai, L.; Hortobagyi, G.N. Targeted therapy in breast cancer: The HER-2/Neu gene and protein. Mol. Cell Proteom. 2004, 3, 379–398. [Google Scholar] [CrossRef] [PubMed]
- Krasniqi, A.; D’Huyvetter, M.; Devoogdt, N.; Frejd, F.Y.; Sörensen, J.; Orlova, A.; Keyaerts, M.; Tolmachev, V. Same-day imaging using small proteins: Clinical experience and translational prospects in oncology. J. Nucl. Med. 2018, 59, 885–891. [Google Scholar] [CrossRef]
- Leelawattanachai, J.; Kwon, K.-W.; Michael, P.; Ting, R.; Kim, J.-Y.; Jin, M.M. Side-by-side comparison of commonly used biomolecules that differ in size and affinity on tumor uptake and internalization. PLoS ONE 2015, 10, e0124440. [Google Scholar] [CrossRef]
- Rinne, S.S.; Orlova, A.; Tolmachev, V. PET and SPECT imaging of the EGFR family (rtk class i) in oncology. Int. J. Mol. Sci. 2021, 22, 3663. [Google Scholar] [CrossRef]
- Pereira, P.M.R.; Abma, L.; Henry, K.E.; Lewis, J.S. Imaging of human epidermal growth factor receptors for patient selection and response monitoring—From PET imaging and beyond. Cancer Lett. 2018, 419, 139–151. [Google Scholar] [CrossRef]
- Dammes, N.; Peer, D. Monoclonal antibody-based molecular imaging strategies and theranostic opportunities. Theranostics 2020, 10, 938–955. [Google Scholar] [CrossRef]
- Bensch, F.; Lamberts, L.E.; Smeenk, M.M.; Jorritsma-Smit, A.; Lub-de Hooge, M.N.; Terwisscha van Scheltinga, A.G.T.; de Jong, J.R.; Gietema, J.A.; Schröder, C.P.; Thomas, M.; et al. (89)Zr-Lumretuzumab PET imaging before and during HER3 antibody lumretuzumab treatment in patients with solid tumors. Clin. Cancer Res. 2017, 23, 6128–6137. [Google Scholar] [CrossRef]
- Dijkers, E.C.; Munnink, T.H.O.; Kosterink, J.G.; Brouwers, A.H.; Jager, P.L.; de Jong, J.R.; van Dongen, G.A.; Schröder, C.P.; Hooge, M.N.L.; de Vries, E.G. Biodistribution of 89Zr-Trastuzumab and PET Imaging of HER2-positive lesions in patients with metastatic breast cancer. Clin. Pharmacol. Ther. 2010, 87, 586–592. [Google Scholar] [CrossRef]
- Menke-van der Houven van Oordt, C.W.; Gootjes, E.C.; Huisman, M.C.; Vugts, D.J.; Roth, C.; Luik, A.M.; Mulder, E.R.; Schuit, R.C.; Boellaard, R.; Hoekstra, O.S.; et al. 89Zr-Cetuximab PET Imaging in Patients with Advanced Colorectal Cancer. Available online: https://pubmed.ncbi.nlm.nih.gov/26309164/ (accessed on 2 December 2020).
- Thomas, G.D. Effect of dose, molecular size, and binding affinity on uptake of antibodies. In Drug Targeting: Strategies, Principles, and Applications; Francis, G.E., Delgado, C., Eds.; Methods in Molecular MedicineTM; Humana Press: Totowa, NJ, USA, 2000; pp. 115–132. ISBN 978-1-59259-075-9. [Google Scholar]
- Menke-van der Houven van Oordt, C.W.; McGeoch, A.; Bergstrom, M.; McSherry, I.; Smith, D.A.; Cleveland, M.; Al-Azzam, W.; Chen, L.; Verheul, H.; Hoekstra, O.S.; et al. Immuno-PET imaging to assess target engagement: Experience from 89Zr-Anti-HER3 MAb (GSK2849330) in patients with solid tumors. J. Nucl. Med. 2019, 60, 902–909. [Google Scholar] [CrossRef]
- Lockhart, A.C.; Liu, Y.; Dehdashti, F.; Laforest, R.; Picus, J.; Frye, J.; Trull, L.; Belanger, S.; Desai, M.; Mahmood, S.; et al. Phase 1 Evaluation of [(64)Cu]DOTA-patritumab to assess dosimetry, apparent receptor occupancy, and safety in subjects with advanced solid tumors. Mol. Imaging Biol. 2016, 18, 446–453. [Google Scholar] [CrossRef]
- Pool, M.; Kol, A.; de Jong, S.; de Vries, E.G.E.; Lub-de Hooge, M.N.; Terwisscha van Scheltinga, A.G.T. (89)Zr-MAb3481 PET for HER3 tumor status assessment during lapatinib treatment. MAbs 2017, 9, 1–9. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yuan, Q.; Furukawa, T.; Tashiro, T.; Okita, K.; Jin, Z.-H.; Aung, W.; Sugyo, A.; Nagatsu, K.; Endo, H.; Tsuji, A.B.; et al. Immuno-PET Imaging of HER3 in a model in which HER3 signaling plays a critical role. PLoS ONE 2015, 10, e0143076. [Google Scholar] [CrossRef] [PubMed]
- Wehrenberg-Klee, E.; Turker, N.S.; Heidari, P.; Larimer, B.; Juric, D.; Baselga, J.; Scaltriti, M.; Mahmood, U. Differential receptor tyrosine kinase PET imaging for therapeutic guidance. J. Nucl. Med. 2016, 57, 1413–1419. [Google Scholar] [CrossRef][Green Version]
- Larimer, B.M.; Phelan, N.; Wehrenberg-Klee, E.; Mahmood, U. Phage display selection, in vitro characterization, and correlative pet imaging of a novel HER3 peptide. Mol. Imaging Biol. 2017, 20, 300–308. [Google Scholar] [CrossRef] [PubMed]
- Ståhl, S.; Gräslund, T.; Eriksson Karlström, A.; Frejd, F.Y.; Nygren, P.-Å.; Löfblom, J. Affibody molecules in biotechnological and medical applications. Trends Biotechnol. 2017, 35, 691–712. [Google Scholar] [CrossRef]
- Malm, M.; Kronqvist, N.; Lindberg, H.; Gudmundsdotter, L.; Bass, T.; Frejd, F.Y.; Höidén-Guthenberg, I.; Varasteh, Z.; Orlova, A.; Tolmachev, V.; et al. Inhibiting HER3-mediated tumor cell growth with affibody molecules engineered to low picomolar affinity by position-directed error-prone PCR-like diversification. PLoS ONE 2013, 8, e62791. [Google Scholar] [CrossRef]
- Da Pieve, C.; Allott, L.; Martins, C.D.; Vardon, A.; Ciobota, D.M.; Kramer-Marek, G.; Smith, G. Efficient [18F]AlF radiolabeling of ZHER3:8698 affibody molecule for imaging of HER3 positive tumors. Bioconjug. Chem. 2016, 27, 1839–1849. [Google Scholar] [CrossRef]
- Dahlsson Leitao, C.; Rinne, S.S.; Altai, M.; Vorontsova, O.; Dunås, F.; Jonasson, P.; Tolmachev, V.; Löfblom, J.; Ståhl, S.; Orlova, A. Evaluating the therapeutic efficacy of mono- and bivalent affibody-based fusion proteins targeting HER3 in a pancreatic cancer xenograft model. Pharmaceutics 2020, 12, 551. [Google Scholar] [CrossRef]
- Martins, C.D.; Da Pieve, C.; Burley, T.A.; Smith, R.; Ciobota, D.M.; Allott, L.; Harrington, K.J.; Oyen, W.J.G.; Smith, G.; Kramer-Marek, G. HER3-mediated resistance to Hsp90 inhibition detected in breast cancer xenografts by affibody-based PET imaging. Clin. Cancer Res. 2018, 24, 1853–1865. [Google Scholar] [CrossRef]
- Rosestedt, M.; Andersson, K.G.; Mitran, B.; Tolmachev, V.; Löfblom, J.; Orlova, A.; Ståhl, S. Affibody-mediated PET imaging of HER3 expression in malignant tumours. Sci. Rep. 2015, 5, 15226. [Google Scholar] [CrossRef]
- Dahlsson Leitao, C.; Rinne, S.S.; Mitran, B.; Vorobyeva, A.; Andersson, K.G.; Tolmachev, V.; Ståhl, S.; Löfblom, J.; Orlova, A. Molecular design of HER3-targeting affibody molecules: Influence of chelator and presence of HEHEHE-Tag on biodistribution of 68Ga-labeled tracers. Int. J. Mol. Sci. 2019, 20, 1080. [Google Scholar] [CrossRef]
- Rinne, S.S.; Dahlsson Leitao, C.; Gentry, J.; Mitran, B.; Abouzayed, A.; Tolmachev, V.; Ståhl, S.; Löfblom, J.; Orlova, A. Increase in negative charge of 68Ga/chelator complex reduces unspecific hepatic uptake but does not improve imaging properties of HER3-targeting affibody molecules. Sci. Rep. 2019, 9, 17710. [Google Scholar] [CrossRef]
- Rinne, S.S.; Leitao, C.D.; Mitran, B.; Bass, T.Z.; Andersson, K.G.; Tolmachev, V.; Ståhl, S.; Löfblom, J.; Orlova, A. Optimization of HER3 expression imaging using affibody molecules: Influence of chelator for labeling with indium-111. Sci. Rep. 2019, 9, 655. [Google Scholar] [CrossRef] [PubMed]
- Rinne, S.S.; Dahlsson Leitao, C.; Saleh-Nihad, Z.; Mitran, B.; Tolmachev, V.; Ståhl, S.; Löfblom, J.; Orlova, A. Benefit of later-time-point PET imaging of HER3 expression using optimized radiocobalt-labeled affibody molecules. Int. J. Mol. Sci. 2020, 21, 1972. [Google Scholar] [CrossRef]
- Vosjan, M.J.W.D.; Perk, L.R.; Visser, G.W.M.; Budde, M.; Jurek, P.; Kiefer, G.E.; van Dongen, G.A.M.S. Conjugation and radiolabeling of monoclonal antibodies with zirconium-89 for PET imaging using the bifunctional chelate p -Isothiocyanatobenzyl-Desferrioxamine. Nat. Protoc. 2010, 5, 739–743. [Google Scholar] [CrossRef] [PubMed]
- Wållberg, H.; Orlova, A. Slow Internalization of Anti-HER2 Synthetic Affibody Monomer 111In-DOTA-ZHER2:342-Pep2: Implications for development of labeled tracers. Cancer Biother. Radiopharm. 2008, 23, 435–442. [Google Scholar] [CrossRef] [PubMed]
- Mitran, B.; Rinne, S.S.; Konijnenberg, M.W.; Maina, T.; Nock, B.A.; Altai, M.; Vorobyeva, A.; Larhed, M.; Tolmachev, V.; de Jong, M.; et al. Trastuzumab cotreatment improves survival of mice with PC-3 prostate cancer xenografts treated with the GRPR antagonist 177 Lu-DOTAGA-PEG2 -RM26. Int. J. Cancer 2019, 145, 3347–3358. [Google Scholar] [CrossRef]
- Orlova, A.; Malm, M.; Rosestedt, M.; Varasteh, Z.; Andersson, K.; Selvaraju, R.K.; Altai, M.; Honarvar, H.; Strand, J.; Ståhl, S.; et al. Imaging of HER3-expressing xenografts in mice using a (99 m)Tc(CO) 3-HEHEHE-Z HER3:08699 affibody molecule. Eur. J. Nucl. Med. Mol. Imaging 2014, 41, 1450–1459. [Google Scholar] [CrossRef]
- Alsaid, H.; Skedzielewski, T.; Rambo, M.V.; Hunsinger, K.; Hoang, B.; Fieles, W.; Long, E.R.; Tunstead, J.; Vugts, D.J.; Cleveland, M.; et al. Non invasive imaging assessment of the biodistribution of GSK2849330, an ADCC and CDC optimized anti HER3 MAb, and its role in tumor macrophage recruitment in human tumor-bearing mice. PLoS ONE 2017, 12, e0176075. [Google Scholar] [CrossRef]
- Terwisscha van Scheltinga, A.G.; Lub-de Hooge, M.N.; Abiraj, K.; Schröder, C.P.; Pot, L.; Bossenmaier, B.; Thomas, M.; Hölzlwimmer, G.; Friess, T.; Kosterink, J.G.; et al. ImmunoPET and biodistribution with human epidermal growth factor receptor 3 targeting antibody 89Zr-RG7116. MAbs 2014, 6, 1051–1058. [Google Scholar] [CrossRef] [PubMed]
- Beylergil, V.; Morris, P.G.; Smith-Jones, P.M.; Modi, S.; Solit, D.; Hudis, C.A.; Lu, Y.; O’Donoghue, J.; Lyashchenko, S.K.; Carrasquillo, J.A.; et al. Pilot study of 68Ga-DOTA-F(Ab’)2-Trastuzumab in patients with breast cancer. Nucl. Med. Commun. 2013, 34, 1157–1165. [Google Scholar] [CrossRef] [PubMed]
- Smith-Jones, P.M.; Solit, D.B.; Akhurst, T.; Afroze, F.; Rosen, N.; Larson, S.M. Imaging the pharmacodynamics of HER2 degradation in response to Hsp90 inhibitors. Nat. Biotechnol. 2004, 22, 701–706. [Google Scholar] [CrossRef] [PubMed]
- Prata, M.I.M.; André, J.P.; Kovács, Z.; Takács, A.I.; Tircsó, G.; Tóth, I.; Geraldes, C.F.G.C. Gallium(III) chelates of mixed phosphonate-carboxylate triazamacrocyclic ligands relevant to nuclear medicine: Structural, stability and in vivo studies. J. Inorg. Biochem. 2017, 177, 8–16. [Google Scholar] [CrossRef] [PubMed]
- Hosseinimehr, S.J.; Tolmachev, V.; Orlova, A. Liver uptake of radiolabeled targeting proteins and peptides: Considerations for targeting peptide conjugate design. Drug. Discov. Today 2012, 17, 1224–1232. [Google Scholar] [CrossRef] [PubMed]
- Brandt, M.; Cowell, J.; Aulsebrook, M.L.; Gasser, G.; Mindt, T.L. Radiolabelling of the octadentate chelators DFO* and OxoDFO* with Zirconium-89 and Gallium-68. J. Biol. Inorg. Chem. 2020, 25, 789–796. [Google Scholar] [CrossRef]
- Bhatt, N.B.; Pandya, D.N.; Wadas, T.J. Recent advances in Zirconium-89 chelator development. Molecules 2018, 23, 638. [Google Scholar] [CrossRef]
- Tsionou, M.I.; Knapp, C.E.; Foley, C.A.; Munteanu, C.R.; Cakebread, A.; Imberti, C.; Eykyn, T.R.; Young, J.D.; Paterson, B.M.; Blower, P.J.; et al. Comparison of macrocyclic and acyclic chelators for Gallium-68 Radiolabelling. RSC Adv. 2017, 7, 49586–49599. [Google Scholar] [CrossRef] [PubMed]
- Gourni, E.; Del Pozzo, L.; Bartholomä, M.; Kiefer, Y.T.; Meyer, P.; Maecke, H.R.; Holland, J.P. Radiochemistry and preclinical PET imaging of 68Ga-Desferrioxamine radiotracers targeting prostate-specific membrane antigen. Mol. Imaging 2017, 16. [Google Scholar] [CrossRef]
- Kaeppeli, S.A.M.; Schibli, R.; Mindt, T.L.; Behe, M. Comparison of Desferrioxamine and NODAGA for the Gallium-68 labeling of Exendin-4. EJNMMI Radiopharm. Chem. 2019, 4, 9. [Google Scholar] [CrossRef] [PubMed]
- Oroujeni, M.; Garousi, J.; Andersson, K.G.; Löfblom, J.; Mitran, B.; Orlova, A.; Tolmachev, V. Preclinical evaluation of [68Ga]Ga-DFO-ZEGFR:2377: A promising affibody-based probe for noninvasive PET imaging of EGFR expression in tumors. Cells 2018, 7, 141. [Google Scholar] [CrossRef] [PubMed]
- van Dijk, L.K.; Hoeben, B.A.W.; Kaanders, J.H.A.M.; Franssen, G.M.; Boerman, O.C.; Bussink, J. Imaging of epidermal growth factor receptor expression in head and neck cancer with SPECT/CT and 111In-labeled cetuximab-F(ab′)2. J. Nucl. Med. 2013, 54, 2118–2124. [Google Scholar] [CrossRef] [PubMed]
- Covell, D.G.; Barbet, J.; Holton, O.D.; Black, C.D.; Parker, R.J.; Weinstein, J.N. Pharmacokinetics of monoclonal immunoglobulin G1, F(ab’)2, and Fab’ in Mice. Cancer Res. 1986, 46, 3969–3978. [Google Scholar] [PubMed]
- Ryman, J.T.; Meibohm, B. Pharmacokinetics of monoclonal antibodies. CPT Pharmacomet. Syst. Pharmacol. 2017, 6, 576–588. [Google Scholar] [CrossRef] [PubMed]
- Abou, D.S.; Ku, T.; Smith-Jones, P.M. In vivo biodistribution and accumulation of 89Zr in mice. Nucl. Med. Biol. 2011, 38, 675–681. [Google Scholar] [CrossRef]
- Rao, K.; Gaughan, L.; Robson, C.; McCracken, S. The Role of the HER2 and HER3 in prostate cancer and their potential as therapeutic targets. Eur. J. Cancer 2016, 61, S177. [Google Scholar] [CrossRef]
- Patra, M.; Bauman, A.; Mari, C.; Fischer, C.A.; Blacque, O.; Häussinger, D.; Gasser, G.; Mindt, T.L. An octadentate bifunctional chelating agent for the development of stable zirconium-89 based molecular imaging probes. Chem. Commun. 2014, 50, 11523–11525. [Google Scholar] [CrossRef]
- Vugts, D.J.; Klaver, C.; Sewing, C.; Poot, A.J.; Adamzek, K.; Huegli, S.; Mari, C.; Visser, G.W.M.; Valverde, I.E.; Gasser, G.; et al. Comparison of the octadentate bifunctional chelator DFO*-PPhe-NCS and the clinically used hexadentate bifunctional chelator DFO-PPhe-NCS for 89Zr-Immuno-PET. Eur. J. Nucl. Med. Mol. Imaging 2017, 44, 286–295. [Google Scholar] [CrossRef] [PubMed]
- Sandström, M.; Lindskog, K.; Velikyan, I.; Wennborg, A.; Feldwisch, J.; Sandberg, D.; Tolmachev, V.; Orlova, A.; Sörensen, J.; Carlsson, J.; et al. Biodistribution and radiation dosimetry of the Anti-HER2 affibody molecule 68Ga-ABY-025 in breast cancer patients. J. Nucl. Med. 2016, 57, 867–871. [Google Scholar] [CrossRef] [PubMed]
| Radioconjugate | Radiochemical Yield (%) (n = 3) | Purity (%) | Stability PBS (%) | Stability Serum 37 °C (%) | ||||
|---|---|---|---|---|---|---|---|---|
| 1 h | 3 h | 24 h | 1 h | 3 h | 24 h | |||
| [89Zr]Zr-DFO-seribantumab | 99.7 ± 0.5 | - | 100 ± 0 | 100.0 ± 0.1 | 100 ± 0 | 97.0 ± 0.7 | 92 ± 3 | 76 ± 4 |
| [89Zr]Zr-DFO-seribantumab-F(ab’)2 | 80 ± 4 | 97 ± 1 | 97.1 ± 0.6 | 96.4 ± 0.8 | 92.4 ± 1.0 | 94.1 ± 0.8 | 93 ± 2 | 77 ± 6 |
| [68Ga]Ga-DFO-seribantumab-F(ab’)2 | 88 ± 2 | 100 ± 0 | 100 ± 0 | 100 ± 0 | - | 15 ± 2 | 17 ± 3 | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rinne, S.S.; Leitao, C.D.; Abouzayed, A.; Vorobyeva, A.; Tolmachev, V.; Ståhl, S.; Löfblom, J.; Orlova, A. HER3 PET Imaging: 68Ga-Labeled Affibody Molecules Provide Superior HER3 Contrast to 89Zr-Labeled Antibody and Antibody-Fragment-Based Tracers. Cancers 2021, 13, 4791. https://doi.org/10.3390/cancers13194791
Rinne SS, Leitao CD, Abouzayed A, Vorobyeva A, Tolmachev V, Ståhl S, Löfblom J, Orlova A. HER3 PET Imaging: 68Ga-Labeled Affibody Molecules Provide Superior HER3 Contrast to 89Zr-Labeled Antibody and Antibody-Fragment-Based Tracers. Cancers. 2021; 13(19):4791. https://doi.org/10.3390/cancers13194791
Chicago/Turabian StyleRinne, Sara S., Charles Dahlsson Leitao, Ayman Abouzayed, Anzhelika Vorobyeva, Vladimir Tolmachev, Stefan Ståhl, John Löfblom, and Anna Orlova. 2021. "HER3 PET Imaging: 68Ga-Labeled Affibody Molecules Provide Superior HER3 Contrast to 89Zr-Labeled Antibody and Antibody-Fragment-Based Tracers" Cancers 13, no. 19: 4791. https://doi.org/10.3390/cancers13194791
APA StyleRinne, S. S., Leitao, C. D., Abouzayed, A., Vorobyeva, A., Tolmachev, V., Ståhl, S., Löfblom, J., & Orlova, A. (2021). HER3 PET Imaging: 68Ga-Labeled Affibody Molecules Provide Superior HER3 Contrast to 89Zr-Labeled Antibody and Antibody-Fragment-Based Tracers. Cancers, 13(19), 4791. https://doi.org/10.3390/cancers13194791









